Bone Biomechanics and Forces
1/21
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
22 Terms
List the different forces which act on a typical long bone
Tension
Compression
Shear
Torsion
Bending
Describe the effects of tension on the microstructure of a long bone
Non-Haversian system: regions under high tensile stress typically exhibit a lack of secondary osteons, which are commonly found in high-compression areas
Mineralization levels: tensile areas often show higher mineralization levels than surrounding tissues, indicating the microstructure is optimized to manage tension
Collagen fibre: tensile stress causes collagen fibers to align, stretch, and undergo molecular slippage, which helps manage and dissipate energy
Describe the effects of compression on the microstructure of a long bone
Microcracks: significant damage causes microcracks to form, under extreme compression, these microcracks can coalesce, leading to "creep" (gradual, permanent deformation) or eventual fracture
Trabecular destruction: long-term compression disrupts the trabecular network and reduces bone mineral density, increasing the risk of collapse
Describe the effects of shear on the microstructure of a long bone
Microcracks: unique arc-shaped microcracks develop within lamella
Cortical sensitivity: shear fatigue is a primary cause of stress fractures, as cortical bone is weaker in shear, making the microstructure highly susceptible to damage
Describe the effects of torsion on the microstructure of a long bone
Lamellar interface failure: shear damage is caused
Osteon rearrangement: rearranged to strengthen the cortex
Mineral-collagen alignment: mineral lamellae arranged around collagen fibres to provide increased resistance
Describe the effects of bending on the microstructure of a long bone
Concave side undergoes compression, convex side undergoes tension
Tensile failure: microcracks may appear in the convex side
Compressive damage: butterfly fragments may form from the concave side
Accumulation of microcracks within the Haversian system
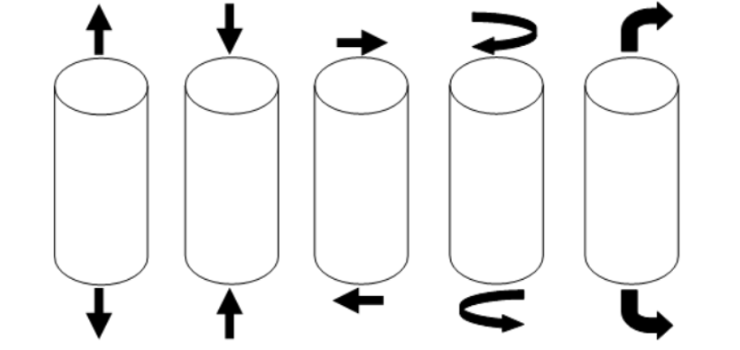
Draw out the following forces acting on a long bone:
Tension
Compression
Shear
Torsion
Bending
Relate biomechanical strength of a typical long bone to the diaphysis structure
Primarily composed of cortical bone, the diaphysis is a hollow cylinder
Highly effective at resisting torsion and bending forces, because mass is distributed away from the neutral axis
Relate biomechanical strength of a typical long bone to the epiphysis structure
Filled with cancellous bone, capped with a thin layer of cortical bone
This allows for the distribution of loads over a larger area at the joints, absorbing energy and transmitting stresses towards the dense cortex
Relate biomechanical strength of a typical long bone to the medullary cavity structure
The hollow center decreases the overall mass, making the bone light, while the cortical shell provides the necessary strength
Describe how bone is flexible
Bone is composed of 70% calcium phosphate, which provides strength, and 30% collagen, which provides flexibility
Describe how bone is malleable
Baby and children's bones are highly malleable due to a higher percentage of collagen and a lower density of minerals compared to adult bones
Explain how bone fatigue may occur
Cumulative microdamage
Repeated loading can create microcracks, especially in high-load areas such as the fetlock or tibia
Muscle fatigue
Reduces muscle ability to reduce shock- causing higher stresses to be transferred directly to the bones
Training intensity
Sudden increases in training speed/duration without adequate recovery time
Hard surfaces
Training on/using hard surfaces can accelerate the fatigue process
Return from breaks
Abrupt increases in work following a period of rest (when bones may have deconditioned), can trigger sudden onset fatigue injuries
Predict the different types of fractures that result from different biomechanical forces
Tension: generally forms small, hairline fractures (stress fractures)
Compression: wedge, crust, burst fractures
Shear: oblique/diagonal fractures
Torsion/rotation: spiral fractures
Bending: oblique/transverse fractures
Outline the stages of bone remodelling
Activation: osteoclast precursors are recruited to the bone surface
Resorption: osteoclasts digest old or damaged mineralized bone
Reversal: mononuclear cells prepare the surface for new bone formation
Formation: osteoblasts fill the cavity with new matrix (osteoid)
What is bone remodelling, and why is it necessary?
A continuous, lifelong process- where mature tissue is removed (resorption), and new bone tissue is formed (ossification)
This maintains skeletal strength, repairs microdamage and regulates calcium balance
Explain Wolff’s Law
States that healthy human bones adapt to the loads under which they are placed, remodeling themselves over time to:
Become stronger when subjected to increased stress
Become weaker when disused
“Form follows function”
Which types of factor lead to bone remodelling and adaptation?
Mechanical factors
Hormonal factors
Lifestyle factors
Describe which mechanical factors can lead to bone remodelling and adaptation
Increased loading (physical activity)
Decreased loading (immobilisation/disease)
Microdamage repair
Shear stress/strain
Describe which hormonal factors can lead to bone remodelling and adaptation
Estrogen/testosterone promote growth and maintenance
PTH released when calcium levels drop to stimulate osteoclasts and release calcium
Calcitriol is crucial for maintaining calcium levels
Growth hormone/IGFs stimulate osteoblast proliferation and bone growth
Describe which lifestyle factors can lead to bone remodelling and adaptation
Chronic diseases create inflammatory environments, stimulating osteoclast activity
Smoking and alcohol inhibit osteoblast activity and promote bone loss
Ageing leads to decreased number of osteoblasts
Insufficient calcium/vitamin D intake increases PTH, resulting in bone loss
Describe the balance between bone resorption and deposition
Resorption: osteoclasts
These break down the bone matrix, releasing minerals (like calcium) into the bloodstream
Deposition: osteoblasts
These produce new bone matrix (collagen and mineral) to replace removed tissue
If this balance is disturbed, it can cause conditions such as osteoporosis (high resorption), or osteopetrosis (high formation)