Intro to the Liver
1/44
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
45 Terms
Liver blood supply
Dual supply: hepatic artery (oxygenated) + portal vein (nutrient-rich)
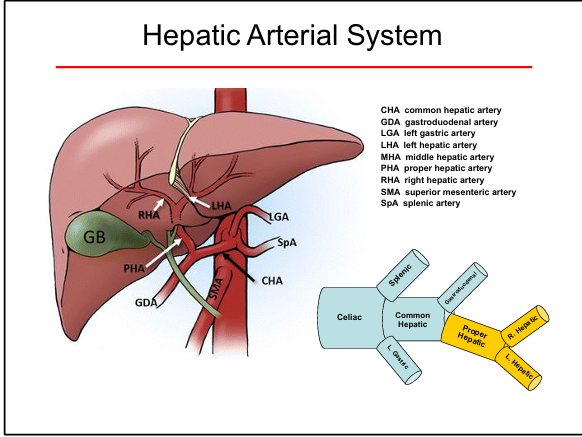
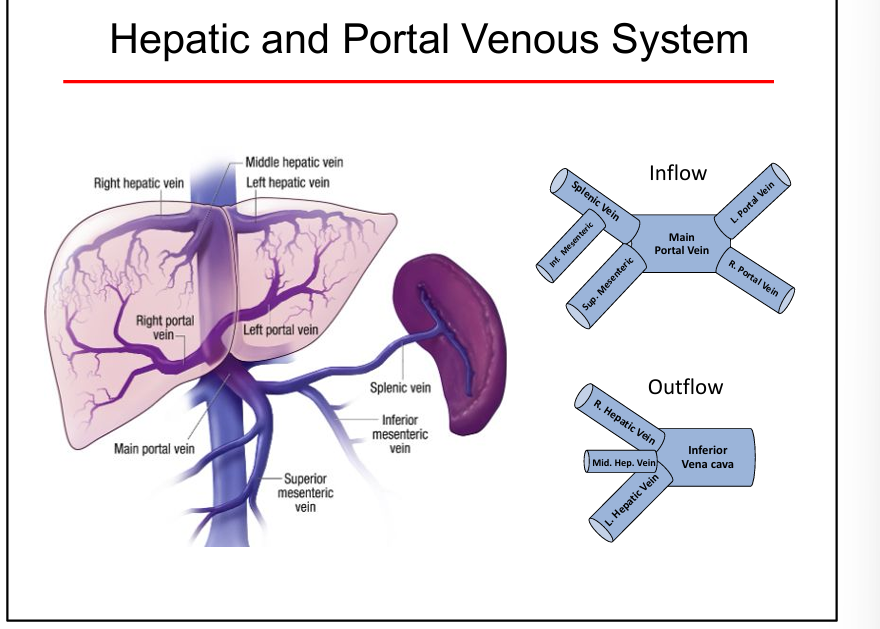

Portal triad components
Portal venule, hepatic arteriole, bile duct
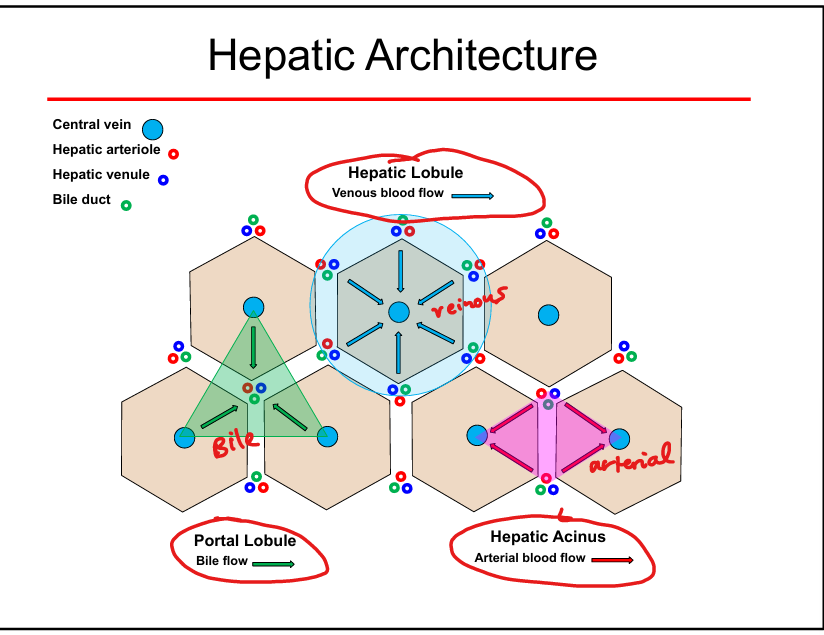

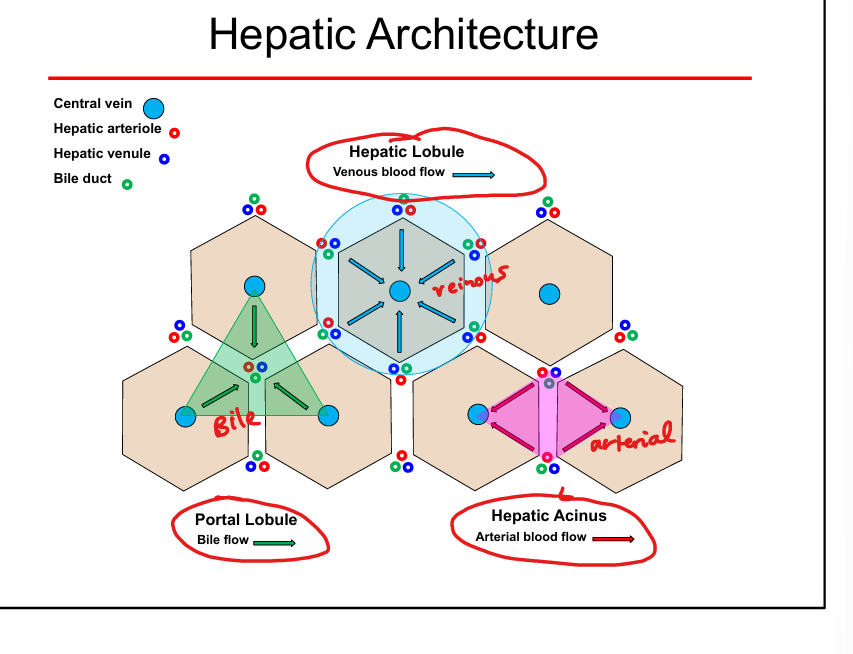
Hepatic lobule blood flow direction
From portal triad → sinusoids → central vein
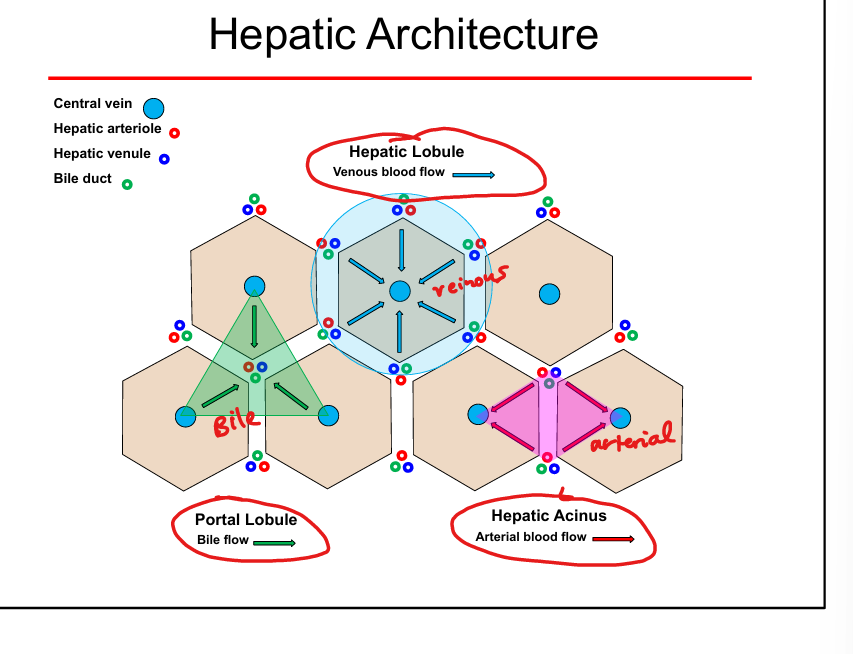

Bile flow direction
From hepatocytes → canaliculi → bile ducts (opposite blood flow)

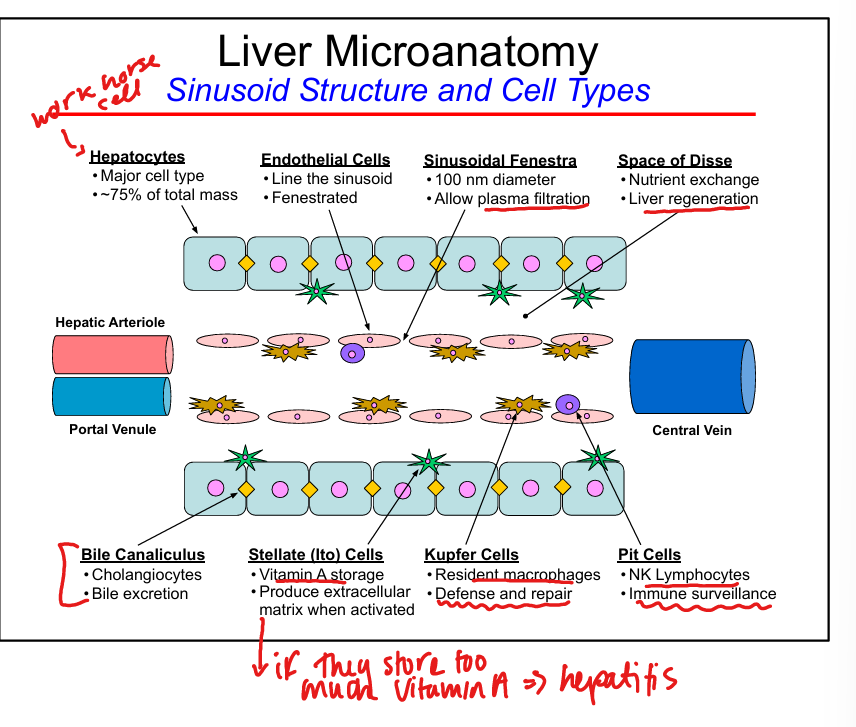
Hepatocyte functions
Protein synthesis, metabolism, detoxification, bile formation
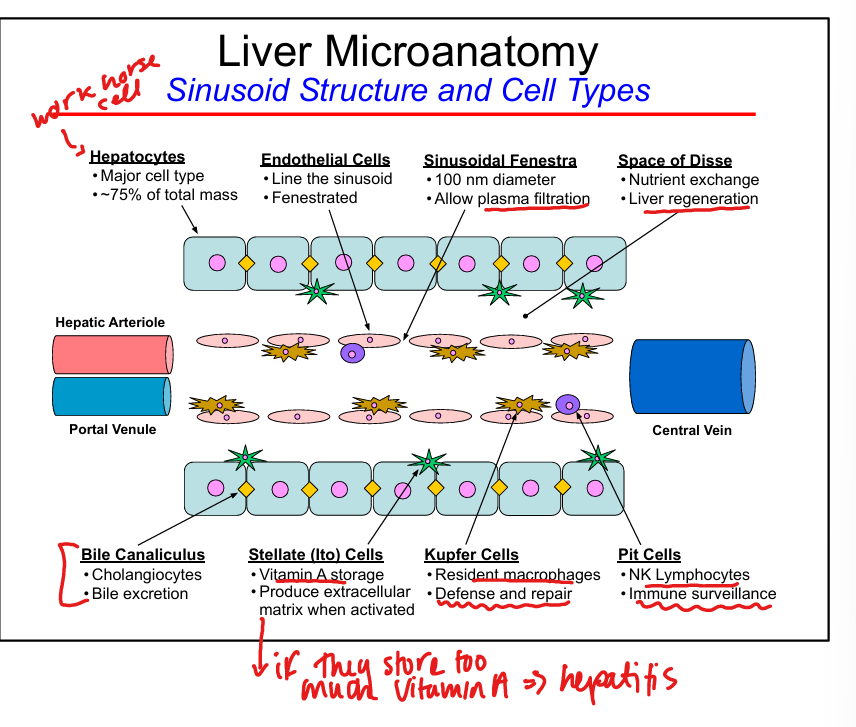

Endothelial cell features
Fenestrated, allow plasma filtration into Space of Disse
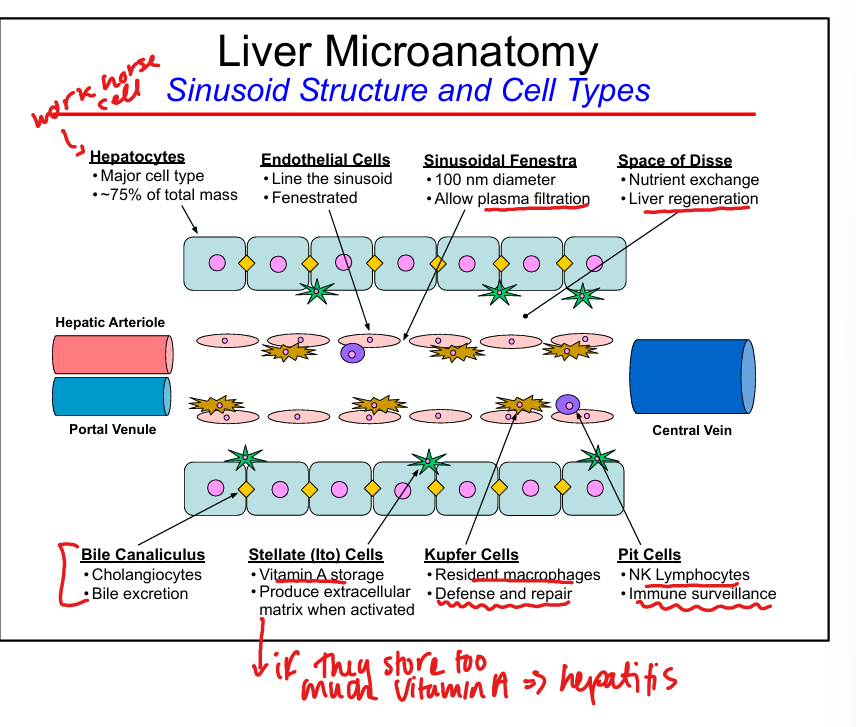

Kupffer cell function
Resident macrophages, phagocytosis, immune surveillance
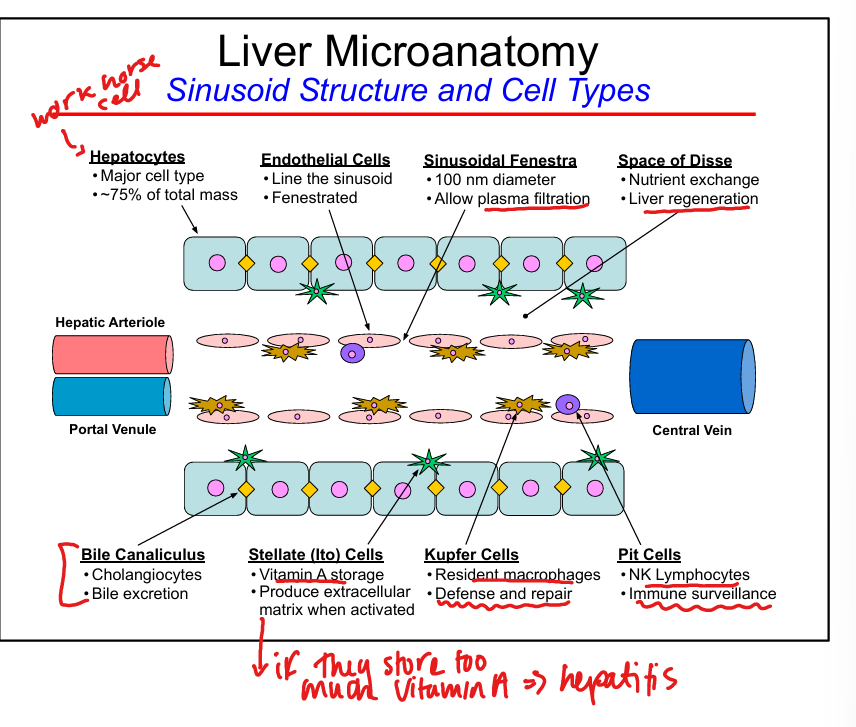

Stellate (Ito) cell function
Vitamin A storage
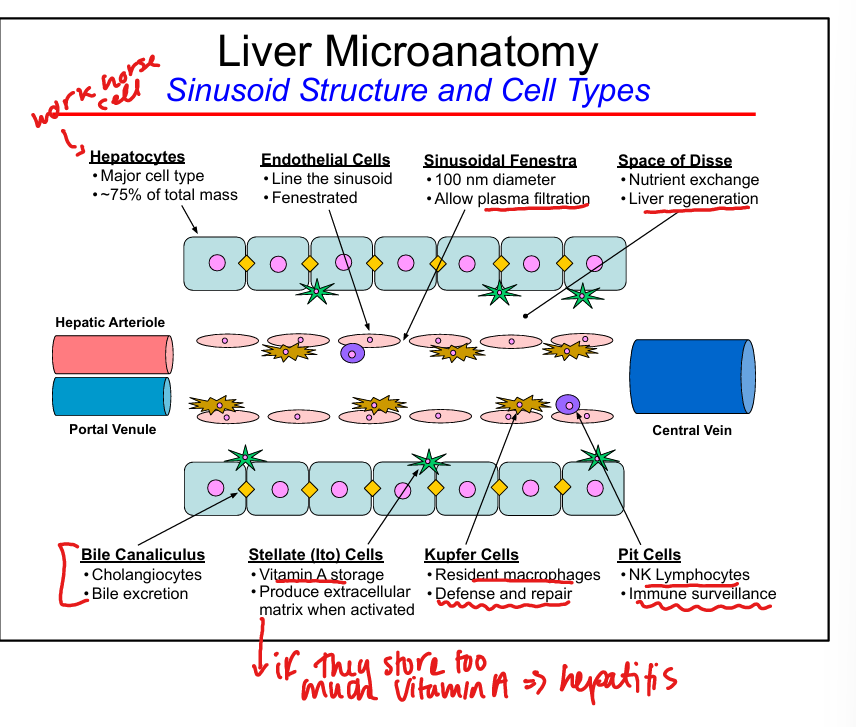

Pit cell function
NK lymphocytes for immune surveillance
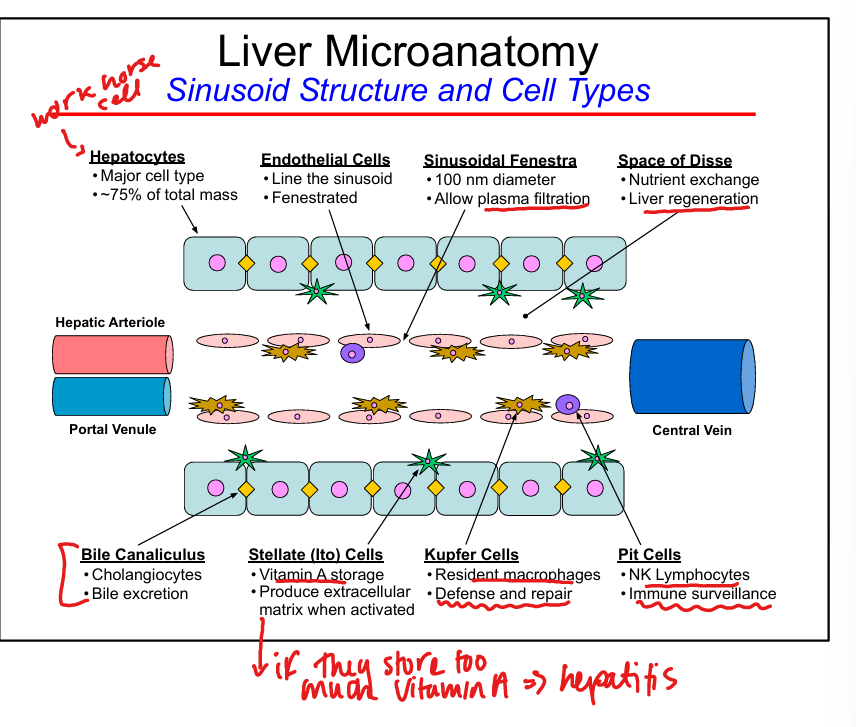

Space of Disse
Site of nutrient exchange between blood and hepatocytes, liver regeneration

Sinusoidal oxygen gradient
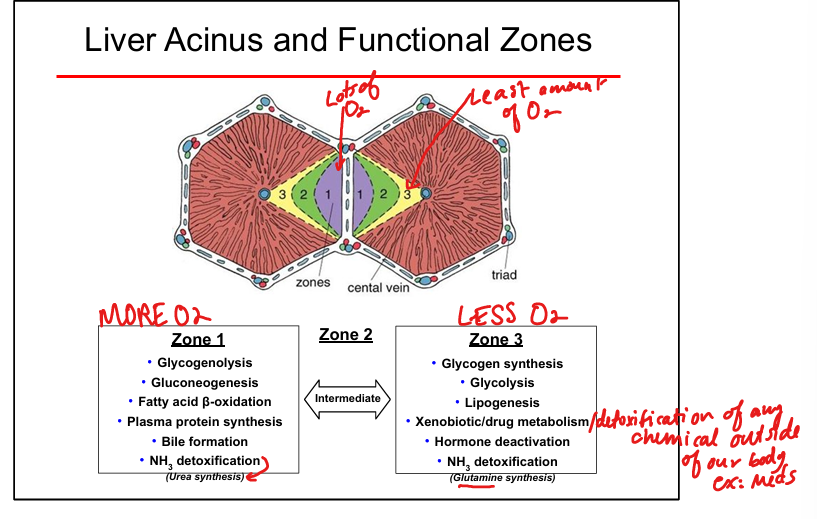
Highest O₂ in Zone 1, lowest in Zone 3
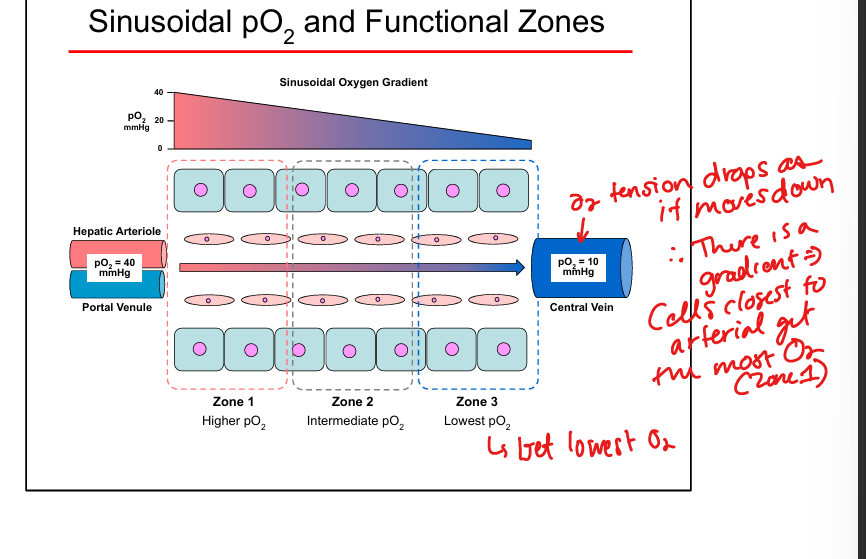

Zone 1 functions
Gluconeogenesis, glycogenolysis, fatty acid β-oxidation, urea cycle(NH3 detox), protein synthesis, bile formation
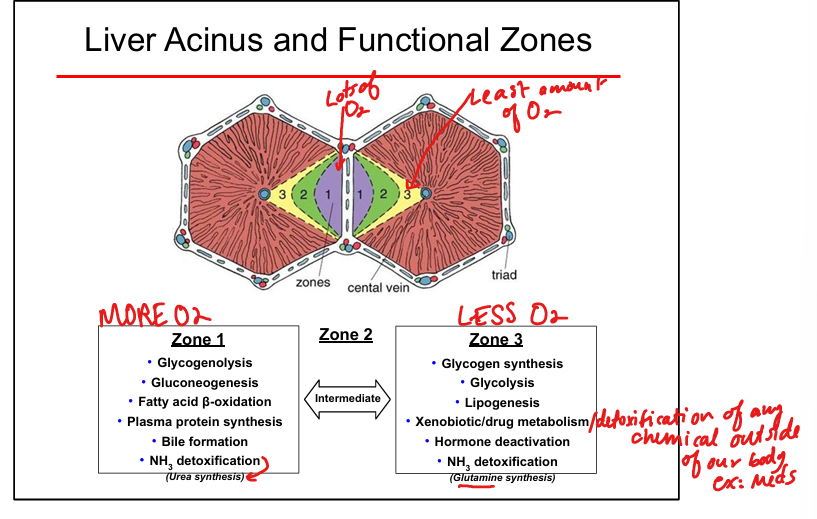

Zone 3 functions
Glycogen synthesis, Glycolysis, lipogenesis, drug metabolism (CYP450), glutamine synthesis, hormone deactivation

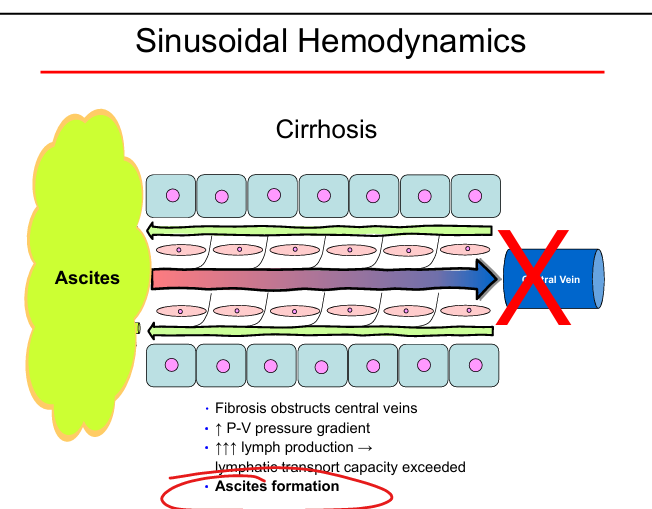
Portal hypertension mechanism
Fibrosis → ↑ portal–venous gradient → ↑ lymph → ascites
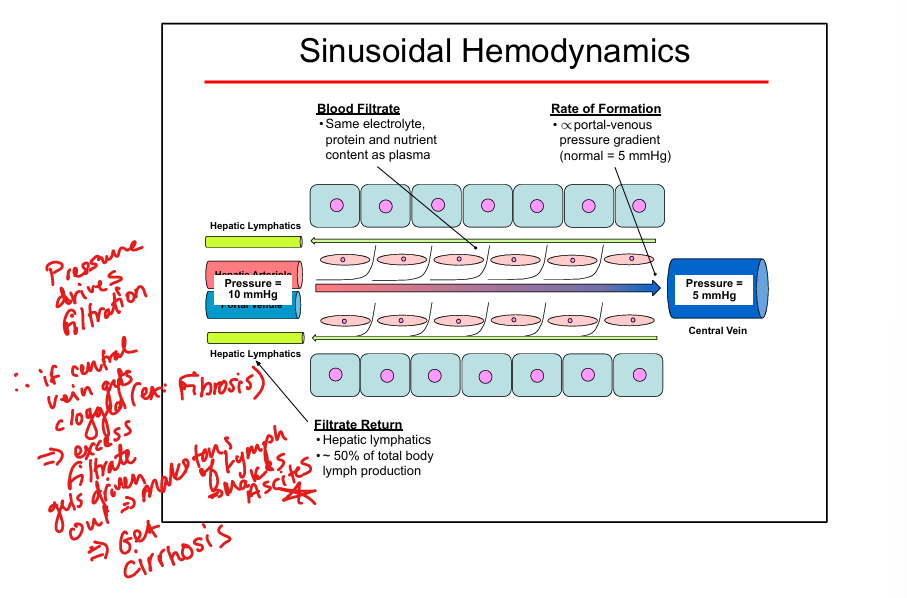
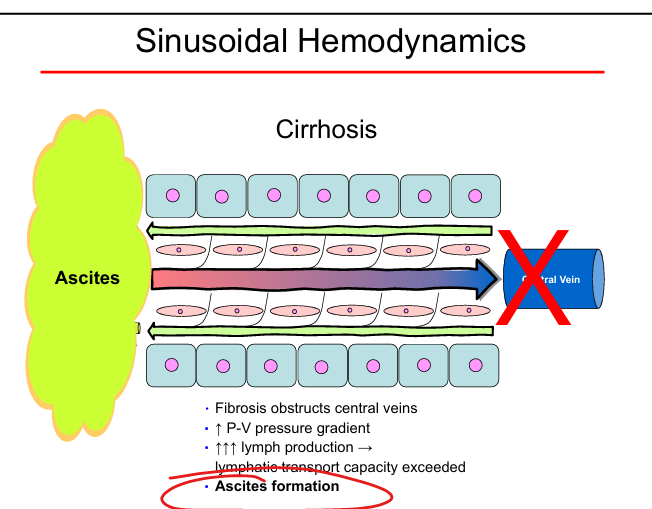

Ascites formation
Lymph production exceeds lymphatic drainage due to cirrhosis

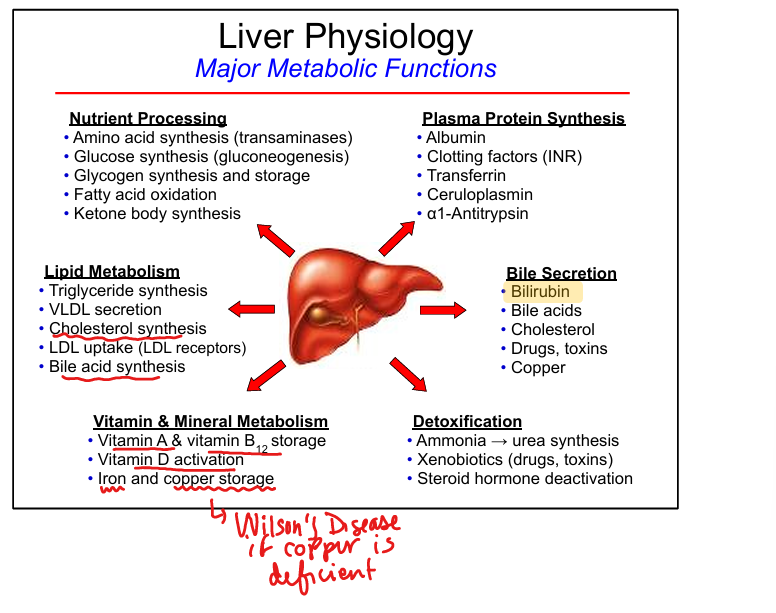
Vitamin storage in liver
Vitamins A, D, B12

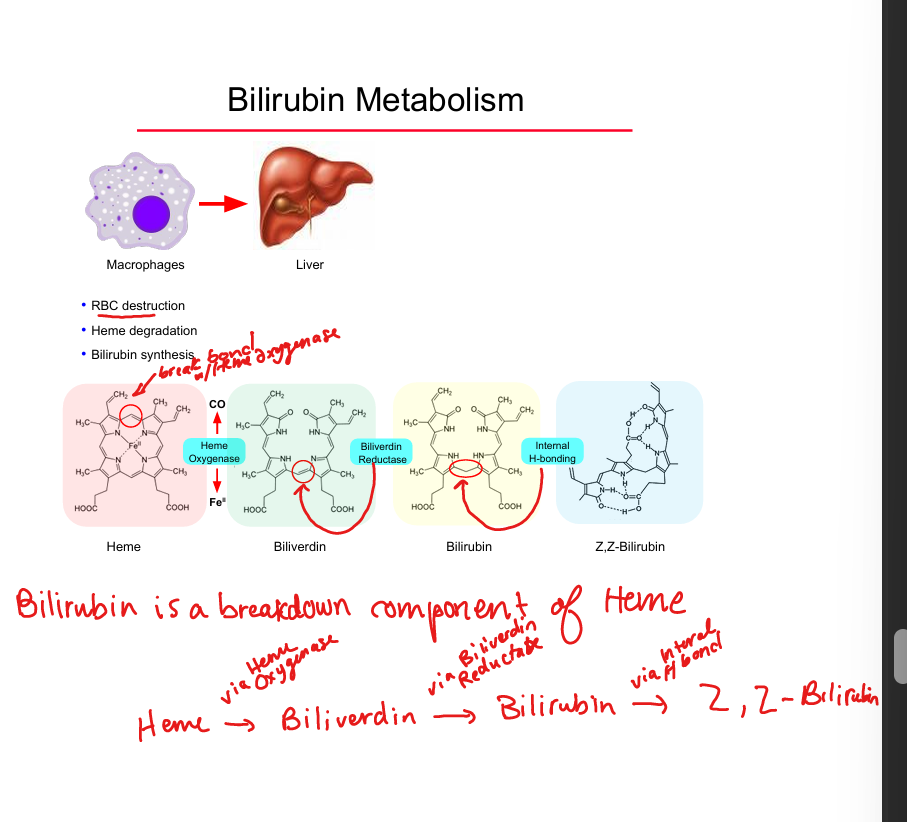
Bilirubin source
Breakdown of heme from senescent RBCs
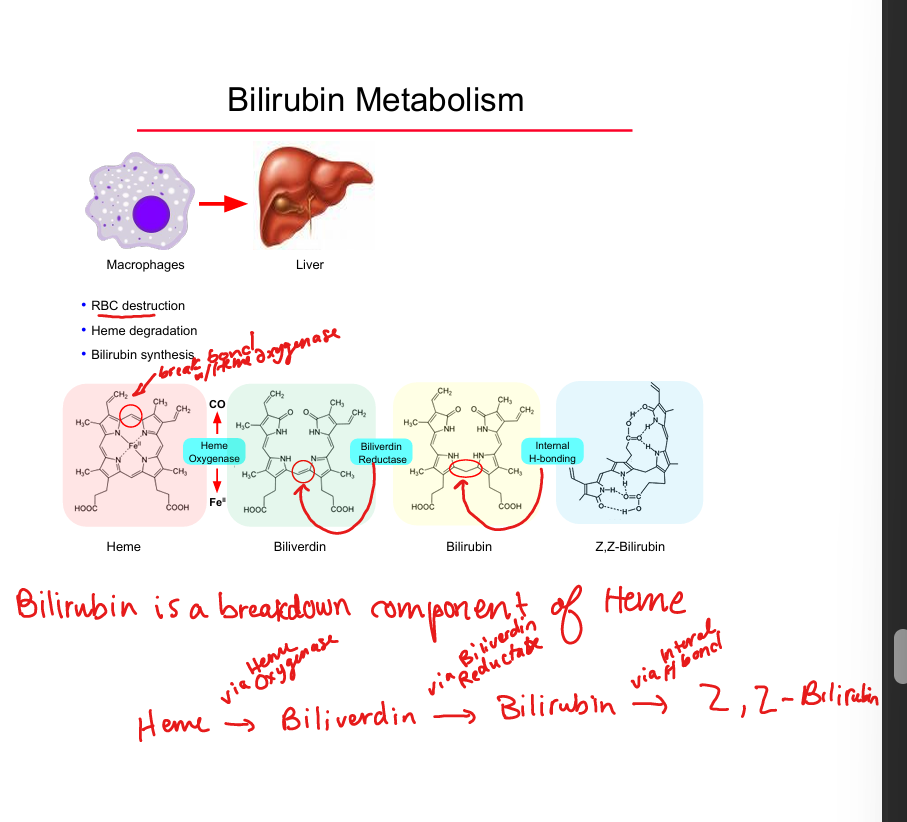

Heme → biliverdin enzyme
Heme oxygenase
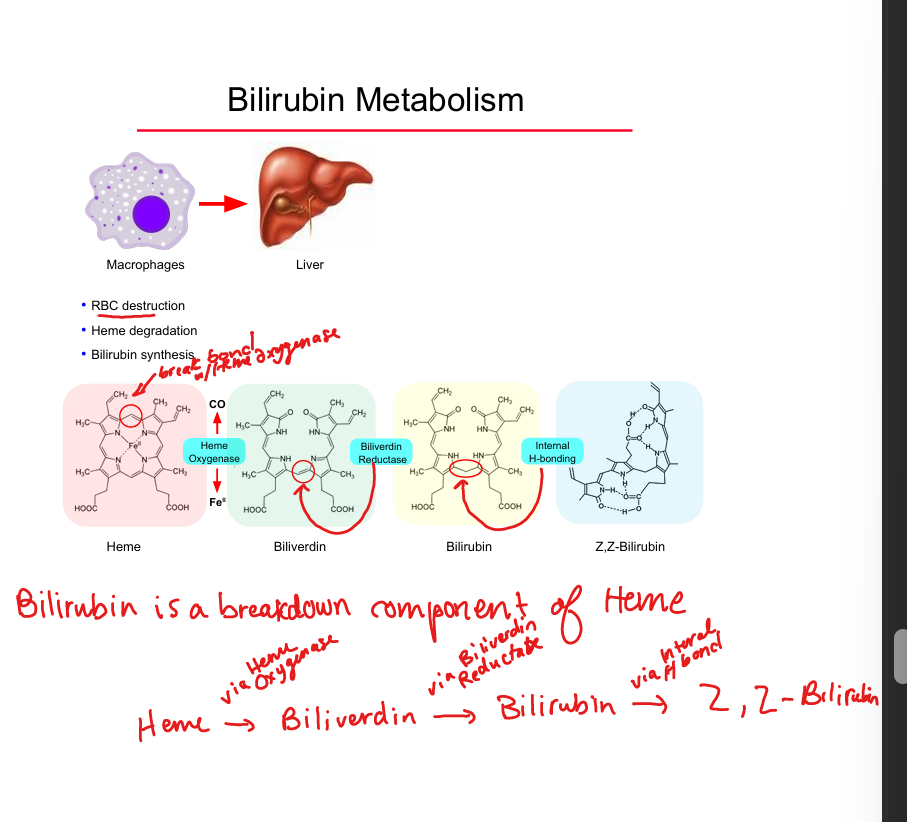

Biliverdin → bilirubin enzyme
Biliverdin reductase

Unconjugated bilirubin transport
Bound to albumin in plasma
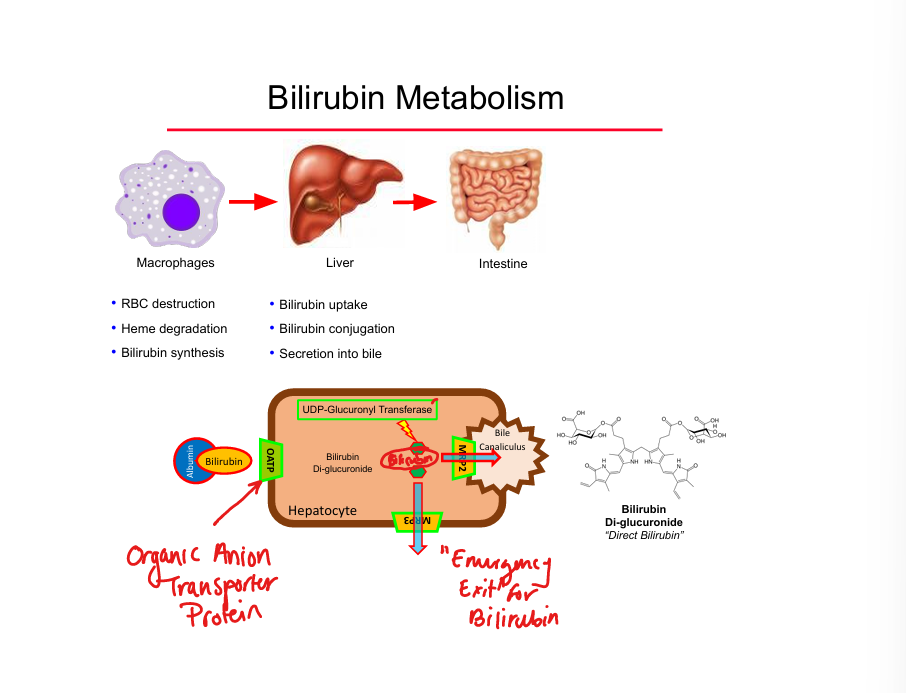

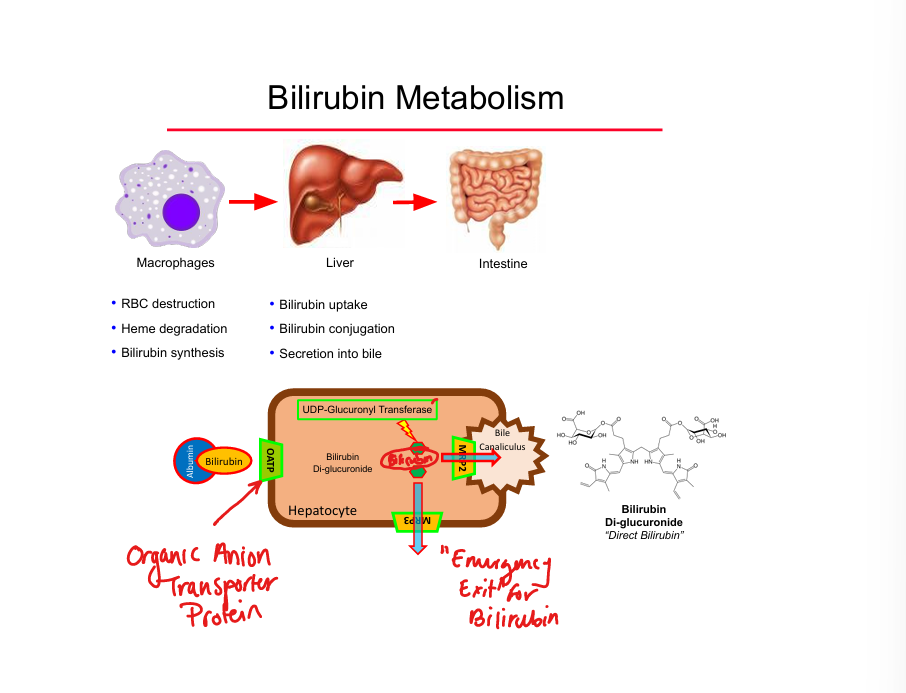
Bilirubin conjugation enzyme
UDP‑glucuronyl transferase (UDP‑GT)
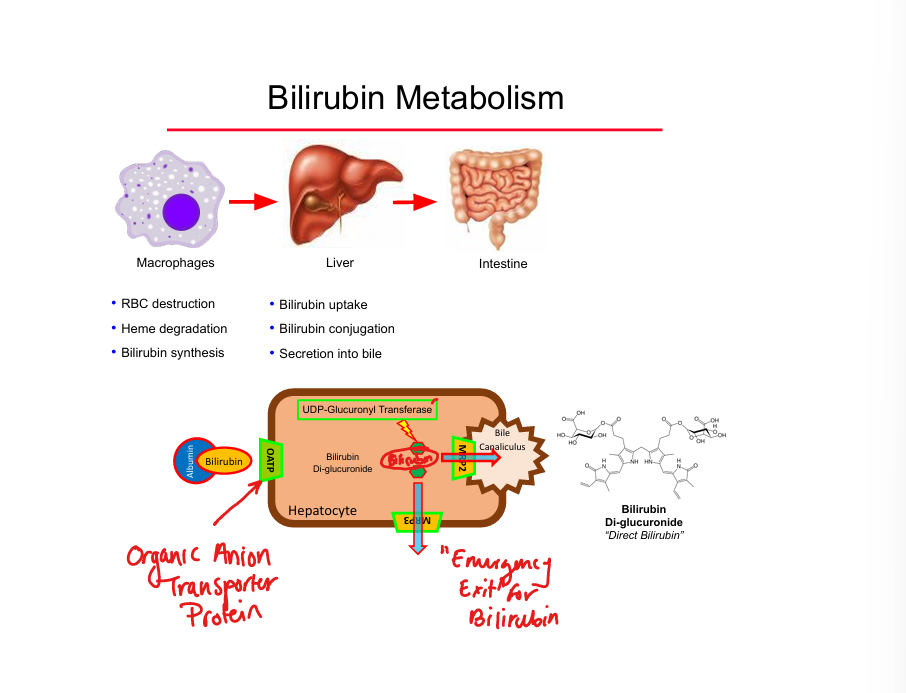

Conjugated bilirubin transporter into bile
MRP2
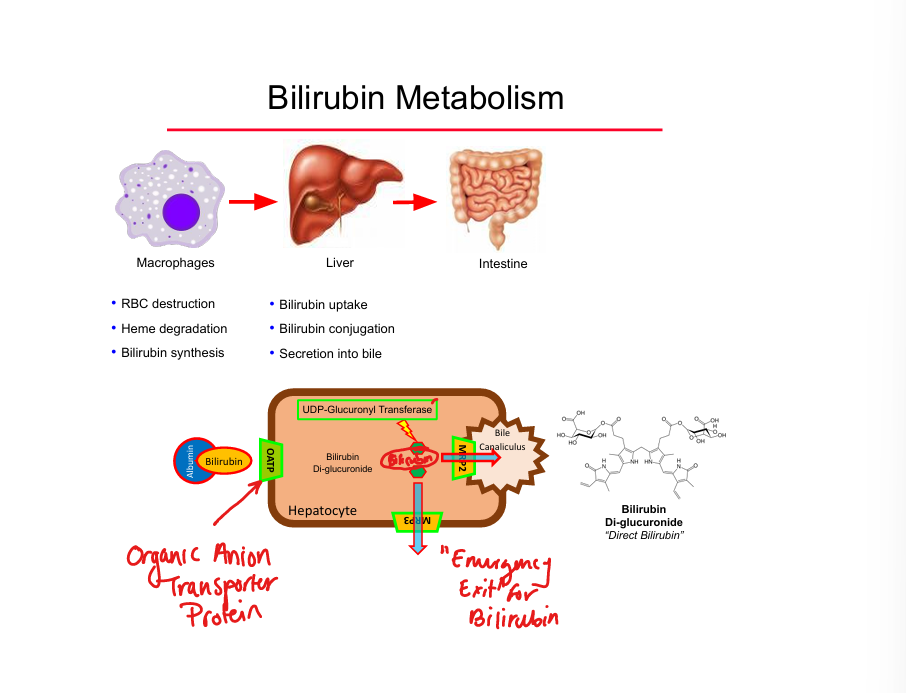

Emergency bilirubin efflux transporter
MRP3

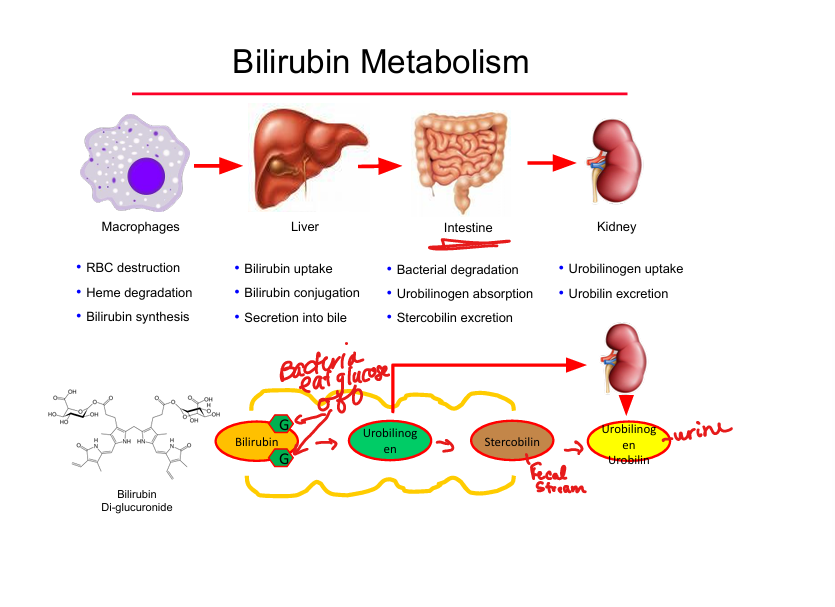
Bilirubin → urobilinogen location
Intestinal bacterial metabolism of glucose on the bilirubin
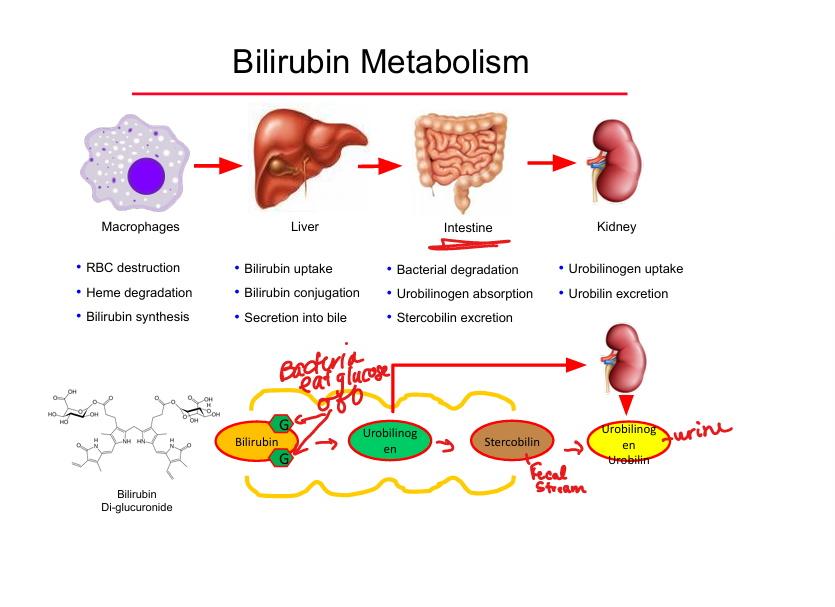

Urobilinogen fates
Reabsorbed → urine (urobilin) OR feces (stercobilin)

Unconjugated hyperbilirubinemia causes
Hemolysis, Gilbert syndrome, Crigler‑Najjar, neonatal jaundice


Conjugated hyperbilirubinemia causes
Dubin‑Johnson, Rotor, cholestasis


Mixed hyperbilirubinemia causes
Hepatocellular injury, bile duct obstruction


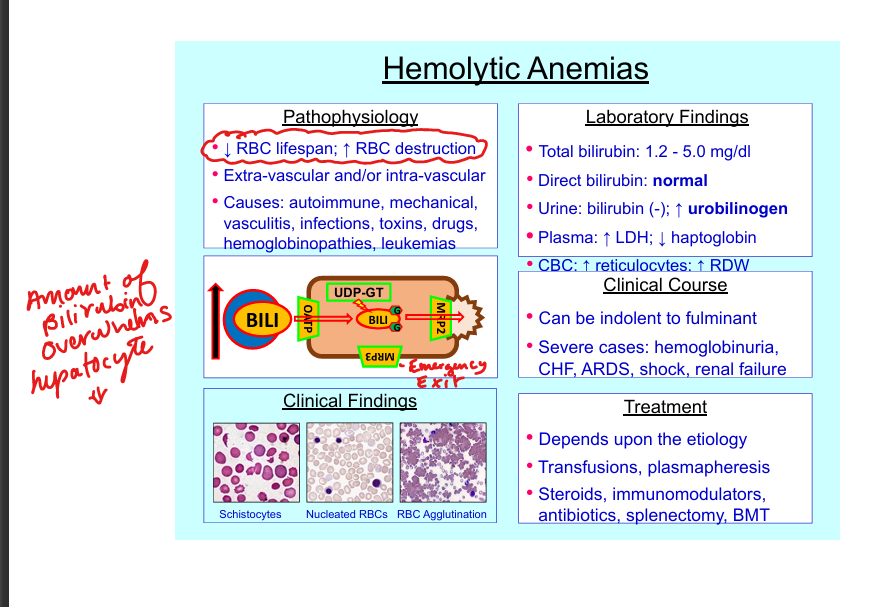
Hemolytic anemia bilirubin pattern + cause
↑ total bili, normal direct, ↑ urobilinogen, no urine bilirubin; all caused by a decreased RBC lifespan and inc RBC destruction

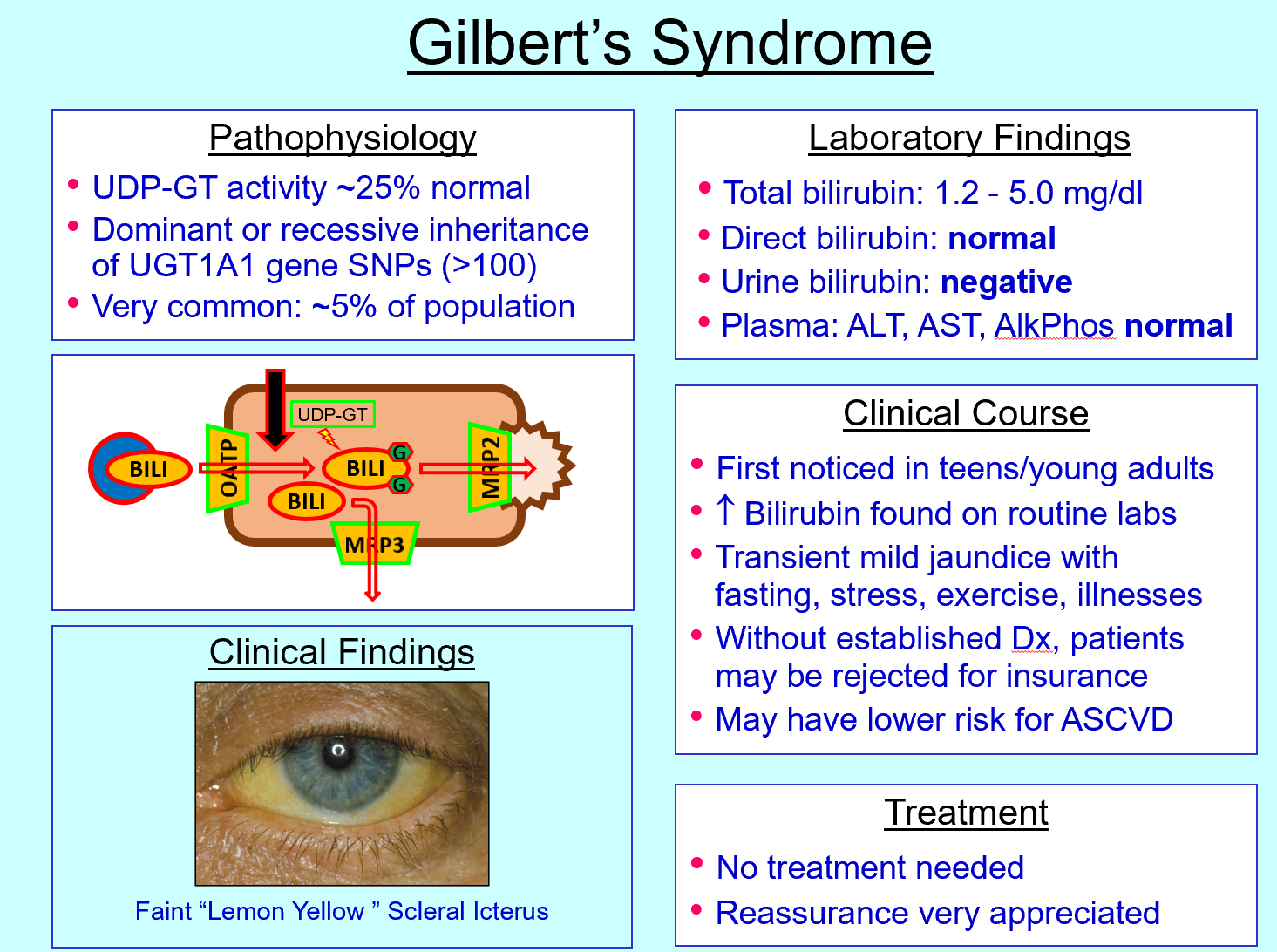
Gilbert syndrome defect
↓ UDP‑GT activity (~25% normal)
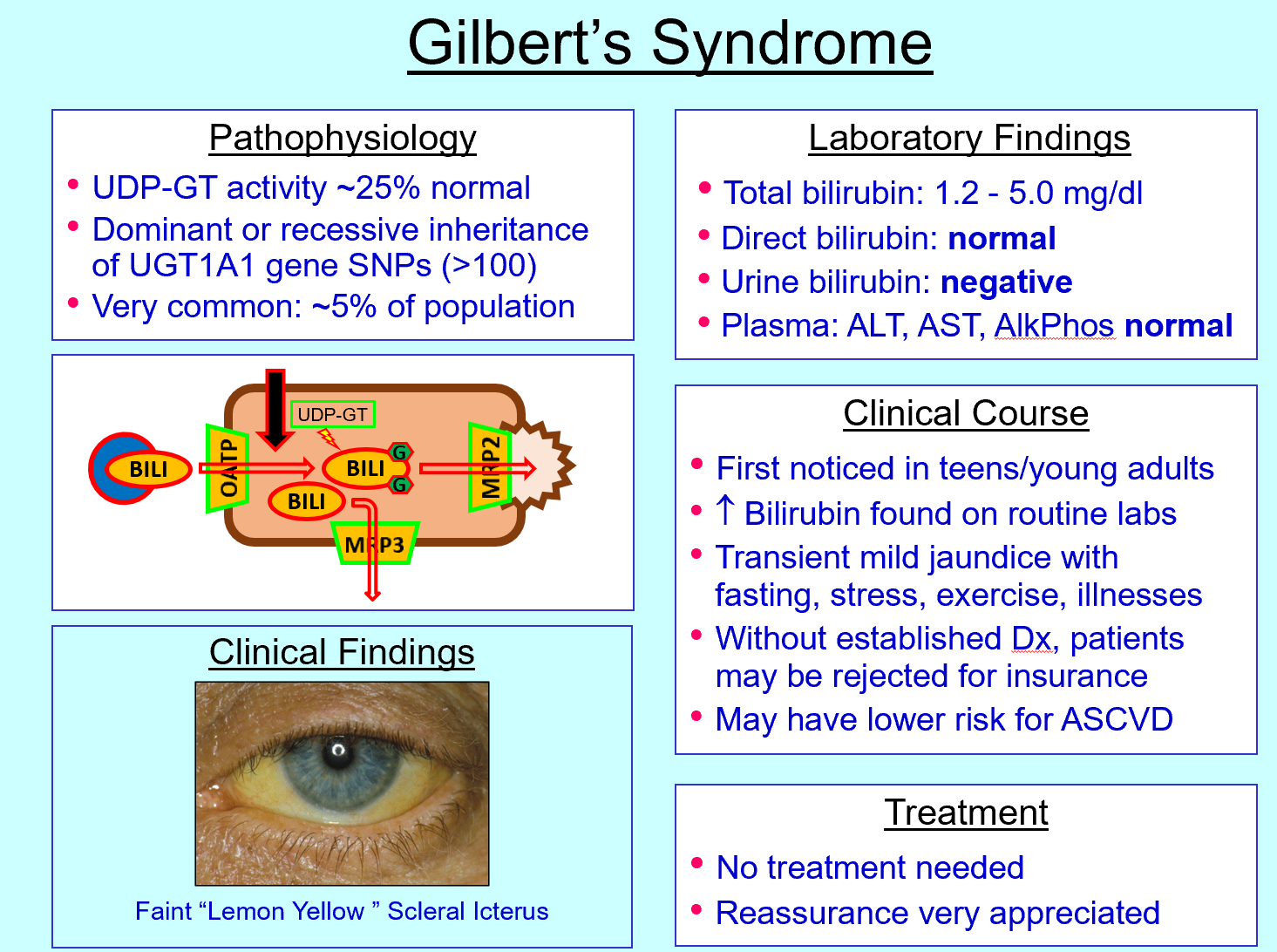

Gilbert syndrome features
Mild jaundice during stress/fasting

Crigler‑Najjar type I defect
Absent UDP‑GT
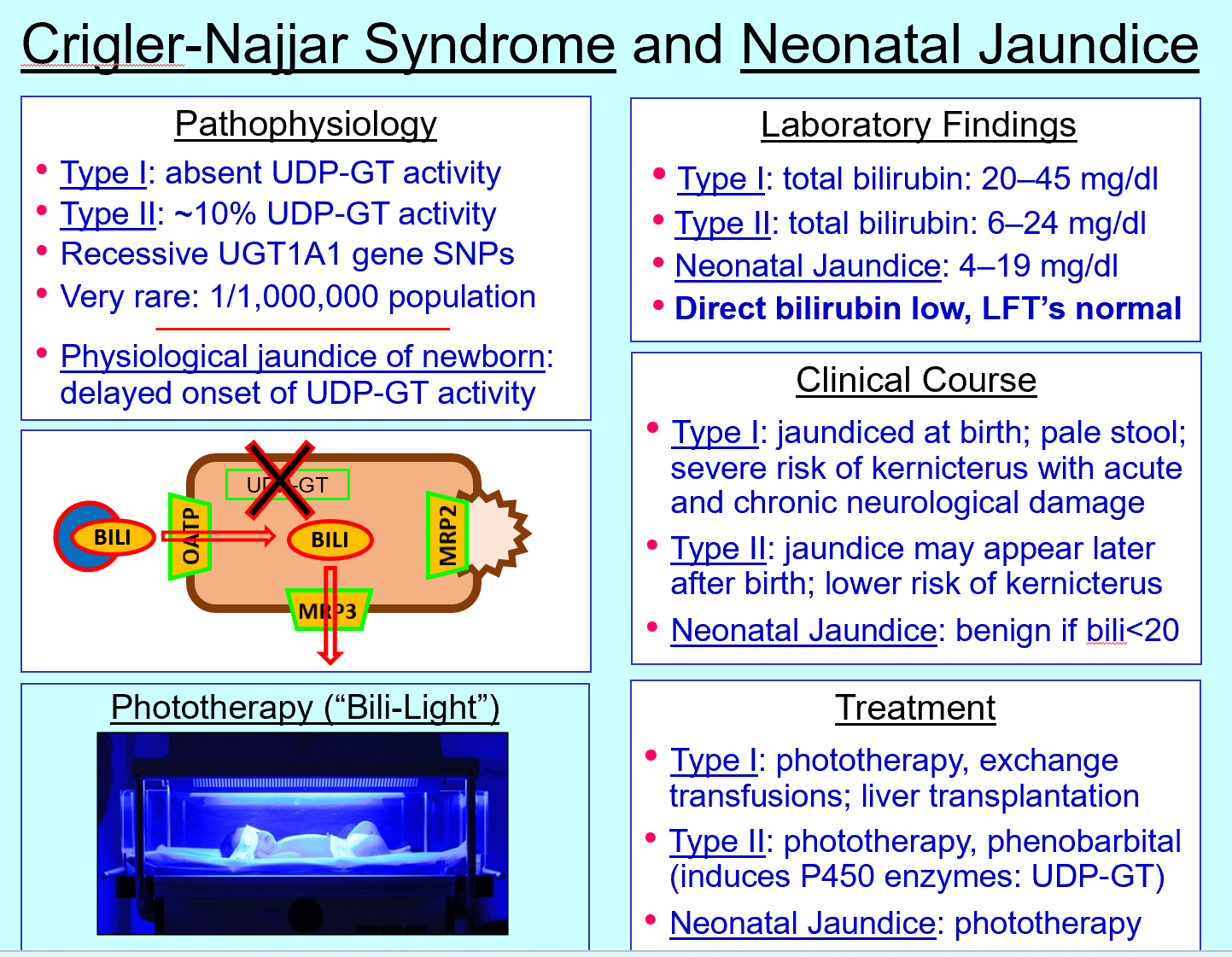

Crigler‑Najjar type I features
Severe unconjugated hyperbilirubinemia, kernicterus risk
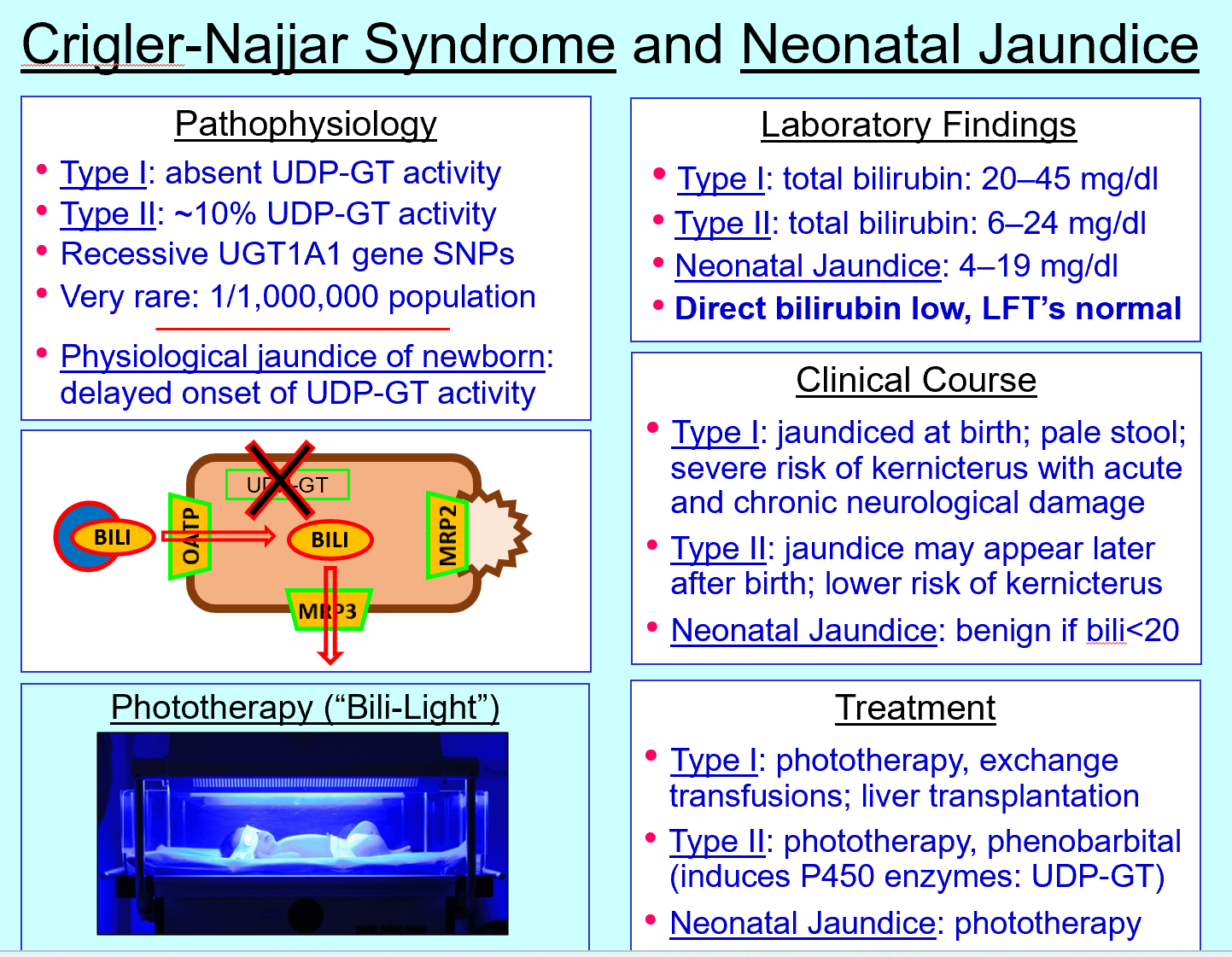

Crigler‑Najjar type II defect
~10% UDP‑GT activity
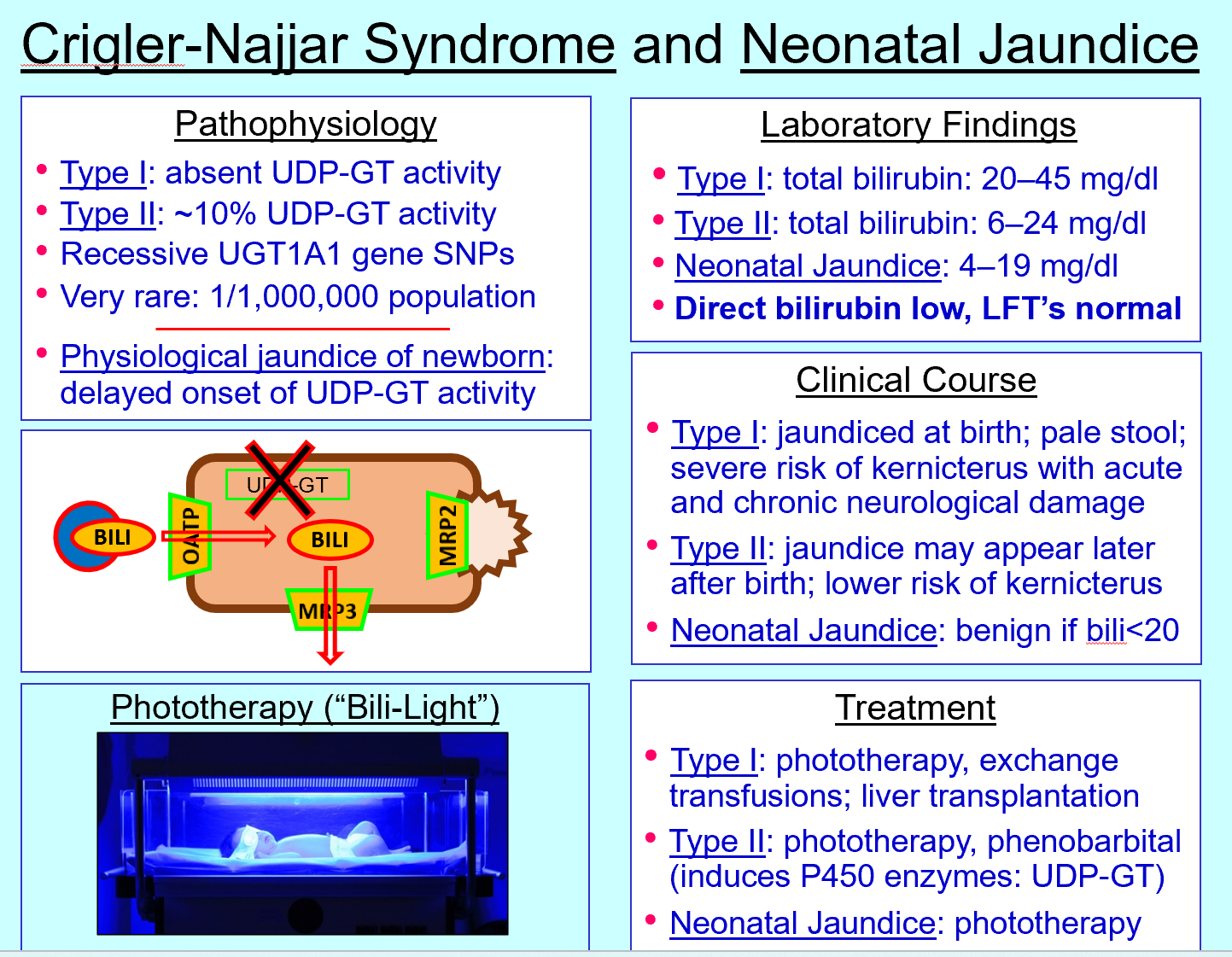

Crigler‑Najjar type II treatment
Phenobarbital (induces UDP‑GT) + phototherapy
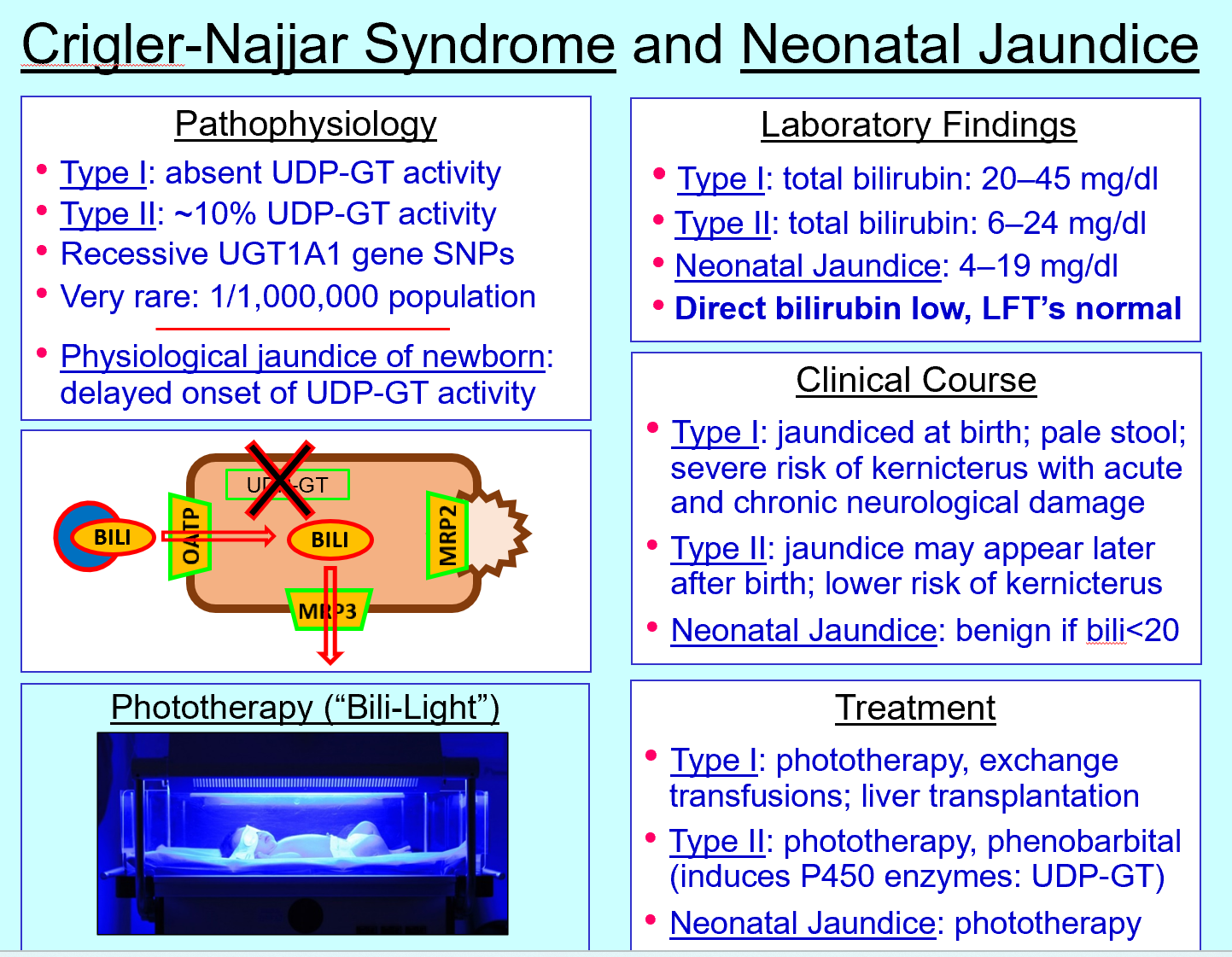

Neonatal jaundice cause
Delayed UDP‑GT activity
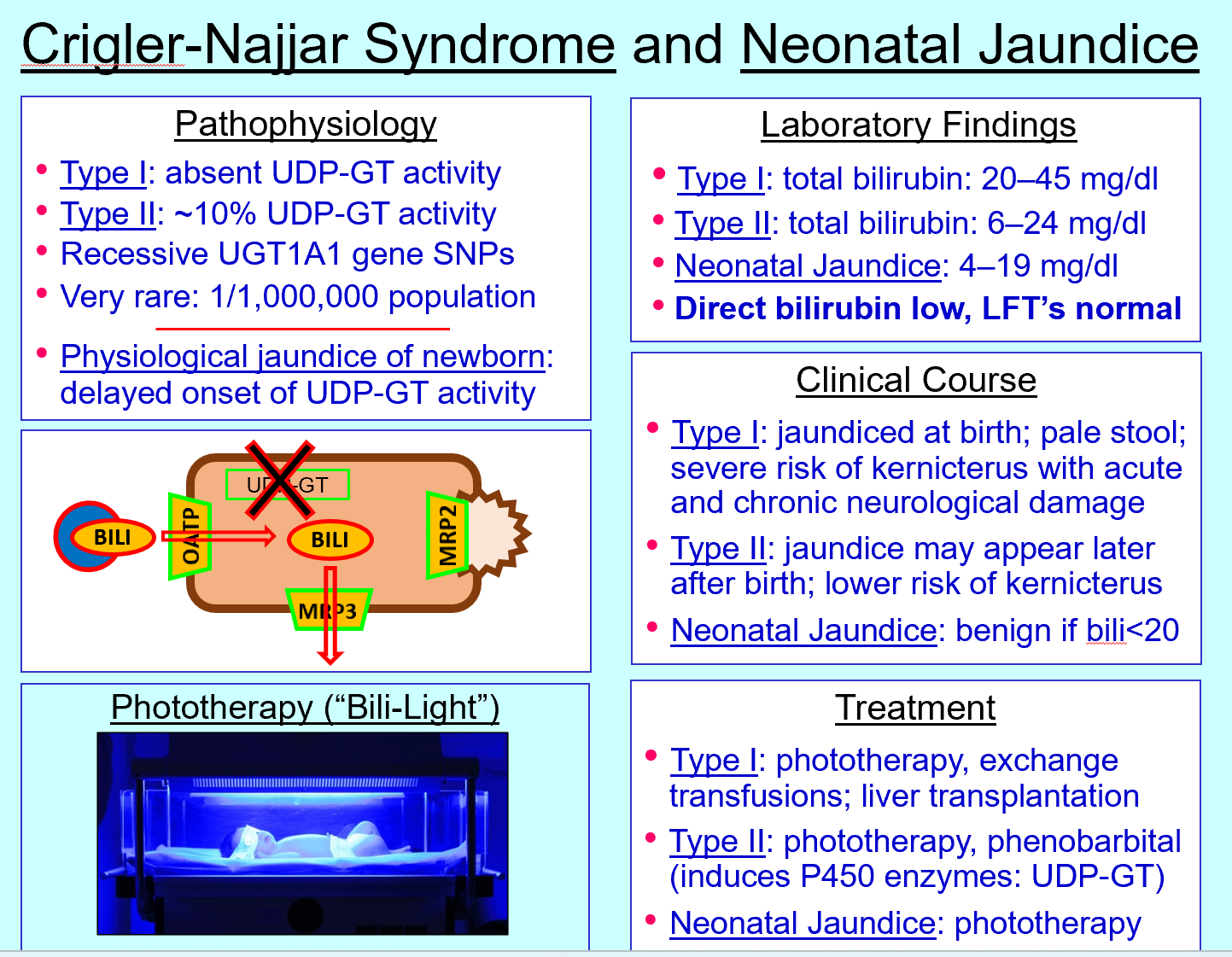

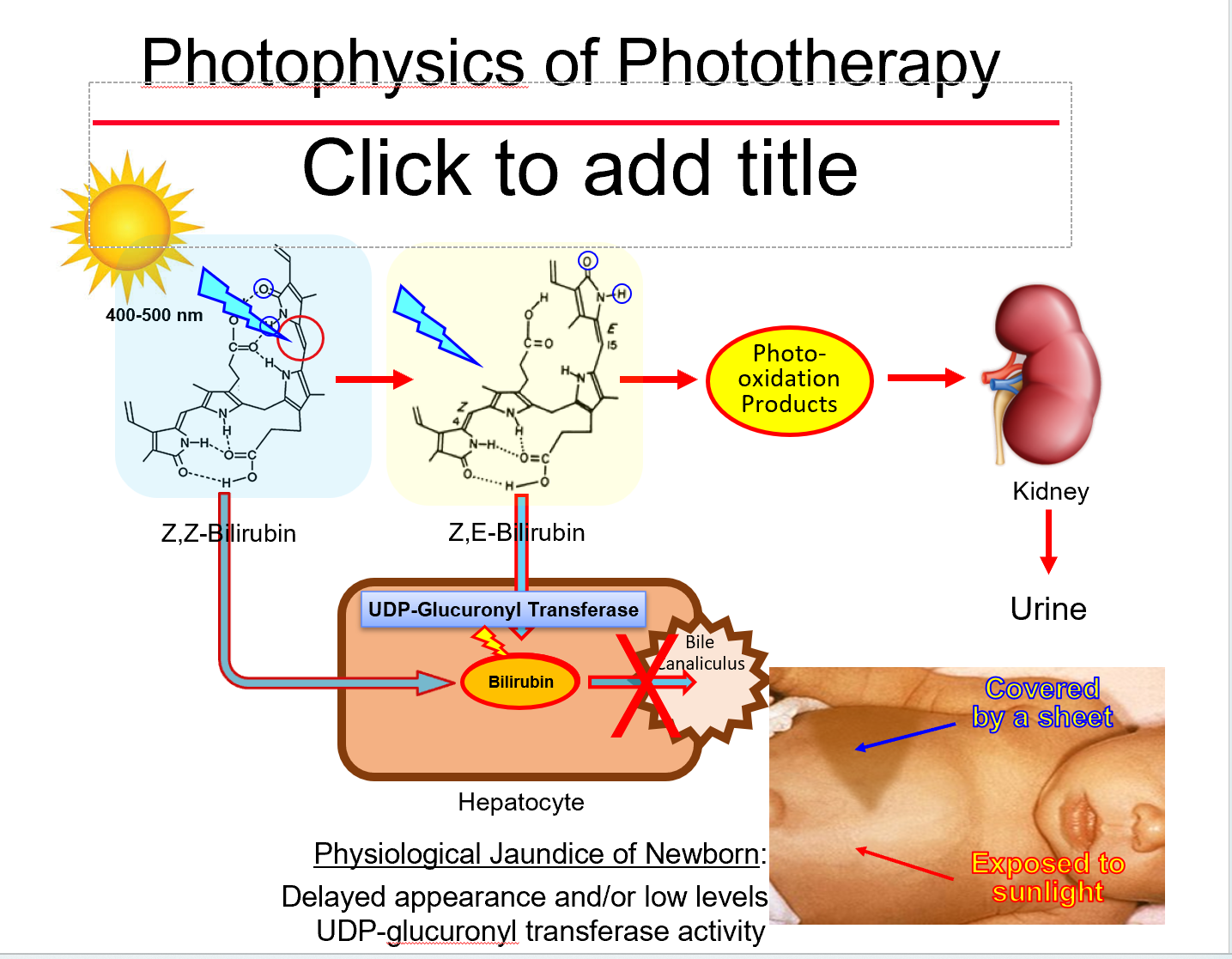
Phototherapy mechanism
Converts bilirubin to water‑soluble isomers excreted without conjugation

Dubin‑Johnson syndrome defect
MRP2 transporter deficiency
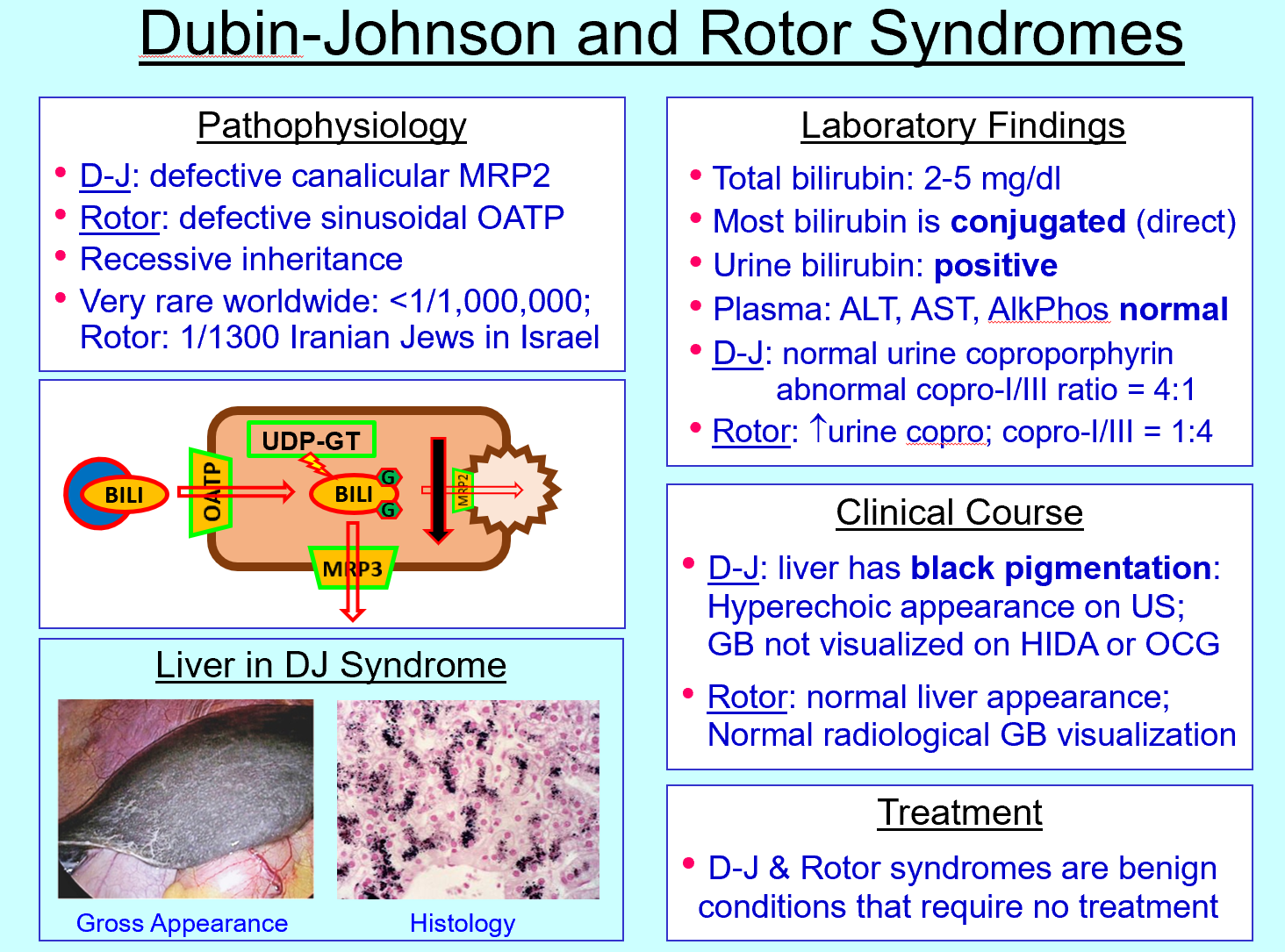

Dubin‑Johnson features
Conjugated hyperbilirubinemia, black liver, benign
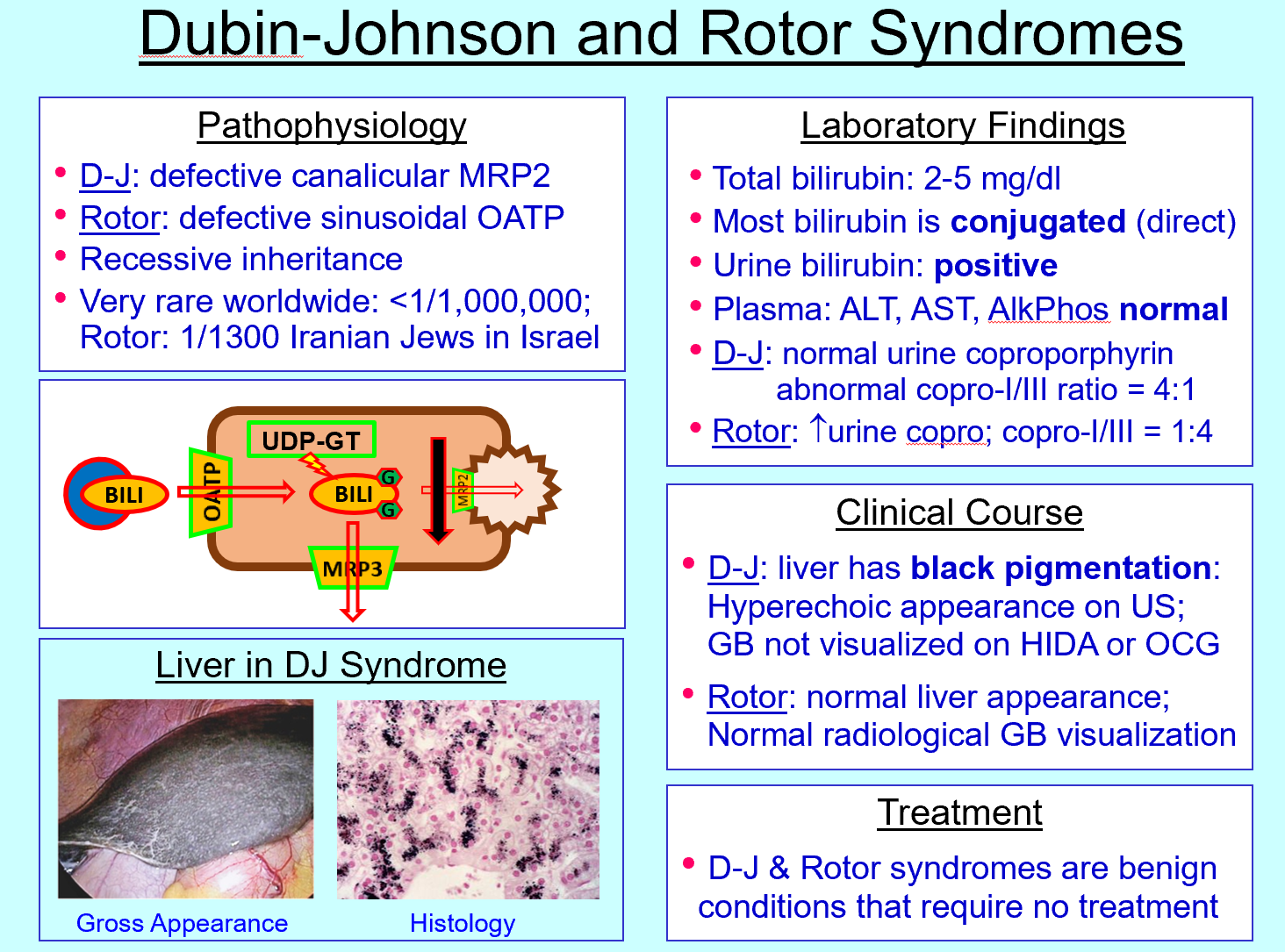

Rotor syndrome defect
OATP transporter defect (sinusoidal uptake)
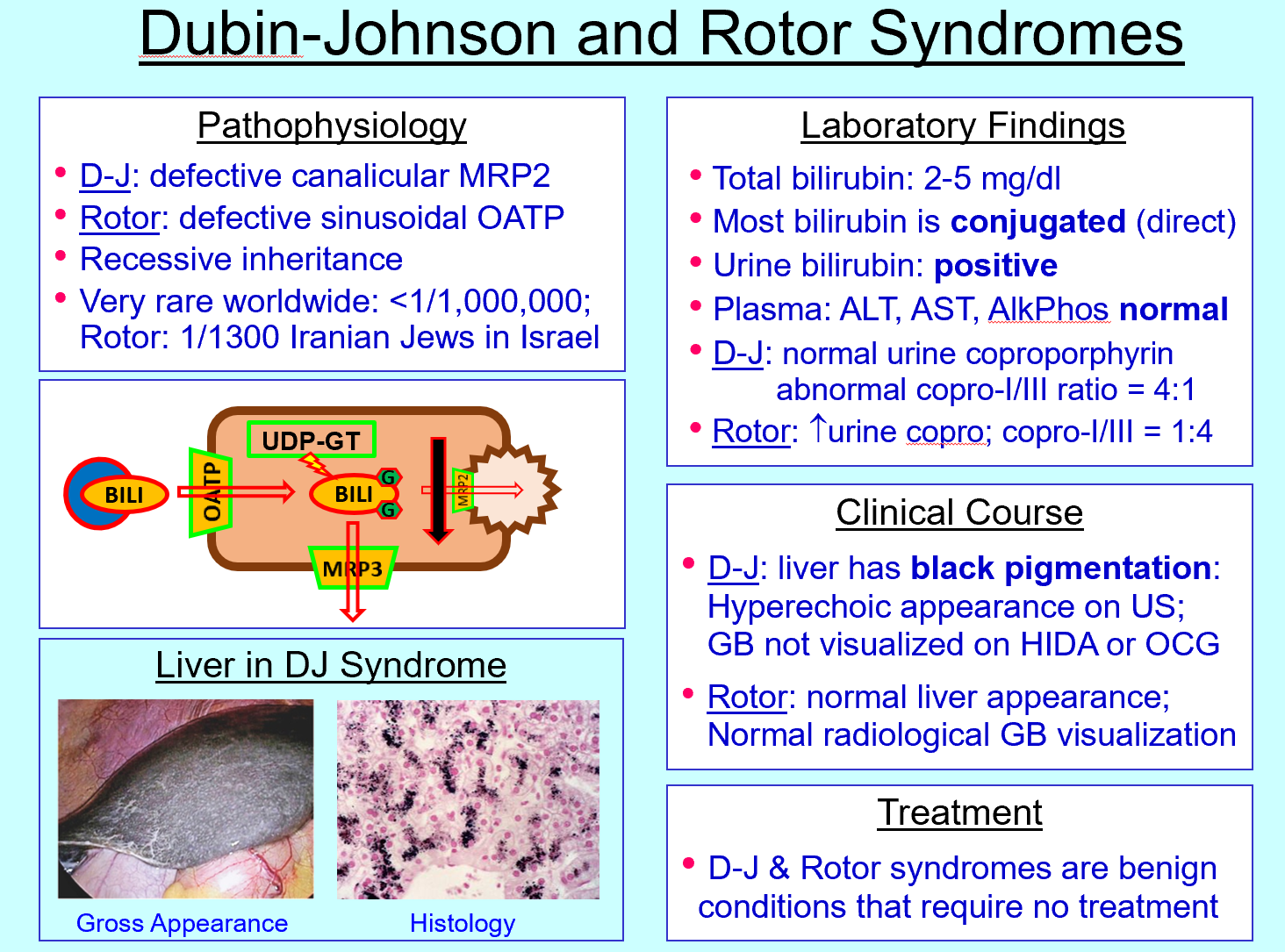

Rotor syndrome features
Bilirubin has difficulty getting into and stored in liver cell via OATP “door” defect» will travel to blood stream »Conjugated hyperbilirubinemia, normal liver pigmentation
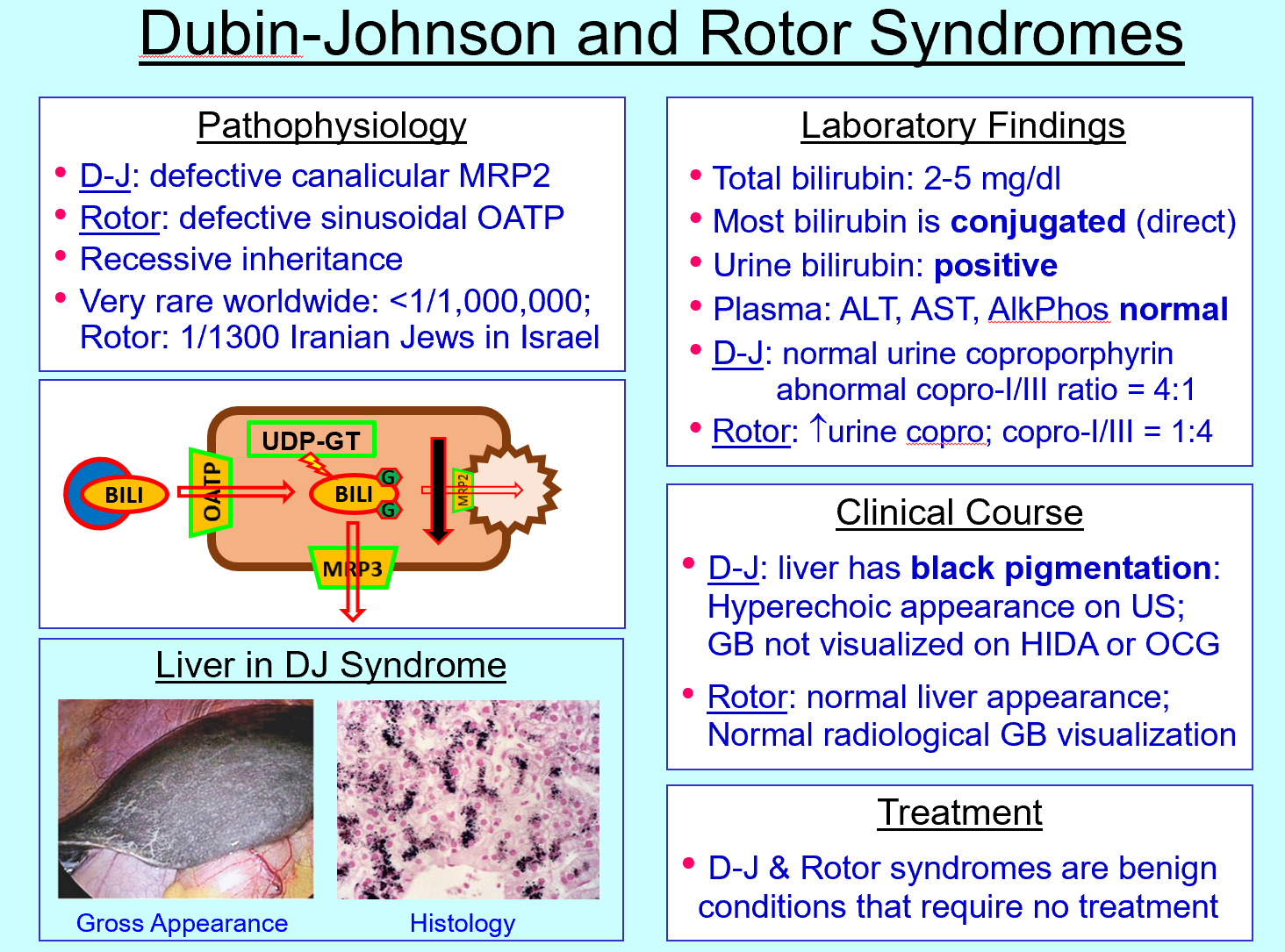

Urine bilirubin significance
Indicates conjugated bilirubin (water‑soluble)
Urine urobilinogen significance
Elevated in hemolysis
Cholestasis bilirubin pattern
↑ direct bilirubin, pale stools, dark urine
Portal vein function
Delivers nutrient‑rich blood from GI tract to liver