Skin Changes and Dry Skin
1/27
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
28 Terms
Glogau Classification System
Developed to objectively measure the severity of wrinkles and photoaging.
Photoaging
Premature skin aging which reflects long-term skin damage from sun exposure
Type I - Mild (Glogau)
No/minimal wrinkles
No/minimal use of foundation
Mild pigment changes - no keratosis (common noncancerous skin growths in older adults caused by years of sun exposure)
Ages 28-35 years
Type II - Moderate (Glogau)
Keratosis is palpable, but not visible
Wrinkles in motion (e.g., smile lines)
Early senile lentigines - age/”liver” spots, hyperpigmented macules in irregular shapes, appearing most commonly in sun-exposed areas of skin (face, back of hands)
Occasional/light foundation
Ages 35-50
Type III - Advanced (Glogau)
Wrinkles at rest
Clear signs of irregular pigmentation
Visible keratosis
Heavy foundation use
Ages 50-65 years
Type IV - Severe (Glogau)
Wrinkles throughout face
Yellow-gray skin
History of malignancy
Foundation cakes/cracks
Ages 60-75 years
Tretinoin
Renova, Retin-A, Retin-A Micro
Topical Tretinoin Indications
Photodamaged skin
Palliation of fine wrinkles
Mottled hyperpigmentation
Tactile roughness of facial skin
Topical Tretinoin MOA
Reduces melanin production
Increases epidermal thickness
Increases keratinocyte turnover
Increased collagen activity
Tretinoin dosing
Apple daily at bedtime
Wash and dry face 20 to 30 minutes before application
Cover affected area lightly; avoid eyes, ears, mouth and nose
Separate administration times of used with AHAs
Goals of therapy (may take up to 6 months for results) - Smoother skin texture, minimization/improvement in wrinkles, lightening of lentigines (small brown patch on skin)
Tretinoin Safety
Increased photosensitivity (use sunscreen)
ADEs: Skin irritation, burning, drying, peeling
Caution: Current or planned pregnancy, breastfeeding - Tazarotene contraindicated
Tazarotene
Tazorac
Topical tretinoin
Adapalene
Differin
Topical tretinoin
Alpha Hydroxy Acids (AHAs) MOA
Used for photoaging
Chemical peel
Removes dry skin from stratum corneum
Increased moisture retention
May contain lactic, glycolic, citric, or malic acid
2-20% concentration: non-peeling
>20%: Peeling
AHA Dosing
Apply to dry skin 10 minutes after cleaning face
Start gradually (e.g. every other night for one week)
Increase as tolerated to max twice daily use
Effects: Increased thickness of epidermis, decreased fine wrinkles, skin mottling, and alteration in pigmentation
AHA Safety
Increased photosensitivity (use sunscreen)
ADEs: Stinging, burning, itching, hypopigmentation, dryness
Safe to use in pregnancy
Onabotulinumtoxin A (Botox)
Derived from Clostridium toxin
Prevents release of acetylcholine from the synapse
Soft tissue augmentation
Prevents release of acetylcholine from the synapse - results in localized paralysis and atonia
Used on the face and neck (cosmetic purposes)
Onabotulinumtoxin A (Botox) Safety
Side effects: Redness and bruising at injection sites
Clinical effect seen in 24-72 hours
Maximum effect may not be evident for 1-2 weeks
May last 3-9 months
Black box warning: Distant spread of toxin effect, which can cause swallowing and breathing problems.
Hydroquinone MOA
Used to treat hyperpigmentation
Bleaching agent
Reduces conversion of tyrosine to dopamine to melanin —> decreases pigmentation of skin
Hydroquinone dosing
OTC products are 2%; Rx products are 4$
Apply thin layer to affected area BID until desired color achieved
Effects seen in 3 weeks to 3 months
Hypopigmentation is reversible upon UVR
Hydroquinone safety
ADEs: tingling, burning, transient inflammation, photosensitivity
CI: sunburn, depilatory cream use, pregnancy
Other options for Hyperpigmentation
Retinoic acid - Can consider combination with hydroquinone
Laser and light therapy - Two to three sessions may destroy melanocytes, spots may fade over several months
Cryotherapy - Can consider for single or closely grouped spot, risk of scarring or discoloration
Actinic Keratoses
Precursors to the development of skin cancers
UV radiation may induce abnormal keratinocyte changes
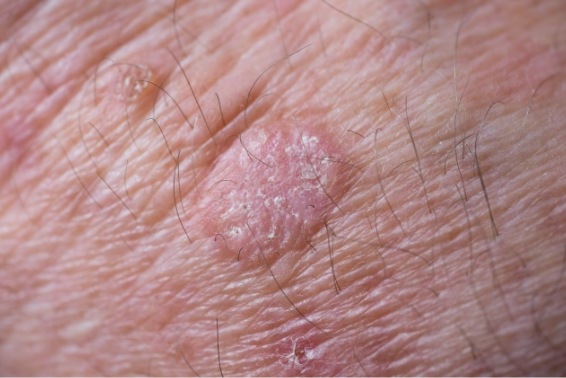
Squamous Cell Carcinoma
Most common in older patients
Risk factors: Fair complexion, prolonged sun exposure/UV radiation, long-term immunosuppression
Usually present as firm, flesh-colored or erythematous papules/plaques
Primarily managed via surgical excision
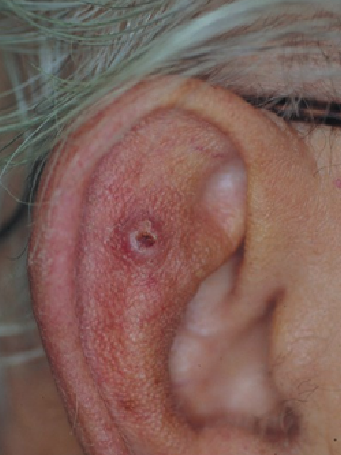
Basal Cell Carcinoma
Usually present as pigmented nodule on head/neck
May develop into ulcerated nodule
Treatment varies, but may involve: Surgical excision, topical imiquimod, antineoplastic agents
Malignant Melanoma
Unless detected early and excised, often produces systemic metastases
Can occur anywhere on the body
Changing mole = get checked
ABCDs of melanoma:
(A) symmetry
(B) Orders irregular or uneven
(C)olor differences within lesion
(D)iameter usually >6 mm
Treated via excision ± antineoplastic agent
Xerosis Treatment Approaches
Goals:
Restore skin hydration
Minimize symptoms
Control exacerbating factors
Non-Pharmacologic treatments
Pat (vs. rub) skin dry
Maintain hydration
Using non-soap cleansers
Warm/cool water for bathing/showeing
Most cases can be treated with humectants or emollients
Xerosis Pharmacologic Options
Humectants - Glycerin, Urea, Hyaluronic acid. Hydrophilic; draw moisture from deeper dermal layers
Emollients: Petrolatum, Propylene glycol, Ceramide. Lipophilic; provide a protective “film” on skip surface to trap moisture
Other: Colloidal oatmeal baths, keratinolytics (AHA, salycylic acid), bath oils (ensure fragrance-free), TCS (for cases of severe pruritis, erythema).