OHD1 intro into the eye 1 (copy)
1/52
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
53 Terms
intro into the eye
diagram of the eye
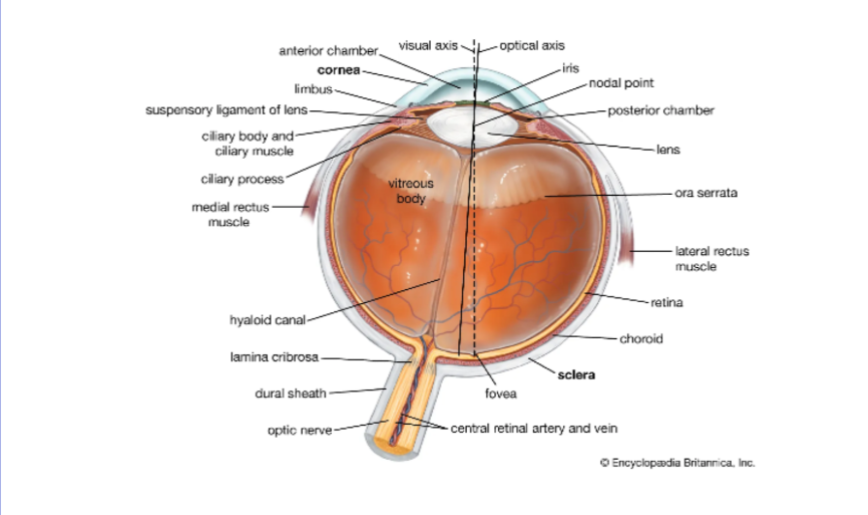
Anatomical planes
temporal/lateral: away from the body
medial/nasal: towards the body midline
cranial; top
caudal; bottom
anterior front posterior back
proximal and distal
planes
sagittal plane is cut through the body into left and right
coronal is ct into the body front and back
transverse is middle
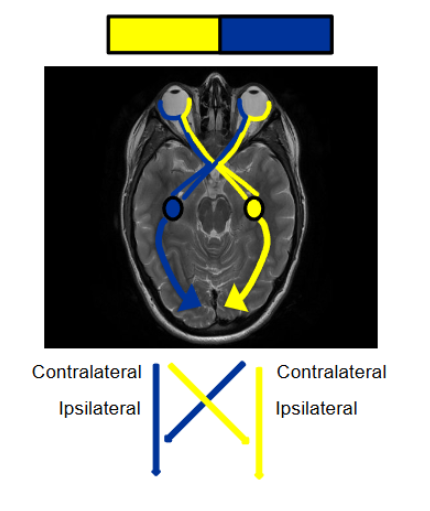
ipsilateral is same side contralateral is opposite
4 types of tissues
epithelial
connective
muscle
nervous
what is a tissue
defined as a collection of similar cells that are specialised to perfomr a common function
epithelial tissues
a thin protective layer
epithelial cells lie on a basement membrane that attaches them to underlying connective tissue
classified by shapes
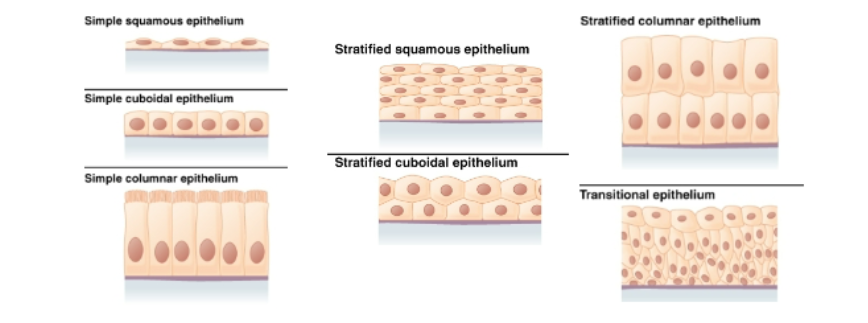
types of epithelial cells
simple squamous
simplecuboidal
simple columnar
stratified squamous
stratified cuboidal
stratified columnar
transitional epithelium
connnective tissues
provide structure and support for other tissue
consists of cells, fibres and extracellular matrix
the fibres found in connective tissue include flexible collagen fibres with high tensile strength that can undergo extensive stretching
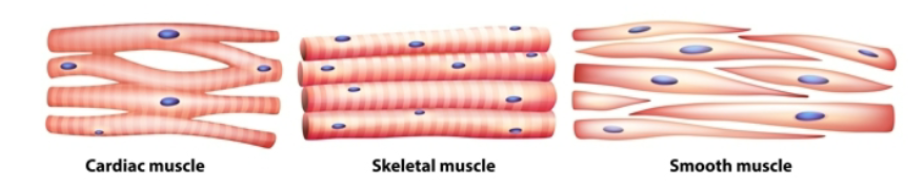
muscle tissues
3 types: cardiac skeletal and smooth
muscles are either striated or smooth and are either under voluntary or involuntary control
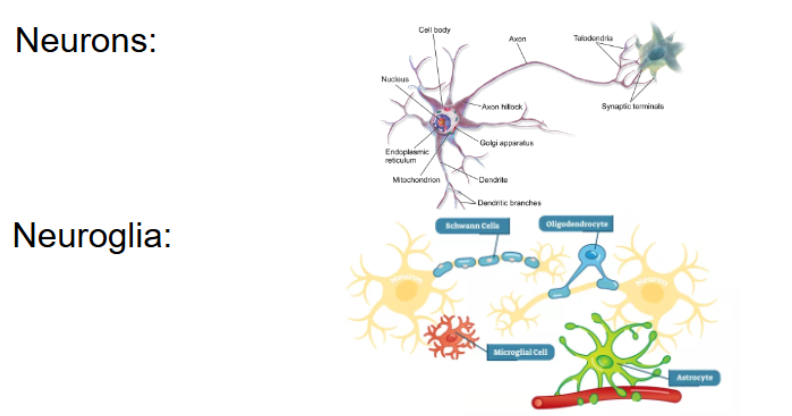
nervous tissue
composed of 2 types of cells
neurons and neuroglia
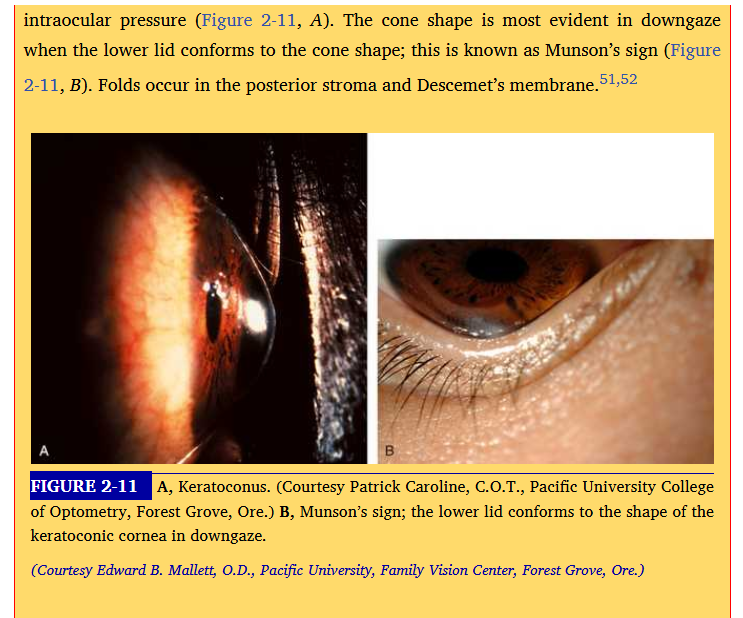
the eyelids or palpebrae
functions of the eyelids:
they cover the globe for protection
contain structures that prodice the tear film
on opening they spread the tear film over the anterior surface of the eye
on closure they move the tears towards drainage areas
the eyelids
the palpebral fissure is the area between the open eyelids
the medial canthus is inner cornerof the eye
lateral canthus is the outer part of the eye
the upper and lower eyelids meet at the corners of the palpebral fissure
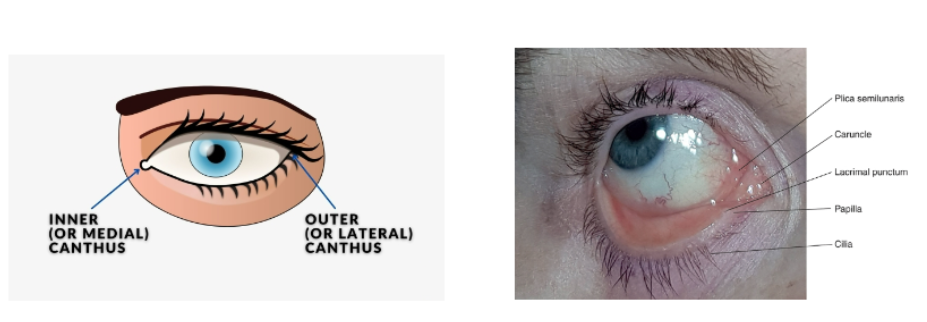
eyelid
the upper eyelid extends to the eyebrows and is divided into the tarsaland orbital parts
the eyelid margi rests againts the globe and contains the eyelashes and the pores of the meibomian glands
you have around 150 eyelashes (cilia) in the upper lid and around 75 in the lower lid
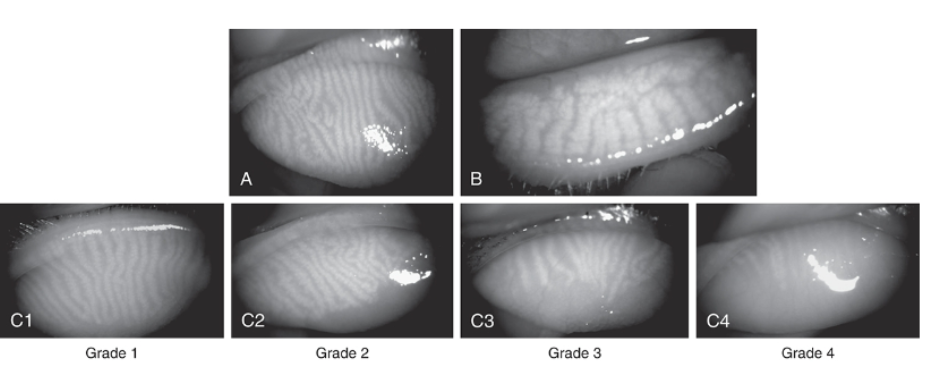
the meibomian gland
produces and secretes meibum
plays role in maintaining the health of the eyes tear film and prpeventing dry eye
in picture grade 4 shows no glands visible so likely person suffers from dry eye
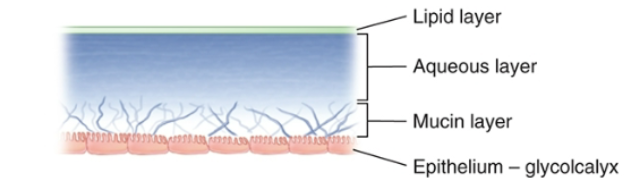
The tear film
the tear film:
keeps the surface of the eye moist
traps debris
provides oxygen to the cornea
provides a smooth refractive surface
contains antibacterial substances
miantains corneal hydration
contains growth factors to mediate conreal wound healing
cornea
can be thought of as the front of a sphere in the front of an eye but is actually more oval.
the radius of the curvature changes between the centre and the periphery of the cornea
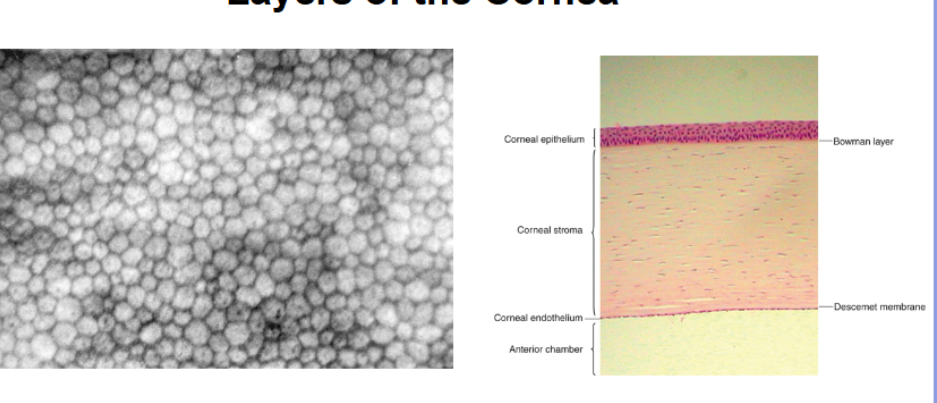
layers of the cornea
corneal epithelium is around 50 microns thick
bowman layer is 8-19 microns thick
corneal stroma is 450-500 microns thick
descemet membrane is 5-15 microns thick
corneal endothelium is normally 5 microns thick
endothelial mosaic forms a leaky membrane
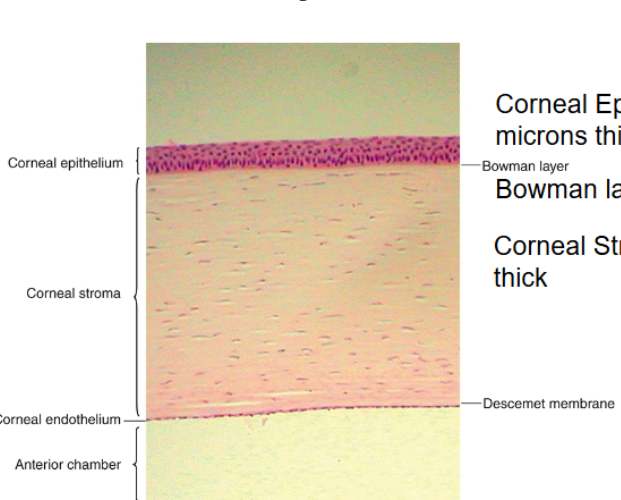
bowmans layer
dense fibrous sheet of interwoven collagen fibrils randomly aranged in a mucoprotein gorund substance.
provide biochemical rigidity and shape to the cornea
posteriorly, as layer transitions into the stroma, the fibrils adopt a more orderly arrangement and merge into bundles if damaged cant regenrate
stroma
middle layer of cornea and it is the tickets
composed of collagen fibrils, keratocytes and extracellular ground substance
the collagen fibrils have a uniform diameter and run parallel to one another , forming flat bundles called llamelae
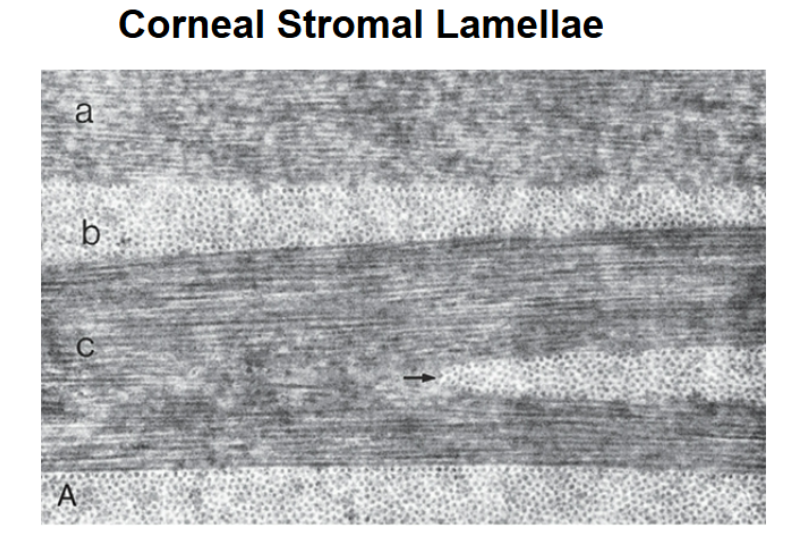
corneal stromal lamellae
a is lamella oriented parallel to the corneal surface
b is lamella oriented perpendicular or at an angle to the conreal surface
c is lamella with keratocyte processes indicated by the arrow embedded between collagen fibres
A is ground substance filling between lamella
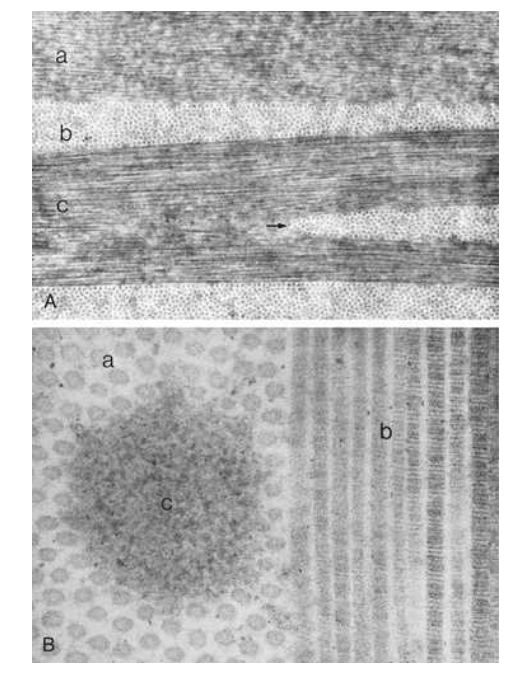
A: view of lamellae cut into 3 planes
a: upper lamella cut obliquely
b: lamella cut in corss section
c: cut longitudinally
arrow shows lamellae split into 2
keratocytes
corneal fibroblasts.
flattenedc cells that lie between and occasionally within the lamellae. cells not distributed randomly; a corkscrew pattern is recognisable from anterior to posterior
have extensive branching joined by gap junctions
maintain the stroma by synthesising collagen and extracellular matric components
descemets membrane
basement membrane od the endothelium
produced ocntinually and therefore thickens throughout life
thickness of descememts membrane changes with increasing age
descemet membrane consists of 2 laminae. the anterior lamina is 3 micrometeres thic, banded appearance and a latticework of collagen fibrils secreted during embyronic development. posterior is nonbanded and homogenous - its the portion secreted by the endothelim
descemets exhibits elastic properties- if torn it will curl into the anterior chamber . very resistant to trauma

endothelium
innermost layer of cornea/. lies adjacent to the anterior chamber and is composed of a single layer of flattened cells. the basal part of each cell rests on the descemets
corneal function
has 2 primary functions:
to refract light and to transmit light
factors that affect the refractive power
the curvature of the anterior conreal surface - more curved light refracted stronger. more refraction so shorter focal point.
change in the refractive index from air to cornea
corneal thickness
the curvature of the posterior corneal surface
change in the refrcative index from cornea to aqueos humor
corneal metabolism
the cornea is metablically active and requires a stable supply of oxygen and glucose
when your eyes are open oxygen is derived primarily from oxygen dissolved in the tear film ( from atmosphere)
glucose and other nutrients and vitamins are absorbed from the aq humor through the leaky endothelium
aquaporins
small integral membrane proteins residing in the plasma membrane, some are water selective and others transport glycerol.
corneal repai- wound healing
corneal injury initiates lots of mechaniss to repair damaged tissure. directed by various biomolecules such as integrins, cytokines and growth factors. corneal integrins are integral membrane glycoproteins that maintain corneal function
bowmans membrane
doesnt regenerate if damaged but will be replaced either by stroma-like fibrous tissue or by epithelium
beneath corneal epithelium made from randomly arranged collagen fibres and provides strucural support
sclera
thick dense connective tissue layer that is continuous with corneal stroma at the limbus.
collagen fibrils are arranged into lamellae but are more irregular than the corneal lamellae
the irregular running of lamellae coupled with the irregular spacing between scleral components induce light scattering which makes the sclera opaque
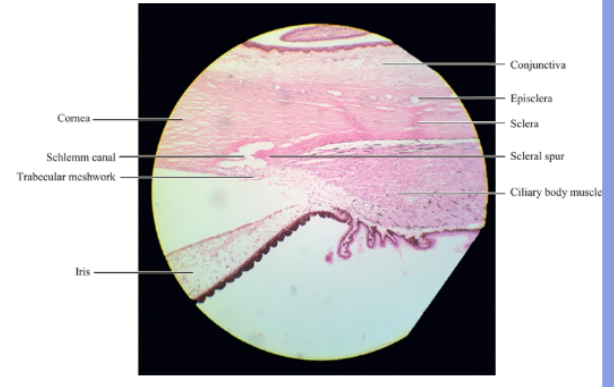
scleral spur
its a region of circularly orientaated collagen bundles that extends from the inner aspect of the sclera
At the posterior edge its fibres blend with the scleralfibres and in cross section looks like a spur
limbus
located t corneascleral junction that encircles the periphery or cornea.
narrow transitional zone and involved in regeneration and nutrition as contains blood vesssels that supply nutrients
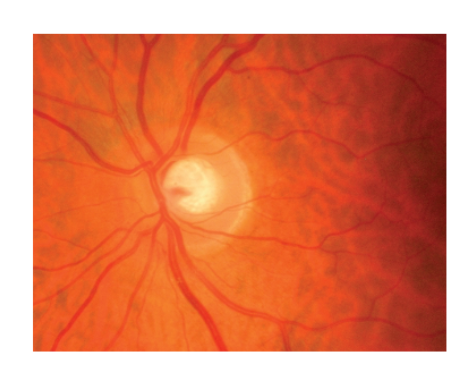
lamina cribosa
the output of the eyeball is via the optic nerve at the back of the eye
its passed through the posterior sclera which is bridged by a network of scleral tissue called lamina cribosa
lamina cribosa is the weakest area of the outer connective tissue
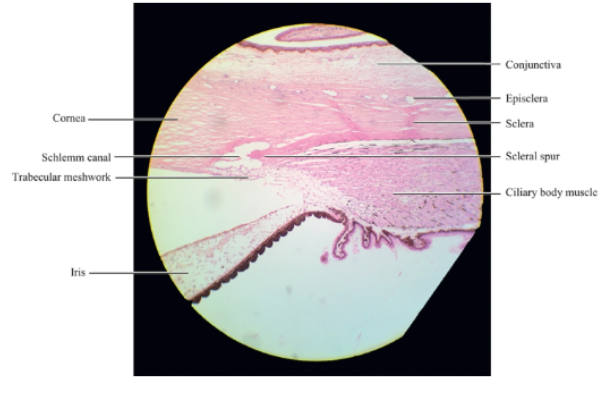
episclera
episclera is a vascularised connective tissue that lies infront of the sclera
episclera is joined to the tenon capsle by stands of connective tissue
tenon capsule: thin fibrous membrane surrounding most of eyeball from optic nerve to the limbus ( the border between the cornea and sclera near front of the eye)
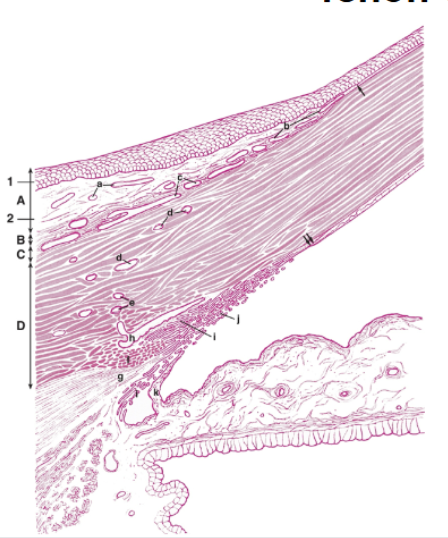
tenon capsule
a thin fibrous sheet of connective tissue that lies in front of the episcleral
contains smooth muscle fibres that regulate the tension of extraocular muscles
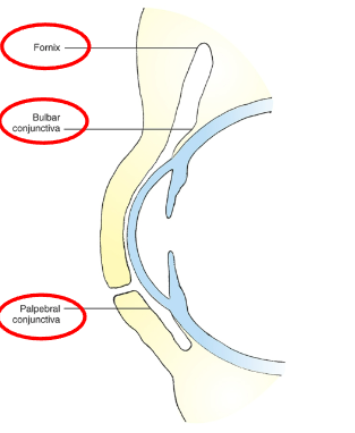
conjunctiva
divided into 3 sections
the bulbar conjunctiva which covers the sclera
the palpebral conjunctiva which lines the eyelids
the conjunctival fornix which is the cul de sac connecting the other 2.
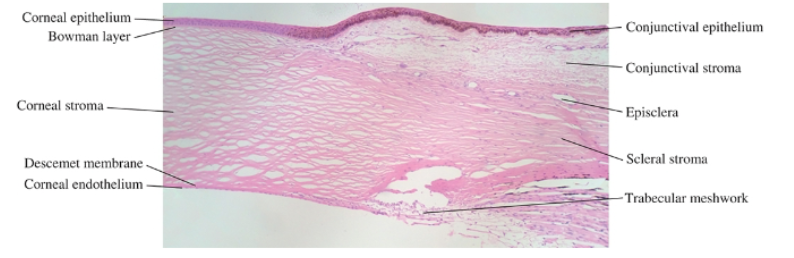
limbus
located at the intersection between cornea and sclera
the external and internal scleral sulci associated with this transtion are clearly visible in cross sections through the limbus
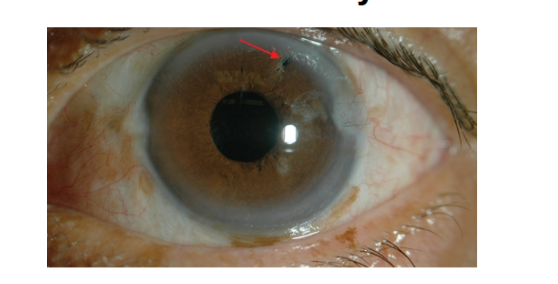
iridectomy
in some cases of glaucoma an iridectomy is performed to facillitate movement of aqueous from the posterior chamber to the anterior chamber
iridectomy uses a laser to make an opening in the iris without exciting tissue
anterior iris epithelium and dilator muscle
the dilator muscle is present from the iris root to a point in the stoma below the midpoint of the sphincter
the dilator muscle causes the pupil to get bigger in low-light conditions (mydriasis)
the anterior iris epithelium continues posteriorly as the pigmented epithelium of the ciliary body
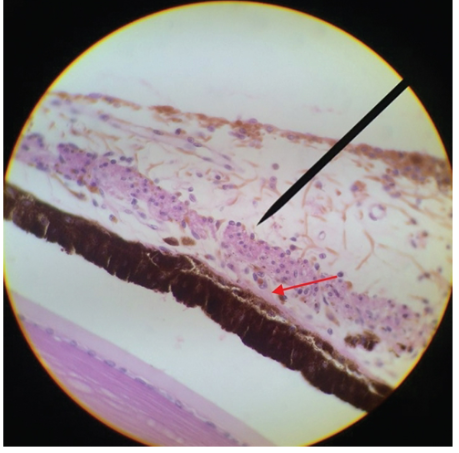
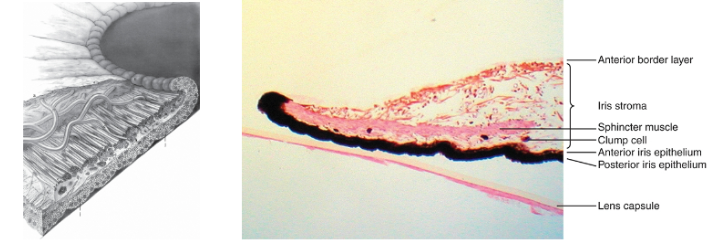
posterior iris epithelium
the second epithelial layer posterior to the stroma is in the posterior iris epithelium a single layer of heavily pigmented columnar cells
the epithelial cells curl around from the posterior iris to the anterior surfave at the pupillary margin forming the pigmented pupillary ruff which encircles the pupil
iris colour
iris colour is determined by a number of factors
the arrangment of connective tissue components in the anterior tissue components in the anterior border layer and stroma, the number of melanocytes and the size and density of melanin granules within the melanocytes
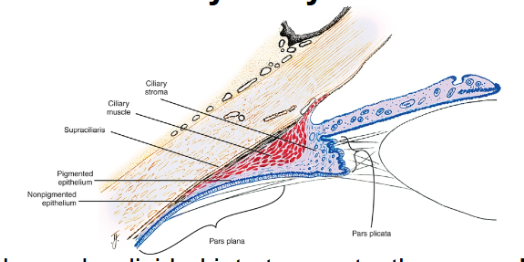
ciliary body
divided into 2 parts: the pars plicata and the pars plana
pars plicata: wider anterior portion containing the ciliary processes
pars plana: flatter region of the ciliary body it extends from posterior pars plicata to the ora serrata
histological features of the ciliary body
the supraciliaris is the outermost layer of the ciliray body adjacent to the sclera
the ciliary muscle is composed of smooth muscle fibres oriented in three directions- longitudinal, radial and circular
more histological features of ciliary body
the stroma of the ciliary body is highly vascularisd and lies between the muscleand the epithelial layers
2 layers of epithelium cover ciliary body and line the posterior chamber and part of vitreous chamber
outer layer of epithelium cells are pigmented and cuboidal while inner layer are non pigmented and columnar
functions of ciliary body
accomodation
production of aqueous and vitreous components
regulation of material allowed in the aqueous
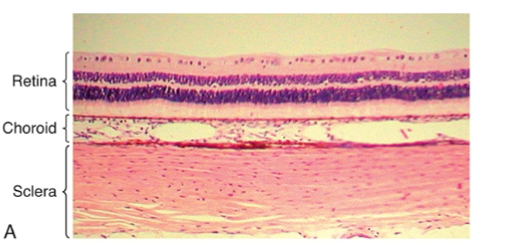
choroid
located between the sclera and the retina
composed of: suprachoroidal lamina. choroidal stroma, choriocapillaris and bruch membrane
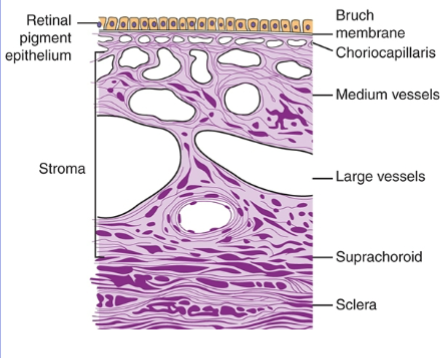
choroid
the suprachoroidal lamina is a thin pigmented layer of connective tissue that lies between the sclera and choroid
choroidal stroma is highly vascularised loose connective tissue with larger vessels occupying the outer layer
more on choroid
the specialised capillary bed within the choroid is called choriocapillaris
the innermost layer of the choroid is Bruch membrane. fine filaments from the RPE merge with fibrils contributing to the tight adhesion between choroid and retina
function of choroid
provide oxygen and nutrients to the outer retina
allow catabolites for the retina to be removed
thermoregulate the retina and interocular pressure drainage