MLS Exam #4 (M)
1/348
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
349 Terms
What is the underlying reason that someone w/ HIV becomes immunosuppressed?
The virus will chronically & progressively deplete CD4 T-cells
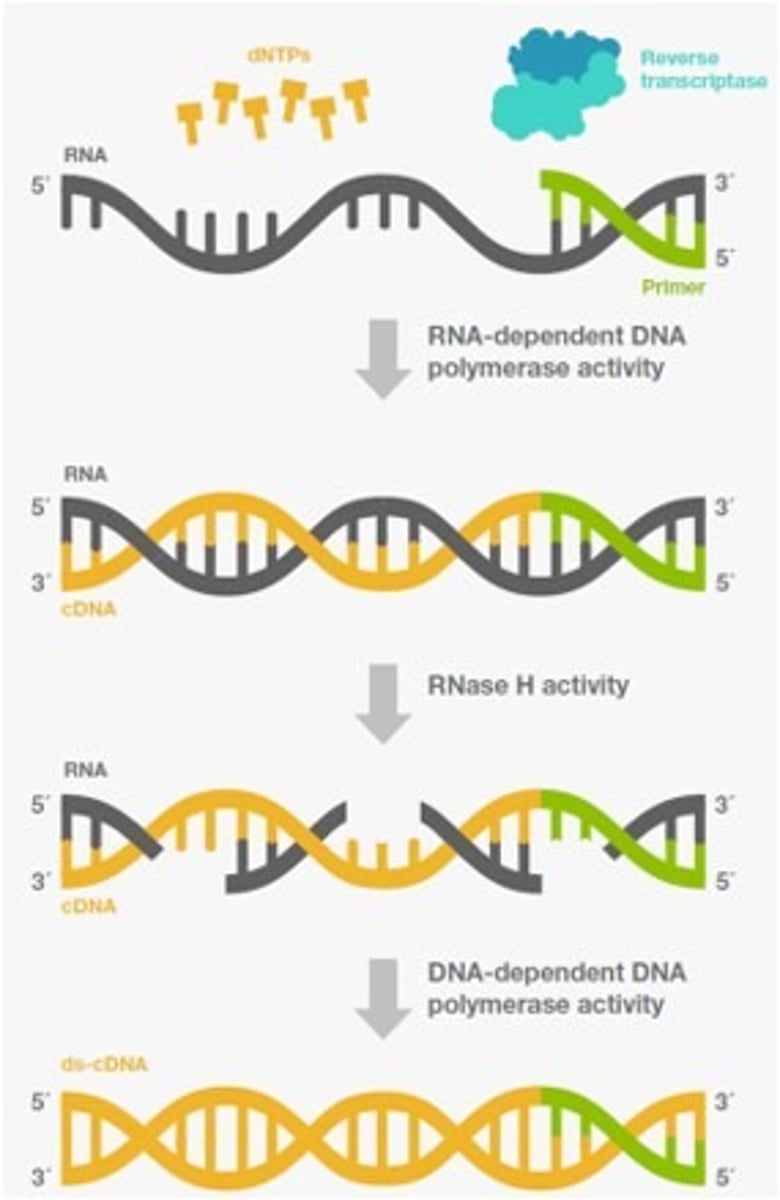
How do the HIV viruses 1 & 2 exert their effects?
Are retroviruses - they use a reverse transcriptase enzyme to create complimentary DNA from an RNA template
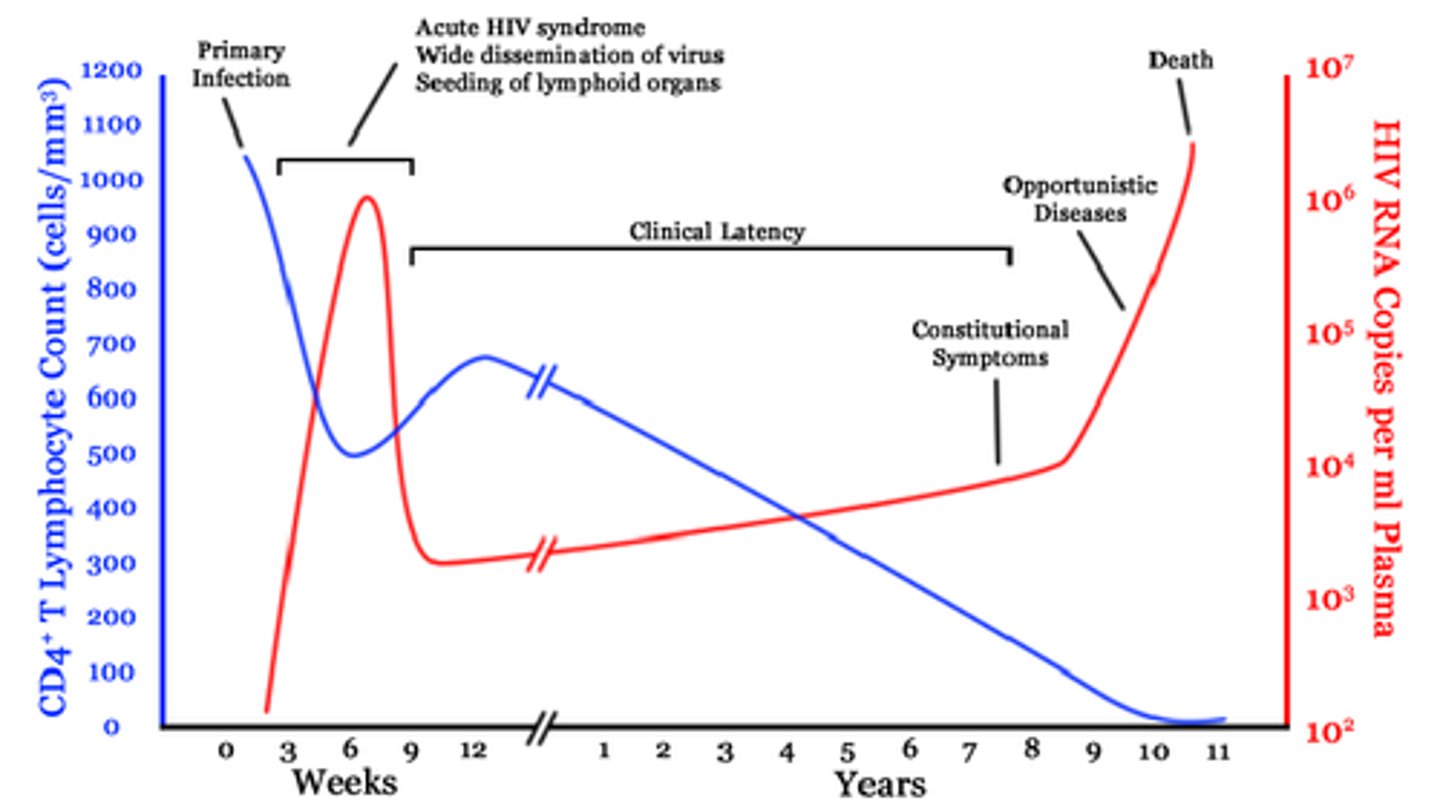
What CD4 count classifies as Stage I (acute), stage II (latent/chronic), & stage III (AIDS) infection, respectively?
Stage I: > 500 cells/mcL
Stage II: 200-499 cells/mcL
Stage III: < 200 cells/mcL
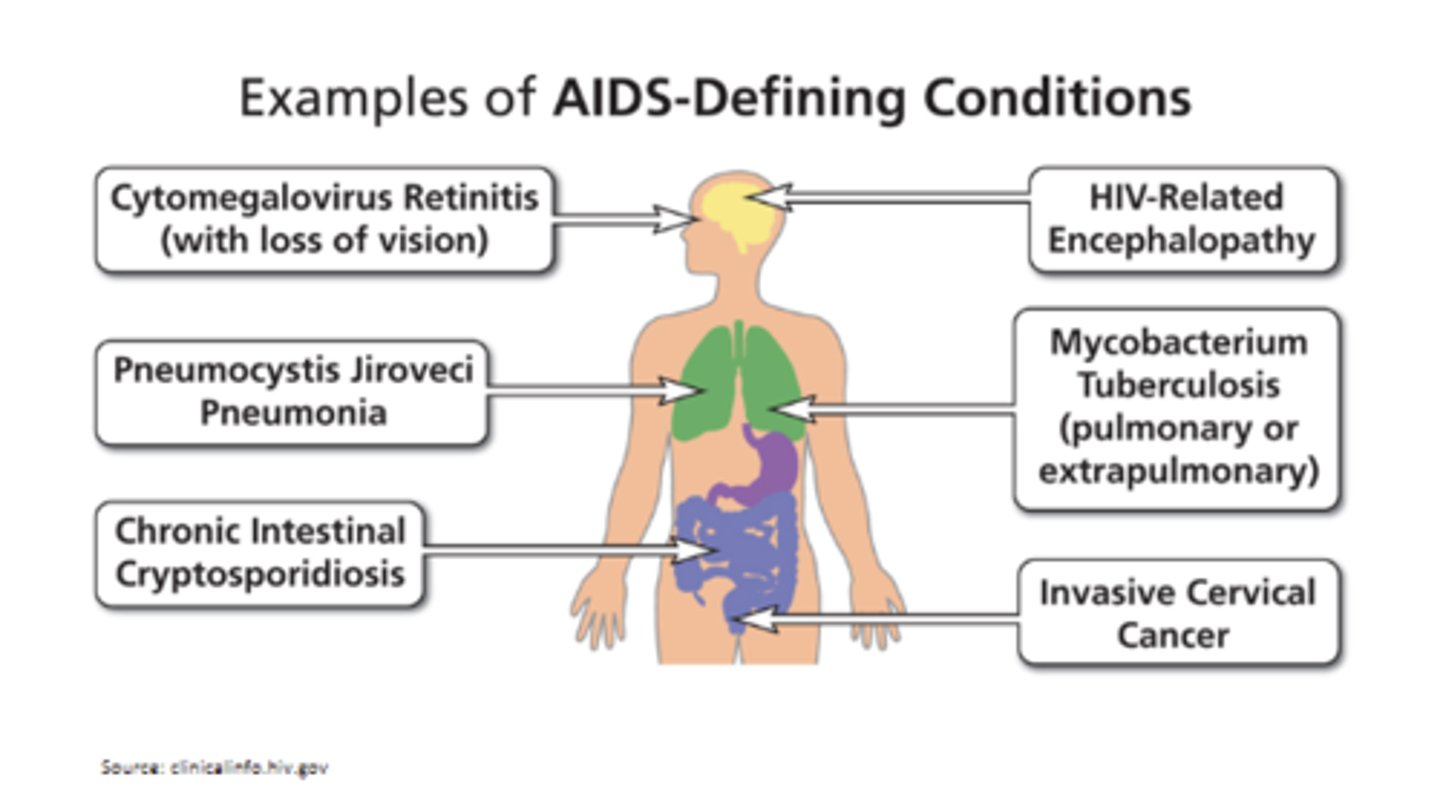
What are some examples of AIDS-defining conditions (indicate patient is severely immunocompromised)?
Esophageal/bronchial candidiasis, CA, Kaposi's sarcoma, Pneumocystis jiroveci pneumonia, disseminated infections, multiple fungal types of infections, TB
How is HIV transmitted?
Primarily blood & blood products; can also be through sexual contact, IV drug use, & perinatal
What are some s/sxs of HIV?
Very generic things such as weight loss, fever, night sweats, LAD, diarrhea, etc.; recurrent infections & generalized LAD are more telling
How is HIV usually screened for & confirmed, respectively?
Screening: HIV-1/2 & p24 antigen combo immunoassay
Confirmation: NAAT (HIV-1/2 antibody differentiation often done before)
In general, what is highly-active antiretroviral therapy (aka HAART)?
Med combos consisting of NRTIs, NNRTIs, & protease inhibitors that are used to treat HIV (many many formulations out there - it is possible for these patients to have viral suppression to the point where they are asymptomatic!)
What are 3 baseline tests we want to do on all HIV-positive patients to monitor the efficacy of HAART?
1) Resistance testing
2) HIV RNA load
3) CD4 count
According to the most recent guidelines, what CD4 count & HIV viral RNA load warrants us starting HAART?
Trick question - we should start therapy ASAP regardless of CD4 count
What is the preferred HAART regimen for HIV?
2 NRTIs (nucleoside reverse transcriptase inhibitors) plus one other agent (protease inhibitor, NNRTI, NSTI)
How is a pre-exposure prophylaxis (PrEP) regimen often dosed? What about a post-exposure prophylaxis (PEP) one?
PrEP: 2-1-1 method (2 pills 24 hrs before high-risk activity, 1 pill 24 hrs after, & another 24 hrs after this)
PEP: start within 72 hrs of exposure & continue for 28 days
What is an example of a prophylactic drug against Pneumocystis pneumonia?
TMP-SMX
What is idiopathic pulmonary fibrosis (IPF), & what may be a possible cause?
Chronic progressive scarring from persistent inflammation; exposures (medications, environmental, occupational, etc.)
What are some s/sxs of IPF? What is a pretty common complication?
Progressive exertional dyspnea, cough, fine b/l basilar end-inspiratory rales, digital clubbing (indicates hypoxia), cyanosis, & possible pulmonary HTN/cor pulmonale; GERD
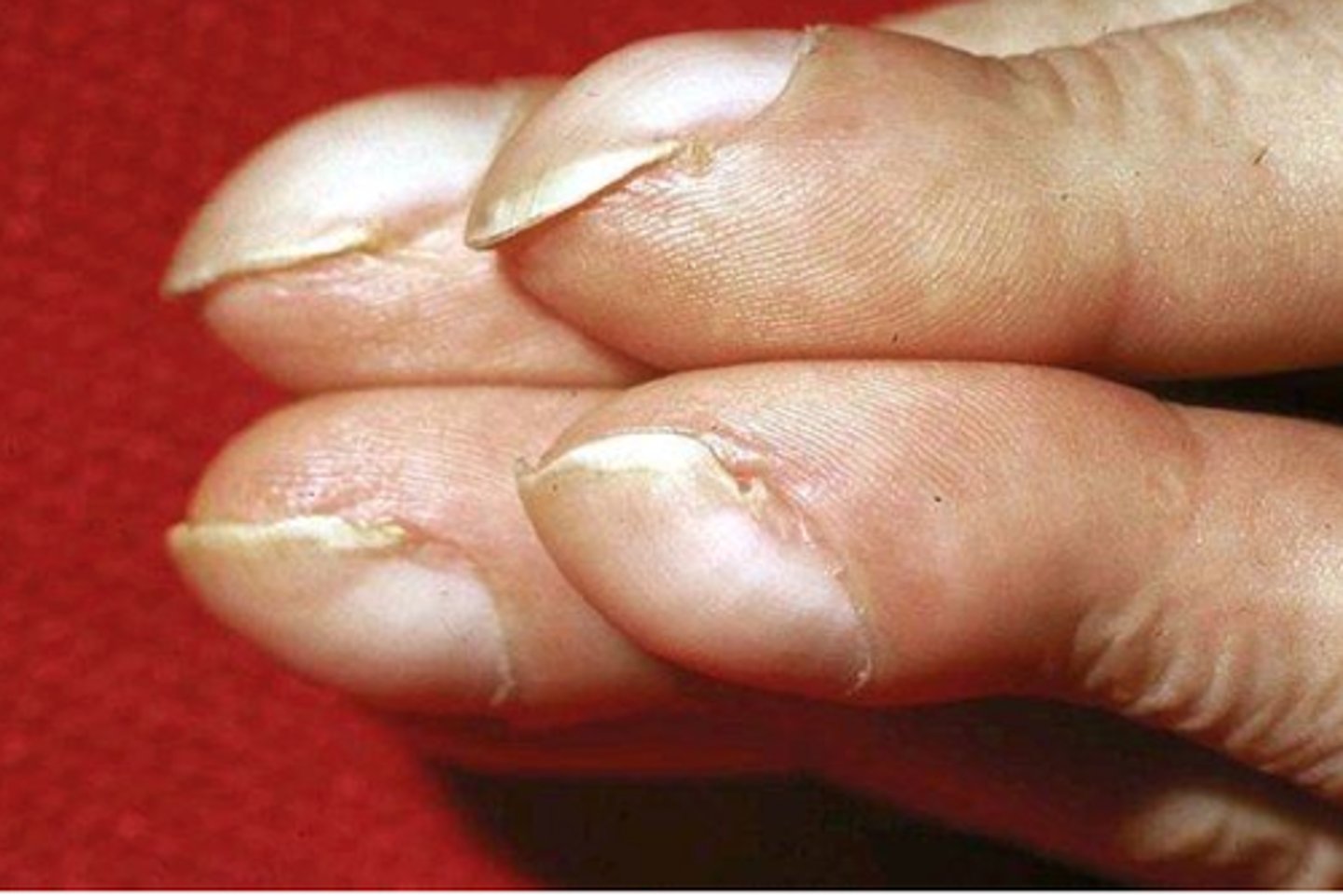
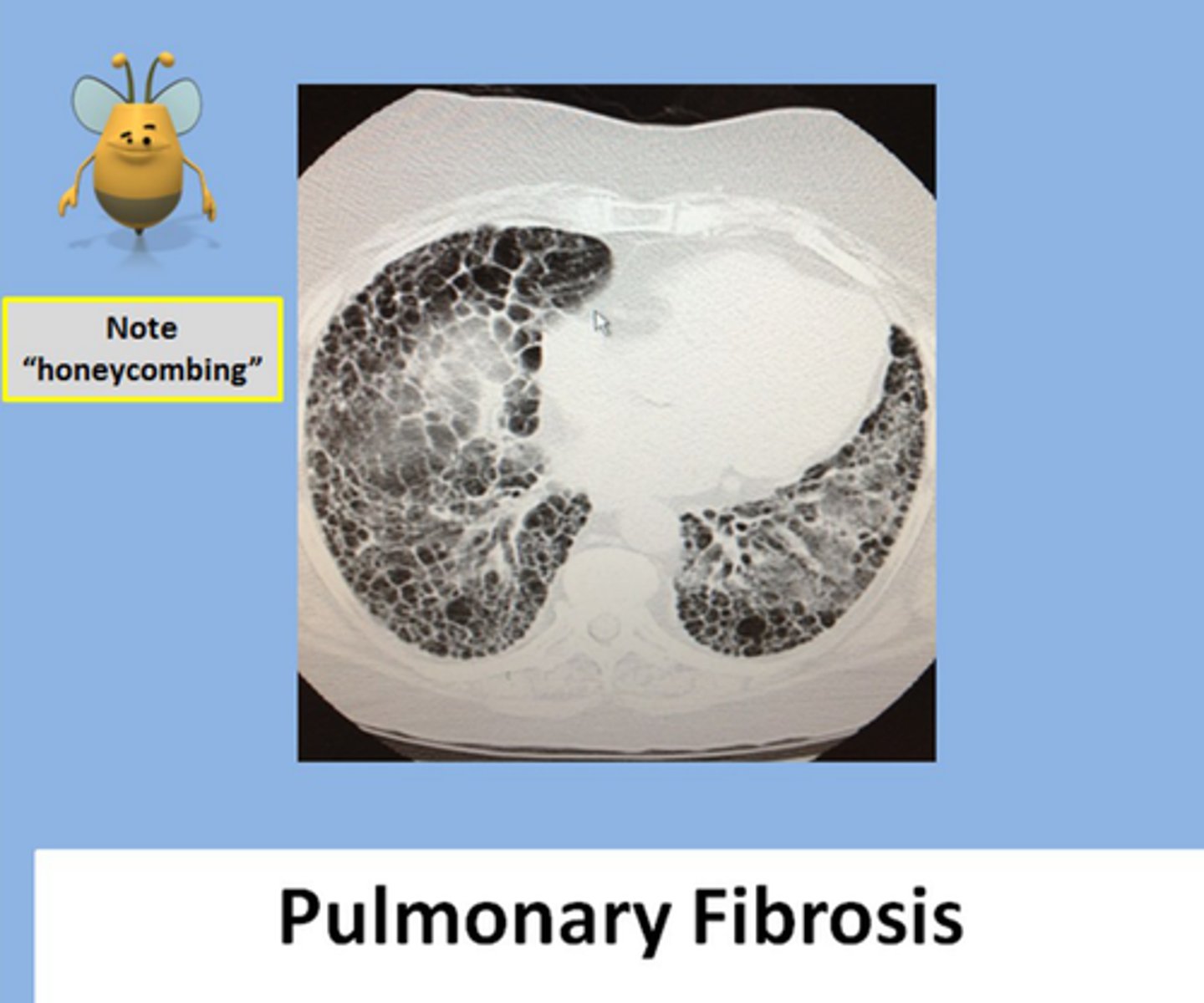
What is the best diagnostic tool for IPF? What is the preferred imaging modality, & what will be seen?
Lung biopsy (via VATS or bronchoscopy); CT (shows fibrosis & "honeycombing" blebs)
What is the definitive treatment for IPF?
Lung transplant (not many other great options tbh)
In general, what is pneumoconiosis?
Umbrella term for any chronic lung disease due to inhalation of various dusts/irritants, often work-related
What is silicosis?
Inhalation of silica dust resulting in chronic inflammation & fibrosis

What is a good diagnostic tool for diagnosing silicosis? What will we see?
CXR; shows progressive massive fibrosis & "eggshell" calcifications (hilar lymph node calcification)
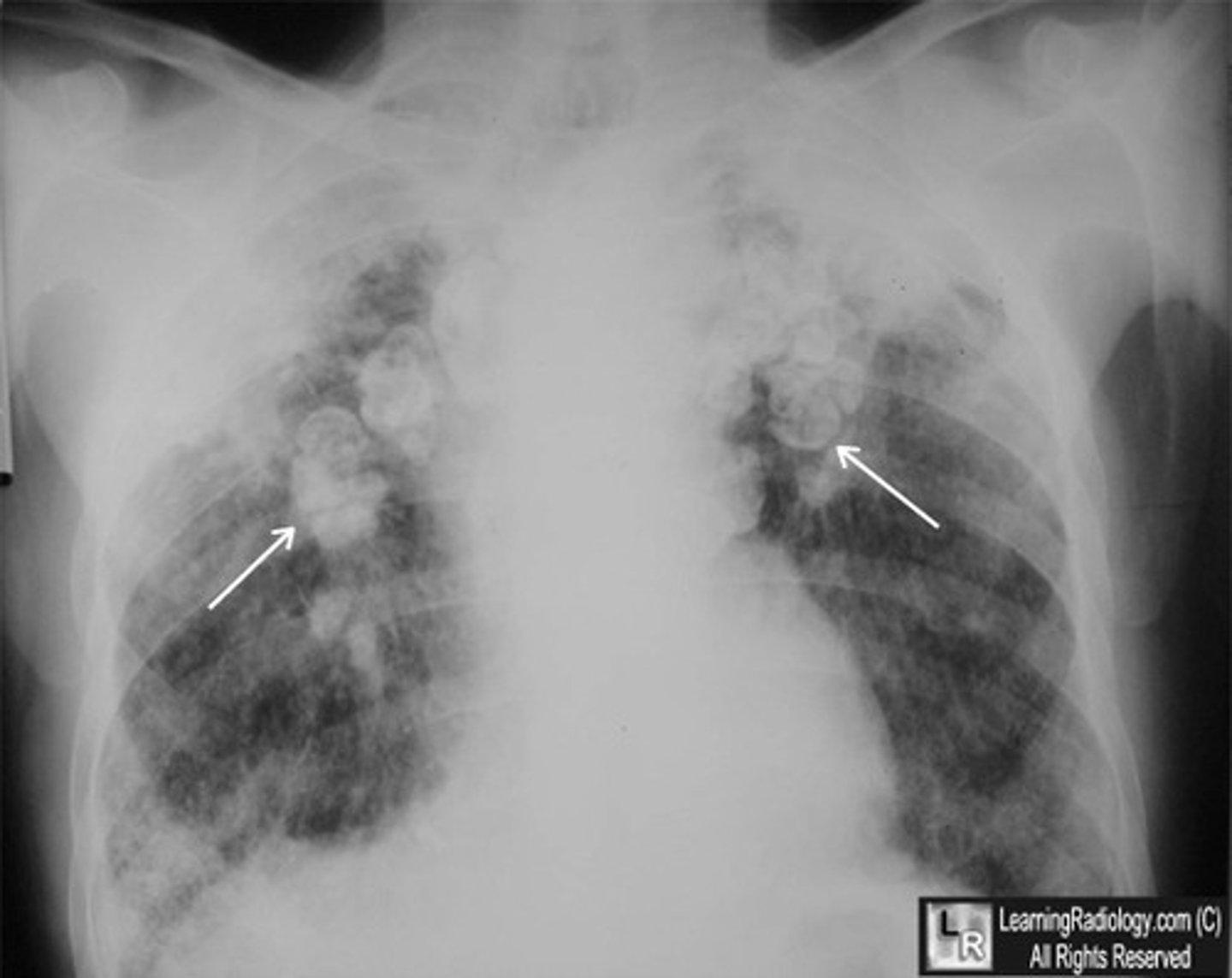
What is another lung pathology we need to rule out in cases of suspected silicosis?
TB (resembles silicosis & can also grow in affected lung areas)
What is coal worker's lung?
Inhalation of coal dust leads to significant scarring & fibrosis
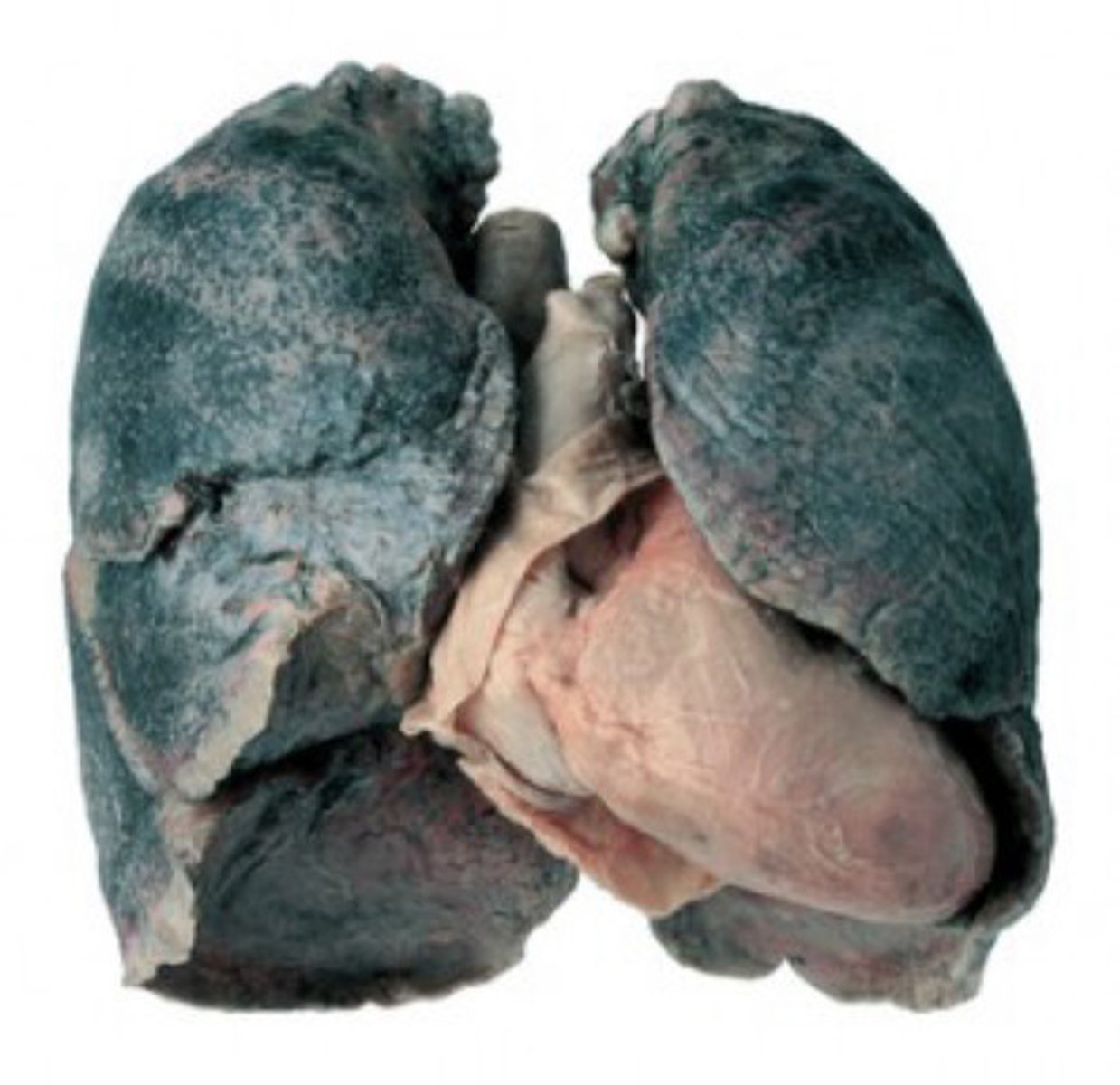
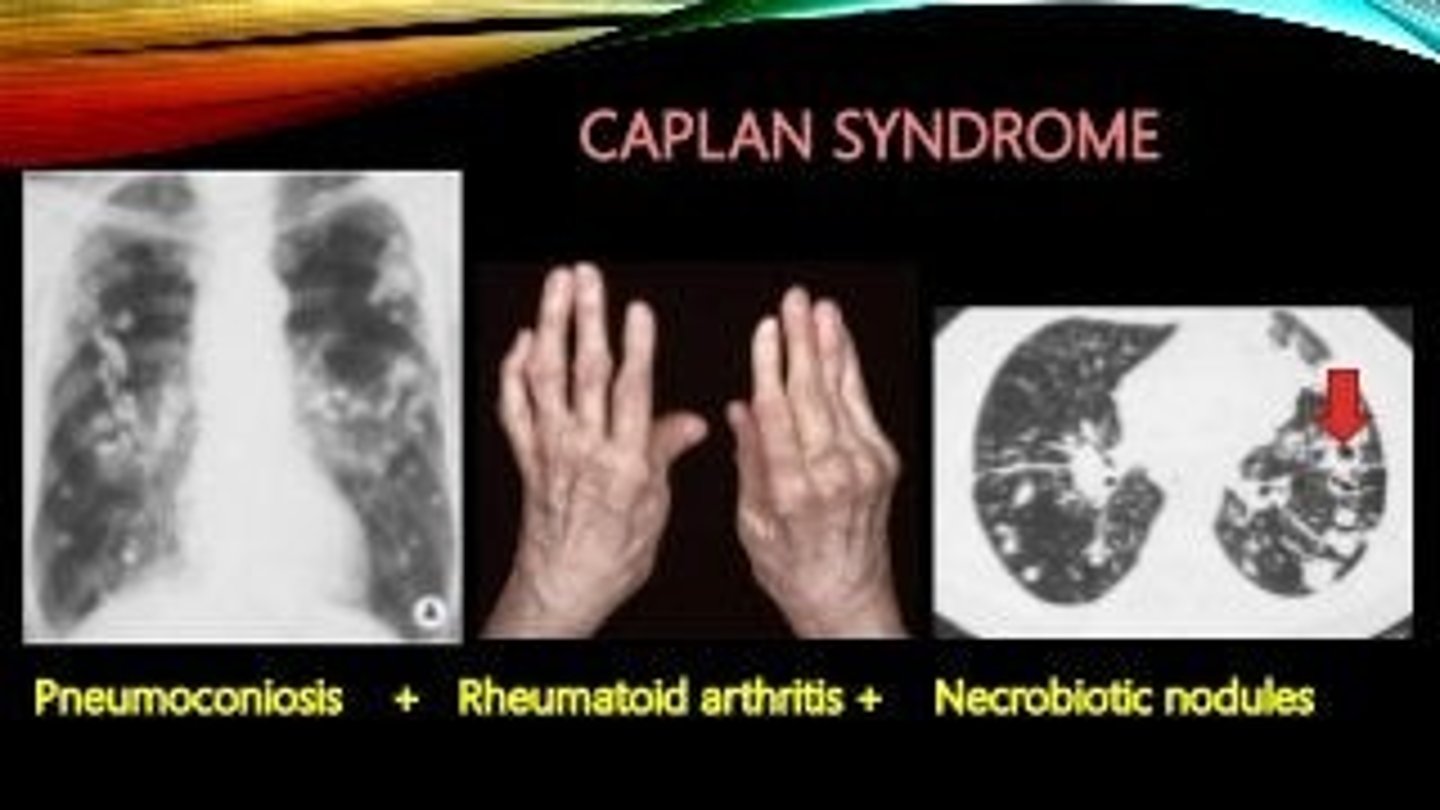
What is Caplan syndrome?
Coal-workers lung + rheumatoid lung nodules/rheumatoid arthritis (possible complication of CWL)
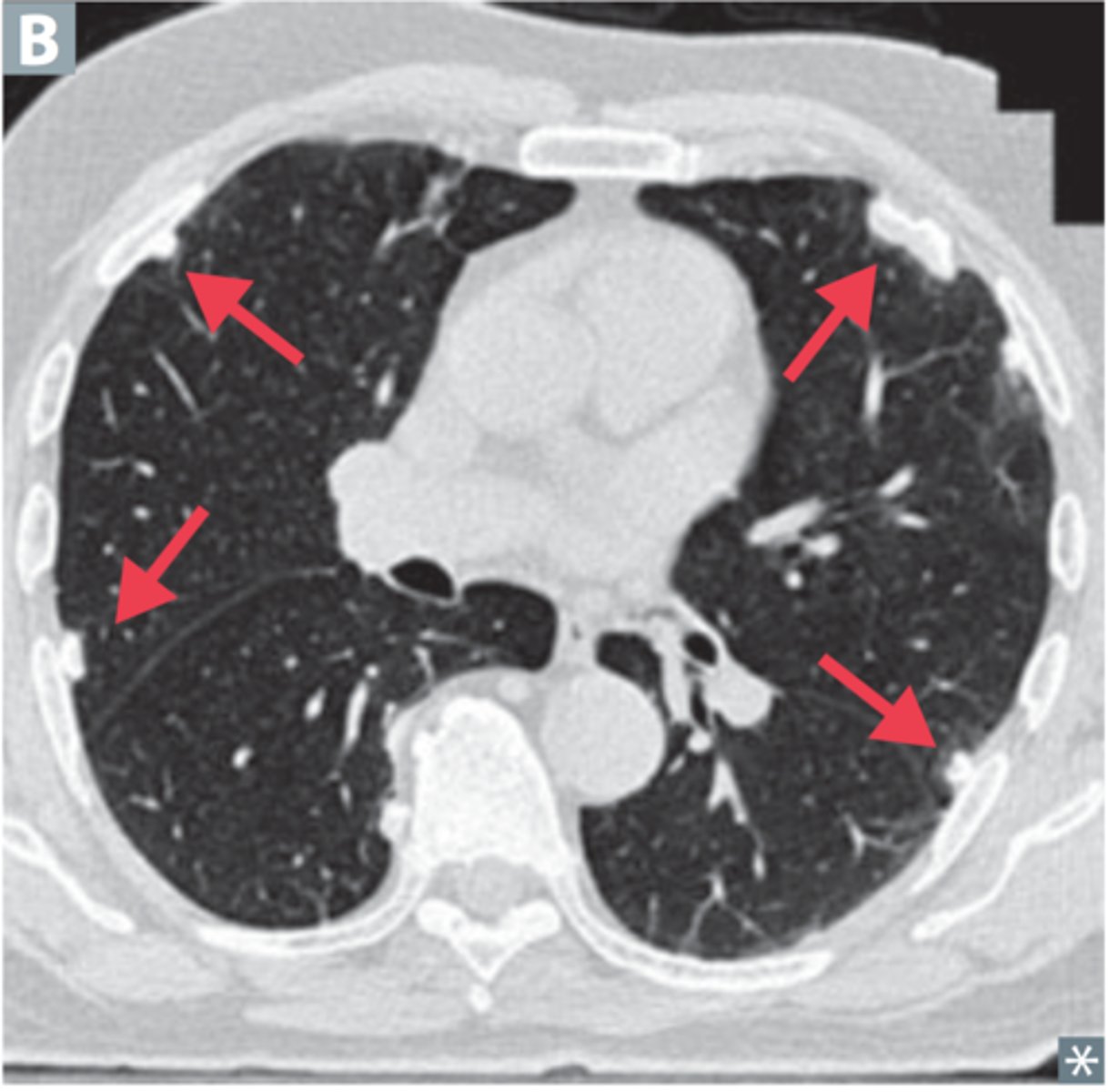
What is asbestosis? What is the best diagnostic test we have?
Inhalation of asbestos fibers leading to inflammation & fibrosis; CT (tends to show most detail, but we often make this diagnosis in context of the patient's hx of asbestos exposure)
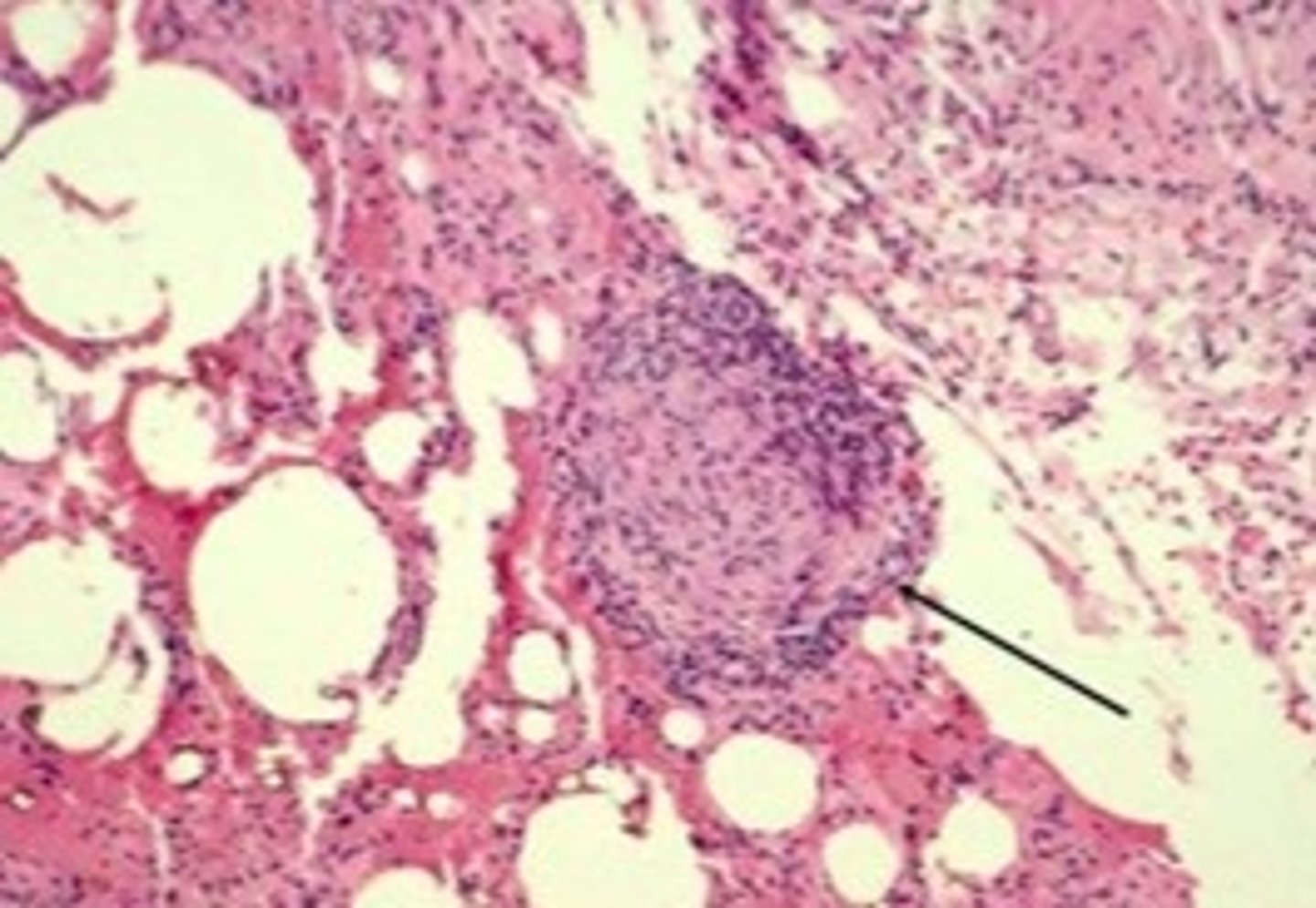
What is berylliosis?
Exposure/inhalation of beryllium (lightweight metal used in some manufacturing processes) resulting in inflammation & fibrosis

How is berylliosis diagnosed? How is it treated?
Beryllium lymphocyte proliferation test (only available at a few major medical centers in the whole US) or biopsy; treated w/ oral corticosteroids
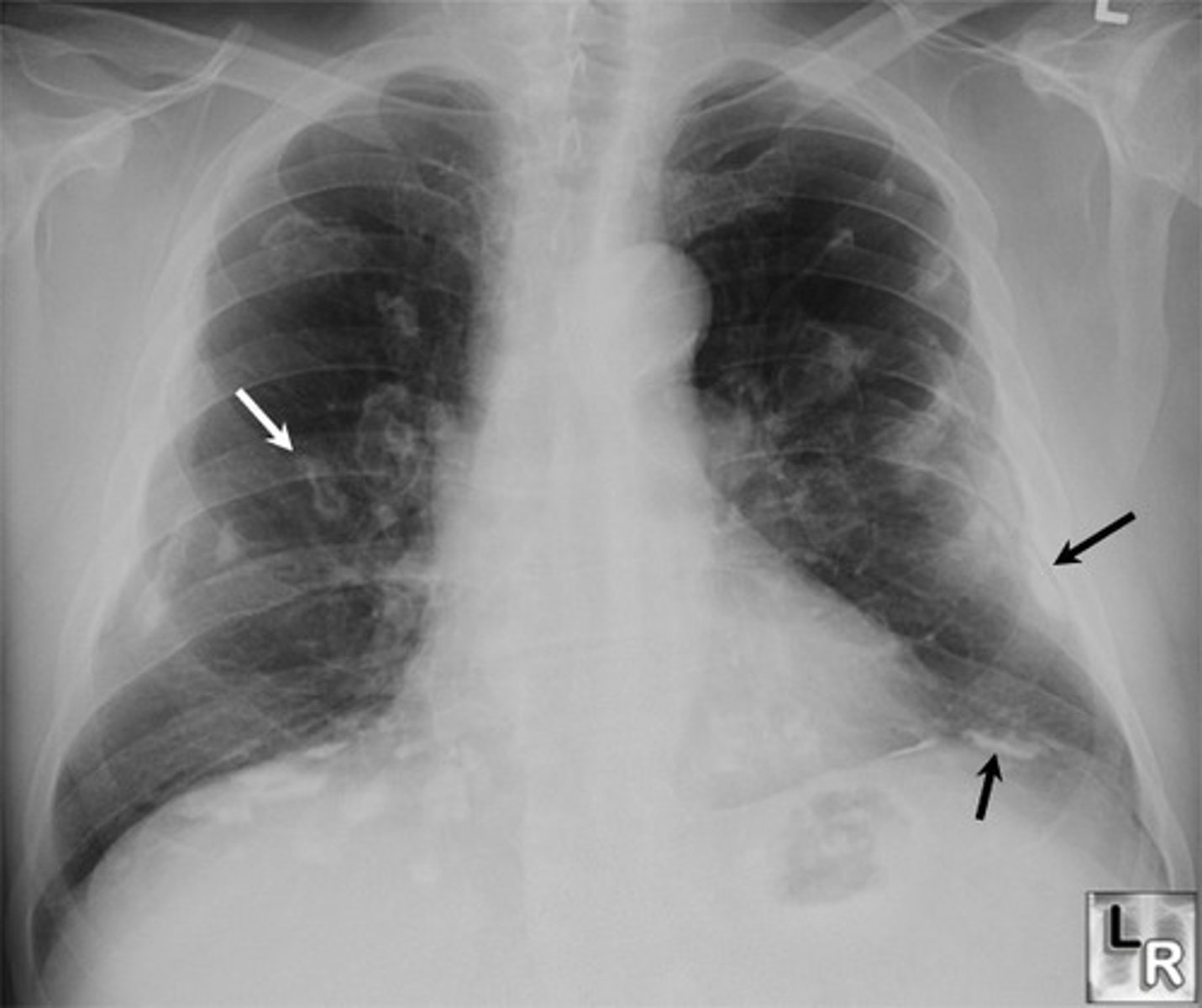
What is byssinosis?
Inhalation of cotton fiber/dust leading to inflammation & fibrosis

What is unique about how byssinosis tends to present clinically? How is it treated?
Sxs are often worse on Mondays (people go back to work on Monday & get re-exposed to the dust; often resembles asthma initially); supportive care
What is the difference between a head injury & a traumatic brain injury (TBI)?
Head injury: any form of trauma to the head regardless of whether or not the patient has sxs of neurological damage
TBI: evidence of damage to the brain as a result of trauma
What are the pathophysiologic changes that occur as a result of a mild TBI (aka a concussion)?
Axonal shearing, metabolic changes, & electrochemical imbalances lead to an energy mismatch (body requires ↑ energy to restore damaged function but has ↓ energy-making capacity)
What Glasgow Coma Scale (GCS) score, loss of consciousness (LOC) duration, & posttraumatic amnesia (PTA) duration classify as a mild TBI?
GCS: 13-15
LOC: < 20 mins - 1 hr
PTA: < 24 hrs
What Glasgow Coma Scale (GCS) score, loss of consciousness (LOC) duration, & posttraumatic amnesia (PTA) duration classify as a moderate TBI?
GCS: 9-12
LOC: 1-24 hrs
PTA: 24 hrs - < 7 days
What Glasgow Coma Scale (GCS) score, loss of consciousness (LOC) duration, & posttraumatic amnesia (PTA) duration classify as a severe TBI?
GCS: < 9
LOC: > 24 hrs
PTA: > 7 days
JUST KNOW: the s/sxs of a TBI are vast and vary depending on the severity. See the attached picture for a list of some common ones
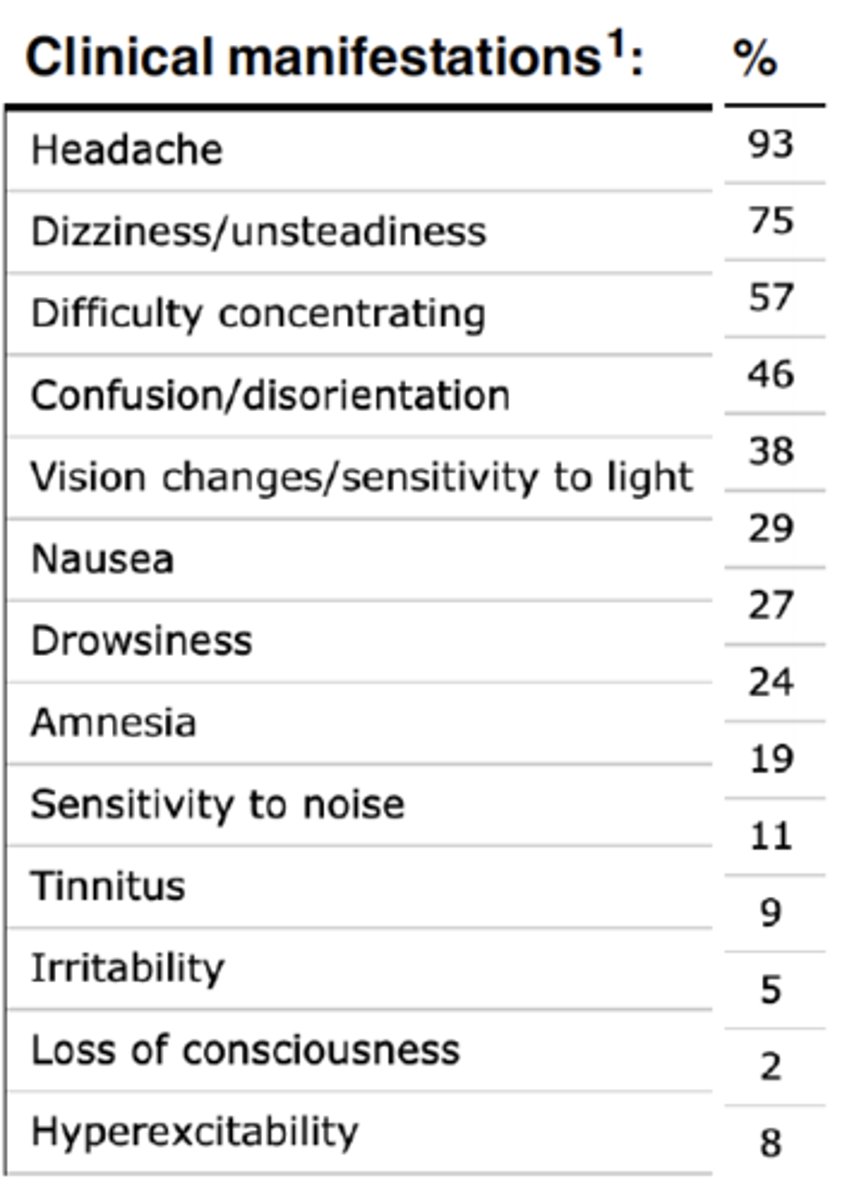
What are the typical components of a physical exam in a case of TBI?
Vitals, awareness & alertness via the GCS, brief cognitive assessment via the SCAT-5, cervical spine assessment, & a neuro exam
What GCS score warrants prompt intubation?
8 or less - these patients are considered comatose
PICTURE ONLY: Glasgow Coma Scale
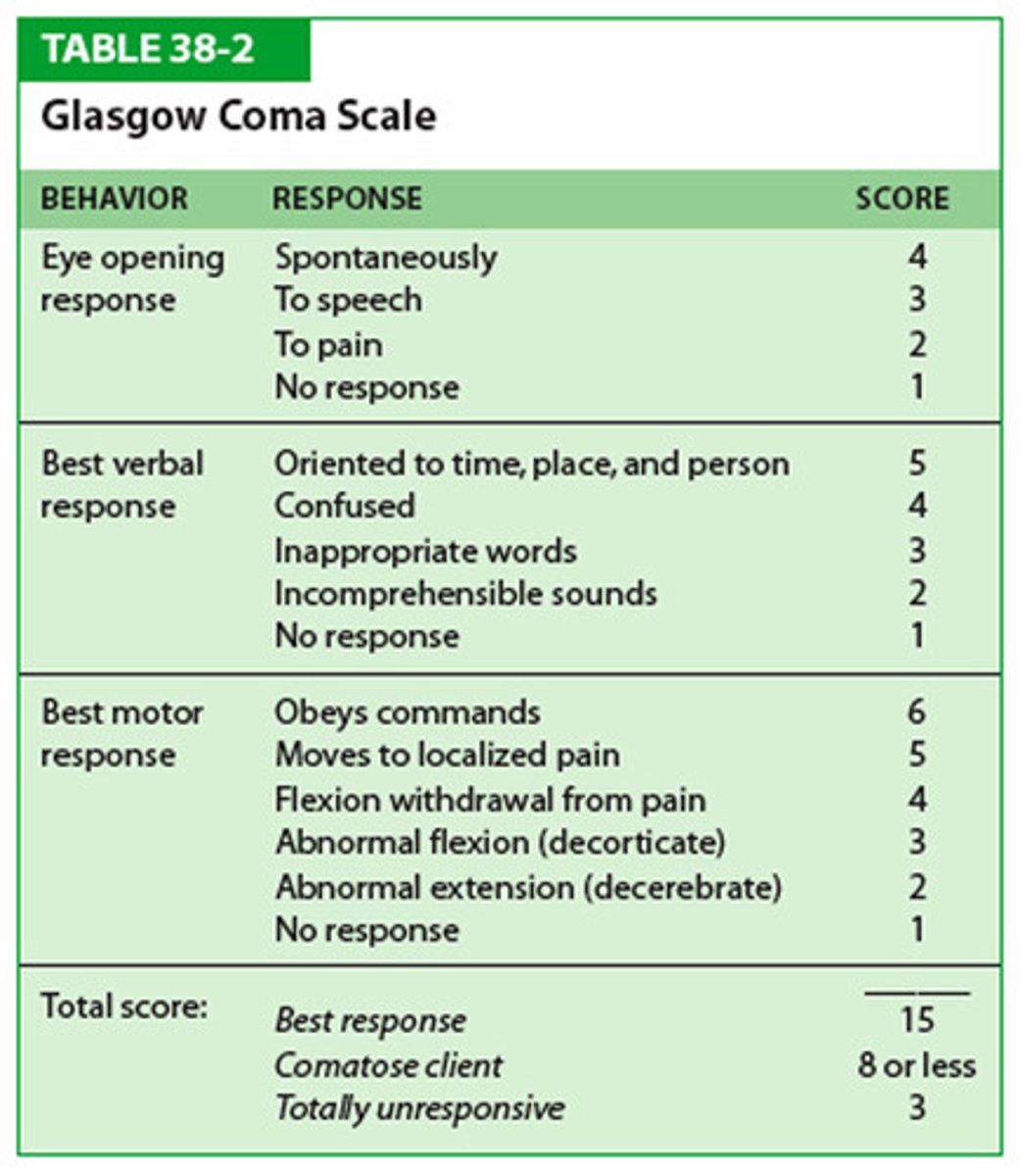
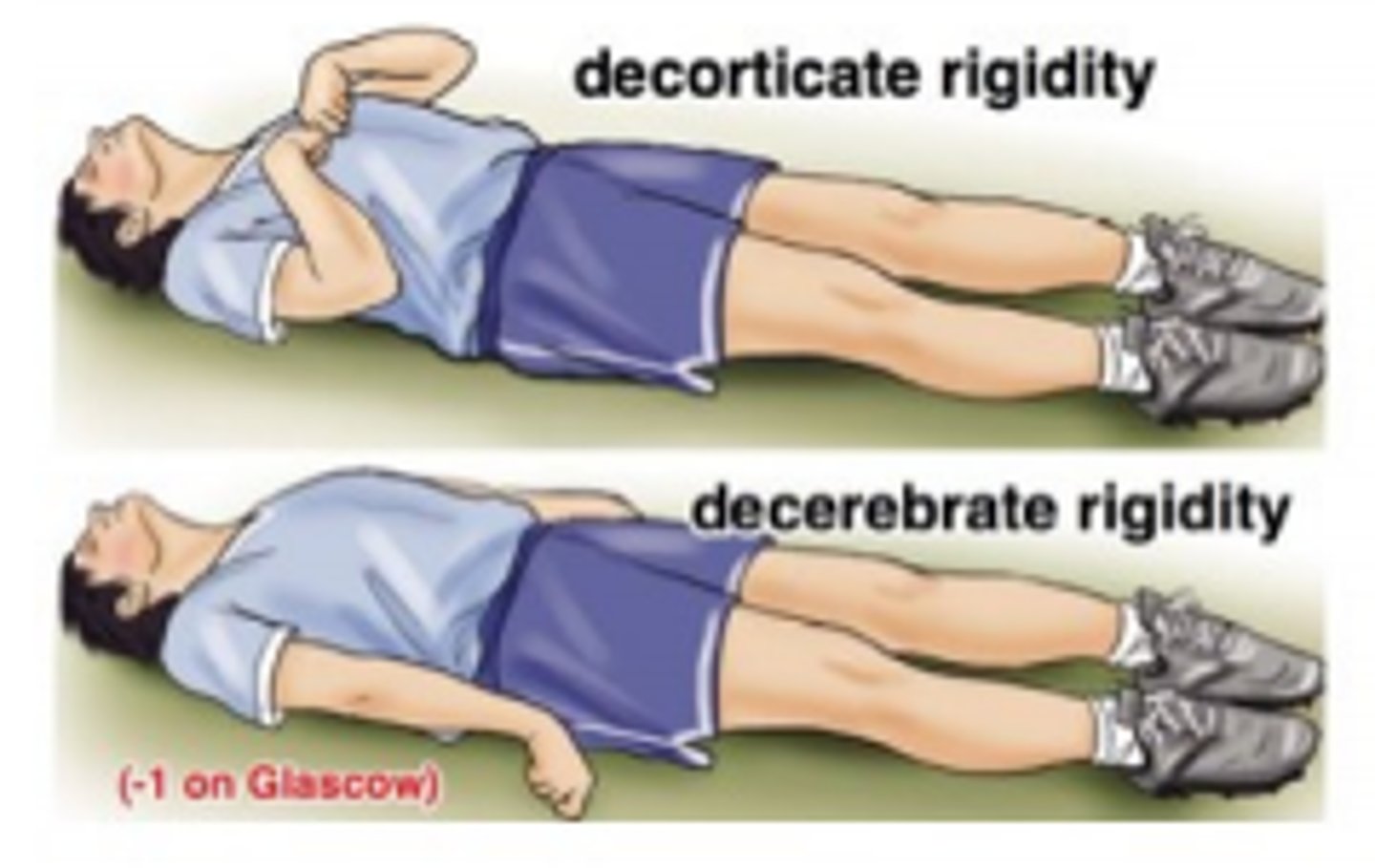
What is the difference between a decorticate & decerebrate posture? Which one is more indicative of a poorer prognosis?
Decorticate: arms flexed & held against chest
Decerebrate: arms extended & internally rotated, wrists & fingers flexed (indicates more severe brain damage often involving the brainstem, poorer prognosis)
What is something a single fixed & dilated pupil may indicate? What about bilateral fixed & dilated pupils?
Single: intracranial hematoma w/ uncal herniation
B/l: ↑ ICP, b/l herniation, certain drugs, severe hypoxia

What are some things bilateral pinpoint pupils can indicate?
Opiate exposure, central pontine lesion
Again, what GCS score classifies as a mild TBI? Is the injury in these cases structural or functional?
GCS score 13-15; functional
What are some s/sxs of a mild TBI (concussion)?
Changes in behavior, abnormal body language, blank stare, shaking head, repeating questions, slowed reaction time, LOC (< ~30 mins), PTA (< 24 hrs)
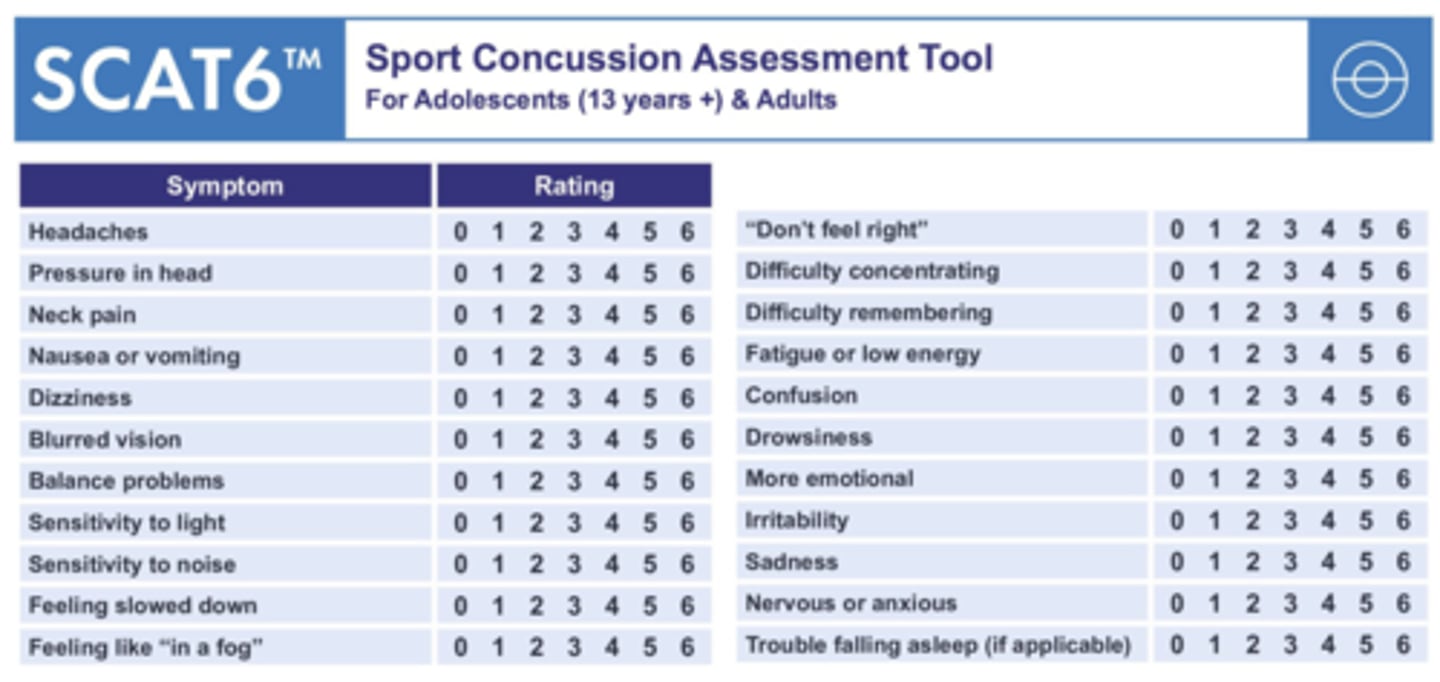
What is the Sport Concussion Assessment Tool (SCAT6) & what is it used for?
Standardized, evidence-based tool for evaluating suspected concussions in individuals ≥ 13 y/o; often used as a sideline assessment
Do most mild TBIs require imaging (CT/MRI)? How are they managed?
No; rest usually in an outpatient setting (can refer to TBI specialist if sxs do not improve/worsen after 3-5 days)
What is the 6-step return-to-activity flow a patient will go through before they can re-join their sport following a mild TBI?
1) No activity
2) Light aerobic activity
3) Sport-specific activity
4) Noncontact drills
5) Full contact practice
6) Return to play
Again, what GCS score classifies as a severe TBI? How does this one differ from a mild/moderate TBI?
GCS score of 3-8; these patients have significant neurological impairment & recovery can span months to years
What is post-concussive syndrome?
Concussion sxs that persist > 3 months after the incident (can sometimes last years)
What is second impact syndrome? Is this serious?
Catastrophic neurological emergency characterized by rapid brain swelling after a second concussion before sxs from a previous one have resolved; YES - 60-80% mortality!!
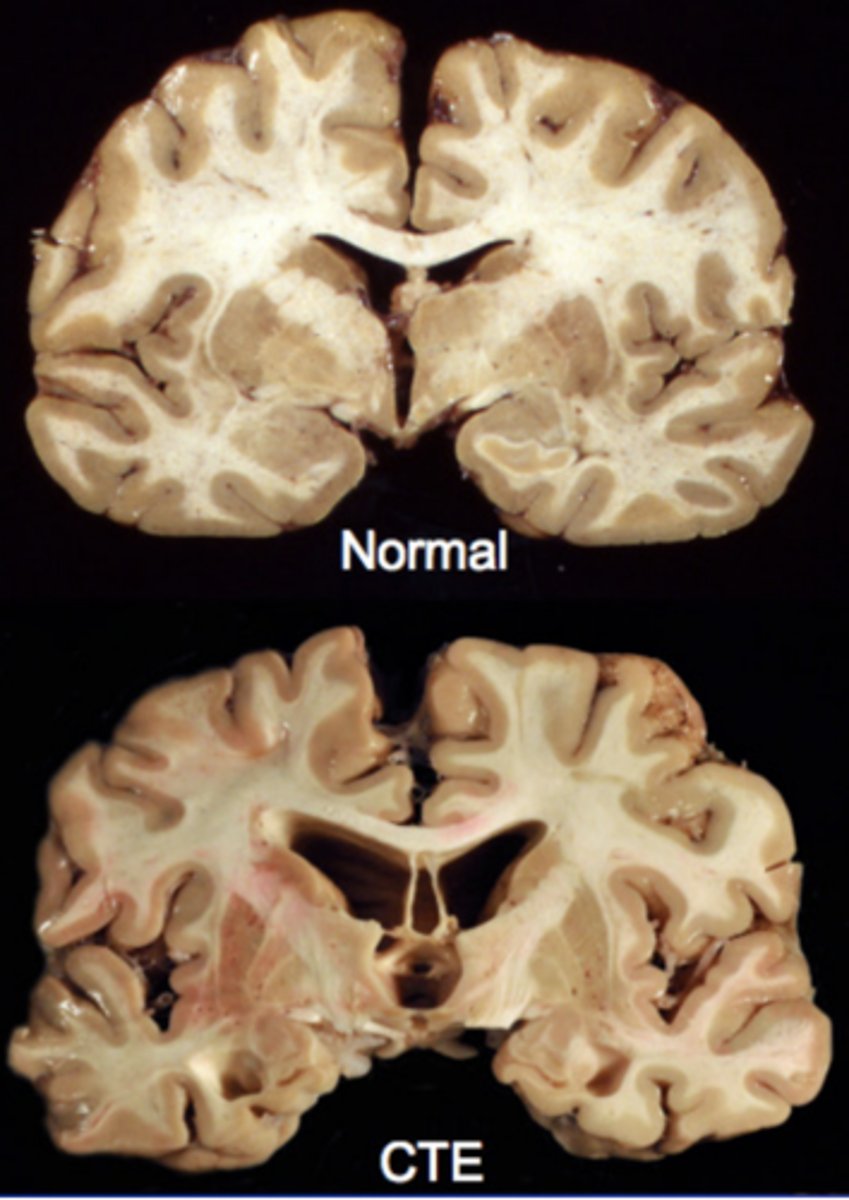
What is chronic traumatic encephalopathy (CTE), & what is it associated with?
Neurodegenerative disease linked to repeated head trauma over a long period of time; increased incidence of suicide & spousal abuse, early dementia, Parkinson-like sxs, impaired judgement, impulsivity, & other abnormalities
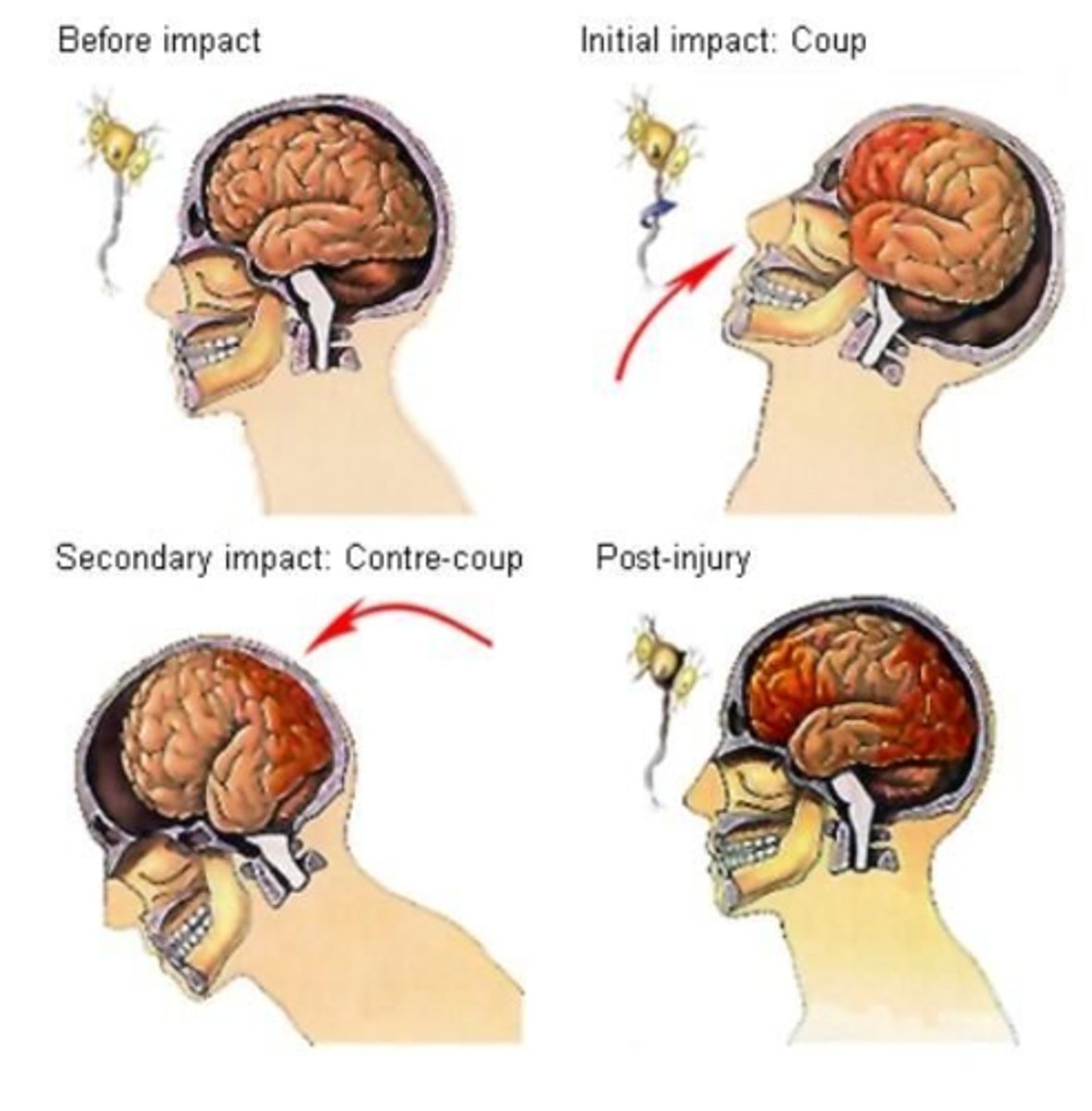
What is a cerebral contusion?
Collision of the brain with the skull resulting in small vessel rupture, multiple microhemorrhages & possible edema of the brain parenchyma
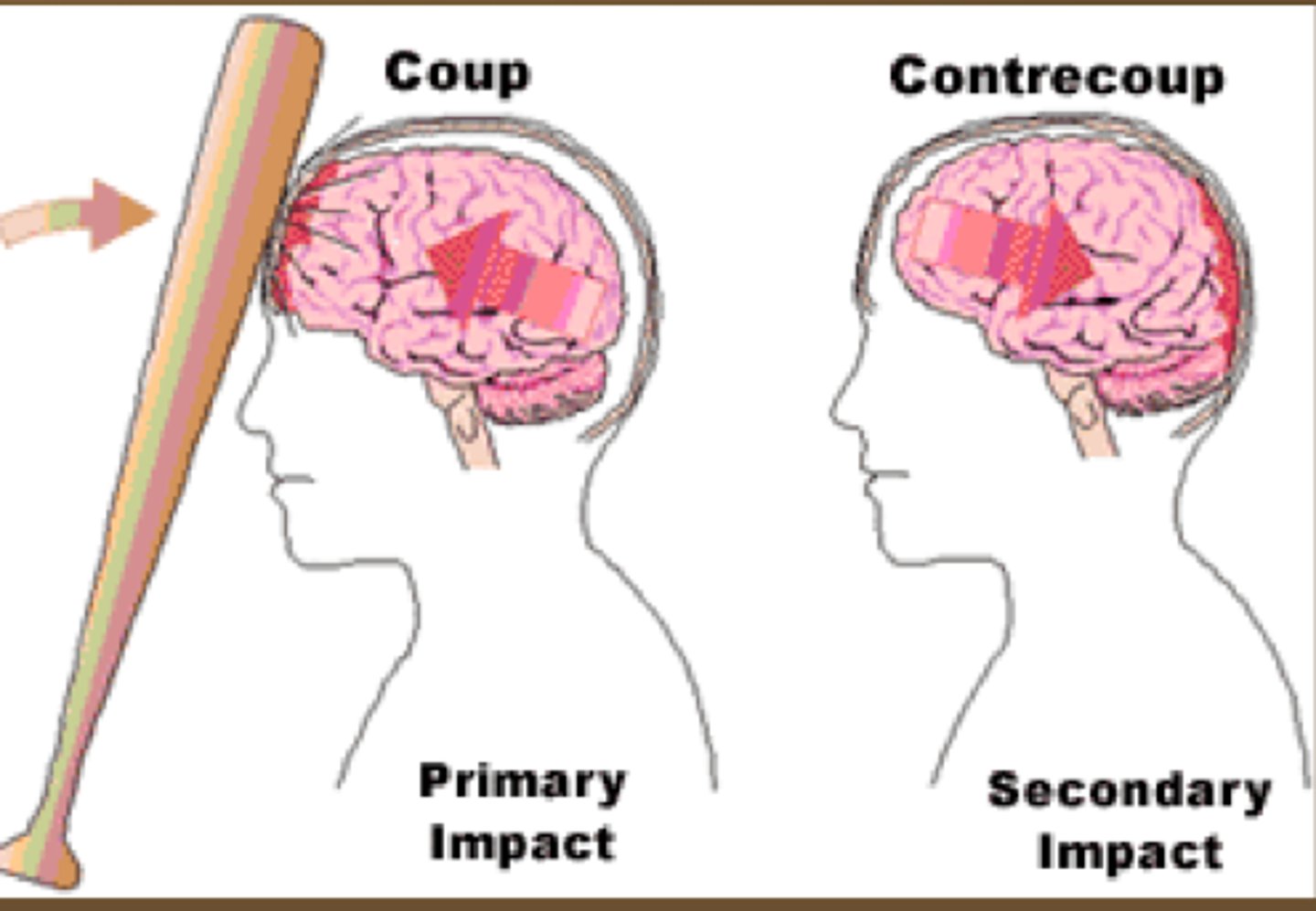
PICTURE ONLY: cerebral contusion
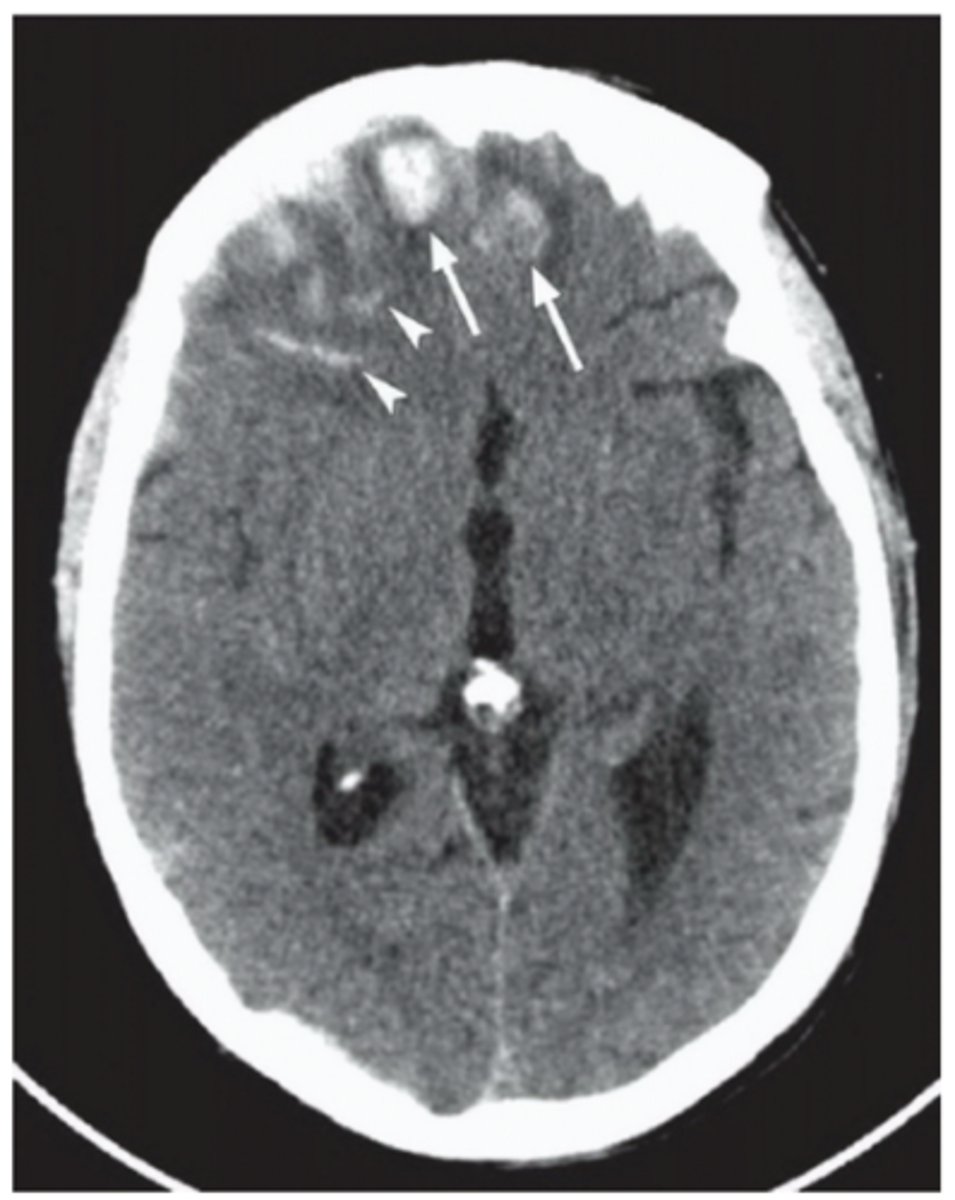
What is a subarachnoid hemorrhage? What is the hallmark symptom of this condition?
Bleeding in the subarachnoid space between the pia & arachnoid mater; sudden severe headache ("thunderclap headache," "worst headache of my life," etc.)
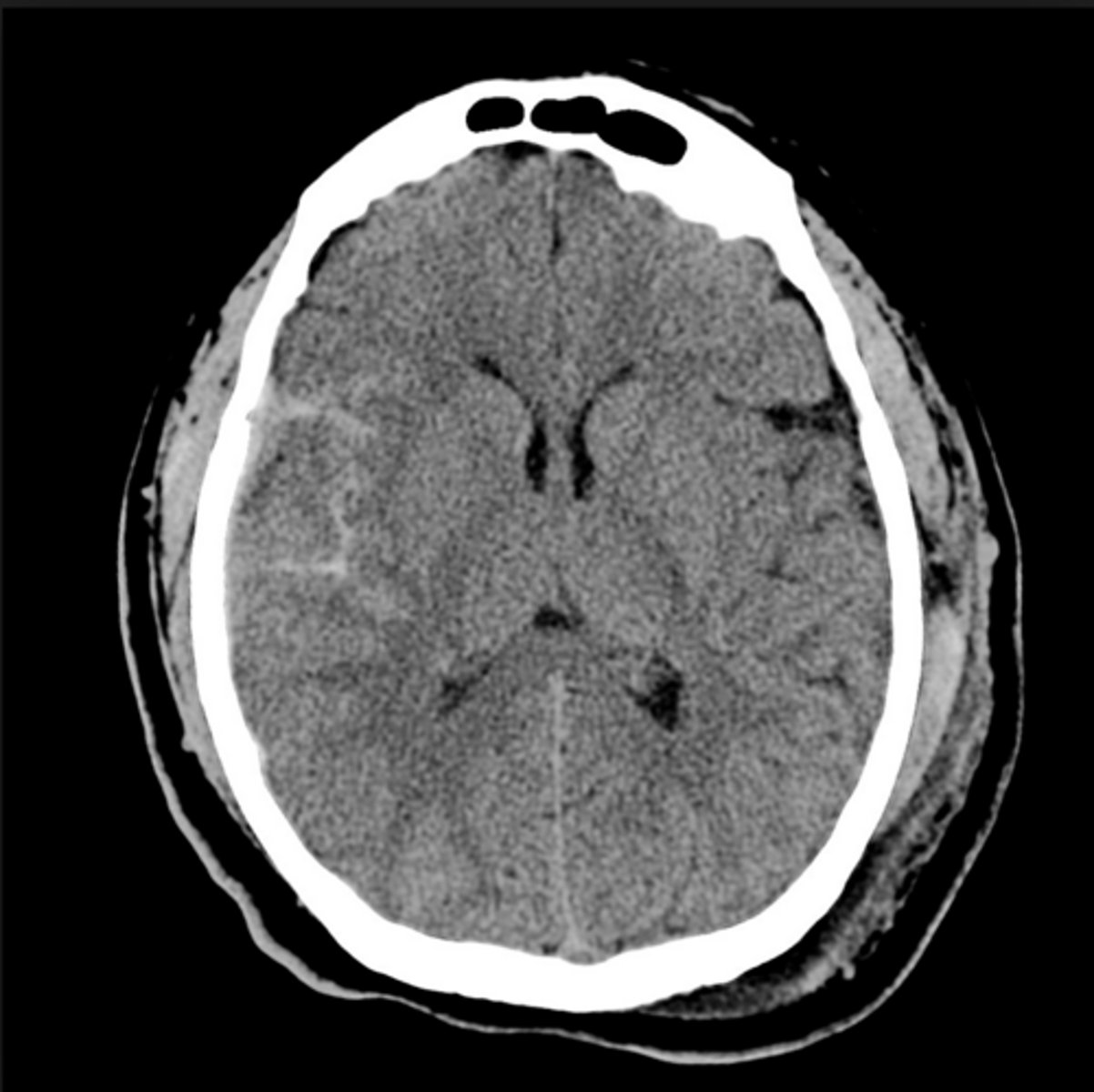
How is a subarachnoid hemorrhage treated?
Admission & neurosurgery consult, repeat head CT within 24 hrs, aggressive management of HTN (very important), pain management
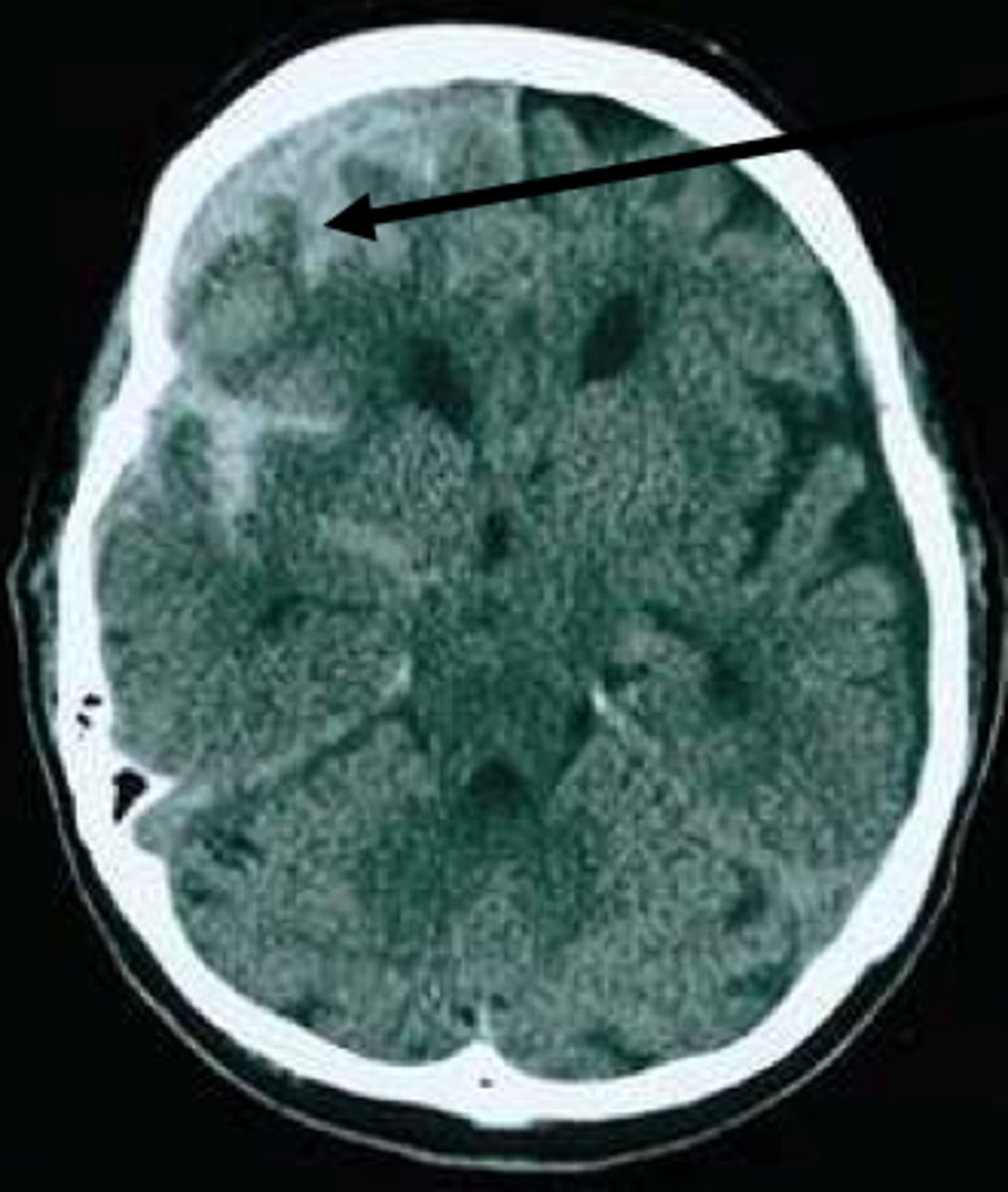
What is an acute epidural hemorrhage, & what is it often caused by?
Accumulation of blood in the potential space between the dura & the skull most commonly due to a laceration of the middle meningeal artery (usually from blunt trauma to the head)
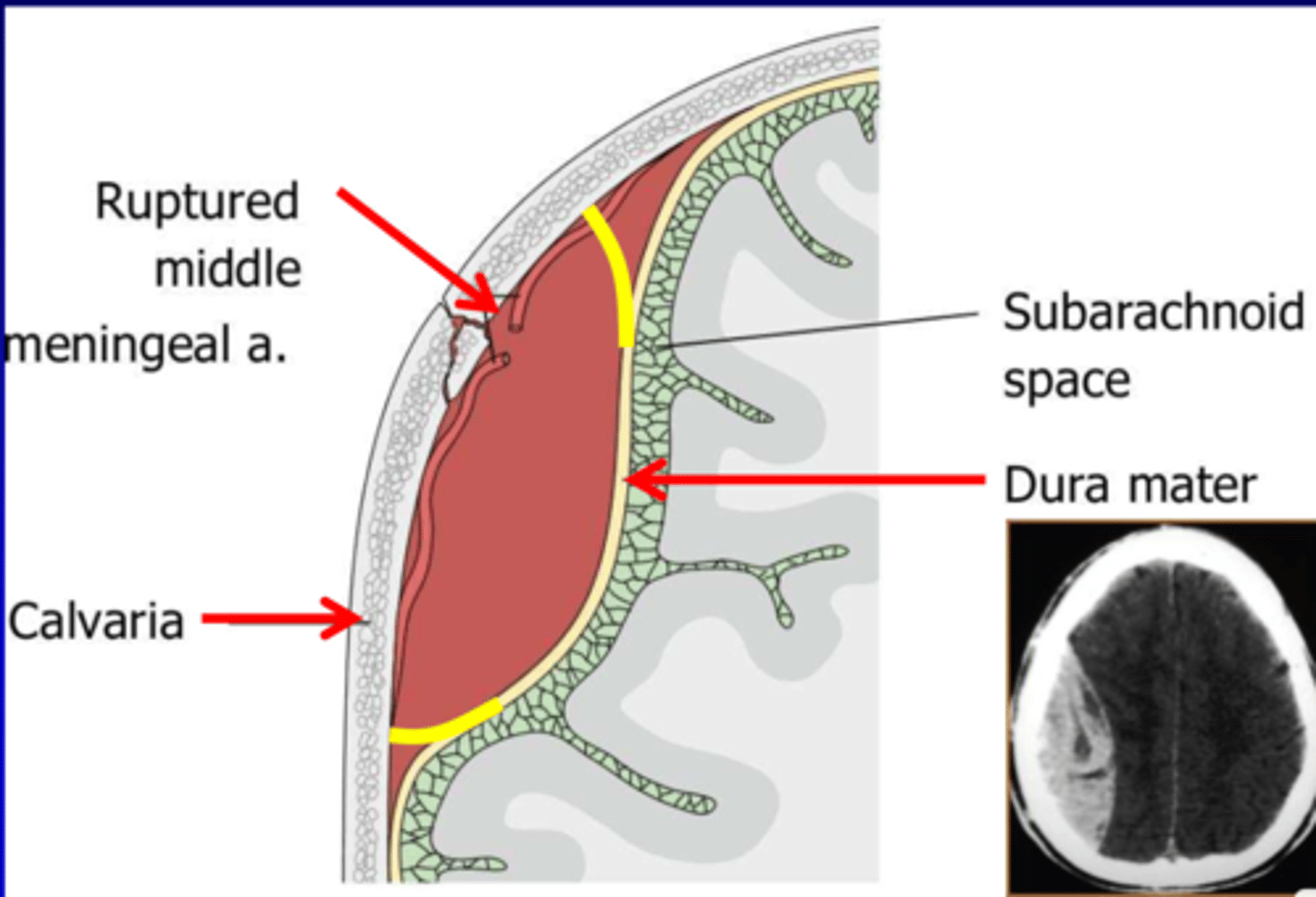
What is a unique clinical presentation feature of acute epidermal hemorrhage?
Presence of a lucid interval: temporary improvement in patient's condition after a severe head injury that can last minutes to hours, but suddenly they lapse into unconsciousness again when the bleeding expands & ↑ ICP (sometimes called a "talk and die")
What is the classic appearance of epidural hemorrhage on imaging? How are these treated?
Biconvex lens shape (football); medical emergencies that require immediate surgical intervention
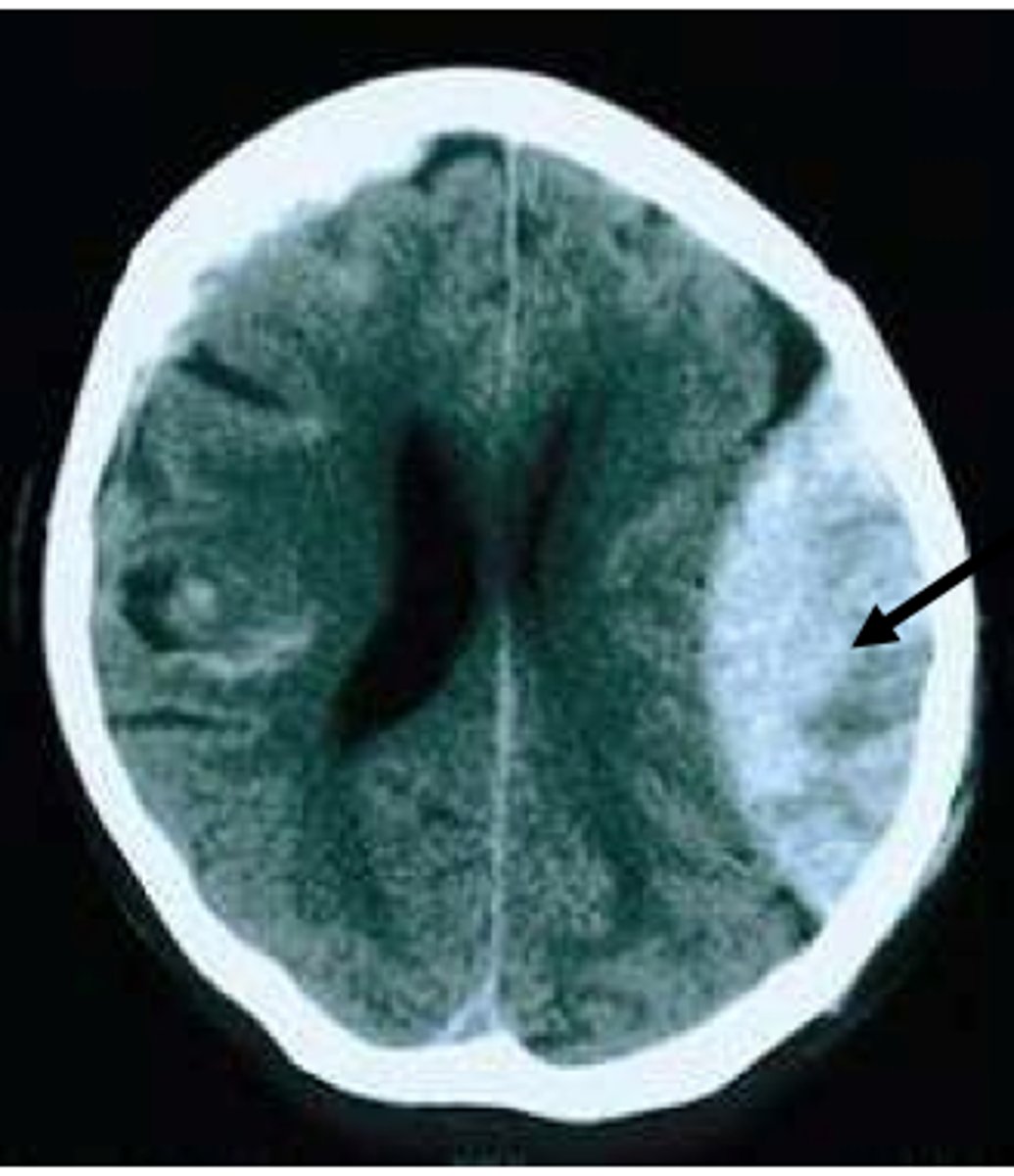
What is an acute subdural hemorrhage, & what is it often caused by?
Accumulation of blood between the inner dura mater & arachnoid mater due to tearing of the bridging veins, often caused by acceleration-deceleration injuries or trauma (esp. in the elderly)
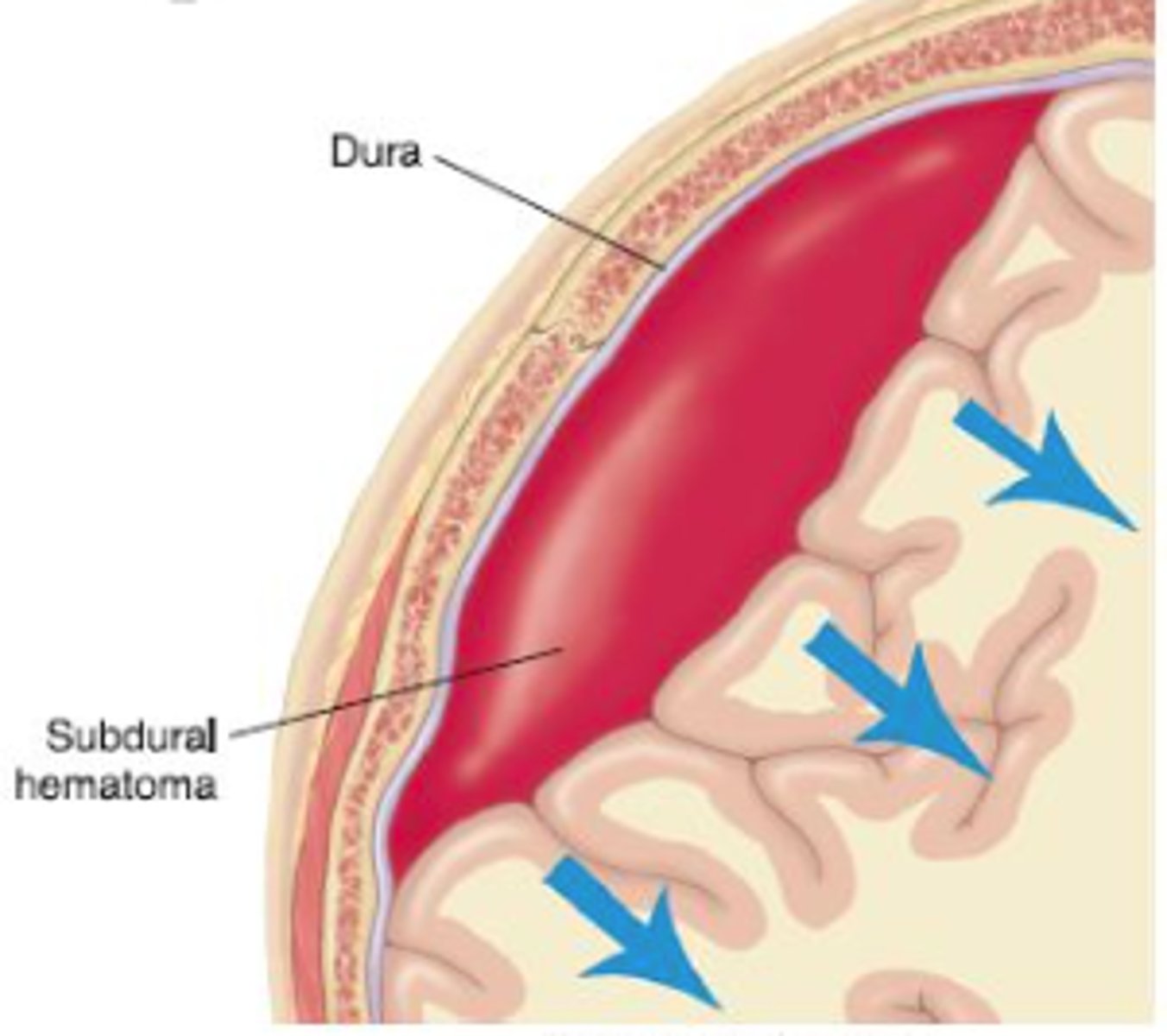
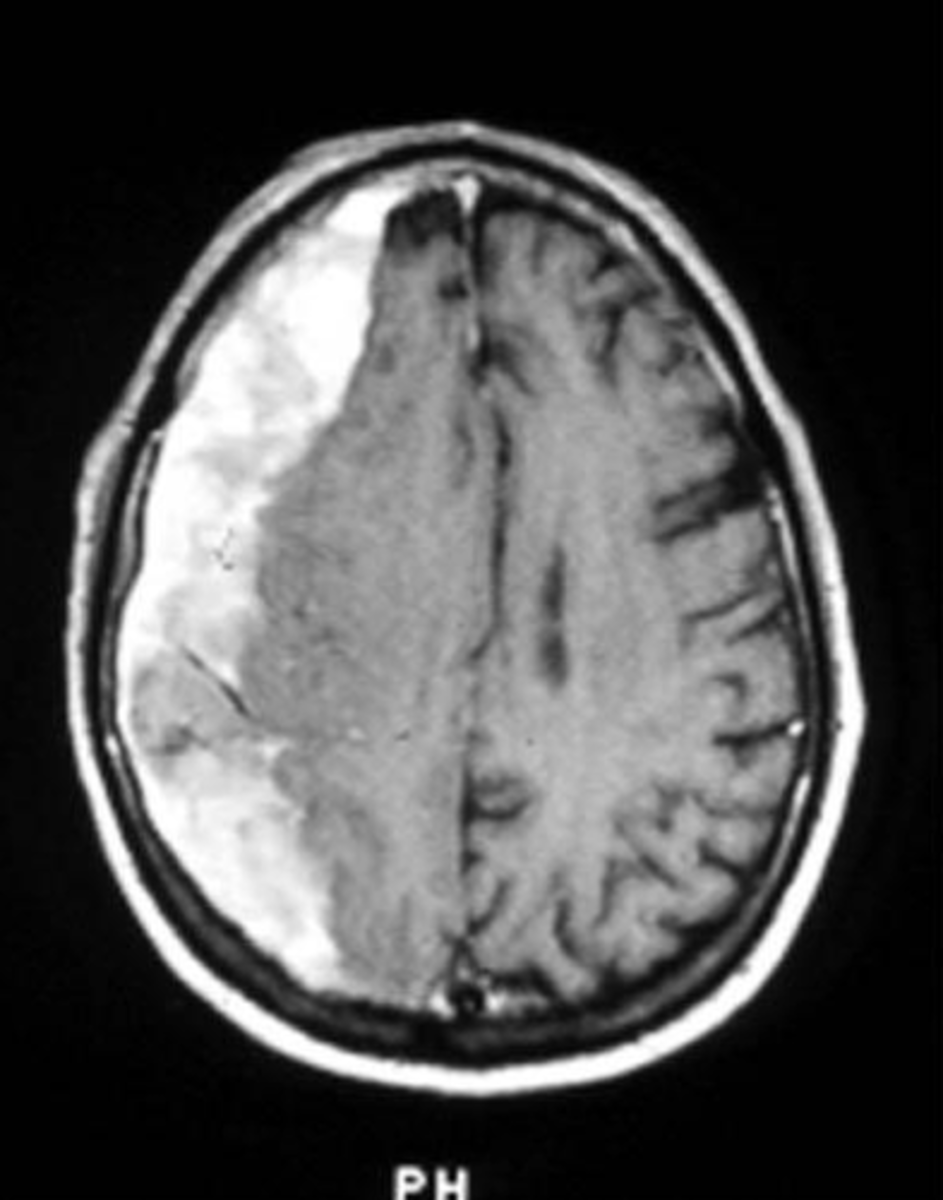
What does a subdural hemorrhage appear as on imaging?
White, crescent-shaped mass between the inner part of the skull & surface of the central hemisphere
PICTURE ONLY: epidural hemorrhage vs. subdural hemorrhage
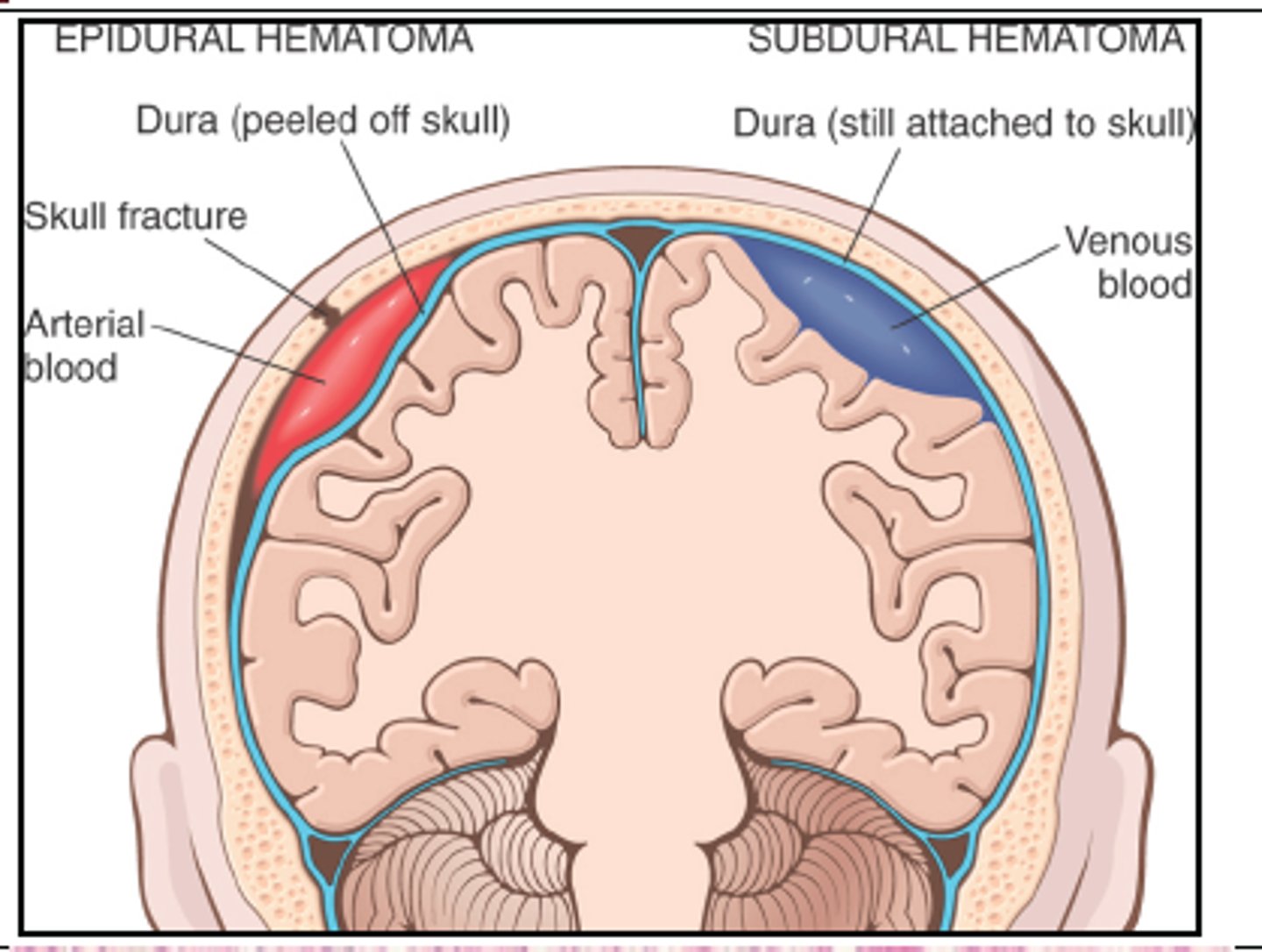
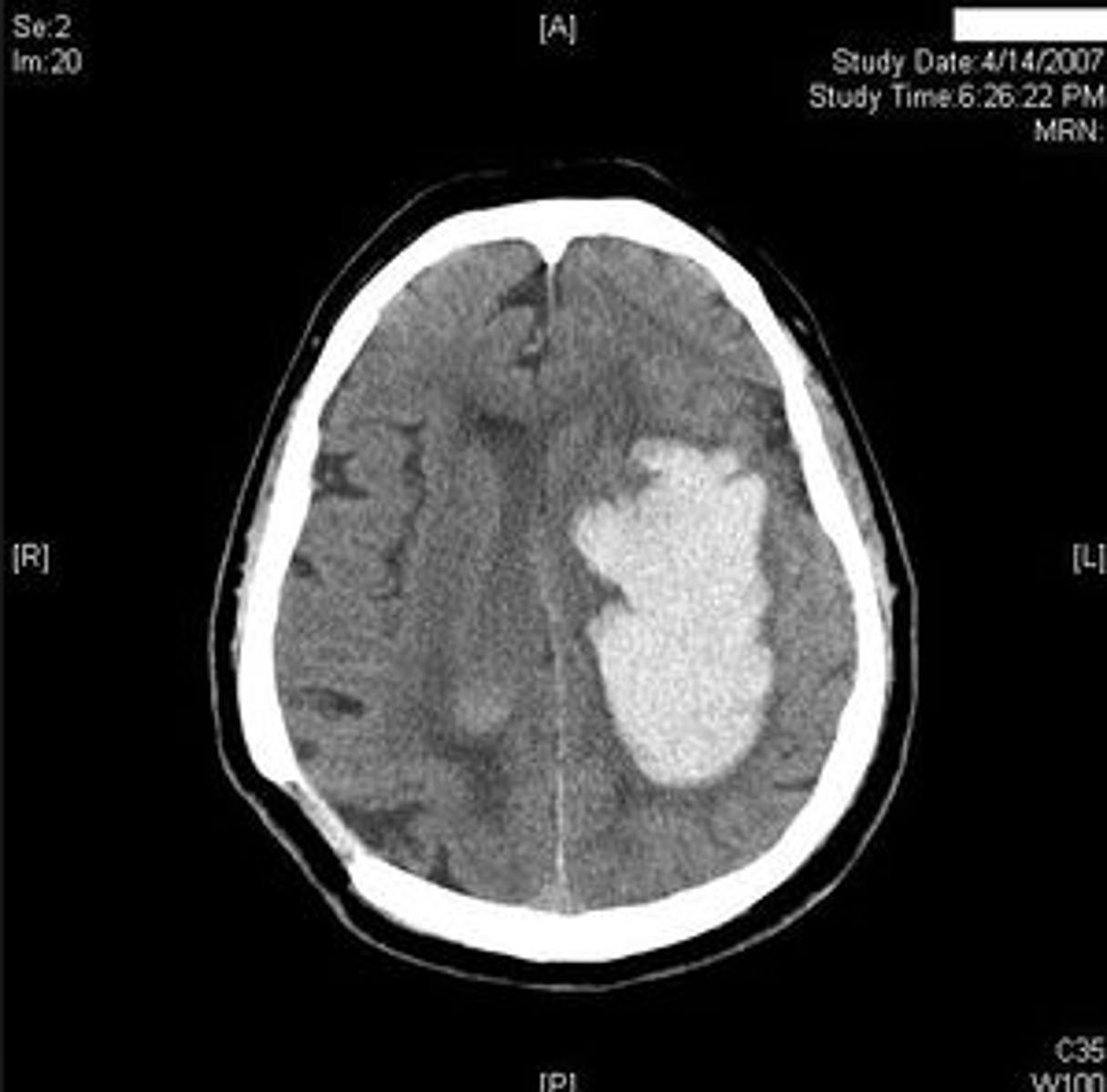
What is an intracerebral hemorrhage, & what does it commonly lead to?
Bleed that occurs within the brain tissue or ventricles itself; common cause of strokes
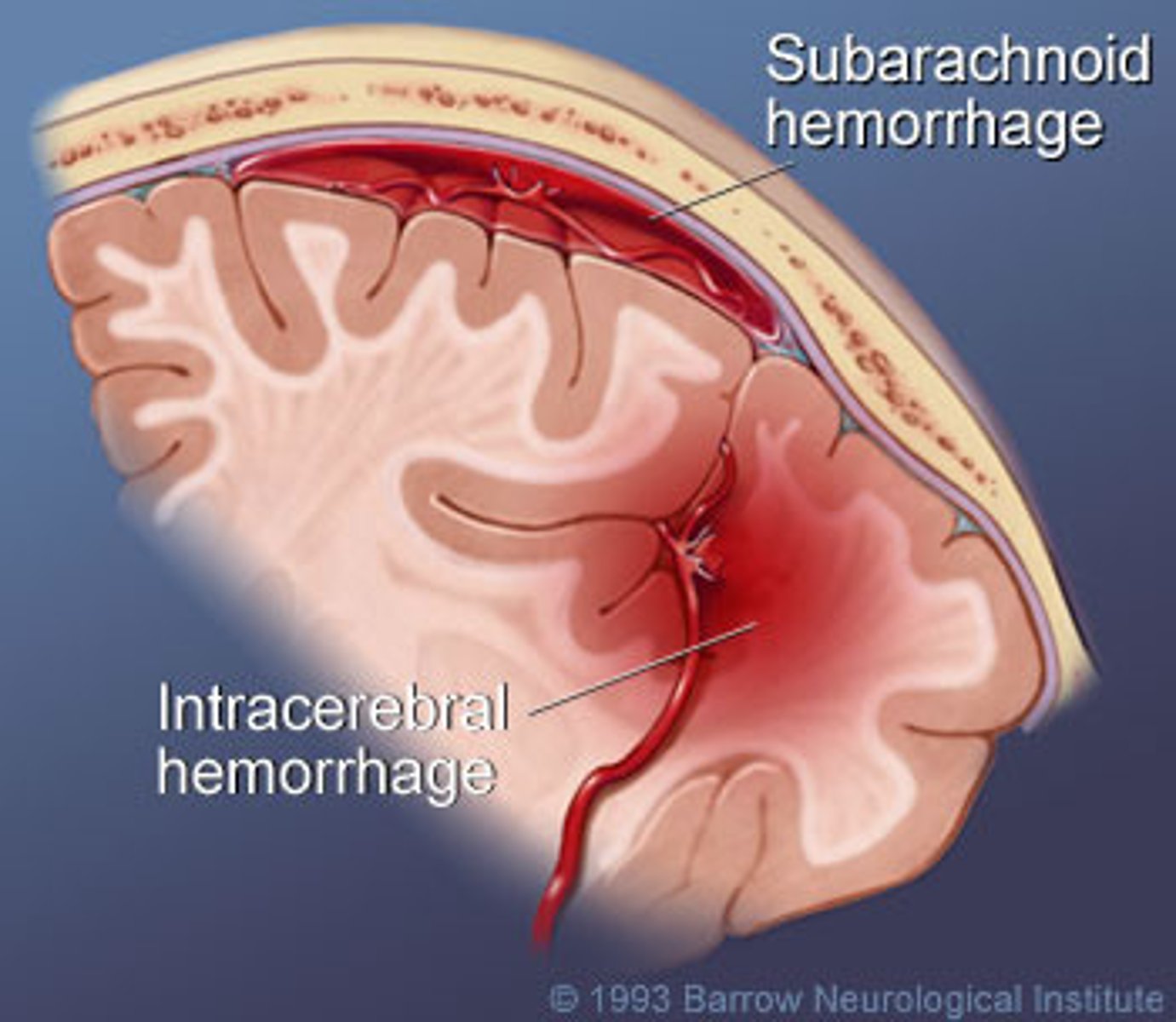
PICTURE ONLY: intracerebral hemorrhage on imaging
What is a middle meningeal artery (MMA) embolization?
Emergent treatment for chronic subdural hematoma that embolizes the middle meningeal artery to prevent it from rupturing
PICTURE ONLY: skull fracture on imaging
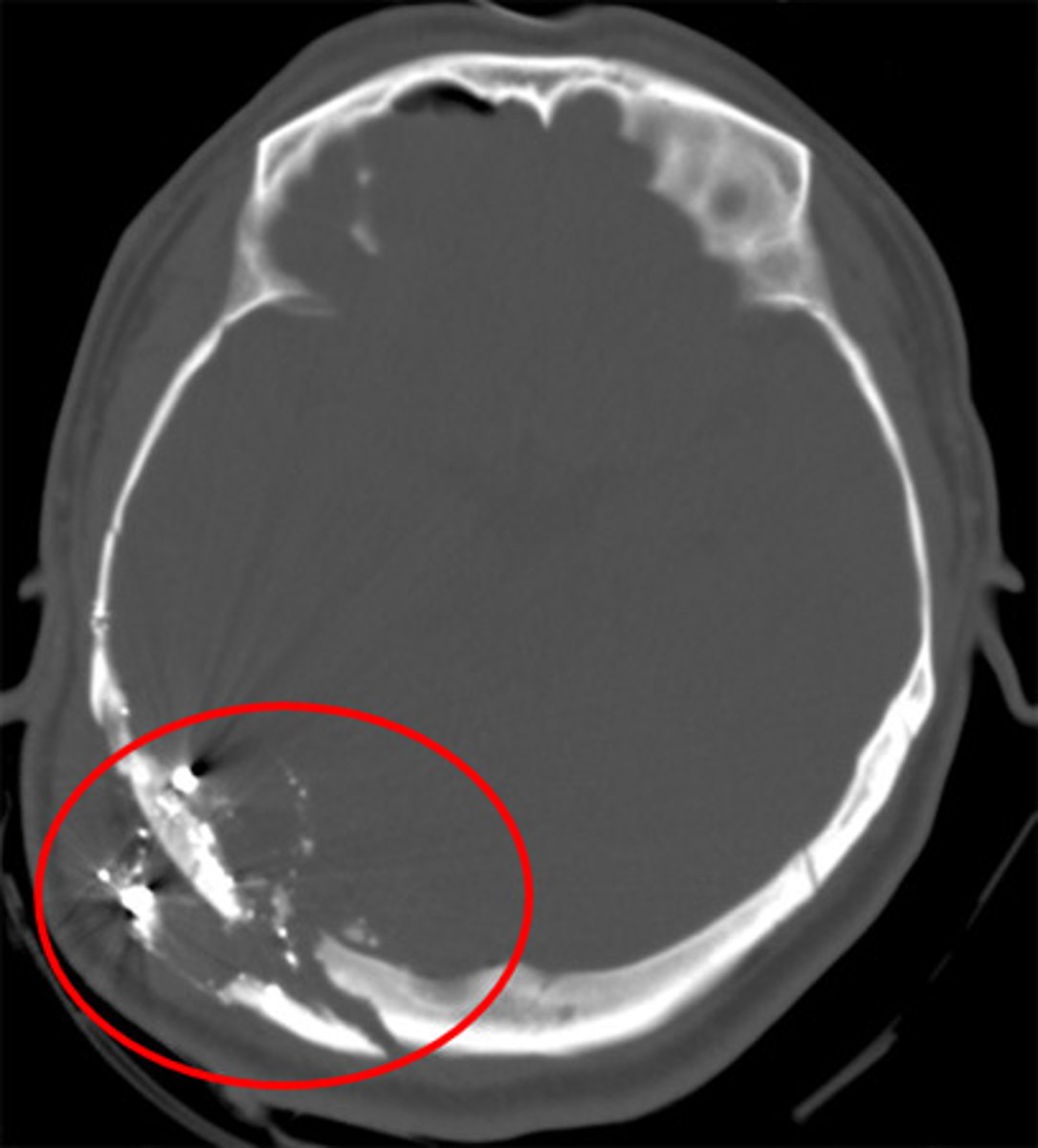
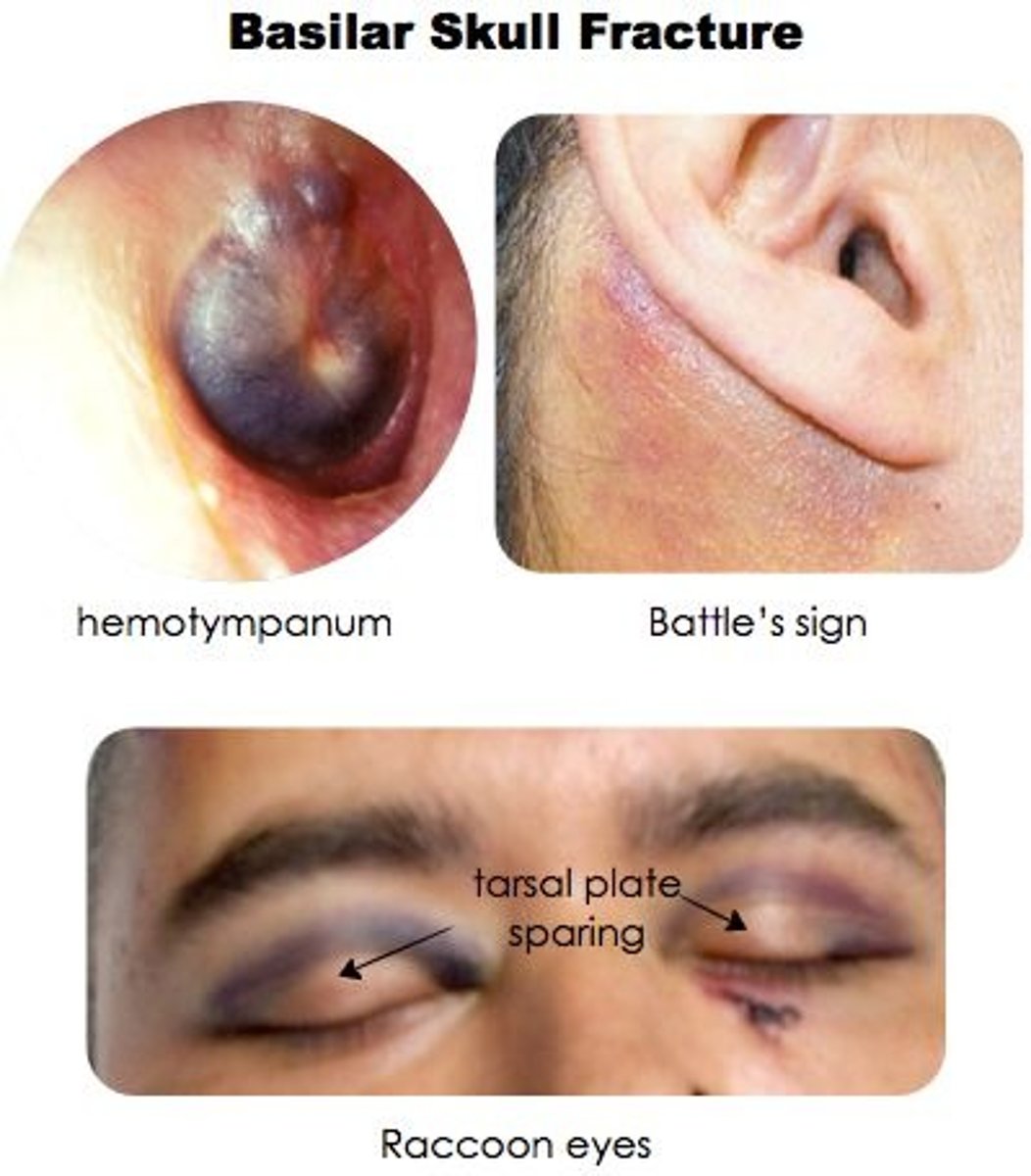
What is a basilar skull fracture, & what are some s/sxs?
Linear fracture that occurs at the base of the skull; CSF otorrhea/rhinorrhea, periorbital ecchymoses ("raccoon eyes"), retroauricular ecchymoses ("battle sign"), hemotympanum
What is a major risk factor for developing primary brain tumors?
Exposure to ionizing radiation
JUST KNOW: CNS tumors can present with a wide array of s/sxs (often focal neurological) depending on their size & the area of the CNS affected. A headache that wakes patients up at night is a classic description for these tumors
What is the preferred imaging modality for diagnosing brain tumors as a whole? What is definitive?
MRI w/ gadolinium contrast; biopsy/histopathology
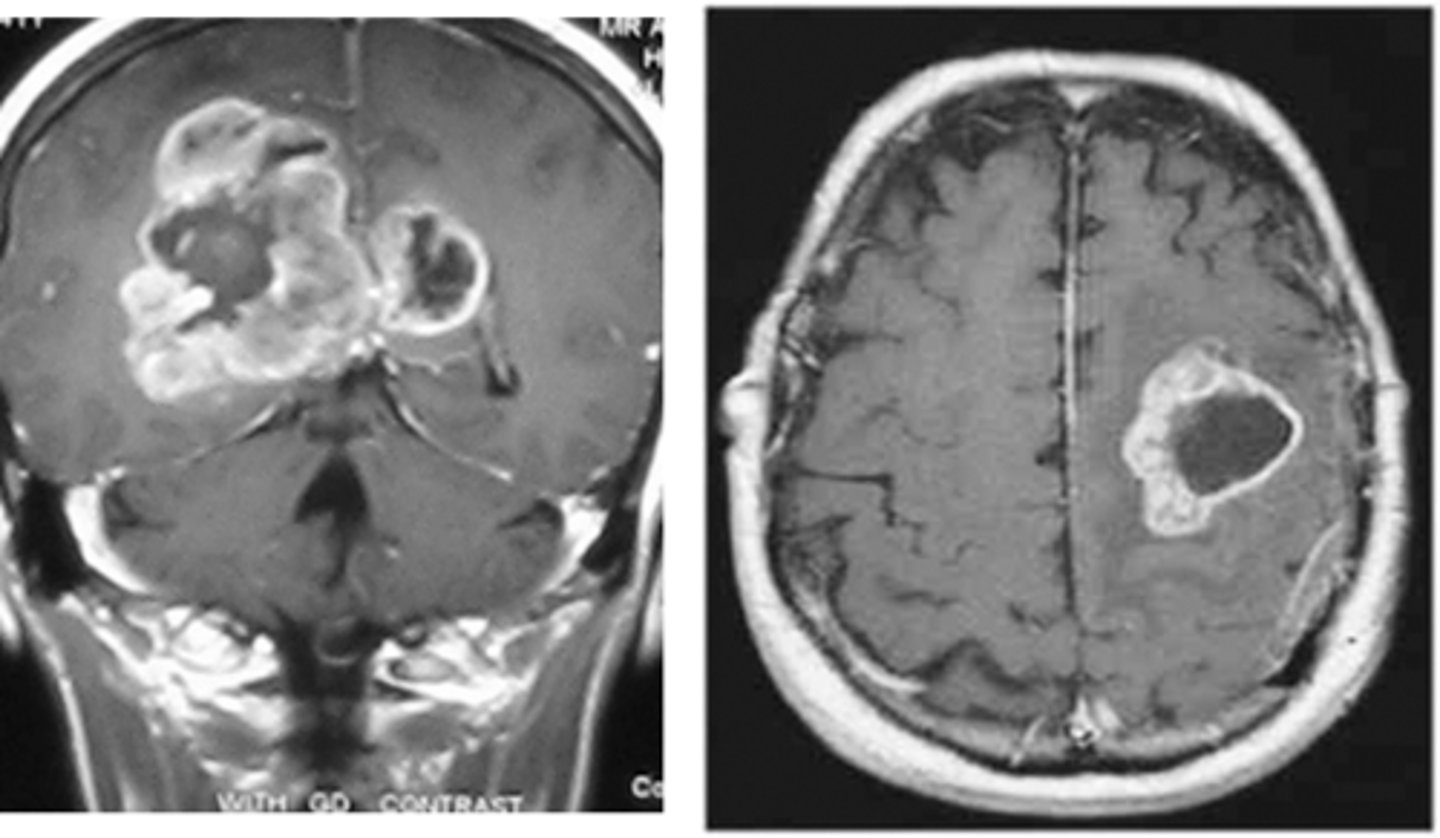
What are the 3 overall types of gliomas (primary malignant brain tumors)?
Astrocytomas, oligodendrogliomas, & ependymomas
What is a glioblastoma, & why is it significant?
Grade IV astrocytoma (aka it's a subtype of an astrocytoma); they are the most common malignant primary brain tumor (are super aggressive & infiltrative - very deadly)
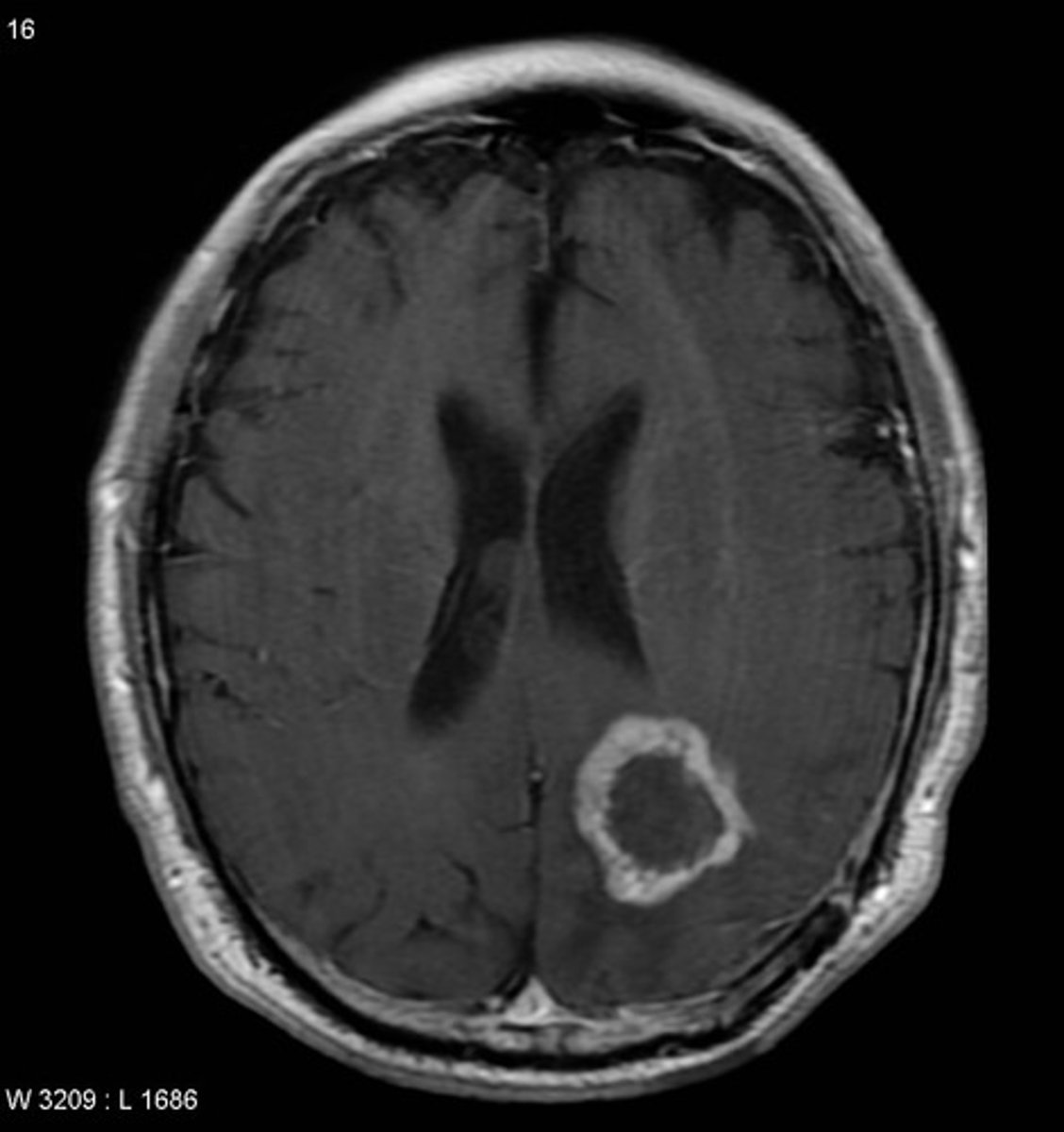
What genetic findings are indicative of an oligodendroglioma?
1p/19q co-deletion & IDH mutation
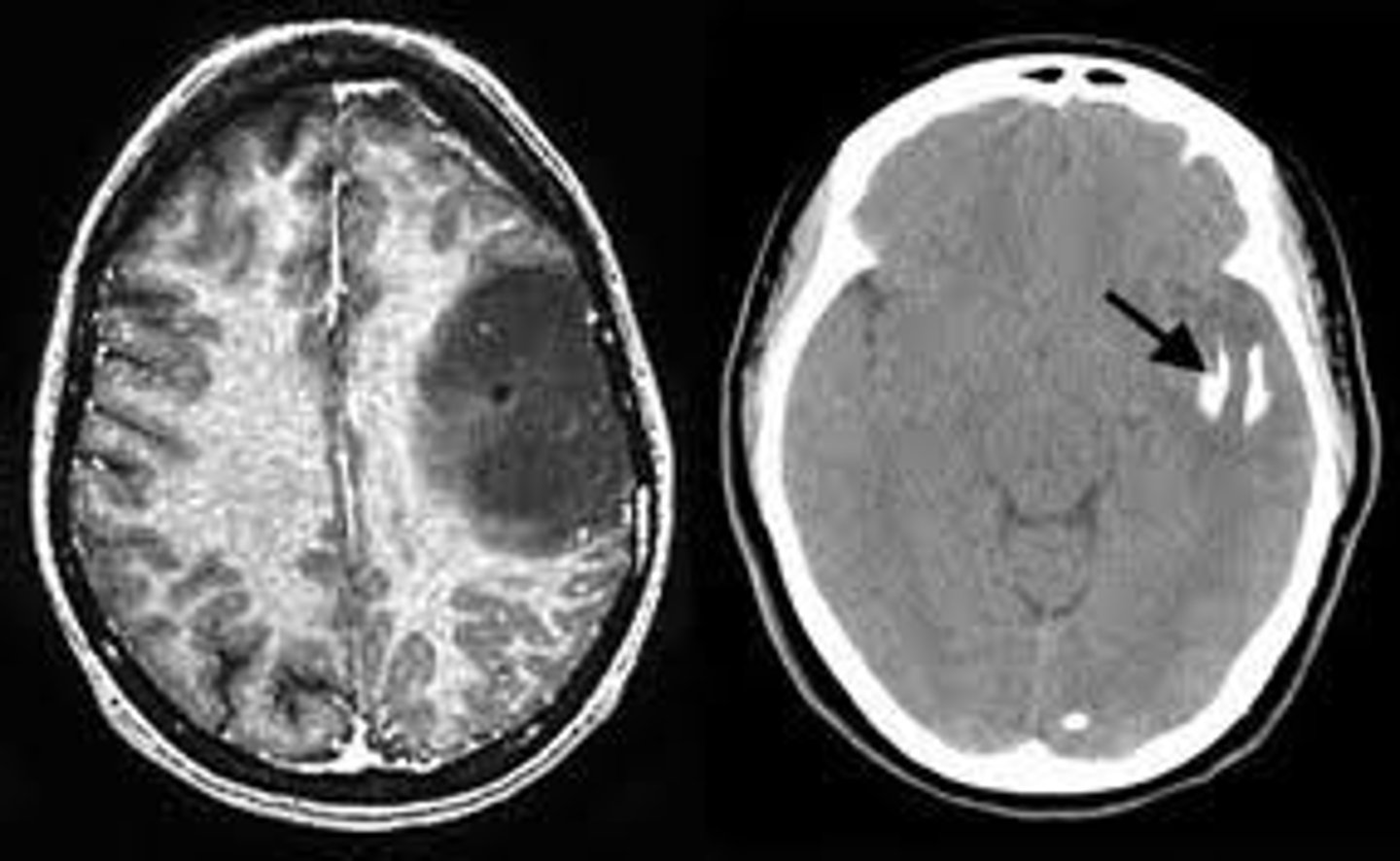
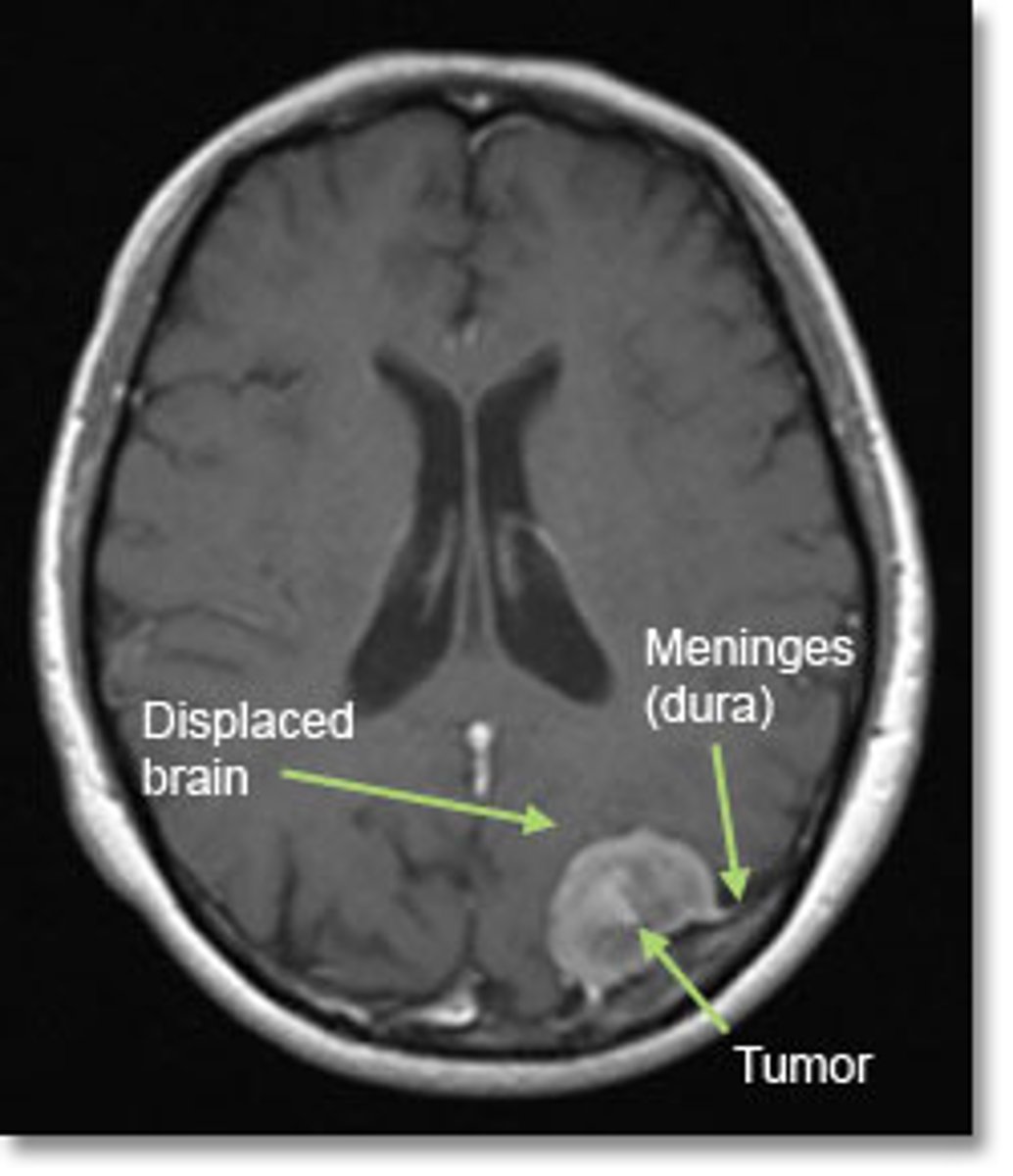
Why is a meningioma significant? Are these usually aggressive?
Most common type of primary brain tumor overall; no - usually found incidentally on neuroimaging & are often benign & slow-growing
What is the most common type of schwannoma?
Vestibular (aka acoustic neuroma - leads to hearing issues such as hearing loss, tinnitus, etc.)
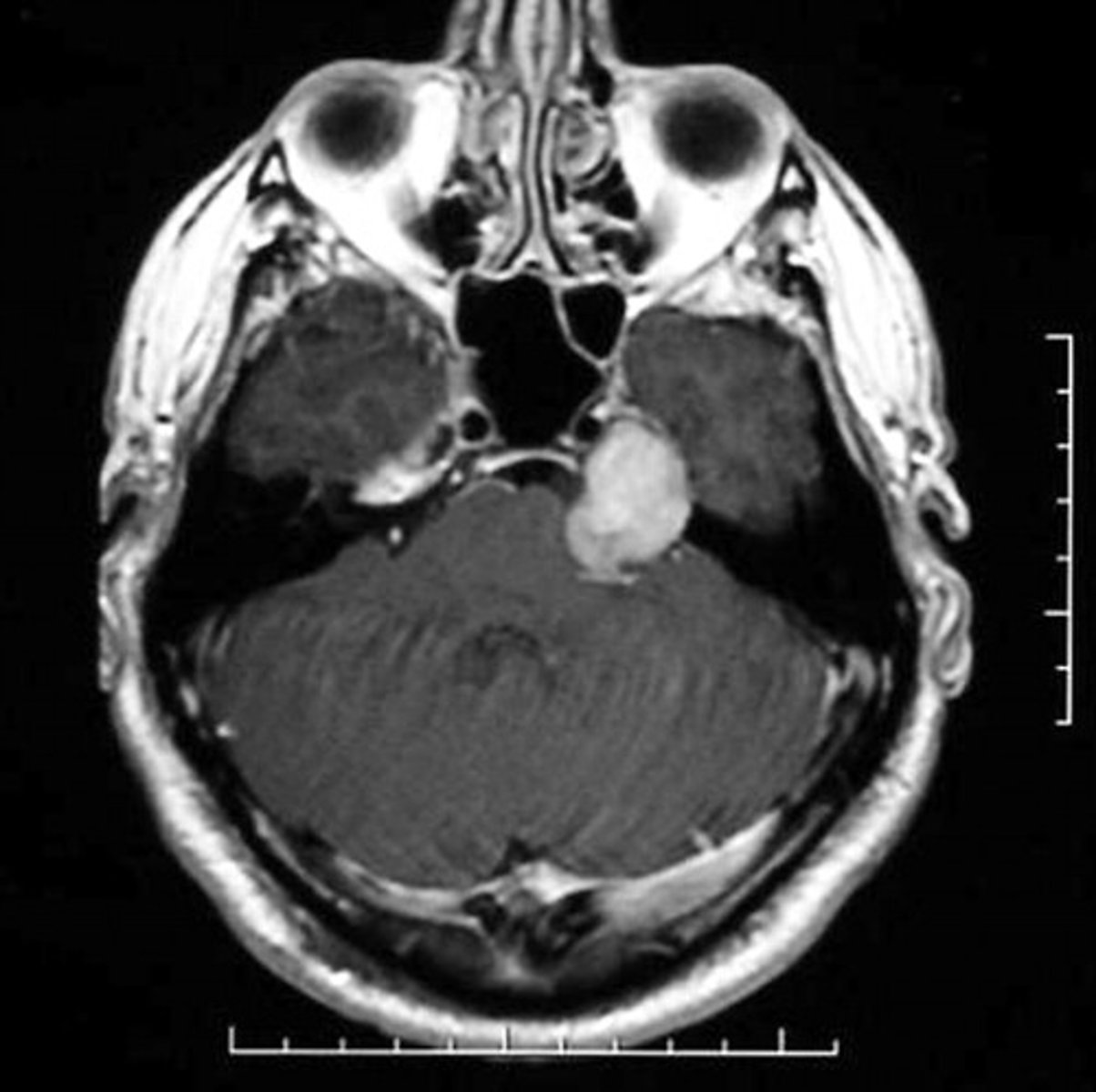
Why are pituitary adenomas significant in terms of their effects on the entire body?
75% are secretory (aka most pituitary adenomas secrete something such as PRL, GH, etc.)
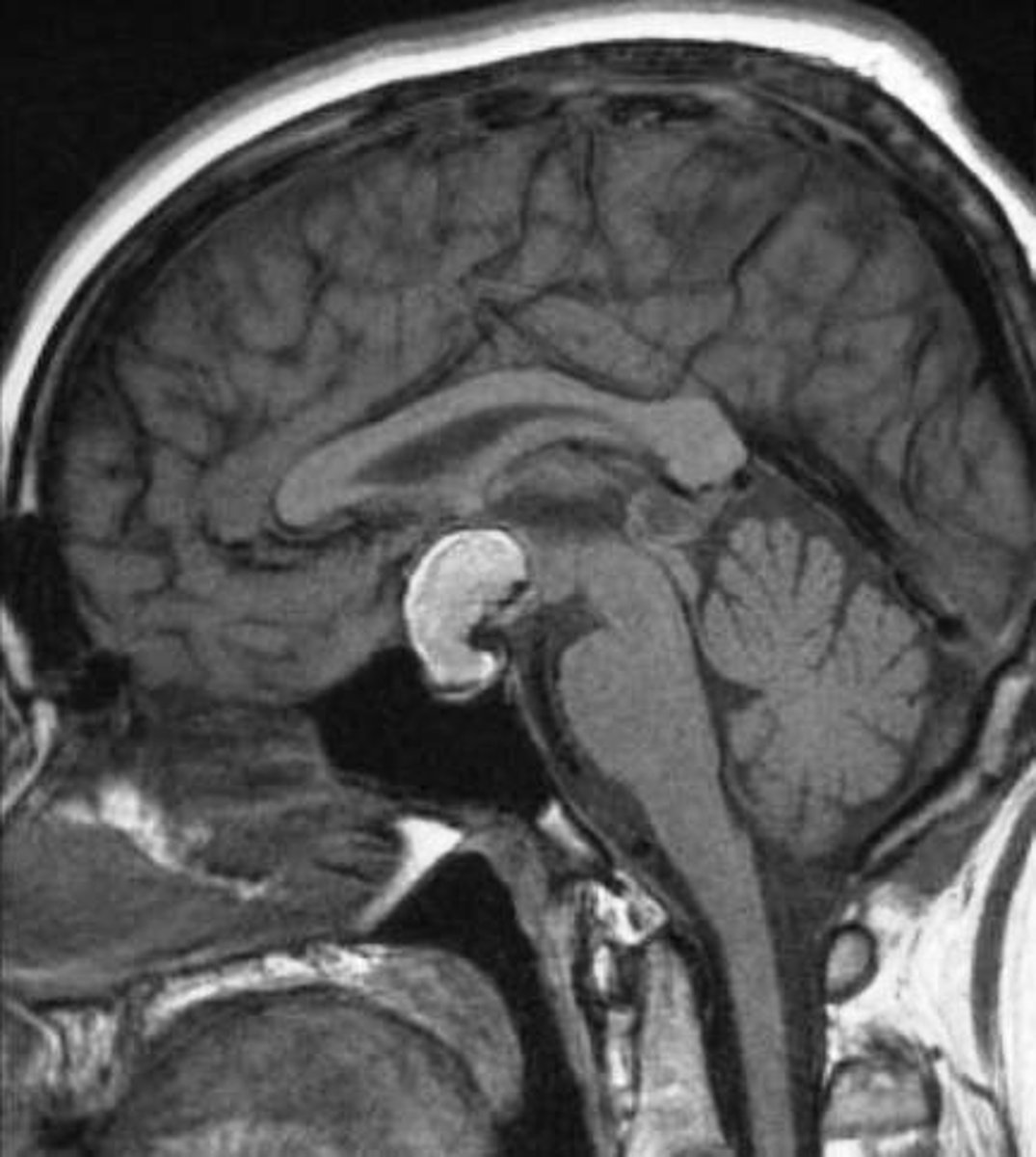
What is bitemporal hemianopsia?
Loss of lateral peripheral fields due to optic chiasm compression (often from a pituitary adenoma)

Why is a medulloblastoma significant?
It is the most common malignant brain tumor of childhood (can spread via the CSF to other parts of the CNS - can lead to obstructive hydrocephalus)
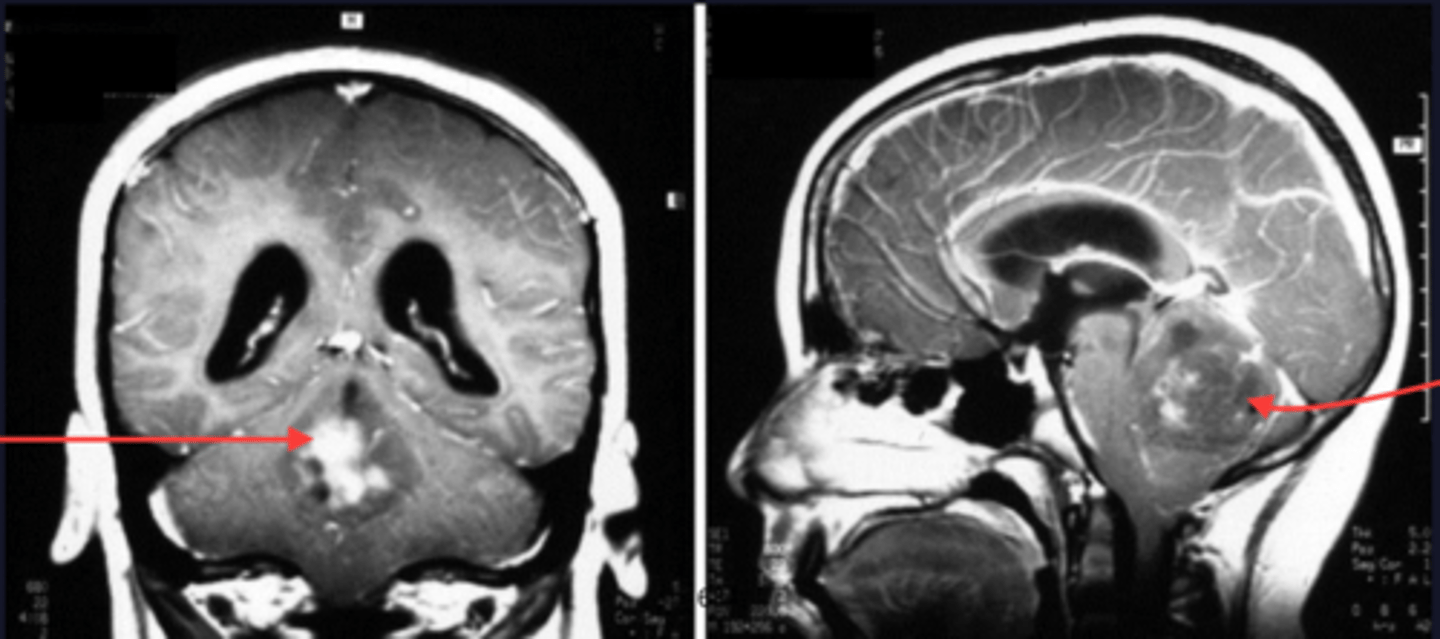
What are some things that put patients at risk of developing a primary CNS lymphoma?
EBV infection, immunosuppression, & being male (keep in mind though that secondary is much more common)
What are the 3 most common cancers to metastasize to the brain?
#1: lung CA (41%)
#2: breast CA (19%)
#3: melanoma (10%)
JUST KNOW: if someone has a PMHX of cancer anywhere and they present with new-onset neurological sxs, we need to think about cancer metastasis to the brain
What is obstructive hydrocephalus, & what are some s/sxs?
Life-threatening complication from brain lesions blocking CSF flow leading to ↑ ICP; dilated & nonreactive pupil, autonomic dysfunction, loss of brainstem reflexes, coma

What is the most common type of spinal tumors (location)? What region of the spinal cord are meningiomas most common in?
Extradural (often metastatic); thoracic region
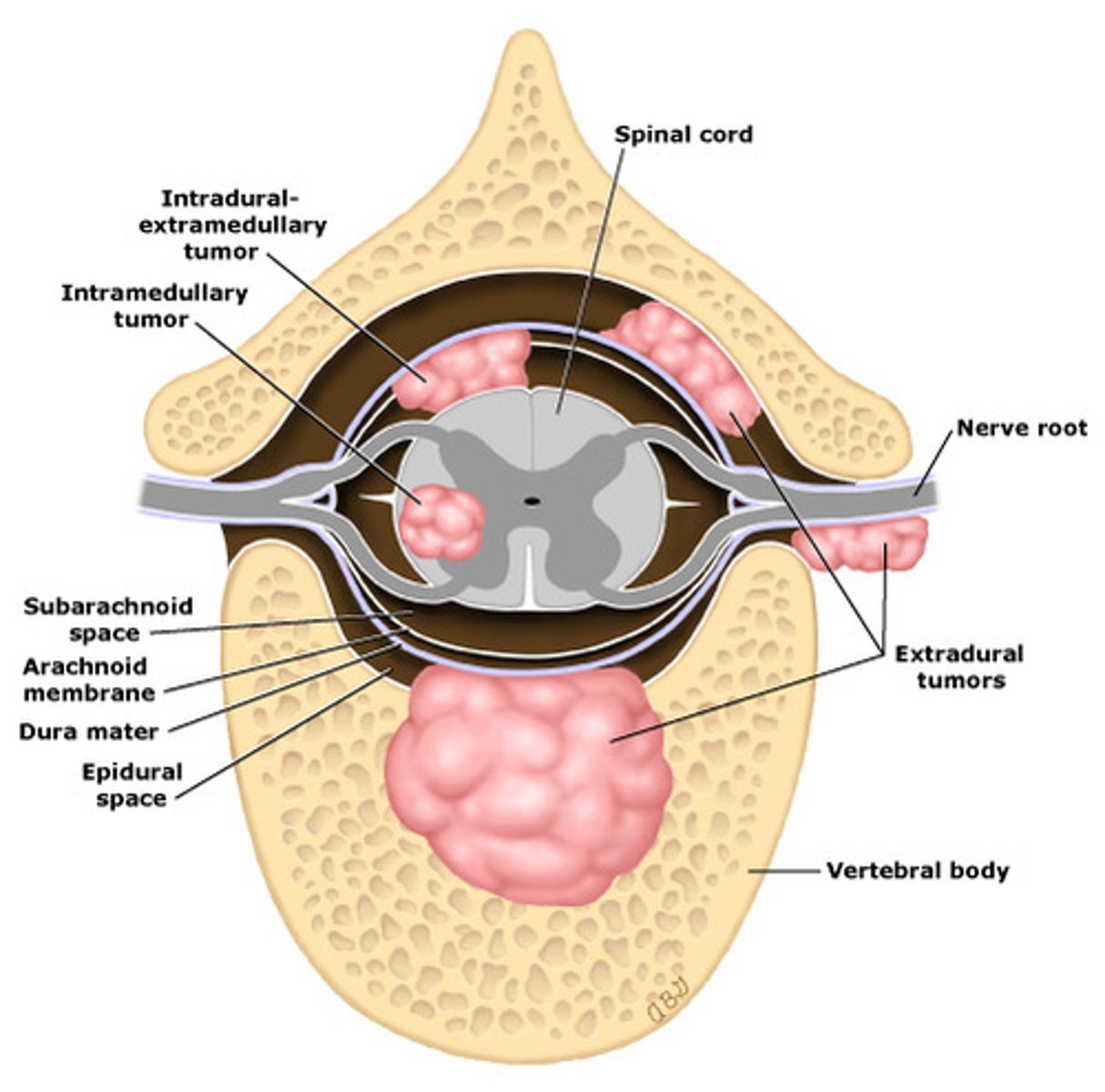
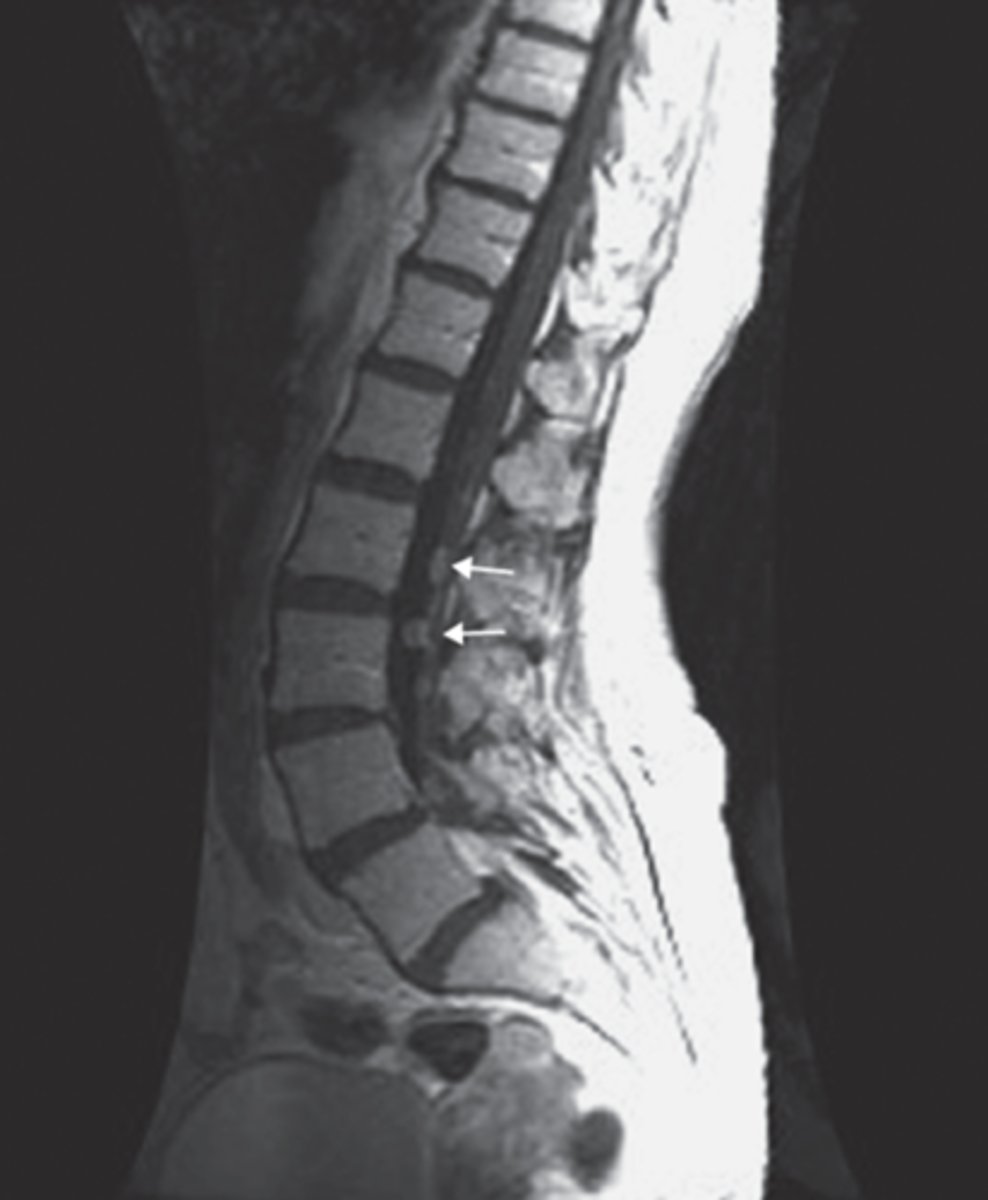
What is the preferred imaging modality to diagnose spinal tumors?
MRI w/ gadolinium contrast
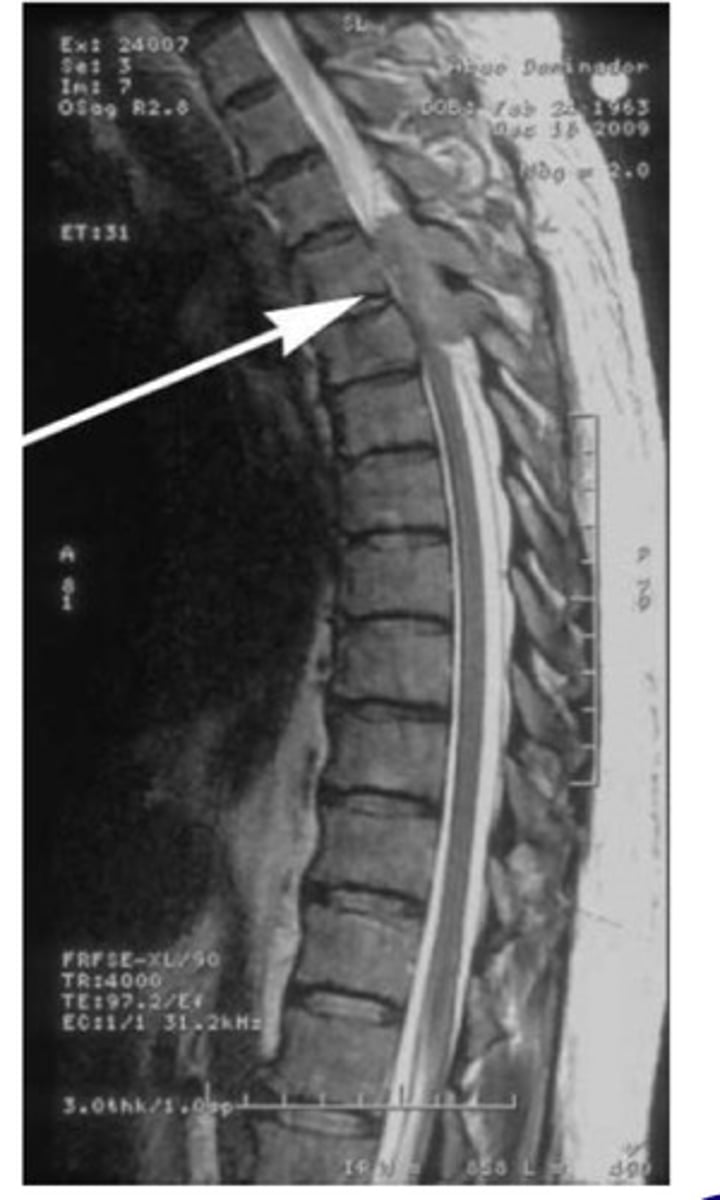
What are the most common cancers to metastasize to the extradural/epidural spinal cord? What is the most common presenting symptom of all types of spinal tumors?
Breast & prostate; back pain
JUST KNOW: just like brain tumors, if someone has a PMHX of cancer anywhere & they start having new-onset back pain, we should NOT dismiss it! We need to consider possible metastasis to the spine
What are leptomeningeal metastases? What is the definitive (gold-standard) diagnostic tool for these?
Metastases to the subarachnoid space; CSF w/ tumor cells (aka positive cytology)
What is Bell's palsy, & how does it usually present? What is it often likely caused by?
Type of mononeuropathy of CN VII leading to an abrupt onset of unilateral upper & lower facial weakness/paralysis; likely due to latent HSV 1 reactivation

What are 2 big risk factors for developing Bell's palsy?
Pregnancy & DM
How is Bell's palsy diagnosed?
Usually clinically as a diagnosis of exclusion (CN VII weakness will be the only neuro abnormality, if other sxs present should do a brain MRI)
How is Bell's palsy managed?
Eye protection (artificial tears, eye patch, glasses/goggles), glucocorticoids +/- antiviral (if palsy is severe)
What is trigeminal neuralgia, & what is it characterized by?
Cranial neuropathy caused by vascular compression or some other irritant of CN V resulting in severe electric shock-like facial pain along the CN V distribution (often unilateral)
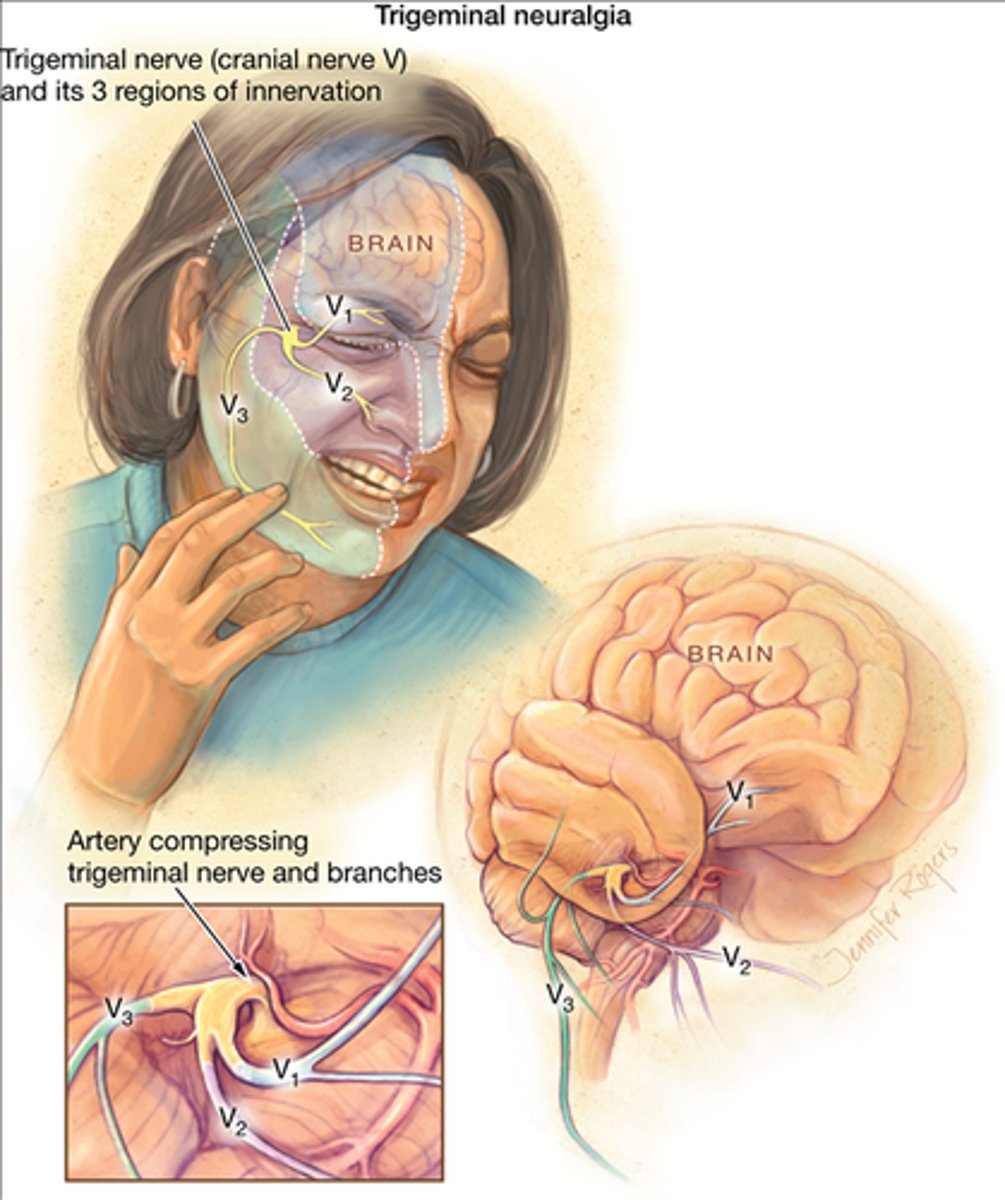
How is trigeminal neuralgia diagnosed & treated?
Diagnosis: MRI/MRA of the brain
Treatment: carbamazepine or oxcarbazepine (anticonvulsant meds); surgery
What is median neuropathy (aka carpal tunnel syndrome), & what are some s/sxs?
Compression of the median nerve; pain, numbness, tingling along median nerve distribution, eventual weakness & thenar atrophy if chronic
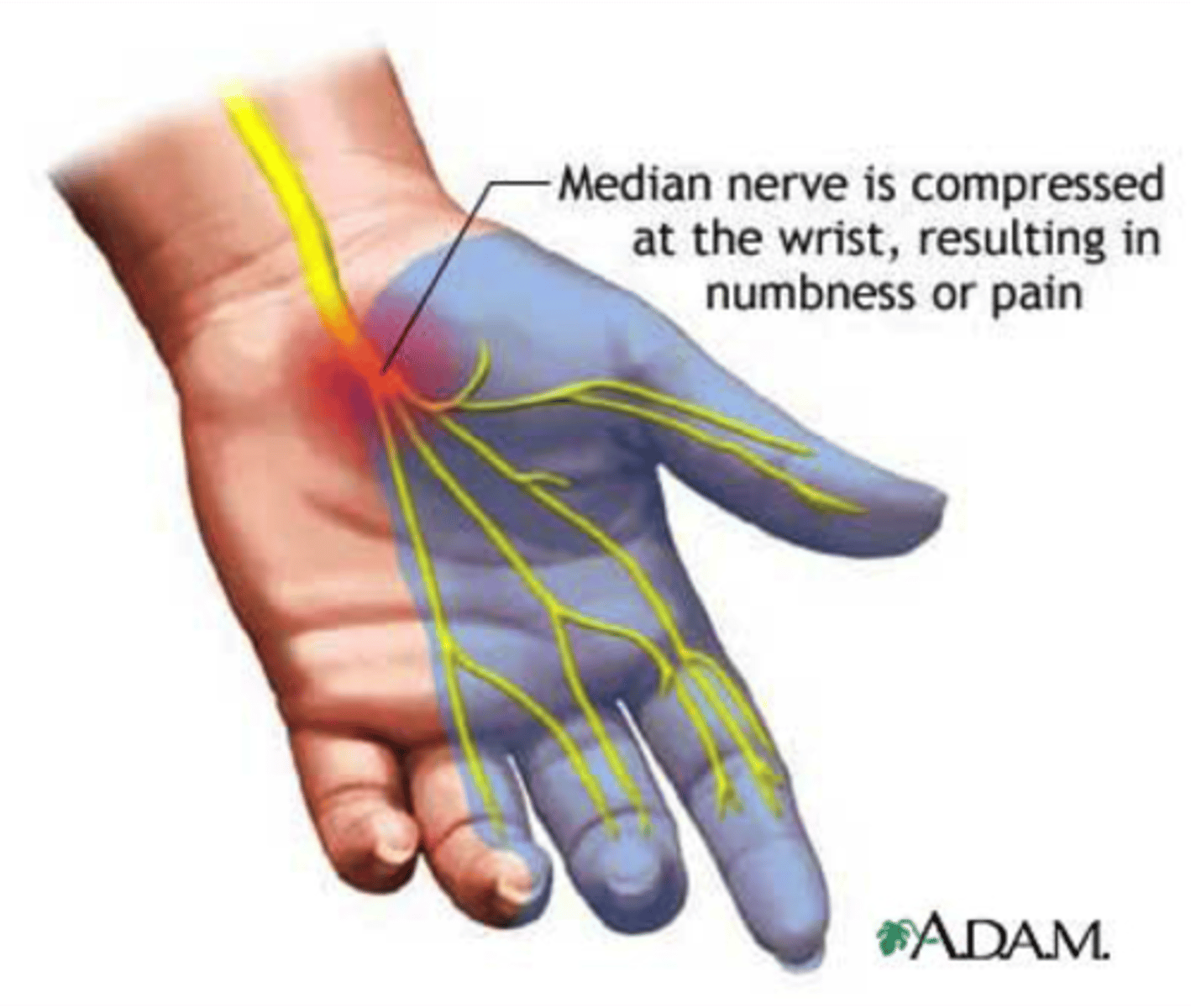
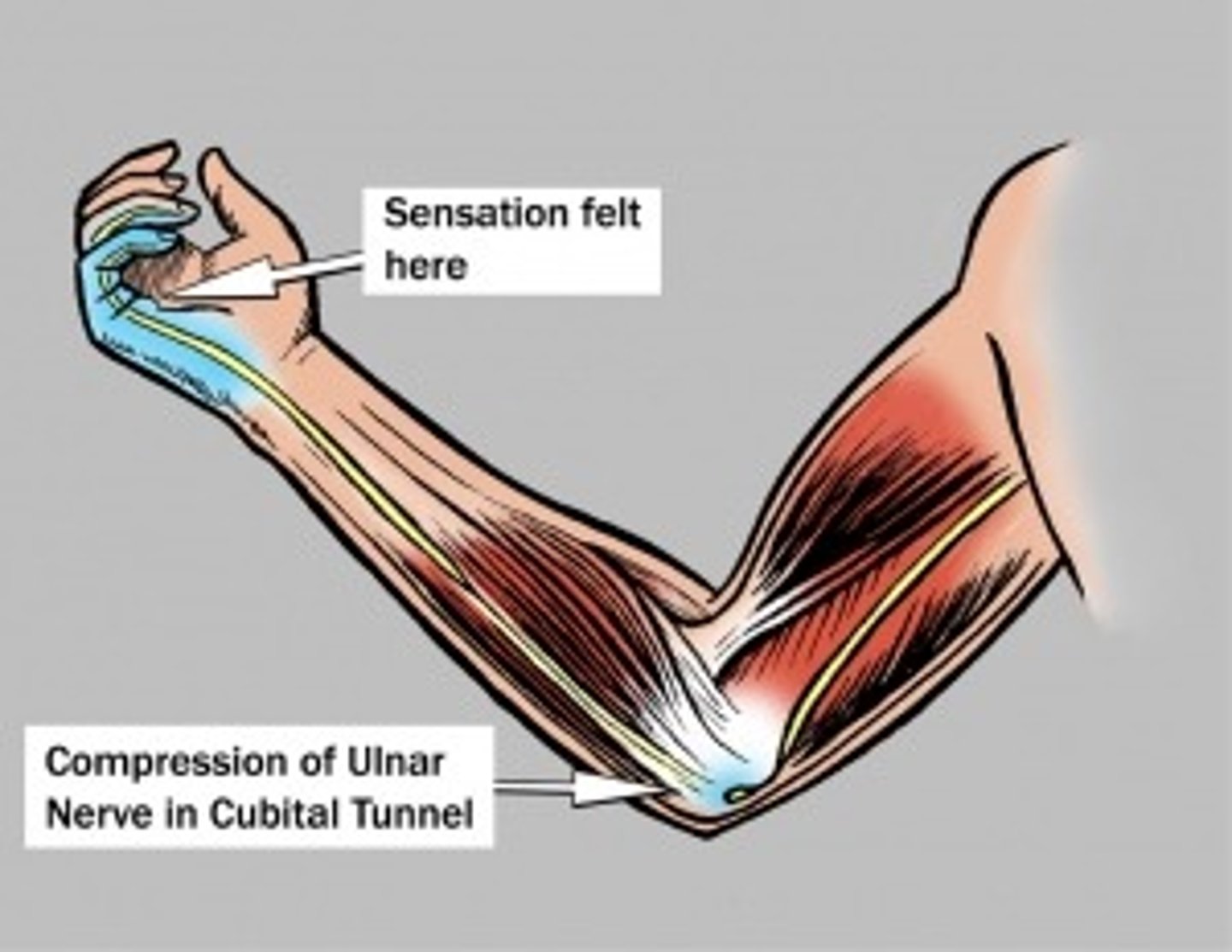
What are some s/sxs of ulnar neuropathy?
Pain, numbness, tingling along ulnar nerve distribution due to nerve compression
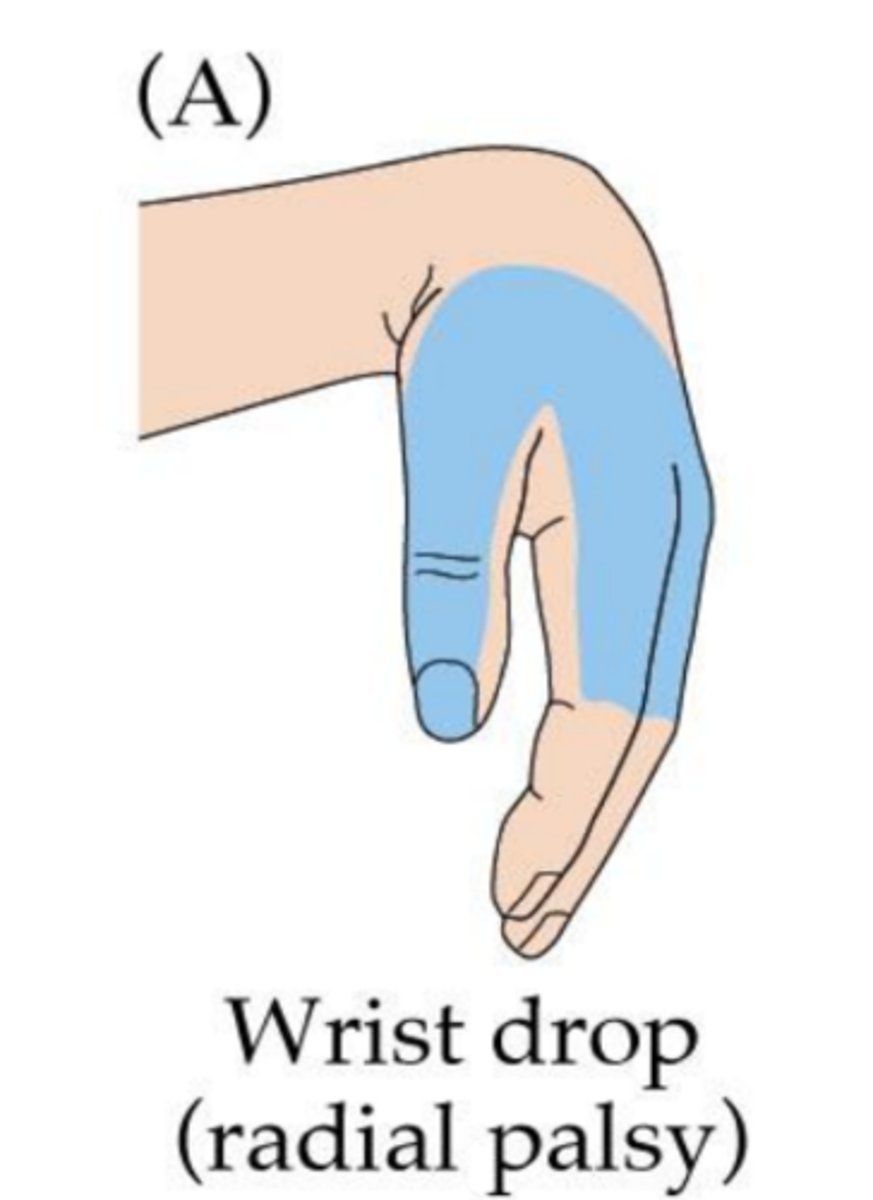
What can be a possible sign of radial neuropathy?
Wrist drop
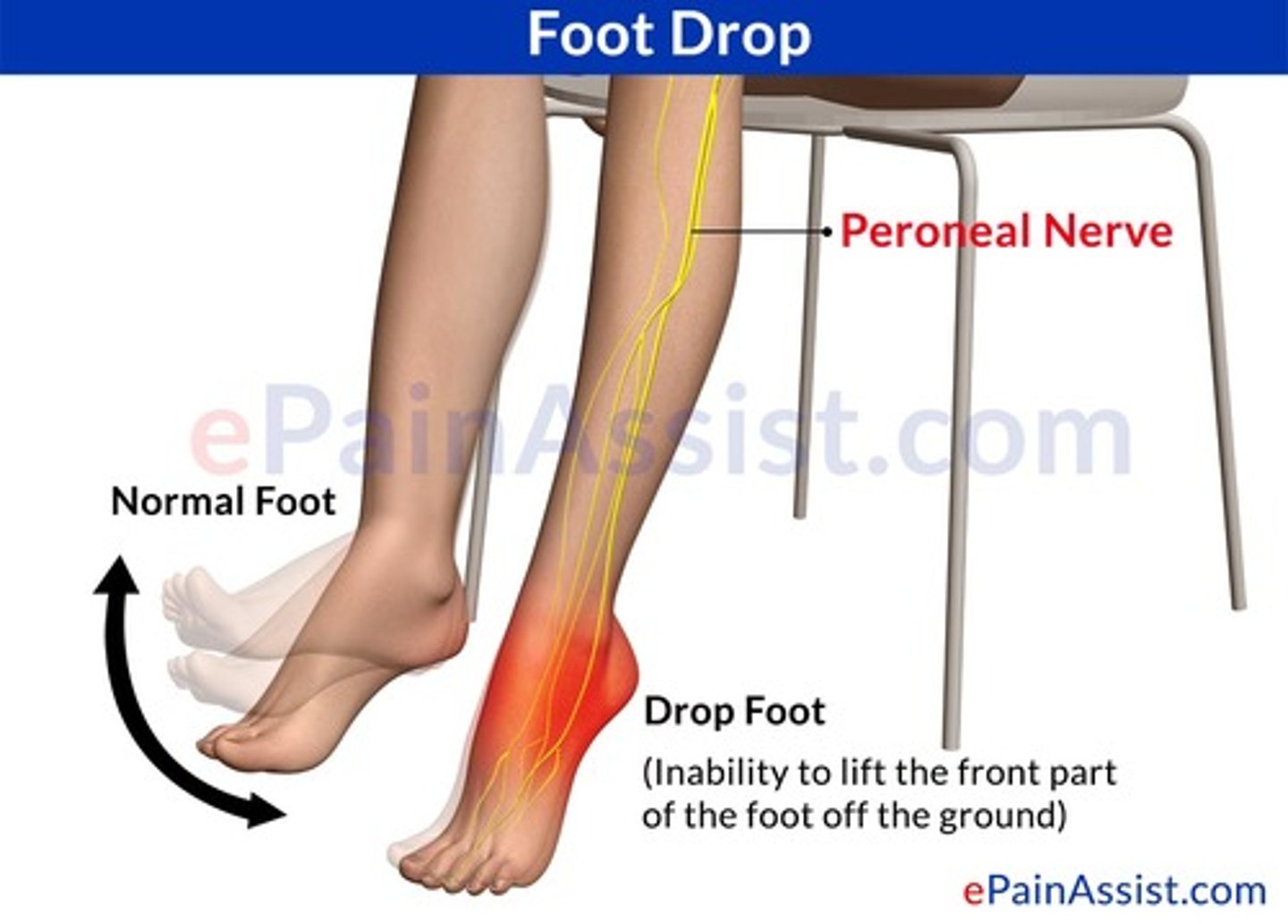
What are some s/sxs of common peroneal mononeuropathy?
Trauma/compression of the nerve results in paresthesias in the lateral lower leg, dorsal foot/1st toe web space, weakness w/ dorsiflexion, & possible foot drop
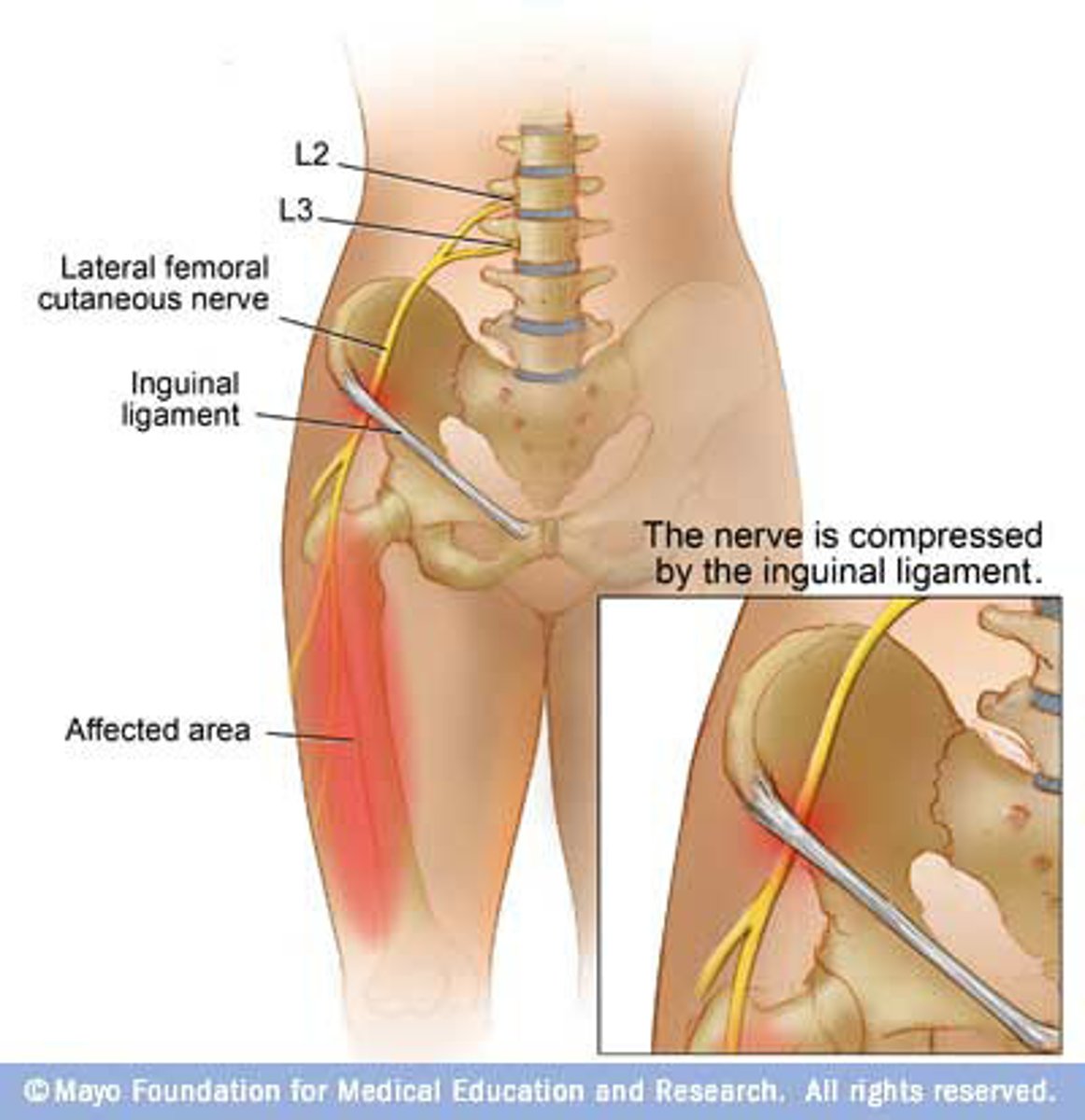
How does lateral femoral cutaneous neuropathy present?
Dysesthesia & sensory loss of the lateral thigh
What are some s/sxs of C6 radiculopathy?
Neck pain, paresthesia to thumb & index fingers, ↓ brachioradialis reflex, weakness in C6-innervated muscles (brachioradialis, wrist extensors)
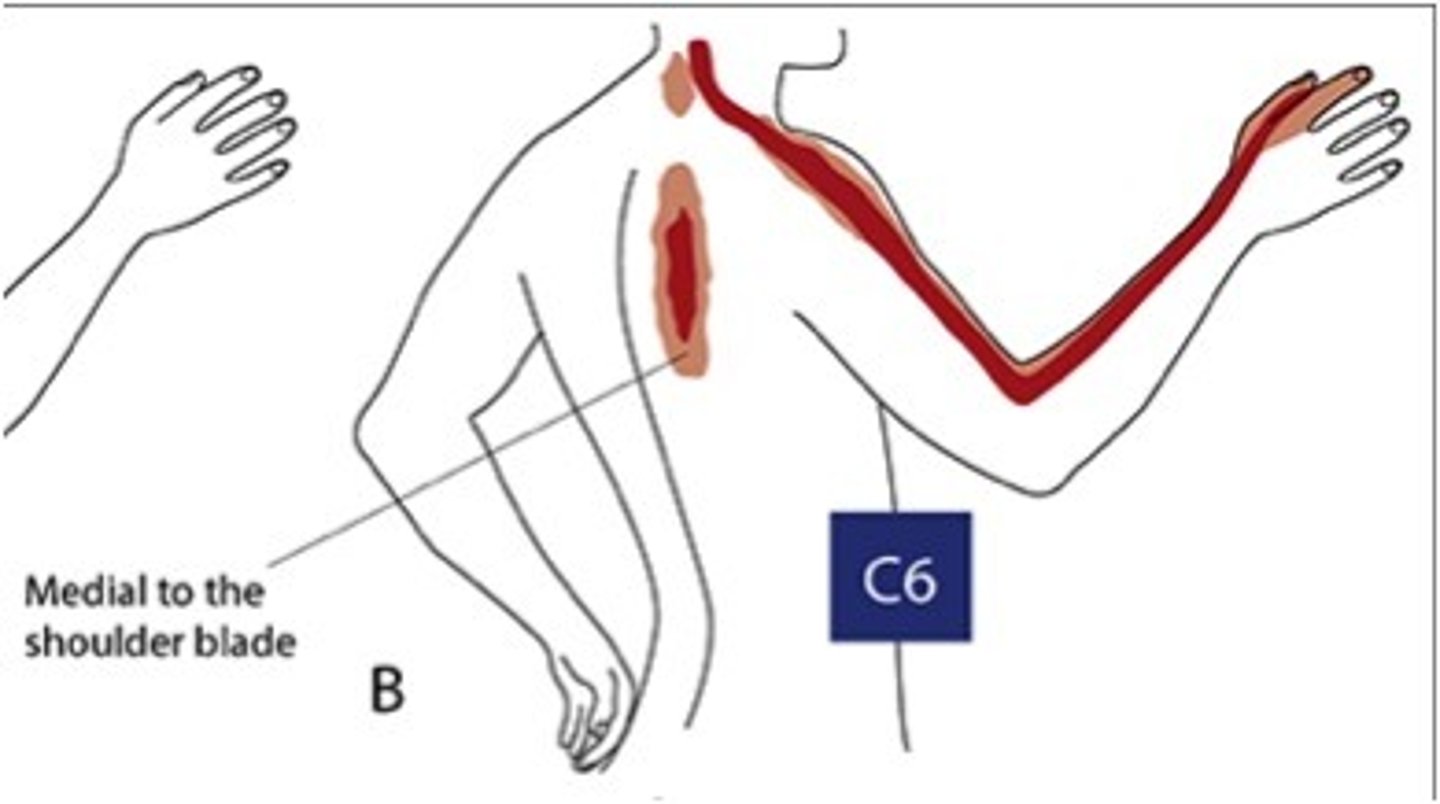
What are some s/sxs of C8 radiculopathy?
Neck pain, paresthesia to ring & little fingers, weakness in C8-innervated muscles (finger flexors)
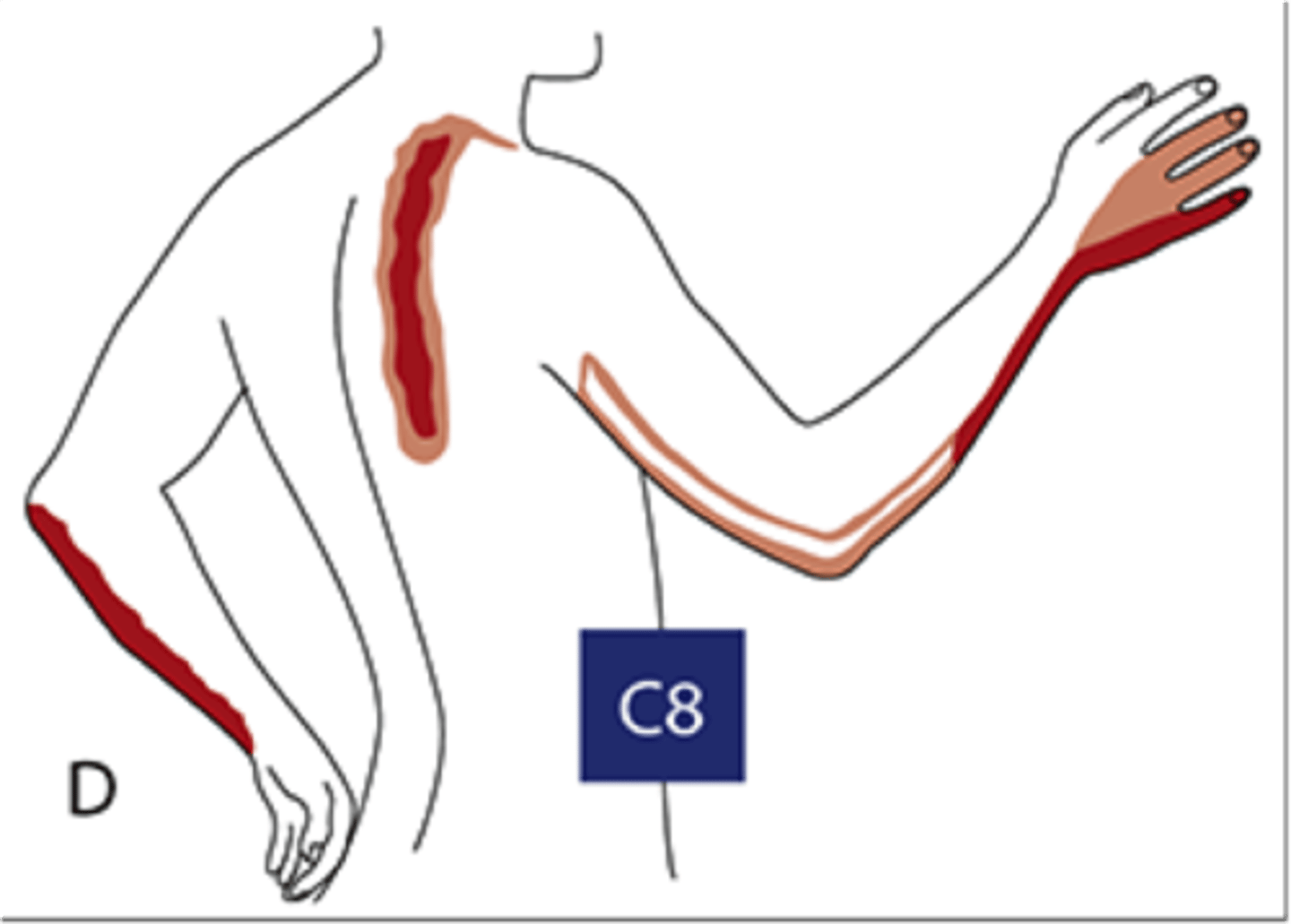
What are some s/sxs of L5 radiculopathy?
Low back pain, paresthesia to top of foot, weakness in L5-innervated muscles (great toe extensors)
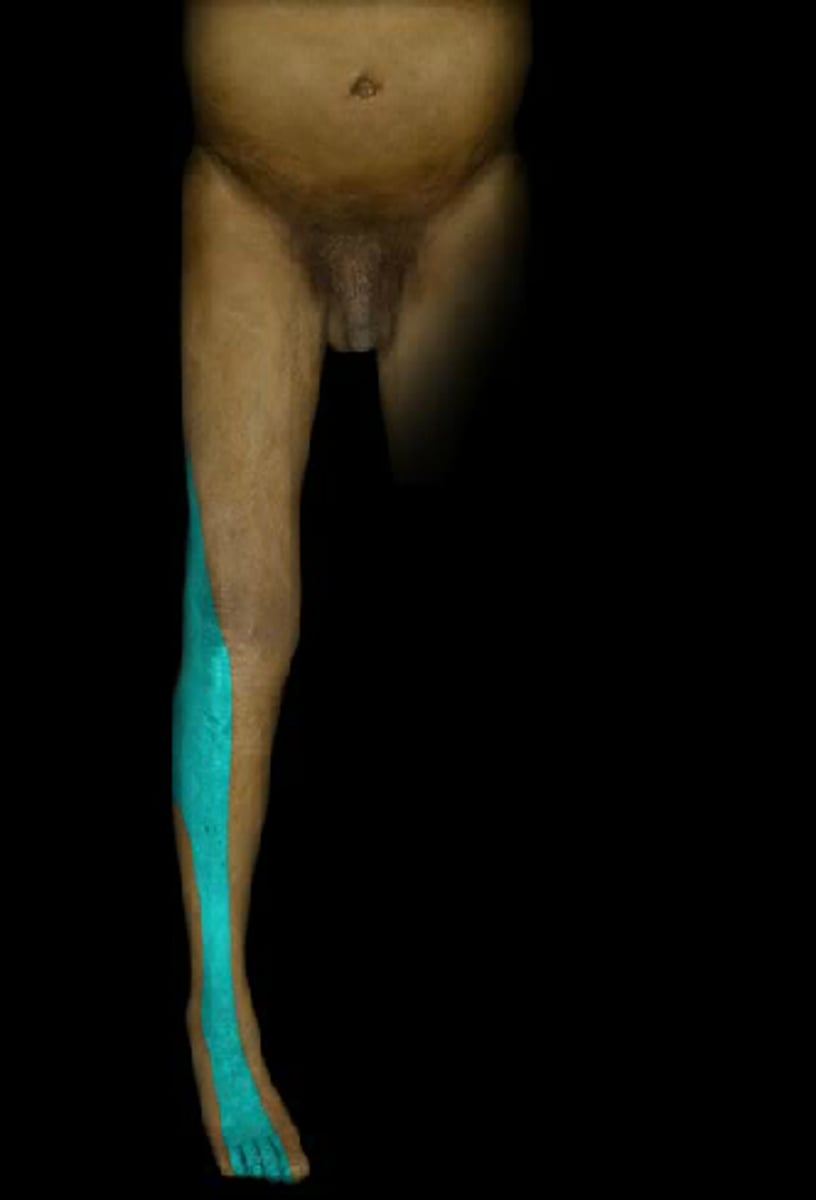
What are some s/sxs of S1 radiculopathy?
Buttock pain, paresthesia down posterior leg to little toe, ↓ Achilles reflex, weakness in S1-innervated muscles (plantarflexors)
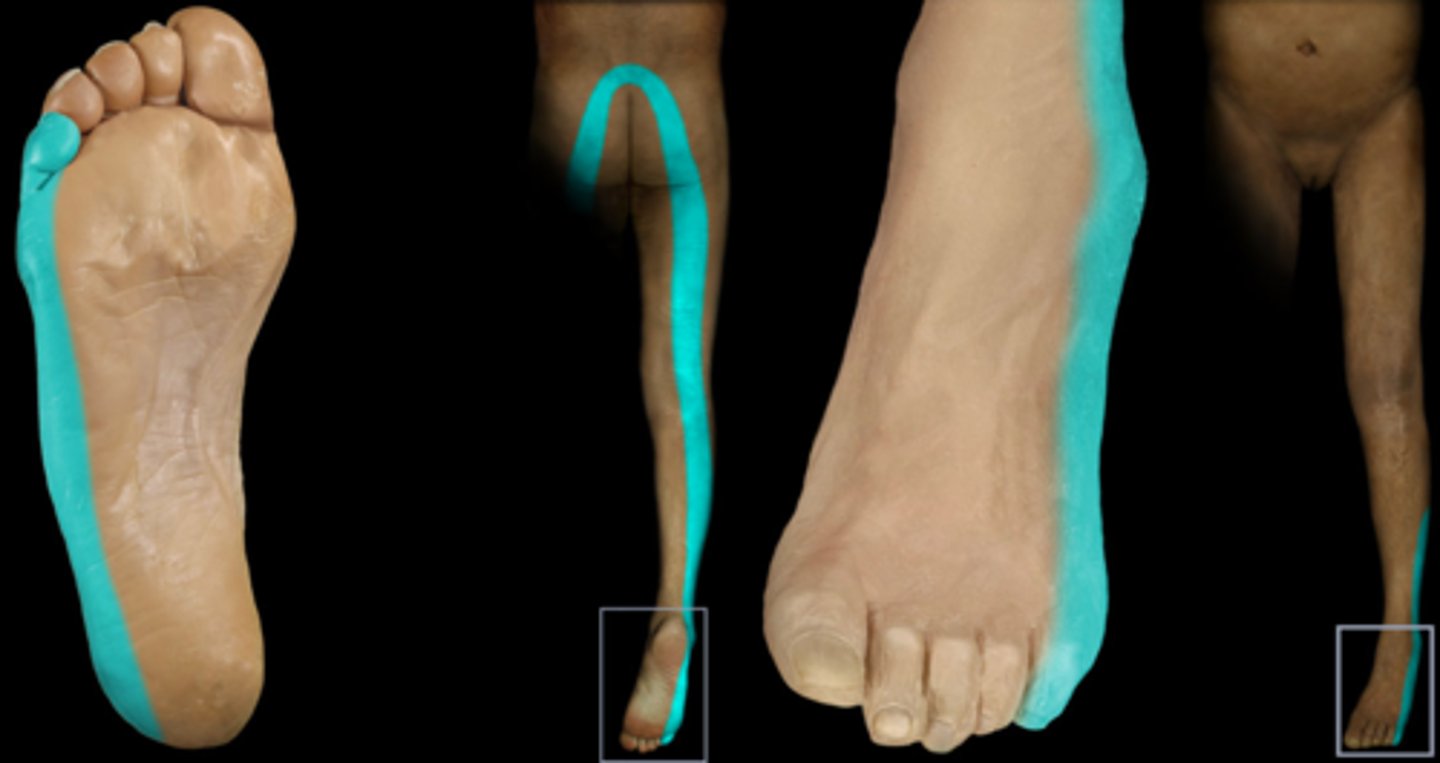
As a general rule of thumb, how do peripheral polyneuropathies tend to present?
Distal symmetric sensory loss (starts in toes) described as a "stocking-glove" pattern along w/ tingling, burning, & deep aching pain