Hypoglycaemia
1/30
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
31 Terms
What is HYPOGLYCAEMIA?
1) Defined as a blood glucose level of below 4 mM (72 mg/dL)
2) Symptoms may develop at higher levels if there is rapid fall of previously elevated levels, although some individuals may show no effects even below 4 mM
3) A rapid fall in blood glucose may produce a phase of sweating, tachycardia and agitation due to activation of the sympathetic nervous system and release of adrenaline & glucagon
What are the SIGNS and SYMPTOMS of Hypoglycaemia?
1) Symptoms: equivalent to cerebral anoxia and may include moodiness, faintness, numbness in arms and hands, blurred vision, confusion, memory loss, dizziness or lethargy that may progress to coma
2) Serious consequences of hypoglycaemia relate to effects on the brain – loss of cognitive function, seizures and coma
3) Loss of consciousness occurs at blood glucose levels of 2.5 mM (45 mg/dL)
4) Rapid restoration of blood glucose (by i.v. glucose or injection of glucagon) is essential and prolonged or repeated hypoglycaemia may result in permanent brain damage
What are the CAUSES of Hypoglycaemia?

What is ALCOHOL-INDUCE Hypoglycaemia?
1) Develops several hours after alcohol ingestion
2) Occurs on depletion of glycogen stores when blood glucose is reliant on hepatic gluconeogenesis
What are the SHORT-TERM consequences of Alcohol-Induced Hypoglycaemia?
In the short-term (24 hours): consumption of alcohol places additional stresses on gluconeogenesis, as alcohol is metabolised primarily in the liver by an unregulated process
What are the LONG-TERM consequences of Alcohol-Induced Hypoglycaemia?
In the long-term (years): consumption of alcohol can result in reduced gluconeogenesis as a result of liver damage and reduced muscle mass (longer term)
Metabolism of Alcohol
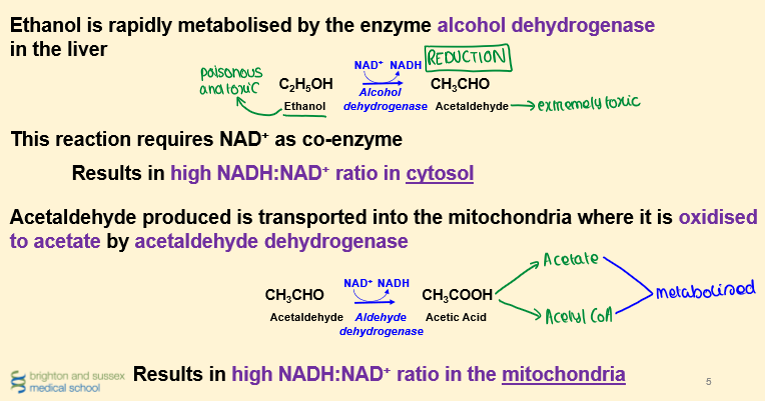
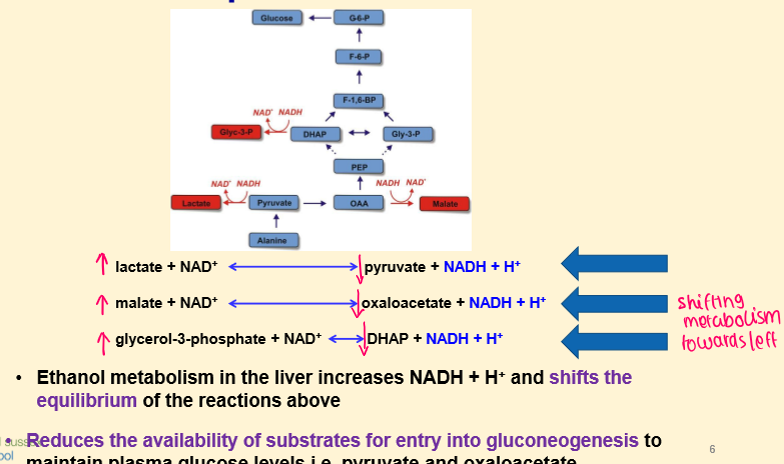
Metabolic Consequences of Alcohol Metabolism
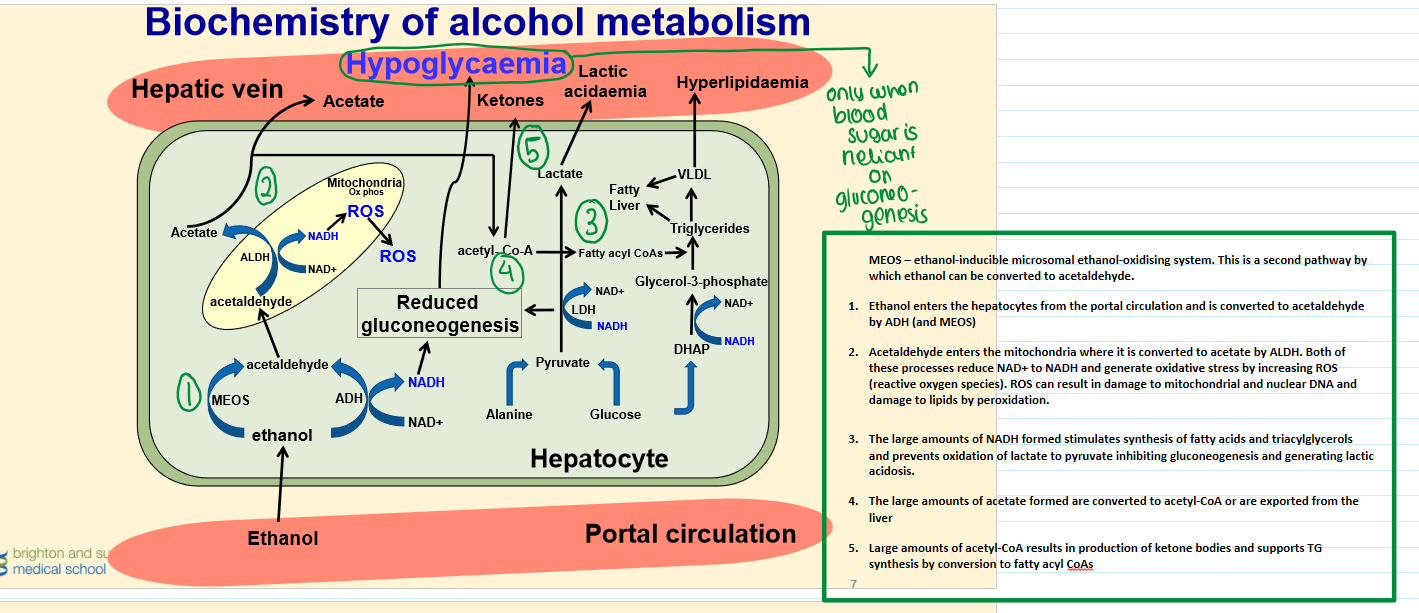
Biochemistry of Alcohol Metabolism
What are the SYMPTOMS of Alcohol-Induced Hypoglycaemia?

Long-term Alcohol Consumption - Effects on Lipid Metabolism

How does FATTY LIVER DISEASE progress?

Long-term alcohol consumption: effects on efficiency of ethanol metabolism

What are the CONSEQUENCES of Accumulation of Acetyl CoA?

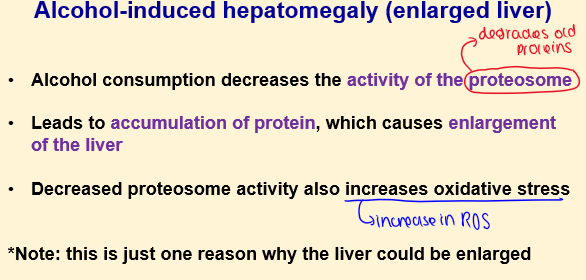
What is Alcohol-Induced HEPATOMEGALY?
What is Alcohol-Induced Thiamine Deficiency

What are the CAUSES of Alcohol-Induced Thiamine Deficiency?
1) Malnourishment
2) Ethanol interferes with GI absorption
3) Hepatic dysfunction, which hinders storage and activation to thiamine pyrophosphate
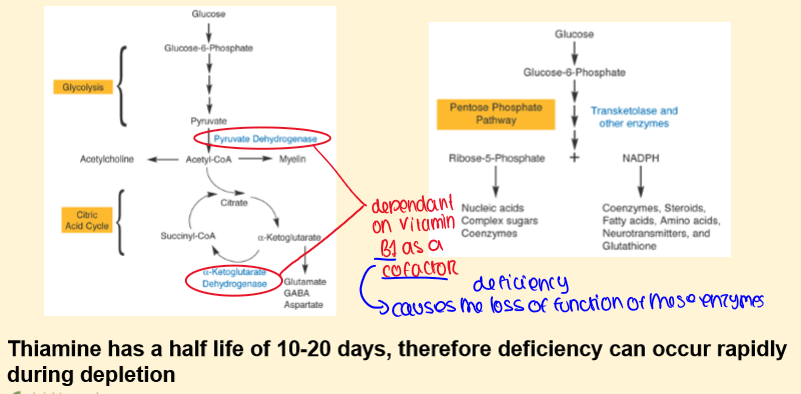
How does THIAMINE act as a COFACTOR for many enzymes?
What are GLYCOGEN STORAGE DISEASES?
1) Inherited diseases in which the stores of glycogen are affected by defects in either the enzymes of synthesis or degradation of glycogen.
2) Many different types depending on which enzyme is affected
3) They are all autosomal recessive except for type IX which is sex-linked
4) All result in the production of an abnormal amount or abnormal type of glycogen
Types of Glycogen Storage Disease
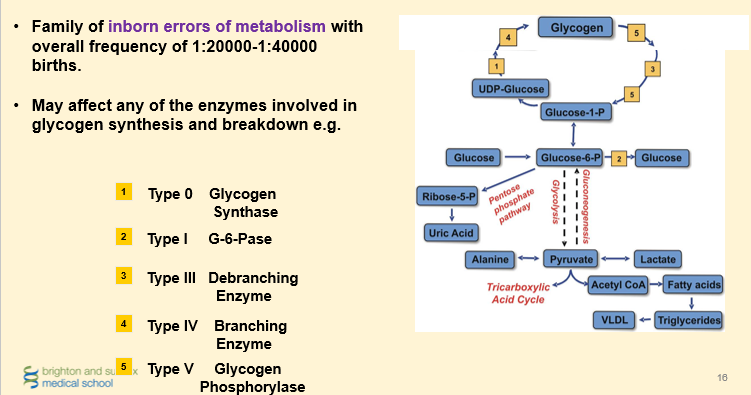
Type I. Von Gierke’s Disease
Affects mainly the liver and kidneys caused by a deficiency in glucose 6-phosphatase
Type II. Pompe’s Disease

Type III Cori’s Disease
1) The amylo 1,6 glucosidase (de-branching enzyme) is deficient.
2) Unable to break down glycogen, resulting in hypoglycaemia.
3) Strangely, symptoms often disappear at puberty.
Type IV Andersen’s disease
1) One of the most severe of these diseases.
2) Liver glycogen in normal amounts but comprises long unbranched chains that have low solubility.
3) Sufferers seldom live beyond five years.
Type V. McArdle’s syndrome
1) Affects muscle glycogen phosphorylase (liver enzyme is normal).
2) Muscle cannot break down glycogen (which accumulates).
3) Sufferers have a low tolerance to exercise and fatigue easily, with painful muscle cramps after exercise.
4) Otherwise, they have a normal life-span.
What is TYPE 1 GSD?

What is the MECHANISM of C=Von Gierke’s Disease?
1) Lack of glucose-6-phosphatase means that glucose cannot be exported from the liver.
2) Results in high levels of G-6-P in the liver & kidney
3) Glucose-6-phosphate is metabolized to lactic acid or converted to glycogen or lipid
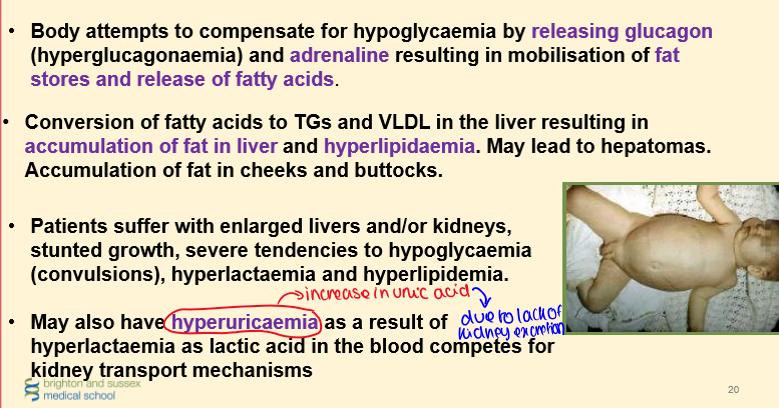
What are the CONSEQUENCES of Von Gierke’s Disease?
This results in:
1) Abnormal levels of glycogen accumulation in the liver and kidney – causing enlargement of the liver and kidneys
2) Increased glycolysis leading to lactic acidosis
3) Increased fatty acid, TG and VLDL synthesis and excretion.
Metabolism in Von Gierke’s Disease
What are the MANAGEMENT and TREATMENT of Von Gierke’s Disease?

Why is Gluconeogenesis inhibited during Oxidation of Alcohol in Liver?
Due to Depletion of Metabolic Requirements