NUR 315 Exam 3 - Discharge Teaching
1/27
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
28 Terms
Role of discharge teaching
Provides anticipatory guidance for patients' needs after discharge
Serves as checkpoint of family's understanding and knowledge gaps
Empowers family to be involved in decision-making
Identifies risk factors
Establishes referrals as soon as possible
Prevents inappropriate discharge and/or readmission and unknowing harm
Support maximum wellness
How to teach
Identify the Teaching Audience
Mother, Legal guardian(s), Support person present, Support person/people for after hospital discharge
Tailoring the Teaching Approach
Use small teaching moments from admission to discharge rather than "all at once"
Better retention
Allows more time for questions and clarifications
Assess health literacy and readiness to learn, extent and recency of maternal-infant care experiences, family/cultural dynamics, what is realistic for the family
Health self-advocacy
Care of body, mind, spirit all necessary to improvement adjustment
Takes several weeks to feel a sense of normalcy
Takes several months to feel adjusted to the new normal
Use your support people as much as possible so you can rest, heal, and care for your baby
Sleep when ever the baby sleeps - other things can wait.
Resumption of daily activities
No driving for 2 weeks after delivery - No driving if taking narcotics
Do not lift anything heavier than baby or diaper bag for 2 weeks
Shower as often as you like - Avoid tub bath or swimming until after postpartum check-up
Gradually resume normal activities, short, mild exercise and increase as tolerated; ambulate - Bleeding could slightly increase after times of activity
Nutrition and elimination
Can take several months to return to pre-pregnancy weight
Do not lose more than 2 lb per week
Continue taking prenatal vitamins
Drink water to meet thirst (extra water intake does not increase breastmilk)
Well-balanced diet high in protein and fiber - add 500 cal/day if breastfeeding
Bowel function should return to normal in a few days - Use stool softeners, do not strain
Uterine and pelvic floor changes
Uterus should be midline and firm
Afterpains (mild contractions) spontaneously and with breastfeeding
Involution of uterus; non-palpable by 2 weeks after delivery
Quicker with primiparous women
Takes longer in multiparous women
Pelvic floor and vaginal tone are reduced (instruct on Kegel exercises)
How to do kegels
Find the right muscles by stopping urination in midstream. You can do Kegels in any position, although it may be easier lying down.
Perfect your technique. Imagine you are sitting on a marble and tighten your pelvic muscles as if you're lifting the marble. Try it for three seconds at a time, then relax for a count of three.
Maintain your focus. Tighten only your pelvic floor muscles. Be careful not to flex the muscles in your abdomen, thighs or buttocks. Avoid holding your breath.
Repeat three times a day. Aim for at least three sets of 10 to 15 repetitions a day.
Pericare and bleeding
Empty bladder frequently
Use peri bottle with clean warm water to rinse perineum
Sitz bath frequently to expedite healing
Bleeding patterns over 2-6 week time frame: Bright red to dark red to brown to yellow-white
Bleeding may increase with activity
Small clots okay, golf-ball or larger not ok
Resumption of menses and sexual activity
If not breastfeeding, menses may return 4-6 weeks after delivery
Breastfeeding tends to delay the return of menses until weaning occurs
Ovulation and fertility can return at any time
Nothing in the vagina for 6 weeks
No body parts or other objects
No tampons
No douching
Breast care
Wear well-fitting bra without underwire
Breastfeed frequently
Ensure correct latch and proper milk transfer
Lanolin cream or olive oil to soothe chafing
OTC pain relievers, ice packs, cabbage leaves, shredded potatoes...
Frequent milk removal, massage, and positioning for clogged ducts
Seek help if you feel lactation is not going well or infant is not feeding well
Psychosocial adjustment
Normal to experience a wide range of emotions - Baby blues vs. Postpartum depression
Allow yourself to modify plans and expectations
Ask for and accept help
Identify support system - Talk with others that can understand
Maternal care contact the provider if:
Temperature 100.4 or greater
Chills, malaise, and flu-like symptoms
Unrelieved pain in back, side, or incision
Bloody or purulent drainage from incision
No bowel movement for four days or longer
Frequent urgency or burning on urination
Hot, firm, red area of the breast
Persistent headache despite taking analgesics
Unilateral swelling in legs
Bleeding remains heavy despite rest
Saturating more than a pad in an hour
Passing multiple clots or clots egg size or bigger
Foul-smelling vaginal bleeding
Social withdrawal
Persistent baby blues or depression

Normal newborn appearance: skin
Tailor the teaching to specific characteristics the newborn
It is common for newborns to develop blemishes or rashes
Dry, peeling skin (desquamation) will resolve on its own
Normal newborn appearance: breasts, genitalia
Mild breast engorgement, Witch's milk: drops of newborn "breastmilk"
Redness and swelling of genitalia, blood-tinged, mucus-like discharge
Resolves within a few days
Normal newborn appearance: head shapes
Egg-shaped, pointed, or flattened head from birth - Molding resolves within a week or so
While the newborn is awake, hold or place the newborn in a variety of positions to prevent placing repeated pressure on the same part of the head
Normal newborn appearance: eyes and ears
Visual acuity about 8-10 inches away from face (feeding distance is perfect!)
Eye color gray-blue or brown at birth
Eye color does not finalize until about 6-12 months after birth
Occasional crossing of eyes until about 4 months after birth
Basic newborn care
Dress in one more layer than an adult would wear
Infants are sensitive to overheating or becoming too cool
File rather than cut nails to prevent accidental clipping of the skin
Use mild non-perfumed soaps and detergents
How to use a suction bulb
Newborn hygiene
Sponge bathe until umbilical cord falls off and circumcision heals
Do not bathe everyday
Test water temperature before bathing (set water heater <120 degrees)
Keep umbilical cord dry, no special cleaning needed
Uncircumcised males: do not forcibly retract foreskin, clean with mild soap and water
Circumcised males: Clean by squeezing warm water over area until healing is complete
Females: Clean from front to back to prevent contamination
Newborn hygiene
Sponge bathe until umbilical cord falls off and circumcision heals
Do not bathe everyday
Test water temperature before bathing (set water heater <120 degrees)
Keep umbilical cord dry, no special cleaning needed
Uncircumcised males: do not forcibly retract foreskin, clean with mild soap and water
Circumcised males: Clean by squeezing warm water over area until healing is complete
Females: Clean from front to back to prevent contamination
Diapering
Change diaper in a safe place and do not leave unattended
Clean thoroughly between skin folds
Expect 6-8 wet diapers in 24 hours
Typical stool color, consistency, and frequency
Stools may become less frequent as the weeks progress
Soothing the baby
ABOUT CRYING
Reasons babies cry
Hungry, wet, hot, cold, overstimulated, bored, need for human contact
Never shake the baby
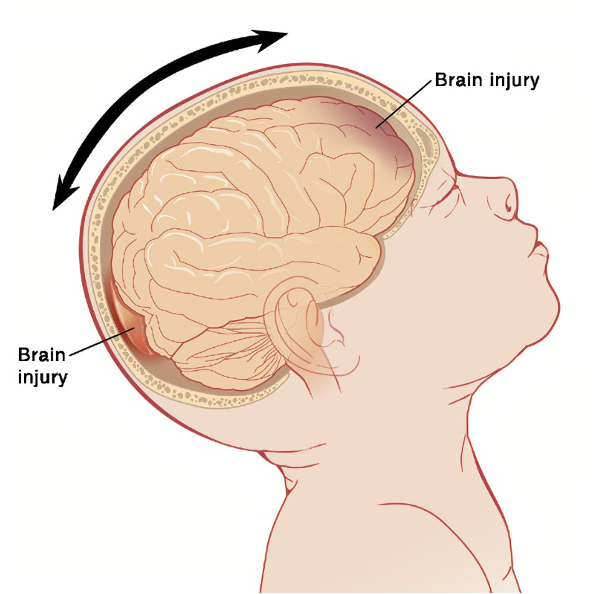
Discuss shaken baby syndrome
A severe form of child abuse caused by violently shaking an infant, leading to brain damage, subdural hemorrhage, and retinal hemorrhages
WAYS TO SOOTHE
Check diaper
Feed
Rock, go for walk or car ride, massage or pat baby
Swaddle
Talk
Background noise
Skin-to-skin
Feeding the baby
Breastfed babies feed on demand, bottle fed babies every 4 hours or less
At least 6+ wet diapers per day and 3+ poopy diaper per day
Basic principles of a good latch reach out for help if concerned
How to prepare formula
Jaundice
Jaundice causes yellowing of the skin and eyes.
In most cases, the appearance of jaundice self-resolves.
Small, frequent feeds and some (limited) time in the sunlight help
Concerning jaundice causes poor feeding, prolonged sleep, true lethargy
Contact pediatrician if there are any concerns!
Sleep patterns
Newborns sleep approx. 16 hours per day for a few hours max.
Neither realistic nor healthy for newborn to sleep through night
Bedtime routines can help newborn differentiate night and day
Day: Light on, wake for feedings, make noise, keep eye contact
Night: Dim lights, keep room quiet, decrease stimulation
Safe sleep environment
Always place infant on back for sleeping until 1 year old
No toys, extra blankets, etc. Nothing in the crib but the baby.
Firm, flat mattress
Crib or bassinet with 4 immovable, tall sides and narrow slats (2 and 3/8")
Do not share sleeping surface
Do consider sharing the sleeping room 6 months to 1 year+
Keep the baby's hands free from the swaddle once able to roll over
Make contingency plans for safe sleeping surfaces
Sudden Infant Death Syndrome and accidental suffocation and strangulation in bed
Sudden Infant Death Syndrome (less common)
Cause is unknown
Possible cause: immature or damaged medulla oblongata does not detect rising CO2 levels, resulting in prolonged apnea
Diagnosed when other causes of death are ruled out by autopsy
Preventing SIDS:
Breastfeed/offer small, frequent feeds
Eliminate or reduce smoke exposure
Discourage excess use of alcohol, sedatives, illegal drugs, etc
Share sleeping room
Consider pacifier use
Accidental Suffocation and Strangulation in Bed (more common)
Preventing ASSB:
All SIDS prevention recommendations, plus...
No crib "spires" or cut-outs
No attachments, crib bumpers, pacifier cords, stuffed animals, blankets, pillows, loose blankets, positioners, etc
No nearby electrical cords, blinds, baby monitor cords
Do not leave sleeping baby in car seat after the drive is done
Do not sleep with baby in arms, especially rocking chairs/couches
Infant car seat safety
Do not leave the infant unattended in the car
Do not have infant in front seats or in seats with air bags
Use a car seat every time the infant is in a vehicle
Keep rear-facing in leveled car seat until 2 years old and as long as the weight-limit of the car seat allows
Okay if infant falls asleep while you are driving, but remove and put in safe sleeping environment once home
Encourage car seat technician to inspect for proper installation
Correctly harness the baby
Newborn care when to contact provider
Vomiting (note color and if projectile)
Lethargic and hard to wake up
Frequent loose stool with excess fluid, mucus or unusually foul odor
No stool for 48 hours
No wet diapers for 12 hours
Changes in typical behavior
Unusual or high-pitched cry
Temperature <97.5 F or >100.4 F
Patches of white found in the baby’s mouth (possible thrush, a fungal infection)
Erythema, purulent drainage around umbilical cord or bleeding more than a few drops
Purulent drainage or bleeding from circumcision
911 if experiencing respiratory distress like oral cyanosis, central cyanosis, difficulty breathing or if unresponsive