Common Drugs for Liver and Pancreas
1/47
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
48 Terms
What are the primary mechanisms of liver injury in veterinary patients?
Oxidative injury, toxins and infectious diseases, cholestatic liver disease, immune-mediated mechanisms, and metal accumulation.
What is the primary metabolic problem associated with hepatic encephalopathy?
Impaired ammonia detoxification.
How does a portosystemic shunt affect drug therapy?
It causes the liver to be bypassed, leading to increased sensitivity to drugs and toxins.
What is the clinical consequence of cholestasis?
Impaired bile flow, which leads to fat and vitamin malabsorption.
What is the definition of cirrhosis in a clinical context?
A structural or morphological diagnosis representing the loss of metabolic liver function.
What are the three main mechanisms by which S-adenosylmethionine (SAMe) supports liver function?
Methylation support (stabilizes membranes), glutathione synthesis (antioxidant protection), and mitochondrial protection (reduces apoptosis).
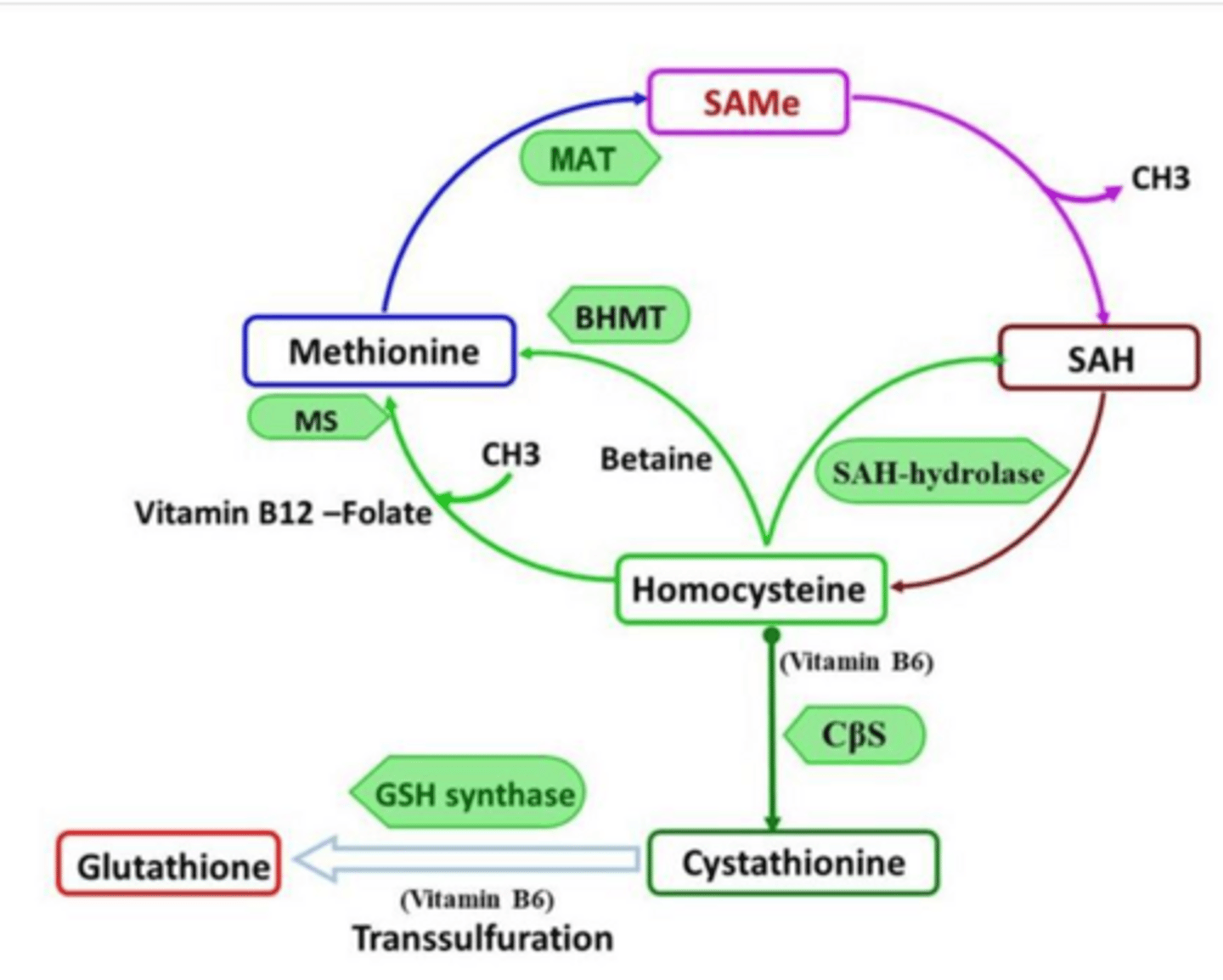
Why is SAMe often combined with silymarin or UDCA?
To achieve a synergistic hepatoprotective effect.
What is the primary therapeutic use of Ursodeoxycholic Acid (UDCA)?
Treatment of cholestatic liver diseases, immune-mediated hepatopathies, and secondary reactive hepatopathies.
What is a major contraindication for the use of UDCA?
Complete extrahepatic bile duct obstruction, due to the risk of bile retention and hepatocellular injury.
How does Silymarin protect hepatocytes?
It stabilizes membranes to prevent toxin entry, scavenges free radicals, promotes protein synthesis for regeneration, and provides anti-inflammatory/antifibrotic effects.

What is the specific antidote for acetaminophen (paracetamol) toxicity?
N-Acetylcysteine.
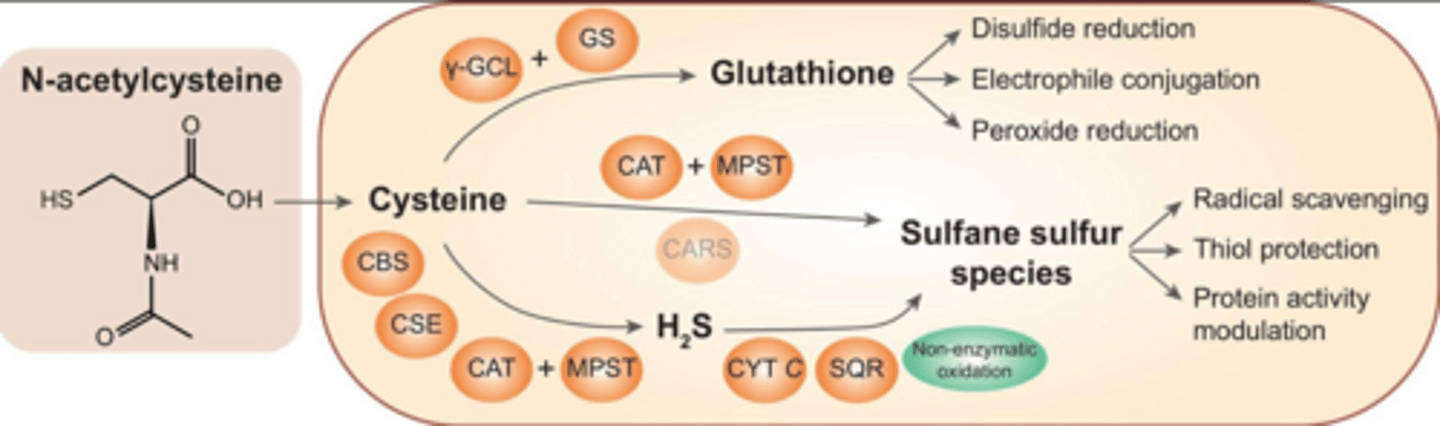
What is the toxic metabolite of paracetamol that N-Acetylcysteine helps neutralize?
N-acetyl-p-benzoquinone imine (NAPQI).
What must always be excluded before administering choleretic or cholagogue drugs?
Extrahepatic biliary obstruction.
Which nutrient is specifically critical for liver health in cats?
Taurine.
What are the dietary management goals for a patient with hepatic encephalopathy?
High-quality, highly digestible protein (with restriction), copper restriction, increased antioxidants, and zinc supplementation.
Which chelating agents are used for managing copper storage disease?
D-Penicillamine and Trientine.
What is the role of zinc salts in treating copper-associated hepatopathy?
They inhibit the absorption of copper from the gastrointestinal tract.
What feature characterizes the drug toxicity seen in the Labrador retriever case study (carprofen)?
It is a rare, unpredictable idiosyncratic reaction affecting only susceptible individuals.
What is the primary function of choleretics?
To increase the production and flow of bile.
What is the primary function of cholagogues?
To stimulate the contraction of the gallbladder to release bile.
What is the clinical significance of rhodanine-positive cytoplasmic granules in hepatocytes?
They indicate copper accumulation, characteristic of copper storage disease.
Which vitamin is often supplemented in hepatic diets to provide antioxidant support?
Vitamin E.
What is the role of L-carnitine in hepatic diets?
It supports lipid metabolism and is often included in diets for patients with hepatic lipidosis or general liver support.
What is the primary goal of antifibrotic therapy in liver disease?
To reduce the progression of scar tissue formation (fibrosis) in the liver.
What is the significance of rhodanine-positive cytoplasmic granules in hepatocytes?
They are indicative of copper accumulation, often associated with copper storage disease.
Which drugs are used for the chelation and urinary excretion of copper in dogs?
Penicillamine and Trientine.
What is the mechanism of action of Zinc in treating copper hepatopathy?
It induces metallothionein synthesis in enterocytes, which reduces copper absorption.
What is the primary hepatoprotective function of S-adenosylmethionine (SAMe)?
It donates methyl groups and supports glutathione synthesis, acting as an antioxidant.
How does Silymarin (Milk thistle) protect hepatocytes?
It scavenges reactive oxygen species (ROS) and stabilizes the hepatocyte cell membrane.
What is the therapeutic role of Ursodeoxycholic acid (UDCA) in liver disease?
It is a choleretic that replaces toxic bile acids, increases bile flow, and reduces immune-mediated injury.

In cases of toxic liver injury, how does N-Acetylcysteine provide protection?
It replenishes glutathione, scavenges ROS, and improves detoxification processes.
What clinical signs are typical of acute toxic hepatopathy in dogs?
Vomiting, lethargy, anorexia, icterus, melena, abdominal pain, and significantly elevated liver enzymes (ALT, AST, ALP).
What is the purpose of using cholestyramine in the decontamination of a hepatotoxic plant ingestion?
To interrupt the enterohepatic recirculation of toxins.
What is the primary goal of Exocrine Pancreatic Insufficiency (EPI) treatment?
To replace missing digestive enzymes (lipase, amylase, protease) to correct maldigestion.
What is the main substance used for enzyme replacement therapy in EPI?
Pancrelipase, typically derived from porcine pancreas.
How should Pancrelipase be administered for maximum effectiveness?
It should be mixed with food at every meal to ensure proper enzyme-food contact.
What are the recommended analgesics for acute pancreatitis in dogs?
Strong opioids such as methadone, fentanyl, or hydromorphone; NSAIDs should be avoided.
Which antiemetics are commonly used in the management of pancreatitis?
Maropitant, ondansetron, and metoclopramide.
What is the therapeutic goal for chronic pancreatitis management?
To control pain, limit flare-ups, and manage exocrine or endocrine insufficiency.
Why is cobalamin (B12) supplementation often used in chronic pancreatitis?
It is an adjunctive therapy to address potential deficiencies caused by malabsorption or pancreatic dysfunction.
When are corticosteroids indicated in the treatment of pancreatitis?
They are often indicated in cats with immune-mediated pancreatitis or triaditis.
What is the mechanism of action of Glipizide in cats with diabetes mellitus?
It stimulates insulin release from the remaining pancreatic beta-cells.
How does Bexagliflozin (Bexacat) lower blood glucose levels?
It blocks SGLT2 transporters in the kidneys, preventing glucose reabsorption and promoting glucosuria.
What is Feline Triaditis?
A condition involving concurrent inflammation of the liver, pancreas, and small intestine.
What is the role of gastrointestinal protectants like Omeprazole in pancreatitis?
To provide gastroprotection and manage acid-related complications during inflammatory episodes.
Why is early enteral feeding recommended in pancreatitis?
To support nutritional needs and maintain gut health, provided the patient can tolerate it.
What is the difference in prognosis between acute and chronic pancreatitis?
Acute pancreatitis is potentially reversible, whereas chronic pancreatitis is progressive and incurable, though manageable.
What is the primary dietary recommendation for dogs with chronic pancreatitis?
Lifelong low-fat dietary control.