BIOL 326 Exam #3
1/72
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
73 Terms
Draw the pathway showing how the stomach generates HCl in parietal cells.
There is always an amount of CO2 in the blood and it can equilibrate inside the cell and can move back and forth across the membranes to combine with H2O to form carbonic acid, catalyzed by the enzyme carbonic anhydrase. The H2CO3 is a weak acid so it dissociates to form H+ and HCO3- (bicarbonate). H+ quickly pumped into the lumen via primary AT (proton pump that requires ATP), of parietal cell. It briefly pumps K+ in from the lumen, then pumps it back out right away. H+ pumped against its concentration gradient into the lumen. 2nd AT of HCO3- out of the cell into the plasma along its gradient in exchange for chloride. Cl- follows movement of H+ into the lumen to produce hydrochloric acid.
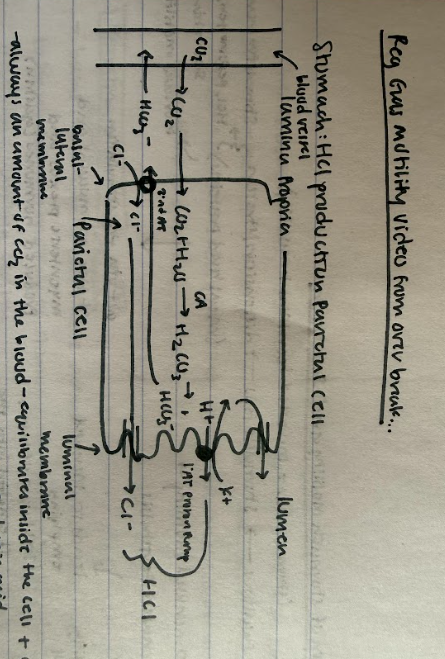
What is the acid production rate of the stomach’s parietal cells dependent on?
carbonic anhydrases ability to combine CO2 and H2O to make H2CO3.
What stimulates the acid production pathway in the stomach? (two main mechanisms)
1) After you eat, food enters the stomach, causing distension, which then triggers the submucosal plexus, which stimulates H+ movement and hormones, such as gastrin (which stimulates H+ proton pump activity), which promotes the cell to produce acid.
2) Proteins in the stomach are detected by cells in the submucosal plexus, which causes a release of gastrin, which increases acid production.
Why are you often tired after you eat?
Bicarb goes up in the plasma as a result of increased acid production, which has a neural effect on the brain and makes you feel tired (this is referred to as the alkaline tide).
What is the flowchart of regulation of stomach motility and secretion after you eat?
Secretion: You eat and swallow a bolus, which fills your stomach. The stomach will feel distension or stretch, which acts as a stimulus for increased HCl, pepsinogen, secretin, and the gastrin hormone secretion into the blood gastrin stimulates motility and secretion). Gastrin release is triggered via the stimulation of the submucosal and myenteric plexus.
Motility: Due to increased motility, you get increased peristalsis: which causes 1) a mixing of food with increased secretions and 2) leads to increased emptying (3 mL wave of chyme is emptied into the duodenum).
Why does the duodenum have to regulate how much chyme enters from the stomach?
Duodenum volume increases as the stomach empties, but it is smaller than the stomach so it can’t handle continuous emptying of the stomach. The duodenum must be able to slow down the stomach’s emptying. It must also slow down the secretory and motility functions of the stomach, until it can handle the contents that have been emptied into it.
Describe the process of inhibition that the duodenum uses to regulate the motility and secretion/ digestive processes of the stomach…
1) Increased distension in the duodenum causes a neural reflex involving both the submucosal and myenteric plexus that inhibits stomach secretions and motility to slow down digestive processes.
2) As stomach empties into the duodenum, the H+ entering the duodenum increases, which is detected by endocrine cells in its lining, which causes the production of the secretin hormone that gets released into the blood and inhibits stomach secretion and motility.
3) If the meal you ate has proteins and fats, these are detected by endocrine cells in the lining of the duodenum (duodenal mucosa) and they secrete the hormone CCK, which inhibits stomach secretions and motility.
The purpose of all of these is to slow down stomach emptying to the point the duodenum can handle.
What happens when the duodenum has dealt with the contents entering from the stomach and motility has moved the contents along?
Distension disappears, fats and acid concentration decrease. The variables that previously inhibited emptying are removed and the stomach begins emptying again. The duodenal volume then goes up again, all of the variables for inhibition are reactivated to slow the stomach activity. (this is a constant cycle the stomach and duodenum go through in between meals).
Why do meals that have fats and proteins take longer to digest than simpler meals?
Because proteins and fats take longer to digest in the duodenum, inhibitory influences of the duodenum on stomach mobility and secretions is greater (due to hormones like secretin + CCK).
What causes vomiting? Describe the mechanism behind it?
Basal electrical rhythm (BER) or basal contractile activity of the stomach and upper intestine need to be abolished (their motility needs to be knocked out). Something toxic in the stomach project to the two ends (the two sphincters of the stomach) and their endings send signals to the medulla (the vomiting center of the brain) to activate the sympathetic nervous system to knock out contractile activity. This causes the stomach and upper small intestine to relax, eliminate BER, and it also stimulates the abdominal skeletal muscles to contract. This puts pressure on the organs, but the glottis is still closed. At some point muscles contract rhythmically and the glottis opens, and all contents of the stomach and upper small intestine are squeezed and forced to the outside. All sphincters are relaxed and opened in this process.
T/F Food in the stomach always leads to slowing down/emptying with distension of the duodenum, but a meal that has fats and proteins in it creates much greater inhibition b/c of the CCK hormone.
True
What happens in the first phase of gastric function: Cephalic Phase?
This is in the mind/head. The sight, thought, or smell of food activates the parasympathetic centers in the brain (the medulla and brainstem), which activates the submucosal plexus and increases the secretion of acid, pepsinogen, or H+ ions, and mucus. The medulla and brainstem also activate the myenteric plexus to increase motility.
What happens in the gastric phase of gastric function? (the second phase)
Food (a bolus) actually enters the stomach. This causes distension which increases activity of the submucosal (which increases secretions) and myenteric plexus (which increases motility) and together they increase peristalsis and increase emptying. The duodenum slows down the motility and secretions activity of the stomach so it occurs at a rate that it can handle. The distension of the stomach also causes G cells in the mucosa to release gastrin, which further increases secretion and motility.
What happens in the intestinal phase of gastric function? (phase 3)
This occurs as emptying starts. The chyme or bolus mixed with gastric juices, very acidic and liquidy enters the duodenum (8-10 cm), which increases distension. This then neurally inhibits gastric motility and secretion (involving activation of the myenteric and submucosal plexus) via two mechanisms…
1) Increase in H+ in duodenum causes secretion of secretin into the blood, which decreases motility/secretory activity of the stomach.
2) Proteins/Fats* are detected and CCK is released, causing decreased motility/secretory activity of the stomach.
Together they slow down digestive processes in the stomach so duodenum can do its thing (slow the rate of emptying)
Absorption starts and duodenum moves contents forward, these inhibitory variables are removed, secretory activity/motility increases again temporarily (circular process to regulate the rate of digestion).
What are the three parts of the small intestine and what takes place in each?
1) Duodenum- short 10-15 cm long, bulk of digestion, secretion enzymes from pancreas + liver received here.
2) Jejunum- longest part, bulk of absorption occurs here.
3) Ileum- link between SI and LI, some absorption (water, bile salts from liver, vitamin B12 for hemoglobin, etc.)
T/F Proteins found in the apical border are different than those found in the basolateral border of columnar epithelial cells in the villi of the small intestine indicating polarity, where the chemical makeup of membranes is different.
True
Draw the small intestine cell structures that maximize surface area…
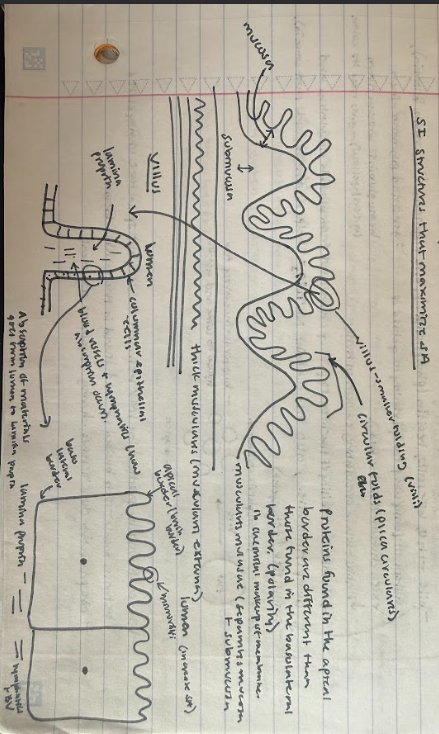
Draw the system of ducts that connects the liver, pancreas, and gallbladder…
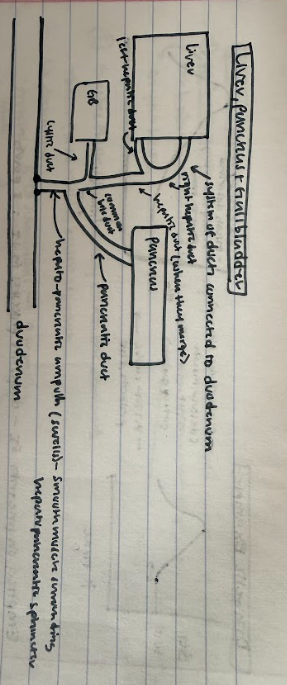
Describe the state of the hepato-pancreatic ampulla and its sphincter when there is chyme in the duodenum and when there isn’t…
No chyme in the duodenum, hepato-pancreatic sphincter closed. When there is chyme in the duodenum, the hepato-pancreatic sphincter is open to allow for pancreatic, liver, and GB secretions to enter the duodenum.
What is the only digestive function of the liver?
To produce and secrete bile. You could survive without this function. Bile is a fancy form of soaps to help you break down fats and speed up digestion.
What is bile composed of?
H2O, bile salts, lecithin (phospholipids), bile pigments (biliverdin and bilirubin-pigments generated when hemoglobin is broken down, producing the green/yellow color in feces), cholesterol, and Na+HCO3- (helps neutralize acids that come in).
What is the only way for your body to get rid of excess cholesterol?
The only way to get rid of excess cholesterol in the body is to get rid of it in the bile.
What do statin drugs do?
They lower circulating cholesterol levels and enhance the ability of the liver to pickup cholesterol from blood in circulation and dump it into bile.
Bile is an emulsifier, what does that mean?
It is a detergent, it can break fat that is insoluble in water into smaller fat droplets in the duodenum so that there is a greater surface area for lipase to come and act on.
What is true about the level of bile production in the body?
Bile continuously produced by the liver between meals, but the sphincter is usually closed between meals, so it gets backed up and stored in the gallbladder. Bile production does increase during digestion of a meal though.
If the gallbladder is removed, where is the excess bile store in?
The hepatic duct because it is distensible and can be stretched.
Describe the structure of the pancreas…
clusters of cells like a bunch of grapes. The main stem is like the hepatic duct and the smaller stems are like individual grapes - spherical units of cells,
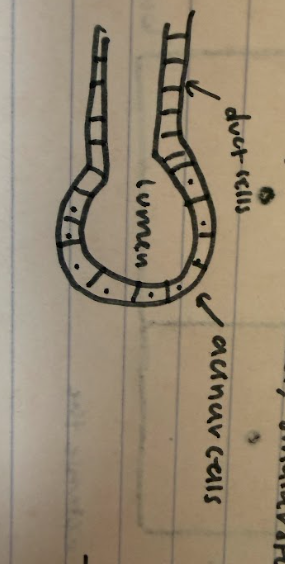
What do the pancreatic cells secrete?
Duct cells produce watery Na+ hCO3- electrolyte solution (neutralizes acidic chyme in the stomach w/ help of bile to aid in digestion).
Acinar cells- secrete enzymes that act in the duodenum (proteinases, amylases, lipases, nucleases)
Why are proteases released in an inactive form from the pancreas?
If they were released in an active form, where they were active right away in the process of getting to the duodenum they would auto-digest ducts and pancreatic structures.
What is the gallbladder and what does it do?
It stores bile produced by the liver in between meals (doesn’t go into the duodenum), helps concentrate bile (removes water from bile, makes it more potent/stronger). The problem is this can cause the formation of gallstones: salts, pigments concentrate and precipitate, lots of gallstones you just remove the gallbladder.
How are liver, pancreatic and GB secretions regulated? Describe the sequence of events…
Stomach emptying and chyme comes into the duodenum
a) H+ enters the duodenum causing secretin to be released into the blood. This then causes 1) the pancreas duct cells to release H2O, Na+HCO3- electrolytes, neutralizes acid so digestion can begin. 2) increases liver bile production
b) meal had fats, proteins, or peptides, causes CCK to be released by endocrine cells in the duodenum into the blood. This causes 1) pancreatic acinar cells to release enzyme rich pancreatic juice into the duodenum 2) increase contraction of GB (adds extra bile to mix chyme), and 3) increase in relaxation of the hepato-pancreatic sphincter (allowing secretions to get into the duodenum).
What is responsible for chemical digestion in the duodenum?
Largely pancreatic enzymes such as amylases, nucleases, lipases that start acting right away, and proteases that get activated later on.
What are the steps for activating the pancreatic proteases?
1) enterokinase(a brush border transmembrane enzyme that’s active site faces the lumen of the apical side of the columnar epithelial cells in the small intestine villi- catalyzes the conversion of trypsinogen into trypsin (the active protease form).
2) The trypsin then works on chymotrypsinogen and procarboxypeptidase that are floating around in the lumen and catalyzes their conversion to chymotrypsin and carboxypeptidase (the active proteinase forms). All of these in the active state break down proteins.
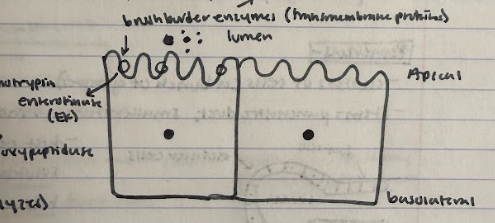
What are the three types of proteinases secreted by the pancreas?
1) Trypsinogen
2) chymotrypsinogen
3) procarboxypeptidase
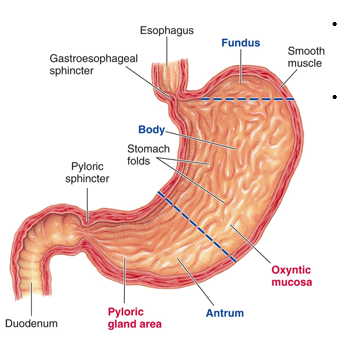
What are the various regions of the stomach? (5)
1) Cardia
2) Fundus- contains pacesetter cells, starts phasic contractions that originate in the fundus and go to the antrum, increasing in strength as you go down
3) Body- contains three smooth muscle layers that get thicker towards the base or sphincter. The muscle acts as a single unit muscle that has phasic- basal electrical rhythms.
4) Antrum (pylorus)
5) Rugae (to confer plasticity)
What are the functions of the stomach? (6)
1) Ingested food storage- coordination of events with the small intestine (empty at a rate that the duodenum can handle) (has a volume of 500-750 mL)
2) bolus converted to chyme in the stomach (liquid suspension) with muscular contraction and gastric juices.
3) initiation of protein digestion (most other digestion starts in the duodenum) - amylase in the mouth works until it gets denatured in the stomach.
4) intrinsic factor secretion- produced by the stomach and is required in the production of VB12- needed for hemoglobin production; otherwise, you are anemic if you can’t absorb VB12.
5) continuation of CH2O digestion in the body
6) alcohol and aspirin absorption (there is no absorption of nutrients across the stomach wall except for these things). (also non-steroidal anti-inflammatories).
What causes gastric reflux disorder?
1) Abnormally high motility
2) Leaky esophagus valve
3) higher than normal acid production
Heart burn caused by too forceful stomach contractions, greater than normal production of acid, or a leaky sphincter (cardia).
Why do we want the cardiac or upper esophageal sphincter to be closed most of the time?
Want it closed to prevent acid from the stomach from coming back up into the esophagus. Esophagus isn’t made to deal with the acidic stomach environment.
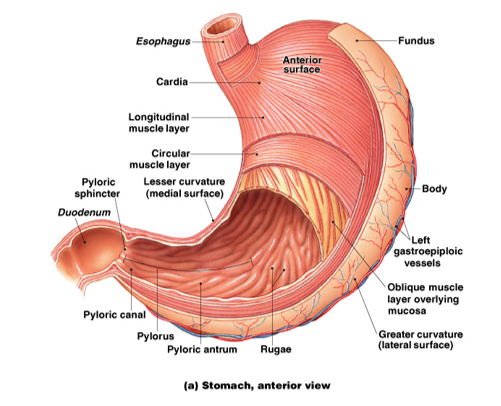
What are the muscular layers of the stomach wall and how do they change in thickness throughout the stomach?
1) outermost = longitudinal muscle layer
2) middle = circular muscular layer
3) oblique muscular layer (innermost)
The muscular layers get thicker as you go towards the antrum, and they get stronger. The musculature of the antrum is much thicker than other areas.
What is true of the cells of the gastric pit?
There are five types of secretory cells within the epithelium (4 of those produce 3 liters of gastric juice released) and the fifth secretes hormones.
What are the five types of secretory cells found in the epithelium of the gastric pits and where are they located primarily?
Closest to the surface: surface mucus cells, mucus neck cells (near gastric pit), base near gastric glands is a mix of: parietal cells, chief cells, and G-cells.
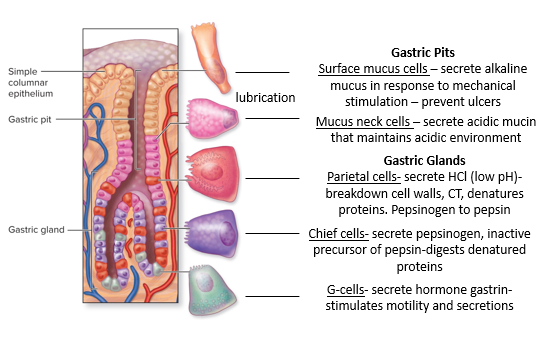
What are surface mucus cells (or surface epithelial cells)?
Found near the surface of the gastric pits, they secrete alkaline mucus in response to mechanical stimulation and prevent ulcers. The alkaline mucous is produced by the top cells and sits in a thick layer on top of the cells. Mucus protects the cells physically from autodigestion by acid and enzymes; alkaline neutralizes any acid that comes in contact with cells.
Produce a thick alkaline mucous, which provides physical protection from acid(don’t want acid to act on cells that line the stomach, just the content of the stomach), and alkaline neutralizes the acid.
What are mucus neck cells?
found near the neck of the gastric pit: secretes acidic mucin that maintains an acidic environment. Mucus neck cells can differentiate further into chief cells (gastric stem cells can give rise to all other gastric cell types).
Produce slightly acidic mucus, want some acid to get into the lumen.
What are parietal cells?
Found near gastric glands, they secrete HCl (low pH), break down cell walls, CT, denatures proteins. Converts pepsinogen to pepsin.
Produce HCl, the source of the acid.
What are chief cells?
Found near the gastric glands, they secrete pepsinogen, inactivate the precursor of pepsin, and digest denatured proteins. They are the most numerous cell type.
Produce pepsinogen, the enzyme that, when activated, starts the process of protein digestion (high acidity of lumen activates it).
What are G-cells?
They secrete the hormone gastrin into the blood and stimulate motility and secretions.
Produce a hormone called gastrin (the most important stimulatory factor in regulating gastric secretions and motility).
T/F The cells of the gastric pit die quickly because of the intense environment of the stomach.
True: especially the surface mucus cells.
What are the only two types of cells in the gastric pit that secrete mucus?
Surface mucus cells and mucus neck cells.
What are the exocrine secretory cells of the gastric pit?
surface mucus cells, mucus neck cells, parietal cells, and chief cells.
What are ECL cells?
They release histamine. They regulate the secretion of some of the secretory cells.
What are the secretory cells of the submucosal plexus regulated by? (3)
1) Ach- stimulates surface epithelial cells, mucous neck cells, parietal cells, and chief cells to release their secretions. Released when there is food in the stomach.
2) Gastrin- gets into the blood and causes all secretory cells to release their mucous. (surface epithelial cells, mucous neck cells, parietal cells, and chief cells). Released when food is in the stomach, released into the bloodstream.
3) Histamine- mainly targets parietal cells to produce more acid.
Sympathetic would inhibit all of this, and parasympathetic would stimulate all of this b/c it releases Ach.
The stomach and mucosa and the gastric glands: Mucous cells
Type of secretory cell: exocrine cells
Product secreted: alkaline mucus
Stimulus for secretion: mechanical stimulation by contents (distension)
Function(s) of secretory product: protects mucosa against mechanical, pepsin, and acid injury
The stomach and mucosa and the gastric glands: chief cells
Type of secretory cell: exocrine cell
Product secreted: pepsinogen
Stimuli for secretion: Ach, gastrin
Function(s) of secretory product: when activated, begin protein digestion
The stomach and mucosa and the gastric glands: Parietal cell
Type of secretory cell: exocrine
Product secreted: hydrochloric acid
Stimuli for secretion: Ach, gastrin
Function(s) of secretory product: activates pepsinogen, breaks down connective tissue, denatures proteins, and kills microorganisms.
The stomach and mucosa and the gastric glands: G cells
Type of secretory cell: endocrine/paracrine cell
Product secreted: gastrin
Stimulus for secretion: protein products, Ach
Function(s) of secretory product: stimulates parietal, chief
The stomach and mucosa and the gastric glands: ECL Cells
Type of secretory cell: endocrine/paracrine
Product secreted: histamine
Stimuli for secretion: gastrin
Function(s) of secretory product: stimulates parietal cells
What is the relationship between G-cells and ECL cells in acid production?
G cells activate ECL cells, which release histamine, which increases parietal cells activity to produce more acid.
In the stomach mucosa and the gastric glands which cells secrete stuff to the outside of the body?
Mucous cells, chief cells, and parietal cells
IN the stomach mucosa and the gastric glands, which cells secrete stuff to the inside of the body (ISF)?
G cells and ECL cells
What is characteristic of the mucus secretion in the stomach? (4)
1) it is derived from surface mucous epithelial cells
2) it has a lubricating function to protect against mechanical injury
3) it provides protection from self-digestion
4) since it is alkaline it protects mucosa against acid injury
(protects its both physically and chemically)
What are mucous neck cells?
Undifferentiated cells that give rise to all other cell types in gastric pits that produce acidic mucus secretion.
What is the purpose of hydrochloric acid secretion in lumen of the stomach? (3)
1) activates pepsinogen
2) Aids in the breakdown of connective tissue and muscle fibers (reducing the size of food particles)
3) Kills microorganisms
In what was are acid production levels reduced (2)
1) Most pharmaceuticals that inhibit acid production target the proton pump (proton pump inhibitors)
2) Antihistamines- lower the effect that histamines have on parietal cell function, reducing HCl production.
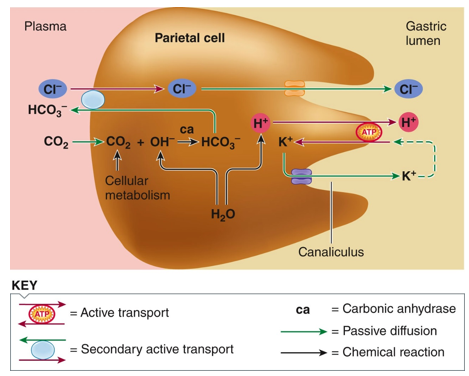
What cells are responsible for hydrochloric acid production?
Parietal cells
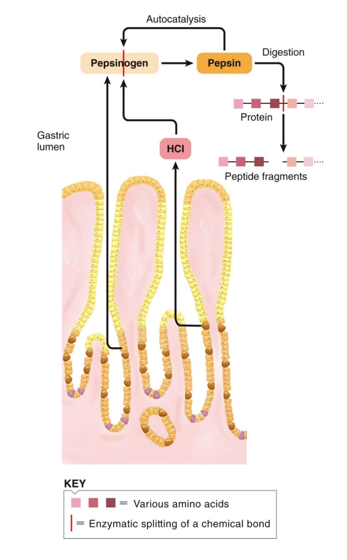
What is characteristic of pepsinogen secretion? (6)
1) Pepsinogen is an inactive enzyme stored in zymogen granules
2) it is released by exocytosis under appropriate stimulation
3) In the lumen, it is activated to pepsin. First, it needs to be activated by the previously secreted acid to convert it to its active form pepsin
4) Initiation of protein digestion.
5) Chief cells produce pepsinogen
5) Pepsin works by taking proteins from the gastric lumen and breaking them down into peptide fragments of amino acids.
6) The ENS (submucosal plexus) stimulated by distension and the presence of proteins stimulates chief cells to release pepsinogen and G-cells to release gastrin.
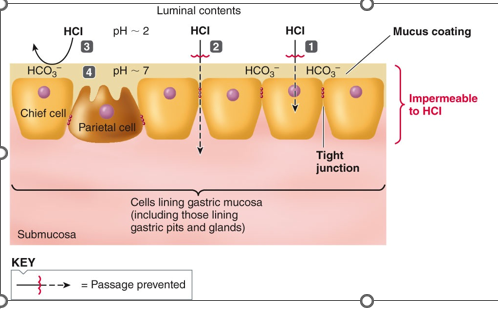
The components of the gastric mucosal barrier enable the stomach to contain acid without injuring itself. The gastric mucosal barrier helps protect from the acidic environment of the stomach and digestive enzymes (proteases) in the stomach lumen. What are four structural features that contribute to this ability?
1) The luminal membranes of the gastric mucosal cells are impermeable to H+, so the HCl and proteases cannot penetrate the cell membranes.
2) The cells are joined by tight junctions that prevent HCl from penetrating between them to get to the lamina propria.
3) A mucus coating over the gastric mucosa serves as a physical barrier to acid penetration. (prevents acid and proteases from coming in contact with the cells).
4) The HCO3- rich mucus also serves as a chemical barrier that neutralizes acid in the vicinity of the mucosa. Even when luminal pH is 2, the mucus pH is 7. The mucus is alkaline-rich and provides a chemical barrier. IF any acid can penetrate and get close to these cells, the acid is neutralized by a thick paste of alkaline mucus.
T/F Anything that breaches the gastric mucosal barrier can lead to acid having negative effects on cells and get into the lamina propria where it degrades it, leading to injury and bleeding (ulcers)
True
What was the original perception of ulcers?
The reason for increased acid production that would degrade the cell membrane and mucosal barrier to get into cells and lamina propria, where it degraded the stomach lining, was that increased acid production was lifestyle related (and therefore ulcers were also lifestyle related). Ex: caffeine and anxiety led to gastric mucosal breach. Could manage them through pharmaceuticals that could regulate acid production, but we couldn’t cure them.
T/F The gastric mucosal barrier protects the stomach lining from gastric secretions.
True
What did Berry Marshal propose and what was his reasoning?
He proposed that those with ulcers had high concentrations of Helicobacter pylori in the mucous layers. (Researchers didn’t believe that this bug could live in the stomach b/c of the high acidity.
Reasoning: The flagellum allows them to drill, spin, and burrow itself into the gastric mucosal barrier, which wasn’t too acidic of an environment b/c the alkaline mucous had neutralized the environment.
This bug produces 90-95% of all ulcers.
In his experiment, he ingested H pylori himself and developed an ulcer, then took medication, and the symptoms subsided.
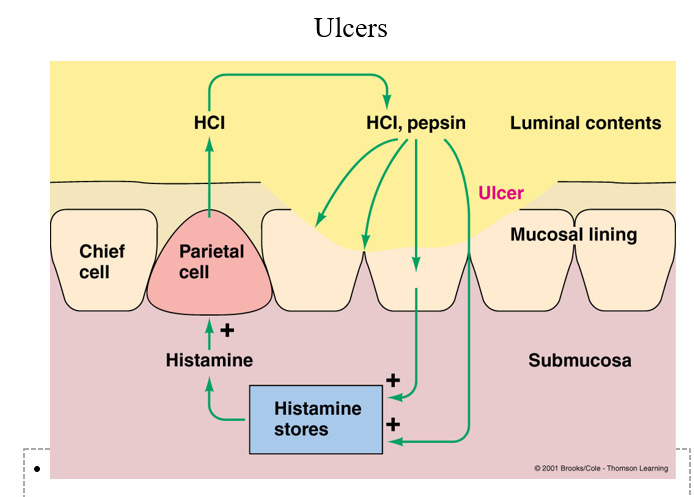
What causes the formation of ulcers and how can you treat it?
1) Helicobacter pylori comes from contaminated water (drinking water with bugs in it).
2) The bug burrows itself into the gastric mucosal barrier- grows and synthesizes proteins.
3) Bug releases secretions (waste products)- they are irritants- irritate the membrane in the cells right under the mucosal layer- some secretions squeeze between cells and trigger mast cells in inflammatory response – these mast cells release histamine (local inflammatory response)
4) Histamine is a potent stimulator of acid production in the parietal cells- this happens all the time, not just when there is food in the lumen (usually only releases acid when gastrin is triggered by food presence and distension of the stomach that triggers the ENS). Histamine stimulates parietal cells to produce acid all the time to the point the concentration of acid overwhelms the mucosal barrier, irritates and destroys and damages the cells- leads to more acid production and more damage ( a never-ending cycle) more inflammation, more histamine production.
Solution: Get rid of the bug, you get rid of the stimulus of this positive feedback loop (5-10 g penicillin-1 time treatment to get rid of the bug).
What are the four aspects of regulation of gastric motility and how are they related?
gastric filling, storage, mixing, and emptying.
As food comes into the stomach, two things happen (you need to be able to store the food and mix it with gastric secretions to start digestion).
Food comes into the stomach, which stimulates secretions to get gastric juices and motility to mix gastric juices with the food. Motility leads to emptying (need to empty slowly, not all at once). Motility needs to go down briefly so you reduce emptying.
T/F Anything that stimulates motility stimulates gastric secretion and vice versa.
True