Lecture 7 Surgical Management
1/66
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
67 Terms
Cleft lip / palate involves more than just the _______
lip and palate
Cleft lip surgery is done mainly for _______
aesthetics
Cleft palate surgery is done mainly for __________
maintaining function
What is the cleft lip repair surgery?
cheilorraphy
When is clef lip repair surgery done?
at least 10 weeks of age
What are the goals of cleft lip repair?
aligning the structures
achieving symmetry
achieving a white roll
minimizing the appearance of scars
What are the two unilateral cleft lip repair techniques?
Millard Technique: Rotation advancement
Tennison-Randall Technique: Z-plasty
Where is the incision for the Millard Technique?
right below the nostrils
Where is the incision for the Tennison-Randall technique?
in the lips
What are the bilateral cleft lip repair techniques?
Broadbent-Manchester
Millard
What are the potential complications of a cleft lip repair?
stenosis of the nasal vestibule
difficulty in nasal breathing and sleep
What is the cleft palate repair surgery?
palatoplasty
What is the timing of cleft palate repair?
9-12 months but may be delayed
What are the goals of cleft palate repair?
separating oral and nasal cavities
normal VP mechanism
minimizing the occurrence of fistulas
optimizing facial growth
How is the palate closed?
in three layers
nasal, mucosa, bones
What does surgical restoration of soft tissue help to?
approximate the maxillary bony segments
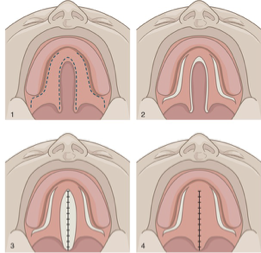
What is this cleft palate repair technique?
Von Langenbeck procedure
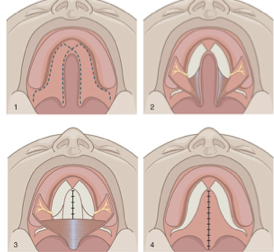
What is this cleft palate repair technique?
Wardill-Kilner
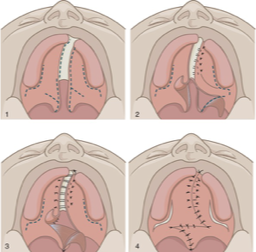
What is this cleft palate repair technique?
Furlow Z-palatoplasty
What are the potential complications of cleft palate repair?
airway compromise
excessive bleeding
velopharyngeal insufficiency
risk for postoperative dehiscence
What is the general agreement on the technique that has the best speech results?
early repair is better for speech results
better results are obtained by experienced surgeons
What is the surgery for VPI?
pharyngoplasty
What is the timing for VPI surgery?
usually after 3 years of age
What are the goals for VPI surgery?
“normalizing” VP closure for speech
avoiding airway compromise
Who are poor candidates for VPI surgery?
significant airway obstruction
neurological condition, particularly if progressive
significant cognitive disability
severe hearing loss or deafness
previous oropharyngeal radiation
a bleeding disorder
a medialized carotid artery in the area of the flap incision
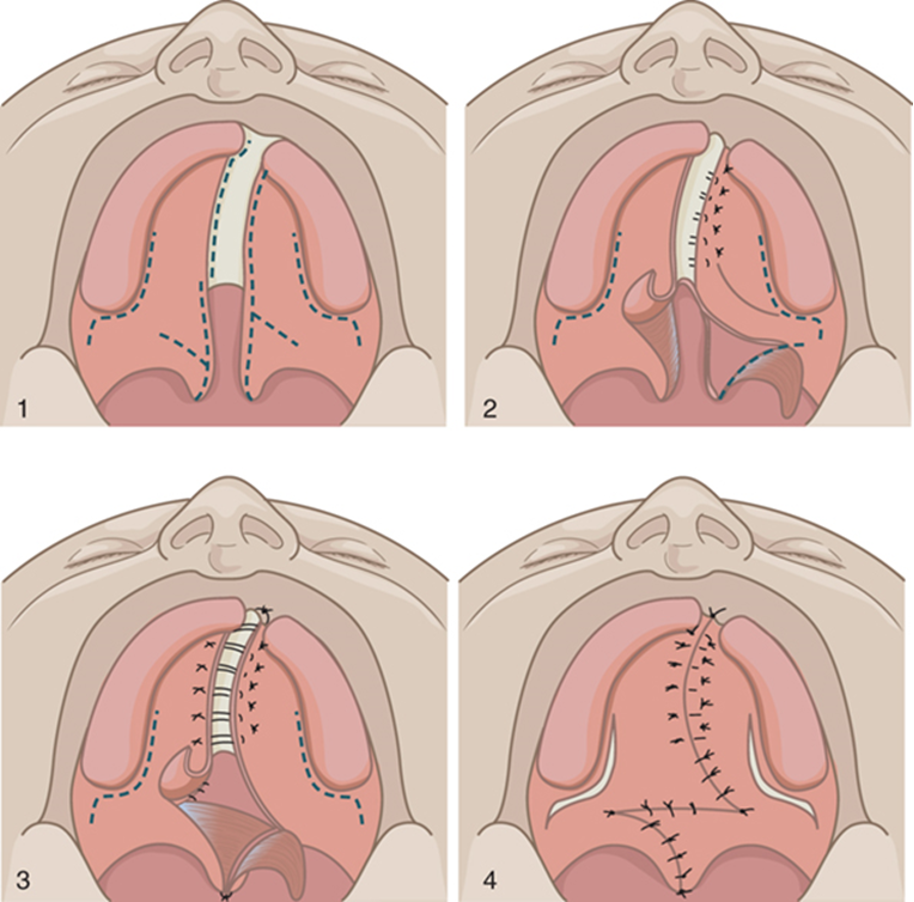
What VPI surgery is this?
Furlow Z-Plasty
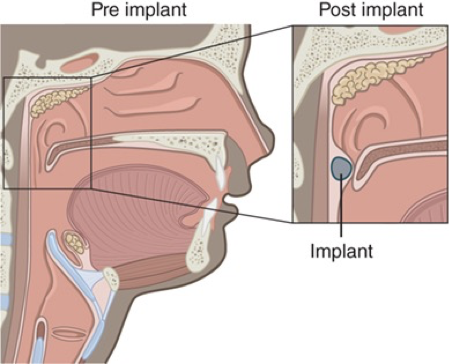
What VPI surgery is this?
Pharyngeal wall augmentation
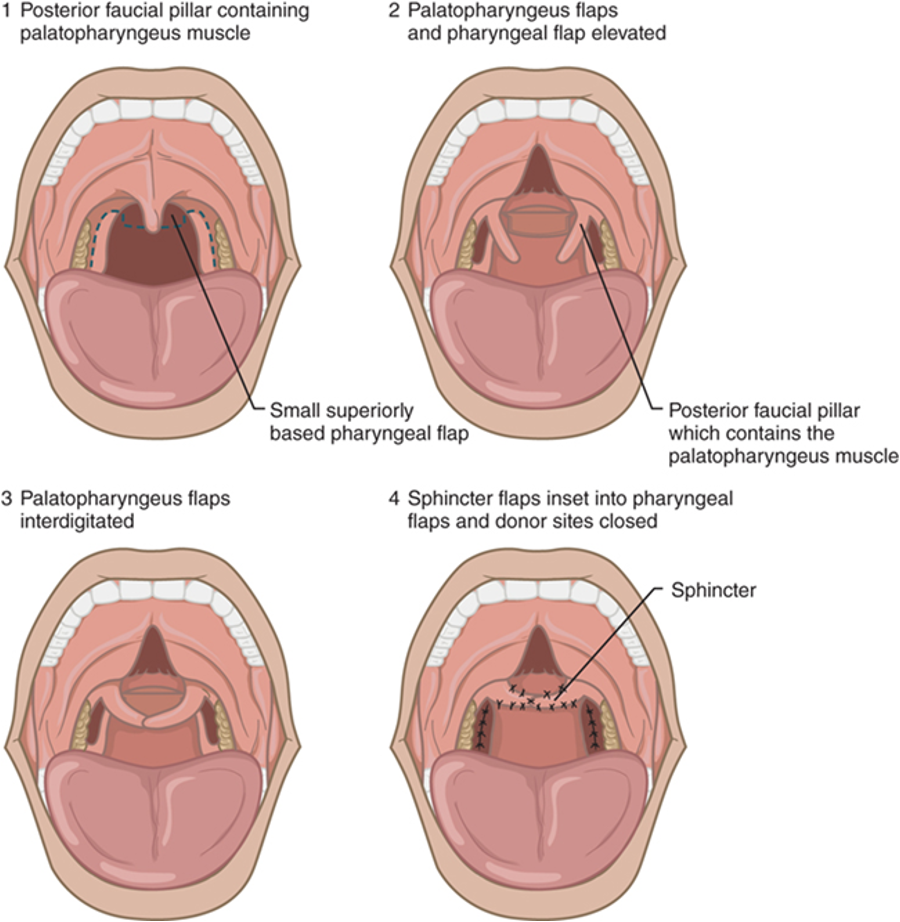
What VPI surgery is this?
Sphincter Pharyngoplasty
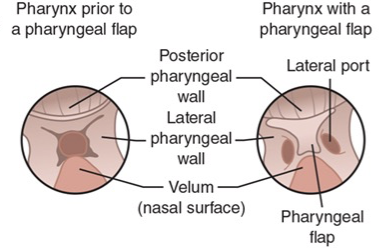
What VPI surgery is this?
Pharyngeal flap
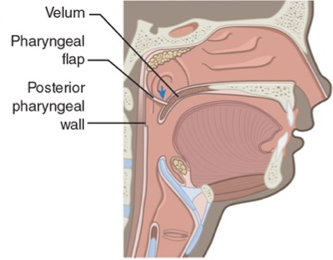
What VPI surgery is this?
Pharyngeal Flap
What are the potential complications of Furlow z-plasty?
prone to oralnasal fistula development
What are the potential complications of pharyngeal augmentation?
may cause infections
may cause extrusion, reabsorption, or migration of the material
What are the potential complications of sphincter or flap?
may dehisce (pull apart)
may result in over-correction or under-correction
Where is the best placement for a flap/sphincter?
high in the nasopharynx in the area of maximum LPW and velar movement
What happens if the flap or sphincter can be seen during an intraoral evaluation?
it is probably too low for speech
it is more likely to cause sleep apnea because it is at the level of the tongue base
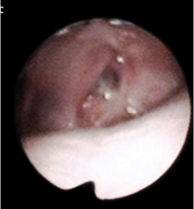
Why is this VPI surgery unsuccessful?
port is too narrow
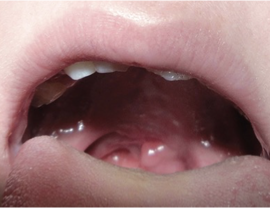
Why is this VPI surgery unsuccessful?
pharyngeal flap is too low
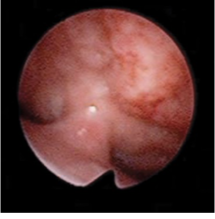
Why is this VPI surgery unsuccessful?
pharyngeal flap is too narrow
What are the measures of success?
normal resonance and no nasal emission
adequate nasal airway and no hyponasality
normal nasometry scores for an objective measure
What is the timing of alveolar bone grafting?
6-11 years
What are the goals of alveolar bone grafting?
to provide bony support for permanent lateral incisor and canine
to improve the dental arch
What are the potential complications of alveolar bone grafting?
bleeding and infection
inadequate bone graft take
breakdown of repair
persistence of the fistula
What are the oronasal fistula repair techniques?
use of local palatal tissue
use of flaps of tissue from turbinates, buccal surface or tongue
often done with the alveolar bone graft (age 6-7)
can be done earlier if it is symptomatic
temporary palatal obturator can be used until the fistula is surgically repaired
What are the potential complications of oronasal fistula repair?
tissue break down
there’s about a 40% recurrence risk with a repair, which gets higher with subsequent repairs
What is the name of the maxillary advancement surgery?
orthognathic surgery
What does orthognathic surgery address?
malocclusion that often occur due to clefts and micrognathia
What is the timing of maxillary advancement surgery?
14-16 years in girls and 16-18 years in boys
What are the goals of maxillary advancement?
to bring the maxilla into proper alignment with the mandible
improves aesthetics and obligatory speech distortions
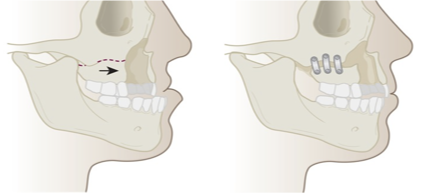
What is this maxillary advancement technique?
Le Fort Technique
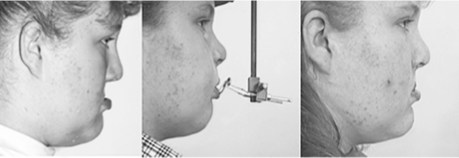
What is this maxillary advancement technique?
distraction technique
What effect does maxillary advancement have on speech sound production?
normalization of occlusion and eliminating obligatory distortions
What effect does maxillary advancement have on upper airway and hyponasality?
when the maxilla is advanced it increases the nasopharynx eliminating airway obstruction
What effect does maxillary advancement have on velopharyngeal function?
advancement of maxilla and advances velum and makes it hard to reach PPW causing hypernasality
What are the potential complications of maxillary advancement?
major blood loss, requiring massive transfusion
infection of facial soft tissues
decreased sensation in the upper lip and midface
loss of teeth or gingiva
relapse of the maxilla and therefore, persistent malocclusion
velopharyngeal insufficiency
Helpful Chart

What is a prosthetic device?
typically used when surgery is not an option or not desired
usually fabricated by a pediatric dentist or a prosthodontist
can be used permanently or temporarily while waiting for surgery
What are the goals of a prothetic device?
to improve both aesthetics and function
What does a fixed bridge replace?
dental segments
What do dentures replace?
all teeth in the arch
What do overlay dentures do?
fit over existing teeth and provide more vertical dimension
What are the goals of feeding obturators?
improving compression of the nipple
reduce nasal regurgitation of liquids
What are the disadvantages of feeding obturators?
dose not obturate the soft palate for suction
extra expense
needs to be redone with growth
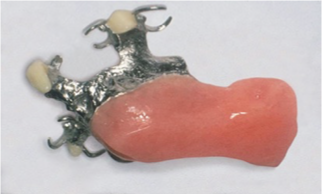
What speech appliance is this?
palatal obturator
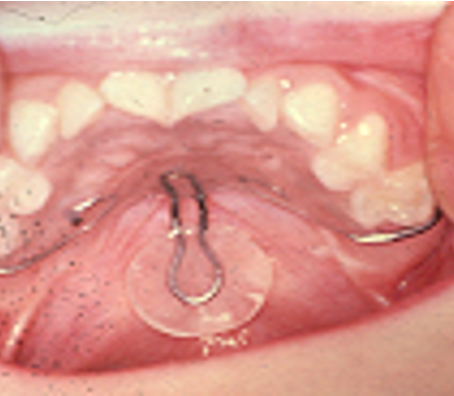
What speech appliance is this?
palatal lift
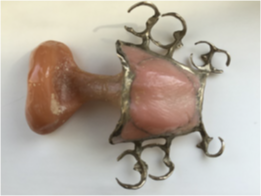
What speech appliance is this?
speech bulb obturator
What are the advantages of prosthetic devices?
used when surgery cannot be done or is being delayed
used for VP incompetence due to neuromotor disorders where surgery is more risky
What are the disadvantages of prosthetic devices?
require frequent adjustments in children
are expensive
can be lost or damaged
need daily cleaning
need manual skill for insertion and removal
may be uncomfortable
do not result in a permanent correction