E1: Ortho - intro
1/83
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
84 Terms
what are cordlike structures that function to attach muscle to bone?
tendons
tendonitis vs tendonosis
tendonitis = inflammation
tendonosis = degenerative process "chronic" W/O inflammation
what structure connects bone to bone, is densely packed connective tissue that consists largely of directionally oriented, high-tensile strength collagen and contributes to stability of joint function by preventing excessive motion?
ligament
review 6 types of synovial joints
:)
synovial fluid analysis:
clear to pale yellow, transparent
WBC < 200
normal
synovial fluid analysis:
slightly deeper yellow, transparent
WBC < 2000
osteoarthritis
synovial fluid analysis:
dark yellow, cloudy, translucent, blurred
WBC < 80,000
inflammatory
synovial fluid analysis:
purulent, dense, opaque
WBC > 50,000
septic
synovial fluid analysis:
red, opaque
hemarthrosis
what is the normal ROM of the knee?
0-130 degrees
what is extensor lag of the knee?
knee lacks 10 degrees to full extension
- seen w AROM
what is flexion contracture?
maximum extension measurement
- seen in PROM
if the joint is in hyperextension, how is ROM measured?
the degree is preceded by a negative sign
(ex = hyperextension of the elbow is -3 degrees)
manual muscle test grading scale
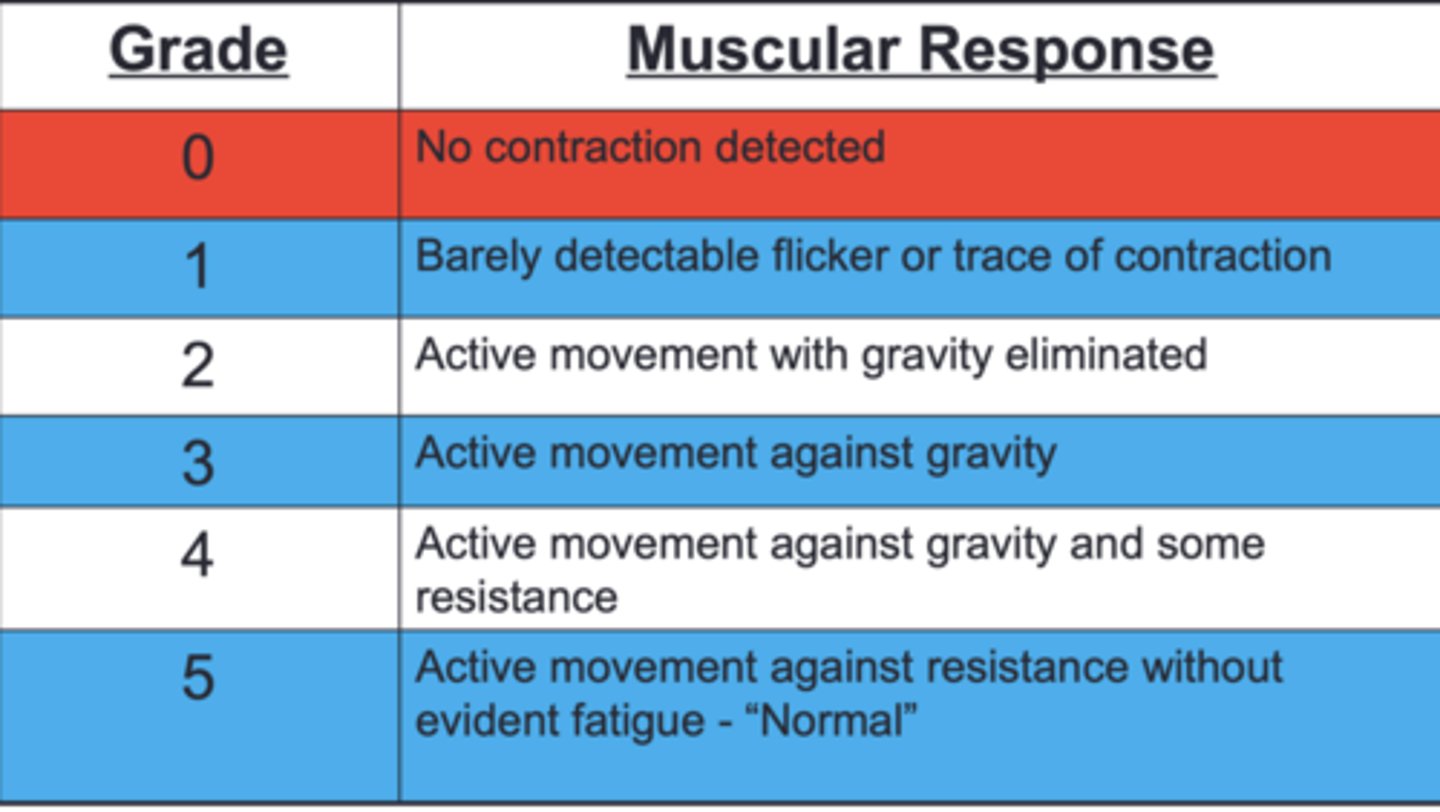
what muscle does the axillary nerve supply, what is the action and what is the area of sensory?
muscle = deltoid
action = shoulder ABduction
sensory = lateral arm
what muscle does the musculotaneous nerve supply, what is the action and what is the area of sensory?
muscle = biceps
action = elbow flexion
sensory = lateral proximal forearm
what muscle does the median nerve supply, what is the action and what is the area of sensory?
muscle = FPL
action = thumb flexion
sensory = tip of thumb, volar aspect
what muscle does the ulnar nerve supply, what is the action and what is the area of sensory?
muscle = first dorsal interosseous
action = ABduction of fingers
sensory = tip of pinky, volar aspect
what muscle does the radial nerve supply, what is the action and what is the area of sensory?
muscle = EPL
action = thumb extension
sensory = dorsum thumb web space
what muscle(s) does the obturator nerve supply, what is the action and what is the area of sensory?
muscle = adductors
action = hip ADDuction
sensory = medial aspect of mid-thigh
what muscle(s) does the femoral nerve supply, what is the action and what is the area of sensory?
muscle = quads
action = knee extensors
sensory = proximal to medial malleolus
what muscle does the perineal- deep branch supply, what is the action and what is the area of sensory?
muscle = EHL
action = great toe extension
sensory = dorm first web space
what muscle does the perineal - superficial branch supply, what is the action and what is the area of sensory?
muscle = peroneus brevis
action = foot eversion
sensory = dorsum of lateral foot
what muscle does the tibial nerve supply, what is the action and what is the area of sensory?
muscle = FHL
action = great toe extension
sensory = plantar aspect of foot
what is considered a "live" x-ray?
fluoroscopy
what is a CT pyelography used for?
evaluates spinal cord or nerve root pathology
what are contraindications to a CT? (we should know this by now)
renal disease
allergy to IV contrast
shellfish allergy
what test provides the MOST detail for evaluating soft tissue?
MRI
is a CT or MRI better for tumor staging?
MRI
(a CT is good to evaluate of you have a tumor but not the best for staging)
what are the major risks of a fluoroscopy?
radiation-induced "burn" and possibility of radiation-induced cancer later in life
commonly used drugs: NSAIDs
blocks prostaglandins via COX1 and COX2
anti-inflam, analgesic, antipyretic
SE = GI ulcers/bleeds; kidney problems
commonly used drugs: COX 2 inhibitors
Celebrex & Meloxicam
- less likely to cause GI ulcers/bleeds
- have ↑ risk of stroke and MI
what diseases are corticosteroid injections used for?
OA, RA, gout, SLE and post traumatic arthritis
- ↓ pain and inflammation
when do you seen effectiveness of a corticosteroid injection?
1-13 wks
what are extra-articular injections used for?
overuse syndromes, athletic injuries, neuropathies, bursitis and tendonitis
what are the most common sites of corticosteroids injections?
subacromial shoulder
lateral epicondylitis
trigger finger
carpal tunnel
what are contraindications of corticosteroid injections?
pyarthrosis
non septic inflam of joint
signs of infection
what are adverse reactions of corticosteroid injections?
joint pain
joint infection
tendon rupture
facial flushing
local skin discoloration
subQ lipodystrophy (fat atrophy)
are narcotics contraindicated in peds fractures?
YES!!!!!!!!!!!
ASA Physical Status Classification System
used to classify the stage of disease and morbidity
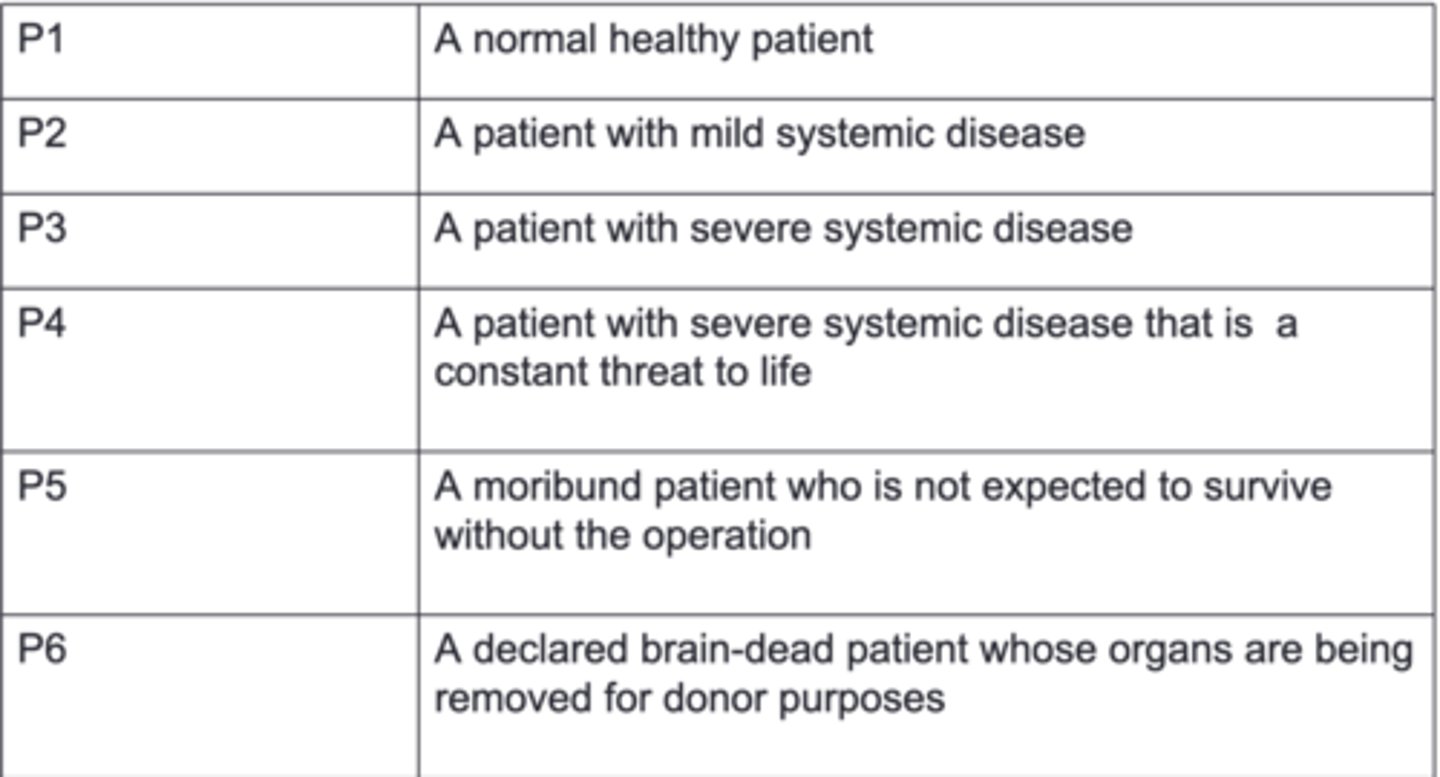
if you do not get consent for a surgery, it is considered __________
battery
what does pre-op consent include?
- warnings/risks of procedure and anesthesia
- planned procedure and alternatives
- permission to perform procedure
- general complications
what are pre-op screening tests?
EKG
stress test (ST changes)
nuclear stress test (ischemia)
dobutamine stress test (mobility of walls w risk of ischemia)
what is general anesthesia used for? what are benefits and risks?
major joint/spine sx
- ↓ need for opiods
- risk of respiratory depression & post sedation
what is epidural & spinal anesthesia used for? what are benefits and risks?
lower extremity sx
- ↓ post sedation in elderly
- risk of epidural hematoma
what are peripheral nerve blocks used for?
UE and LE sx
what is IV regional anesthesia used for?
short procedures of forearm, wrist and hand (aka Bier Block)
which drugs have a risk factor of liver disease and chronic EtOH abuse?
tylenol
acetam/codeine (Tylenol 3)
aceta/hydrocodone (Norco)
acetam/oxy (Percocet)
acetam/tramadol (ultracet)
which drugs have risk factors of GI symptoms?
ASA
ASA/hydrocodone (Lortab ASA)
calcium
ibuprofen
what is a risk factor of enoxaparin?
renal failure
what is a risk factor of fentanyl transdermal?
respiratory depression
head injury
hepatic or renal impairment
what is a risk factor for heparin sodium?
blood dyscrasias
dont give IM
monitor coag hemoccult
what are risks of morphine?
respiratory depression & brain injury
- caution in opioid dependent pts and elderly
what are risks of tramadol?
respiratory depression & brain injury
- caution in opioid dependent pts
what is the drug of choice for pre-op ABX for ortho procedures?
Ancef
what classification system is used to classify open fractures?
Gustilo Classification
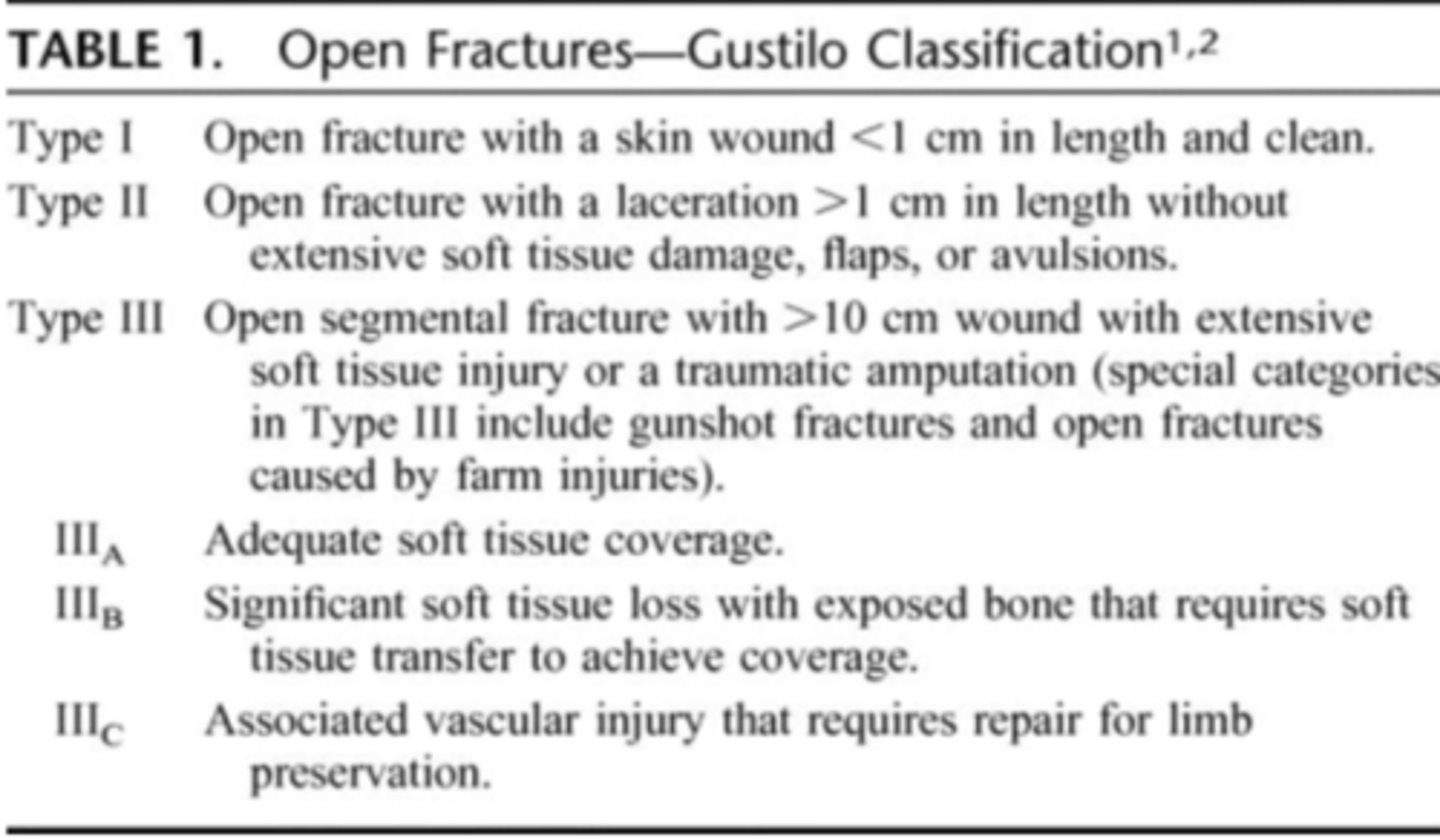

which type of open fracture:
skin wound < 1 cm in length and clean
type 1
does a type 1 open fracture require surgery?
no
which type of open fracture:
laceration > 1 cm in length w/o extensive soft tissue damage, flaps or avulsions
type 2
which type of open fracture:
open segmental fracture w > 10 m wound w extensive soft tissue injury or traumatic amputation
type 3
surgeon uses a pencil-sized, flexible, fiberoptic instrument to make 2-3 small incisions to remove bone spurs, cysts, damaged lining or loose fragments in the joint
arthroscopy
the long bones of the arm or leg are realigned to take pressure off the joint
osteotomy
procedure where a surgeon eliminates the joint by fastening together the ends of the bone via pins, plates, screws or rods
- eliminate the joint's flexibility
joint fusion
procedure where a surgeon removes parts of the bone and creates an artificial joint w metal or plastic components
joint replacement
procedure where a surgeon reduces the fracture and reinforces it with instrumentation INSIDE the pt via plates, screws or rods
open reduction internal fixation (ORIF)
procedure where a surgeon reduces the fracture and applies instrumentation through the skin and reinforced w a metal frame
- utilized when a cast doesnt allow for proper alignment
open reduction external fixation
procedure where a surgeon manipulates. pt's joint under anesthesia
- common for "frozen shoulders", TKA and TSA
manipulation under anesthesia (MUA)
what are post-op complications?
DVT
Pulm elmbolism
fever
compartment syndrome
foot drop
excessive drainage
chest pain
hypo/HTN
dyspnea
renal oliguria or anuria
virchow's triad for DVT
stasis
hypercoagulability
endothelial injury
what criteria is used to diagnose a DVT?
Well's criteria

diagnostic test for DVT
duplex US or venogram
treatment for DVT
levonox
what are internal causes of compartment syndrome?
bleeding or tissue edema into facial compartments
what is an external cause of compartment syndrome?
cast is too tight
what are the 5 P's of compartment syndrome?
pain out of proportion
pallor
paresthesias
poikiothermia
paralysis
pulseless
what is the treatment for compartment syndrome?
remove tight dressing
if > 30 mmHg = fasciotomy
which type of contraction produces a muscle contraction w/o moving the joint angle; length of the muscle does NOT change?
isometric contraction
which type of contraction has manual or mechanical resistance applied as the muscle moves through the ROM, the length of the muscle DOES change. May be concentric(shortens) or eccentric (lengthens)
isotonic contraction
which type of contraction does the muscle shorten and contract, occurring at a constant rate of speed?
isokinetic contraction
open chain vs closed chain exercises
open = distal segment is free, contraction is mainly concentric
closed = distal segment is not free, movements are functional
absolute contraindications to exercise
recent MI
ischemic EKG changes
UA
uncontrolled arrythmia
3rd deg AV block
acute CHF
type of walkers
platform = pts w UE fxs
hemiwalker = stroke pts
rolling walker = Parkinson's pts
types of crutches
platform = fxs
Lofstrand (forearm) = long-term disabilities
axillary = temporary diasbilities
which limb should a cane be used on?
opposite side of injured limb (it reduces stress)