human microbiota
1/14
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
15 Terms
what is microbiota
they are groups of micro-organisms living in a specific environment
they are not usually harmful and are actually vital to our health
individuals microbiota is unique to their age, diet lifestyle and the time of year
they can be describes as indigenous human commensals as they benefit from being on the human and the human also benefits from them being there as they protect against pathogens
but they can be opportunistic pathogens as they can cause harm if normal conditions change like during burns, injury weakened immunity and they can cause disease.
what is the function of the gut microbiome
it is essential for the breakdown of our food
synthesis of vitamins B12 and vitamin K
potentially involved in obesity, allergies, immune disorders too
describe the microbiota on the skin
its divided into 3 microenvironments
dry skin ( arms and legs ), moist skin areas ( armpits ), areas rich with sebaceous glands ( oily skin )
typically contains gram positive bacteria ( they contain a thick cell wall resistant to drying )
e.g streptococcus and staphylococcus
they dont usually cause disease but skin wound can lead to infection
e.g staphylococcus aureus
describe the microbiota on the upper respiratory tract ( nose and throat )
extensive bacterial flora
typically consists of streptococcus and staphylococcus
bacteria like , Neisseria meningitidis and haemophilus influenzae can cause bacterial meningitis
describe the microbiota in the lower respiratory tracts ( trachea, lungs )
it is usually sterile
but its a common site of infection typically chest infections and pneumonia and tuberculosis
describe the microbiota in the digestive system- mouth
its a very complex microbial ecosystem
the mouth is split into different micro-environments: tongue, cheeks gum, teeth
cheeks and gums- facultative aerobes (e.g. streptococcus)
tooth enamel- facultative aerobes ( e.g. streptococcus )
where the teeth meets the gum- anaerobes
e.g. Bacteroides, actinomyces= they can cause gum disease and
describe the microbiota in the main digestive system ( the stomach, small intestines and large intestines)
stomach
acidic environment with less than 10CFU/ml ( colony forming units )
Heliobacter pylori which may cause stomach ulcers are present
small intestines
the duodenum has around 103 -104 CFU/ml
the ileum has more due to being even less acidic around 105 - 107 CFU/ml
large intestines
contains the must microbiomes
big mix of gram positive and gram negative bacteria unique to the person
they contain anaerobes and facultative anaerobes. the most common is Bacteroides fragilis and Escherichia coli ( e.coli)
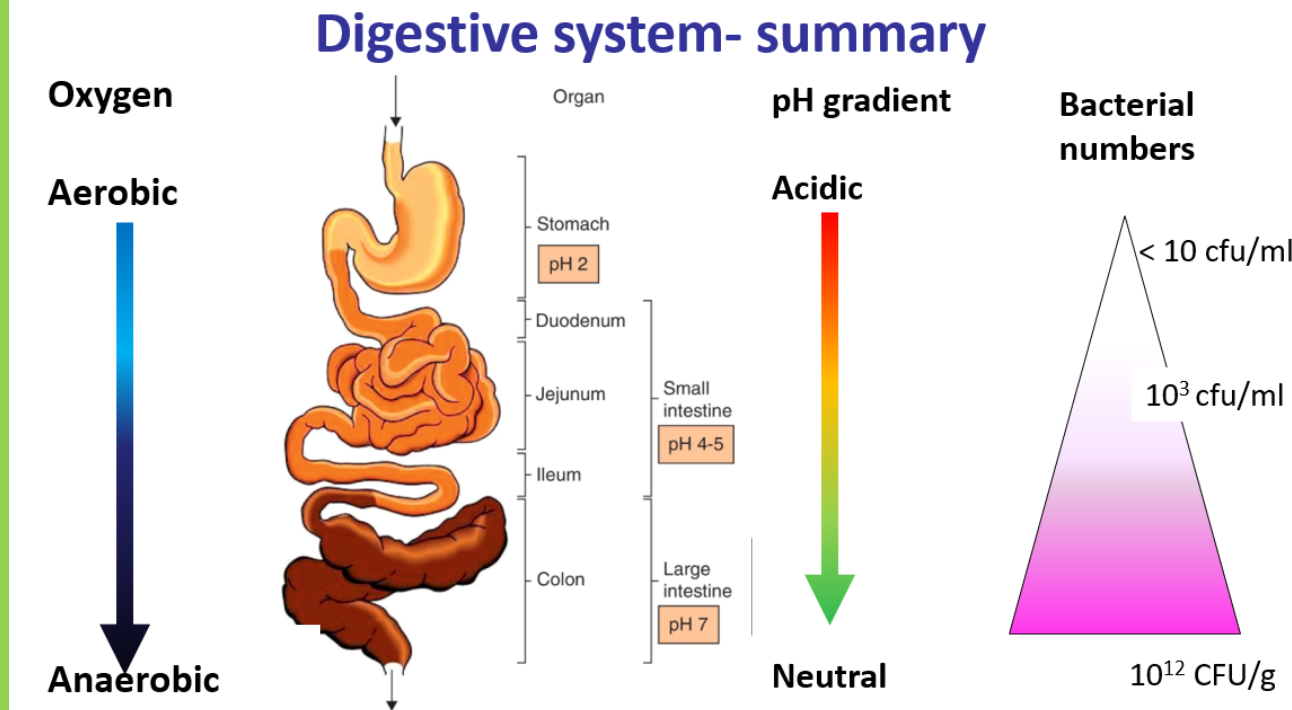
when acidity decreases what happens to the bacterial growth
bacterial growth increases
e.g. the small intestines compared to the stomach
describe the microbiota in the urinary tract
kidneys, ureters and bladder
usually sterile as otherwise can cause kidney infection
urethra
it has a flushing effect which removes most bacteria but ones like e.coli contain small like hair
lightly colonised. typically staphylococcus epidermis
its a frequent site of infection ( UTI) due to e.coli
describe the microbiota in the female genitalia tract
it contains a very complex microbiota, which depends of age, childbirth, menstrual cycle and menopause
the vagina is an acidic environment
it contains candida albicans ( a yeast ) that can cause a thrush infection infection
since we are already covered in bacteria why don’t we get more infections ?
as we have various barriers to infection,
what are the barriers against infection
the natural microflora must compete with the pathogens for adhesion to sites and food
the skin which acts as a physical barrier
there are also mucosal defences
non-specific defences: blood and tissues
explain how the skin is able to act as a physical barrier against pathogens
epidermis ( thin outer layer )
physical barrier
dry, acidic
shedding cells
indigenous bacteria decrease colonisation
sweat glands
they produce lysozyme which break down peptidoglycan so the gram positive bacteria are more prone to the break
sebaceous glands ( associated with hair follicles )
lysosomes
oily sebum which is acidic
these both inhibit bacterial growth
lymphoid tissue
induces local inflammatory response
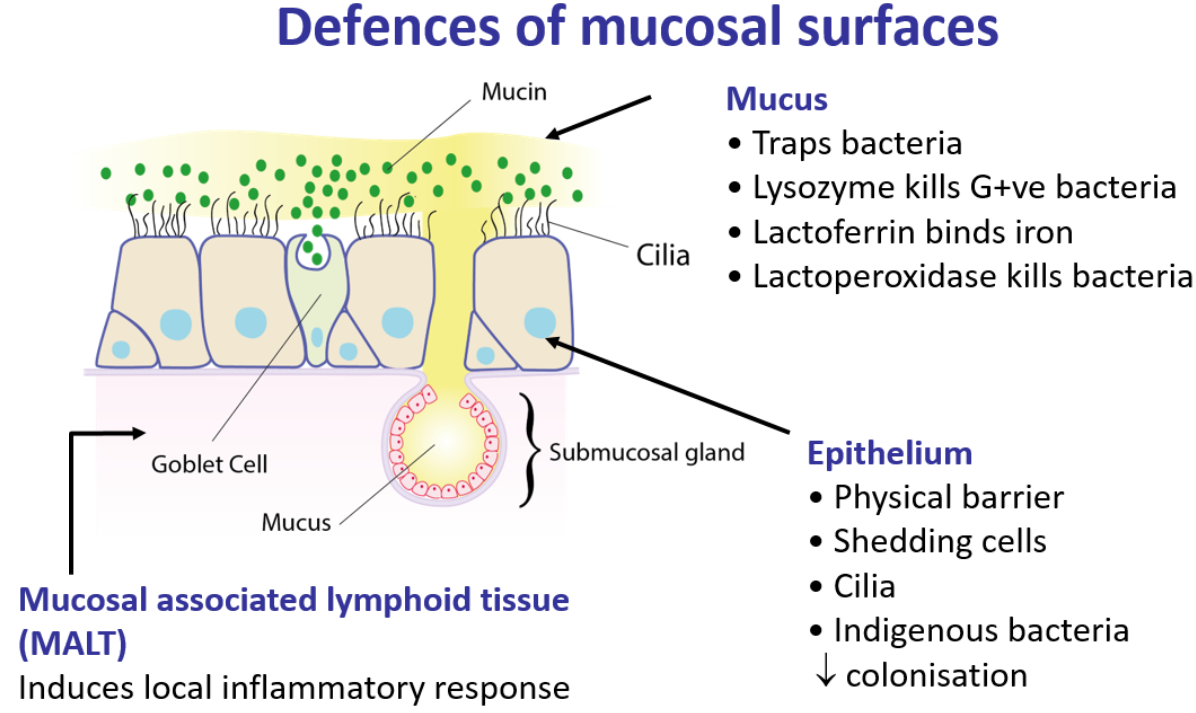
what are the barriers/defences of the mucosal surfaces
mucus
it traps bacteria
has lysozyme that kills gram positive bacteria
lactoferrin that binds iron
lactoperoxidase which kills bacteria
epithelium
acts as a physical barrier
shedding cells
cilia
indigenous bacteria which decrease colonisation
lymphoid tissues
induces local inflammatory response
what are the barriers to infection in the blood and tissue
there are a variety of cells that go and mop up pathogens
this is done by the granulocytes- basophils, neutrophils and eosinophil they are activated when there’s inflammation
also monocytes which can go onto produce macrophages and they can kill bacteria by phagocytosis
there are also other defences such as the: complement system, transferrin and mannose-binding lectin