Hearing & Vision PPT
1/54
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
55 Terms
At the completion of this module, the learner will be able to:
1.Explain the importance of sensory function and the impact of sensory deficits on older adults.
2.Describe the effects of aging on sensory function.
3.List measures to promote healthy sensory function in older adults.
4.Identify signs of and nursing interventions for older adults with cataracts, glaucoma, macular degeneration, and hearing impairment.
5.Identify the most common cause of blindness in people over 65 years.
OBJECTIVES
OBJECTIVES
what are the effects of aging on vision?
•Reduced elasticity and stiffening of the muscle fibers of the lens (presbyopia)
•Visual acuity declines 2/2 reduced pupil size, opacification of the lens and vitreous, loss of photoreceptor cells in retina
•Light perception threshold decreases
•Dark and light adaptation takes longer, difficulty with vision at night
•Increased sensitivity to glare
•Distortion in depth perception and reduced peripheral vision
•Produce fewer tears (dry eyes)
•Increased incidence of blindness
what are some communication challenges related to vision in the OA?
•Facial expressions and gestures may be missed or misinterpreted.
•Limitation of lip reading and written communication.
•Remaining aware of current events through newspapers, socialization using social media, playing games may be hampered.
how do we promote healthy vision?
•Routine examinations including tonometry by ophthalmologist
•Consideration of financial ability to receive treatment; community resources, Medicare
•Prompt evaluation of symptoms that may indicate a visual problem: burning or pain in eye, blurred or double vision, redness of conjunctiva, spots, headaches, etc.
•Variety of disorders can cause damage to retina: arteriosclerosis, diabetes; nutritional deficiencies, hypertension can lead to visual impairment
•Vitamin, nutrients and fatty acids are essential
what are the portions of NURSING assessment for vision in OAs?
•Nurses need to be skilled at assessing vision and hearing function and presence of deficits
—•Assess with each visit or hospitalization
—•Ask about assistive devices used
•Correct implementation of assistive techniques to promote maximum sensory function
what are some nursing problems related to vision or hearing loss/deficit?
•Self-care deficits; potential negative self-concept
•Sleep disturbances; day and night disregulation
•Communication deficit
•Pain; risk of injury
•Anxiety; risk of social isolation
•Reduced social engagement; reduced activity
define cataracts
•Clouding of the lens and loss of transparency
•Leading cause of low vision in older adults
what are the risk factors for cataracts?
exposure to ultraviolet B, diabetes, cigarette smoking, high alcohol consumption, eye injury
your pt presents w the following:
•Visual acuity not affected at first; as opacification continues, vision distorted, decreased night vision, blurred objects, glare from sunlight and bright lights extremely bothersome; nuclear sclerosis develops, lens becomes yellow or yellow-brown, pupil changes color
what’s going on?
cataracts
what the tx for cataracts/surgery?
Need for surgery must be evaluated on an individual basis:
•If single cataract, may not need surgery
•Concentrate on strengthening existing visual capacity, reducing limitations, using safety measures
define glaucoma
•Damage to the optic nerve from an above normal intraocular pressure (IOP)
•Second leading cause of blindness in older adults
•Incidence: occurs in people over 40, increases in prevalence with age
what are the causes of glaucoma
•exact cause unknown; associated with increased size of lens, iritis, allergy, endocrine imbalance, emotional instability, family history; drugs with anticholinergic properties can exacerbate glaucoma
(•Types: acute, chronic)
what are the characteristics of ACUTE glaucoma?
•Severe eye pain, headache, nausea, and vomiting
•Rapid increase in tension and edema of ciliary body, dilation of pupil; vision becomes blurred, blindness will result if not corrected within a day = needs early treatment
how do we dx acute glaucoma?
with ophthalmoscope and tonometry to measure IOP; gonioscopy
how do we tx acute glaucoma?
carbonic anhydrase inhibitors (ex: acetazolamide (Diamox), mannitol, urea, and glycerin; iridectomy
what are the characteristics of chronic glaucoma?
•(open angle)
•Most common form
•Screening is important for early detection
your pt presents w the following:
peripheral vision becomes slowly impaired, frequent changing of eyeglasses; as progresses, central vision affected, tired feeling in eyes, headaches, misty vision, seeing halos around lights, cloudy appearance to cornea, iris fixed and dilated; may affect one or both eyes
what’s going on?
chornic glaucoma
how is chronic glaucoma dx and treated?
•Diagnosis with ophthalmoscope and tonometry to measure IOP; gonioscopy
•Treatment/management: miotic & carbonic anhydrase inhibitor; surgery; laser trabeculoplasty
what happens if vision is lost in glaucoma?
•Vision lost cannot be restored
what are the features of care and prevention of complications for glaucoma?
•Avoiding situations or activities that increase IOP
•Avoid emotional stress
•Careful monitoring of all medications
•Carry card or wear bracelet – stating type of glaucoma and medication
•Avoid abuse and overuse of the eyes
what are the features of pt compliance for glaucoma tx?
•compliance can be challenging
•Memory, manual dexterity
define macular degeneration?
•Most common cause of blindness in adults over the age of 65
•Damage or breakdown of the macula leading to loss of central vision
what’re the causes of macular degeneration?
•involutional macular degeneration (most common) associated with aging; exudative macular degeneration results from injury, infection
what’s the tx of macular degeneration?
laser therapy, magnifying glasses, high-intensity reading lamps, other aids
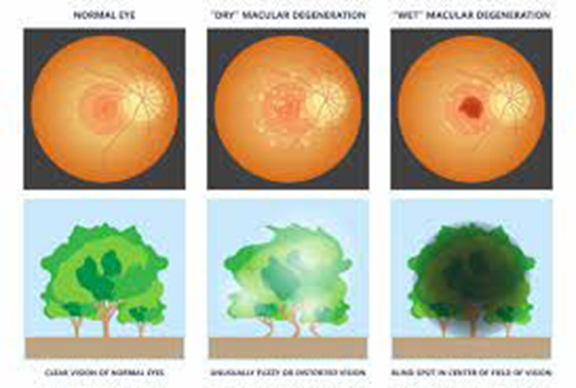
macular degeneration visual
macular degeneration visual
what’s is the part of the eye that processes what you see directly in front of you. Controls central vision.
the macula (what’s affected in macular degen)

vision visual
vision visual
what’s going on when there;s a detached retina?
•Forward displacement of the retina
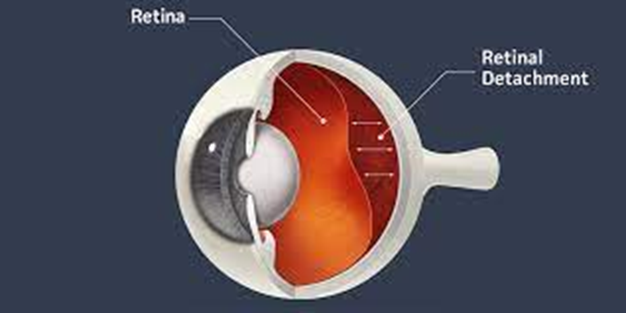
detached retina visual
detached retina visual
your pt presents w the following:
•Gradual or sudden: perception of spots moving across eye, blurred vision, flashes of light, feeling that a coating is developing over eye; blank areas of vision progress to complete loss of vision
what’s going on?
detached retina
what are the portions of tx for detached retina?
•Prompt treatment to prevent continued damage and eventual blindness
•Treatment/management: initially, bed rest and eye patches; surgery (electrodiathermy, cryosurgery, scleral buckling, photocoagulation)
what are the nursing interventions for a detached retina?
•Help patient feel as safe as possible (bilateral eye patches)
•Frequent checks, communication, verbal stimuli
•Easy access to call light
•Minimize anxiety, enhance psychological comfort
•Avoid physical and emotional stress
•Emphasize importance of periodic examinations
•Often must remain head down for several days/weeks after surgery
what’s a corneal ulcer?
•Inflammation of the cornea accompanied by a loss of substance
what are some predisposing factors to corneal ulcers?
febrile states, irritation, dietary deficiencies, lowered resistance, cerebrovascular accident
what can corneal ulcers cause?
•May scar or perforate, leading to destruction of cornea and blindness
your pt presents w the following:
affected eye may appear bloodshot, increased lacrimation, pain, photophobia
what’s going on?
corneal ulcer
what’s the tx/management for corneal ulcer?
•Cycloplegics, sedatives, antibiotics, heat
•Sunglasses to ease discomfort of photophobia
•Treat underlying cause: infection, abrasion, foreign body
•Corneal transplants
what are the BROAD nursing considerations when tx a pt w vision loss?
•Face person when speaking
•Use several soft indirect lights not a single glaring one
•Use large print reading material
•Place frequently used items within visual field
•Avoid use of low-tone colors; use bright ones
•Use contrasting colors on doorways and stairs and for changes in levels
•Identify personal belongings, room with unique design rather than letters or numbers
what’re some ways we can promote healthy hearing?
•Encourage prompt/complete treatment of infections
•Prevention of trauma to ear
•Regular audiometric examinations
•Assessment for impacted cerumen
• Irrigation (discourage cleaning with q-tip)
•Education
• Environmental noise; protection from exposure
what are the effects of aging on hearing?
•Communication difficulty( Age-related sensorineural hearing loss (presbycusis); Impacted cerumen)
•Self-conscious of limitation and avoid interactions leading to social isolation
•Underlying cause determined by professional evaluation(Audiometric examination)
what are the characteristics of hearing deficits in the OA?
•Incidence/prevalence: majority of older adults, higher in men
•Causes: exposure to loud noise, recurrent otitis media, trauma, ototoxic medications, diabetes, tumors of nasopharynx, hypothyroidism, syphillis, psychogenic factors
define Presbycusis
agre related hearing loss
what can cause inner ear problems?
•Vascular disorders, viral infections
what can cause middle ear problems?
•Otosclerosis
what can cause tinnitus?
ear injury, medications, cardiovascular disease
what’s the tx for tinnitus?
•correcting underlying problem, medications, coping strategies, alternative therapies
what types of infxs can cause hearing deficits?
•Middle ear infections less common in older adults
Usually accompany more serious disorders, e.g., tumors, diabete
what external ear features can cause hearing deficits?
•Dermatoses, furunculosis, cerumen impaction, cysts, neoplasms
what are the characteristics of hearing aids?
•Need for complete audiometric examination by
an otologist or audiologist
•Requires a prescription
•Variety of styles
•Improves hearing, does not return to baseline
•Difficulties with using a hearing aid: all sounds amplified
•Education: start by wearing hearing aid for short periods of time each day, gradually increase time used; avoid use in noisy environments
what are the features of hearing aid CARE?
•Turn aid off or remove battery when not being worn. Store in safe, padded container.
•Clean at least weekly
•Protect from exposure to extreme heat (e.g., hair dryers), cold weather, or moisture.
•When changing battery, turn off first.
•Keep several new batteries available (Typically, a battery will last about 80 hours.)
how often do hearing aids need to be cleaned and how is this done?
•at least weekly
•Wipe off and use toothpick, pipe cleaner, or pick to clean channel. Do not use alcohol, can cause drying and cracking. Avoid having hairspray, gels, or other chemicals come in contact with aid.
what are the portions of pt care for those w hearing deficits?
•Impaired hearing associated with social isolation, depression, risk of dementia, higher mortality rate
•Encourage audiometric testing as deficit may not be age-related
•Alert neighbor to help in emergencies, place close to nursing station, provide written information
•Provide touch as a means of sensory stimulation as well as expressions of warmth and caring
Is the following statement true or false?
It’s okay for your patient to purchase a hearing aid from a catalog if he or she is having financial difficulties.
False
(Rationale: A hearing aid should never be purchased without being specifically prescribed. Sometimes older persons will attempt to improve hearing by purchasing an aid through a private party or a mail-order catalog, which often results in disappointment and a waste of money from an already limited budget. The nurse is in a key position to educate the older individual on the importance of consulting an otologist before purchasing a hearing aid.)
Is the following statement true or false?
Patient compliance with treatment for glaucoma can be challenging for the older adult population.
True
Rationale: Compliance with the treatment regimen for glaucoma can be a challenge for the older adult. The silent nature of glaucoma, difficulties in instilling eye drops, and the cost of the medications may contribute to a lack of adherence to the plan of care.
Which type of visual problem is associated with macular degeneration?
Rationale: Macular degeneration is the most common cause of blindness in people over age 65 and involves damage or breakdown of the macula, which results in loss of central vision.
Loss of central vision