Cardio/Renal 26 - Glomerular Filtration and Clearance II (Dr. Olgun)
1/97
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
98 Terms
What has the following 3 essential functions:
1) They function as filters, removing metabolic products and toxins from the blood and excreting them through the urine.
2) Regulate the body's fluid status, electrolyte balance, and acid-base balance.
3) Produce or activate hormones that are involved in erythrogenesis, Ca2+ metabolism, and the regulation of blood pressure and blood flow.
Kidneys
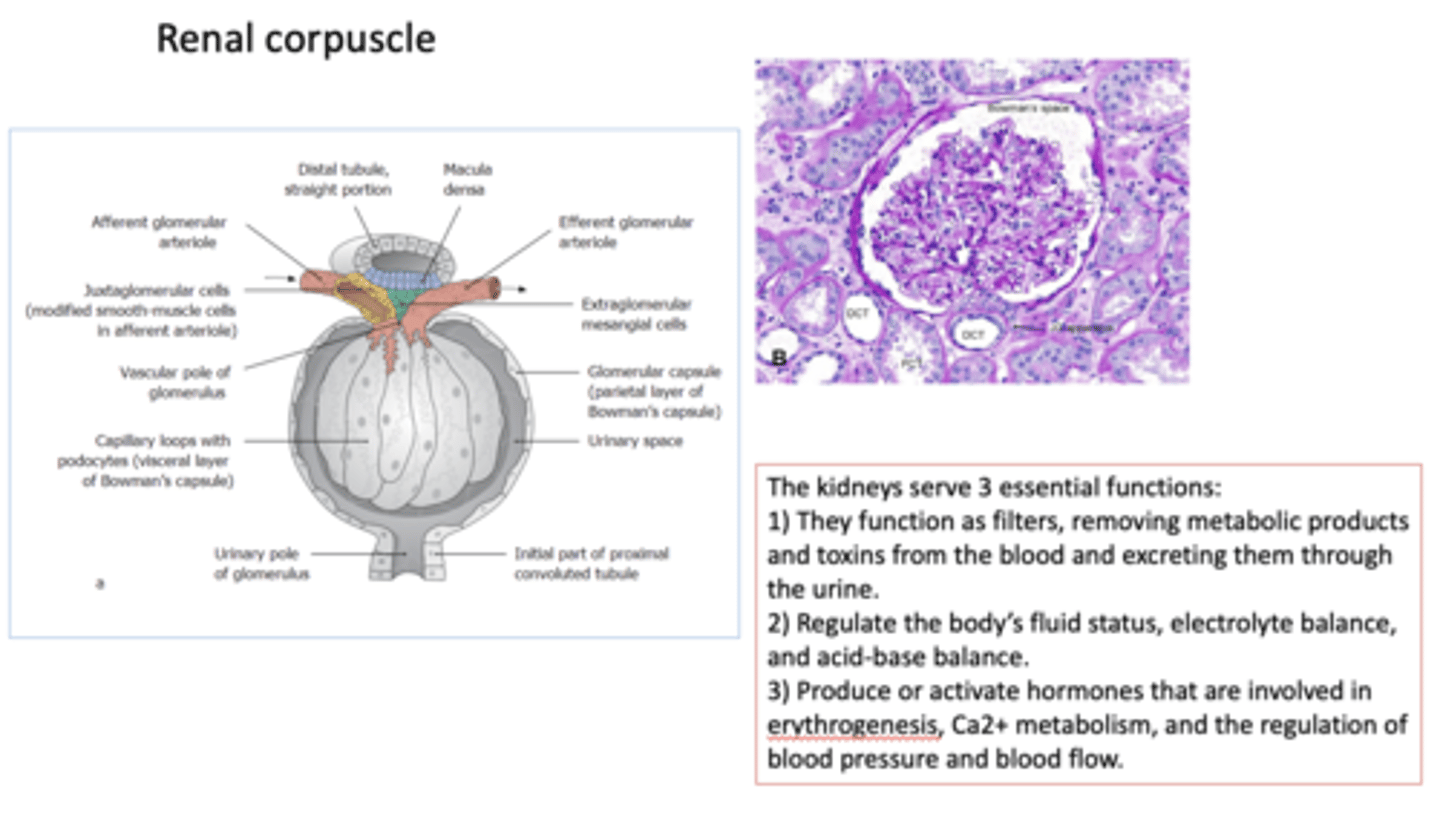
in patients with hypertension, what blood vessels decrease arterial pressure to enter the glomerular capillaries to allow for proper filtration?
afferent arteriole
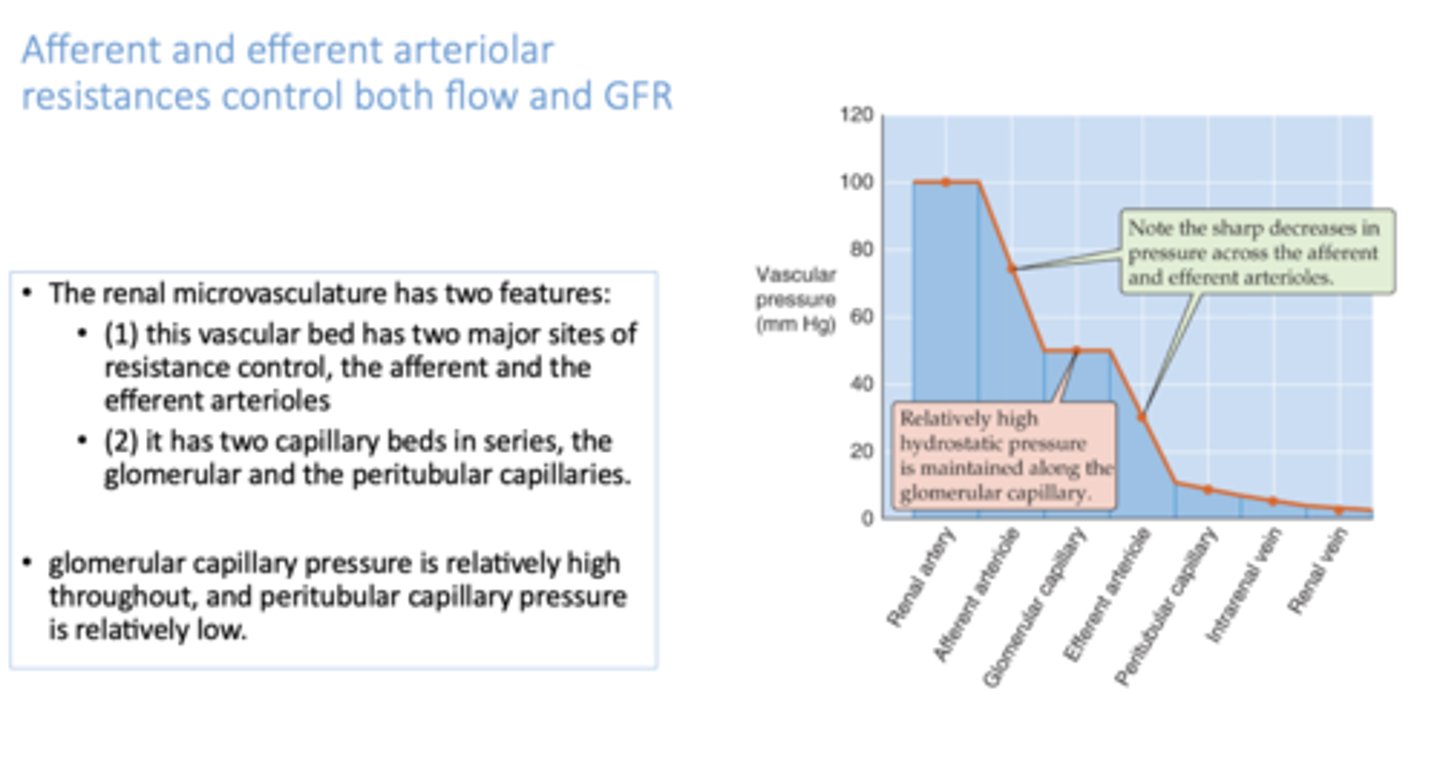
in patients with hypertension, what blood vessels decrease arterial pressure entering the peritubular capillaries to allow for proper GFR?
efferent arteriole
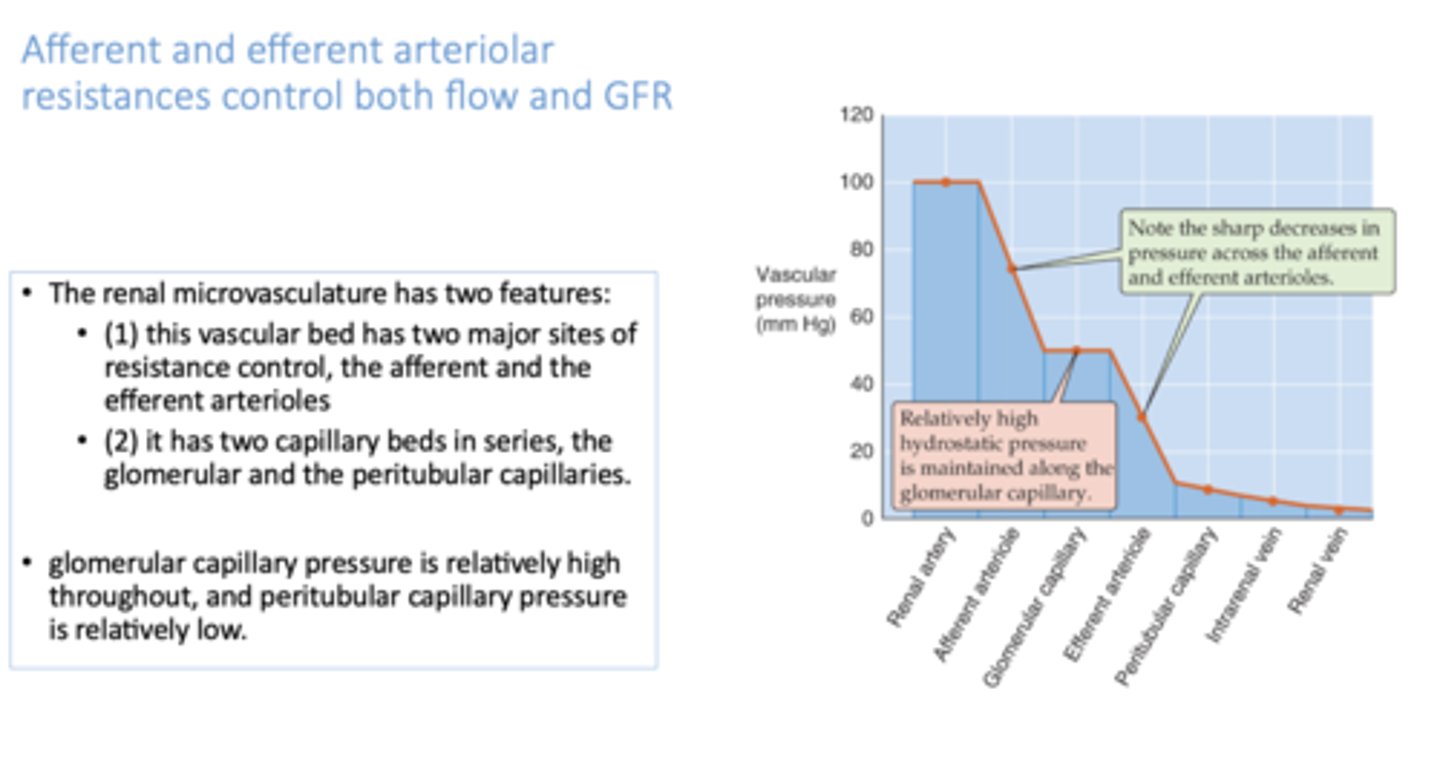
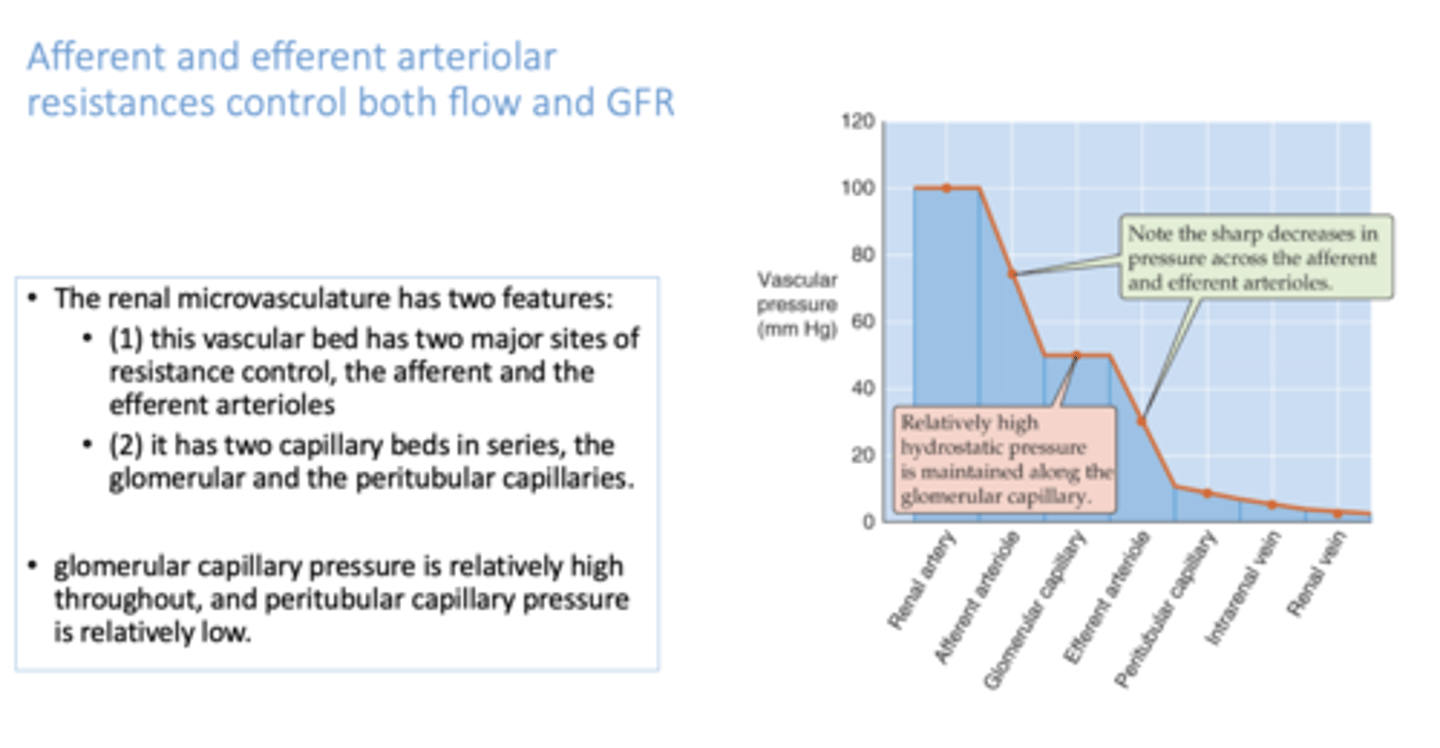
The ______________ has two features:
(1) this vascular bed has two major sites of resistance control, the afferent and the efferent arterioles
(2) it has two capillary beds in series, the glomerular and the peritubular capillaries.
renal microvasculature
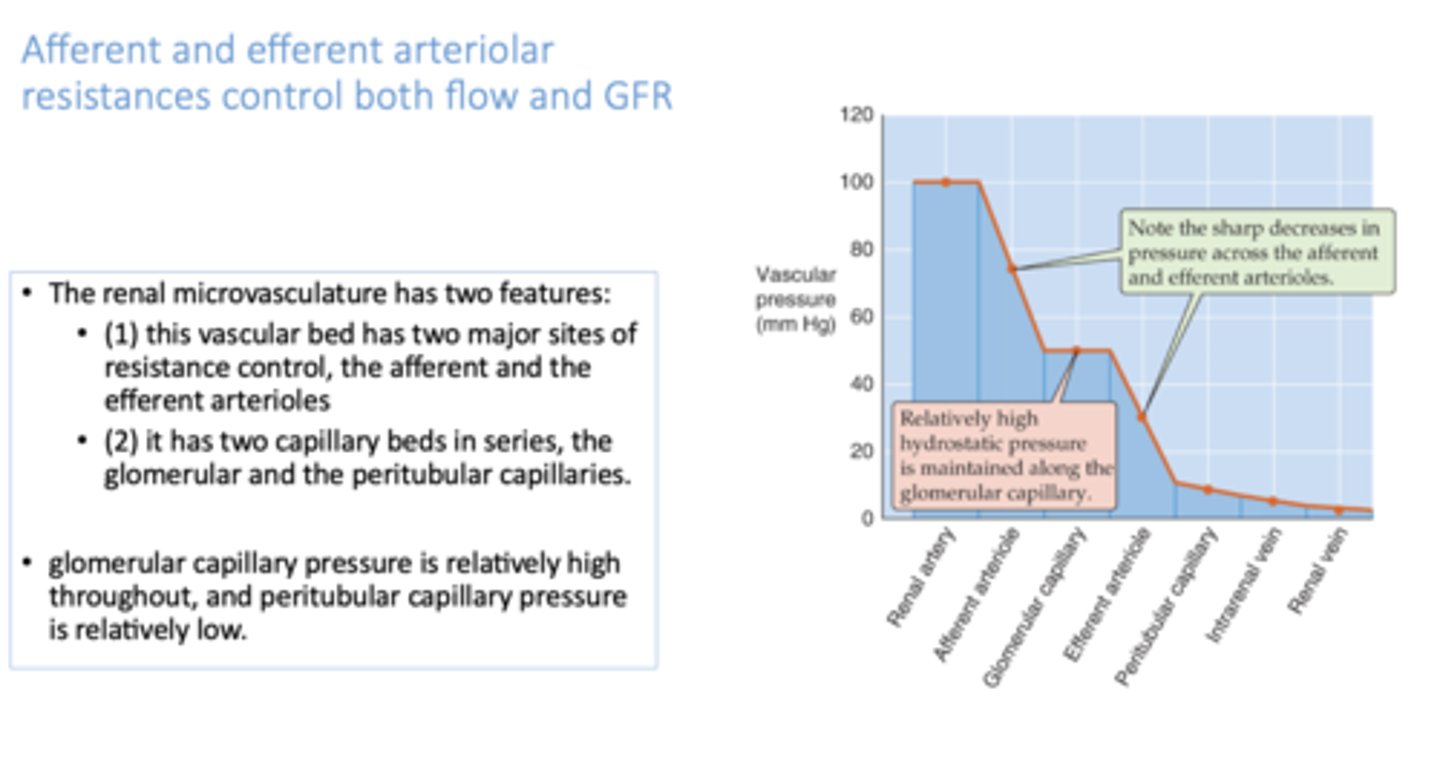
Constricting the afferent arteriole—while relaxing the efferent arteriole does what?
lowers pressure in glomerular capillary
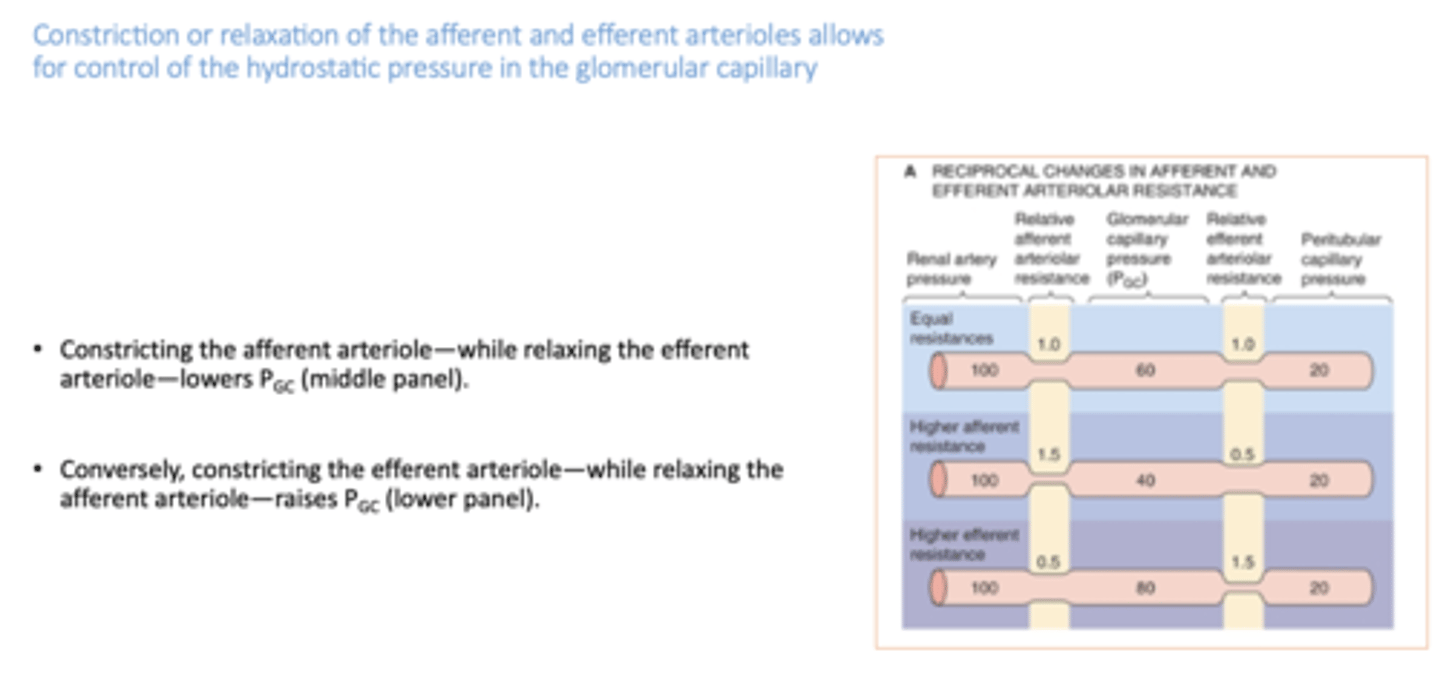
Constricting the efferent arteriole—while relaxing the afferent arteriole does what?
increases pressure in glomerular capillary
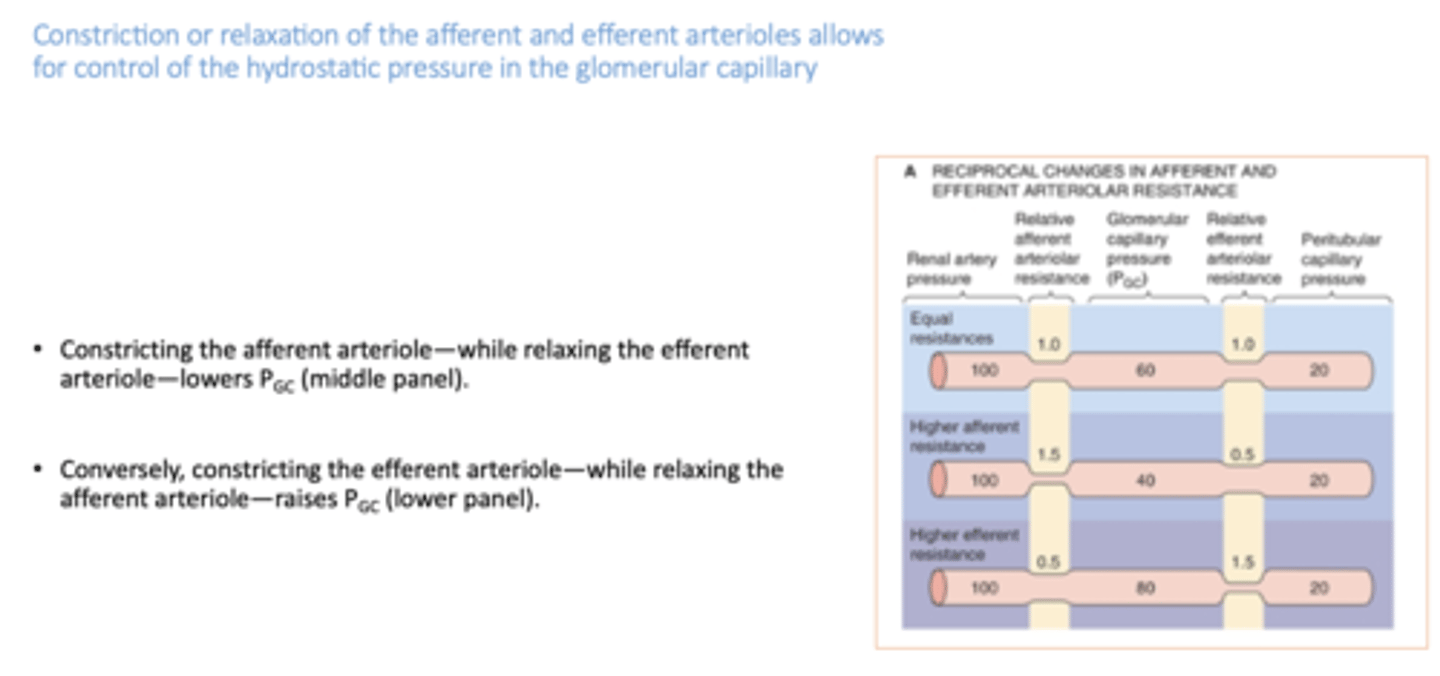
although both afferent and efferent arterioles contract to regulate flow through capillaries, in a patient with hypertension, which capillary bed will experience relatively high pressure throughout?
glomerular capillaries
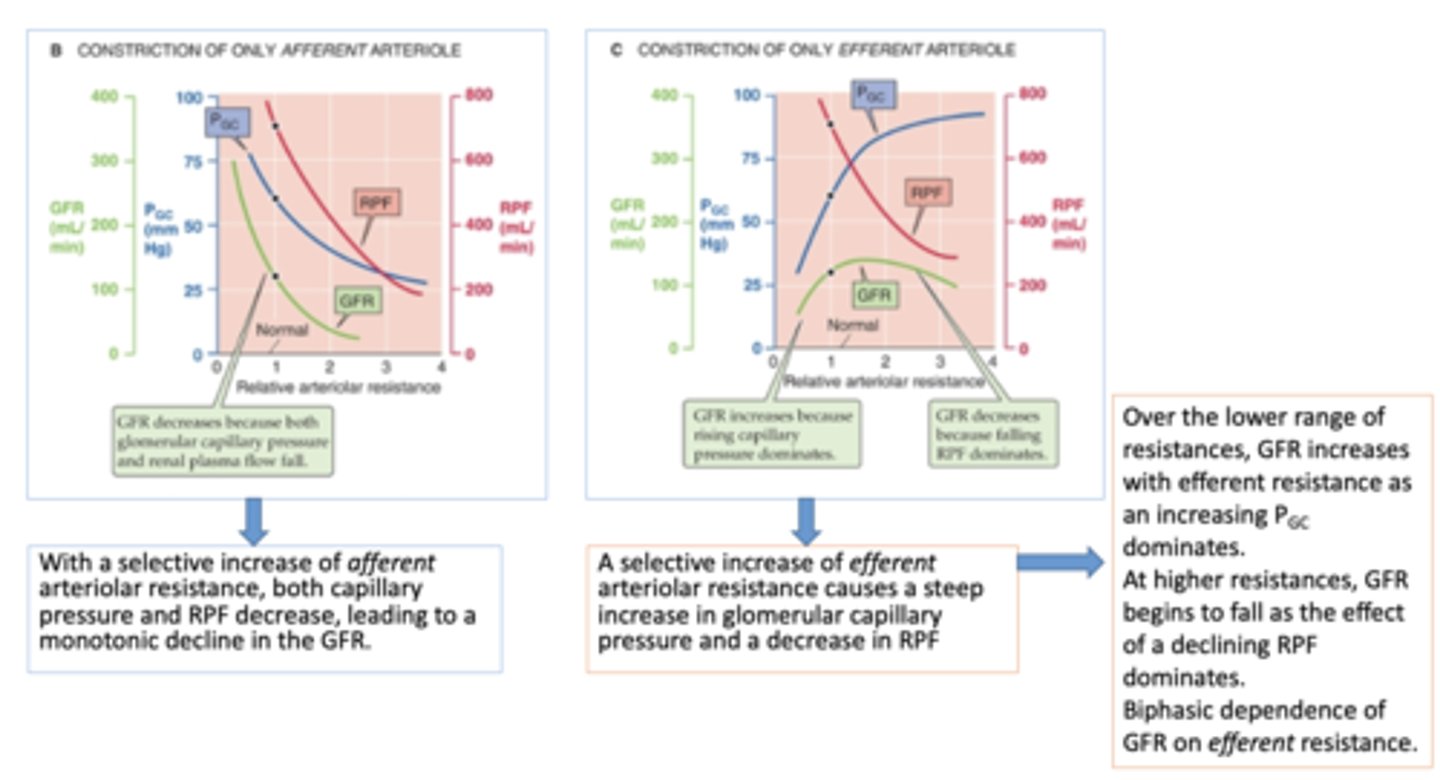
With a selective increase of ______________ arteriolar resistance, both capillary pressure and RPF decrease, leading to a monotonic decline in the GFR.
afferent
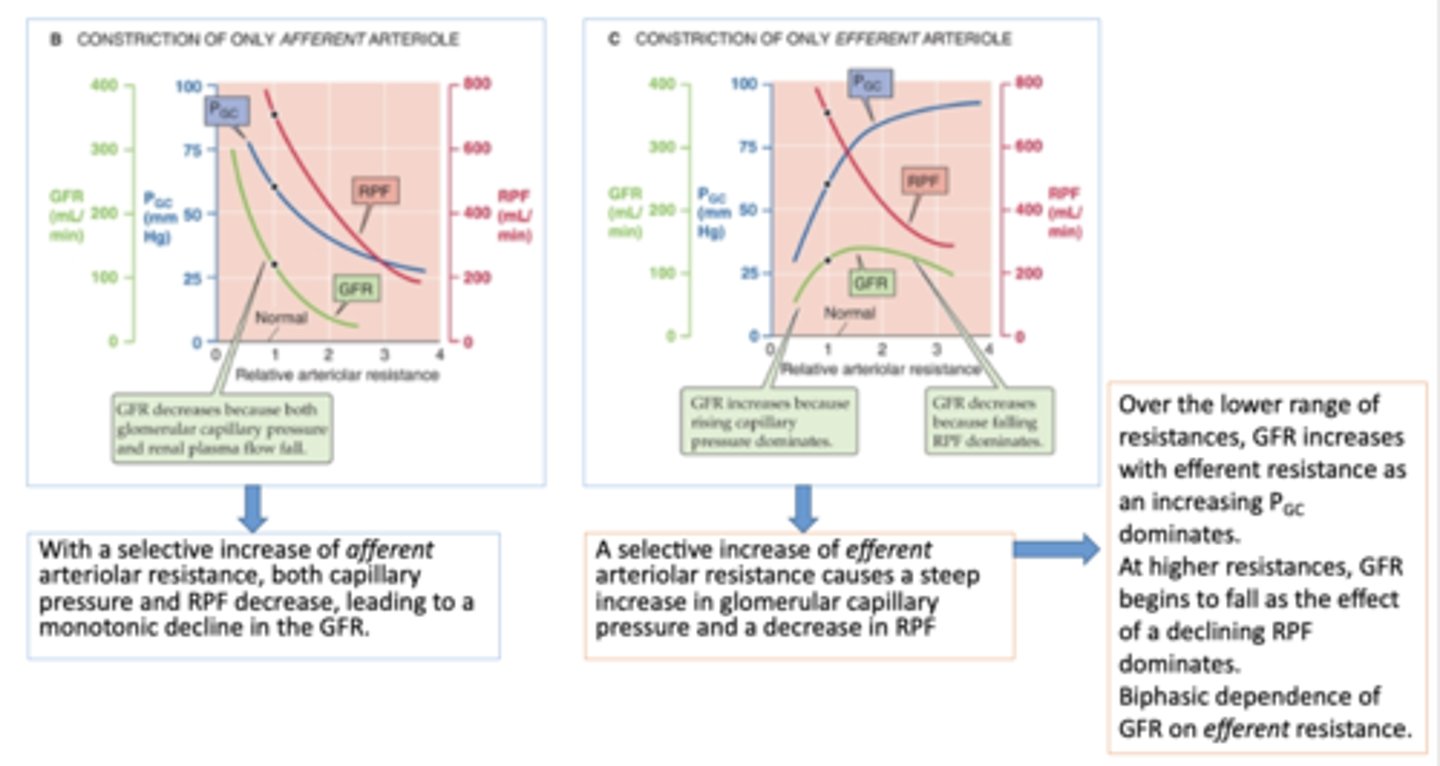
A selective increase of ______________ arteriolar resistance causes a steep increase in glomerular capillary pressure and a decrease in RPF
efferent
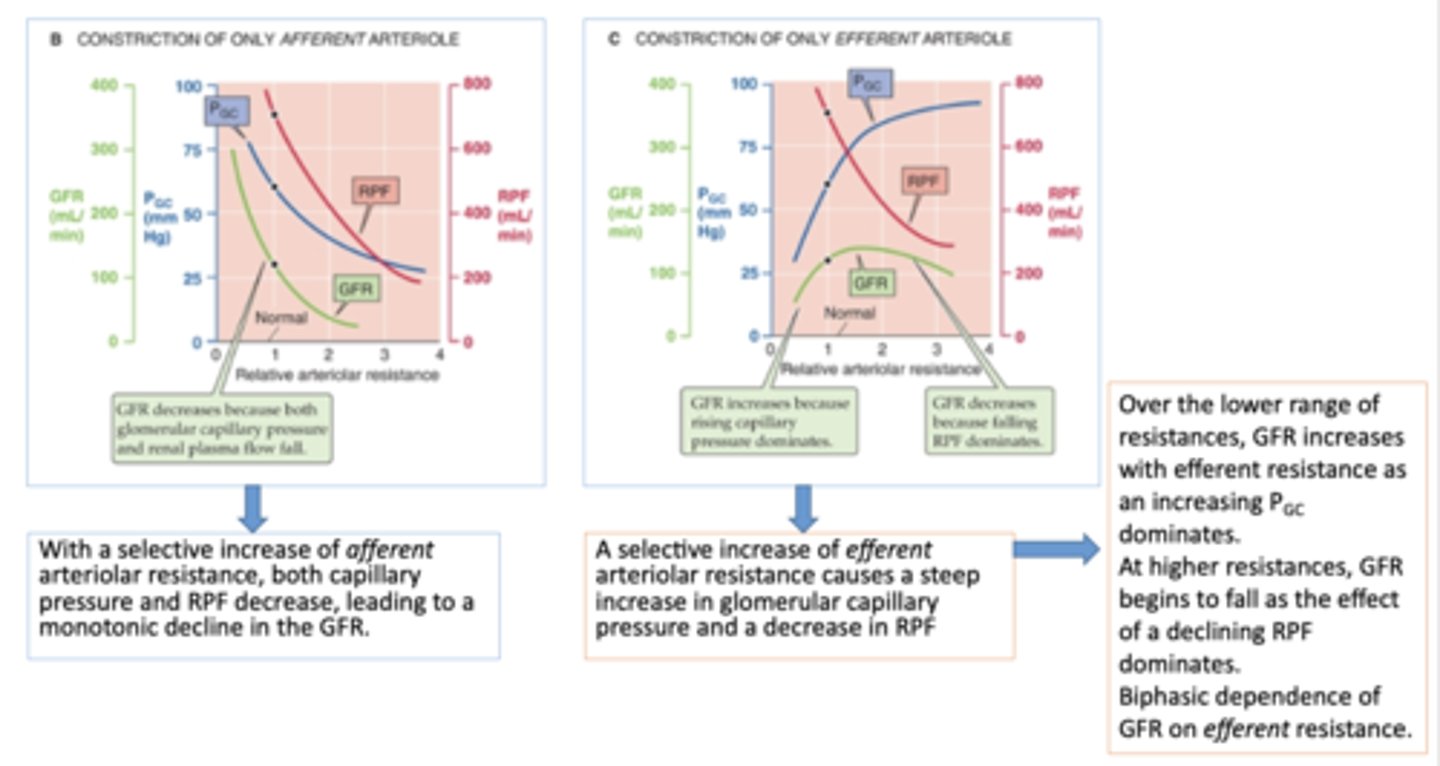
Which arteriole resistance has a biphasic dependence of GFR?
Efferent
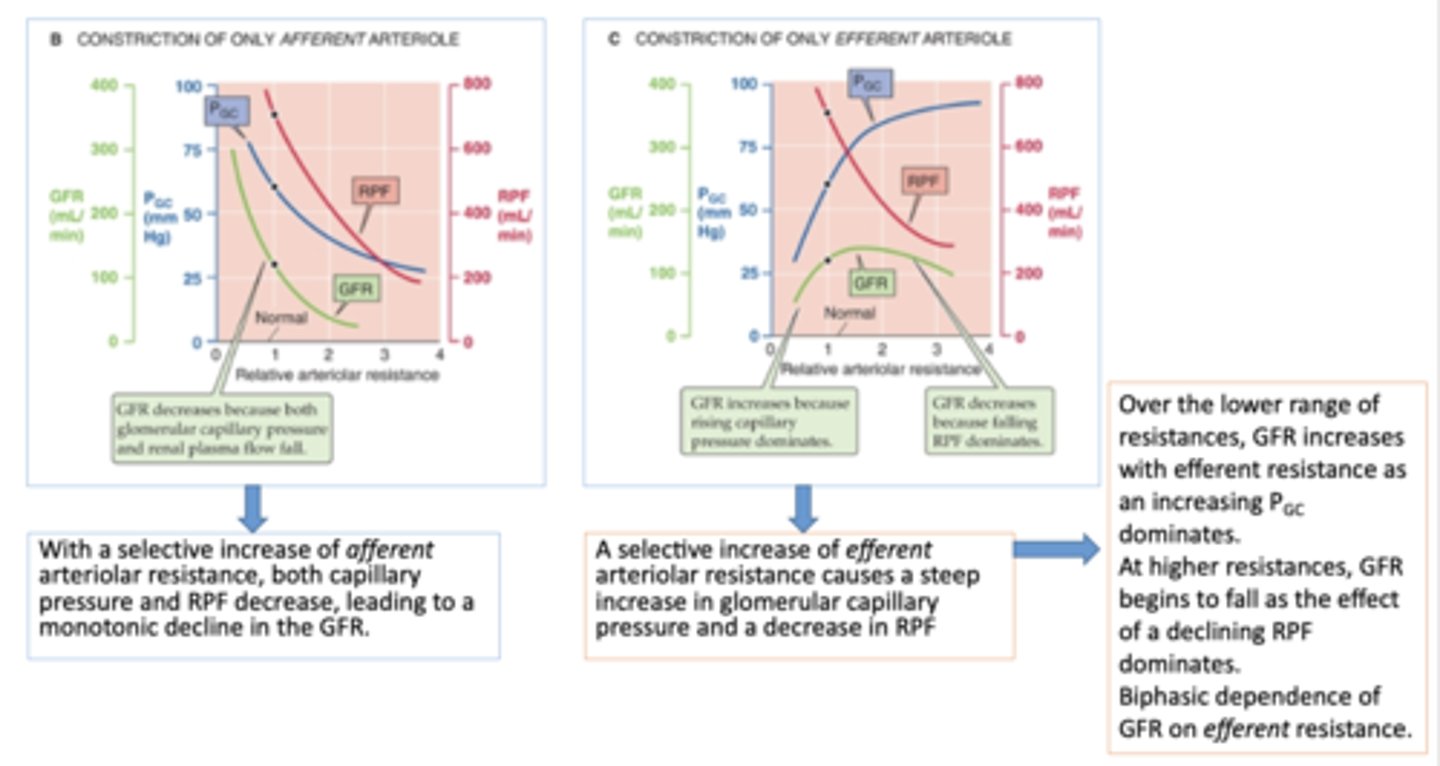
Afferent arteriolar resistance ____________ when there is a large increase in RPF following a loss of renal tissue (for example, after nephrectomy in a kidney donor).
Decreases

An example of a predominantly efferent arteriolar effect is seen after administration of ANG II inhibitors (e.g., captopril) to patients with hypertension. Administering such agents not only ____________ blood pressure, but also often leads to a significant ____________ in GFR
decreases, fall

although both afferent and efferent arterioles contract to regulate flow through capillaries, in a patient with hypertension, which capillary bed will experience relatively low pressure throughout?
peritubular capillaries
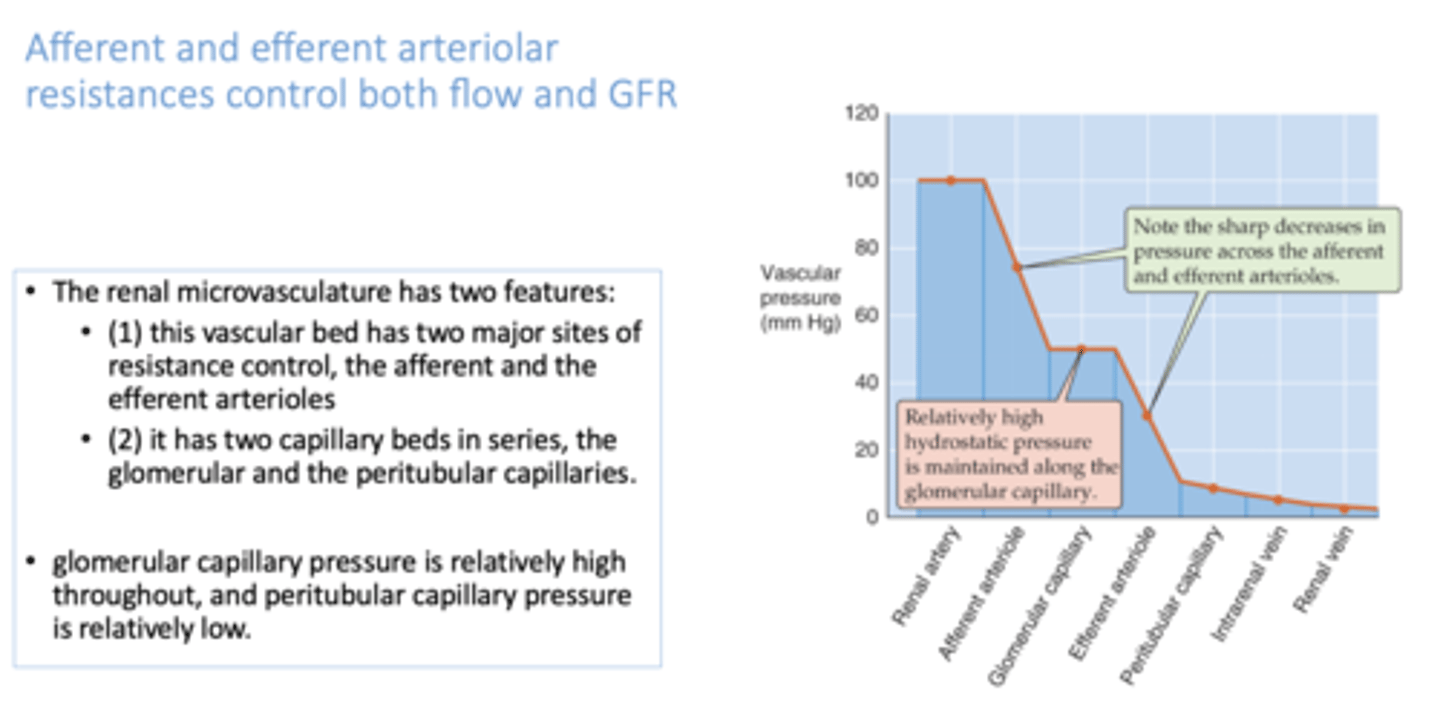
constriction on only afferent arterioles will cause a ______ in glomerular capillary pressure
decrease
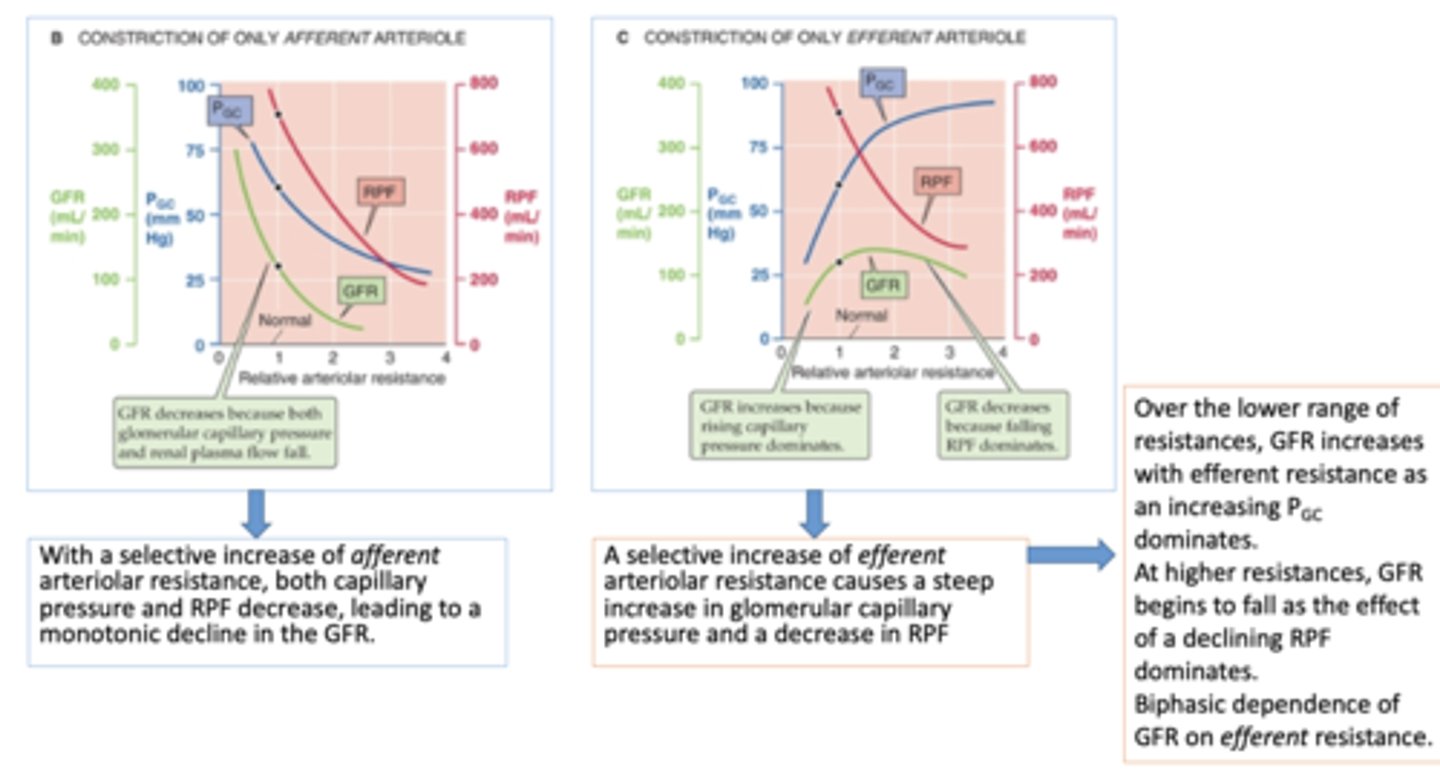
constriction on only afferent arterioles will cause a ______ in renal plasma flow
decrease
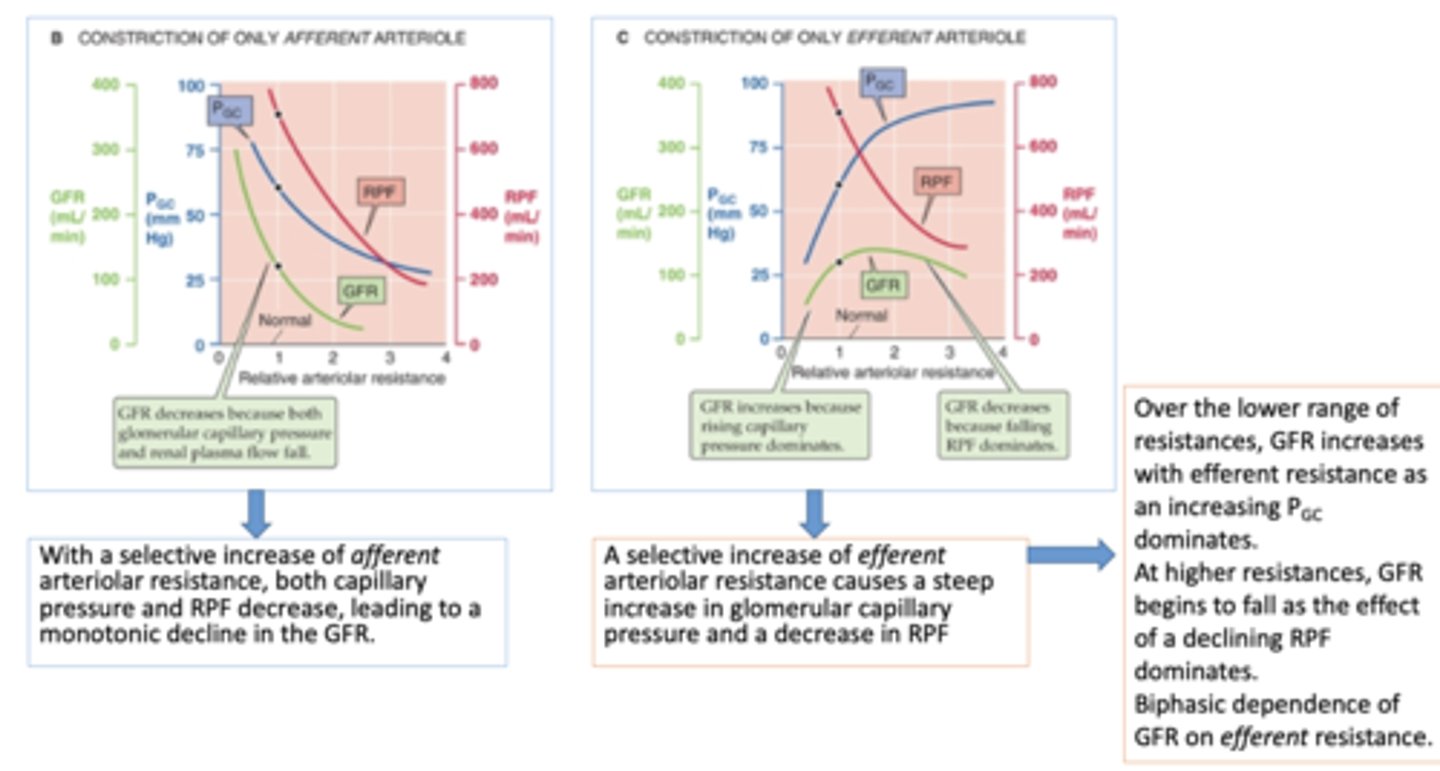
constriction on only afferent arterioles will cause a ______ in glomerular filtration rate GFR
decrease
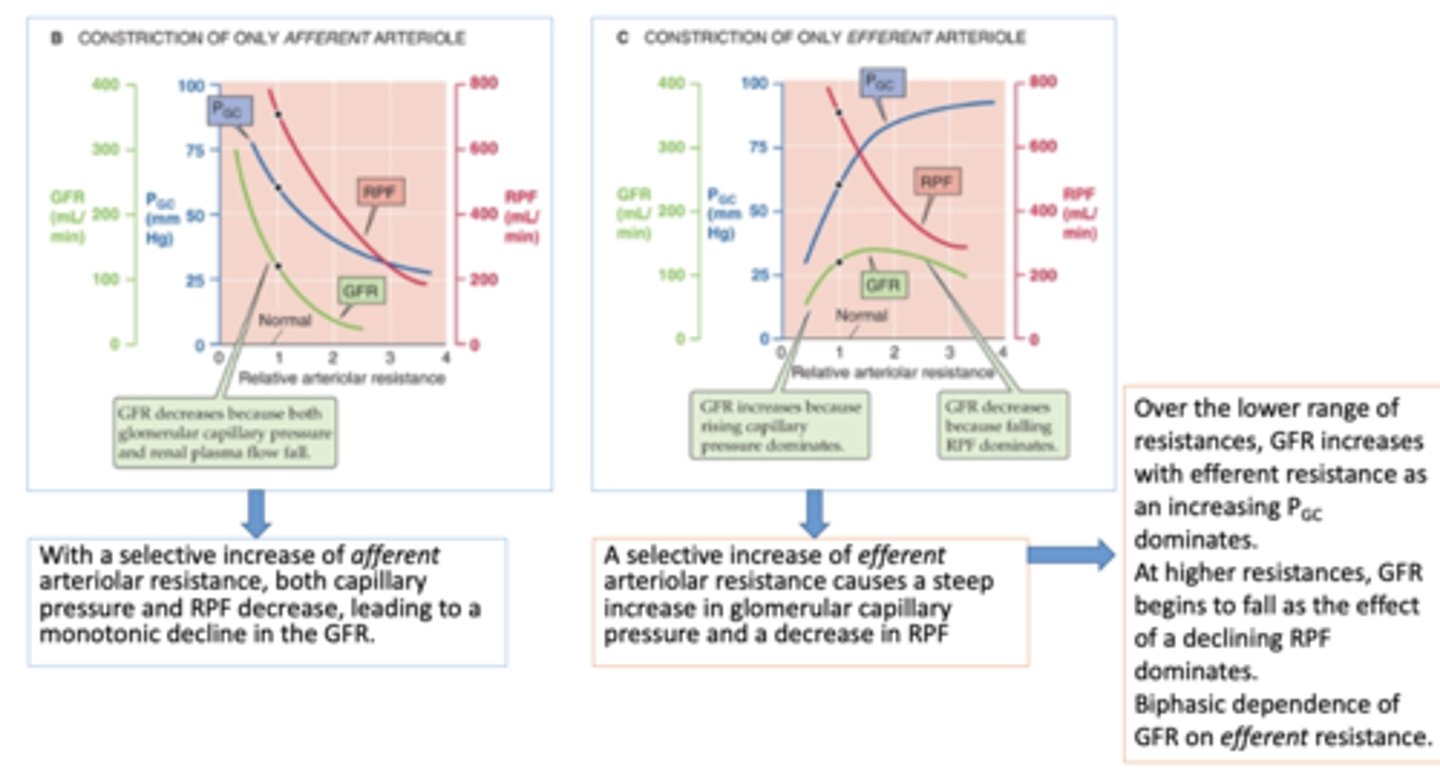
constriction on only efferent arterioles will cause a ______ in glomerular capillary pressure
increase
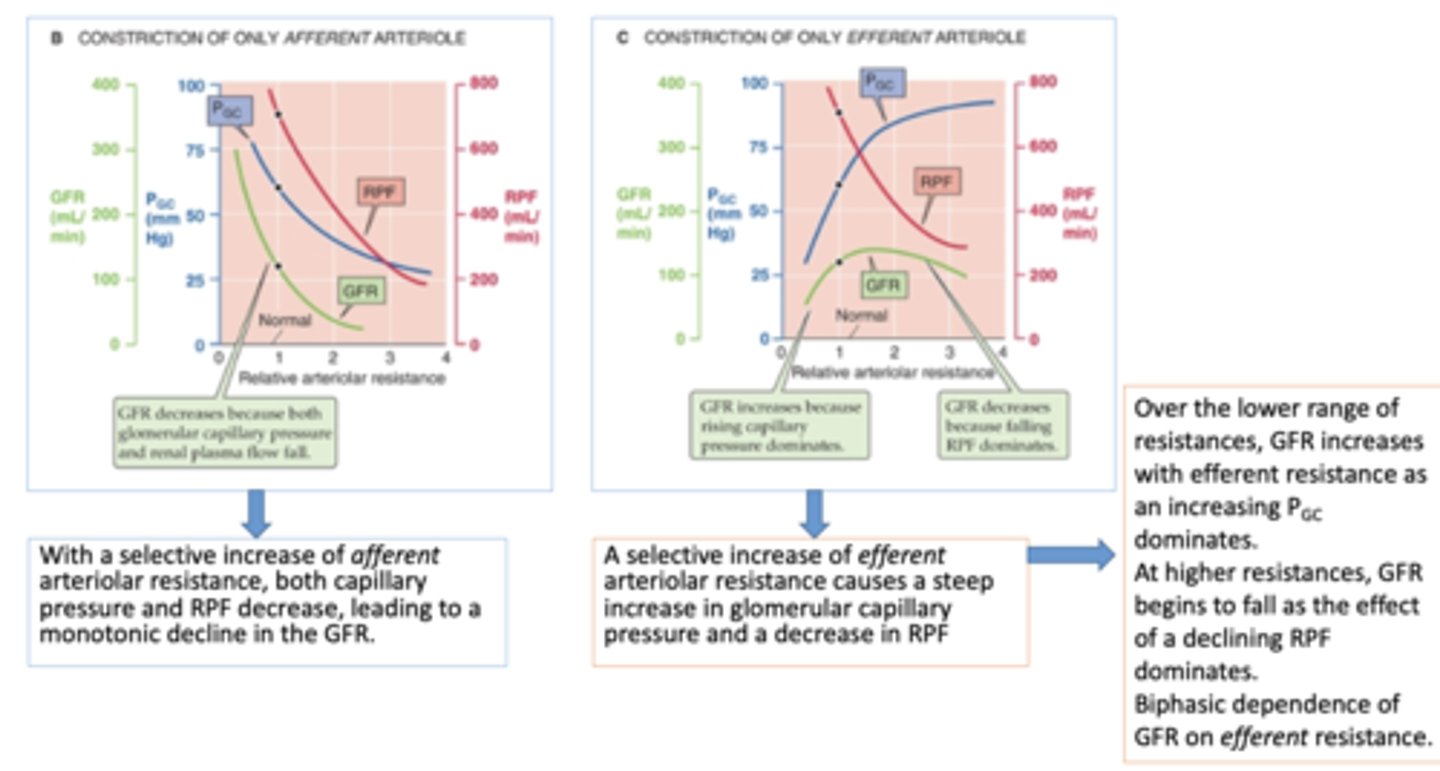
constriction on only efferent arterioles will cause a ______ in renal plasma flow
decrease
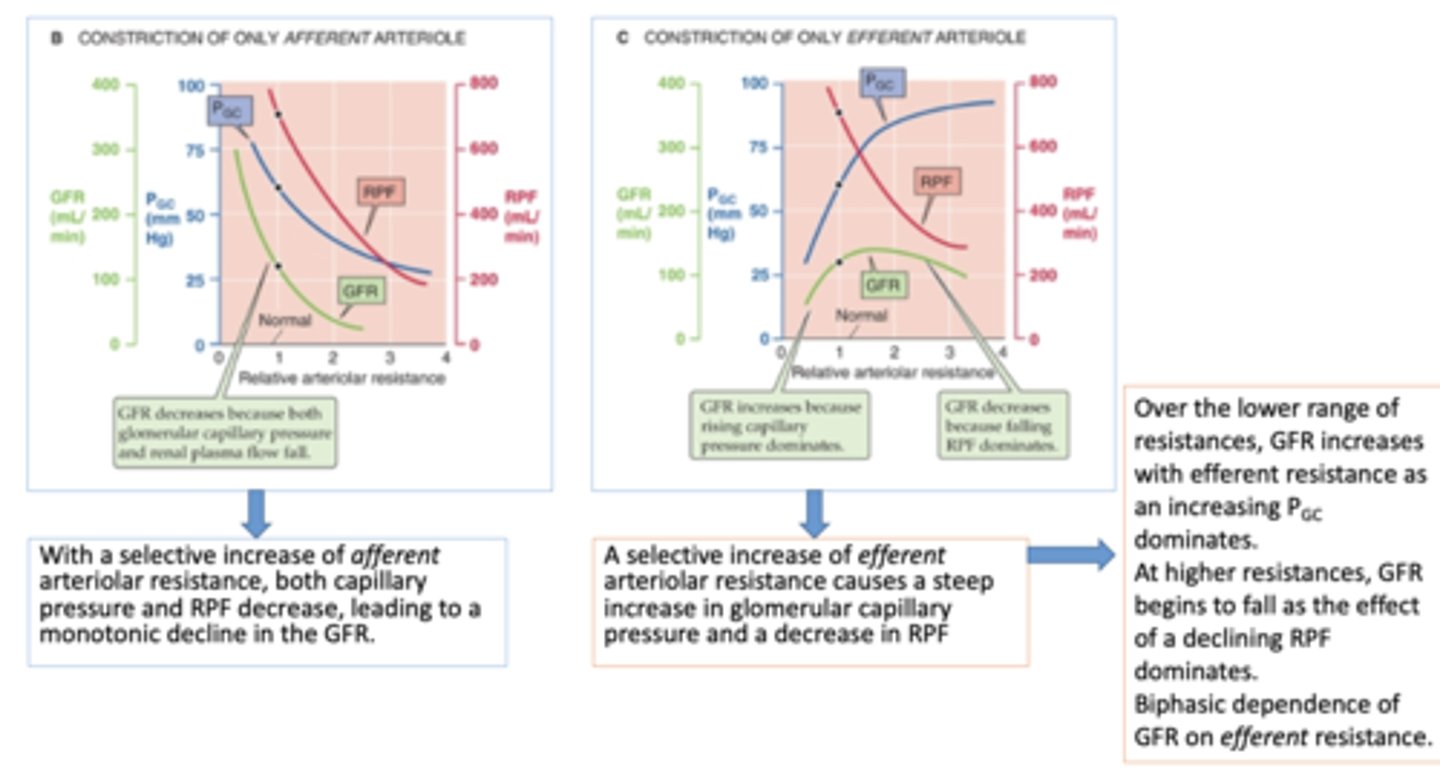
constriction on only efferent arterioles will cause a ______ in glomerular filtration rate GFR while rising capillary pressure dominates
increase
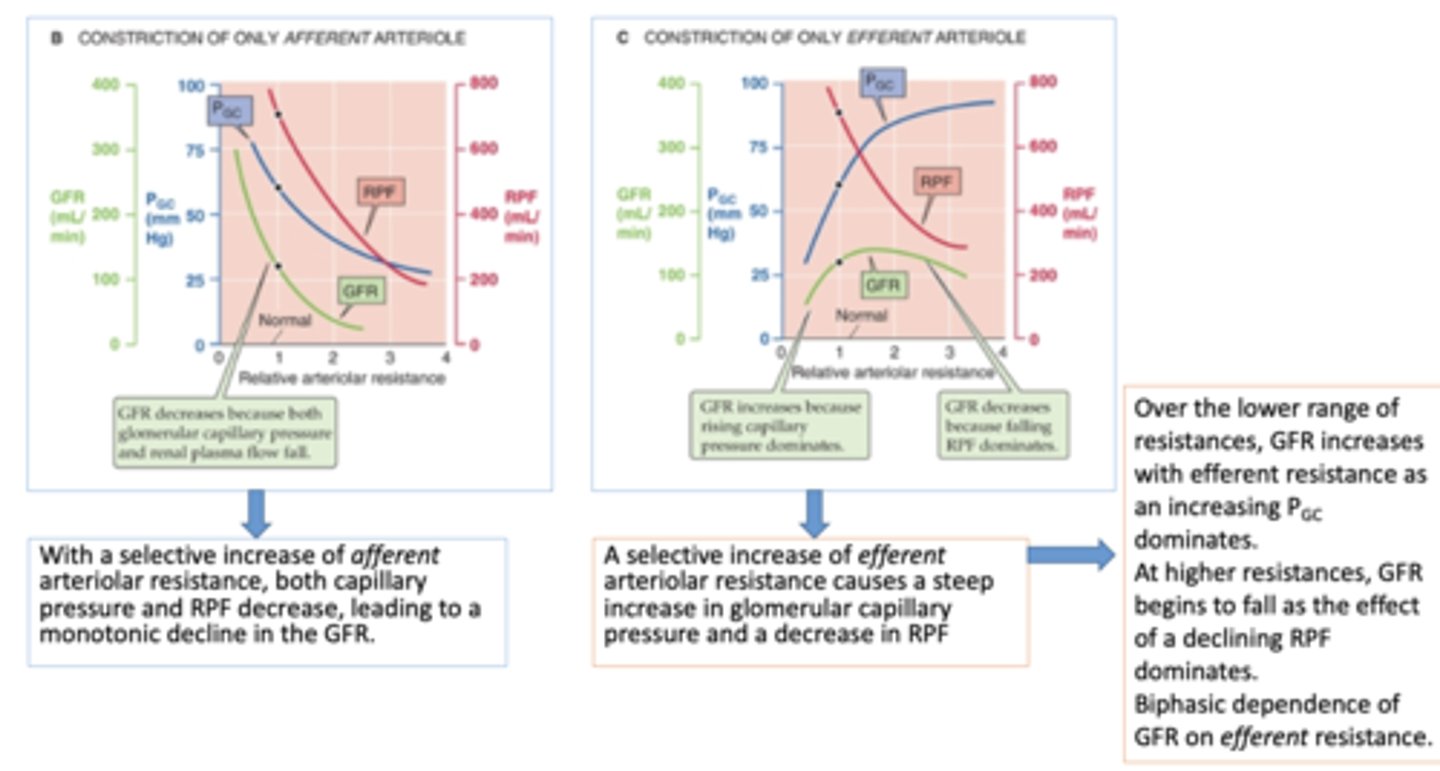
constriction on only efferent arterioles will cause a ______ in glomerular filtration rate GFR while falling RPF dominates
decrease
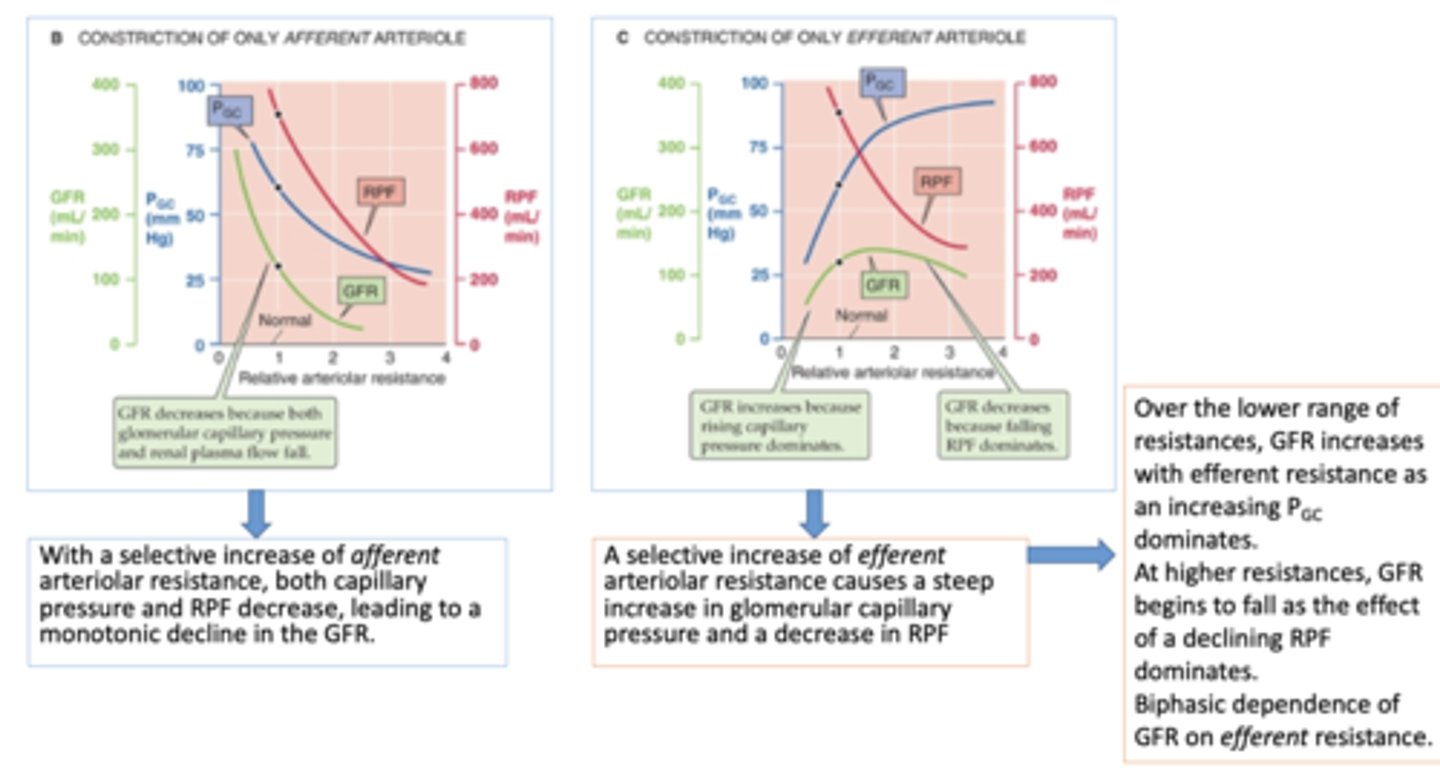
what causes the increase phase on GFR during efferent restriction?
increasing capillary pressure
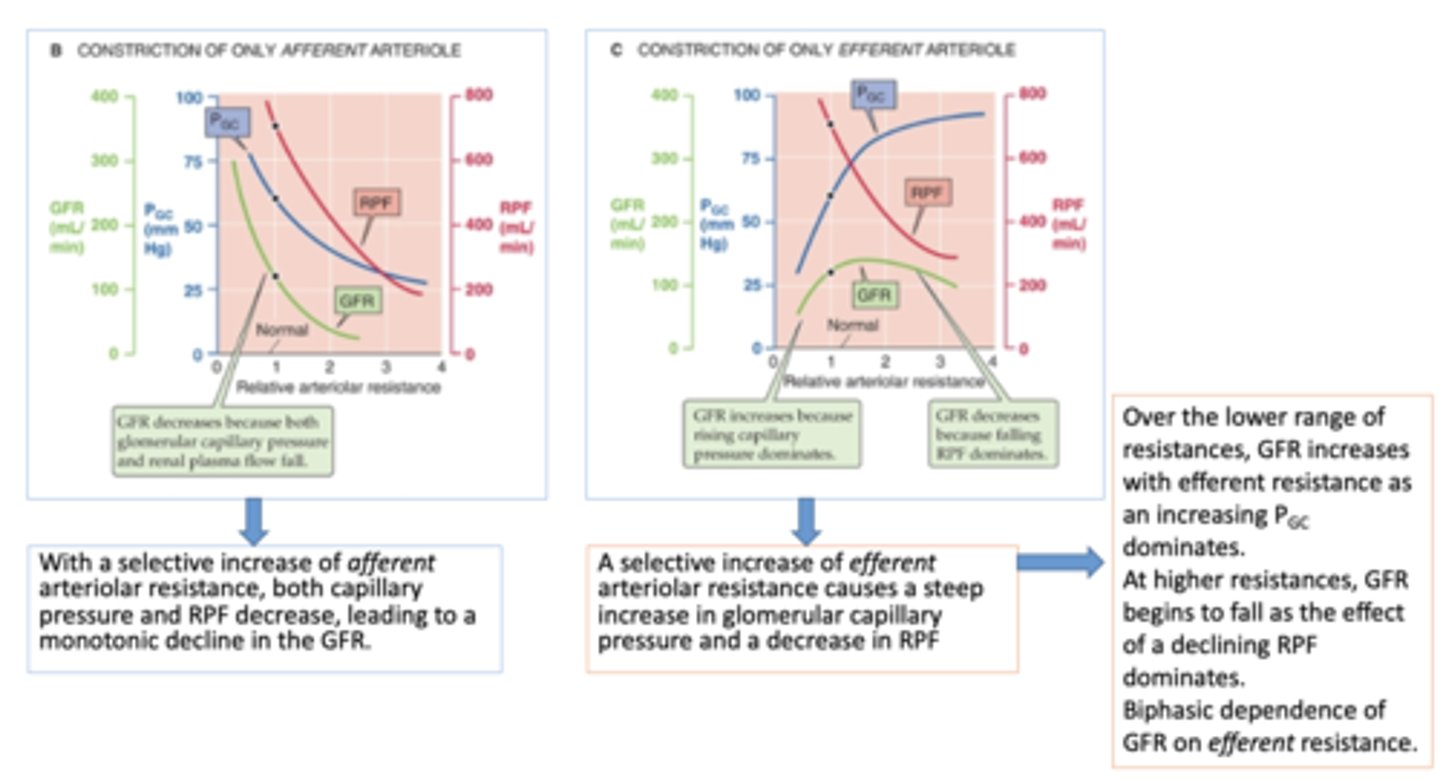
what causes the decrease phase on GFR during efferent restriction?
falling RPF dominates
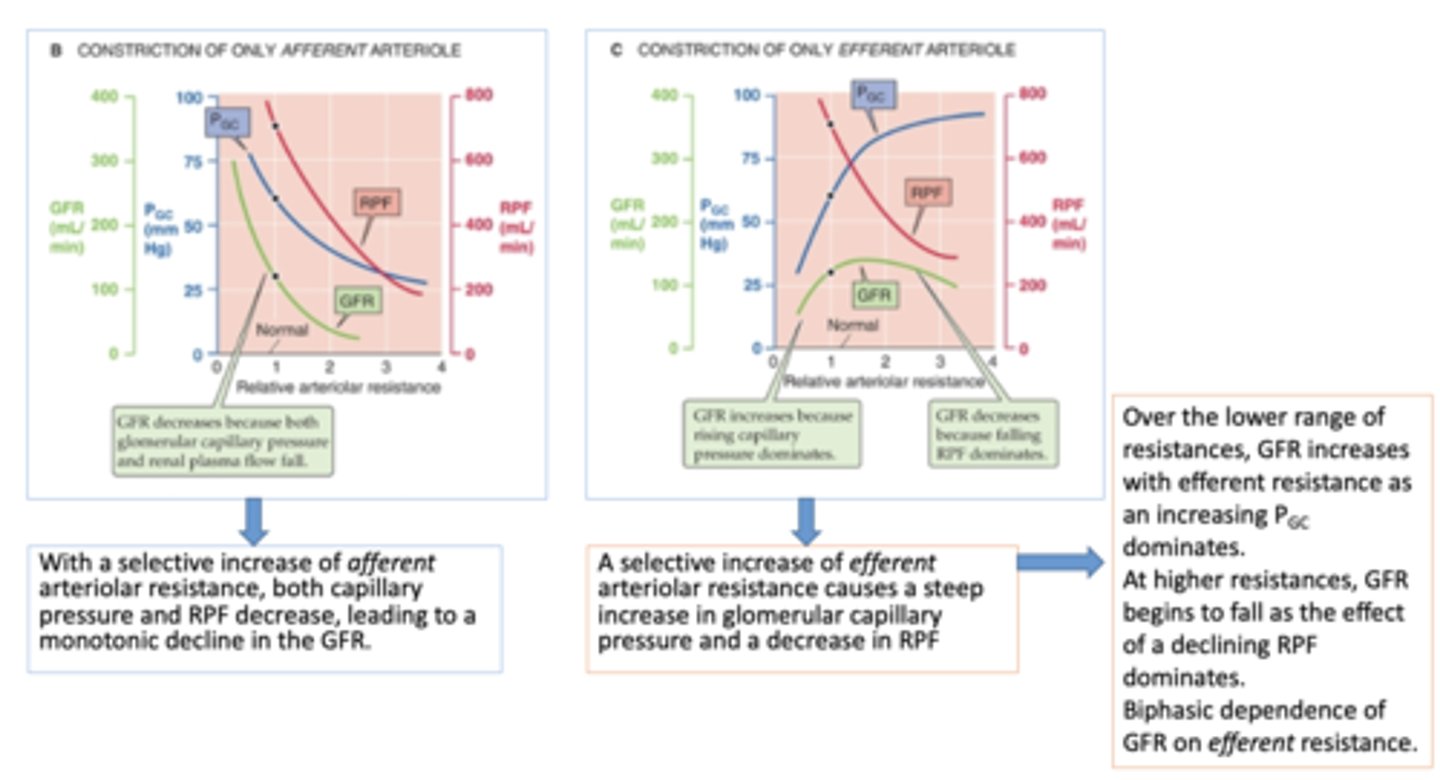
t/f: Under physiological conditions constriction of afferent or efferent arterioles do not happen in isolation
true
Afferent arteriolar resistance decreases when there is a large increase in RPF following a loss of renal tissue. A clinical example of this is ___________
kidney donation

In kidney donation, GFR in the remaining kidney _________, owing primarily to a dramatic decrease in the resistance of the afferent arteriole
nearly doubles

a realistic clinical example of predominantly efferent arteriole pressure change can be caused by...
administration of ANG II inhibitors to patients with hypertension

for reabsorption to occur in the peritubular capillaries, you need ____ hydrostatic pressure at the capillary bed
low
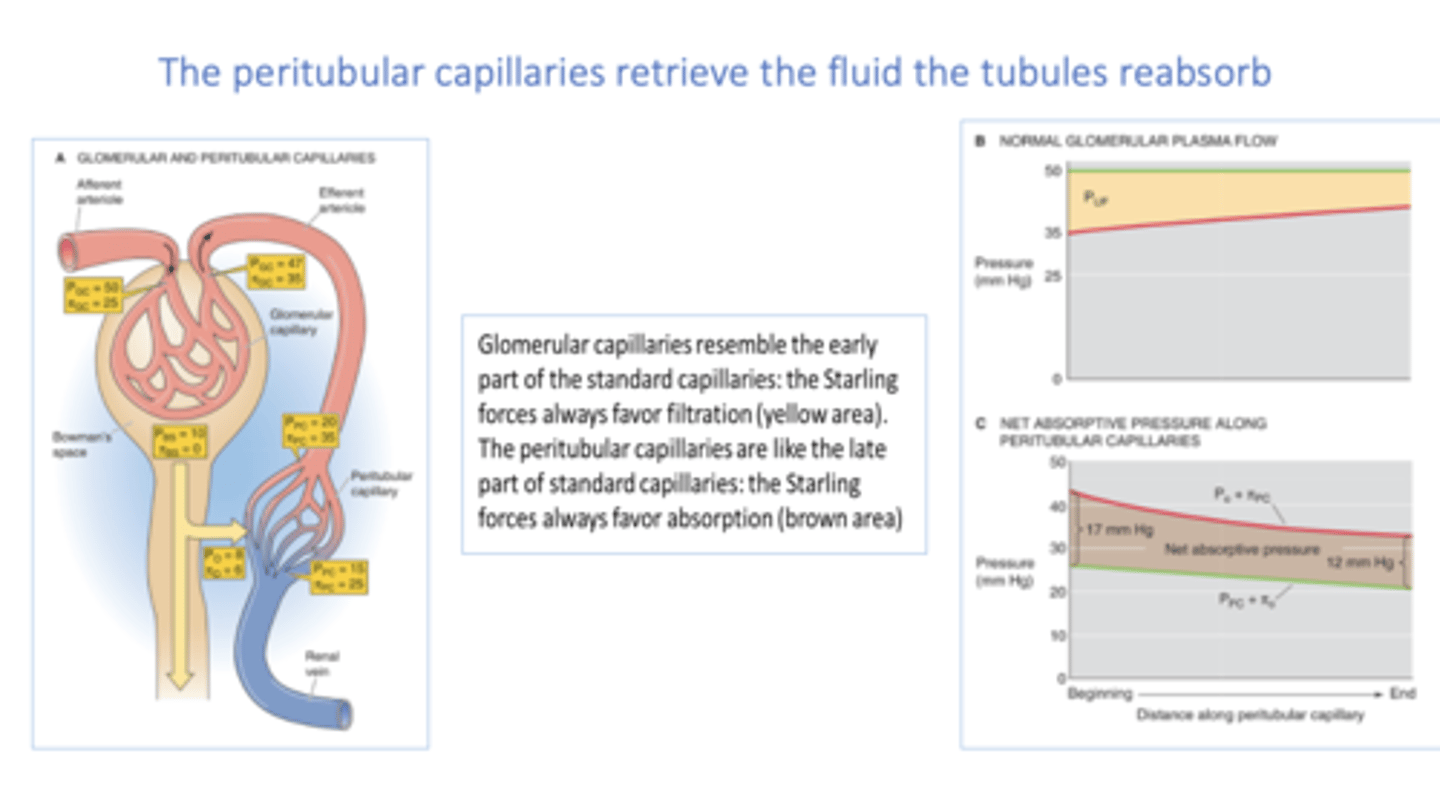
for reabsorption to occur in the peritubular capillaries, you need ____ oncotic pressure at the capillary bed
high
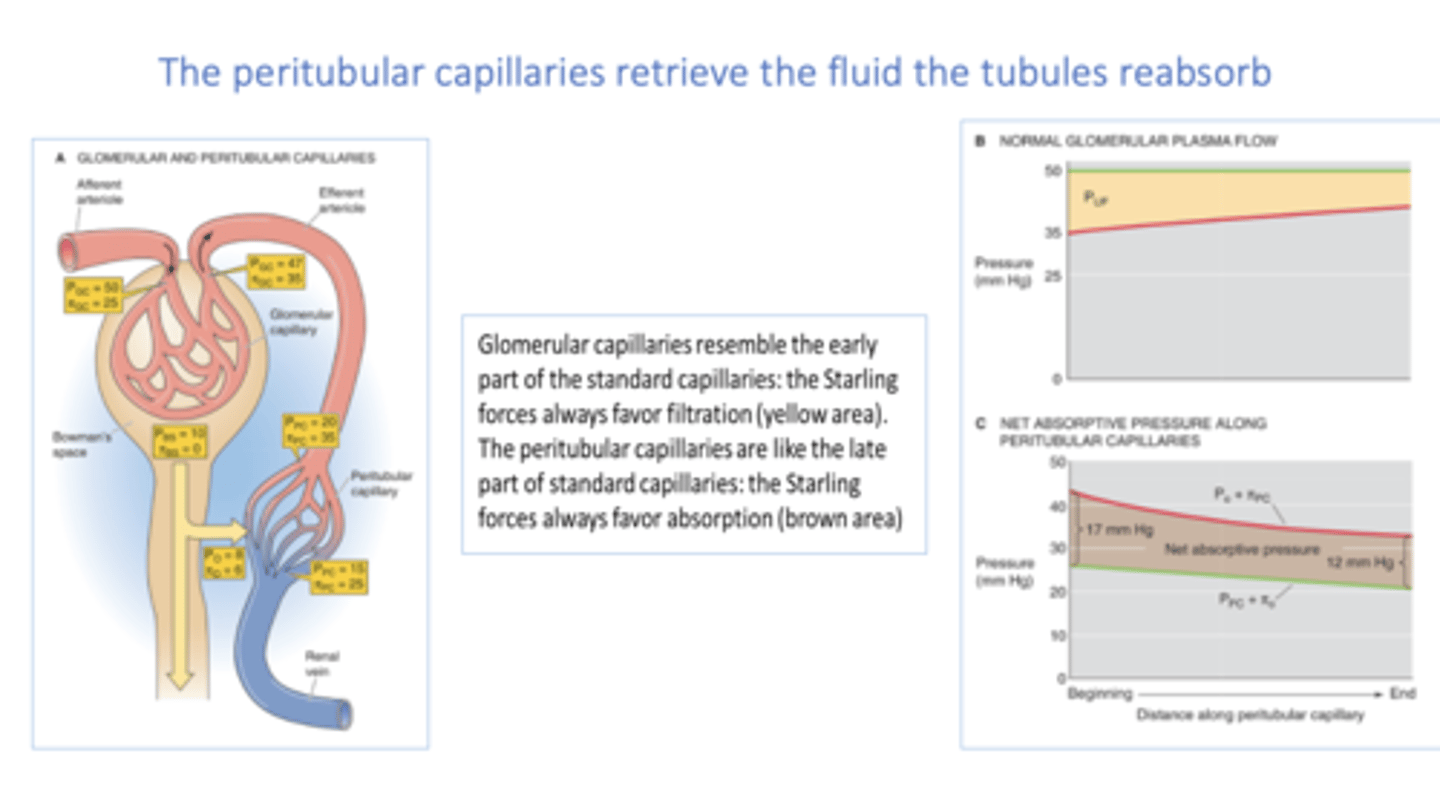
volume expansion effect on oncotic pressure entering peritubular capillaries:
decrease
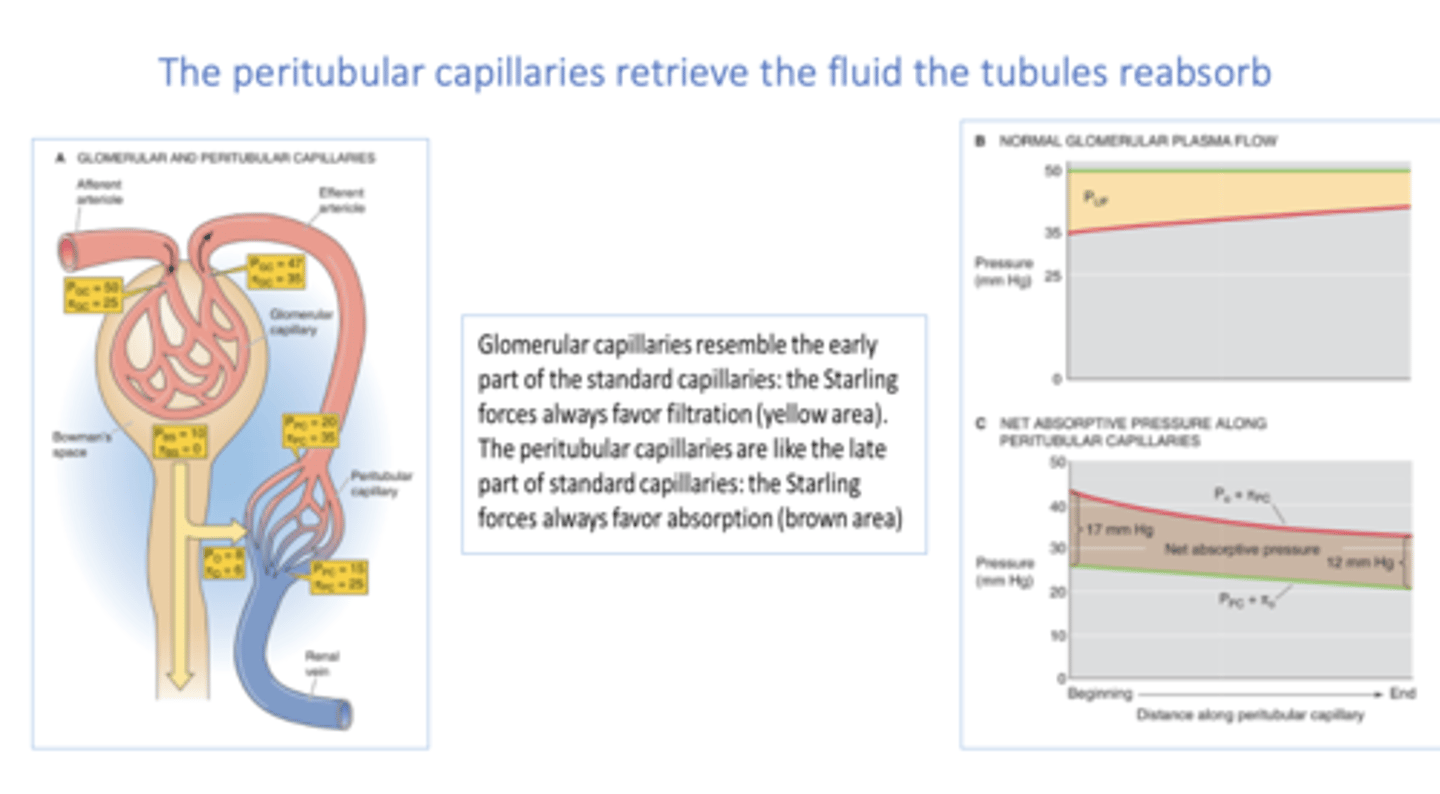
volume expansion effect on hydrostatic pressure entering peritubular capillaries:
increase
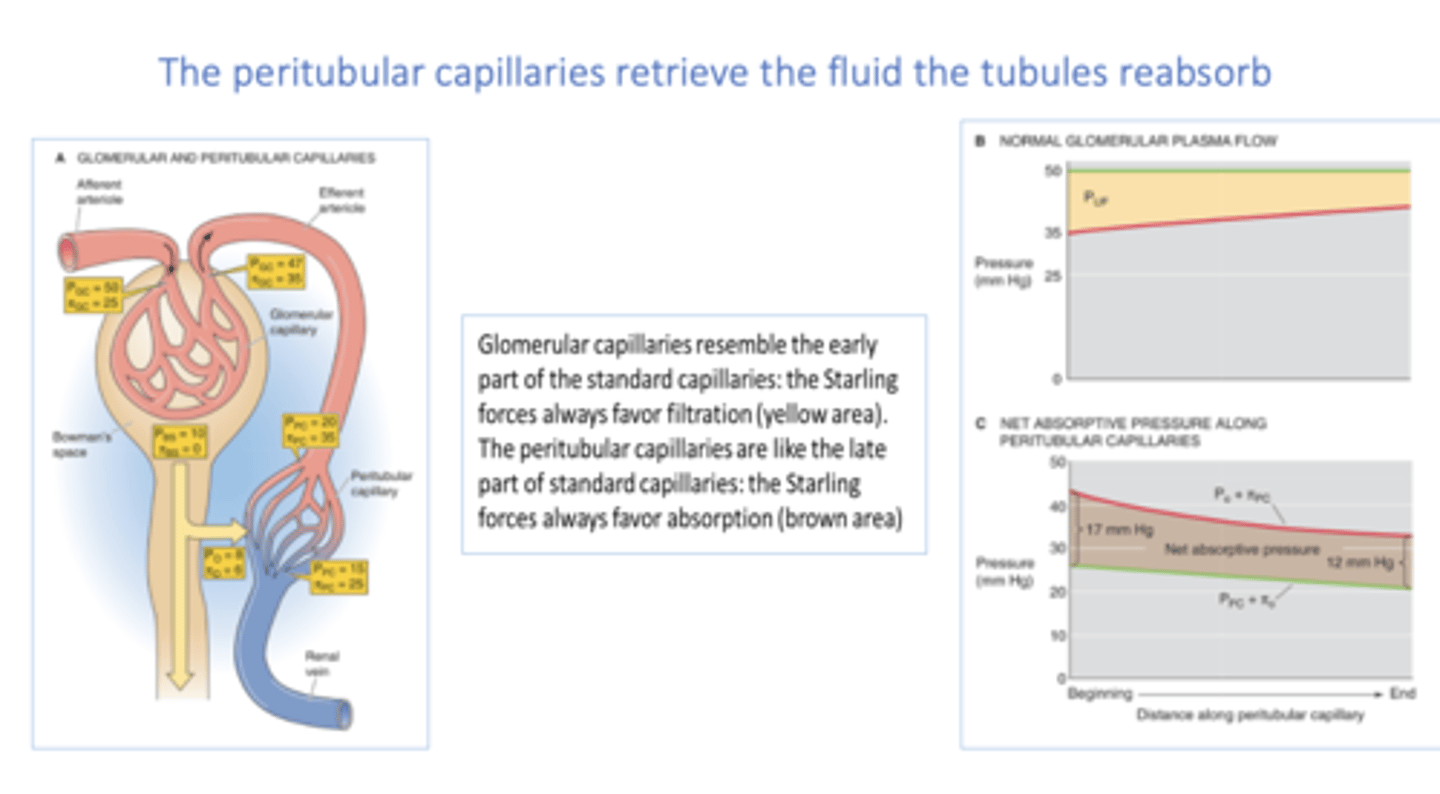
a ______ in oncotic pressure and a ______ in hydrostatic pressure will decrease fluid uptake by peritubular capillaries
decrease, increase
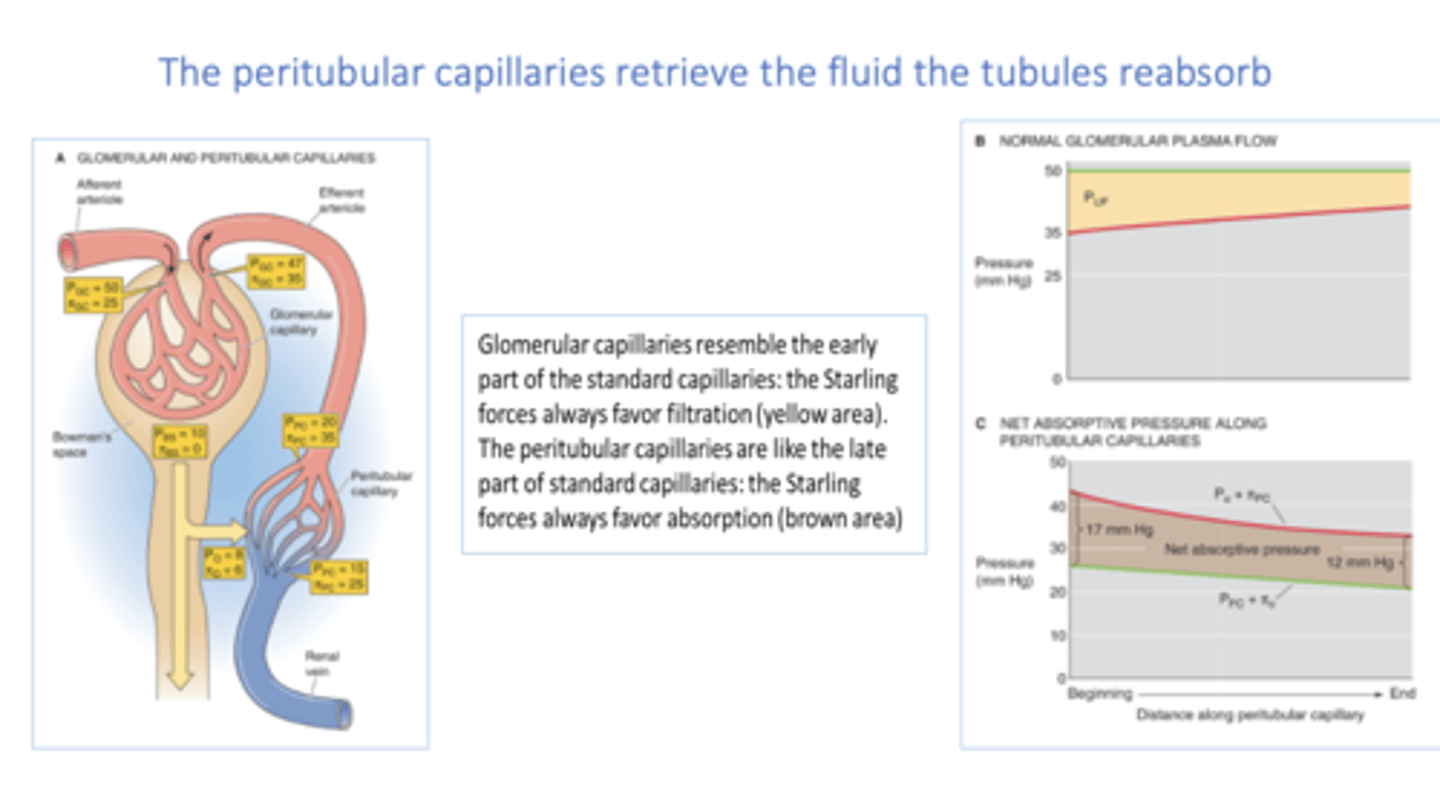
a ______ in oncotic pressure and a ______ in hydrostatic pressure will increase fluid uptake by peritubular capillaries
increase, decrease
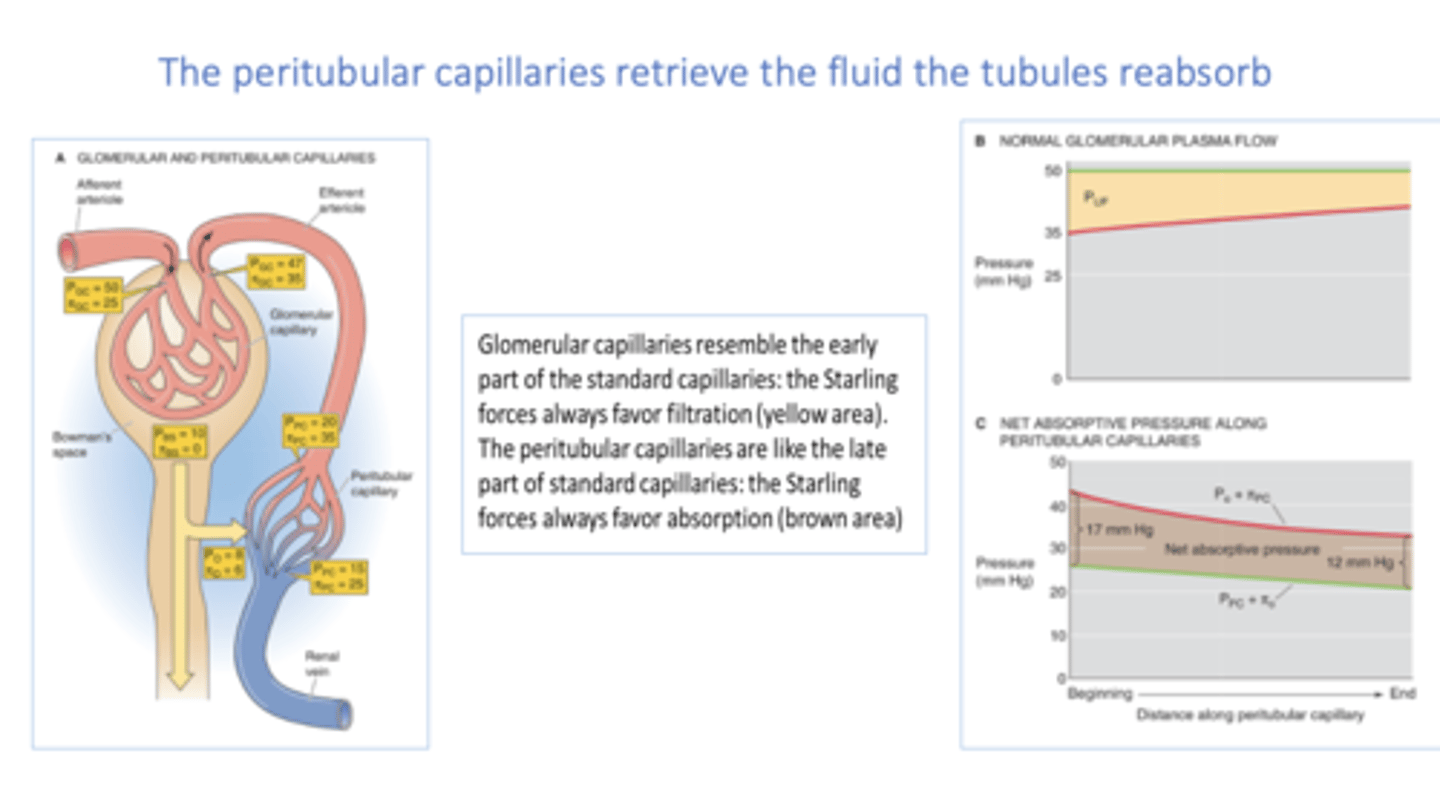
The _____________ provide nutrients for tubules and retrieve the fluid the tubules reabsorb
peritubular capillaries
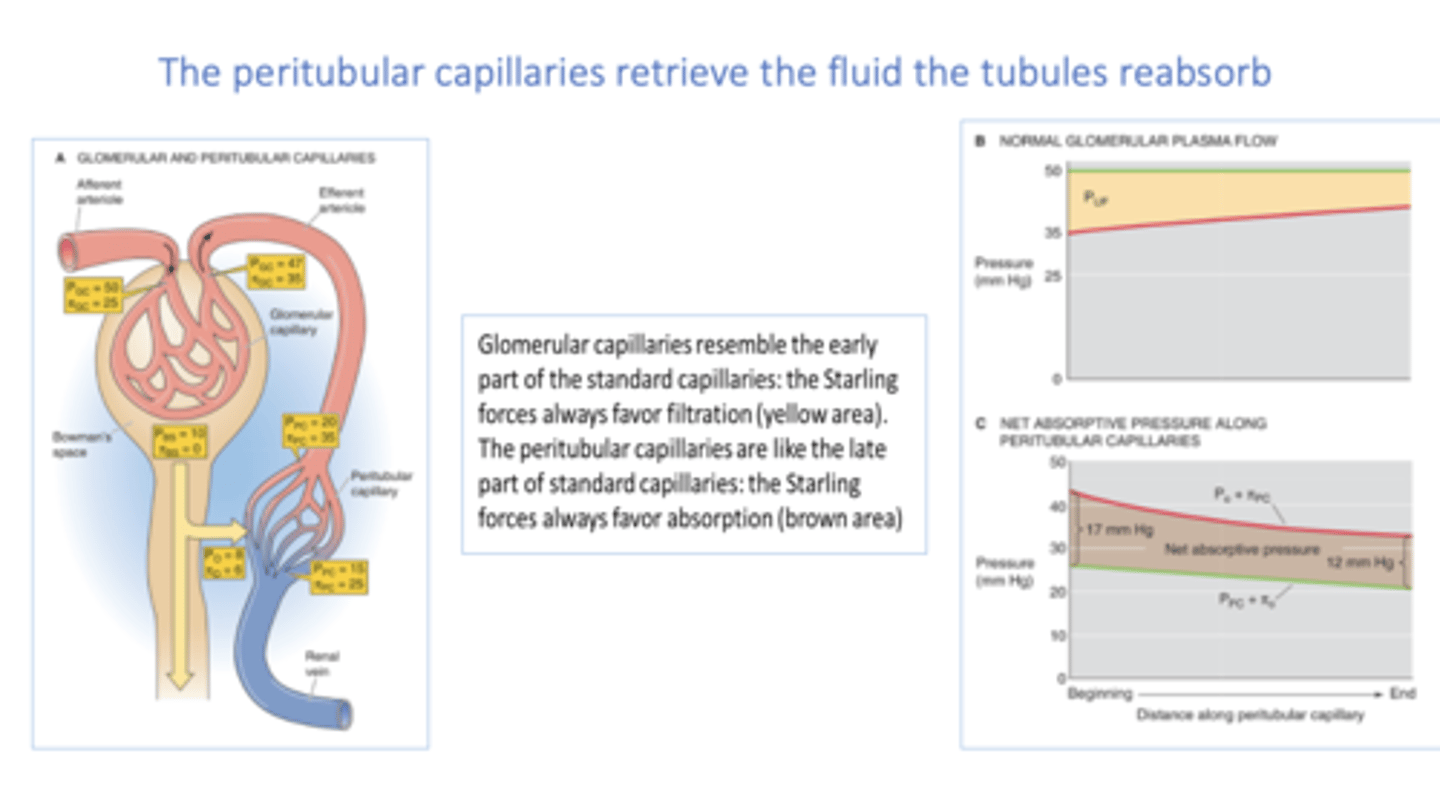
The clearance of p-aminohippurate (PAH) is a measure of ____________
Renal Plasma Flow (RPF)
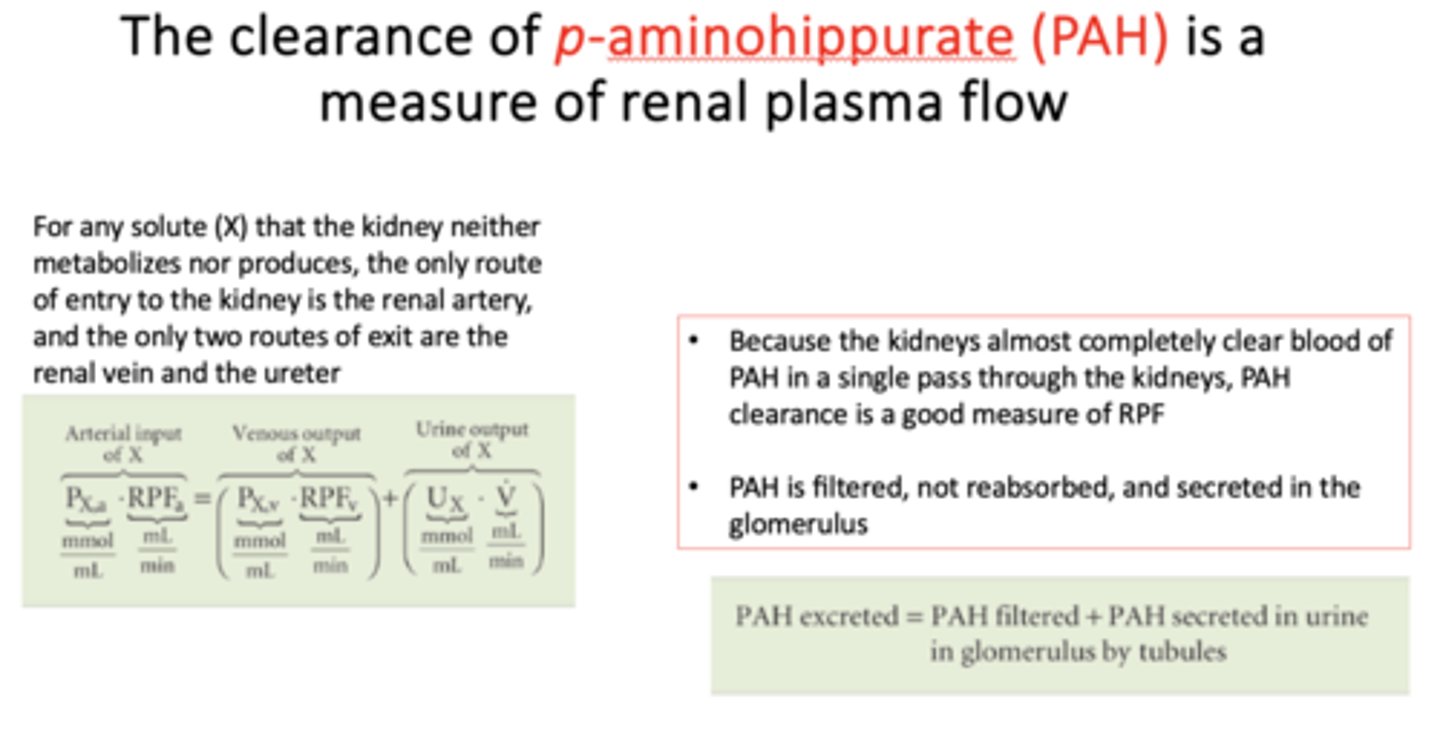
The clearance of ____________ is a measure of renal plasma flow
p-aminohippurate (PAH)
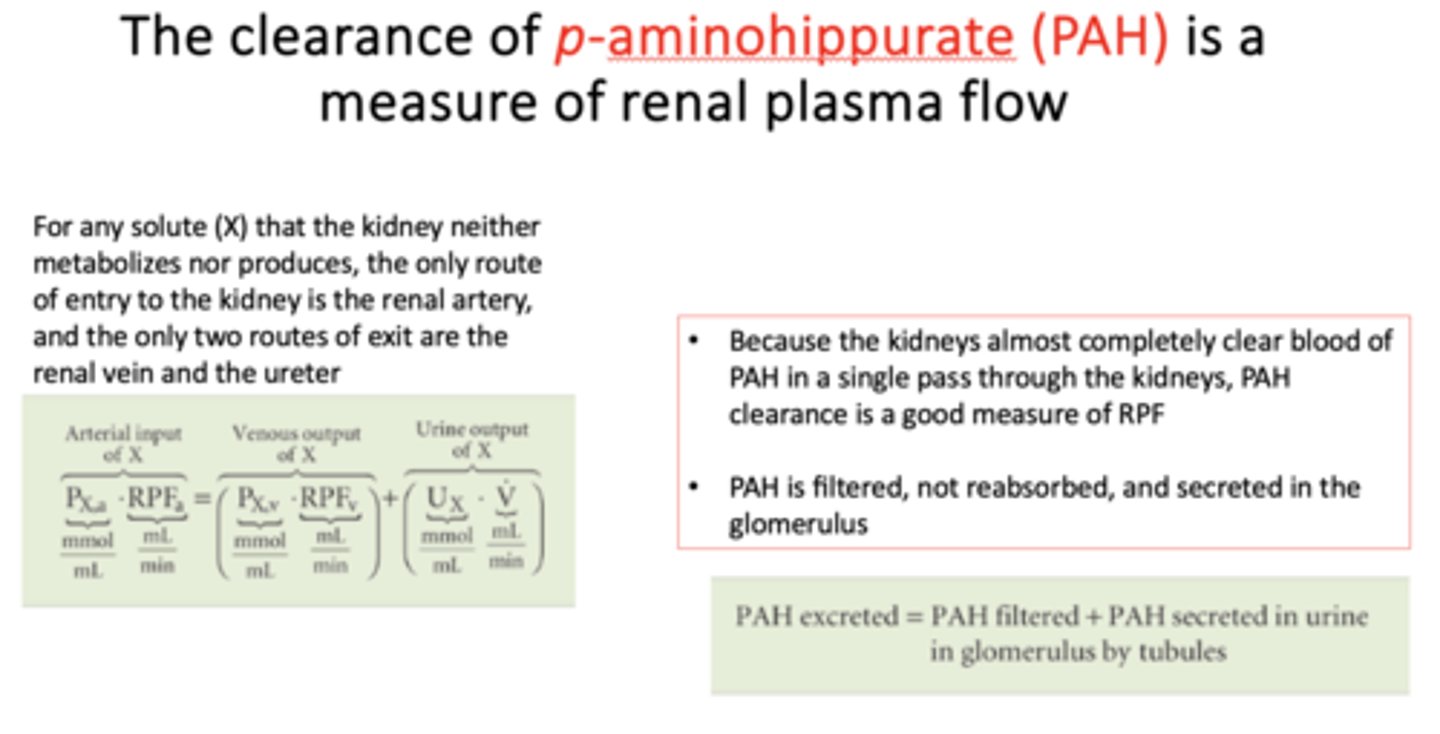
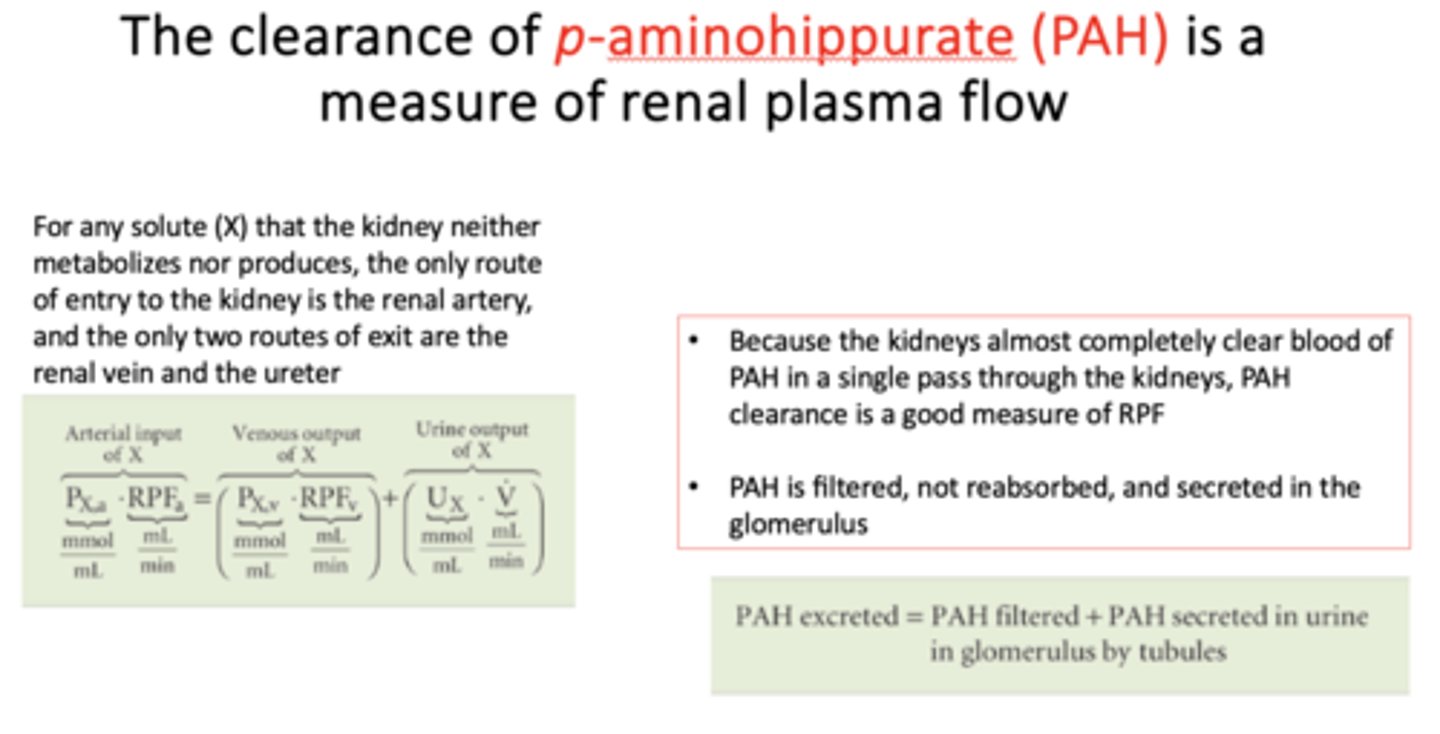
p-aminohippurate (PAH) is ______ and _____by glomerulus
A. Secreted
B. Filtered
C. Reabsorbed
A & B (filtered, secreted only; not reabsorbed)
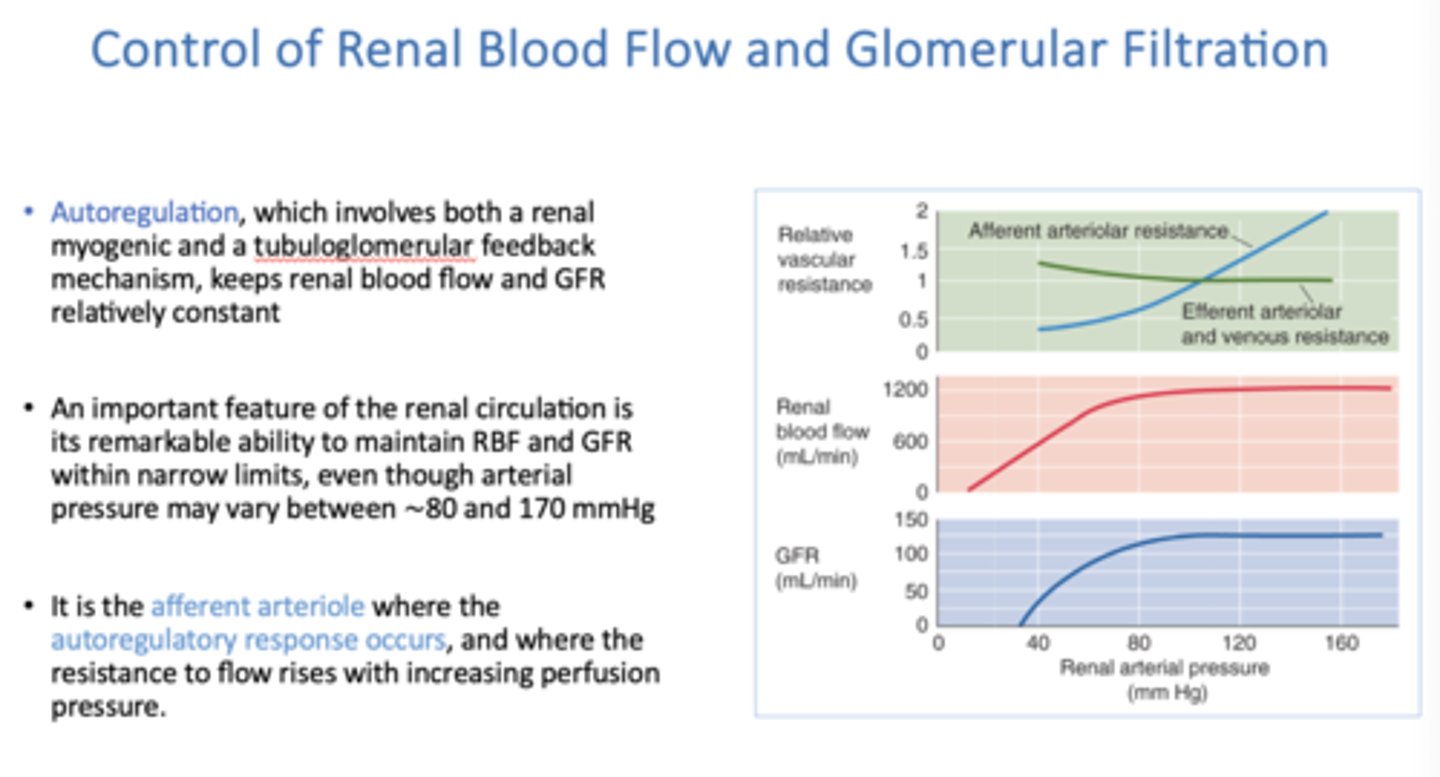
_____________ involves both a renal myogenic and a tubuloglomerular feedback mechanism, keeps renal blood flow and GFR relatively constant
Autoregulation
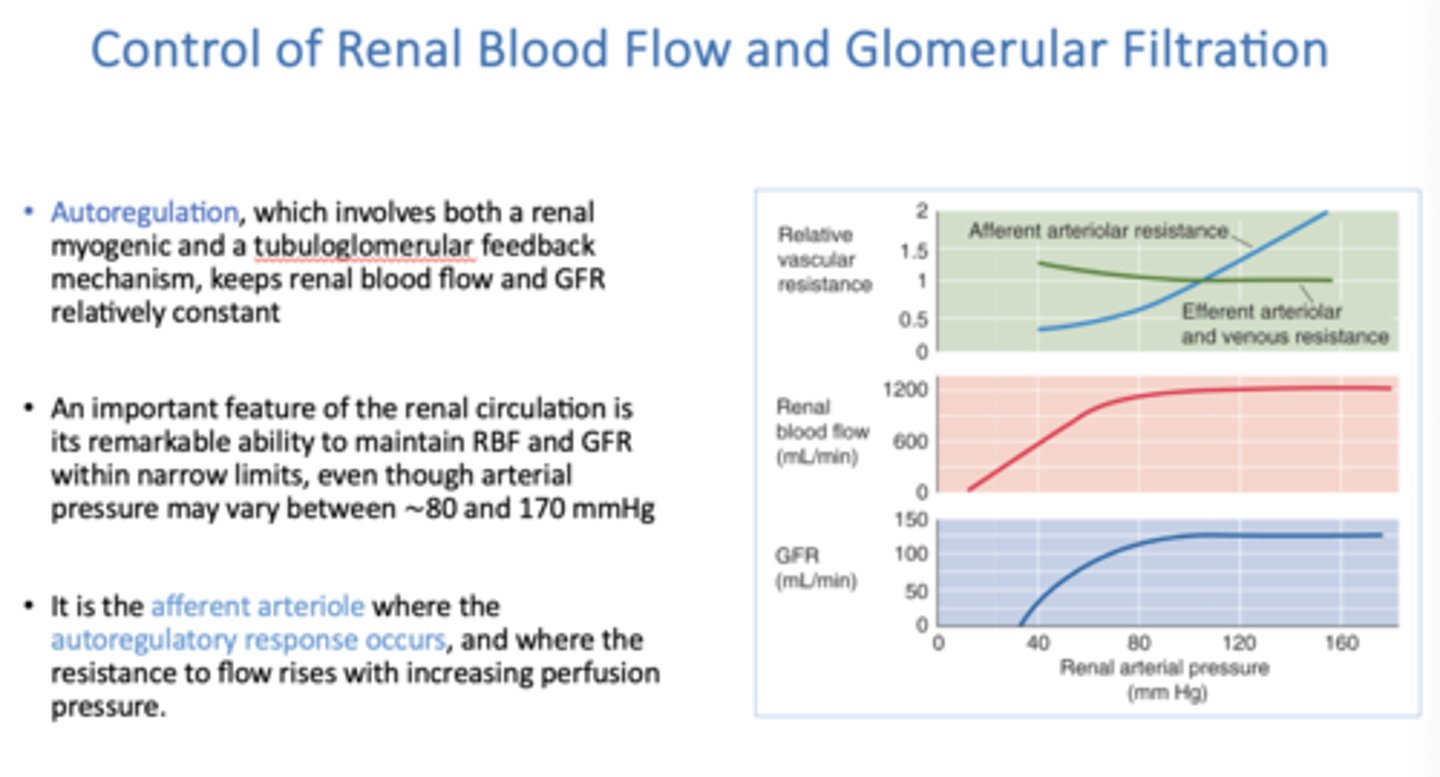
autoregulation of BP acts on what blood vessel?
afferent arteriole
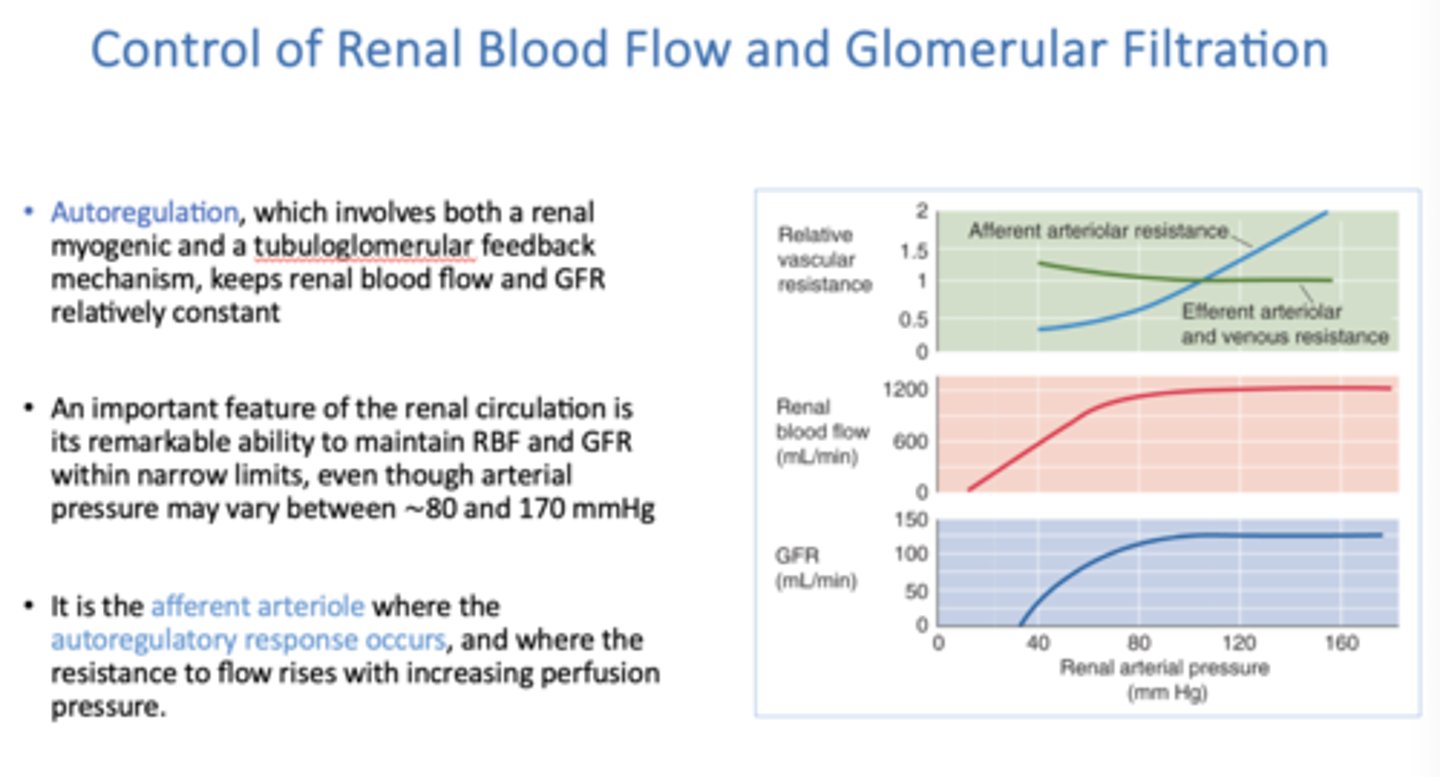
Two basic mechanisms underlie renal autoregulation:
- Renal myogenic response of the smooth muscle of the afferent arterioles,
- Tubuloglomerular feedback (TGF) mechanism

where does the autoregulatory response occur, and where does the resistance to flow rises with increasing perfusion pressure?
afferent arteriole
What mechanism is the following?
- The afferent arterioles have the ability to respond to changes in vessel circumference by contracting or relaxing
- The mechanism of contraction is the opening of stretch-activated, nonselective cation channels in vascular smooth muscle.
- The resultant depolarizing leads to an influx of Ca2+ that stimulates contraction
myogenic response

The ___________ mediates the TGF mechanism
juxtaglomerular apparatus

What mechanism is the following?
The macula densa cells sense an increase in GFR and, with feedback, translate this to a contraction of the afferent arteriole, a fall in Pgc and RPF, and hence a decrease in GFR
tubuloglomerular feedback (TGF) mechanism
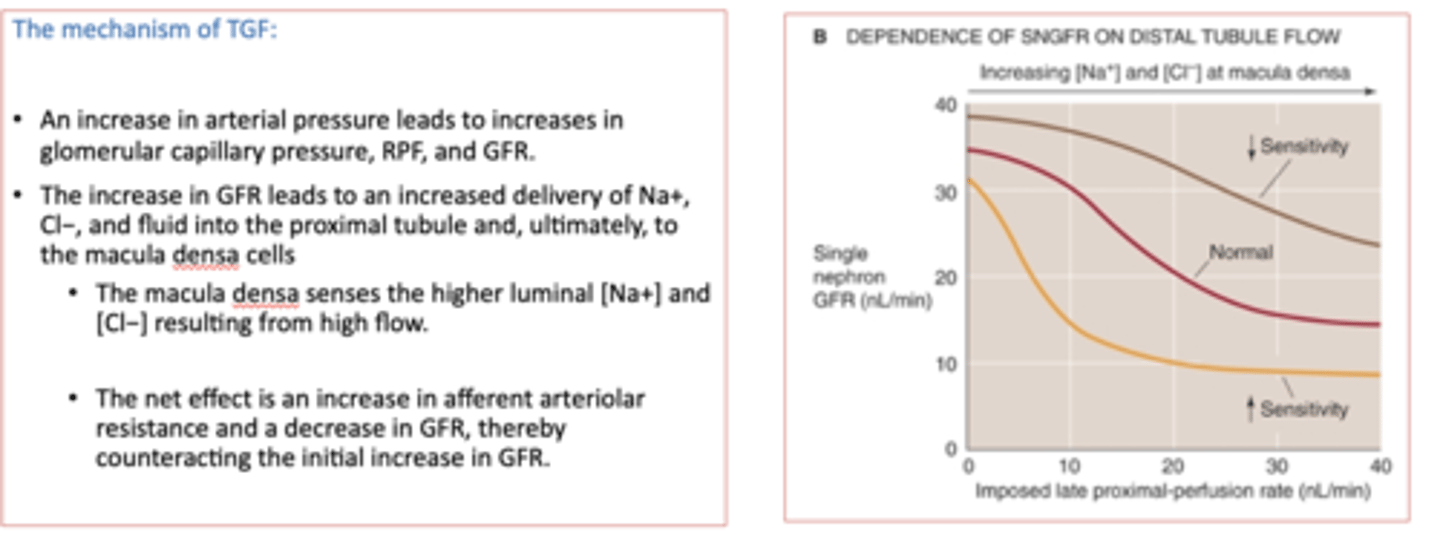
the myogenic response is mediated by what ion?
Ca++

if the sensitivity of the tubuloglomerular feedback (TGF) mechanism increases it will _____ the GFR
decrease
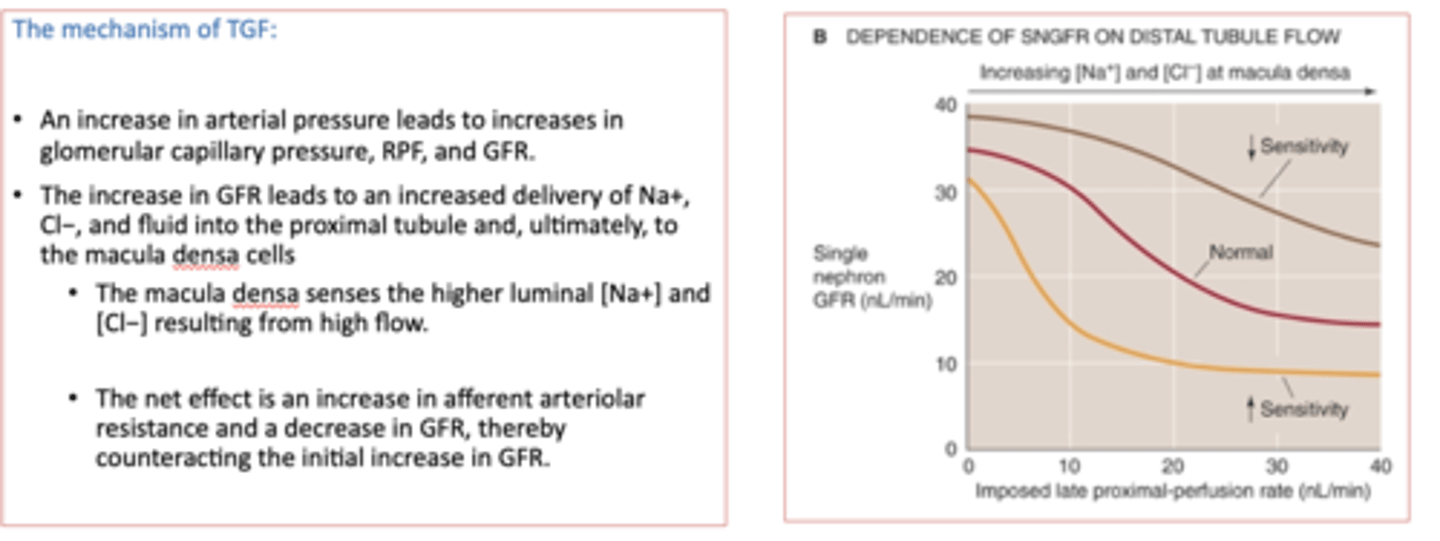
if the sensitivity of the tubuloglomerular feedback (TGF) mechanism decreases it will _____ the GFR
increase
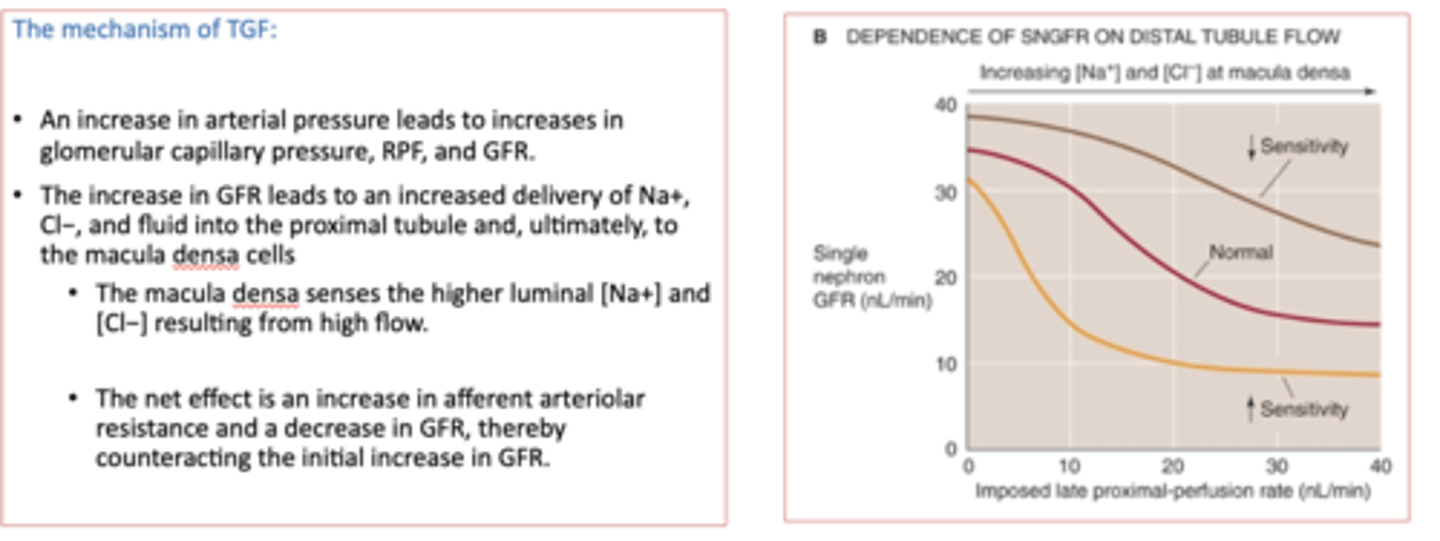
there is a ______ relationship between the tubuloglomerular feedback (TGF) mechanism and GFR
inverse
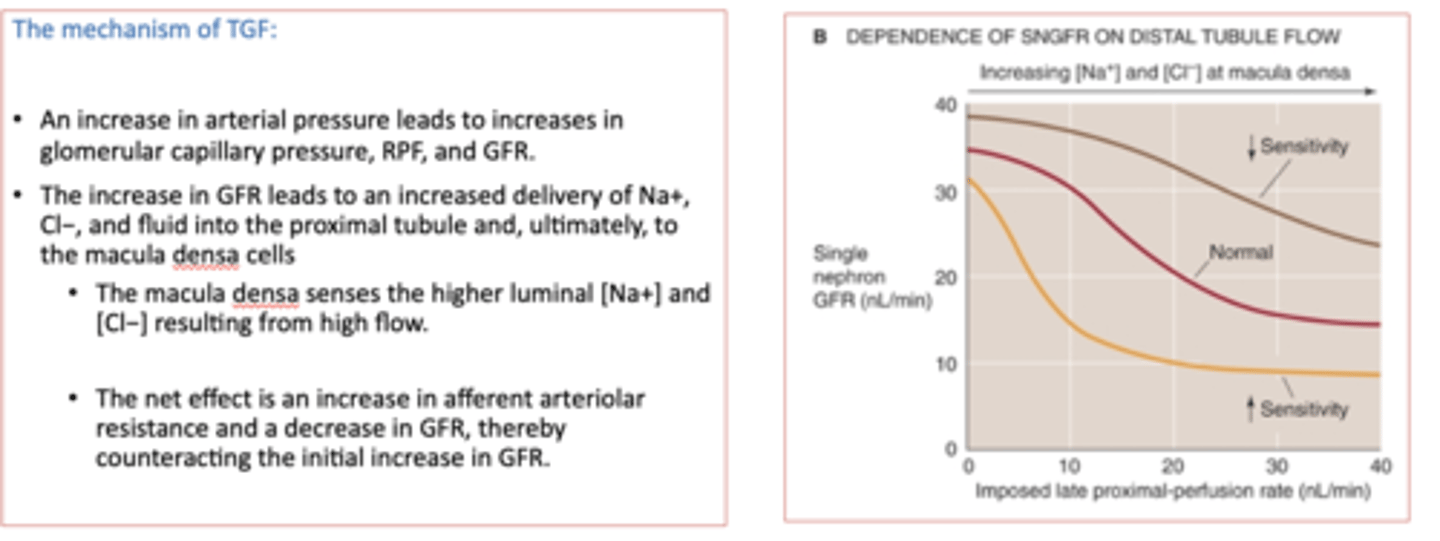
tubuloglomerular feedback (TGF) mechanism causes ________ of the afferent arterioles
vasoconstriction
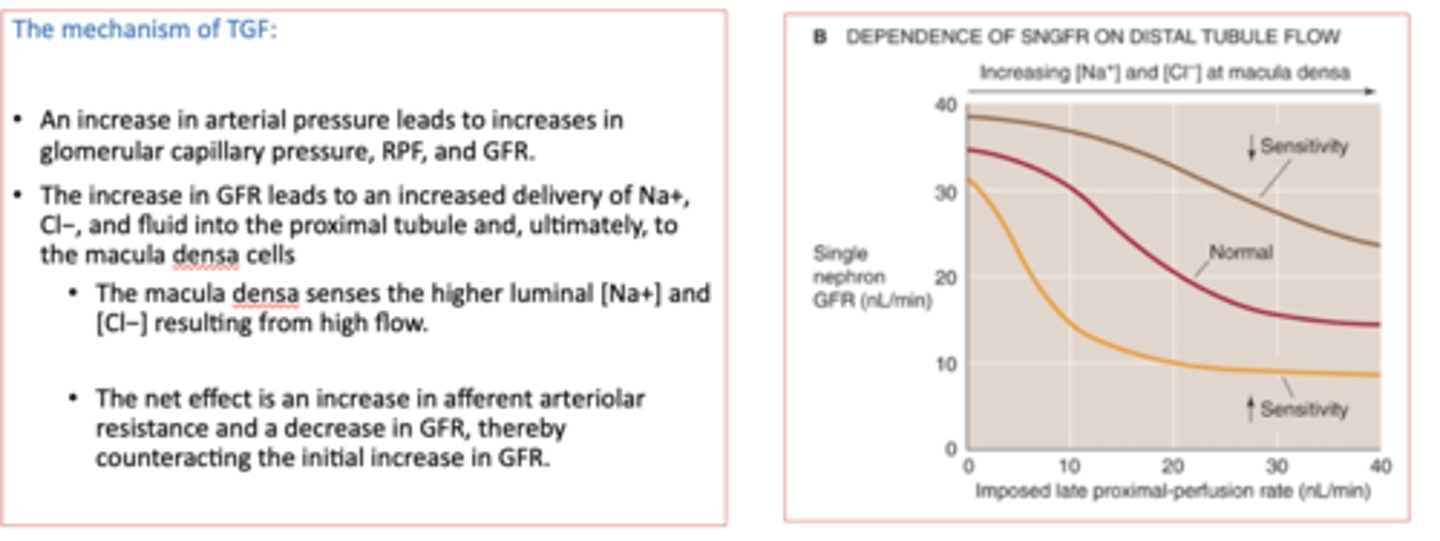
Four factors that modulate renal blood flow and GFR play key roles in regulating effective circulating volume:
(1) Renin-angiotensin-aldosterone axis
(2) Sympathetic nervous system
(3) Arginine vasopressin (AVP or antidiuretic hormone, ADH)
(4) Atrial natriuretic peptide (ANP)

in the Renin-angiotensin-aldosterone axis, angiotensinogen is made by the __________ and released into the blood
liver

in the Renin-angiotensin-aldosterone axis, renin is made by the _______________
juxtaglomerular cells

in the Renin-angiotensin-aldosterone axis, renin is stored in the _______________
juxtaglomerular apparatus

in the Renin-angiotensin-aldosterone axis, Angiotensin-converting enzyme (ACE) is made by the:
lungs

in the Renin-angiotensin-aldosterone axis, aldosterone is made by the:
adrenal cortex

_____________ catalyzes the conversion of angiotensinogen to angiotensin I
renin

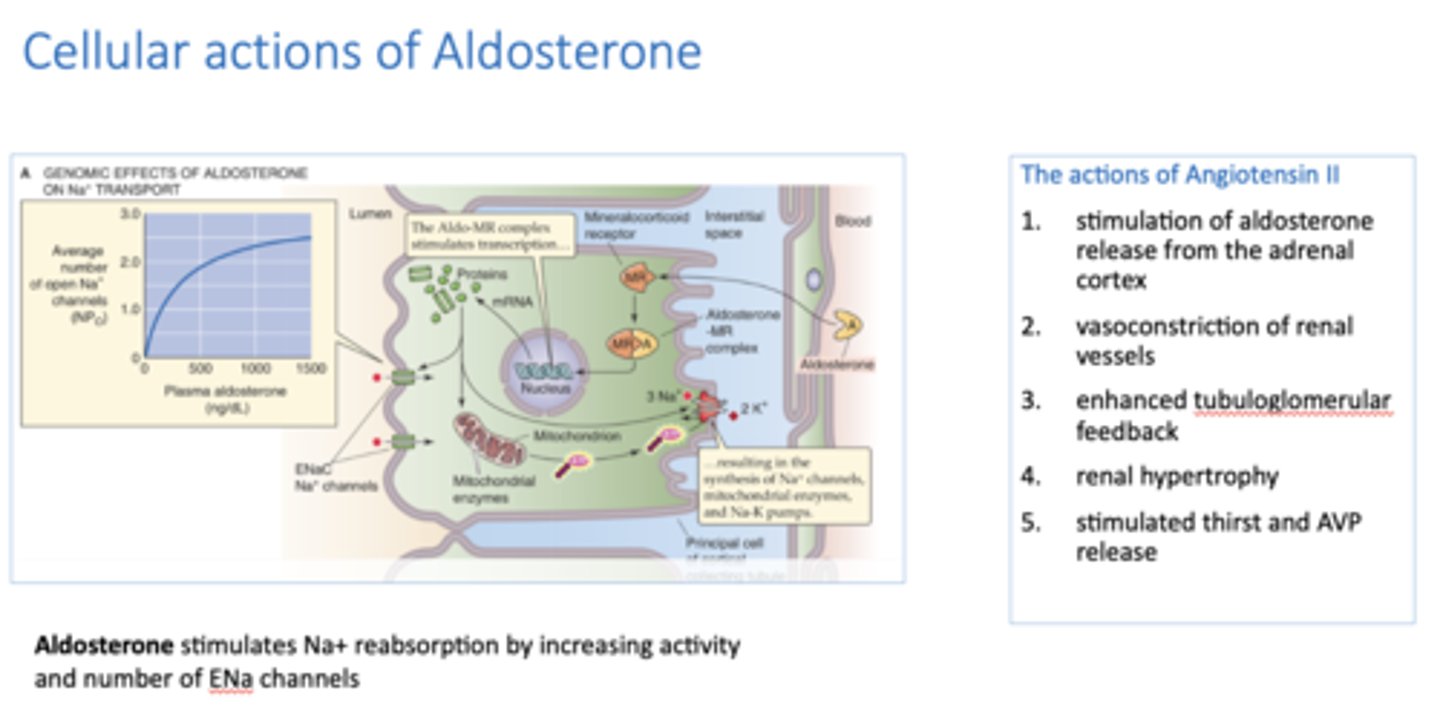
_________ stimulates Na+ reabsorption by increasing activity and number of ENa channels
aldosterone

aldosterone stimulates ______ reabsorption by the initial tubule and the CCT, and by medullary collecting duct
Na+

What can lead to severe Na+ depletion, contraction of the ECF volume, and circulatory insufficiency?
lack of aldosterone that occurs in adrenal insufficency (aka Addison Disease)

These are the cellular actions of what?
1. stimulation of aldosterone release from the adrenal cortex
2. vasoconstriction of renal vessels
3. enhanced tubuloglomerular feedback
4. renal hypertrophy
5. stimulated thirst and AVP release
Angiotensin II
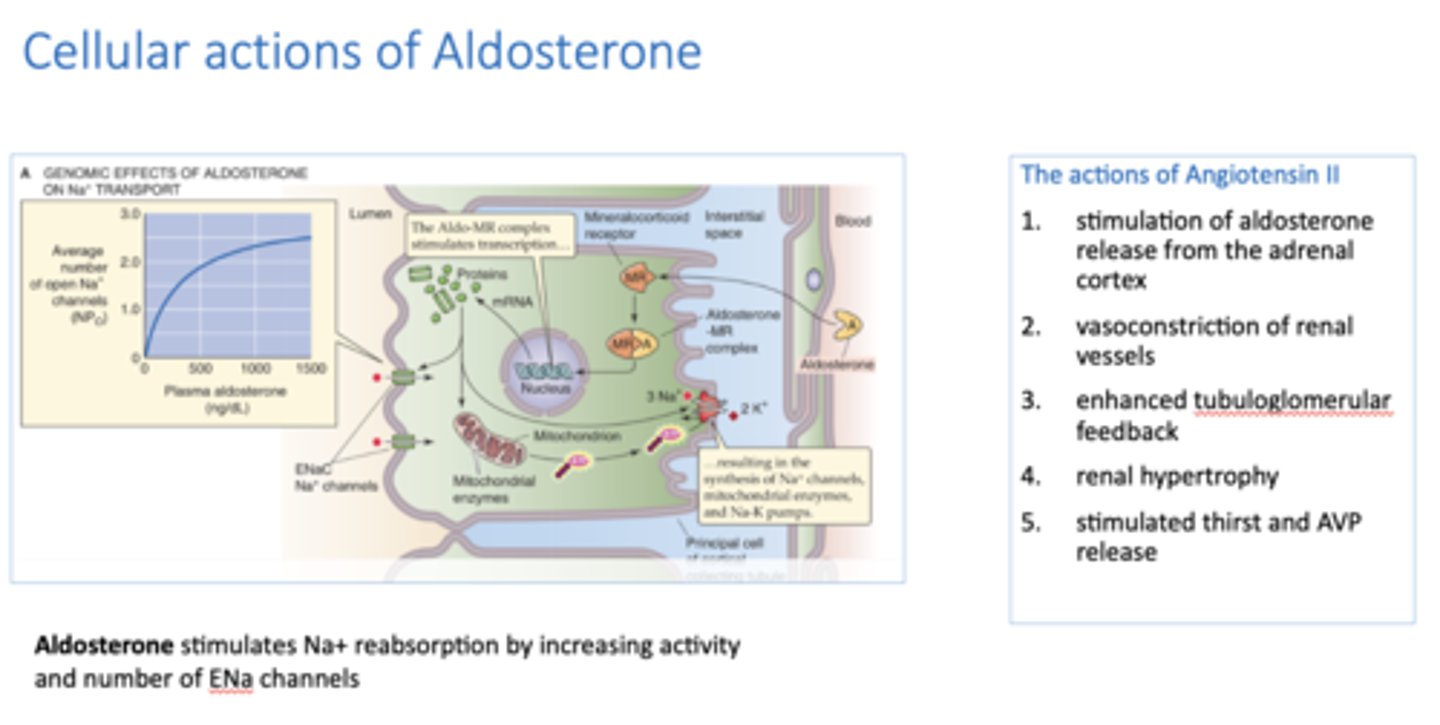
____________ stimulates Na+ reabsorption by increasing activity and number of ENa channels
Aldosterone
sympathetic system will ______________ both afferent and efferent arteriolar resistances
increase

sympathetic stimulation on the kidneys will cause a ______________ in afferent and efferent resistance, decreasing RBF and GFR
increase

sympathetic stimulation on the kidneys will cause a ______________ on RBF
decrease

sympathetic stimulation on the kidneys will cause a ______________ on GFR
decrease

With maximal nerve stimulation, however, afferent vasoconstriction predominates and leads to drastic reductions in both _________ and _________
RBF, GFR

In response to increases in the osmotic pressure of the extracellular fluid, the posterior pituitary releases ______________
arginine vasopressin (aka ADH)

main goal of this polypeptide is to increase water absorption in the collecting ducts
arginine vasopressin (aka ADH)

Despite physiological fluctuations of circulating AVP levels, total RBF and GFR will:
remain constant

__________ may decrease blood flow to the renal medulla, thereby minimizing the washout of the hypertonic medulla; this hypertonicity is essential for forming a concentrated urine.
arginine vasopressin (aka ADH)

_________ inserts aquaporin channels to the apical side of tubular cells
AVP
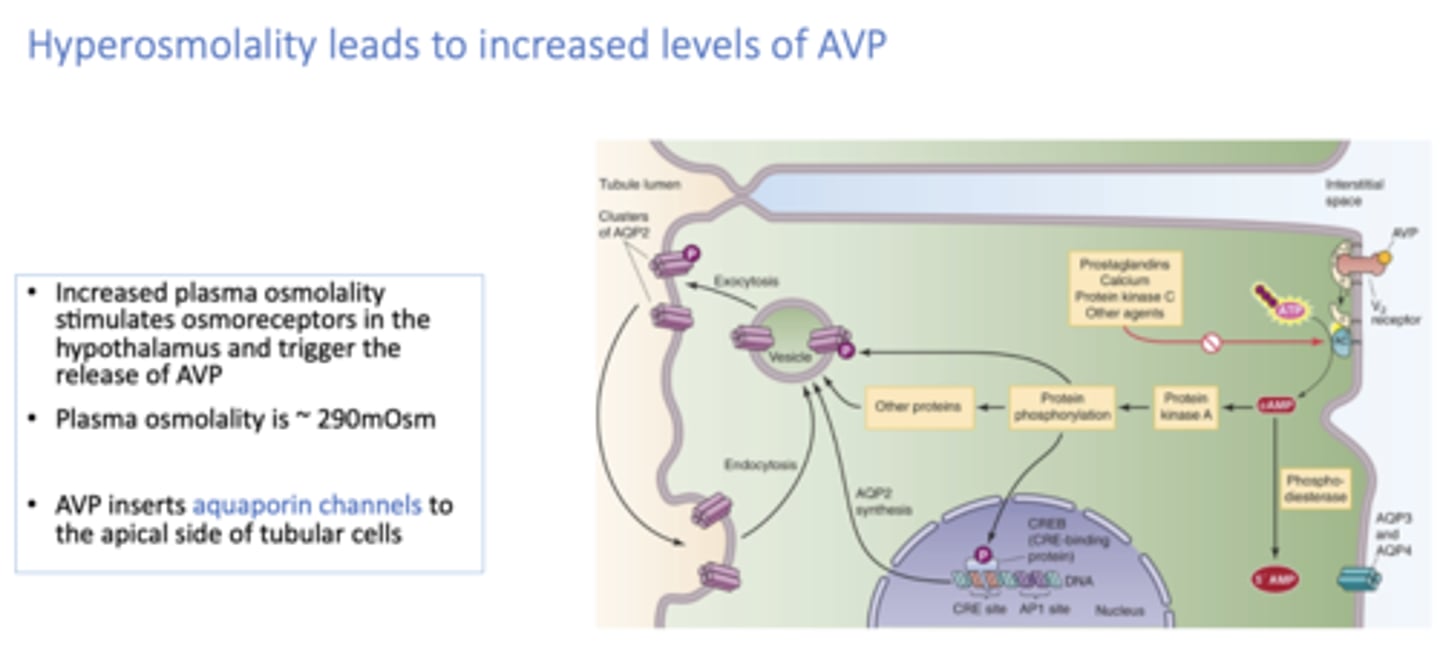
__________ leads to increased levels of AVP
hyperosmolality
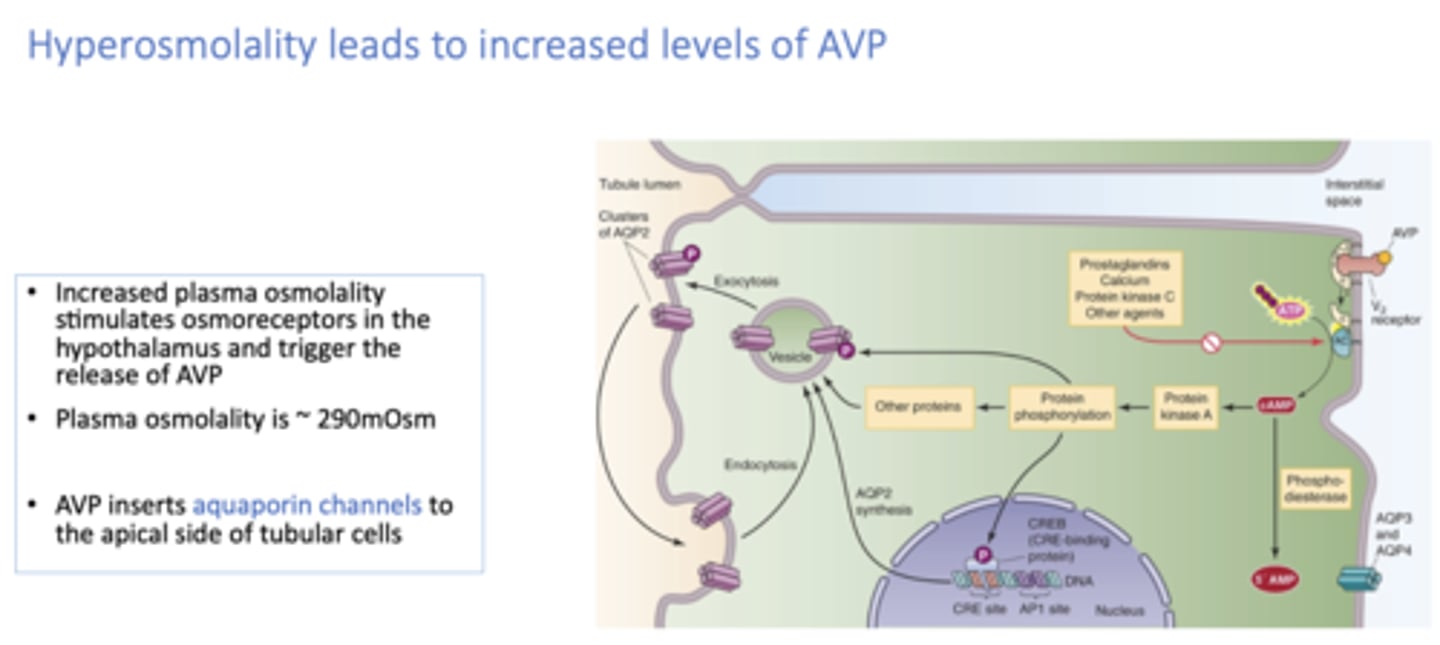
Pain, nausea, and several drugs (e.g., morphine, nicotine, and high doses of barbiturates) ___________ AVP/ ADH secretion
stimulate

Alcohol and drugs that block the effect of morphine (opiate-antagonists) ________ AVP/ADH secretion
inhibit

What are 3 types of non-osmotic stimuli that can increase AVP secretion?
- Reduced effective circulating volume (hemorrhagic shock & hypovolemic shock)
- Volume expansion
- Pregnancy

A 21-year-old student celebrates the end of final exams at a party where they consume large amounts of an alcoholic beverage (beer). Before the party, their urine flow was 1 mL/min and urine osmolarity was 400 mOsm/L. Which of the following sets of changes occur in the student following the consumption of the alcoholic beverage?
1. Free water clearance
2. Urine osmolarity
3. ADH
A. 1 - ↑ 2 - ↓ 3 - ↓
B. 1 - ↓ 2 - ↓ 3 - ↓
C. 1 - ↓ 2 - ↓ 3 - ↑
D. 1 - ↑ 2 - ↓ 3 - ↑
A. 1 - ↑ 2 - ↓ 3 - ↓

alcohols effect on ADH secretion:
decrease

alcohols effect on urine osmolarity (concentration):
decrease (more dilute)

alcohols effect on free water clearance:
increase

pain/nicotine/opioids' effect on ADH secretion:
increase

pain/nicotine/opioids' effect on urine osmolarity (concentration):
increase (reduces water in the urine, making it more concentrated)

pain/nicotine/opioids' effect on free water clearance:
decrease

Atrial myocytes release _______ in response to increased atrial pressure
ANP (atrial natriuretic peptide)

ANP (atrial natriuretic peptide) effect on blood vessels such as afferent and efferent arteriole:
vasodilation

What 3 factors can decrease TGF sensitivity?
- ANP
- High protein diet
- Volume expansion

ANP (atrial natriuretic peptide) effect on TGF sensitivity:
decrease

ANP (atrial natriuretic peptide) effect on RPF:
increase

ANP (atrial natriuretic peptide) effect on GFR:
increase

ANP (atrial natriuretic peptide) effect on renin secretion:
decrease

t/f: ANP affects renal hemodynamics indirectly, by inhibiting secretion of renin (thus lowering ANG II levels) and AVP
true

___________ decreases blood flow to the renal medulla, minimizing the washout of the hypertonic medulla, which is essential for forming a concentrated urine
ADH

The renal effect of _________ is to vasodilate, which is opposite to the effects of epinephrine and norepinephrine
dopamine

Dopamine action on renal blood vessels:
vasodilation

Prostaglandins action on renal blood vessels:
vasodilation

_______________ provide a buffer against excessive vasoconstriction, especially during increased sympathetic outflow to the kidney or activation of the renin-angiotensin system
prostaglandins

Nitric Oxide action on renal blood vessels:
vasodilation

Cause local, strong vasoconstriction to reduce RBF and GFR
leukotrienes

Leukotrienes action on renal blood vessels:
vasoconstriction

Name 4 Vasoactive agents that modulate RBF and GFR
- Dopamine
- Prostaglandins
- Nitric oxide
- Leukotrienes
