Lambing: Practical Rotation
1/52
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
53 Terms
Describe the 3 stages of labour in ewes
2-6hrs: cervical dilation, behavioural changes, abdominal contractions, water bag appearance
1hr: passage of the lamb through the birth canal
Within 2-3hrs of stage 2: repulsion of the foetal membranes
When should you intervene to assist with lambing?
Ewe trying to lamb for >1hr with no delivery
No progress once lamb visible at vulva for 20 mins
Frequent, powerful contractions but no delivery progress
Ewe started to lamb and then stopped
Lamb’s head visible but no forelimbs
Foetal head and only one limb visible
Only tail visible
Large and swollen lamb at vulva
Parts of 2 limbs visible
Brown/smelly discharge
Vaginal prolapse identified
What are the consequences of dystocia for lambs?
Increased mortality rate
Higher incidence of neonatal infections
Slower weight gain
Increased costs of medication/care
What are the consequences of dystocia for ewes?
Reduced colostrum/milk let down
Poor mothering behaviour
Higher costs of medication/care
Potentially reduced future fertility
Draw out the 9 types of presentation in lambing ewes
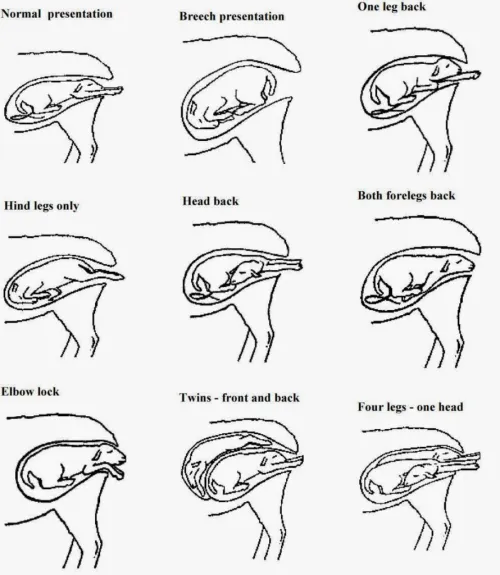
What should you remember when assisting with lambing?
Hygiene is very important: use arm length, disposable gloves and plenty of lubricant
Gentle manipulation- uterus can be damaged if care is not taken, particular attention should be paid to protecting the uterine wall from hooves when re-positioning
Do not use excessive traction
What are the colostrum requirements of lambs?
50ml/kg in the first 2hrs of life
250ml/kg during the first 24hrs of life
Describe the wet adoption fostering technique
Rub fetal fluids from the ewe's own newborn lamb all over the foster lamb's head, back, and tail
If the ewe has already licked her lamb dry, use a bucket to mix fluids with warm water to coat the foster lamb
Introduce the foster lamb first, then her own, allowing her to lick both
Describe the skinning fostering technique
Remove the skin from the dead lamb and create a "jacket" for the foster lamb
Ensure the skin covers the lamb's body, leaving it on for a few days until the ewe accepts the scent
Describe the adopter crate fostering technique
The ewe is secured in a head-lock crate, allowing her to stand but preventing her from turning away or attacking the new lamb, this allows the lamb to suckle safely
Ewes are usually kept in these crates for 2–7 days
How can you identify the sex of a lamb?
Males: lift the tail, you will see 2 distinct testicles
Females: no testicles are present
Why and when do we castrate lambs?
Why: prevents inbreeding, allows effective breeding management, influences carcass composition and growth (higher amounts of fat)
When: if lambs are intended for slaughter at a young age, there is probably no need to castrate
Why and when do we tail dock lambs?
Why: reduces amount of faecal contamination in the tail, reducing fly strike risk
When: if fly strike is not a problem in the area, there is probably no need to tail dock
How do we tail dock/castrate lambs?
Apply a tight rubber band around the testicles/tail, fairly high up
What temperature should newborn lambs be, and how could you tell if they are hypothermic?
Temperature should be 39-40℃
37-39℃= moderate hypothermia
< 37℃= severe hypothermia
How can you treat ill lambs?
Intraperitoneal glucose injection (20% glucose)
Dry lamb and place in a warming box
Stomach tubing: measure length of tube needed (mouth to shoulder), then place the tube in the side of the lamb’s mouth and insert it- lamb should not gasp
Describe ‘watery mouth’- including when lambs are affected, cause, treatment and prevention
Typically affects lambs from 12-36hrs old
Main cause is E.coli
Treatment- antibiotics, antiinflammatory drugs
Prevention- ensuring good hygiene and adequate colostrum intake
Describe ‘joint ill’- including clinical signs, cause and transmission
Hot, swollen and painful joints
Caused by Streptococcus dysgalactiae
May enter orally or via navel, docking, castrating or tagging wounds
Describe Entropian, including what it is, the effects and the treatment
Lower eyelid rolls in and eyelids rub against surface of the eye
Makes lamb’s eyes runny, and the cornea cloudy
Treatment- injections of penicillin parallel to the eyelid, or application of Michel clips to the eyelid to hold the eyelid out
Outline the effect and treatme/prevention of Coccidia
Effect: scour (often bloody) and straining in lambs from 5 weeks-3 months, poor growth rates in lambs
Treatment: anticoccidials, avoid mixing lambs of different ages
Outline the effect and treatment/prevention of nematodes
Effect: diarrhoea and reduced growth rates
Treatment: grazing management, quarantine and anthelmintics
Outline the effect and treatment/prevention of fluke
Effect: reduced lambing percentages, reduced growth rates and sudden death
Treatment: avoiding grazing areas where there might be mud snails, using flukicides when appropriate and quarantine
Outline the effect and treatment/prevention of mites
Effect: scratching, weight loss and fleece loss
Treatment: endectocides such as sheep dip
Outline the effect and treatment/prevention of chewing lice
Effect: scratching, weight loss and fleece loss
Treatment: ectoparasiticides and shearing
Outline the cause and treatment/prevention of blow fly strike
Cause: flies are attracted to soiled fleece, and lay eggs- larvae hatch, lacerate and liquefy the skin and attract more flies, resulting in severe wounds and maggot infestation
Treatment: improving fly control and hygiene, removing fleece around back end (dagging) and protecting wounds with fly repellent
Outline the effect and treatment/prevention of ticks
Effect: high numbers of ticks may cause anaemia, leading to weakness and may also transmit other diseases such as louping ill
Treatment: ectoparasiticides
Draw out the life cycle of a typical sheep nematode
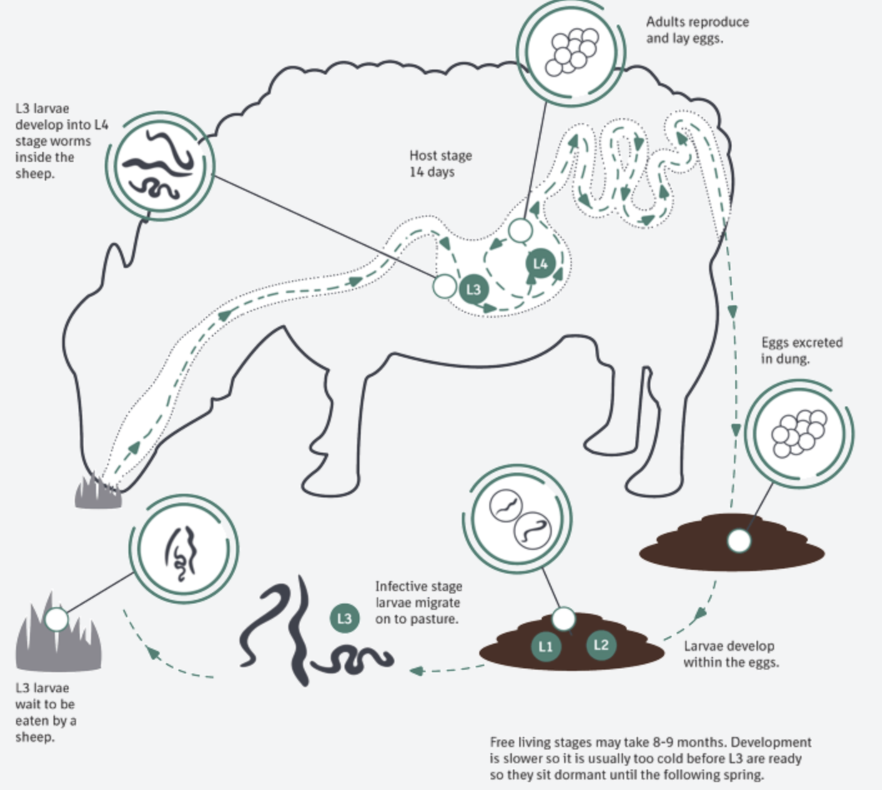
Describe the different classes of wormer
BZ (Benzimidazoles)- white drenches
LV (Levamisoles)- yellow drenches
ML (Macrocyclic-lactones)- clear drenches
AD (Amino Acetonitrile Derivatives)- orange drenches
SI (Multi-actives)- purple drenches
Describe the steps taken to prevent against lameness
Vaccinate: supports improving flock immunity against lameness-causing bacteria
Cull: identify and remove sheep with severe/repeated bouts of lameness
Avoid: minimise infection spread during handling and on pasture, avoid high-risk environments, maintain dry tracks and prevent foot damage
Treat: treat all lame sheep promptly to reduce disease spread (antibiotics, foot sprays)
Quarantine: isolate lame/newly introduced sheep for at least 28 days
Describe the transmission and prevention of abortion by Toxoplasma gondii (protozoan)
Transmission:
Ingestion of oocysts shed in the faeces of infected cats
Highly resistant in the environment, can survive for months/years on pasture/feed
Prevention:
Isolate all ewes that have aborted, remove infectious materials, give vaccines
Describe the transmission and prevention of abortion by Chlamydia abortus (bacterial)
Transmission:
Contact with infected placentas, aborted foetuses or vaginal discharges
Prevention:
Isolate all ewes that have aborted, remove infectious materials, give vaccines, antibiotics are sometimes given
Describe the transmission and prevention of abortion by Campylobacter foetus/jejuni (bacterial)
Transmission:
Usually enters through carrier animals, spreading through contaminated feed, water or direct contact
Prevention:
Isolate all ewes that have aborted, remove infectious materials, no vaccines are available
Describe the infectious disease Caseous lymphadenitis (CLA), including the cause, transmission, clinical signs and control
Cause: Corynebacterium pseudotuberculosis
Transmission: contact with infective pus that drains from abscesses around lymph nodes
Clinical signs: abscesses containing thick, green pus- which may rupture
Control: quarantine new stock, culling animals with abscesses, disinfecting shearing equipment, antibiotics are generally ineffective, vaccines are not widely available
Describe the infectious disease Maedi visna (MV), including the cause, transmission, clinical signs and control
Cause: a lentivirus
Transmission: respiratory secretions, milk and colostrum
Clinical signs: lungs and CNS, pneumonia, chronic mastitis and neurological signs may develop
Control: testing flock, culling positive animals, using replacement stock from flocks certified free of MV
Describe the infectious disease Ovine pulmonary adenocarcinoma (OPA), including the cause, transmission, clinical signs and control
Cause: a retrovirus
Transmission: respiratory secretions, possibly milk and colostrum
Clinical signs: chronic pneumonia- coughing, weight loss, etc
Control: there is no treatment, but affected sheep should be isolated and culled promptly
Describe the infectious disease Johne’s disease, including the cause, transmission, clinical signs and control
Cause: Mycobacterium avium subspecies paratuberculosis (MAP)
Transmission: contaminated faeces
Clinical signs: weight loss, diarrhoea, decreased milk production
Control: testing and culling infected animals and offspring, vaccine available in some regions
Describe the infectious disease Border disease, including the cause, transmission, clinical signs and control
Cause: pestivirus (BVD)
Transmission: contact with infected secretions
Clinical signs: stillbirths, birth of weak lambs with neurological/developmental issues, high rates of ewe infertility
Control: quarantine and testing new stock, identification of affected animals, good biosecurity
Describe the clostridial condition ‘pulpy kidney‘, including the clostridial cause and clinical signs
Cause: C perfringens (D)
Clinical signs: sudden death in weaned lambs (younger if ewes not vaccinated)
Describe the clostridial condition ‘struck‘, including the clostridial cause and clinical signs
Cause: C perfringens (C)
Clinical signs: sudden death in adult sheep
Describe the clostridial condition ‘lamb dysentery‘, including the clostridial cause and clinical signs
Cause: C perfringens (B)
Clinical signs: sudden death in lambs, blood tinged diarrhoea
Describe the clostridial condition ‘tetanus‘, including the clostridial cause and clinical signs
Cause: C tetani
Clinical signs: ascending spastic paralysis, lateral recumbancy, seizures, death
Describe the clostridial condition ‘botulism‘, including the clostridial cause and clinical signs
Cause: C botulinum
Clinical signs: flaccid paralysis followed by death
Describe the clostridial condition ‘black disease‘, including the clostridial cause and clinical signs
Cause: C novyi
Clinical signs: sudden death in late summer/early autumn
Describe the clostridial condition ‘braxy‘, including the clostridial cause and clinical signs
Cause: C septicum
Clinical signs: sudden death in weaned lambs in winter
Describe the clostridial condition ‘blackleg‘, including the clostridial cause and clinical signs
Cause: C chauvoei
Clinical signs: lameness, pyrexia, dullness, anorexia, sudden death
Describe the clostridial condition ‘malignant oedema‘, including the clostridial cause and clinical signs
Cause: C septicum
Clinical signs: swelling of the head
Describe Schallenberg virus, including transmission, clinical signs and control
Transmission: midge vector
Clinical signs: abortions, malformed lambs
Control: vaccination
Describe Bluetongue virus, including transmission, clinical signs and control
Transmission: midge vector
Clinical signs: depression, fever, mouth ulcers, coronary band inflammation
Control: vaccination
Describe foot and mouth disease, including transmission, clinical signs and control
Transmission: aerosol, people, fomites
Clinical signs: fever, mouth and hoof vesicles
Control: culling
Describe scrapie, including transmission, clinical signs and control
Transmission: milk, colostrum, secretions
Clinical signs: incoordination, odd behaviour, weight loss
Control: culling and resistant breeding
When should you start health planning?
Ideally 8 weeks before tupping at the start of the sheep year
Can also be 6 weeks after the end of lambing
What are some common diseases in new stock?
Ezoonotic abortion
Maedi visna
Caseous lymphadenitis
OPA
CODD
OrfSheeb scab
Roundworms and liver fluke
Describe the key points of health planning
Biosecurity section is essential
Health planning helps to monitor disease outbreaks and give advance warnings
Can be recorded by paper, wall planner, computerised or web-based
Record: production figures, treatments, disease, blood sampling results
Health planning is a requirement for the Sheep Welfare Code and certain farm assurances