Unit 3.7- Homeostasis and the kidney
1/125
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
126 Terms
Define homeostasis
The mechanism by which a constant internal environment is achieved within a living organism
Why is the regulation of the internal environment important?
Regulate temperature and pH- denaturing of enzymes
Water potential of blood- too dilute leads to cells bursting, too concentrated leads to cells shrinking
What does homeostasis prevent?
Large fluctuations around a set point- the body is kept in dynamic equilibrium
What do homeostatic control systems involve?
A negative feedback system
Define negative feedback
When a displacement from a set point results in corrective mechanisms that reduce the displacement
Explain the negative feedback system that controls the glucose conc in the plasma
Too high:
Pancreas detects
Releases insulin
Increases uptake of glucose into cells
Glucose converted into glycogen store
too low:
Pancreas detects
Releases glucagon
Increases conversion of glycogen back into glucose
Glucose released back into blood
Neg feedback system that controls core body temp?
Temp too high:
-thermoregulatory system in brain detects blood temp
-arteries to skin capillaries dilate so more heat is lost from skin
-increased sweating- high latent heat of water so evaporating causes cooling as thermal energy used
Temp too low:
Thermoregulatory centre in brain detects blood temp
Vasoconstriction so less heat lost from skin
Increased shivering- involuntary contraction of muscles under skin-> ATP produced-> heat produced as product
What is positive feedback?
When an effector increases a change
What does oxytocin do?
stimulates uterine contractions at the end of pregnancy
What is excretion?
The removal of waste products of metabolism from the body
What is metabolism?
sum of all chemical reactions in the body
What are the three ways that water is removed from the body?
Urine, exhalation and sweat
What are some excretory organs and what is excreted from them?
Lungs- exhaled air- CO2 and H2O
Kidneys- urine- urea, creatinine, uric acid
Skin- sweat- urea
Liver- faeces- bile pigment
What metabolic process produces:
CO2 and H2O?
Urea, creatinine and uric acid?
Urea?
Bile pigment?
Respiration
Deamination, breakdown of muscle, breakdown of nucleic acid
Deamination
Breakdown of Hb
What are the two functions of the kidney?
1. Excretion
2. Osmoregulation
Define excretion
The removal of waste products of metabolism
What do the two kidneys do?
Filter the blood and remove waste as urine
What is deamination?
The removal of NH2 from excess amino acids
Where does deamination occur?
liver
What happens to the ammonia?
It is converted to urea in liver as ammonia is highly toxic
How is the urea transported?
In the blood
What is osmoregulation?
The control of the water content and solute composition of body fluids such as the blood, tissue fluid and lymph
Where are the kidneys found?
Dorsally in the abdomen
What are the parts of the urinary system?
Vena cava
Aorta
Renal artery
Renal vein
Kidney
Ureter
Bladder
Urethra
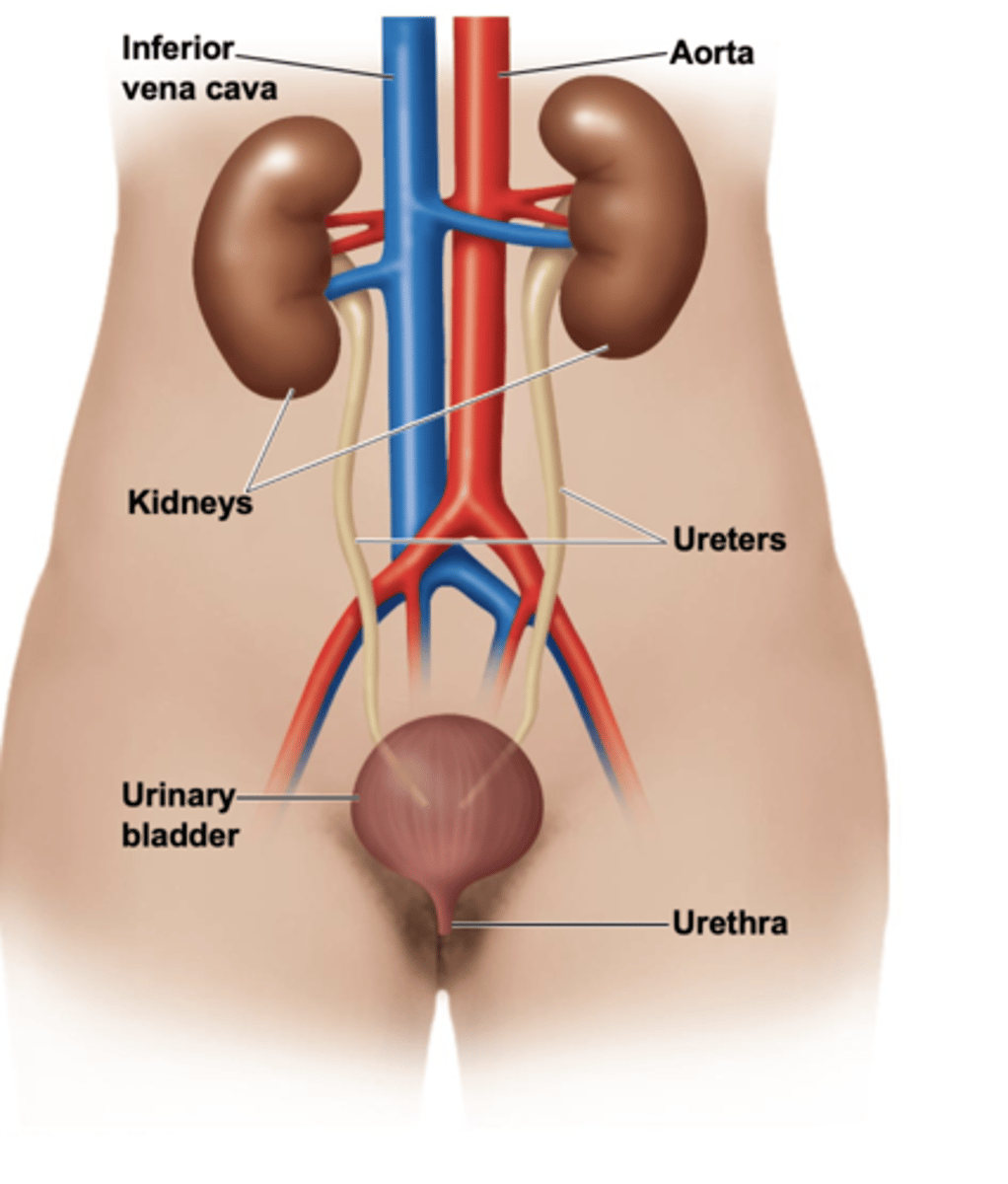
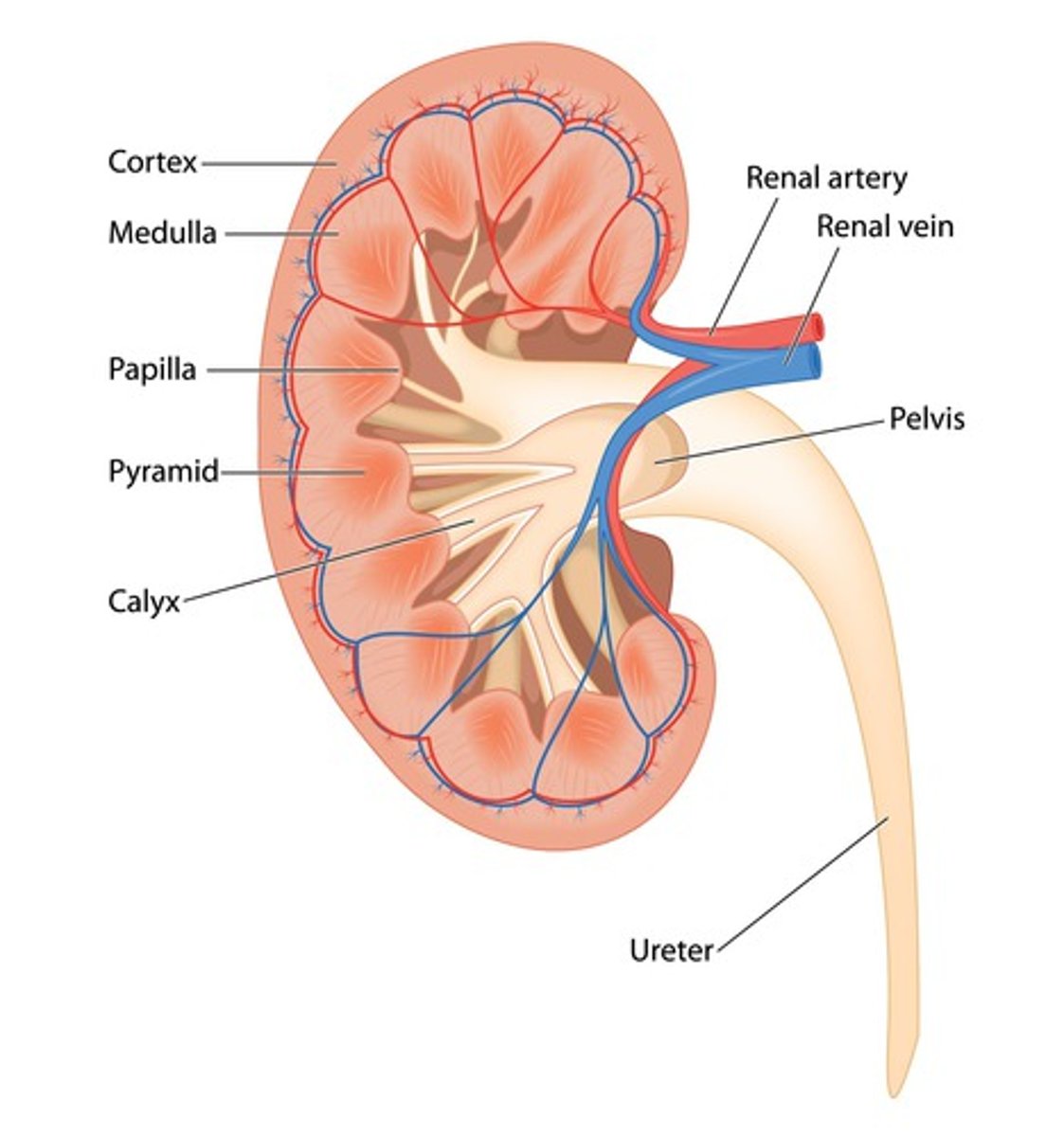
Label a kidney
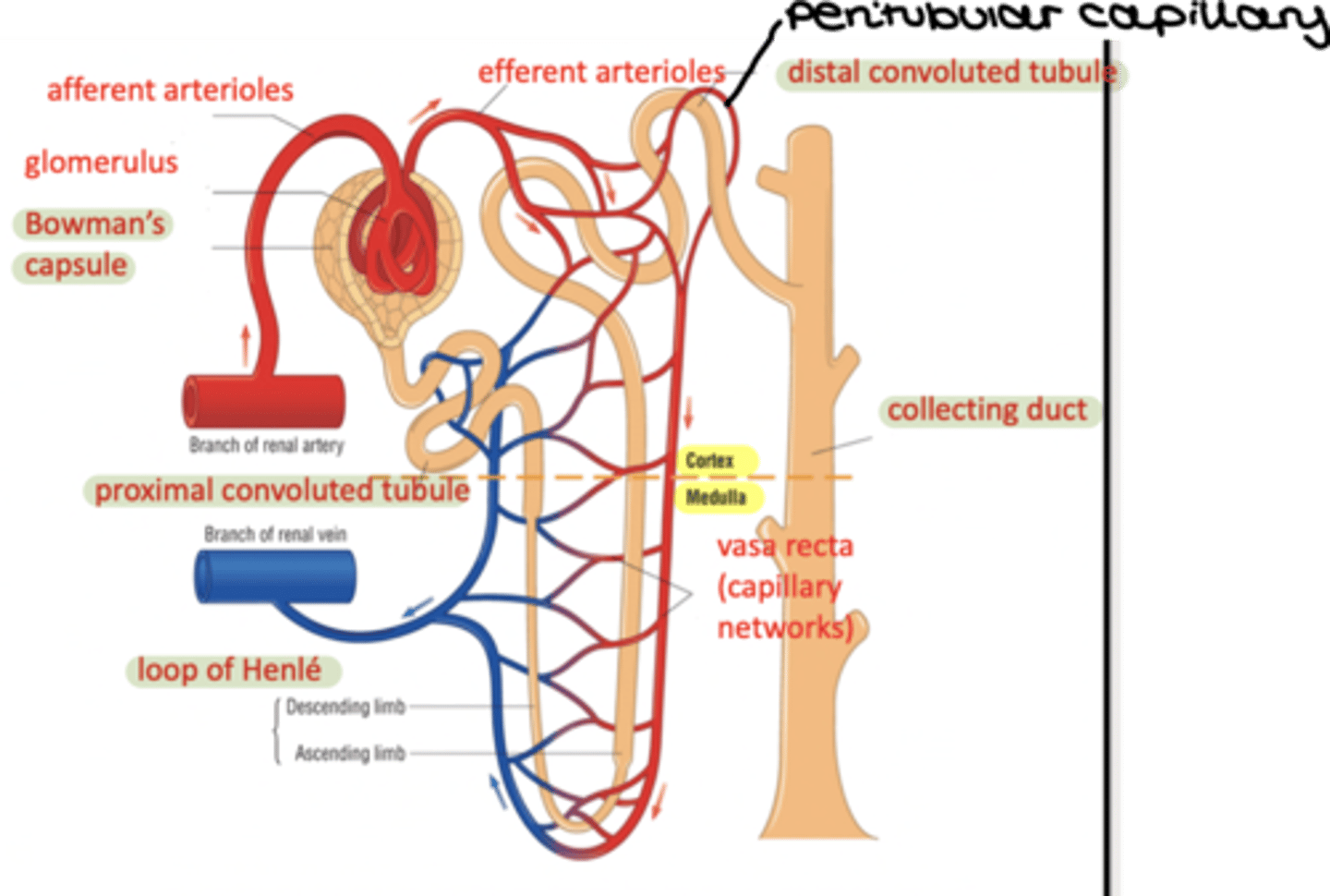
Label the structure of the nephron
Where do each of the kidneys receive its blood supply from?
the renal artery
What happens in the renal vein?
The filtered waste products are excreted by the kidneys as urine
What does urine pass down?
The ureter
What is the bladder?
A muscular sac that stores urine
What is at the base of the bladder?
A sphincter muscle which relaxes during urination so that urine passes out of the body along the urethra
What are the nephrons?
Filtering units
What is the outer cortex?
Where filtration takes place in the nephrons. It has a dense capillary network which receives blood from the renal artery
Where are the renal pyramids?
The medulla
What do the renal funnels collect urine into?
The pelvis
What does the nephron start with?
The Bowman's Capsule in the cortex
What is below the capsule?
The proximal convoluted tubule
What does this lead into?
The loop of henle which runs into the medulla and then back out to the cortex
What does the nephron then form?
The distal convoluted tubule
What does this join to?
A collecting duct which carries the urine through the medulla to the pelvis
What is ultrafiltration?
Fine filtration under very high hydrostatic pressure of small soluble molecules from the blood plasma in the glomerulus to form glomerular filtrate in Bowman's capsule
Why is there high blood pressure in the glomerulus?
1. Diameter of the afferent arteriole entering the glomerulus is greater than the efferent arteriole leaving the glomerulus
2. Blood comes from the renal artery, which is a branch of the aorta, which has blood under high pressure as it has just left the heart
What small molecules are filtered?
Salts
Water
Amino acids
Glucose
Urea
What are too large to be filtered?
Proteins- albumin and globulins
Red blood cells and white blood cells
What is the glomerulus and Bowman's space separated by?
3 layers: the endothelium of the capillary, the basement membrane and the epithelium of Bowman's capsule
What does the endothelium of the capillary have?
fenestrations
What is the basement membrane?
The selective barrier (molecular sieve)
What is the epithelium of Bowman's capsule made up of?
Squamous epithelial cells called podocytes
What do they have?
Pedicels which wrap around a capillary pulling it closer to the basement membrane
What are the gaps between the pedicels called?
Filtration slits
What does the blood that flows from the glomerulus into the efferent arteriole have?
A low water potential as much water has been lost and a high protein concentration remains
Percentage blood filtered=
volume of filtrate produced a minute/ volume of blood entering kidneys per minute x 100
What is selective reabsorption?
The uptake of specific molecules and ions from the glomerular filtrate in the nephron back into the bloodstream
Where does selective reabsorption occur?
proximal convoluted tubule
What is fully reabsorbed?
Amino acids, glucose
What remains in the nephron to be excreted in the urine?
Salts, water and urea
How is the PCT adapted for selective reabsorption?
-Large surface area due to its length
-Large surface area due to microvilli
-Cuboidal epithelial cells have many mitochondria providing ATP for active transport
-Has a close association with the peritubular capillaries of the vasa recta
-Epithelial cells have tight junctions between them. They prevent seepage of reabsorbed materials back into the filtrate
-Epithelial cells have invaginations called basal channels that increase the surface area of the cell membrane at the basement membrane side
How are
salts
water
amino acids
glucose
urea reabsorbed?
Active transport
Osmosis
Co-transport
Co-transport
Diffusion
Describe the process of co-transport
Movement of sodium ions out of the cell by active transport maintains a low conc inside the cell
This maintains a concentration gradient of sodium ions between the lumen and inside the cell
This ensures that sodium ions keeps diffusing into the cell by facilitated diffusion and therefore ensures the continued movement of glucose into the cell by cotransport.
A high concentration of glucose can therefore be maintained within the cell, meaning that it can continue to move out of the cell down a conc grad by fac diff
Define secondary active transport
Uses previously established gradient of Na or hydrogen ions to move other chemicals
What is the glucose threshold and why might it be crossed?
The level of glucose in the blood at which glucose starts to appear in a person's urine.
Transporter proteins become saturated with glucose molecules
A healthy person would never have glucose in their urine, but a person with diabetes might have elevated blood glucose levels that exceed the glucose threshold
At the end of the PCT, what happens?
The filtrate is isotonic with the blood plasma
What takes place following the PCT?
Further water reabsorption of water in the Loop of Henle, DCT and collecting duct
PCT rate of concentration graph
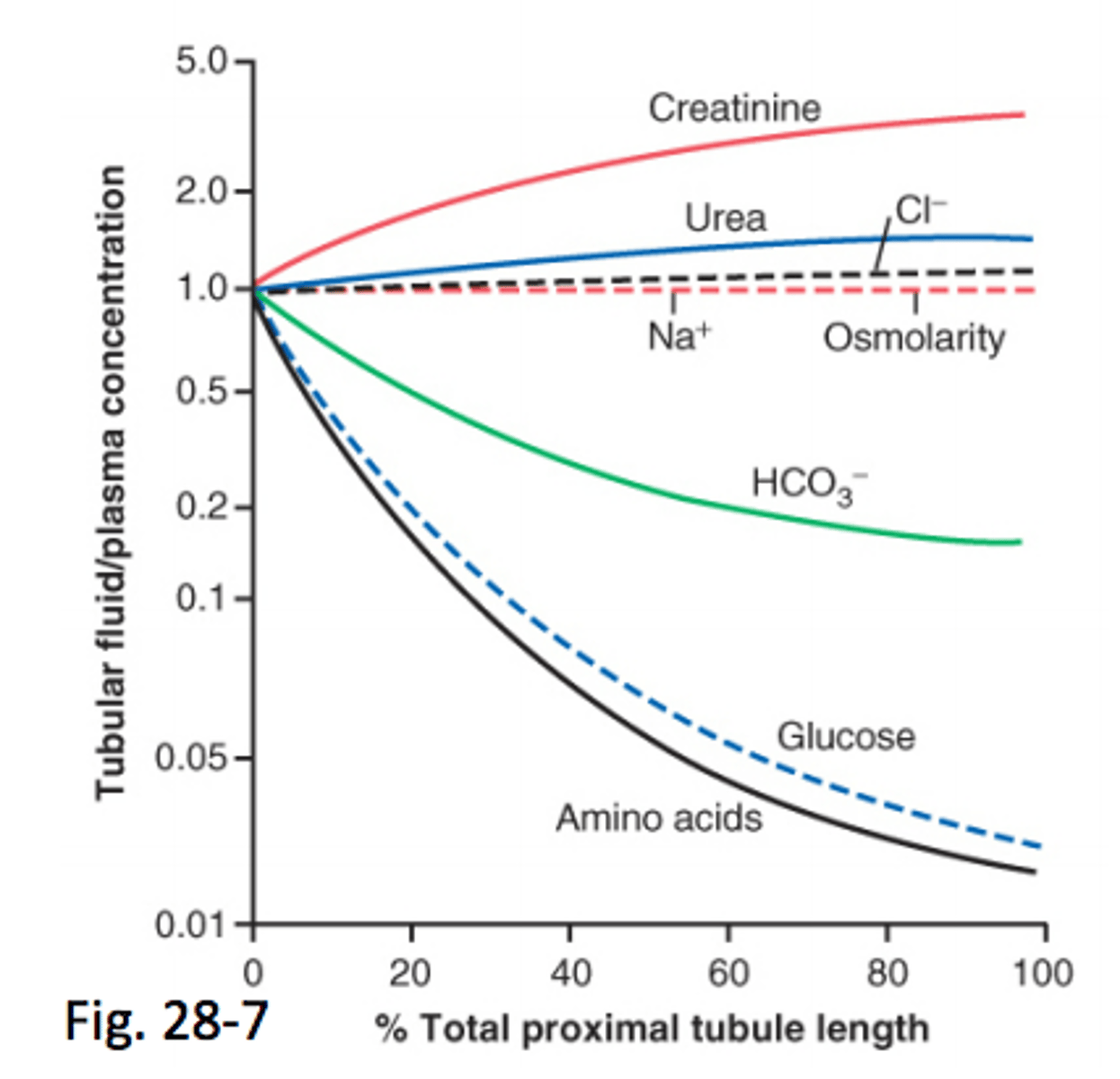
Explain this graph
Glucose and amino acids get selectively reabsorbed across the proximal convoluted tubule into the bloodstream so their concentrations decrease
Identify this
Glomerulus and Bowman's capsule so the cortex of the kidney
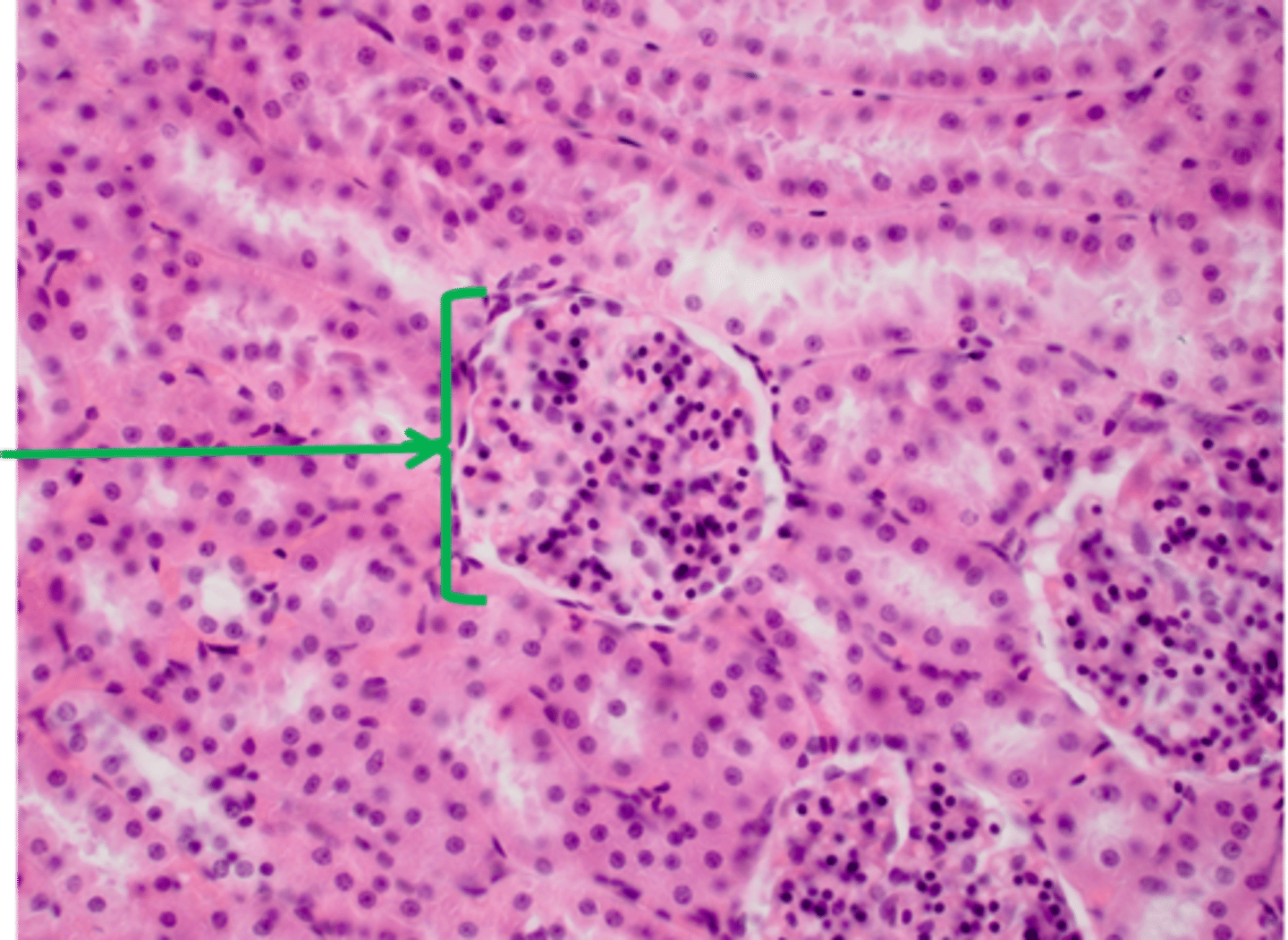
And this
Distal convoluted tubule and proximal convoluted tubule
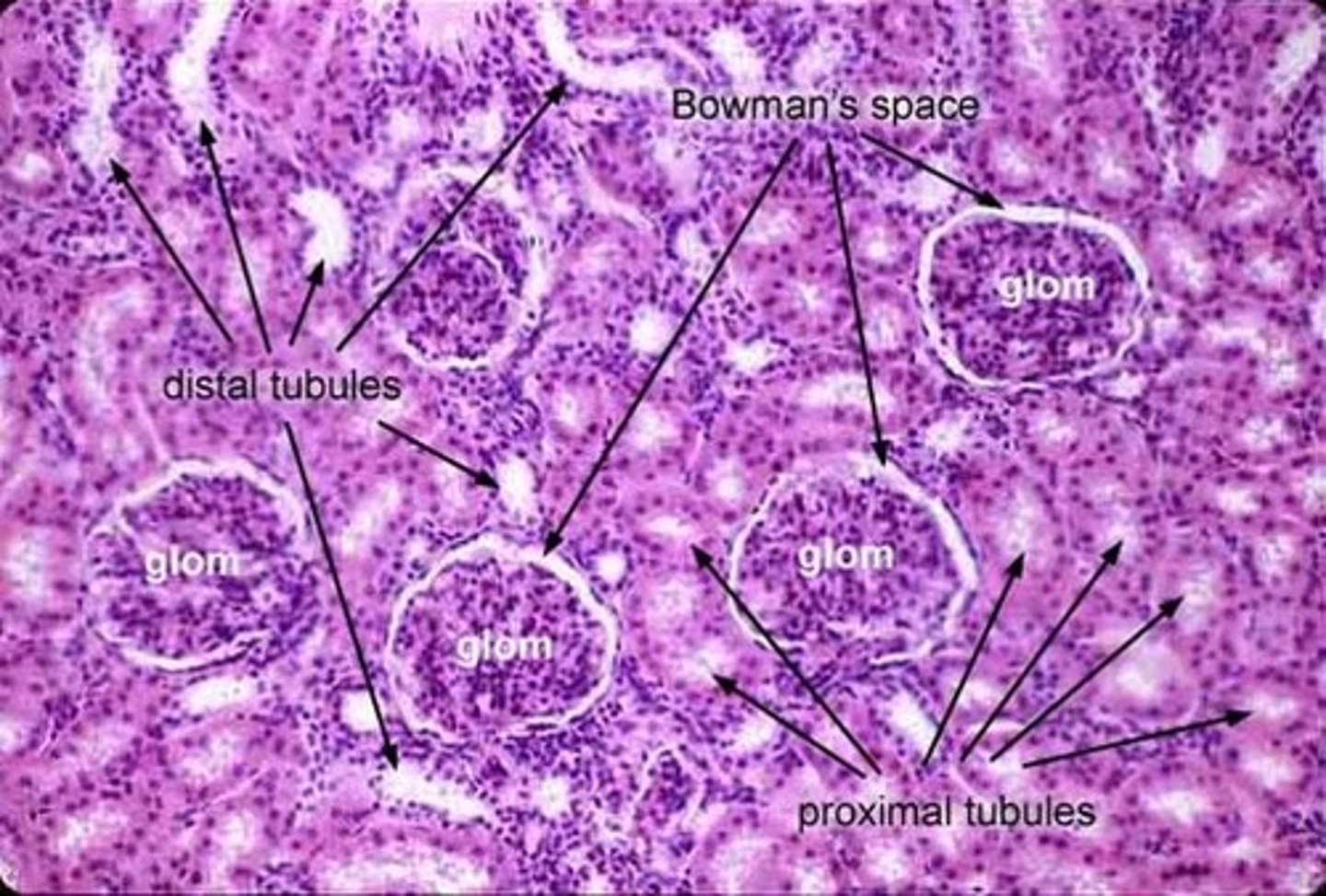
How do they differ in this?
PCT- fuzzy edge due to brush border of microvilli, smaller diameter of lumen
DCT- bigger lumen (wider diameter), less brush border
What is this
Thick walled ascending limb of loop of henle
Thin walled descending limb of loop of henle
Collecting duct- large internal and external diameter
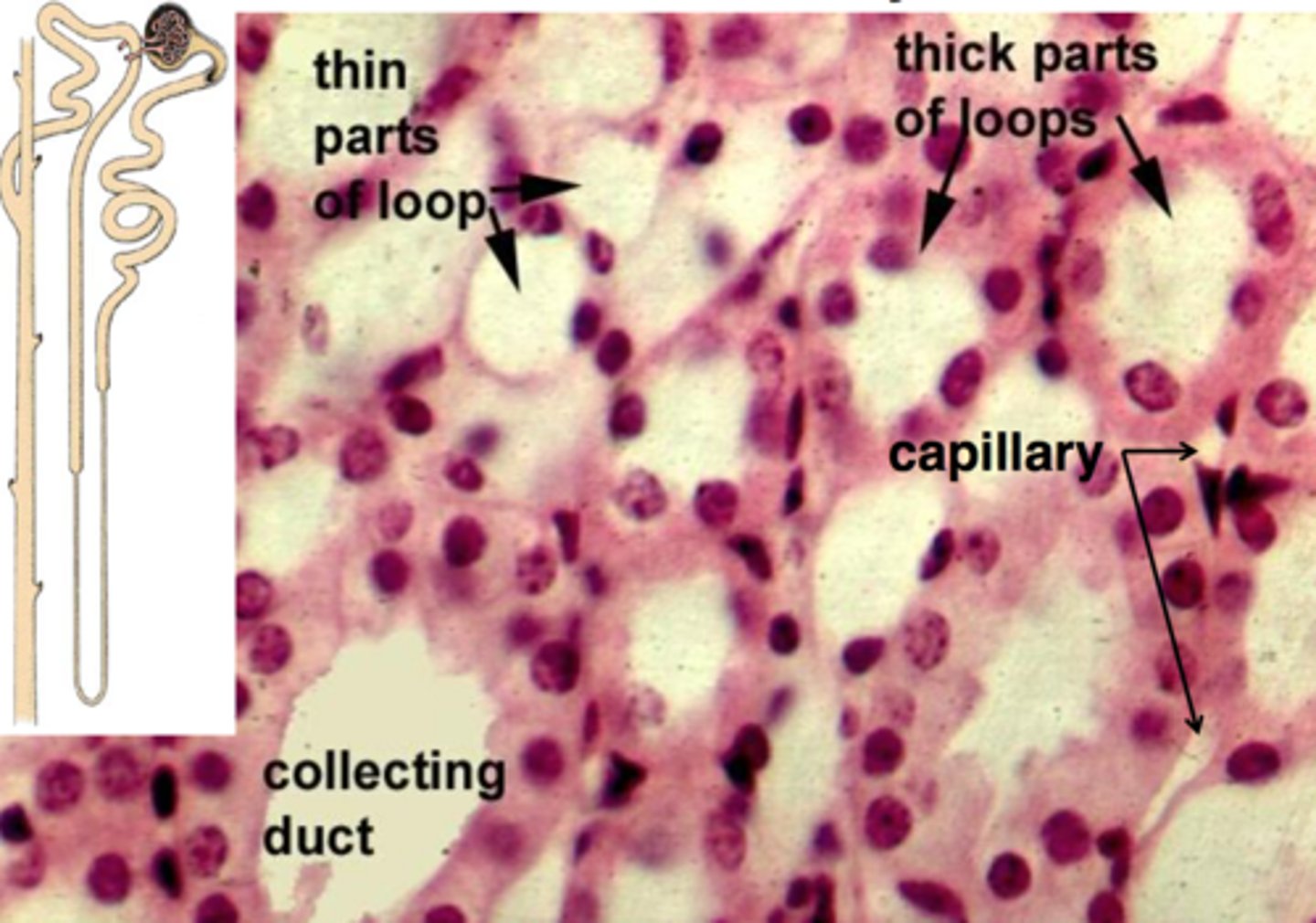
What is the role of the loop of Henle?
To set up a concentration gradient of salts in the tissue fluid of the medulla so that water can flow out of the collecting duct by osmosis should the body become dehydrated
How does the loop of Henle work?
Na+ and Cl- are actively transported out of the ascending limb against a conc grad into the tissue fluid in the medulla
The filtrate becomes less concentrated inside the ascending limb as you go up- higher water potential
Water will move down a water potential gradient by osmosis from the descending limb into the tissue fluid of the medulla, reducing the water potential of the filtrate as you go down the descending limb
Some Na+ and Cl- ions will diffuse into the descending limb, making the filtrate more concentrated
What type of system is this?
A counter current multiplier system
What is the general rule for the loop of henle?
The longer the loop of Henle, the more concentrated the base will be
What happens in the collecting duct?
Water moves down a water potential gradient out of the filtrate ie urine gets more concentrated
Why do diabetics urinate more?
The filtrate in the collecting duct will have a lower water potential than usual, as there will be more glucose in the filtrate, so less water will leave the collecting duct by osmosis down a water potential gradient and so more will be excreted in the urine
Salts and loop of henle??
How does the body gain water?
Drinking, eating
How does the body lose water?
Sweating, excretion, exhalation
What is a negative feedback loop used for?
To restore the normal osmotic concentration in the blood
What is the negative feedback loop under?
Hormonal control
What is the first thing that happens when you're dehydrated?
The osmoreceptor cells detect a fall in the water potential of the blood
Where are osmoreceptors located?
hypothalamus of the brain
What do osmoreceptors do?
Send nervous impulses to the co-ordinator
What is the co-ordinator?
The hypothalamus in the brain
What does the co-ordinator do?
Makes ADH (anti-diuretic hormone) and stores it in the posterior pituitary gland
What else happens to the ADH?
It is released into the bloodstream
What happens because of this?
The effector is effected
What happens?
The ADH binds to receptor proteins on the wall of the collecting duct and DCT of the kidneys
What does this do?
Makes the DCT and CD more permeable to water
What are aquaporins?
Intrinsic membrane proteins which have a pore through which water molecules move
What happens to the aquaporins?
They are added to the cell membranes
What does this allow?
More water to be reabsorbed from the filtrate into the hypertonic tissue fluid within the medulla by osmosis and then into the vasa recta
What will this result in?
An increase in the water potential of the blood back to the set point
What happens then?
This information is fed back to the hypothalamus and less ADH is produced
What will happen if insufficient water can be reabsorbed?
Hypothalamus will trigger thirst
What will happen if the water potential of the blood increases as a result of drinking too much water?
The opposite
What is frequent urination known as?
Diuresis
What does ADH cause?
A small volume of concentrated urine to be produced and for H2O to be reabsorbed into the blood
What does kidney failure result in?
Toxic levels of urea and an inability to remove excess water
What does this lead to?
Bodily fluids increasing in volume and are diluted, which compromises the metabolism
What may kidney failure be due to?
-Diabetes
-High blood pressure (damage to the capillaries of the glomerulus prevents ultrafiltration)
-Auto-immune disease
-Infection
-Crushing injuries