Male Reproductive System
1/114
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
115 Terms
Gonads -
organs where gametes are produced
The scrotum: Supporting
structure for testes
scrotum: Sac
of skin and superficial fascia
scrotum: Its external positioning
keeps the testes lower than core body temperature
The Scrotal Septum
divides the scrotum into two sacs interiorly, each contains one testis
Dartos muscle:
is found in subcutaneous tissue and in septum, bundles of smooth m. fibers, contraction gives skin wrinkled appearance
Cremaster muscle is
a band of skeletal muscle that is a continuation of internal oblique muscle
Contraction of Dartos muscle and cremaster
muscles brings testes closer to body for warmth
Descent of testes: Develop
near kidney on posterior abdominal wall
Descent of testes: Descends
into scrotum by passing through inguinal canal
Descends into scrotum by passing through inguinal canal TAKES PLACE…
during 7th month of fetal development
Testes: tunica vaginalis,
derived from peritoneum
Testes: tunica albuginea,
the fibrous capsule of the testis
Septa
(extensions of tunica albuginea) divide the testis into 250-300 lobules, each containing 1-4 seminiferous tubules
Spermatogenesis:
The sequence of events that produces sperm in the seminiferous tubules of the testes
Spermatogenesis starts with
diploid spermatogonia which are stem cells for sperm.
Spermatogenesis begins at
puberty in males
spermatogenesis: Mitosis of the spermatogonia to
maintain a stem cell line for life
spermatogenesis: each mitotic division of spermatogonia results in
type A or type B daughter cells
Spermatogenesis: Type A cells
remain and maintain the germ line
Spermatogenesis: Type B cells
move toward the lumen and differentiate into primary spermatocytes that will undergo meiosis
Primary spermatocytes
undergo meiosis I, forming two haploid cells called secondary spermatocytes
Secondary spermatocytes
undergo meiosis II and their daughter (4) cells are called spermatids
Spermatids
are small round cells seen close to the lumen of the tubule
Late in spermatogenesis,
spermatids are haploid but nonmotile
Spermiogenesis –
spermatids lose excess cytoplasm and form a tail, becoming sperm
Sertoli Cells
Support and protect the developing spermatogenic cells in several ways
Sertoli Cells: Nourish
developing sperm
Sertoli Cells: Phagocytize
excess cytoplasm
Sertoli Cells: Control
movements of spermatogenic cells and release sperm into lumen
Sertoli Cells: Joined by
tight junctions to form the Blood-Testis Barrier
Sertoli Cells: Joined by tight junctions to form the Blood-Testis Barrier
Isolates the developing gametes from the blood preventing an immune response against the spermatogenic cell’s surface antigens which are recognized as foreign by immune system
Sertoli Cells: Produce
fluid for sperm transport, secrete hormone inhibin
Leydig (Interstitial) Cells
Clusters of cells in between adjacent seminiferous tubules
Leydig Cells: Secrete
testosterone
Sperm Major Regions: Head
contains DNA and has a helmetlike acrosome containing hydrolytic enzymes that allow the sperm to penetrate and enter the egg
Sperm major regions: Midpiece
contains mitochondria spiraled around the tail filaments
Sperm major regions: tail
a typical flagellum produced by a centriole
Each day _______ complete spermatogenesis
300 million sperm
Hormonal control of the Testes
GnRH stimulates anterior pituitary secretion of FSH and LH.
Hormonal control of testes: FSH
initiates spermatogenesis
Hormonal Control of testes: LH
assists spermatogenesis and stimulates production of testosterone.
Effect inhibin: sertoli cells release
inhibin
Sperm production is sufficient: inhibits FSH
secretion by the anterior pituitary
Sperm production is sufficient: decreases
sperm production
Sperm production is proceeding too slowly: less inhibin
is released by the sertoli cells
Sperm production is proceeding too slowly: more
FSH will be secreted
Sperm production is proceeding too slowly: sperm production
will be increased
Testosterone
controls the growth, development, functioning, and maintenance of sex organs
testosterone: stimulates
bone growth, protein anabolism, and sperm maturation
testosterone: stimulates development
of male secondary sex characteristics.
testosterone stimulates final
steps spermatogenesis
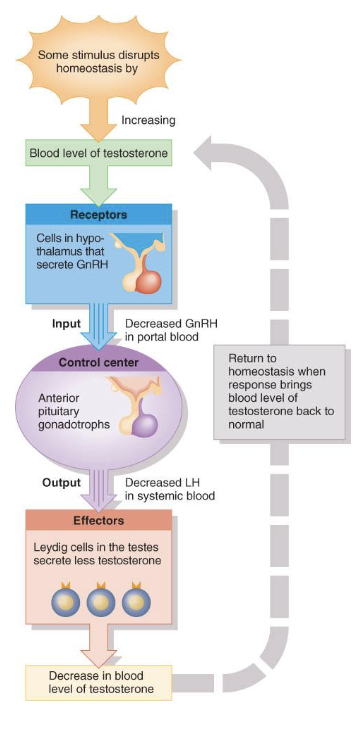
testosterone: Negative feedback
systems regulate testosterone production.
Seminiferous tubules
converge to form the tubulus rectus conveys sperm to rete testis to efferent ductules to epididymis
Spermatic cord –
encloses PNS and SNS nerve fibers, blood vessels, and lymphatics that supply the testes
Pathway of sperm flow
Seminiferous tubules
Straight tubules
Rete testis
Efferent ducts
Ductus epididymis
Ductus (vas) deferens
Epididymis
1.5in long along posterior border of each testis
epididymis: has
Head, body and tail region
epididymis: multiple
efferent ducts become a single ductus epididymis in the head region (20 feet if uncoiled)
edpi
epididymis: site of
sperm maturation
Sperm may remain in storage here for at least a month, after which they are either expelled or degenerated and reabsorbed
The ductus epididymis is lined by
stereocilia that increase surface area for absorption
Ductus Deferens
18 inches-Runs from the epididymis through the inguinal canal into the pelvic cavity
ductus deferens: Propels
sperm from the epididymis to the urethra
ductus deferens: lined by
mucosal membrane of pseudostratified columnar epithelium and lamina propria, 3 layers of smooth muscle in muscularis
ductus deferens: conveys
sperm during sexual arousal from epididymis to urethra by peristalsis
ductus deferens: Can store
sperm for several months or reabsorb
ejaculatory ducts
are formed by the union of the ducts from the seminal vesicles and ducti deferens; their function is to eject spermatozoa into the prostatic urethra.
The male urethra
is the shared duct of the reproductive and urinary systems which serves as a passageway for semen and urine.
urethra (8 inch long passageway)
Prostatic urethra
Membranous urethra
Penile (spongy) urethra
3 Accessory Glands: Seminal Vesicles: Lie on
the posterior wall of the bladder and secrete 60% of the volume of semen
Semen –
viscous alkaline fluid containing fructose, ascorbic acid, coagulating enzyme (vesiculase), and prostaglandins
3 Accessory Glands: Seminal Vesicles: Join
the ductus deferens to form the ejaculatory duct
3 Accessory Glands: Seminal Vesicles: Sperm and seminal fluid
mix in the ejaculatory duct and enter the prostatic urethra during ejaculation
Alkaline, viscous fluid
neutralizes vaginal acid & male urethra
fructose
prostaglandins
coagulation proteins
Accessory Glands: Prostate Gland
Doughnut-shaped gland that encircles part of the urethra inferior to the bladder
Accessory Glands: Prostate Gland: milky
slightly acid fluid, which contains citrate, enzymes, and prostate-specific antigen (PSA), accounts for one-third of the semen volume
Accessory Glands: Prostate Gland: plays role in
activation of sperm
Accessory Glands: Prostate Gland: enters the
postatic urethra during ejaculation
Prostrate Gland: Single organ
size of chestnut
inferior to bladder
pH 6.5 fluid
citric acid
enzymes for seminal liquefaction
Prostate gland: many
duct openings p
prostate gland: enlarges
with age
Accessory Glands: Bulbourethral Glands
Paired Pea-sized glands inferior to the prostate
Accessory Glands: Bulbourethral Glands: Produce thick,
clear mucus prior to ejaculation that neutralizes traces of acidic urine in the urethra
Accessory Glands: Bulbourethral Glands: mucus
for lubrication
Accessory Glands: Bulbourethral Glands: Ducts
open into spongy urethra
semen: provides
transport medium and nutrients (fructose), protects and activates sperm, and facilitates their movement
Prostaglandins in semen:
Decrease the viscosity of mucus in the cervix
Stimulate reverse peristalsis in the uterus
Facilitate the movement of sperm through the female reproductive tract
semen: realtive
alkalinity of semen neutralizes the acid environment found in the male urethra and female vagina
Seminalplasmin –
antibiotic chemical that destroys certain bacterias
semen: clotting
factors coagulate semen immediately after ejaculation, then fibrinolysin liquefies the sticky mass
semen: only
2-5 ml of semen are ejaculated, but it contains 50-130 million sperm/ml
Penis
contains the urethra and is a passageway for the ejaculation of semen and excretion of urine
penis: body composed
of three erectile tissue masses filled with blood sinuses
Body composed of three erectile tissue masses filled with blood sinuses
paired corpora cavernosa penis
unpaired corpus spongiosum penis
corpora cavernosa
upper paired, erectile tissue masses
corpus spongiosum
lower erectile tissue mass, surrounds urethra, ends at glans penis
corpus sponginosum and corpora cavernosa surrounded by
tunica lbuginea
Erection –
during sexual excitement, the erectile tissue fills with blood causing the penis to enlarge and become rigid
Corpus spongiosum –
surrounds the urethra and expands to form the glans and bulb of the penis