EXAM #3 - LIFECYCLE NUTRITION - KENT STATE UNIVERSITY
1/68
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
69 Terms
what is considered middle childhood?
5-10 years
What is considered preadolescence/school-age?
ages 9-11 years for girls; ages 10-12 years for boys
what are the benefits of eating breakfast for a child?
improves academic performance, leads to better memory, concentration, and better overall nutrition
What are the benefits for children of having family dinner together?
increases language skills - young kids learned 1000 rare words at the dinner table compared to only 143 from parents reading storybooks aloud; better academic performance - adolescents who ate all family meals 5-7x per week were twice as likely to get A's; higher self-esteem; greater sense of resilience; physical development - utensil use; lowers risk of substance abuse, teen pregnancy, depression & suicidal thoughts, developing eating disorders, and obesity
what is the BMI-for-age for children growth charts? Overweight? Obese? Prevalence of each for 6-11 year-olds?
Overweight - 85th to 95th percentile; obese - >95th percentile; 15% of children are obese and 30% are overweight - more common in Hispanic and black children
What are consequences of restricting children's intake, especially their access to foods?
imposing controls and restrictions of "forbidden foods" may increase desire and intake of the foods causing the children to be less able to regulate their intake to meet their needs.
What are the macronutrient recommendations for children?
Energy (carbs) - needs vary based on activity level and body size; Protein - 0.95g/kg bodyweight; Fat - acceptable range = 25-35% of calorie intake including source of omega-3 and -6 fatty acids with <7% being saturated fats and limiting cholesterol and trans fats
What are dietary recommendations for children that don't include macronutrients?
consume iron-rich foods including meats, fortified cereals, dry beans, & peas; increase fresh fruits and vegetables, whole grains breads, & cereals for an increased amount of fiber; calcium intake of 1300 mg/day from dairy products and calcium-fortified foods and Vitamin D from sun exposure and fortified foods allows for healthy bone formation and growth during puberty
How does recommended child food intake compare to their actual food intake?
saturated fat is actually 11% compared to 7%; total fat intake is excessive in black and Mexican American girls as well as black boys; caffeine is increasing due to increase in soft-drink consumption; calcium intake falls short of RDA; and fast food is consumed by 33% of children each day
What are the dietary supplements recommended for children?
supplements are not needed if children eat a varied diet and get ample physical activity; if needed, do not excess tolerable UL
what are some nutrients that may require some special attention for children adhering to a vegetarian diet?
Protein, iron, B-12, Calcium, D, Omega-3s, Zinc
What is the most significant indicator of childhood obesity?
most significant predictor - parental obesity due to parents who struggle from their own BW and eating behaviors are more restrictive in their kids' food consumption, which increases cravings for forbidden foods and makes children less able to regulate their needs; other predictors include genetic factors, environmental factors, behavioral factors, early onset of BMI rebound, low Selenium status, low cognitive stimulation, etc.
average screen time for children
8-10 year olds = 6 hours; 11-13 = 8 hours; each additional hour of TV viewing increases obesity by 2%; 33% of obese children are watching TV >5 hours while only 11% watch TV <2 hrs
what is the recommended saturated fat intake for children over 2 years of age?
<7% recommended
What is the recommended number of hours of nutrition education in elementary school classrooms? What is the actual number of hours?
50 hours of education are required to facilitate behavior change while the average actual number of hours of nutritional education is 13 hours' worth of education
What is the recommended number of hours of physical activity for children per day? What is the percentage of children that hit this goal?
60 minutes of physical activity recommended per day; only 20% of children reach that level of activity with only 7.9% of middle and junior high schools require daily physical activity
what are three ways of parental obesity that increase obesity in their children?
genetics, children are given the parents genes which can often have genes linking to obesity; Environmental factors, parents that are obese are often consuming larger amounts of food and unhealthy food, they shape the child's environment often playing a major role in what their children eat; access to unhealthy foods, if children have easy access to unhealthy foods it may lead to unhealthy habits and a high level of consumption
what are some characteristics of overweight children when compared to normal weight peers?
they are often taller, have advanced bone ages, experience earlier sexual maturity, look older, and are at a higher risk for obesity related chronic diseases
Comparing quality of diets for children ages 7-9 compared to younger children
Children ages 7 to 9 have a lower diet quality than younger children. Most children do not meet recommended intakes of vegetables or meat
What are some different causes of dental caries in children?
seen in half of children aged 7 to 9; can be reduced by limiting sugary snacks and sticky carbohydrates such as raisins; choose fruits, vegetables and grains; regular meal and snack times; Rinse mouth after eating
What are some factors that influence a child's body image?
body image is tightly related to self-esteem; unrealistic media ideals of appearance lower body satisfaction and self-esteem; mother's concern for her own weight may increase her influence over her daughter's food intake and body image; young girls are preoccupied with weight and body size at an early age; imposing controls and "forbidden foods" may increase desire & intake of the foods
What percentage of females hope to be thinner? At what age?
by third grade, 40% of girls express a desire to be thinner; by adolescence, 80% want to be thinner
What is the school health index (SHI)?
The school health index helps -identify strengths and weaknesses in health promotion policies and strategies; develop an action plan; involve stakeholders (teachers, parents, students, community) in improving school policies and programs
During what period of time does peer pressure become greatest?
middle adolescence - ages 15-17; may lead to better or worse dietary intake
What hormone promotes lipogenesis during physical growth in adolescence?
estrogen stimulates lipogenesis
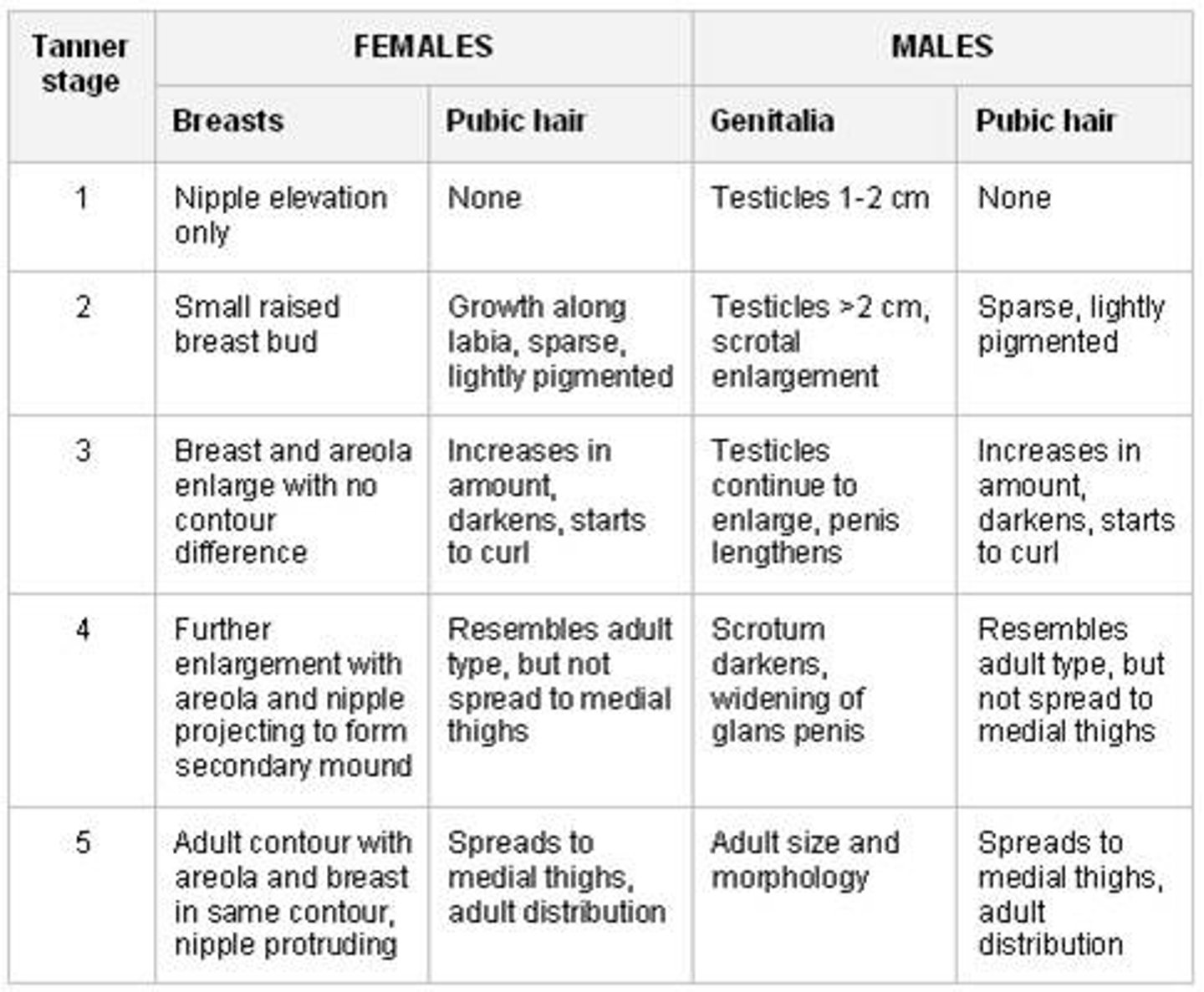
What is the Tanner Scale?
measures levels of sexual maturation in male and female development; males experience testicular/penile development and pubic hair while females experience breast development and pubic hair
At what period of life do adolescents reach peak velocity? Both males and females?
males - experience peak velocity of growth around 14.4 years of age while growth continues to until about 21 years of age; females - experience peak velocity of growth 6 to 12 months prior to menarche development which develops anywhere between the age of 8 and 17 years of age; menarche occurs 2 to 4 years after breast buds develop
What is the difference in fat mass increase between the sexes?
Females experience a 120% increase in fat mass during growth and development; 17% body fat is required for menarche and 25% body fat is needed to maintain normal menstrual cycles; men do not experience periods of purposeful fat mass increase during period of growth and development (ask Ha)
What is a factor that contributes to increased need iron? Used to prevent iron deficiency during this period.
Iron needs increase in adolescents due to a rapid rate of linear growth, an increase in blood volume, menarche (in females), and increase in strenuous activity such as sports that require ATP production, micronutrients including iron (within ETC) are used for E production
What are some factors influencing longevity in older adults?
According to CDC, longevity depends on many different factors. 10% - access to high-quality health care; 19% - genetics; 20% - environment; 51% - lifestyle factors - besides not smoking, a diet and exercise contribute most to longevity
Lifespan
maximum number of years someone might live
life expectancy
the average time a person will live, based on factors like gender and birth year
centenarian
a person who reaches 100 years of age or more
super-centenarian
a person who reaches 110 years of age or more
What is the life expectancy in the US?
78 years of age
What countries has the highest life expectancy?
Monaco (90);
What are the three theories of aging?
programmed aging, wear-and-tear theories, and free radical or oxidative stress theory
What is programmed aging theory?
Programmed aging believes that aging is a programmed, natural part of genetics
What is the wear-and-tear theories?
Wear-and-tear theories says cells and tissues have vital parts that wear out resulting in aging
What is the free radical or oxidative stress theory?
Free radical or oxidative stress theory is reactive oxygen species (ROS) damaging cells over time, factors such as smoking, ozone, UV light, and environmental pollutants all play a role in aging.
What are some benefits of calorie restriction?
A calorie restricted diet that meets micronutrient needs may prolong a healthy life; a human study found that a 15-25% kcal reduction led to a decrease in BMR by 10%, oxidative stress by 20%, BP & cholesterol, and Inflammatory factors
What are physiological changes in older adults that influence nutritional status?
Older adults experience physiological changes in organ function, which in turn cause body composition changes, GIT changes, Bone loss, decreased cardiac output, and neurological system changes, sensory ability, oral health, hunger & thirst sensations, and immune function having an increased susceptibility to infections
During what period of life does LBM decrease? How much of a decrease?
Lean body mass decreases on average 2-3% per decade in the form of sarcopenia; a decrease in muscle, minerals inc. bone, and water starting at or around the age of 50-59 with BMI peaking around this time and stabilizing before it slowly begins to drop around the age of 70; this occurs due to a decreased BMR resulting from LBM reduction
What is sarcopenia?
age-associated muscle loss
What is atrophic gastritis? Causes? Prevalence? Consequences?
Atrophic gastritis is chronic inflammation of gastric mucosa with loss of secretory cells affecting 1/3 of age 60+; main causes of Atrophic gastritis include an autoimmune disorder without a cure and H. Pylori; atrophic gastritis causes inadequate acid production increasing the risk of bacterial growth, vit. B-12 deficiency, and nutrient malabsorption; decreases absorption of folate; causes poor absorption of Vitamin B-12
What are the consequences of sarcopenia?
over time sarcopenia causes a 2-3% LBM decrease per decade; sarcopenia causes a decrease in muscle, minerals such as bone, and water; it has the biggest effect on weight status
What is the biggest physiological change in elderly that affects weight status?
Decrease in LBM/sarcopenia (ask Ha)
What age does BMI peak?
50-59 years of age
What is the name for the calories that need to be reduced to offset decreased physical activity and BMR reduction in the elderly?
"Discretionary calories"; usually requires 70-100 fewer kcal
what are discretionary calories?
calories consumed after all nutritional values have been met
What vitamin may increase all-cause mortality?
Vitamin E - can increase hemorrhage risk and all-cause mortality; single supplement of vitamin E causes all-cause mortality
What are some of the nutrients that are often low in older adults' diets?
Complex CHO/fiber which aid with constipation, diverticulosis -> diverticulitis, and cholesterol & blood sugar control; Vitamin D, E, & folate; dairy, fruits, vegetables
What are the causes of vitamin B-12 deficiency in older adults?
B-12 deficiency is often caused by the body's inability to use it efficiently; Atrophic gastritis can cause poor absorption of vitamin B-12; macrocytic anemia - alongside a folate deficiency causes damage to the myelin sheath leading to neurological deficits
What are some nutritional risk factors for the elderly?
Elderly individuals are at increased risk of both malnutrition (undernutrition) and obesity; decreased mobility leading the individual to be dependent on others shopping for groceries and preparing their meals; polypharmacy causing someone to not want to eat or drink anything; diseases that decrease appetite, absorption, and increase requirements; oral health problems such as the loss of teeth and having a poor dentition; mental problems/dementia; use of alcohol; others includes decrease in income, social isolation, loss of loved ones, lack of social interaction, and depression
What is the hydration status of elderly individuals?
Water intake is low in older people, with 20-30% being at a high risk of dehydration; recommended intake sitting at 8 glasses per day or abt. 2 liters
Why dehydration can be dangerous?
Dehydration can lead to kidney stones, blood clotting, rapid, weak pulse, low BP, or passing out/death
What are some tips for elderly individuals to stay hydrated?
Some tips include being cautious with chocking (ask Ha), experimenting with temp, trying something more savory like hot soup broth, and having popsicles, smoothies, milkshakes, ensure, sports drinks, etc.
What are some dietary supplements that may be recommended to the elderly?
Calcium, vitamin D, multivitamins, Vit. B-12, Folate, Magnesium, creatine, etc.
What is the recommendation for physical activities to maintain/increase muscle mass?
Recommendations to maintain/increase muscle mass include muscle strengthening that involves all major muscle groups on two or more days per week; at least 150 minutes per week of moderate intensity aerobic activity; drinking water when exercising; and ensuring adequate intake of protein for muscle building
Determine
Disease
dEtermine
eating poorly
deTermine
Tooth loss/mouth pain
detErmine
Economic hardship
deteRmine
Reduced social contact
deterMine
Multiple medicines
determIne
involuntary weight loss/gain
determiNe
Needs assistance in self-care
determinE
Elder years above age 80
DETERMINE
Disease
Eating poorly
Tooth loss/mouth pain
Economic hardship
Reduced social contact
Multiple medicines
Involuntary weight loss/gain
Needs assistance in self-care
Elder years above age 80