Pleural Disease - Clin Med 2
1/42
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
43 Terms
What does this refer to
Accumulation of fluid in the pleural space due to the manifestation of underlying disease
Nearly half of all pleural effusions in the United States are accounted for by a combination of lung cancer and breast cancer
Pleural effusion
What does this refer to
Recent respiratory infections or fever, specifically ask about pneumonia
History of CHF, renal or liver impairment, pulmonary hypertension, PE, malignancies (or red flag symptoms), occupational history, medication use
History of Pleural Effusion
What does this refer to
Fluid accumulation in the pleural space is a common occurrence caused by both benign and serious conditions.
United States alone, it is estimated that approximately 1.5 million cases of pleural effusions are diagnosed annually, with 16% requiring thoracentesis
Epidemiology of Pleural Effusion
What does this refer to

Pathophysiology of Pleural Effusion
What does this refer to (Classification of Pleural Effusion)
Imbalance of fluid forces (hydrostatic)
Protein forces (oncotic) external to pleural space.
Transudative
What does this refer to (Classification of Pleural Effusion)
Disease process
Systemic
Focal
Exudative
What does this refer to
Vary with etiology
Small amount of fluid is usually asymptomatic
MC symptoms are dyspnea, cough, and pleuritic chest pain
Presentation of Pleural Effusion
What does this refer to
Vary depending on etiology
Specific to respiratory system
Nonspecific
Small amount usually asymptomatic
Three most common symptoms are dyspnea, cough, and pleuritic chest pain.
Exertional dyspnea (rapid)
Severity correlates with effusion size
Cough
Nonspecific mild and nonproductive
Severe-(infective)
Fever, sweating and fatigue
Pleuritic Chest Pain
Degree of inflammation
Signs and Symptoms of Pleural Effusion
What does this refer to
Large effusion may result in contralateral tracheal shift, asymmetric chest expansion, and tachypnea
Decreased or absent tactile fremitus, dullness to percussion over the fluid area, and uni- or bilaterally diminished or absent breath sounds
Pleural friction rub heard on auscultation if inflammatory process or post thoracentesis
Physical Examination of Pleural Effusion
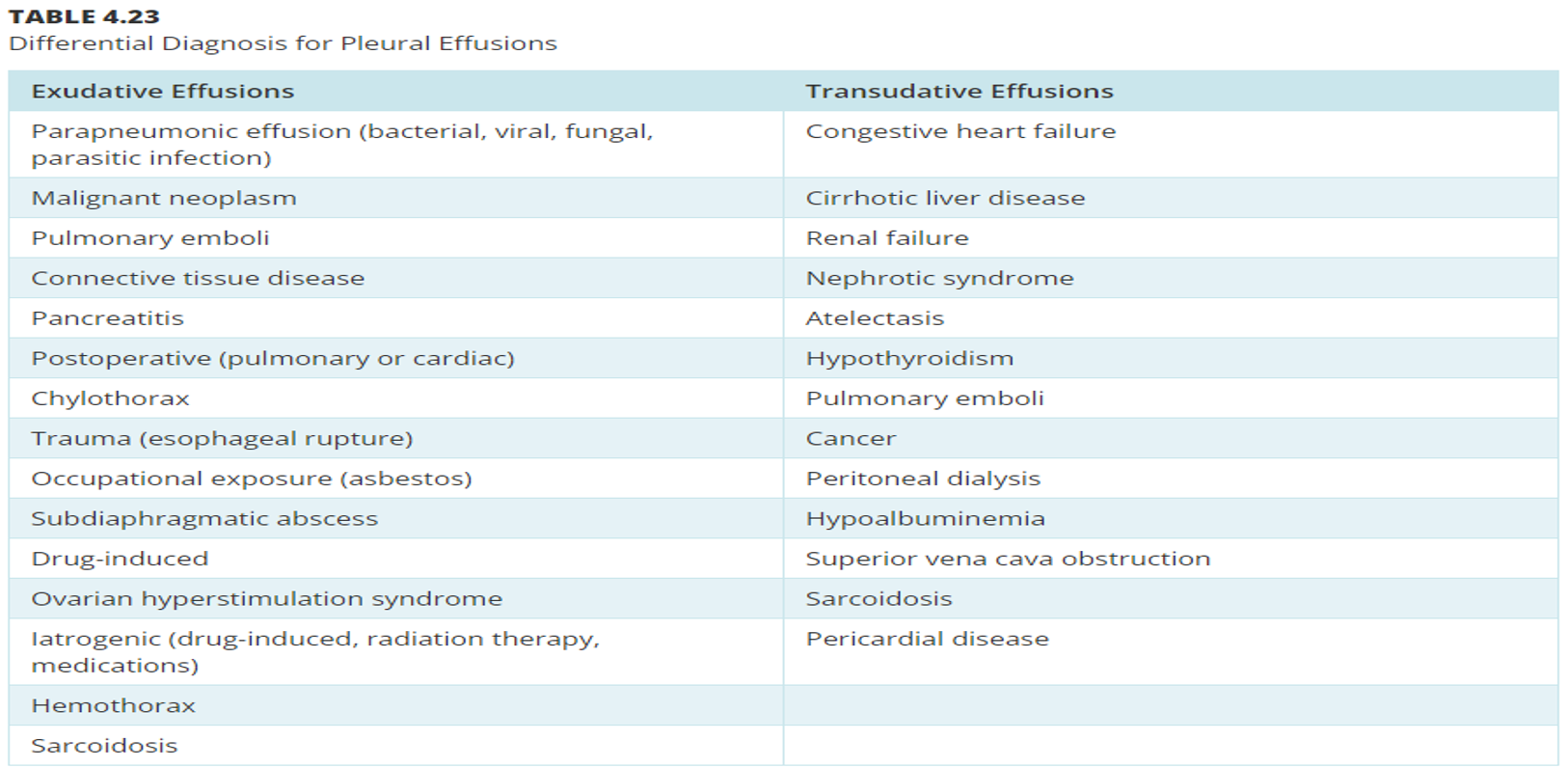
What does this refer to
Differential Dx of Pleural Effusions
What does this refer to
Chest US or CXR, possible CT
Thoracentesis and fluid analysis
Diagnostic Studies of Pleural Effusions
What does this refer to

Exudates
What does this refer to
Varies by primary condition
Symptomatic patients may require a large-volume thoracentesis and/or insertion of a pleural drain
Asymptomatic patients and patients with transudative pleural effusions, in general, do not require tube thoracostomy or pleural interventions but are closely followed (every 3 to 6 weeks) for clinical and radiographic observation.
Management of Pleural Effusion
What does this refer to
Treat underlying disorder
Possibly Abx Therapy, Diuretics, ultrafiltration, & Anticoagulation
Symptomatic
Thoracentesis
+/- insertion of pleural drain
Treatment for Pleural Effusion
What does this refer to
Water on the lungs
Common and several diseases can cause this effusion
Heart failure most common
Severity/seriousness depends on primary cause
Treatment based on symptoms
Recurrent effusions, may need meds to stop fluid
Fluid accumulation ongoing could be cancer.
Patient Education of Pleural Effusion
What does this refer to
Abnormal collection of gas, usually air, in the pleural space and subsequent collapse of the lung
Pneumothorax
What does this refer to
2 forms
Nonspontaneous (Traumatic and iatrogenic)
Known precipitating factors
Spontaneous (Primary and Secondary)
No obvious precipitating factors
male-to-female ratio of 3.3:1
average age of 34 years old for males and 40 for females
Tall, thin, male
Connective tissue disorders
Smoking
Scuba diving, high altitudes and flying
Epidemiology of Pleural Disease
What does this refer to
A ________ is the presence of air or gas in the pleural space due a breach in the visceral or parietal pleura, either by trauma or spontaneous rupture.
opposing forces provide a slight suction on the lung to keep it expanded throughout the respiratory cycle
Air enters the pleural space from loss of integrity of the chest wall or alveolar sac
The exact pathogenesis of spontaneous alveolar rupture is unclear
Pathophysiology of Pneumothorax
What does this refer to
Clinical presentation and medical history vary depending on the type of pneumothorax
The chest pain typically resolves within 24 hours
Primary Spontaneous Pneumothorax
What does this refer to
Varied based on type
Development closely correlated with underlying disease
Abrupt onset of dyspnea and pleuritic chest pain on ipsilateral side
History of significant risk factors including recent accident or trauma, smoking, malignancies, COPD, infection (especially HIV, Pneumocystis jiroveci, toxoplasmosis and Kaposi sarcoma), illicit drug use, air travel should be considered.
A history of prior pneumothorax is important as the recurrence rate is high
History of Primary Spontaneous Pneumothorax
What does this refer to
Varied based on severity and cause
Chest tightness.
Easy fatigue.
Rapid heart rate.
Bluish color of the skin caused by lack of oxygen.
Nasal flaring.
Chest wall retractions.
MC are chest pain and dyspnea
Usually thin, tall adolescent males is typically greatest risk
Presentation of Primary Spontaneous Pneumothorax
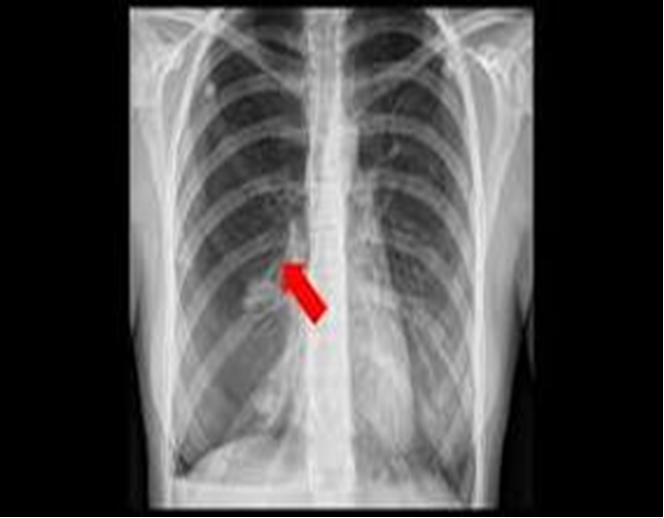
What does this refer to
Ranging from normal to severe distress
Possible unequal breath sounds, hyperresonance with percussion on ipsilateral side, decreased tactile fremitus, tachycardia, pulsus paradoxus, hypotension, jugular venous distention
Physical Examination of Primary Spontaneous Pneumothorax
What does this refer to
CT
High index of suspicion in an unstable patient requires immediate needle decompression
Diagnostic Studies for Primary Spontaneous Pneumothorax
What does this refer to
Observation and supplemental oxygen for all patients
Additional considerations
Treatment of the underlying lung disease, simple aspiration, tube or catheter thoracostomy, thoracoscopy, mechanical ventilation
Management of Primary Spontaneous Pneumothorax
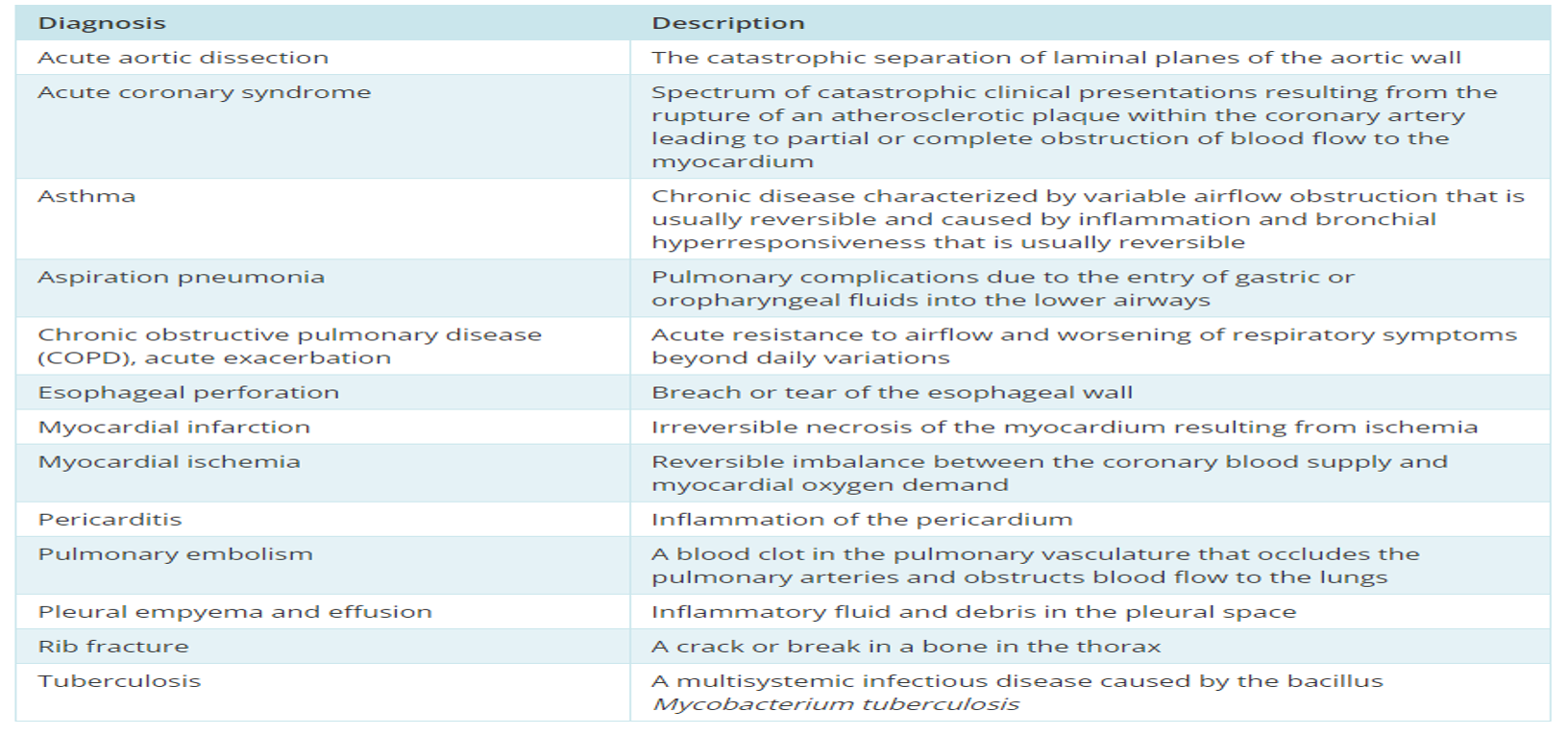
What does this refer to
Differential Dx of Primary Spontaneous Pneumothorax
What does this refer to
Diagnosis of pneumothorax is based on clinical suspicion and the history and physical examination are key to the diagnosis
Clinical interpretation of the presenting signs and symptoms is crucial for the correct diagnosis
Unstable patients with a clinical high suspicion of a pneumothorax require urgent decompression with needle decompression or tube thoracostomy before imaging.
In stable patients, the presence of the pneumothorax should be confirmed by imaging, which will also provide information on the extent and possible cause.
Evaluation of Primary Spontaneous Pneumothorax
What does this refer to
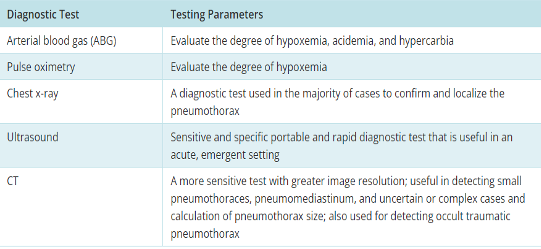
Diagnostic tests for pneumothorax
What does this refer to
Observation and supplemental oxygen therapy are recommended for all patients with a ________. Oxygen therapy accelerates the rate of pleural air absorption. In asymptomatic patients with small ________, oxygen administration is usually the only treatment needed.
Observation
Supplemental oxygen
Treatment of the underlying lung disease
Simple aspiration
Tube or catheter thoracostomy
Thoracoscopy
Mechanical ventilation
Treatment of a pneumothorax depends not only on the clinical setting but also on the etiology and associated comorbidities
Treatment for pneumothorax
What does this refer to

Patient education for pneumothorax
What does this refer to
Condition in which the pleura becomes inflamed. Sharp chest pain that worsens with deep breathing (coughing, sneezing, and chest wall movements)
Viral infx most common but can be pneumonia (MRSA)
Treat with NSAIDS such as ibuprofen
Pleuritic Chest Pain
What does this refer to
Innervated by somatic nerves (which senses pain due to trauma/inflammation
Inflammation then triggers local pain receptors
Phrenic nerve innervated the diaghragm (which causes the referred pain ipsilateral neck/shoulder)
Pathophysiology of Parietal Pleura
What does this refer to
Diaphoresis
Nausea
Palpitations
Pain-Sharp pain and stabbing is typical for noncardiac chest pain
Near the diaphragm, get referred pain to neck and/or shoulder
Presentation of Pleuritic Chest Pain
What does this refer to
Audible raspy breathing on auscultation
Tachycardia
Tachypnea
Physical Exam of Pleuritic Chest Pain
What does this refer to
Pericarditis
Costochondritis
Pneumonia
Differential Dx ofPleuritic Chest Pain
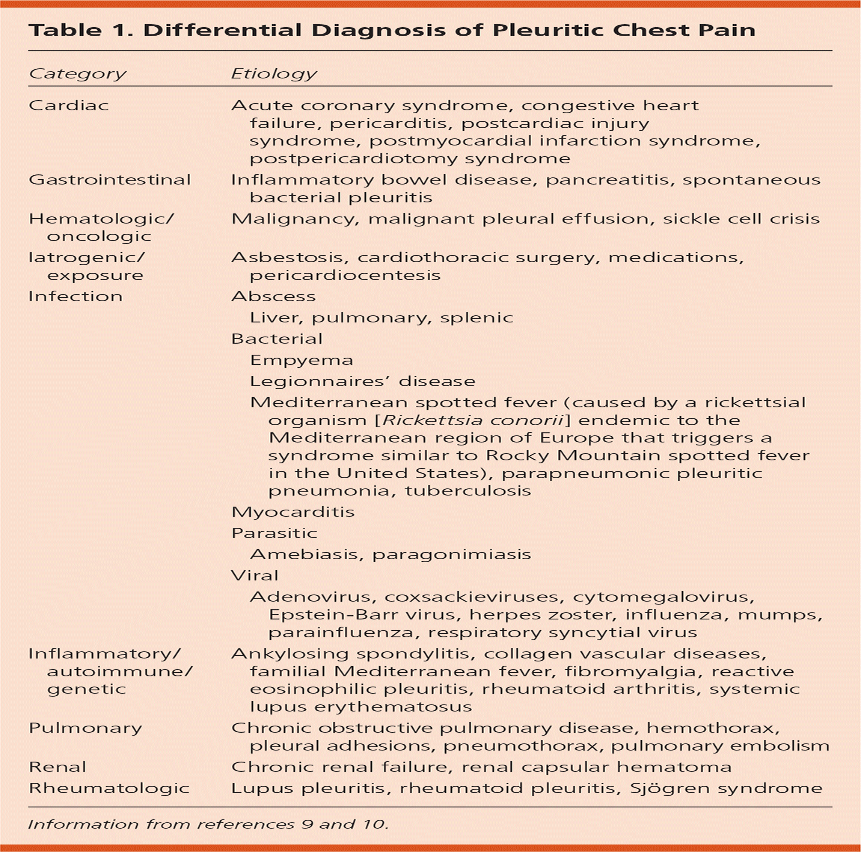

What does this refer to
Differential Diagnosis of Pleuritic Chest Pain
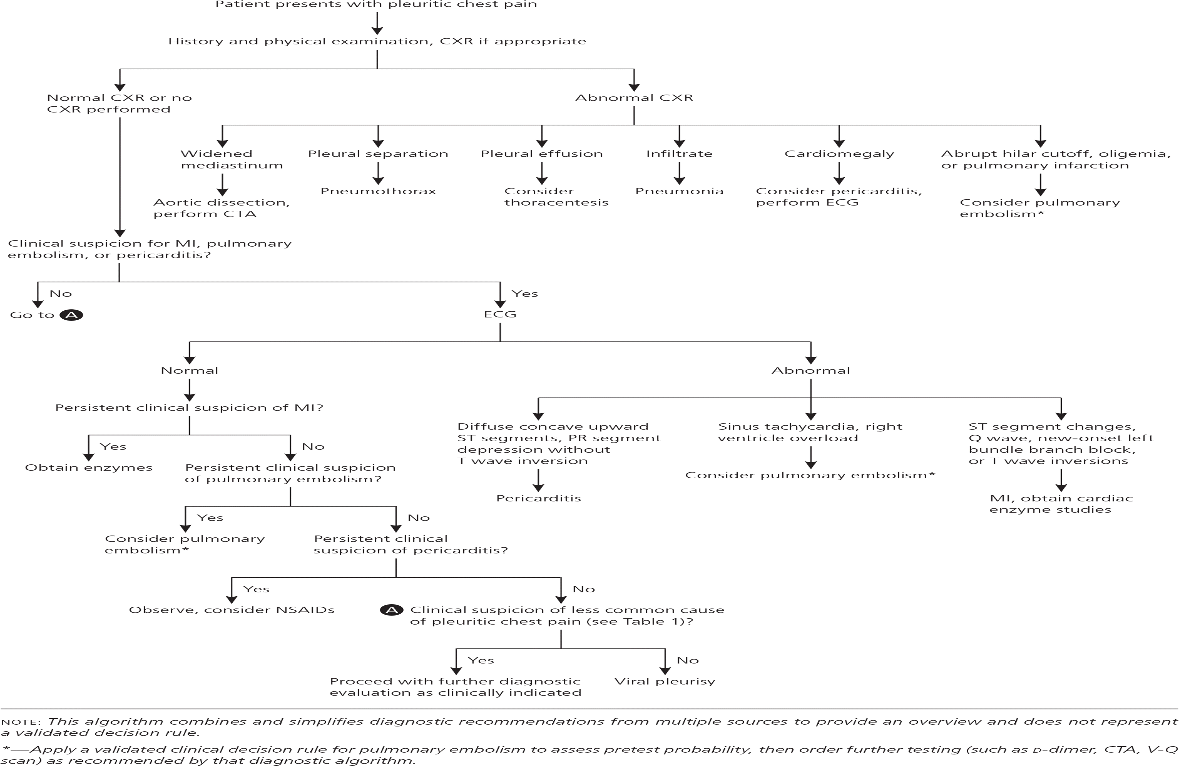
What does this refer to
Outpatient Diagnosis of Pleuritic Chest Pain.
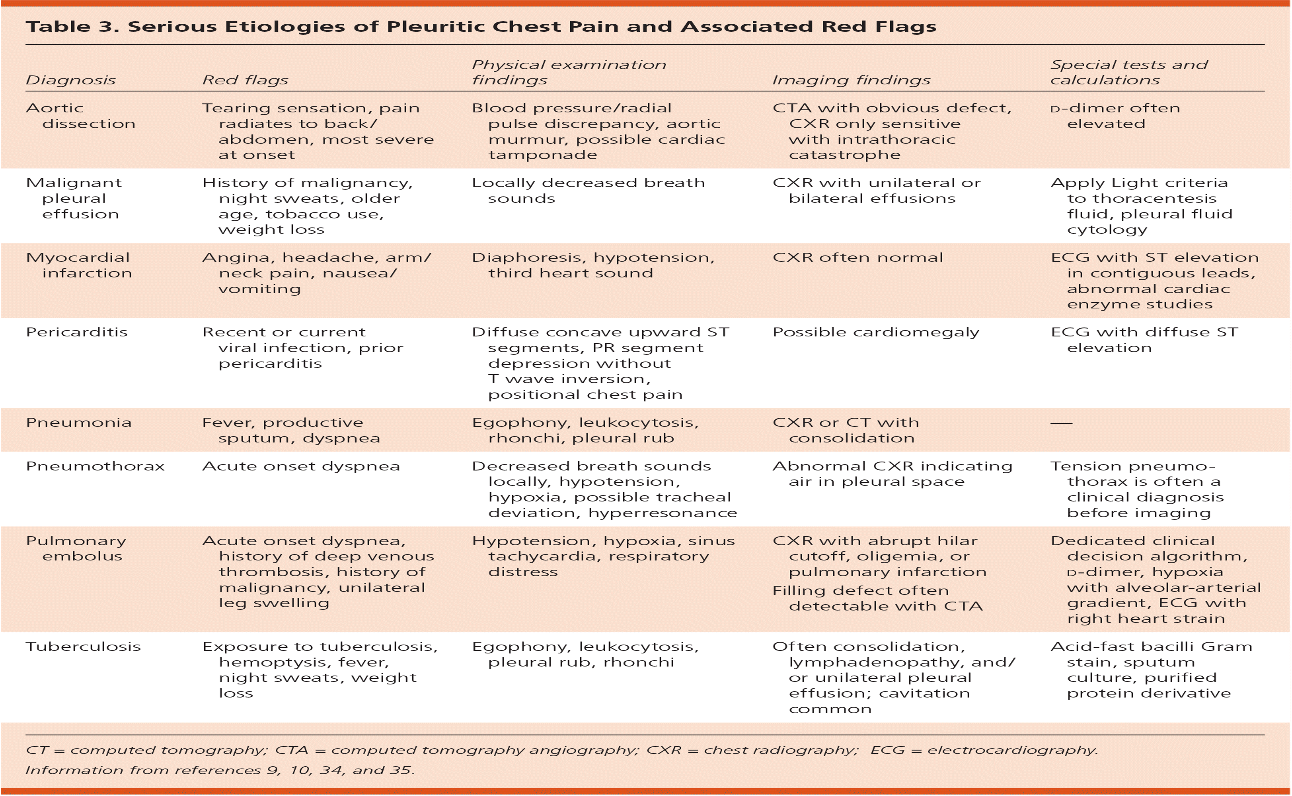
What does this refer to
Serious Etiologies of Pleuritic Chest Pain and Associated Red Flags
What does this refer to
Most are viral infx
Pain and symptoms resolve in 2-4 weeks
NSAIDS
Corticosteroids-for intolerant to NSAIDS
Nonviral Infection
Treat based on cause
Abx treatment
Colchicine for familial Mediterranean Fever
Refractory cases interleukin-1 or 6 inhibitor
Treatment of Pleuritic Chest Pain
What does this refer to
More likely to occur with malignancy, renal failure and rheumatoid pleurisy
Pleurodesis
Follow up
Very important with smokers, ones with persistent, or older than 50yo
Resolution of the abnormality @ 6weeks post-treatment
Recurrent Cases of Pleuritic Chest Pain
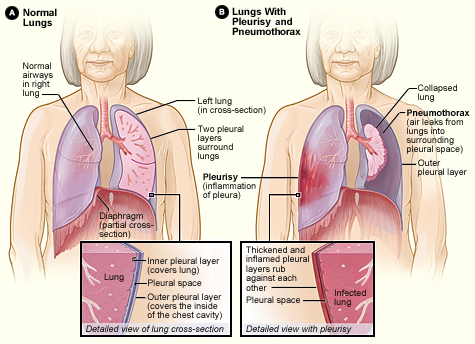
What does this refer to
SOB
What does this refer to
_____________ present with overlapping symptoms that can sometimes cloud the diagnosis. Compare and contrast the pathophysiology, historical features, physical examination findings, and diagnostic studies of COPD and interstitial lung disease.
Chronic obstructive lung disease and interstitial lung disease
What does this refer to
______________ is a heterogeneous group of disorders. Compare and contrast the findings found on CXR and CT scan with idiopathic pulmonary fibrosis, sarcoidosis, connective tissue interstitial lung disease, and eosinophilic interstitial lung disease.
Interstitial lung disease
What does this refer to
____________ is a cardiovascular manifestation of pulmonary disease leading to hypertrophy or dilatation of the right ventricle. List the pulmonary conditions that lead to cor pulmonale.
Cor Pulmonale