MCB exam unit 3
1/376
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
377 Terms
In table 18.1 who is most likely protected from the disease, as observed by the test results over time
Patient D
The rise in herd immunity against a population can be directly attributed to
-vaccinations
-increased use of antibiotics
-antibiotic-resistant microorganisms
-none of the answers is correct
-improved handwashing
vaccinations
which of the following is NOT a verified exception in the use of Koch's postulates
some pathogens can cause several disease conditions
some diseases have poorly defined etiologies
some human diseases have no other known animal host
some diseases are not caused by microbes
some diseases are noncommunicable
some diseases are noncommunicable
In table 18.1, who showed seroconversion during these observations?
Patient B
Patient A
Patient C
Patient D
Patient A
The most frequently used portal of entry for pathogens is the
-mucous membranes of the respiratory tract
-skin
-mucous membranes of the gastrointestinal tract
-all of these portals equally
-parenteral route
mucous membranes of the respiratory tract
Which of the following are NOT lymphocytes?
helper T cells
NK cells
cytotoxic T cells
B cells
M cells
M cells
Commensalism is best described as a(n)
- relationship in which a microorganism causes disease
- source of contamination
- relationship between two organisms where both members benefit
- relationship between two organisms where only one member benefits and the other is unharmed
- unsuccessful invasion due to the presence of preexisting microbes
relationship between two organisms where only one member benefits and the other is unharmed
Biological transmission differs from mechanical transmission in that biological transmission
-involves fomites
-involves reproduction of a pathogen in an arthropod vector prior to transmission
-works only with noncommunicable diseases
-requires direct contact
-occurs when a pathogen is carried on the feet of an insect
involves reproduction of a pathogen in an arthropod vector prior to transmission
A reservoir is
- any microorganism that causes disease
- an environment that is free of microbes
- a source of microbial contamination
- a condition in which organisms remain in the body for a short time
- a source of microbes for laboratory testing
a source of microbial contamination
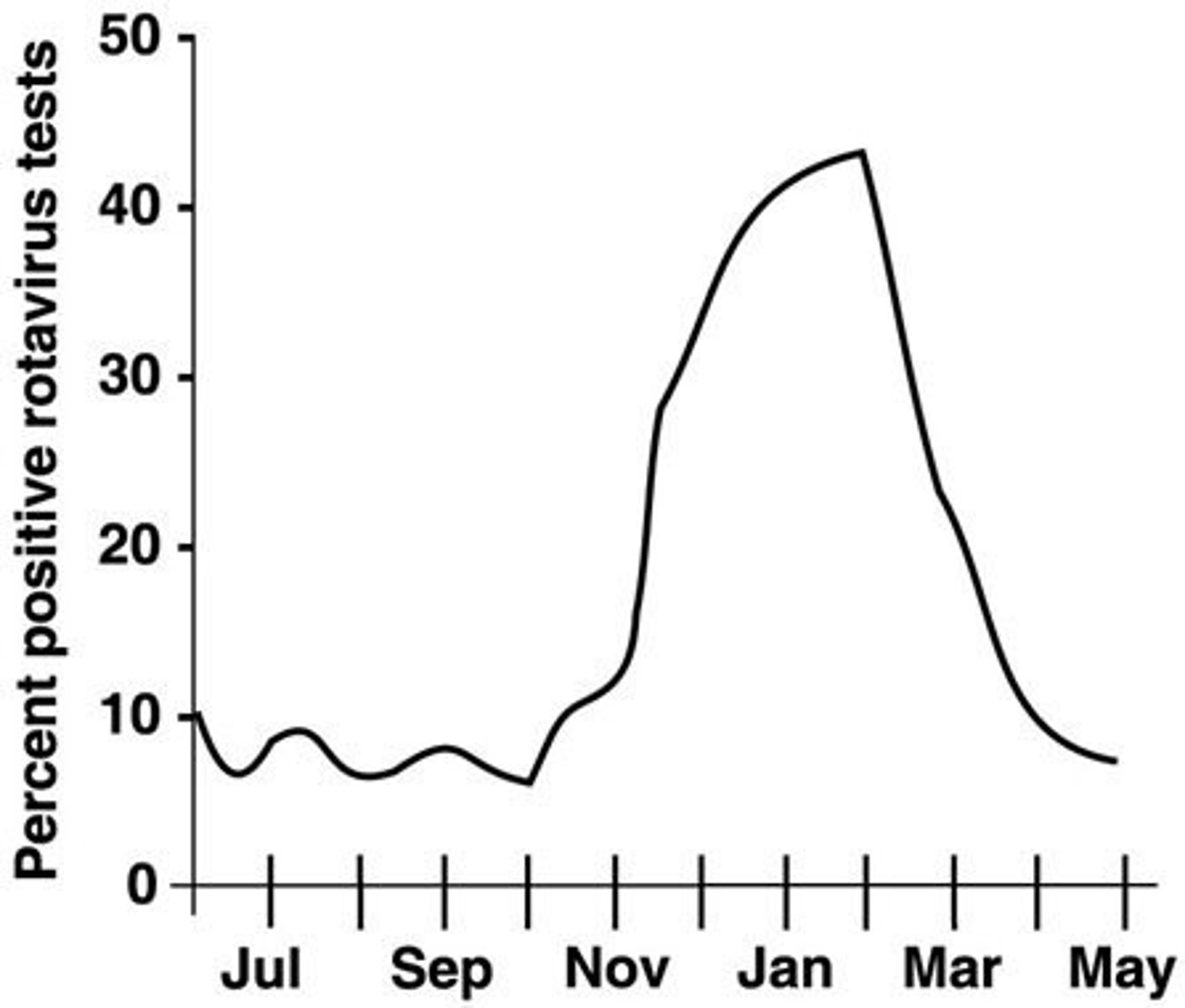
In Figure 14.2, which one of the following choices has the highest morbidity rate?
- July
- December
- October
- November
December
The ID50 is
- the dose that will cause an infection in 50 perfect of the test population
- the dose that will kill 50 percent of the test population
- a measure of pathogenicity
- the dose that will kill some of the test population
- the dose that will cause an infection in some of the test population
the dose that will cause an infection in 50 percent of the test population
All of the following are examples of entry via the parenteral route EXCEPT
-injection
-surgery
-hair follicle
-skin cut
-bite
hair follicle
The function of the "ciliary escalator" is to
- propel inhaled dust and microorganisms away from the mouth, toward the lower respiratory tract.
- remove microorganisms from the lower respiratory tract.
- remove microorganisms from the gastrointestinal tract.
- trap microorganisms in mucus in the upper respiratory tract.
- trap inhaled dust and microorganisms in mucus and propel it away from the lower respiratory tract.
trap inhaled dust and microorganisms in mucus and propel it away from the lower respiratory tract.
Which of the following is the best definition of "microbial antagonism"?
- the ability of microbiota to mutate into pathogens
- the presence of normal microbiota that can become pathogens under certain conditions
- the presence of pathogens on the surface of the skin, which will invade the body through abrasions
- the presence of normal microbiota that protect the body by competing with pathogens in a variety of ways to prevent pathogens from invading the body
- the presence of resident bacteria on the surface of the body and in cavities that connect to the surface
the presence of normal microbiota that protect the body by competing with pathogens in a variety of ways to prevent pathogens from invading the body
Which of the following cells increase in number during an infection with parasitic worms?
-basophils
-neutrophils
-lymphocytes
-macrophages
-eosinophils
eosinophils
Innate immunity
-is slower than adaptive immunity in responding to pathogens
-involves a memory component
-is nonspecific and present at birth
-provides increased susceptibility to disease
-involves T cells and B cells
is nonspecific and present at birth
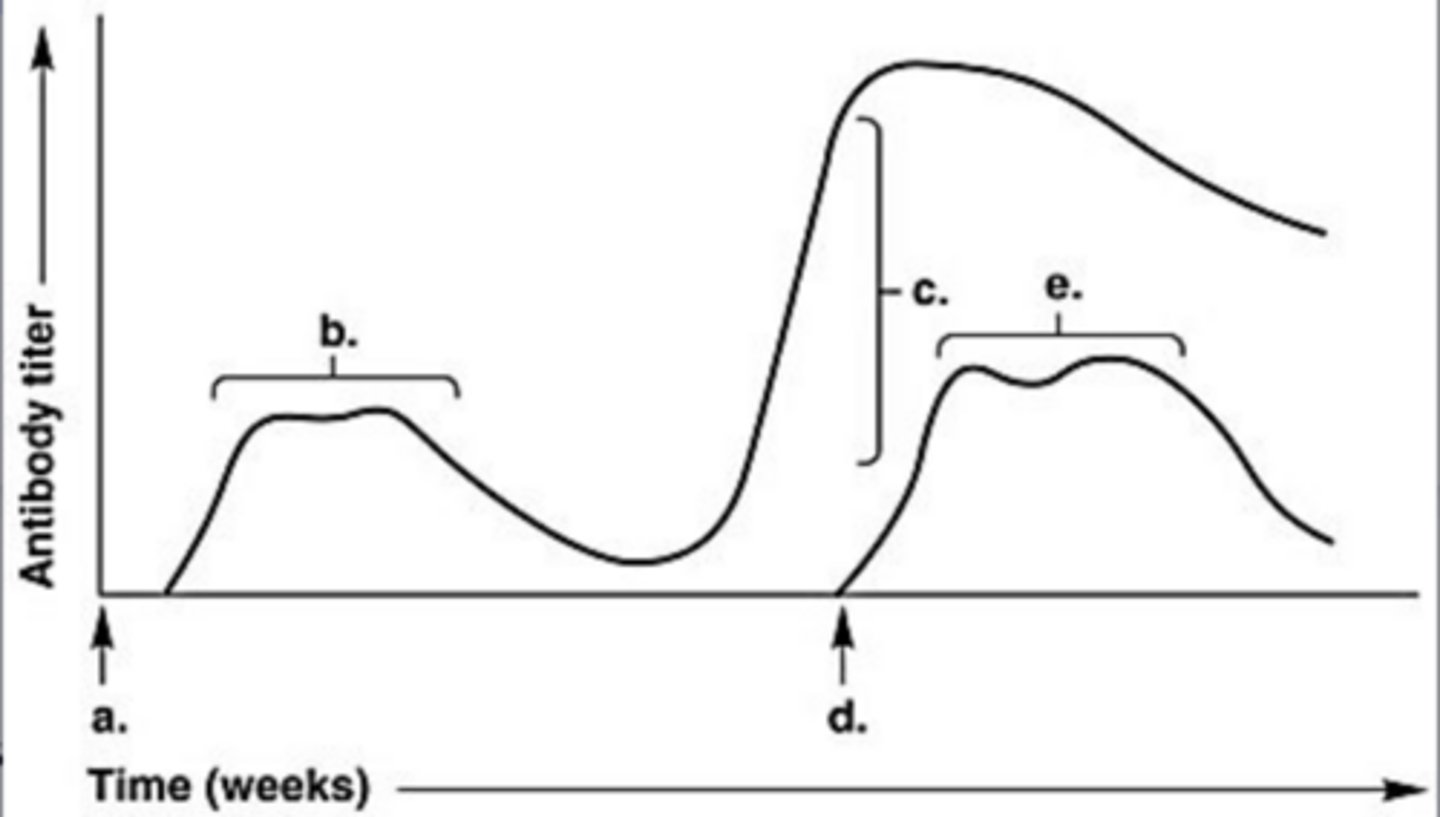
In Figure 17.1, which letter on the graph indicates the highest antibody titer during the patient's response to a second and distinct/different antigen?
- c
- a
- d
- b
- e
e
The antibodies that typically bind to large parasites are
- IgM
- IgE
- IgA
- IgD
- IgG
IgE
Which of the following is NOT a characteristic of B cells?
-they recognize antigens associated with MHC I
-they are responsible for the memory response
-they originate in bone marrow
-they have antibodies on their surfaces
-they are responsible for antibody formation
they recognize antigens associated with MHC I
Large antibodies that agglutinate antigens are
- IgG
- IgM
- IgA
- IgE
- IgD
IgM
Which of the following statements regarding ELISAs is TRUE?
- they require large amounts of serum
- they can be used to detect antibody or antigen
- they involve the use of membrane filters
- they are not quantitative
- the antibody label is a fluorescent molecule
they can be used to detect antibody or antigen
The bacterium Staphylococcus aureus is commonly found in the nasal cavity of healthy people. If inhaled into the lungs, however, it may cause pneumonia. Staphylococcus aureus is best described as
• a parasite.
• a mutualist symbionc partner.
• both resident microbiota and opportunistic pathogen.
• resident microbiota.
• transient microbiota.
both resident microbiota and opportunistic pathogen.
A person is exposed to rotten wood with fungal growth and develops blastomycosis. No one taking care of him/her becomes ill.
Blastomycosis is an example of a ......__ disease.
- subacute
- noncommunicable
- latent
- chronic
- contagious
noncommunicable
Symptoms of intense inflammation and shock occur in some gram-positive bacterial infections due to
- erythrogenic toxin.
- membrane-disrupting toxins.
- A-B toxins.
- superantigens.
- lipid A.
superantigens
Superantigens produce intense immune responses by stimulating lymphocytes to produce
- exotoxins.
- leukocidins.
- interferons.
- cytokines.
- endotoxins.
cytokines
A pathogen is best described as
- a source of microbial contamination.
- a microorganism that remains with the person throughout life.
- any microorganism that causes disease.
- an organism that remains in the body for a short time.
-a microorganism that may cause a disease under certain circumstances.
- any microorganism that causes disease.
Which of the following is an effect of opsonization?
- cytolysis
- increased margination of phagocytes
- increased diapedesis of phagocytes
-increased adherence of phagocytes to microorganisms
- inflammation
increased adherence of phagocytes to microorganisms
Macrophages arise from which of the following?
-eosinophils
-monocytes
-neutrophils
-basophils
-lymphocytes
monocytes
A vaccine against HIV proteins made by a genetically-engineered vaccinia virus that has infected a eukaryotic cell line is a(n)
• conjugated vaccine.
• toxoid vaccine.
• inactivated whole-agent vaccine.
• nucleic acid vaccine.
• subunit vaccine
subunit vaccine
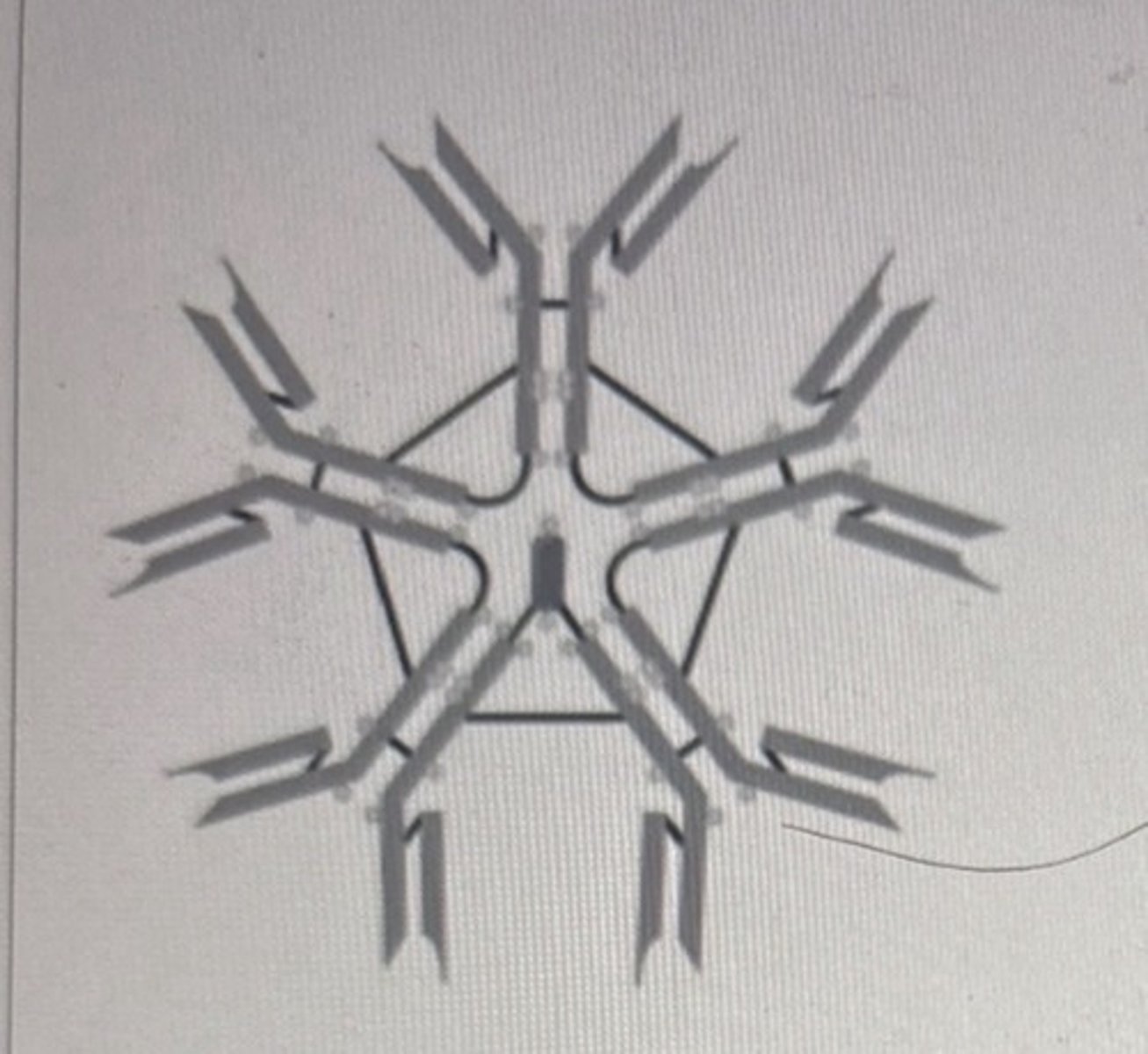
The type of immunoglobulin illustrated in Figure 16.1 is
- IgE.
- lgA.
• IgG.
• IgD.
• IgM.
IgM
What is the result when a dendritic cell phagocytizes a microbe and processes it?
• display of epitope-MHC I complexes on the surface of the cell
- suppression of the immune response to the microbe
• display of microbial epitope-MHC II complexes on the cell surface
- activation of the dendritic cell to become a plasma cell
- display of microbial fragments with CD8 glycoproteins
display of microbial epitope-MHC II complexes on the cell surface
What antibacterial chemical is present in tear fluid?
-interferon
-complement
-lysozyme
-antibodies
-defensins
lysozyme
Which of the following best describes IgM antibodies?
* They are the most common type of antibody in the blood during the initial stages of an immune response.
• They can cross the placenta to provide passive immunity.
• They are the antibody class found in body secretions.
• They interact with phagocytes and NK cells.
• They cause basophils and eosinophits to degranulate.
They are the most common type of antibody in the blood during the initial stages of an immune response.
The antimicrobial effects of AMPs include all of the following EXCEPT
-inhibition of phagocytosis.
-lysis of bacterial cells.
-inhibition of cell wall synthesis.
-destruction of nucleic acids.
-pore formation in bacterial membranes.
inhibition of phagocytosis.
The condition known as microbial antagonism may be defined as
a) an unsuccessful microbial invasion due to the presence of preexisting microbes
b) a relationship between two organisms where one member harms the other
c) a relationship between two organisms where both members benefit
d) a relationship between two organisms where only one member benefits
e) microorganisms that remain with a person throughout life
a) an unsuccessful microbial invasion due to the presence of preexisting microbes
Which of the following statements about healthcare-associated infections is FALSE
a) they may be caused by normal microbiota
b) they may be caused by drug-resistant bacteria
c) they may be caused by opportunists
d) the patient was infected before hospitalizatione) they occur in compromised patients
d) the patient was infected before hospitalization
The ability of some microbes, such as Trypanosoma or Giardia alter their surface molecules and evade destruction by the host's antibodies is called
-lysogenic conversion
-cytopathic effect
-antigenic variation
-virulence
-cytocidal effect
-antigenic variation
Endotoxins are
a) A-B toxins
b) associated with gram positive bacteria
c) molecules that bind nerve cells
d) part of the gram negative cell wall
e) excreted from the cells
d) part of the gram negative cell wall
The lectin pathway for complement action is initiated by
-lectins of the microbe
-mannose on the surface of microbes
-gram-negative cell walls
-gram-positive cell walls
-mannose on host membranes
mannose on the surface of microbes
TLRs attach to all of the following EXECPT
-AMPs
-PAMPs
-LPS
-peptidoglycan
-flagellin
-AMPs
Which of the following leukocytes are called "agranulocytes" because of the absence of granules in their cytoplasm revealed by basic or acid dyes
a) eosinophils
b) both basophils and eosinophils
c) neutrophils
d) basophils
e) lymphocytes
e) lymphocytes
Lysozyme and the antibiotic penicillin have similar mechanisms of action in that they both cause damage to the bacterial
a) ribosomes
b) DNA
c) cell wall
d) cell membrane
e) capsule
c) cell wall
What type of immunity results from vaccination
a) artificially acquired active immunity
b) artificially acquired passive immunity
c) naturally acquired active immunity
d) naturally acquired passive immunitye) innate immunity
a) artificially acquired active immunity
The importance of M cells concerns
-ability to migrate along the intestinal tract
-having microvilli to facilitate antigen capture
-facilitation of contact between antigens in the intestinal tract and the immune system
-presentation of epitopes in MHC II molecules
-preventing damage to adaptive immune system cells
facilitation of contact between antigens in the intestinal tract and the immune system
Cytokines released by Th1 cells
a) convert B cells to T cells
b) directly kill parasites
c) activate CD8+ cells to CTLs
d) convert Th2 cells to Th1 cells
e) convert Th1 cells to Th2 cells
c) activate CD8+ cells to CTLs
ADCC is a process that is most effective in destroying
a) extracellular viruses
b) bacterial pathogens
c) prionsd) eukaryotic pathogens
e) bacterial toxins
d) eukaryotic pathogens
The most prevalent antibody class in the blood is
a) IgD
b) IgM
c) lgE
d) IgA
e) IgG
e) IgG
Isolated and purified hepatitis B virus surface antigen can be used in a
a) subunit vaccine
b) attenuated whole-agent vaccine
c) conjugated vaccine
d) inactivated whole-agent vaccine
e) toxiod vaccine
a) subunit vaccine
A patient shows the presence of antibodies against diphtheria toxin. Which of the following statements is FALSE
a) the patient may have the disease
b) the patient was near someone who had the disease
c) the patient may have been vaccinated
d) a recent transfusion may have passively introduced the antibodies
e) the patient may have had the disease and has recovered
b) the patient was near someone who had the disease
fomites are
inanimate objects involved in the indirect contact transmission of pathogens
During a six-month period, 239 cases of pneumonia occurred in a town of 300 people. A clinical case was defined as fever 39°C lasting >2 days with three or more symptoms (i.e., chills, sweats, severe headache, cough, aching muscles/joints, fatigue, or feeling ill). A laboratory-confirmed case was defined as a positive result for antibodies against Coxiella burnetii. Before the outbreak, 2000 sheep were kept northwest of the town. Of the 20 sheep tested from the flock, 15 were positive for C. burnetii antibodies. Wind blew from the northwest, and rainfall was 0.5 cm compared with 7 to 10 cm during each of the previous three years.
The method of transmission of the disease in situation 14.1 was
vehicle
The condition called parasitism is characterized as a(n)
relationship between two organisms where one member harms the other
Patients developed inflammation a few hours following eye surgery. Instruments and solutions were sterile, and the Limulus assay was positive. the patient's inflammation was due to
endotoxin
Cytopathic effects are changes in host cells due to
viral infections
all of the following are iron-binding proteins in humans EXCEPT
a. transferrin
b. lactoferrin
c. ferritin
d. hemoglobin
e. siderophorin
siderophorin
Which of the following statements is TRUE?
-complement increases after immunization
-all of the complement proteins are constantly active in serum
-factors B, D, and P cause cytolysis
-there are at least thirty complement proteins
-complement activity is antigen specific
there are at least thirty complement proteins
Microbial molecules detected by phagocytes are called
PAMPs
Which cell becomes a macrophage when leaving the bloodstream?
monocyte
which of the following is the best definition of epitope
a. specific regions on antigens that interact with perforins
b. specific regions on antigens that interact with antibodies
c. specific regions on antigens that interact with haptens
d. specific regions on antigens that interact with T cell receptors
e. specific regions on antigens that interact with MHC class molecules
specific regions on antigens that interact with antibodies
which of the following statements about T lymphocytes is FALSE
a. T lymphocytes directly attack cells and produce the cell-mediated response
b. there are three types of T lymphocytes
c. T lymphocyte has TCRs that recognize antigen only if it is bound to MHC
d. T lymphocytes produce antibody molecules
e. T lymphocytes are called such because they mature in the thymus
T lymphocytes produce antibody molecules
Class II MHC are found on
professional antigen presenting cells
the specificity of an antibody is due to
the variable portions of the H and L chains
which of the following bacterial components would most likely result in B cell stimulation by T-independent antigen
capsule
which of the following is NOT an advantage of live attenuated vaccine agents?
a. the elicit lifelong immunity
b. they require few or no boosted immunization
c. they stimulate by cel-mediated and humoral immune response
d. the immune response generated by the vaccine closely mimics a real infection
e. they occasionally revert to virulent forms
they occasionally revert to virulent forms
which of the following statements regarding ELISAs is TRUE
a. they can be used to detect antibody or antigen
b. they involve the use of membrane filters
c. they require large amounts of serum
d. the antibody label is a fluorescent molecule
e. they are nor quantitative
they can be used to detect antibody or antigen
A healthcare-associated infection (traditionally known as a nosocomial infection) is
-always caused by medical personnel
-acquired during the course of hospitalization
-always caused by pathogenic bacteria
-always present, but is inapparent at the time of hospitalization
-only a result of surgery
Acquired during the course of hospitalization
Which of the following is the CORRECT sequence of a disease process?
-prodromal period, convalescence, incubation, illness, decline
-convalescence, incubation, prodromal period, illness, decline
-incubation, convalescence, prodromal period, illness, decline
-incubation, prodromal period, illness, decline, convalescence
-illness, convalescence, incubation, prodromal period, decline
incubation, prodromal period, illness, decline, convalescence
Lysogenic bacteriophages contribute to bacterial virulence because
-bacteriophages
-kill human cells
-give new gene sequences to the host bacteria
-kill the bacteria, causing release of endotoxins
-carry plasmids
-produce toxins
Give new gene sequences to the host bacteria
Endotoxins are
-molecules that bind nerve cells
-associated with gram-positive bacteria
-part of the gram-negative cell wall
-A-B toxinsexcreted from the cell
Part of the gram-negative cell wall
Activation of C3a results in
-increased blood vessel permeability
-cell lysis
-acute inflammation
-opsonization
-attraction of phagocytes
acute inflammation
Which of the following statements is TRUE?
-Beta interferon attacks invading viruses
-Alpha interferon promotes phagocytosis
-Alpha interferon acts against specific viruses
-All three types of interferons have the same effect on the body
-Gamma interferon causes bactericidal activity by macrophages
Gamma interferon causes bactericidal activity by macrophages
Which of the following is the best definition of antigen?
-a protein that combines with antibodies
-a chemical that combines with antibodies something foreign in the body
-a pathogen
-a chemical that elicits an antibody response and can combine with these antibodies
A chemical that elicits an antibody response and can combine with these antibodies
Which of the following cells is NOT an APC?
-dentritic cells
-mature B cells
-None of the answers is correct; all of these are APCs
-natural killer cells
-macrophages
Natural killer cells
The antibodies found in mucus, saliva, and tears are
-IgG
-IgD
-IgE
-IgM
-IgA
IgA
Which of the following destroys virus-infected cells?
-TH
-CTL
-B cells
-Treg
-dendritic cells
CTL
Which of the following statements about natural killer cells is FALSE?
-They are stimulated by an antigen
-They destroy virus-infected cells
-They destroy cells lacking MHC I
-They destroy tumor cells
-None of the answers are correct; all of these statements are true
They are stimulated by an antigen
A reaction between antibody and particulate antigen is called a(n)
-neutralization reaction
-complement fixation
-precipitation reaction
-agglutination reaction
-immunofluorescence
Agglutination reaction
Dead Bordetella pertussis can be used in a(n)
-inactivated whole-agent vaccine
-subunit vaccine
-attenuated whole-agent vaccine
-toxoid vaccine
-conjugated vaccine
Inactivated whole-agent vaccine
Symptoms of disease differ from signs of disease in that symptoms
always occur as part of a syndrome.
are changes observed by the physician.
are changes felt by the patient.
are specific for a particular disease.
are changes felt by the patient.
If a prodromal period exists for a certain disease, it should occur right prior to
-convalescence.
-decline.
-incubation.
-illness.
illness
Table 15.2
Which organism in Table 15.2 most easily causes an infection?
Shigella
Treponema pallidum
The answer cannot be determined based on the information provided.
Legionella pneumophila
E. coli 0157:H7
Legionella pneumophila

The ID50 is
the dose that will cause an infection in some of the test population.
the dose that will cause an infection in 50 percent of the test population.
the dose that will kill 50 percent of the test population.
the dose that will kill some of the test population.
a measure of pathogenicity
the dose that will cause an infection in 50 percent of the test population.
The complement protein cascade is the same for the classical pathway, alternative pathway, and lectin pathway after the point in the cascade where the activation of __ takes place.
-C2
-C1
-C5
-C6
-C3
C3
Which of the following is found normally in serum?
-interferon
-histamine
-TLRs
-leukocytosis-promoting factor
-complement
complement
Which of the following are NOT lymphocytes?
helper T cells
NK cells
cytotoxic T cells
M cells
B cells
M cells
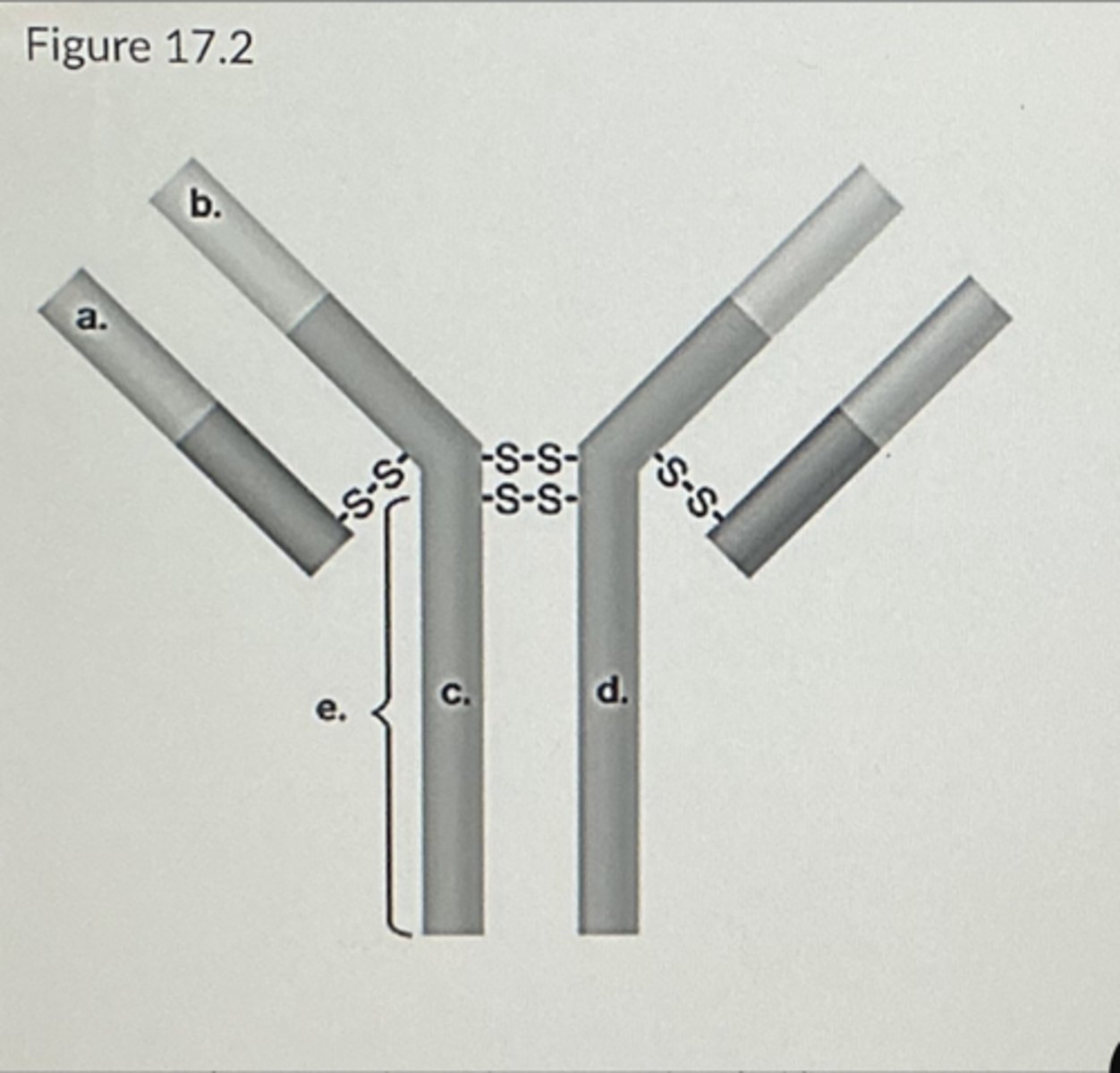
In Figure 17.2, which areas represent antigen-binding sites?
c and d
a and c
a and b
b and c
b and d
a and b
A new virus is discovered that causes cells to lyse. Which of the following types of assay would be useful for diagnosing infection with this virus?
-agglutination
-viral neutralization
-complement fixation test
-both agglutination and complement fixation tests
-viral hemagglutination
viral neutralization
A person exposed to hepatitis A virus may be treated with an injection of antibody molecules. This type of treatment is
immunization.
passive immunotherapy.
adjuvant therapy.
vaccine therapy.
serology
passive immunotherapy
Which of the following definitions is INCORRECT?
• epidemic: a disease that is constantly present across the world
• sporadic: a disease that affects a population occasionally
• pandemic: a disease that affects a large number of people in the world in a short time
O endemic: a disease that is constantly present in a population
• incidence: number of new cases of a disease
epidemic: a disease that is constantly present across the world
Situation 14.1
During a six-month period, 239 cases of pneumonia occurred in a town of 300 people. A clinical case was defined as fever ≥ 39°C lasting >2 days with three or more symptoms (i.e., chills, sweats, severe headache, cough, aching muscles/joints, fatigue, or feeling ill). A laboratory-confirmed case was defined as a positive result for antibodies against Coxiella burnetii. Before the outbreak, 2000 sheep were kept northwest of the town. Of the 20 sheep tested from the flock, 15 were positive for C. burneti antibodies. Wind blew from the northwest, and rainfall was 0.5 cm compared with 7 to 10cm during each of the previous three years.
The method of transmission of the disease in Situation 14.1 was
- indirect contact.
- droplet.
- vehicle.
- vector-borne.
- direct contact.
vehicle
Which of the following patterns of disease does the patient experience no signs or symptoms?
-prodromal
-decline
-convalescence
-incubation
-both incubation and convalescence
incubation
Siderophores are bacterial proteins that compete with the host's
-white blood cells.
-receptors.
-antibodies.
-red blood cells.
-iron-transport proteins
iron transport proteins
The alternative pathway for complement activation is initiated by
-factors released from damaged tissues.
-lipid-carbohydrate complexes and C3.
-factors released from phagocytes.
-antigen-antibody reactions.
-C5-C9.
lipid-carbohydrate complexes and C3.
A Treg cell deficiency could result in
- transplant rejection.
-. autoimmunity.
- increased severity of bacterial infections.
O increased number of bacterial infections.
O increased number of viral infections.
autoimmunity
An ELISA for Hepatitis Chas 95 percent sensitivity and 90 percent specificity. This means that the test
• detects 5 percent of the true positive samples and has 10 percent false positive results.
-. detects 5 percent of the true positive samples and has 90 percent false positivé results.
• detects 95 percent of the true positive samples and has 10 percent false positive results.
O detects 95 percent of the true positive samples and has 90 percent false positive results.
O detects 90 percent of the true positive samples and has 5 percent false positive results.
detects 95 percent of the true positive samples and has 10 percent false positive results.
Transient microbiota differ from normal microbiota in that transient microbiota
are present for a relatively short time.
Situation 14.1During a six-month period, 239 cases of pneumonia occurred in a town of 300 people. A clinical case was defined as fever ≥ 39°C lasting >2 days with three or more symptoms (i.e., chills, sweats, severe headache, cough, aching muscles/joints, fatigue, or feeling ill). A laboratory-confirmed case was defined as a positive result for antibodies against Coxiella burnetii. Before the outbreak, 2000 sheep were kept northwest of the town. Of the 20 sheep tested from the flock, 15 were positive for C. burnetii antibodies. Wind blew from the northwest, and rainfall was 0.5 cm compared with 7 to 10 cm during each of the previous three years.Situation 14.1 is an example of
a zoonosis.
Siderophores are bacterial proteins that compete with the host's
iron-transport proteins.
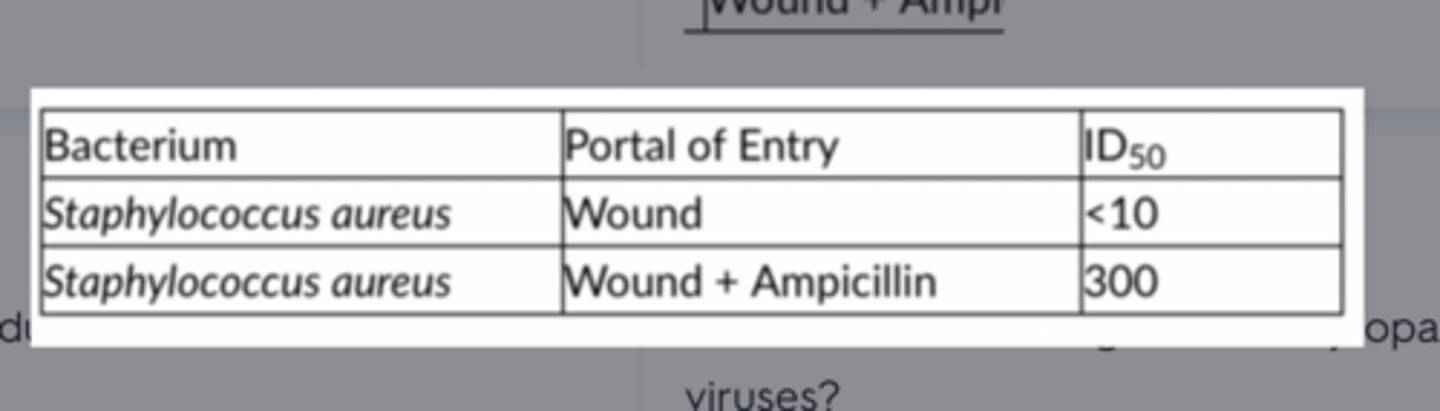
Table 15.1 shows the ID50 for Staphylococcus aureus in wounds with and without the administration of ampicillin before surgery. Based on the data, the administration of ampicillin before surgery
decreases the risk of staphylococcal infection.

Which of the following is NOT a cytopathic effect of viruses?
toxin production