MB2080: Topic 5 - Liver Physiology
1/60
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
61 Terms
Main functions of the liver
metabolism
protein synthesis
protection & clearance of toxins
solubilise, transport & storage
Liver blood supply
hepatic artery — oxygenated blood from the heart to liver
hepatic portal vein — deoxygenated, nutrient & toxin-rich blood from gut spleen & pancreas to liver (for detoxification)
hepatic central vein — deoxygenated blood from liver to heart
Liver blood supply %
30% — hepatic artery
70% — hepatic portal vein
Liver lobule
hexagonal functional unit of the liver
Liver lobule structure
central (hepatic vein) in the middle
portal triad at each corner of the lobule
Sinusoids
blood vessels within the liver that run between hepatocytes
Bile canaliculi
channels between adjacent hepatocytes that collect bile and transport it toward larger bile ducts
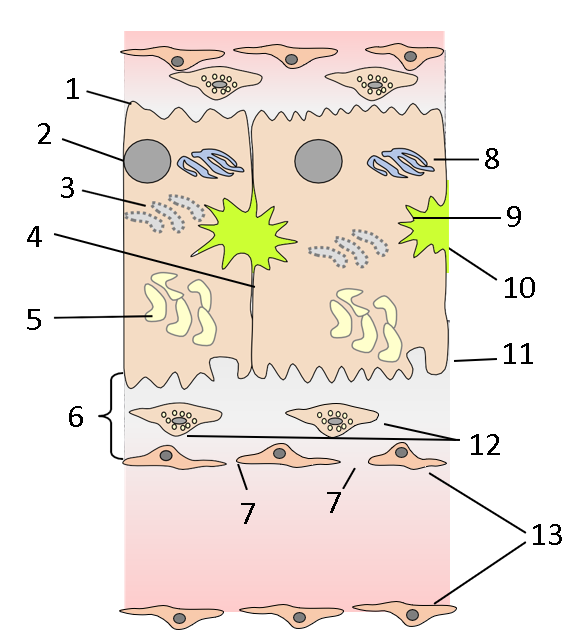
Label this diagram
microvilli
nucleus
RER
tight junction
SER
space of Disse
fenestrations
Golgi body
apical membrane
bile canaliculus
basolateral membrane
hepatic stellate cells
endothelium (of sinusoid)
Components of a portal triad
hepatic artery
hepatic portal vein
bile duct
Features of zone 1
peri-portal region
maximal oxygenation & nutrients
most resistant to circulatory compromise
1st to regenerate
Zone 1 reactions
amino acid catabolism
gluconeogenesis
glycogen degradation
ureagenesis
oxidative energy metabolism
Features of zone 3
peri-central region
minimal oxygenation
maximal toxins & metabolites
least resistant to circulatory compromise
Zone 3 reactions
lipogenesis
glycolysis
glycogenesis
bile acid biosynthesis
biotransformation of gas
Zone 2
mid lobular region
Effect of insulin on the liver
β-cells secrete insulin into blood stream (when blood glucose levels are high)
insulin binds to IRS-1 on the hepatocyte membrane
increased GLUT2 translocation to hepatocyte membrane leading to increased glucose uptake from the bloodstream
activation of glycogen synthase
activation of hexokinase
activation of acetyl CoA carboxylase to store excess glucose as triglycerides
Glycogen synthase
converts glucose into glycogen
Hexokinase
converts glucose to pyruvate
Acetyl CoA carboxylase
converts pyruvate to fatty acids to store excess glucose as triglycerides
Effect of glucagon on the liver
α-cells secrete glucagon into blood stream (when blood glucose levels are low)
reduced GLUT2 translocation to hepatocyte membrane leading to reduced glucose uptake from the bloodstream
activation of glycogen phosphorylase
activation of glucagon-6-phosphatase
releases glucose into the bloodstream
Glycogen phosphorylase
breaks down glycogen by catalysing the phosphorolysis of -1,4-glycosidic bonds
Glucose-6-phosphatase
converts glucose 6-phosphate to glucose releasing glucose into the bloodstream
Specific non-essential amino acids
alanine
glycine
proline
tyrosine
aspartic acid
glutamic acid
arginine
serine
cysteine
asparagine
glutamine
Non-essential amino acids
amino acids naturally synthesized by the body
Specific essential amino acids
histidine
isoleucine
leucine
lysine
methionine
phenyl-alanine
threonine
tryptophan
valine
Essential amino acids
amino acids not synthesized by the body which need to be absorbed from diet
Protein synthesis by hepatocytes
triggered by certain hormones (such as insulin)
influenced by the availability of amino acids
occurs in balance with protein degradation and intake
Proteins synthesized by the liver (and examples)
plasma proteins e.g. albumin
coagulation factors e.g. fibrinogen
pro-hormones e.g. angiotensinogen
lipoproteins e.g. low-density lipoprotein (LDL)
Function of lipoproteins
enable transport of insoluble lipids and cholesterol throughout the body
Examples of lipoproteins
chylomicrons (high content of triglycerides & cholesterol but minimal protein)
LDL (low density lipoprotein, high content of fats compared to protein)
HDL (high density lipoprotein, high content of protein compared to fats)
Protein catabolism
deamination of amino acids into α-keto acids and ammonia
Urea cycle
process of converting toxic ammonia into non-toxic urea for excretion from the body via the urine