metabolic and rheumatic disorders - lecture 32
1/42
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
43 Terms
An older patient comes into the clinic with joint stiffness, a limited range of motion in the joints and pain especially in the knees when they try to sit or stand.
Their job (school custodian) requires walking and lifting during the majority of the day and this has been difficult for them to carry out.
They are concerned they will not be able to continue working and are asking you for advice on how to fix the problem.
What do you tell them?
lifestyle modifications
exercise recommendations
medications (pain management)
physical therapy
ice
Most prevalent degenerative joint disease
Osteoarthritis
Osteoarthritis
the leading cause of physical disability in US
- 528 million people (worldwide)
- No treatments to reverse osteoarthritis
- Patients are on long-term palliative care
- Contributes to rising healthcare costs
- Contributes to loss of workforce

osteoarthritis (OA)
Loss of cartilage in synovial joints
Damaged joint cartilage tries to heal itself
-- Creating osteophytes or spurs
-- Cartilage contains more water, less collagen
-- Cartilage becomes weak, rough, eroded
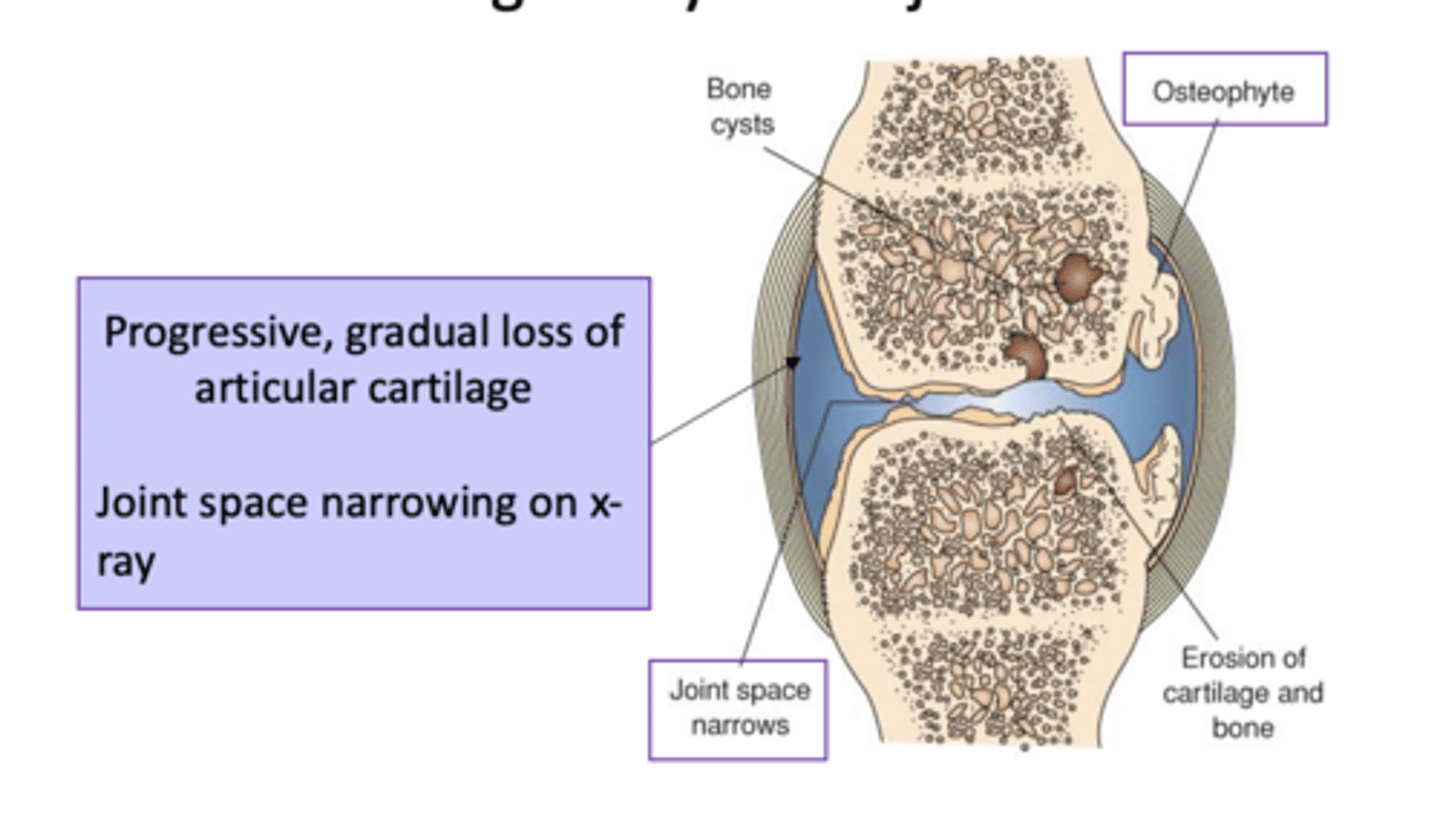
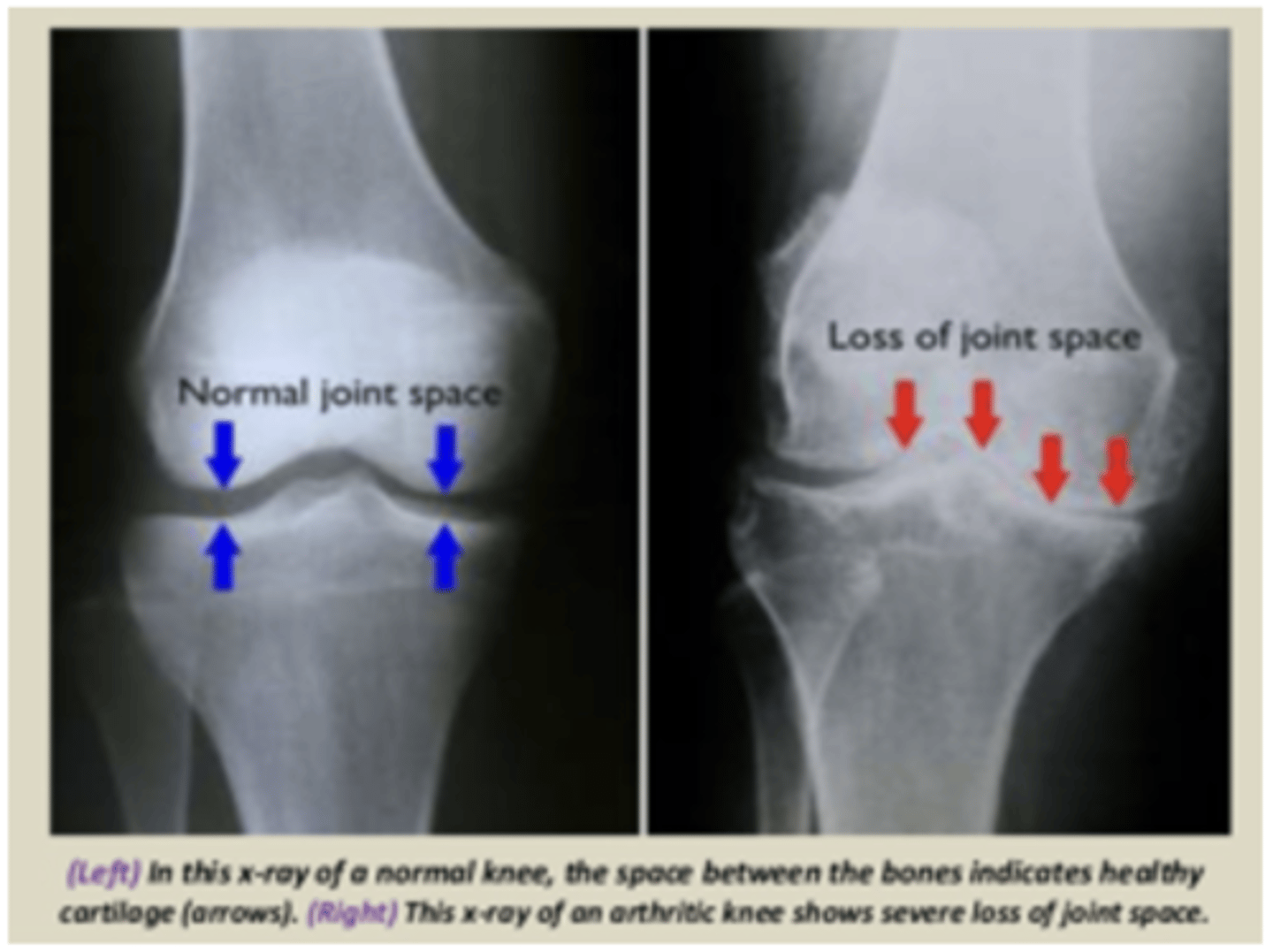
Osteoarthritis (OA)

Healthy cartilage (knee)
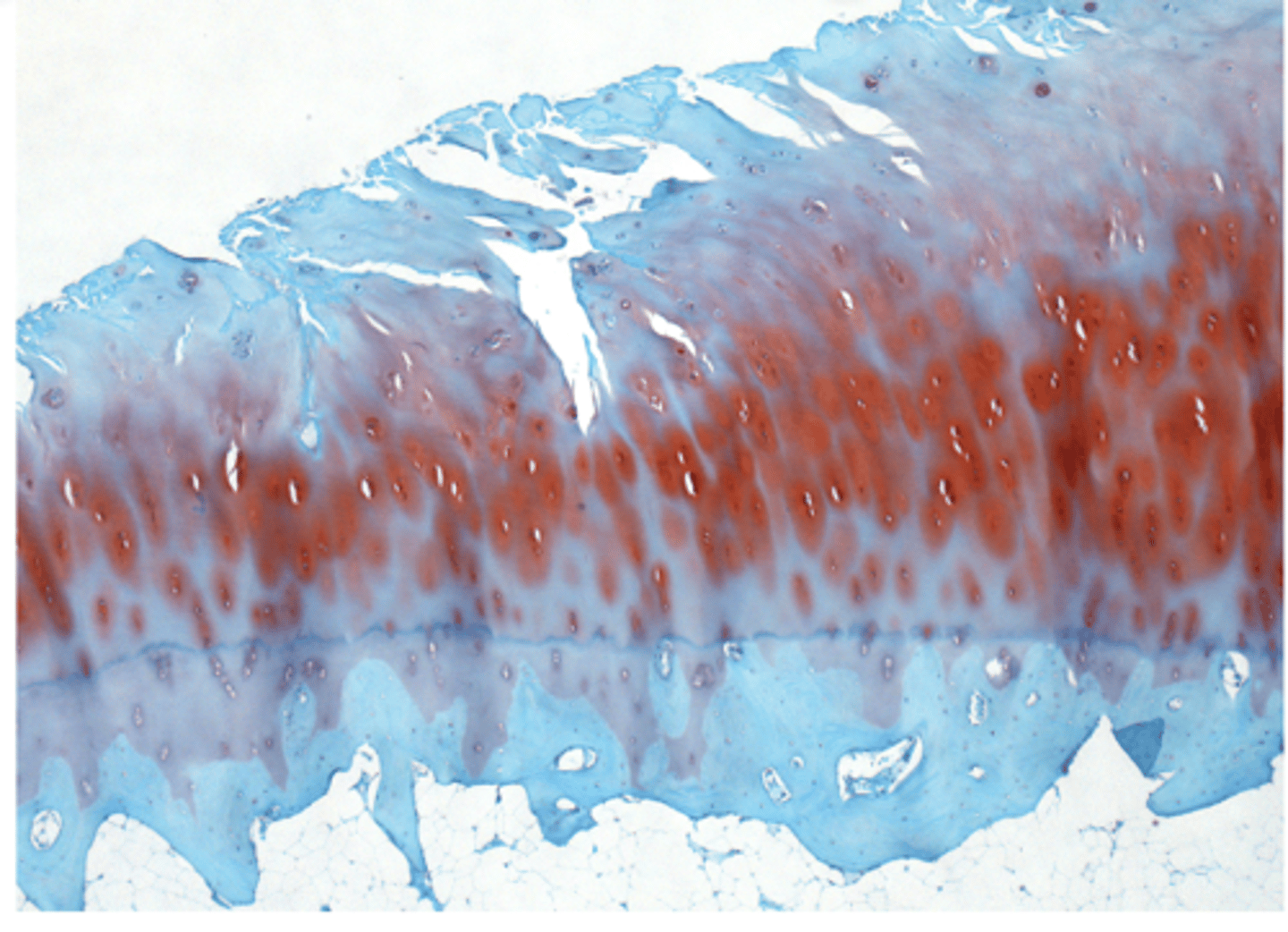
Osteoarthritic cartilage (knee)
pathogenesis of osteoarthritis
Symptoms:
- Joint pain, stiffness, instability
- Limited movement
- Deformity
Risk factors:
-Obesity
- Injury when young
- Advanced Age
- Sex (male younger, female older)
Treatment
(symptom management):
- Joint protection (exercise, rest, weight management)
- Acetominophen or NSAIDs
- Corticosteroid injections
- Total joint replacement (severe cases)
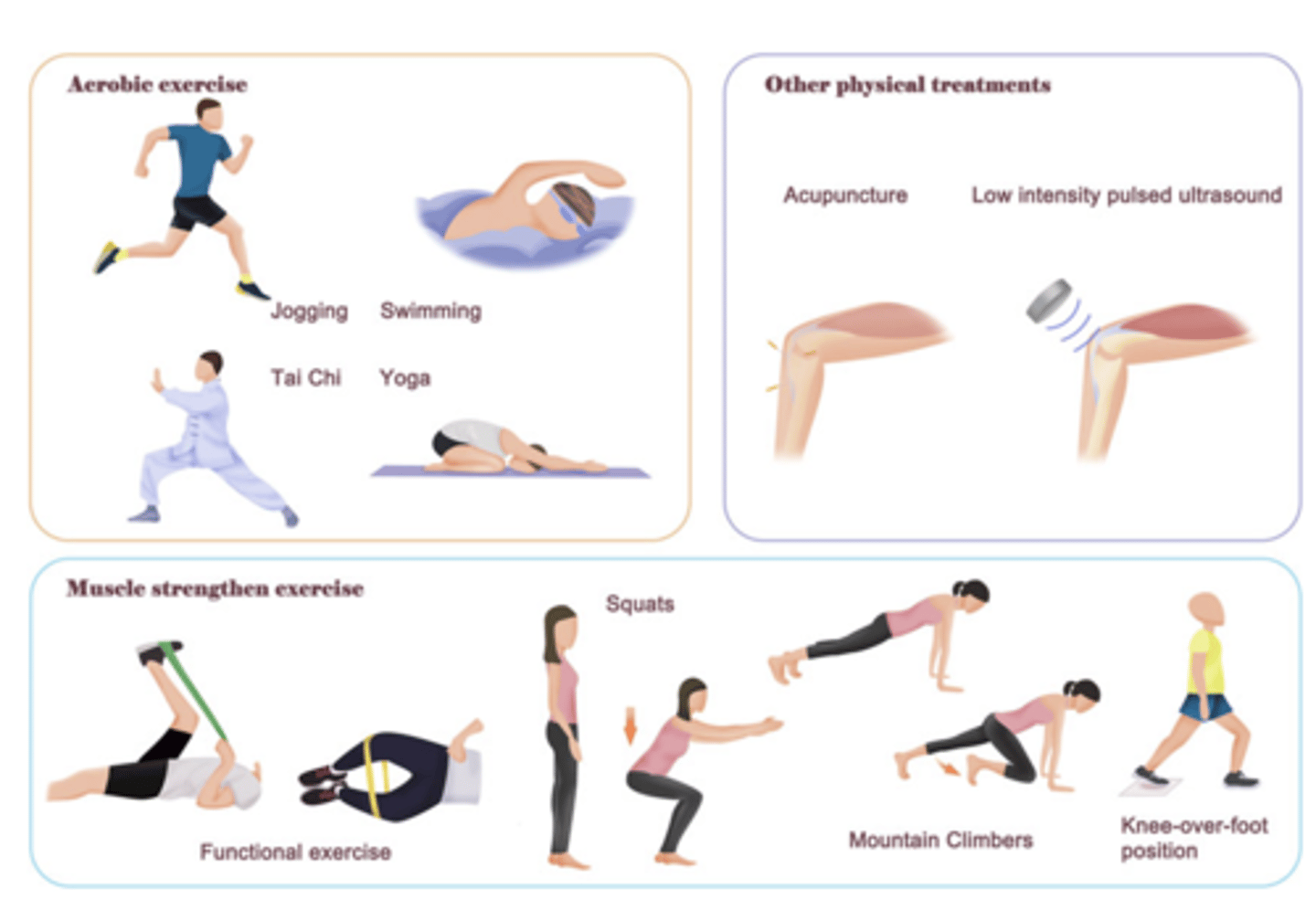
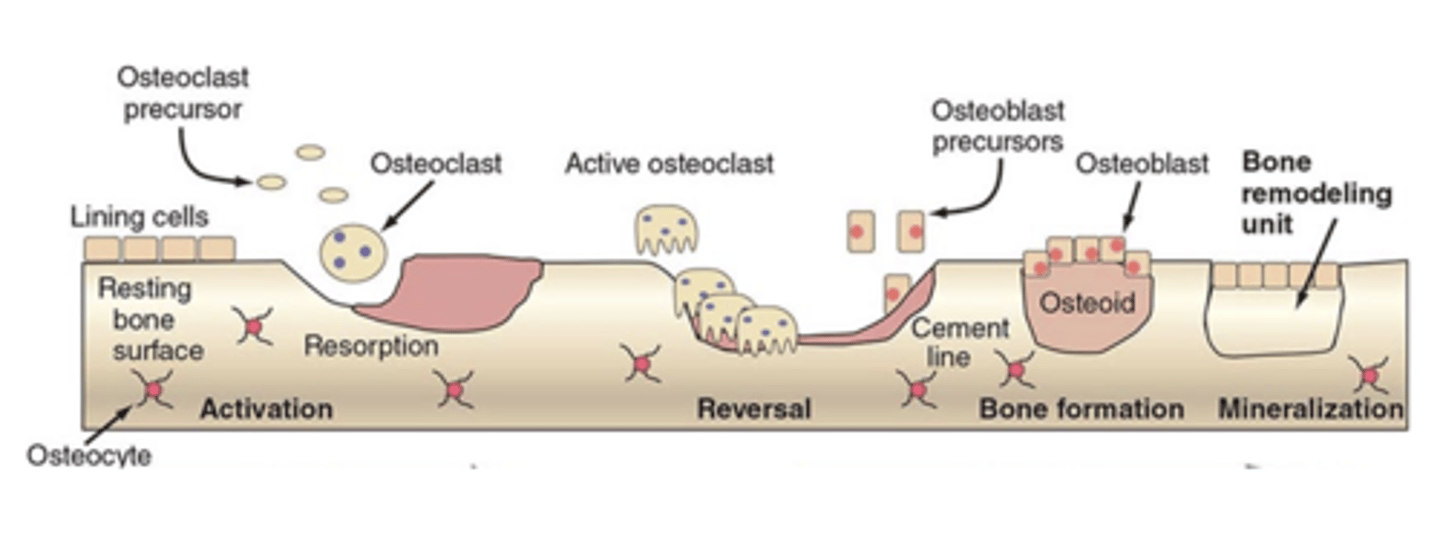
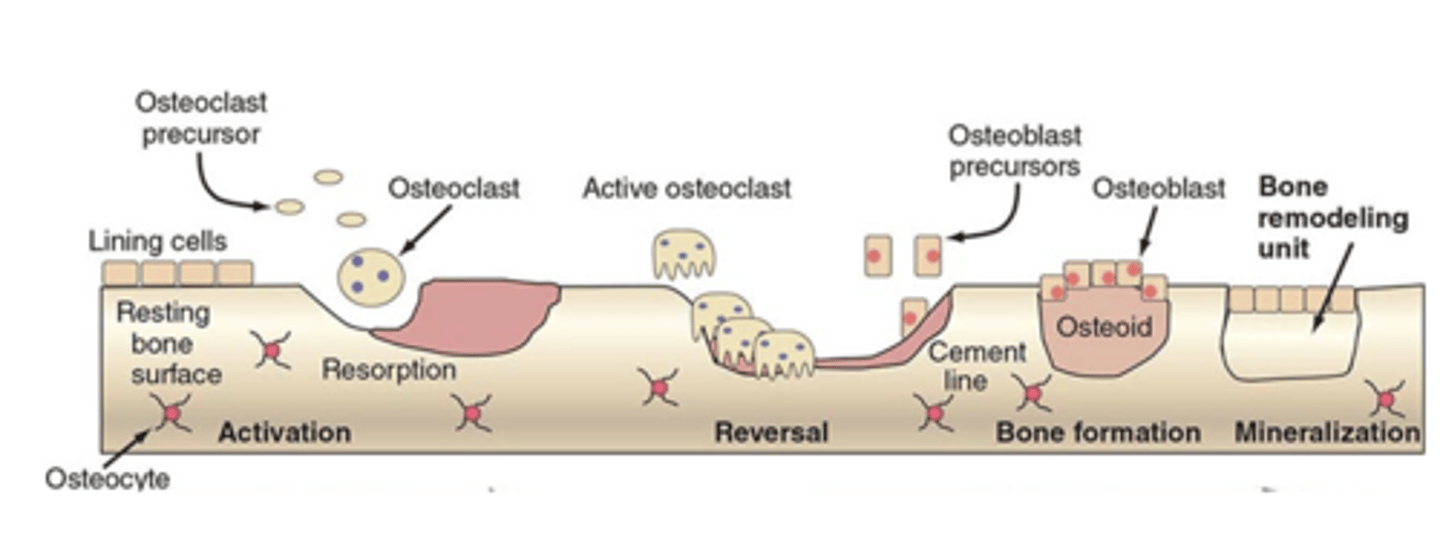
metabolic bone disease
Disorders of bone metabolism (bone remodeling) result in structural changes to the skeleton. These changes include decreased bone mass and diminished bone strength.
A younger patient comes into the clinic who wants to be able to keep their highly active construction job for the next 50 years
Their father had osteoarthritis at a young age and they are asking for help to prevent muscle, bone and joint problems.
What do you tell them?
lifestyle adjustments
exercise
healthy habits
protective measures
encouragement
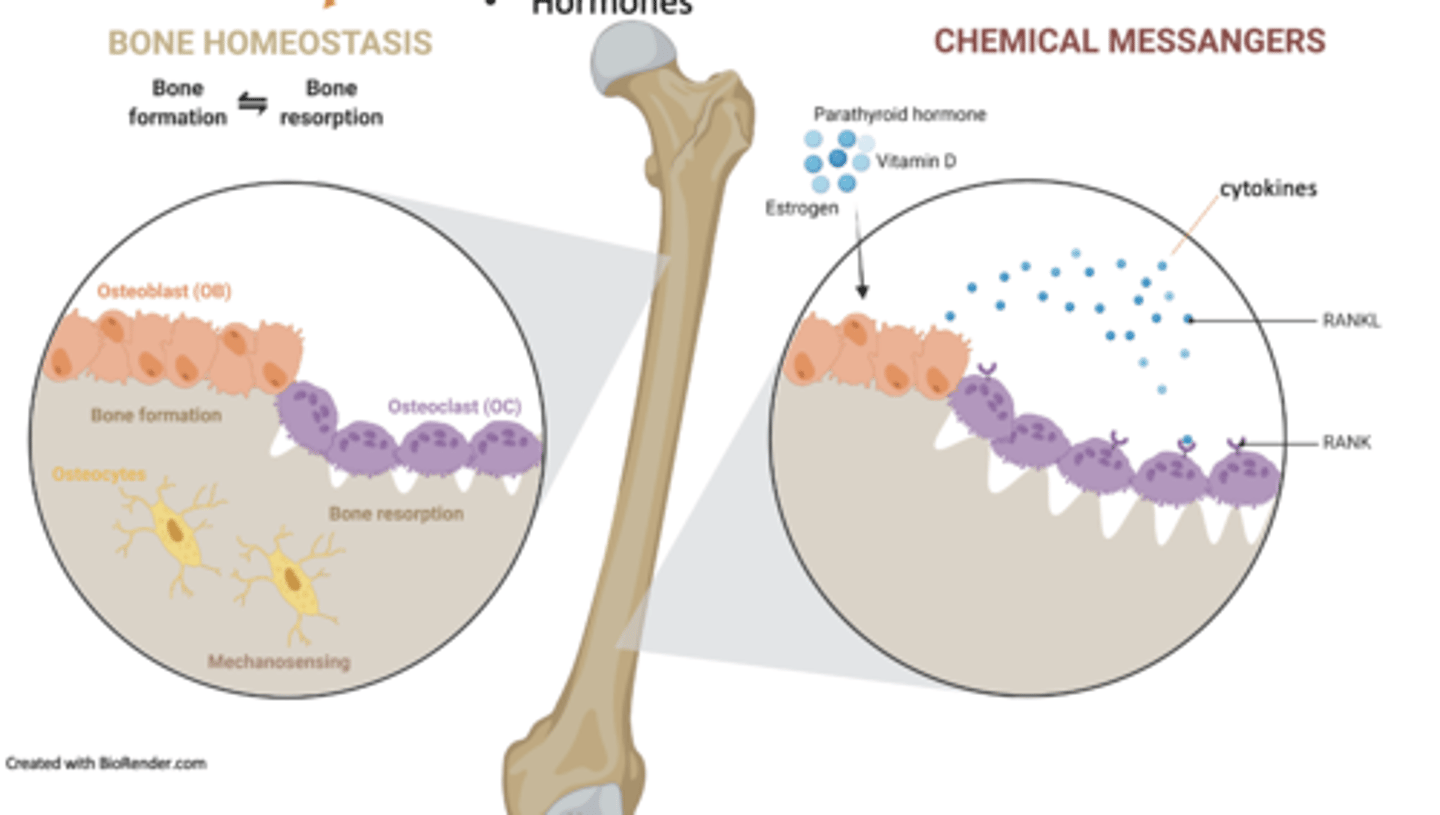
what are the Major influences on bone homeostasis
Mechanical stress
Calcium and phosphate levels
Cytokines
Hormones
what are the 4 types of metabolic bone disease
Osteopenia
Osteoporosis
Osteomalacia
Paget's disease
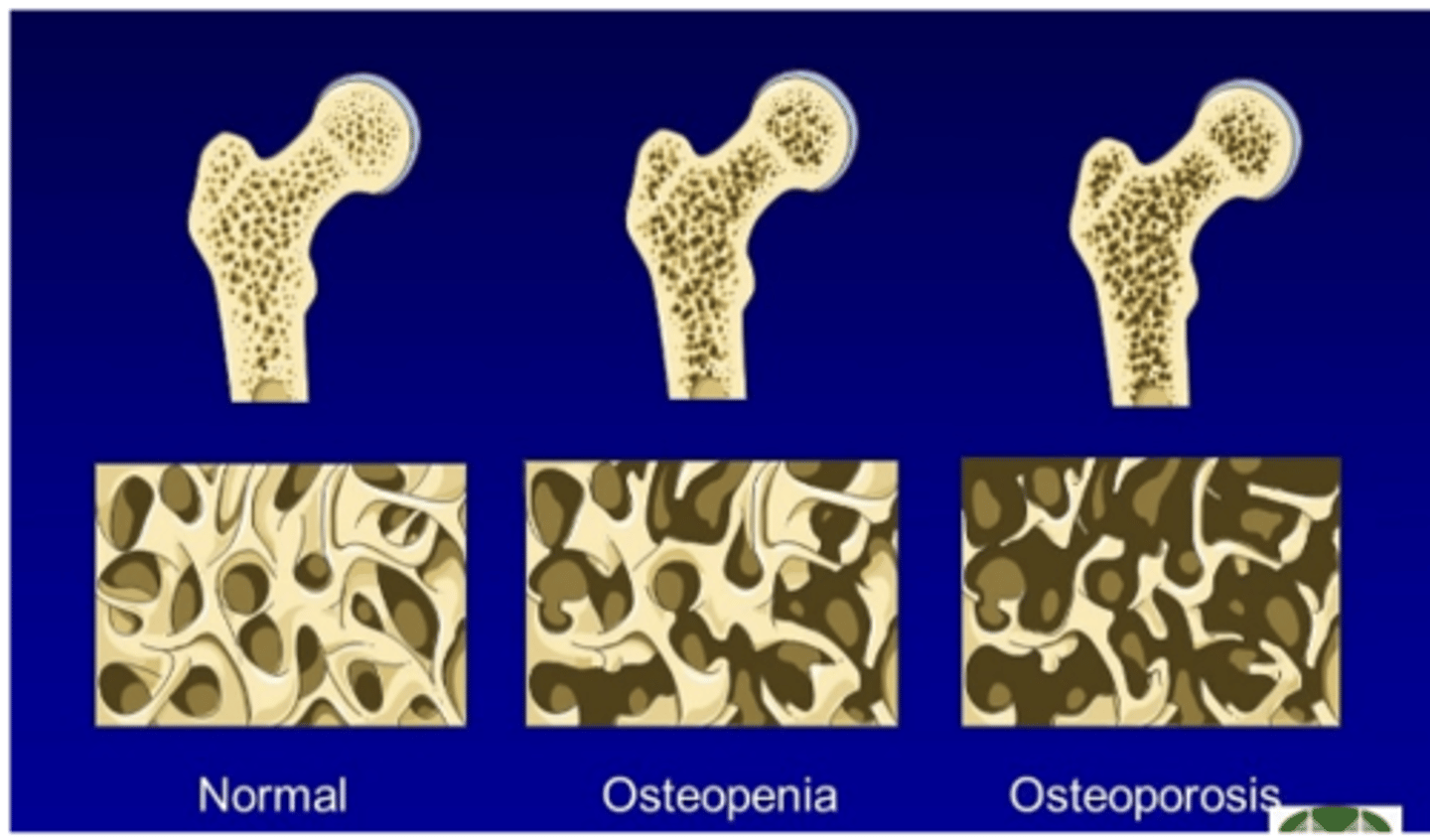
osteopenia
Reduction in bone mass
-- Term used to describe lack of bone mass on x-ray (not a diagnosis)
-- Measured as Bone Mineral Density >1 standard deviation below young adult reference population
Causes:
-- Decrease in bone formation
-- Inadequate bone mineralization
-- Excessive bone resorption
______________ is present in:
-- Osteoporosis
-- Osteomalacia
-- Malignancies such as multiple myeloma
-- Endocrine disorders such as hyperparathyroidism and hyperthyroidism
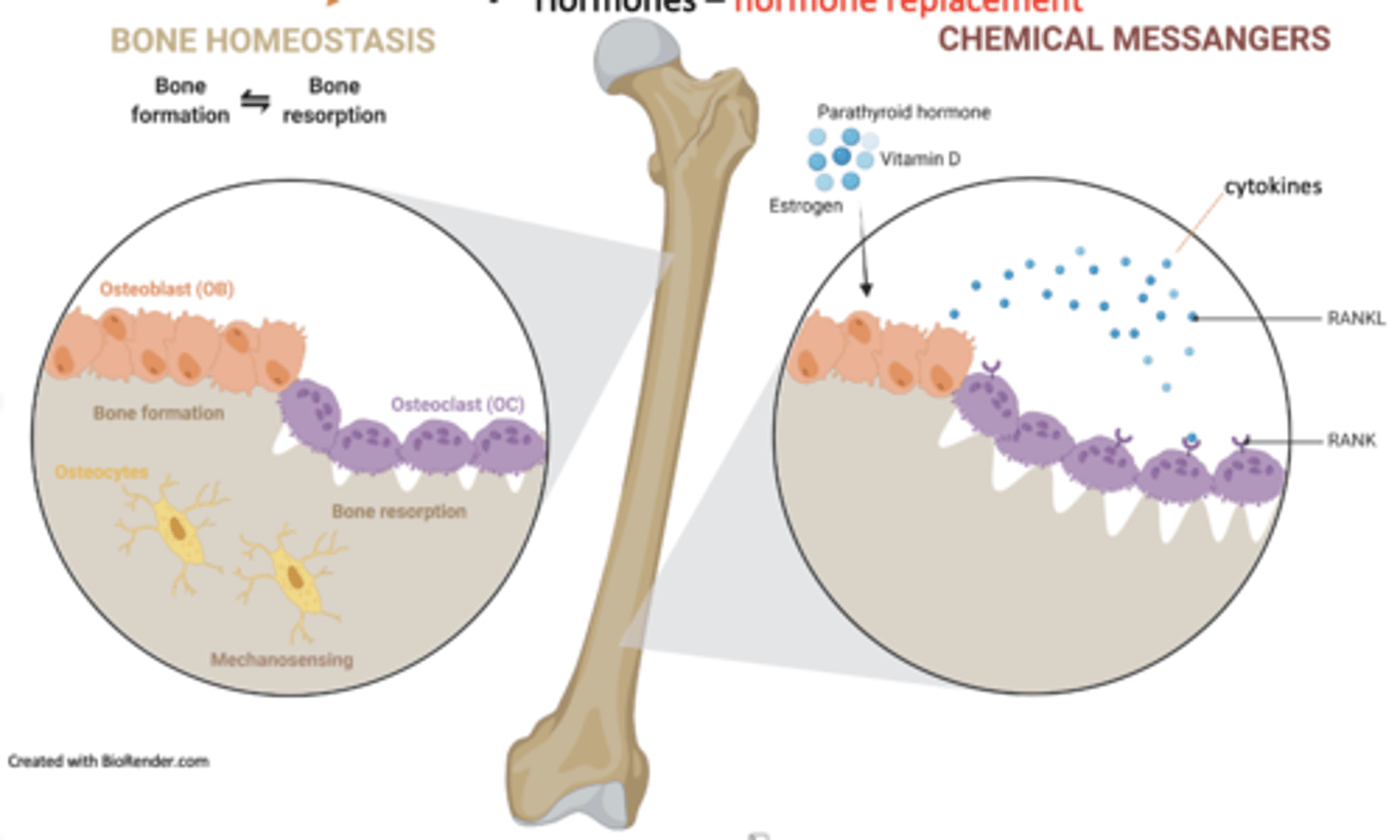
what are the Major influences on bone homeostasis
Mechanical stress -Exercise
Calcium and phosphate levels -Diet
Cytokines
Hormones – hormone replacement
osteoporosis
Severely decreased bone mass
Increased susceptibility to fractures
Bone density > 2.5 SD below young adult reference population
>1 to 2.5 SD below is osteopenia without osteoporosis
risk factors:
Personal Characteristics
Advanced age
Females
Ethnicity (white or Asian)
Small bone structure/low body weight Postmenopausal
Family history
Lifestyle (modifiable)
Sedentary
Calcium/Vitamin D deficiency
Malnutrition Smoking
Excessive alcohol intake
Excessive caffeine intake (*)
Medications
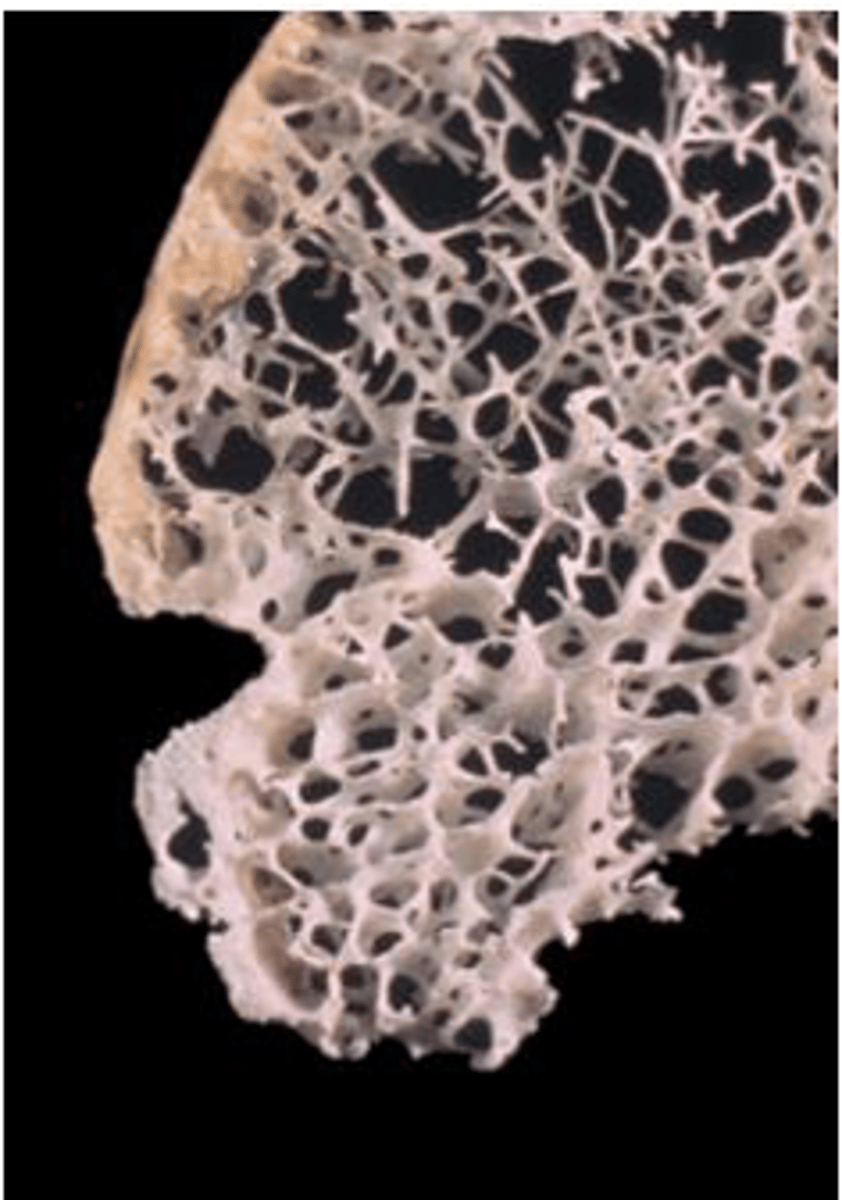
osteoporosis (2)
First manifestation: Sudden fractures
-- Vertebral compression fracture
-- Fracture of vertebra(e), hip, pelvis, humerus
Wedging & collapse of vertebrae
-- Loss of height in the vertebral column
-- Kyphosis- Dowager hump
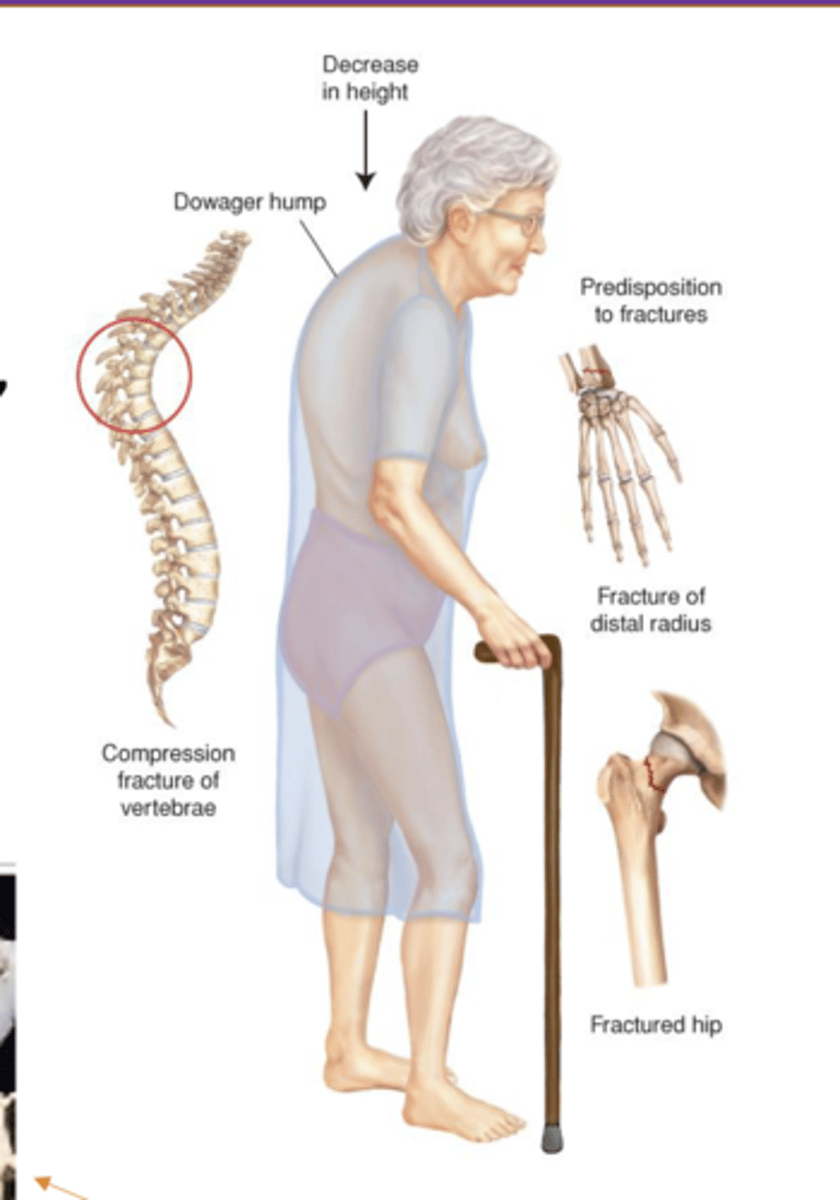
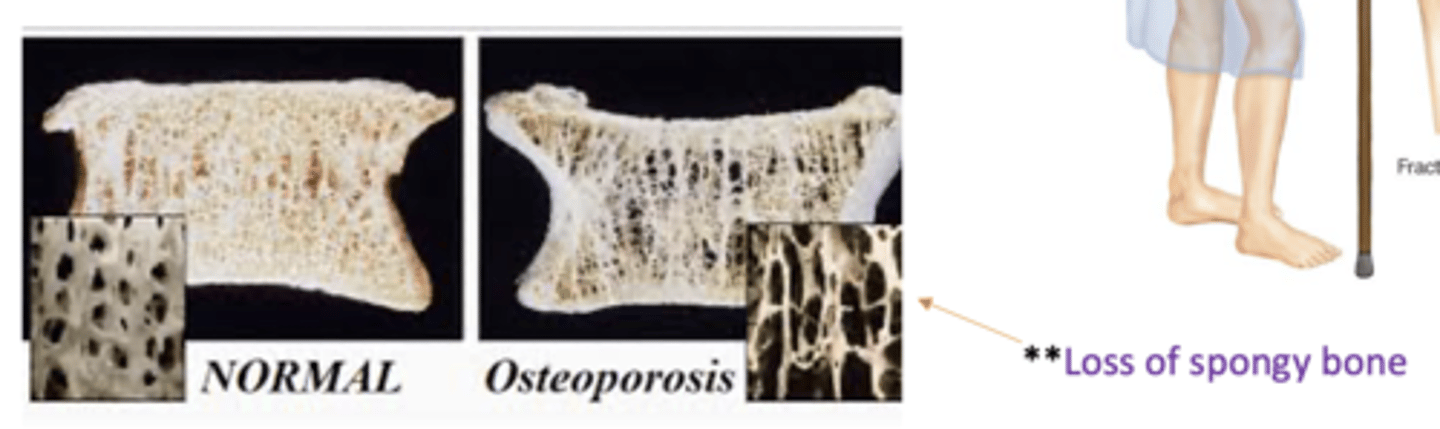
loss of spongy bone
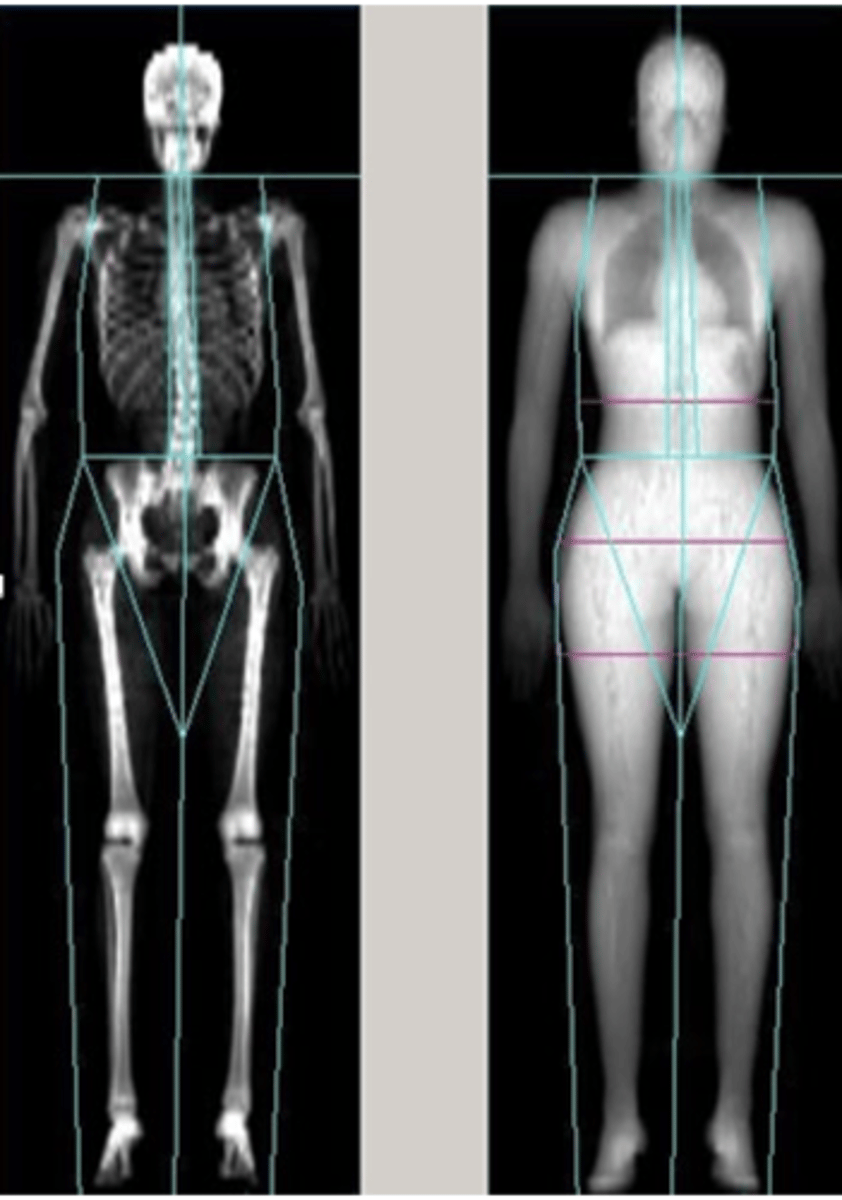
diagnosis and treatment (osteoporosis)
Dual-energy X-ray absorptiometry (DXA or DEXA)
DXA is recommended for:
-- All people 65 years and older
-- Women 60 to 64 years with increased fracture risk
Imaging options:
-- Whole body
-- Lumbar
-- Femur
-- Wrist
Treatments:
-- Exercise (weight-bearing)
-- Calcium, vitamin D
-- Medications (e.g., bisphosphonates)
RED-S
Relative energy deficiency in sports

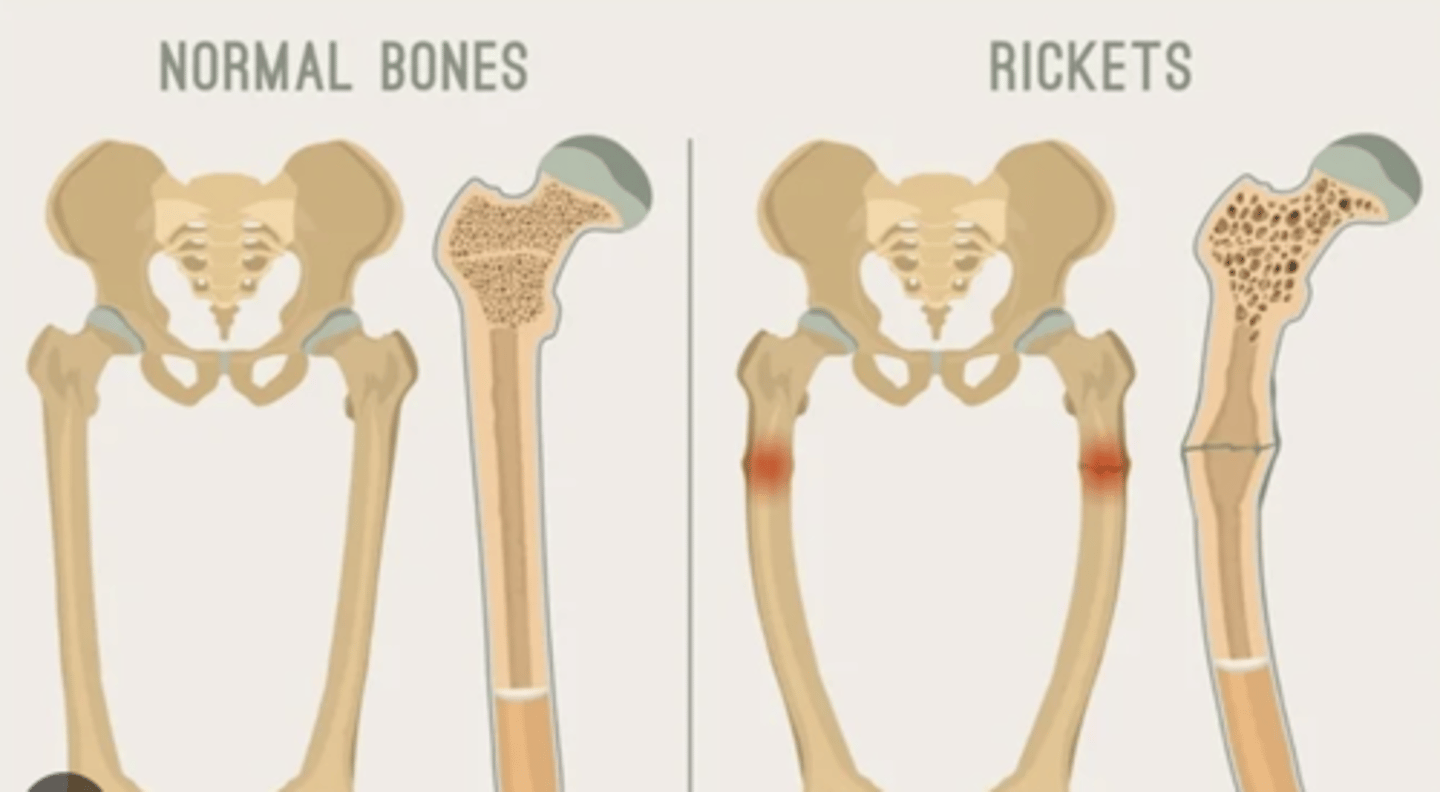
normal bone/rickets
Osteomalacia
Degradation versus lack of mineralization
in children because it refers to the growth plate not properly mineralizing. osteomalacia is more of the performed osteon, no longer able to mineralize = adults and children alongside ________
rickets
osteomalacia (2)
Softening of bone in adults due to inadequate mineralization
Two main causes
(1)Insufficient calcium absorption from the intestine or vitamin D deficiency (most common)
(2)Phosphate deficiency due to increased renal losses or decreased intestinal absorption
Risk factors:
- Elderly (deficient diets & malabsorption)
- Long-term anticonvulsant or diauretic treatment
Results in:
- Bone pain & tenderness
- Fractures
- Deformities (gravity, muscle weakness, bone softening)
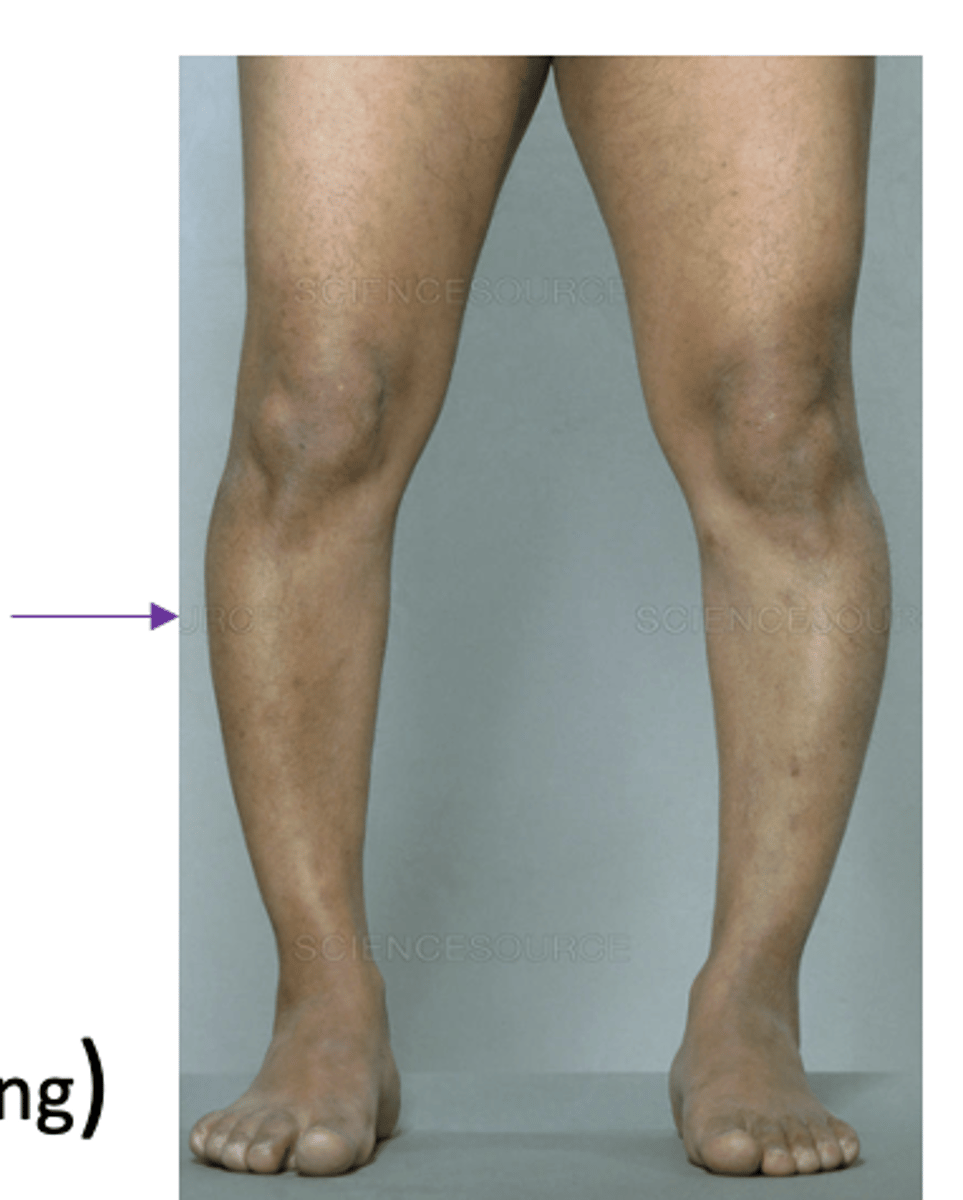
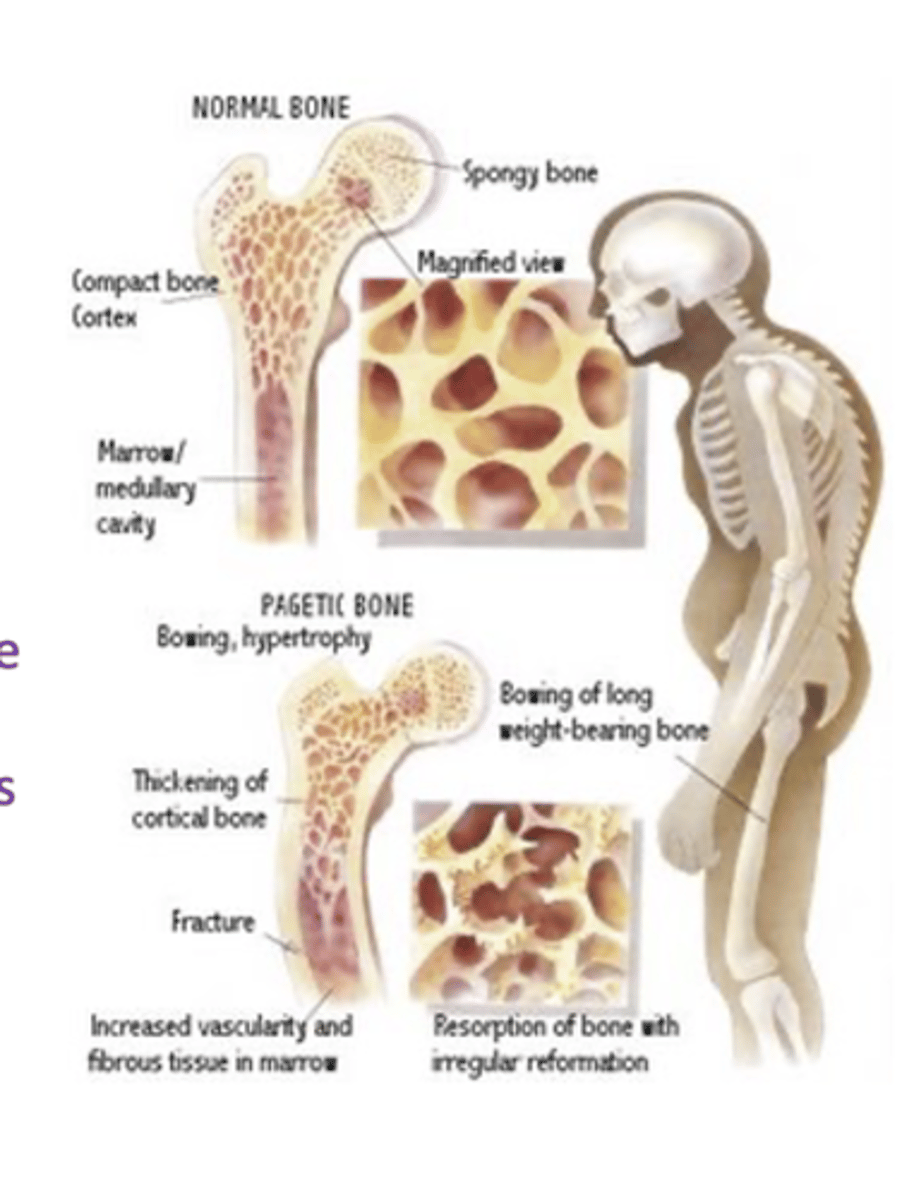
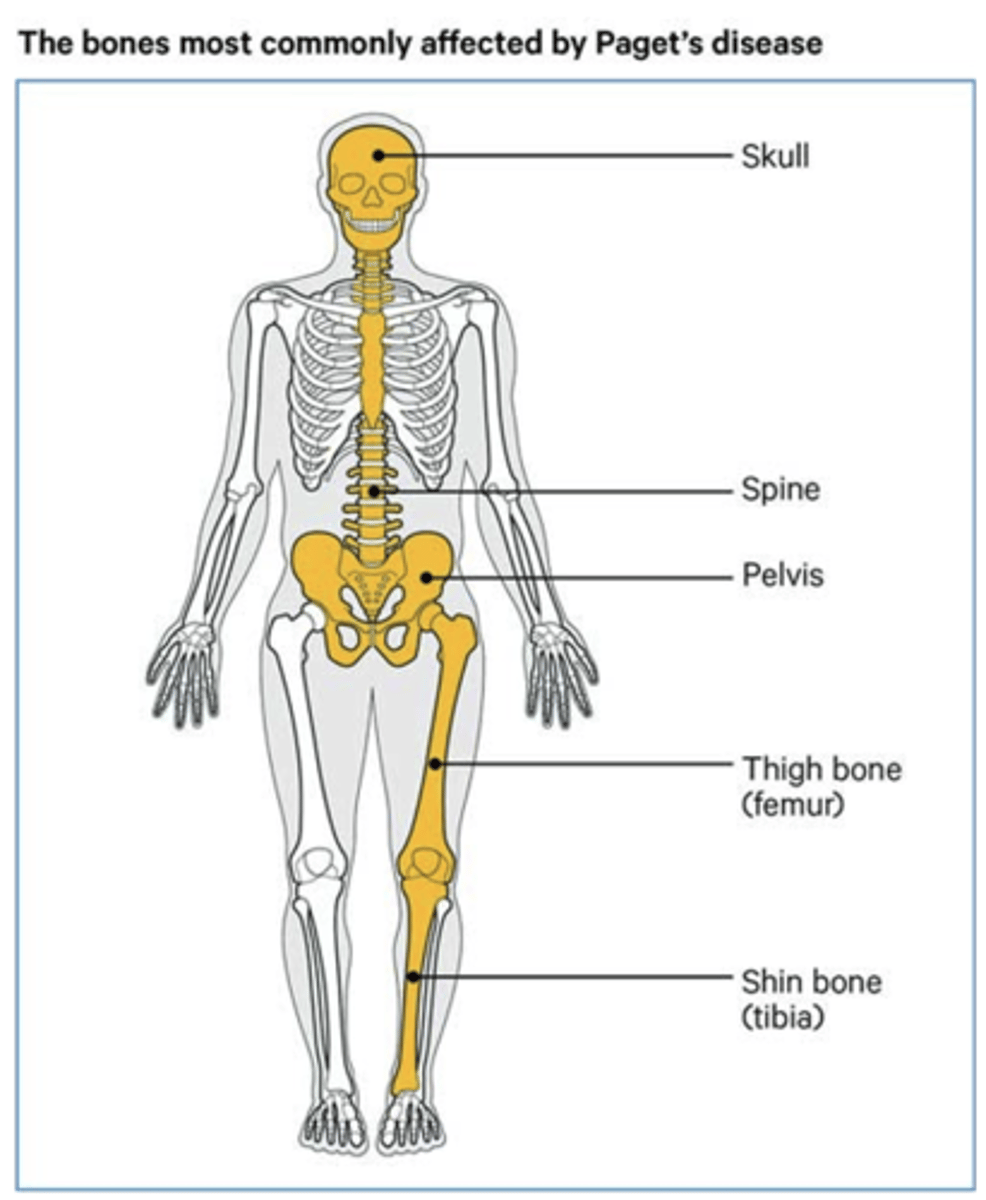
paget's disease
Focal degradation with unpatterned rebuilding
Paget’s Disease (Osteitis Deformans)
Second most common metabolic bone disease after osteoporosis
- Often asymptomatic (~70%)
- ~3% of US population
- ~10% of people 80+ yrs
Characterized by
- Focal areas of excessive osteoclast-mediated bone resorption
- Disorganized osteoblast-mediated bone repair
- Disorganized, thickened, but soft bones
Genetic and environmental influences:
- Mutations in RANK pathways
- Viral origin debated
paget's disease (2)
Symptoms:
- Bone pain, abnormal bone curvatures, brain compression, impaired motor function, deafness, atrophy of the optic nerve
- Tumors and tumor like conditions
Treatment:
- Anti-inflammatory agents
- Bone resorption inhibitors
- Bisphosphonates
- Calcium/Vitamin D

Summary Metabolic Bone disorders
Rheumatic Disorders
Inflammatory disorders, often autoimmune, that cause degenerative musculoskeletal tissue changes.
An older patient comes into the clinic with joint stiffness, a limited range of motion in the joints and pain especially in the knees when they try to sit or stand.
Their job (school custodian) requires walking and lifting during the majority of the day and this has been difficult for them to carry out.
They are concerned they will not be able to continue working and are asking you for advice on how to fix the problem.
Testing reveals elevated antibody levels against self.
rheumatoid disorder
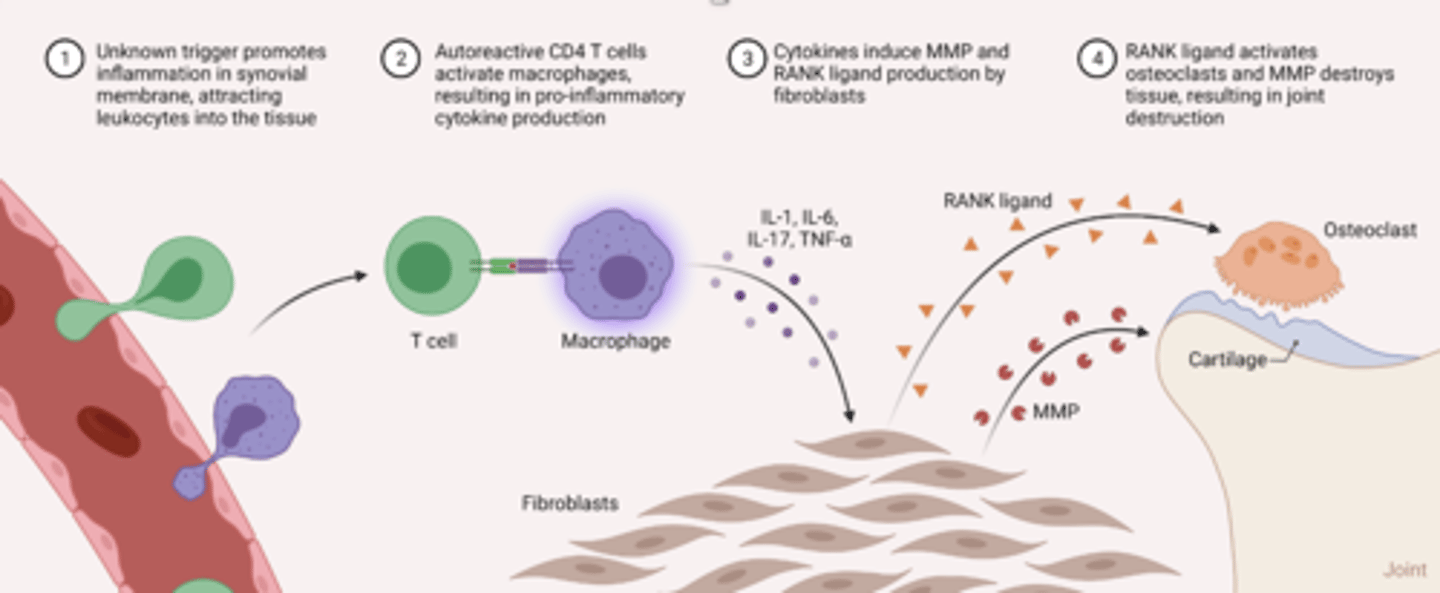
Systemic, chronic autoimmune disease
Peak incidence between 40 and 50 years
Genetic predisposition (HLA type) + immunological trigger
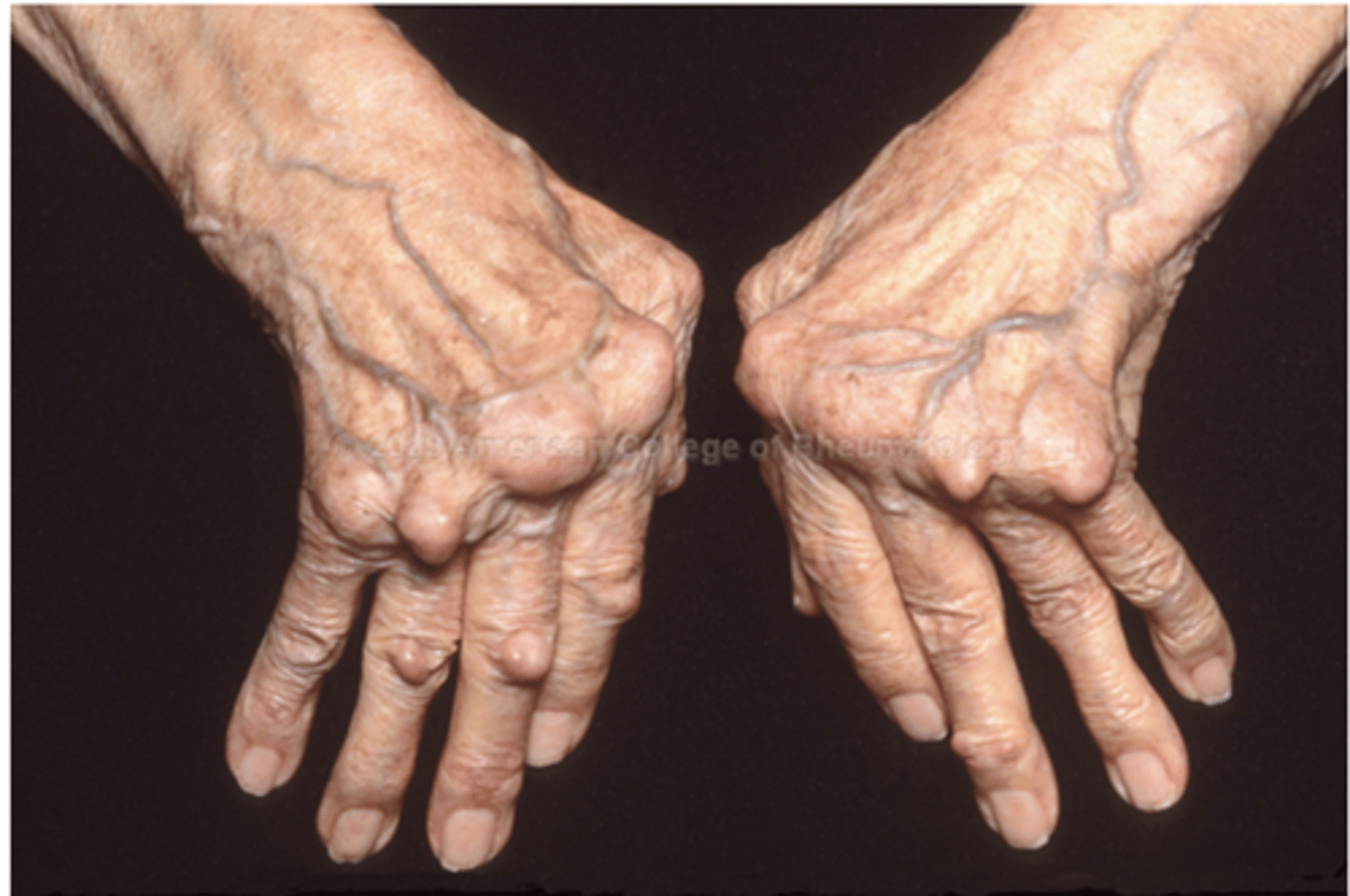
Articular Manifestations of rheumatoid arthritis
Usually symmetrical and polyarticular
Joint pain and stiffness
Subluxation of joints &
spindle-shaped appearance
Progressive joint destruction
-- Misalignment of bone
-- Swelling and thickening
-- Limitation of movement
classification and treatment of rheumatoid arthritis
Criteria include four or more of the following:
1. Morning stiffness for 1+ hours, present for 6+ weeks
2. Simultaneous swelling of 3+ joints for 6 + weeks
3. Swelling of wrist, metacarpophalangeal, or proximal interphalangeal joints for 6+ weeks
4. Symmetric joint swelling for 6+ weeks
5. Rheumatoid nodules
6. Serum rheumatoid factor (RF) and anti-CCP
7. Radiographic changes on hand or wrist
Treatments:
- Rest and therapeutic exercise
- Medications: NSAIDs, corticosteroids, antirheumatics, monoclonal antibodies
- Surgery
- Occupational Therapy: Splinting (anti-deformity positions), ADL retraining, joint protection strategies
An older patient comes into the clinic with joint stiffness, a limited range of motion in the joints and pain especially in the knees when they try to sit or stand.
Negative for RF and anti-CCP (if positive it would have been rheumatoid arthritis)
X-ray does not show joint space narrowing or cartilage damage
Now what?
systemic lupus erythematosus (SLE)
Systemic Lupus Erythematosus (SLE)
Chronic autoimmune disease that can affect any organ system
-- “The great imitator”
-- Widespread inflammation and tissue damage
--- Joints, skin, brain, lungs, kidneys, blood vessels
-- Blood test: anti-nuclear Ab (ANA)
Primarily seen in young females (15-40 years)
-- Incidence higher in some families
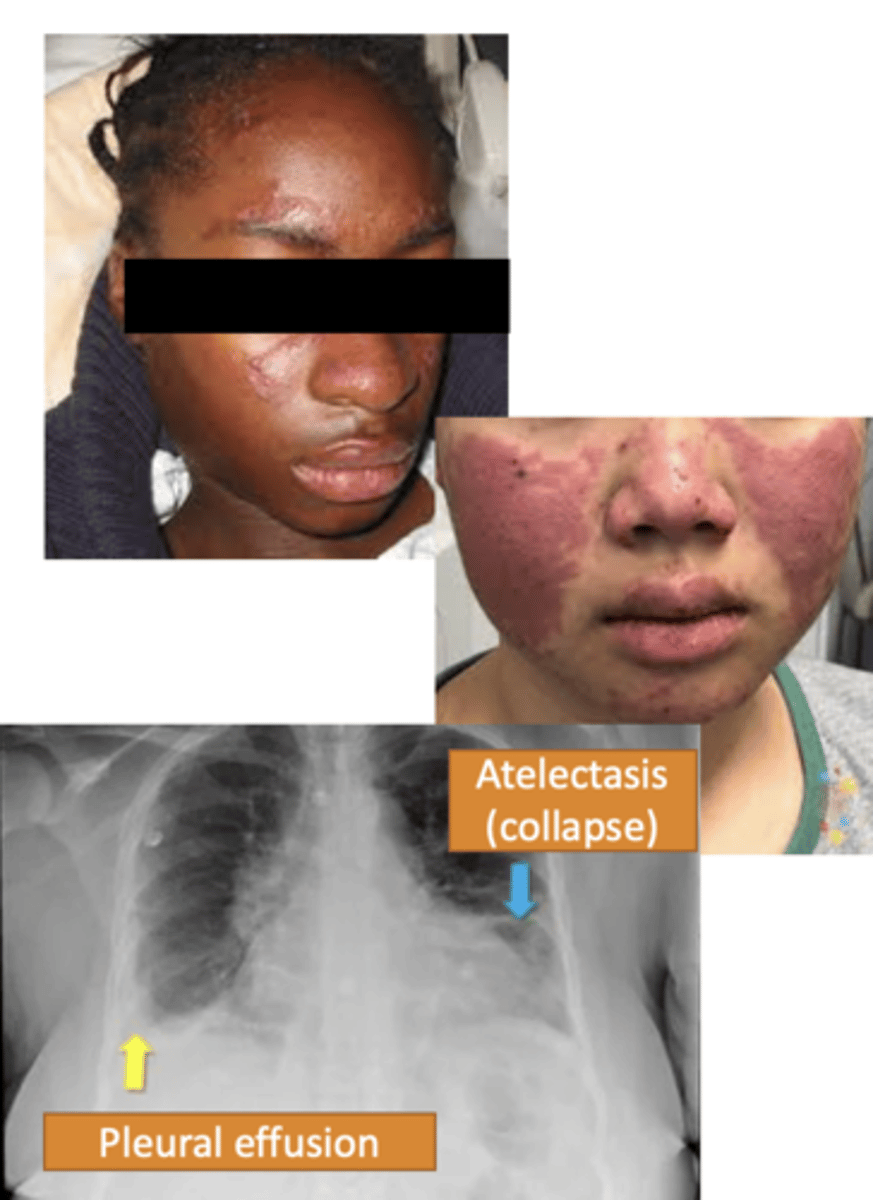
butterfly rash
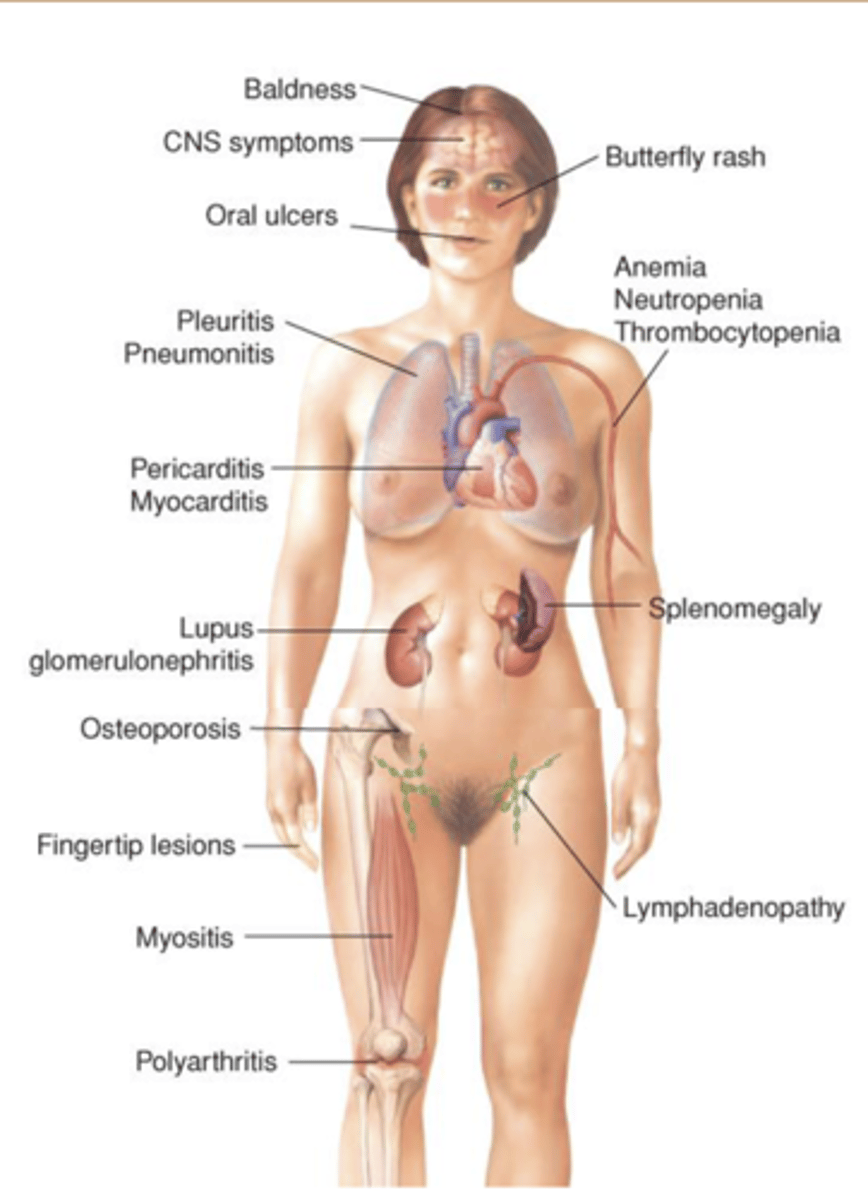
Systemic Lupus Erythematosus (SLE) (2)
Defective elimination of self-reactive B cells and increase in antibody production, causing tissue damage
Treatment
- NSAIDS
- Antimalarial drugs for lupus rashes or musculoskeletal manifestations
- High-dose corticosteroids for acute symptoms
- Monoclonal Antibodies
-- Block B cell antibody production
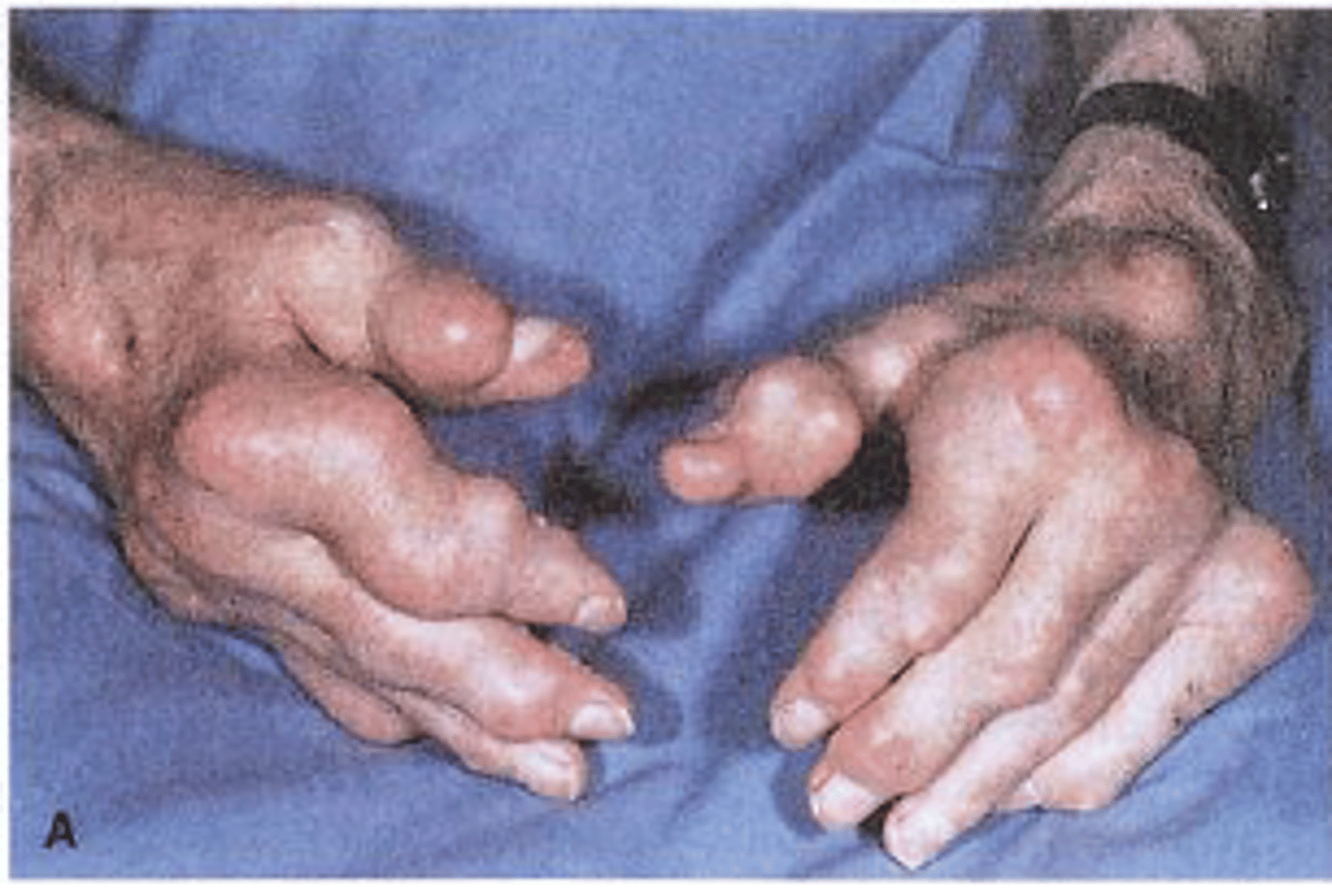
gout
An older patient comes into the clinic with joint stiffness, a limited range of motion in the joints and pain especially in the knees when they try to sit or stand.
Still suspect inflammatory issues (swollen joints)
X-ray does not show joint space narrowing or cartilage damage but does show calcified crystals within the joint
Gout - Crystal-Induced Arthropathies
presents as:
(1) Acute gouty arthritis
(2) Tophi- accumulation of crystalline deposits in articular surfaces, bones, soft tissue, and cartilage
(3) Gouty nephropathy or renal impairment
(4) Uric acid kidney stones
Elevated serum uric acid
-- Overproduction or excessive breakdown of purines (adenine and guanine)
-- Decreased uric acid excretion
Primary: Cause unknown or metabolic error; hyperuricemia
Secondary: Due to underlying disorder
Most commonly affects men
Uric acid management: Low-purine diet, medications (e.g., xanthine oxidase inhibitors)

Summary Rheumatic Bone disorders
1. What is the primary difference between osteopenia and osteoporosis?
A. Osteopenia is irreversible; osteoporosis is reversible
B. Osteopenia has a greater risk of fracture than osteoporosis
C. Osteopenia represents a milder decrease in bone density compared to osteoporosis
D. Osteopenia affects only the elderly; osteoporosis affects all ages
c. Osteopenia represents a milder decrease in bone density compared to osteoporosis
2. Which of the following best differentiates osteomalacia from Paget's disease?
A. Osteomalacia is associated with excessive bone remodeling
B. Paget's disease is characterized by defective mineralization
C. Osteomalacia results from vitamin D deficiency, while Paget's involves disorganized bone remodeling
D. Both conditions are caused by parathyroid hormone deficiency
c. Osteomalacia results from vitamin D deficiency, while Paget's involves disorganized bone remodeling
3. What is a key immunological feature of rheumatoid arthritis (RA)?
A. Localized wear and tear of joint cartilage
B. Uric acid crystal deposition in joints
C. Autoantibody production and synovial inflammation
D. Deficiency of vitamin C affecting collagen formation
C. Autoantibody production and synovial inflammation
4. Which feature distinguishes rheumatoid arthritis from osteoarthritis?
A. RA typically affects weight-bearing joints first
B. RA is associated with systemic symptoms and symmetrical joint involvement
C. Osteoarthritis is an autoimmune disorder
D. RA results from direct mechanical injury
b. RA is associated with systemic symptoms and symmetrical joint involvement
5. What is a characteristic manifestation of systemic lupus erythematosus (SLE)?
A. Asymmetric joint involvement
B. Butterfly-shaped rash across the face
C. Increased uric acid in serum
D. Bone overgrowth
B. Butterfly-shaped rash across the face