Lecture 6: Anesthesia Monitoring Equipment (copy)
1/37
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
38 Terms
What are the 6 ACVAA monitoring guidelines?
1. Ensure adequate blood flow (circulation)
2. Ensure adequate arterial blood oxygenation
3. Ensure ventilation is adequately maintained
4. Ensure body temperature does not seriously deviate from normal
5. Maintain legal record of significant events and enhance recognition of trends in monitored parameters
6. Ensure responsible person is aware of patient status at all times during anesthesia and recovery
What diagnostics are involved in basic anesthetic monitoring?
•Anesthetic depth signs
•Heart/Pulse rate, rhythm and pulse quality
•Respiratory rate and effort
•Noninvasive blood pressure (NIBP)
•Temperature
•Mucous membrane color & CRT
•Pulse oximetry (SpO2)
•End tidal carbon dioxide (ETCO2) = capnography
What are the basic anesthetic depth signs?
Eye position
Respiratory rate and pattern
Muscle relaxation→Jaw and rear tone (knowt will not let me use actual word)
Heart/Pulse rate
Response to stimulation (procedure)
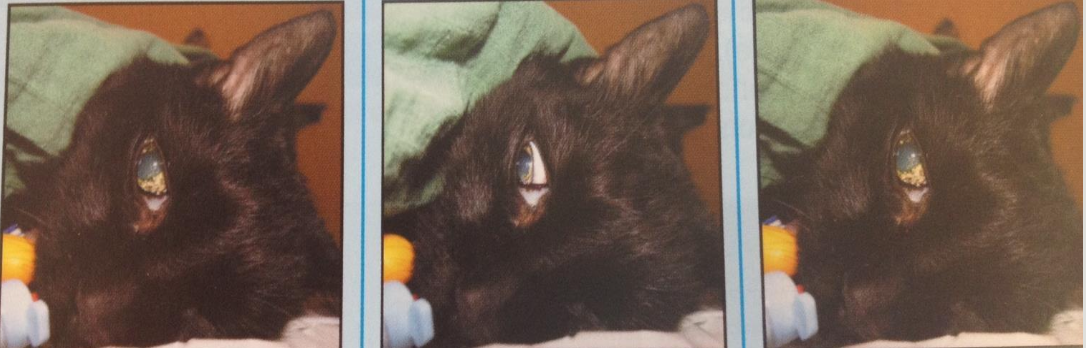
Which of these has adequate anesthesia and why?
the middle because the eye is rotated
When monitoring depth, how can you evaluate heart/pulse rate and rhythm?
1. Palpate pulses or heart beating
2. Esophageal or regular stethoscope
3. Ultrasonic Doppler device to detect the sound of blood flow in the artery.
4. ECG
5. SpO2-plethysmograph wave
What anesthetic depth information does pulse quality give?
subjective measurement of arterial filling and pressure → some idea of stroke volume and vasoreactivity
What are some sites to evaluate pulse quality for SA and LA?
femoral pulse
tongue
lateral saphenous
LA: transverse facial artery and jugular vein
What does each part of the ECG represent
P wave: atrial depolarization (contraction)
PR interval: time it takes for the electrical impulse to travel from SA node, through the atria, to the AV node, and into the ventricles, marking the delay before ventricular depolarization (QRS complex) begins
QRS complex: ventricular depolarization
ST segment: plateau when ventricles are contracting
T wave: ventricular repolarization (resetting)
What are the clinical uses for ECG besides HR and rhythm?
electrolye abnormalities
How are small animal (lead II) ECG leads placed?
◦ White lead ➔ Right elbow
◦ Black lead ➔ Left elbow
◦ Red lead ➔ Left stifle or abdomen
How are large animal (lead I or base apex) ECG leads placed?
◦ White lead ➔ Right jugular furrow
◦ Black lead ➔ left axilla region
◦ Red lead ➔ Any site remote from the heart
How are respiratory rate and effort evaluated during anesthetic depth monitoring?
1. Start by observing the patient’s thorax or the movement of reservoir bag
2. Esophageal stethoscope – passed to level of the heart
3. Various breathing frequency monitors can be employed ➔ give off an audible “beep”
4. Respirometer can be used to determine tidal volume (TV) and minute volume
5. Capnograph may also display RR Look at the wave!
What are the 2 main indirect noninvasive methods for obtaining blood pressure?
doppler and oscillometric
How does a doppler measure blood pressure?
use inflatable cuff to occlude blood flow in an artery, as the pressure in the cuff is released the Doppler detects the return of blood flow by reflection of sounds waves from moving RBCs
Where is a blood pressure cuff placed on dogs and cats?
the cuff goes on a limb (forelimb or hindlimb) or the tail base, and the probe is placed distal (further down) to the cuff, over an artery
Why should Doppler reading be kept > 80-90mmHg?
to be sure patient is not hypotensive
How is oscillometric blood pressure measured?
Blood flow through the arteries causes vibrations in arterial wall ➔ translated to air in the blood pressure cuff➔ detected and transduced into electrical signals to produce a reading
What are the advantages and disadvantages of doppler blood pressure?
Advantages:
Audible pulse rate and rhythm
Some technical skills required to place, but able to quickly obtain reading
Disadvantages:
Does not give you all variables, SAP/DAP/MAP
Not as accurate as direct BP, especially as patient becomes hypotensive
Accuracy affected by selecting correct cuff size
What are the advantages and disadvantages of oscillometric blood pressure?
Advantages:
Easy to place on limb
Some can be set to run automatically
Determines HR, SAP, MAP, and DAP
Disadvantages:
Actual pressure reading takes longer than Doppler
Not as accurate as Doppler method, especially in the following situations (but constant improvement): hypotensive patient, small patients, patient movement, arrhythmias, vasoconstriction
How is temperature monitored during anesthesia?
thermometer or temperature probe positioned in esophagus, intranasally, or in rear (knowt won’t let me use the actual word)
What does MM color and CRT grossly assess during anesthetic monitoring?
patient perfusion
What indirectly estimates % oxygen saturation of Hb and also displays the pulse rate (plethysmograph)?
SpO2
How is SpO2 measured?
Spectrophotoelectric device is applied over non-haired skin with pulsatile blood flow → Red and infrared light are absorbed differently by oxygenated and deoxygenated Hb. This difference is calculated and the % Hb saturation is displayed numerically
What SpO2 value is indicative of severe hypoxemia?
SpO2 of 90% = PaO2 of 60 mmHg
What effects the accuracy of SpO2?
•poor circulation due to vasoconstriction, hypotension, hypothermia
•movement artifact
•pigmentation
•tissue thickness
•anemia
•carbon monoxide and cyanide poisoning ➔ falsely high reading
•methemoglobinemia ➔ reads in the mid 80’s
•ambient light?
What is ETCO2?
inspired and expired CO2 concentration measured by capnography
What is a normal ETCO2?
35-45 mmHg
What is increased ETCO2 indicative of?
hypoventilation, hyperthermia
What is decreased ETCO2 indicative of?
hyperventilation, airway obstruction, hypothermia, decreased cardiac
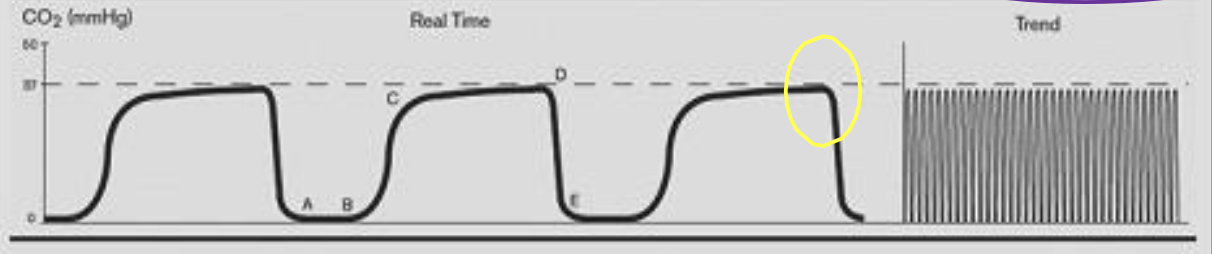
This is a normal capnograph. What do A-B, B-C, C-D, D, and D-E represent?
A-B: baseline
B-C: expiratory upstroke
C-D: expiratory plateau
D: end-tidal concentration
D-E: inspiration


Which capnography sensor is which?
top: sidestream
bottom: mainstream
How does capnography work?
CO2 produced in cells → carried to lungs → exhaled
CO2 molecules absorb infrared light → concentration determined by comparing measure absorbance with know standard
How is capnography a useful monitoring tool?
RR and estimation of PaCO2
Diagnose disconnection or leak, V/Q mismatch, alveolar dead space, bronchoconstriction, airway obstruction, decreased cardiac output, return of spontaneous circulation during CPR, rebreathing of CO2
determine if patient is correctly intubated
What are the normal temperature limits under general anesthesia?
98-102.5
What are the normal HR limits under general anesthesia for dogs, cats, horses, and ruminants?
dogs: 50-160
cats: 100-200
horse: 28-50 (foal up to 80)
ruminants: 48-90 for cows and 60-150 for sheep or goats
What are the normal respiration limits under general anesthesia?
10-20 bpm
What are the normal SpO2 limits under general anesthesia?
95-100%
What are the normal blood pressure limits under general anesthesia?
Hypotension defined as MAP < 60 and SAP < 80 (equine keep MAP > 70)