BMS 251 - Exam #3
1/138
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
139 Terms
Functions of respiratory system
Respiration (Oxygen and CO2 exchange between atmosphere and body cells)
Ventilation (Breathing)
Pulmonary Gas Exchange (External Respiration)
Tissue Gas Exchange (Internal Respiration)
Cellular Respiration
General functions of respiratory system
Air passageway
Site of exchange O2 and CO2
Detection of odors
Sound production
Structural organization of RS
Upper and lower respiratory tracts
Functional organization of RS
Conducting and respiratory zone
Structure of mucosa membrane
Respiratory tract: Psuedostratified ciliated columnar epithelium
Traps foreign particles (mucus) and removes trapped particles out of respiratory tract (cilia)
From nasal cavity to alveoli, epithelium gets thinner
Regions of the nasal cavity
Olfactory region
Respiratory region
Nasal vestibule
Olfactory region
Detects odors
Olfactory epithelium is in mucus membrane
Contains olfactory receptors to detect odors
Respiratory region
Conditions incoming air
Conchae: produce turbulence in inhaled air to increase contact of air with mucosa (warm, cleanse, humidify)
Nasal vestibule
Traps large particulates
Vibrissae: course hair that serve to trap inhaled pathogens & debris
Function of pharynx
Passageway for air and food
Mucosa and tonsils protect from ingested substances
Eustachian tubes equalize pressure on either side of tympanic membranes
Three regions of pharynx
Nasopharynx: Respiratory only, leads to auditory tubes, pharyngeal tonsils, psuedostratified ciliated columnar epithelium
Oropharynx: Respiratory and digestive, lingual and palatine tonsils, nonkenatinized stratified squamous epithelium
Laryngopharynx: Respiratory and digestive, nonkenatinized stratified squamous epithelium
Structure and function of larynx
Inferior to pharynx, superior to trachea
Passageway for air, prevent aspiration of ingested material, speech, sneeze/cough reflex, valsalva manuever
How does the larynx contribute to sound production?
Exhaled air vibrates the vocal folds
Structure and function of the trachea
Windpipe
Inferior to larynx, anterior to espohagus
Carries oxygen
Has cartilage rings
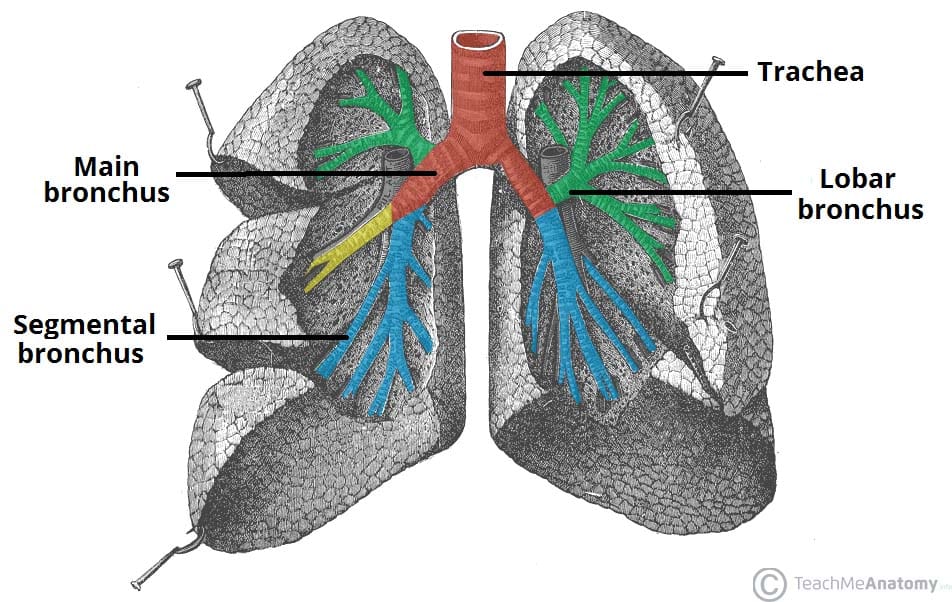
Structural subdivisions of bronchial tree
Main bronchi
Lobar bronchi
Segmental bronchi
Smaller bronchi
Location and function of smooth muscle in bronchial tree
Transitions to smooth muscle in bronchioles
To allow for bronchocontriction and bronchodilation
Bronchoconstriction
Limits airflow in bronchial tree
Limits entry of harmful substances
Bronchodilation
Maximizes airflow in bronchial tree
Maximizes O2 delivery and CO2 removal
Sympathetic NS
Terminal bronchiole
Epithelium and smooth muscle
Marks the transition from conducting zone into respiratory zone
Respiratory bronchiole
Thin walls, sparse alveoli, smooth muscle
Transport air and begin gas exchange
Alveolar ducts
Thin walls, smooth muscle
Pathway to alveolar sacs
Alveoli
Simple squamous epithelium surrounded by capillaries
Primary site of gas exchange
Alveolar Type I cells
Facilitate rapid diffusion of gases
Alveolar Type II cells
Provide surfactant to reduce surface tension and prevent collapse
How do alveoli provide surface area for pulmonary capillaries?
Act as microscopic balloon-like sacs to create a highly-vascularized network
Structure and function of respiratory membrane
Alveolar-capillary membrane
Function is pulmonary gas exchange (oxygen and CO2 exchange)
Pleural membrane
Two thin membranes (visceral (inside) and parietal (outside)) that enclose the lungs and line the chest cavity to create a fluid-filled space for breathing
Pleural cavity
Fluid-filled space between parietal and visceral membranes
How does pleural membrane keep lungs inflated?
Creating a low-pressure cavity to create a suction membrane. Elastic recoil allows stretch and inward pull
Bronchopulmonary segments of lungs
Functional units of the lungs
Encapsulated in connective tissue supplied by own segmental bronchus, branch of pulmonary artery & vein.
Respiration
The movement of respiratory gases between atmosphere and systemic cells of the body (pulmonary ventilation, pulmonary gas exchange, gas transport, tissue gas exchange)
Pulmonary ventilation
Movement of gases between atmosphere & alveoli
Pulmonary gas exchange
Exchange of gases between alveoli & the blood in pulmonary capillaries
Gas transport
Transport of gases in the blood to the systemic cells of the body
Tissue as exchange
Exchange of gases between blood in systemic capillaries and systemic cells of the body
Ventilation
Moving air in and out of the lungs to facilitate gas exchange
Physiological process of pulmonary ventilation
Inspiration and expiration driven by pressure differences
Quiet breathing
Rhythmic breathing at rest
Forced breathing
Vigorous breathing during exercise
Four steps of pulmonary ventilation
1. Autonomic nuclei in brainstem control skeletal muscles of breathing
2. Muscles of breathing contract/relax to change volume of thoracic cavity
3. Volume changes in thoracic cavity establish pressure gradient between lungs & atmosphere
4. Air moves down the pressure gradient
How are pressure gradients established by skeletal muscles?
By changing the pressure in the thoracic cavity
Inspiration expands thoracic cavity
Expiration shrinks thoracic cavity
Boyle’s Law
Inverse relationship between pressure and volume
If volume increases, pressure decreases
If volume decreases, pressure increases
Nervous system structures involved in breathing
Medullary respiratory center (ventral and dorsal)
Pontine respiratory center
Physiological events of quiet breathing
Sensors (chemoreceptors, central and peripheral)
Respiratory center
Respiratory muscles
How is pulmonary ventilation controlled by CNS?
Chemoreceptors send signals to ventral respiratory center to control rate and depth of breathing
What is the difference between central and peripheral chemoreceptors?
Central detects CO2 in CSF
Peripheral receptors detect low O2 and pH
Other reflexes that alter breathing rate and depth
Mechanoreceptors (detect stretch in lungs, prevent over-inflation, receptors send signals to respiratory center to stop inhalation)
Proprioceptors (stimulated by skeletal muscle movement, more movement = greater breathing depth)
Irritant receptors (stimulated by pain/inhaled particles, causes sneezing/coughing)
Airflow
The amount of air that moves into and out of the respiratory tract with one breath
How do pressure gradients and resistance determine airflow?
The difference in interpulmonary pressure and atmospheric pressure and resistance from elasticity of lungs control airflow
Partial pressure
The amount of pressure each gas contributes to the total pressure
within a mixture of gases
How do total pressure and % of gas impact partial pressure?
If total gas increases while gas concentration stays the same, partial pressure decreases. If % of gas increases while total gas stays the same, partial pressure increases.
Partial pressure gradient
A difference in the partial pressure of one specific gas between two locations
Will diffuse down partial pressure gradients to even out concentration
Pulmonary gas exchange
Passive diffusion of oxygen (O2) into and carbon dioxide (CO2) out of pulmonary capillaries across the respiratory membrane, driven by partial pressure differences.
Anatomic features of respiratory membrane for efficient breathing
Large surface area
Extremely thin membrane
Ventilation-perfusion coupling
The matching of air flow (ventilation) to blood flow (perfusion) in pulmonary alveoli to maximize oxygen uptake and carbon dioxide removal.
Ensures that well-ventilated areas receive high blood flow, while poorly ventilated areas are bypassed, optimizing efficient gas exchange
Tissue gas exchange
The process where oxygen diffuses from systemic capillaries into body tissues and carbon dioxide diffuses from tissues into the bloodstream.
Pulmonary v. tissue gas exchange
Pulmonary oxygenates blood
Tissue delivers oxygenated blood to cells and removes CO2
Why does partial pressure in the blood change depending on location?
More oxygen is necessary in certain parts of the body
Why is hemoglobin essential to oxygen transport?
Carries more oxygen than plasma can dissolve
How is CO2 transported in the blood?
Dissolved in plasma
Bound to amino groups in hemoglobin
Transported in plasma as bicarbonate
Conversion of CO2 to HCO3-
CO2 diffuses into erythrocytes
Carbonic anhydrase catalyzes formation of HCO3-
HCO3- leaves erythrocyte and moves into plasma
Three substances carried by hemoglobin
O2
CO2
Nitric oxide (NO)
Most important variable that influences binding of O2 to hemoglobin
Partial pressure of oxygen
How do variables that increase metabolism impact hemoglobin?
Increased metabolism (lower pH, high PCO2, high temp) cause hemoglobin to release oxygen molecules
Hormones that active feeding center
Ghrelin (stomach
Hormones that activate satiety center
CCK (small intestine)
Insulin (pancreas)
Leptin (adipose tissue)
Organs of the GI tract
Oral cavity
Pharynx
Esophagus
Stomach
Small intestine
Large intestine
Anal canal
Accessory digestive organs
Teeth
Tongue
Salivary glands
Liver
Gallbladder
Pancreas
Functions of digestive system
Ingestion (entry of substance)
Motility (mix and move substance through GI tract)
Secretion (release of substances to aid in digestion)
Digestion (breakdown of substances)
Absorption (transport of materials to lymph or blood)
Elimination (excretion of undigested components)
Digestion
Mechanical: physically making food smaller (chewing, stomach churning)
Chemical: use of enzymes to break down complex molecules into simple molecules
Motility
Smooth muscle in the wall of GI tract contract and relax to move GI contents
Segmentation: mixing
Perstalsis: wave of contraction
Absorption
Digested substances are transported from the lumen of the GI tract through epithelium
Most absorbed through blood
Lipids and lipid-soluble vitamins absorbed in lymph
Systems that regulate digestive system
Nervous system (enetric and autonomic, parasympathetic/sympathetic)
Endocrine system
Location of ENS
Neurons and glis embedded in gut wall as ganglia
Innervate smooth muscle and glands of GI tract
Location of ANS
Innervates muscle and glands of GI tract (direct control)
Neurons of ENS (indirect control)
Sympathetic - decreases activity
Parasympathetic - increases activity
Short reflex
Local, only involves ENS
Alters GI activity in local segment of tract
Long reflex
Involves CNS & ANS
Alters activity in most of GI tract & accessory organs
Receptors in the digestive system
Chemoreceptors (chemical, trigger digestive enzymes)
Baroreceptors (physical, detect stretch)
Located in mucosa and submucosa walls
Mastication
Chewing
Composition and function of saliva
99.5% water, 0.5% solutes (enzymes, mucin, lysozyme and antibodies)
Moisten food, chemical digestion, cleanse oral cavity, prevent bacterial growth
How stomach participates in digestion
Holds place for ingested food
Chemical & mechanical digestion
Absorption
Regulates entry of chyme in small intestine
Secretory cells in gastric epithelium
Surface mucous cell
Mucous neck cell
Parietal cell
Chief cell
G-cell
Secretions of gastric cells
Alkaline mucus - coat inner stomach, protect from acidity
HCl - breaks down plant walls and denatures proteins, activates enzymes, creates optimal pH from pepsin and acidic lipases
Gastric lipase - digests fats, active in low pH of stomach
Pepsinogen - breaks down denatured enzymes, active in low pH of stomach
Gastrin - hormone released into blood, stimulates stomach motility and secretions
Cephalic reflex
Sensory input and thoughts of food sent to medulla oblongata
Medulla integrated into and increases PS output to stomach
Stomach increases contractions and secretions
Gastric reflex
Baro & chemoreceptors in stomach are activated and send info to medulla oblongata
Medulla processes info and increases PS output to stomach
Stomach increases contractions and secretions
Intestinal reflex
Chemoreceptors in small intestine are activated and send info to medulla
Medulla processes info to decreases PS output to stomach
Stomach decreases contractions and secretions
Primary function of small intestine
Finishes chemical digestion
Primary site for absorption of nutrients and water
Function of circular folds
Increase surface area, slow down movement of food
Function of villi and microvilli
Increase surface area for absorption
Small intestine secretion cells
Simple columnar epithelium: absorbs nutrients
Goblet cells: produces mucin
Enter endocrine cell: secretes CCK & secretin
Paneth cell: secretes lysozome
Liver in the digestive process
Produce bile
Pancreas in the digestive process
Releases pancreatic juices which chemically digest all macromolecules and neutralize acidic chyme
Gallbladder in digestive process
Store and release bile into duodenum
Function of bile
Neutralize acidic chyme
Emulsification of lipids (bile salts)
Elimination of bilirubin & cholesterol
Regulation of accessory glands
Secretin & CCK and autonomic nervous system
Motility in the small intestine
Segmentation dominates early intestinal phase (mixes chyme with accessory digestive secretions & brush border enzymes)
Peristalisis dominates late intestinal phase (propel chyme towards the large intestine)
Gastroileal reflex
Initiated during gastric & intestinal phase
Ileum contracts
Ileocecal valve relaxes
GI contents enter cecum
Primary function of large intestine
Absorption of remaining water & electrolytes
Vitamin synthesis by colonic bacteria (K & B5)
Formation, storage, and elimination of feces
Peristalsis in large intestine
Slow
Short reflex
Haustral churning in large intestine
Hastrum stretches as it fills with fecal material
Stretch stimulates contraction of hastrum
Mixes and moves material to distal hastra
Short reflex