PSYC 301: Aging & Neurodegeneration
1/35
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
36 Terms
what is normal cognitive aging?
differential impacts on some cognitive domains over others
LTM & WM decline but vocab stays relatively stable
processing speed declines
individual variation
what are 4 normal brain changes in aging?
1) volume loss
2) neurotransmitter depletion
3) decreased blood flow
4) white matter damage
what is normal socioemotional changes of aging?
smaller but better quality social networks w/ higher proportion of emotionally close partners
greater emotional stability & emotional complexity in daily life
what are considered normal brain changes of aging?
small degree of alzheimer’s pathology & neuronal loss
what are abnormal brain changes of aging?
increasing forgetfulness
language, attention, exec function, problem solving, & visuospatial intact
drive without difficulty
taking more time to remember
behaviour & mood stable
what are characteristics of MCI?
changes in attention & memory that is noticeable to the person, friends, & family
cognitive difficulties in excess of normal aging; preserved activities of daily living
what is dementia?
impairment of multiple cognitive functions & activities of daily living
what causes dementia & does it typically onset?
syndrome caused by multiple diseases
middle-to-late adulthood
what are early symptoms of alzheimer’s disease?
confusion
irritability
anxiety
deterioration of speech
what are later symptoms of AD?
difficulties w/ even simple responses or behaviours (swallowing, speech)
what predicts the progression from MCI to AD?
older age
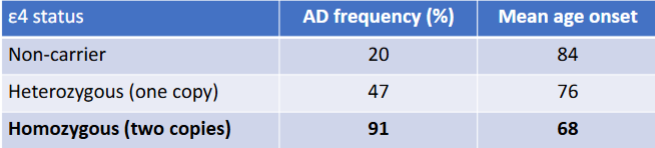
APOE E4 status
MTL atrophy on MRI
positive amyloid on PET scan
molecular markers in CSF (low AB, elevated total tau & phosphorylated tau)
what is the clinical significance of apo-e status?
everyone has 2 Apo-E genes
protein that plays a role in cholesterol transport & involved in normal metabolism of amyloid beta
3 forms: E2, E3, E4
what are 3 characteristics of AD?
1) neurofibrillary tangles
2) amyloid plaques
3) volume loss
what are neurofibrillary tangles?
tauopathy
act as prions
cell structure is compromised
intracellular
what is tauopathy?
tau proteins are hyperphosphorylated, misfold, & build up
what are amyloid plaques?
proteins take on large, collapsed forms & build up in the extracellular space
what is volume loss?
progressive loss of both cells & synapses, appearing 1st in MTL structures involved in memory
what 3 MTL structures does volume loss occur in?
entorhinal cortex
amygdala
hippocampus
what are structural changes that occur in the progression of AD?
disease spreads thru brain, causing progressive loss of connections between neurons, & then neurons themselves
later stages, the brain shrinks & the cerebral cortex appears shrivelled & the fluid-filled venticles are expanded
what are microscopic changes that occur in the progression of AD?
accumulations of amyloid plaques form between neurons
microtubules associated w/ tau protein accumulates in neurofibrillary tangles & they persist after neurons have died
what are the 3 theories of AD?
1) neurofibrillary (tau) hypothesis
2) amyloid cascade hypothesis (dom)
3) lithium deficiency theory
what is the neurofibrillary hypothesis?
holds that misfolded tau is the causal agent
what is the evidence for this theory?
tau pathology correlates w/ cognitive impairment better than AB
what is the problem w/ this theory?
tau mutation alone does not seem to cause AB plaques
what is the amyloid cascade hypothesis?
holds that amyloid plaques are the primary symptom & cause all others
what is the evidence for this theory?
trisomy 21
what are the problems w/ this theory?
high-plaque normals
amyloid drugs keep failing
what is the lithium deficiency theory?
holds that amyloid plaques bind endogenous lithium, reducing its normal function in the brain, & that lithium depletion activates microglia, impairing their ability to degrade amyloid
what is the evidence for this theory?
mice models have used supplementing w/ a form of lithium that avoids binding amyloid, preventing pathological changes & memory loss
what is the problem w/ this theory?
no human studies
what are 3 treatments for AD?
1) cholingeric agonists
2) NDMA receptor antagonist
3) target modifiable risk factors
what can cholingeric agonists help w/?
can help prevent decline in learning & memory
what can NDMA receptor antagonists help w/?
can prevent damage to neurons
what are modifiable risk factors?
depression
smoking
social isolation
what is a biomarker for AD?
CSF biomarkers for AD are related to amyloid & tau are helpful but not 100% definitive
what do the biomarkers for AD mean for patients?
can inform diagnostic, treatment, & referral decisions
return of biomarker results must be done w/ care
“wasn’t all in my head” => relief
"make meaning out of struggles”