Tissue bio exam 3
1/76
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
77 Terms
Skin
organ, the largest of the body, functions to provide sensory information, homeostasis (regulates body temperature), protects against pathogens, and provides a physical barrier, also antigen processing, is excretory in function (excretes sweat, oil, electrolytes, etc), and metabolizes calcium (which forms vitamin D3 and B), and pheromones
layers of the SKIN
epidermis (epithelium) and dermis (connective tissue), hypodermis (largely white fat)
Layers of the EPIDERMIS
Stratum basale, stratum spinosum, stratum granulosum, stratum lucidum, stratum corneum, stratum disjunctum
What kind of tissue makes up the epidermis?
KERATINIZED stratified squamous epithelium
What is found in the dermis?
Neurons, glands, blood vessels, sensory receptors, lymphatic vessels, muscle, hair follicles
Layers of the DERMIS
Papillary layer, reticular layer
Papillary Layer
rests right under the epidermis of the skin, point of contact between the epidermis and dermis, thin (made of loose CT), fibers are randomly woven together like felt (made of collagen and connective tissue)
Dermal Papillae
the parts of the dermis that extend into the epidermis between each rete ridge of the epidermis
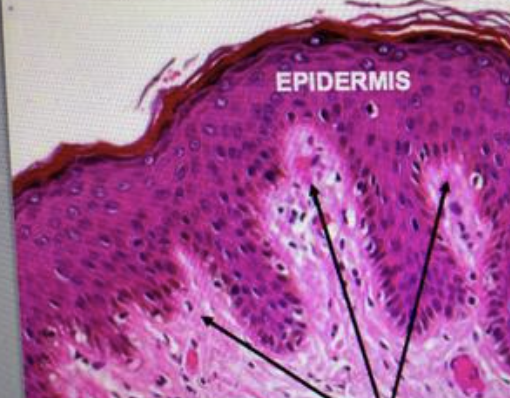
Rete ridges
The parts of the epidermis that extend into the dermis
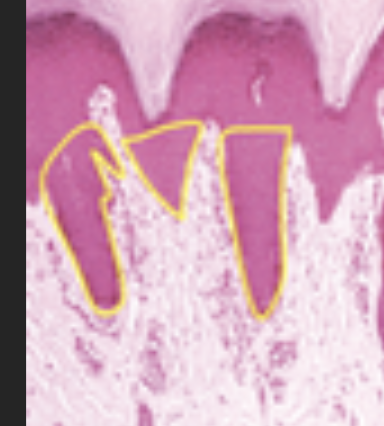
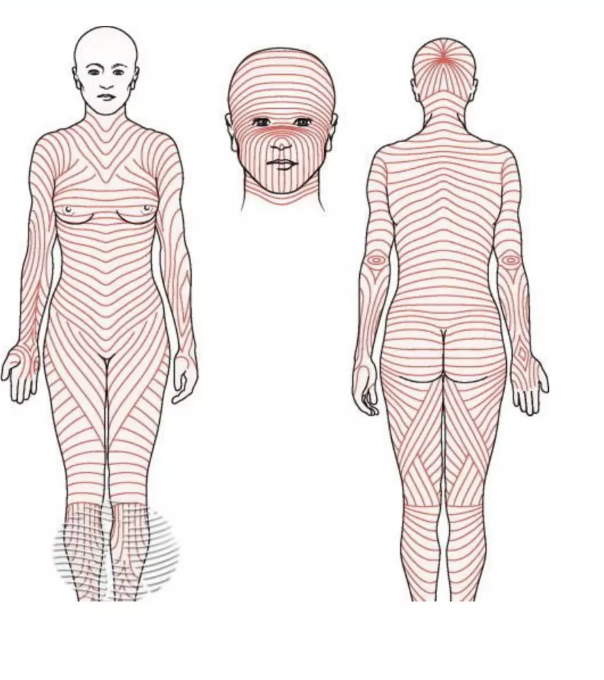
Reticular layer of the dermis
made of dense CT, collagen and elastic fibers form long parallel lines (non-random orientation) called langer lines (image is of langer lines)
True dermal ridges
Where we have prints (fingerprints)

hypodermis
under the dermis, subcutaneous, largely white fat, provides insulation, energy storage, and protects the body from harm, connects skin to muscle and bone
stratum basale
bottom layer of the epidermis (closest to the dermis), also called the stratum germinativum, where cell division occurs, vary between cuboidal and columnar cells, clear cells (melanocytes) are present here
Malpighian layer
the combination of the stratum spinosum and basale is called this
stratum spinosum
Cells are well defined, halos around each cell, intercellular space between cells, prickly appearance (finger like projections attached by way of desmosomes)
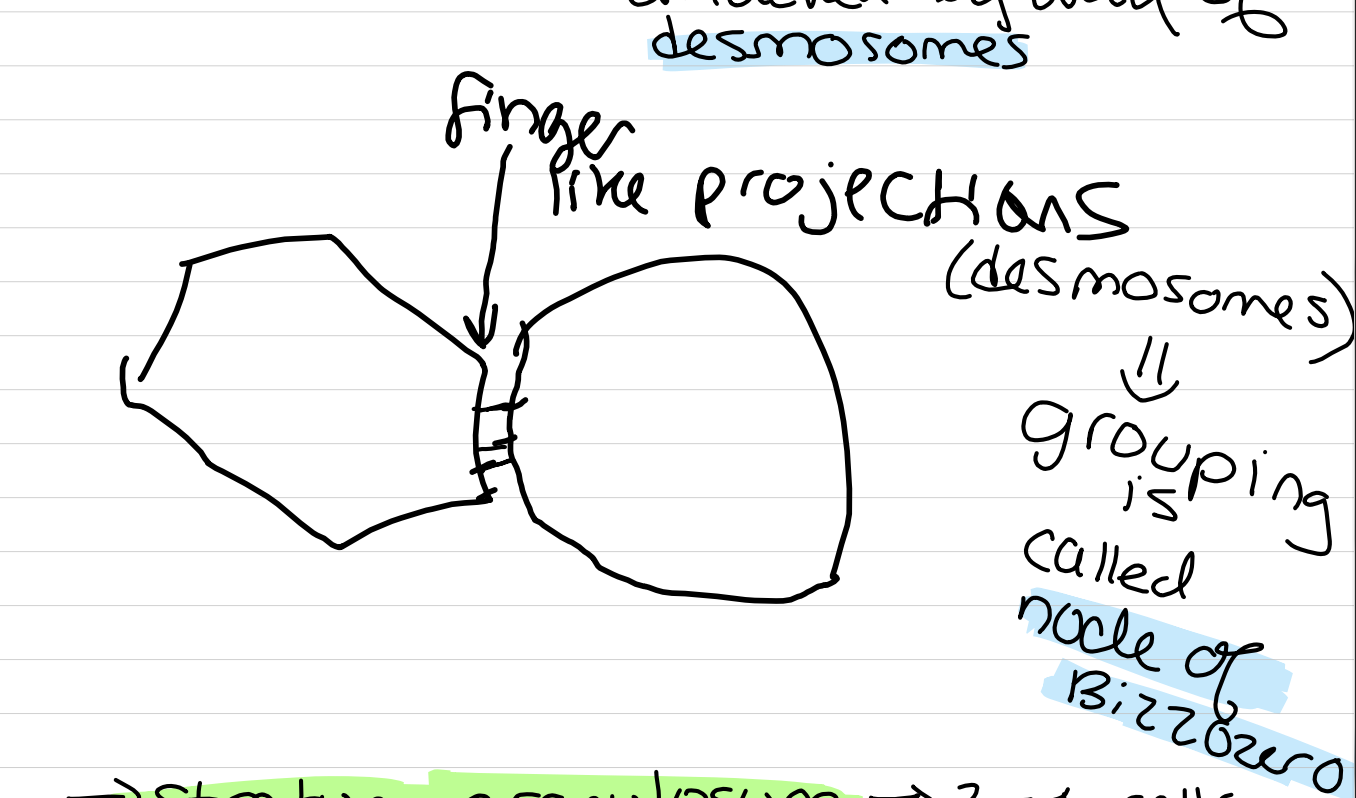
node of blizzozero
a grouping of desmosomes
stratum granulosum
2-4 cells thick, granular in nature (dark, basophilic granules made of keratohyaline), as you go up the layer, granules increase in number and size, first step in forming keratin
what forms keratin?
kertatohyaline and cytokeratin (an intermediate filament known as a tonofilament)
stratum lucidum
only found in thick skin (the soles of the feet and palms of the hands), cells are flattened and clear, nuclei are gone, eleiden now fills the cells (eleiden is an intermediate of keratohyaline and cytokeratin, and acts as a precursor to keratin)
thin vs thick skin
"thick skin” is a term used to describe when the epidermis has a stratum lucidum, it does NOT refer to the actual size of the epidermis
thin skin refers to everywhere else on the body which does NOT have a stratum lucidum
stratum corneum
cells are dead, have keratin now, varies in thickness, thickest layer, in areas we have friction, this layer is the thickest (provides a barrier to friction through callouses)
4 cells of the epidermis
keratinocyte, melanocytes, langerhan cells, merkel cells
cytomorphisis
when a cell type experiences a number of changes in its anatomy (like keratinocytes)
the formation of keratin
in the stratum basale: basal cells are active, they divide and make cytokeratin which composes tonofilaments, high number of ribosomes which are acids (makes the tissue basophilic), moves from basement membrane and goes toward the stratum spinosum
in the stratum spinosum: tonofilaments become tonofibrils, which are bound by filaggrin (functions to intersent into desmosomes and hemidesmosomes), upper layers of the spinosum become less basophilic with more cytokeratin (which is acidophilic)
in the stratum granulosum: stops making cytokeratin, starts making keratohyaline granules (KG), which are basophilic, 1-5 µm in diameter with no membrane, not secretory, do not leave the cell, make of filaggrin, phosphate rich proteins and RNA (which both explain intense basophilia), reactive, react with tonofilaments/fibrils, reaction forms eleiden (which makes the keratin)
desmosomes
bind cells together
hemidesmosomes
bind the epidermis to the dermis by way of the basement membrane (tonofilaments and fibrils reinforce this binding)
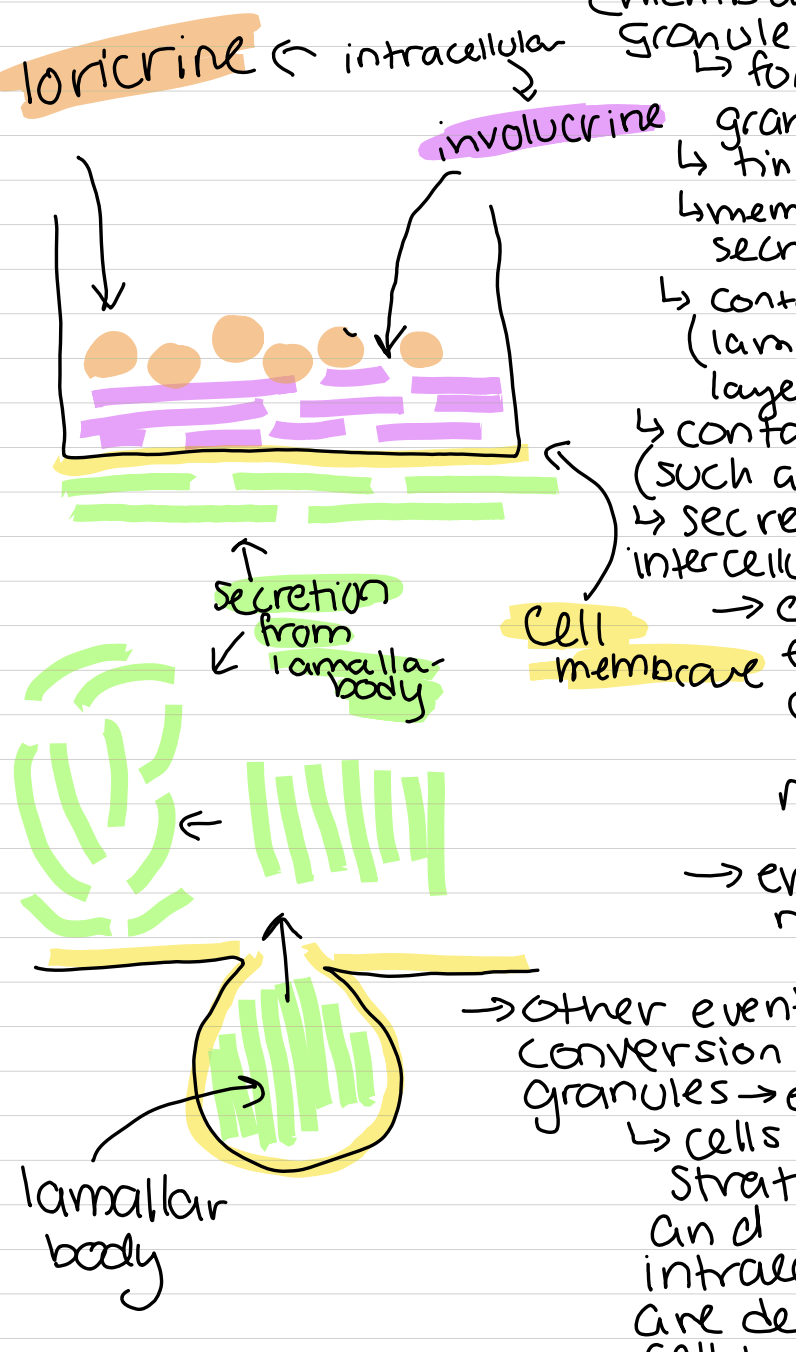
Lamellar bodies or obland bodies or membrane coating granules
forms in the stratum granulosum, tiny 1/10 - ½ µm, membrane bound, secretory, contain thin layers (lamallae) of lipid layers, secrete enzymes (such as serine protease), secrete lipid layer into intercellular space (cell above takes fats from other cell and makes its cell membrane thicker), enhances water resistence
other events besides the conversion from granules —> eleiden —> keratin
cells move into stratum granulosum and 2 insoluble intracellular proteins are deposited on the cell membrane (loricrin and involucrin), causes the formation of a barrier between internal environment (living cells) and the external environemnt (dry, dead cells of the stratum lucidum and corneum), inactive enzyme (serine protease) is neural in the granulosum (but as it moves to the lucidum and corneum, pH falls and the enzyme activates, causing it to target desmosomes, and break them down, causing flattened, dead cells to separate from the corneum)
melanocytes
produce melanin, come from the ectoderm from the neural crest (also where keratinocytes come from), found in the stratum basale, in contact with basement membrane, more of these cells where there is contact with the sun (and the scrotum of a male for some reason?), do not form junctions with keratinocytes, look like an astrocyte
how is melanin made?
Stage 1 melanosome: start with very small (250 nm) membrane bound vesicle, that arise from the golgi apparatus (secretory vesicle), carries a variety of proteins including the enzyme tyrosinase
Stage 2 melanosome: other (structural) proteins begin to form a grid like structure that has a uniform periodicity (forms a framework for melanin to be deposited (also called a premelanosome)
stage 3 melanosomes: have tyrosine (an Amino Acid), tyrosine is made into DOPA which is made into melanin, once melanin is deposited onto framework, then it becomes stage 3
when the vesicle is filled, enzyme activity decreases
stage 4 melanosomes: mate melanosome (filled with melanin) —> transported to cell processes
Transferred to surrounding keratinocytes in stratum spinosum (called cytokine secretion), melanosomes never enter extracellular space, process involves phagocytosis of the melanocyte cell process by the keratinocytes
phagocytosis
when a cell membrane engulfs a particulate or vesicle
skin pigment
melanin is MADE in the melanocytes, but, our skin’s pigment is due to the melanin in the keratinocytes
Langerhans cells
in the middle/center of the epidermis (called rete ridges), morphologically speaking similar to melanocytes, also called epidermal dendritic cells, come from blood cells in the bone marrow (mesoderm), macrophages, they monitor the epidermis for antigens that might pass through the skin
if they encounter an antigen, they will break it down on the cell’s surface, they they migrate out of the epidermis to a lymph node where the lymph node responds
involved in an immune response called delayed type hypersensitivity reaction (including contact dermatitis — like poison ivy or oak)
Birbeck granules are found in the cytoplasm of these cells, look like tiny tennis rackets, unique to langerhans cells, function is unknown
merkel cells
epithelial cell origin (modified basal cells), found in the stratum basale, also called tactile cells, have cell processes similar to a dendrite, attached to keratinocytes by desmosomes (unique to other cells in this way), have numerous secretory vesicles (400 nm in diameter, dense or neurosecretory granules contain chemicals called catecholamines like epinephrine or norepinephrine), basal surface is basement membrane and interacts with axon terminals of the afferent nervous system (pseudounipolar), sensory receptor to light touch
sensory neuron and merkel cell together form merkle’s corpuscle
receptors common to skin
free nerve endings, meisner’s corpuscle, pascinian corpuscle
free nerve endings
penetrate into epidermis as far as the stratum granulosum, endings are naked (unencapsulated), detects pain (nociception)
pascinian corpuscle
by the hypodermis (encapsulated), not very sensitive, deep pressure
meisner’s corpuscle
encapsulated, lighter pressure, located in the dermal papallae
Respiratory system
the system of the body responsible for gas exchange (which occurs specifically in the lungs)
what are the 2 regions of the respiratory system?
conducting region and respiratory region
conducting region
nose to terminal bronchioles (long distance), passageway for the transporting of air to the lungs, conditions air as it passes through various parts (adjusts for humidity and removes particulates), sense of smell, production of speech
respiratory region
respiratory bronchiole to alveoli (short distance), functions to exchange gas
nasal cavities
there are 2, which are separated by the septum, with 2 parts in each: the vestibule and nasal fossae
vestibule of the nasal cavity
cavity of the nose (occurs on the OUTSIDE of the skull, on the protruding part of the nose), functions to condition the air, vibrissae catch large particulates, chamber is small
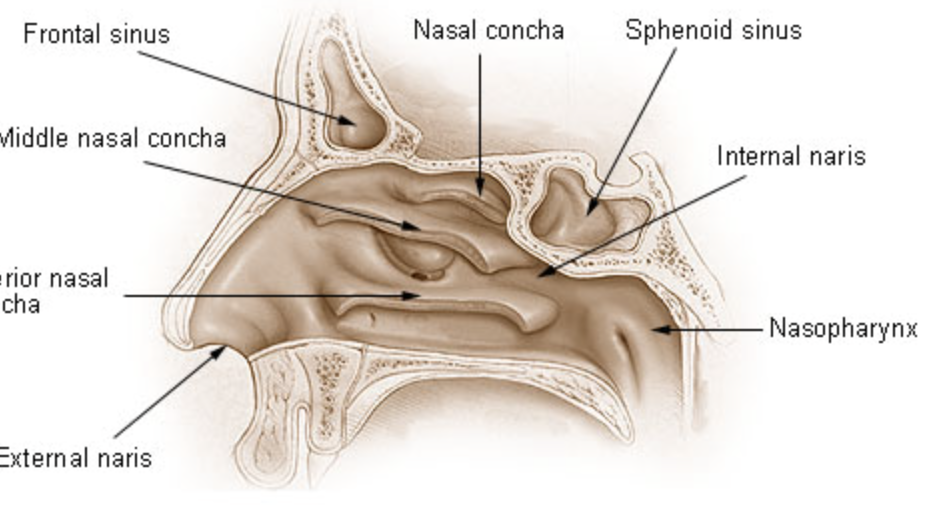
nasal fossae
occur in the skull, surrounded by bone, larger cavity, lateral surface has 3 bony, shelf like projections out of the fossae (superior, middle and inferior, with superior closest to the eyes and inferior closest to the mouth), functions to condition air, increases surface area of nasal fassae (increases contact between air and bony surfaces), causes air to swirl (helps with conditioning)
venus plexus (aka swell bodies)
nasal fossae is covered by epithelium, under epithelium has a branching network of blood vessels called — 2 per body, every 20-30 minutes will swell like a balloon filled with blood, and pushes epithelium outward, decreasing airspace (which increases resistance to flow of air and air goes into the other cavity), as one inflates, the other deflates (advantage because nose gets dry)
swell bodies are sensitive to allergens (when you can’t breathe, it’s because they’re both closing at the same time)
counter current system
air flows from front to back, blood is carried from back to front, larger vessels deliver blood to the posterior region of the nasal fossae (further from the nose)
Heat leaves the blood and warms the air
Surface epithelium in nasal cavities
vestibule is line with non keratinized stratified squamous epithelium (transition epithelium) (change from skin to respiratory epithelium)
epithelium of the nasal fossae
typical respiratory epithelium, composed of ciliated psuedostratified columnar epithelium (most abundant), cilia moves mucous and anything trapped in mucous out of airways (very important function), compromised in kartager’s syndrome)
goblet cells
produce mucous in columnar cells
brush cells in respiratory epithelium
columnar, have microvilli, on their basal surface they form synapses with sensory neurons of the trigerminal nerve (pseudounipolar neurons), general sensation (can generate a sneeze)
cells in nasal fossae
ciliated pseudostratified columnar epithelium, goblet cells, small granule cells, basal cells
basal cells in respiratory epithelium
line the basement membrane (stem cells)
exception to typical respiratory epithelium
superior concha and roof of the nasal fossae (both are within the nasal fossa)
cells of olfactory epithelium
olfactory cells, sustentacular cells, basal cells, brush cells
olfactory cells
afferent (sensory) bipolar neursons, axons penetrate through the basement membrane into the connective tissue and form the fibers of the olfactory nerve
cell body and dendrites are in the epithelium, dendrites go into the aprical surface, ends of dendrites have elongated non-motile cilia which lie flat on the aprical surface, cilia contain receptors for chemicals that have odors (called odorants)
sustentacular cells
most numerous of the epithelium (have microvilli), support olfactory cells, produce odorant binding protein (carrier molecule that helps deliver odorants to receptors)
basal cell of the olfactory epithelium
lies on the basement membrane, stem cells, have the potential to replace any cells in the epithelium (including olfactory cells)
bowman’s glands
an important structure, simple serus acini, olfactory glands, they secrete a watery (serus) secretion onto the epithelium— secretion keeps the surface wet (serves as a solvent for odorants), glands produce secretion continuously (no need for stimulation) helps to wash away old odorants and keeps the surface clean for new ones, located in the lamina propria (CT)
respiratory epithelium
continuous from fossae to larynx, 2 exceptions to respiratory epithelium in the larynx: epiglottis and vocal chords; both have NON keratinized stratified squamous epithelium
trachea
begins at the larynx, extends from the neck to the thorax (chest cavity), about 10 in long, rigid tube (stays open because of crescent shaped rings of hyaline cartilage), when it ends it divides once into 2 passageways
Primary bronchi
the two passageways the trachea becomes, each enter a lung and divides 9-12 more times into smaller passageways called bronchi
bronchioles
smaller than bronchi, what the bronchi divide into don’t have hyaline cartilage
diagram of the respiratory tree
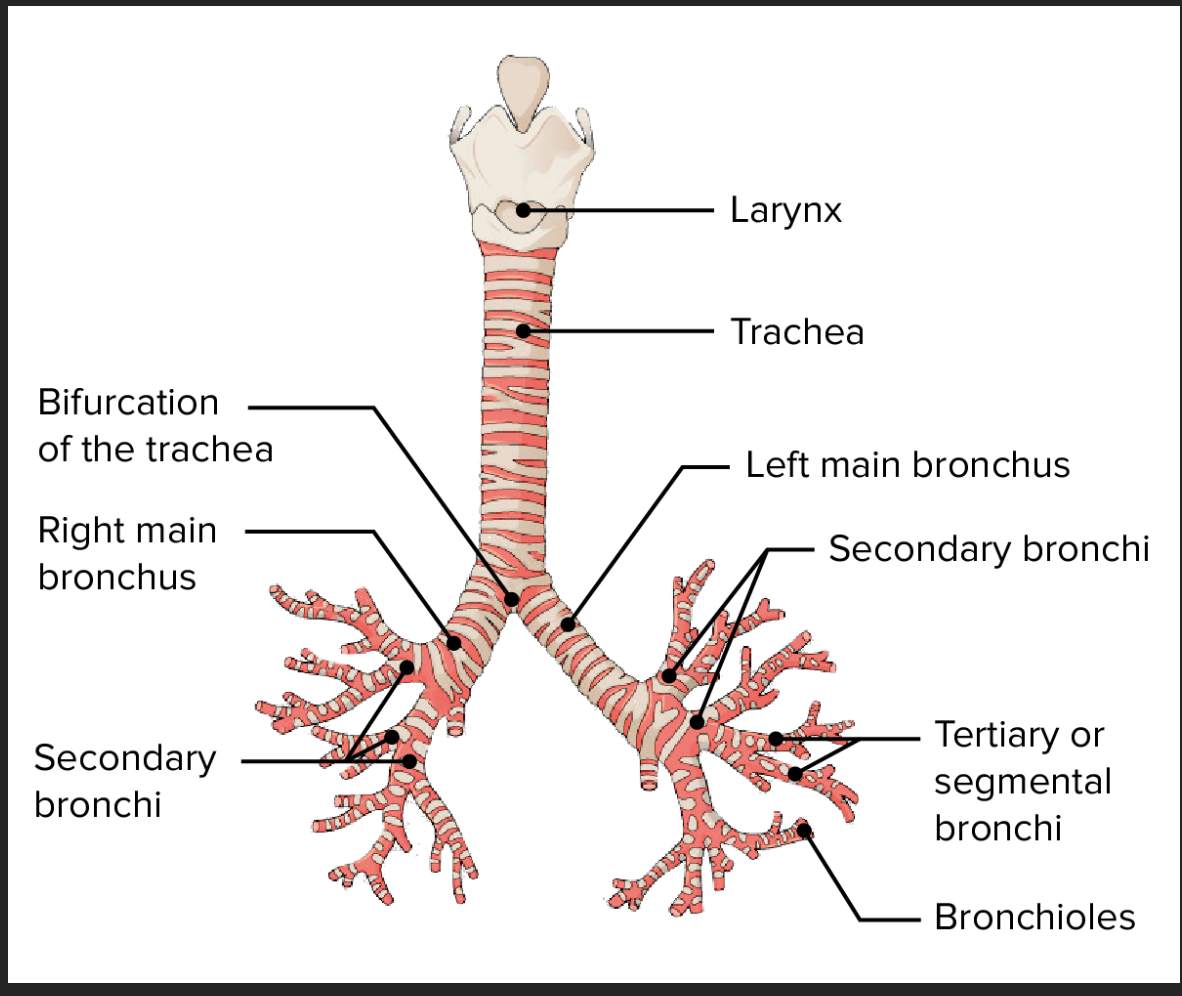
Small granule cell (kulchitsky cell)
respiratory epithelial cell, a part of the diffuse neuroendocrine system (DNES), component cells throughout the body (including the digestive tract), secretory granules (100-300 nm), 2 cell types based on the composition of the granules
Catecholamines: epinephrine, norepinephrine, dopamine; part of APUD cells (amine precursor uptake and decarboxylation), which is what makes them hormones
Other chemical categories: serotonin, peptides, polypeptides
Have a paracrine effect
paracrine
hormones that have localized effects on only one part of the body
endocrine
hormones that have affects on other parts of the body
terminal bronchioles
last part of the conductive portion, changes in the surface epithelium and lamina propria:
surface epithelium changes in heigh (no more stratified)
New cell (club cells) which secrete active agents (lipoprotein which lowers surface tension and prevents collapse of airways) and club cell secretory protein (CC16) which protects the lining by regulating inflammatory processes (antiviral); dome shaped cells
Goblet cells are gone (normally— in smokers, they are present — sign of cancer)
smooth muscle in the lamina propria (controlled by the autonomic NS) — vagas nerve (parasympathetic) controls contraction of the smooth muscle and contraction of the airways, sympathetic NS controls dilation of the airways (relaxation of the smooth muscle) — asthma is caused by these airways causing problems (epinephrine mimics the SNS)
terminal bronchioles divide into respiratory bronchioles
where the respiratory region begins, surface epithelium is identical EXCEPT alveoli are now present (which are expansions of the airways colored in pink below)
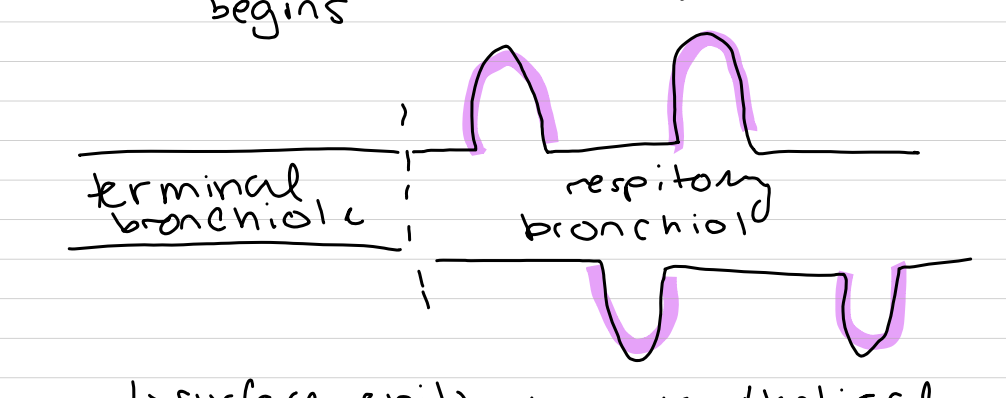
alveoli
simple squamous epithelium where gas exchange occurs
alveolar sac
most efficient airways, cluster of alveoli (end of respiratory system)
alveolar duct
more alveoli than passageways
3 types of cells in alveolar epithelium
type 1 pneumocyte (squamous alveolar cell), type 2 pneumocyte (great alveolar cell), brush cell
dust cell
NOT EPITHELIAL CELL, alveolar macrophage, wanders around engulfing particulates, when full, you sneeze or cough them out
type 1 pneumocyte
97% of alveolar surface, very thin cell
type 2 pneumocyte
3% of alveolar cells, dome shaped, have secretory granules called lamellar bodies, when secreted, known as a pulmonary surfactant (DPPC)
DPPC
phospholipid, most important single component of making the surfactant (decreases surface tension so alveoli can expand), similar to club cell