Chapter 19: Disorders associated with the immune system
1/35
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
36 Terms
allergies and asthma
Observation that there are fewer allergies in tribal populations and children growing up on farms compared to the number of allergies in children in urban settings
Possibly due to wider range of microbial exposures in farm setting; also led to lower asthma rates
inflammatory bowel disease
Possible link of lack of normal microbiota metabolic products leading to chronic inflammatory state
hypersensitivity
an immune response that causes damage to the body rather than protection
antigenic response that results in undesirable effects (ex. allergies)
occurs in individuals who have been sensitized by previous exposure to an antigen (allergen)
antigenic response
body’s immune reaction to an antigen
allergen
antigen that causes an allergic or hypersensitivity reaction; when sensitized individual is exposed to antigen again body’s immune system reacts to it in damaging manner
sensitized
have memory cells
immunopathology
Study of hypersensitivity reactions
four types of hypersensitivity
anaphylactic, cytotoxic, immune complex, delayed cell-mediated
hygiene hypothesis
suggests that limiting exposure to pathogens may lower immune tolerance and the ability to cope with harmless antigens
type I anaphylactic
Occurs minutes after a person sensitized to an antigen is reexposed to that antigen or allergen
Antigens combine with IgE antibodies that are attached to mast cells and basophils
Mast cells and basophils undergo degranulation, which releases mediators
Histamine: increases the permeability of blood capillaries
Leukotrienes: cause prolonged contraction of smooth muscles
Prostaglandins: affect smooth muscle and increasemucus secretion
degranulation
the cells release stored inflammatory chemicals called mediators
first stage of anaphylactic
1. First exposure = sensitization
The first time a person encounters an allergen (such as pollen, peanuts, or bee venom):
the immune system produces IgE antibodies
IgE attaches to:
mast cells
basophils
At this stage, the person is sensitized but may not yet have symptoms
second stage
When the person encounters the same allergen again:
the antigen binds to IgE antibodies on mast cells/basophils
this triggers degranulation : The cells release stored inflammatory chemicals called mediators.
This occurs within minutes, which is why it is called immediate hypersensitivity.
histamine
increases the permeability of blood capillaries
Leukotrienes
cause prolonged contraction of smooth muscles
Prostaglandins
affect smooth muscle and increase mucus secretion
Systemic anaphylaxis
(anaphylactic shock)
Results when an individual sensitized to an antigen is exposed to it again
Involves cardiovascular and respiratory systems causing shock and breathing difficulties or death
Allergic mediators cause dilation of peripheral blood vessels resulting in plummeting blood pressure (shock)
Injected antigens or bee stings may produce more dramatic responses
Treated with epinephrine which constricts blood vessels and increases blood pressure
Localized anaphylaxis
Usually associated with limited body regions
Immediate, temporary, less severe
Ingested antigens, inhaled antigens, contact antigens
Pollen, fungal spores, dust mites, animal dander, nuts, seafood
Symptoms depend on the route of entry
Hay fever: upper respiratory symptoms
Asthma: affects lower respiratory tract
Bronchial constriction, mucus build-up
Treatment: bronchodilators, leukotriene blockers
Preventing Anaphylactic Reactions
allergy testing
desensitization
allergy testing
Antigens are inoculated beneath the epidermis to test for a rapid inflammatory reaction (wheal)
desensitization
Increasing dosages of antigen injected beneath the skin
Produces I g G, which act as blocking antibodies to intercept and neutralize antigens
Type II (Cytotoxic) Reactions
Activation of complement by the combination of IgG or IgM antibodies with an antigenic cell
Causes cell lysis or damage by macrophages
transfsion reactions
transfusion reactions
most familiar cytotoxic hypersensitivity reaction where RBCs are destroyed as a result of reacting with circulating antibodies
reactions involve (ABO and Rh antigens; blood group systems)
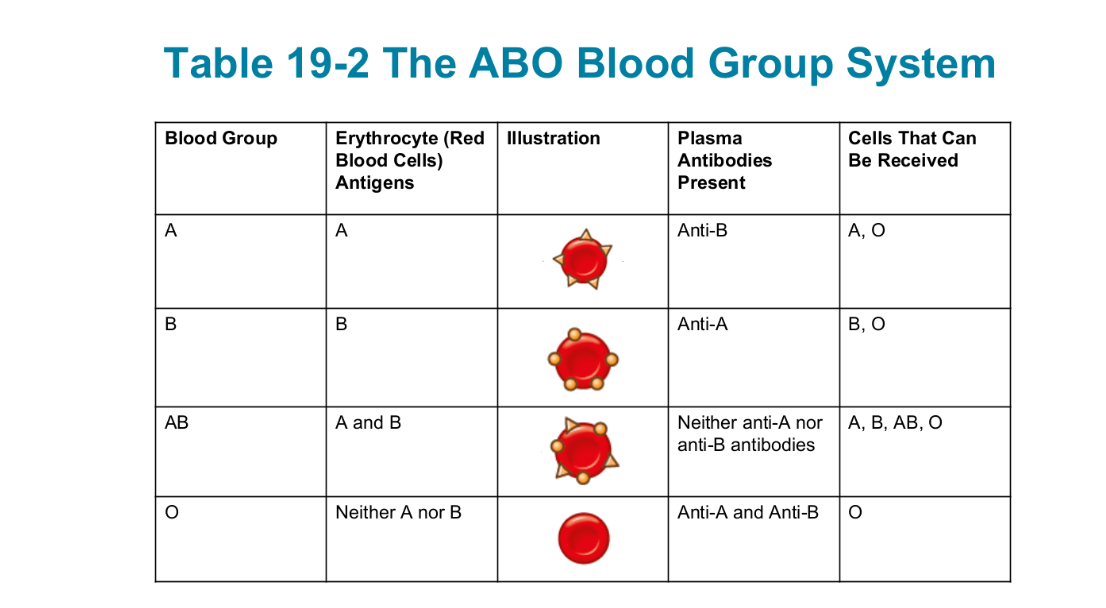
ABO blood group system
the classification of human blood into 4 principal types (A, B, AB, O)
Antibodies form against certain carbohydrate antigens on R B Cs
A antigens, B antigens, or both
Type O red blood cells: lack both A and B antigens
person’s ABO type depends on the presence or absence of carbohydrate antigens located on the cell membranes of RBC
involves 3 carbs. antigens on surface of cells (A, B, H): type O only has H antigen
Rh blood group system
Rh factor antigen (Rh+) is found on RBCs of 85% of the population
Rh+ blood given to an Rh- recipient will stimulate the production of anti-Rh antibodies in the recipient
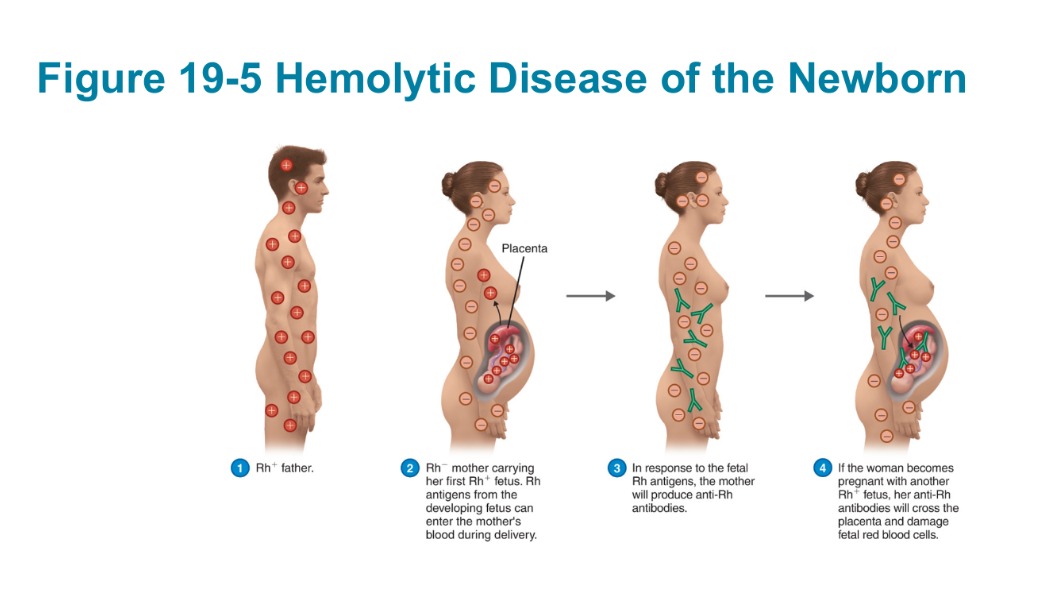
Hemolytic disease of the newborn (H D N B)
Rh- mother with an Rh+ fetus may produce anti-Rh antibodies if sensitized during pregnancy or birth
Subsequent Rh+ fetuses will receive anti Rh- antibodies (produced by maternal memory B cells) which damage fetal RBCs
Prevention: Rho G A M® shots to mother at 28 weeks and shortly after delivery
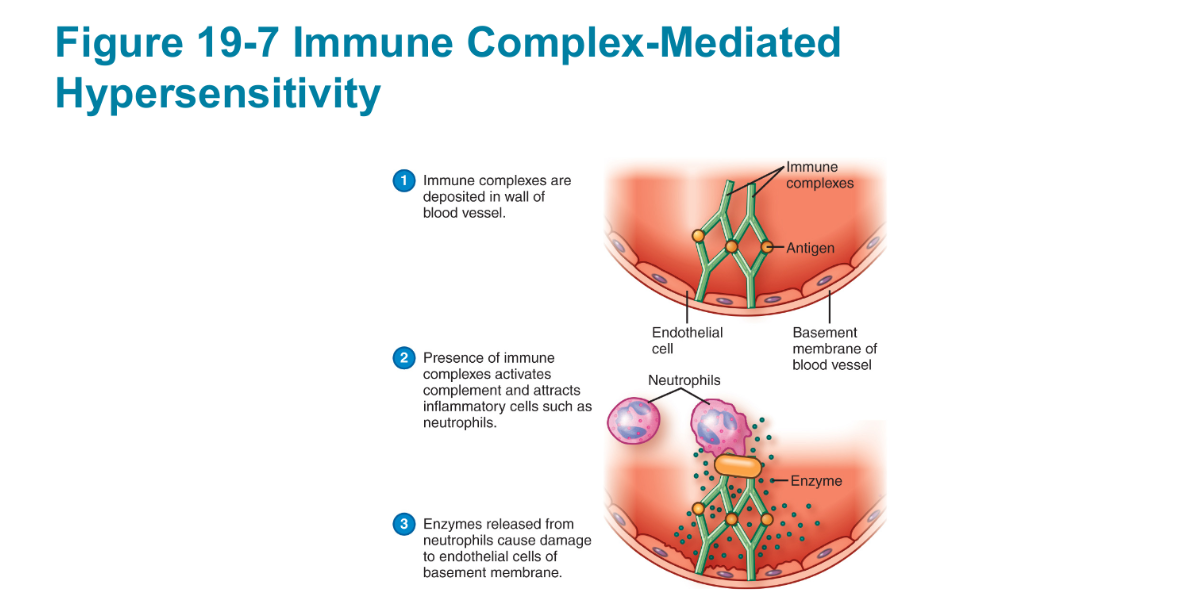
Type III (Immune Complex) Reactions
Antibodies form against and react with soluble antigens in the serum
Form immune complexes that lodge in the basement membranes beneath the cells (usually IgG)
Activate complement, causing inflammation
Immune complexes form only when there is a certain ratio of antigen and antibody
Type IV (Delayed Cell-Mediated) Reactions
Cell-mediated immune responses caused by T cells
Delayed hypersensitivity
On first exposure, antigens are phagocytized and presented to receptors on T cells, causing sensitization
No obvious reaction on this exposure
Re-exposure to antigen causes memory cells to release destructive cytokines
Reaction takes a day or more to develop after antigen exposure
The delay represents the time for participating T cells and macrophages to migrate and accumulate
Delayed cell-mediated hypersensitivity reactions on the skin
Skin test for tuberculosis
Allergic contact dermatitis
Haptens combine with proteins in the skin, provoking an immune response
Allergic response to poison ivy, cosmetics, metals, and latex
immune surveillance
Cancer cells arise frequently and are removed; concept where cancer cells arise in body and that they’re eliminated by immune system
RhoGAM shots
anti-Rh antibodies, combine with any fetal Rh+ RBCs that have entered the mother’s circulating reducing risk of sensitization to the Rh antigen
cancer cells
cell becomes cancerous when it under goes transformation and begins to proliferate without control
cancer
represents a failure of the body’s defenses including immune system
immune system and cancer
Cancer cells have tumor-associated antigens that mark them as nonself
CTLs, activated macrophages, and N K cells can destroy cancer cells
Limitations
No antigenic epitope for the immune system to target
Tumor cells reproduce too rapidly
Tumor becomes invisible to the immune system
immunotherapy
Endotoxins from bacteria (Coley’s toxins) stimulate that interferes with the blood supply of cancers
Vaccines used for prophylaxis
Cervical, anal, and throat cancer (H P V), liver cancer(hepatitis B)
Monoclonal antibodies
Herceptin for breast cancer
Immunotoxin combines a Mab with a toxic agent
Targets and kills a tumor without damage to healthycells
immunotoxin
combines a MAB with a toxic agent
Targets and kills a tumor without damage to healthy cells