W14. Medical Imaging of the Chest
1/230
Earn XP
Description and Tags
continue at 163
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
231 Terms
What do the ABCs of radiograph assessment stand for?
Alignment
Bone density
Cartilage spaces
Soft tissues
What can radiographs show about soft tissues?
Gross form such as muscle mass but not fine soft tissue detail
Why can soft tissues still be somewhat differentiated on radiographs?
There is enough variation in shades of gray to distinguish skin fat and muscle
What kinds of changes do radiographs usually show?
Significant changes
What is Computed Tomography (CT)?
An x-ray technology that creates very high-resolution thin slices of axial anatomy
How can CT images be displayed?
In different planes or reconstructions
What is the difference between a radiograph and a tomograph?
A radiograph sees the whole body region (BOOK)
A tomograph shows individual slices (INDIVIDUAL PAGES)
Ex in photo: fx deep in the tibial plateau is easier seen on a CT scan
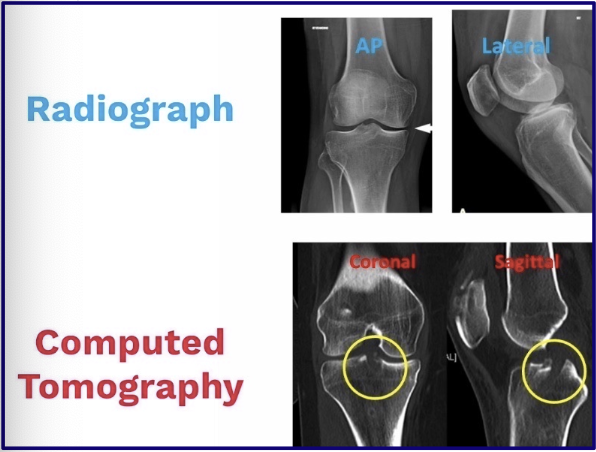
How are radiodensities of tissues represented on CT?
By shades of gray
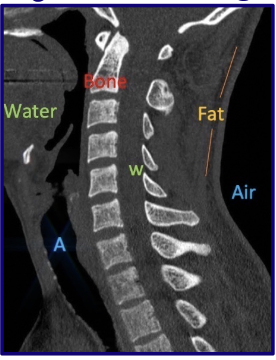
How does air appear on CT?
Air → Black
black Nike air forces
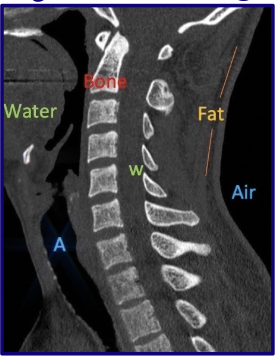
How does fat appear on CT?
Fat → Gray-Black
fat g(r)ays wearing black
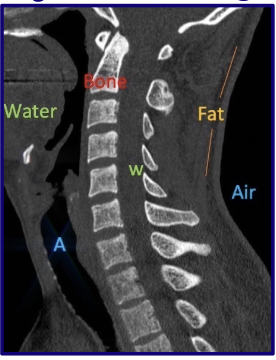
How does water appear on CT?
Water → Gray
dirty gray water
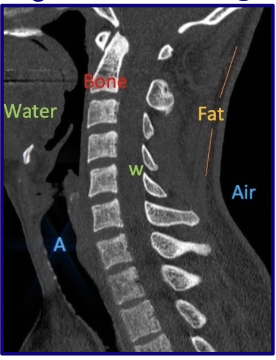
How does bone appear on CT?
Bone → White
white bones
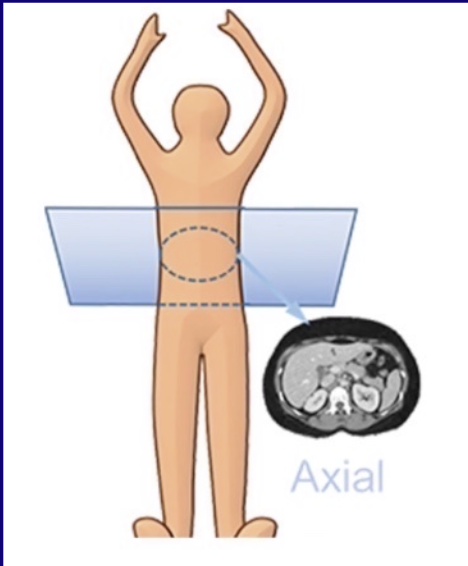
How is the CT image displayed?
As though the patient is supine and you are looking through the feet in axial view
What is windowing in CT?
A contrast enhancement technique that lets you visualize groups of radiodensities one at a time
Humans see 32 shades of gray, computers see thousands
CT scan can differentiate a 1% change in radiodensity, but it cannot be put all in one image, so it uses “windows” to visualize groups of radiodensities one at a time
Why is windowing important in CT?
It gives CT high sensitivity by emphasizing different tissue density ranges
What are the common CT windows?
Bone window and soft tissue window
Will show the ranges of raiodensities based on chosen tissue window
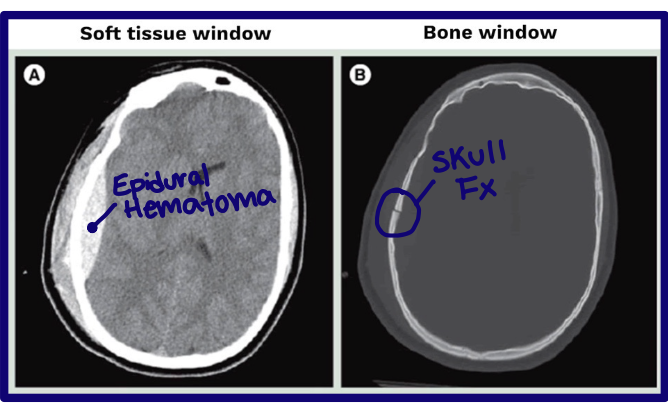
What does window level allow?
Discrimination between tissues of similar densities
What can a soft tissue window show well?
Soft tissues such as brain gray and white matter
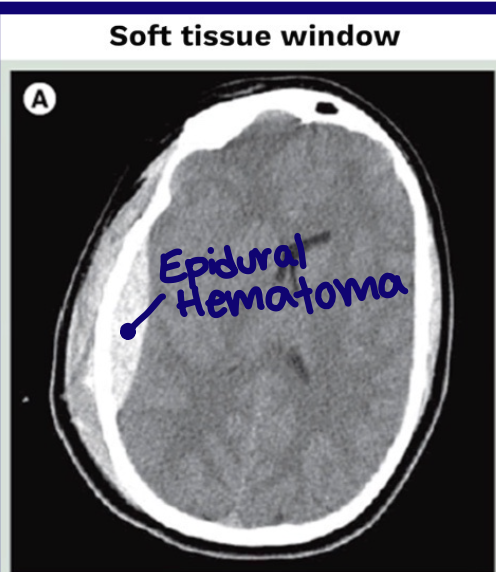
What can a bone window show well?
Cortical bone and cancellous bone
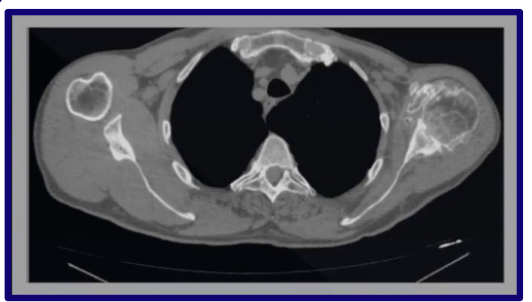
What are common clinical indications for CT?
Life-threatening injury evaluation
Complex & subtle fractures
Loose bodies in a joint
Degenerative changes
Spinal stenosis
What are the major advantages of CT?
Fast image acquisition time
Images bone and soft tissue in one series
Can view large body regions
Best in emergencies
Excellent bone definition
Why is CT often preferred over MRI for cortical bone?
Better cortical bone definition
Less time-consuming ⏰
Less expensive 💰
Less claustrophobia
Metal implants are generally less of an issue
What is the major disadvantage of CT?
High radiation exposure

What is MRI?
A cross-sectional imaging technique using a magnetic field and radiofrequency signals to generate images from hydrogen nuclei in water molecules
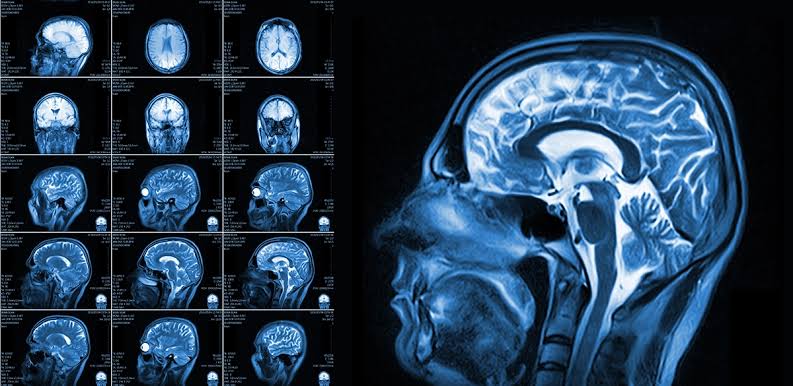
How are coronal MRI images viewed?
From the front facing the patient
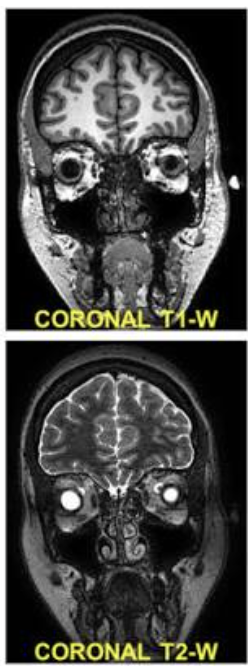
How are sagittal MRI images viewed?
From one side of the body to the other
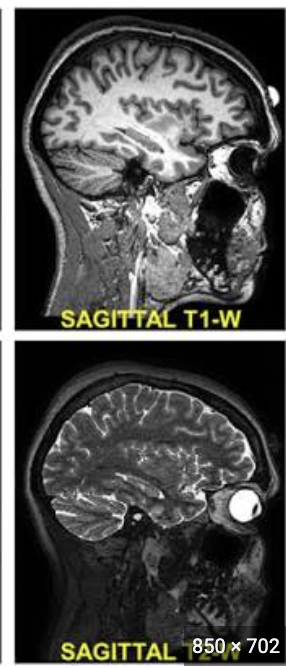
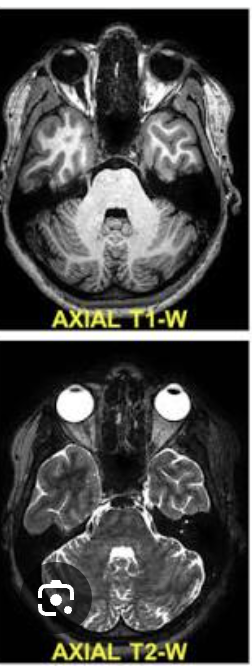
How are axial MRI images viewed?
From the feet toward the head like CT
What are the three basic components of MRI?
Scanner
Operator console
Computer
The SOCk
How does MRI work in basic terms?
Scanner creates a small magnetic field
Hydrogen protons in water molecules in tissues align with a magnetic field
Then a radiofrequency pulse disrupts them, then released energy is converted into an image
Why do different soft tissues look different on MRI?
Different tissues have different water content and release absorbed energy at different rates
What determines the construct of an MRI image?
The sequence used
What are the two common MRI sequences?
T1-weighted and T2-weighted
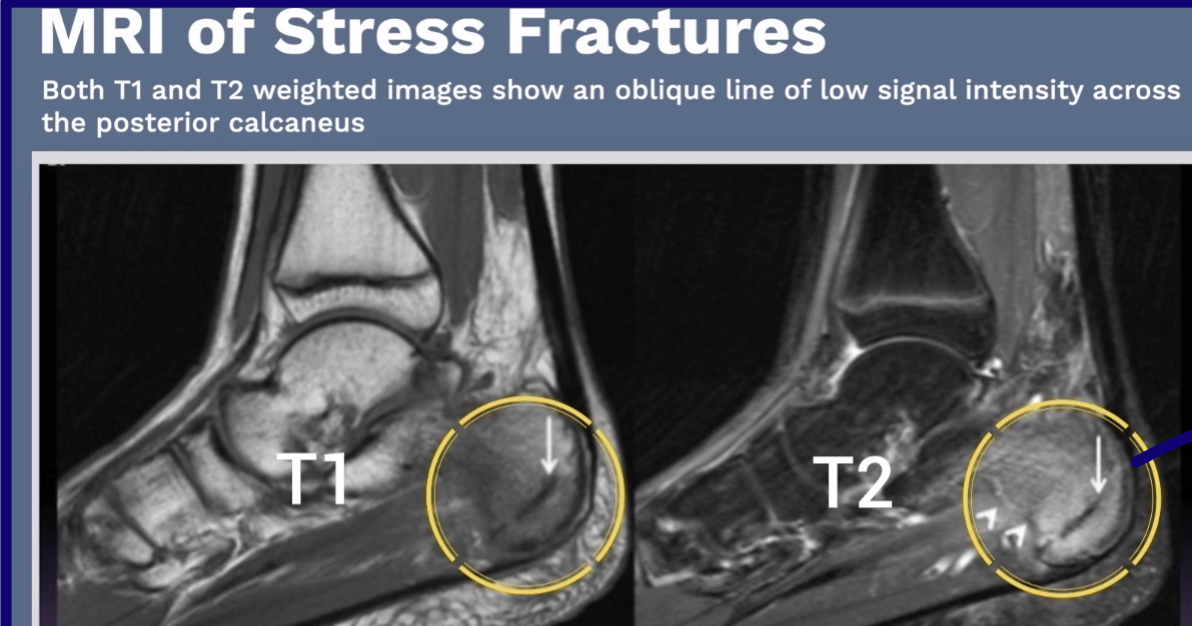
What is a basic tenet of MRI?
Define anatomy (T1)
Detect abnormal fluid (T2)
Hint: H2O → T2
White = edema in photo
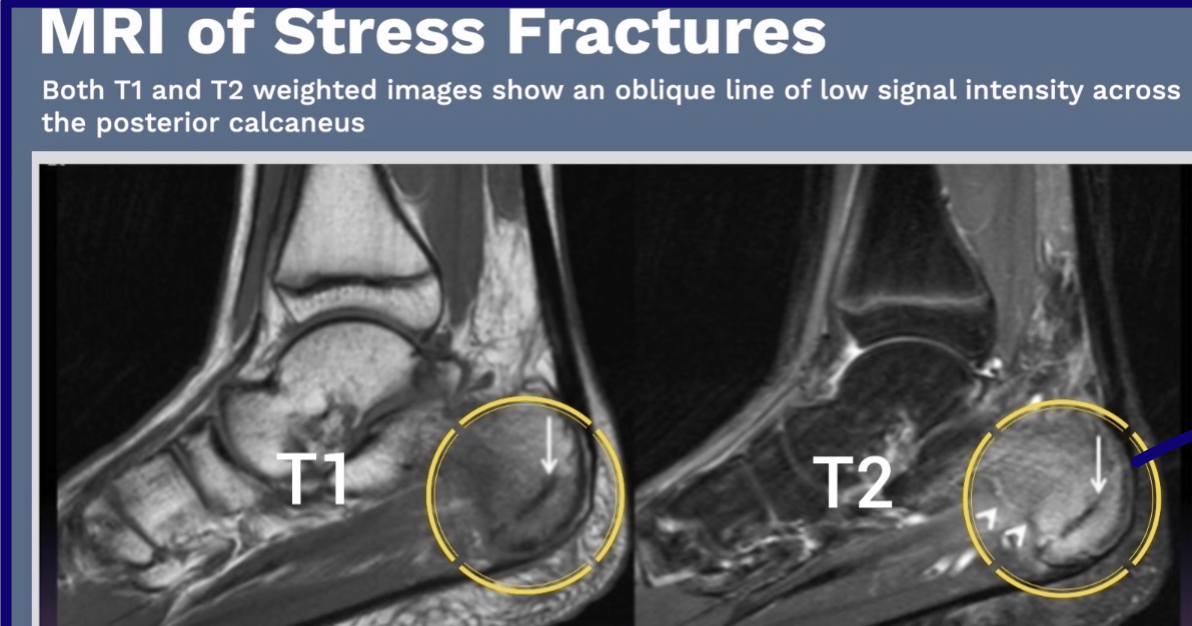
How does pathology often appear on MRI?
Pathology commonly involves edema or inflammation
What does high signal intensity mean on MRI?
Brighter image
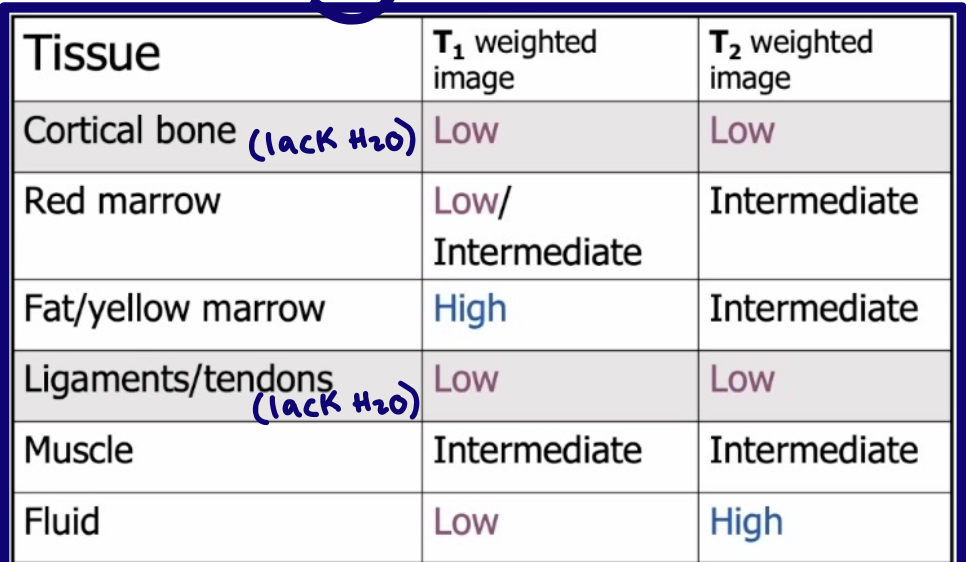
What does low signal intensity mean on MRI?
Darker image
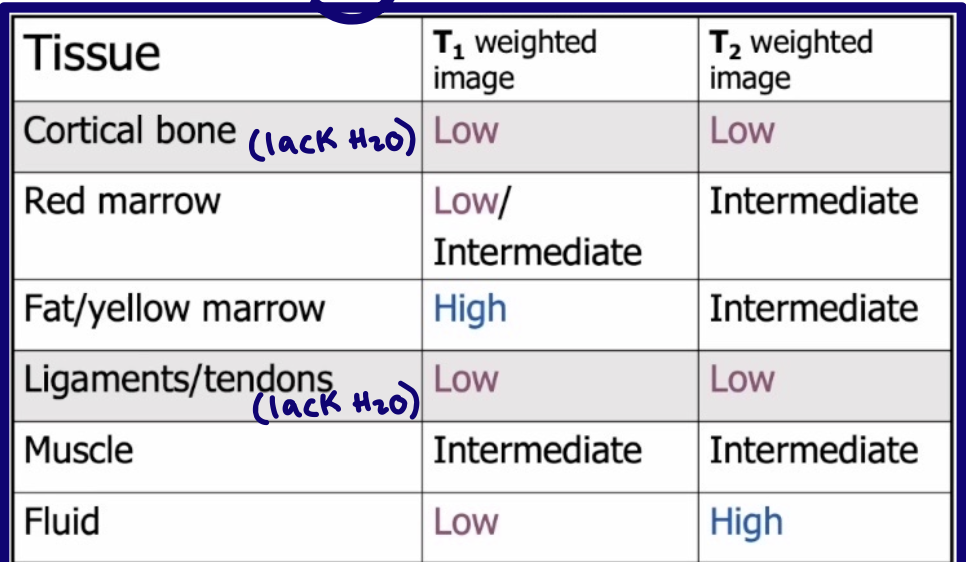
How does water or edema usually appear on T2-weighted MRI?
Bright
What are common clinical indications for MRI?
Soft tissue injuries
Bone marrow changes
Intervertebral disc pathology
What is a limitation or disadvantages or contrindications of MRI for bone?
Cortical bone is not well seen because of low signal intensity
Longer time
Claustrophobia
High cost
Metal implant contraindications
What can ultrasound diagnose in vascular medicine?
Arterial and venous disease throughout the body
How can ultrasound be used in procedures?
To guide nerve blocks
How is ultrasound used in ophthalmology (eyes)?
To measure eye length and see inside lesions
How is ultrasound used in otolaryngology (ears, nose, throat)?
It is the preferred imaging modality for thyroid tumors and lesions
How is ultrasound used in newborns?
To assess the brain
How can ultrasound be used in pulmonary or thoracic care?
To visualize lungs in diagnosis of lung cancer
How is ultrasound used for the bladder?
To check retained fluid volume
How is ultrasound used in MSK imaging?
To image soft tissues such as tendons ligaments and nerves
What are major general features of ultrasound?
Noninvasive
No known ill effects
Provides dynamic information
What is ultrasound imaging based on?
Tissue absorption of sound waves and reflection at tissue interfaces
What are the three components of diagnostic ultrasound?
Pulser
Transducer
Scan converter or monitor
What does the pulser (component 1/3) do in ultrasound?
Produces waves of electrical energy
What does the transducer (component 2/3) do in ultrasound?
Converts electrical pulses to sound waves and receives reflected waves back from tissues
Does diagnostic ultrasound increase tissue temperature?
No
Do the patient and imager have to remain static during ultrasound?
No
How are ultrasound images usually oriented?
In short axis and long axis relative to the structure examined
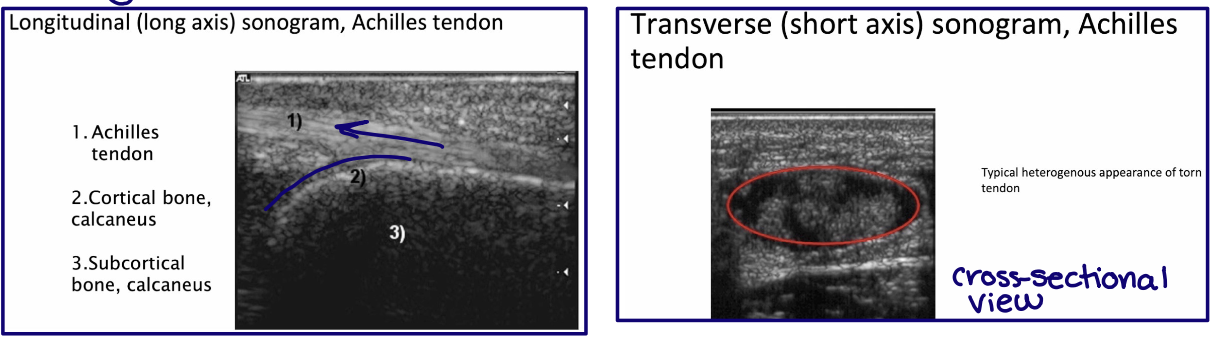
Why do tissues not have fixed ultrasound appearances like on CT or MRI?
Reflection intensity depends on the:
Tissue interface
Beam angle
Tissue type
What does echogenic mean?
Tissues ability to return an echo or signal during ultrasound
What does hyperechoic (bright) mean?
Tissues that reflect a lot of sound energy
Bright
What does hypoechoic (dark) mean?
Tissues that reflect little sound energy
Dark
What does anechoic mean?
No reflection
What is one of the best uses of ultrasound?
Imaging soft tissue structures (tendons, ligaments, & nerves) in a dynamic functional state
What are disadvantages of ultrasound?
Operator dependent
Does not penetrate bone
Cannot cross air interfaces
Hard to image obese patients
Which modality is best for bone imaging?
Bone → CT
Which modality is best for soft tissue imaging?
Soft tissue → MRI
Which modality can rival MRI for soft tissue imaging in some cases?
2nd best for soft tissue → Ultrasound
What are the general advantages of a chest x-ray?
Quick
Cheap
Noninvasise
Useful for thoracic and nearby structures (thyroid, GI, bony thorax)
Why is the bony thorax important on chest radiograph?
Bones help identify:
Soft tissue anatomy
Lesion location
How is thoracic spine radiography different from chest x-ray?
Thoracic spine → HIGH contrast & A-P
Chest x-ray → LOW contrast & P-A
PA-PA’s chest
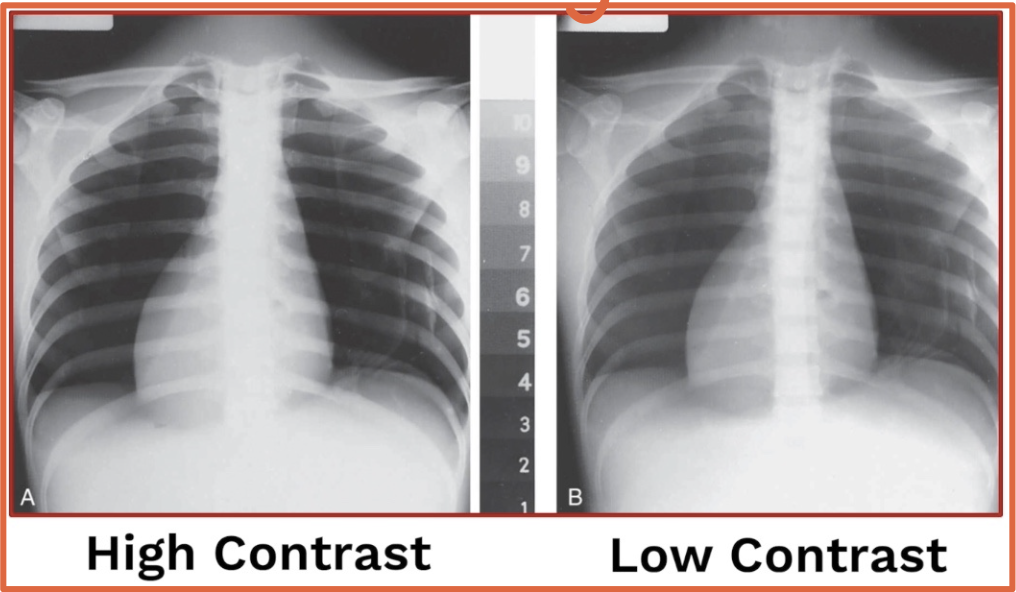
What chest x-ray view is usually preferred when possible?
PA
double check this
Why is PA preferred over AP for chest x-ray?
AP magnifies the heart and lungs
What happens if the patient cannot stand for a chest x-ray?
The film is taken AP
How many anterior & posterior ribs are typically seen on an adequate chest x-ray?
6 anterior ribs
10 posterior ribs
Which ribs are usually easiest to count on chest x-ray?
Posterior ribs because they are furthest from the image receptor and can be traced back to the vertebrae → magnified the greatest
What happens to the anterior ribs on chest x-ray?
Anterior ribs become more radiolucent near the costal cartilages
What respiratory structures are commonly identified on chest imaging?
Larynx
Trachea
Bronchi
Lungs
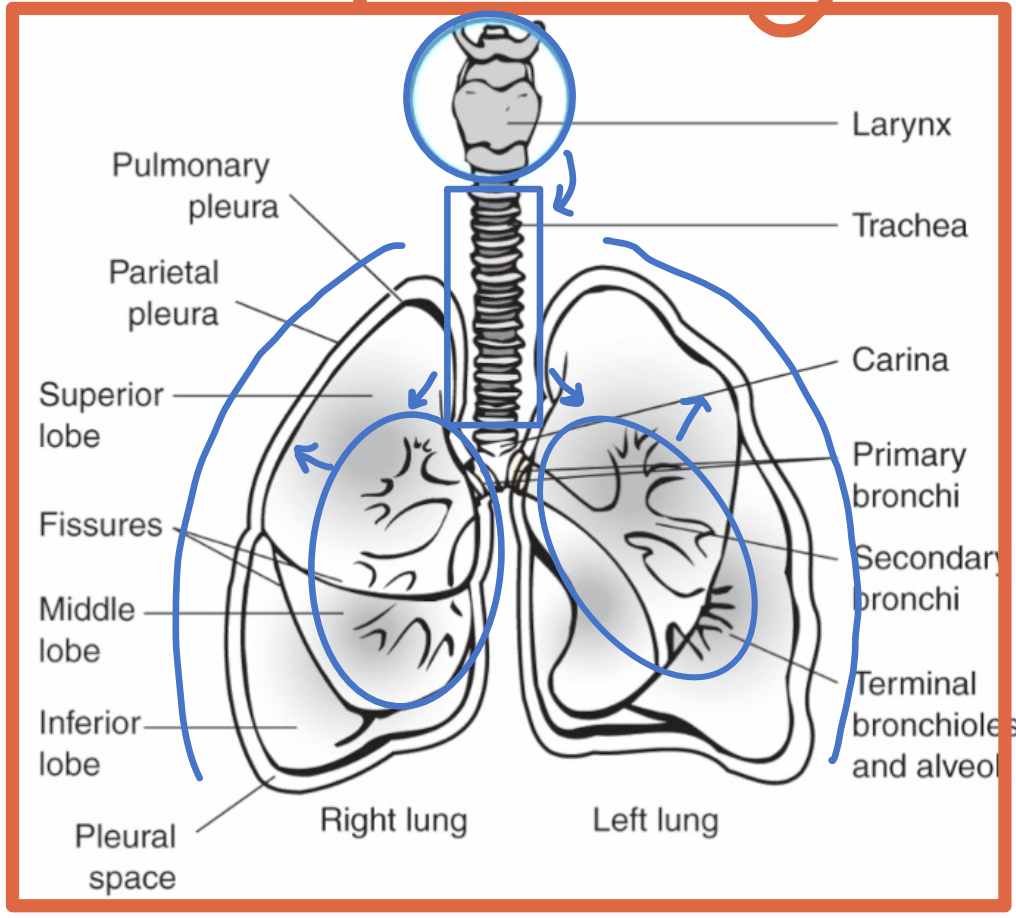
What is the pleura?
A double-walled sac surrounding each lung
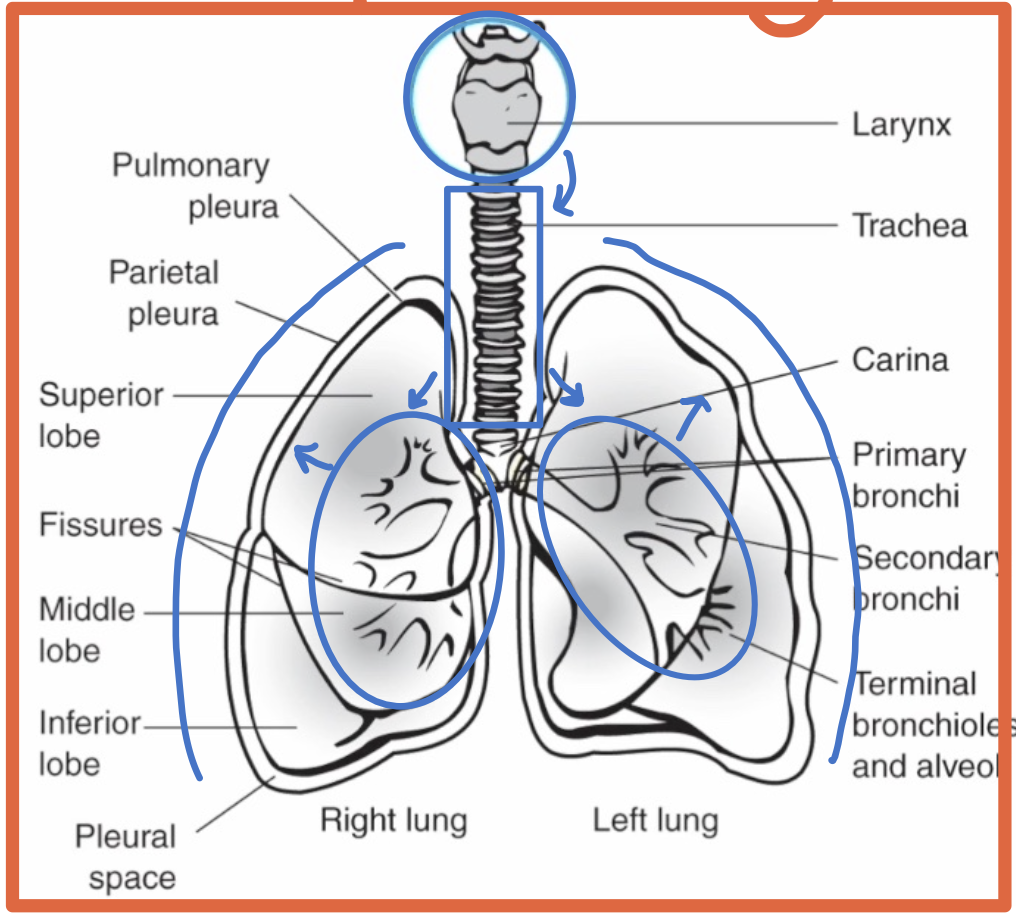
What is the parietal pleura?
The outer pleural layer lining the chest wall and diaphragm
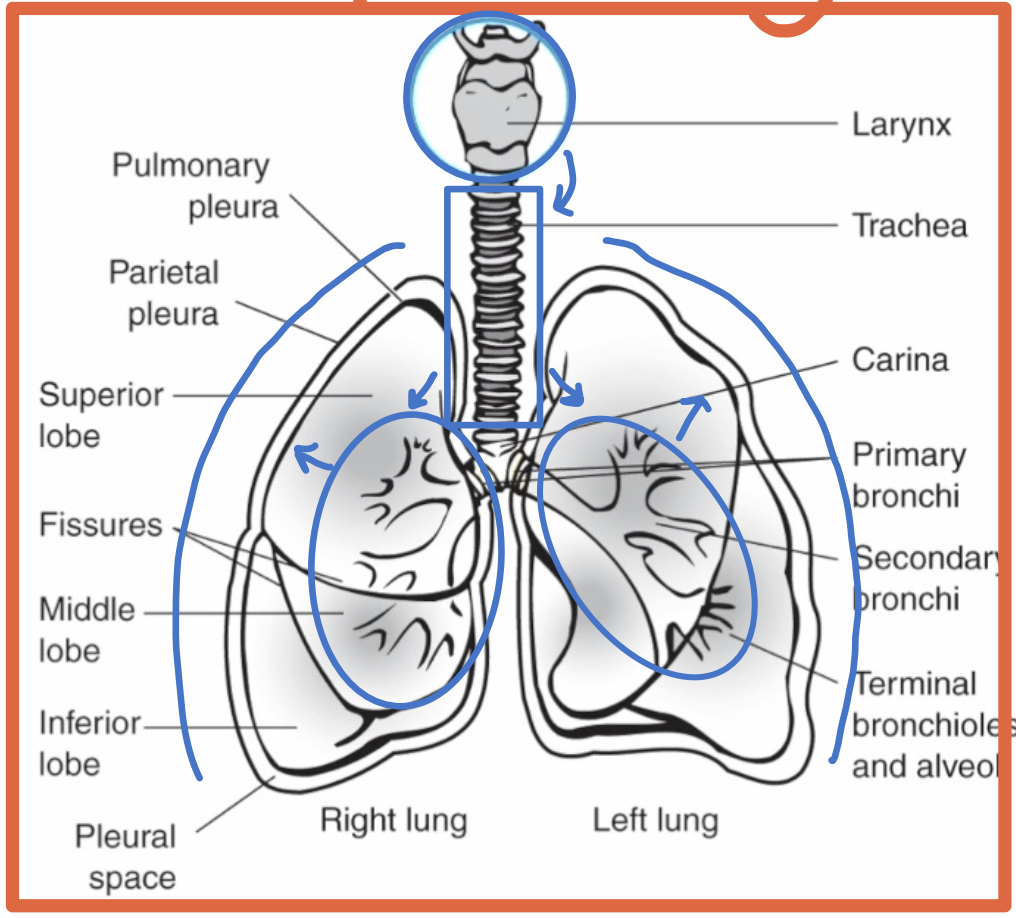
What is the visceral pleura?
The inner pleural layer covering the lung surface and dipping into fissures
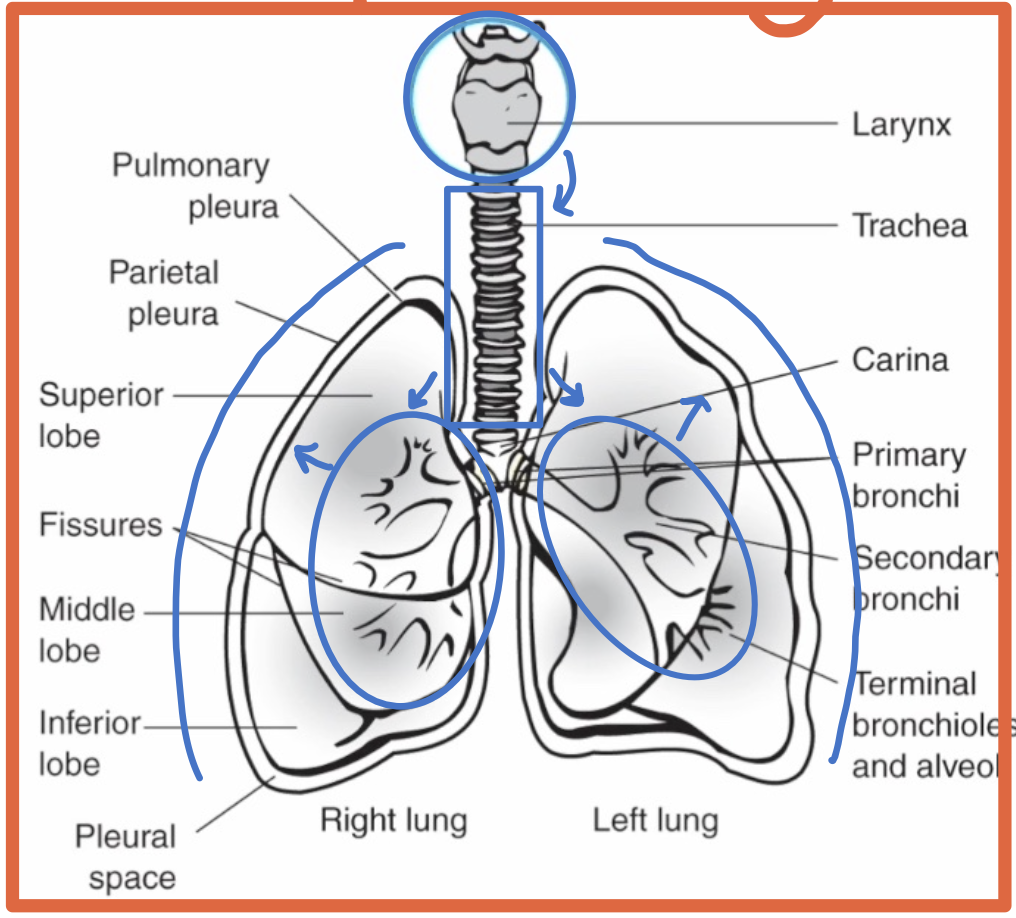
What is the pleural space?
The space between the parietal and visceral pleura
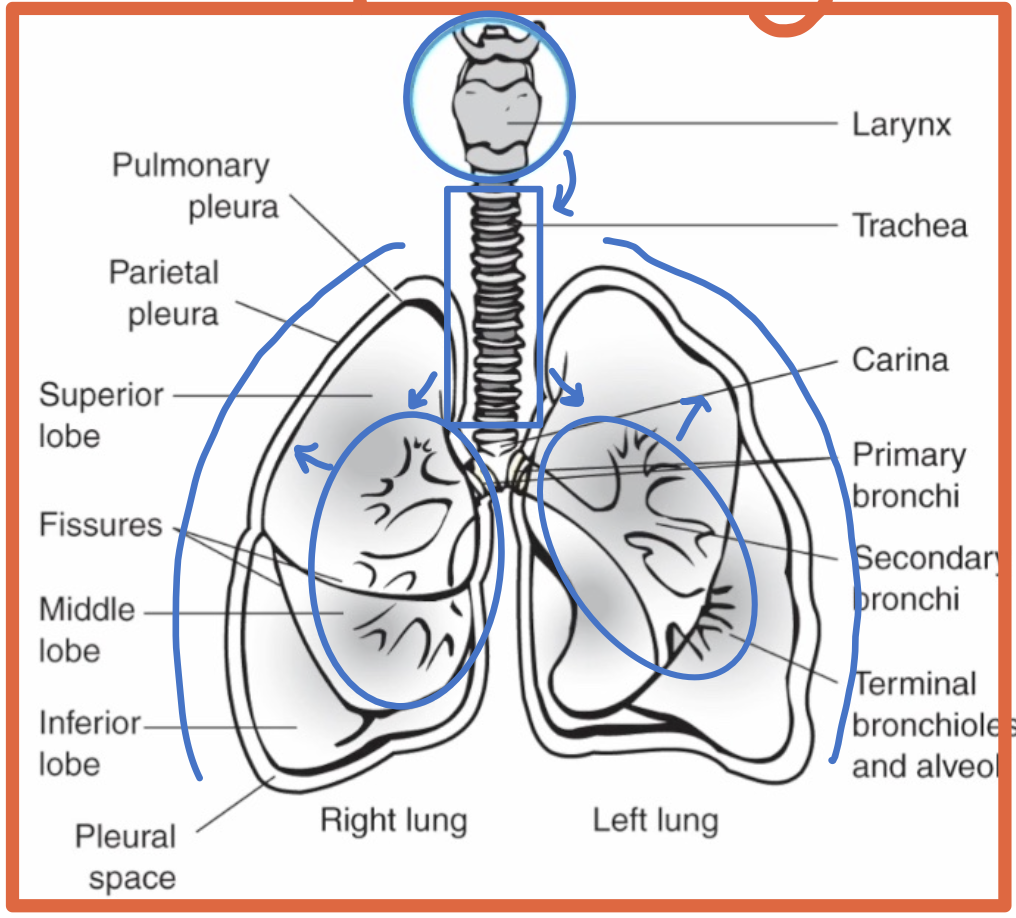
What is the cardiothoracic ratio?
A radiographic estimate of heart size
What is a normal adult cardiothoracic ratio?
The heart width should be less than half the chest width at the level of the diaphragm
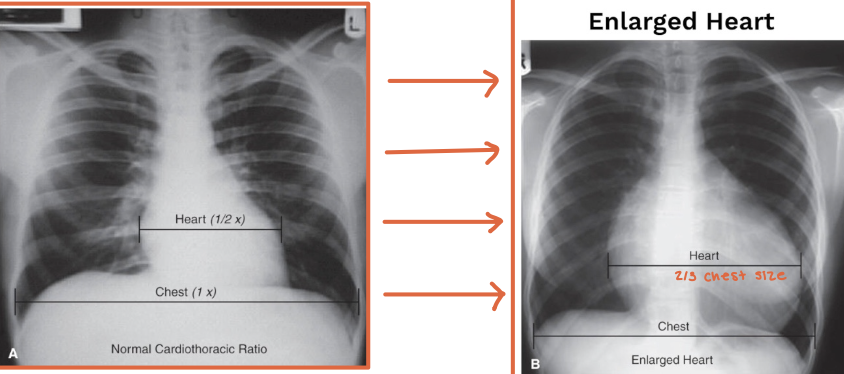
What is the mediastinum?
The space between the lungs bounded by the sternum anteriorly and spine posteriorly
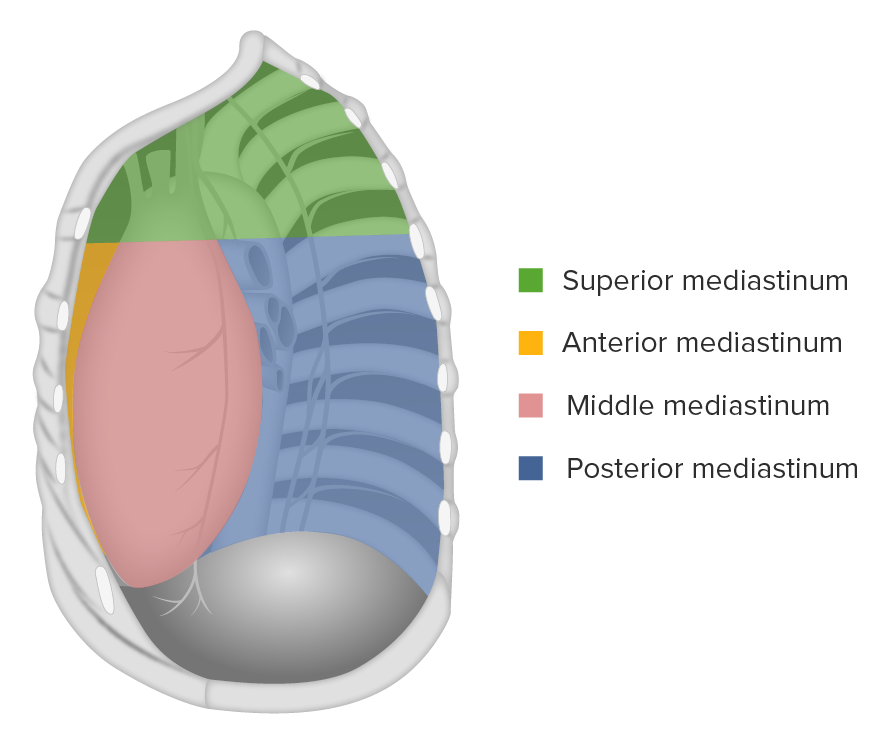
What major structures are in the mediastinum?
Heart
Great vessels
Trachea
Esophagus
All have similar radiodensity, besides air filled
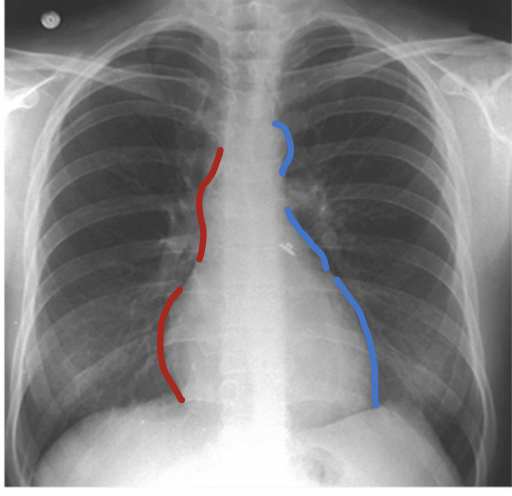
What mainly forms the right mediastinal border?
Superior vena cava
Right atrium
What are the three major bumps on the left mediastinal border?
Aortic arch or knob
Left atrial appendage
Left ventricle
What is the hilum?
The lung root of the mediostinum where bronchi, arteries, veins, and nerves enter and exit the lungs
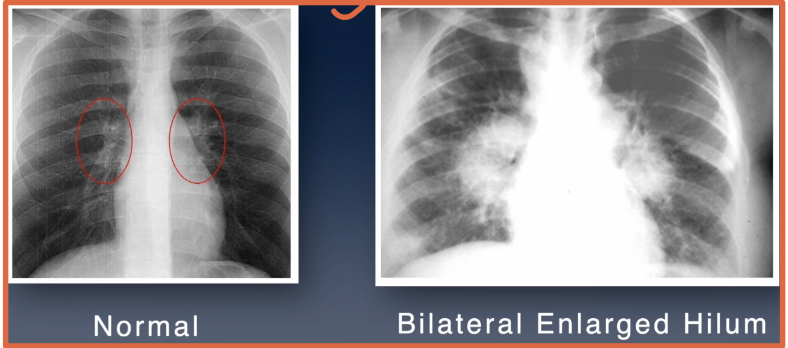
What can hilar (hilum) enlargement suggest?
Lymph node or tumor inflammation
Pulmonary venous or arterial hypertension
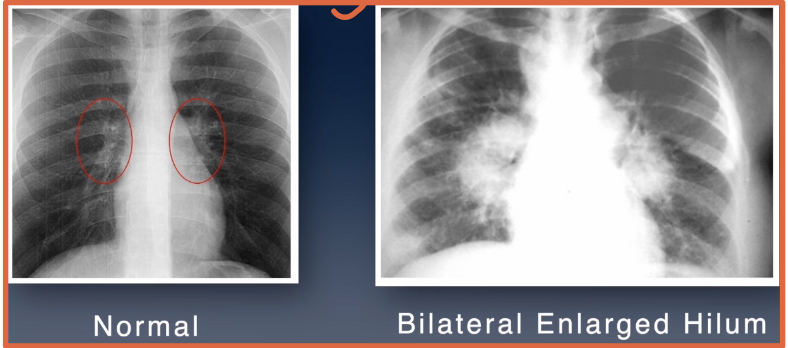
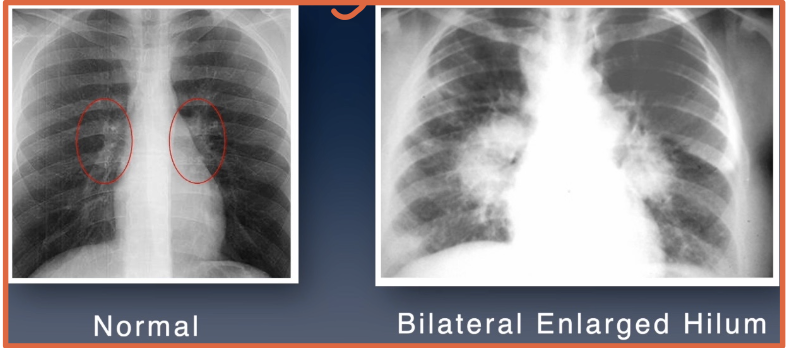
What disease example in the notes can cause hilar enlargement from lymph node swelling?
Sarcoidosis
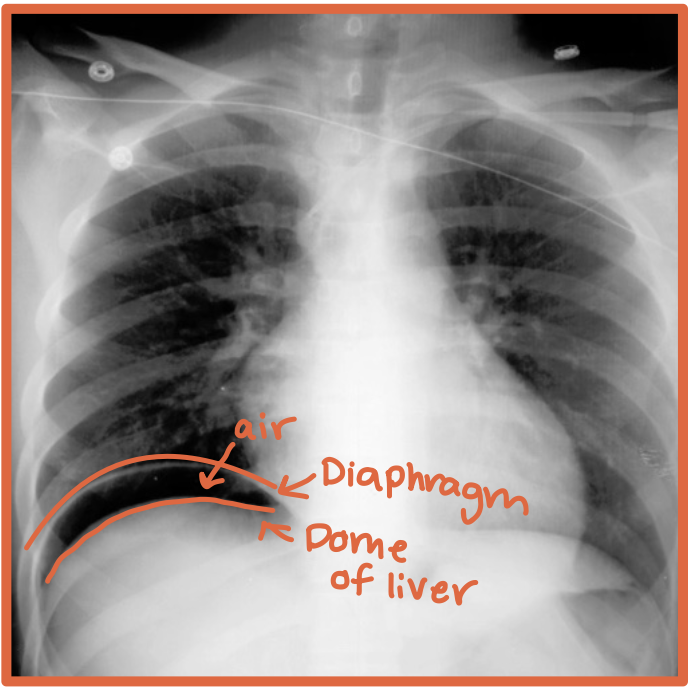
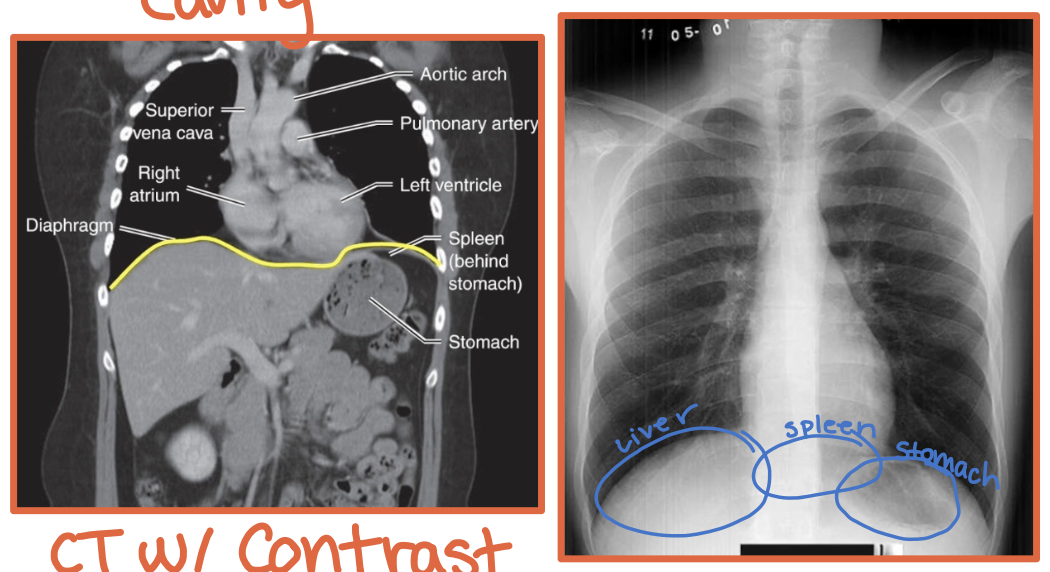
What is the diaphragm?
A thin curved sheet of muscle separating the thoracic and abdominal cavities
What is a costophrenic angle/sulcus?
The sharp recess where the diaphragm meets the chest wall
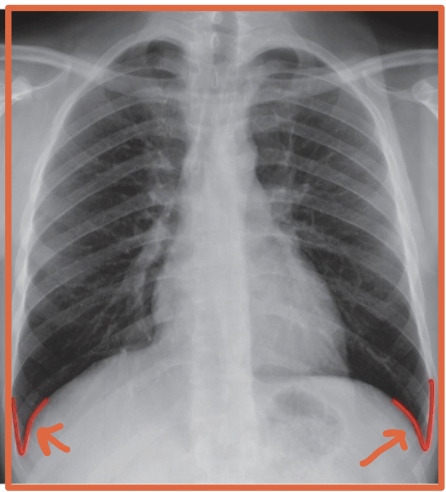
Why are the costophrenic angles/sulcus clinically important?
Pleural fluid collects there
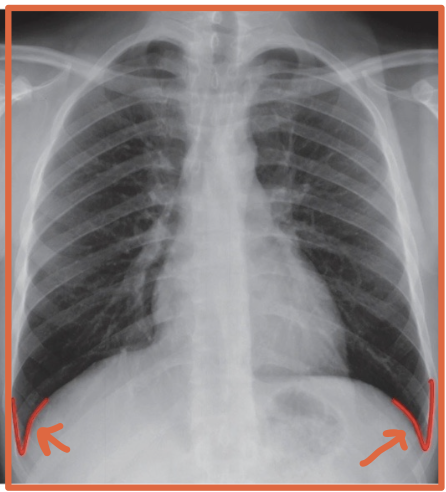
What is a hemidiaphragm?
A term used to describe a half of s diaphragm because they often act seperately
Split L + R
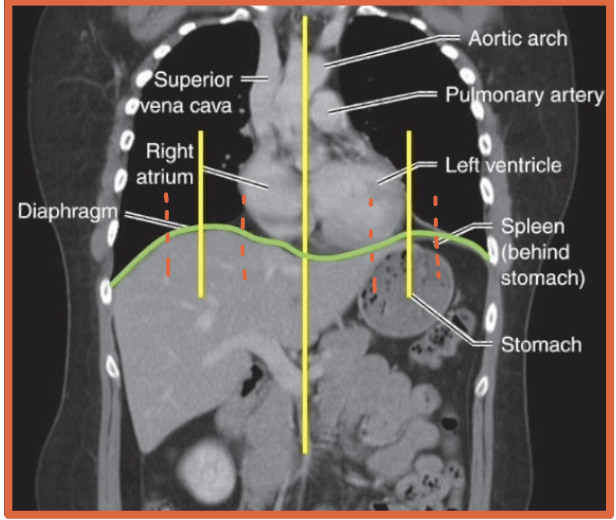
Where is the liver located relative to the hemidiaphragms?
Under the right hemidiaphragm
R + Liver = River
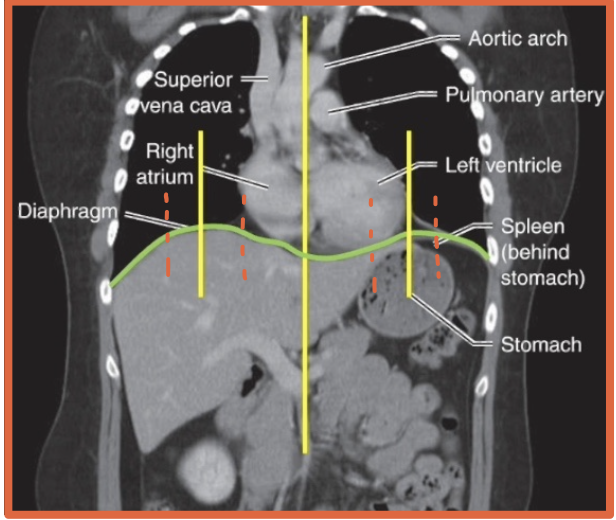
Where is the stomach located relative to the hemidiaphragms?
Under the left hemidiaphragm
Stomach took an L
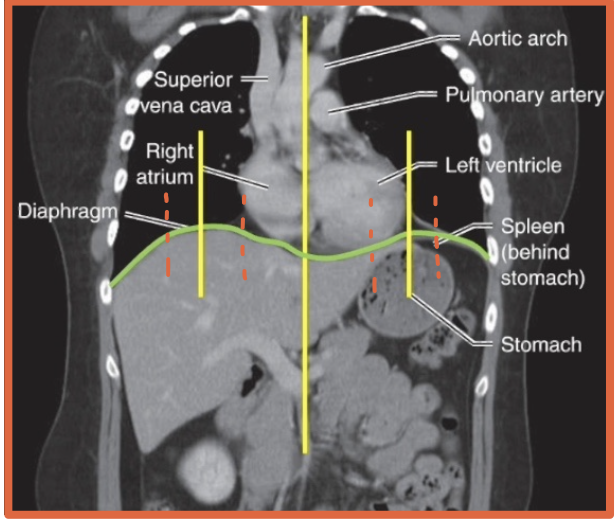
At about what rib level should the diaphragm reach on a good inspiratory chest x-ray?
Around the 10th posterior rib
What can cause a flattened diaphragm?
Any condition that increases lung volume
Ex: Emphysema or large pleural effusions
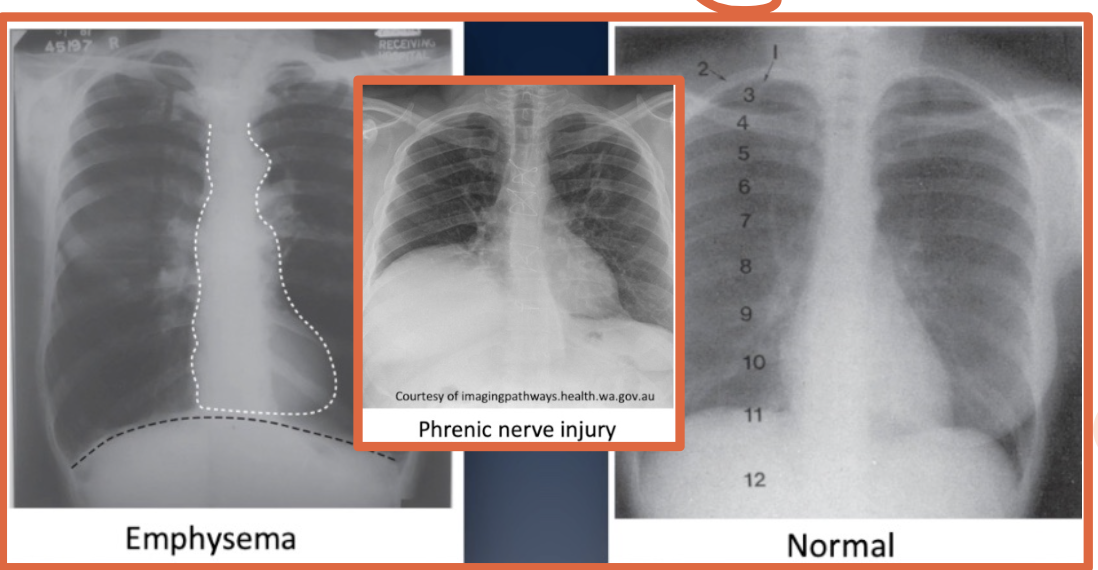
What can cause an elevated diaphragm?
Excessive peritoneal fluid from ascites, cirrhosis of the liver, or phrenic nerve injury
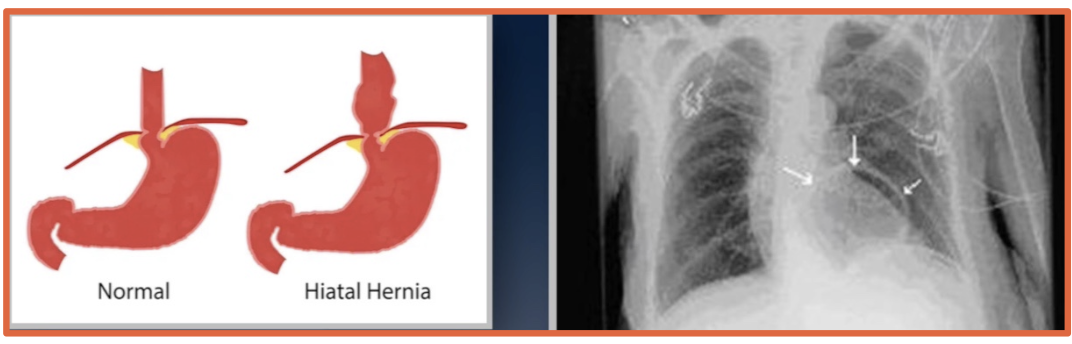
What is a hiatal hernia on chest imaging?
Part of the stomach herniates upward through the esophageal hiatus
What does free air below the hemidiaphragms on imaging mean?
Free air outside the bowel in the peritoneal cavity, usually suggesting bowel perforation
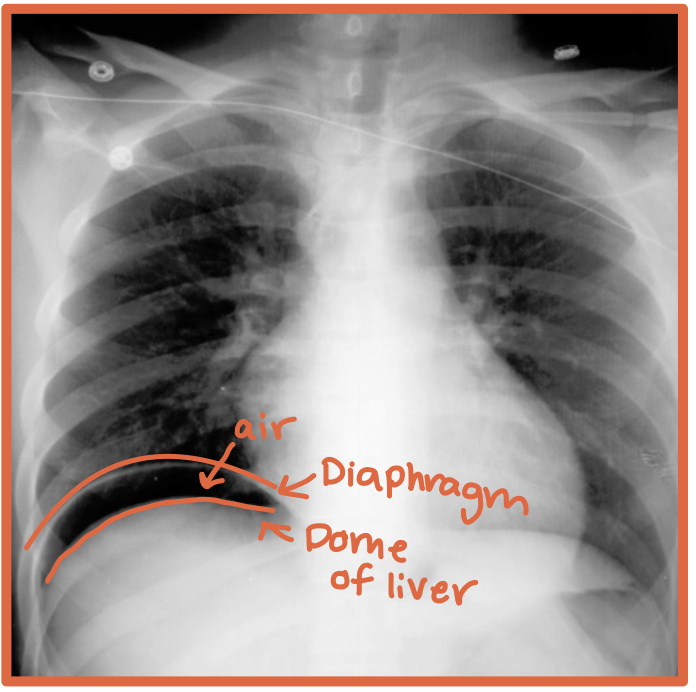
What gas is normal to see in the abdomen on imaging?
Gastric or bowel gas inside the GI tract