L2- Genetic, molecular and cellular basis of cancer intro
1/28
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
29 Terms
what are the main facts and stats about cancer
More than 350,000 new cases registered annually.
Breast, lung, bowel and prostate cancer account for over 50% of cases
One in two lifetime risk of diagnosis.
One in four will die from cancer
Disease risk rises significantly with age: ~65% occur in people over 65.
200 types- heterogenous
what is cancer
A heterogeneous group of diseases in which single cells acquire the ability to proliferate abnormally, resulting in an accumulation of progeny
Cancers are those tumours that have acquired the ability to invade through surrounding normal tissues
The most advanced form of this invasive process is metastasis, a state in which cancer cells escape from their original location, travel through the blood or lymphatic systems and take up residence at distant sites”
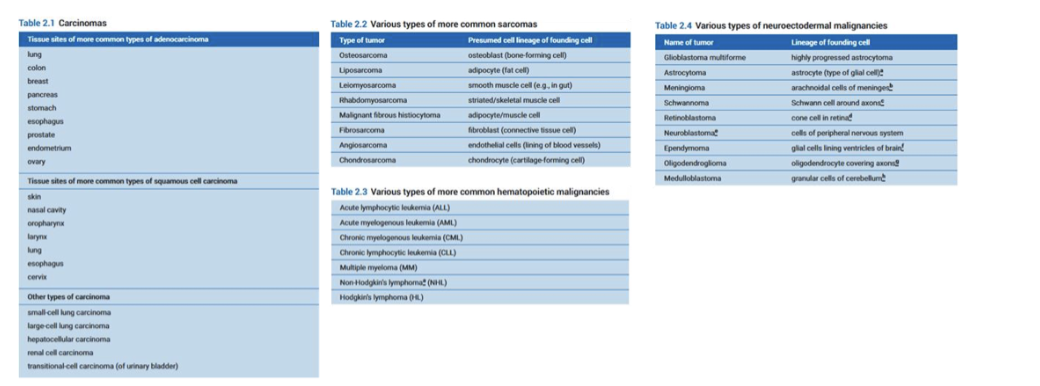
give some examples of classifications of cancers
Carcinomas- from epithelial tissues
Sarcoma- from soft tissue
Haematological- lymph blood (leukaemia and lymphoma)
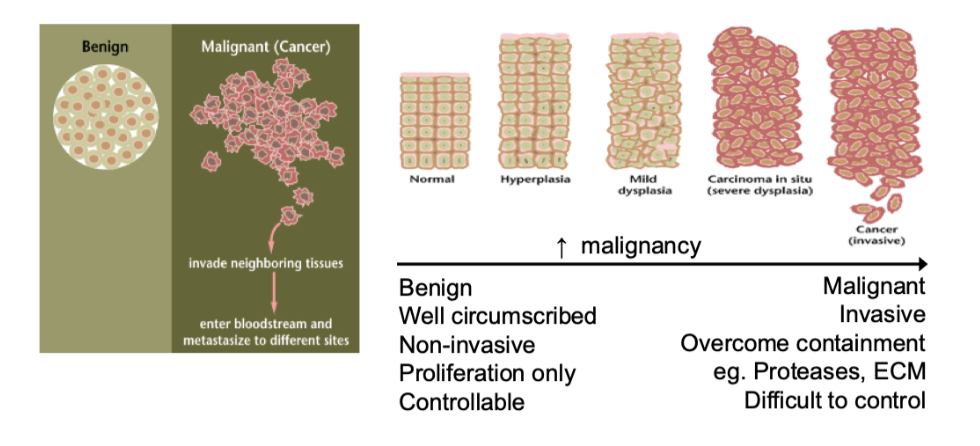
what are the different types of tumour
benign- localised, non invasive
malignant- capable of invasion and metastasis
how does a benign tumour become malignant
Spectrum of tissue states and how cancerous they are
Hyperplasia- more cells than normally would be
Mild dysplasia- more cells and start to lose their organisation, shape and size
Cancer- invasive, leave and go to other body sites
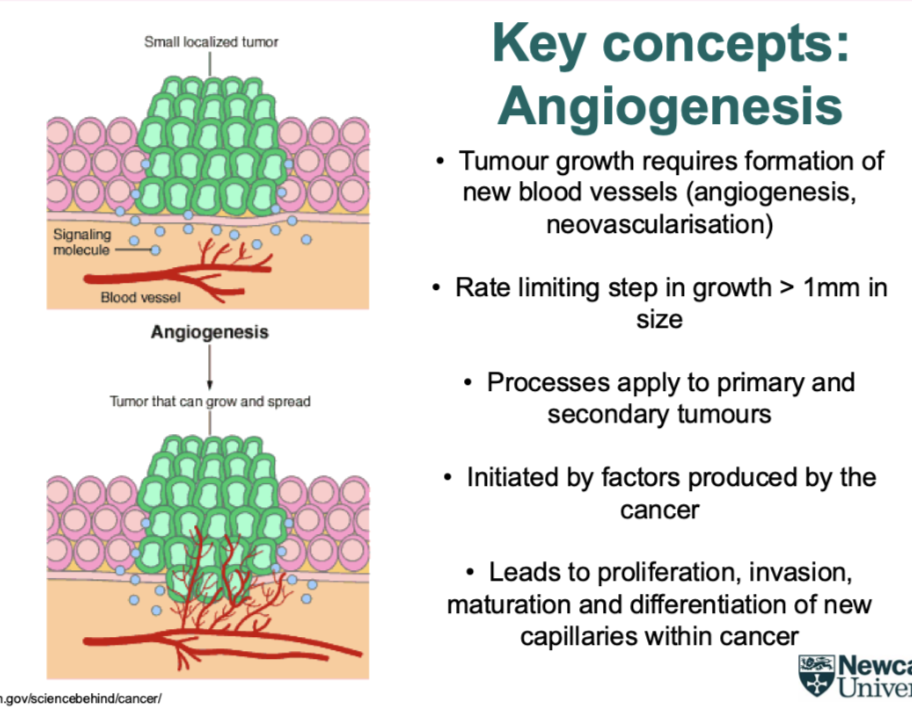
what is angiogenesis
Describes the way a cancer can recruit its own blood supply
Cancer cells reach a point they become self limiting
So form own blood supply
Secreted signalling molecules to make blood vessel to move up to the cancer
Cancer cells closer to nutrients, easier to get rid of waste products- continue to grow
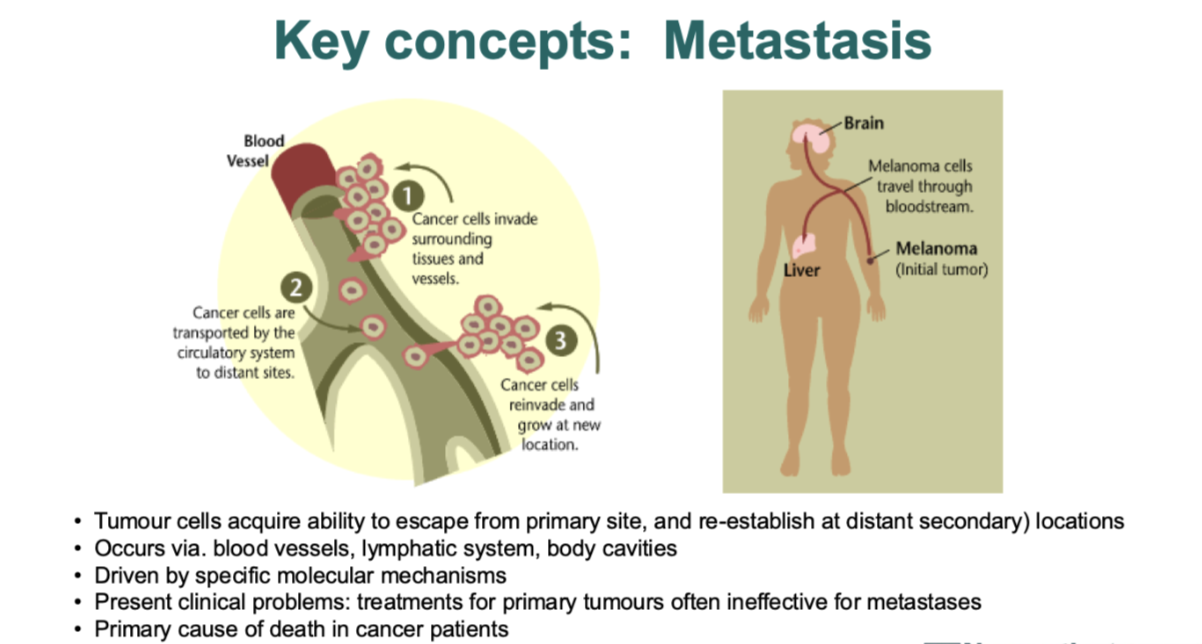
what is metastasis
tumor cells can escape from primary site and re establish ar a distant secondary location(s)
by blood vessels, lymphatic system and body cavities
primary cause of death in cancer patients
Dependent on the individual cancer where the metastasis ends up
But some commonly go to certain places e.g. initial melanoma tumour often travel to the brain
Harder to treat after metastasis
what is the mutational theory of cancer
Mutation:
A stably inherited change in the genetic material
Cancer can result from:
• Germ-line mutations- Passed down from parents to progeny
• Somatic mutations- Happen in the population as we go through life in individual cells
what is the evidence for the genetic basis of cancer
Evidence of mutations in cancer genomes- found to change the behaviour of cells
Susceptibility to some cancers inherited in families (approximately 5% of all cancers)
Mutations found in sporadic cancers and subsequently found to be transforming
Chromosomal changes are common in cancers
Some cancers associated with particular chromosomal abnormalities
Agents that damage DNA are thought to increase the susceptibility to cancer development
Some diseases are thought to arise from defects in DNA repair mechanisms that result in an elevated cancer risk
Infection with certain viruses associated with development of specific cancer
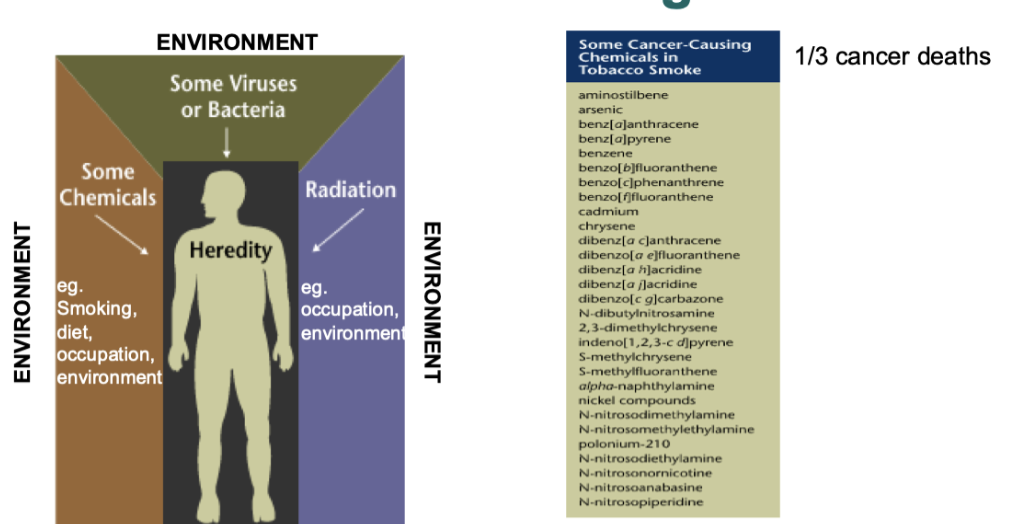
what are some cancer risk actors and carcinogens
Heredity- may be inherited predisposition to cancer
Environment we are exposed to
Chemical- smoking diet occupation
Viral
Radiation
Add up to make our cancer risk
Biggest factor is carcinogens in tobacco smoke
what are the types of mutations found in cancers
Chromosome number changes
Chromosome translocations
Amplifications
• Interstitial gains and losses (10’s – 1,000,000’s bps)
• Small deletions, insertions and single base pair mutations
• Epigenetic mechanisms – promoter hypermethylation
• Exogenous sequences
• e.g. viruses in cervical cancer (HPV), Burkitt’s lymphoma (EBV), Hepatocellular carcinomas (hepatitis virus) and Kaposi’s sarcoma (HIV virus)- viral DNA inserted into the genome
why is cancer such a rare event at the cellular level
DNA repair mechanisms
Apoptotic (cell death) mechanisms
Mutations in many genes do not affect cell growth
Most DNA does not code for protein
Rapidly dividing cells (eg intestinal epithelium and skin) are lost from the body so it does not matter if they contain mutations (unless they occur in a stem cell population)
Many cells do not divide all the time- they differentiate and lose their potential to divide (e.g. muscle cells)
No single mutation can circumvent these defences
what makes cancer a multi step disease
Multiple successive errors/cell (~6-7) are required to circumvent this protection and give rise to abnormal growth and a malignant cancer.
Chances of this are rare.
However, two general mechanisms allow this progression to happen
what is clonal evolution
accumulation and selection of multiple mutations in cancer
First mutation in one cell that makes changes to the cell causing more clones of that cell- much bigger target for second mutation to come along
The process repeats
Thought it has to happen at least 5-6 times
Some mutations can make the cell more prone to acquire more mutations- so make cells accumulate more quickly and more likely to mutate
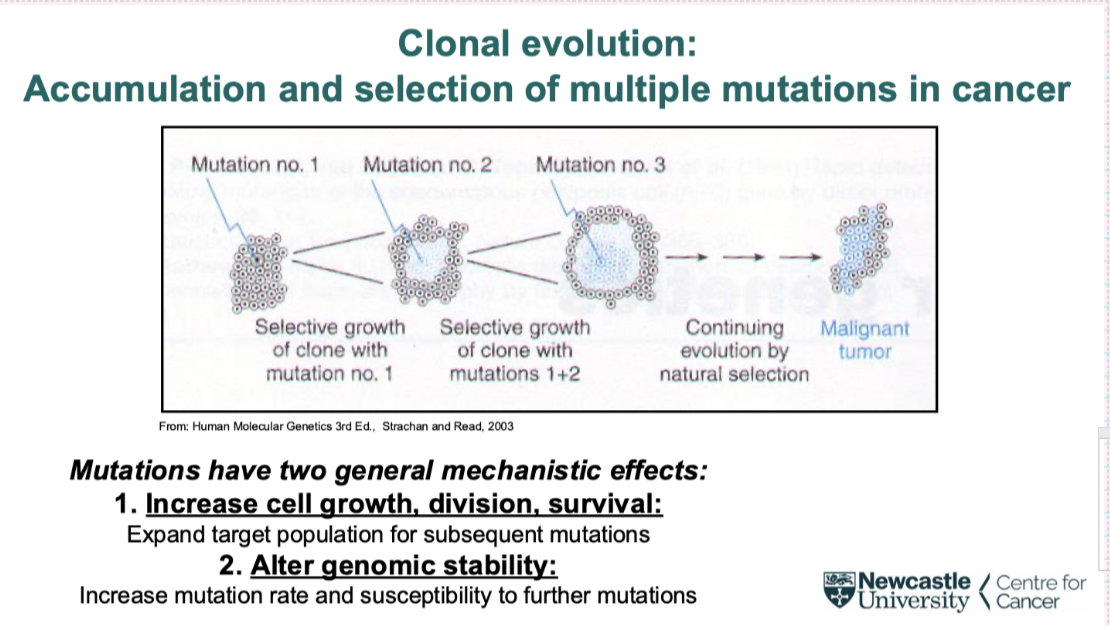
what are the 2 general mechanistic effects of mutations
1. Increase cell growth, division, survival:
Expand target population for subsequent mutations
2. Alter genomic stability:
Increase mutation rate and susceptibility to further mutations
what types of genes are targets of mutations in cancer
two general categories
oncogenes
tumor suppressor genes
what are oncogenes
normal cellular version- proto-oncogenes
Normal activity promotes proliferation, growth, invasion etc.
Gain-of-function mutations in cancer (1 allele):
Excessive or inappropriate activity
Dominant- only need mutation in one allele, transforming
can be switched on or off- constantly on in cancer cells
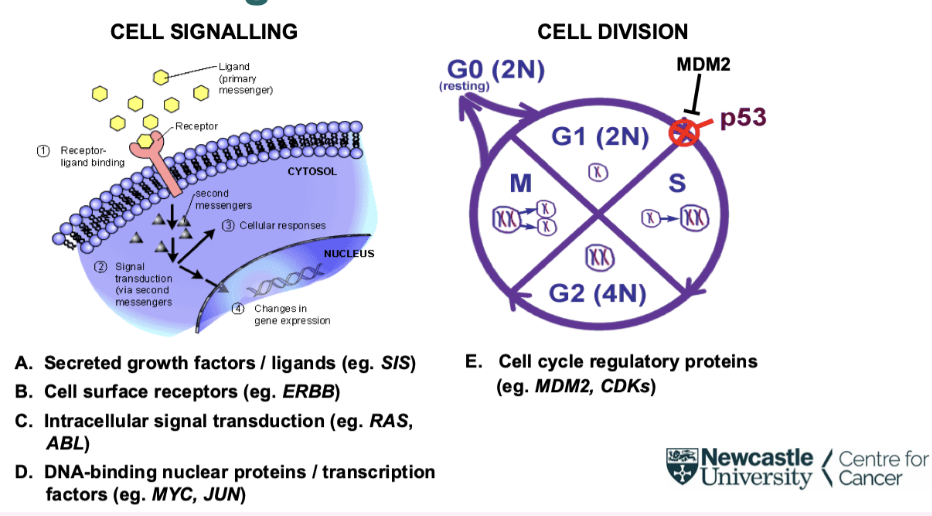
how are oncogenes responsible for growth control
See different oncogenes mutated at different parts of their signalling pathway
Some oncogenes that can drive the cell cycle directly, or feed into it
how are proto oncogenes activated
activation involves inappropriate fixed gain of function- activated in one of two ways
Quantitative – increase in production of unaltered product
Actual protein doesn’t change- just more of it there
2, Qualitative – production of modified or novel product
Mutation that changes the product- e.g. does job more efficiently
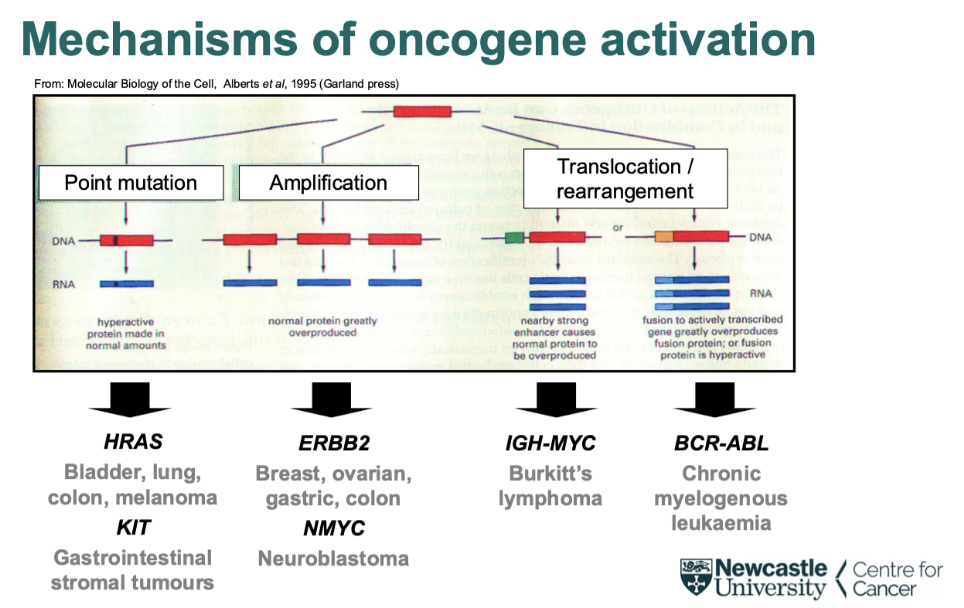
what are the 3 different mechanisms of oncogene activation
Point mutation- single aa change that typically changes activity
Amplification- more quantitative change
Translocation/rearrangement-
Genes that come together on gene fusion to make new gene product e.g. BCRA-ABL
Bring genes into different regulatory areas e.g. Burkitt's lymphoma- oncogene put into really active area of genome
what is the normal role of tumour suppressor genes
inhibit events leading to cancer
(eg. negative regulation of cell cycle, pro-apoptotic, genomic stability and repair)
Loss of function mutations (affecting 2 alleles) required for inactivation and cancer development
2 copies of gene that both play suppressor role, if lose one still have another, need to lose both copies for them to be inactive
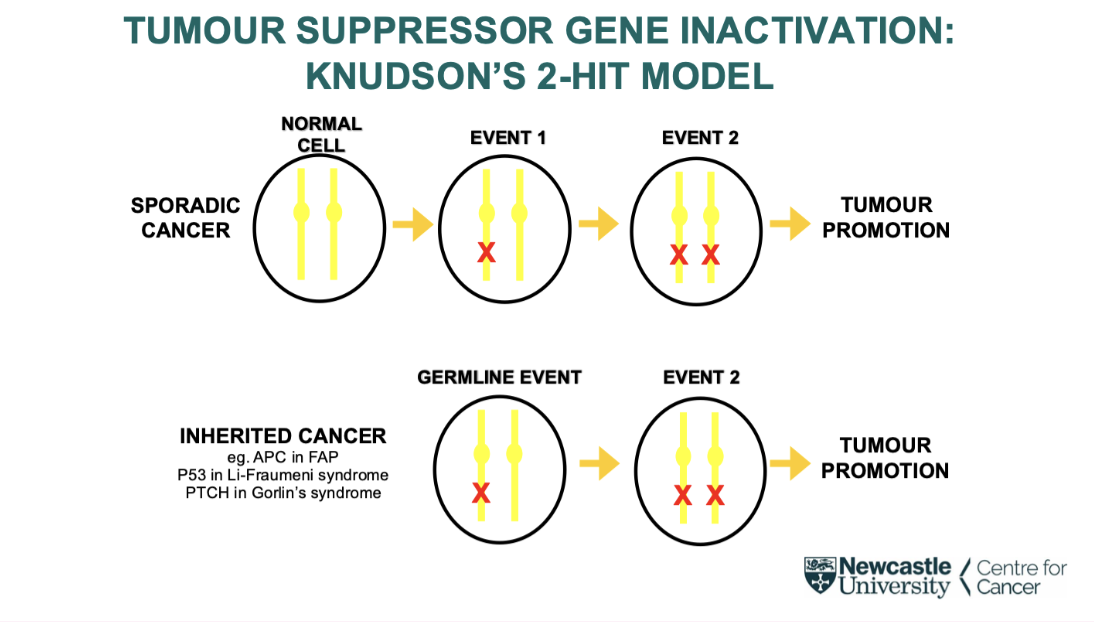
what is Knudson’s 2 hit model for tumour suppressor gene inactivation
Tumour suppressor can be one of the mutations out of the 6-7 needed, but they need two hits to knock each allele out
Sporadic cases take longer and occur much later in life as have two already instead of one
Most inherited cancer caused by inherited inactive tumour suppressor gene
Only need a second mutation
Happen earlier in life
Can Happen in multiple tissues
what types of mutation affect tumor suppressor genes
Mutations detected in TS genes are typically consistent with gene inactivation
Deletions- Single bases to entire gene or surrounding region
Truncating (insertions / deletions / nonsense (point)) eg. frameshifts, introduction of premature stop codon
Missense (point)- Point mutation usually causes a change in shape instead of affecting activity directly
Affect critical protein regions or protein structure
Can be dominant negative (eg. P53)
Compare vs. point activating mutations in oncogenes
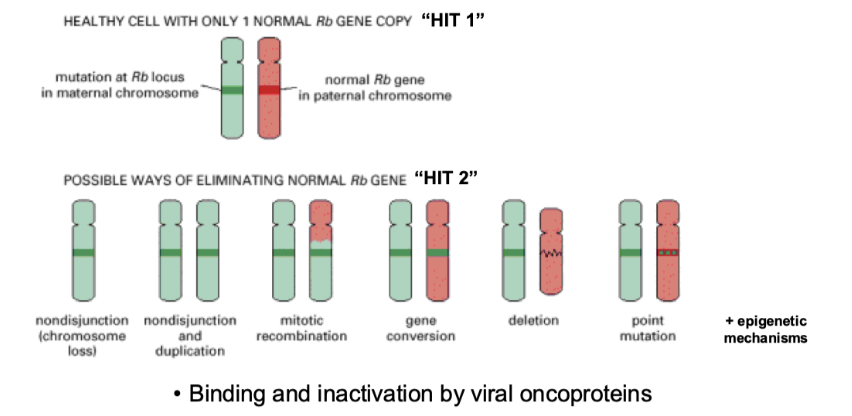
what are the possible mechanisms of tumour suppressor gene inactivation
Crossover events- causing 2 faulty copies not 1
Viruses produce viral proteins that bind to tumour suppressor genes and knock them out- not genetic
what are the 2 functions of tumour suppressors
gatekeepers
caretakers
some can act as both
how do some TS act as gatekeepers
Stop proliferation- growth related tumour suppressors
Transcriptional regulators of the cell cycle (RB1)
Cyclin dependent kinase inhibitors (eg. INK4a)
Cell adhesion regulators (E cadherin)
Angiogenesis regulators (VHL
how do some TS act as caretakers
Genes that look after state of genome and DNA stability and repair
Transcriptional regulation and DNA repair (BRCA1 and 2)
Mismatch DNA repair (MSH2, MLH1, PMS1, MSH6)
how do some TS act as both gatekeepers and caretakers
Transcriptional regulators of cell cycle arrest or apoptosis (P53)
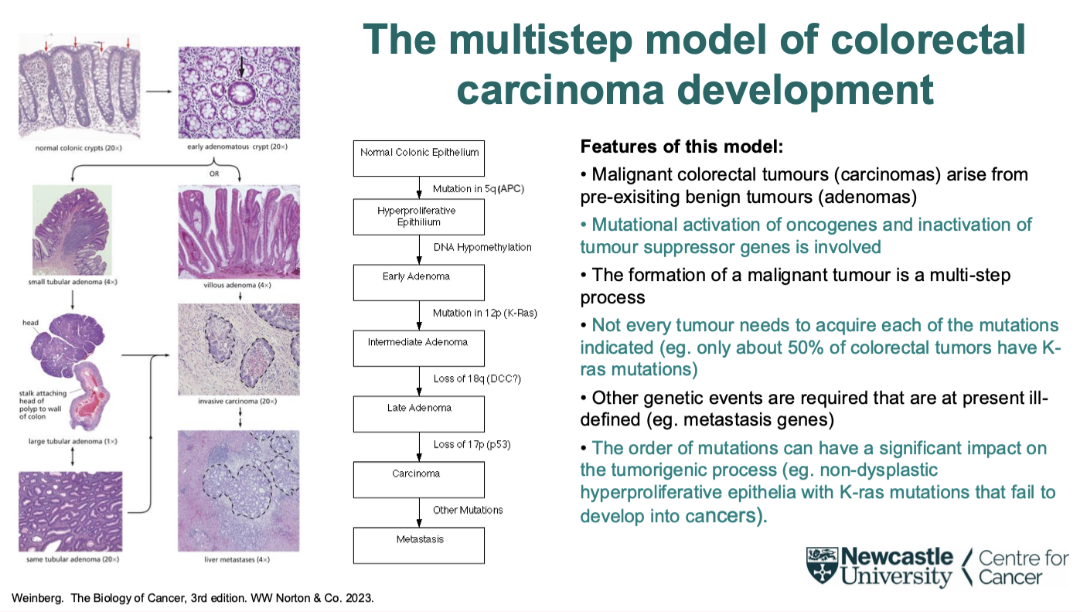
what is the multi step model of colorectal carcinoma development
Large range of stages of colorectal carcinoma
5-7 that can be readily biopsied
Each stage- different type of mutation involved
Eg TS mutation early
P53 later
Shows you do ned multiple genes to be mutation in a given cancer