Neuropathology IV: Infections and Demyelinating Diseases
1/134
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
135 Terms
-bacteria
-virus
-fungus
-parasite
-prion
What are the 5 main types of CNS infections, considering the cause?
-hematogenous
-direct implantation
-local extension
-transport along peripheral nerves
What are the 4 main routes of entry to the CNS?
-arterial blood supply (most common)
-retrograde venous spread from anastomoses between veins of face and venous sinuses of skull
What are 2 examples of the hematogenous route of infection to the CNS?
-traumatic -> open penetrating trauma
-iatrogenic -> lumbar puncture (rare)
What are 2 examples of the direct implantation route of infection to the CNS?
-sinusitis (mastoid/frontal)
-infected tooth
-osteomyelitis in spine or cranium
What are 3 examples of the local extension route of infection to the CNS?
*rabies
*herpes-simplex
What are 2 examples of infection being transported along peripheral nerves to the CNS?
meningitis
What is the most common CNS infection?
-acute pyogenic meningitis (bacterial)
-acute aseptic meningitis (viral)
-chronic meningitis (mycobacteria, fungus, spirochetes)
-chemical meningitis
-carcinomatous
What are the 5 main types of meningitis?
based on age range of affected individuals
How do the pathogens differ in acute pyogenic meningitis infections?
neonates
Which group, neonates, children, or the elderly, has the most unique set of acute pyogenic meningitis-causing bacteria?
-group B streptococcus
-E. coli
-Listeria monocytogenes
SEL
What are the 3 bacterial species responsible for causing acute pyogenic meningitis in neonates?
-Neisseria meningitidis (associated with Waterhouse-Friedrichsen Syndrome)
-Streptococcus pneumoniae
-Haemophilus influenzae (virtually eliminated due to vaccination)
NIP - neisseria, influenza, pneumonia
What are the 3 bacterial species responsible for causing acute pyogenic meningitis in children?
-Streptococcus pneumoniae
-Neisseria meningitidis
-E. coli
-Staph aureus
NESP
What are the 4 bacterial species responsible for causing acute pyogenic meningitis in the elderly?
-patients with shunt infection
-patients with neurosurgery
-patients with skull fracture
What are 3 medical conditions that can lead to bacterial meningitis in patients?
-S. epidermidis
-S. aureus
What are the 2 bacteria associated with bacterial meningitis in patients with shunt infection?
-S. epidermidis
-S. aureus
What are the 2 bacteria associated with bacterial meningitis in patients with neurosurgery?
-S. pneumonia
-H. influenzae
What are the 2 bacteria associated with bacterial meningitis in patients with skull fracture?
Neisseria meningitidis (associated with Waterhouse-Friedrichsen Syndrome) in children
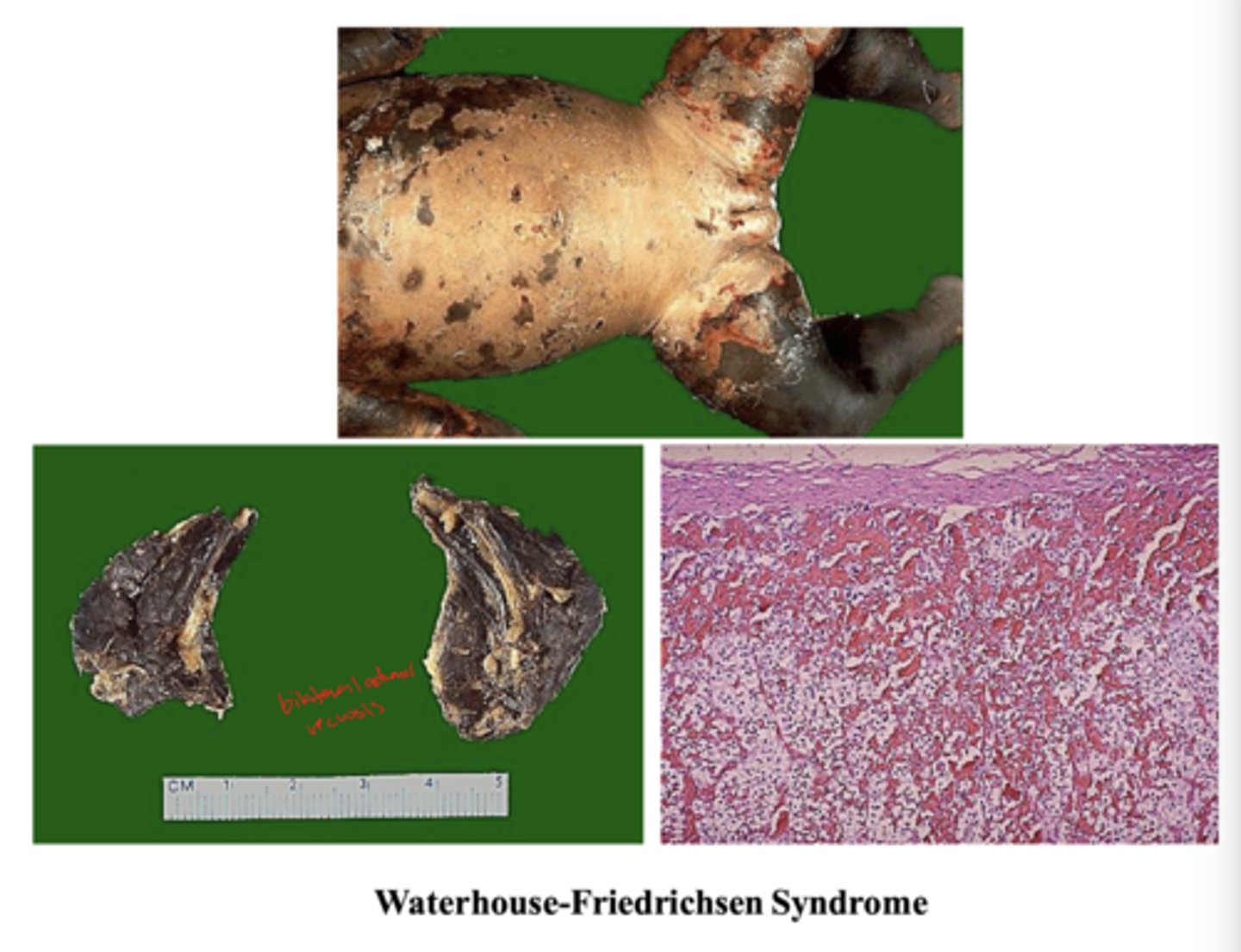
-headache
-nuchal rigidity
-clouding consciousness
-fever (can be absent in up to 50% of cases)
-irritability
What are the 5 main clinical features of acute pyogenic meningitis?
-pleocytosis, more cells -> especially neutrophils
-high protein
-low glucose
-bacteria on smear or culture
What are the 4 main CSF features from lumbar puncture in acute pyogenic meningitis?
remember -> neutrophils form pus
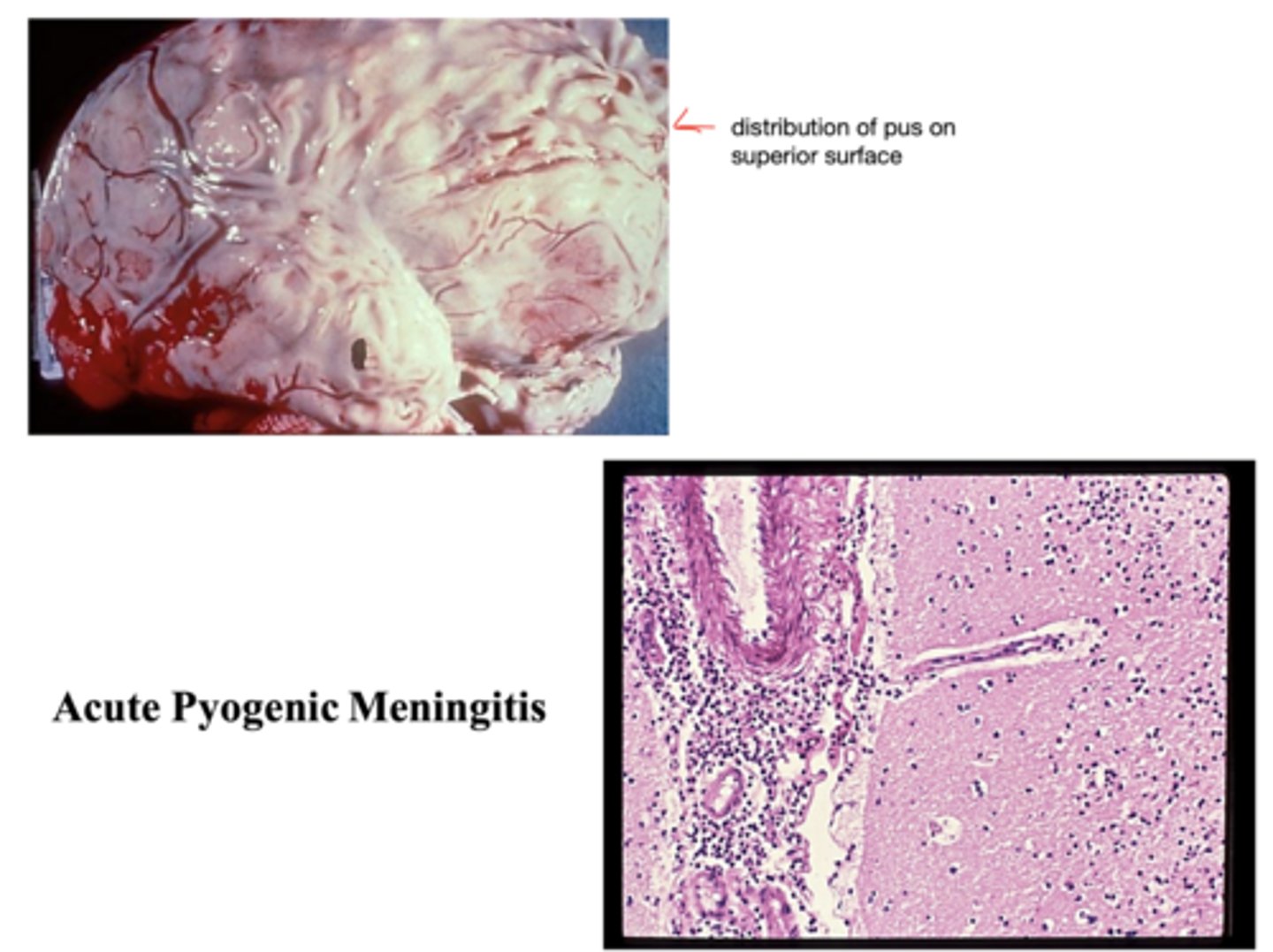
-common
-uncommon
What are the 2 types of acute viral meningitis?
*enterovirus
*HSV-2
*West Nile Virus (WNV)
What 3 viruses are involved in common acute viral meningitis?
*HSV1
*Epstein-Barr virus (EBV)
*varicella zoster virus (VZV)
*HIV
*HHV-6
What 5 viruses are involved in uncommon acute viral meningitis?
similar to bacteria, but usually less severe/sudden onset:
-headache
-nuchal rigidity
-clouding consciousness
-fever (can be absent in up to 50% of cases)
-irritability
What are the 5 main clinical features of acute viral meningitis?
-pleocytosis, more cells -> especially lymphocytes
-slightly elevated protein
-normal glucose
-viral culture/PCR positive
What are the 4 main CSF features from lumbar puncture in acute viral meningitis?
-M tuberculosis
-Cryptococcus
-Histoplasma
-Coccidioides immitis
-syphilis
What 5 infections cause chronic meningitis?
greyish, gelatinous, viscous exudate covers the base of the brain
What happens in tuberculosis meningitis, a form of CNS tuberculosis?
-elevated protein
-low glucose
What are the 2 main features of the CSF in tuberculosis meningitis?
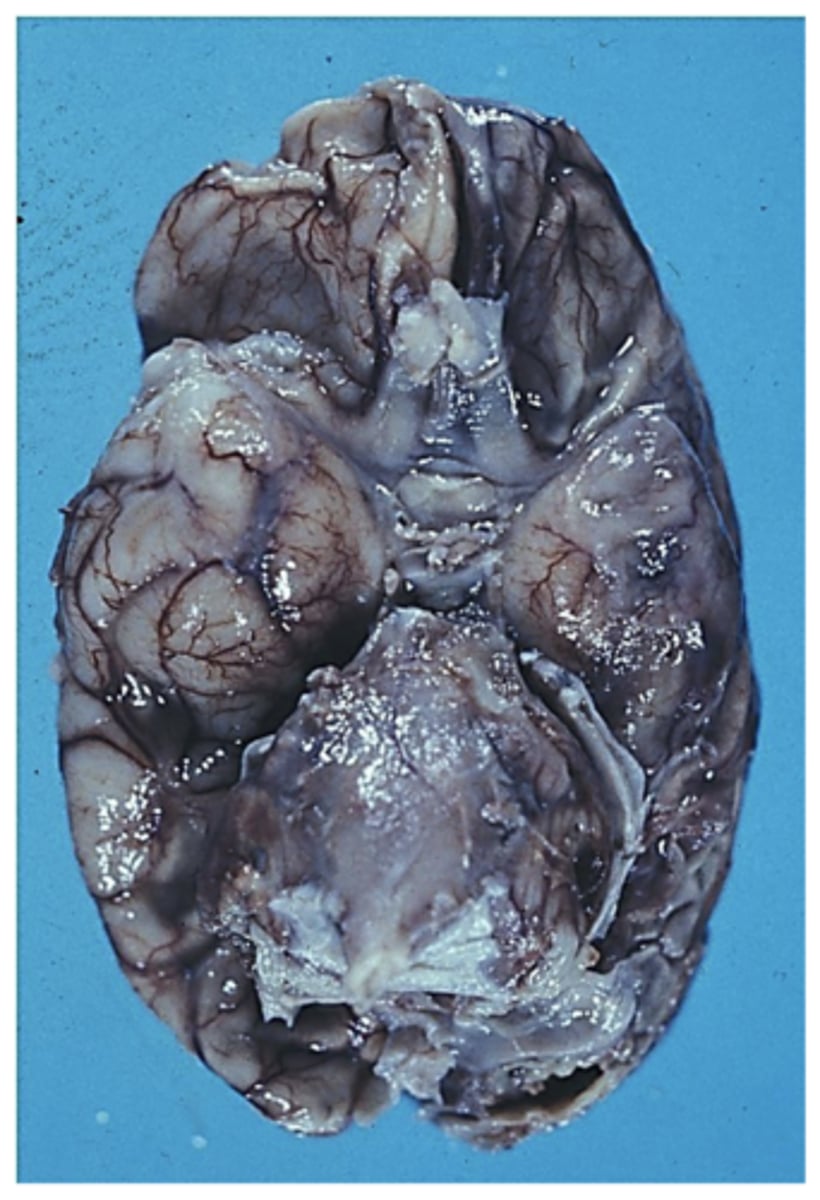
it is the most common form of fungal meningitis
What is the significance of Cryptococcus meningitis?
pigeon droppings (C. neoformans)
What is the source of Cryptococcus meningitis?
-AIDS
-immunocompromised
What are the 2 main populations at risk of Cryptococcus meningitis?
"soap bubble" cysts in parenchyma
What is the physical manifestation of Cryptococcus meningitis like?
budding yeast seen with India ink and mucicarmine
What is the histologic presentation of Cryptococcus meningitis like?
Cryptococcus meningitis:
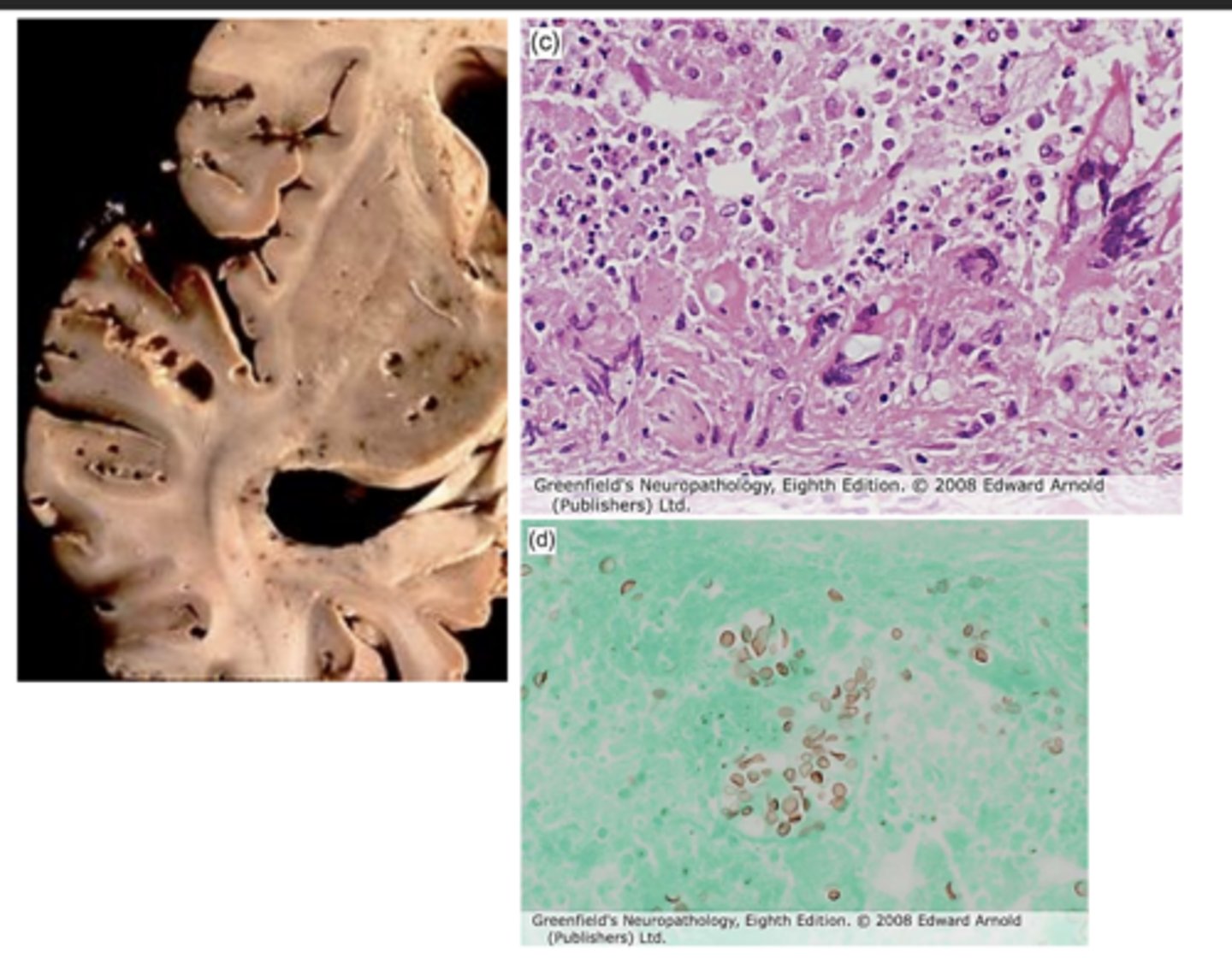
bacterial infections
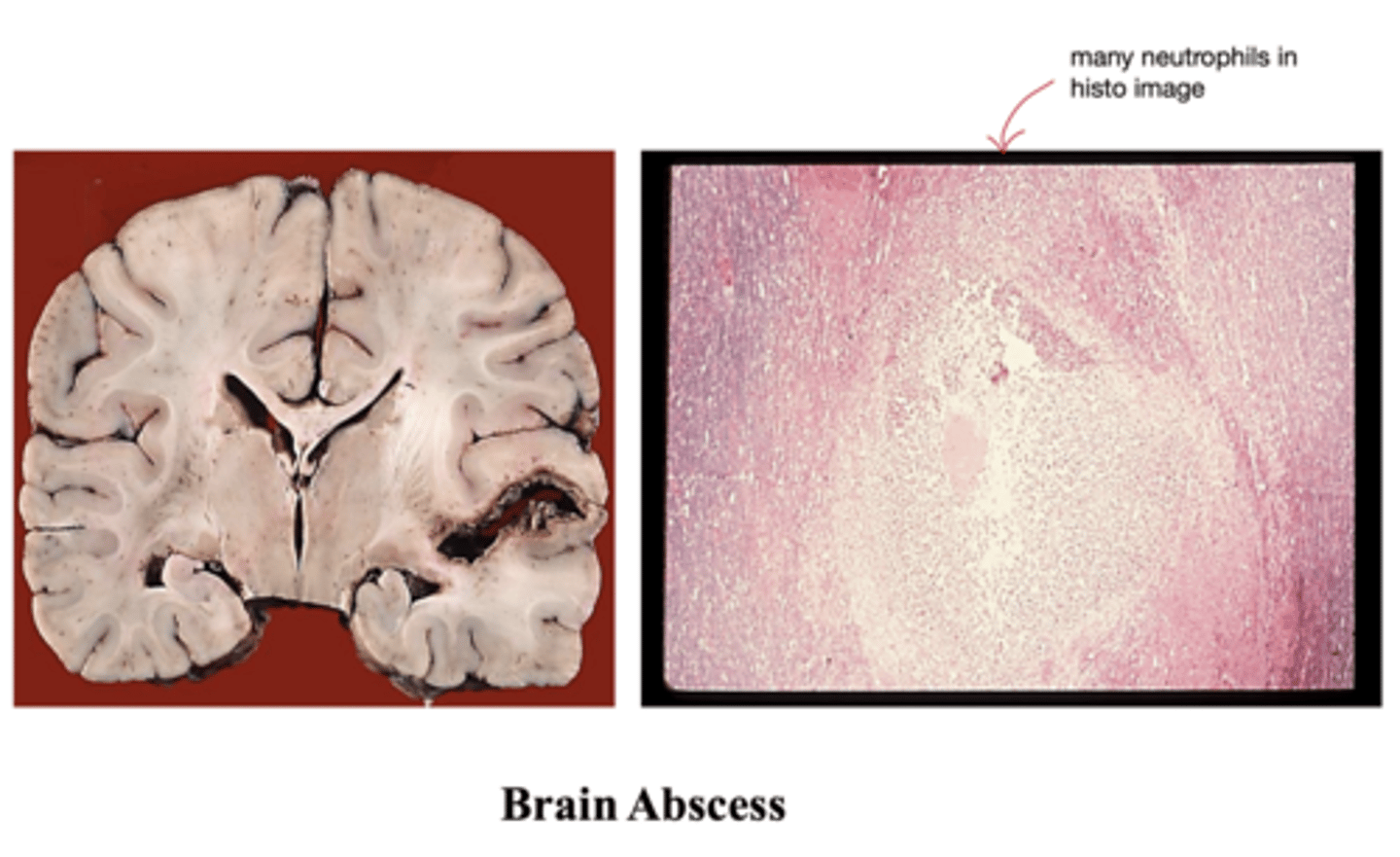
What are brain abscesses most often caused by?
-direct implantation of organisms
-local extension from adjacent foci -> ex: mastoiditis
-hematogenous
-predisposing factors
What are the 4 methods of bacterial infections reaching the brain to cause a brain abscess?
-acute bacterial endocarditis (septic emboli)
-chronic pulmonary infections (bronchiectasis)
What are 2 main predisposing factors to brain abscess from bacterial infection?
brain tumor; ring-enhancing lesions
What may a brain abscess mimic, and explain?
discrete destructive lesions with central necrosis surrounded by rim of granulation/fibrous tissue
What is a brain abscess lesion like?
progressive focal deficits and general signs related to increased ICP
What are the main behavioral symptoms associated with a brain abscess?
direct culture of drained abscess, rather than CSF
What is the method of assessing the composition of a brain abscess?
high mortality rate
What is mortality like for a brain abscess?
surgery + antibiotics ASAP!
What is the treatment of a brain abscess like?
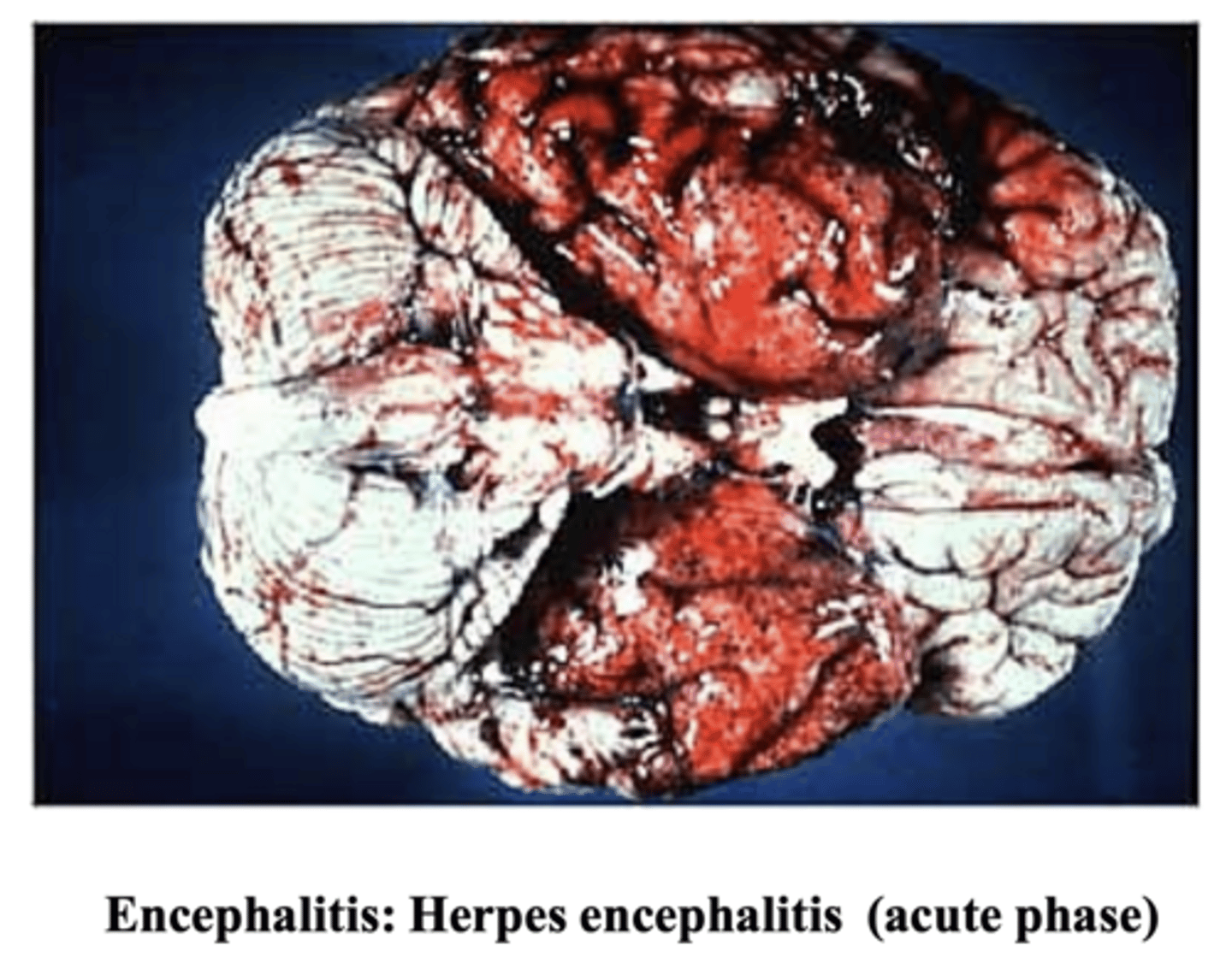
-arbovirus (WNV)
-enterovirus
-herpes simplex
-EBV
-cytomegalovirus (CMV)
-mumps
-JC
What are the 7 viruses that can cause encephalitis?
*HSV-1
*HSV-2
With what 2 viruses is the pathological change from encephalitis that occurs in the temporal lobe more commonly seen?
-WNV
-rabies
With what 2 viruses is the pathological change from encephalitis that occurs in the brainstem more commonly seen?
-polio
-WNV
With what 2 viruses is the pathological change from encephalitis that occurs in the spinal cord more commonly seen?
-edema
-congestion
-hemorrhage
-herniation (in severe cases)
-> not very unique/specific
What are the 4 main gross manifestations of encephalitis?
-microglial nodules
-neuronophagia
-perivascular lymphocytic infiltrate
-viral inclusions
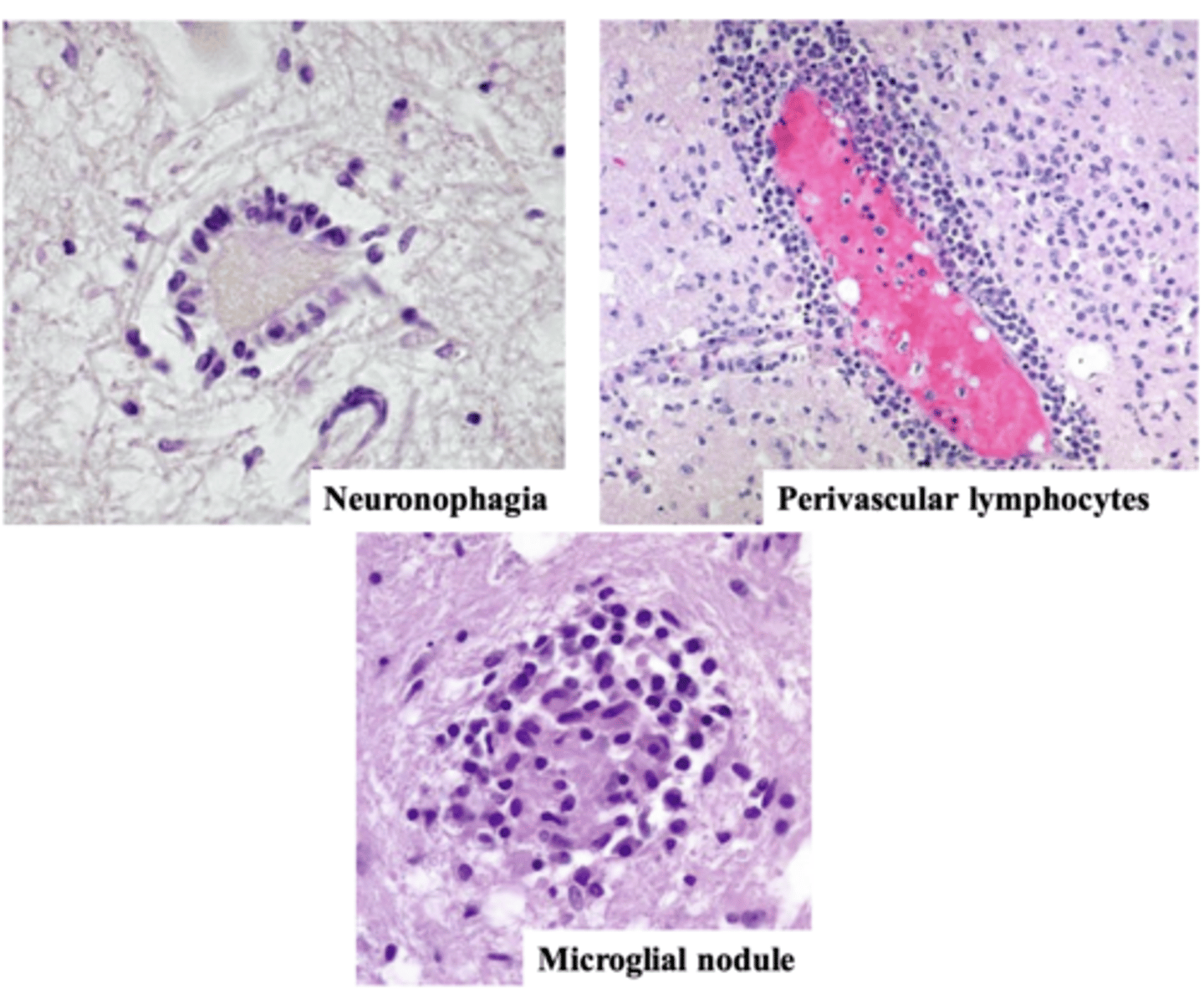
What are the 4 main characteristics of encephalitis in microscopic analysis?
microscopic presentation of encephalitis (not specific for any type of virus -> with any of them)
-protazoa
*toxoplasma
*amebiasis (Naeglaria)
*acanthamoeba
*malaria
-metazoa
*cysticercosis
*echinococcus
-Rickettsia
*typhus
*rocky mountain spotted fever
What are the 3 main types of parasitic infection, and examples of each?
immunocompromised patients -> consumption of undercooked meat and contamination with cat feces
In what individuals does toxoplasmosis occur, and how?
AIDS
What condition is toxoplasmosis an indicator disease of?
-cysts (Bradyzoites)
-free forms (Tachyzoites)
-> at the border with viable tissue
What 2 forms does Toxoplasma gondii bacteria exist in, and explain?
immunohistochemistry
How can toxoplasmosis infection be confirmed?
underlying HIV infection
What do most patients with CNS toxoplasmosis disease have?
typical cerebral mass lesion with ring-enhancing lesion and surrounding edema
What does a CT scan in CNS toxoplasmosis show?
periventricular pattern of infection
What is a less common presentation of CNS toxoplasmosis on MRI scan?
a) CT scan of typical cerebral mass lesion with ring-enhancing lesion and surrounding edema
b) MRI scan showing less common periventricular pattern of infection -> histopathology showed necrosis to a depth of 1 cm, with abundant ziotes
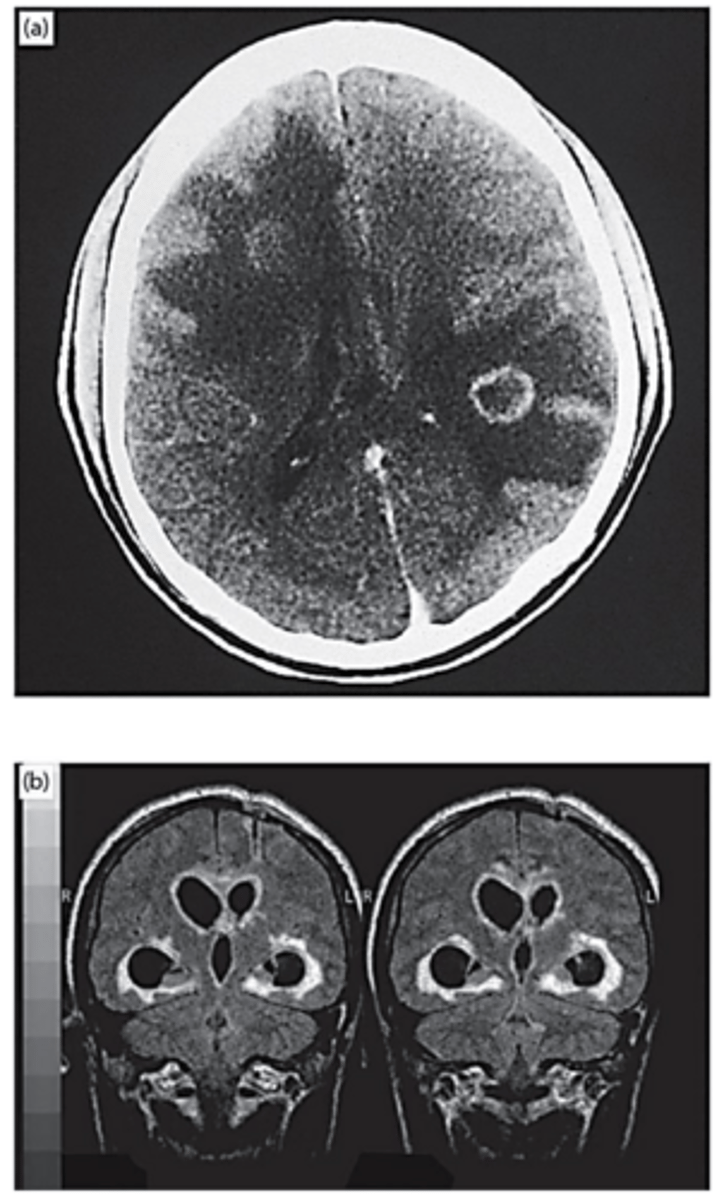
CNS toxoplasmosis -> Toxoplasma gondii
just for reference -> he said not to focus on this

CNS demyelinating disorder
What type of condition is progressive multifocal leukoencephalopathy (PML)?
reactivation of latent JCV infection
What is the cause of progressive multifocal leukoencephalopathy (PML)?
immunocompromised patients (~80% cases of AIDS)
In what population does progressive multifocal leukoencephalopathy (PML) occur?
Natalizumab treatment
What treatment can lead to progressive multifocal leukoencephalopathy (PML)?
polyomavirus -> BKV & SV40 (and JCV)
What 2 infections, besides JCV, can contribute to progressive multifocal leukoencephalopathy (PML)?
-sensory deficits
-hemianopsia
-cognitive dysfunction
-aphasia
-gait disturbance
-seizures (less common)
What are the 6 main clinical presentations of progressive multifocal leukoencephalopathy (PML)?
-multifocal white matter lesions predominantly in subcortical cerebral white matter and cerebellar peduncles
-gray matter lesions in basal ganglia, thalamus
What 2 main features does imaging reveal in progressive multifocal leukoencephalopathy (PML)?
small ovoid, yellow-tan foci of discoloration maximal near cortical gray-white matter junction
What are the macroscopic features of progressive multifocal leukoencephalopathy (PML)?
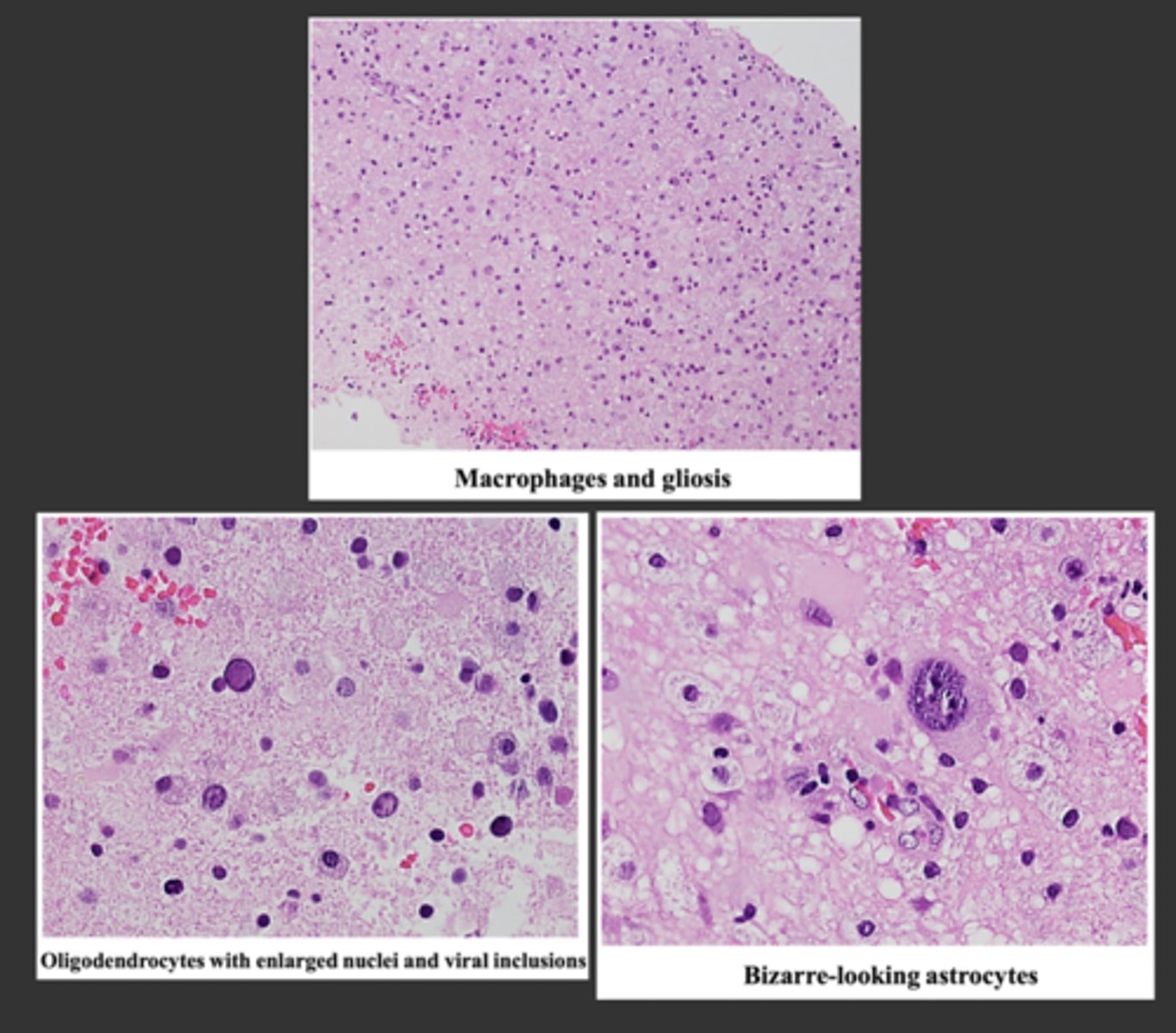
-demyelination, oligodendrocyte loss, nuclear oligodendrocyte inclusions
-virally infected cells often Ki-67(+), p53(+)
-cytological bizarre enlarged astrocytes
What are the 3 main microscopic features of progressive multifocal leukoencephalopathy (PML)?
microscopic features of progressive multifocal leukoencephalopathy (PML):
detection of JC virus DNA by PCR in CSF
What is the main method of diagnosing progressive multifocal leukoencephalopathy (PML)?
HIGH!
*72-90% sensitivity
*~100% specific
What is the sensitivity and specificity in the detection of JC virus DNA by PCR in CSF to diagnose progressive multifocal leukoencephalopathy (PML)?
-immunohistochemistry (SV-40)
-EM (not often)
-in situ hybridization
What are 3 alternative methods of diagnosing progressive multifocal leukoencephalopathy (PML)?
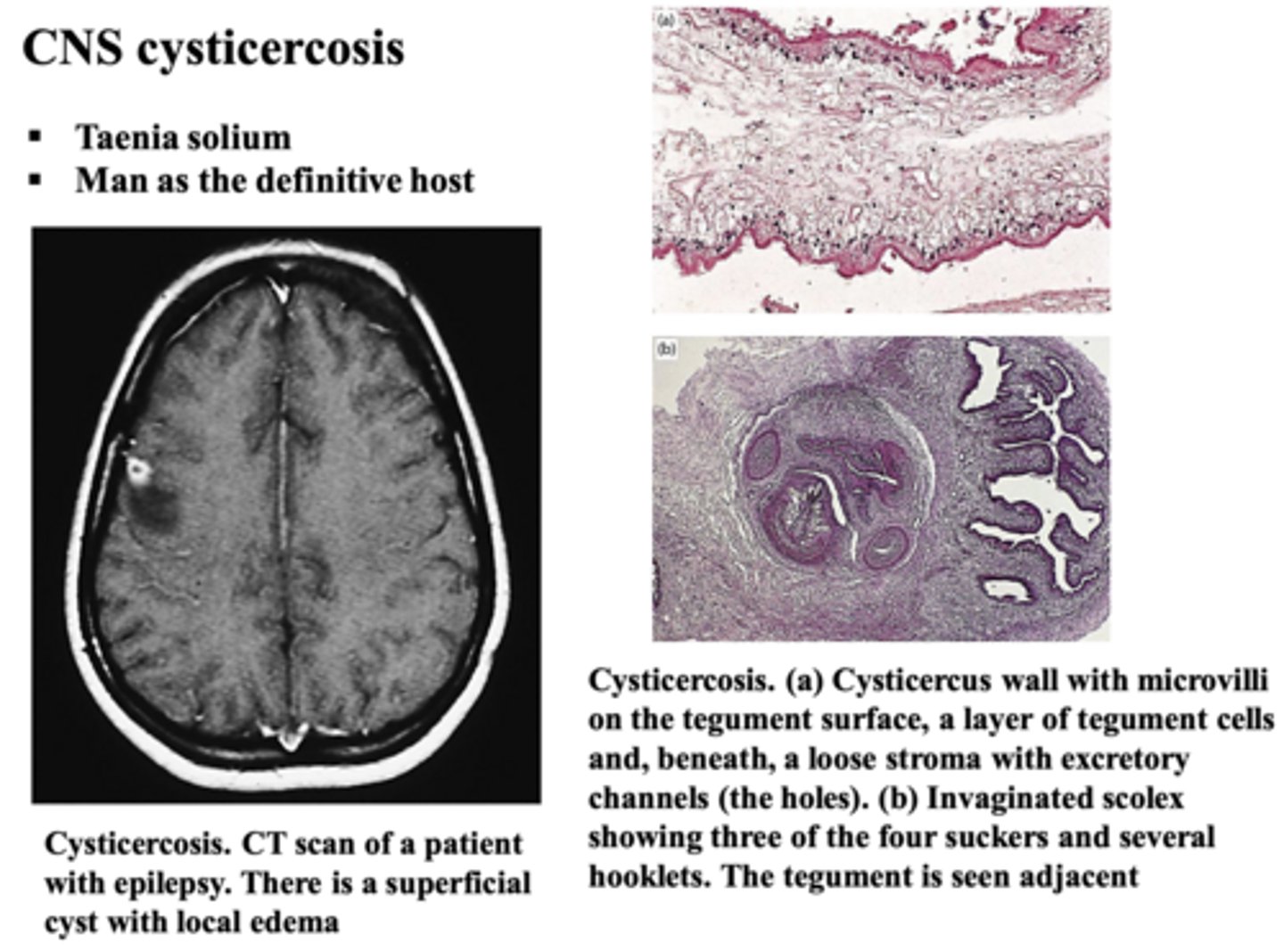
Taenia solium, pig tapeworm -> consider travel history bc can indicate tapeworm infection
What is the cause of Cysticercosis?
single or multiple cysts form in the parenchyma or ventricles or subarachnoid space
What happens to the brain in Cysticercosis?
minimal inflammation
What is the condition of Cysticercosis like when the parasite is alive?
inflammatory response and calcification occurs after parasite death
What is the condition of Cysticercosis like when the parasite is dead?
humans only
What is the definitive host of Taenia solium?
insulation of axons that improves speed and efficiency of conduction
What is myelin?
-CNS, brain
-PNS, nerves
What are the 2 locations where demyelinating diseases occur?
oligodendrocytes
What is responsible for myelination in the CNS?
50 axons
How many axons does 1 oligodendrocyte myelinate?
Schwann cells
What is responsible for myelination in the PNS?
1 axon
How many axons does 1 Schwann cell myelinate?
a broad range of pediatric and adult neurological diseases
What is demyelination a major feature of?
multiple etiologies
What is the etiology of demyelinating diseases?
diverse clinical presentations and syndromes
What clinical presentations and syndromes is demyelination associated with?
-clinical history
-neurological examination
-CSF
-neuroimaging
-neurophysiological studies
Based on what 5 things is demyelination diagnosed?
destruction of normal myelin with relative preservation of axons
What is demyelination characterized by?
*Multiple sclerosis
*Neuromyelitis optica
*Acute disseminated encephalomyelitis (ADEM)
*Acute necrotizing hemorrhagic encephalomyelitis (ANHEM)
*Progressive multifocal leukoencephalopathy (PML)
*Central pontine myelinolysis (CPM)
*Guillain-Barré Syndrome
What are 7 examples of demyelinating diseases?
multiple sclerosis (MS)
What is the most common autoimmune demyelinating disorder?
20-50 -> before puberty or after 60 years is rare
What is the age of onset of MS like, and explain?
polysymptoms (numerous, varied symptoms rather than a single defining one):
*motor
*cognitive
*sensory
What are the symptoms of MS like, and explain?
white matter lesions separated in time and space
What is the hallmark criteria for MS diagnosis?
M:F = 1:2
What is the prevalance of MS in males vs females?
initiated by helper T cell acting against myelin antigens
What is the mechanism of MS development?
periventricular or subcortical lesions
What lesions does imaging of MS reveal?