Renal physiology IV - Water and electrolyte balance
1/18
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
19 Terms
water and body fluids
• Water is the solvent of life.
• Microbes, plants and animals are up to 70% water.
Water is the major constituent of:
• Blood.
• Lymphatic fluid.
• Cerebrospinal fluid.
• Aqueous humour.
• Milk and colostrum.
• Saliva.
• Tears.
• Sweat.
• Bile.
• Semen and secretions of sexual accessory glands.
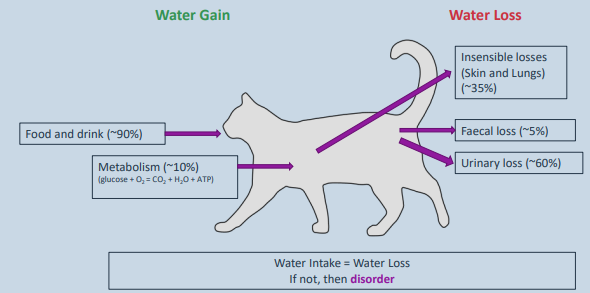
waterbalance
Species differences – dry climate animals have smaller faecal and urinary losses. Some species can derive all the water they need from metabolic water
fluid and electrolyte balance
Electrolytes are minerals in your body that have an electric charge. They are in blood, urine, tissues, and other body fluids. Electrolytes are important because they:
• Balance water.
• Balance acid/base (pH) level.
• Move nutrients into cells.
• Move wastes out of cells.
• Make sure that nerves, muscles, the heart, and the brain function.
Sodium, calcium, potassium, chlorine, phosphate, and magnesium are all electrolytes. Obtained through nutrition.
electrolytes and non electrolytes
• Dissolved compounds dissociate into ions.
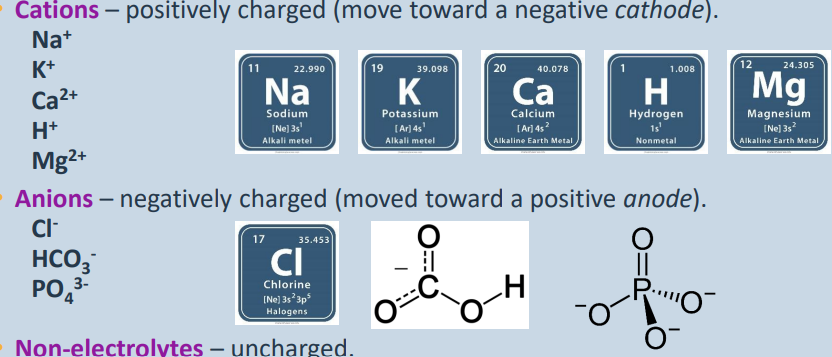
Cations – positively charged (move toward a negative cathode).
Na+
K+
Ca2+
H+
Mg2+
Anions – negatively charged (moved toward a positive anode).
ClHCO3-
PO43-
Non-electrolytes – uncharged.
Urea
Glucose
Amino acids (some)
disturbances to water and electrolyte balance
Electrolyte levels can change (too low or too high) when the amount of water changes (dehydration or overhydration).
• Causes include:
• Drugs.
• Vomiting.
• Diarrhoea.
• Sweating.
• Renal problems.
Water disturbance.
• ↑water volume i.e. oedema.
• ↓water volume i.e. dehydration.
Electrolyte disturbances.
• Hypo/hypernatraemia (disturbances in blood Na+).
• Hypo/hyperkalaemia (disturbances in blood K+).
• Hypo/hypercalcaemia (disturbances in blood Ca2+).
• Hypo/hyperchloraemia (disturbances in blood Cl-).
• Etc.
physiological fluid “compartments”
Three major compartments:
• Intracellular Fluid (ICF).
• Interstitial Fluid (Part of ECF).
• Plasma Fluid (Part of ECF).
Intracellular Fluid – fluid within all the cells of the body.
• Separated by plasma membrane.
• Permeable to water (via aquaporins).
• Impermeable to ions (except by specific channels and pumps).
• Impermeable to proteins.
Interstitial Fluid (ISF) or tissue fluid is a solution that bathes and surrounds the cells of multicellular animals.
• It is the main component of the extracellular fluid (ECF), which also includes plasma and transcellular fluid.
Plasma Fluid – main constituent of blood.
• Separated by capillary walls.
• Permeable to all but large proteins
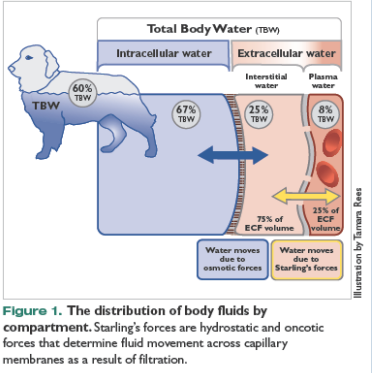
physiological fluid “compartments” cont.
• The ICF lies within cells and is the principal component of the cytosol/cytoplasm. The ICF makes up about 60% of the total body water.
The ECF accounts for the other 40% of the total body water.
• Approximately 20% of the ECF is plasma.
• Approximately 75% of the ECF is interstitial fluid (ISF/IF).
• Approximately 5% of the ECF is “other” fluid or transcellular fluid.
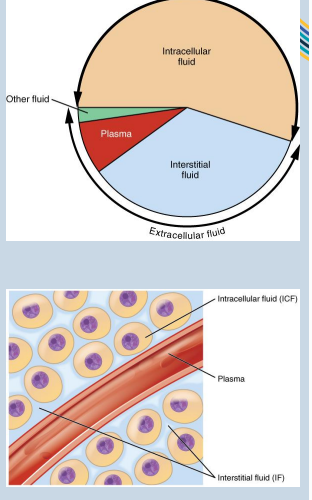
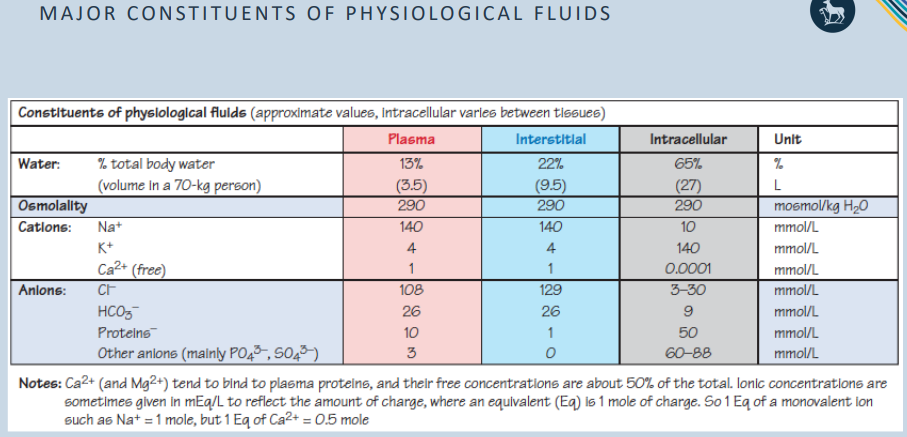
fluidmovement between ecf compartments
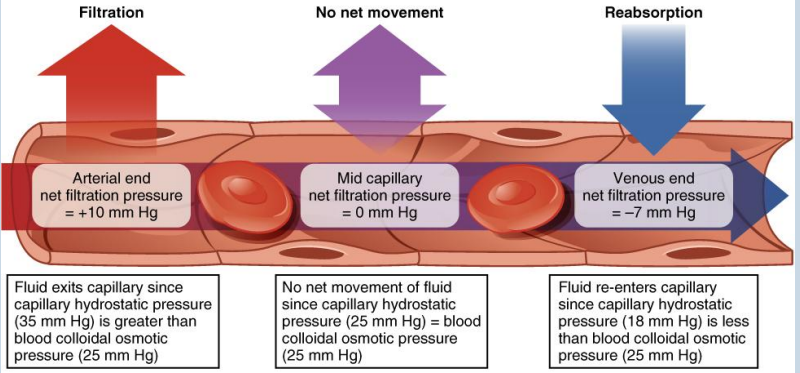
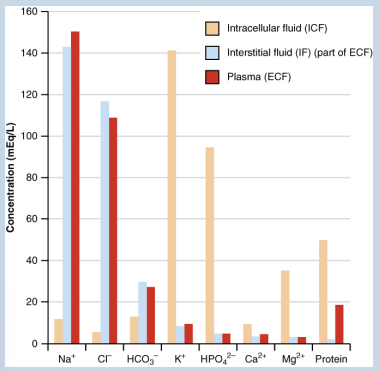
electrolytes in fluid compartments
• The compositions of the two components of the ECF - plasma and ISF - are more similar to each other than either is to the ICF
• Blood plasma has high concentrations of sodium, chloride, bicarbonate, and protein
• The ISF has high concentrations of sodium, chloride, and bicarbonate, but a relatively lower concentration of protein
• The ICF has elevated amounts of potassium, phosphate, magnesium, and protein
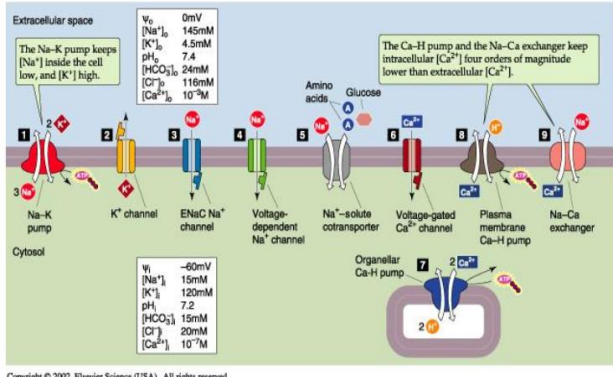
major transport systems involved in electrolyte balance
1. Na+/K+ ATPase.
2. K+ channel.
3. Epithelial Na+ channel.
4. Voltage-dependent Na+ channel.
5. Na+ -solute co-transporter.
6. Voltage-gated Ca2+ channel.
7. Organellar Ca2+/H+ pump.
8. Plasma-membrane Ca2+/H+ pump.
9. Na+/Ca2+ exchanger.
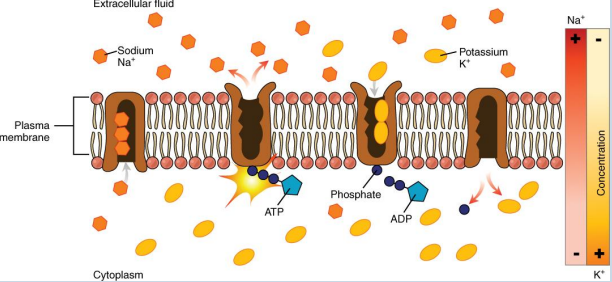
Na+/K+ pump
• Powered by ATP to transfer Na+ out of the cytoplasm and into the ECF.
• The pump also transfers K+ into the cytoplasm.
• For every ATP molecule that the pump uses, three Na+ are exported, and two K+ are imported.
• Net export of a single positive charge per pump cycle.
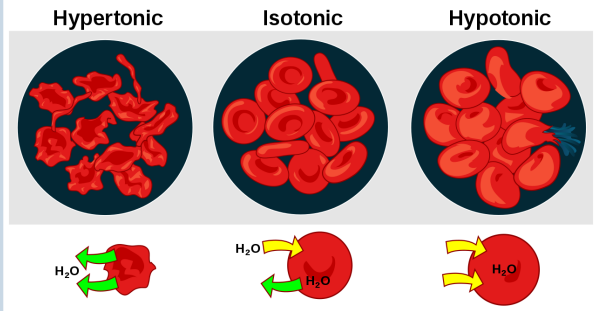
water transport - effects of hypotonicity and hypertonicity on cell volume
Hypertonic solution:
• Higher solute content than ICF.
• Water moves out of cells and cells shrivel (crenated)
Isotonic solution:
• Balanced solute content to ICF.
• Free movement of water in balance
Hypotonic solution:
• Lower solute content than ICF.
• Water moves into cells and cells swell or lyse.
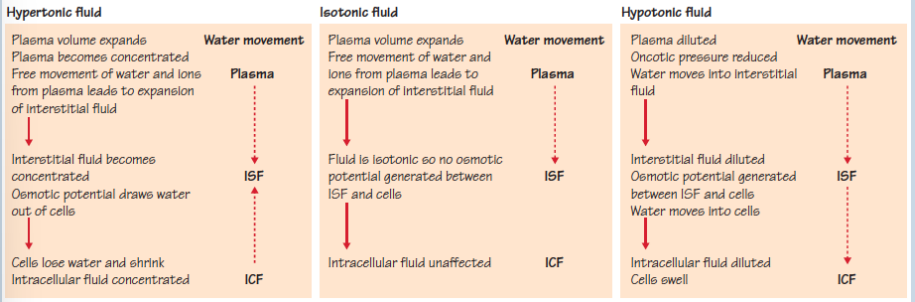
effects of ingesting fluids of differing osmotic potential
Carrie, a 16 year-old FN Birman cat is dull and anorexic. Skin
turgor is reduced, and mucous membranes are tacky. You
estimate 5-10% dehydration. What fluids would you like to give
and how?
Questions:
• Crystalloid or Colloid?
• Crystalloids contain small solutes (<500 Da).
• Colloids contain large solutes (>10 kDa).
Crystalloid – need to replace lost water and lost electrolytes.
Like with like.
• When might you give a colloid?
Large solutes remain in vascular compartment to hold more fluid there so useful when plasma volume reduced such as haemorrhage.
Questions:
• Isotonic, hypotonic or hypertonic?
Isotonic – need to replace lost fluid and solutes without
overloading ICF with fluid (hypotonic) or drawing fluid from
ICF (hypertonic).
• When might you give each type?
Hypotonic not very useful clinically as rarely have fluid loss
without electrolyte loss as well. Hypertonic can function like
colloid but only short-term as fluid will be lost from ICF as a
result. Animal can replace ICF with long-term drinking so
sometimes used in large animals
What routes could you give fluids?
Orally, subcutaneous and IV.
• How much fluid?
Calculate fluid deficit, calculate maintenance requirements
and add together. Determine safe rate to administer (this will
be covered in later years).
Like with like.
Volume with volume.
Rate with rate
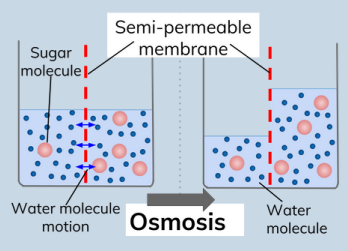
how does water move across membranes lawl
• Osmosis – key point is semi-permeable membrane.
• Cell membrane acts as a barrier to most molecules.
• Specialised channels and transporters facilitate movement
across the membrane.
• Therefore, cell membranes are semi-permeable.
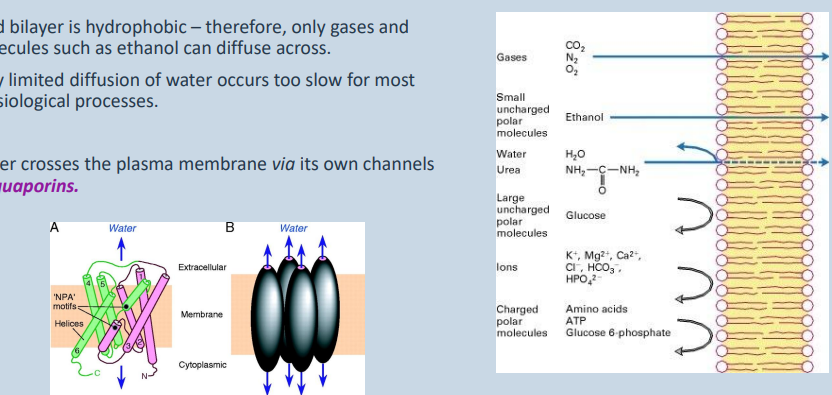
• Lipid bilayer is hydrophobic – therefore, only gases and molecules such as ethanol can diffuse across.
• Only limited diffusion of water occurs too slow for most physiological processes.
• Water crosses the plasma membrane via its own channels – aquaporins.
regulation of renal Na+ and water reabsorption
Three hormone systems play an important role in the regulation of extracellular fluid volume and osmolarity through their actions on renal reabsorption of Na+ and water.
• Antidiuretic hormone (ADH).
• The renin-angiotensin-aldosterone system.
• Atrial natriuretic hormone
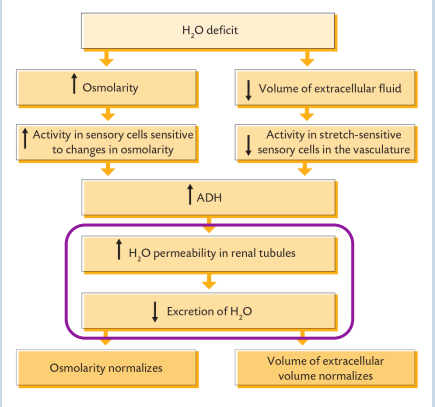
water balance - renal control
• The kidney plays an important role in adjusting water
reabsorption.
• When water losses from the body result in a decrease
in ECF volume and increase in osmolarity –
hypothalamus responds.
• Anti-diuretic hormone (ADH) produced in neurons of
hypothalamus.
• ADH released from posterior pituitary.
• ADH binds to ADH receptors in distal convoluted
tubule and collecting duct epithelial cells.
• ADH receptor is G-protein coupled, activates cAMP
which activates protein kinase A.
• Results in insertion of aquaporin 2 channels into apical
membrane of tubular epithelial cells.
• More water reabsorption in the distal renal tubular
system
electrolyte balance - renal control
• The kidney also plays an important role in adjusting the balance of electrolytes.
• Reduced Na+ and reduced blood volume/pressure detected in juxtaglomerular apparatus (JGA).
• JGA granular cells secrete renin.
• Renin converts angiotensinogen to angiotensin I.
• Pulmonary capillary endothelial cells convert angiotensin I to angiotensin II via angiotensin converting enzyme (ACE).
• Angiotensin II has many effects, one of which is to stimulate aldosterone production from the zona glomerulosa of the adrenal gland.
• Aldosterone binds to mineralocorticoid nuclear receptor to increase transcription of new Na+ and K+ channels and new Na+/K+ ATPase pumps.
• Increases Na+ reabsorption and K+ secretion.
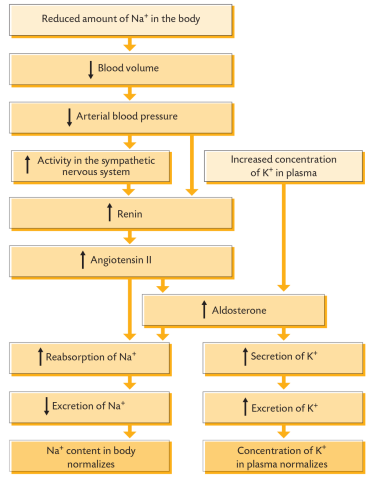
electrolyte balance - renal control
Atrial natriuretic peptide (ANP) produced by atrial wall cardiomyocytes in response to atrial stretch.
• Brain natriuretic peptide (BNP) produced by some CNS neurons and ventricular cardiomyocytes in response to higher BP or blood volume.
• Urodilatin produced in distal tubular epithelial cells.
• Act to dilate afferent arterioles increasing GFR.
• Suppress reabsorption of Na+ in distal tubular cells.
• Antagonistic to aldosterone.