Anesthesia Quiz 1-2
1/93
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
94 Terms
All the following are reasons why we intubate our patients EXCEPT?
So we don't have to monitor our patient respiratory rate
What is the safe PSI rate of oxygen to be delivered to a patient?
15 psi
What part of the anesthesia machine prevents excess buildup of pressure?
pop-off valve
When administering a breath to an anesthetized small patient, the pressure monometer should not exceed ______ cm H2O.
20 cm H2O
This scavenging system requires a vacuum and duct system, and typically includes a scavenger interface to regulate the vacuum.
Active Scavenge
The absorbent granules in the CO2 absorbing canister typically have an _____ hour duration of use before needing to be replaced.
8-10 hours
Mechanical dead space is the area where inhaled and exhaled gases mix, which can ultimately lead to increased end-tidal CO2 levels. What are some effects of increased end-tidal CO2? Check all that apply.
Increased intracranial pressures
Peripheral Vasoconstriction/vasodilation
Respiratory acidosis
The selection of a breathing circuit is based on the patient’s weight. A non-rebreathing system is used for patients weighing more than 5 kg, while a rebreathing system is appropriate for patients weighing less than 5 kg.
False - Non-rebreathing - patients do not rebreathe CO2 is for patients less then 5kgs Rebreathing - patients do rebreathe CO2 is for patients more then 5kgs
The Murphy eye, located on an endotracheal tube, is a small hole situated just below the cuff. What is the primary function of the Murphy eye?
Minimizes the risk of asphyxiation in the event the end of the tube is blocked
You are evaluating a patient's level of consciousness (LOC) and find the patient in a sleeplike state, nonresponsive to verbal stimulus but arousable by painful stimulus. The patient is:
Stuporous
You are evaluating a patient and notice the patient has a mildly decreased level of consciousness (LOC) and can be aroused with minimal difficulty. The patient is:
lethargic
Using the ASA physical status classification system, a patient who is anemic or moderately dehydrated would be classified as:
P3
Which is of the following is NOT a sign of fluid overload?
Sunken eyes
Which of the following is NOT a crystalloid solution?
Dextran
The fluid type most appropriate for replacing moderate losses due to dehydration would be:
Isotonic crystalloids
Which of the following general guidelines about body fluids in a normal adult animal is INCORRECT?
About 40% of the body weight is water
What is a common equipment-related error that puts patients at risk for barotrauma?
Closure of the pop-off valve
Mucous membranes are an indication of blood flow to peripheral tissues. A patient presents to the clinic with yellow-colored mucous membranes. This is an indication of what?
Bilirubin accumulation
How much of the synthetic colloid will remain in the plasma 24 hours after administration?
30-60%
Which diagnostics are included in a big four? Please check all that apply.
PCV
TP
Glucose
BUN
Brown mucous membrane caused by:
Acetaminophen toxicity in cats; intravascular hemolysis
Pale/white mucous membrane caused by:
Blood loss, shock, decrease in peripheral vessel blood flow
Yellow (icteric) mucous membrane caused by:
Hepatic or biliary disorder and/or hemolysis
Blue (cyanotic) mucous membrane caused by:
Hypoxemia

Below is an image of an anesthetic machine. Please identify each part from 1-12.
1. Vaporizer
2. ET Tube
3. Flow Meter
4. Unidirectional Valve
5. Pressure Monometer
6. Reservoir bag
7. O2 flush valve
8. CO2 canister, sodasorb
9. inhale/exhale tube, bain tube, circuit tube
10. Fresh gas inlet
11. Scavenge tube
12. Oxygen
Sassy is a 32 lb mixed-breed dog presenting to the clinic for a routine dental prophylaxis. Dr. Daniels has asked you to calculate her fluid rate at 5mls/kg/hr for the procedure. How many mL/hr of LRS (Lactated Ringer's Solution) will Sassy receive? Round to the nearest tenth if applicable! Show ALL work for full credit.
Your Answer:
32 lbs / 2.2 = 14.5 kgs
14.5 kgs x 5 mls = 72.5 mls
72.5 mls/hr of LRS
Sassy is a 32 lb mixed-breed dog presenting to the clinic for a routine dental prophylaxis. Following the procedure, Dr. Daniels would like Sassy to be on a 2ml/kg/hr fluid rate for 4 hours in effort to improve her hydration status. How much fluid in total following the procedure will Sassy receive? Round to the nearest tenth if applicable! Show ALL work for full credit.
Your Answer:
32 lbs / 2.2 = 14.5 kgs
14.5 kg x 2 ml = 29 mls
29 mls X 4 hours = 116 mls
116 mls of fluid in total.

Please match the arrows to the correct term.
Purple arrow
Pop-off valve
Orange arrow
Occlusion valve
In equine patients, which class of tranquilizers is known to cause penile prolapse, specifically paraphimosis?
Phenothiazines
What type of drug is Atropine?
Anticholinergic
What are three of the most commonly used routes for premedication administration in anesthesia?
IV, IM, SQ, PO
Which class of drugs, when administered intravenously, can cause significant peripheral vasoconstriction and reflex bradycardia?
Alpha 2 Adrenergic Agonist
Which of the following drugs are classified as tranquilizers? (Select all that apply.)
Alpha 2 adrenergic agonist
Phenothiazines
Benzodiazepine
True or False: Diazepam, zolazepam, and midazolam are classified as minor tranquilizers and are ideal for use in very young, sick, or geriatric dogs and cats.
True, Diazepam
Which of the following drugs is an Alpha 2 Adrenergic Agonist?
Xylazine
True or False. Anticholinergics are used to treat tachycardia and increase salivary secretions.
False anticholinergics
True or False. Drugs such as ketamine or Telazol cause muscle rigidity and should be combined with a tranquilizer or opioid to improve muscle relaxation.
True, muscle rigidity
___________ is used to reverse the effects of dexmedetomidine in dogs, cats, and exotic species.
Atipamezole
Commonly used opioids include all EXCEPT: (select all that apply.)
Dexmedetomidine, Xylazine, Methadone, Hydromorphone, Morphine, Midazolam, Fentanyl, Propofol
Dexmedetomidine
Xylazine
Midazolam
Propofol
Which opioid is classified as both an agonist and an antagonist?
Butorphanol
True or False: Opioids cause mydriasis (pupil dilation) in dogs and miosis (pupil constriction) in cats.
False, opposite.
MAC of Sevoflurane in dogs is _________?
2.4%
Which of the following is NOT a side effect of inhalant anesthetics?
Hypertension
The MAC of Isoflurane in dogs is _________?
1.3%
Which of the following drugs are included in the “chill protocol”? (Select all that apply) GTA
Gabapentin, Trazodone, Acepromazine
Administration of this induction agent too slowly can result in myoclonus:
Propafol
Unlike other induction agents, this drug typically causes only mild apnea but is associated with a rough recovery. Which drug is being described?
Alfaxalone
This inhalant anesthetic has low blood-gas solubility and lower potency, making it ideal for anesthesia in equine patients. Which inhalant is being described?
Sevoflurane
This type of fluid rapidly, but temporarily, draws water into the intravascular space and helps support blood pressure. Which fluid is being described?
Hypertonic fluid
1A. Dolly weighs 10kgs and would need a 10mcg/kg/hr CRI of Fentanyl (50mcg/ml) and a 10mcg/kg/min CRI of 2% Lidocaine during surgery. How many mls/hr of each drug would Dolly receive?
1B. Post surgery, Dr. Davis would like to continue the Fentanyl (50mcg/ml) for Dolly at 2mcg/kg/hr for 5 hours. How many mls/hr will Dolly receive? How many mls total will Dolly receive over 5 hours? (Show all work to receive full credit)
Your Answer:
1A) 10kg x 10mcg/kg/hr = 100mcg/hr
100mcg/hr / 50mcg/ml = 2mL/hr of fentanyl
Lidocaine: 10kg x 10mcg/kg/min = 100mcg/min
100mcg/min x 60 min = 6,000 mcg / 1000 mcg = 6mg/hr / 20mg/ml = 0.3 ml/hr of Lidocaine
1B) 10kg x 2mcg/kg/hr = 20mcg/hr
20mcg/hr / 50mcg/ml = 0.4 ml/hr of Fentanyl
0.4ml/hr x 5 hr = 2ml total recieved over 5 hours.
Princess, a 20kg boxer, was given 12mls of Propofol (10mg/ml) for induction. What was she given in mgs? What was her mg/kg dose? (Show all work to receive full credit)
Your Answer:
12ml x 10mg/ml = 120mg given.
120mg / 20kg = 6mg/kg of Propofol
How many mls of Acepromazine (10mg/ml) will a 1000lb equine patient require at a dose of 0.04mg/kg? (Show all work to receive full credit)
Your Answer:
1000/2.2 = 454.54 kg
454.54kg x 0.4mg/kg = 18.18 mg
18.18mg / 10mg/ml = 1.8ml of Ace
Cassie is a 25 kg mixed-breed dog, and the total blood volume of a dog is 90 mL/kg. She comes into the clinic, and the DVM asks you to calculate her total blood volume and determine how much blood she could safely lose if 20% of her blood volume is lost. (Show all work to receive full credit)
Your Answer:
25kg x 90ml/kg = 2250 mL Total Blood Volume
2250ml x 20% = 450mL can be safely lost.
This stage of anesthesia is subdivided into 4 different planes of anesthesia based on eye movement, pupil size, and eyelid movement.
Stage 3
This stage of anesthesia is known as the period of involuntary movement. Within this stage of anesthesia, the patient can go through an excitement stage and have involuntary reactions such as vocalizing, struggling, or paddling.
Stage 2
This stage of anesthesia is known as the anesthetic overdose stage. Within this stage, the patient may experience a dramatic drop in heart rate and blood pressure.
Stage 4
Subjective monitoring consists of physical assessment. All are included in subjective monitoring EXCEPT......
Blood Pressure
__________ is produced by the contraction of the left ventricle as it propels blood.
Systolic
________ measures the percentage of oxygen bound to hemoglobin.
Pulse Oximetry
A ______ in CO2 can indicate hyperventilation (alkalosis) in a patient under anesthesia.
Decrease
Monitoring patient under anesthesia help maintain legal records, record all drugs administered to the patient, and enhance recognition of trends or unusual values for physiological parameters. A minimum of what should be recorded? Check all that apply.
Heart rate, Blood pressure, and Oxygenation
This type of blood pressure monitoring gives a continuous reading of the blood pressure throughout the procedure and is more accurate.
Direct blood pressure
Blood gases are used to measure the blood pH, and the dissolved oxygen and carbon dioxide gas in the arterial blood. Which value is use as a invasive method of monitoring the CO2?
PACO2
Pain is recognized as a complex phenomenon comprising several distinct types. This type of pain is characterized by an immediate onset of pain. Please match the term to the definition.
Acute pain
Pain is recognized as a complex phenomenon comprising several distinct types. This type of pain is characterized by the pain originating from organs. Please match the term to the definition.
Visceral pain
Pain is recognized as a complex phenomenon comprising several distinct types. This type of pain is characterized by having a long duration of pain. Please match the term to the definition.
Chronic pain
Pain is recognized as a complex phenomenon comprising several distinct types. This type of pain is characterized by pain occurring at the site of the tissue injury due to the release of chemical mediators. Please match the term to the definition.
Inflammatory pain
What drug is ideal for treating windup pain?
Ketamine
The pathway of pain in the body is referred to as nociception with four main steps. During this step, signals are transmitted to the brain, where they are processed and recognized. Please select the correct term.
Perception
The pathway of pain in the body is referred to as nociception with four main steps. During this step, signals are conducted to the spinal cord via the peripheral nerves. Please select the correct term.
Transmission
All are physiologic signs of pain under anesthesia EXCEPT:
Hypotension
Constant release of pain mediators can lead to other known conditions. One condition seen is when there is an increase in sensitivity to a painful stimulus, usually seen clinically as an exaggerated response to stimuli. Please select the correct term.
Peripheral hypersensitivity
True or False. All species show pain in the same way. This can include but not limited to vocalizing, hunched back, and biting.
True
Regional/Local anesthetic blocks are important because they reduce the MAC of inhalant being used, lower the recovery time, and help avoid using general anesthesia in large animal patients such as equine and bovine. The retrobulbar block will block the orbit and optic nerve. When done correctly, the eye should look exophthalmic. True or False. This block can be used in most ophthalmology cases?
False
Regional/Local anesthetic blocks are important because they reduce the MAC of inhalant being used, lower the recovery time, and help avoid using general anesthesia in large animal patients such as equine and bovine. What block is used to block the half of the maxilla on which the block is performed?
Maxillary block
Regional/Local anesthetic blocks are important because they reduce the MAC of inhalant being used, lower the recovery time, and help avoid using general anesthesia in large animal patients such as equine and bovine. What block is used to block the maxilla rostral to the first premolar and can be using in procedures such as a rhinoscopy.
Infraorbital block
Regional/Local anesthetic blocks are important because they reduce the MAC of inhalant being used, lower the recovery time, and help avoid using general anesthesia in large animal patients such as equine and bovine. This block is used to block the forelimb from the distal half of the humerus to the toes and can be used in procedures such as elbow scopes or forelimb fractures.
Brachial plexus block
Regional/Local anesthetic blocks are important because they reduce the MAC of inhalant being used, lower the recovery time, and help avoid using general anesthesia in large animal patients such as equine and bovine. This block is used to block the perineum, rectum, and tail. It is the regional technique of choice with cats who are blocked.
Sacrococcygeal epidural
When performing a semimembranosus/semitendinosus IM injection, which nerve are you wanting to avoid?
Sciatic
During intubation, a cat trachea is much more sensitive than a dog trachea and more prone to trachea injuries. When intubating a cat, what is the max amount of air to use when inflating the cuff on the endotracheal tube?
5 mls
All are classified as agents that could be use for induction EXCEPT:
Acepromazine
There are many complications of intubation. One common complication is aspiration during the recovery period of anesthesia. Which complication is aspiration associated with?
Underinflation
There are many complications of intubation. One common complication is the diameter of the tube being too large. All are signs of the tube diameter being too large EXCEPT:
Reduces or block the flow of oxygen to the patient
True or False. Placement of the ECG electrodes does not matter as long as they cross the heart.
True
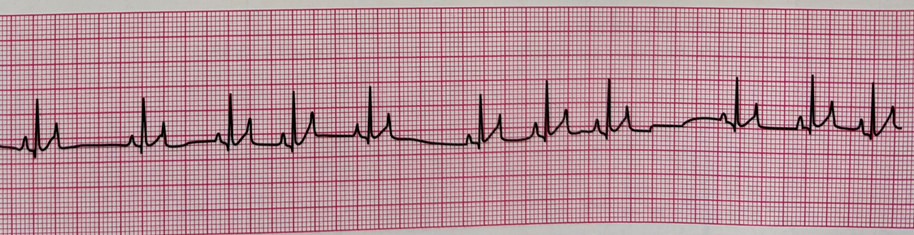
The ______ arrhythmia is common under anesthesia for dogs. It is characterized by longer than normal spaces between QRS complexes and corresponds with breathing. Please name the arrhythmia shown below.
Sinus
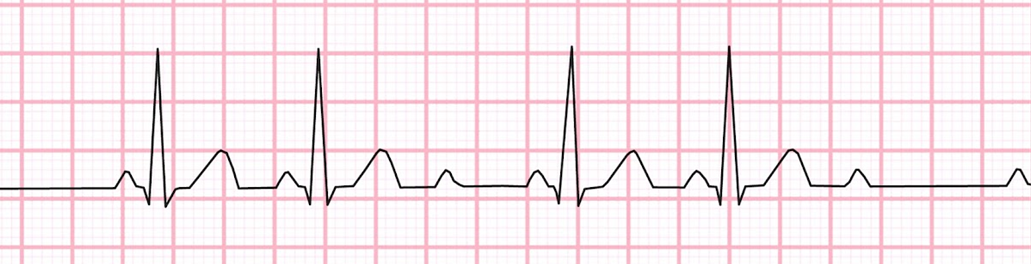
The _____ arrhythmia has no lengthening in the P-R intervals. It is characterized by a "lonely p wave" with no corresponding QRS complex. Please name the arrythmia shown below.
Mobitz type 2
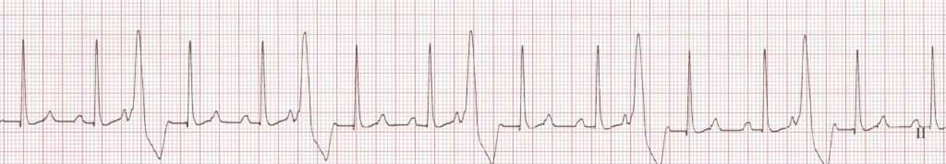
The ___ arrhythmia is characterized by wide and bizarre QRS complexes without a P wave. There are different types of this arrhythmia which include unifocal, multifocal, and runs. Please name the arrhythmia.
PVC
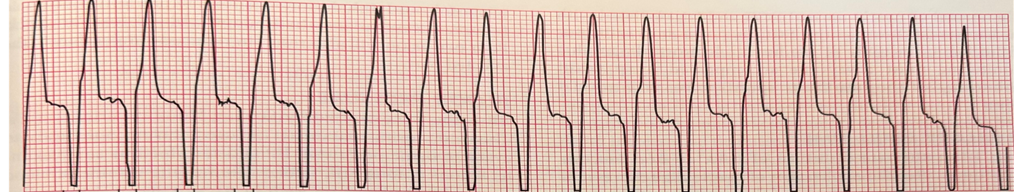
The ________ arrhythmia is fast and characterized by bizarre looking QRS complexes with no P or T wave. This arrhythmia can be treated with Lidocaine or beta blockers if the arrhythmia is stable. Please name the arrhythmia shown below.
Ventricular Tachycardia
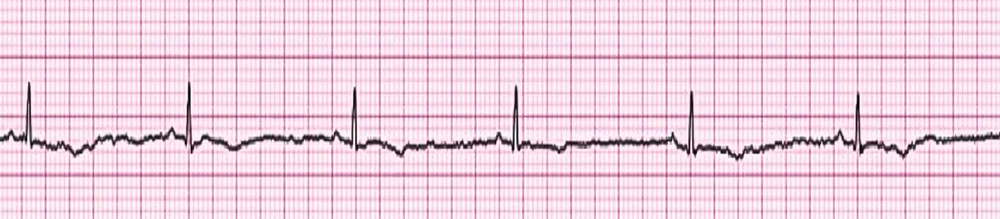
The _________ arrhythmia is characterized by no palpable pulse or electrical activity. Compressions are required for this arrhythmia. Please name the arrhythmia shown below.
Asystole
Part 1:
Duke, a 5-year-old, 36 kg male neutered canine, comes into the clinic for a TPLO. The doctor would like for you to use Acepromazine at 0.02 mg/kg with a concentration of 1 mg/ml and Hydromorphone at 0.2 mg/kg with a concentration of 10 mg/ml. How many mls of each drug will you give? Show all work, including units, to receive full credit.
Your Answer:
ACE
36kg x 0.02mg/kg = 0.72 mg of Ace
0.72mg of Ace / 1ml/1mg = 0.72ml or 0.7ml rounded to the tenths of Ace
Hydromorphone
36kg x 0.2mg/kg 7.2 mg of Hydro
7.2mg Hydro/ 1ml/10mg = 0.72ml or 0.7ml rounded to the nearest tenths of Hydro.
* I know its supposed to throw us off getting the same amount of mls for both but it all comes down to the concentrations.
Part 2:
Like all opioids, the side effects of this drug class include vomiting, but Hydromorphone is the opioid most likely to cause a patient to vomit. The doctor would like you to add Cerenia at 1 mg/kg with a concentration of 10 mg/ml, to be given IV after the premedications are administered and a catheter is placed. How many mls of Cerenia will you give Duke? Show all work, including units, to receive full credit.
Your Answer:
36kg x 1mg/kg = 36mg of Cerenia
36mg / 1ml/10mg = 3.6ml of Cerenia
Part 3:
After induction, the doctor asks you to give a lumbosacral epidural using PF Morphine at 0.1 mg/kg with a concentration of 1 mg/ml and 0.5% Bupivacaine at a dose of 0.5 mg/kg. Calculate how many mls of each drug you will give Duke. Show all work, including units, to receive full credit.
Your Answer:
Morphine
36kg x 0.1mg/kg = 3.6mg
3.6mg / 1ml/1mg = 3.6ml of Morphine
Bupivacaine
36 x 0.5mg/kg = 18mg
0.5% -> 5mg/ml of Bupi
18mg / 1ml/5mg = Bupivacaine
Part 4:
During surgery, you notice Duke is very reactive to stimuli when the doctor begins drilling to prepare for screw plate and screw placement. He states the epidural has failed and would like you to start a Fentanyl CRI. This opioid is short-acting, so you must give a bolus before starting the CRI. The doctor would like you to administer a Fentanyl bolus at 5 mcg/kg with a concentration of 50 mcg/ml. After the bolus, he would like you to start the Fentanyl CRI at 7 mcg/kg/hr. How many mls of Fentanyl will you give for the bolus, and what will be the ml/hr rate for the CRI? Show all work, including units, to receive full credit.
Your Answer:
Fentanyl Bolus
36kg x 5mcg/kg = 180mcg
180mcg / 1ml/50mcg = 3.6ml of Fentanyl for Bolus
Fentanyl CRI
36kg x 7mcg/kg/hr = 252mcg/hr
252mcg/hr / 1ml/50mcg = 5.04 ml of 5mls when rounded of Fentanyl
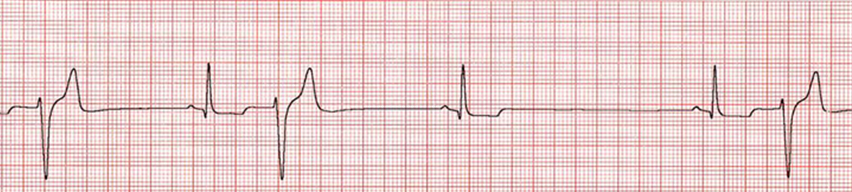
The arrhythmia is characterized by bizarre looking QRS complexes with no P or T wave. It is typically associated with slow heart rates and treated with anticholinergics. Please name the arrhythmia shown below.
Escape Beats