GYN Pathology
1/151
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
152 Terms
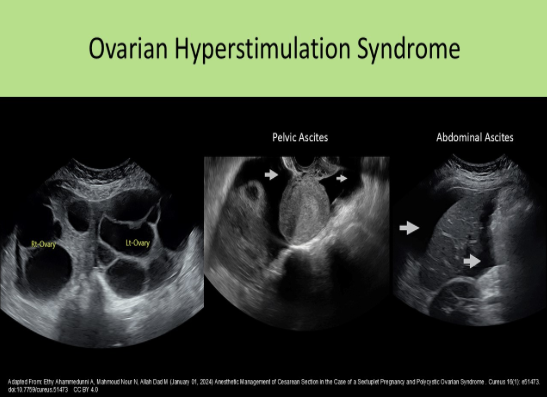
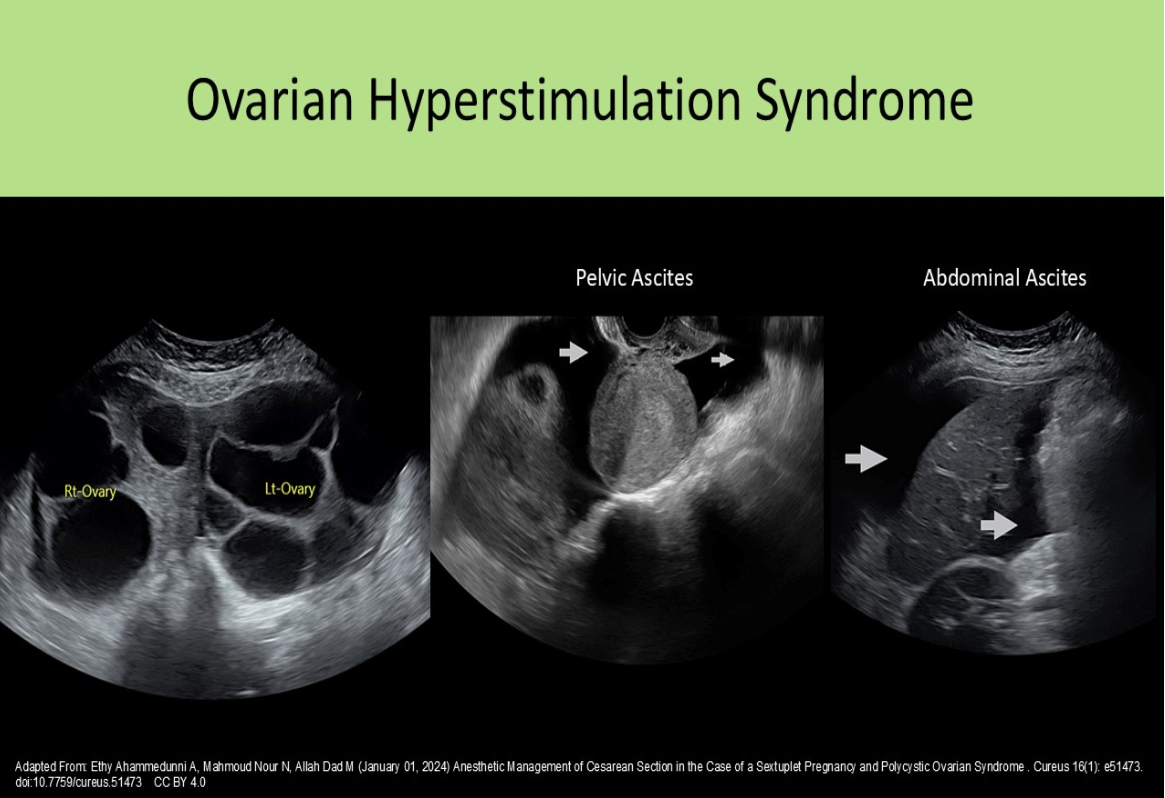
Ovarian hyperstimulation syndrome:
A. causes the ovaries to atrophy and testosterone levels rise
B. causes the uterine muscularis to become edematous
C. leads to reduced blood flow within the ovarian tissue surrounding the follicles
D. increases the risk for ovarian torsion
D. increases the risk for ovarian torsion
Ovarian hyperstimulation can lead to enlarged ovaries (>5cm) that are engorged with follicles. This causes an increased risk for ovarian torsion. The endometrium (not the muscularis) may become edematous in response to the increased hormonal levels.
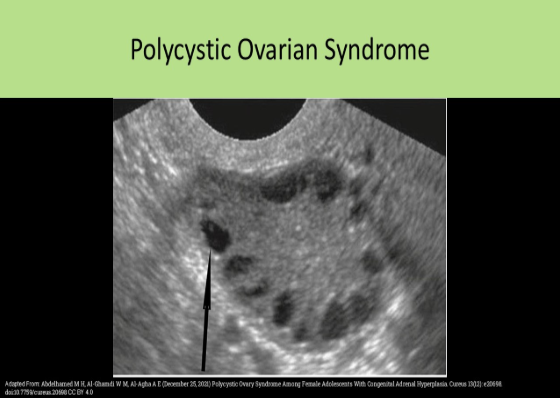
Polycystic ovarian disease usually demonstrates multiple follicles:
A. <20mm along the periphery of the ovary.
B. >15mm centrally and along the periphery of the ovary.
C. <5mm centrally and along the periphery of the ovary.
D. <10mm along the periphery of the ovary.
D. <10mm along the periphery of the ovary.
Polycystic ovarian disease usually demonstrates multiple follicles <10mm along the periphery of the ovary. This finding is described as the string of pearls sign.
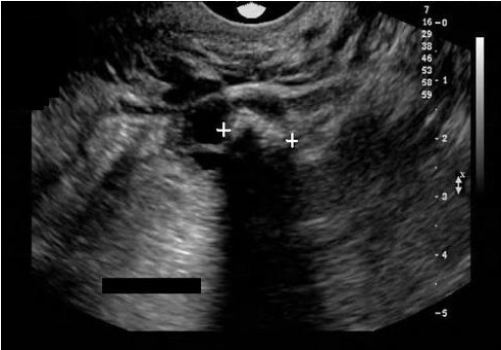
A 26 yr old female presents with pelvic pain and prior left oophorectomy due to cyst formation. Which of the following best describes the findings on the image?
A. The calipers are measuring a large echogenic mass with dirty shadowing which most likely represents a large fecalith in the bowel.
B. The calipers are measuring a large echogenic mass with dirty shadowing which most likely represents an obstruction in the bowel.
C. The calipers are measuring a large echogenic mass with posterior shadowing which most likely represents a dermoid cyst.
D. The calipers are measuring a large echogenic mass with posterior shadowing which most likely represents a chocolate cyst.
C. The calipers are measuring a large echogenic mass with posterior shadowing which most likely represents a dermoid cyst.
Note the classic "tip of the iceberg" sign of the dermoid within the ovarian tissue. Note the small area of visible ovarian tissue with follicles adjacent to the echogenic dermoid formation.
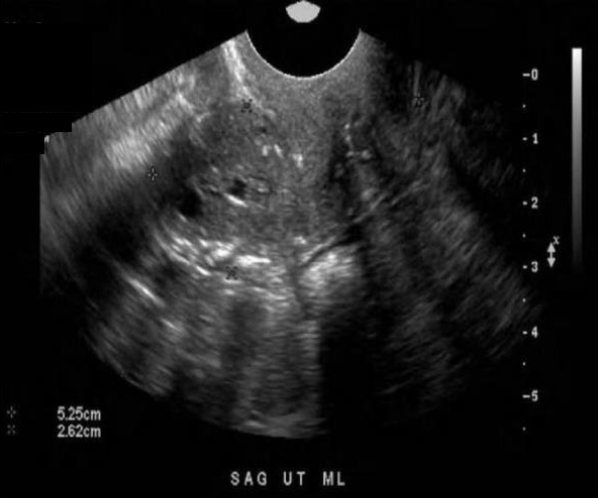
A 65 yr old postmenopausal female presents with a recent history of spotting. She does take a regimen of Tamoxifen from a previous diagnosis of breast cancer but no other medications are used. Which of the following statements is true regarding the ultrasound findings?
A. The endometrium is thickened and heterogeneous which can be normal in a patient using Tamoxifen.
B. The uterus is atrophied and fibroids have formed causing the heterogeneous appearance.
C. The endometrium is thickened and heterogeneous which is abnormal and D&C should be performed to rule out adenocarcinoma.
D. The endometrium is thickened and heterogeneous due to the presence of polyps.
A. The endometrium is thickened and heterogeneous which can be normal in a patient using Tamoxifen.
The uterus demonstrates a heterogeneous texture with calcifications seen in the periphery. The endometrium is very heterogeneous and thickened. Tamoxifen can cause the endometrium to appear thickened, irregular, and cystic.
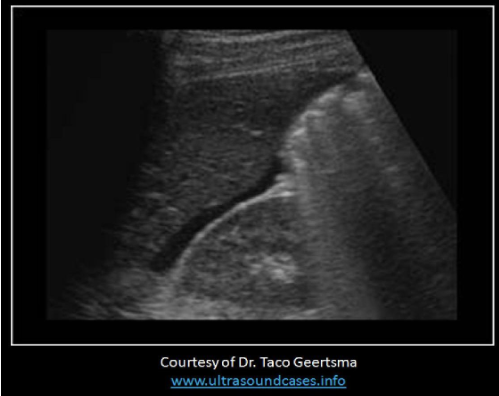
The findings on the image are expected in patients with:
A. normal ovulation
B. twin gestation
C. multiple large uterine fibroids
D. ovarian hyperstimulation syndrome
D. ovarian hyperstimulation syndrome
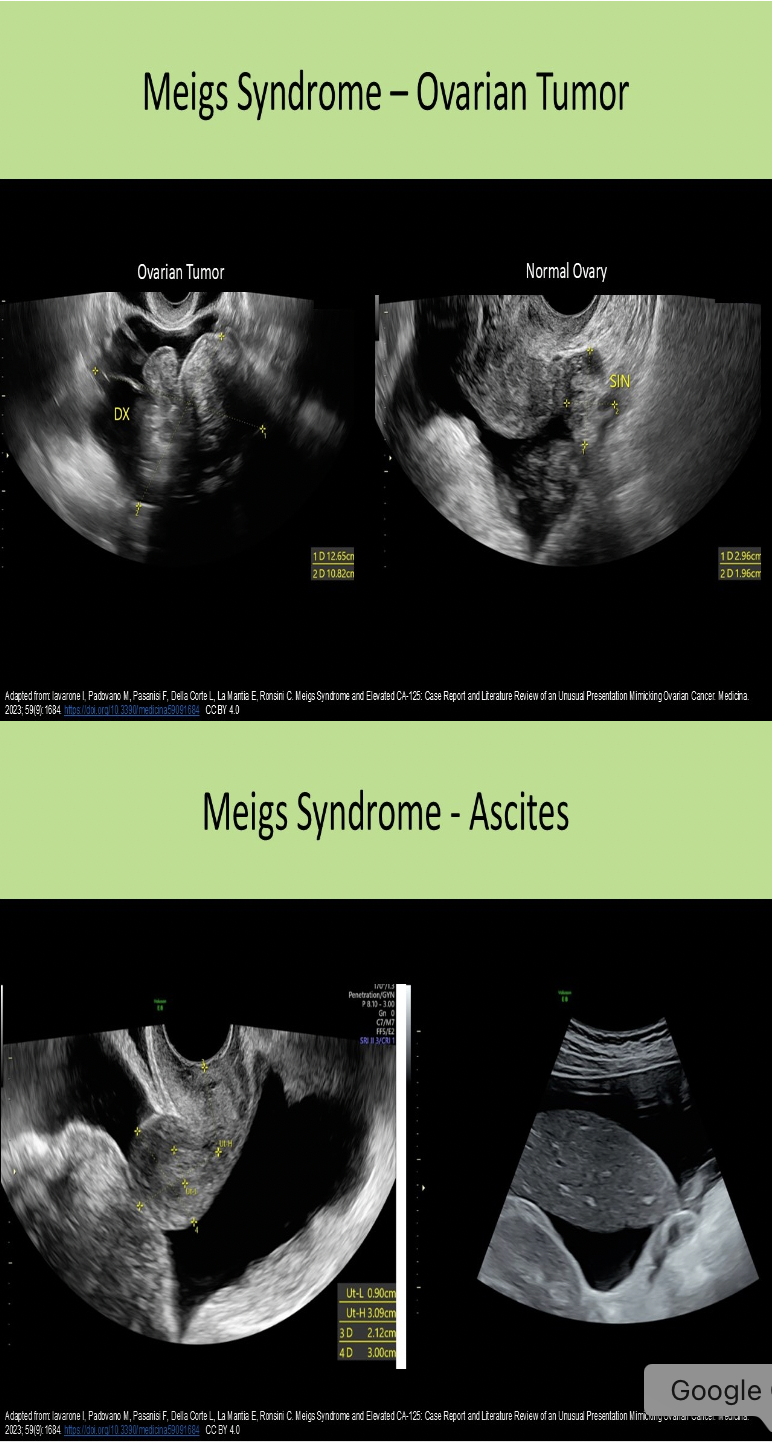
The image demonstrates ascites with fluid in the Morison pouch. It is a common finding with ovarian hyperstimulation syndrome, Meigs syndrome and Fitz Hugh Curtis syndrome.
Which of the following findings is most suggestive of cervical stenosis in a 64 year old female?
A. hydrosalpinx
B. hematometrocolpos
C. hydrometrocolpos
D. hydrometra
D. hydrometra
Cervical Stenosis refers to narrowing of the cervical canal. It can be caused by tumors, infection, polyps, scar tissue formation prior surgery or radiation therapy. In postemenopausal patients, fluid is retained in the endocervical canal. In premenopausal patients, it can cause amenorrhea and hematometra. Because the blockage is at the cervix, the vagina would not be dilated with fluid accumulation from the blockage = no hematometrocolpos or hydrometrocolpos.
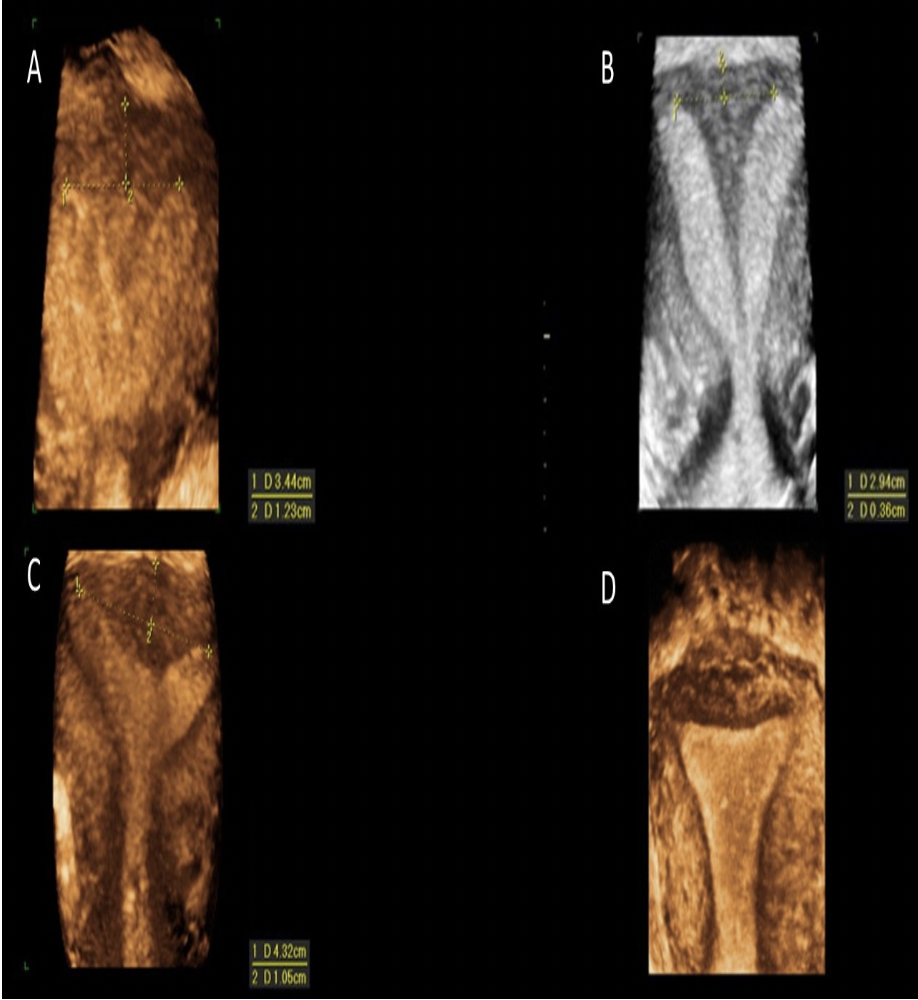
Which of the images demonstrates a subseptate uterus?
A
B
C
D
A
Image A: Subseptate uterus - note the distance measured from the cornual plane to the fundus is greater than 5mm. This measurement is used to differentiate a septate uterus (complete or partial) from a bicornuate uterus, The angle between the horns is also acute with a depth to the endometrium estimated at greater than 1.5 cm. This method is used to differentiate a septate and arcuate uterus.
Image B: Bicornuate Uterus - note the distance measured from the cornual plane to the fundus is less than 5mm. A septate uterus (complete or partial) has a greater than 5mm distance to the fundus and a bicornuate uterus has a less than 5mm distance to the fundus.
Image C: Arcuate Uterus - note the distance measured from the cornual plane to the fundus is greater than 5mm. This measurement is used to differentiate a septate uterus (complete or partial) from a bicornuate uterus, The angle between the horns is also obtuse with a depth to the endometrium estimated at less than 1.5 cm. This method is used to differentiate a septate and arcuate uterus.
Image D: Normal Uterus, no dip and rounded fundus
Which of the following ovarian neoplasms is composed of ectodermal tissues?
A. cystic teratoma
B. serous cystadenoma
C. mucinous cystadenoma
D. Brenner tumor
A. cystic teratoma
Ectodermal tissue refers to teeth, hair, bone tissue. A cystic teratoma (dermoid) is composed of a mixture of ectodermal tissue.
Virilization is associated with:
A. Krukenberg tumor
B. Androblastoma
C. Granular Cell tumor
D. Endometrioma
B. Androblastoma
Sertoli-Leydig Cell tumor AKA Androblastoma AKA Arrhenoblastoma is an ovarian tumor that secretes testosterone. The testosterone levels cause hirsutism, male pattern baldness, decreased breast size and deepening of the voice.
All of the following sonographic findings are associated with ovarian hyperstimulation syndrome, except?
A. ascites
B. pleural effusion
C. bilateral ovarian enlargement >5cm
D. increased echogenicity of the ovaries
D. increased echogenicity of the ovaries
Ascites and pleural effusion can be associated with ovarian hyperstimulation due to changes in blood characteristics and reduced renal filtration function. The ovaries are enlarged bilaterally (>5cm) with the formation of numerous cysts over 2cm.
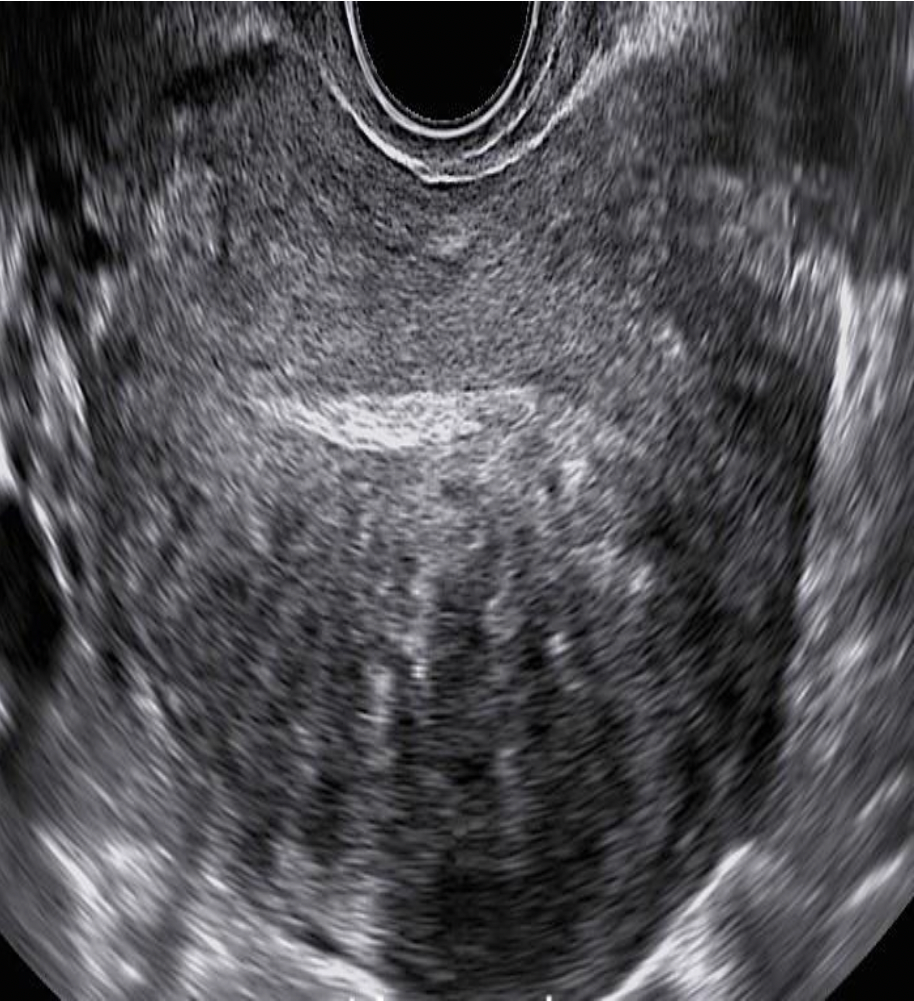
A 47yr old patient presents with menorrhagia and mild midline, lower pelvic pain. The findings on the image are most suggestive of:
A. fibroid formation
B. leiomyosarcoma
C. hydatidiform mole
D. adenomyosis
D. adenomyosis
Note the mottled appearance of the myometrium. Adenomyosis can lead to a swiss cheese appearance of the uterus with venetian blind-like shadowing. There is no distinct mass formation to indicate fibroid, which would have a more whirled appearance in the myometrium. A molar pregnancy would not typically cause menorrhagia.
Malignant germ cell tumors of the ovary:
A. demonstrate significantly reduced CA125 levels
B. are most commonly seen in patients 5-25yrs of age
C. cause significant pain, bleeding and thrombosis of the ovarian vein
D. are treated with methotrexate injections
B. are most commonly seen in patients 5-25yrs of age
Malignant Germ Cell Tumors arise from germ cells of ovary. They cause elevated CA125 levels. These tumors are most common in children and young adults age 5-25yrs. EX: Dysgerminoma, Endodermal Sinus Tumor, Solid Teratoma, Choriocarcinoma
________ and granulosa cell tumors are benign ovarian neoplasms that secrete estrogen.
A. Sertoli Leydig cell tumors
B. Fibromas
C. Thecomas
D. Mucinous cystadenomas
C. Thecomas
Which of the following is a common cause of abnormal uterine bleeding?
A. leiomyomas
B. hormone replacement therapy
C. polycystic ovarian syndrome
D. oral contraceptives
A. leiomyomas
Dysfunctional uterine bleeding (DUB) is caused by abnormalities in the endocrine system, while abnormal uterine bleeding (AUB) is caused by uterine lesions.
Which type of ovarian tumor is referred to as displaying the Sonographic "tip of the iceberg" sign due to a high fat/bony content?
A. Cystadenocarcinoma
B. Angiomyolipoma
C. Cystic teratoma
D. Brenner's tumor
C. Cystic teratoma
A dermoid cyst is usually composed of ectodermal tissues such as bone, hair and teeth causing a strong anterior reflection and posterior shadowing.
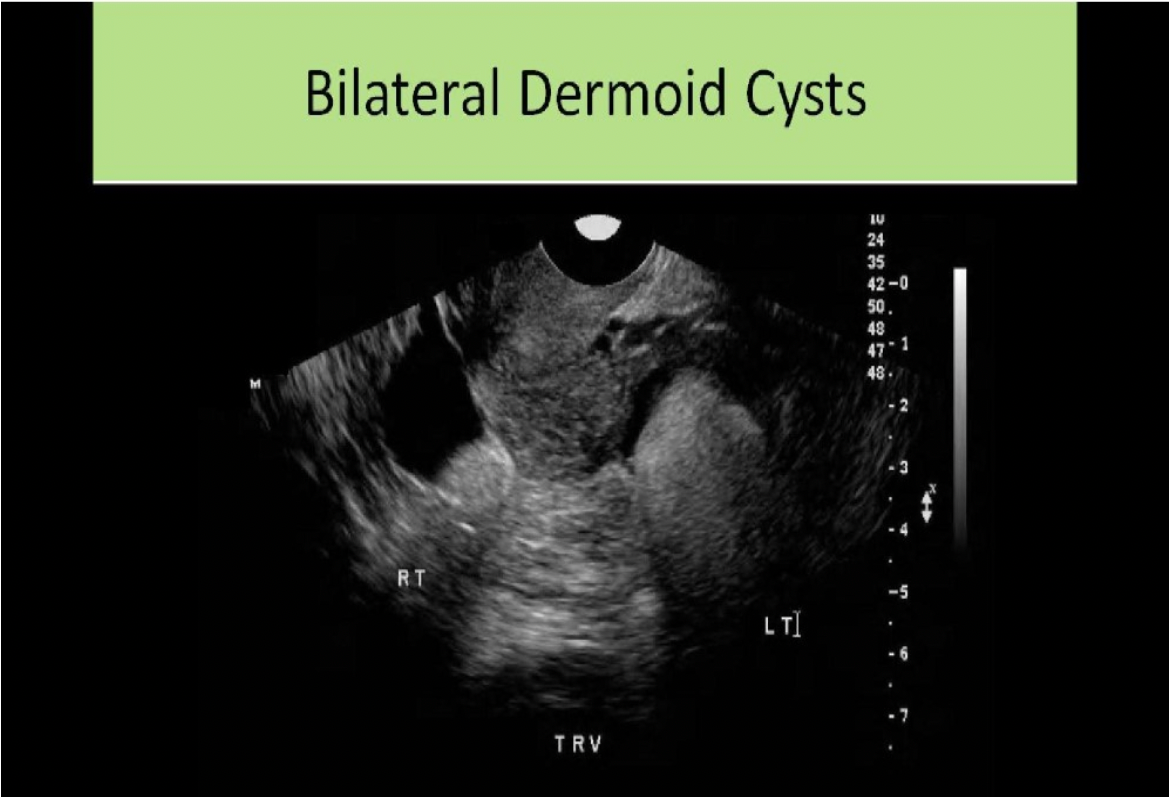
_______ syndrome refers to intrauterine adhesions of the endometrial lining caused by C-section or D&C.
A. DiGeorge
B. Fitz-Hugh-Curtis
C. Asherman
D. Mirizzi
C. Asherman
Asherman syndrome refers to intrauterine adhesions of the endometrial lining caused by C-section or D&C. It is related to reduced fertility and increased risk of miscarriage.
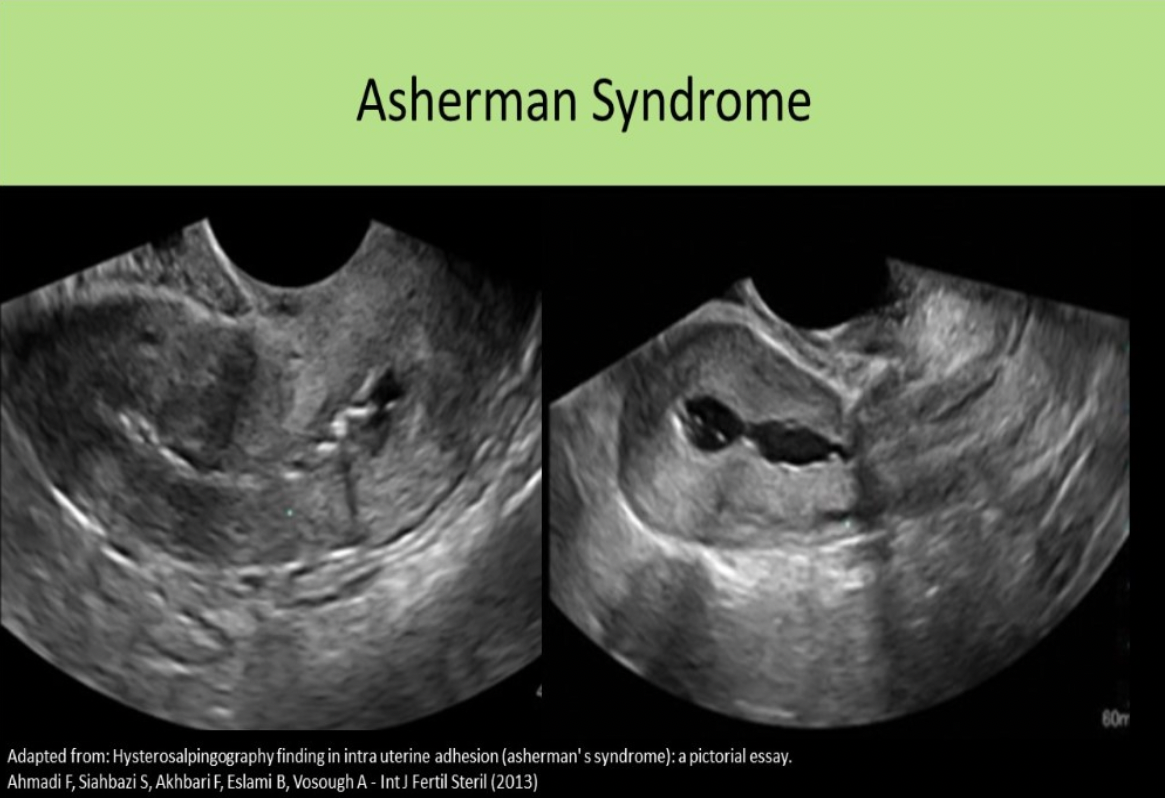
Which of the following is the leading cause of infertility?
A. sperm abnormalities
B. tubal damage from PID
C. endometriosis
D. anovulation
D. anovulation
Causes of infertility include Ovulation difficulties, Endometriosis, Fibroids, Tubal damage, Abnormal sperm, and IUD. Ovulatory difficulties are the most common cause.
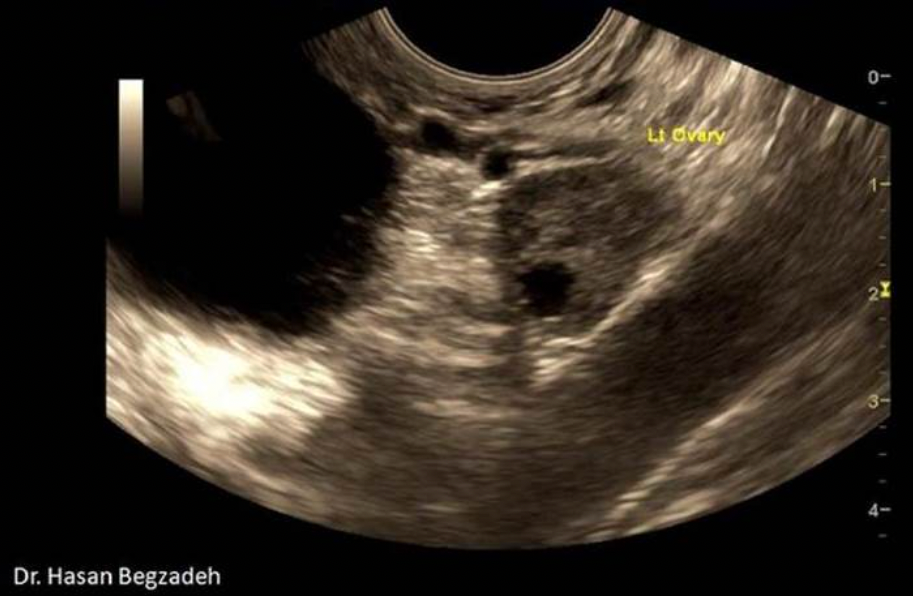
What is the round, anechoic structure demonstrated on the sagittal image of the left adnexa?
A. urinary bladder
B. large nabothian cyst
C. pedunculated leiomyoma
D. paraovarian cyst
D. paraovarian cyst
The image demonstrates a paraovarian cyst. A nabothian cyst would be found in the cervix. There is no visible uterine/cervical tissue surrounding the cyst. The bladder would demonstrate a thick muscular wall and would not normally be identified in this sagittal plane. A fibroid would appear as a hypoechoic mass with posterior shadowing
A 19yr old female presents for a pelvic ultrasound due to intermittent pelvic pain on the left side and abnormal menstrual cycles. She states she has had no recent sexual activity, but her last LMP was 10 weeks ago and she recently had a positive home pregnancy test. The ultrasound demonstrates a solid mass with cystic degeneration on the left ovary. These findings are most suggestive of:
A. Krukenberg tumor
B. serous cystadenocarcinoma
C. choriocarcinoma
D. mucinous cystadenocarcinoma
C. choriocarcinoma
Choriocarcinoma of the ovary is an aggressive malignancy most common in patient 5-25yrs of age. It causes elevated bhCG levels than can lead to a positive urine pregnancy test in a non-pregnant female. It can lead to precocious puberty in children. The mass formation is usually unilateral and very large. Both types of cystadenocarcinoma are primarily cystic with nodule formation and/or septations. Krukenberg tumors are solid, but usually bilateral.
Which of the following is not an expected finding with Fitz Hugh Curtis syndrome?
A. inflammation of the Glisson capsule
B. PID
C. peritonitis
D. Krukenberg tumor
D. Krukenberg tumor
Fitz Hugh Curtis syndrome involves a pelvic inflammatory disease that progresses into the right upper quadrant and the Glisson capsule. Ascites forms in the Morison pouch. Peritonitis can lead to the formation of perihepatic adhesions.
Ovarian malignancy:
A. is most commonly diagnosed at stage Ill or greater
B. requires monthly screening protocols for those with a family history
C. is the 2nd leading cause of cancer death in women
D. will cause decreased serum levels of CA125
A. is most commonly diagnosed at stage Ill or greater
Ovarian Cancer Facts:
6th leading cause of cancer death in women
Most women have stage Ill or greater when diagnosed
Postmenopausal ovaries should not exceed 2cm in any dimension or 8cc volume
Increased risk for ovarian cancer with echogenic foci in ovarian parenchyma
Screening performed annually for those with a family history
Elevated CA125 levels are commonly associated
Which of the following is associated with Asherman syndrome?
A. Elevated CA 125
B. Amenorrhea
C. Dysuria
D. Menometrorrhagia
B. Amenorrhea
Asherman Syndrome refers to adhesions of the endometrial lining due to uterine trauma.
Common symptoms include amenorrhea, hypomenorrhea, recurrent miscarriage and infertility.
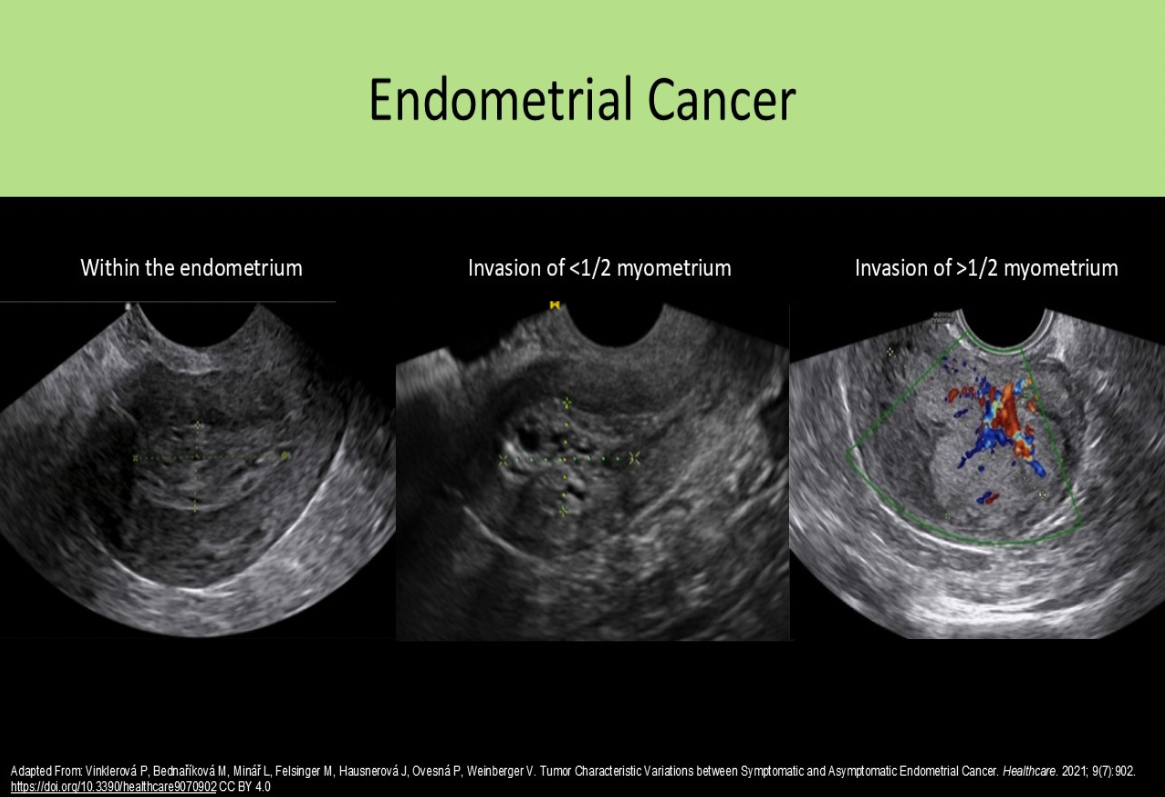
In stage I endometrial cancer, the cancer has invaded the:
A. pelvic lymph nodes
B. myometrium in the body of the uterus
C. ovaries
D. the cervix
B. myometrium in the body of the uterus
Stage 0 = precancerous cells
Stage | = confined to the body of the uterus (invades myometrium)
Stage Il = extends into the cervix
Stage Ill = extends into true pelvis
Stage IV = metastasis
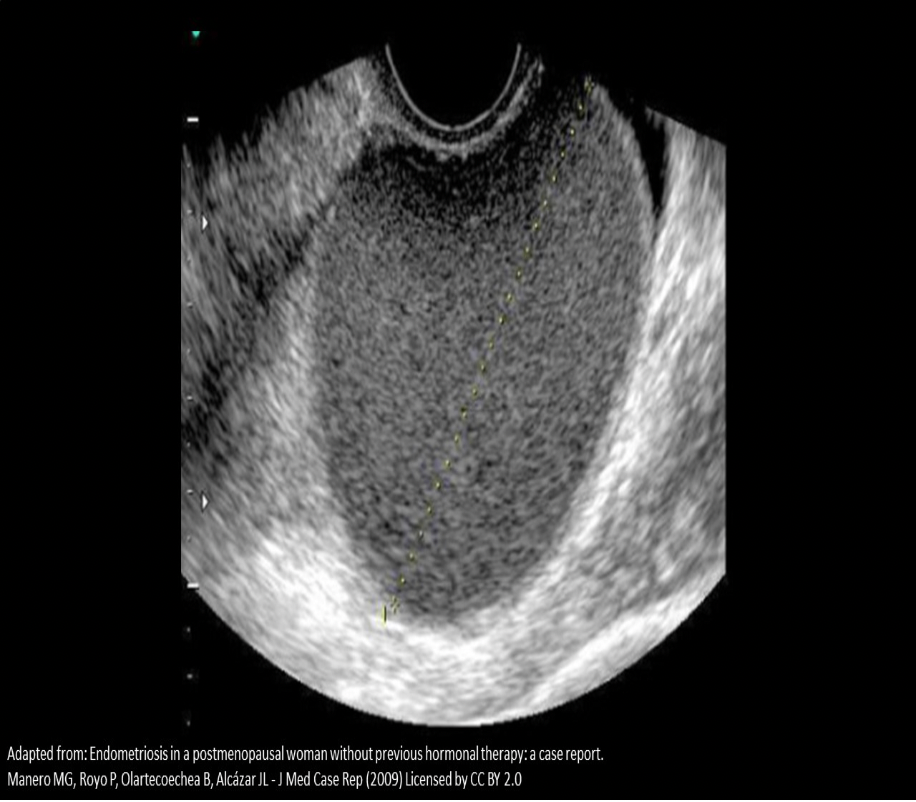
A 20 year old female complains of dysmenorrhea and menorrhagia. She states her menstrual cycle occurs every 28 days and her LMP was 21 days ago. The image displayed is from the transvaginal scan performed for this patient. Which of the following is the most likely diagnosis for the findings displayed?
A. Adenocarcinoma
B. Pyosalpinx
C. Endometrioma
D. Hematometrocolpos
C. Endometrioma
The image displays an endometrioma with homogeneous texture and mild posterior enhancement. Painful, heavy bleeding is also consistent with endometriosis.
Adenocarcinoma usually affects the uterus and cystadenocarcinoma affects the ovaries and has a complex appearance. Pyosalpinx would present as an infection and demonstrate fluid collections and debris levels in structures adjacent to the ovary.
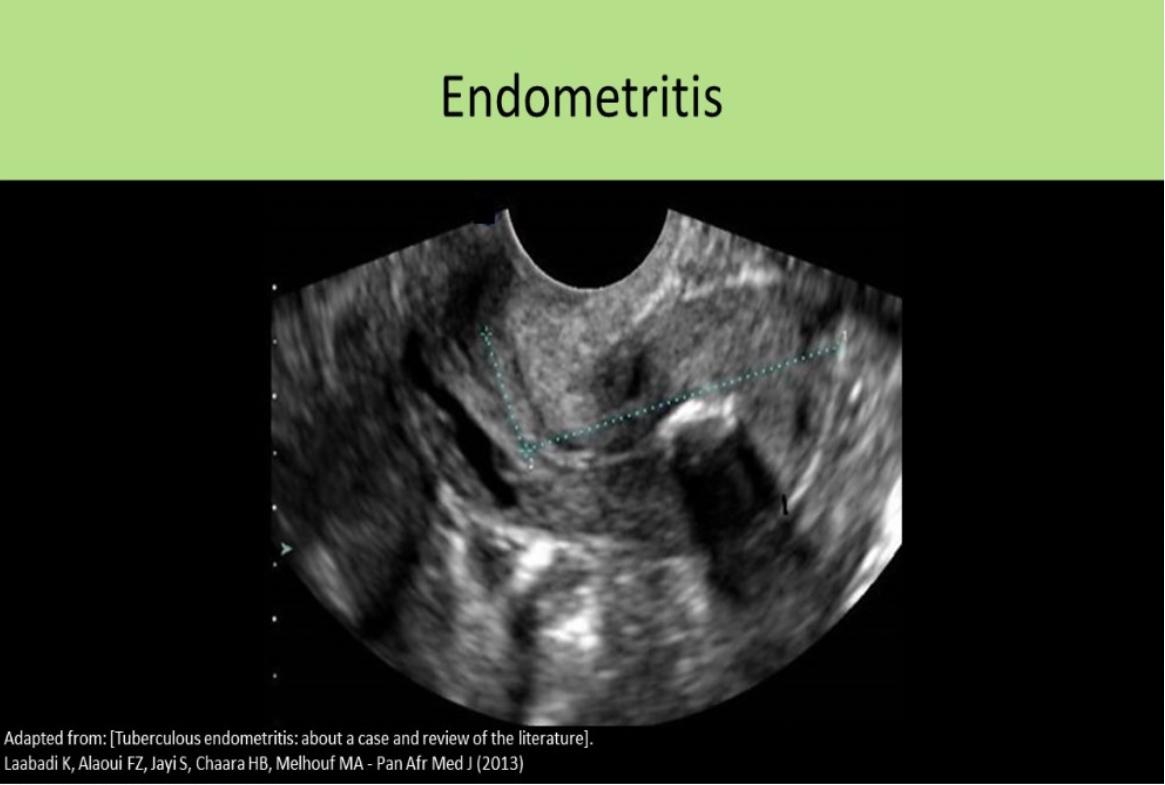
What is the first stage of PID that is identified sonographically?
A. Endometritis
B. Hydrosalpinx
C. Tubo-ovarian abscess
D. Pyosalpinx
A. Endometritis
4 Stages of PID: PID is an ascending infection, starts in uterus and moves upward into tubes/ovaries
Acute endometritis, endometrial fluid/debris/air, fluid in posterior cul-de-sac Acute salpingitis, fluid or pus within tubes, "shaggy" appearance of tube walls
Acute tubo-ovarian abscess
Chronic Infection
Which of the following is the most likely symptom of endometriosis?
A. menorrhagia
B. amenorrhea
C. menometrorrhagia
D. hypomenorrhea
A. menorrhagia
The ectopic endometrial tissue will follow the same hormonal cycle as the normal endometrium. Most patients exhibit regular cycles but have very heavy and painful menses = menorrhagia. Hypomenorrhea indicates lighter menses and amenorrhea indicates absent menses. Menometrorrhagia indicates irregular cycles with heavy bleeding.
Which of the following is a part of Meigs syndrome?
A. leiomyomas and hydronephrosis
B. renal agenesis
C. ascites and pleural effusion
D. ascites, pleural effusion and scalp edema
C. ascites and pleural effusion
Meigs syndrome = pelvic ascites and pleural effusion with benign ovarian tumor, most commonly a fibroma
Which of the following patients has the highest risk of developing pyometra?
A. 15 yr old female with an imperforate hymen
B. 40 year old female with fibroids
C. 70 year old female with uterine adenocarcinoma
D. 24 year old female with an IUD
C. 70 year old female with uterine adenocarcinoma
Pyometra refers to the accumulation of pus in the uterine cavity. The median age of presentation is 65 years. Most cases are in postmenopausal females with underlying uterine/endometrial malignancy. Other less common causes include foreign bodies, puerperal infections or uterine anomalies. Symptoms include purulent vaginal discharge and pelvic pain. It can lead to uterine rupture and peritonitis. Treatment involves removing the pus by drainage through the cervix and antibiotics. Any associated malignancy would need to be treated separately.
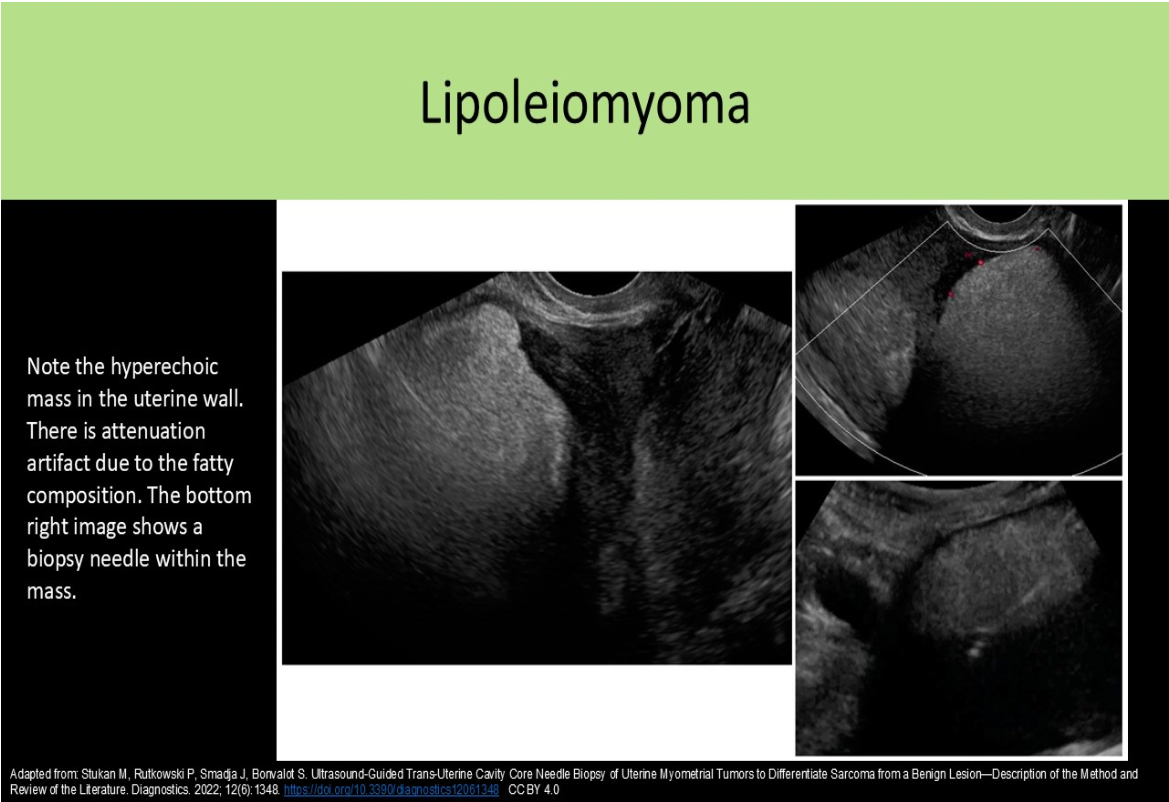
A lipoleiomyoma will be hyperechoic to the myometrium due to increased levels of:
A. connective tissue
B. fatty tissue
C. ectodermal tissue
D. striated muscle tissues
B. fatty tissue
Lipoleiomyomas form due to degeneration of smooth muscle cells in a leiomyoma. The symptoms are similar to leiomyomas of the same size and location. Sonographic findings include: Hyperechoic fatty mass with a partially hypochoic muscular rim, Posterior acoustic attenuation
What is the most common cause for pelvic inflammatory disease?
A. poor hygiene
B. bladder infection
C. chlamydia
D. tuberculosis
C. chlamydia
Which of the following is a failure of fusion defect of the uterus that is commonly associated with ipsilateral renal agenesis?
A. arcuate uterus
B. bicornuate uterus
C. septate uterus
D. imperforate hymen
B. bicornuate uterus
A bicornuate uterus is failure of fusion defect. The two mullerian ducts do not fuse properly and there are two separate uterine tracts with a bicornuate uterus. 80% of cases of bicornuate uterus are associated with renal defects, typically ipsilateral agenesis. An arcuate uterus and septate uterus are failure of dissolution/resorption defects. Most uterine defects are associated with abnormal developments in the urinary system.
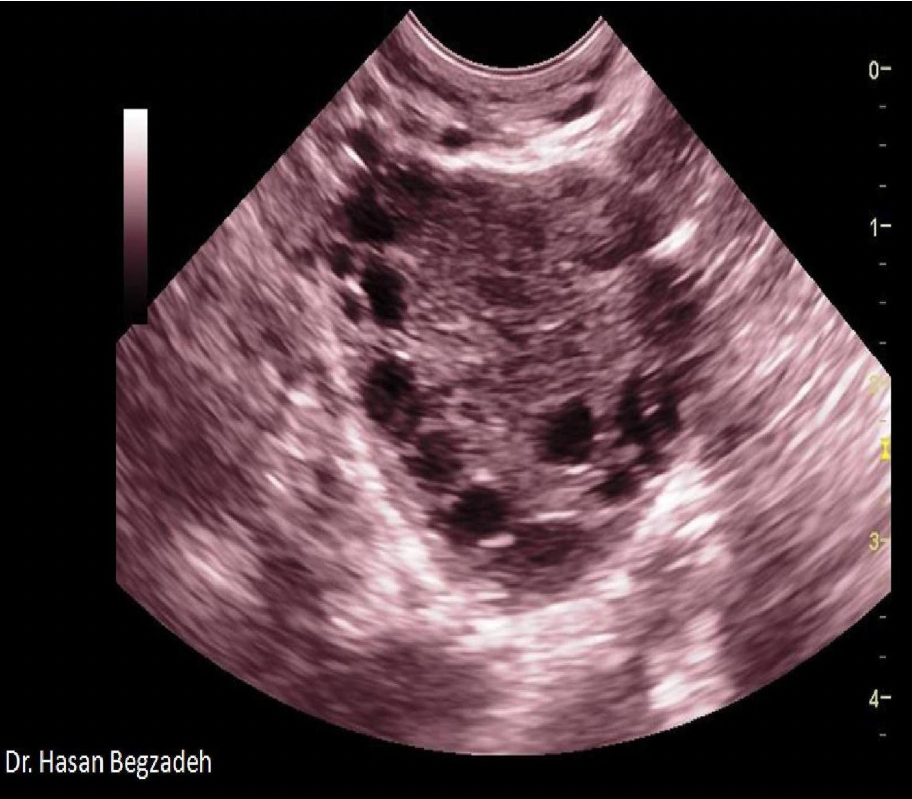
All of the following are associated symptoms/complications related to the findings displayed on the image, except:
A. Infertility
B. Hirsutism
C. Alopecia
D. Amenorrhea
C. Alopecia
Polycystic ovarian disease is demonstrated on the image. Note the "string of pearls" formation of the follicles along the rim of the ovary. Alopecia refers to the loss of hair from the body and has not been associated with PCOD.
Acute ovarian torsion:
A. will present as an atrophied ovary with no of blood flow detected by color Doppler
B. is most common in postmenopausal patients
C. is associated with large, pedunculated leiomyomas
D. is considered a critical finding that requires immediate intervention
D. is considered a critical finding that requires immediate intervention
The ovary will enlarge in the acute phase of torsion due to obstructed outflow. Complete torsion will demonstrate an absence of blood flow in the ovary. Ovarian torsion is considered a critical finding that requires immediate intervention. It most commonly occurs in pediatric patients. Ovarian hyperstimulation syndrome and ovarian tumors increase the risk of torsion.
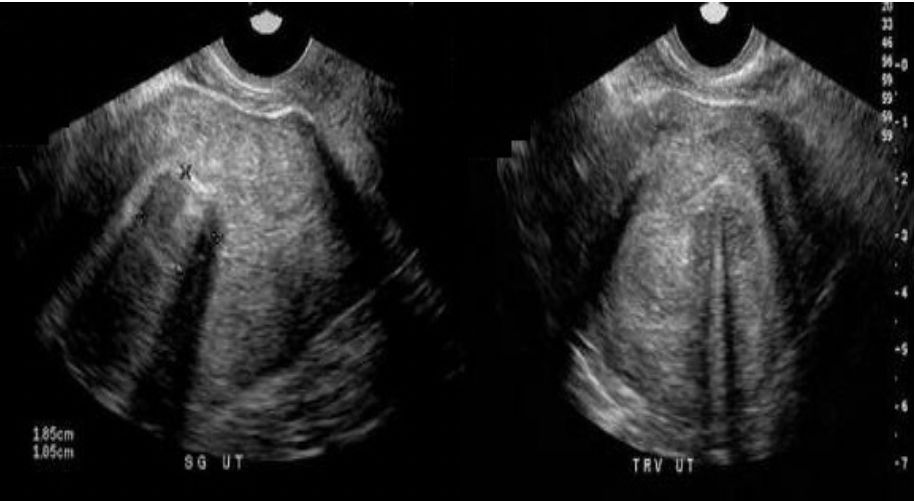
What type of fibroid is seen in the image displayed?
A. Intramural
B. Submucosal
C. Subserosal
D. Pedunculated
B. Submucosal
The fibroid has formed just beneath the endometrial layer of the uterus which is referred to as submucosal. Fibroids that form within the muscle wall layer are termed intramural fibroids. If the fibroid forms just beneath the outer uterine layer it is referred to as a subserosal fibroid. Least commonly, pedunculated fibroids form adjacent to the uterus and are only attached with a small stalk.
Which of the following maternal abnormalities can be caused by a large fibroid uterus?
A. hydronephrosis
B. gestational diabetes
C. systemic HTN
D. pulmonary vein dilatation
A. hydronephrosis
The uterus can cause extrinsic compression of the distal ureters which causes hydronephrosis.
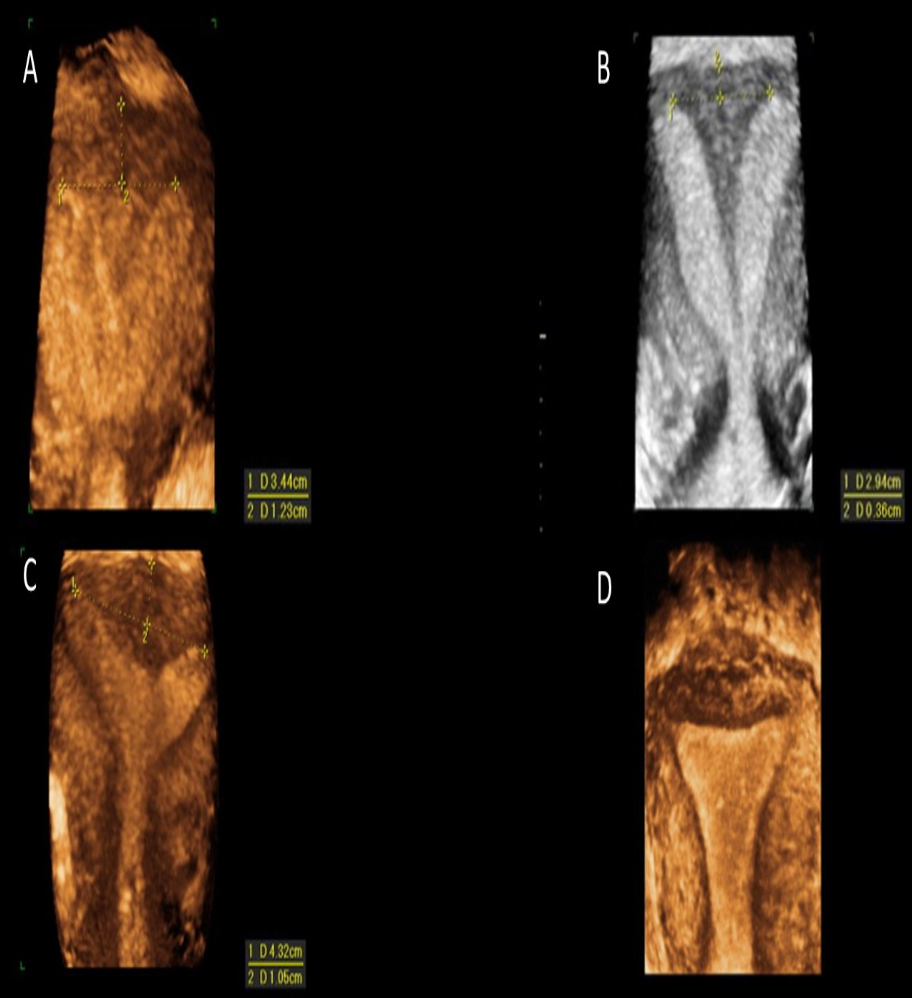
Which of the images demonstrates an arcuate uterus?
A
B
C
D
C
Image A: Subseptate uterus - note the distance measured from the cornual plane to the fundus is greater than 5mm. This measurement is used to differentiate a septate uterus (complete or partial) from a bicornuate uterus, The angle between the horns is also acute with a depth to the endometrium estimated at greater than 1.5 cm. This method is used to differentiate a septate and arcuate uterus.
Image B: Bicornuate Uterus - note the distance measured from the cornual plane to the fundus is less than 5mm. A septate uterus (complete or partial) has a greater than 5mm distance to the fundus and a bicornuate uterus has a less than 5mm distance to the fundus.
Image C: Arcuate Uterus - note the distance measured from the cornual plane to the fundus is greater than 5mm. This measurement is used to differentiate a septate uterus (complete or partial) from a bicornuate uterus, The angle between the horns is also obtuse with a depth to the endometrium estimated at less than 1.5 cm. This method is used to differentiate a septate and arcuate uterus.
Image D: Normal Uterus, no dip and rounded fundus
A patient presents for a first trimester scan due to an enlarged uterus and right ovary on clinical exam. The uterus demonstrates a molar pregnancy. Which of the following is an expected ovarian finding?
A. thecoma
B. dermoid cyst
C. theca lutein cyst
D. androblastoma
C. theca lutein cyst
Theca lutein cysts are associated with increased levels of hCG in the blood. Molar pregnancy causes excessive levels of hCG in the blood.
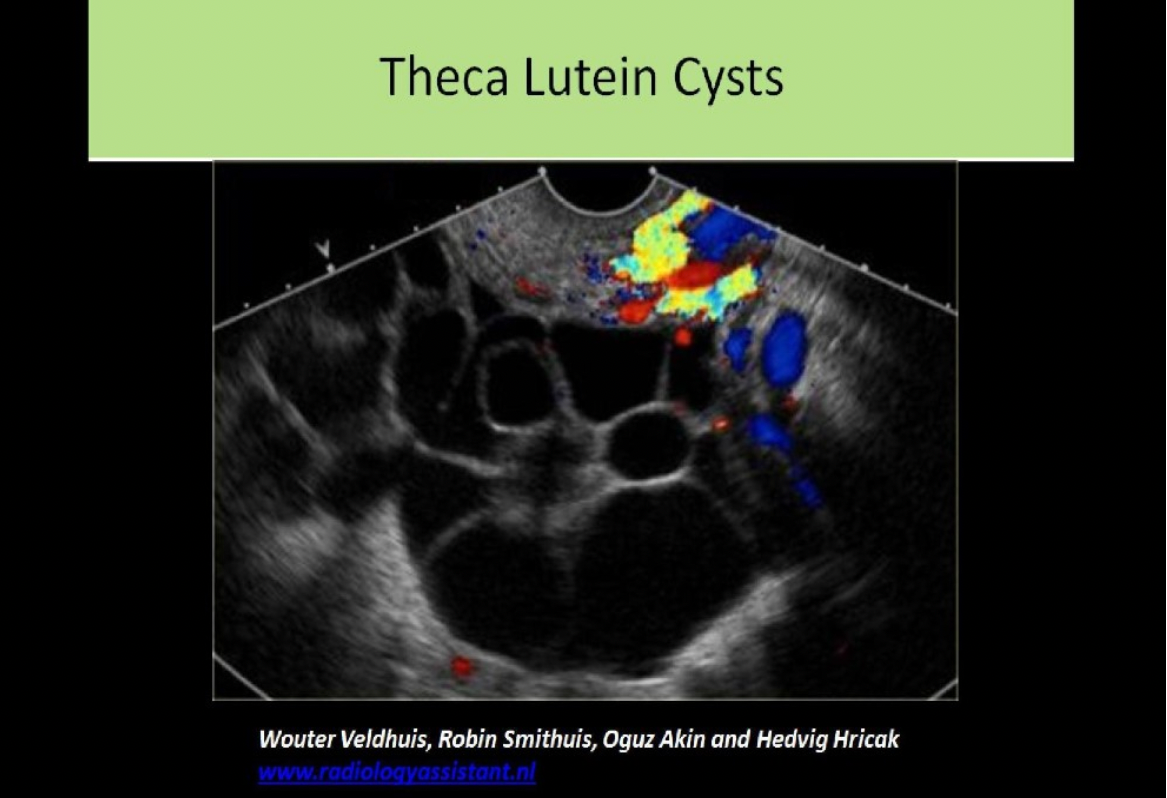
Hydrosalpinx and pyosalpinx are differentiated from pelvic veins using:
A. graded compression
B. harmonic imaging
C. color Doppler
D. water enema
C. color Doppler
Hydrosalpinx and pyosalpinx are differentiated from pelvic veins using color Doppler.
Hydrosalpinx and pyosalpinx are differentiated from bowel loops by visualizing peristalsis within the bowel.
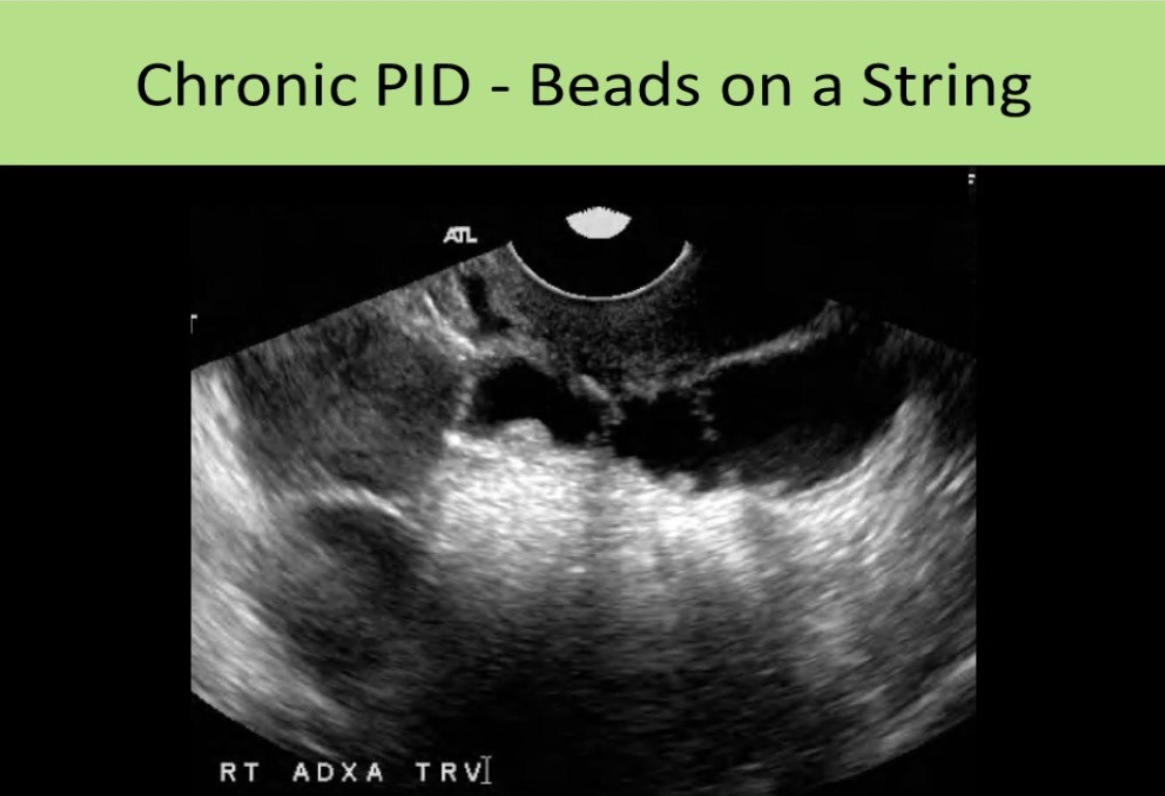
Which of the following is a common sonographic sign of acute PID?
A. beads on a string sign
B. cogwheel sign
C. thin walled, anechoic avascular adnexal structure
D. ≤5mm wall thickness of the fallopian tube
B. cogwheel sign
4 Stages of PID:
Stage 1: Acute endometritis
Stage 2: Acute salpingitis - thick-walled with acute infection (>5mm); Cogwheel sign, free fluid in pelvis
Stage 3: Acute tubo-ovarian abscess
Stage 4: Chronic Infection: hydrosalpinx with thin-walled fallopian tube (<5mm); Beads-on-a-String sign
A patient presents for an ultrasound due to the uterine size not matching the high levels of bhCG for expected age of the pregnancy. The uterus is enlarged with a heterogeneous mass in the uterine cavity that appears to have invaded the uterine wall into the peritoneum. The pelvic nodes appear normal and the liver is clear. These findings are most consistent with:
A. retained products of conception
B. hydatidiform mole
C. chorioadenoma destruens
D. choriocarcinoma
C. chorioadenoma destruens
A hydatidiform mole is contained within the uterus. Chorioadenoma destruens refers to an invasive malignant molar pregnancy. The mass of abnormal tissue will usually only invade the uterus and surrounding pelvic structures. Choriocarcinoma can have the same heterogeneous appearance but normally spreads through the uterus and metastasizes to the liver.
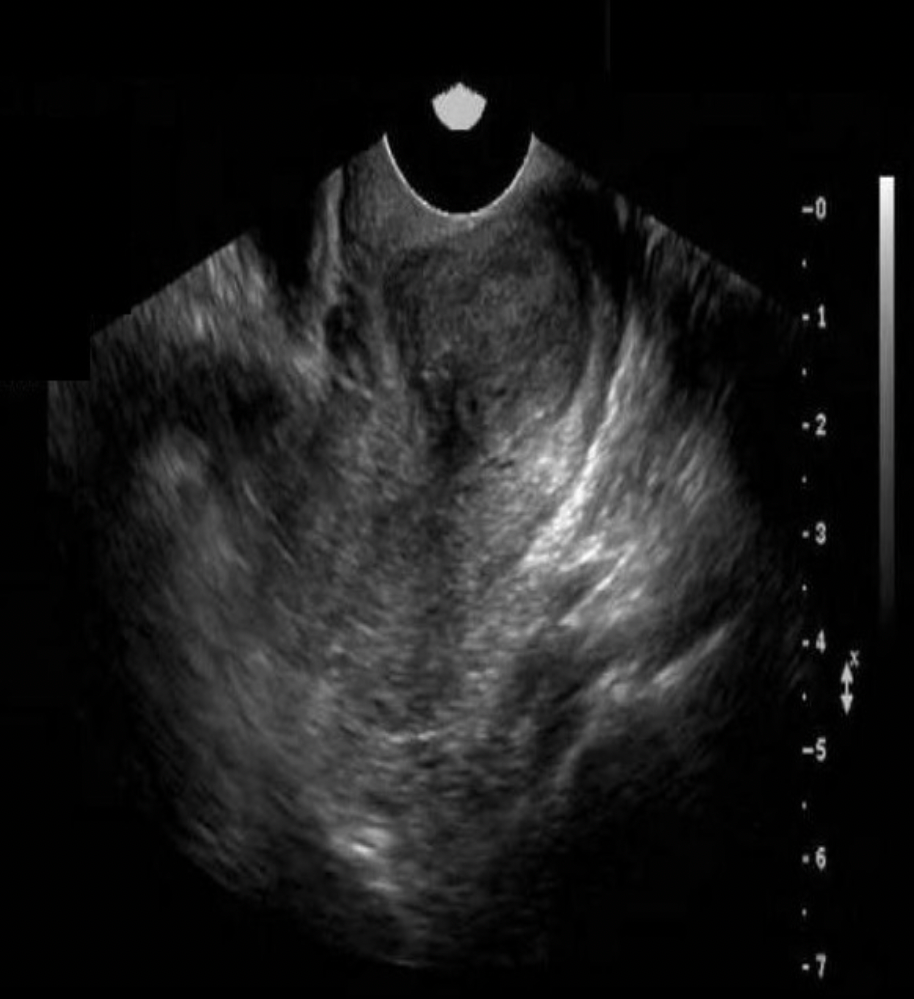
A 30yr old patient presents with pelvic pressure and dyspareunia for a pelvic ultrasound. She had a partial hysterectomy 1 yr ago. Which of the following statements best describes the findings displayed?
A. There is a solid mass in the cervix, most likely carcinoma.
B. A large complicated nabothian cyst is present.
C. There is a large chronic hematoma remaining in the cervix.
D. There has been fibroid formation within the remaining uterine tissue left behind unintentionally.
A. There is a solid mass in the cervix, most likely carcinoma.
The solid mass is too homogeneous to be a fibroid forming in the remaining tissues. A hematoma and a nabothian cyst would both present with a different appearance and varying enhancement. The image displays a solid tumor related to cervical carcinoma.
Which of the following is a common sonographic sign of chronic PID?
A. cogwheel sign
B. beads on a string sign
C. endometritis
D. tubular, thick walled, hypervascular adnexal structure
B. beads on a string sign
Chronic PID: hydrosalpinx, thin-walled fallopian tube (<5mm)
Beads-on-a-String sign - remnants of the endosalpingeal folds demonstrate multiple 2-3mm nodules that project into the lumen
A peritoneal inclusion cyst may also be seen as a loculated fluid collection surrounding the uterus and ovaries.
Hydrosalpinx and pyosalpinx are differentiated from pelvic veins using color Doppler.
Hydrosalpinx and pyosalpinx are differentiated from bowel loops by visualizing peristalsis within the bowel.
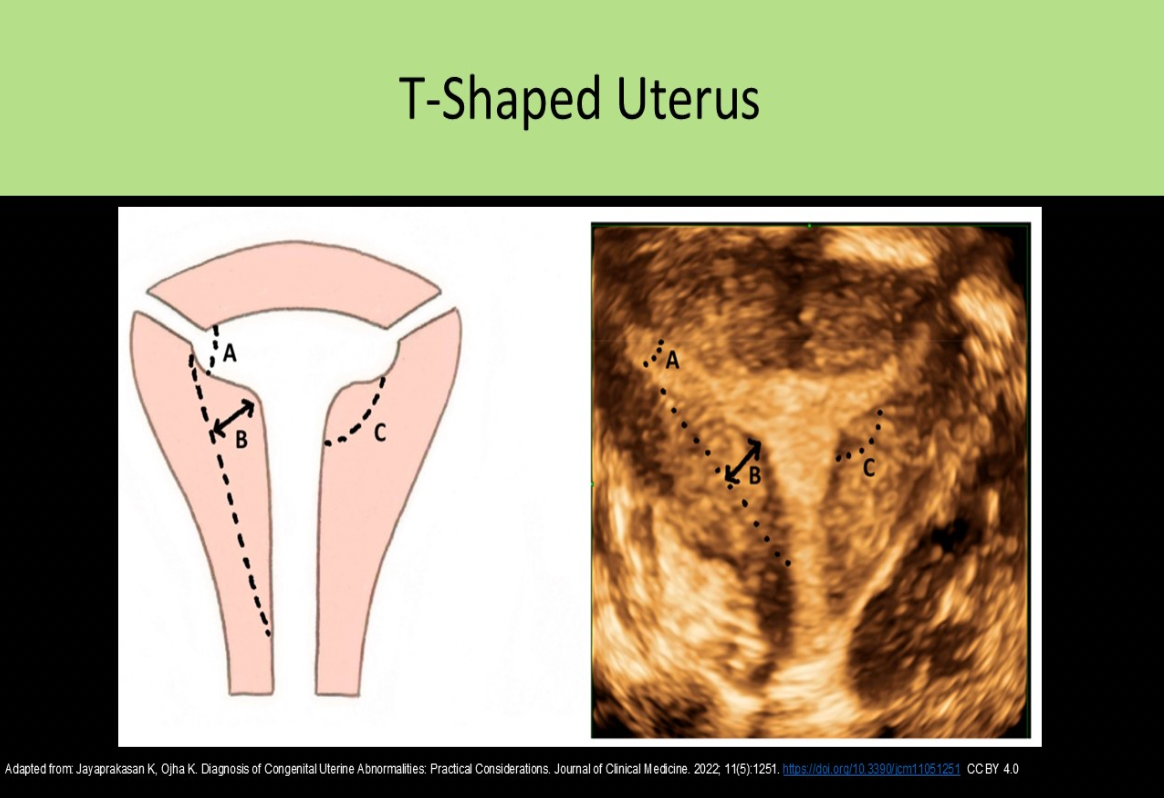
A T-shaped uterus is most commonly associated with:
A. personal exposure to diethylstilbestrol
B. personal history of smoking
C. maternal exposure to diethylstilbestrol
D. maternal alcohol abuse
C. maternal exposure to diethylstilbestrol
Women took diethylstilbestrol to prevent spontaneous abortion 1940 - 1960. Daughters of these women have demonstrated uterine anomalies including a T-shaped uterus.
Which of the following can cause fibroid enlargement or endometrial thickening in a postmenopausal patient?
A. ovarian thecoma
B. ovarian theca lutein cyst
C. cessation of Tamoxifen treatment
D. cessation of estrogen replacement therapy
A. ovarian thecoma
Ovarian thecomas produce estrogen and if present in a postmenopausal patient, they could cause vaginal bleeding. The estrogen levels can also cause fibroids to grow.
Tamoxifen and ERT cause bleeding in postmenopausal women. Stopping the therapy would reduce the chances of PM bleeding. Theca lutein cysts are associated with high hCG levels.
______ is the msot common adnexal mass
A. dermoid
B. serous cystadenocarcinoma
C. fibroid
D. ovarian cyst
D. ovarian cyst
An ovarian cyst is the most common adnexal mass. The cystic teratoma(dermoid) is the most common solid ovarian tumor.
Risk factors associated with leiomyosarcoma include nulliparity, obesity, prior history of pelvic radiation and:
A. recurrent pelvic inflammatory disease
B. prior C-section
C. tamoxifen use
D. polycystic ovarian disease
C. tamoxifen use
Leiomyosarcoma is a rare, malignant tumor of myometrium. They are usually found in females in their mid 50s. Other risk factors include nulliparity, obesity, radiation therapy and tamoxifen use. The symptoms are very similar to a benign leiomyoma. they are very hard to differentiate from benign leiomyoma sonographically. They do demonstrate a rapid increase in size with degenerative changes and internal necrosis. They are typically an intramural mass with blurred borders due to infiltration. The pelvic region should be evaluated for metastasis and lymphadenopathy.
Which of the following is the most commonly occurring germ cell tumor of the ovary?
A. embryonal cell carcinoma
B. benign cystic teratoma
C. yolk sac tumor
D. malignant dysgerminoma
B. benign cystic teratoma
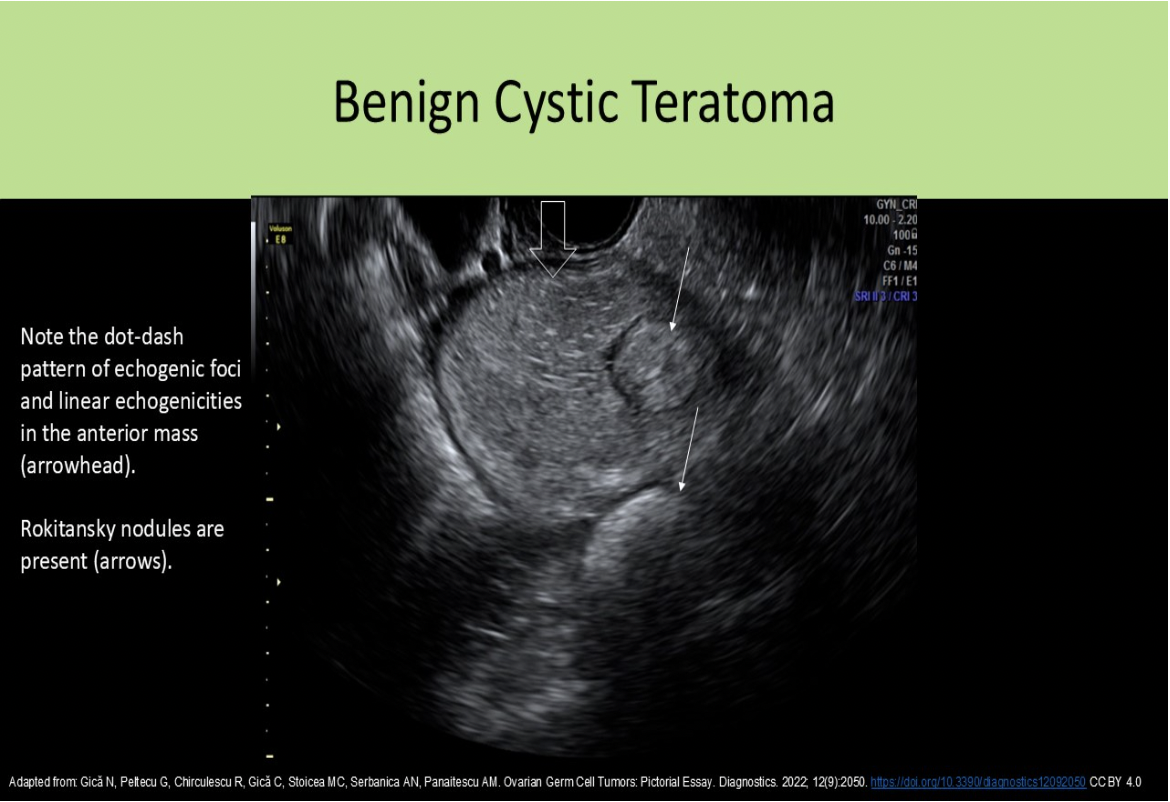
Blood in the fallopian tubes is called _____ and pus in the fallopian tubes
is called ______
A. hydrosalpinx, hematometrocolpos
B. hydrosalpinx, pyometra
C. hematosalpinx, pyosalpinx
D. hematometrocolpos, pyometra
C. hematosalpinx, pyosalpinx
Hydrosalpinx - fluid in the fallopian tubes
Hematosalpinx - blood in the fallopian tubes
Pyosalpinx - pus in the fallopian tubes
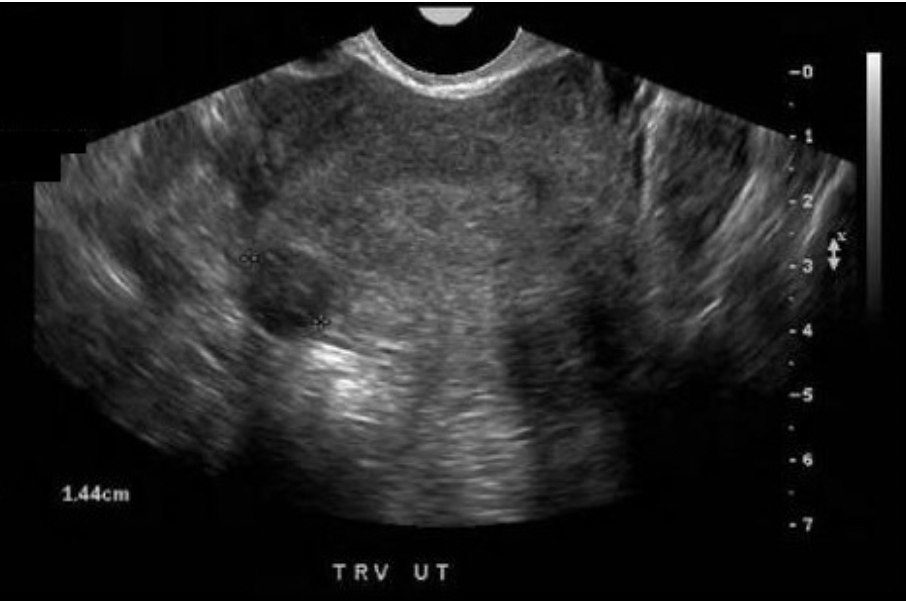
What type of fibroid is seen on the image displayed?
A. submucosal
B. pedunculated
C. intramural
D. subserosal
D. subserosal
A fibroid that has formed just beneath the endometrial layer of the uterus is referred to as submucosal. Fibroids that form within the muscle wall layer are termed intramural fibroids. If the fibroid forms just beneath the outer uterine layer it is referred to as a subserosal fibroid. Least commonly, pedunculated fibroids form adjacent to the uterus and are only attached with a small stalk.
A/an ______ is a type of germ cell malignancy of the ovary, while a _______ is an epithelial-stromal malignancy of the ovary.
A. Dysgerminoma, Serous Cystadenocarcinoma
B. Endometrioid Tumor, Dysgerminoma
C. Serous Cystadenocarcinoma, Mucinous Cystadenocarcinoma
D. Mucinous Cystadenocarcinoma, Serous Cystadenocarcinoma
A. Dysgerminoma, Serous Cystadenocarcinoma
Most ovarian malignancies originate from the epithelial-stromal tissues. Serous-cystadenocarcinoma, Mucinous Cystadenocarcinoma, Endometrioid, Transitional cell, and Clear cell tumors are epithelial-stromal tumors. Dysgerminoma is a germ cell tumor of the ovary.
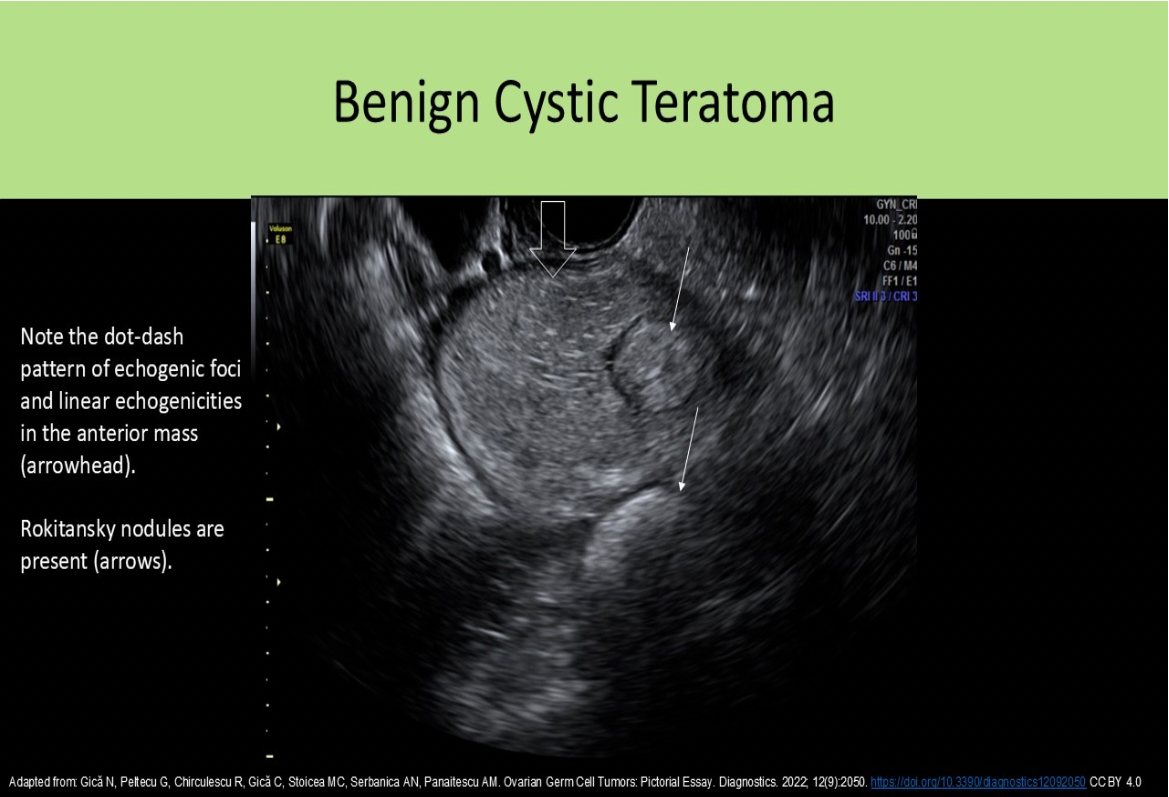
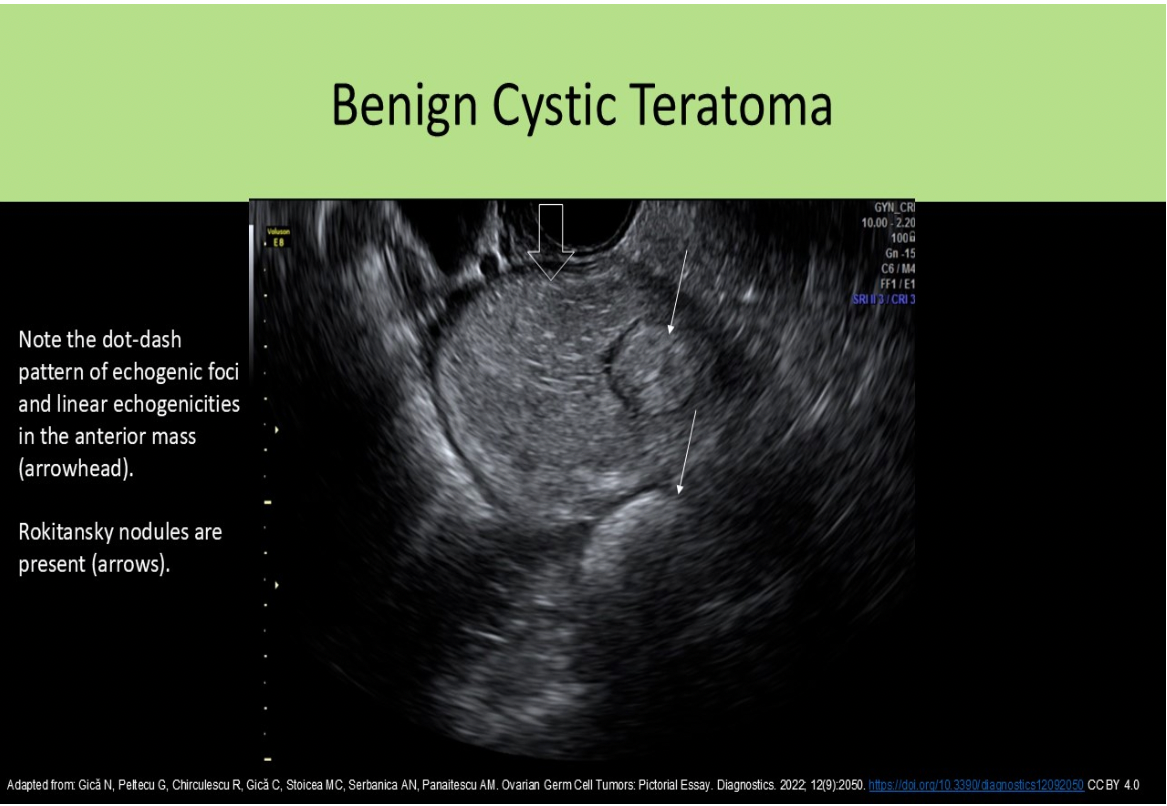
A Rokitansky nodule is commonly identified with what type of pelvic mass?
A. serous cystadenoma
B. focal adenomyosis
C. mucinous cystadenoma
D. cystic teratoma
D. cystic teratoma
A Rokitansky nodule is another term used to describe the dermoid plug.
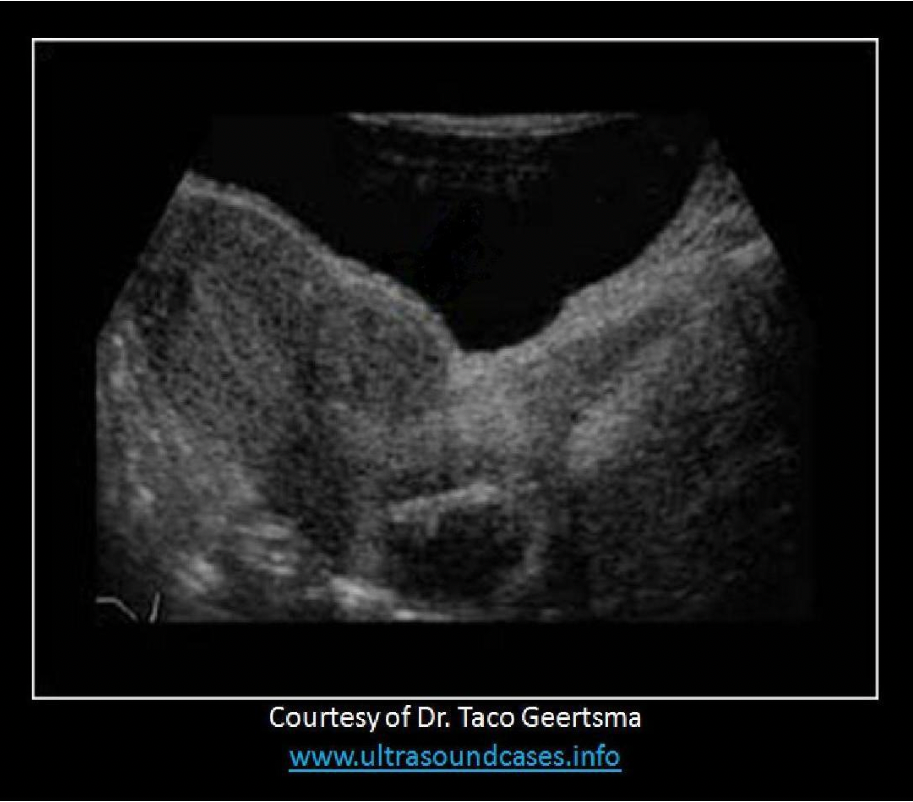
A patient presents with irregular bleeding and pelvic pain for the last two months. Which of the following statements best describes the image displayed?
A. There is a submucosal fibroid present.
B. There are multiple fibroids present in the body of the uterus and cervix.
C. There is a subserosal fibroid present with an IUD in the uterine cervix
D. There is a tampon present in the cervix
C. There is a subserosal fibroid present with an IUD in the uterine cervix
The hypochoic mass with shadowing in the anterior uterus is consistent with a fibroid. The fibroid is located just beneath the outer layer of the uterine wall which indicates a subserosal fibroid. The echogenic linear structure with shadowing located in the cervix is consistent with an IUD that is displaced.
What is the most common uterine mass/tumor?
A. Endometrial polyp
B. Leiomyoma
C. Brenner tumor
D. Serous Cystadenoma
B. Leiomyoma
Fibroids are the most common acquired uterine abnormality
Which of the following ovarian tumors is commonly a part of Meigs Syndrome?
A. cystadenoma
B. androblastoma
C. fibroma
D. teratoma
C. fibroma
Meigs syndrome = pelvic ascites and pleural effusion with benign ovarian tumor (fibroma 80-90%, thecoma, granulosa cell tumor)
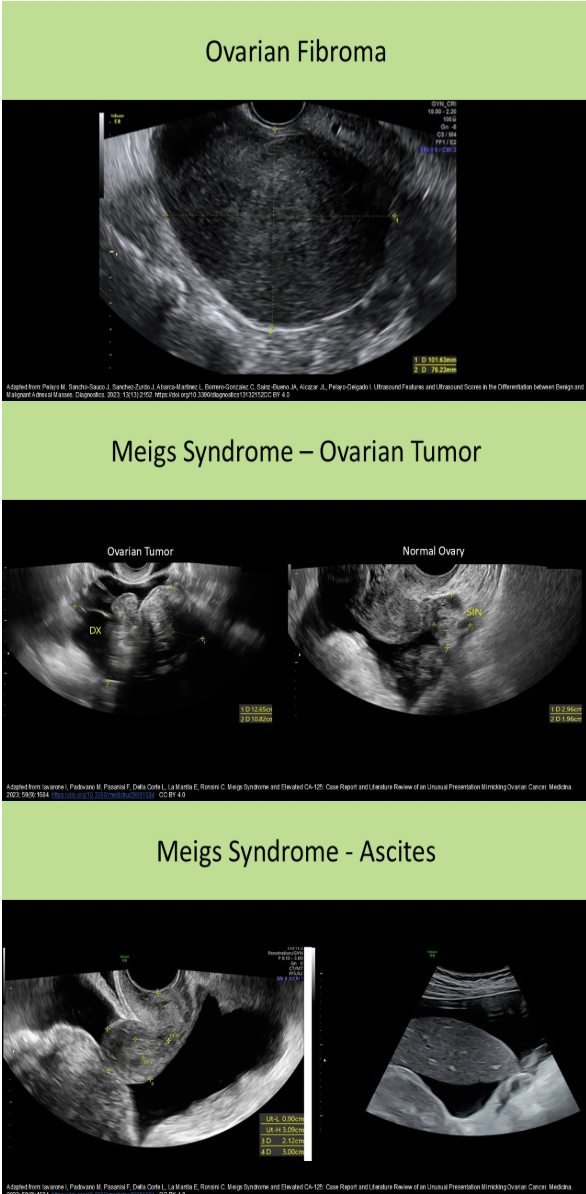
Which of the following ovarian tumors most commonly occurs in the postmenopausal woman?
A. Sertoli-Leydig cell tumor
B. Teratoma
C. Serous Cystadenoma
D. Granulosa Cell tumor
D. Granulosa Cell tumor
Most Common in Premenopausal - Cystic Teratoma (Dermoid Cyst), Serous Cystadenoma, Mucinous Cystadenoma, Sertoli-Leydig cell tumor
Most Common in Postmenopausal - Granulosa Cell Tumor (Theca Luteal Cell Tumor), Thecoma, Fibroma,
A 50 yr old female presents for a pelvic ultrasound after ascites was identified on an upper abdominal exam. A thin walled, multiloculated cystic ovarian mass with papillary projections is identified in the right ovary. The left ovary and uterus are unremarkable.
These findings are most suggestive of:
A. theca lutein cyst
B. Krukenberg tumor
C. dysgerminoma
D. serous cystadenocarcinoma
D. serous cystadenocarcinoma
A serous cystadenocarcinoma is the malignant version of the serous cystadenoma. The malignant multiloculated cystic mass usually demonstrates internal nodules or papillary projections. Ascites is also a common finding with these malignant pelvic tumors.
Most primary malignancies of the ovary originate in the
A. lateral region of the ovary
B. space between the fimbriae of the fallopian tube and the ovary
C. medulla tissues
D. epithelial-stromal tissues
D. epithelial-stromal tissues
Most primary malignancies of the ovary originate in the epithelial-stromal tissues. Serous, Mucinous, Endometrioid, Transitional cell and clear cell tumors are epithelial-stromal tumors.
The evaluation of IUD placement in the uterine cavity includes the measurement of:
A. the thickness of the device
B. the distance from the IUD to the uterine fundus
C. the span of the wings of the device
D. the distance to the uterine cornua on both sides
B. the distance from the IUD to the uterine fundus
Sonographic Evaluation of IUD Placement: Endovaginal and 3D ultrasound are preferred
. Demonstrate the length of the device within the endometrial cavity
. Measure the distance from the device to the uterine fundus
. Document the orientation of the IUD to the long axis of the uterus
. Image both arms/wings of the device
. Document the arms/wings are at 90-degree angle to the shaft
. Locate the retrieval string position
. LNG-IUD should demonstrate mildly echogenic arms/wings with an echogenic shaft
. Copper IUD should demonstrate 2 parallel strongly echogenic structures with
posterior shadowing and reverberation artifacts
. The retrieval string should appear as an echogenic linear structure
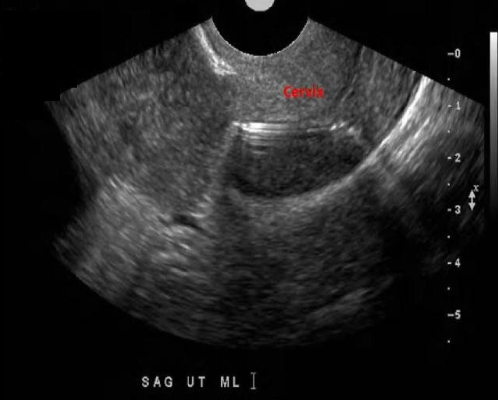
The image of the cervix demonstrates which of the following?
A. Normal cervix with echogenic area due to perpendicular incidence with two layers of the cervical canal
B. Normal cervix with abnormal placement of an IUD
C. Normal cervix with normal placement of an IUD
D. Normal cervix with tampon inserted
B. Normal cervix with abnormal placement of an IUD
The echogenic linear structure within the cervix is consistent with an IUD. The uterine fundus is the correct location for the IUD.
What is the most common cause for postmenopausal bleeding?
A. endometrial hyperplasia
B. endometrial adenocarcinoma
C. fibroids
D. endometrial atrophy
D. endometrial atrophy
As the endometrium atrophies and thins in the postmenopausal patient, a small amount of vaginal bleeding can occur. This is the most common cause of postmenopausal bleeding. Ultrasound will demonstrate an endometrium <5mm in thickness if the bleeding is due to normal changes with menopause.
A patient presents for a pelvic ultrasound due to a palpable, pliable, rounded, mobile mass in the vaginal canal. What will be the most likely findings on the exam?
A. Gartner cyst
B. Fibroid
C. Nabothian cyst
D. Brenner cyst
A. Gartner cyst
A Gartner cyst is a cyst that forms in relation to the Gartner ducts in the vagina
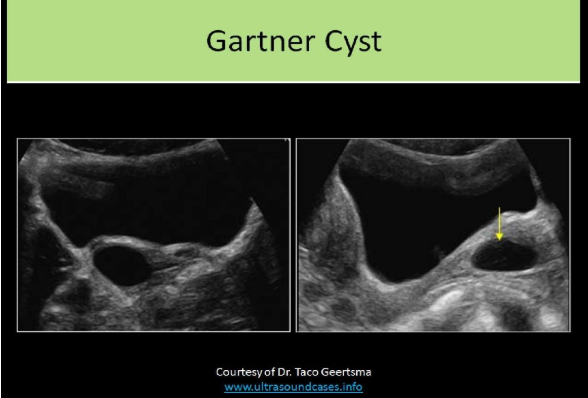
Which of the following is related to abnormal testosterone production?
A. dysmenorrhea
B. menometrorrhagia
C. hirsutism
D. dyspareunia
C. hirsutism
Hirsutism refers to male pattern hair growth in a female. This is a common symptom of disorders related to androgen production such as polycystic ovarian disease and androblastomas.
An ovarian mass with the dot-dash pattern internally is most likely:
A. a teratoma
B. a dysgerminoma
C. a mucinous adenoma
D. a mucinous adenocarcinoma
A. a teratoma
The dot-dash pattern refers to the sonographic appearance of the dermoid mesh . Short and long echogenic lines caused by hair in the mass can be identified in an ovarian teratoma.
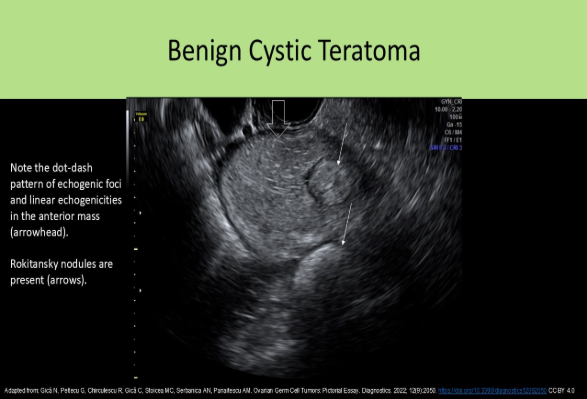
A paraovarian cyst is also known as:
A. Morgagni or Gartner duct cyst
B. Gartner duct or Mesonephric cyst
C. Mesonephric cyst or Nabothian cyst
D. Morgagni or mesonephric cyst
D. Morgagni or mesonephric cyst
Paraovarian cysts arise from the tissues of the broad ligament, composed of predominantly mesothelium. They can also form paramesonephric cysts AKA Mullerian cysts and mesonephric or fallopian tube remnants (mesonephric cyst or Wolffian cyst). A hydatid cyst of Morgagni is an acquired cyst of the broad ligament. A Gartner duct cyst is located in the vaginal tract.
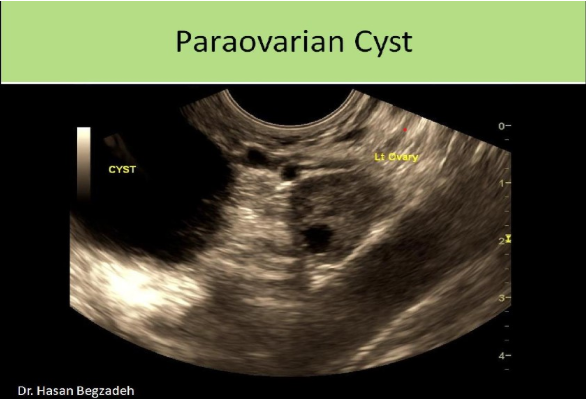
What is the greatest risk factor for cervical carcinoma?
A. multiple sexual partners
B. smoking
C. human papilloma virus infection
D. early onset of sexual activity
C. human papilloma virus infection
The greatest risk factor for development of cervical cancer is human papilloma virus (HPV) infection. Other risk factors include becoming sexually active early in life, multiple sexual partners, smoking, use of OCP, mother took DES while pregnant with the patient
Congenial uterine anomalies can be caused by improper fusion of the ______
A. Gartner ducts
B. Mullerian ducts
C. Meckel ducts
D. Nabothian ducts
B. Mullerian ducts
Congenital uterine anomalies are caused by improper formation, fusion, separation or absence of the Mullerian ducts
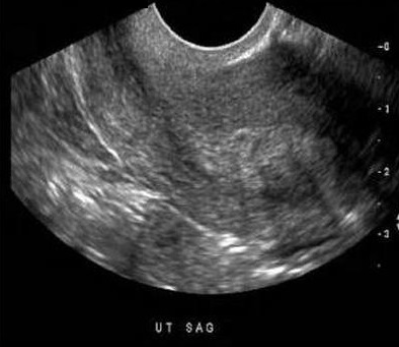
Where is the fibroid located in the uterus?
A. anterior fundal
B. posterior fundal
C. anterior cervix
D. posterior body
A. anterior fundal
The uterus is retroflexed and the fibroid is located on the anterior fundus
A 35yr old patient presents with post-coital bleeding, low back pain and watery vaginal discharge. Lab
testing is within normal limits. She had a partial hysterectomy at age 30 due to complications from
multiple fibroids. These clinical findings are most suggestive of:
A. cervical cancer
B. choriocarcinoma
C. endometrial carcinoma
D. pelvic inflammatory disease
A. cervical cancer
Symptoms of cervical carcinoma:
Early Stages: bleeding after intercourse or pap tests
Advanced Stages: low back pain, bladder discomfort, enlarged lymph nodes, watery discharge
With a surgical history of partial hysterectomy, endometrial carcinoma would not be considered. Choriocarcinoma is a complication of pregnancy. Normal lab testing and no other reported symptoms of infection would rule out PID.
Pseudomyxoma peritonei is a complication of which type of ovarian tumor?
A. mucinous cystadenocarcinoma
B. dermoid cyst
C. endodermal sinus tumor
D. serous cystadenoma
A. mucinous cystadenocarcinoma
Pseudomyxoma peritonei is a complication of mucinous cystadenocarcinoma. The mucus secretions from the tumor enter the peritoneal cavity and compress the organs causing symptoms of pain, bowel obstruction, and or urinary obstruction.
Which ovarian tumor causes serum levels of alpha fetoprotein to rise?
A. mucinous cystadenocarcinoma
B. Krukenberg tumor
C. dysgerminoma
D. yolk sac tumor
D. yolk sac tumor
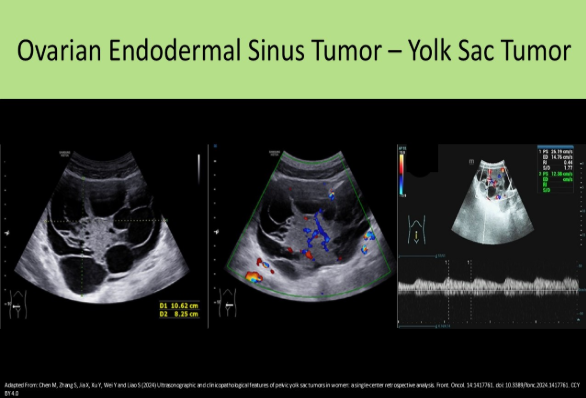
Endodermal Sinus Tumor AKA yolk sac tumor, is highly malignant. They usually present in adolescence and cause increased AFP levels in the blood. The other choices are related to elevated CA125 levels.
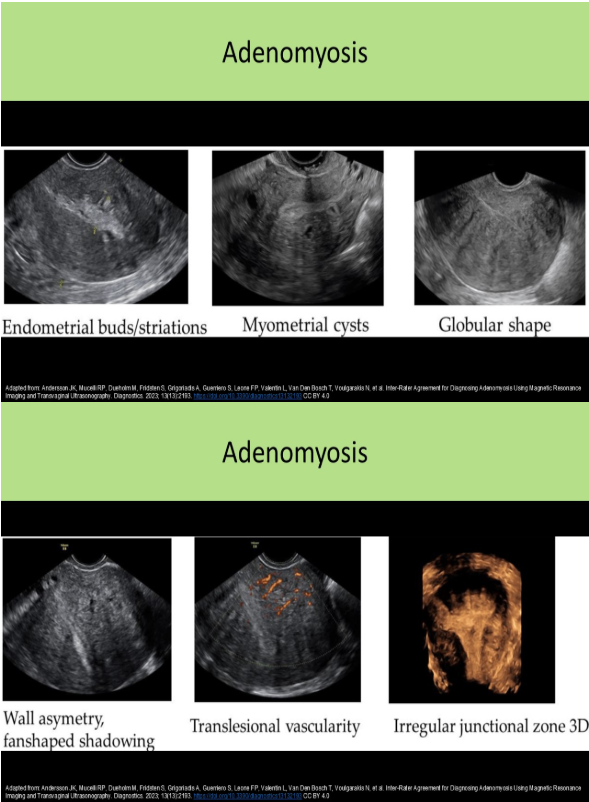
The uterus is enlarged and demonstrates multiple myometrial cysts <6mm in size and several subendometrial echogenic nodules. What is the most likely cause for these findings?
A. endometrial carcinoma
B. endometrial atrophy
C. adenomyosis
D. endometrial abscess
C. adenomyosis
Adenomyosis refers to the abnormal location of endometrial tissue in the myometrium.
Sonographic Findings:
Thickened, heterogeneous myometrium
Subendometrial echogenic nodules
Small myometrial cysts / subendometrial cysts (<6mm)
"Swiss cheese" appearance of muscle
Striated vertical edge shadows/"venetian blind" shadowing without a discrete mass
Enlarged globular uterus with smooth contour
Which of the following is a common cause of dysfunctional uterine bleeding?
A. endometrial polyps
B. hormone replacement therapy
C. leiomyomas
D. endometrial carcinoma
B. hormone replacement therapy
Dysfunctional uterine bleeding (DUB) is caused by abnormalities in the endocrine system, while abnormal uterine bleeding (AUB) is caused by uterine lesions. PCOS, oral contraceptive use and HRT can cause DUB. AUB is caused by fibroids, polyps and other uterine lesions.
Which of the following is a contraindication for IUD placement?
A. Endometrial hyperplasia
B. Adenomyosis
C. Active pelvic inflammatory disease
D. Fibroid uterus
C. Active pelvic inflammatory disease
Contraindications to IUD Placement:
Current pregnancy
Active infection - PID, sexually transmitted disease
Untreated cervical or endometrial cancer
Some congenital uterine malformations
Current IUD already in place
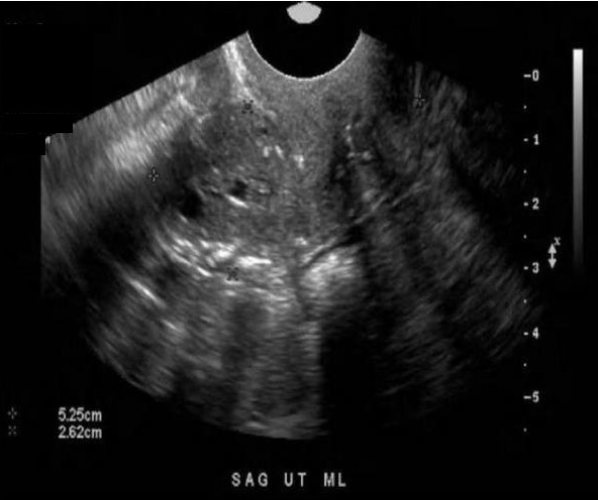
All of the following are associated risk factors for the endometrial findings displayed, except:
A. Estrogen replacement therapy
B. Tamoxifen therapy
C. Multiparous
D. Polycystic Ovarian Disease
C. Multiparous
The image demonstrates uterine adenocarcinoma. Nulliparous women have shown a much higher incidence of adenocarcinoma. A multiparous woman would have a low risk of incidence of the abnormality. There are several other factors increase the risk of endometrial cancer, such as taking estrogen after menopause, birth control pills, or tamoxifen; the number of menstrual cycles (over a lifetime), pregnancy, obesity, certain ovarian tumors, and polycystic ovarian syndrome
A negative uterine sliding sign is most suggestive of:
A. normal anatomy
B. extrapelvic endometriosis
C. bicornuate uterus
D. pelvic inflammatory disease
B. extrapelvic endometriosis
In patients with suspected endometriosis, the uterine sliding technique can be performed to evaluate extrapelvic involvement. Gentle transducer pressure is applied to evaluate the motion of the rectum across the posterior aspect of the uterus and cervix. The sliding sign is positive if normal motion is observed. If no motion is observed, extrapelvic endometriosis is suspected and laparoscopy will be performed.
Hydrosalpinx and pyosalpinx are differentiated from bowel loops by:
A. using color Doppler
B. position relative to the ovary
C. visualizing peristalsis within the bowel
D. harmonic imaging
C. visualizing peristalsis within the bowel
Hydrosalpinx and pyosalpinx are differentiated from bowel loops by visualizing peristalsis within the bowel. Hydrosalpinx and pyosalpinx are differentiated from pelvic veins using color Doppler.
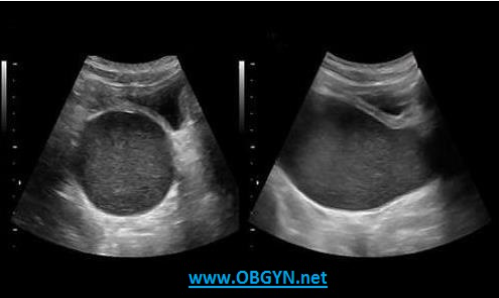
What is the most common cause of the uterine abnormality on the image?
A. trauma
B. imperforate hymen
C. ovarian hyperstimulation
D. endometriosis
B. imperforate hymen
The image demonstrates hematometrocolpos. The blood from menses is unable to escape the uterus/vagina. This is most commonly caused by an imperforate hymen.
Chronic pelvic inflammatory disease can lead to:
A. an emergency hysterectomy
B. the formation of a uterine septum
C. the formation of cervical polyps
D. an emergency salpingectomy
C. the formation of cervical polyps
Chronic PID leads to hydrosalpinx, thin-walled, nodular fallopian tube, and peritoneal inclusion cyst formation. It has also been associated with cervical polyp formation.
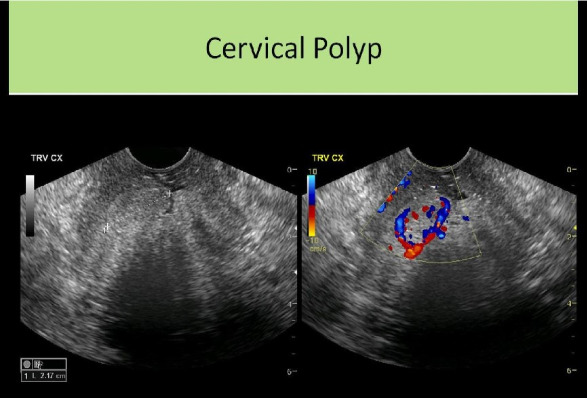
Which of the following describes a way to differentiate uterine adenomyosis from a leiomyomatous uterus?
A. Adenomyosis demonstrates significant posterior enhancement, while a leiomyomatous uterus will demonstrate varying degrees of shadowing.
B. Leiomyomas will demonstrate increased vascularity centrally, while tissues affected by adenomyosis are avascular.
C. A leiomyomatous uterus will have a lobulated uterine contour, while adenomyosis demonstrates a smooth uterine contour
D. The sonographic appearance of both abnormalities is essentially the same and MRI is usually performed to make the differentiation.
C. A leiomyomatous uterus will have a lobulated uterine contour, while adenomyosis demonstrates a smooth uterine contour
Adenomyosis leads to an enlarged globular uterus with smooth contour (fibroid formation usually causes lobulated uterine contour). Adenomyosis causes diffuse increase in vascularity of the affected area (fibroids demonstrate peripheral vascularity).
A 55 year old female presents for a follow up pelvic ultrasound due to pelvic pain, vaginal spotting and an enlarged uterus on clinical examination. The prior exam 4 months ago demonstrated a 4cm intramural fibroid and 6mm endometrium. She has no history of hormone replacement therapy, but does take Tamoxifen regularly. The current ultrasound exam demonstrates a 7mm endometrium and a 6cm intramural, non-circumscribed, heterogenous, hypoechoic mass in the body of the uterus. These findings are most suggestive of:
A. cervical carcinoma
B. leiyomyoma
C. adenocarcinoma
D. leiomyosarcoma
D. leiomyosarcoma
Leiomyosarcoma is a rare, malignant tumor of myometrium. They are usually found in females in their mid 50s. Other risk factors include nulliparity, obesity, radiation therapy and tamoxifen use. The symptoms are very similar to a benign leiomyoma and they are very hard to differentiate from benign leiomyoma sonographically. They do demonstrate a rapid increase in size with degenerative changes and internal necrosis. They are typically an intramural mass with blurred borders due to infiltration. The pelvic region should be evaluated for metastasis and lymphadenopathy.
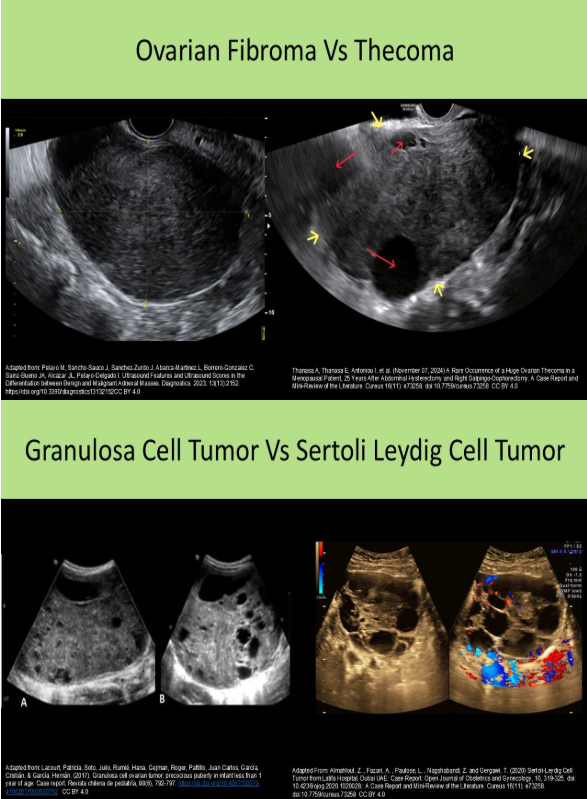
When comparing the sonographic appearance, a thecoma resembles a/an ______ and a granulosa cell tumor resembles a/an _____
A. fibroma, androblastoma
B. dermoid tumor, fibroma
C. fibroma, dermoid tumor
D. androblastoma, mucinous cystadenoma
A. fibroma, androblastoma
Fibromas and thecomas are generally hypoechoic with posterior shadowing. Granulosa cell tumors and androblastomas are generally complex with cystic components.
Which of the following is a failure to form defect of the uterus that is commonly associated with ipsilateral renal agenesis?
A. bicornuate uterus
B. uterine didelphys
C. unicornuate uterus
D. arcuate uterus
C. unicornuate uterus
A unicornuate uterus is caused by the failure of one of the mullerian ducts to form. A single horn forms on an asymmetrically shaped uterus with lateral displacement. Ipsilateral renal agenesis or pelvic kidney are commonly associated renal defects. A bicornuate uterus and uterine didelphys are failure of fusion defects. An arcuate uterus is a failure of resorption defect. Most uterine defects are associated with abnormal developments in the urinary system.
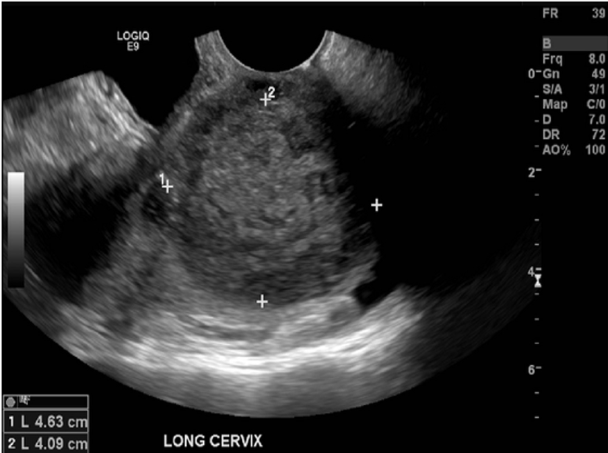
A 66yr old female presents for a pelvic ultrasound due to abnormal vaginal discharge, pelvic pain and
bloating. The attached image is from the ultrasound exam. These findings are most suggestive of:
A. hematometra and an large endometrial polyp
B. pyometra and cervical carcinoma
C. hydrometra and cervical carcinoma
D. hydrometrocolpos and cervical carcinoma
C. hydrometra and cervical carcinoma
The image demonstrates cervical carcinoma. It is typically seen in premenopausal women, but postmenopausal women can be affected, Note the bladder anterior to the mass/cervix. Anechoic fluid is seen in the endometrial cavity due to the obstruction by the mass. Because the fluid is anechoic and the patient is postmenopausal, it is most likely serous fluid and not menstrual blood or pus. -metra = uterus, -colpos = vagina. The fluid is only present in the uterus because the cervix is blocked. . The patient has cervical cancer and hydrometra.
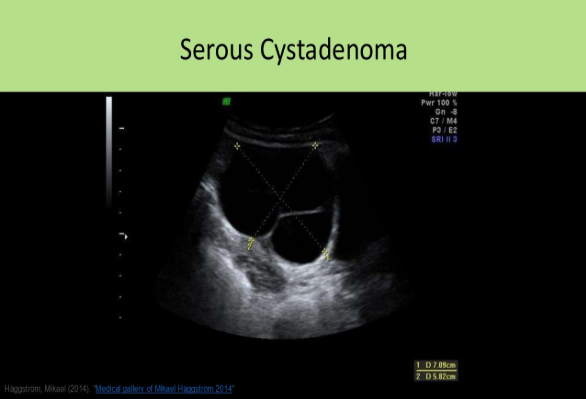
A 64 year old female presents for a pelvic ultrasound due to pain and bloating. She has no surgical history and takes no medications. The ultrasound exam demonstrates a normal uterus, left ovary, and a single 5cm unilocular, anechoic cyst of the right ovary. These findings are most suggestive of:
A. serous cystadenoma
B. papillary cystadenoma
C. functional cyst
D. mucinous cystadenoma
A. serous cystadenoma
A large, anechoic, unilocular cyst in a postmenopausal woman is most likely a serous cystadenoma. Although serous cystadenoma are more prevalent in women 20-50, they can occur in postmenopausal women. A postmenopausal patient that is not taking hormones or other medications that might influence ovarian function will not have a functional cyst. Papillary cystadenoma will demonstrate papillary excrescences. Mucinous cystadenoma will demonstrate loculations and internal debris.
Which of the following terms refers to pain associated with sexual intercourse?
A. amenorrhea
B. dyspareunia
C. menorrhagia
D. mittelschmerz
B. dyspareunia
Dyspareunia refers to pain associated with sexual intercourse. Amenorrhea refers to the absence of menstruation. Mittelschmerz refers to the pain associated with ovulation. Menorrhagia refers to excessive bleeding with menstruation.
Which of the following is a defect caused by failure of dissolution of the Mullerian ducts?
A. uterine arcuatus
B. uterine bicornis, unicollis
C. uterine bicornis, bicollis
D. uterine didelphys
A. uterine arcuatus
The other choices are failure of fusion defects
Which of the following ovarian tumors contains both epithelial and stromal components?
A. serous cystadenoma
B. mucinous cystadenoma
C. thecoma
D. cystadenofibroma
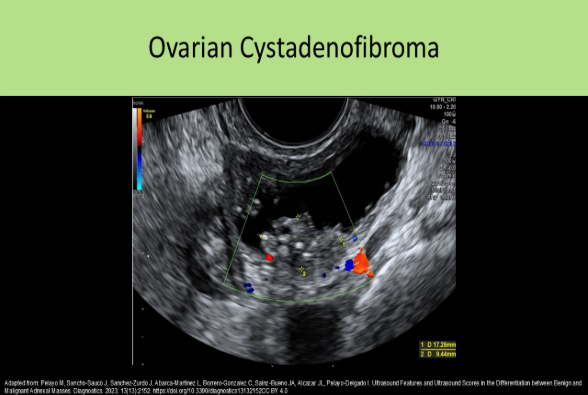
Cystadenofibroma is composed of epithelial and stromal tissues of the ovary. Epithelial cells make up the cystadenoma. A thecoma is composed of theca cells.
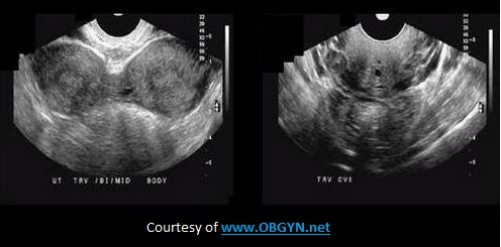
What congenital abnormality is seen on the image?
A. uterine bicornis bicollis
B. uterine arcuatus
C. uterine bicornis unicollis
D. uterine subseptus
C. uterine bicornis unicollis
Bicornis - 2 uterine horns
Unicollis - 1 cervix
Endometrial hyperplasia in a premenopausal female is diagnosed when the endometrial thickness in the secretory phase exceeds
A. 14mm
B. 18mm
C. 12mm
D. 10mm
B. 18mm
The endometrium in the secretory phase is considered normal when the thickness is between 9 -18 mm
Which of the following is related to an increased risk of developing ovarian or endometrial cancer?
A. Lynch syndrome
B. human papilloma virus vaccine
C. early menopause
D. multiparity
A. Lynch syndrome
Risk factors for ovarian cancer:
Age 50-59
Nulliparity
Early onset of menses/late menopause
Family history
Lynch syndrome - autosomal dominant genetic disorder that increases the risk of several types of cancer, including ovarian and endometrial
HER2/neu - gene that increases the risk of breast and ovarian cancer
Polycystic ovarian disease
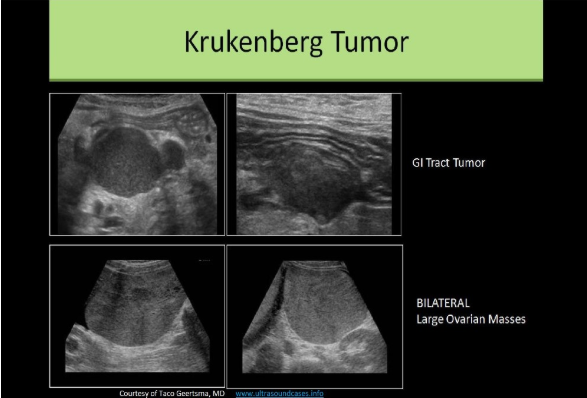
A patient presents for a pelvic ultrasound due to pain and bloating. She has a history of Gl tract carcinoma. Which of the following is the most likely sonographic finding in the pelvis?
A. Lymphadenopathy and bilateral ovarian cyst formation
B. Krukenberg tumor of the ovary and peritoneal cysts
C. Lymphadenopathy and Krukenberg tumor of the ovary
D. Lymphadenopathy and Brenner tumor of the ovary
C. Lymphadenopathy and Krukenberg tumor of the ovary
A Krukenberg tumor of the ovary is a metastatic tumor most commonly from a GI primary. Lymphadenopathy refers to the enlargement of lymph nodes. This is a common finding in the area of a malignancy. The liver should also be evaluated for metastasis in cases of Krukenberg tumor formation.
Spotting between cycles and infertility are common symptoms related to:
A. Gartner duct cyst
B. endometrial polyp
C. hematometra
D. endometriosis
B. endometrial polyp
Symptoms of endometrial polyps include abnormal premenopausal or postmenopausal bleeding and infertility history. Polyps do not usually cause pain or cramping with the abnormal bleeding. Endometriosis causes heavier than normal regular cycles.
A 30yr old female presents for a pelvic ultrasound due to amenorrhea. She states her cycles slowed and stopped over the last few months. She also complains of reduced breast size. These clinical findings are most suggestive of:
A. thecoma
B. fibroma
C. arrhenoblastoma
D. teratoma
C. arrhenoblastoma
Arrhenoblastoma is also known as a Sertoli-Leydig cell tumor. It is usually benign and occurs in premenopausal patients, age 20-40yrs. The tumor causes increased testosterone levels which can lead to masculinization (virilization). Oligomenorrhea occurs and as the tumor grows and testosterone increases, amenorrhea develops. Virilization refers to a female that develops male sex characteristics, such as hirsutism, male pattern baldness, voice deepening and breast atrophy.
Which of the following is least likely to cause PID?
A. Ruptured appendix
B. Tuberculosis
C. Lithium exposure
D. TORCH infections
C. Lithium exposure
Lithium exposure is related to cardiac malformation of the fetal heart (Ebstein syndrome). Causes for PID include Chlamydia (#1), Gonorrhea, TORCH infections, Poor hygiene, Tuberculosis, Non-sterile surgical instruments, Child birth, Intrauterine contraception, Intercourse with a man with urethritis, and Ruptured appendix.
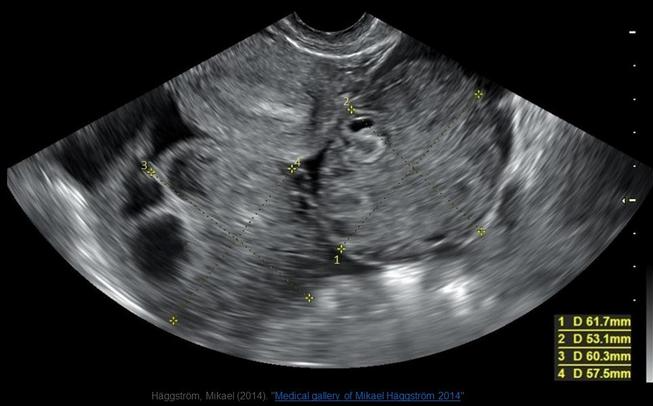
The image displayed is from pelvic ultrasound from a 27yr old female complaining of pelvic fullness. The findings on the image are consistent with:
A. ovarian lymphoma
B. Krukenberg tumors
C. ovarian hyperstimulation syndrome
D. bilateral endometriomas
C. ovarian hyperstimulation syndrome
Note the size of both ovaries and the free fluid in the pelvis. This image is taken after the retrieval process has been performed. Note the multiple collapsed follicles on the left ovary. The endometrium also appears to be in the secretory phase. This patient has completed a round of stimulation treatments recently.
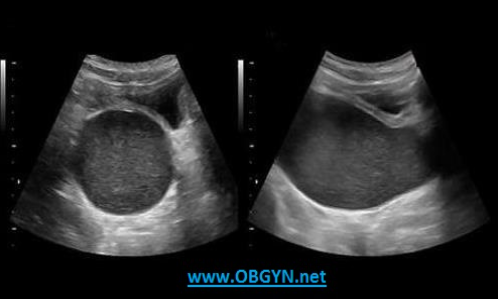
A 12yr old presents with pelvic pain and bloating. She states she has not yet had her first menstrual cycle. The ultrasound findings are most suggestive of:
A. endometriosis
B. endometrial hyperplasia
C. hematometrocolpos
D. thecoma
C. hematometrocolpos
Hematometrocolpos is usually caused by an imperforate hymen. The menstrual blood becomes trapped in the uterus causing dilatation.
Which of the following is associated with precocious puberty?
A. serous cystadenoma
B. cystic teratoma
C. mucinous cystadenoma
D. granular cell tumor
D. granular cell tumor
A granular cell tumor secretes estrogen that causes postmenopausal bleeding and breast changes. If found in young patients, it leads to precocious puberty
A patient presents with an LMP 7 weeks ago. Her chart shows she has been treated three times for PID over the last 4 years. This patient has an increased risk of ________
A. molar pregnancy due to the possible fibrosis of the tubes and uterine cavity from the PID.
B. conjoined twins due to the possible adhesions in the uterus from the PID.
C. ectopic pregnancy due to possible tubal adhesions from the PID.
D. spontaneous abortion due to the fibrosis of the uterine cavity from the PID.
C. ectopic pregnancy due to possible tubal adhesions from the PID.
Which of the following correctly describes the ultrasound appearance of a Copper IUD?
A. a linear echogenicity within each of the proximal fallopian tubes
B. a circular echogenic structure located centrally in the fundal area
C. a T-shaped anechoic area within the endometrial cavity
D. 2 parallel strongly echogenic structures with posterior shadowing and reverberation artifacts
D. 2 parallel strongly echogenic structures with posterior shadowing and reverberation artifacts
Sonographic Evaluation of IUD Placement: Endovaginal and 3D ultrasound are preferred
. Demonstrate the length of the device within the endometrial cavity
. Measure the distance to the uterine fundus
. Document the orientation of the IUD to the long axis of the uterus
. Image both arms/wings of the device
. Document the arms/wings are at 90-degree angle to the shaft
. Locate the retrieval string position
. LNG-IUD should demonstrate mildly echogenic arms/wings with an echogenic shaft
. Copper IUD should demonstrate 2 parallel strongly echogenic structures with posterior shadowing and reverberation artifacts
. The retrieval string should appear as an echogenic linear structure
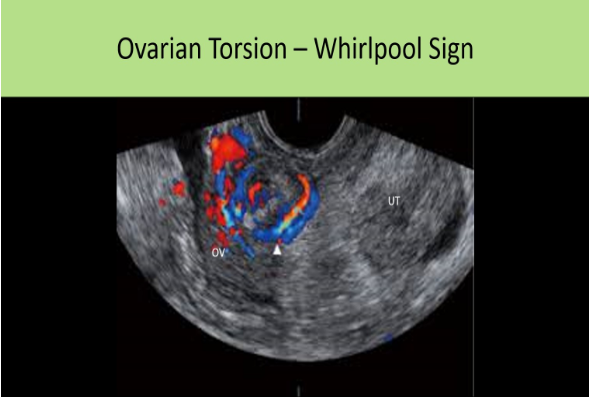
The whirlpool sign is demonstrated with:
A. molar pregnancy
B. ovarian torsion
C. hydrosalpinx
D. ectopic pregnancy
B. ovarian torsion
The torsion of the vascular pedicle may appear as an ill-defined adnexal mass adjacent to the ovary. In cross section, the adjacent mass can have a target appearance = "whirlpool" sign