All Examplars + CP
1/142
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
143 Terms
Complication
Name a complication of cerebral palsy.
Difficulty with ambulation
Decreased nutrition
Respiratory issues
Difficulty speaking
Difficulty with ambulation
Cerebral Palsy patients have difficulty ambulating related to spasticity, muscle weakness and muscle rigidity.
Pathophysiology
What is cerebral palsy
A non progressive disorder that affects posture, body movement and muscle coordination
Manifestations
A nurse is assessing a 7 month old infant. The mother states “My baby is having a hard time sitting up. When he does sit up, there is always support behind him, or I help him.” The nurse suspects what condition for the infant?
Rationale:
Cerebral Palsy
Rationale:
Normal Child Milestone
Head control = 2-3 months
Sitting unsupported = 6-9 months
Walking = 12-28 moths
A 7 month child should be able to sit unsupported according to normal developmental milestones. The nurse should suspect possible cerebral palsy
Risk Factors
What are the risk factors for a child to develop cerebral palsy
structure abnormalities
ischemia or hypoxia in prenatal, perinatal or postnatal stages
infection (strep)
preterm
child abuse (head trauma)
Manifestations
What manifestation would parents first observe in their children when it comes to possible cerebral palsy
Rationale:
tonic bite and feeding difficulties
Rationale:
CP causes poor control of muscles. The infant does not have voluntary control of the muscles in their mouth
Manifestations
A mother fells and bruised her stomach. The mother states that she is worried about CP in her unborn child. The mother asks “what signs should I look out for if I suspect CP?” The should respond with
Rationale:
the most significant signs of CP are
Ataxia = unsteady gait
toe walking
Nurse Intervention
A nurse is speaking with the parents of a child suspected of CP. Parents explain significant signs of CP. The parents ask “what can we do to help our child with this condition” What is the nurses response.
Rationale:
Start the child in early stimulation programs
Rationale:
The use of therapeutic modalities such as physical therapy, occupational therapy, and speech therapy will be essential in promoting mobility and development in the child with cerebral palsy. The earlier the treatment begins, the better chance the child has of overcoming developmental disabilities
Treatment
A child with with CP is taking baclofen for their muscle spasticity. What education should the nurse provided about this drug
Rationale:
Don’t stop the drug abruptly
Rationale:
Stopping the drug abruptly can cause painful spams to return
Pathophysiology
What is hydrocephalus
An excessive accumulation of CSF in the ventricles of the brain causing them to swell
Manifestations
What are the three common sigs of hydrocephalus in a child
enlarged head
sun setting eyes
poor feeding
Nurse Interventions
A child is finished their surgery for the ETV. What should the nurse do to prevent ICP
Rationale:
Lay the child on their side, on the opposite side of where they got the shunt
Nurse Intervention
A nurse is caring for a pediatric patient and notes bulging fontanelles . In addition, the nurse notes sun setting eyes, vomiting, lethargy, and irritated. What should the nurse suspect and what should the nurse do
Rationale:
signs if ICP
contact the provider
Rationale:
bulging fontanelles, sun setting eyes, vomiting, lethargy, and irritated are signs of increased ICP. Doctor should be notified due to emergency
Nurse Intervention
A nurse is caring for a child post ETV shunt. What signs should the nurse look for when it comes to monitoring signs of potential ICP from a blocked shunt.
pupillary dilation
Nurse Education
A nurse is providing education to the parents of an infant who has finished ETV surgery. What should the nurse educate when it comes to the infant and the shunt
do shunt care to prevent infection
dont elevate the head of the bed to reduce ICP risk
keep the child flat for 24-48 hours to reduce fluid shifts
Manifestations
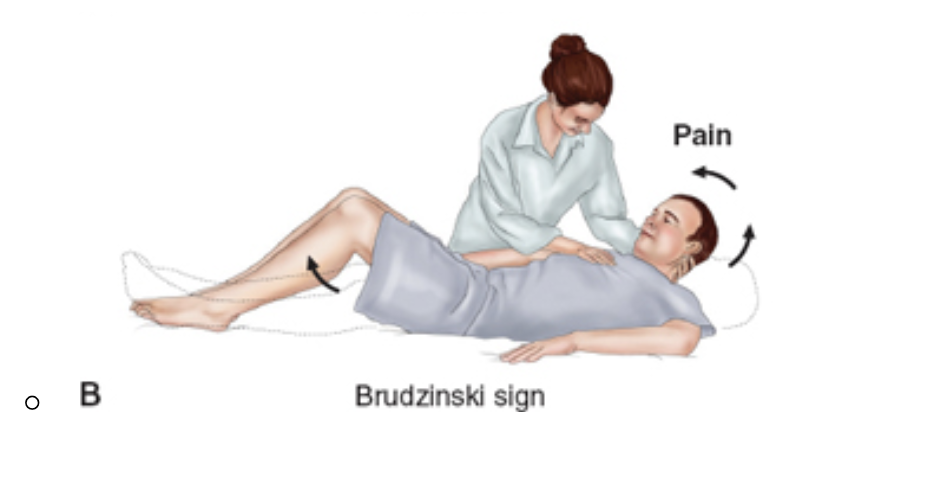
A nurse is caring for a patient with suspected meningitis. The nurse helps the patient flex their neck upwards. When the neck is flexed, the knees and the hips also flex. What would the nurse call this maneuver
Brudzinski Sign
Manifestations
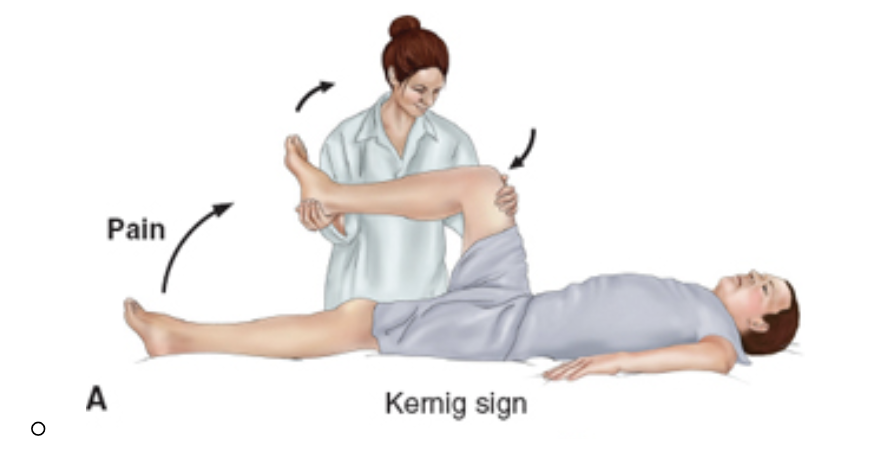
A nurse is caring for a patient with suspected meningitis. The nurse helps the patient extend their leg. The patient complains of pain. How would the nurse interpret this maneuver
Kernig’s Sign
Pathophysiology
inflammation of meningeal layer. The infection spreads vias the bloodstream and and can lead to ICP
Meningitis
Patho
A nurse is explaining the two main causes of meningitis. What should the nurse say?
strep pneumoniae
neisseria meningitidis
Risk Factors
A nurse is education teens about demographics who are an increased risk for contracting meningitis. What should the nurse say?
crowded areas
college dorms
military dorms
All carry the increased risk to develop meningitis
Diagnostics
A nurse is carrying for a patient with suspected meningitis. What might the nurse suggest to obtain a definitive confirmation to meningitis
CT
LP
Rationale
the lumbar puncture pulls the CSF and uses a gram stain to detect pathogen that causes meningitis
Nurse Interventions
A nurse performs a positive brudzinski sign and suspects possible meningitis. What precautions should the nurse take take during the care of the patient
Rationale:
isolate them immediately
use droplet precautions
Rationale:
pathogen is highly contagious
Nurse Education
A nurse is providing meningitis vaccination information to the parents of a pre-teen boy. What information should the nurse provide about the vaccine
Educate to vaccinate at around 11-12 years old and again at 16
Treatment
Name: Rifampin, Ciprofloxacin, Ceftriaxone, ampicillin, Penicillin G Used for treatment of meningitis Nurse Consideration: |
Name: Rifampin, Ciprofloxacin, Ceftriaxone, ampicillin, Penicillin G Used for treatment of meningitis Nurse Consideration:
|
Nurse Education
A nursing student is caring for a patient who is brain dead. The nurse following the rules of 100, and making sure the patient is ready for organ procurement. What places a patient un able to donate their organs
HIV
Hep B
active TB
Nurse Education
A nursing student is asking about the Rules of 100. How can the nurse best explain this process
Rationale:
Use the Rule of 100
O2 = 100
Urine output = 100 ml / hr (call the doctor if it drops)
BP = 110
Temp = 100 (97 to 102)
Rationale:
these interventions allow for the organs to stay viable before procurement
Nurse Interventions
A patient has been declared brain dead. Who must be contacted if the family members what more clarification on the status of their brain dead relative
Organ Procurement organization
Manifestations
A nurse is caring for a patient who is brain dead. What manifestations might the brain nurse see upon inspection
Pt cant respond to command
Pt is flaccid
Pupils are unreactive
No occulocephalic reflex
No stimulation to supra-orbital stimulation
No ocular vestibular reflex
No gag reflex
No spontaneous respiration
Nurse Interventions
A nurse is assessing a child with a brain tumor. The nurse palpates the fontanelles and notices bulging. What do these signs indicate and what should the nurse do
indicates increased ICP and to contact the HCP
Rationale:
An emergency
Treatment
A nurse notes ICP in a child with a brain tumor, what should the nurse admin
Rationale:
dexamethasone
Adverse Effects
hyperglycemia
hypokalemia
muscle weakness
Rationale:
a med that can lower ICP
Treatment
A child is recovering from an operation to remove their brain tumor. The nurse is worried about cerebral edema. What medication should the nurse anticipate the HCP to order
mannitol
hypertonic dextrose
Rationale:
reduces cerebral edema that can turn into ICP
Nurse Interventions
A nurse is caring for a post op child who has had brain tumor surgery. The nurse is concerned about CSF leaks. What can the nurse do to reduce the risk of leakage
provide a quiet non stimulating room '
check dressing and nares for CSF leaks
lay flat
Manifestation
A nurse is caring for a post-op child. The nurse suspects brain herniation. What signs might the nurse see?
crushing’s triad
body temp changes
nuchal rigidity
sluggish pupils
Manifestations
A nurse assess a child an notices that they do not have PERLA, but a fixed and a dilated pupil. How should the nurse interpret this
a neurosurgical emergency
Areas of the brain and how they are affected by a brain tumor
Frontal Lobe | |
Parietal Lobe | |
Temporal Lobe | |
Occipital Lobe | |
Cerebellum | |
Brainstem | |
Frontal Lobe | planning, problem solving, movement, emotion, speech |
Parietal Lobe | 5 sense, pain and space perception |
Temporal Lobe | hearing, language, memory and emotion |
Occipital Lobe | vison, color, distance |
Cerebellum | voluntary movement and balance |
Brainstem | HR, RR, BP |
Pathophysiology
What is traumatic brain injury
an injury to the skull or the brain that is severe enough to interfere with normal function
Pathophysiology
What is coup and counter coup
a serious traumatic brain injury where the front of the brain is damaged from the direct impact and the opposite side hits the side of the skull
Pathophysiology
why is counter coup more severe than the initial site of impact
Rationale:
the jerking backwards of the brain hits the back part of the skull. MVA, falls and shaking infant syndrome are increase risk factors to counter coup
Rationale:
increases the risk for hemorrhage
Pathophysiology
What is the Monroe Kellie hypothesis and how is that connected to ICP
The cranial vault:
brain
blood
CSF
1/3 will increase in volume, then the other two must decrease in volume or there will be an increase in ICP
Complications
what are the two complications a skull fracture cause
cerebral hypoxia
ischemia
Nurse interventions
A nurse suspects a basal skull fracture and clear fluid is leaking from the pts ears. What diagnostics can the use to determine CSF possibility
check with a glucose monitor or halo test
Manifestation
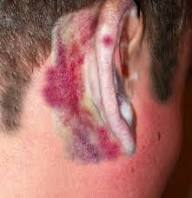
A nurse assess bruising over the mastoid process of the ears, what is the condition called
battle sign
Diagnostic
A patient came in with a possible skull fracture and might have a consussion, what diagnostic tool might the nurse use to determine the extent of the fracture
A CT scan (first line)
MRI
Glasgow scale = 15 is best
Nurse Education
A patient that suffered a skull fracture is about to go home. What education should the nurse provide to the patient and the family
educate on the symptoms to watch out for
watch the patient for 24-48 hours after the brain injury
The patient can sleep but wake them every 3-4 hours in the first 24-48 hours
avoid screen time for a few days
avoid aspirin and ibuprofen (acetaminophen is okay)
avoid heavy weight lifting
Manifestations
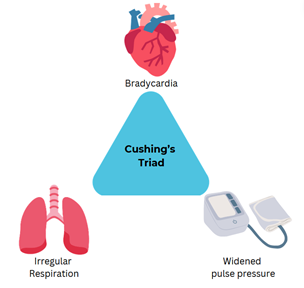
A patient had a head injury and is entering the late stages of the injury. The nurse suspects Crushing Triads. What would the nurse see upon presentation
widened pulse pressure (high systolic/low diastolic BP)
bradycardia (low heart rate)
irregular respiration
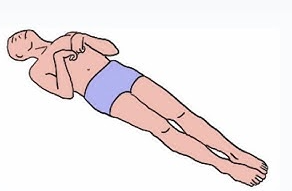
Manifestation
decorticate
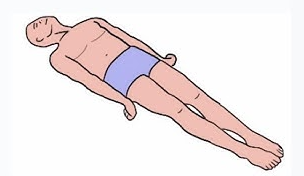
Manifestations
decerebrate
Pathophysiology
what is a epidural hematoma
Manifestations
Rationale:
bleeding between the dura and the inner surface of the skull
unconscious with brief lucid intervals
headache
NV
Rationale:
these bleed is arterial in nature and bleeds FAST
Pathophysiology
what is a SUBDURAL hematoma
Manifestations
Rationale:
bleeding between the dura and the arachnoid layer of the meninges
decreased LOC
headache
ipsilateral pupil dilation
Rationale:
venous bleed and a slow bleed
Pathophysiology
what vertebra are mostly involved in spinal cord injuries
C1-C5
T12
L1
Pathophysiology
What are the two types of spinal cord injuries
Rationale
primary
secondary
Rationale:
Primary- is direct physical trauma to the spinal cord
secondary- after a primary injury, the injury becomes on going and progressive
Manifestation
what are the symptoms of a spinal cord injury that develops into spinal shock
↓ DTR
Spinal reflex and sensation
flaccid apparency below the level of injury
Nurse intervention
A nurse is caring for a patient who has
HR: 54
TEMP: 97 at 11 am , 99 11:30 am, 100 at 12 pm
BP: systolic of 87
How should should the nurse interpret these findings and what should she do
Rationale:
these are signs of neurogenic shock and should contact the HCP
Pathophysiology
Why is a secondary spinal cord injury dangerous
Rationale:
edema can form within 24 hours and create permeant tissue damage
Which action should the nurse recognize has the highest priority for a patient who was admitted 16 hours earlier with a C5 spinal cord injury?
Assessment of respiratory rate and effort
Cardiac monitoring for bradycardia
Administration of low-molecular-weight heparin
Application of pneumatic compression devices to legs
Assessment of respiratory rate and effort
Edema around the area of injury may lead to damage above the C4 level, so the highest priority is assessment of the patient’s respiratory function
Manifestations
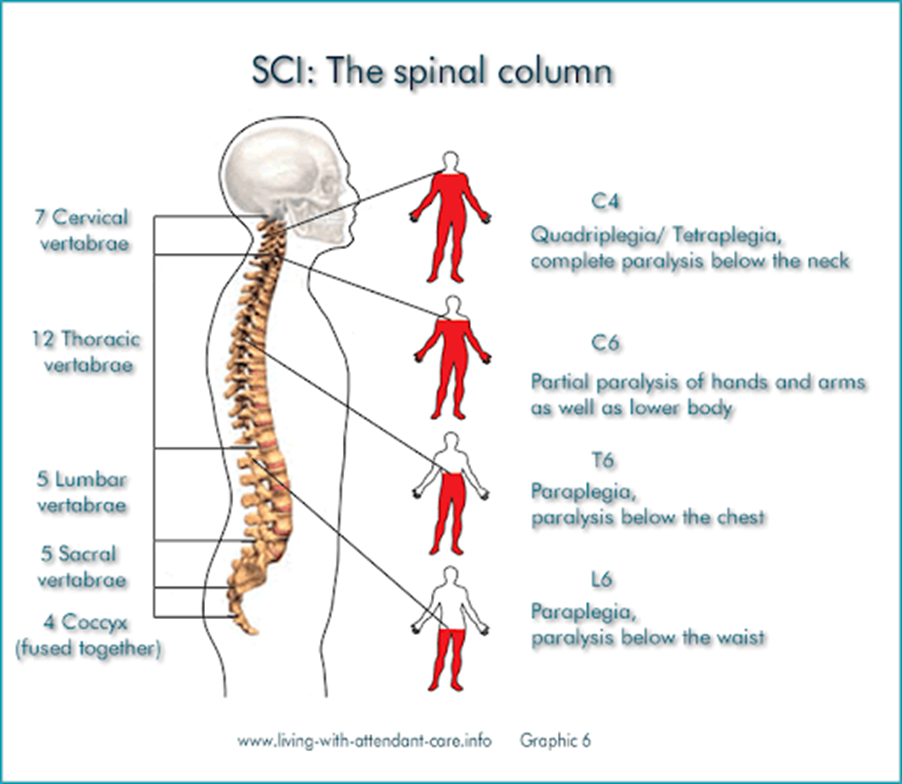
What type of paralysis can be noted if there is damage C4. C6, T6 areas of the spinal cord
C4 = complete paralysis below the neck
C6 = partial paralysis of hand and arms
T6 = paralysis below the chest
Treatment
What medications can be given to pts who have low HR and low RR and have a spinal cord injury
atropine
Nurse Interventions
A nurse is caring for a spinal cord injury patient and is using a Halo Brace. What should the nurse to reduce the risk of infection
provide pin care everyday
Rationale:
the screws are entering the skull via the skin. Break in skin and bone integrity can lead to infections. Care is needed to prevent this
Pathophysiology
what is autonomic dysreflexia
a life threatening condition that can result from spinal cord injuries that affect T6 or higher
Risk Factor
Why is damage to the T6 area of the spinal cord important to understand the triggers of autonomic dysreflexia
Rationale:
T6 is the area of the CNS the sends and receives info to signal to the body of full bladders or bowel impactions.
Rationale:
Damage to the T6 causes the body to not feel when the bladder is full or the bowels are impacted. Full bladder or bowels is the biggest trigger for autonomic dysreflexia
Nurse Interventions
A nurse is caring for a patient who has a T6 spinal cord injury. The nurse take a BP of 160/ 88, HR of 34 and assess the patients bladder- the bladder is hard and distended upon palpation. What is the primary intervention (3 steps)
Rationale:
raise the HOB 45'
Contact the HCP
Do a straight catherization
Rationale:
Damage to the T6 causes the body to not feel when the bladder is full or the bowels are impacted. Full bladder or bowels is the biggest trigger for autonomic dysreflexia. A straight catheterization with remove the built up urine reducing the risk that comes with a full bladder. Elevating the HOB helps reduce the pressure
A BP of 20-40 mm Hg above the baseline + bradycardia (30-40 bpm) + full bladder = autonomic dysreflexia S/S
Treatment
If a patient is experiencing automatic dysreflexia, what medications are given
Rationale:
Nitroglycerin Paste
Rationale:
Nitro will decrease the elevated blood pressure from the autonomic dysreflexia crisis
Manifestations
what are the manifestations of autonomic dysreflexia
hypertension
diaphoresis above the injury
bradycardia
Nurse Interventions
A nurse has assessed for bladder distension and bowel impaction. The nurse notes no distention and impaction. What other nursing interventions should the nurse do to determine triggers to autonomic dysreflexia
assess for skin breakdown, tight clothes and laying on the call light
Pathophysiology
what is a fracture and how are they classified
a disruption or break in bone continuity
Classification
Complete or incomplete
open or closed
stable or unstable
Pathophysiology
Describe the 6 types of fractures
transverse = straight across
spiral =
greenstick = split or bent
comminuted = crumbled
oblique = across / down the bone
pathologic = diseased bone fracture
Manifestations
what are the manifestations of a bone fracture
edema / swelling
pain
muscle spasm
deformities
confusion
Risk Factors
what are the risk factors to fractures
Rationale:
elderly
post menopause
high risk activities
Rationale:
post menopausal women are more at risk due to the development of osteoporosis. As a result, their bones are weaker and will break.
Pathophysiology
what are the stages of bone healing
Rationale:
fracture hematoma- a blood clot forms at the fracture
granulation tissue-
callus formation- C.T. forms a callous at the end parts of the fracture
ossification- the bone hardens
consolidation and remodeling- the callous is reformed and the bone has shape again
Nurse Interventions
why is fracture reduction like manipulation, reduction and traction devices important nursing interventions for fractures
these intervention keep the bone aligned properly
Nurse Interventions
Give examples of fracture immobilization tools / interventions
external cast = a physical cast placed over the fracture
internal or external fixation = using pins to immobilize the fracture
maintenance traction = (bucks traction) used in the hospital to immobilize the fracture
Nurse Interventions
What interventions are needed if a patient has open fractures
Rationale:
surgical detriment
tetanus / antibiotics
Rationale:
fractures that have open wounds are at increase risk for infection. Cleaning and admin of drug therapy early reduce the risk of infection development.
Nurse Interventions
After a fracture has be immobilized. what should nurse do to prevent complications
Rationales
The nurse should do neuro checks every hour
turn every 2 hours
keep the cast dry
elevate above the head
Rationale:
to make sure they don’t have nerve damage and have good blood flow
to reduce pressure injuries risk
protect skin integrity / infection
Treatment
what is a skin traction boot
Rationale:
A skin traction boot is a immobilization device were weights are hanging off the end of the bed.
Rationale:
the weights must never touch the ground because the tension is what helps immobilize and align the fracture to heal properly
it also helps reduce muscle spasms
Treatment
A nurse just finished obtaining report on a patient who fell 6 stories. The patient has a fracture on the right femur. The nurse is notified that the patient is on a Skeletal Traction Bed Frame. An order is placed for 10lbs to hang from the traction device. The nurse notes that the patient’s device only has 2lbs. What should the nurse do?
Rationale:
Contact the HCP
Rationale:
In order for the traction device to work, tension must be created. Improper weight will reduce said tension and prevent the immobilization/ alignment needed to heal the fracture. Contact the HCP to correct the weight.
Nurse Intervention
If a patient is on alignment devices to correct the fracture, what should the nurse do to reduce infection
Rationale:
pin care everyday
Rationale:
pins are breaking skin integrity. Break in skin integrity can lead to infection at the points of entry
Nurse Education
what education should the nurse provide to the patient who has a cast
Rationale:
DO NOT
get it wet
remove padding
insert objects
put lotion in the cast
bear weight
cover it with plastic
Rationale:
adding water to the internal section of the cast / objects can increase the risk for infection due to breaks in skin integrity
DO
keep it dry
cover it before showering
use a blow dryer to dry the cast after showering
elevate above the heart for the first 48 hours
move the extremities
report odor, drainage, pain, swelling, discoloration of finger/toes, tingles
educate the patient to do their cast and fracture appointment follow ups
Rationale:
Keeping the inside of the cast reduces the risk of infection
Risk Factors
what are the risk factors to have an amputation for
middle / older adults = PVD, atherosclerosis, DM
young adults = trauma (vets)
osteomyelitis
frostbite
Diagnostics
What are the diagnostics needed to determine if a patient might need an amputation
Rationale:
X ray
CT or MRI
vascular studies
Rationale:
CT and X rays can help determine if osteomyelitis is present. The disease increase the risk for amputation
vascular studies show how far down the blood travels and help the doctor determine how much to cut
Nurse Interventions
A nurse is caring for a patient who will undergo surgery to amputate his left leg. What should the nurse educate / tell the patient prior to the start of the surgery
get consent prior to start of the surgery
explain the reason for the amputation
Nurse Intervention
A nurse is caring for a patient post-op from surgery. The patient underwent a left leg amputation. The nurse assess the incision site and notes lots of bright red blood saturating the gauze. What should the nurse do first.
Rationale:
Contact the HCP
Rationale:
the sutures may have opened up and caused hemorrhage. Circulation is being compromised . The patient needs to return to the operating room to fix the sutures. Life threatening
Nurse Intervention
What should the nurse assess after an amputation surgery
Rationale:
do circulation checks
do neuro checks
Rationale:
circulation checks establish good perfusion or lack there of
to monitor for neuro damage or compartment syndrome
Pathophysiology
Compartments syndrome is a decrease in pressure within a compartment that decompresses blood vessels, nerves, and/or tendons in the leg, arm, and shoulder.
True
False
Rationale:
False
Rationale:
Compartment syndrome is an increase in pressure directly related to tissue swelling.
Pathophysiology
What is phantom leg syndrome
Rationale:
Pain in a missing body part
Rationale:
the nerves are severed at the site of amputation. The brain is still sending signals to that area indicating pain
Treatment
A patient states “i got my amputation surgery 3 weeks ago, but I’m feeling pain where my leg use to be” What should the nurse do?
Give the pain medication
Risk Factor
what increases the risk to develop compartment syndrome
trauma
tight dressing or cast
hemorrhage into compartment
Manifestations
What are the 6 Ps of compartment syndrome
pain
pallor
pressure
paresthesia
paralysis
pulseless
Rationale:
If a patient complains of any of these signs, then they are at risk for compartment syndrome. Notify the provider ASAP.
Diagnostic
what test is used before and after exercise to determine compartment syndrome risk
intercompartment pressure test
Treatment
A patient is at risk for compartment syndrome. What surgical treatment must be done
Rationale:
fasciotomy
Rationale:
this procedure relieves pressure caused by the syndrome. If not done, then the patient might need an amputation
Treatment
Name:
Mannitol
MOA:
Treatment
Name:
Mannitol
MOA:
used to decreased the high blood pressure when a pt has increased ICP
Pathophysiology
what are tonic-clonic seizures
the most common type of seizures. Involuntary miscle contractions and loss of consciousness.
Manifestations
what are the two most common symptoms of tonic clonic seizures
muscle rigidity
jerking movements
lasts 1-2 mins
Nurse intervention
During the Seizure
>5 mins →
Place them on seizure precautions
Monitor LOC and keep airway
If the seizure lasts more than 2 mins
During the Seizure
>5 mins → emergency → call 911 → keep track of duration and start time of seizure
Assess if the patient has had a head strike → to determine further damage.
Place them on seizure precautions
Protect pt- don't restrain them and place them on their side → to prevent aspiration
Have padded side rails
Monitor LOC and keep airway
Make sure suction and Ambu bag are at bedside
If the seizure last more than 2 mins
call 911 and note the start and duration of the seizure
Pathophysiology
what will a patients post ictal state be after a tonic clonic seizure
they will be hard to arouse and allow them to sleep
Nurse Interventions
what are common interventions a nurse can obtain when a pt is at risk of an active seizure
document the start and duration of the seizure
know which body parts are moving
Diagnostics
what are the diagnostics for generalized seizures
Rationale:
EEG
MRI
SPECT
Rationale:
EEG show the seizure type
MRI show lesions on the brain
SPECT show which part of the brain is causing the seizure
Pathophysiology
what is a and absent / petite mal seizure
Manifestations
they space out and stare and don’t respond
Manifestations
lasts seconds
automatisms- sudden and repetitive motions (knee pats)
Pathophysiology
what is a and atonic seizure
Manifestations
Rationale:
when there is a lack of muscle tone and they completely pass out
Manifestations
slump over
Rationale:
the sudden slump over increase the risk for head trauma
Risk Factor
what is the biggest risk factor for someone to develop seizures
Not compliant anti-seizure meds
Pathophysiology
what is a focal seizure and what are its subtypes
Complications
originate in one area of the brain
simple partial- their conscious will stay intact
complex partial- impaired conscious
Complication
the focal seizure can go from simple to complex
Pathophysiology
what are febrile seizures. They have a rapid recovery of the post ictal state
tonic clonic seizures but with a high fever