Anatomy - Exam 4
1/95
Earn XP
Description and Tags
Chapter 9
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
96 Terms
Functions of muscles
Movement, stability, control of openings, heat production, glycemic control
Movement muscle funtion
Move body parts and body contents (breathing, circulation, digestion)
Stability muscle function
Maintain posture by preventing unwanted movements and stabilize joints by maintaining tension
Control of openings muscle function
Control of sphincters
Heat production muscle function
Skeletal muscles produce 85% of our body heat
Glycemic control muscle function
Muscles absorb and store glucose which helps regulate blood sugar
Skeletal muscle
Long, cylindrical multinucleate cells with striations → voluntaryand is responsible for the movement of bones and maintenance of posture
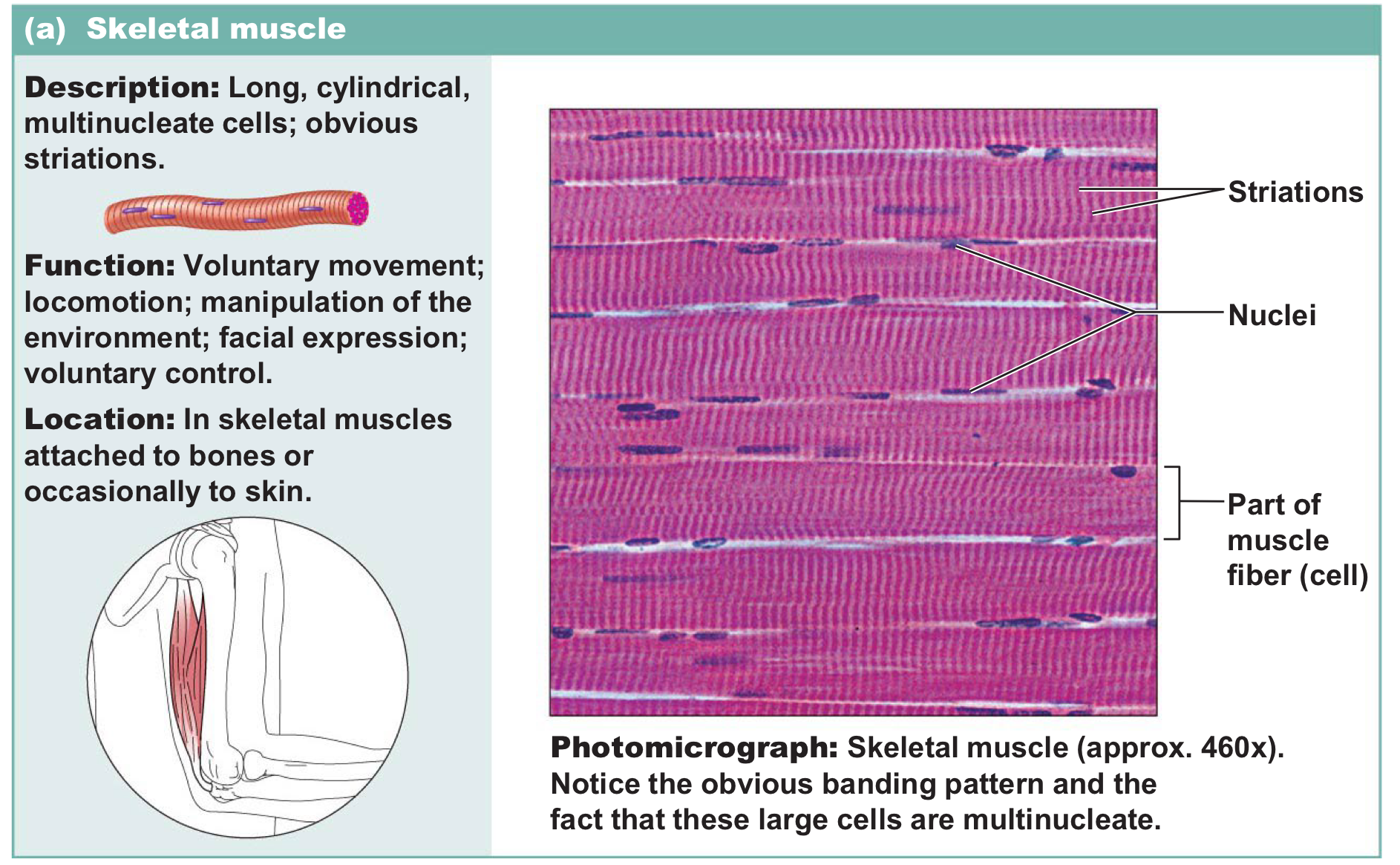
Cardiac muscle
Branching, striated uninucleate cells that connect through intercalated discs → involuntary and responsible for pumping blood throughout the body
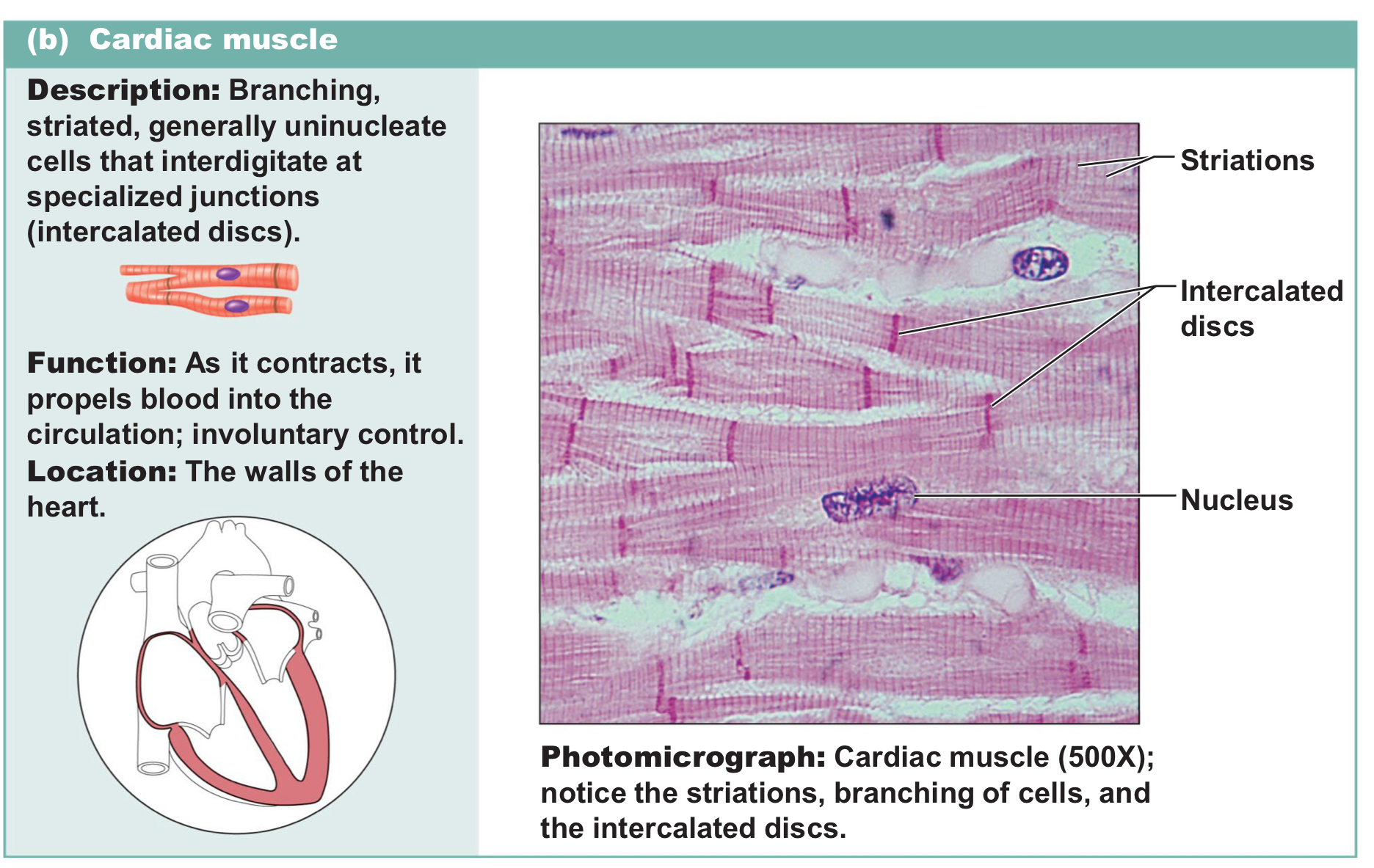
Smooth muscle
Spindle shaped cells with central nuclei and don’t have striations → involuntary and control movement in hollow organs
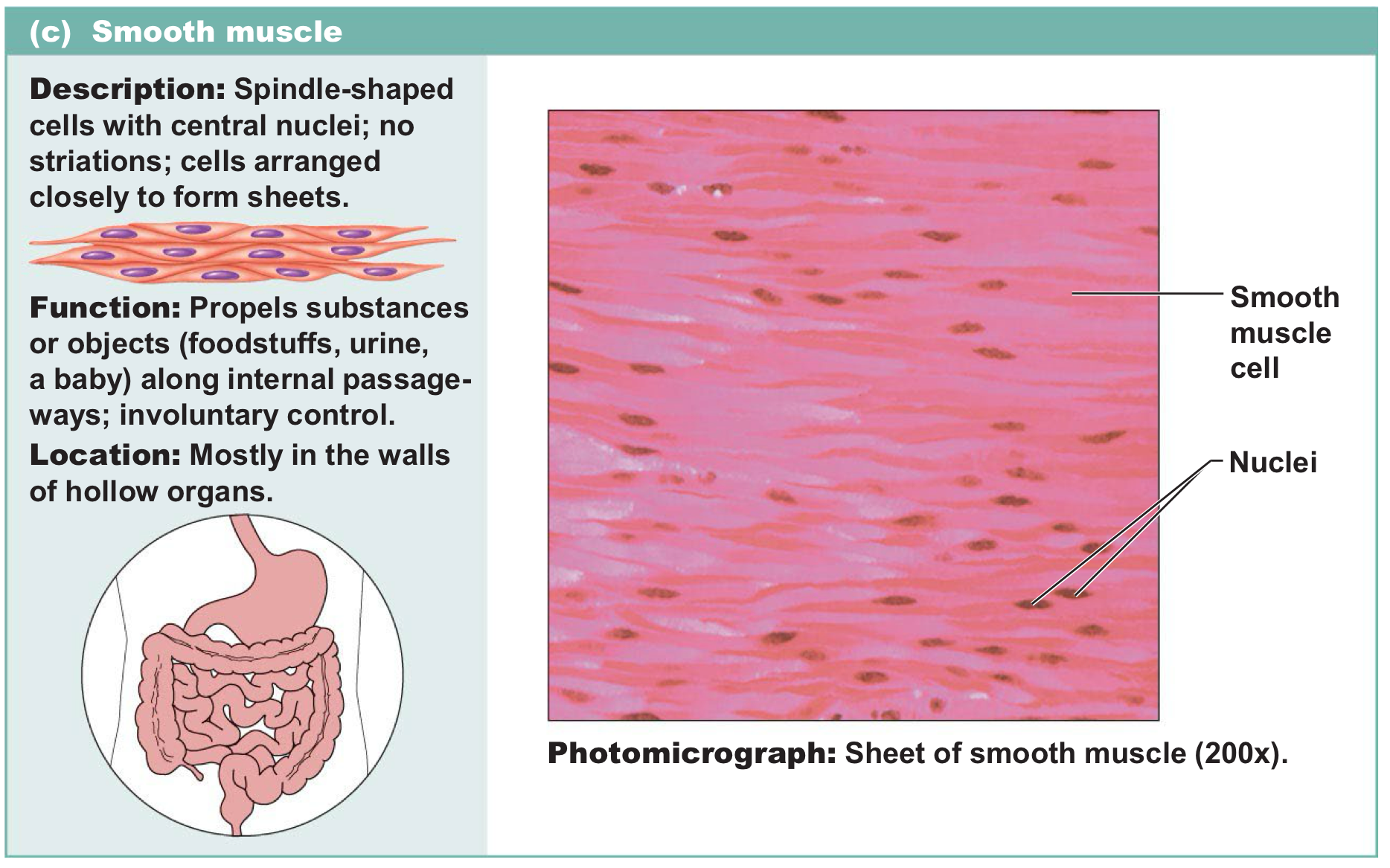
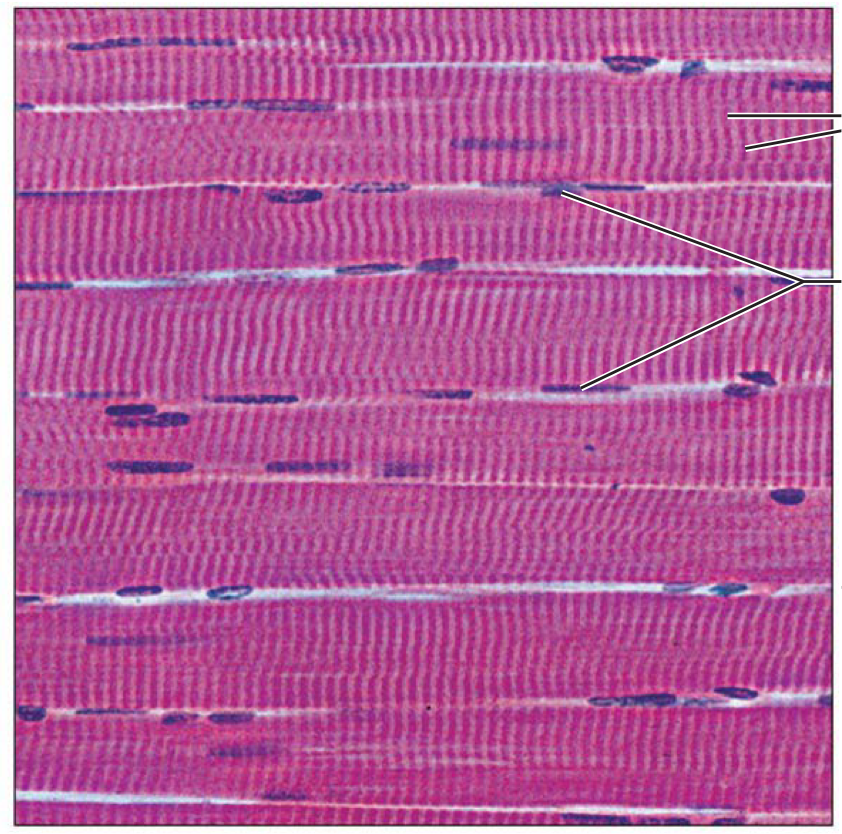
Skeletal muscle
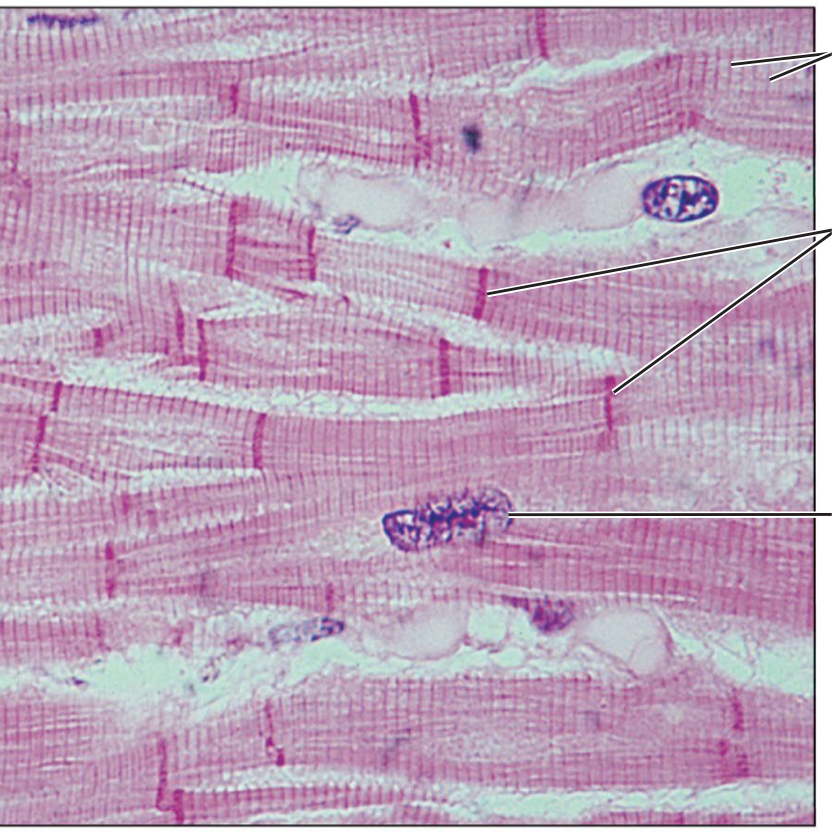
Cardiac muscle
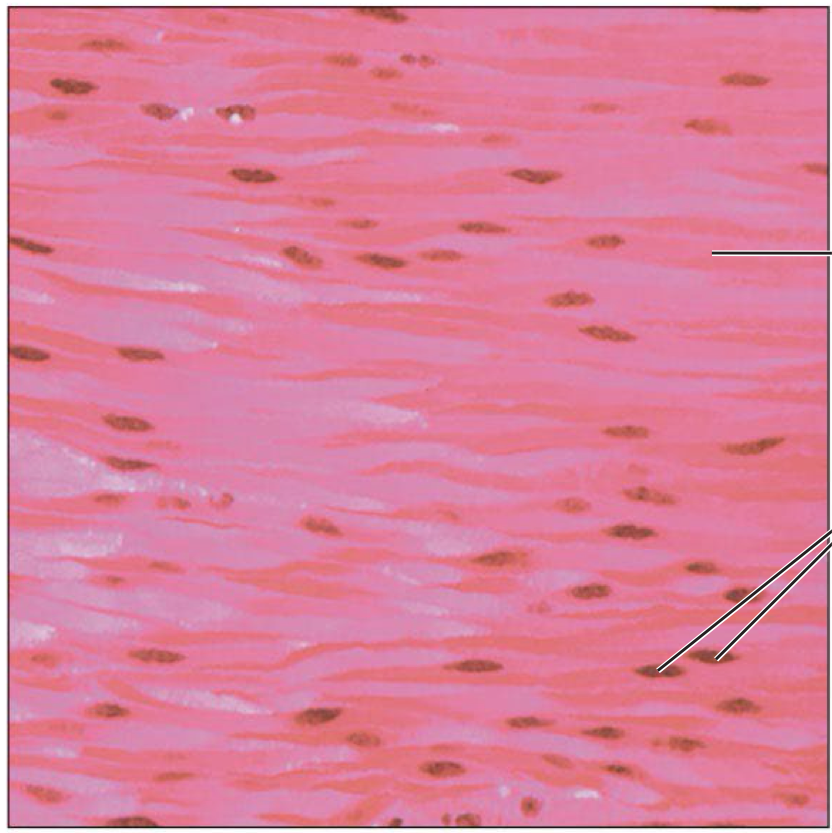
Smooth muscle
3 kinds of muscle
Skeletal, cardiac, and smooth
Myology
Study of the muscular system
What are muscles specialized for
Converting the chemical energy in ATP into mechanical energy for movement
Endomysium
Thin connective tissue around each muscle fiber → allows room for capillaries and nerve fibers, provides chemical environment for muscle fiber
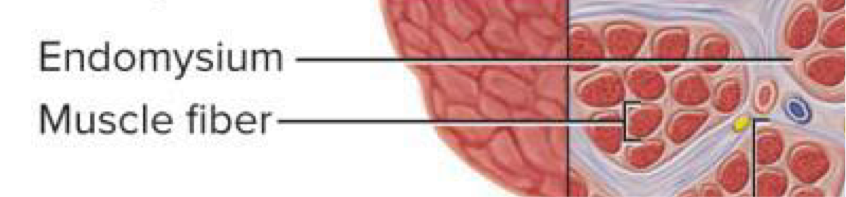
Perimysium
Thick layer of connective tissue that wraps muscle fascicles → carries nerves, blood vessels, and stretch receptors
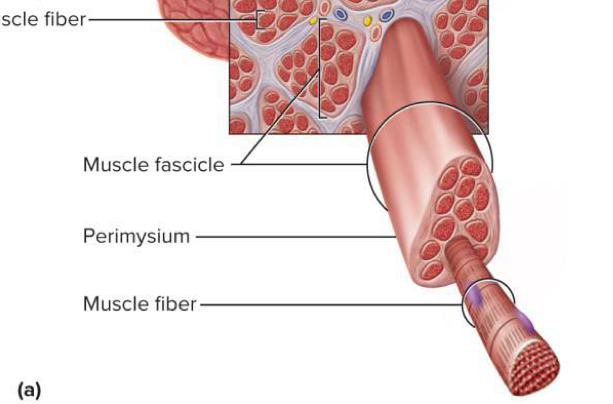
Fascicles
Bundles of muscle fibers wrapped together → wrapped by the perimysium
Epimysium
Fibrous sheath surrounding entire muscle → outer surface blends into fascia and inner projections (parts that move inward in between muscle fascicles) help form perimysium
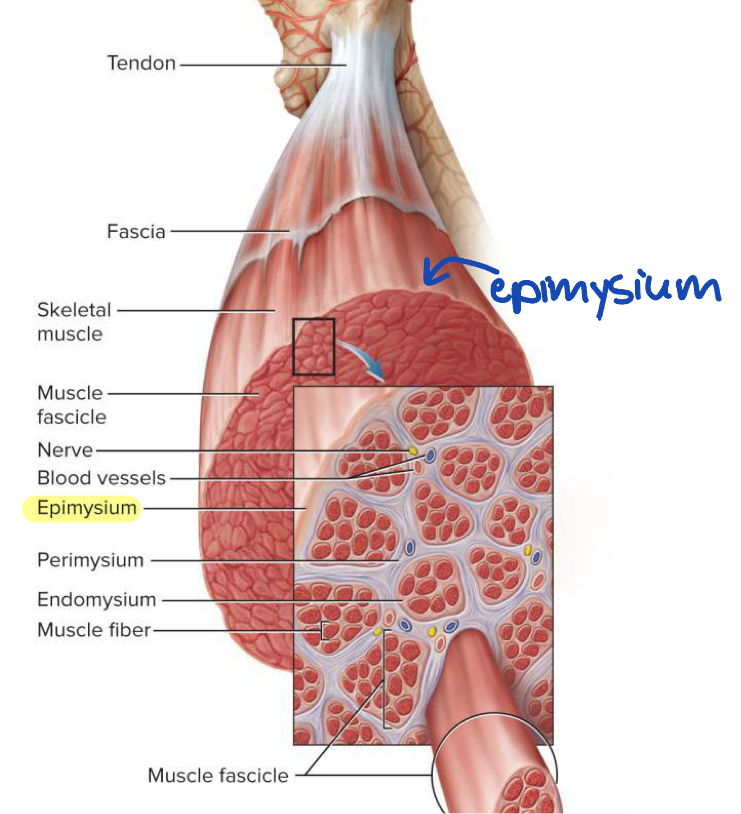
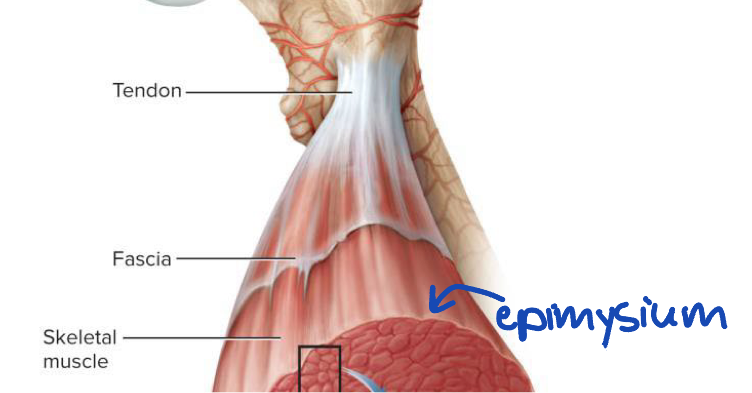
Fascia
Sheet of connective tissue that covers entire muscle and separates neighboring muscles or muscle groups from each other and the subcutaneous tissue
What determines the strength of a muscle and the direction it pulls?
The orientation of the fascicles within the muscle
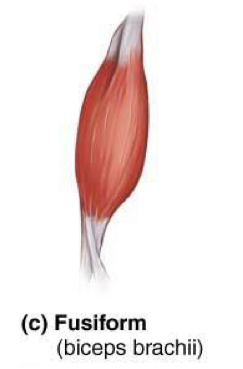
Fusiform muscles
Thick in the middle and taper at both ends → ex: biceps brachii
Parallel muscles
Uniform width (doesn’t taper) and has parallel fascicles → ex: sartorius

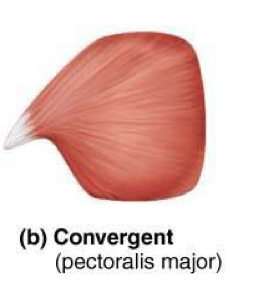
Triangular (convergent) muscles
Broad at one end and narrow at the other → ex: pectoralis major
Circular muscles (sphincters)
Form rings around body openings → ex: obicularis oris

Pennate muscles
Feather shaped and there are 3 types
Unipennate
Bipennate
Multipennate
Unipennate muscles
Fascicles attach to one side of tendon and run at an angle → ex: extensor digitorium longus
Think of feather with the tendon being the shaft and barbs only coming off one side

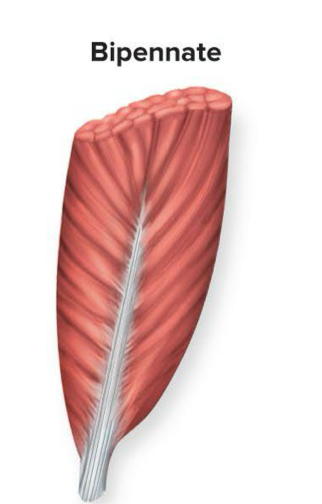
Bipennate muscles
Fascicles attach to both sides of a central tendon and run at an angle → ex: rectus femoris
Think of a feather with the tendon being the shaft and barbs coming off both sides
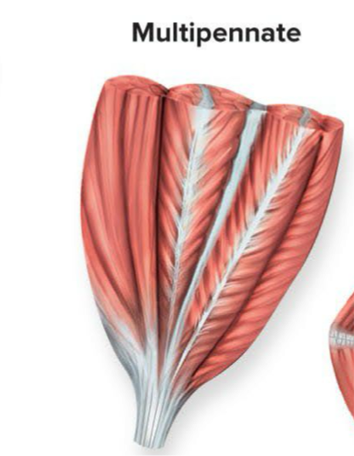
Multipennate muscles
Fascicles attach to multiple tendons within the muscle and are arranged in several feather like sections → ex: deltoid
Think of many feathers bundled together
Muscle compartment
Group of muscles that function together enclosed by fascia → also contains nerves and blood vessels that supply the muscle group
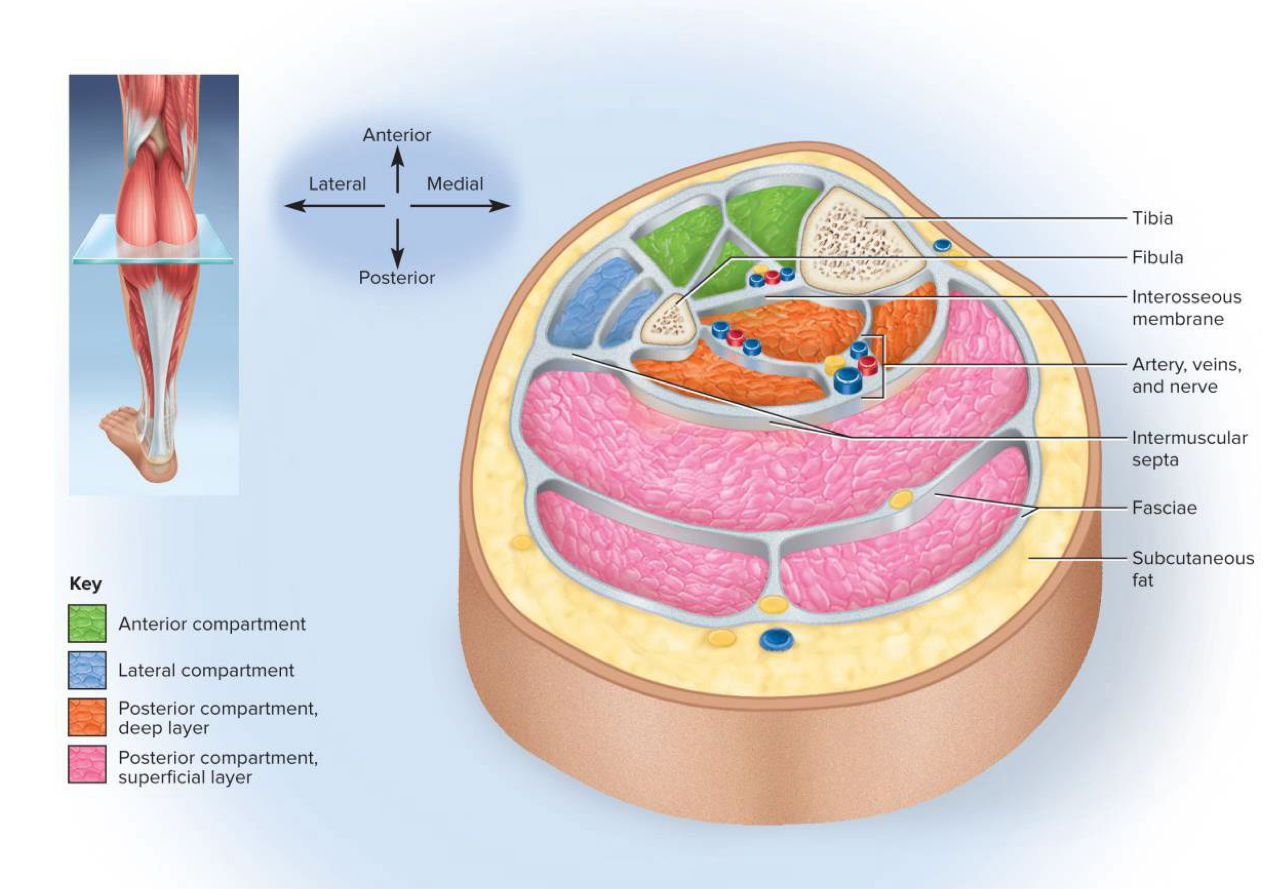
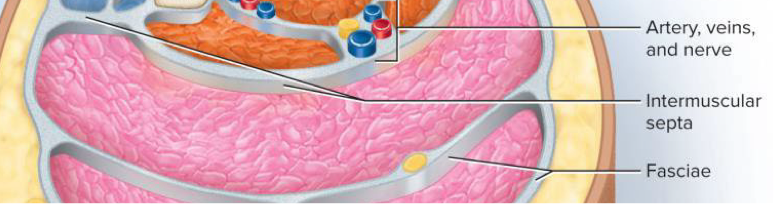
Intermuscular septa
Very thick fascia that separate muscle compartments from each other
Indirect attachment to bone
Tendons connect muscle to bone → muscle doesn’t directly touch the bone
Direct (fleshy) attachment to bone
Muscle seems to emerge directly from bone → little separation between muscle and bone
Aponeurosis
Flat, broad tendon → sheet-like tendon
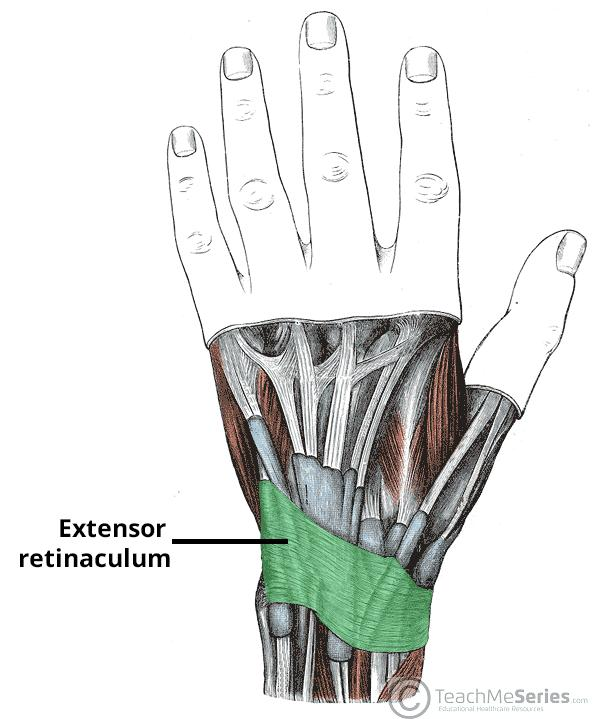
Retinaculum
Band of thickened fascia around joints that helps stabilize tendons and maintain their proper position → holds tendons in place at joints
Intrinsic muscle
Muscle that originates and inserts in the same region → muscles located entirely within a specific structure (ex: hand, foot, tongue)
Provide fine motor control and precise movement
Extrinsic muscle
Muscle that originates outside of the structure it acts on → finger movements are from extrinsic muscles in the forearm
Agonist
Muscle producing most of the force during a particular action → also known as the prime mover
Ex: the biceps brachii is the agonist when flexing the elbow
Synergist
Muscle that assists the prime mover (agonist) → may contribute additional force, stabilize nearby joint, or modify the direction of movement
Ex: the brachioradialis acts as a synergist to the biceps brachii during elbow flexion
Antagonist
Muscle that opposes the actions of the prime mover (agonist) → often relaxes while the agonist contracts
Can contract to prevent excessive movement or stabilize the joint during movement
Ex: the triceps brachii are the antagonist in flexing the elbow → when the biceps contract, the triceps relax to allow the movement
Antagonist pairs
Muscles that act on opposite sides of a joint → oppose each other’s actions during movement
Ex: biceps brachii and triceps brachii
Fixator
Muscle that prevents movement of bone → stabilizes a joint or body part during an action
Ex: the brachialis acts as a fixator in flexing the elbow by stabilizing the elbow joint
Innervation of a muscle
Refers to the nerve that stimulates a muscle
Spinal nerves innervate…
Muscles below the neck
Cranial nerves innervate…
Muscles of the head and neck → numbered CN I to CN XII
How much blood does the muscular system receive each minute at rest?
1.24 L of blood per minute at rest (about 25% of total cardiac output) → during exercise more blood is pumped to the muscles (muscles get a higher percentage of the cardiac output)
How much blood does the muscular system receive during heavy exercise?
~11.6 L per minute (about 75% of total cardiac output) → during strenuous activity, blood flow to muscles increases significantly to meet oxygen demands and the muscles receive more of the total cardiac output
Universal characteristics of muscle
Contractility
Excitability (responsiveness)
Extensibility
Elasticity
Conductivity
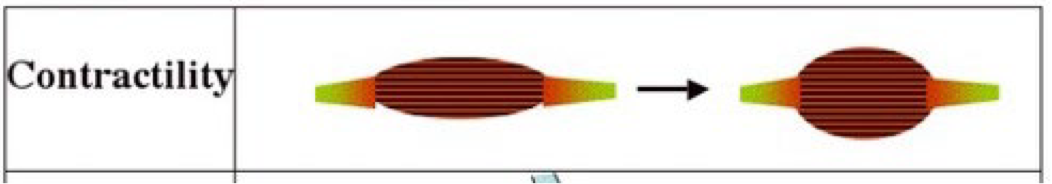
Contractility
Ability of a muscle to shorten (contract) when stimulated
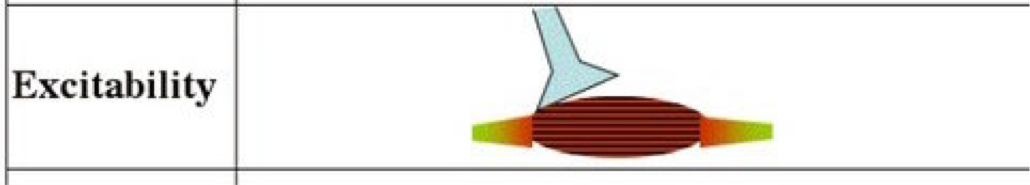
Excitability (responsiveness)
Ability of a muscle to respond to chemical signals, stretch, and electrical charges across the plasma membrane → this characteristic enables muscle fibers to receive stimuli and initiate a contraction
Extensibility
Muscles are capable of being stretched between contractionsand can extend beyond their resting length without damage

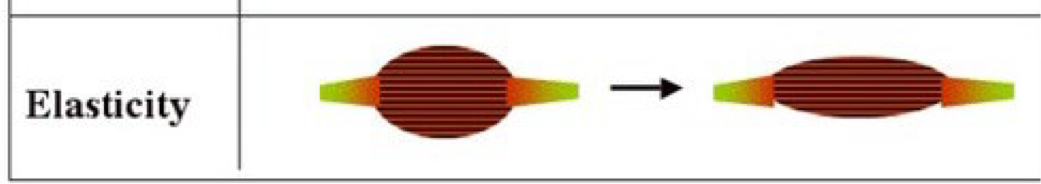
Elasticity
Ability of a muscle to return to its original rest length after being stretched
Conductivity
Local electrical excitation sets off a wave of excitation that travels along the muscle fiber
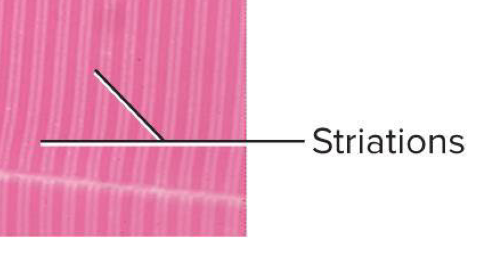
Striations
Alternating light and dark transverse bands in skeletal muscle → result from the arrangement of internal contractile proteins (actin and myosin filaments)
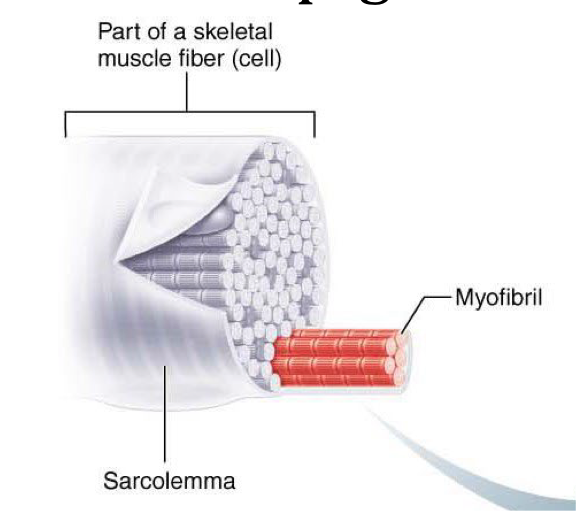
Sarcolemma
Plasma membrane of a muscle fiber
Sarcoplasm
Cytoplasm of a muscle fiber that contains organelles and myofibrils, as well as other components vital for muscle contraction
Myofibrils
Long protein cords occupying most of sarcoplasm inside muscle fiber (cell) → made of repeating sarcomeres lined up end to end
Glycogen
Carbohydrate (polysaccharide) stored in muscle fibers to provide energy for exercise → acts as a ready-to-use fuel source
Myoglobin
Red protein in muscle cells that binds oxygen, facilitating oxygen storage and transport during muscle contraction.
Red, oxygen-binding protein found in muscle cells → stores oxygen inside muscle fibers and releases it when the muscle needs it like during exercise
Source of SOME oxygen needed for muscle activity
Myoblasts
Stem cells that fused to form each muscle fiber early in development
Satellite cells
Unspecialized stem cells (myoblasts) that remain between the muscle fiber and endomysium (connective tissue around each muscle fiber)
Play a role in regeneration of damaged skeletal tissue
Outside of sarcolemma
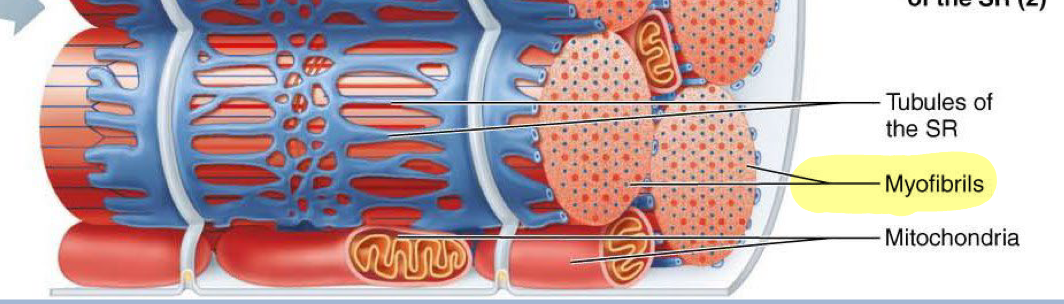
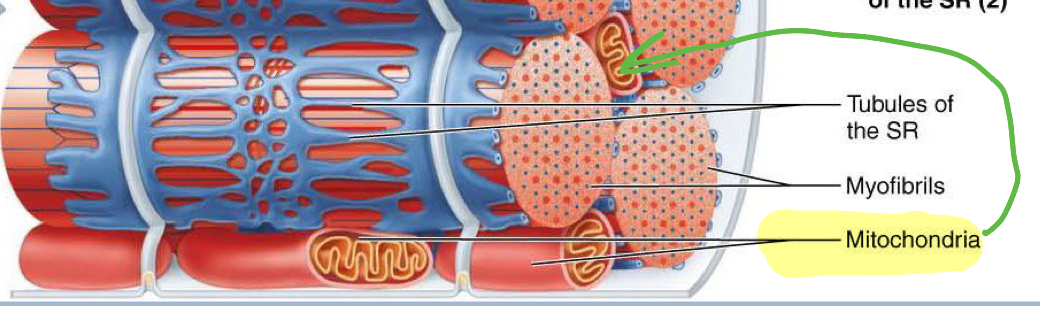
Mitochondria location muscle fiber (cell)
Packed into spaces between myofibrils
Sarcoplasmic reticulum (SR)
Smooth ER that forms network around each myofibril and stores calcium ions, playing a crucial role in muscle contraction

Terminal cisterns
Dilated sacs of sarcoplasmic reticulum (SR) that store calcium ions and release them to initiate muscle contraction → located and A-band and I-band junctions on myofibrils
Forms “triad” with transverse tubule → 2 terminal cisterns with 1 transverse tubule in the middle
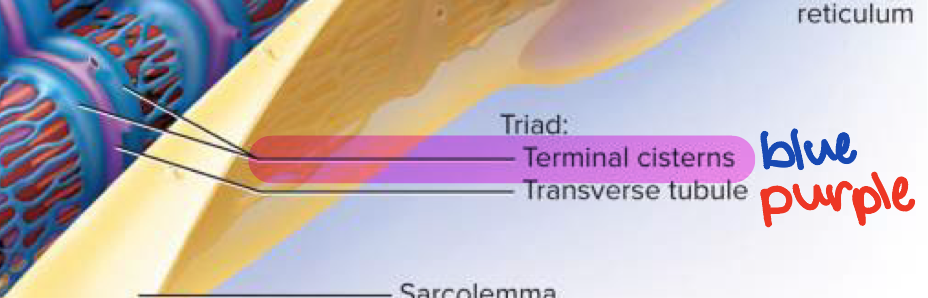
Transverse tubules (T tubules)
Inward “tunnels” of the sarcolemma that run through the muscle fiber and create the triad with terminal cisterns → openings of transverse tubules found in sarcolemma
Carry electrical signals (action potentials) from the surface quickly to the interior of the muscle fiber → makes sure all parts contract simultaneously

Triad
Structure formed by T tubule and two terminal cisterns associated with it → one T tubule with a terminal cistern on each side
ensures rapid uniform conduction at the A-I junction
Thick filament
Myofilament made of several hundred myosin molecules → each molecule is shaped like a gold club where two chains are intertwined to form a shaft like tail with a double globular head at the end
Think of intertwined chains as shaft of club and the 2 globular heads as the clubhead
Heads on half on the thick filament angle to the left and the heads on the other half angle to the right with a bare zone with no heads in the middle
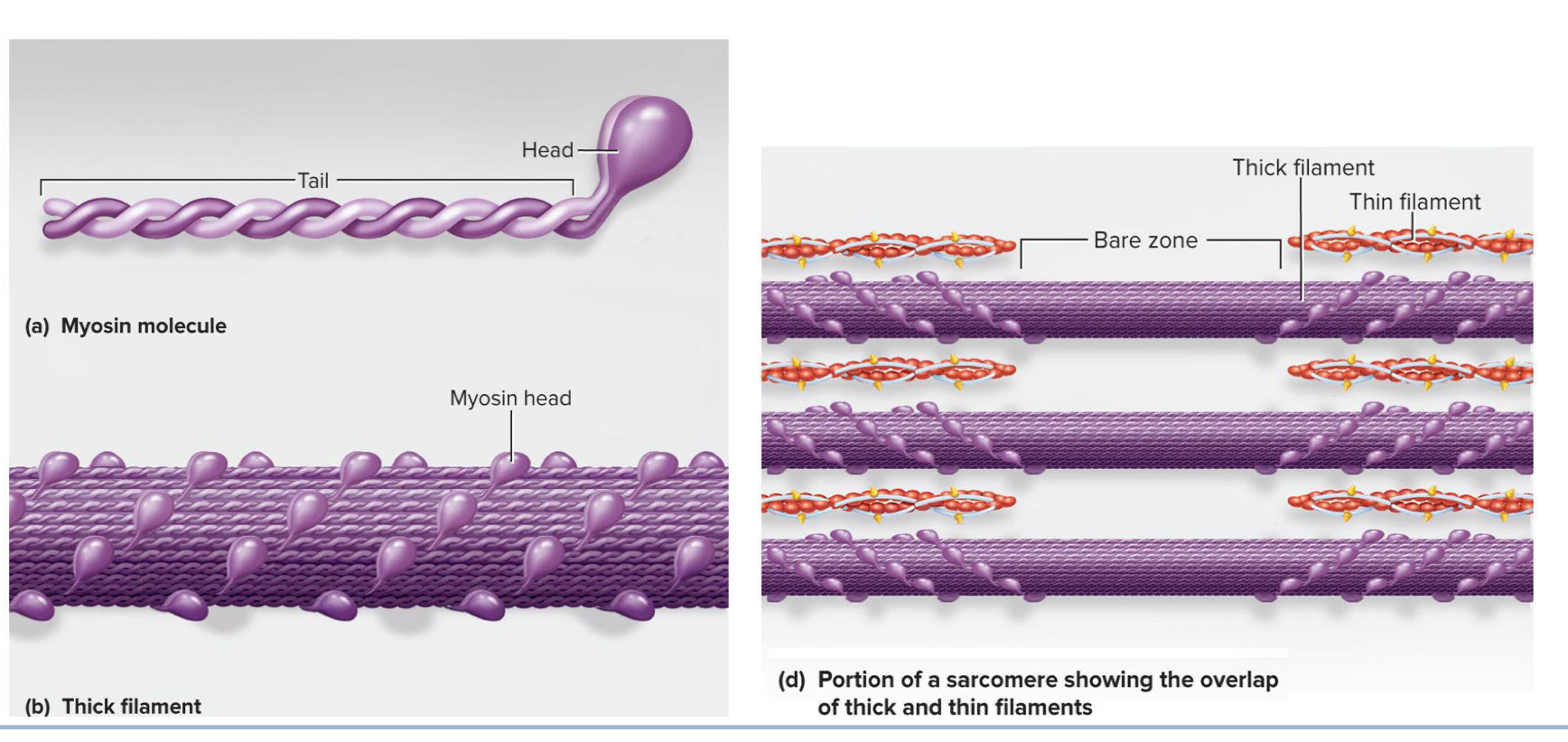
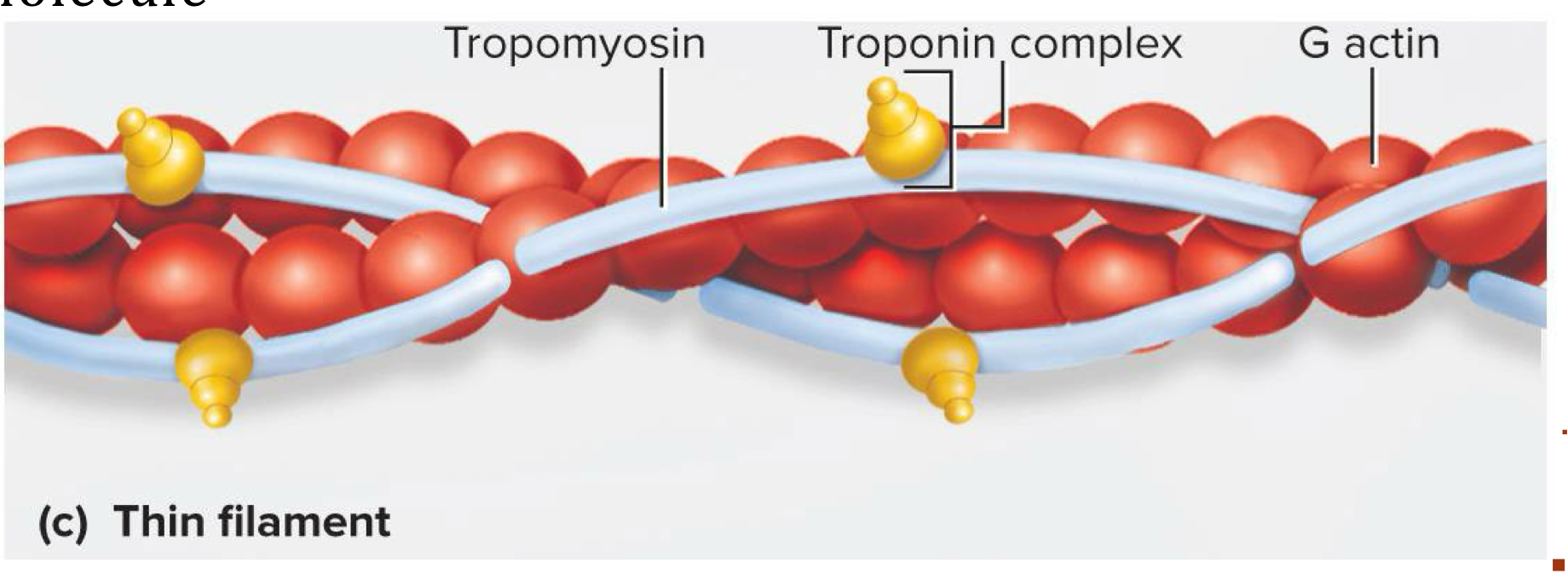
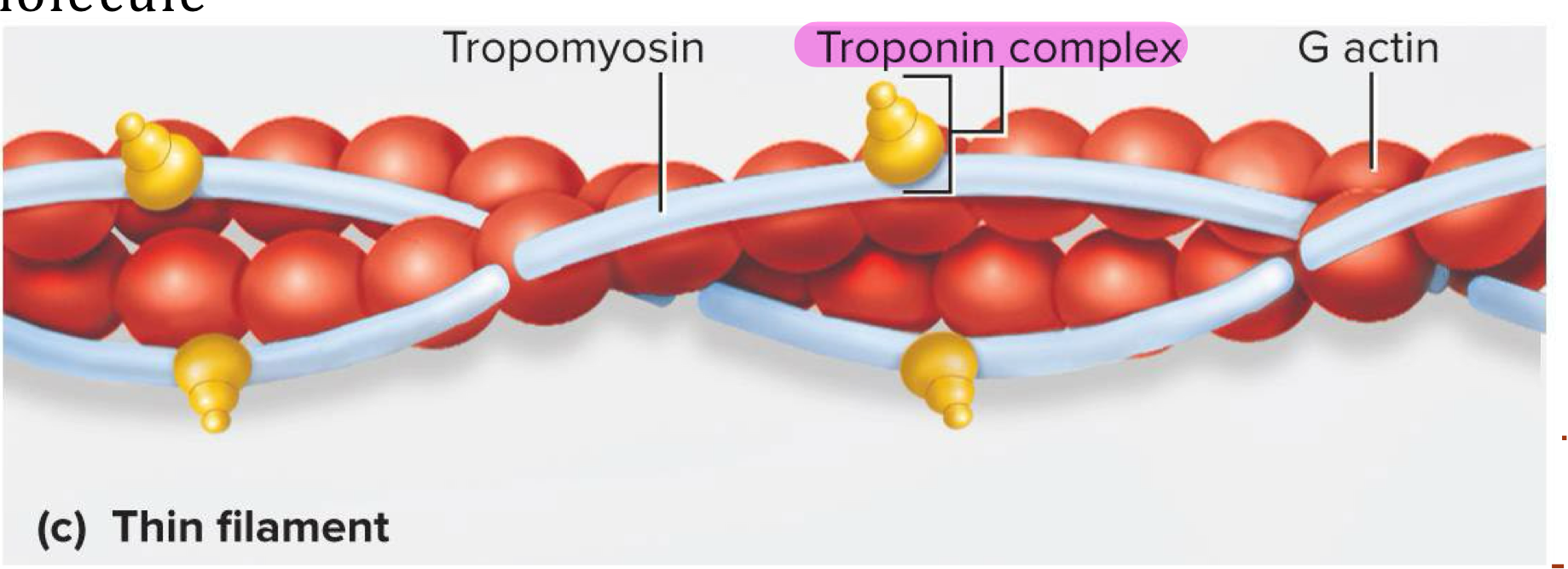
Thin filament
Myofilament made of 2 intertwined fibrous (F) actin strands → fibrous (F) actin strand made of string of globular (G) actin subunits each with an active site that can bind to myosin head
Has tropomyosin molecules and troponin molecules
Tropomyosin molecules
Long protein that runs along actin strands and block the myosin binding sites at rest → each tropomyosin molecule blocks 6-7 active sites
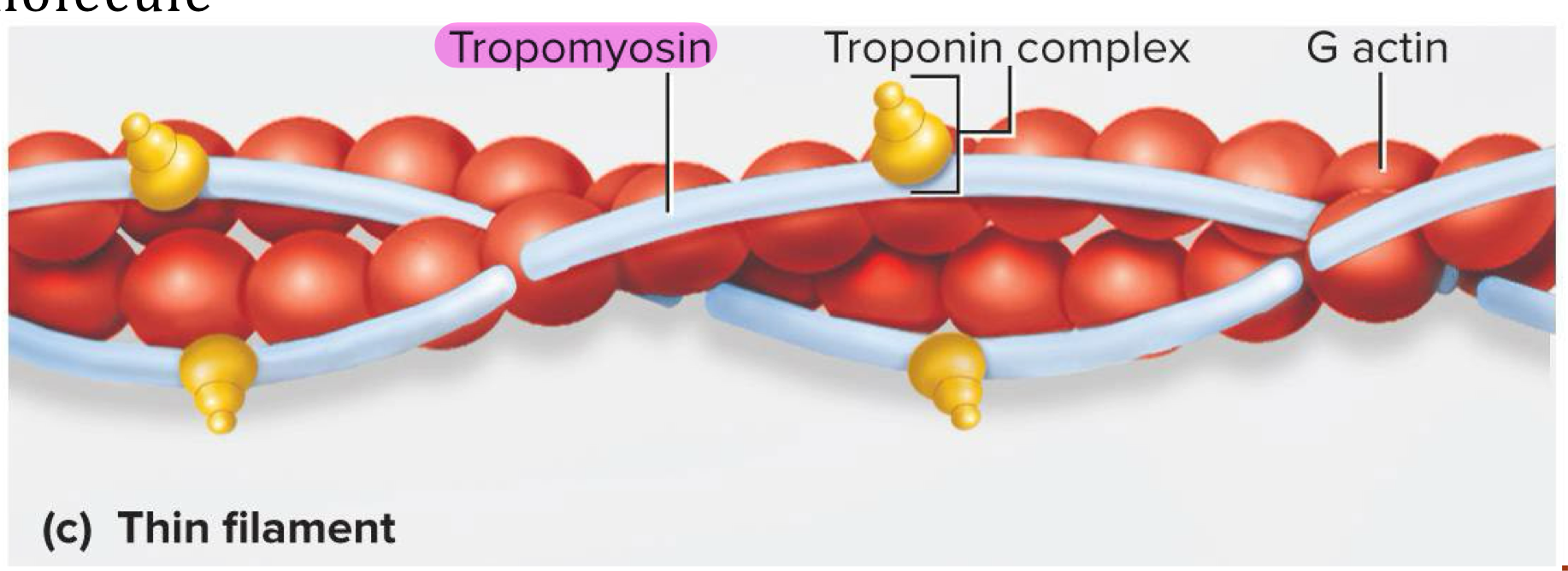
Troponin molecules
Small calcium binding protein on each tropomyosin molecule → when calcium binds to troponin, the tropomyosin molecules move and uncover the myosin binding sites on actin strands
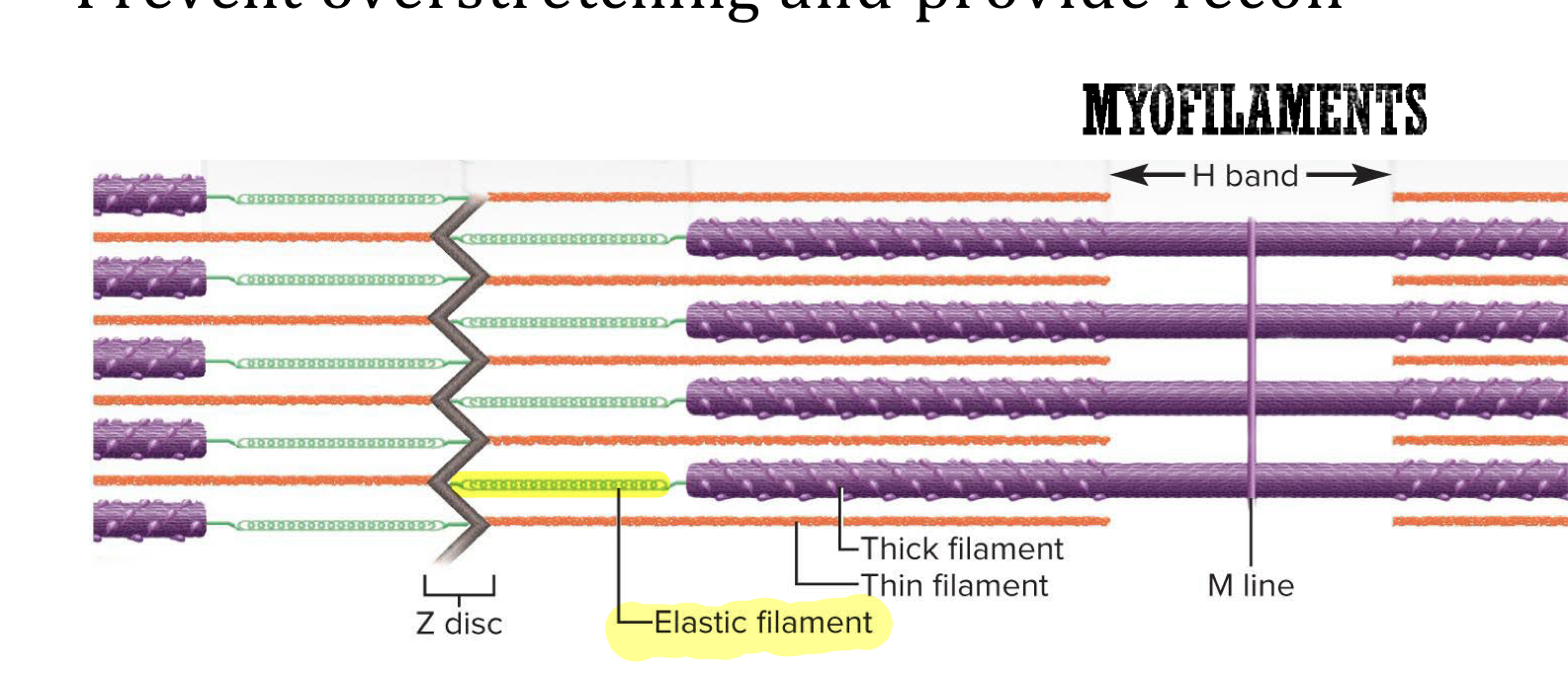
Elastic filament
Myofilament made of titin proteins (huge, springy proteins) that provide elasticty, prevent overstretching, and anchor thick filaments → run through the core of thick filament and anchor it to Z-disc and M-line
Helps maintain muscle alignment
When the muscle is stretch titin stretches and then pulls the thick filament back into position
Contractile proteins
Myosin and actin proteins are responsible for the work of contraction
Regulatory proteins
Tropomyosin and troponin act like switch that determines when fiber can and can’t contract
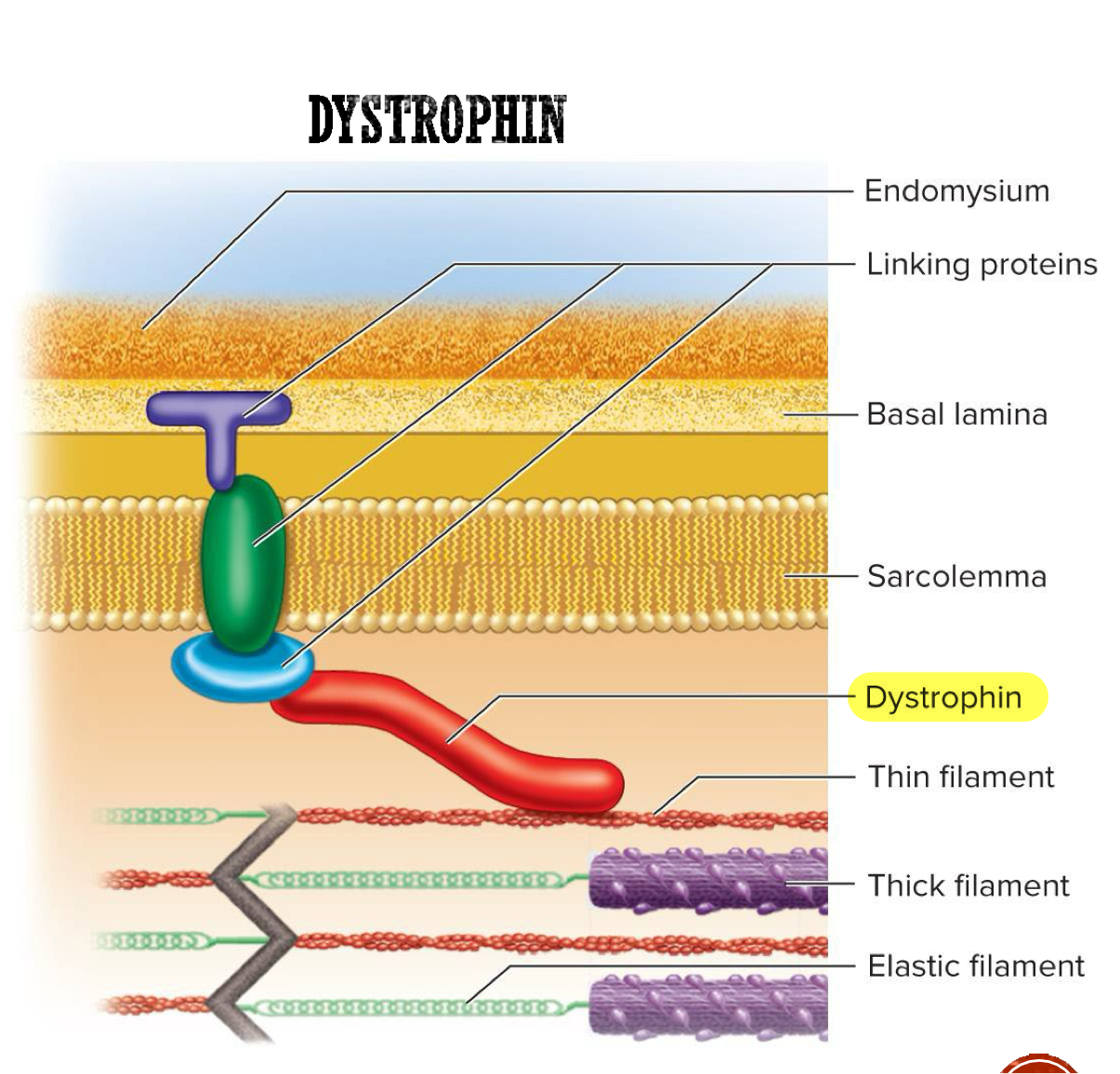
Dystrophin
Protein that links actin in outermost myofilaments to membrane proteins that link to endomysium (connective tissue around muscle fibers) → transfers forces of muscle contraction to connective tissue leading to tendon
Acts as shock absorber
Striations are alternating…
A-bands (dark) and I-bands (light)
A-band
Dark bands of myofibrils where thick (myosin) filaments overlap with thin (actin) filaments
H band = middle of the A-band and its not as dark because it contains only thick filaments, with no overlap from thin filaments (also where there are no myosin heads from thick filaments)
M-line = middle of H band
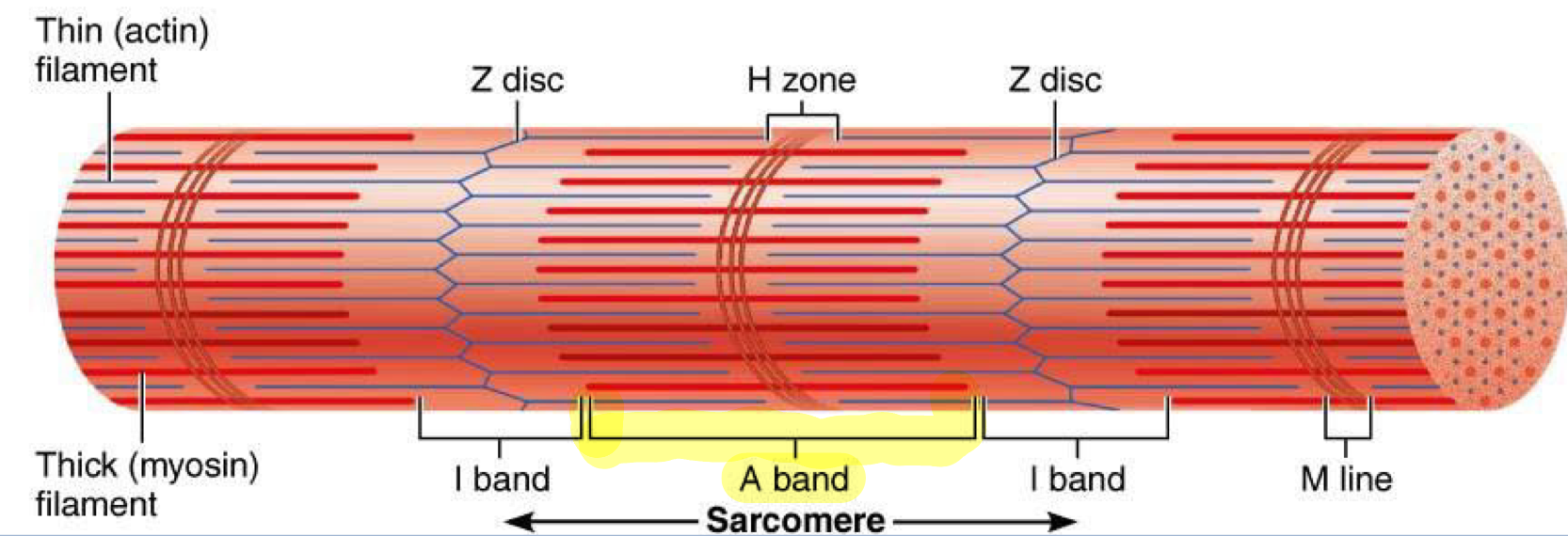
I-band
Light bands of myofibrils that contain only thin (actin) filaments and no thick (myosin) filaments, located on either side of the A-band
Also contains Z-disc
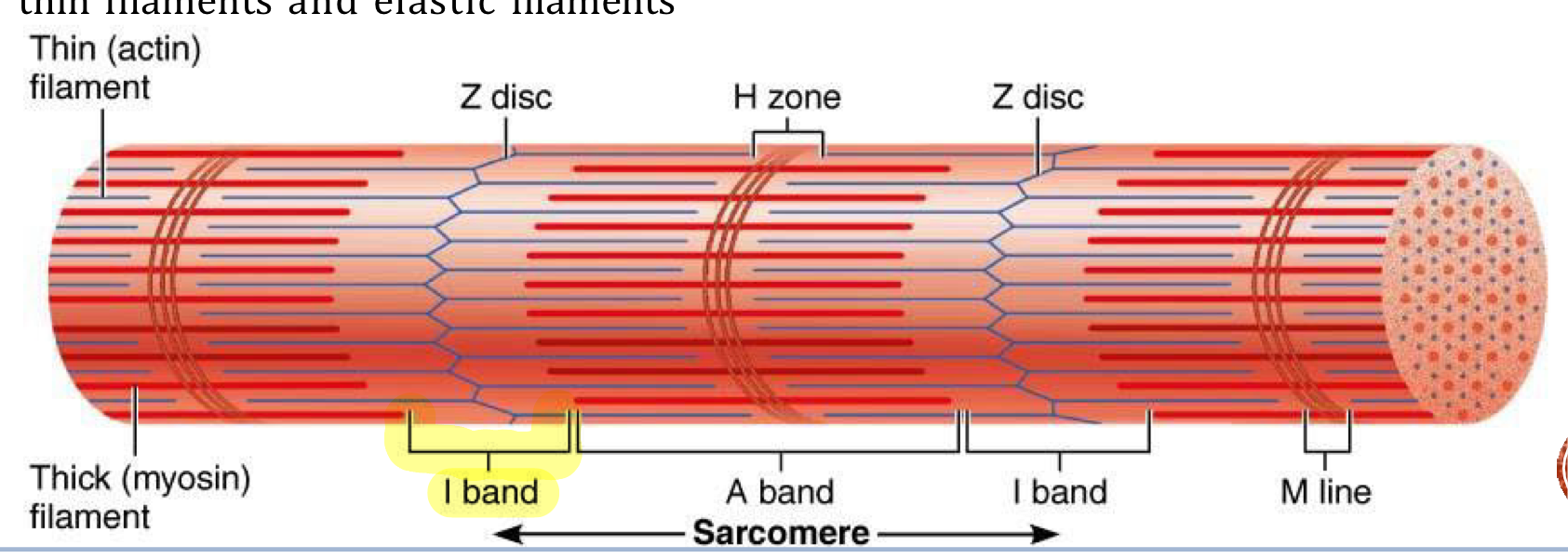
Z-disc
Dense protein plate that acts as an anchor for thin and elastic filaments, connecting them between adjacent sarcomeres
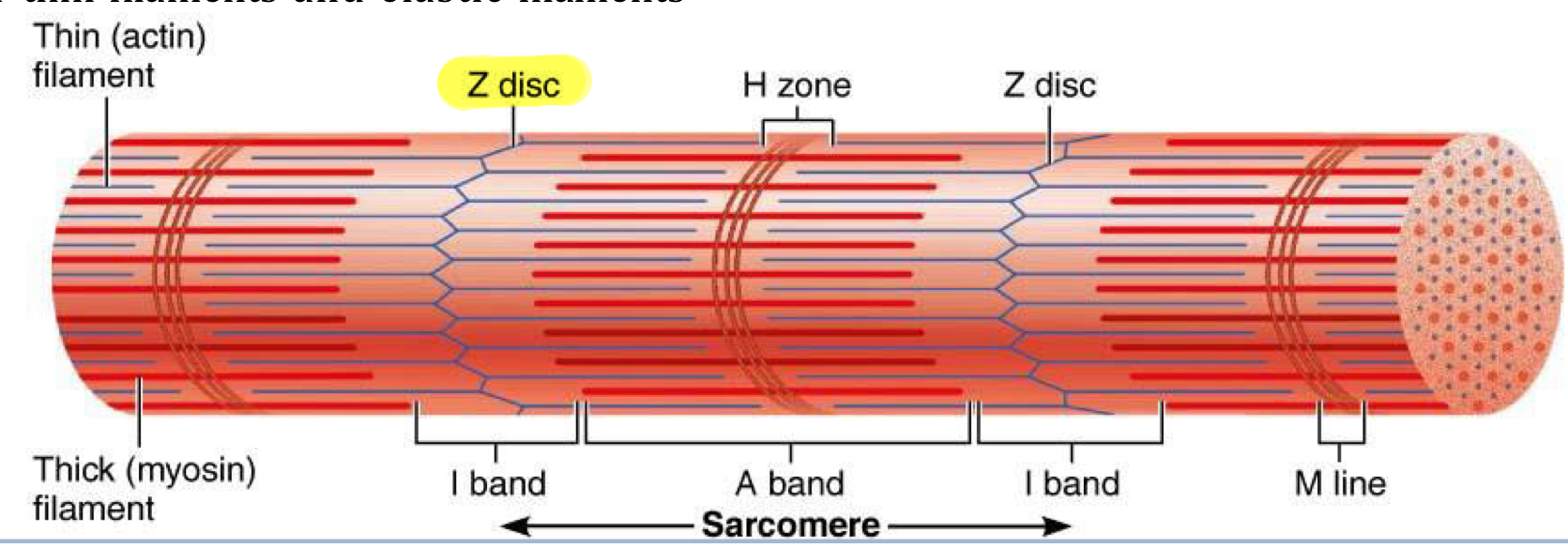
Sarcomere
Segments of myofibrils from z-disc to z-disc → functional contractile unit of muscle fiber
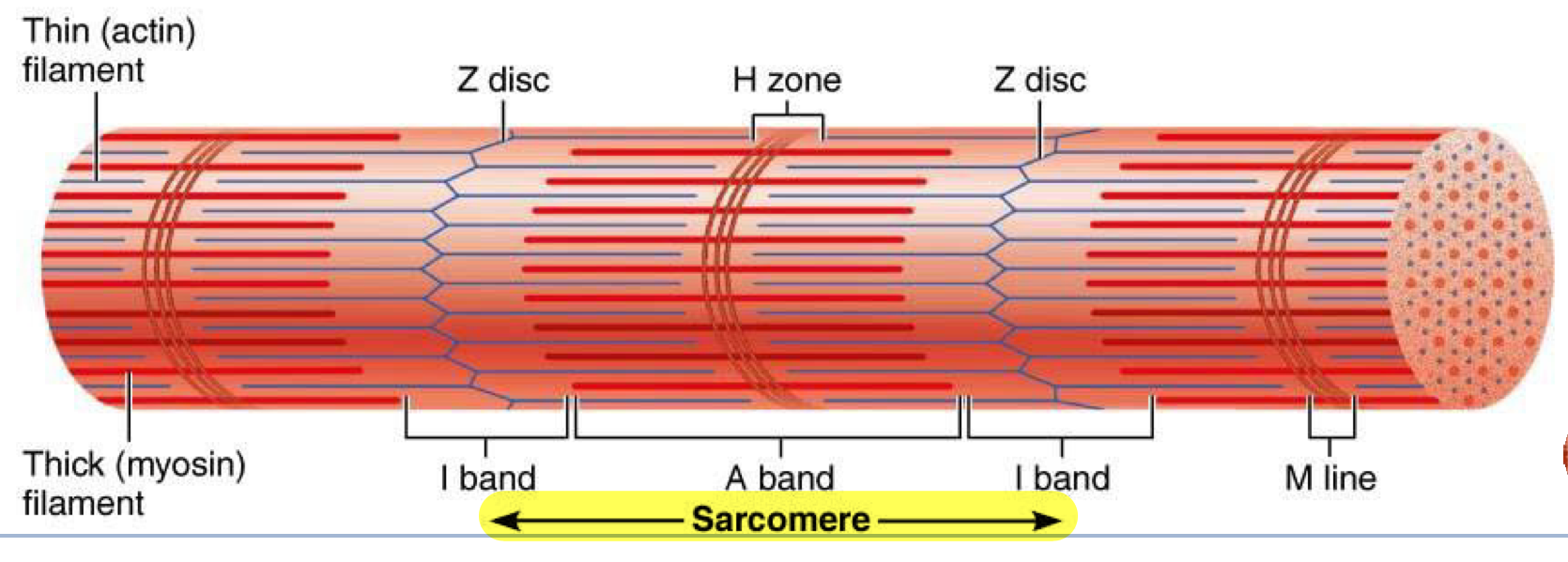
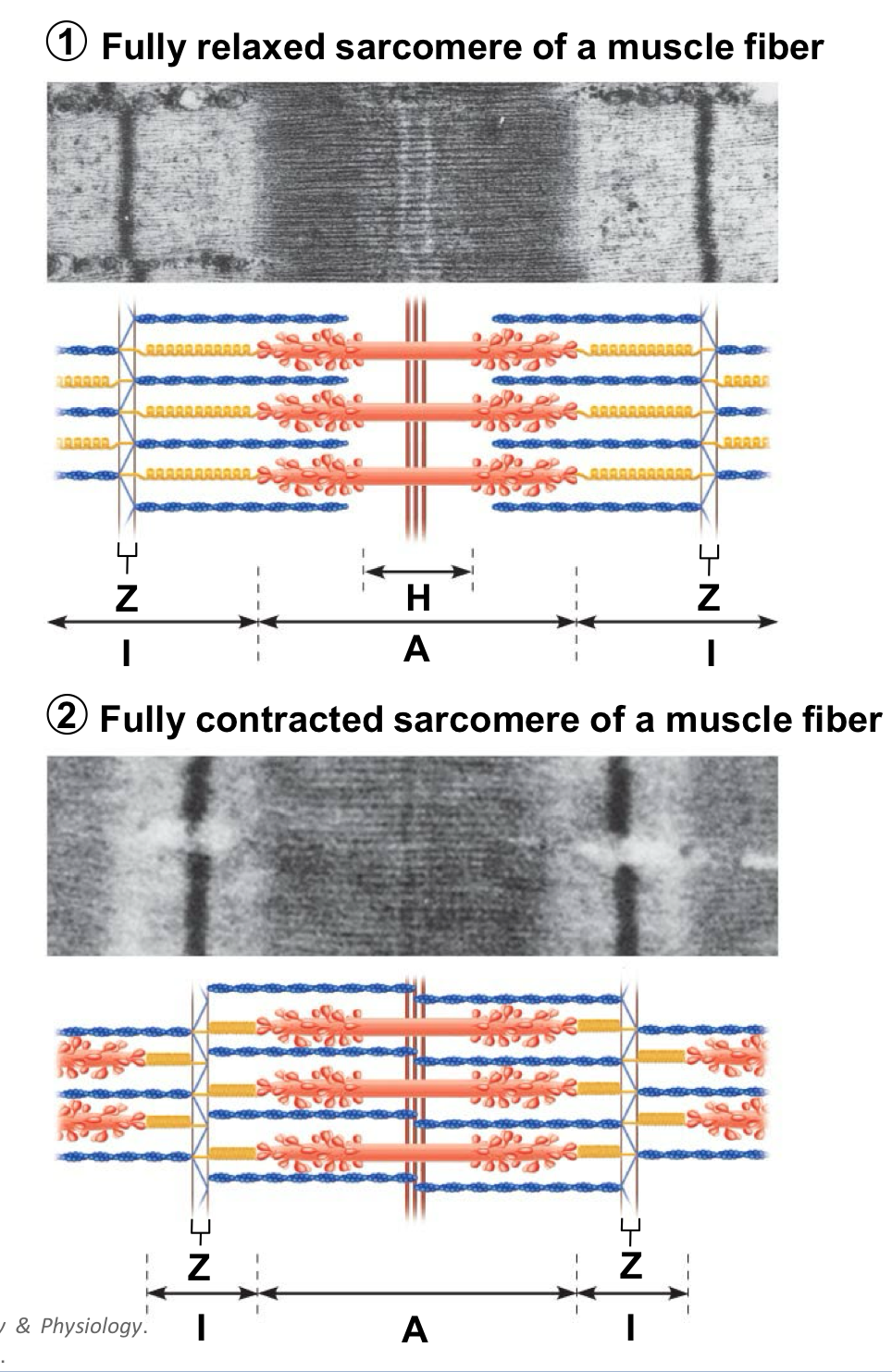
Muscle cells shorten because…
their individual sarcomeres shorten → Z-discs are pulled closer together as thick and thin filaments slide past each other during contraction
neither thick or thin filaments change length during muscle shortening, only the amount of overlap between them changes
Structural hierarchy of skeletal muscle from biggest to smallest
Muscle
Muscle fascicles
Muscle fibers
Myofibrils
Sarcomeres
Myofilaments
Sliding filaments start when…
Myosin heads bind to actin to form cross bridges→ thick filaments pull the thin filaments toward the center of the sarcomere (H band and M line), causing contraction
Z-discs are pulled closer to M-line → I-bands shorten because overlap increases → H band (area with only thick filaments) disappears → A bands move closer together but their lengths stay the same
Denervation atypohy
Shrinkage of paralyzed muscle when nerve remains disconnected
Somatic motor neurons
Nerve cells whose bodies are int he brainstem and spinal cord that serve skeletal muscles
Their axons that lead to the skeletal muscle = somatic motor fibers
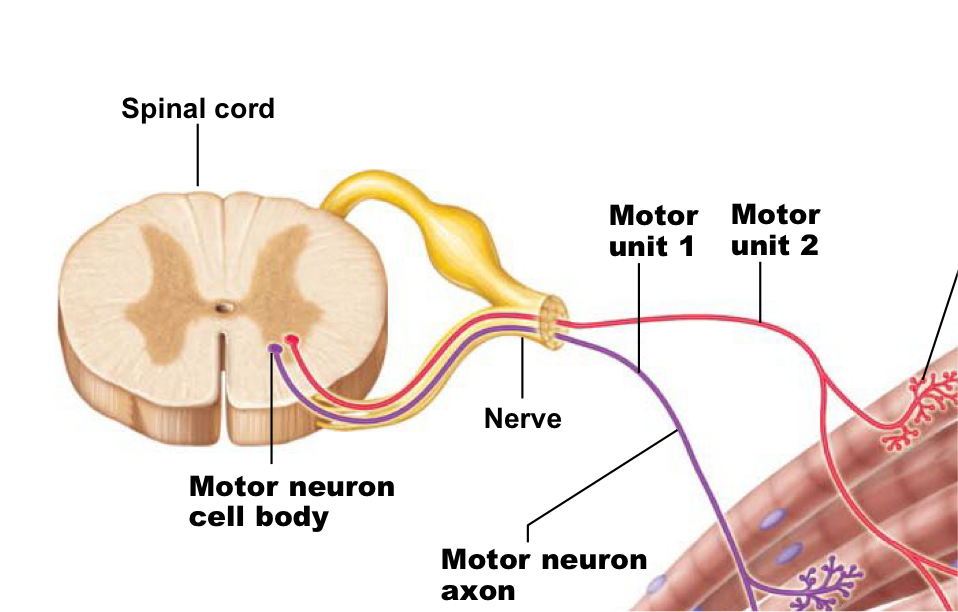
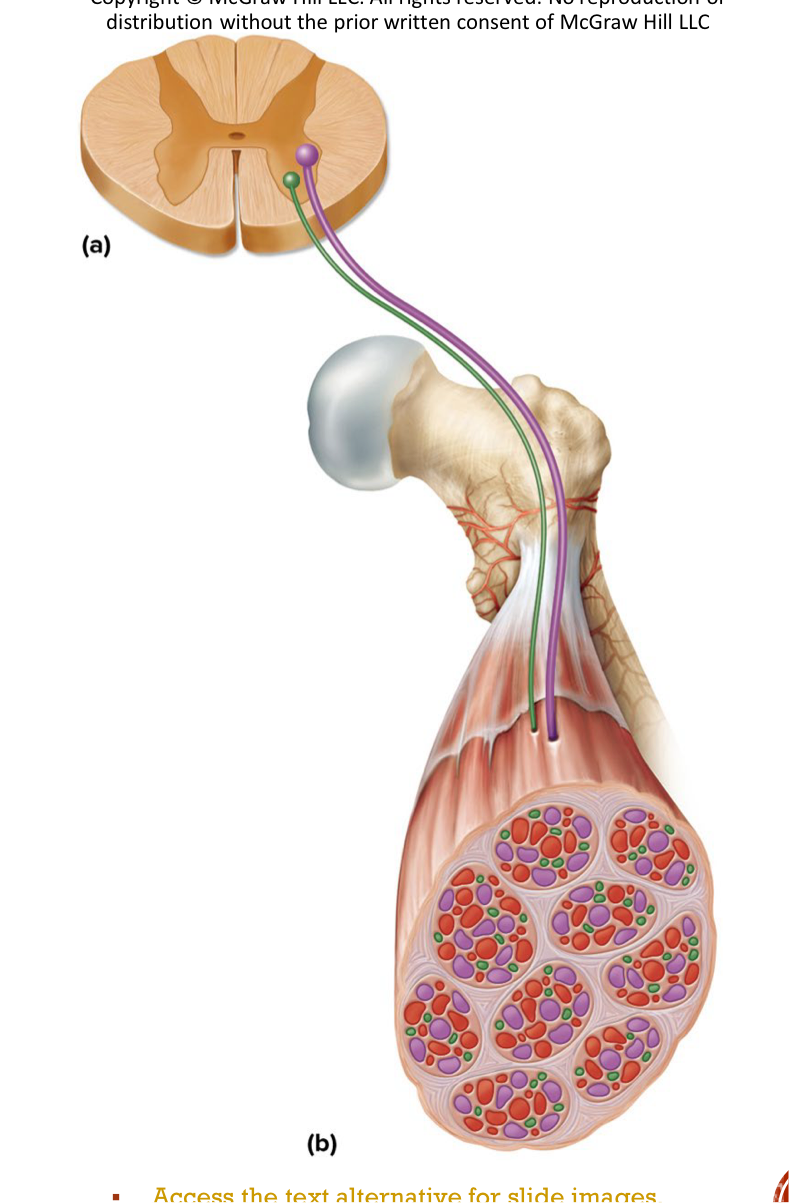
Motor unit
One nerve fiber and all the muscle fibers innervated by it → muscle fibers of one motor unit are dispersed throughout the muscle
Produce weak contraction over wide area and provide ability to sustain long term contraction as motor units take turns contracting
Effective contraction usually requires contraction of several motor units at once
Small motor units
Fine degree of control → 3-6 muscle fibers per neuron (ex: eye and hand muscles)
Average motor units
~200 muscle fibers per neuron
Large motor units
More strength than control → up to 1,000 muscle fibers per neuron (ex: leg muscles)
Powerful contractions by large motor units
Muscle action potential
Sodium gates open in plasma membrane of muscle fibers and sodium flows into cell down gradient
Depolarization → inside of plasma membrane becomes more positive because of more Na+
Sodium gates close and potassium gates open
Potassium rushes out of cell and repolarization occurs → membrane becomes negative again because of loss of positive ions
Potassium channels close
Difference between resting membrane potential (RMP) and action potential
RMP is seen in waiting excitable cell while action potential is a quick event seen in a stimulated excitable cell
Acetylcholine (ACh)
Initiates muscle contraction when released from synaptic vesicles of axon terminal (through exocytosis) and binds to receptors on muscle cell membrane, allowing sodium influx and triggering an action potential
Acetylcholinesterase (AChE)
Breaks down ACh, allowing for muscle relaxation
Excitation of muscle fibers
Action potential arrives at axon terminal of neuromuscular junction and ACh is released from synaptic vesicles
ACh binds to receptors on sarcolemma (motor end plate) and open ligand-gated Na+ channels resulting in depolarization/end plate potential (more positive = less negative charge)
Action potiential initiated in muscle fiber → it travels along the sarcolemma and T tubules
Terminal cisterns of SR release calcium which binds to troponin molcules, tropomyosin moves and exposes myosin binding sites on actin strands
Myosin binds to actin (formation of cross bridge) and contraction begins
Relaxation after contraction
Nervous stimulation stops, so ACh stops being released
ACh is broken down by AChE
Calcium is reabsorbed by terminal cisterns of SR → troponin loses calcium and tropomyosin moves back to blocking myosin binding sites
Tension decreases and muscle returns to resting state
Spastic paralysis
State of continual contraction of the muscles becuase AChE can’t degrade ACh → possible suffocation
Some pestisides contain cholinesterase inhibitors
Ex: lockjaw
Flaccid paralysis
State in which the muscles are limp and cannot contract → Botulism prevents ACh release