Quiz 5 Content - Implant-Supported Fixed Restorations Part 2 ONLY (Dr. Muftu)
1/71
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
72 Terms
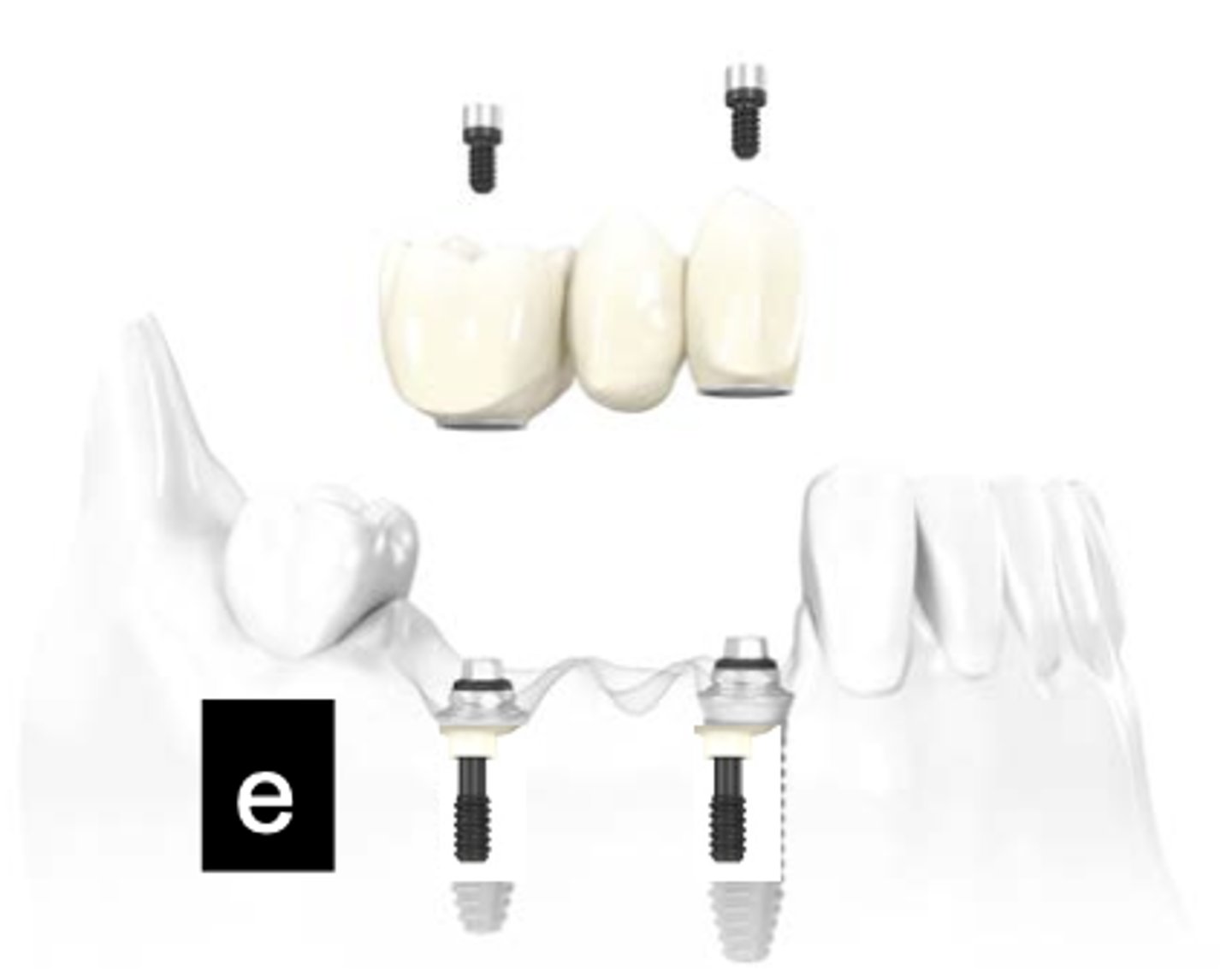
Implant supported, Screw retained
What type of implant does this show?
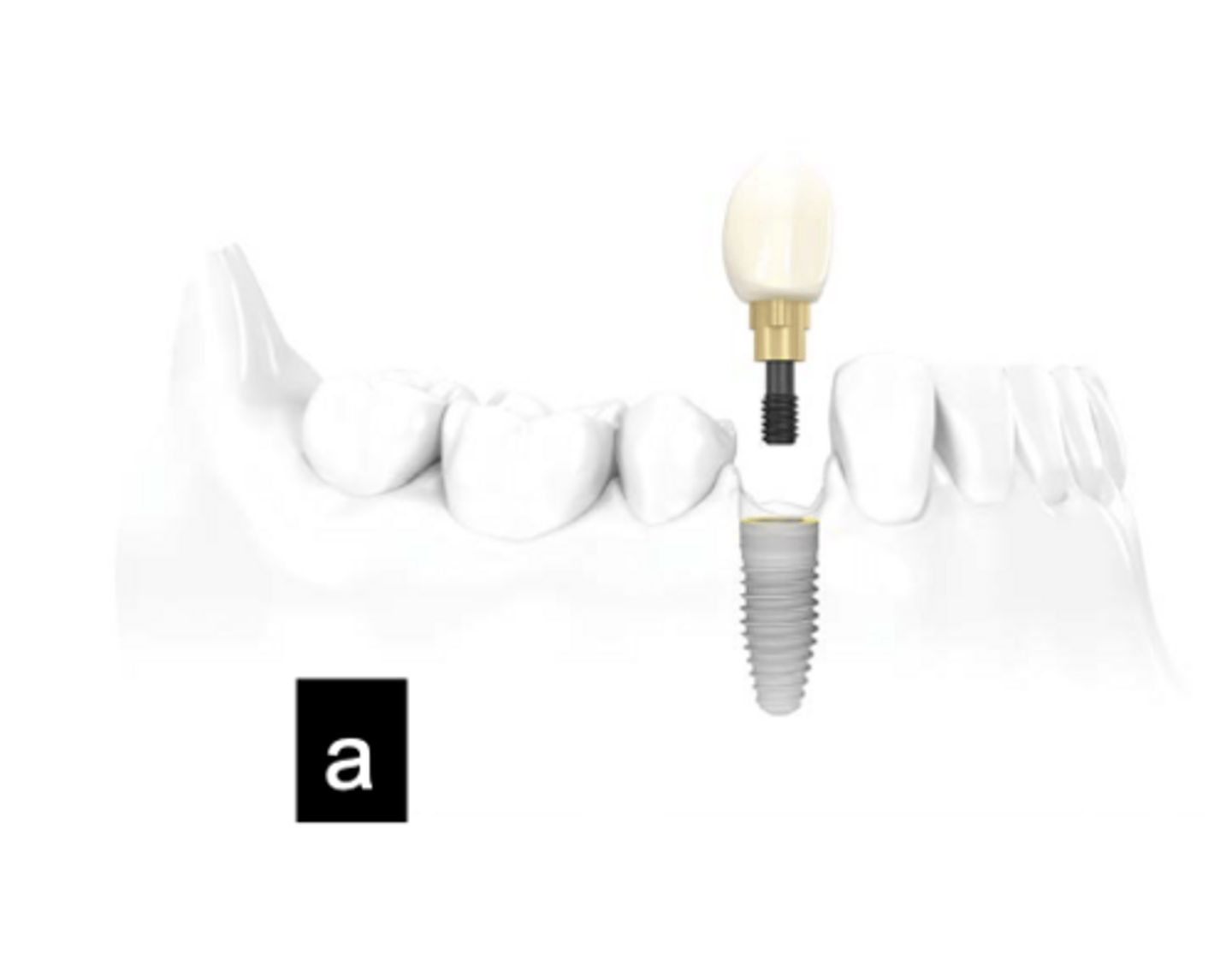
Abutment supported, Cement retained
What type of implant does this show?
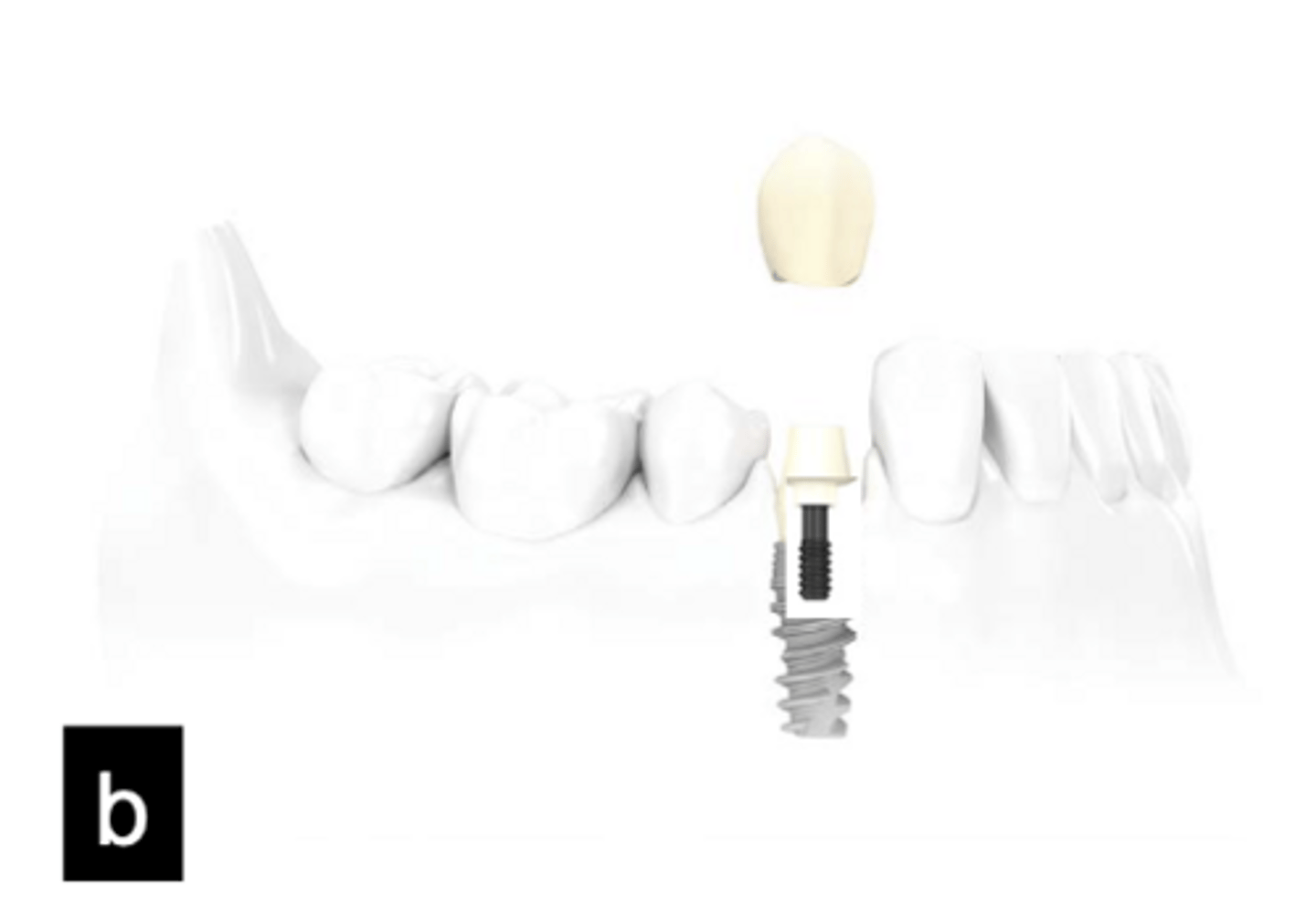
Implant supported, Screw retained
What type of implant does this show?
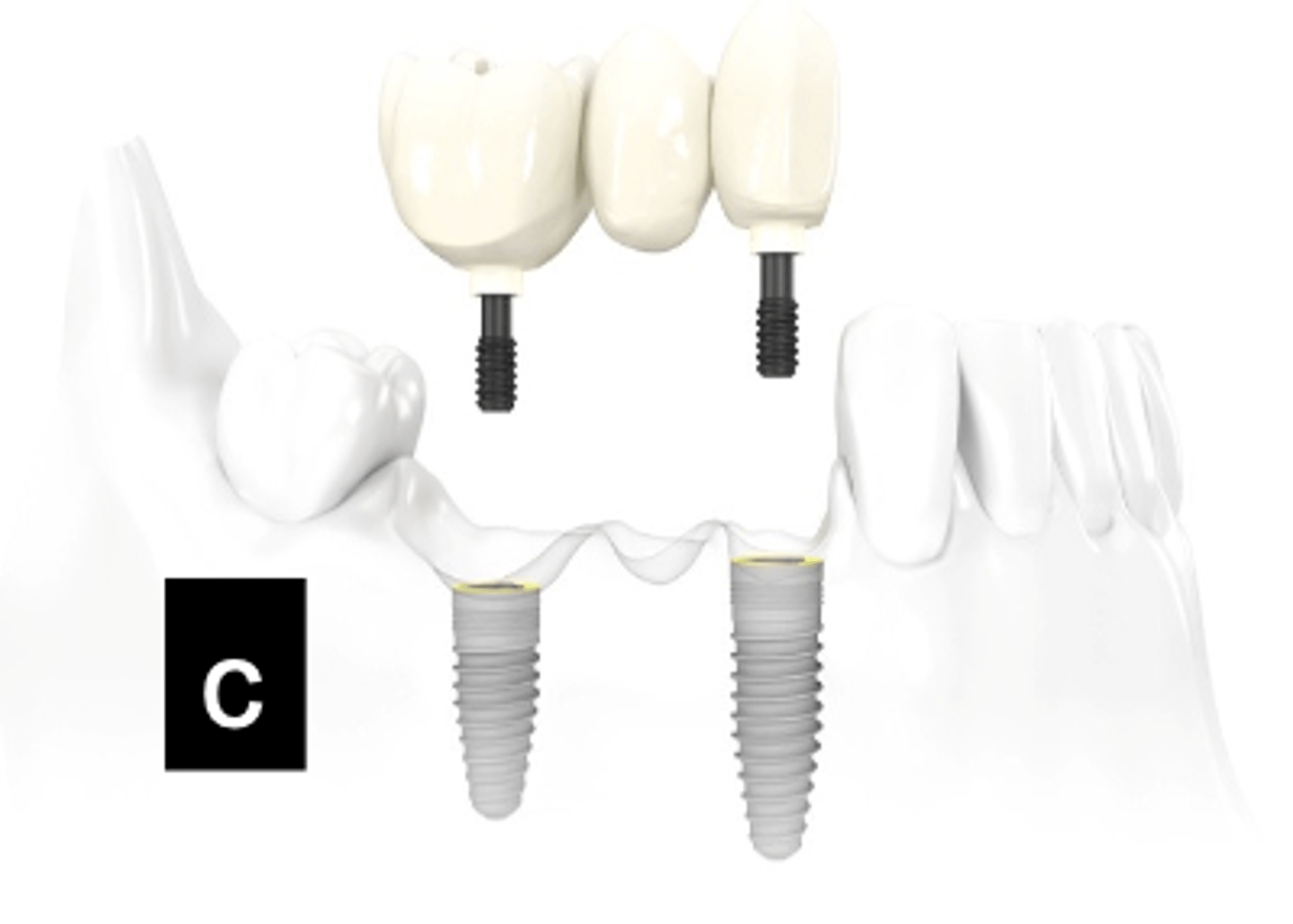
Abutment supported, cement retained
What type of implant does this show?
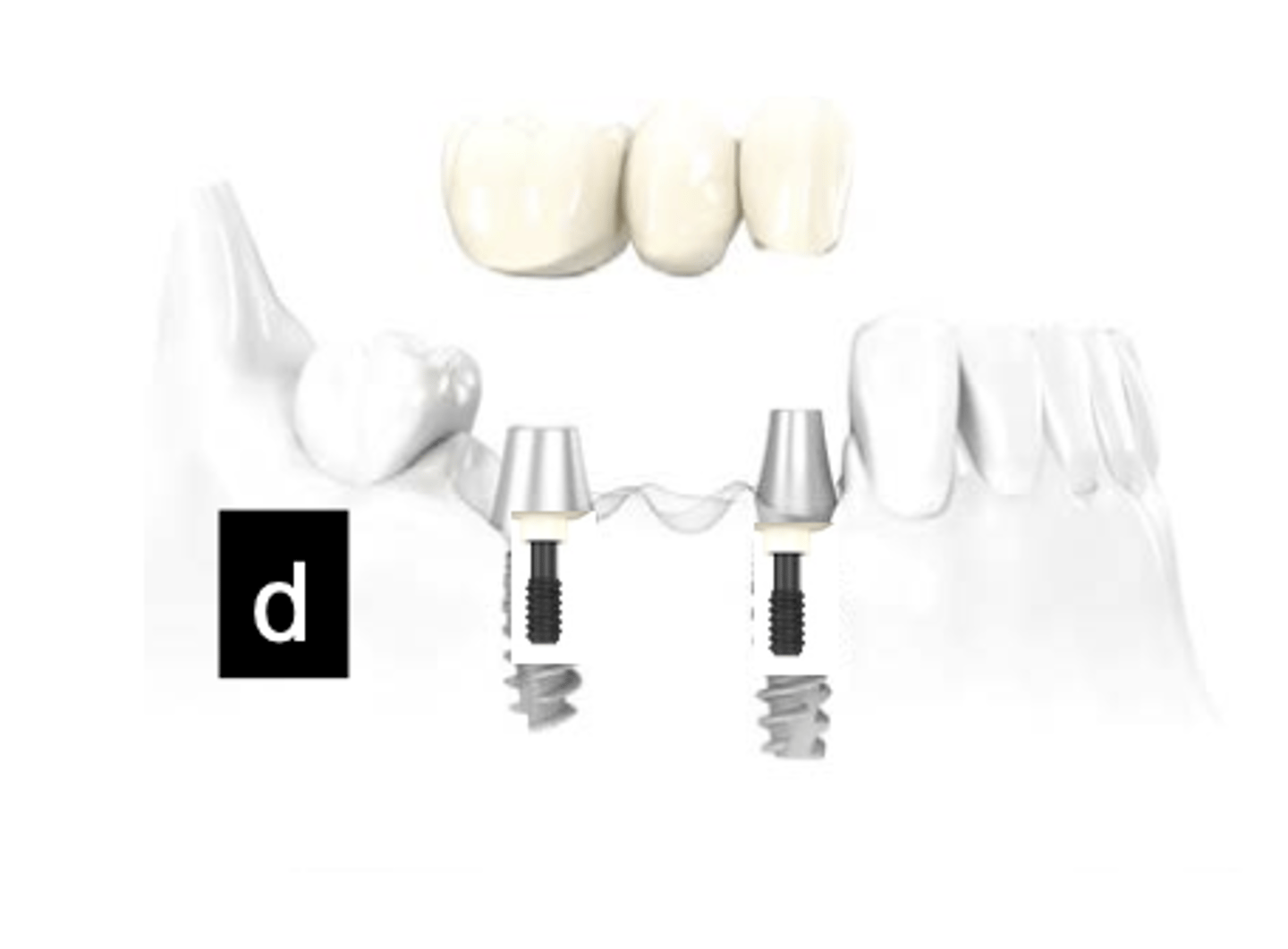
Abutment supported, screw retained
What type of implant does this show?
ADA-CDT codes
What is used for...
- Insurance, billing, standardization purposes
- Identifies materials, type of support, but not restoration retention mechanisms
Temporary abutments
What has the following characteristics?
- Available in Titanium or Plastic (indicated for max. 3 months intraoral use)
- Available for internal and external connection
- Retentive grooves to engage acrylic temporary materials
- Extended length designed for customization as per clinical requirements
engaging temporary abutment
ID the part:

non-engaging temporary abutment
ID the part:

cement
screw
What are the 2 types of retention for an implant?
e - should be passivity
All of the following are factors to consider when deciding cement vs. screw retention EXCEPT:
a. ease of fabrication and cost
b. esthetics
c. retrievability
d. occlusion
e. activity
f. delivery
g. retention
h. biological/technical complications
i. implant position, angulation
Screw retained implant
The following are indications for what type of implant?
- In situations of minimal interarch space
- To avoid a cement margin and the possibility of cement residue
- When retrievability is of importance
- In the esthetic zone, to facilitate tissue contouring and conditioning in the transition zone (emergence profile)
True
T/F: It is critical to place the implant in correct position for screw retained restorations. Cement retained restorations are more "forgiving" if the implant is not placed in an ideal position/ angle
Cement retained implant
(It is further recommended that the clinician understand that the procedures involved with cement retention for implant-supported crowns are not simple and should be carried out with great caution)
The following are indications for what type of implant?
- For short-span prostheses w/ margins at or above tissue level to simplify fabrication procedures
- To enhance esthetics when the screw access hole is visible or in cases of malposition of the implant
- When an intact occlusal surface is desirable
- To reduce initial treatment costs
Prefabricated abutment
ID the part:

Prefabricated abutment
What type of abutment...
- Frequently titanium
- Mostly engaging
- Mostly used for cement type
- Less expensive
- Measured from platform to gingival margin
Prefabricated (stock) implant abutments
What type of abutment...
- Used to work well
- Was less costly than custom abutments
- Emergence profile could not be customized
- Restorations were cement retained
- Not the first choice today
Custom abutment
What type of abutment...
- Most frequently for cement type restorations
- Can be made of cast gold alloy, titanium or ceramic
- All should be 'engaging' type for single unit restorations
- More expensive than prefabricated cement type abutments
- Better esthetics (emergence profile)
hybrid abutment
What type of abutment...
- An individually milled ceramic (lithium disilicate or Zr abutment) which is luted to the Ti base
- Shape, emergence profile and esthetic properties of this abutment can be ideally adjusted with the design software
Prefabricated
_________ abutments do not alter emergence profile, since
their cross section is round and the resulting tissue profile is
round
Full anatomical dimensions
What type of abutment?
- Larger-diameter abutment provided with the best emergence profile possible
- Surgical incision for placement may be required
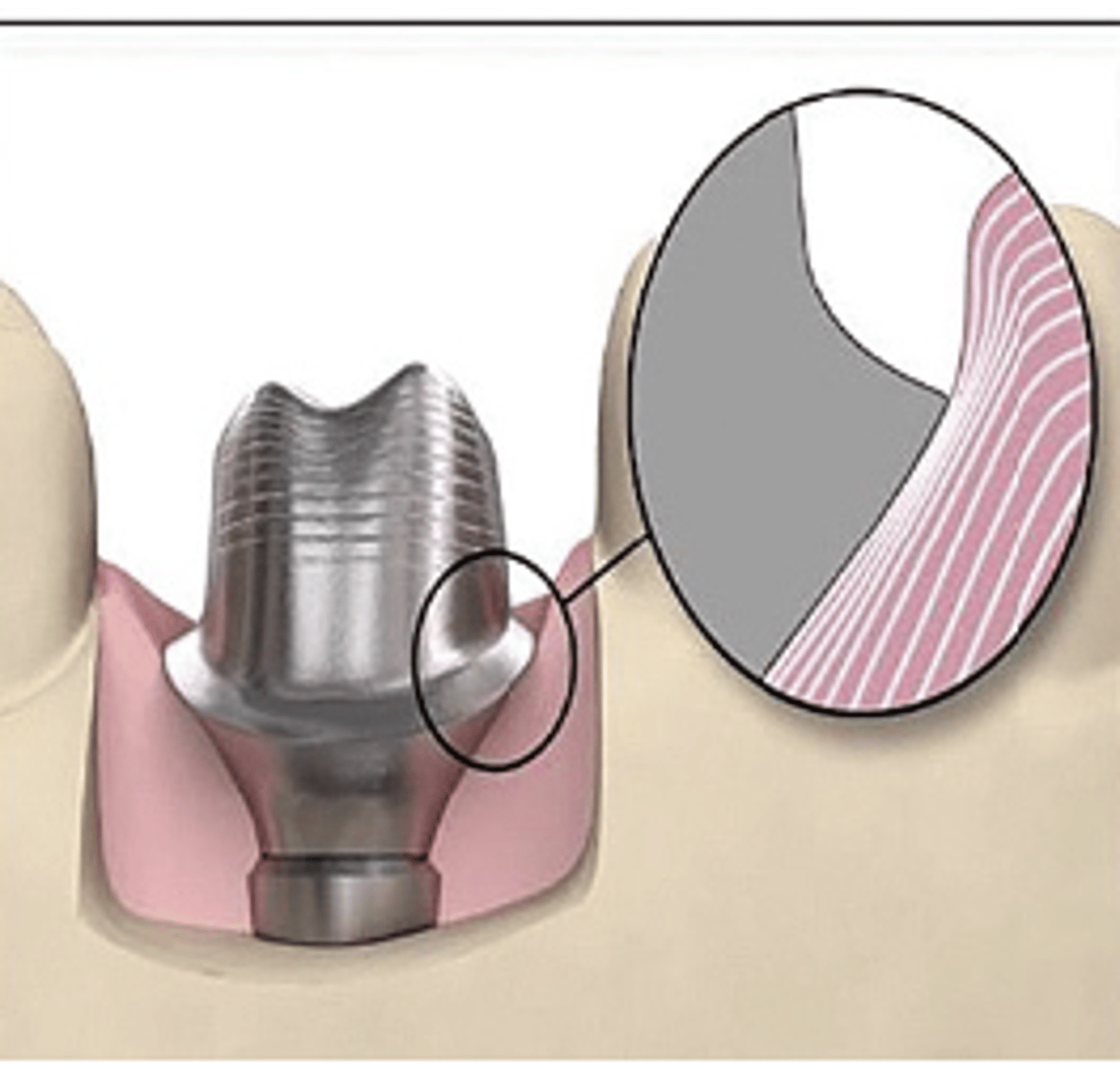
Support tissue
What type of abutment?
- Anatomically shaped abutment will be up to 0.2 mm larger than the sulcus of the silicone model of soft tissue provided with the desired emergence profile
- "Easy" insertion
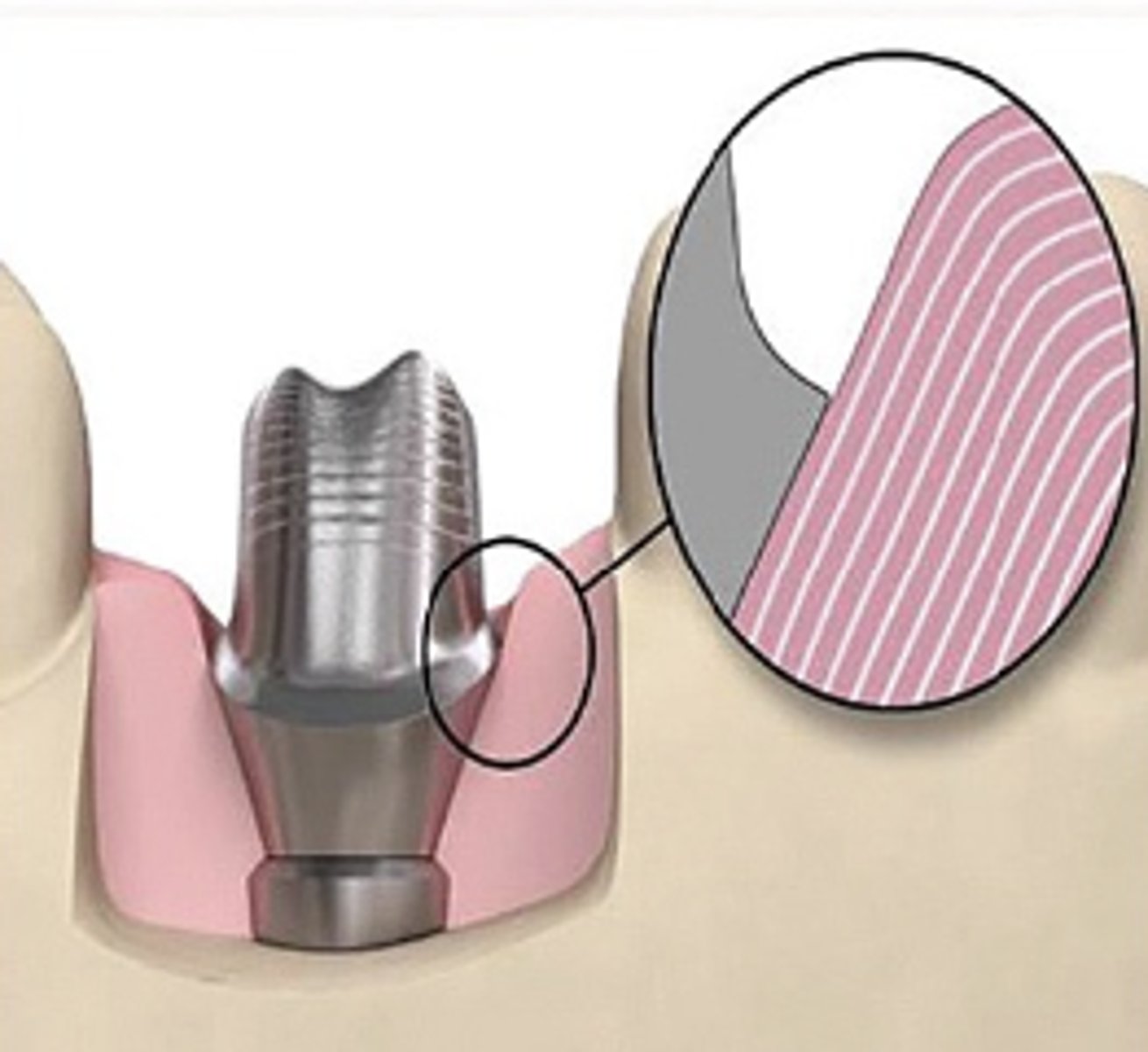
No tissue displacement
What type of abutment?
- Smallest-diameter, non-anatomically shaped abutment with no soft tissue support
- Abutment will not touch the soft tissue
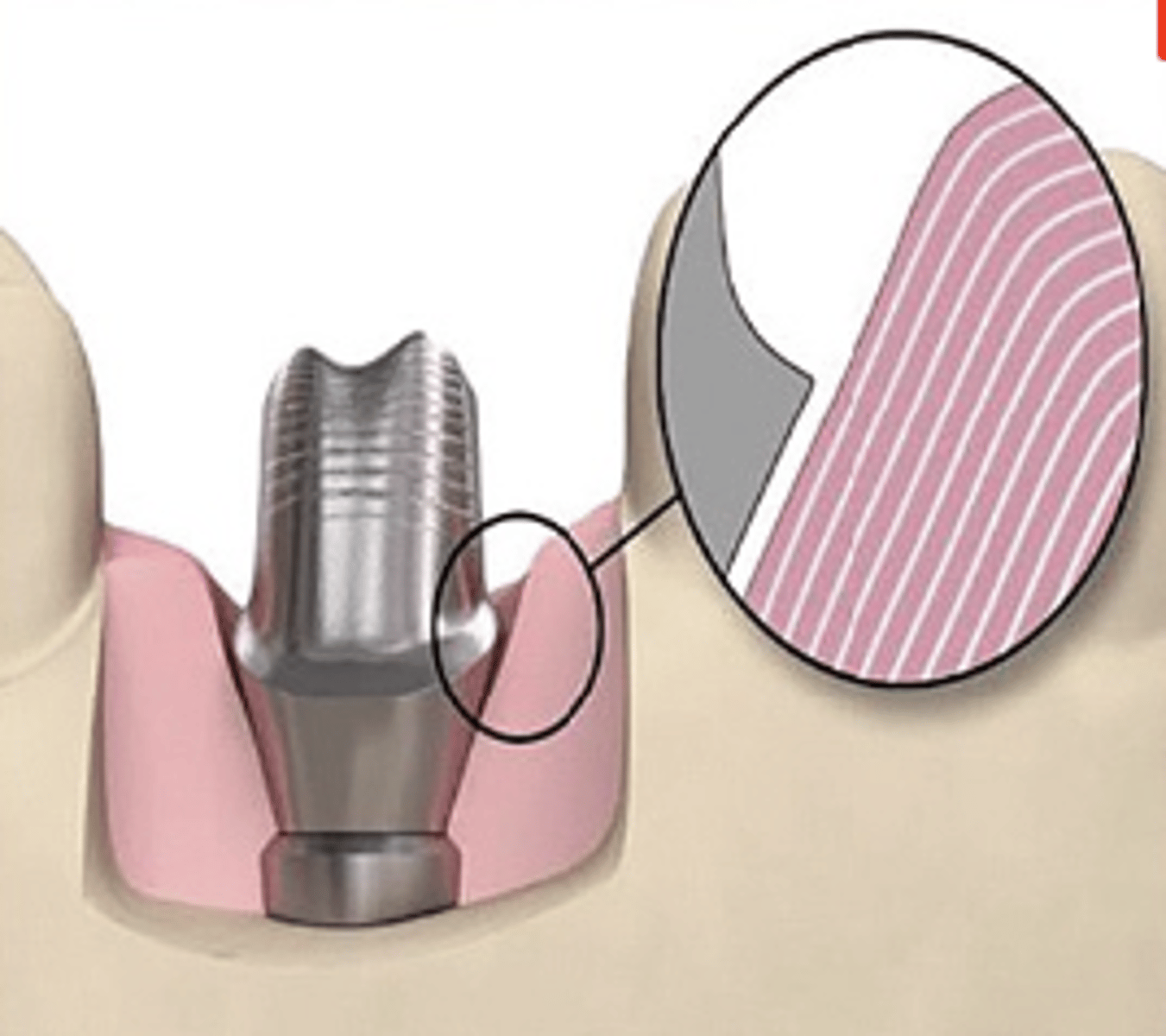
Angulated screw channel (ASC)
What has the following characteristics?
- By Nobelbiocare in 2016
- TUSDM predoctoral clinic started 2019
- Only for conical implant abutment connection mechanism
- Ceramic restorations or abutments on titanium inserts
- Screw access hole can be up to 25 degree off long-axis
- Uses special screw and screw driver (Omnigrip)
Angulated screw channel (ASC)
ID the part:
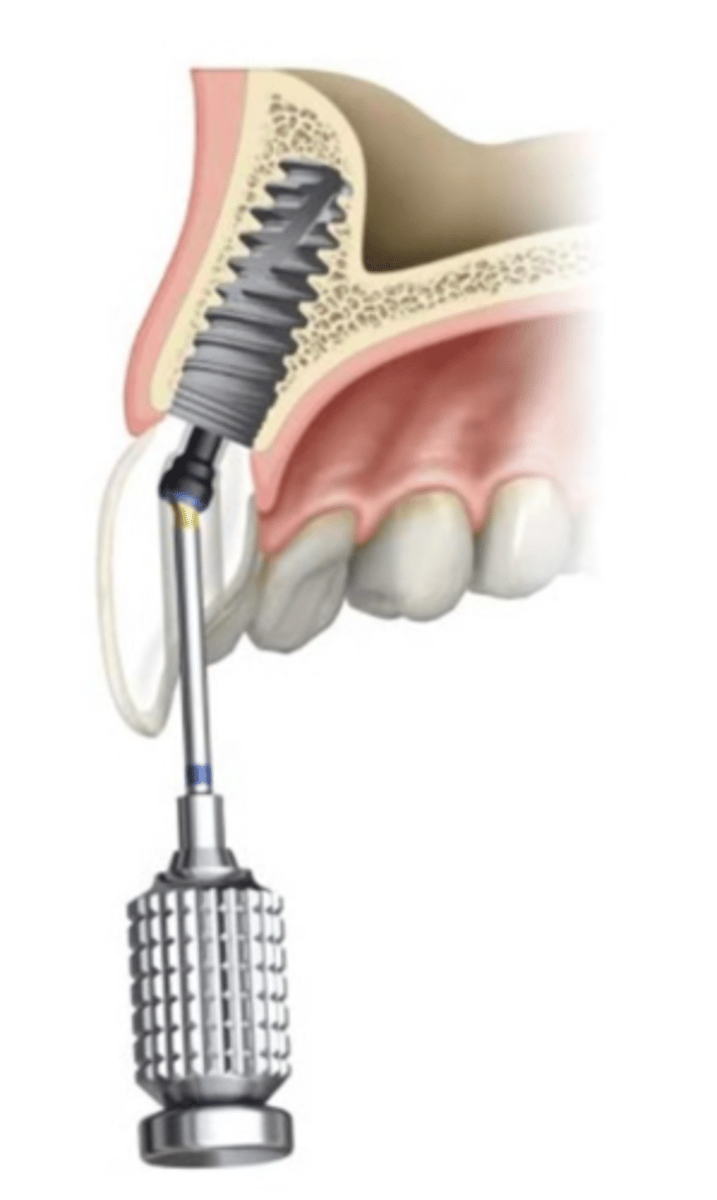
"Angled Solution" (Corrections up to 25 degrees)
What is the product from Straumann that is similar to the Angulated screw channel (ASC)?
Implant-supported ceramic crown *layered
ID the type of restoration:
- Secured directly onto implant
- Screw-retained
- Porcelain veneered over a Zr CAD/CAM engaging abutment (designed to support veneering porcelain)
- *The crown shown is layered but it can also be monolithic
- - Check lecture on Dental Porcelain
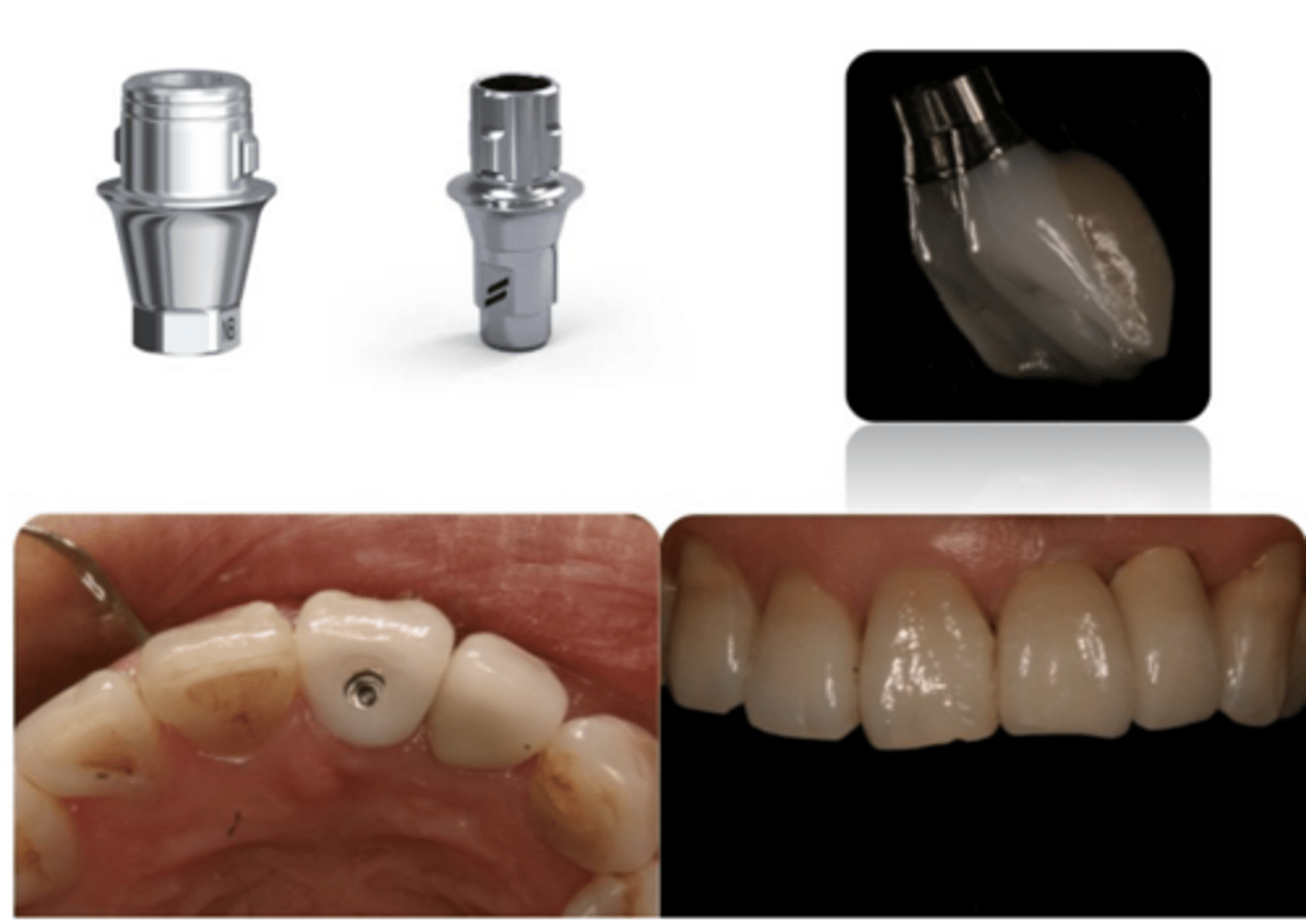
Hybrid "Screwmentable" option
ID the type of restoration:
- Implant-supported, a screw-retained restoration type that has gained more popularity recently
- Offer a promising alternative to traditional designs by combining the advantages of screw-retained and cement-retained restorations
Hybrid "Screwmentable" option
These are advantages of what restoration?
- Passive fit
- Retrievability
- Extraoral cementation
- Tissue-friendly prosthesis design
- Improved esthetics
Multiunit abutments
What type of abutment?
- Used for splinted crowns or FPDs
- Restoration can be PFM, ceramic, or full metal

Angles multiunit abutment
What type of abutment at the red box?
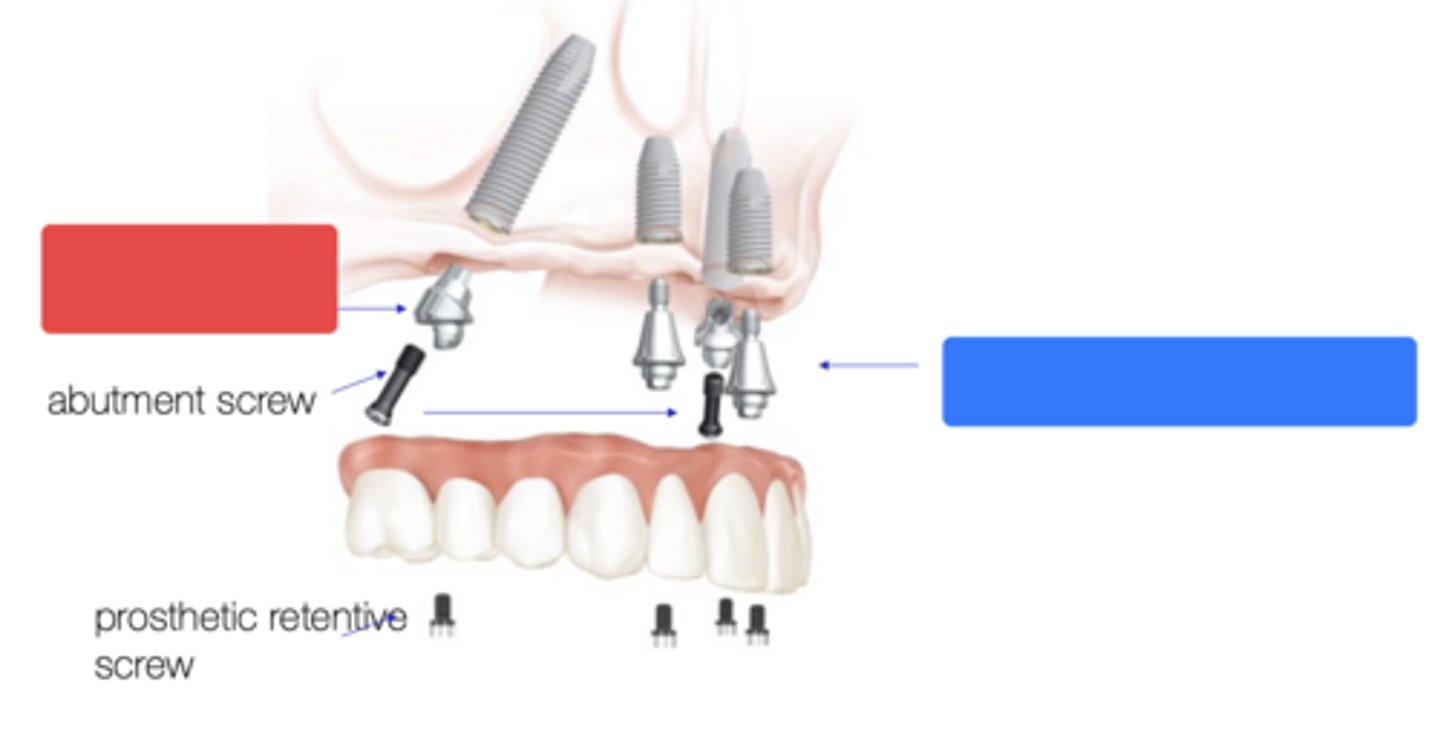
Straight multiunit abutment
What type of abutment at the blue box?
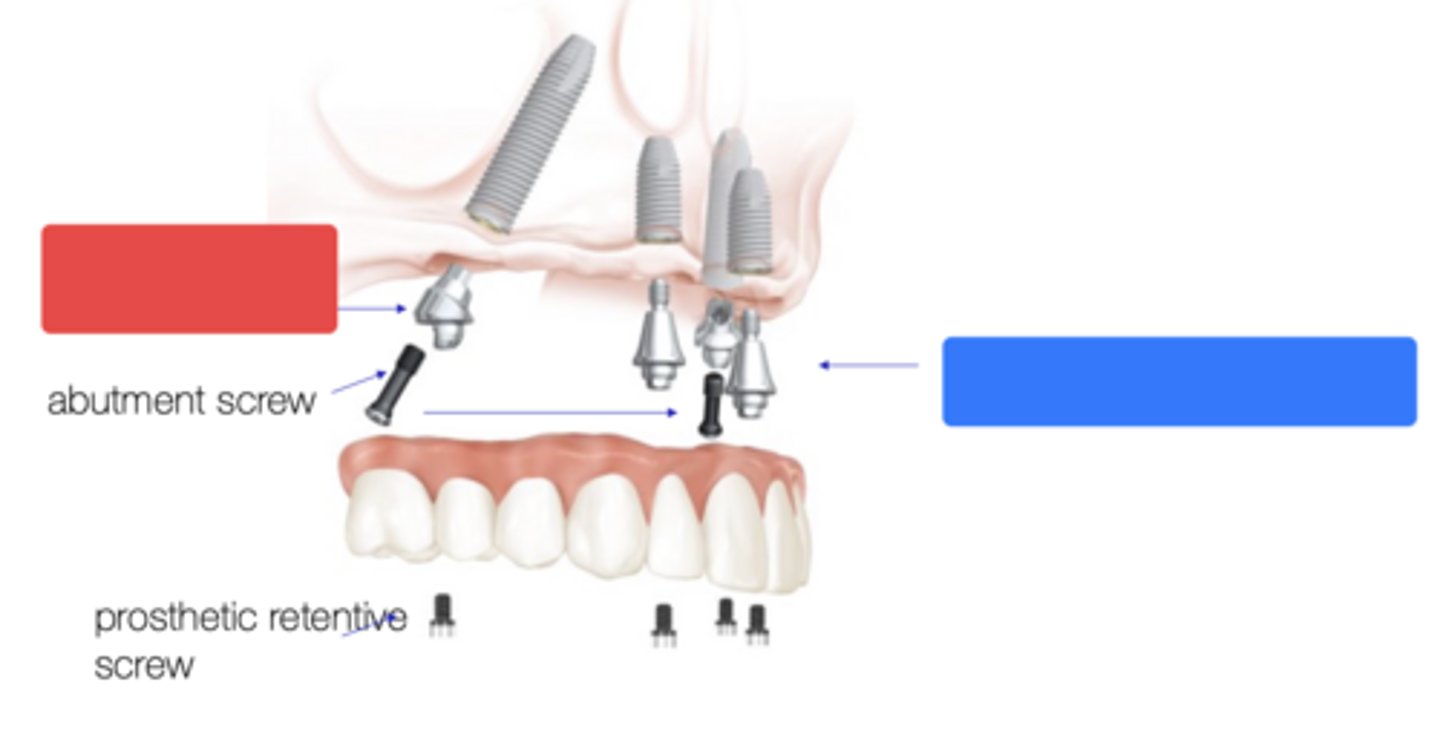
Implant
For screw-retained multiple unit restorations, use ____ support if implants are <3 mm subgingival and parallel to each other
Abutment
For screw-retained multiple unit restorations, use ____ support if implants are placed very subgingival and/or not parallel to each other
abutment
cement-retained multiple unit restorations are ALWAYS ________ supported
– Accuracy of the master casts must be verified with a verification jig
– PFM restorations require a ‘framework try-in”
– Non-engaging abutments must be used for screw-retained restorations
– Engaging abutments must be used for cement-retained restorations
The treatment sequence of multiple units is similar to single units, except... (4)
- Path of insertion
- Location of finish line
- Emergence profile
For cement-retained multiple unit restorations, what 3 things have to be considered?
- Position
- Angulation
- Interocclusal Distance
- Tissue depth/Contour
What does PAIT stand for?
“PAIT” analysis using traditional workflow
These are the steps for what workflow?
1. Make implant-level soft tissue cast
2. Mount cast
3. Cover implant with aluminum foil
4. Set up missing tooth to ideal form and position
5. Duplicate a wax up cast
6. Fabricate a clear thermoplastic template
7. Attach guide pin(s) to the implant
8. Retrofit and make access hole to facilitate seating of the clear template
9. Use PAIT to analyze proper abutment selection
Guide pin
What has the following characteristics?
- Type of laboratory screw used in the fabrication of a prosthetic restoration.
- Surgical or restorative adjunctive marker used to indicate implant angulation or location when preparing osteotomy sites
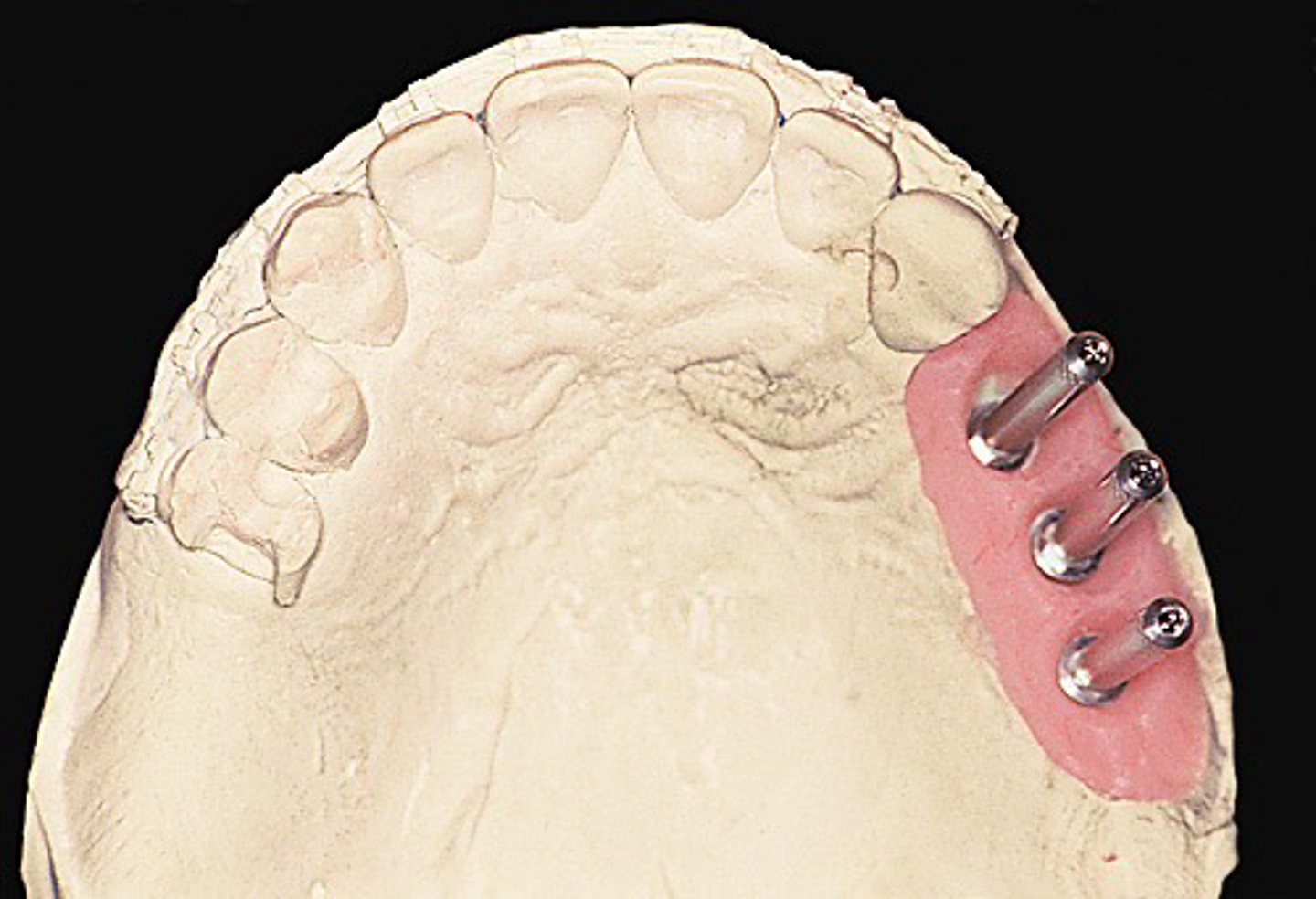
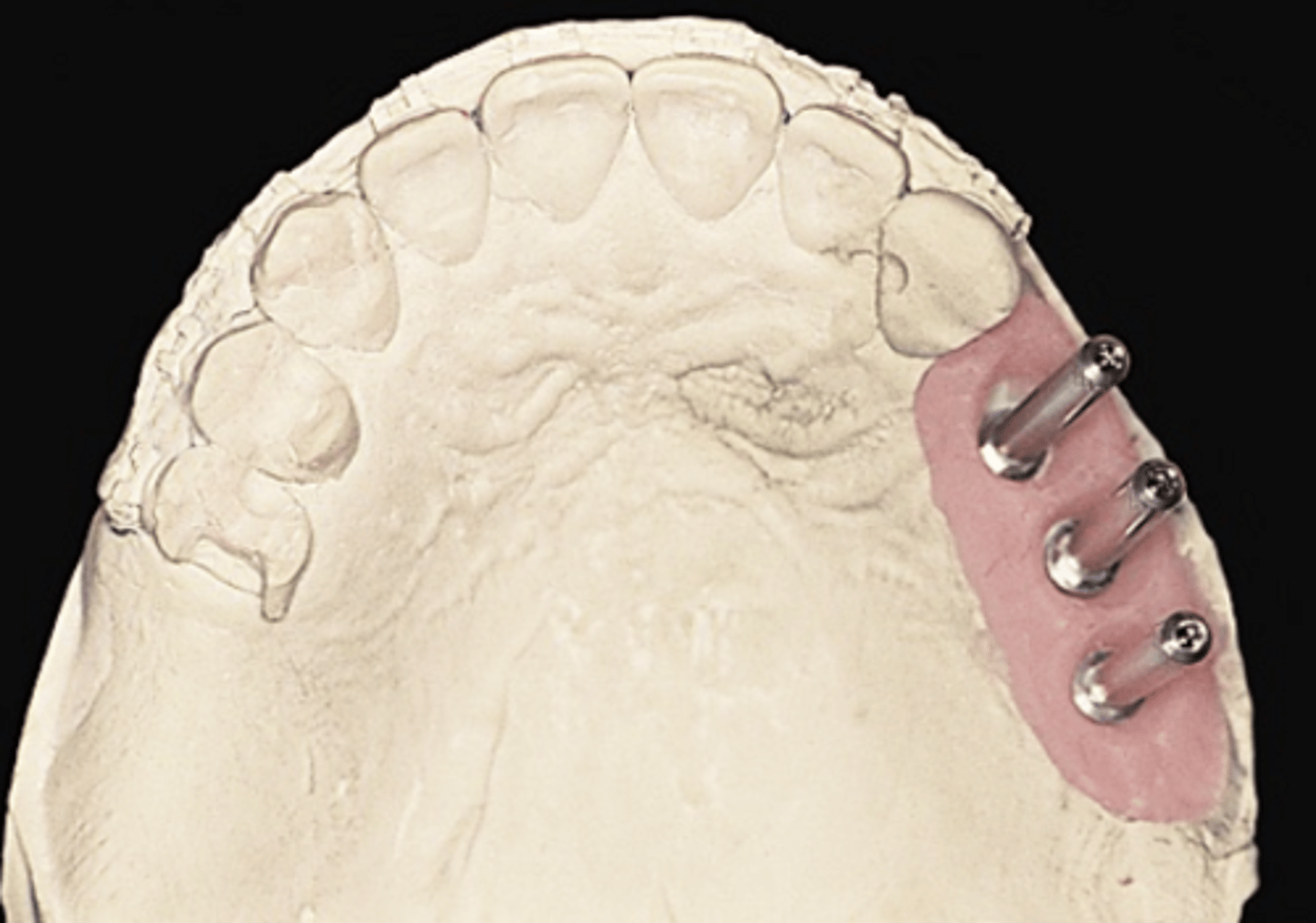
Impression coping screw
What can be used as a guide pin on the cast?
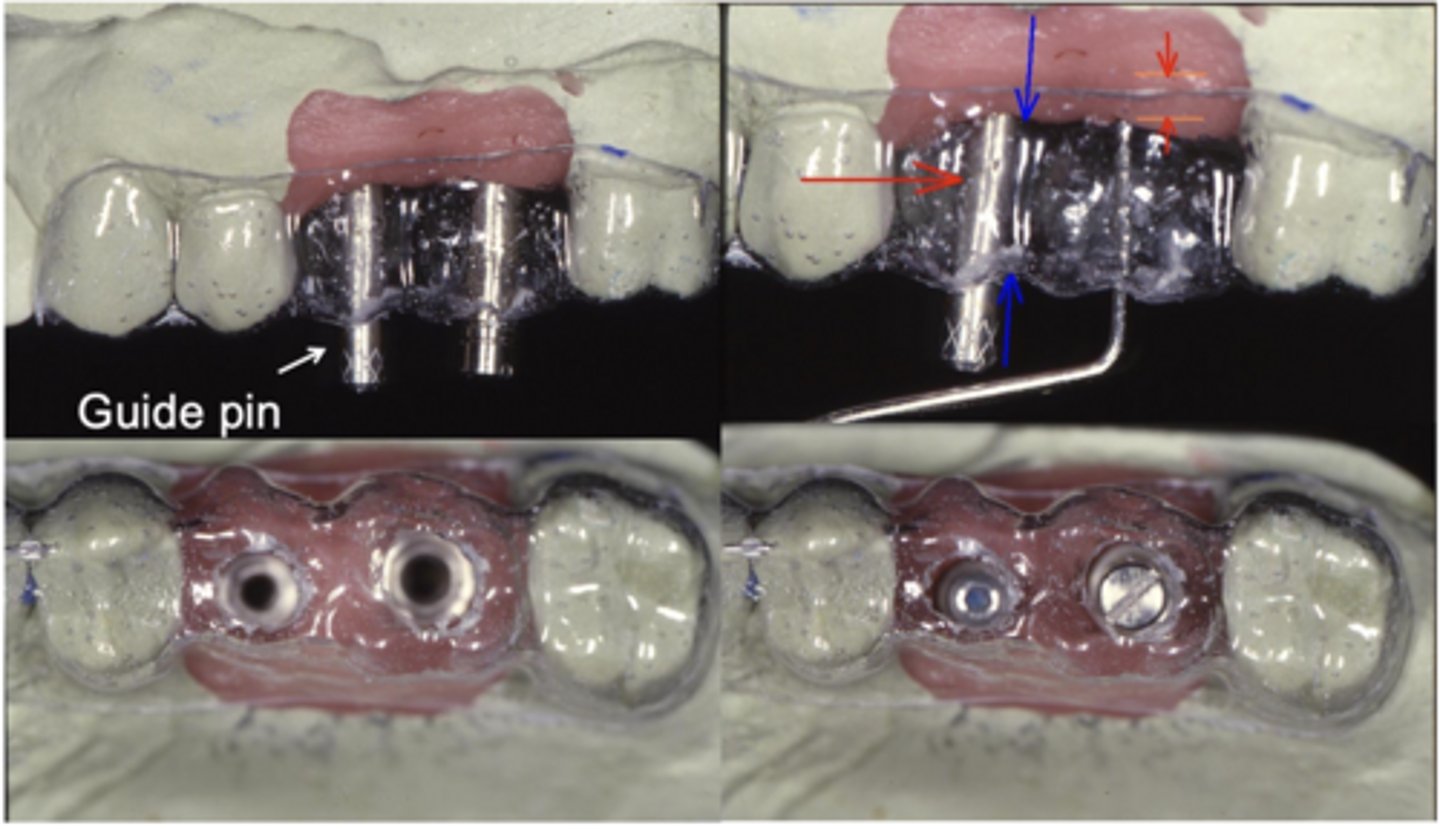
PAIT (Position, Angulation, Interocclusal Distance, Tissue depth/Contour)
What do you have to check on the implants in relation to intended restorations?
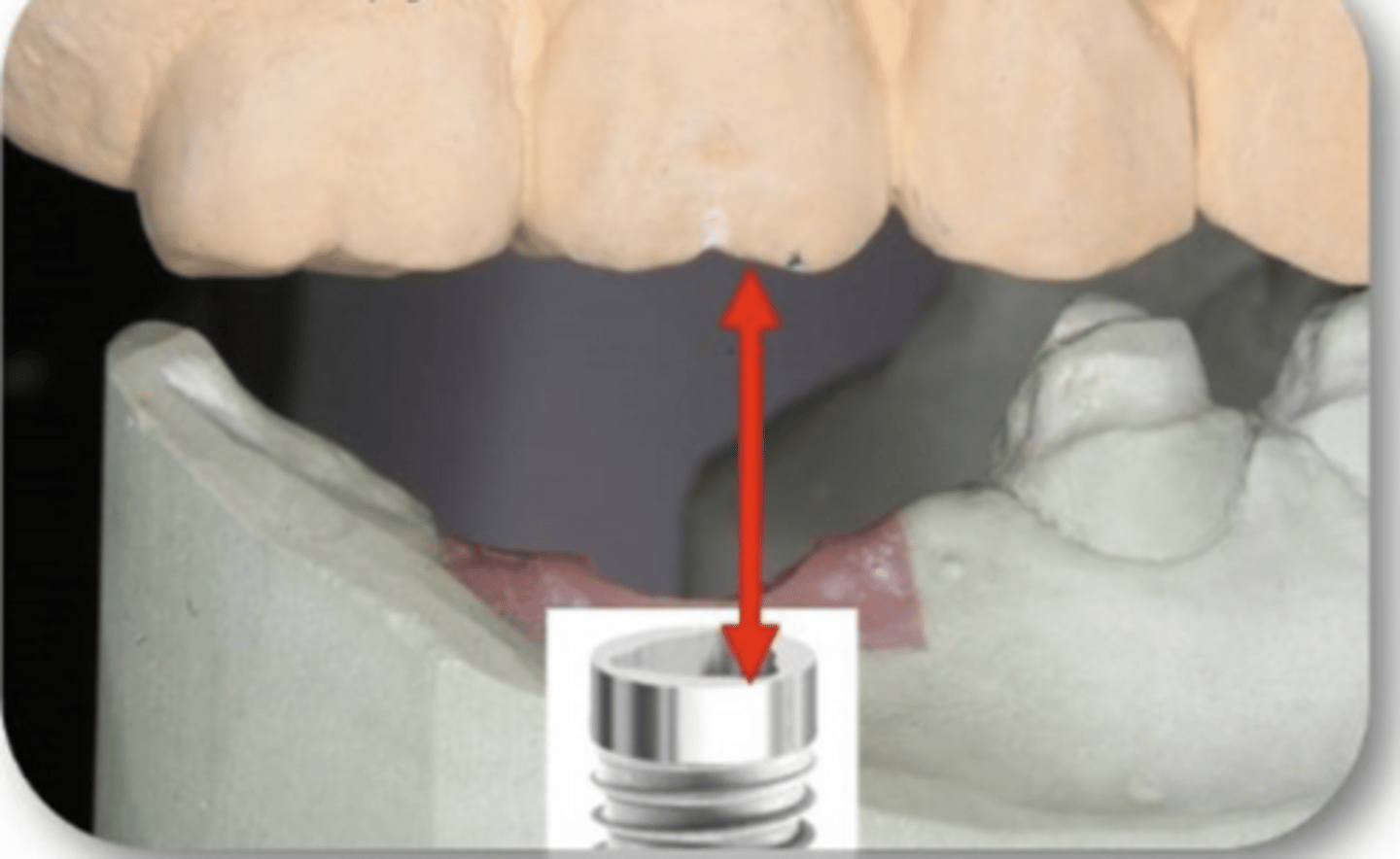
Interocclusal space
Define the following:
- Measure of the distance between the implant platform and the opposing tooth
- Limited space may dictate choice of retention (cement vs. screw) for the restoration
Interocclusal space
What is the red arrow measuring?
Tissue depth/contour
Define the following:
Measure the distance (at buccal, lingual, mesial, distal) between the implant platform and the gingival margin

Tissue depth/contour
What PAIT feature determines the collar (cuff) height of the abutment?
Restoration insertion
What is this describing?
- General principles for inserting an implant- supported prosthesis are very similar to those for delivering a tooth-supported prosthesis
- Complexity is higher when using implant- supported prostheses since they can have multiple components that fit together very precisely along limited paths of insertion
True
T/F: If the prosthesis is not correct on the models, it is not going to be correct in the patient's mouth
Checking the model
What are you checking here?
- Implant analog firmly retained on the cast
- Soft-tissue model (Gi-Mask) correctly represents the peri- implant soft tissues and is intact
- Access to implant analog clear of any obstruction
- Correct articulation of mounted casts
Checking the restoration
What are you checking here?
- Proximal contacts
- Marginal adaptation
- Occlusion
Prevents seating
Dental floss should pass with slight resistance. What happens if proximal contacts are too tight?
Food impaction
Dental floss should pass with slight resistance. What happens if proximal contacts are too light?
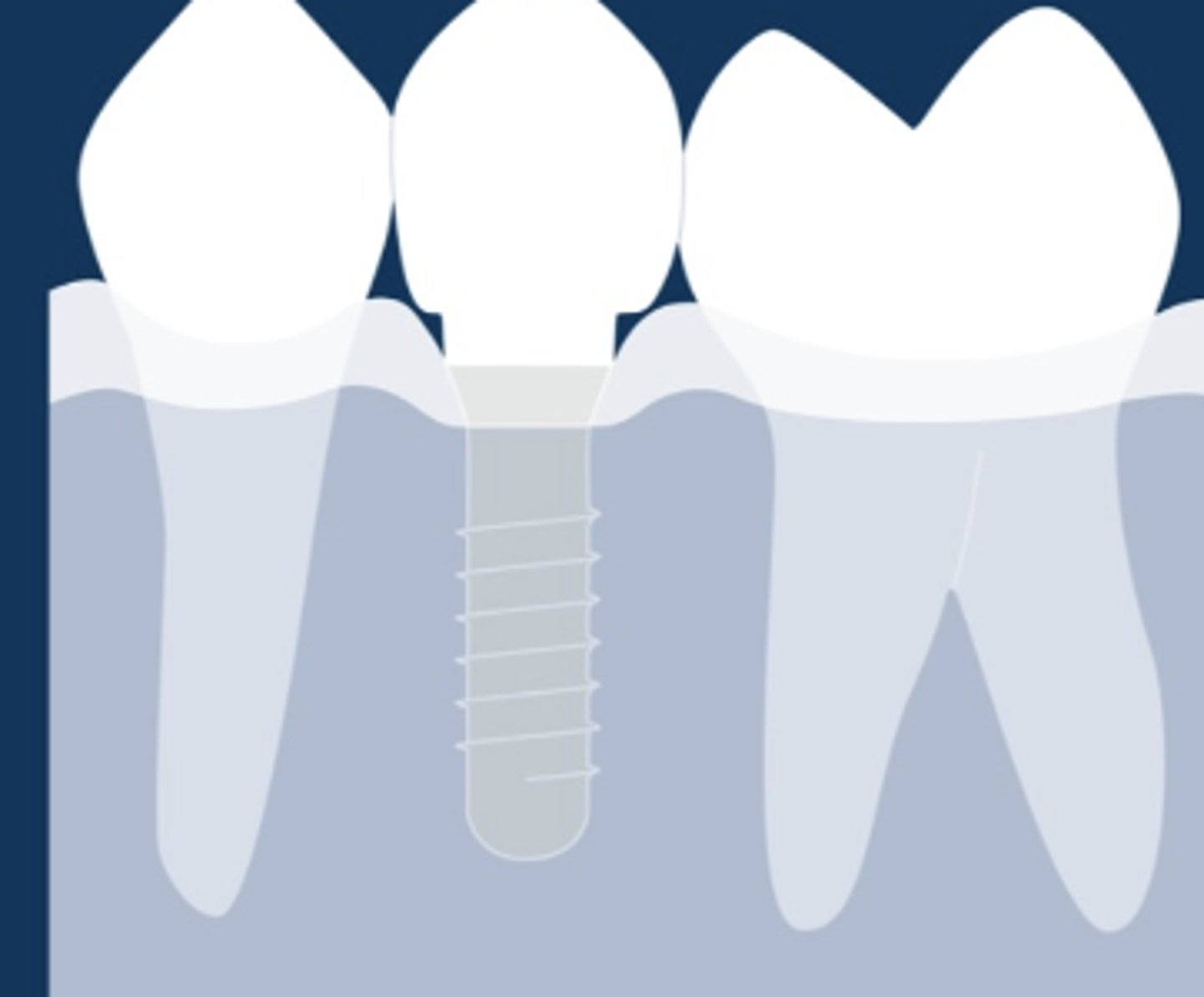
Yes
Is this emergence profile appropriate?
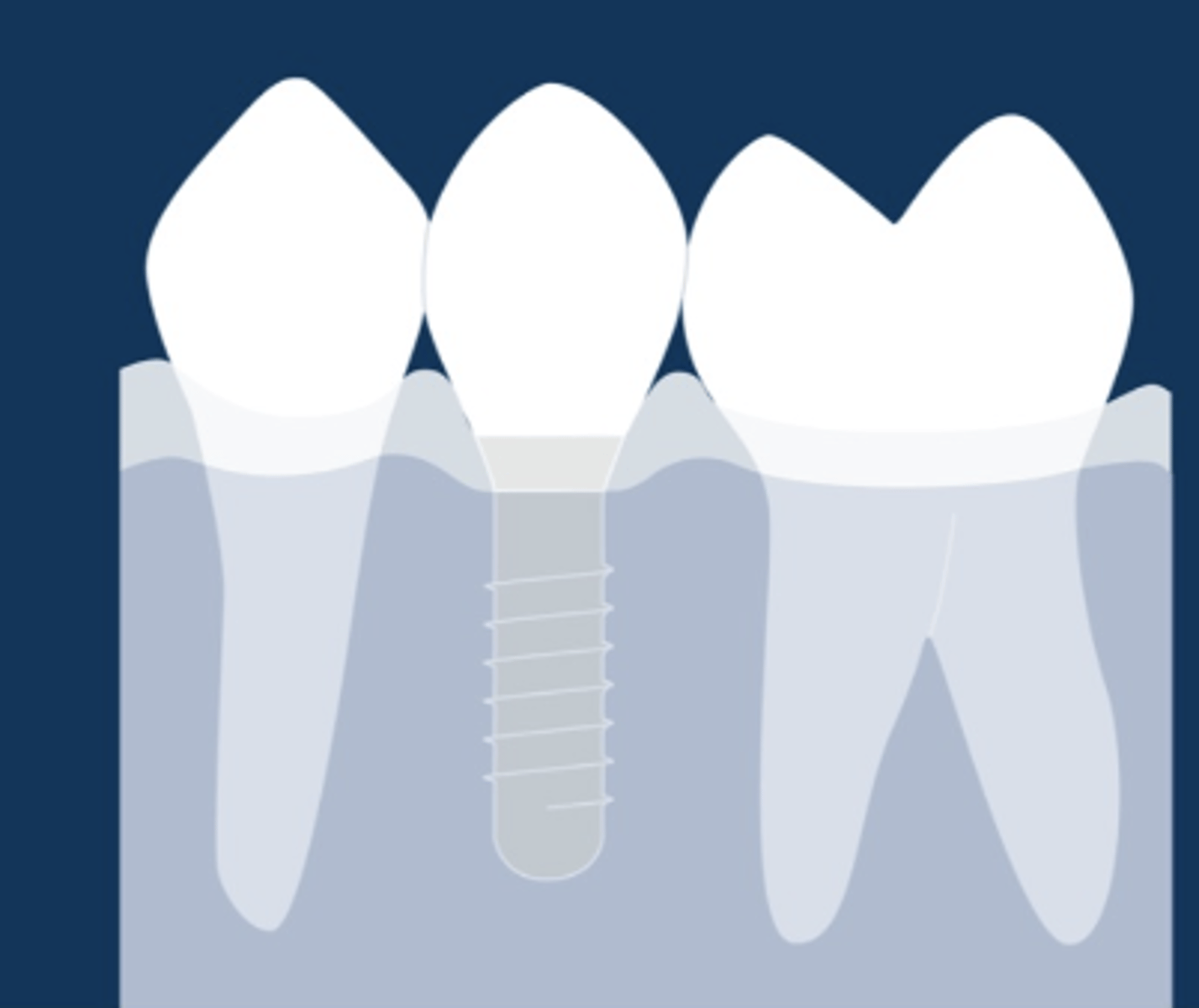
No
Is this emergence profile appropriate?
position
Define the following:
The location of the implant in relation to the intended prosthesis
- May require correction using abutments
- Unfavorablity may lead to under/overcontoured crowns or putting the implant to sleep
Angulation
Define the following:
- B M L D divergence from the intended path of insertion/prosthesis
Articulating paper: accufilm and shimstock
What materials should be used to check occlusion for an implant?
Cement retained single crown
These are the steps for what type of crown?
1. Seat the abutment and hand tighten the abutment screw
2. Verify seating with radiograph
3. Seat crown
4. Check proximal contacts, fit and occlusion
5. Esthetics
6. Tighten screw with torque wrench
7. Seal access hole
8. Cement with PROVISIONAL CEMENT
Screw retained single crown (Abutment and crown = 1 piece)
These are the steps for what type of crown?
1. Check proximal contacts after hand tightening the abutment screw
2. Verify seating with radiograph
3. Check occlusion, esthetics
4. Tighten screw with torque wrench
5. Seal access hole
6. Recheck occlusion
Framework has to be tried in for passive fit
The Framework try-in/insertion sequence for a cement retained multiple unit implant is similar to single units cement-retained EXCEPT:
One-Screw Test (Sheffield Test)
What has the following characteristics?
Test to determine passive fit when trying in or delivering a multiple-unit implant-supported prosthesis
One-screw test (Sheffield Test)
What has the following characteristics?
By inserting a screw in one end of the prosthesis and then observing whether the prosthesis lifts off of other implant or abutment platforms, the clinician can determine the presence or absence of movement when that single screw is tightened, either by clinical or radiographic visualization of the prosthesis
- Ideally, there should be no movement or lift-off of the prosthesis from its passive seating.
Cut and solder framework or remake
How could you fix this if it does not have a passive fit?

Access holes
Define the following:
Opening in a replacement tooth's occlusal or lingual surface of an implant-retained prosthesis that provides entrance for abutment or prosthesis screw placement or removal
Sealing screw access hole(s)
What process is this?
- Tighten screw with appropriate (recommended) torque
- Apply intermediate soft material
- In order not to damage crown or screw, when reopening the obturation with a diamond bur, chose a material, that can be easily removed
- Recommended material options: e.g. cotton pellet, guttapercha, silicone, temporary composites such as e.g. 'Fermit'/'Telio CS inlay'
- Finalize obturation with a suitable light curing composite restorative material (universal / posterior use, depending on indication)
- Ensure correct occlusion, finish, polish
- Cotton pellet + composite
- Gutta percha + composite
- Teflon tape + composite
Screw access holes HAVE to be sealed and can be sealed with (3)
- Retrievability (type of cement, abutment factors)
- Avoid excess (residual) cement
When choosing cementation always think about (2)
Subgingivally
Residual cement increased as margins were located more __________
10x
At 2 - 3mm subgingival, residual cement is _____x as much as at 0 - 1mm
True
T/F: Excess cement can cause peri-mucositis or peri-implantitis
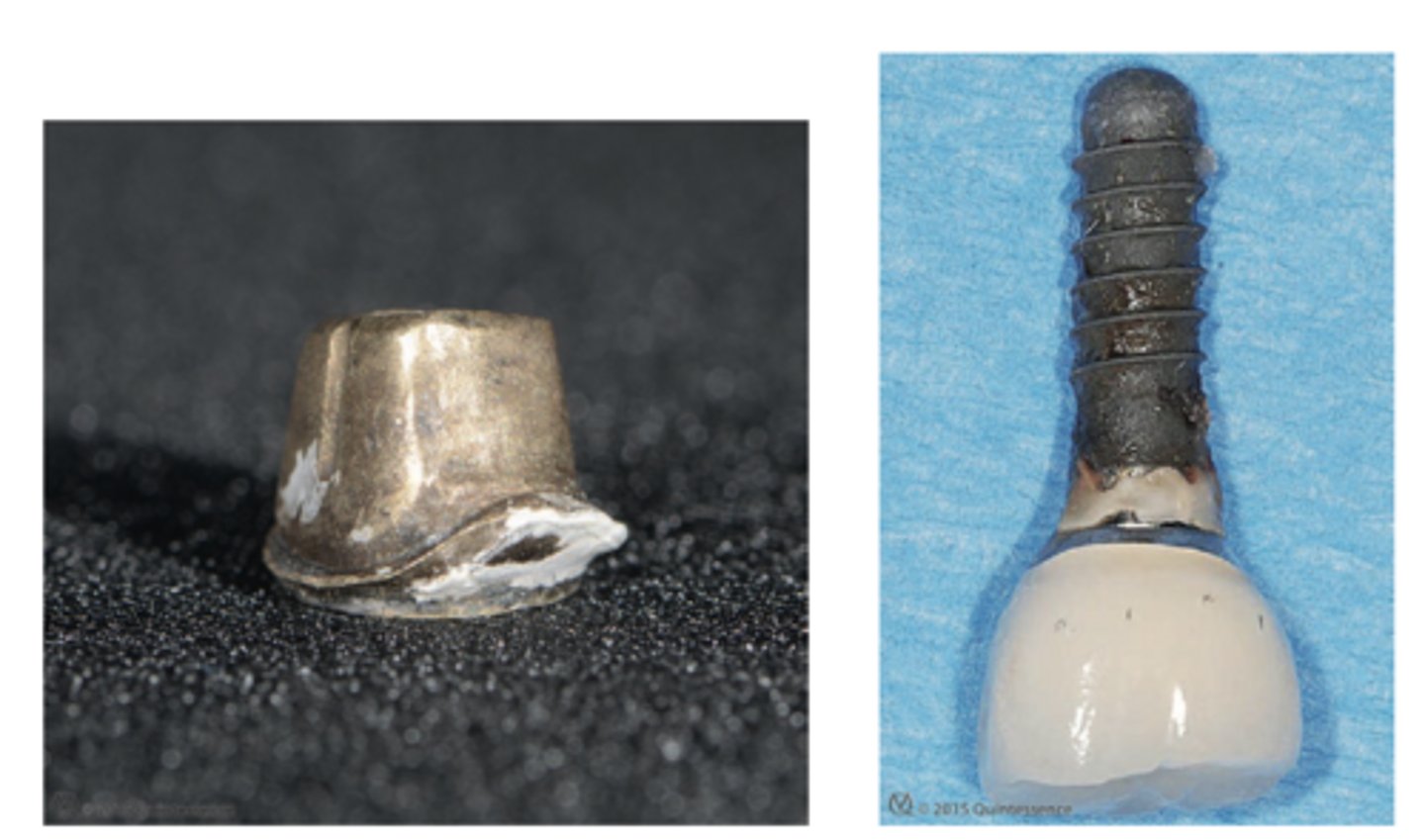
- The implant crown is lined with a spacer (PTFE tape)
- Fast-setting polyvinyl siloxane is injected in the crown
What is the ideal way to use cement to place a crown?
ALL CHOICES
Which of the following methods will result in impaction of cement into the periimplant sulcus if the prosthesis has a subgingival margin?
A) Gross application
B) Brush application
C) Rim application