Hormones, cell signalling, transport and kinetics
1/89
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
90 Terms
What is autocrine signalling?
affects cells producing the signalling factor
What is paracrine signalling?
Diffuse short distance to affect cells nearby
What is endocrine signalling
acts on target cells at a distance from site of synthesis
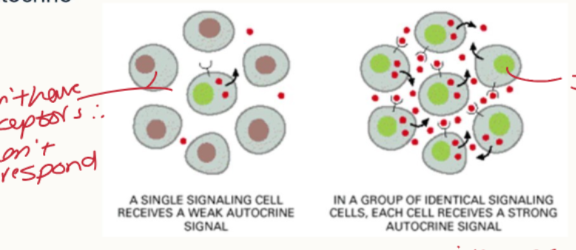
How can autocrine signalling affect local cells?
In a group of identical signalling cells, each cell can receive a strong autocrine signal.
a single signalling cell receives a weak autocrine signal
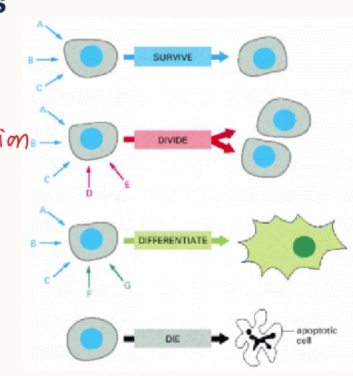
what are the 4 cellular decisions post signalling?
survive
cell growth/division/proliferation
differentiate
die/apoptosis
What are the two types of hormone
lipid soluble
water soluble
Outline lipid soluble hormones:
how are they transported
how to they enter cells
how do they affect cells
carrier proteins in blood
diffuse through plasma membrane
alters expression of genes at level of nucleus
Outline water soluble hormones
how are they transported
how to they enter cells
how do they affect cells
easily travel in blood
bind to receptors on surface of cell
intracellular events
what are most water soluble signalling molecules?
growth factors
water soluble hormones
MOST SIGNALLING MOLECULES
What are examples of lipid soluble hormone
steroid hormones
thyroid hormones
retinoids
vitamin D
Give 3 example locations of lipid soluble hormone production and what they produce
Adrenals: androgens, cortisol, corticosterone and aldosterone
Ovaries: estradiol
testes: testosterone, dihydrotestosterone
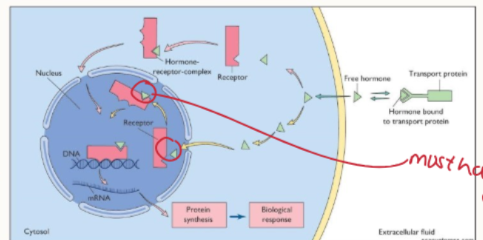
What happens when a hormone binds to its nuclear receptor?
hormone binds
receptor is activated, moves to nucleus
active receptor binds to DNA
regulates transcription of specific target genes
Outline the process of lipid soluble hormone signalling
hormone released from transport proteins
hormone enters cell
binds to nuclear receptor
bound receptor enters nucleus and binds to DNA
transcriptional regulation of target genes
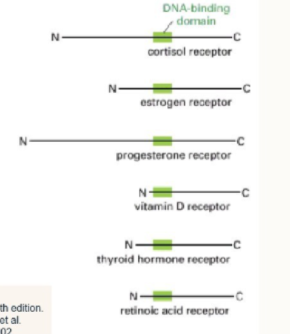
What are the 3 domains of a nuclear receptor?
transcription activating domain
DNA-binding domain
hormone-binding domain
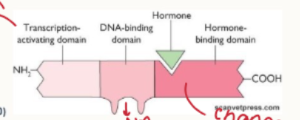
How do nuclear receptors vary?
all have similar domains: all have 3 parts.
vary in the N- and C- terminal regions
this allows ligand binding specificity
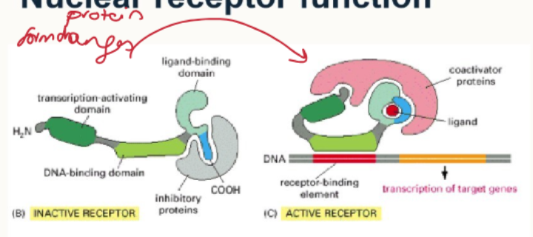
How does the nuclear receptor become activated?
hormone binds
conformational change in shape, exposing the DNA binding site.
Protein joins with co-activator proteins which regulate activation and repress nearby target genes.
Outline water soluble hormones:
What do they interact with
what do they induce
membrane-bound receptors: inhibitory or stimulatory
intracellular signal transduction pathways
What are the 5 enzymes/pathways involves in water soluble hormone signalling
adenyl cyclase (cAMP)
guanyl cyclase (cGMP)
phospholipase C, IP3 and DAG
Tyrosine kinase
ion channels
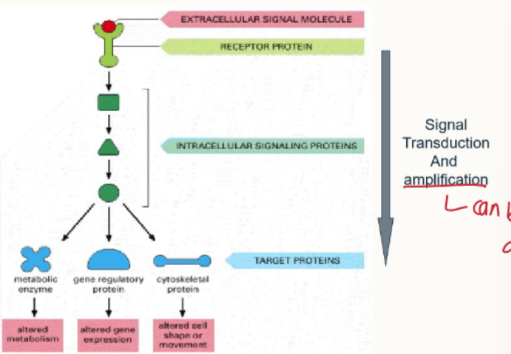
what is the intra-cellular signalling pathway
signals sent from the cell membrane where the bound ligand binds to its complementary receptor.
signals are transduced through the signalling pathway: they can be amplified
Give an example of water soluble hormones for:
Adenyl cyclase
guanylyl cyclase
phspholipase C
tyrosine kinase
ion channels
ACTH, ADH, FSH, LH and TSH
rare atrial natruiretic peptide
hypothalamic hormones, TRH, GnRH
insulin, prolactin, growth hormone, IGF
hormones using multiple pathways
What is the structure of the receptor for water soluble hormones
extracellular domain: binds to hormone
transmembrane domain
intracellular/cytoplasmic domain
Which domain of the cell membrane receptor changes during signalling?
cytoplasmic domain undergoes conformational change
this activates the signalling pathway
Growth factors vs cytokine?
SAME THING
growth factors are used in terms of growth
cytokines in terms of immunology
both perform paracrine and autocrine action
Functions of growth factors and cytokines?
cell division
cell differentiation
programmed cell death
aberrant function of growth factors/cytokines are implicated in cancer
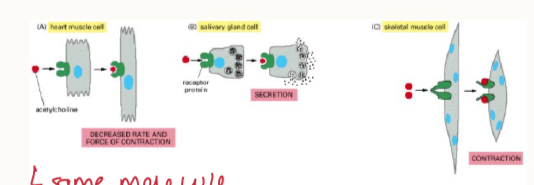
Does a hormone have the same effect on each cell?
NO = pleiotropy
may have a different effect on different cell types
What is the relevance of half lives with hormones?
must regulate responses
signal must be withdrawn → response fades
different hormones have different half lives depenidng on rate of destruction/removal of molecules and promptness of response when the signal is removed.
What factors contribute to a hormone’s half life?
rate of destruction/removal of molecules
promptness of response when a signal is turned on/off
rate of synthesis
modifications of proteins
Define half life
time taken for the concentration of a signalling molecule to fall by half
what are the 4 classes of cell surface receptors
Ion-channel linked receptors
G-protein linked receptor
Tyrosine kinase-linked receptor
receptors with intrinsic enzymatic activity
What is involved with each of these signalling receptors:
Ion-channel linked receptors
G-protein linked receptor
Tyrosine kinase-linked receptor
receptors with intrinsic enzymatic activity
rapid synaptic signalling
act indirectly to activate a separate plasma membrane bound protein
directly associated with enzyme they activate
functions directly as enzyme
Outline how ion channels work
signal molecule binds to receptor
opens/closes channel
ions move into cell by diffusion
excitability of post-synaptic cell altered
Give 4 examples of ion channels
post-synaptic membranes
neuromuscular junction
nicotinic ACh receptor
GABA receptors
What are second messengers?
small intracellular signalling molecules
generated by receptor activation (amplification of signal)
diffuse rapidly away
pass signal on →activate other proteins
give 4 examples of secondary messengers
cAMP
cGMP
diacylglycerol - DAG, lipid soluble
Ca2+ ions
Name the 5 proteins involved in intracellular signalling
scaffolds
relays
adaptors
amplifiers
modulators
briefly outline what each of these function are:
scaffolds
relays
adaptors
amplifiers
modulators
holds proteins within pathway, not affected by signals
pass signal on
can stimulate/repress response
amplify signals/transduce them
can affect signal
What are the 2 key processes in cell signalling
protein phosphorylation by protein kinases
reversal of protein phosphorylation - phosphoprotein phosphatase
What are the two types of protein phosphorylation
of serine/threonine residues
of tyrosine residues
What can phosphorylation alter?
enzyme activity
protein stability
protein interactions
What is a G-protein coupled receptor
single polypeptide chain with a central hydrophobic region that spans plasma membrane 7 times
How does G protein signalling work?
what type of hormone is involved
what other proteins are involved
give an example
water soluble
membrane protein, G protein, target protein (enzyme or ion channel).
muscarinic ACh receptor
what is a G-protein?
guanine-nucleotide binding protein: a signal transducing protein
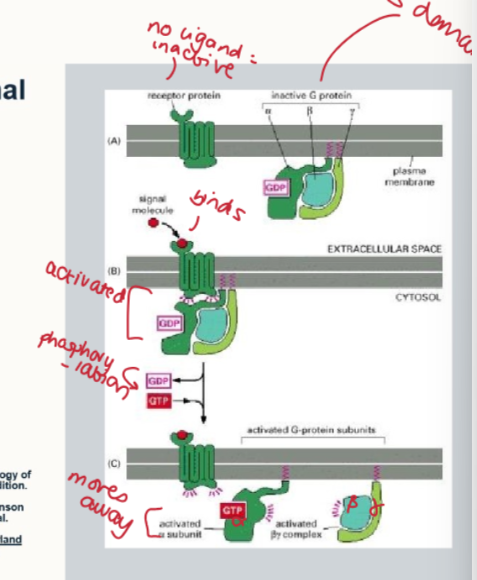
what are the 3 mains steps of G protein mediated signal transduction
no ligand = inactive receptor
binding of ligand recruites the G protein complex
GTP replaces GDP
G alpha and beta proteins dissociate
G alpha and beta subtunits regulate 2nd messengers: including adenylate cyclase
How can G-proteins act as inhibitors and stimulators?
depending on the hormone that binds!
if the hormone is stimulating → stimulating activity
if the hormone is inhibitory → inhibition
Outline the process of the stimulatory effect mediated by adenylate cyclase - give an example of this signalling
subunit of G protein activates adenylate cyclase
ATP → cAMP
cAMP acts as catalytic subunit of pKA (protein kinase A)
pKa is part of cascade of intracellular phosphorylations.
example = epinephrine acting through adrenergic B- receptor
How can one hormone molecule result in a large response?
1 hormone can trigger many cAMP molecules to be produced, which amplifies the response
Give an example of how a G-protein can inhibit adenylate cyclase
Norepinephrine acts through the alpha-2 receptor on the pre-synaptic nerve
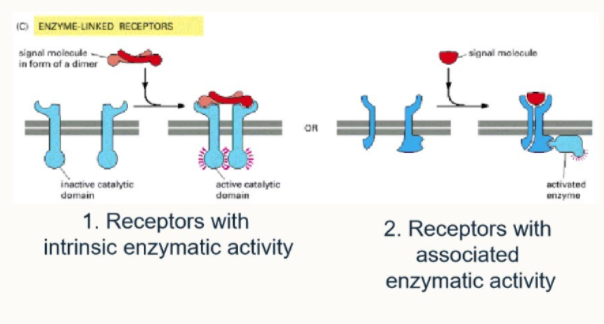
What are the two pathways of enzyme linked receptors
function directly as enzymes
directly associated with enzymes they activate
What are the 6 classes of enzyme linked receptors?
receptor tyrosine kinases
tyrosine-kinase-associated receptors
receptor like tyrosine phosphatases
receptor serine/threonine kinases
receptor guanyl cyclases
histidine-kinase-associated receptors (rarer)
What do each of these do:
receptor tyrosine kinases
tyrosine-kinase-associated receptors
receptor like tyrosine phosphatases
receptor serine/threonine kinases
receptor guanyl cyclases
histidine-kinase-associated receptors (rarer)
phosphorylate tyrosine on intracellular signalling molecules
associate with intracellular proteins with tyrosine kinase activity
remove phosphate group from tyrosine on intracellular proteins
phosphorylate serines/threonines on regulatory proteins
catalyse production of cytosolic cGMP
2 parts: kinase phosphorylates itself and passes on phosphate to intracellular signalling protein
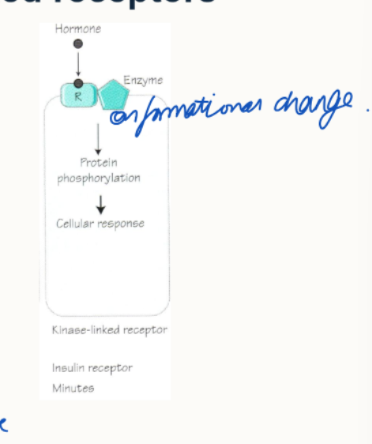
How to tyrosine kinase-linked receptors work?
they lead to the phosphorylation of intracellular signalling proteins
e.g. insulin and IGF-1 proteins
How do tyrosine kinase receptors activate multiple pathways?
phosphorylation of the receptor’s intracellular domains creates a docking surface for other cell signalling proteins
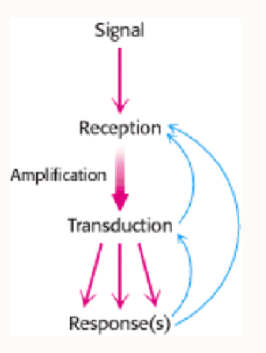
Outline the principle of a signal transduction pathway
when the ligand binds to the receptor it triggers protein kinases this leads to the activation of the desired protein(s) leading to the response.
What is meant by intracellular molecular switches and what are the two main classes of them?
They’re intracellular proteins + signal
they recover the signalling pathway by returning active proteins to inactive
Types:
phosphorylation (gain or loss changes signal)
GTP binding
For each type of molecular switch, what is the active form and what is the inactive
Phosphorylatioin: Gain = on, Lose = off
GTP/GDP:GDP bound = inactive, GTP bound = active
How may a cell response to a hormone be delayed or prolonged in duration
the primary response turns on secondary response proteins
simultaneously shuts off primary response genes
Why are some hormones responses abrupt, rapid and transient?
the response may depend on the binding of more than one intracellular molecule to a target molecule
nuclear receptor level: >1 activated hormone receptor complex must bind to DNA toa ctivate gene
cell surface level: similar binding principle may operate in a cascade
How can modulating receptor activity and density alter sensitivty to a signal? Give 5 examples
receptor sequestration
receptor down-regulation
receptor inactivation
inactivation of signalling protein
production of inhibitory protein
What are the 2 major communication systems
endocrine
nervous
Name the 12 endocrine glands
pineal
hypothalamus
pituitary
thyroid
parathyroid
adrenals and kidney
pancreas
testes
ovaries
skin
placenta
adipose tissue
What are the 4 organ-endocrine glands
heart
intestine
kidney
placenta
What do each of these produce as a hormone?
heart
intestine
kidney
placenta
Atrial natruiretic peptide (ANP)
cholecystokinin, gastrin
Active D3, EPO
chorionic gonadotropins (stimulate progestins)
What are the 4 characteristics of a hormone
chemical agents
synthesised and secreted by glands
circulate in blood to other parts of the body
stimulate specific tissues
what are the 3 classifications by function of hormones
classical (genuine) hormones
neurohormones
local hormones (paracrine signalling)
What is a classical hormone and what is an example
secreted from endocrine cells, diffuse into blood, transported by transporters via blood to target tissue
cortisol
What is a neurohormone and give 2 examples
synthesised within neuroendocrine cells
secreted from nerve terminals
diffuse into blood vessels and transported
examples:
CRH: corticotrophin releasing hormone
ACTH
What are local hormones and the two mechanisms by which they act?
diffusioni of hormone into intersistial fluid
paracrine and autocrine
Give an example of a water-soluble hormone and lipid-soluble hormone and how they’re transported in the blood
catacheolamines (epinephrine) - freely transported
cortisol and thyroid hormones - bound to transport proteins (cortisol binding globulin CBG)
Give 3 examples of specific lipid soluble hormone binding proteins and their hormones
cortisol-binding protein - cortisol
vitamin D-binding globulin - vit D
thyroid-binding globulin - T3 and T4
Give two examples of non-specific lipid soluble hormone binding proteins
Albumin - steroids
prealbumin - T3 and T4
Where are transport proteins produced and degraded, what is a potential clinical relevance?
liver
liver failure
how can we consider a free hormone?
active
What is the general percentage between bound vs free hormones
significantly more is bound than free
What can affect the amount of free hormone in the blood?
binding protein conc
hormone level
What are the 3 functions of transport proteins
serve as hormone reservoir
act as hormone buffers
reduce hormone loss via kidneys
Outline hormone reservoirs
free hormone diffuses into cells
used as it binds to receptors
equilibrium is reached
this reservoir is used to replace free hormone in the blood
e.g. thyroid hormones
Outline the purpose of hormone buffers
respond to increased hormone secretion
only use 50% binding capacity
short-term peaks in synthesis absorbed
raise amount of hormone in circulation
How is hormone loss reduced?
Being bound to transport proteins - can’t filter through glomerulus in kidney
What are the plasma concentrations the result of?
rate of secretion in blood
rate of removal from blood
What are 3 elimination mechanisms
enzymatic degradation
within target cells after binding recpetor
via liver and kidneys
What is fast action elimination
e.g. epinephrine
rapid release (from adrenal medulla)
immediate action on tissues (heart)
fast return to normal (few seconds)
water soluble hormone binds receptors
enzymatically degraded w/in cell
Outline slow elimination
e.g. thyroxine (T4)
circulates as mostly bound or free (lipid-soluble)
bound hormone resists degradation
either: converted to T3 (enters cell and alters gene expression)
OR converted into water-soluble compounds by liver → excretion in urine
what are 4 factors that affect hormone responses
variation by tissue (pleiotropy)
time (species, age, specific hormone)
dose and choice
status of target tissue
Give two examples of steroid therapy and their uses
prednisolone sodium succinate → ultra short acting corticosteroid for shock
dexamethasone - long-acting corticosteroid for immuno-suppression
How may target tissues with:
hypertrophy
atrophy
affect hormone effect?
more function tissue → exaggerated response
less function tissue → inadequate response
what is the clinical relevance of steroid treatment?
Steroid withdrawal e.g. dexamethasone (corticosteroid)
it suppresses normal synthesis and secretion from the adrenal gland
adrenal gland atrophies
CRISIS if withdrawn suddenly
How do we measure hormones?
v. small measurements:
picomol, nanomol
cortisol and thyroid: ng/mL
ACTH: pg/mL
insulin: uU/mL or mU/L
what are two assays we can use to test for hormones?
RIA: radioimmunoassay - highly sensitive - measures free hormone
ELISA - measures total
How do RIAs work?
known concentration of hormone is radiolabelled and bound by Abto form an Ab-hormone complex
unlabelled hormone being tested is added and competes w. labelled hormone
the resulting complexes are precipitated using a secondary Ab and the radiolabelled measured.
Compare known start amount of radiolabel to what we get → find conc of unknown hormone
What is the:
clearance rate
secretion rate
use radioactively labeled hormone or halt secretion
if conc remains stable, assume secretion = clearance