Host parasite relationships
1/49
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
50 Terms
host
organism which provides nutrients to another organism
Parasite
an organism that lives on or in a host and from which it derives nutrients and environmental conditions necessary for growth and reproduction
Host and parasite are in a dynamic interaction, the outcome of which depends upon the properties of the host (susceptibility) and of the parasite.
What are the 2 important elements that control the interaction between a host/parasite?
The hosts own susceptibility / defence mechanisms or immunity employed against the parasite
The virulence factors exhibited by bacteria that enable them to invade and damage the host and to resist host defences
Colonisation
growth of microorganisms on body surfaces with no recognizable reaction in the host i.e. no inflammatory response
Infection is a result of,
Interaction between a host and a multiplying microorganism that usually involves tissue penetration and results in a host response i.e. inflammation to eliminate the microbe or to protect the host against further invasion or reinfection
Pathogenicity
ability of a microorganism to cause damage in a host
Virulence
measure of capacity of a microorganism to infect or damage a host → the degree of pathogenicity
Virulence factors
factors responsible for virulence of a microorganism because they influence it’s ability to cause disease by affecting its invasiveness and/or its toxicity e.g. adhesins, toxins, secretory systems
Adhesin
a surface structure or macromolecule that binds a bacterium to a specific surface
Receptor
a complementary macromolecular binding site on a (eukaryotic) surface that binds specific adhesins e.g. Tir receptor (translocated intimin receptor) encoded by the T3SS in EPEC/EHEC
3 Types of symbiotic associations
1. Mutualism
– mutually beneficial relationship between two species
2. Commensalism
– a relationship between two species in which one is benefited and the other is not affected → not always the case
3. Parasitism
– a relationship between two species in which one benefits to the detriment of the other
Normal flora
Microorganisms normally present in the healthy body are collectively called normal flora and include:
– commensalistic or mutualistic relationship with the host
– colonise specific sites → tissue tropism e.g. vagina has Lactobacillus sp. present → create low pH environment that prevents the growth of pathogenic fungi e.g. Candida albicans or bacteria
Normal flora - 3 main sites of colonisation
1. STERILE COMPARTMENTS eg. blood, CSF, synovial fluid, deep tissues, presence of microbes diagnostically significant
2. SITES WITH LOW NUMBERS eg. stomach, upper small intestine, finding sizable numbers suggest disease
3.SITES WITH LARGE NUMBERS eg. skin, mouth, nasopharynx, colon, where high microbial populations are normal and beneficial.

What factors lead to the non static, constant composition of normal flora at these sites
individual components waxes and wanes in relation to age, sex, diet, temperature, antibiotics → wipe out bacteria and allow opportunistic pathogens to thrive, resulting in dynamic changes in overall flora.
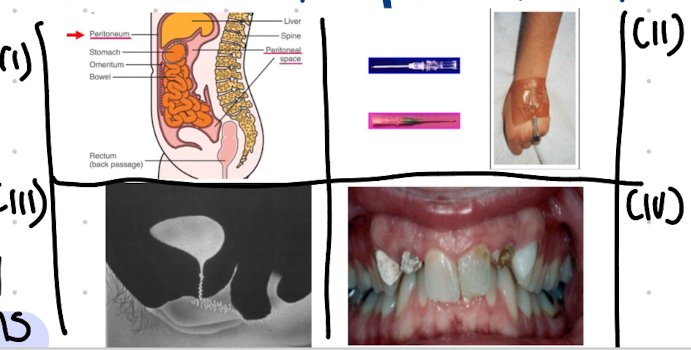
What are examples of normal flora associated infection, when host defence is lowered/ normal flora is transferred to a sterile/ new site in the host?
i. Bacteroides in abdominal infections eg peritonitis.
ii. Staphylococcus epidermidis in intravenous catheter infections.
iii. Escherichia coli in UTIs
iv. Dental plaques, caries and periodontal disease.
Why are normal flora important?
Physically block (microbiological barrier) pathogens from adhering to and colonising
Produces fatty acids, peroxides or bacteriocins which inhibit or kill pathogens “colonisation resistance”
Vitamin synthesis e.g. vit K and B by E.coli and some Bacteroides spp.
Prime immune system + immune tolerance → stimulate production of cross-reactive Ab which cross-react with related pathogens
What can happen when antibiotics wipe healthy normal flora?
eg. antibiotics which severely affect flora
i. yeasts infections in mouth and vagina → Oral candidiasis
ii. Clostridioides difficile infections
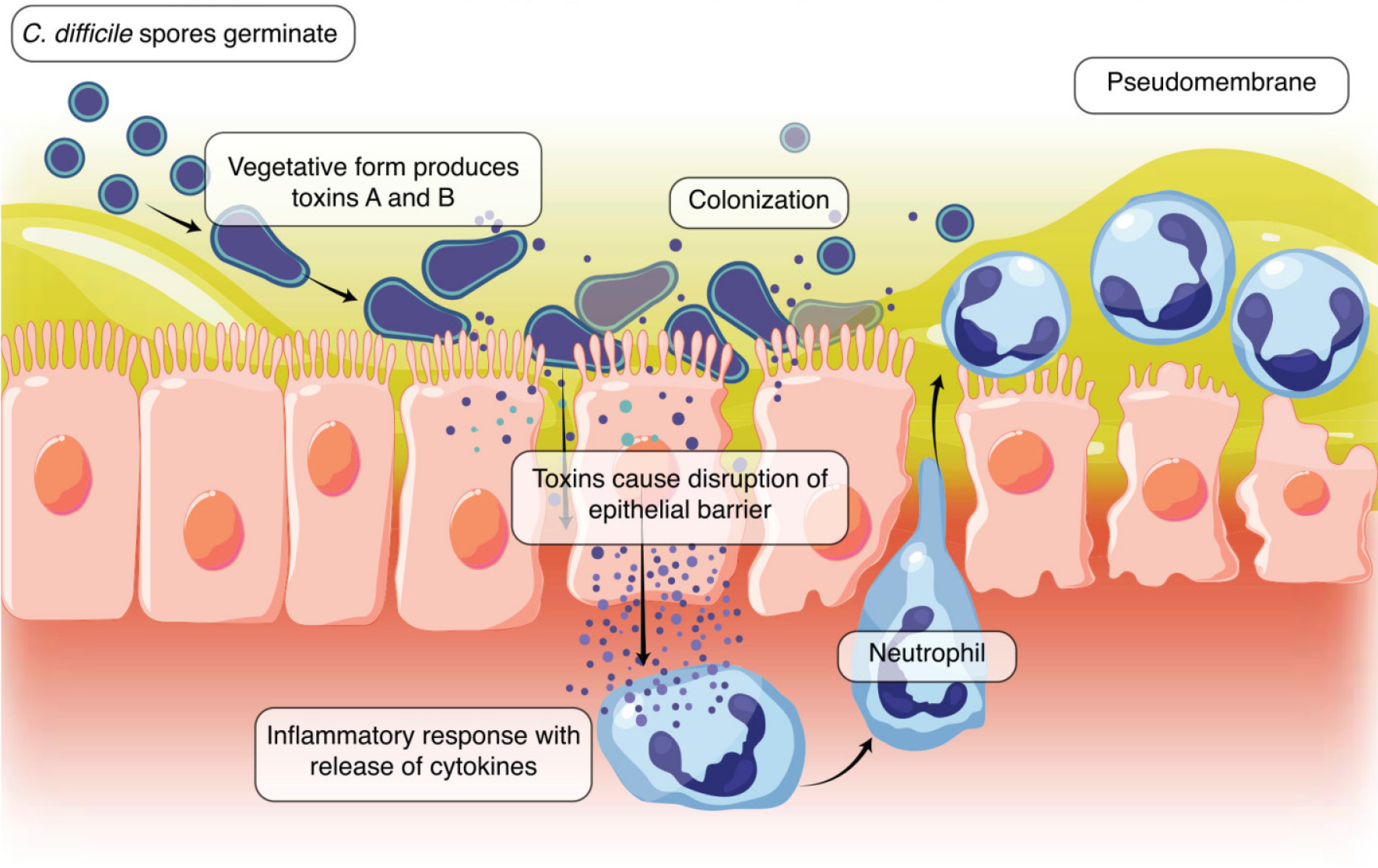
What is C. diff?
C.Clostridioides difficile (. ) is a gram-positive, anaerobic, spore-forming bacterium responsible for antibiotic-associated diarrhea and colitis.
It causes infection by releasing exotoxins ( A and B) that damage the intestinal mucosa, typically following disruption of normal gut flora. . spores are highly resistant to disinfectants and can survive for months on surfaces
Invasiveness and microbial pathogenesis
The ability to invade tissues:
Encompasses mechanisms for colonisation (adherence and initial multiplication)
By the ability to bypass or overcome host defence mechanisms
The production of extracellular substances ("invasins") which facilitate the actual invasive process
Toxigenesis and microbial pathogenesis
the ability of microbes to produce toxins that damage host tissues and disrupt normal cellular functions.
This process can lead to disease symptoms and immune response activation.
5 Traits of a successful pathogen
Colonise a body surface.
Replicate or spread within the host.
Can metabolically adapt to the host environment.
Evade the host defence system.
Find a new host (spread within the community).
7 steps in pathogenesis
Encounter
Entry
Attachment to host cells
Local or general spread in the body
Cell and tissue damage
Evasion of host defences
Transmission to new host
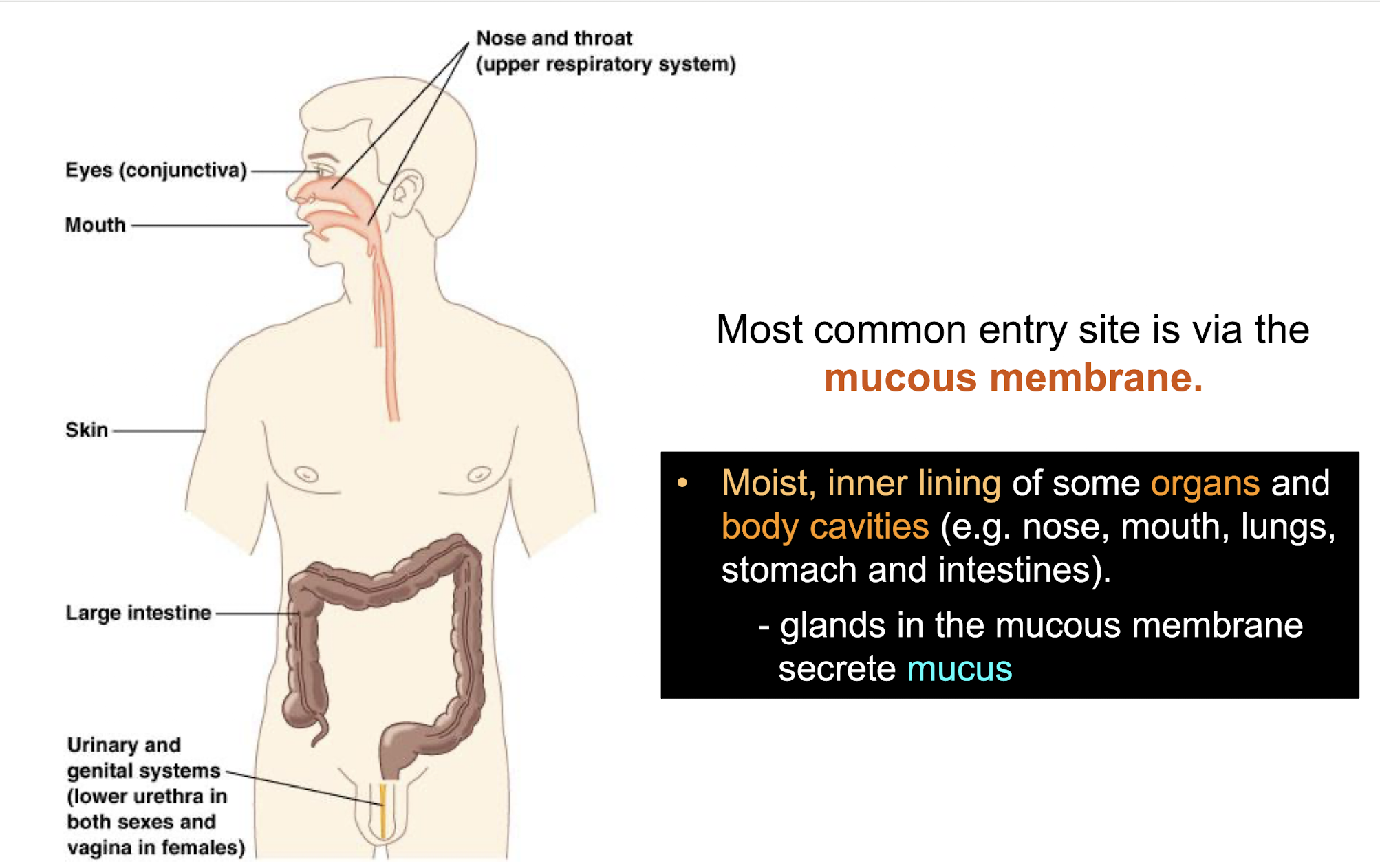
Why is the mucous membrane the most common site of entry for pathogens?
As it is a moist inner lining due to mucus production by goblet cells secreting mucins, where many of the mucosal surfaces are washed by fluids:
– mucus in the upper respiratory tract and the gut
– movement of urine in the urinary tract
Thus bacteria have developed strategies to multiply and cause infection by fixing its position and becoming established onto the mucus membrane via adhesins / receptor proteins
2 main adherence strategies by bacteria
• Fimbriae (common pili)
– rigid hair-like structures protruding from bacterial surface
• Afimbrial adhesins
– lectins (carbohydrate-binding proteins)
– M protein
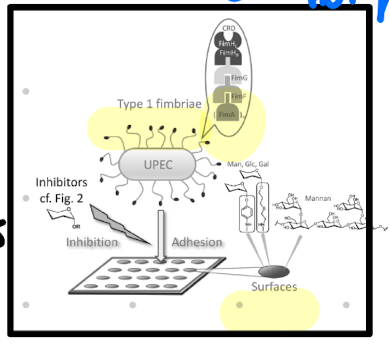
How is bacterial adherence specific to certain cell types?
Specificity accounts for pathogens distinctively infecting certain organs of the body and not others.
• Receptors are expressed only by specific cell types restricting infection accordingly
– receptors are also ubiquitous and organisms have no tissue restriction
What are the 3 possible events post-attachment?
A. Multiplication on cell surface, producing toxins which cause damage e.g. V. cholerae, C. diphtheriae
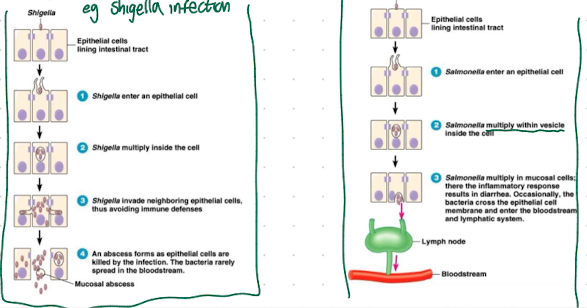
B. Penetration and multiplication within epithelial cells (Shigella, Enteroinvasive E. coli).
C. Penetration through or between epithelial cells and systemic spread through blood or lymphatics to target sites
e.g. Salmonella, disseminated gonococcal infections
Invasins
extracellular substances such as proteins i.e. enzymes that act locally to damage host cells / or have the immediate effect of facilitating the growth and spread of the pathogen
Spreading factors
a descriptive term for a family of bacterial enzymes that affect tissue matrices and intercellular spaces, thereby promoting the spread of the pathogen
What are the 4 main bacterial spreading factors (invasins)?
– Hyaluronidase
• depolymerise hyaluronic acid ("ground substance") of connective tissue
– Collagenase
• breaks down collagen
– Neuraminidase
• degrades neuraminic acid, an intercellular cement of the epithelial cells
– Streptokinase and Staphylokinase
• convert plasminogen to plasmin which digests fibrin
What are two examples of cell-membrane acting invasins?
Phospholipases → hydrolyse phospholipids in cell membranes
Lecithinases → destroy lecithin in cell membranes
Result in pores (due to membrane insertion that cause cell lysis or enzymatic attack on phospholipids which destabilise the membrane
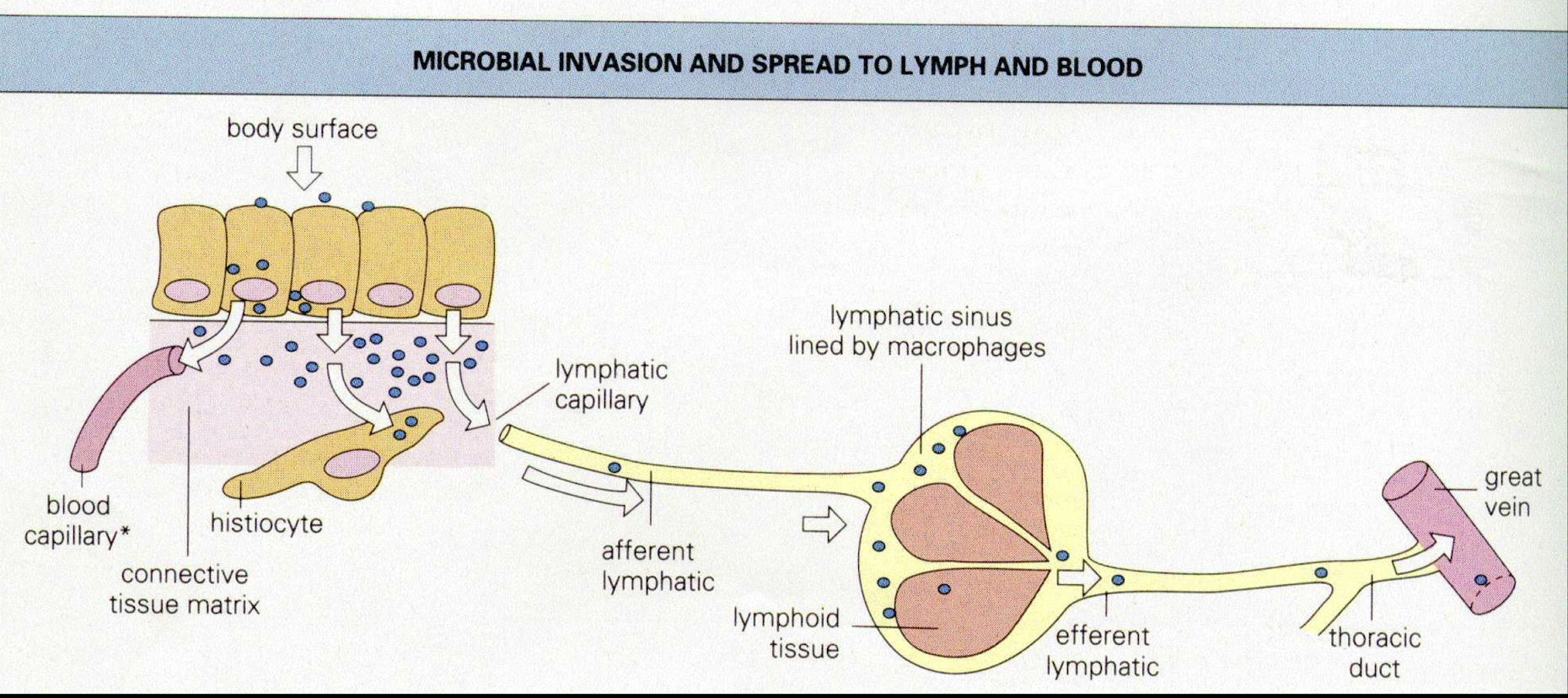
What are the two main routes which bacteria can spread to other tissues?
1. Lymphatic spread → system is designed to filter out particular material such as bacteria but is less efficient when:
• there is high lymph flow due to acute tissue inflammation
• there is a high concentration of organisms
• allows for spread of phagocytosis-resistant organisms
2.Vascular system spread → most convenient route
– must be resistant or be able to evade the complex vascular system immune defences
• some organisms can transmit freely within the plasma (Bacillus anthracis and Leptospira species)
• other organisms can survive and transported in mononuclear cells (Mycobacterium and Listeria monocytogenes)
how do pathogens evade host defences by antigenic disguise?
Via opsonising antibodies or complement:
• Bacteria may be able to coat themselves with host proteins such as fibrin or fibronectin.
• Able to hide their own antigenic surface components from the immunological system
examples:
– S. aureus possess coagulase that cause fibrin to deposit on the cell surface
– Fibronectin coat of Treponema pallidum
– Hyaluronic acid capsule of Streptococcus pyogenes
how do pathogens evade host defences by persistence at sites inaccessible to the immune response?
Intracellular pathogens can evade host immune responses as long as they stay inside of infected cells and don’t allow microbial antigen to form on the cell surface.
• Seen in macrophages infected with Brucella or Listeria.
• The macrophages support the growth of the bacteria while protecting against immune responses.
how do pathogens evade host defences by using soluble bacterial antigens to absorb antibodies?
• Some bacteria can liberate antigenic surface components in a soluble form into the tissue fluids.
• These soluble antigens are able to combine with and "neutralize" antibodies before they reach the bacterial cell
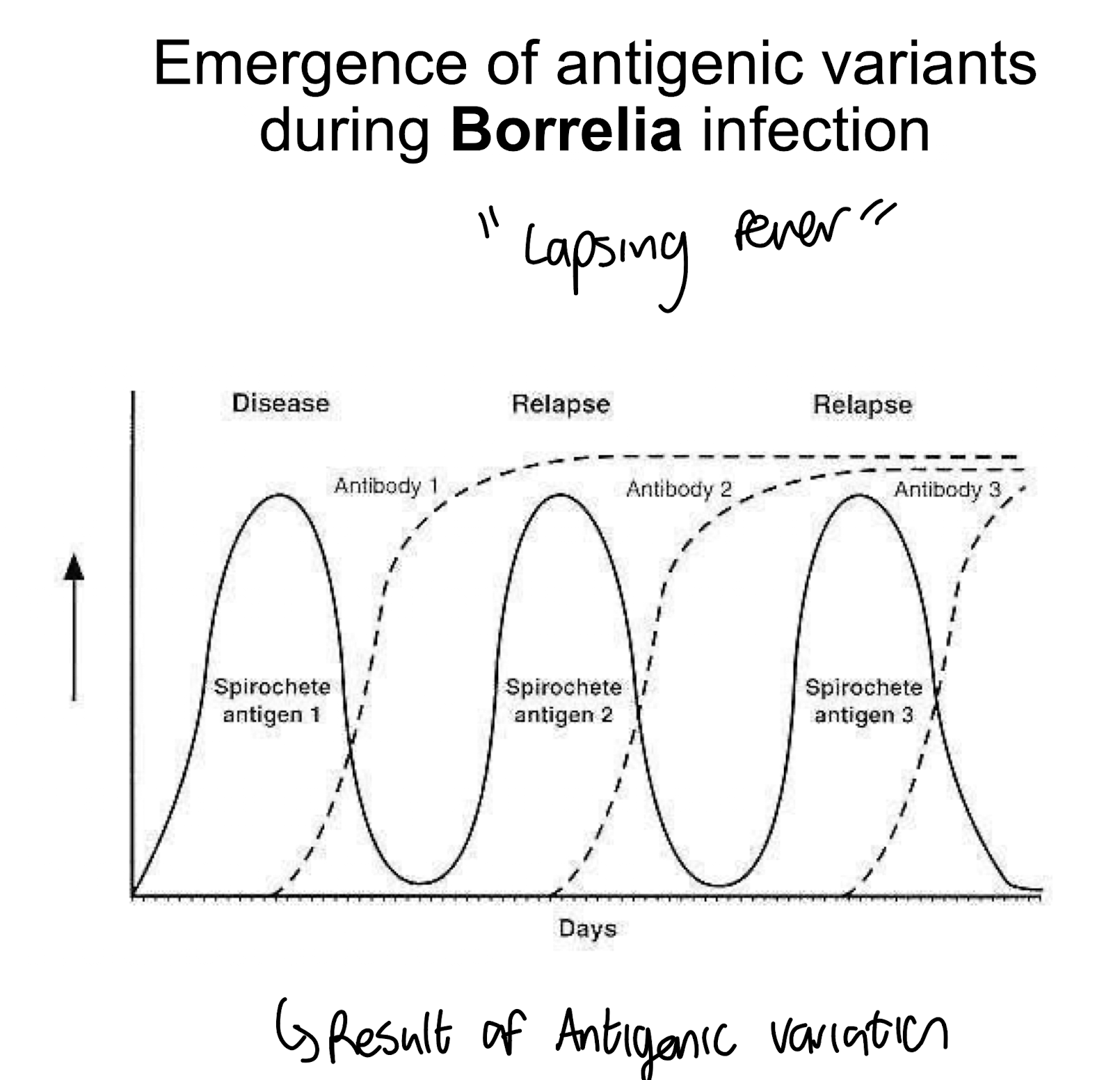
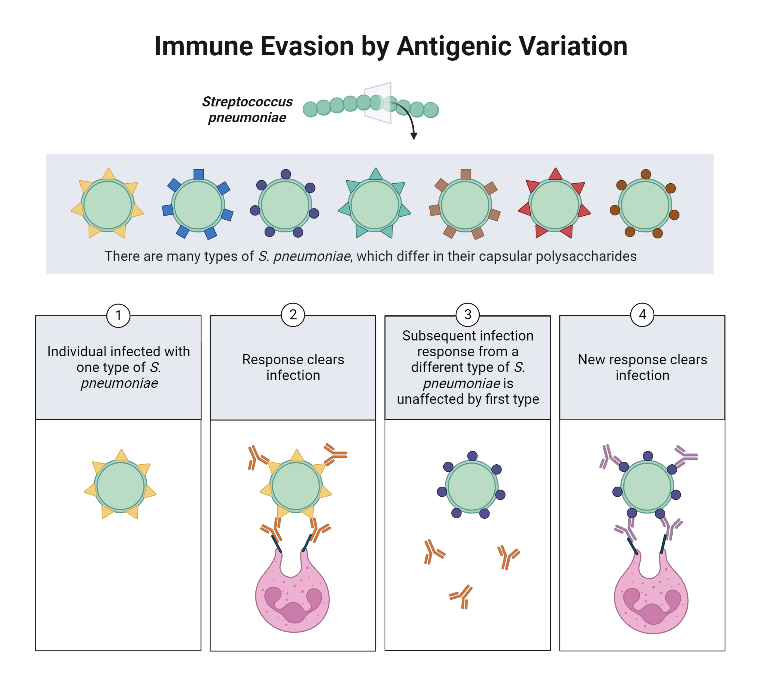
How do bacteria evade host defences by antigenic variation?
Pathogenic bacteria can change surface proteins, especially OMP, that are the targets of antibodies.
• This makes the original antibody response obsolete by using new proteins that do not bind the previous Ab
e.g. Seen in Borrelia infections → Lapsing fever
6 main virulence factor types?
Adherence factors
Invasion factors
Capsules
Exotoxins
Endotoxins
Siderophores
What are exotoxins?
They are heat-labile proteins secreted predominantly by Gram-positive bacterial cells into their surrounding environment during exponential growth, without disrupting its cell structure, and have varying levels of potency ranging from mild to lethal
Main features of exotoxins
• Strongly antigenic and elicit specific antibodies called antitoxins.
• Tissue-specific.
• May act at the site of colonisation and play a role in invasion or act at tissue sites remote from the original point of bacterial invasion or growth.
• May be modified chemically by phenol or formaldehyde to produce a toxoid.
Toxoid
a chemically modified exotoxin that is no longer toxic but retains the ability to stimulate an immune response.
How are exotoxins classified?
Their cellular or tissue target of action
e.g. enterotoxins, neurotoxins
Their mechanisms of action
i.e. proteolytic toxins, adenosine diphosphate [ADP]-ribosylating toxins, adenylate cyclase toxins
The organisms that produce them
e.g. pertussis toxin, cholera toxin
Their major biologic effects
e.g. dermonecrotic toxin, oedema-producing toxin
Their intracellular targets
e.g. small molecular-weight G proteins such as Rho
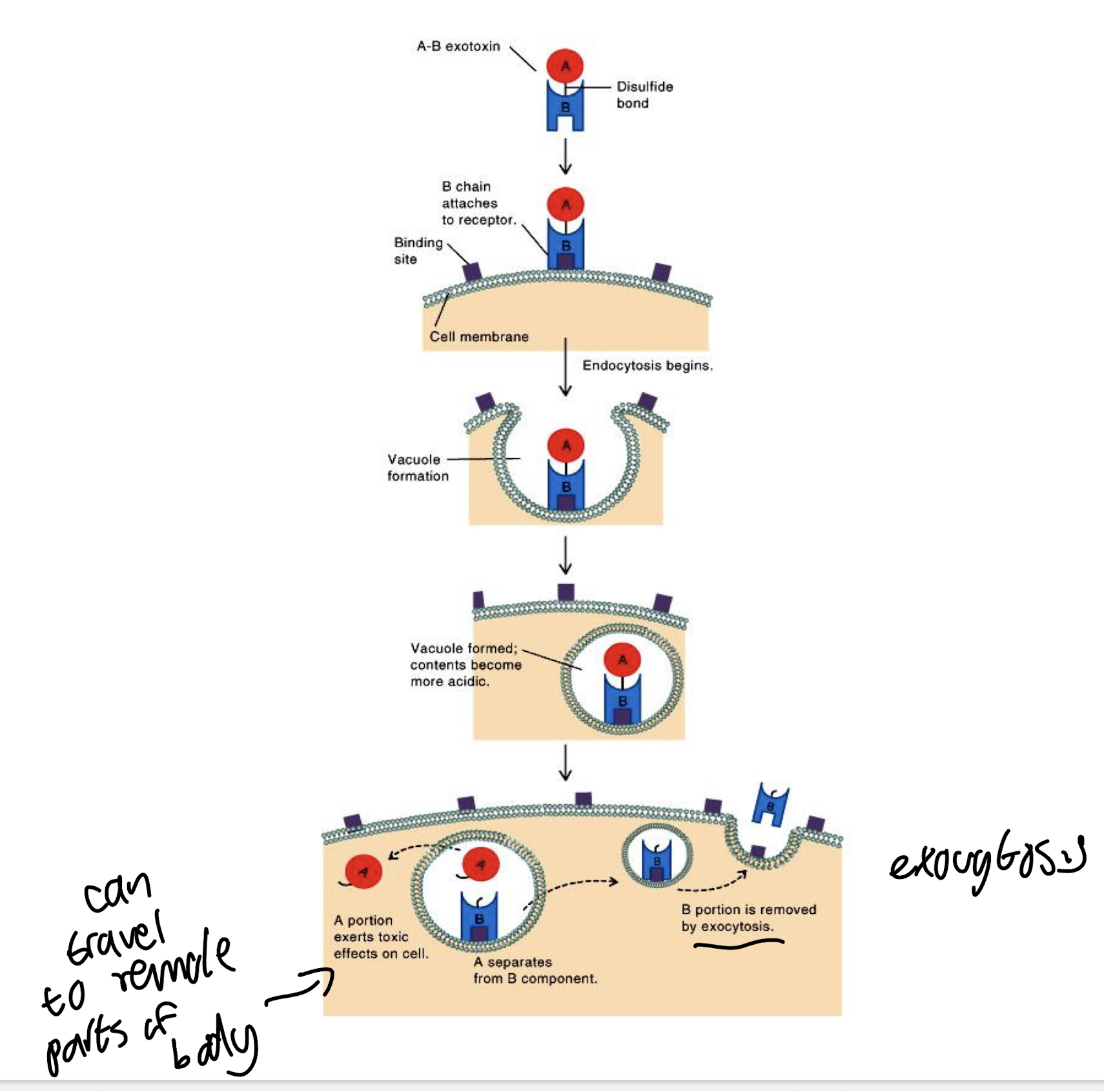
What is the structure and function of A-B exotoxins?
Made of two portions:
B portion binds to specific receptors on target cells via specific surface molecules, allowing entry of the A portion, determines host cell specificity of the exotoxin
A portion mediates toxic activity, typically acting by removing the ADP-ribosyl group from NAD, attaching it to. host cell proteins causing protein malfunctioning/inactivation
e.g. diphtheria toxin. shiga toxin and cholera toxin
How do membrane disrupting exotoxins work?
• Lyses host cells by disrupting the plasma membrane.
Two known types:
Pore-forming in the membrane causing leakage of cytoplasm and water entry
Ones which act as phospholipase
• These toxins are cytotoxins because they can affect any host cell.
• Also referred to as "haemolysins" due to their effect on erythrocytes.
• Examples include listeriolysin and alpha-toxin.
What are ‘Superantigens’ ?
Exotoxins which can bind to MHC class II molecules on many antigen-presenting cells surfaces directly
• This leads to the stimulation of many T-cells and an excessive production of IL-2 and other inflammatory cytokines.
→ Exaggerated immune response can result in shock e.g. include toxic shock syndrome toxin-1 (TSST-1) of Staphylococcus aureus
What are endotoxins?
Toxins that are part of the outer-membrane of the Gram-negative bacterial cell wall i.e. LPS, released when the bacteria die or divide.
Trigger immune responses, causing fever and inflammation, and can lead to severe reactions in humans, such as septic shock.
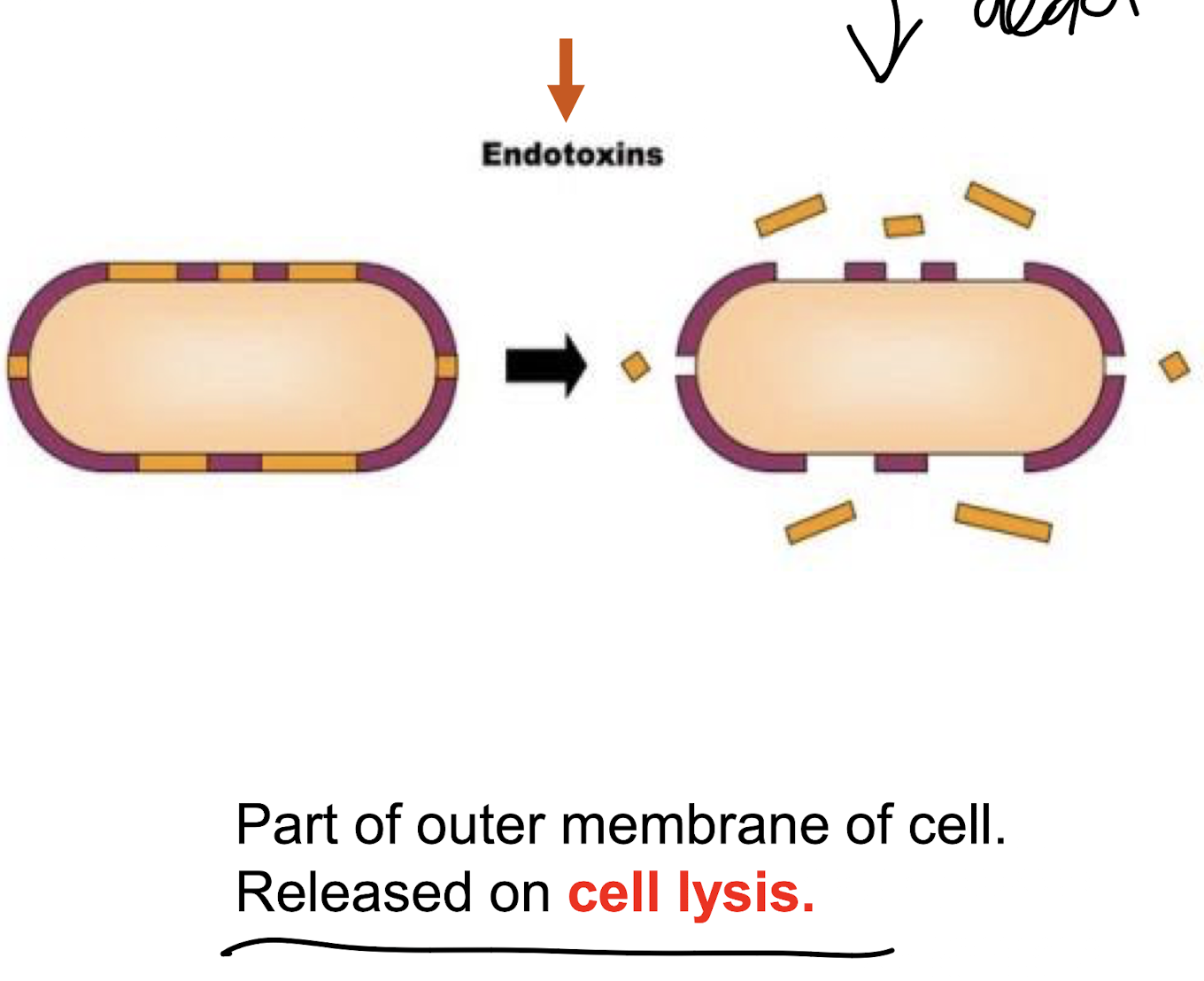
Features of endotoxins?
• Is exclusive to and an integral component of Gram-negative bacteria.
• Remain associated with the cell wall until disintegration of the bacteria.
• Relatively heat-stable, relatively less toxic.
• Similar toxicities for most tissues and cells.
• Not convertible to toxoids
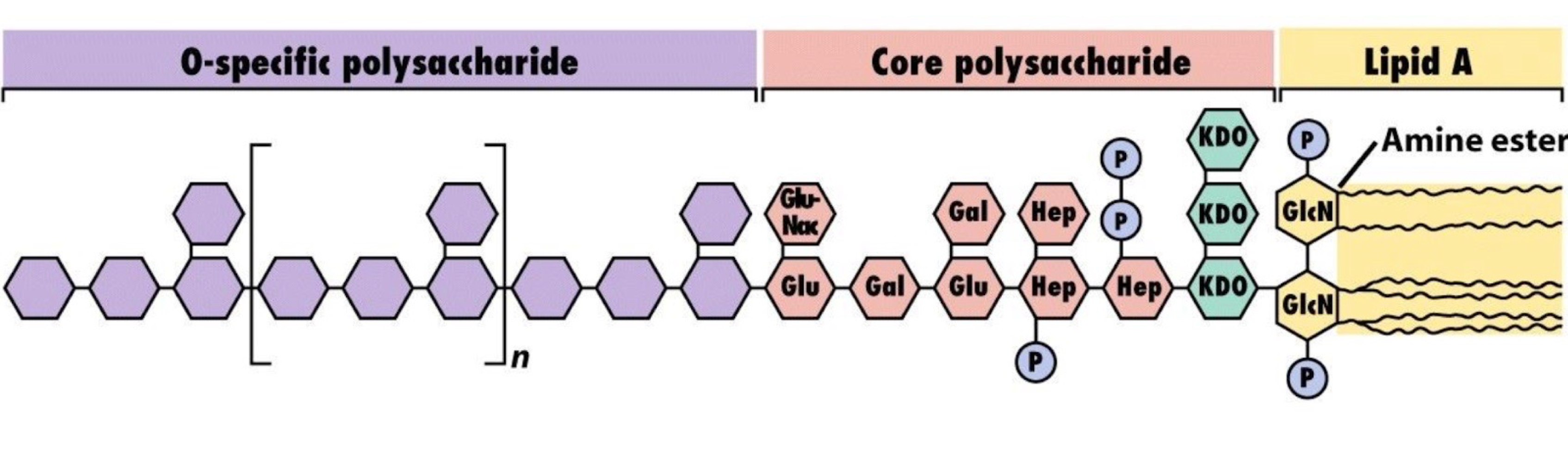
What are the 3 main components of LPS?
1. Lipid A → confers toxicity
2. Core (R) antigen → provides structural integrity to the LPS molecule.
3. Somatic (O) antigen or O polysaccharide → makes complex water soluble and enables immune recognition.
What are the 3 main inflammatory effects caused by the LPS endotoxin during Gram-negative bacteraemia?
1. Complement activation
2. Activation of several humoral systems resulting in:
– coagulation: a blood clotting cascade that leads to coagulation, thrombosis, acute disseminated intravascular coagulation
– plasmin activation which leads to fibrinolysis and haemorrhaging
– kinin activation releases bradykinins and other vasoactive peptides which causes hypotension
3.Stimulation of lysosomal enzymes, IL-1, TNF & other cytokines by macrophages
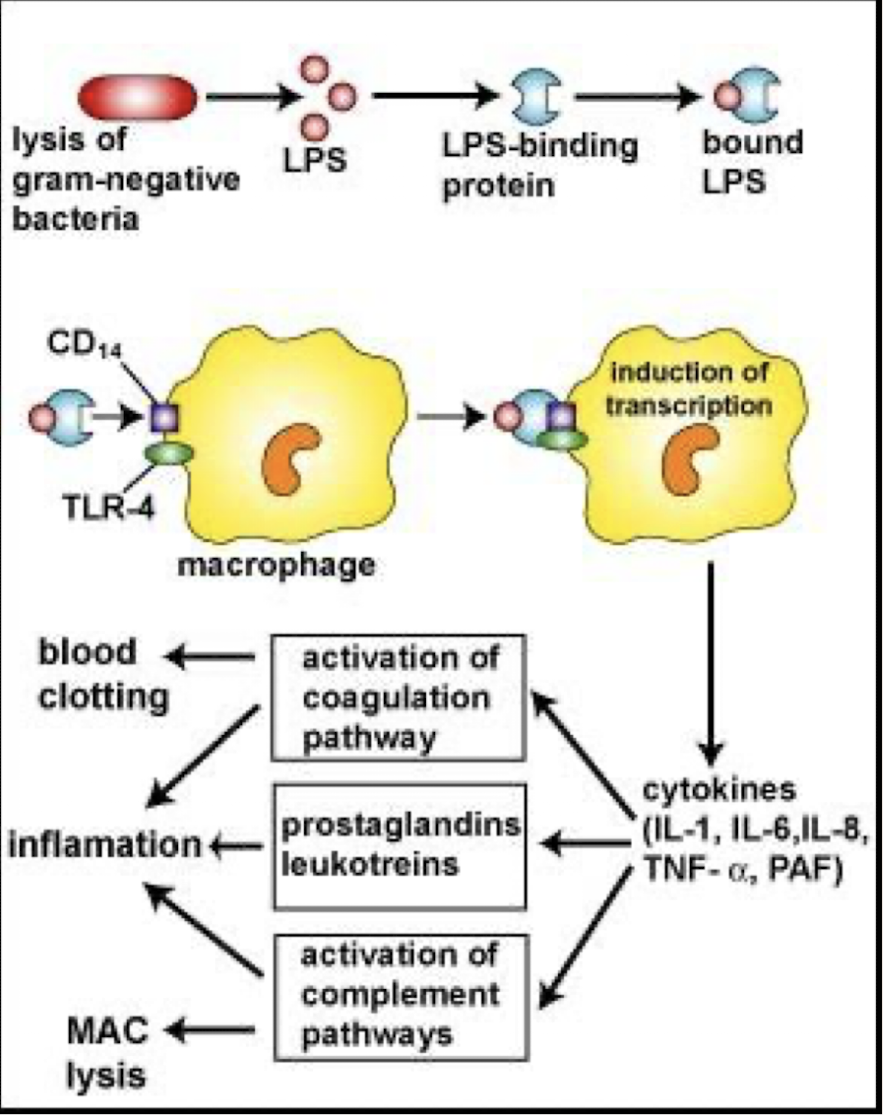
The net effect of LPS is to induce ________, __________, _________ and ____________
inflammation, intravascular coagulation, haemorrhage and shock.
Exotoxin vs Endotoxin summary
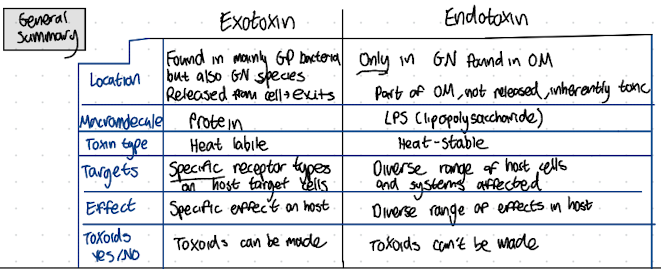
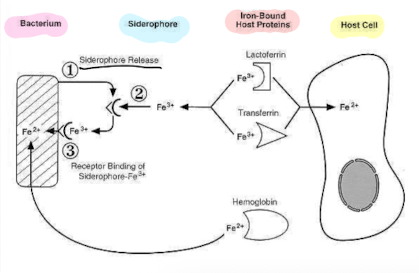
How is the use of siderophores by bacteria a virulence factor?
Siderophores are high-affinity iron-chelating compounds produced by bacteria to scavenge iron from the host.
This ability provides a critical nutrient advantage, enhancing bacterial survival and proliferation during infection.
• Bacteria need trace amounts of iron for growth, Fe in human body is tightly bound either in haemoglobin, transferrin or lactoferrin.
– high Fe2+ affinity
– acquire Fe2+ and deliver to bacteria