Chem unit 4 Liver, cardiac, and renal
1/80
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
81 Terms
What are the two sources of blood for the liver
Hepatic artery (25%) and portal vein (75%)
Where does the portal vein originate from
Intestines
What are the two major cell types in the liver
Hepatocytes and kupffer cells
What are kupffer cells
Macrophages acting as phagocytes
List the breakdown of RBCs
Heme→ biliverdin → indirect bili → direct bili→bile→urobilinogen→urobilin
What is the result of an increase in conjugated bili
Urine bilirubin
What is the result of an increase in unconjugated bili
An increase in urine urobilinogen
Equation for total bilirubin
Indirect+ direct bilirubin
How does the liver work in carbohydrate synthesis
Storing glycogen and degrading glycogen when needed
What is the name of the detoxification and drug metabolism system
Cytochrome P-450 system
What are the two phases of cytochrome P-450
1: addition of polar group
2: sulfation
What coagulation related results are good markers of liver disease
Increased PT and decreased albumin
How does the catabolism of amino acids occur in the liver (what is produced/ what is this converted to)
Ammonia is produced from catabolism and is converted to urea, urea excreted in the kidneys
What is caused by impaired clearance of ammonia
Hyperammonemia and brain damage
What is a porphyria
Defect in heme synthesis (sometimes done by liver)
What color is urine with large amounts of porphyrins
Red or “port wine” color
What porphyrins are tested for in the urine
Porphobilinogens and delta aminolevulinic acid
What is unconjugated bilirubin bound to
Albumin
What happens to unconjugated bilirubin in the liver
It is conjugated and is then water soluble
What drug is a hepatotoxic in excess
Acetaminophen
What is the name of the intermediate metabolite formed during acetaminophen overdose
NAPQI
What is the main effect of alcohol on the liver
Fatty liver disease
NADH is formed during alcohol processing which inhibits fatty acid oxidation leading to excess TAGS (can’t be stored in liver)
What are alcoholics also at risk for
Pancreatitis due to increased triglycerides
What is increased in prehepatic jaundice
Indirect and total bilirubin
What is elevated in hepatic jaundice
Unconjugated and conjugated bilirubin (total)
What is elevated in post hepatic jaundice
Serum conjugated bilirubin, ALP, GGT
What are the lab results for Reye syndrome
Abnormal liver enzymes and elevated ammonia, but bilirubin level is no elevated
What is the name of hepatic jaundice in infants after birth
Kernicterus
What is the main source of error in bilirubin specimens
Exposure to fluorescent light/sunlight
What is used in the jendrassik grof method for measuring bilirubin
Caffeine-benzoate-acetate
What is in aliquot 1 for bilirubin analysis and what does this measure
Diazotized sulfanilic acid and this measured direct (conjugated) bilirubin
What does aliquot 2 contain and what does it measure
Caffeine-benzoate-acetate, this measures total bilirubin by reacting with direct and indirect bilirubin to form azobilirubin
What reagent is used to measure urobilinogen
Ehrlich’s reagent
What does a complete absence of urobilinogen from stool and urine indicate
Complete biliary obstruction
What aminotransferase are elevated in hepatitis
AST and ALT
Which aminotransferase is liver specific
ALT
When is ALP elevated
Biliary tract obstruction, bone disorders
When is 5’NT elevated
Biliary tract obstruction
When is GGT elevated
Liver specific- highest in biliary tract obstruction or alcohol ingestion
Which liver tests measure hepatic synthetics ability
Serum albumin and PT time
Which liver function tests measures nitrogen metabolism
Plasma ammonia levels
What does coronary heat disease manifest as
Myocardial infarction
What does cerebrovascular disease manifests as
Stroke
What does peripheral arterial disease manifests as
Localized pain in arms and legs
What does aortic atherosclerotic disease manifests as
Aneurysms
Cardiac biomarkers are normal in unstable angina, elevated in MI (T/F)
True
What happens to arteries in atherosclerosis
Accumulation of lipids, smooth muscle cells, macrophages, and connective tissue (plaque build up)
What is the development of atherosclerotic plaques called
Atherogenesis
What is a fundamental feature of atherogenesis
Inflammation
What are some of the early biomarkers for MI
LD, CK, flipped LD
When can CK also be elevated
Muscular dystrophy and other skeletal muscle disorders
CK>6% ?
Suggestive of MI
CK<3%?
Suggestive of skeletal muscle damage
What is the calculation for the CK-MB index
CK-MB/total CK activity x100
What are the 3 isoforms of troponin
TnT, TnI, TnC
How do troponin levels change after MI
Rises 4-8 hrs after, peaks at 12-14 hrs, remains elevated for 10 days
What troponin isoforms are preferred for myocardial necrosis
TnI, TnT
When is BNP increased
Congestive heart failure
How does BNP effect blood pressure
Decreases blood pressure by increasing Na and water excretion, causing vasodilation
What is used to monitor endogenous levels of BNP
NT-pro-BNP
What other risk assessment markers are used for MI
high sensitivity CRP, homocysteine levels
What does pulmonary embolism develop from
Deep vein thrombosis
What is often measured for PE
D-dimers
What does D-dimers test
Current or recent coagulation and fibrinolysis
Explain the functions of the PCT, loop of hence, DCT, and collecting ducts
PCT: tubular reabsorption
LOH: aids in reabsorption of water, sodium, and chloride
DCT: adjusts for electrolyte and acid-base regulation, control of ADH and aldosterone
CD: final site for concentration or dilution of urine
How is urea made
Final product of protein catabolism
What is creatinine derived from
Derived from muscle phosphocreatine
What is Uric acid dependent on
Endogenous purine degradation
What happens to non protein nitrogen compounds in renal failure
Urine output decreases, increase in plasma urea and creatinine lvls, decrease in urine urea and creatinine levels
What stimulates ADH secretion
Increased plasma osmolality
What does ADH do
Increase permeability of distal convoluted tubules and collecting ducts to water
What does the kidney synthesize
Renin, EPO, 1,25-dihydroxy vitamin D3, prostaglandins
What is the best test for describing kidney function and for determining GFR
Creatinine clearance
How do you calculate creatinine clearance
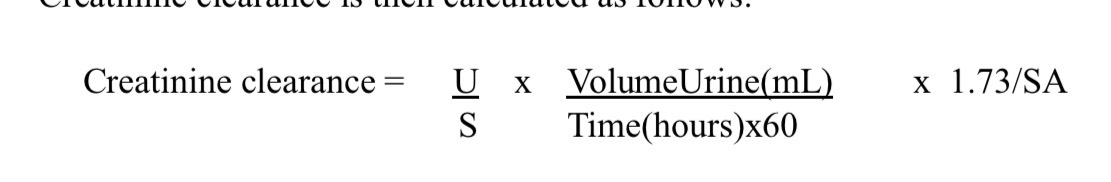
What are some other clearance measurements for kidneys
Urea and cystatin C
What does urine osmolality measure
Assesses the concentration ability of kidneys
What does microalbuminuria measure and for what patients is it used for
Small amounts of albumin in the urine, used for diabetes mellitus patients
What is a sign of renal disease in urinalysis
Protein in the urine
What are the lab results for glomerular diseases
Elevated bUN and creatinine, decreased GFR
What are the associated urinalysis results for acute glomerulonephritis, chronic glomerulonephritis , and nephrotic syndrome
AGN: hematuria and proteinuria, RBC casts
CGN: waxy and broad casts, cellular casts
NS: proteinuria, hypoalbuminemia, hyperlipidemia, and lipiduria
What causes renal hypertension
Decreased perfusion to the kidneys