Microbiology Exam 3
1/171
Earn XP
Description and Tags
chapters 31 and 32
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
172 Terms
In general, infectious diseases that are commonly fatal are newly evolved relationships between the parasitic organism and the host. Why is this?
the immune system has not recognized a disease, so it is not ready to fight it off. it has never seen it before
viruses / the pathogen mutate to a less severe form, leading to coexistence
parasite
organism that lives on or within a host organism
metabolically dependent on the host
causes disease
pathogenicity
ability of parasite to cause disease
virulence
degree or intensity of pathogenicity
determined in part by pathogen’s ability to survive outside host
what are the three characteristics that determine virulence?
infectivity
invasiveness
pathogenic potantial
infectivity
ability to establish focal point of the infection
invasiveness
ability to spread to adjacent tissues
pathogenic potential
ability to cause damage to host
explain the observation that different pathogens infect different parts of the host
different parts of the body have different environmental conditions so some grow more optimally in different places
viruses need to attach to specific receptors
mode of transportation or spread
Three factors impacting the outcome of host-parasite relationships
number of organisms infecting the host
the degree of pathogenicity (virulence)
host’s defenses or degree of resistance
signs
objective changes in body that can be directly observed
symptoms
subjective change experienced by patient
disease syndrome
set of characteristic signs and symptoms
course of infectious disease
incubation period
prodomal stage
period of illness
convalescence
incubation stage
period after pathogen entry, but before signs and symptoms appear
prodomal stage
onset of signs and symptoms
not clear enough for diagnosis
period of illness
disease is most severe and has characteristic signs and symptoms
convalscence
signs and symptoms begin to disappear
understand this graph
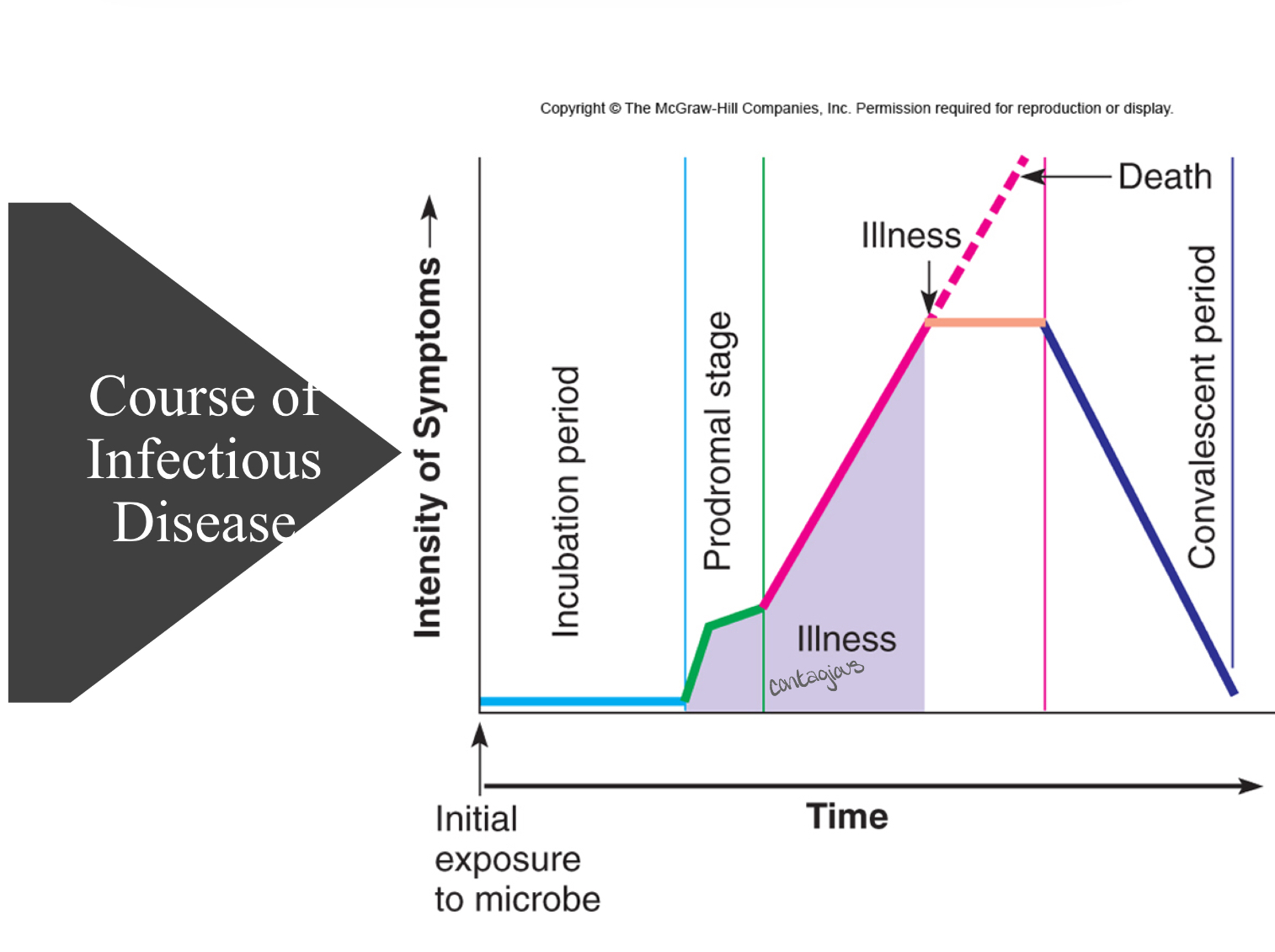
how to tell what pathogen caused the disease
Koch’s postulate
clinical micro lab
important for isolation and identification
determines susceptibility to antimicrobial agents
source
location from which pathogen is immediately transmitted to host
can be inanimate or animate
period of inactivity
time during which source is infectious or is disseminating the organism
reservoir
site or natural environmental location in which pathogen is normally found
sometimes functions as the source of pathogen
carrier
infected individual who is a potential source of infection for others
(human)
4 types of carriers
active
healthy
incubatory
convalescent
(all human)
active carrier
has overt clinical case of disease
healthy carrier
harbors the pathogen but is not ill
incubatory carrier
is incubating the pathogen in large numbers and is in the beginning stages of disease
convalescent carrier
has recovered but continues to harbor large numbers of the pathogen
zoonoses
animal diseases that can be transmitted to humans
(animal)
zoonoses transmission to humans
direct or indirect
contaminated milk
inhaling dust particles contaminated by animal excreta
eating insufficiently cooked meat
vectors
organisms that spread disease from one host to another
e.g. mosquitoes, ticks, flies
(animals)
4 main routes of transmission
airborne
contact
vehicle (indirect mode)
vector-borne
airborne transmission
pathogen suspended in air and travels up to 1m from source to the host
droplet nuclei
can remain airborne for long time, travel long distances
usually propelled from respiratory tract (sneeze, cough, vocalization)
contact transmission
coming together or touching of source/reservoir and host
direct and indirect contact
direct contact
person to person
physical interaction between source/reservoir and host
e.g. kissing, touching, sexual contact
indirect contact
involves an intermediate (usually inanimate)
e.g. eating utensils, bedding, door handles
vehicle transmission
inanimate object involved in pathogen transmission
common: single vehicle spreads pathogen to multiple hosts
e.g. water, food, surgical instruments, bedding, etc.
fomites
object that is not harmful itself but is able to harbor and transmit pathogenic organisms
vector-borne transmission
Transmission can be either external or internal
external (mechanical):
passive carriage of pathogen on body of vector
no growth of pathogen during transmission
e.g. flies carry Shigella on their feet from a fecal source to a plate of food
internal:
pathogen is carried within the vector
e.g. rat fleas carry Yersinia pestis (cause of plain)
2 factors effecting susceptibility
defense mechanism of the host
pathogenicity of the pathogen
nutrition, genetic predisposition, and stress also play a role
how do pathogens leave the host
active or passive escape
active escape
active movement of the pathogen to portal of exit
e.g. parasites migrate through the body, reach the surface, and exit
passive escape
most common
excretion in feces, urine, droplets, or saliva
non-specific immune system
acts as first line of defense, acts immediately
offers resistance to any microbe or foreign material
lacks immunological memory
occurs to the same extent each time a microorganism is encountered
another name for non-specific immune system
innate immune system
specific immune system
resistance to specific foreign agent
has memory
effectiveness increases on repeated exposure to agent
another name for specific immune system
adaptive immune system
antigens
something recognized as foreign
specific in shape
invoke immune responses
cause specific cells to replicate
innate immune system cells & tissues
granulocytes
macrophages
dendritic cells
NK cells
(inflammation & cell cooperation)
innate immune system physical barriers
skin
mucous membranes
(resident responders)
prevent pathogens from entering the body
first line of defense
effectiveness impacted by age, genetics, nutrition, and personal hygiene
innate immune system chemical mediators
defensins
lysozyme
complement
(opsonization)
acquired immune system cells & tissues
T cells
B cells
(opsonization, resident responders, inflammation)
leukocytes
white blood cells
involved in both immune systems
hematopoesis
development of white blood cells in bone marrow
(leukocytes)
comparison of white and red blood cells
there are way more red blood cells, but white blood cells fight infections
monocyte
immature macrophage
macrophage
highly phagocytic
reside in tissues
variety of surface receptors
toll-like receptors
toll-like receptors
recognize LPS (gram negative bacteria)
granulocytes
cytoplasm contains granules, during an infection/infalmmation granulocytes rush to the area and release granules, these can kill microorganisms
3 classes of granulocytes
basophil
eosinophil
neutrophil
basophil
allergies and hypersensitivity reactions
eosinophils
allergies and parasitic infections
neutrophils
migrate to sites of tissue damage and attack bacteria
dendric cells
contain more surface area
contact invading pathogen
uses 3 Ps
3 Ps
phagocytosis
process (break into smaller pieces)
presentation (on outer surface)
lymphocytes
specific population of white blood cells
major cells of the immune system
what two populations are included in lymphocytes
B cells & T cells
lymphocytes in action
require a specific antigen to bind to a surface receptor (B or T cell)
lymphocytes divide once activated
some form memory cells
memory cells
subset of lymphocytes that will respond later in host’s life when antigen is present again
B lymphocytes
B cells
mature in bone marrow
after maturation and activation, these are called plasma cells and produce antibodies
T lymphocytes
T cells
mature in the thymus (next to heart)
require antigen binding to surface receptors for activation and replication
primary organs and tissues
sites where lymphocytes mature and differentiate into antigen-sensitive mature B and T cells
includes bone marrow and thymus
secondary organs and tissues
area where lymphocytes may encounter and bind antigen
followed by proliferation (dividing) and differentiation into fully mature effector cells
includes spleen (filters blood) and lymph nodes (filters lymph)
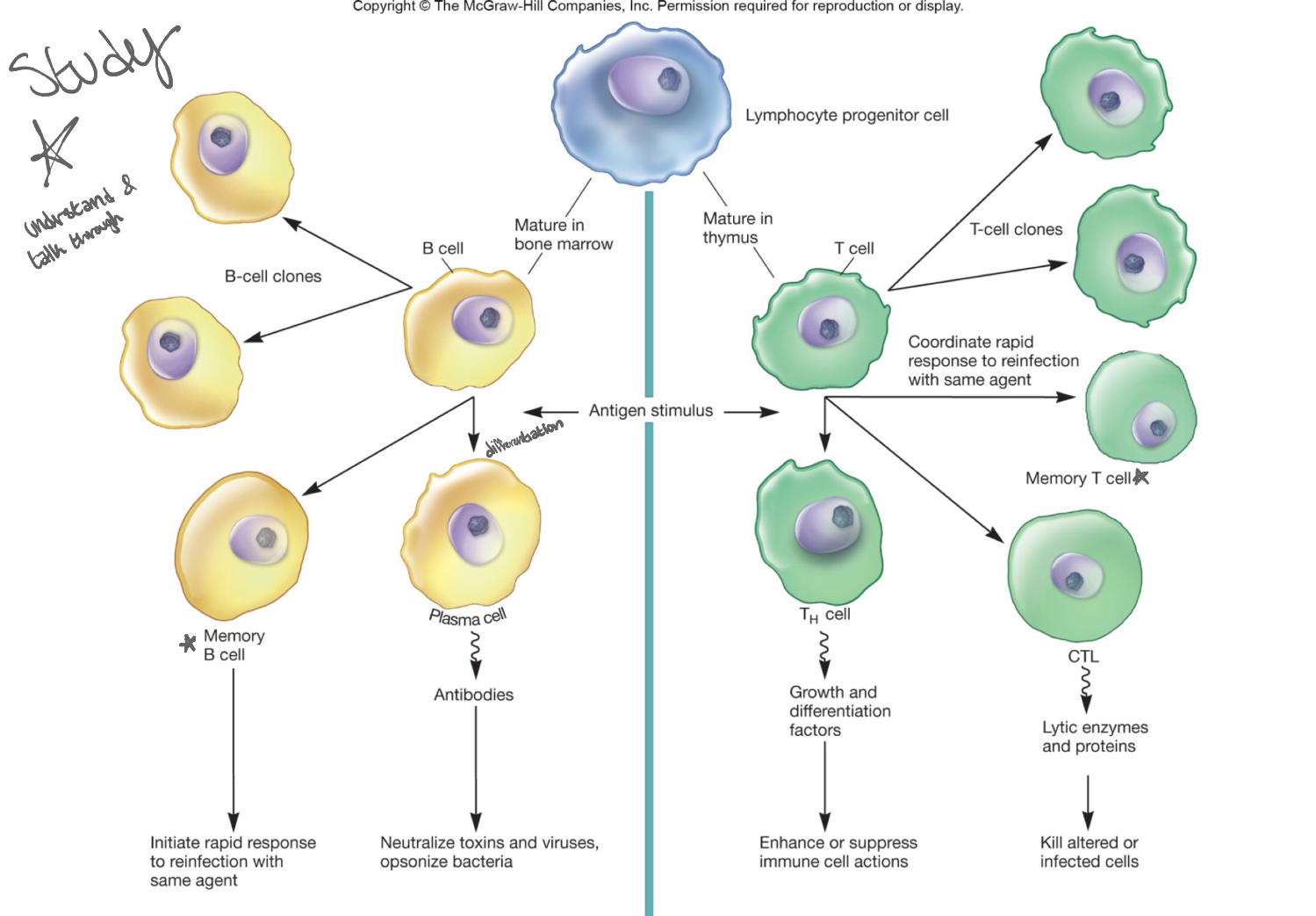
understand and talk through this diagram
Lymphocyte cells develop into B cells (bone marrow) and T cells (thymus). When exposed to an antigen, both undergo clonal expansion (make identical copies).
B cells → become plasma cells (produce antibodies to neutralize pathogens) and memory B cells (enable faster response if the same antigen returns).
T cells → become:
Helper T cells (TH): release signals that regulate and activate other immune cells
Cytotoxic T cells (CTL): directly kill infected or abnormal cells
Memory T cells: allow a faster response to future infections
phagocytosis
engulf
process by which phagocytic cells recognize, ingest, and kill extracellular microbes
e.g. macrophages, dendritic cells, and neutrophils
mechanisms for recognition of microbe by phagocyte
opsonin-independent recognition
opsonin-dependent recognition
opsonin-independent pathogen recognition
Common pathogen components are non-specifically recognized to activate phagocytes
pathogen-associated molecular patterns (PAMPs) detected by pattern recognition receptors (PRRs)
example: toll-like receptors
PAMP meaning
pathogen associated molecular patterns
PRR meaning
pattern recognition receptors
PAMPs
conserved microbial molecular structures that occur in patterns
detected by phagocyte
unique to microbes, not present in host
LPS of gram-neg, peptidoglycan of gram-pos, or flagella
recognized my PRRs on phagocytic cells
toll-like receptors (TLRs)
PRRs that function exclusively as signaling receptors
recognize and bind unique PAMPs of viruses, bacteria, or fungi
binding is communicated to the host cell nucleus which initiates the host response
steps of phagocytosis
binding of specific microbial components to receptors of phagocyte
microbes can be internalized as part of a phagosome
toxic oxygen products are produced which can kill invading microbes
what happens to microbial invaders once they have been killed and digested
exocytosis
antigen presentation
exocytosis
after neutrophils break down microbes, the fragments are expelled
opsonin-independent mechanism of pathogen recognition
PAMPs (on microorganism) are recognized by toll-like receptors (on the phagocytic cell)
PAMPs are molecular signatures of infection
allows innate immune system to distinguish self from microbial non-self
how do opsonins promote phagocytosis?
by tagging foreign pathogens, bridging them to phagocytes (like macrophages and neutrophils), and overcoming negative electrical charges that cause repulsion
inflammation
nonspecific response to tissue injury
can be caused by a pathogen or physical trauma
acute inflammation is the immediate response of body to injury or cell death
4 cardinal signs of inflammation
redness
warmth
pain
swelling
acute inflammatory response: chemical mediators
chemokines
selectins
integrins
chemokines
released by injured cells
activate the endothelium on nearby capillaries
selectins
cell adhesion molecules on activated capillary endothelial cells
integrins
adhesion receptors on neutrophils
attach selectins
acute inflammatory response: processes
margination
diapedesis
extravasation
margination
neutrophils stick to endothelium
stop rolling
diapedesis
neutrophils change shape and squeeze through the endpthelial wall
extravasation
neutrophils move into the tissue and migrate to the site of injury
skin - how do they protect
inhospitable environment for microbes
shedding of outer layers
pH is slightly acidic
high NaCl conc.
drying
mucous membrane - how do they protect
form a protective coating that resists penetration and traps microbes
often bathed in lysozyme, which breaks down peptidoglycan
where are mucous membranes found
eye, respiratory, digestive, and urogenital system