Prosthetic Post surgical considerations
1/29
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
30 Terms
what are the types of prosthetist intervention?
closed amputation
open amputation
myodesis
myoplasty
what is closed amputation?
elective procedure
skin is closed after amputation
what is open amputation?
wound is left open over amputation stump and is not closed
done as an emergency procedure in the case of life threatening infection (severe infection, severe crush injury)
what is myodesis
muscle is sutured to the bone
what is myoplasty ?
muscle is sutured to the opposite muscle group under appropriate tension
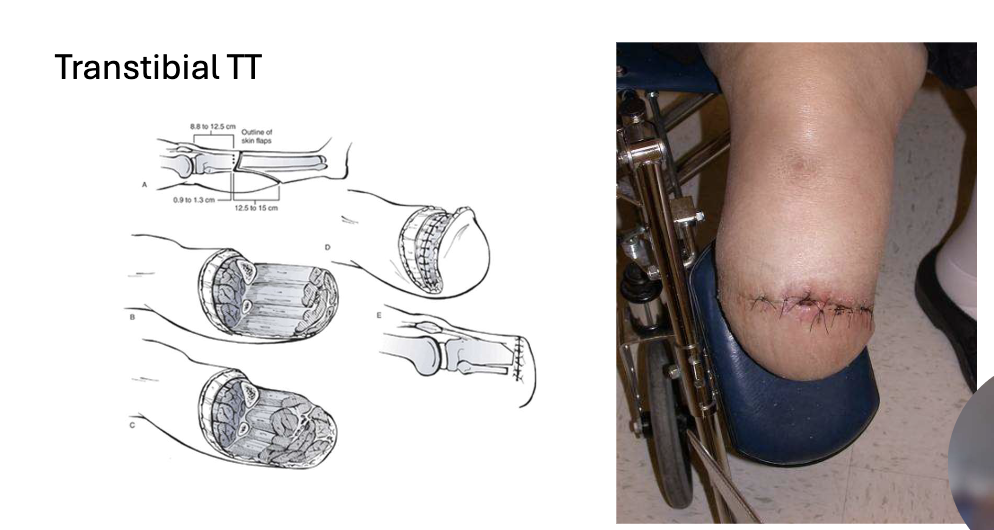
Types of post surgical residual limbs
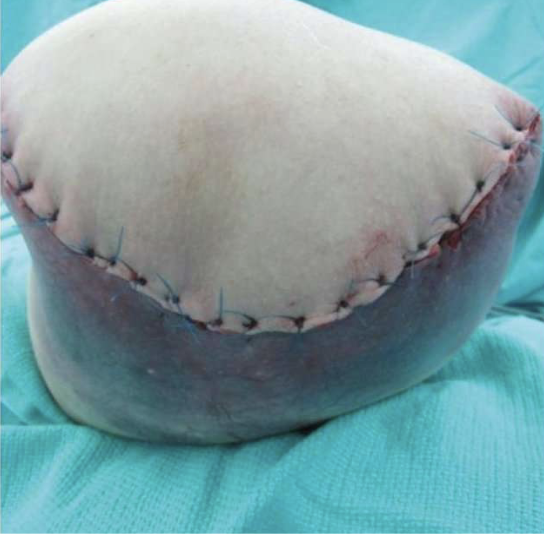
Things to observe on new RL
Dog Ears
Sutures
Tissue density/ skin condition
Color
Drainage/ Discharge
Odor
Transfemoral TF
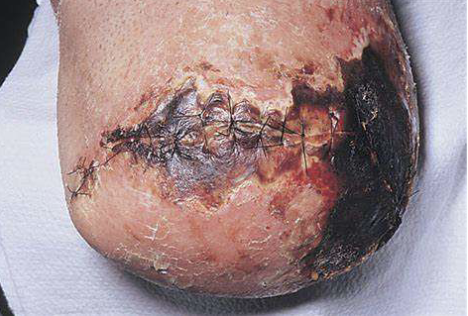
Infection/ Necrotic tissues
complications
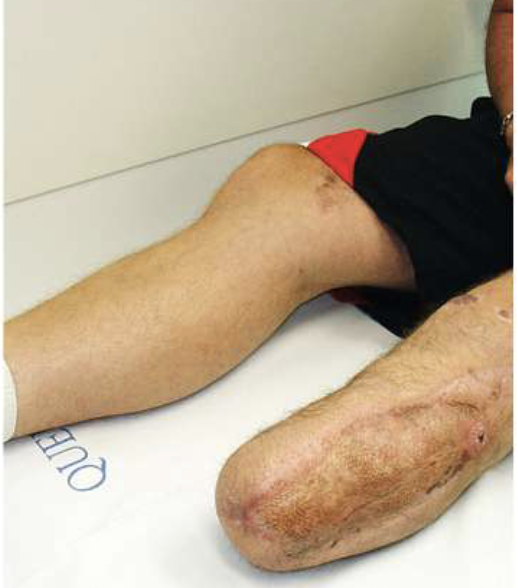
TT with Skin graft
What is the impact from these conditions?
Healing rate , Strength/endurances, Safety
What is to be anticipated?
Patient participation, Motivation Limitations
What do we do?
Encourage, Educate, Protect
Educate patient and family- what to expect, have them involved in the care plan
Manage pain- medications, mirror therapy, desensitization methods, breathing time
Stress Safety- awareness of phantom sensation ,fall risk, use of assistive devices, caution when mobile
Facilitate Healing- wound care, AROM to tolerance, Limb protection , residual limb shaping/edema control
Promote return of independence-
cardiovascular gain, endurance, mobility, ambulationPrepare for D/C & prosthetic care- RL manipulation/desensitization/ prevent contractures
objectives
soft - ace bandage
rigid - cast
semi rigid = “crash helmet”
types of dressings
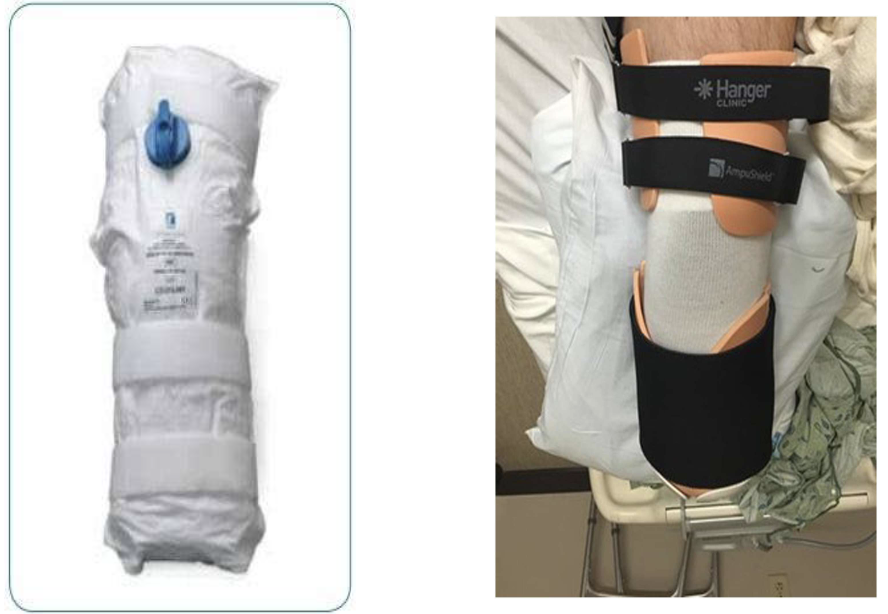
removable semi rigid dressings
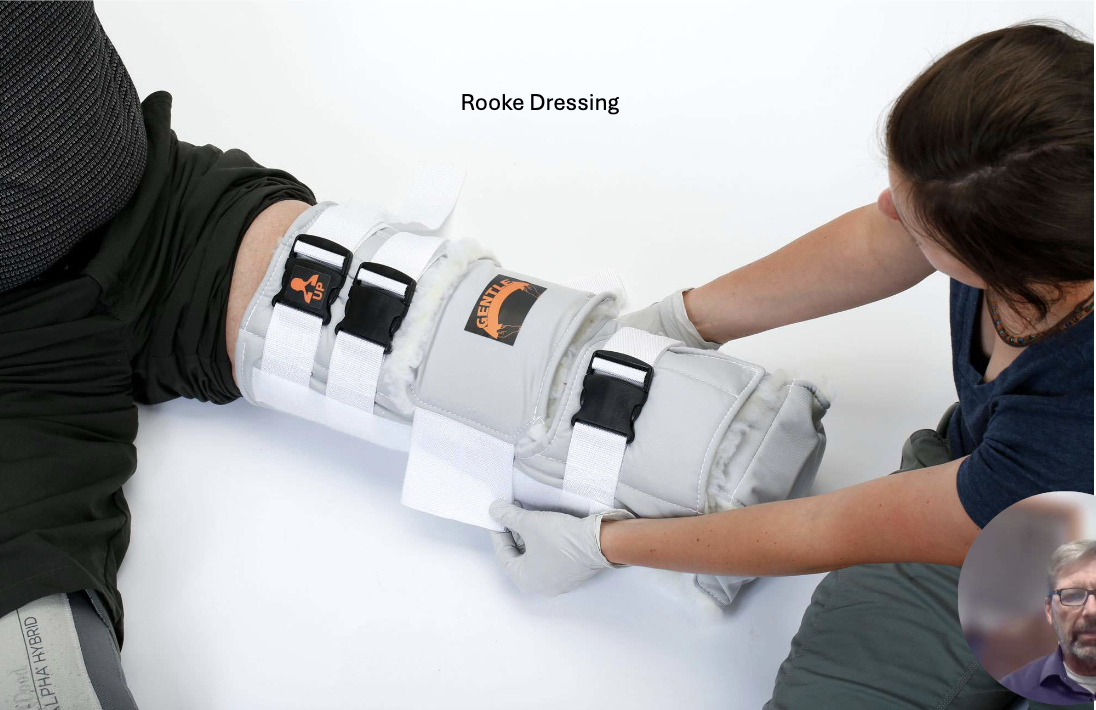
Rooke Dressing
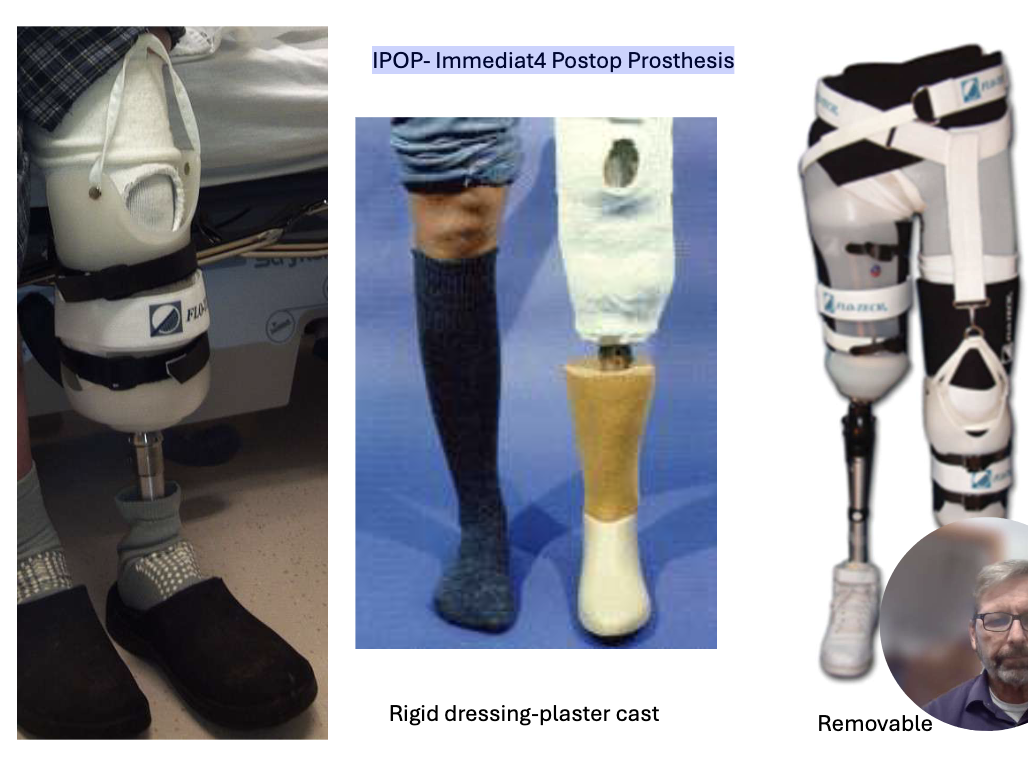
IPOP- Immediat4 Postop Prosthesis
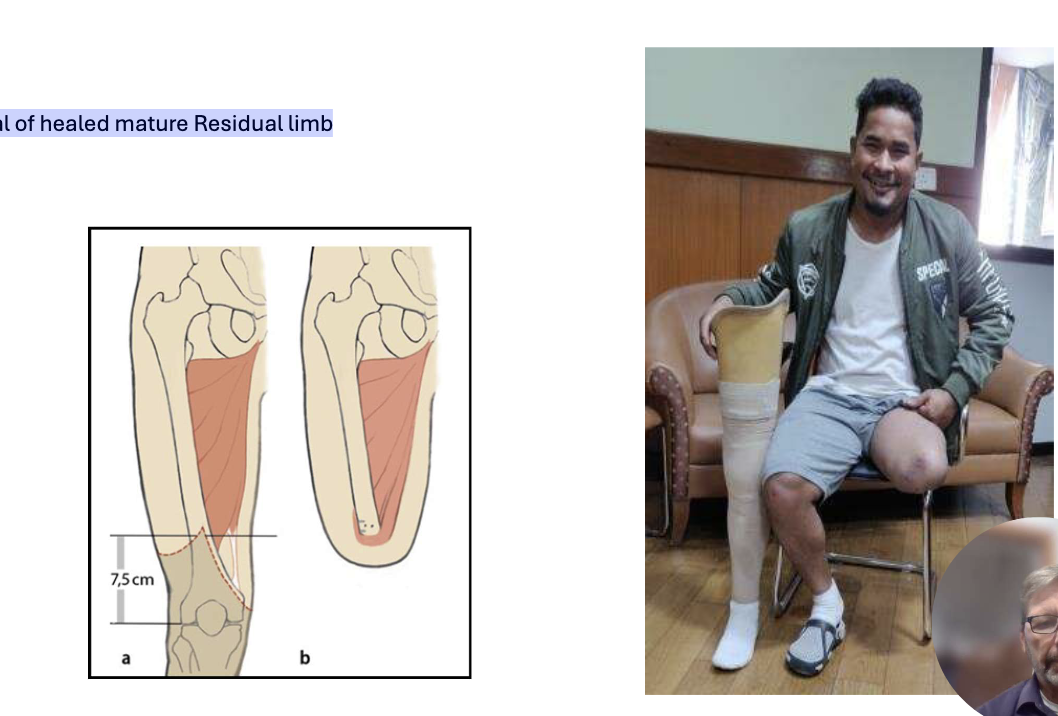
Goal of healed mature Residual limb
Cause- trauma vs vascular vs cancer
Level- higher amputation equates to greater function lost, increased energy requirement
Patient age- endurance, strength, & balance influenced by the patient’s age
History- what was the person able to do before? What is their home like?
Impact on recovery rate
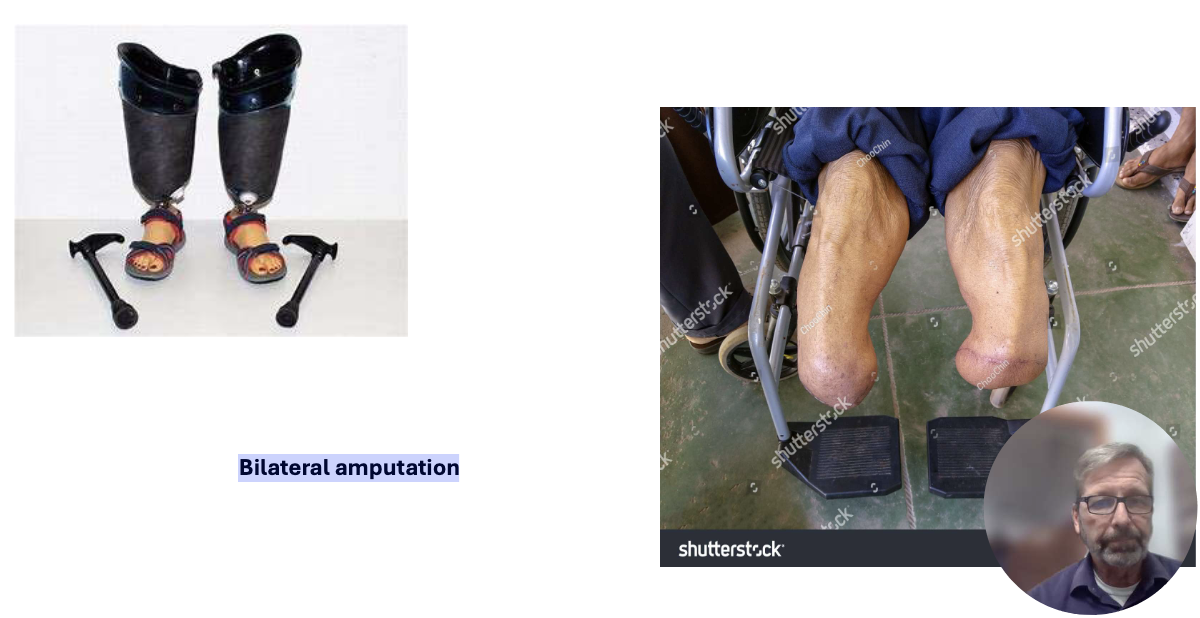
Bilateral amputation
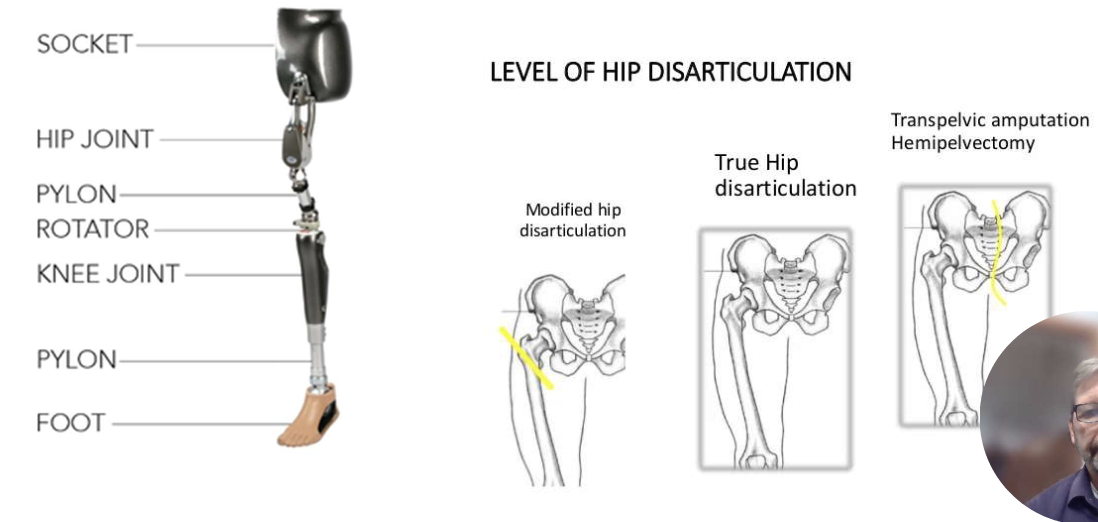
Hip Disarticulation/ hemipelvectomy
Similar to the implant technology of joint replacements and dental replacements.
Currently, FDA Approved for TF only.
Started in England and Australia
Now offered in specialized clinics in the USA (NYU Langome)
Candidates are currently TF amputees due to cancer or Trauma
Patients with failed or potential problems with conventional socket fittings/suspension.
First stage implant anchor insertion with 6 months recovery time NWB
Second procedure for the attachment implant with slow weight bearing for 6 months before full weight bearing with prosthesis
Complications can be - Risk of failure, infection and limited K3 activity( no high impact)
Benefit of some proprioception, increased wear time tolerances, and increased function
Osseointegration (2 stage OPRA)
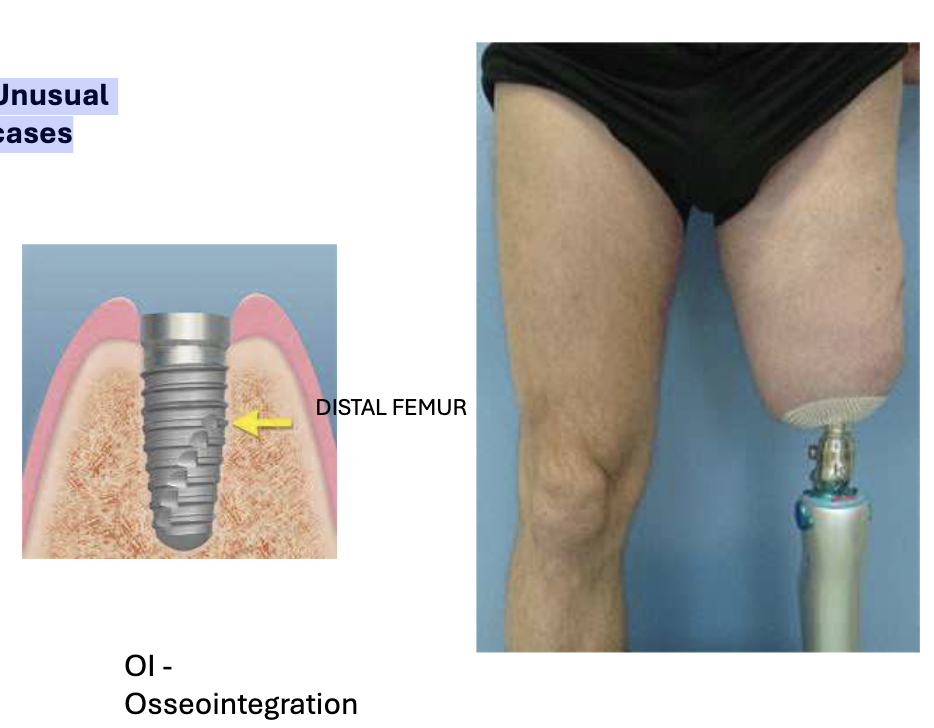
Unusual cases
The Ertl procedure emphasizes bony and soft tissue reconstruction to create a stable, dynamic limb.
Tibiofibular Bone Bridge:
Myoplasty:
Neurolysis:
Improved End-Bearing: .
Improved Prosthetic Fitting:
Ertl Procedure
what is Tibiofibular Bone Bridge:
It involves creating a bone bridge (synostosis) between the cut ends of the tibia and fibula, aiming for a stable, broad tibiofibular articulation.
what is Myoplasty
A myoplasty (muscle attachment to bone) is performed to cover the distal stump and improve muscle function.
what is neurolysis
Nerves are identified, placed on stretch, and transected as proximal as possible to eliminate neuroma formation.
what is improved end-bearing
The goal is to allow patients to bear more weight comfortably on their residual limb, potentially improving gait and function
what is improved prosthetic fitting
The stable, reconstructed limb is designed to facilitate easier and more functional prosthetic fittings.
This surgical procedure was pioneered in 2002 by Gregory A.
Dumanian, MD, a plastic surgeon at Northwestern Medicine,
and Todd Kuiken, MD, PhD, a physiatrist and professor at the
Northwestern University McCormick School of Engineering. It was
originally developed to help people who had limbs amputated
control their upper limb prosthetics. In their research, Dr.
Dumanian and Dr. Kuiken observed an unexpected benefit of TMS
surgery: reduced phantom limb pain and neuroma.
Targeted muscle reinnervation- TMR