Pathogenic Gram-Positive Bacteria: Staphylococcus, Streptococcus, Bacillus, Clostridium, Mycobacterium, and Propionibacterium
1/112
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
113 Terms
What color do Gram-positive bacteria stain?
Purple
What are the two major groups of Gram-positive bacteria based on DNA content?
Low G + C bacteria (Firmicutes) and High G + C bacteria (Actinobacter)
What is a common characteristic of Staphylococcus bacteria?
They are normal members of human microbiota and can be opportunistic pathogens.
What type of anaerobes are Staphylococcus bacteria?
Facultative anaerobes
How do Staphylococcus bacteria typically arrange themselves?
In grapelike clusters
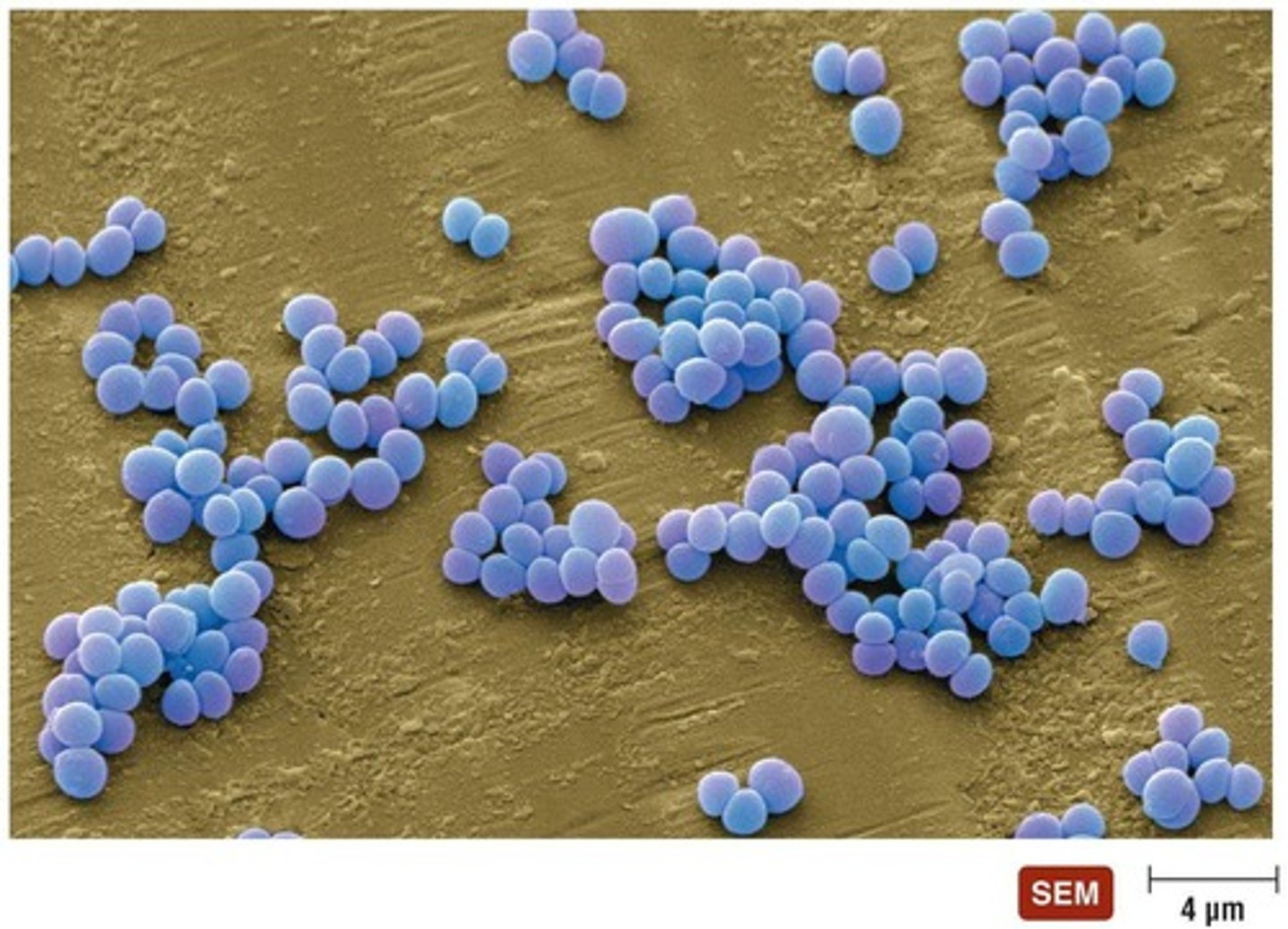
What is a notable feature of Staphylococcus regarding environmental conditions?
They are salt-tolerant and can survive on environmental surfaces.
What are the two species of Staphylococcus commonly associated with human diseases?
Staphylococcus aureus and Staphylococcus epidermidis
What is the more virulent strain of Staphylococcus?
Staphylococcus aureus
What is one way Staphylococcus can evade the immune system?
By producing Protein A, which binds to IgG and inhibits opsonization.
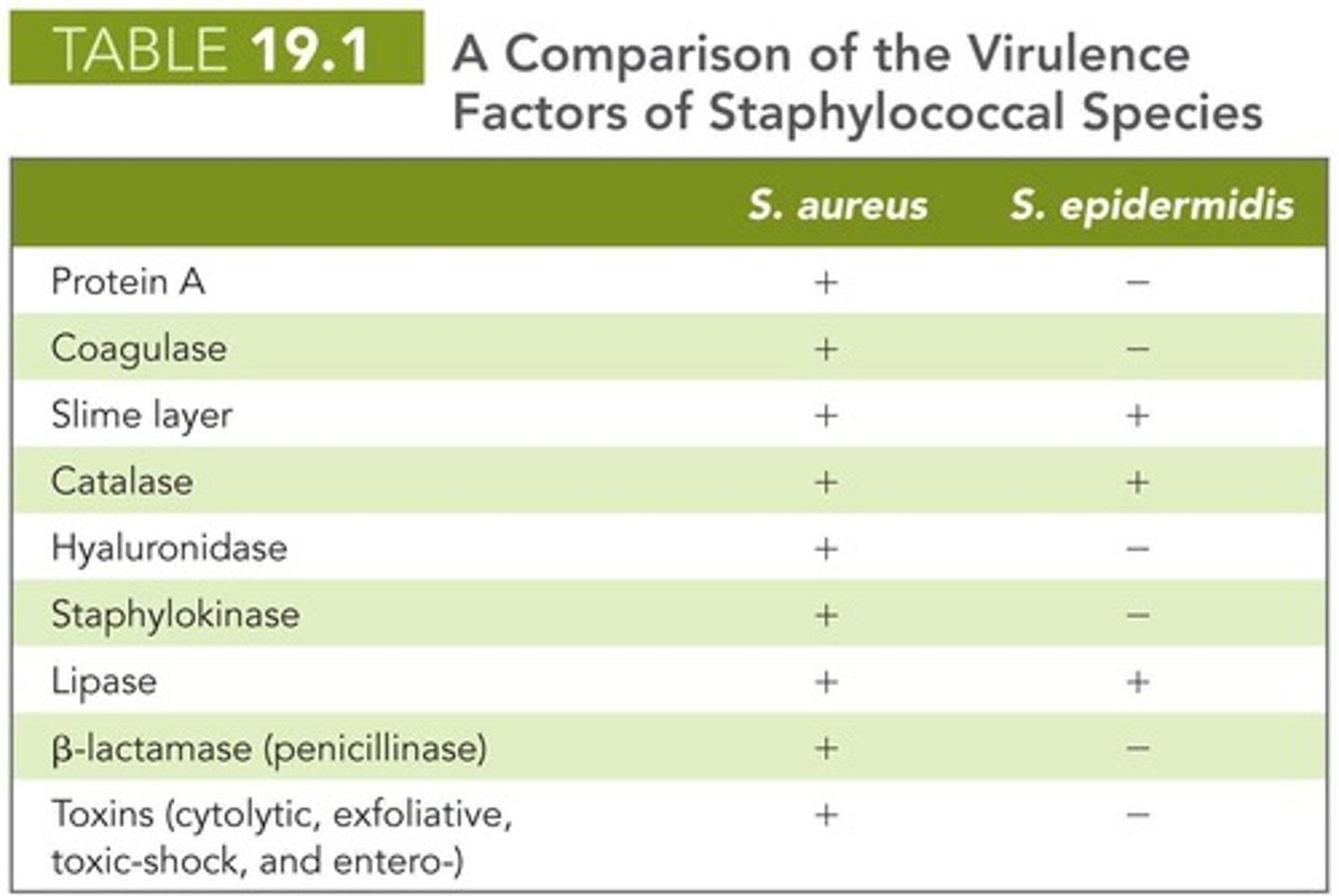

What enzyme produced by Staphylococcus triggers blood clotting?
Cell-free coagulase
What toxin produced by Staphylococcus can cause toxic shock syndrome?
Toxic-shock syndrome (TSS) toxin
What is the primary cause of food poisoning associated with Staphylococcus?
Ingestion of enterotoxin-contaminated food
What is the main characteristic of cutaneous diseases caused by Staphylococcus?
They involve various skin conditions with pyogenic lesions.
What is the condition called when pus fills the lungs due to Staphylococcus infection?
Empyema
What is the primary method of preventing Staphylococcus infections in healthcare settings?
Hand antisepsis
What type of bacteria is Streptococcus classified as?
Facultative anaerobes
How are Streptococcus bacteria often categorized?
Based on Lancefield classification into serotypes.
What is the pathogenicity factor of Group A Streptococcus (Streptococcus pyogenes) that destabilizes complement?
M protein
What disease is characterized by inflammation of the pharynx with pus?
Pharyngitis (strep throat)
What autoimmune response can occur as a complication of untreated streptococcal pharyngitis?
Rheumatic fever
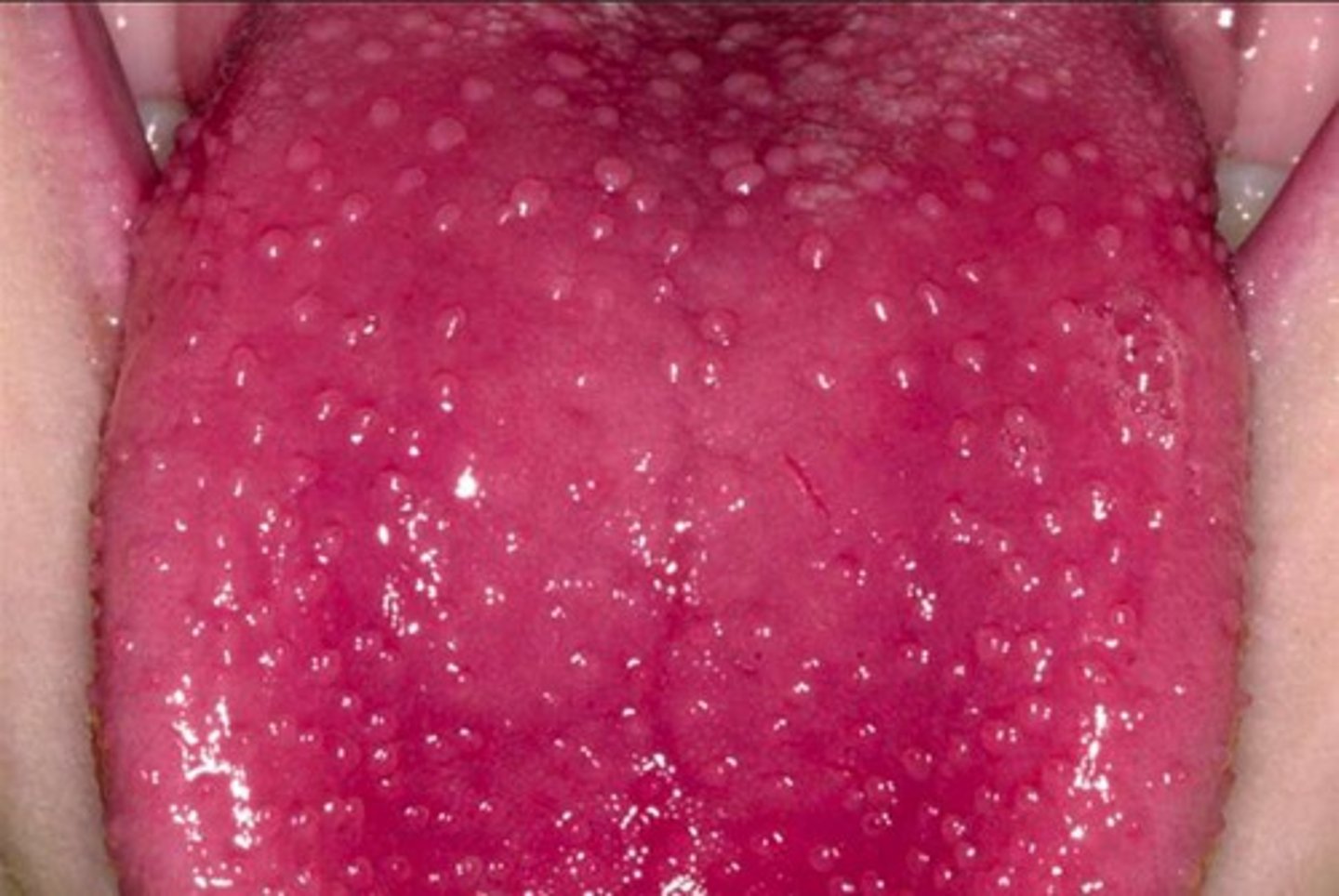
What toxin can cause a rash and strawberry tongue in scarlet fever?
Erythrogenic toxins
What is the role of hyaluronidase in Streptococcus infections?
It facilitates the spread of bacteria through tissues.
What is the significance of deoxyribonucleases produced by Streptococcus?
They reduce the firmness of pus and facilitate bacterial spread.
What is the primary transmission method for Streptococcus infections?
Via respiratory droplets
What is the treatment for methicillin-resistant Staphylococcus aureus (MRSA) infections?
Vancomycin
What structural component of Streptococcus helps it evade phagocytosis?
Hyaluronic acid capsule
What is the term for the presence of bacteria in the blood?
Bacteremia
What condition occurs when inflammation damages the lining of the heart due to Streptococcus?
Endocarditis
What is Group A Streptococcus?
Streptococcus pyogenes
What diseases are associated with Group A Streptococcus?
Pyoderma, erysipelas, streptococcal TSS, and necrotizing fasciitis
What is pyoderma?
A pus-producing lesion often on exposed skin
What is erysipelas?
Infection and inflammation of lymph nodes surrounding a streptococcal infection
What does streptococcal TSS cause?
Severe multisystem infections, organ failure, shock, and death
What is necrotizing fasciitis?
A condition where streptococci enter the body and spread along the fascia, destroying tissue
What is glomerulonephritis?
Inflammation caused by antibody-bound streptococcal antigens accumulating in the kidneys
How is Group A Streptococcus diagnosed?
By the presence of Gram-positive bacteria in short chains or pairs and rapid strep tests for respiratory infections
What is the treatment for Group A Streptococcus infections?
Penicillin is effective
What is Group B Streptococcus?
Streptococcus agalactiae
How is Group B Streptococcus distinguished from Group A?
By group-specific cell wall antigens and a smaller zone of beta-hemolysis
What diseases are associated with Group B Streptococcus?
Neonatal bacteremia, meningitis, and pneumonia
What is the primary method for diagnosing Group B Streptococcus?
Enzyme-linked immunosorbent assay (ELISA) test
What is the treatment for Group B Streptococcus infections?
Penicillin or ampicillin
What is the Viridans group of Streptococci?
Alpha-hemolytic streptococci that lack group-specific carbohydrates
What is Streptococcus pneumoniae commonly known for?
Causing pneumococcal pneumonia and other respiratory diseases
What is the pathogenesis of Streptococcus pneumoniae?
It has a polysaccharide capsule for protection and can evade phagocytosis
What are the common diseases caused by Streptococcus pneumoniae?
Pneumonia, sinusitis, otitis media, bacteremia, and meningitis
How is Streptococcus pneumoniae diagnosed?
Through Gram stain of sputum smears and confirmed with the Quellung reaction
What is Bacillus anthracis?
The bacterium that causes anthrax
What are the three clinical manifestations of anthrax?
Gastrointestinal anthrax, inhalation anthrax, and cutaneous anthrax
What is the primary route of transmission for Bacillus anthracis?
Inhalation, inoculation through skin breaks, or ingestion of spores
What is the treatment for anthrax?
Many antimicrobials are effective against Bacillus anthracis
What is Clostridium?
Anaerobic, endospore-forming bacilli found in soil and gastrointestinal tracts
What diseases are caused by Clostridium perfringens?
Food poisoning and gas gangrene
What is gas gangrene?
A condition caused by Clostridium perfringens where endospores germinate and produce toxins leading to necrosis
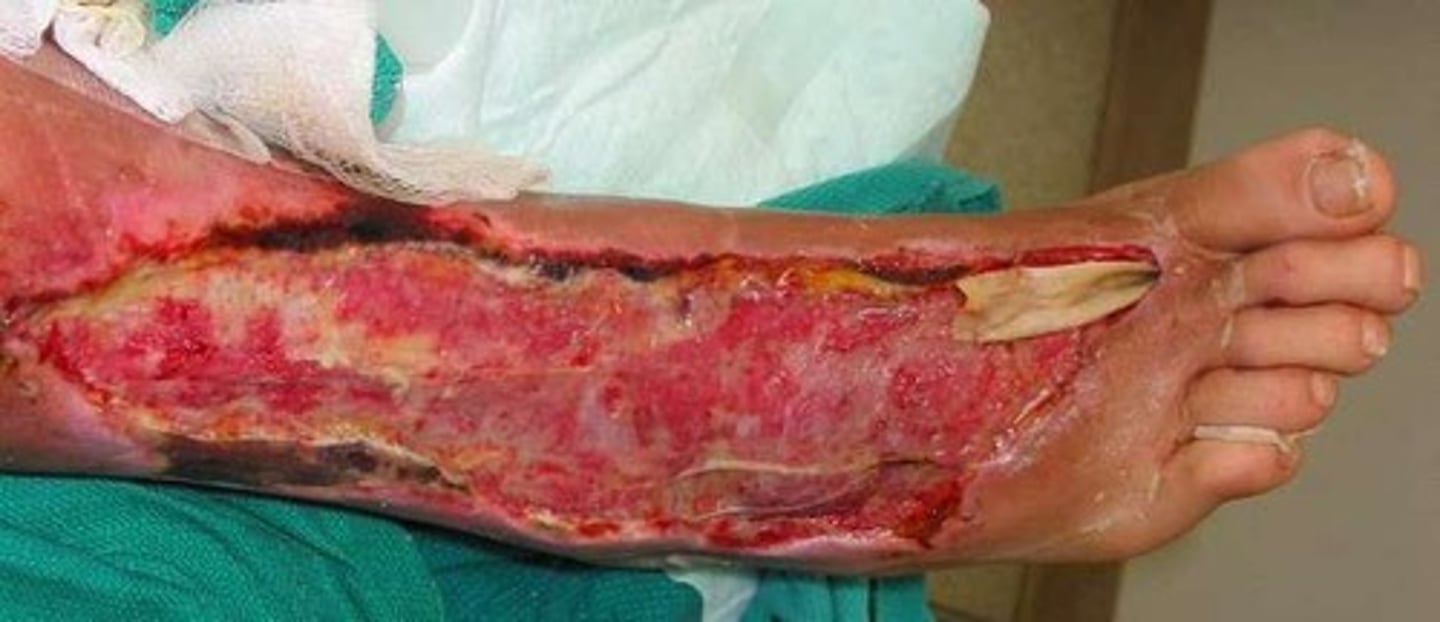
What are the characteristics of Clostridium species?
They produce histolytic toxins, enterotoxins, and neurotoxins
What is Clostridium perfringens known for?
It is associated with food poisoning and gas gangrene.
How is Clostridium perfringens diagnosed?
By the presence of a minimum bacterial load in food or feces and the appearance of gas gangrene.
What is the treatment for gas gangrene caused by Clostridium perfringens?
Removal of dead tissue, administration of antitoxin and penicillin, and hyperbaric oxygen therapy.
What preventive measure can reduce cases of food poisoning from Clostridium perfringens?
Refrigeration of foods.
What is Clostridium difficile?
A motile, anaerobic intestinal bacterium that produces toxins A and B.
What condition can Clostridium difficile cause in patients taking antibiotics?
Pseudomembranous colitis.
How is Clostridium difficile diagnosed?
By isolating the organism from feces and demonstrating the presence of toxins by immunoassay.
What is the treatment for serious Clostridium difficile infections?
Antibiotics and discontinuation of the causative antimicrobial drug.
What is Clostridium botulinum known for?
It produces botulism toxins that cause flaccid paralysis.
What are the three manifestations of botulism?
Foodborne botulism, infant botulism, and wound botulism.
What is the fatality rate of type A botulinum toxin?
60-70%.
How is botulism diagnosed?
Symptoms are diagnostic, and a mice assay can test for the type of toxin.
What is the treatment for botulism?
Washing the intestinal tract, administering neutralizing antibodies, and antimicrobial drugs in infant and wound cases.
What is Clostridium tetani responsible for?
Causing tetanus, characterized by muscle spasms and lockjaw.
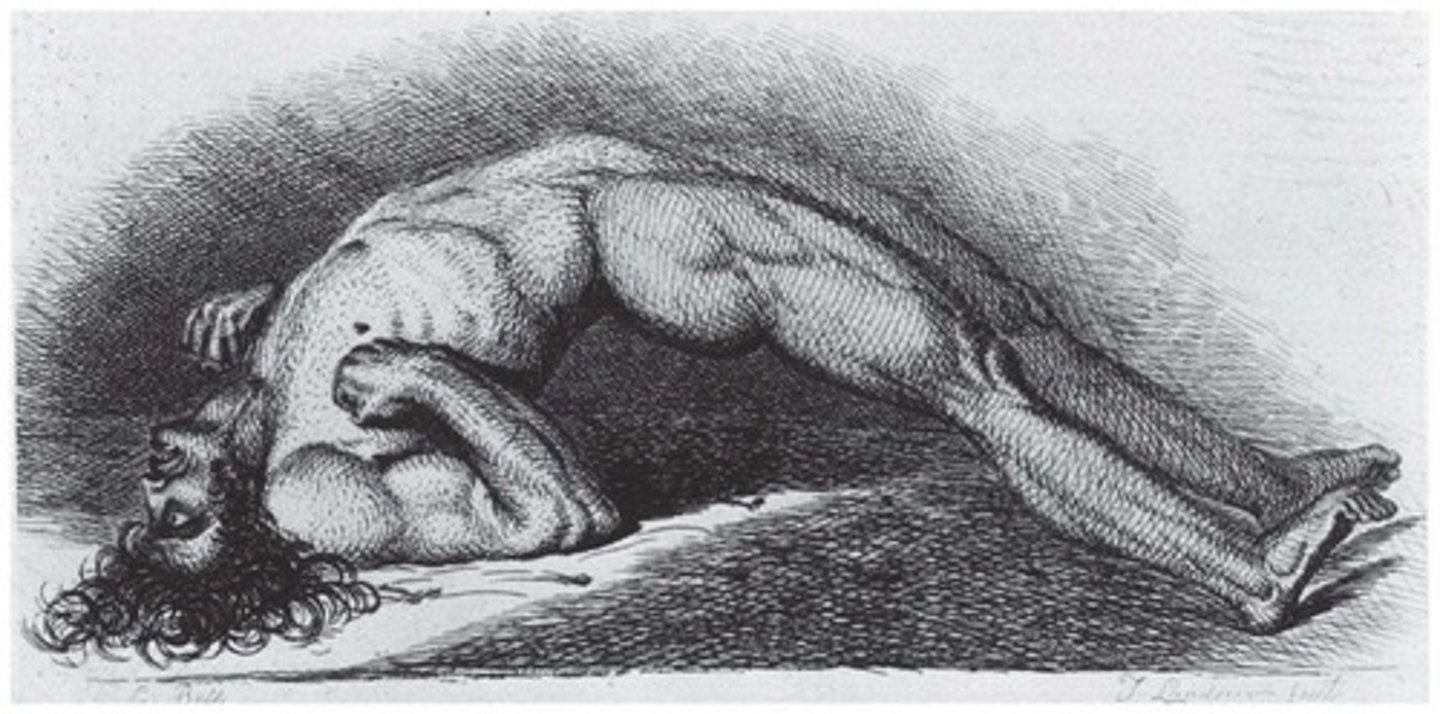
What is the mechanism of action of tetanospasmin toxin?
It blocks inhibitory neurons, causing continuous muscle contractions.
What is the mortality rate for tetanus?
About 50%.
How is tetanus diagnosed?
By characteristic muscular contraction.
What is the prevention method for tetanus?
Immunization with tetanus toxoid.
What is Listeria monocytogenes?
A non-endospore-forming bacillus that can cause listeriosis.
How does Listeria monocytogenes evade the immune system?
By growing within phagocytes and using Listeriolysin O to avoid digestion.
What are the potential consequences of Listeria infection in pregnant women?
Premature delivery, miscarriage, stillbirth, or meningitis in the newborn.
What is the primary route of transmission for Listeria monocytogenes?
Contaminated food and drink.
What is the role of actin tails in Listeria monocytogenes infection?
They help the bacterium move within and between host cells.
What are the symptoms of foodborne botulism?
Nausea, blurred vision, dizziness, abdominal pain, and paralysis.
What is the treatment for minor Clostridium difficile infections?
Discontinuation of the causative antimicrobial drug.
What is the significance of proper canning in relation to Clostridium botulinum?
It is crucial for preventing botulism.
What is the characteristic symptom of tetanus?
Initial tightening of the jaw and neck muscles, known as lockjaw.
What are the two toxins produced by Clostridium difficile?
Toxin A and Toxin B.
What is the role of hyperbaric oxygen therapy in treating gas gangrene?
It helps to remove the anaerobic environment and promote healing.
What bacterium is pushed into a pseudopod and can cause meningitis?
Listeria
What are mycoplasmas known for?
They are the smallest free-living microbes that lack cell walls.
What is the primary disease associated with Mycoplasma pneumoniae?
Primary atypical pneumonia, also known as walking pneumonia.
How is Mycoplasma pneumoniae primarily spread?
By nasal secretions among people in close contact.
What is the characteristic structure of Corynebacterium?
Pleomorphic, non-endospore-forming bacteria that divide via snapping division.
What disease does Corynebacterium diphtheriae cause?
Diphtheria.
How is diphtheria transmitted?
Via respiratory droplets or skin contact.
What toxin does Corynebacterium diphtheriae produce?
Diphtheria toxin, which inhibits polypeptide synthesis in eukaryotes.
What is the most effective way to prevent diphtheria?
Immunization with the DTaP toxoid vaccine.
What is a unique feature of Mycobacterium species?
Their cell wall contains mycolic acid, resulting in slow growth and resistance to many antimicrobial agents.
What disease is caused by Mycobacterium tuberculosis?
Tuberculosis (TB).
What are the three types of tuberculosis?
Primary tuberculosis, secondary/reactivated tuberculosis, and disseminated tuberculosis.
What happens during primary tuberculosis?
It results from the initial infection with M. tuberculosis.
What occurs during secondary/reactivated tuberculosis?
M. tuberculosis breaks the stalemate and reestablishes an active infection.
What is the incubation period for leprosy caused by Mycobacterium leprae?
It can be several years.
What are the two forms of leprosy?
Tuberculoid (neural) leprosy and lepromatous leprosy.