Hormones of pregnancy, menopause and contraception
1/59
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
60 Terms
How do sex hormones act via intracellular receptors to regulate gene expression?
Receptors have ligand-binding and DNA-binding domains
Hormone binding triggers translocation to the nucleus
Receptor binds to hormone-response elements (HREs) on DNA
Receptors dimerise, which is essential for function
Name the 3 different types of receptors of sex hormones:
Androgen receptors (AR)
Estrogen receptors (ER)
Progesterone receptors (PR)
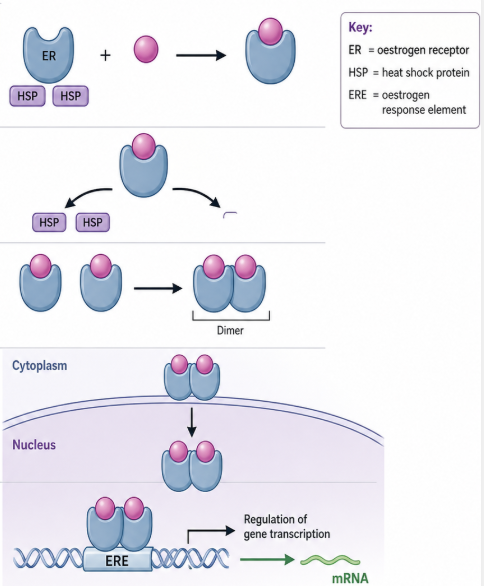
How does the oestrogen receptor act to regulate gene expression?
Oestrogen binds to its receptor
Heat shock proteins dissociate, activating the receptor
The oestrogen receptor dimerises
The oestrogen-receptor dimer complex binds to DNA at “oestrogen response elements” to regulate gene transcription.
What are oestrogen response elements (EREs)?
Specific DNA sequences that the oestrogen-receptor complex binds to in order to regulate gene expression.
How does the progesterone receptor (PR) regulate gene transcription?
The progesterone receptor is a nuclear receptor that binds progesterone and then attaches to specific DNA sequences called progesterone response elements (PREs) to regulate gene transcription.
What are the isoforms of the progesterone receptor and their function?
PR-A and PR-B
Both bind progesterone, but PR-B mainly mediates the stimulatory effects of progesterone.
What are the actions of oestrogens?
Reproductive system:
Stimulate endometrial growth
Thicken vaginal mucosa
Thin cervical mucus
Female characteristics:
Development of secondary sexual characteristics
Breast duct development
Hormonal control:
Increase GnRH secretion (hypothalamus)
Decrease LH secretion (pituitary)
Metabolic effects:
Increase protein synthesis
Promote bone growth
Decrease circulating cholesterol
CNS:
Multiple effects on brain function
Which phase is progesterone produced?
In the luteal phase
What are the actions of progesterone?
Hormonal control:
Decreases GnRH secretion
Uterus:
Stimulates secretory activity in the endometrium
Cervix:
Increases viscosity of cervical mucus
Breasts:
Promotes glandular development
Other effects:
Increases basal body temperature
What are oestrogen preparations?
Forms of oestrogen used clinically, e.g. natural oestrogens and synthetic oestrogens
Give examples of natural oestrogen preparations:
Oestradiol
Oestrone
Oestriol

Give examples of synthetic oestrogen preparations:
Mestranol
Ethinylestradiol
Diethylstilbestrol
What are the routes of administrations for oestrogen preparations?
Oral, transdermal, intramuscular, implantable, topical
What do SERMs stand for?
Selective Estrogen Receptor Modulators
Why do SERMs have tissue-specific effects?
Different tissues express different oestrogen receptor types (ER-α and ER-β)
Binding causes different receptor conformations
This leads to tissue-specific responses that can be oestrogen-like or anti-oestrogenic
What is the clinical use of SERMs?
They are used to treat certain cancers (e.g. tamoxifen in breast cancer)
What are progestogen preparations?
Progestogen preparations are drugs that mimic the effects of progesterone and are used in hormonal therapies.
What are the two main types of progestogen preparations?
Natural progesterone derivatives
Synthetic derivatives of testosterone.
Give examples of natural progesterone derivatives.
Hydroxyprogesterone, medroxyprogesterone, and dydrogesterone.
Give examples of testosterone-derived progestogens.
Norgestrel, desogestrel, and ethynodiol.
What age does menopause typically occur?
45-55 years
What is menopause caused by?
Ovarian failure
What happens in menopause?
Ovarian function declines, so less oestrogen and progesterone are produced. This leads to gonadotropins are secreted in greater amounts because of the loss of negative feedback. FSH levels rise significantly.
Name the 3 phases of menopause:
Perimenopause
Menopause
Postmenopause
Phase 1) Perimenopause
Fluctuation in hormone levels
Can last 2-8 years
Phase 2: Menopause
Oestrogen levels drop
1 year after cessation of menstrual cycle
Phase 3: Postmenopause
Oestrogen levels continue to drop
What are the symptoms of menopause?
Hot flushes of skin
Night sweats
Palpitations
Low mood/anxiety
Impaired memory/brain fog
Recurrent headaches/ migraines
Vaginal atrophy
Development of osteoporosis ( risk hip & spine fractures)
Why is oestrogen good for bones?
Oestrogen helps maintain bone mineral density by reducing bone loss.
How does oestrogen therapy affect osteoporosis risk?
Oestrogen replacement therapy helps maintain bone mass and reduces the risk of fractures
What is raloxifene and how does it affect bone?
Raloxifene is a selective oestrogen receptor modulator (SERM) that mimics oestrogen’s effects on bone to maintain bone density.
What type of oestrogen is typically used in HRT?
Natural oestrogens are usually used rather than more potent synthetic oestrogens.
When are oestrogens combined with progestogens in HRT?
Oestrogens are combined with progestogens in women who have an intact uterus to protect the endometrium.
How can oestrogen-only HRT be given with progesterone?
Oestrogen can be given separately (e.g. patch, gel, spray), with progesterone added as a tablet or intrauterine device.
What are the beneficial effects of HRT?
Reduces postmenopausal osteoporosis
Relieves vasomotor symptoms such as hot flushes
Improves cholesterol profile by lowering LDL
What are the risks associated with HRT?
Increased risk of breast cancer
Increased risk of uterine cancer
Increased risk of blood clots
What is the overall risk–benefit profile of HRT?
For most women, the benefits of HRT outweigh the risks, although cardiovascular effects remain uncertain.
What are the different types of contraception?
Barrier methods (caps, diaphragms, condoms)
Intra-uterine (IUD) coil
Oral contraceptives (combined hormonal contraceptives, emergency contraception, progestogen only contraceptives)
What hormones are used in the combined oral contraceptive pill?
Oestrogen and progestogen
Oestrogen (e.g. ethinylestradiol, mestranol)
Progestogen (e.g. levonorgestrel, desogestrel, gestodene)
How is the combined oral contraceptive pill typically taken?
It is usually taken for 21 days followed by a 7-day break, or as a 28-day continuous regimen.
How does oestrogen in the combined pill prevent ovulation?
Oestrogen inhibits FSH secretion via negative feedback on the pituitary, preventing follicle development.
How do progestogens in the combined pill prevent pregnancy?
They inhibit LH secretion to prevent ovulation, thicken cervical mucus to block sperm, and thin the endometrium to reduce implantation.
What are the common (mild) side effects of combined oral contraceptives (COCs)?
Nausea
Weight gain due to fluid retention
Mild hypertension
Breast tenderness
What are the serious side effects of combined oral contraceptives (COCs)?
Venous thromboembolism
Stroke and myocardial infarction (especially in smokers over 35)
Increased risk of breast and cervical cancer
How is the progestogen-only contraceptive taken?
It is taken continuously without a break.
How does the progestogen-only contraceptive prevent pregnancy?
Thickens cervical mucus, making it difficult for sperm to pass
Alters the endometrium, reducing the likelihood of implantation
Inhibits LH release, which may suppress ovulation
What additional effect can progestogen-only contraceptives have in some women?
They can fully suppress ovulation and gonadotrophin secretion, leading to amenorrhoea.
What are progestogens also used for?
Treating menstrual disorders
What methods are used for emergency contraception?
Copper intrauterine device (IUD)
Levonorgestrel
Ulipristal
How does emergency hormonal contraception work?
It prevents pregnancy mainly by delaying or inhibiting ovulation through suppression of the LH surge.
What is the time window for levonorgestrel and ulipristal in emergency contraception?
Levonorgestrel: effective within 72 hours
Ulipristal: effective up to 120 hours (5 days)
What are the side effects of emergency contraception?
Nausea, vomiting (which may affect absorption), and breast tenderness, with possible cardiovascular and metabolic effects.

What is mifepristone?
Mifepristone is an antiprogestogen that acts as a progesterone receptor antagonist, blocking the effects of progesterone.
Why is mifepristone used with misoprostol?
Misoprostol is a prostaglandin analogue that induces uterine contractions, helping to complete the termination of pregnancy.
What is the clinical use of antiprogestogens like mifepristone?
Medical abortion
How are prostaglandins produced from membrane phospholipids?
Membrane phospholipids are converted by phospholipase A₂ into arachidonic acid, which is then converted by cyclooxygenase into prostaglandins.
What are the main products of arachidonic acid metabolism and their functions?
Prostaglandins: involved in inflammation and vascular effects
Thromboxanes: involved in blood clotting
Leukotrienes: act as inflammatory mediators
Which hormones stimulate uterine contractions to induce labour?
Oxytocin and prostaglandins
Which hormones inhibit uterine contractions?
Progestogens relax the uterine wall and help maintain pregnancy
β2-adrenoceptor agonists inhibit contractions of the pregnant uterus
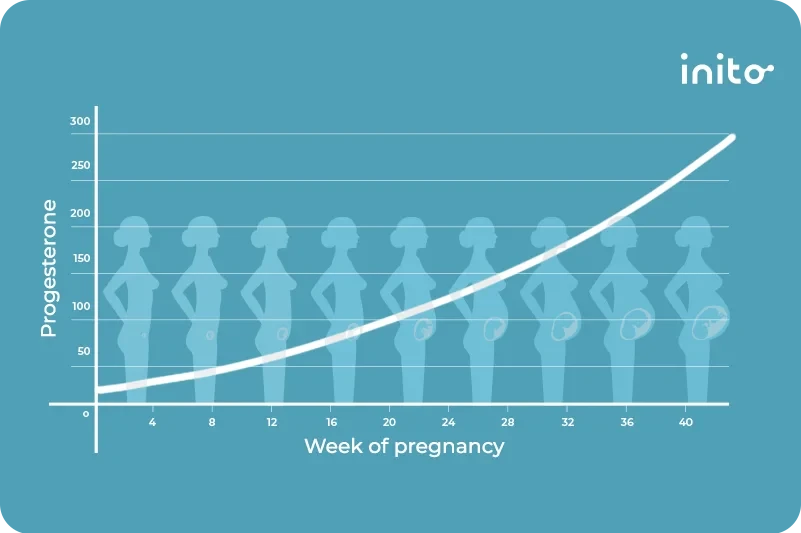
What is the role of progestogens in pregnancy?
Progestogens relax the uterine wall and maintain cervical length
This helps prevent premature labour and miscarriages