Digestive system
1/19
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
20 Terms
Enteric motor system
“Second brain”
Governs GI tract from esophagus to anus
Sensory and motor neurons within submucosal and myenteric plexuses
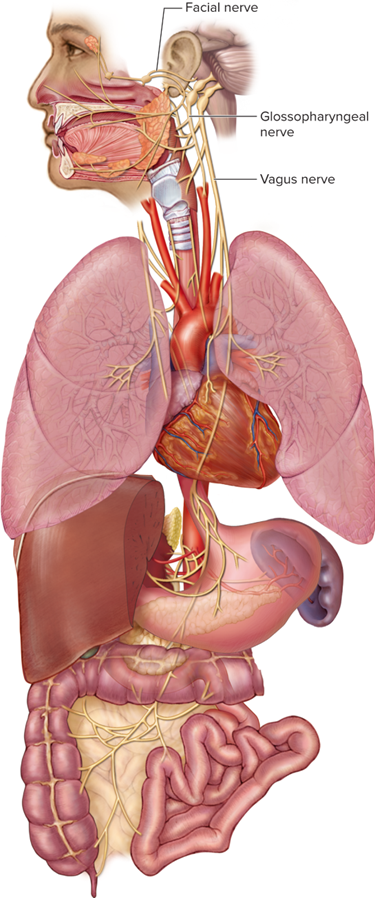
Short reflex
Local reflex
Only involves ENS
Coordinates small segments of the GI tract
Long Reflex
Involves sensory input to CNS and autonomic output
Coordinates GI tract motility
Secretes
And controls accessory digestive organs
Phases of swallowing
Voluntary phase - Tongue pushing food/bolus toward pharynx
Pharyngeal phase - Uvula closes nasopharynx; epiglottis closes larynx
Esophageal phase - Bolus moves through esophagus
Gastric pit and glands
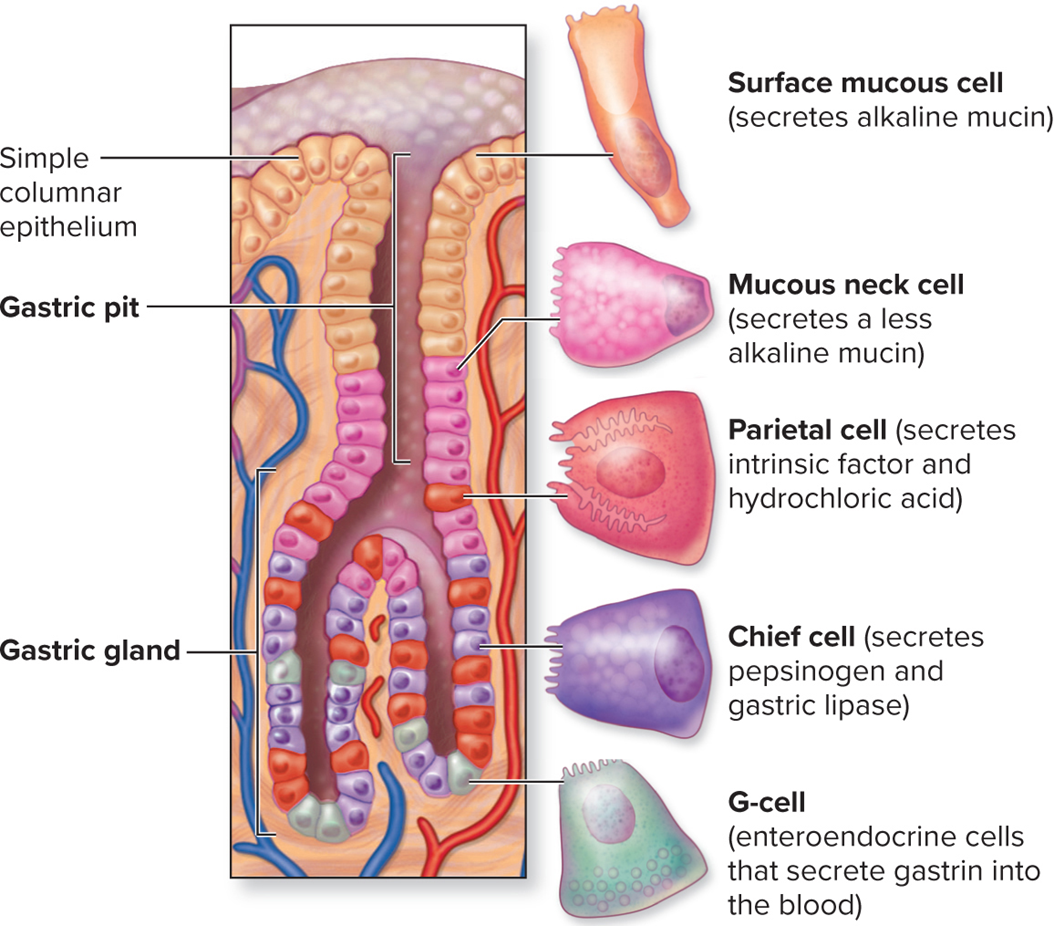
Parietal cells - HCl and intrinsic factor
Chief cells - Pepsinogen to break down protein
G-Cell - Gastrin
Surface mucous cell - Alkaline mucin
Mucous neck cell - Less alkaline mucin
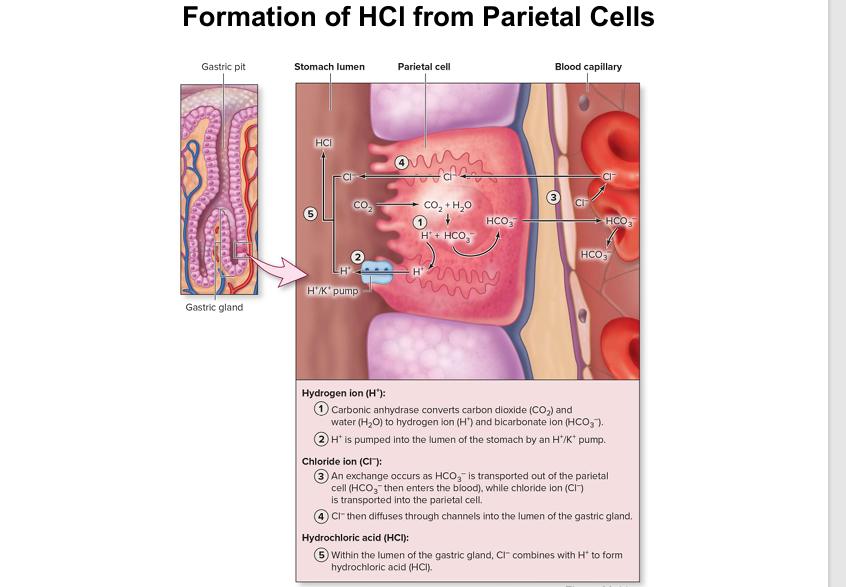
Parietal cell creation diagram
Quick notes: HCO₃- goes out of cell and Cl- gets pulled into the cell
Gastrin
Enteroendocrine cells
Secreted by the G-cells
Stimulates secretions and motility (more contraction)
Regulation of digestive processes in the stomach
Regulation is stimulated by Reflexes
Cephalic
Gastric
Intestinal
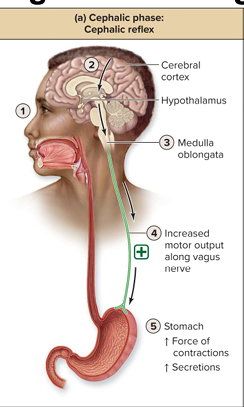
Cephalic reflex
Cerebral cortex sends sensory signals to medulla oblongata
Activation: Sensory receptors
Motor output: Vagus nerve to stomach
Effect: Stimulated to increase force of contraction and release of secretions
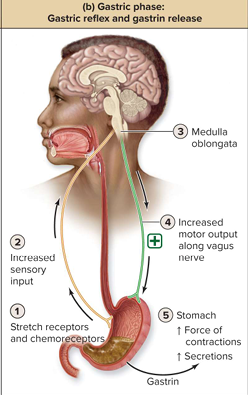
Gastric Reflex
Initiated by presence of food
Activation: Stretch receptors in stomach; Chemoreceptors detecting protein or high pH in stomach contents
Motor output: Increases motor output of vagus nerve
Effect: Increases force of contraction and release of secretions
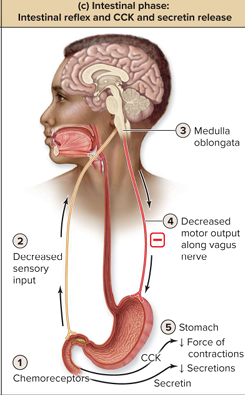
Intestinal reflex
Initiated by acidic chyme in duodenum
Activation: Chemoreceptors detecting low pH
Motor Output: Is decreased
Effect: Decreases force of contraction and release of secretions
Bile
Secreted by liver; contains no digestive enzymes
Water, bicarbonate ions, bile salts, pigments, cholesterol, lecithin, mucin
Neutralizes acidic chyme and eliminates bilirubin
Common bile duct
Merge between cystic duct of gallbladder and common hepatic duct
Enters duodenum through major duodenal papilla
Glucagon
Released by alpha cells of pancreas
Effect: Increase glycogenolysis, and gluconeogenesis; decrease glycogenesis
Defecation
Rectum contents stimulate stretch receptors in rectal wall
Sensory input to spinal cord
Motor output along parasympathetic neurons
Smooth muscle of sigmoid colon contract; internal anal sphincter relaxes
Conscious decision to defecate is controlled by cerebral cortex; external anal sphincter relaxes
Fecal transplant
Low cost and low risk
Fecal matter is placed in colon of patient via enema or colonoscopy
Treats: Crohn disease, ulcerative colitis, irritable bowel syndrome
Carbohydrate digestion
Initiated first by salivary amylase via salivary glands
Does not occur in stomach
Resumes in small intestine
Salivary amylase in stomach
Inactivated in stomach due to low pH
Protein digestion in small intestine
Enzyme release: Trypsinogen, chymotrysinogen, and procarboxypeptidase via pancreas
Enteropeptidase activates enzymes
Enzymes breakdown partial proteins into amino acids
Brush border enzymes dipeptidase and aminopeptidase completely breakdown the proteins into amino acids