Chapter 25 - Digestive System
1/47
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
48 Terms
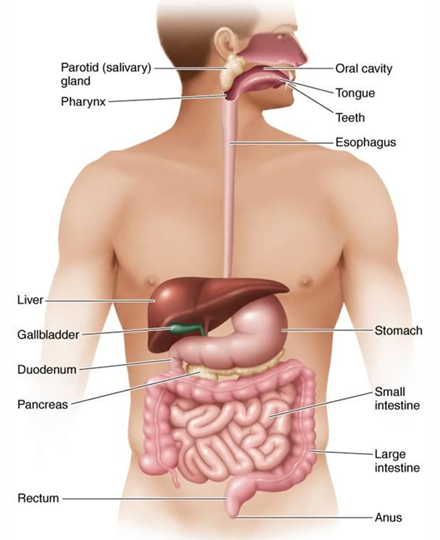
GI Tract or Alimentary Canal
Mouth
Pharynx (throat)
Esophagus
Stomach
Small and large intestine
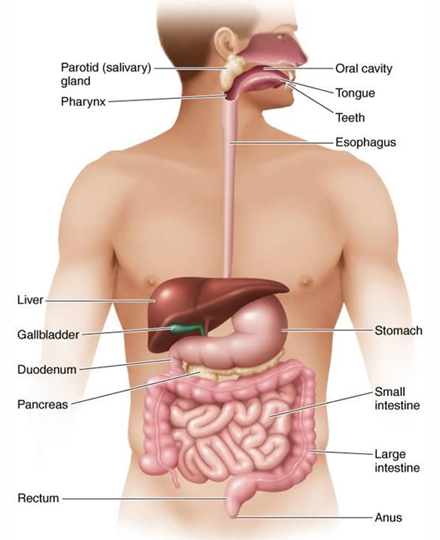
Accessory Structures of the GI Tract
Teeth and tongue
Salivary glands
Liver
Gallbladder
Pancreas
What is the structure and function of the digestive system?
Absorption of foods
25 tons of food pass through the GI tract in a lifetime
70% of the immune system is located in the intestinal tract
Gut-associated lymphoid tissue (GALT)
Lymph nodes
Peyer’s patches
Normal Microbiota of the Digestive System
Millions of bacteria per mL of saliva
Few microorganisms in the stomach
Due to HCl production
Small intestine
Paneth cells
Granule-filled phagocytic cells; produce defensins
Large numbers of bacteria in the large intestine
Anaerobes and facultative anaerobes
100 billion bacteria per gram of feces
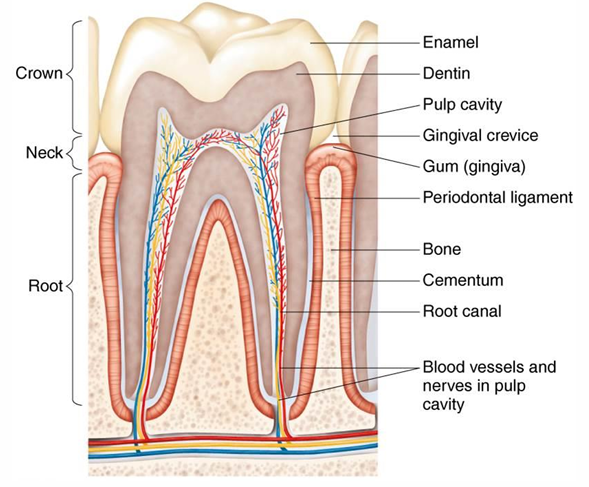
A Healthy Human Tooth: 3 Main Aspects
Root, neck, and crown
Dental Plaque
Biofilms involved in the formation of dental caries
Dental Caries (Tooth Decay)
Pathogen → Primarily streptococcus mutans
Symptoms → Discoloration or hole in tooth enamel
Treatment → Removal of decayed area
Prevention → Brushing, flossing, reducing dietary sucrose
*Decay can reach pulp, which contains the blood supply and nerve cells, which may advance to the soft tissues and lead to abscesses
Periodontal Disease
Pathogen → Various, primarily Porphyromonas spp.
Symptoms → Bleeding gums, pus pockets
Treatment → Removal of damaged area; antibiotics
Prevention → Plaque removal
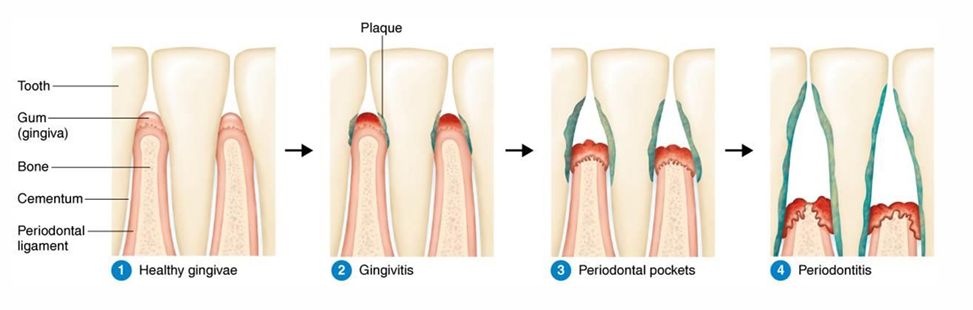
The Stages of Periodontal Disease
Healthy gingivae
Gingivitis → Inflammation and infection of the gums
Periodontal pockets → Bone and tissue supporting the teeth are destroyed
Periodontitis
Acute Necrotizing Ulcerative Gingivitis (trench mouth)
Pathogen → Prevotella intermedia
Symptoms → Pain with chewing, halitosis (bad breath)
Treatment → Removal of damaged area; antibiotics
Prevention → Brushing & flossing
Staphylococcal Food Poisoning
Pathogen → Staphylococcus aureus
Symptoms → Nausea, vomiting, and diarrhea
Intox/Infec → Intoxication (enterotoxin)
Diagnostic Test → Phage Typing
Treatment → None
*Toxin produced when the organism is allowed to incubate in food (temp abuse)
*S. aureus outgrows most bacteria in high osmotic pressure & high temp
Shigellosis (bacterial dysentary)
Pathogen → Shigella spp.
Symptoms → Tissue damage and dysentery (blood in feces)
Intox/Infec → Infection (endotoxin and Shiga toxin, exotoxin)
Diagnostic test → Isolation of bacteria on selective media
Treatment → Usually none needed
*Oral rehydration
*Membrane ruffle
Salmonellosis
Pathogen → Salmonella enterica
Symptoms → Nausea and diarrhea
Intox/Infec → Infection (endotoxin)
Diagnostic test → Isolation of bacteria on selective media, serotyping
Treatment → Oral rehydration
*Replicates in macrophages
*Incubation of 12-36 hours
*Membrane ruffle → Lymph node → Bloodstream
Typhoid Fever
Pathogen → Salmonella Typhi
Symptoms → High fever, significant mortality
Intox/Infec → Infection (endotoxin)
Diagnostic Test →Isolation of bacteria on selective media, serotyping
Treatment → Requires antibiotic-susceptibility testing
Preventative → Vaccine
*Spread through phagocytes
*1-3% of patients become chronic carriers and harbor organism in the gallbladder
Cholera
Pathogen → Vibrio cholerae; O:1 and O:139
Symptoms → Diarrhea with large water loss
Intox/Infec → Infection (exotoxin)
Diagnostic Test → Isolation of bacteria on selective media
Treatment → Rehydration; doxycycline
*Associated with salty waters
*Causes “rice water stools”
*Increases when sanitization and sewage disposal systems are compromised
Vibrio parahaemolyticus Gastroenteritis
Pathogen → V. parahaemolyticus
Symptoms → Cholera-like diarrhea, but generally milder
Intox/Infec → Infection (enterotoxin)
Diagnostic Test → Isolation of bacteria on 2-4% NaCl
Treatment → Rehydration
*Saltwater
*Raw oysters and crustaceans
Escherichia coli Gastroenteritis
Pathogen → EPEC, EIEC, EAEC, ETEC
Symptoms → Watery diarrhea
Intox/Infec → Infection (exotoxins)
Diagnostic Test → Isolation on selective media, DNA fingerprinting
Treatment → Oral rehydration
*Reservoir = cattle
*Causes the host cells to form pedestals where bacteria attach
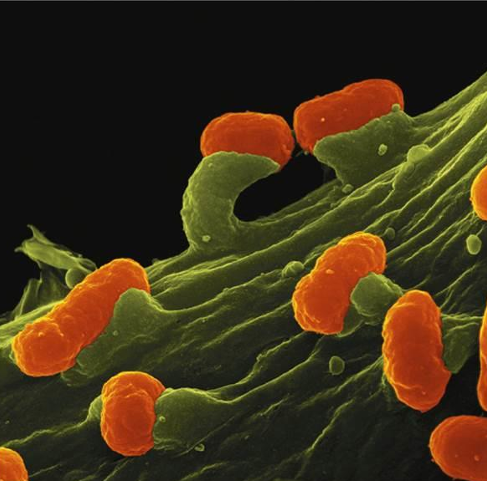
Shiga Toxin-Producing Enterohemorrhagic E. Coli
Pathogen → E. coli O157:H7
Symptoms → Shigella-like dysentery; hemorrhagic colitis, HUS
Intox/Infec → Infection, Shiga toxin (exotoxin)
Diagnostic → Isolation, sorbitol fermentation test, DNA fingerprinting
Treatment → Intravenous rehydration, serum electrolyte monitoring
Campylobacter Gasteroenteritis
Pathogen → Campylobacter jejuni
Symptoms → Fever, abdominal pain, diarrhea
Intox/Infec → Infection
Diagnostic Test → Isolation in low O2, high CO2
Treatment → Azithromycin
*Leading cause of foodborne illness in the US → intestines of poultry
Helicobacter Peptic Ulcer Disease
Pathogen → Helicobacter pylori
Symptoms → Peptic ulcers
Intox/Infec → Infection
Diagnostic Test → Ultra breath test, bacterial culture
Treatment → Antibiotics
*Leads to ulceration of the Stomach wall
Yersinia Gastroenteritis
Pathogen → Yersinia enterocolitica
Symptoms → Abdominal pain and diarrhea, usually mild; may be confused with appendicitis
Intox/Infec → Inection (endotoxin)
Diagnostic Test → Culture, biochemical or molecular tests
Treatment → Oral rehydration
*Transmitted by uncooked meat and pork
*Grows at 4 degrees celcius
Clostridium perfringens Gastroenteritis
Pathogen → Clostridium perfringens
Symptoms → Usually limited to diarrhea
Intox/Infec → Infection (exotoxin)
Diagnostic Test → Isolation of 10^6 endospores/g feces
Treatment → Oral rehydration
*Obligately anaerobic rod, causes gas gangrene
*Symptoms 8-10 hours after ingestion
C. difficile-Associated Diarrhea
Pathogen → Clostridium difficile
Symptoms → Mild diarrhea to colitis; 1-2.5% mortality
Intox/Infec → Infection (exotoxin)
Diagnostic Test → Cytotoxin assay
Treatment → Vancomycin, fidaxomicin
Bacillus cereus Gastroenteritis
Pathogen → B. cereus
Symptoms → May take form of diarrhea, nausea, vomiting
Intox/Infec → Intoxication
Diagnostic Test → Isolation of > 10^5 B. cereus/g food
Treatment → None
*Spores survive heating
*Common in soil and vegetation
Hepatitis A
Pathogen → Hepatitis A virus, Piornaviridae
Symptoms → Mostly subclinical; fever, headache; malaise, jaundice in severe cases; no chronic disease
Incubation Period → 2-6 weeks
Transmission → Ingestion
Diagnostic Test → IgM antibodies
Treatment → Immunoglobulin
Vaccine → Inactivated virus; postexposure = immune globulin
*Entry via the oral-fecal route
*Multiplies in the epithelial lining of the intestinal tract → liver, kidneys, and spleen
Hepatitis B
Pathogen → Hepatitis B virus, Hepadnaviridae
Symptoms → Frequently subclinical; similar to HAV, but no headache; more likely to progress to severe liver damage; chronic disease occurs
Incubation period → 4-26 weeks
Transmission → Parenteral; sexual contact; blood and bodily fluids
Diagnostic Test → IgM antibodies
Treatment → Interferon and nucleoside analogues
Vaccine → Genetically modified vaccine produced in yeast
*dsDNA; resembles retrovirus
*The spherical and filamentous particles are unassembled components of the virion without nucleic acids
Incubation period
How long it takes for you to develop symptoms after exposure to an infectious disease
Food intoxication
Consuming toxins already present in food
Symptoms appear quickly - after a few hours
Antibiotics are NOT helpful, because it’s caused by the toxins produced, not the bacteria itself
Food infection
Caused by microorganisms that have to grow and multiply in the body
Symptoms appear after a longer period of time
Hepatitis C
Pathogen → Hepatitis C virus, Flaviviridae
Symptoms → Similar to HBV, more likely to become chronic
Incubation Period → 2-22 weeks
Transmission → Parenteral, often transfusion-transmitted
Diagnostic Test → PCR for viral RNA
Treatment → Enzyme inhibitors, interferon, and ribavirin
Vaccine → None
*Kills more in the U.S. than AIDS
Hepatitis D
Pathogen → Hepatitis D virus, Deltaviridae
Symptoms → Severe liver damage; high mortality rate; chronic disease may occur
Incubation Period → 6-26 weeks
Transmission → Parenteral; requires coinfection with Hep B
Diagnostic test → antibodies with PCR for viral RNA
Treatment → None
Vaccine → HBV vaccine is proactive
*Acute = coinfection; chronic = superinfectionH
Hepatitis E
Pathogen → Hepatitis E virus, Caliciviridae
Symptoms → Similar to HAV, but pregnant women have high mortality; no chronic disease
Incubation period → 2-6 weeks
Transmission → Ingestion
Diagnostic test → Antibodies against HEV or HEV RNA
Treatment → None
Vaccine → None
*Spread by fecal-oral transmission
Mumps
Pathogen → Mumps virus, Paramyxoviridae
Symptoms → Painful swelling of parotoid glands
Incubation period → 16-18 days
Diagnostic Test → Symptoms; virus culture
Prevention → Attenuated vaccine (MMR vaccine)
*Transmitted in the saliva and respiratory secretions
*May cause orchitis (swelling of testes), meningitis, ovary inflammation, and pancreatitis

Viral Gastroenteritis (rota)
Pathogen → Rotavirus
Symptoms → Vomiting, diarrhea for 1 week
Incubation period → 1-3 days
Diagnostic test → enzyme immunoassay for viral antigens in feces
Prevention → Attenuated vaccine
Viral Gastroenteritis (nora)
Pathogen → Norovirus
Symptoms → vomiting, diarrhea for 2-3 days
Incubation period → 18-48 hours
Diagnostic test → PCR
Prevention → Handwashing
Ergot Poisoning (fungal)
Pathogen → Claviceps purpurea
Symptoms → Restricted blood flow to limbs (gangrene); hallucinogenic
Reservoir → Mycotoxin produced by fungus growing on grains
Diagnostic Test → Finding fungal sclerotia in food
Treatment → None
Aflatoxin Poisoning (fungal)
Pathogen → Aspergillus flavus
Symptoms → Liver cirrhosis; liver cancer
Reservoir → Mycotoxin produced by fungus growing on food
Diagnostic Test → Immunoassay for toxin in food
Treatment → None
*Likely found on peanuts
Giardiasis (protozoan)
Pathogen → Giardia intestinalis
Symptoms → Protozoan adheres to intestinal wall, may inhibit nutritional absorption; diarrhea
Reservoir → Water; mammals
Diagnostic Test → FA
Treatment → Metronidazole; nitazoxanide
Cryptosporidiosis (protozoan)
Pathogen → Cryptosporidium hominis, C. parvum
Symptoms → Self-limiting diarrhea; may be life-threatening in immunosuppressed patients
Reservoir → Cattle; water
Diagnostic Test → Acid-fast stain
Treatment → Nitazoxanide
*Transmitted through drinking water
Cyclosporiasis
Pathogen → Cyclospora cayetanensis
Symptoms → Water diarrhea
Reservoir → Humans; birds; usually ingested with fruits and vegetables
Diagnostic test → acid-fast stain
Treatment → Trimethoprim and sulfamethoxazole
*Oocysts are ingested from drinking feces-contaminated water
Amebic Dysentery (amebiasis)
Pathogen → Entamoeba histolytica
Symptoms → Ameba lyses epithelial cells of intestine, caused abscesses; significant mortality rate
Reservoir → Humans
Diagnostic test → Microscopy; EIA
Treatment → Metronidazole
*Feces contain blood and mucus
Tapeworms (helminthic)
Pathogen → Taenia saginata (beef), T. solium (pork), Diphyllobothrium latum (fish)
Symptoms → Adults cause few symptoms; pork tapeworm larvae may encyst in many organs (neurocysticercosis) and cause damage
Reservoir → Intermediate host: cattle, pigs, fish
Definitive host: humans
Diagnostic test → Microscopic exam of feces
Treatment → Praziquantel; niclosamide
*Taeniasis: adult tapeworm infects the intestine; Cysticercosis: infection with the larval stage by ingesting eggs; Ophthalmic cysticercosis: larvae lodge in the eye; Neurocysticercosis: larvae develop in the central nervous system
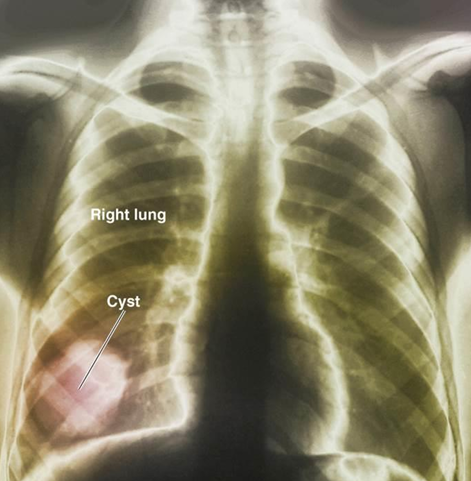
Hydatid Disease (helminthic)
Pathogen → Echinococcus granulosus
Symptoms → Larvae form in body; may be very large and cause damage
Reservoir → Intermediate host: sheep, humans
Definitive host: dogs
Diagnostic test → Serology; X-ray exam
Treatment → Surgical removal; albendazole
*Develops a hydatid cyst that can grow and hold up to 15 liters of fluid; May rupture, causing anaphylactic shock
Pinworms (helminthic)
Pathogen → Enterobius vermicularis (tiny nematode)
Symptoms → Itching around anus (eggs laid around anus)
Intermediate & definitive hosts → humans
Diagnostic test → microscopic exam
Treatment → Pyrantel pamoate
Hookworms (helminthic)
Pathogen → Necator americanus, Ancylostoma duodenale
Symptoms → Large infections may result in anemia
Reservoir → Larvae enter skin from soil; definitive hosts: humans
Diagnostic test → Microscopic exam
Treatment → Mebendazole
*Attaches to the intestinal wall and feeds on blood and tissue
Ascariasis (helminthic)
Pathogen → Ascaris lumbriocoides
Symptoms → Helminths live off undigested intestinal contents, causing few symptoms
Intermediate & definitive hosts → humans
Diagnostic test → microscopic exam
Treatment → Mebendazole
*Thirty percent of the worldwide population is infected
*Larvae develop into adult worms in the intestinal tract and emerge from the anus, mouth, or nose
Whipworm (helminthic)
Pathogen → Trichuris trichiura
Symptoms → Diarrhea, malnutrition
Intermediate & definitive hosts → Humans
Diagnostic test → Microscopic exam of feces
Treatment → Albendazole, mebendazole
*Eggs are ingested and enter the intestinal glands.
*Feeds on cell contents and blood
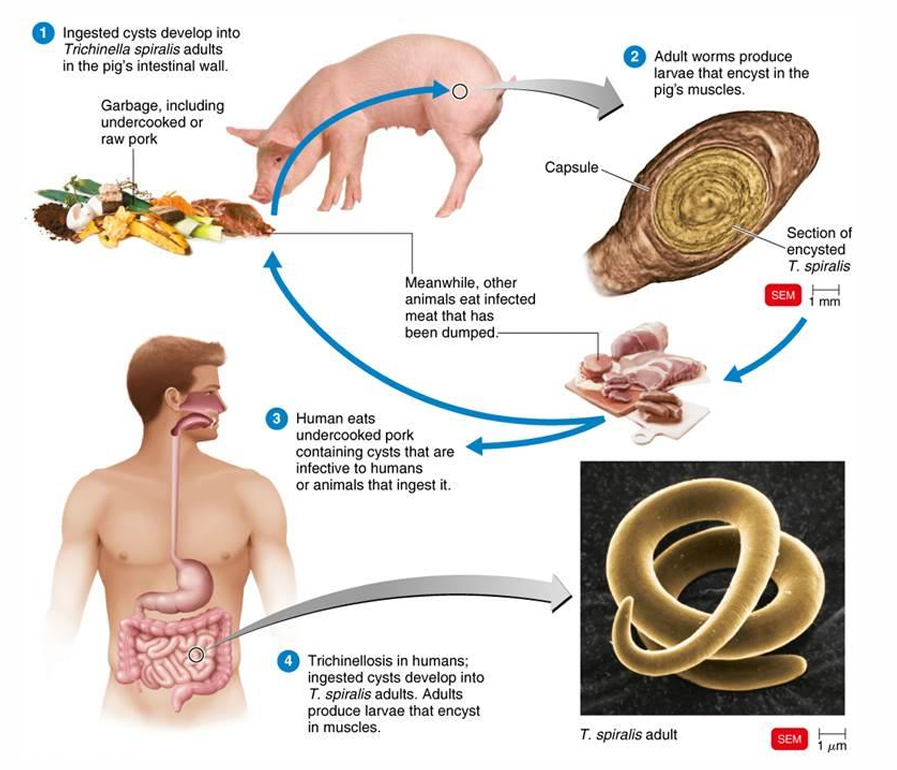
Trichinellosis (helminthic)
Pathogen → Trichinella spiralis, T. nativa
Symptoms → Larvae encyst in striated muscle; usually few symptoms, but large infections may be fatal (Fever, eye swelling, gastrointestinal upset)
Intermediate & definitive hosts → mammals\
Diagnostic test → Biopsy; ELISA
Treatment → Mebendazole; corticosteroids