NCLEX: Mark Klimek - Lecture 3 (CCBs, Cardiac Arrhythmias, Chest Tubes, Congenital Heart Defects, & Infectious Disease and Precautions)
1/90
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
91 Terms
What do Calcium Channel Blockers do?
They relax and slow down the heart.
What cardiac effects do Calcium Channel Blockers have?
(-) Inotropic, chronotropic, and dromotropic
What is an inotropic agent?
Drugs that alter the contractility of the heart.
(+) Strengthens contractility = Improved CO
(-) Weakens contractility = Decreased CO
What is a chronotropic agent?
Drugs that alter the heart rate.
(+) Increased rate of impulse at SA node = Increased HR
(-) Decreased rate of impulse at SA node = Decreased HR
What is a dromotropic effect?
Changes of the rate of electrical impulses in the heart.
(+) Increased speed travel from SA to AV.
(-) Decreased speed travel from SA to AV.
What are the 3 issues that you would want to relax and slow down the heart?
"A, AA, AAA"
Anti-hypertensives
Anti-Anginal drugs
Anti-Atrial Arrhythmias
What are the main side effects of Calcium Channel Blockers?
Headache and hypotension
What are some Calcium Channel Blocker drugs?
Drugs ending in "-dipine," NOT just "-pine!"
Also... Verapimil, Cardizem (Diltiazem)
What route is Cardizem (Diltiazem) given?
Continuous IV drip
Before putting a patient on CCB, what are the parameters to assess?
Assess for BP.
Hold if SBP <100.
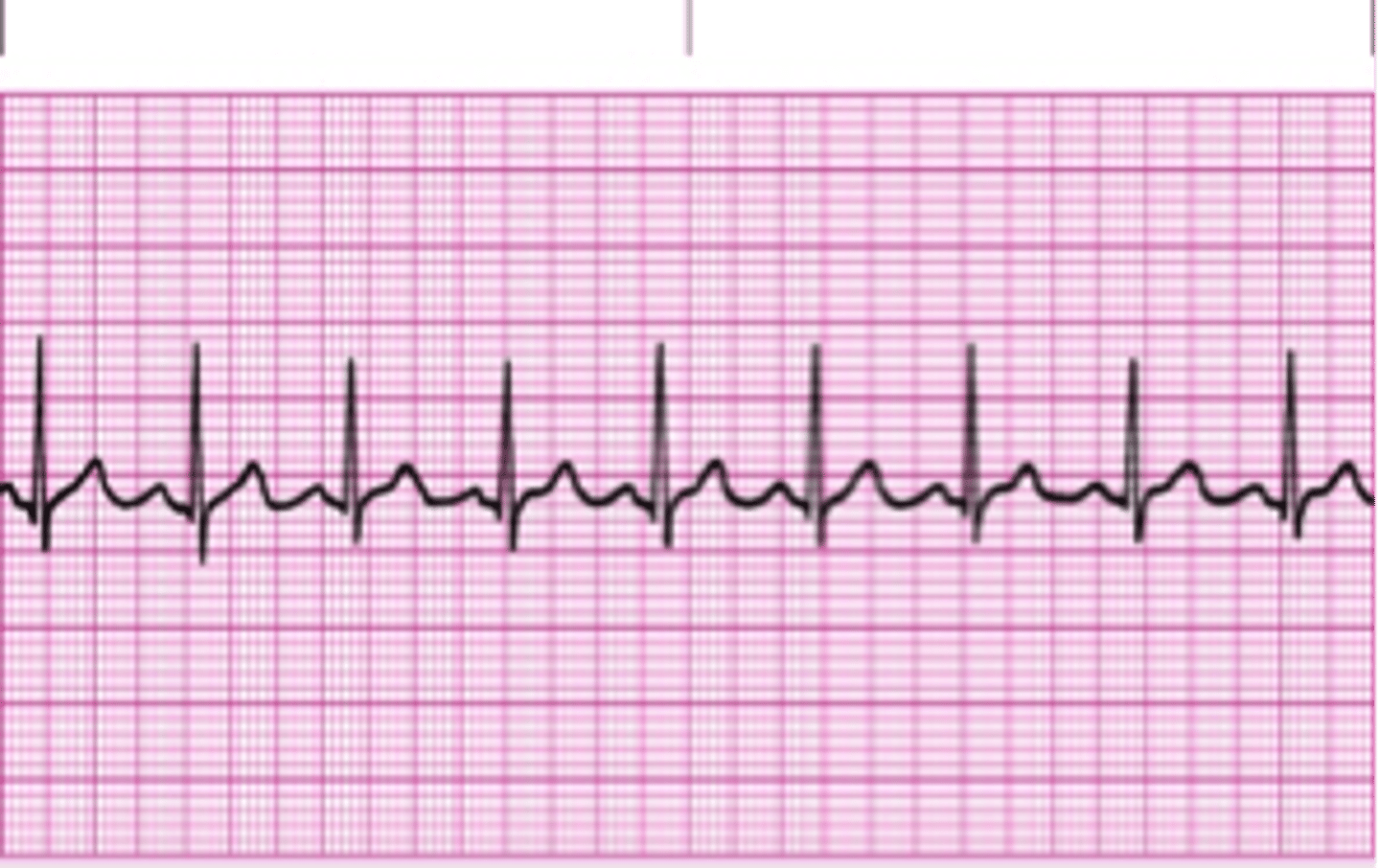
There is a P wave, followed by a QRS, followed be a T wave for every complex. Peaks of the P wave is equally distant to the QRS, and fall within 5 small boxes.
Normal Sinus Rhythm
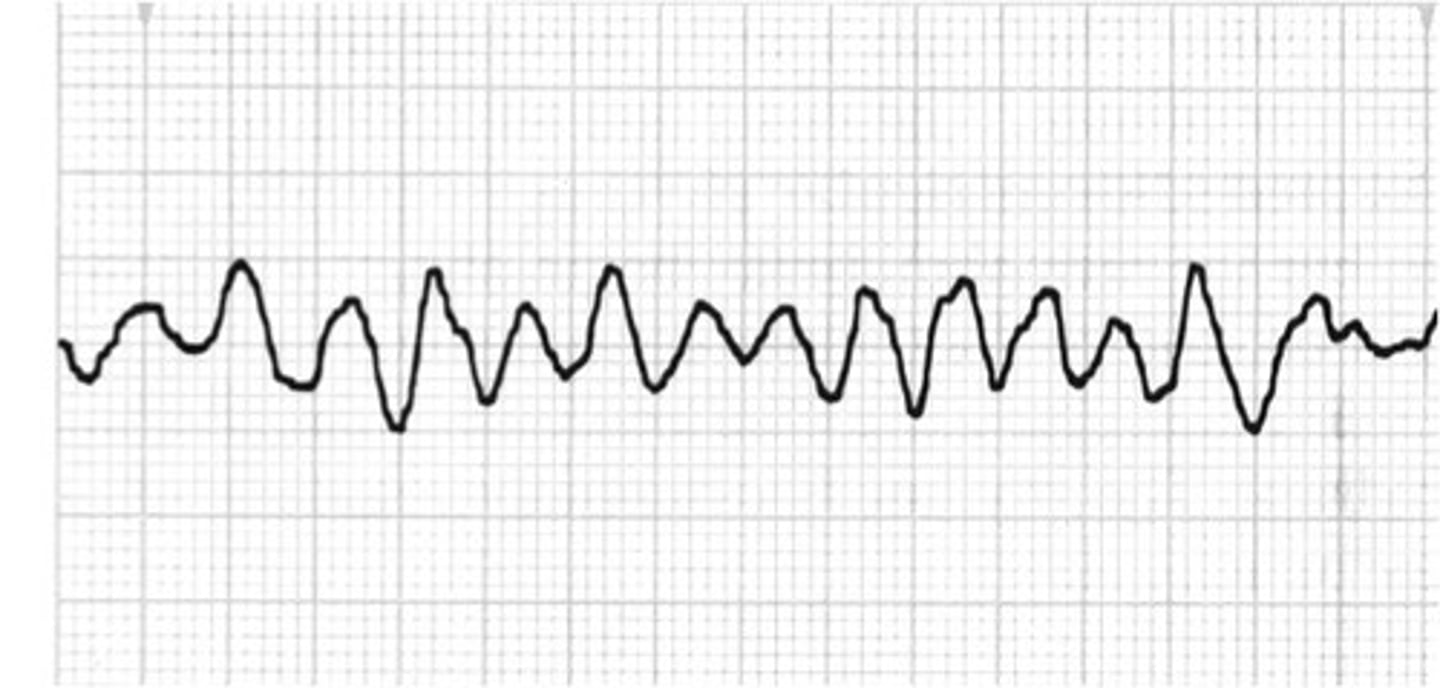
There is no pattern or regularity.
Ventricular Fibrillation
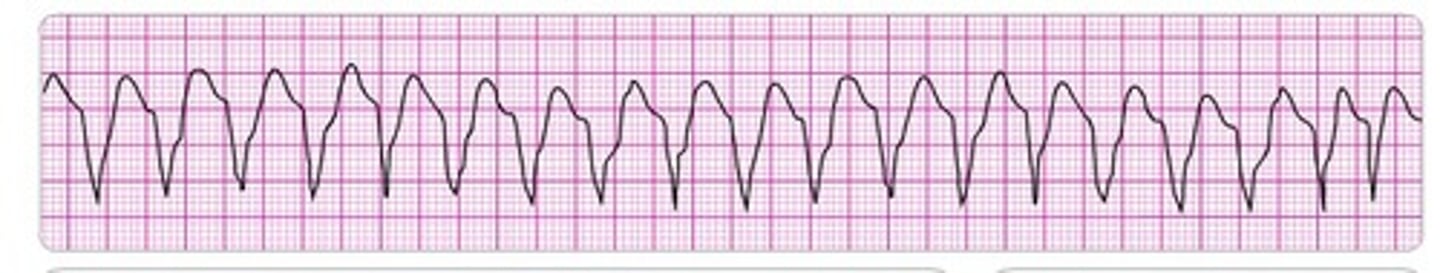
Sharp peaks or hills with a pattern.
Ventricular Tachycardia
A lack of QRS complex.
Asystole
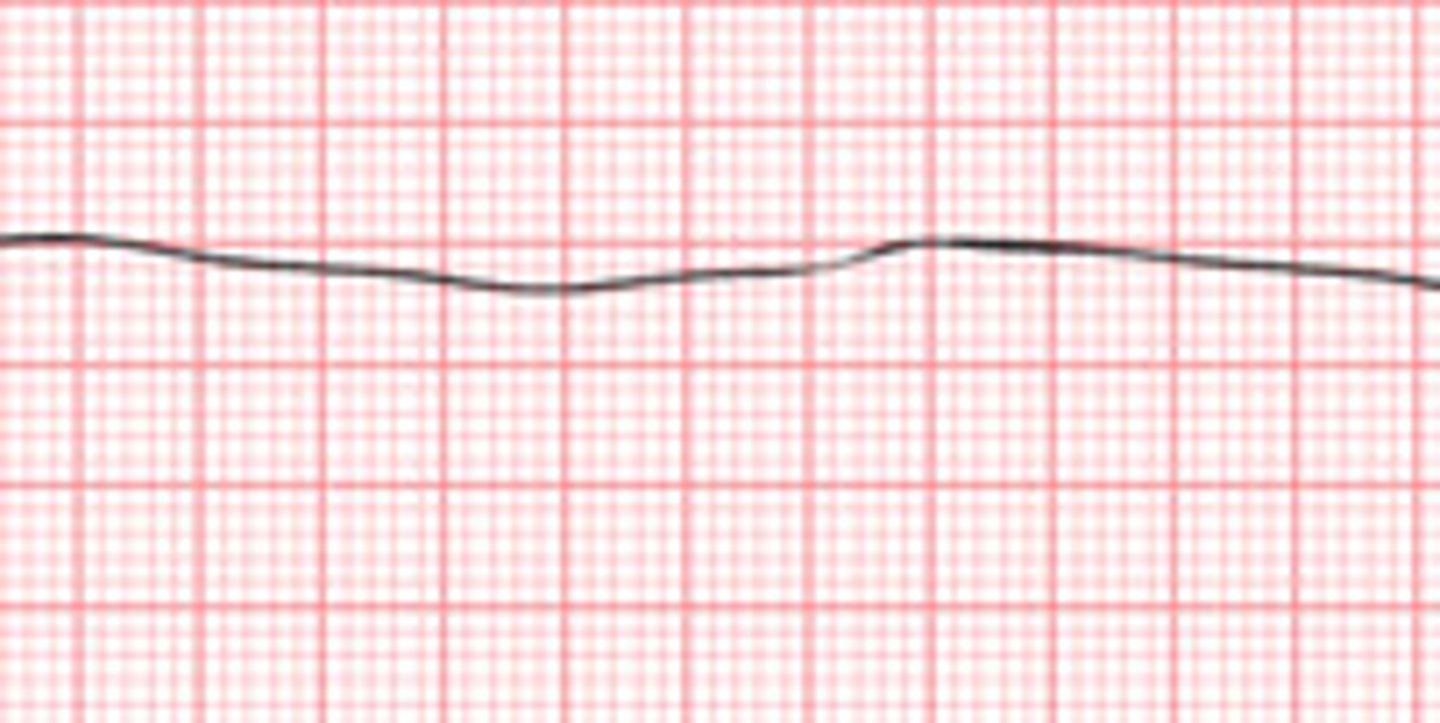
A sudden flat line.
Asystole
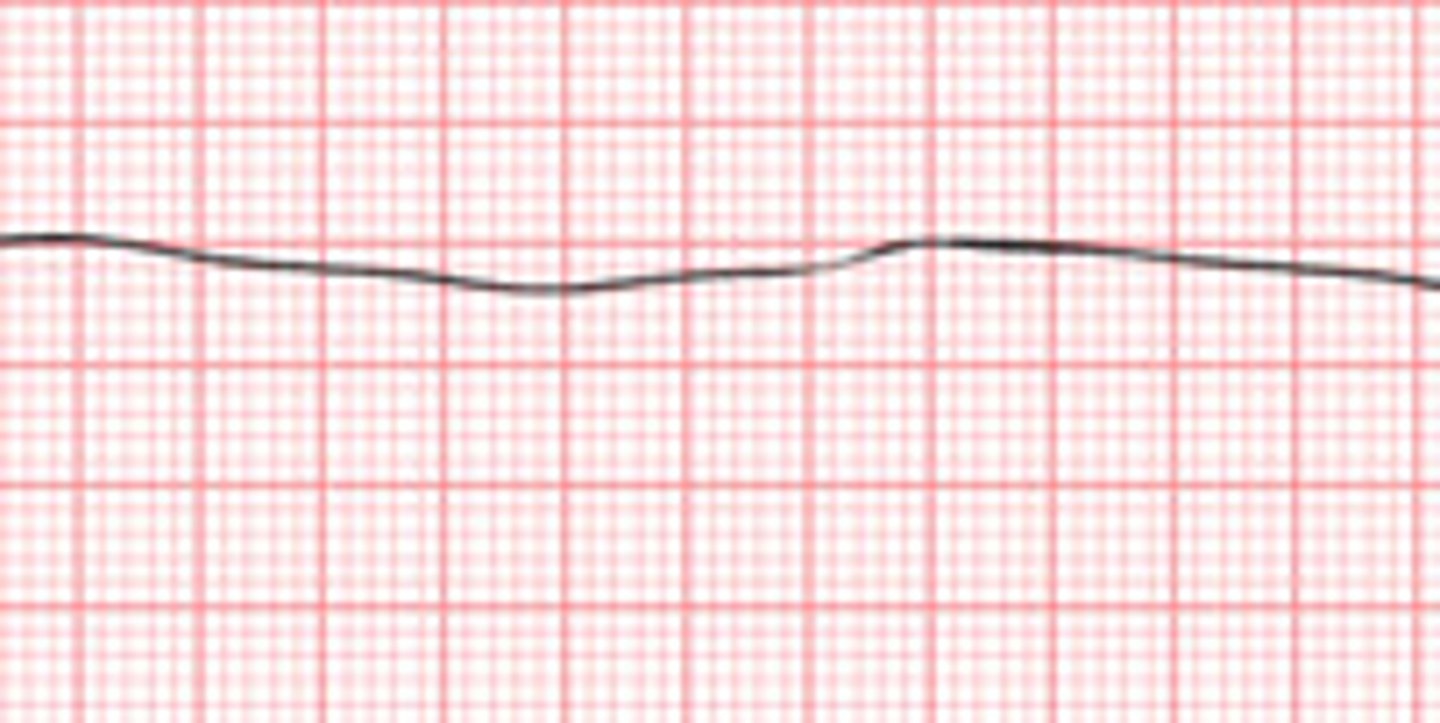
If a questions mentions QRS depolarization, then it's talking about which chamber of the heart?
Ventricular
If a questions mentions P-wave, then it's talking about which chamber of the heart?
Atrial
P-waves in the form of a saw tooth wave.
Atrial flutter
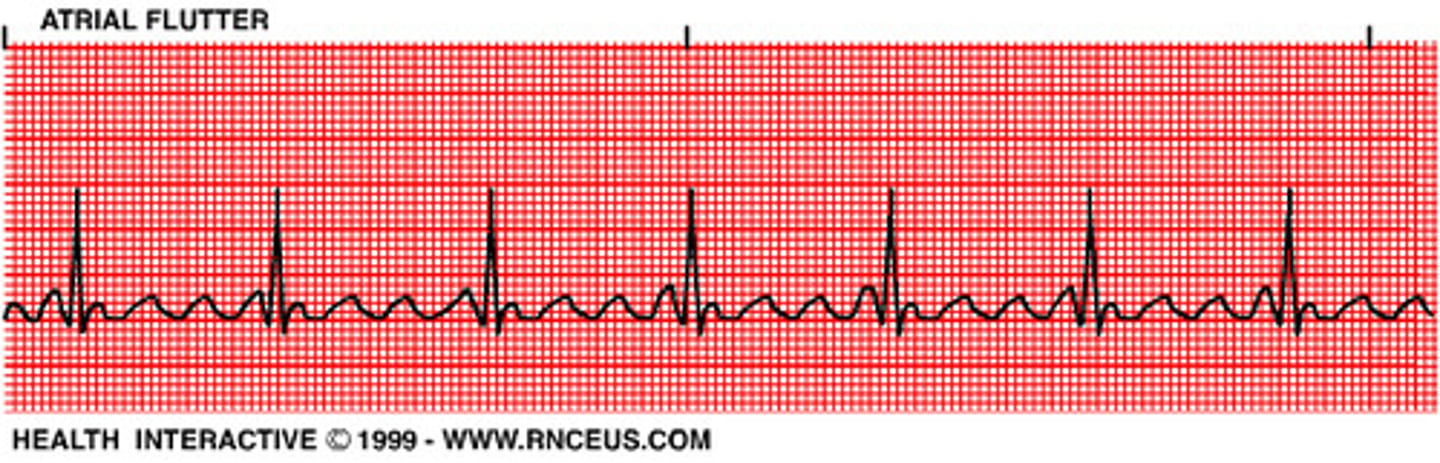
Chaotic (fib) P-wave patterns
Atrial fibrillation
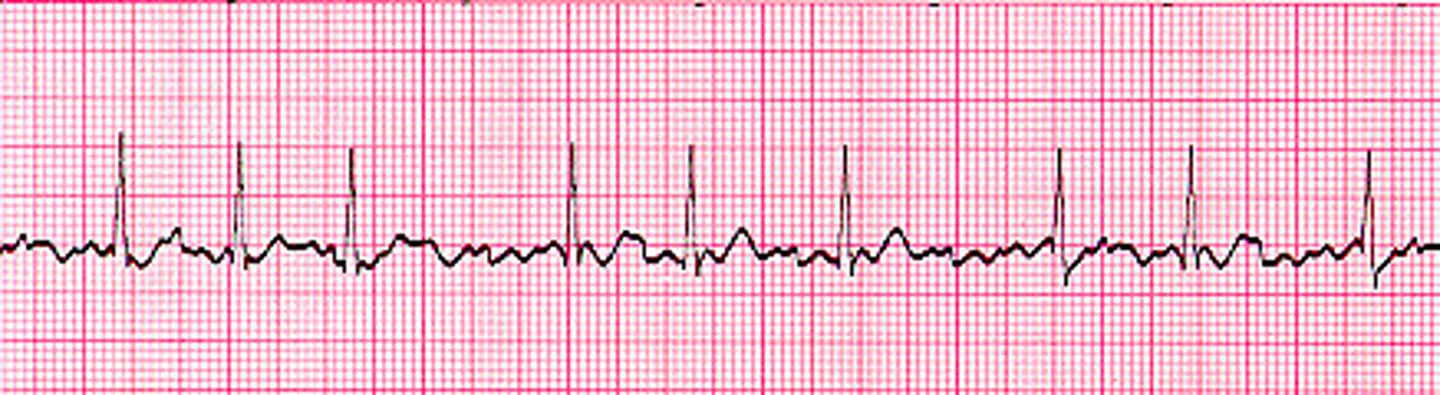
Chaotic (fib) QRS complexes.
Ventricular fibrillation
Bizarre (tach) QRS complexes.
Ventricular tachycardia
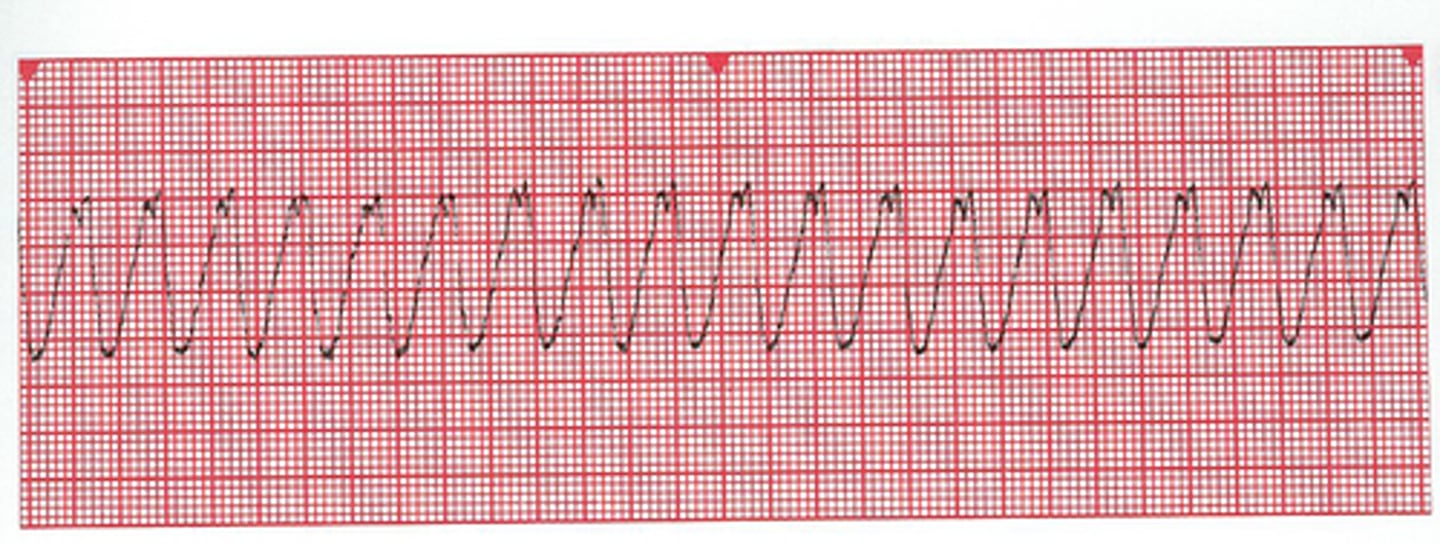
Periodic wide bizarre QRS complexes.
PVC (Premature ventricular contractions)
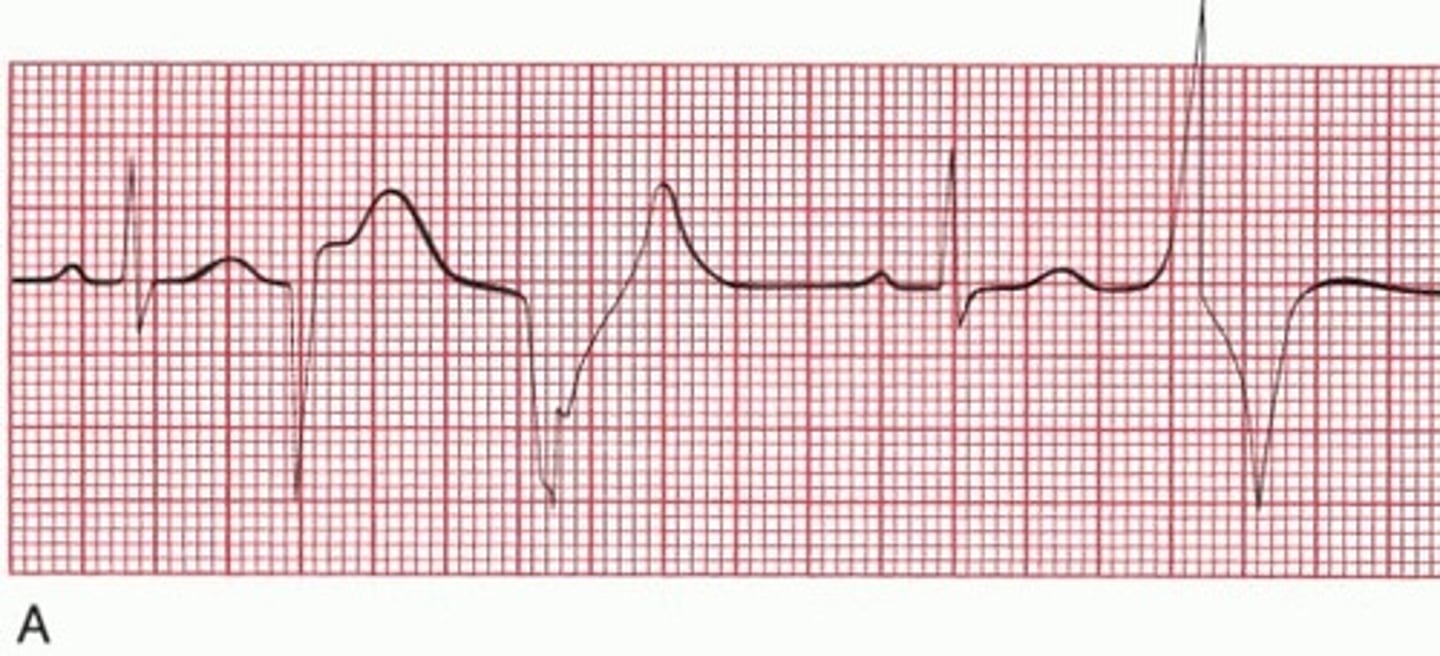
A short run of V-tachs.
PVC (Premature ventricular contractions)
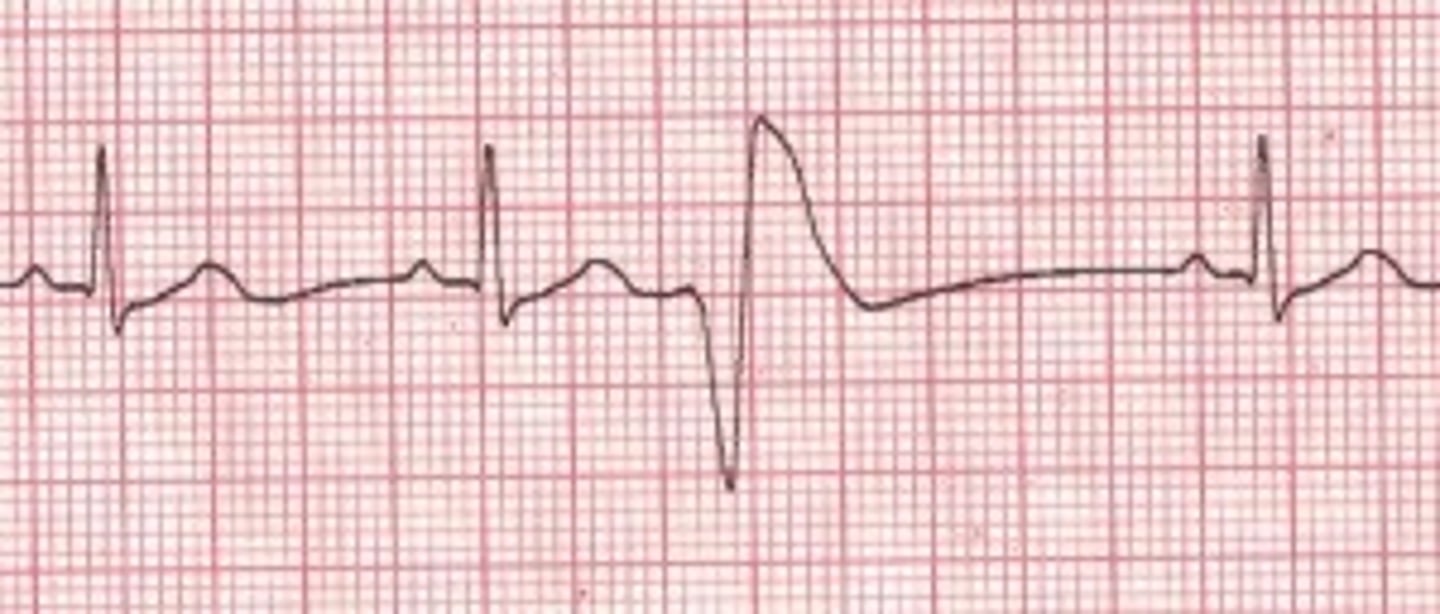
What are the 3 circumstances that can bump PVCs from LOW priority to MODERATE priority?
- If there are 6 or more PVCs in a minute
- If there are more than 6 PVCs in a row
- R on T phenomenon (PVC falls on a T-wave)
Which arrhythmia(s) is/are lethal and HIGH priority?
Asystole and V-fib = Both have low or no CO (pulse).
Which arrhythmia(s) is/are potentially lethal?
V-tach = Has a CO (pulse).
What is the treatment for PVCs?
Ventricular = Lidocaine and Amiodarone
What is the treatment for V-tach?
Ventricular = Lidocaine and Amiodarone
What is the treatment for Supraventricular arrhythmias?
Atrial = "ABCDs"
Adenosine: RAPID push <8secs w/ flushing
Beta-blockers: ends in "-olol"
C: CCBs
D: Digitalis (Digoxin), Lanoxin
What cardiac effects do Beta-blockers have?
(-) Inotropic, chronotropic, and dromotropic
What side effects do beta-blockers have?
Headache and hypotension
What is the treatment for V-fib?
Defibrillation
What is the treatment for Asystole?
Epinephrine and Atropine
Why do you not shock Asystole?
Already flat-lined.... Won't respond to defibrillation.
What is the purpose of chest tubes?
To re-establish negative pressure in the pleural space of the lung(s).
What is the pleural space?
Space between parietal (chest wall) and visceral (lung) pleura
Chest tube that removes AIR is called....
Pneumothorax
Chest tube that removes BLOOD is called....
Hemothorax
Chest tube that removes AIR & BLOOD is called....
Hemopneumothorax
A chest tube is placed in a pt for a hemothorax (blood). What would you (the RN) report to the physician?
a. Chest tube is not bubbling
b. Chest tube drains 800 mL in the first 10 hours
c. Chest tube is not draining
d. Chest tube is intermittently bubbling
Think "what is the chest tube supposed to do?"
c. Chest tube is not draining
A chest tube is placed in a pt for a pneumothorax (air). What would you (the RN) report to the physician?
a. Chest tube is not bubbling
b. Chest tube drains 800 mL in the first 10 hours
c. Chest tube is not draining
d. Chest tube is intermittently bubbling
Think "what is the chest tube supposed to do?"
a. Chest tube is not bubbling
Top location of lung is called...
Apical
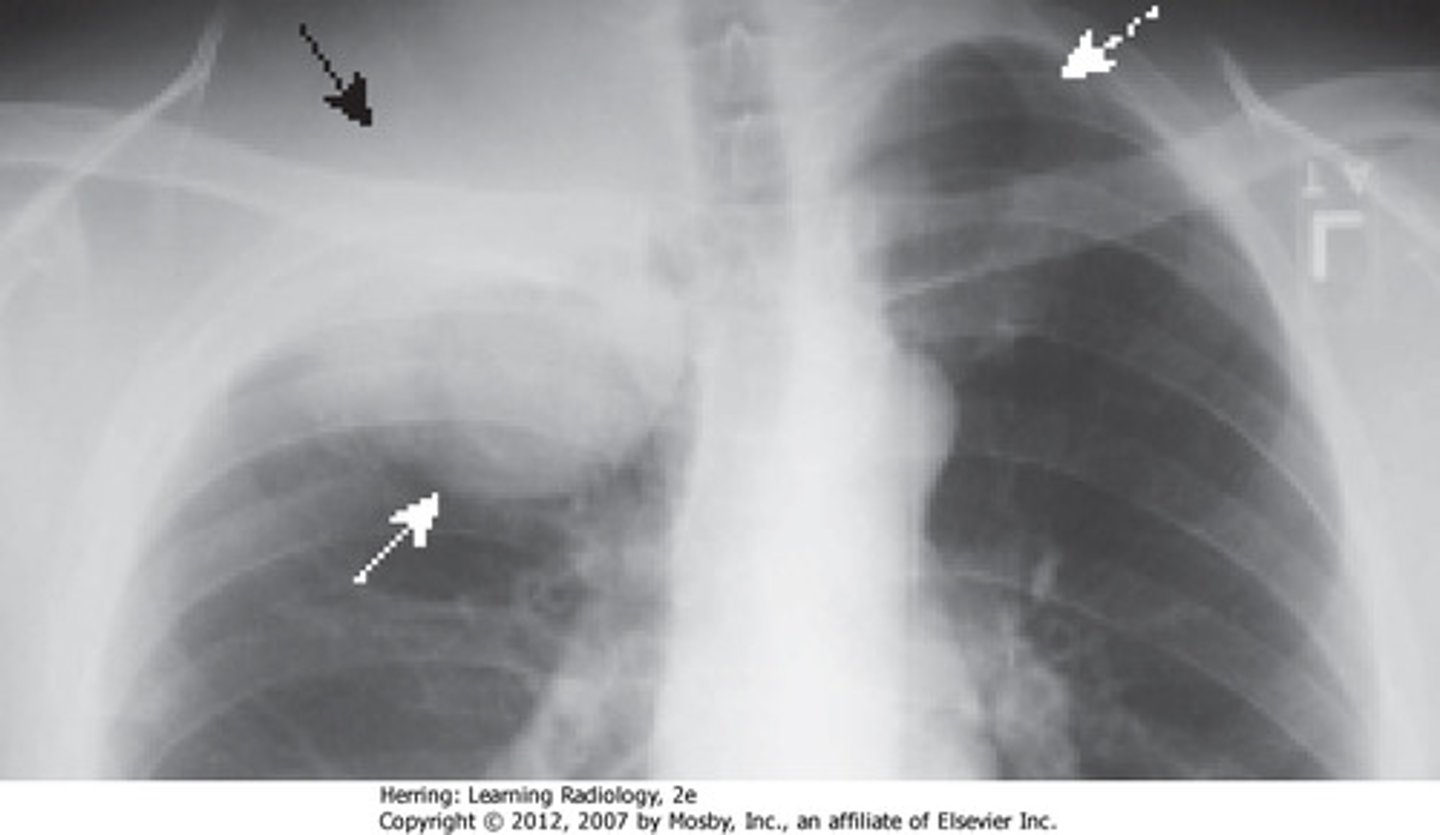
Apical chest tube removes...
Air
Base location of lung is called...
Basilar
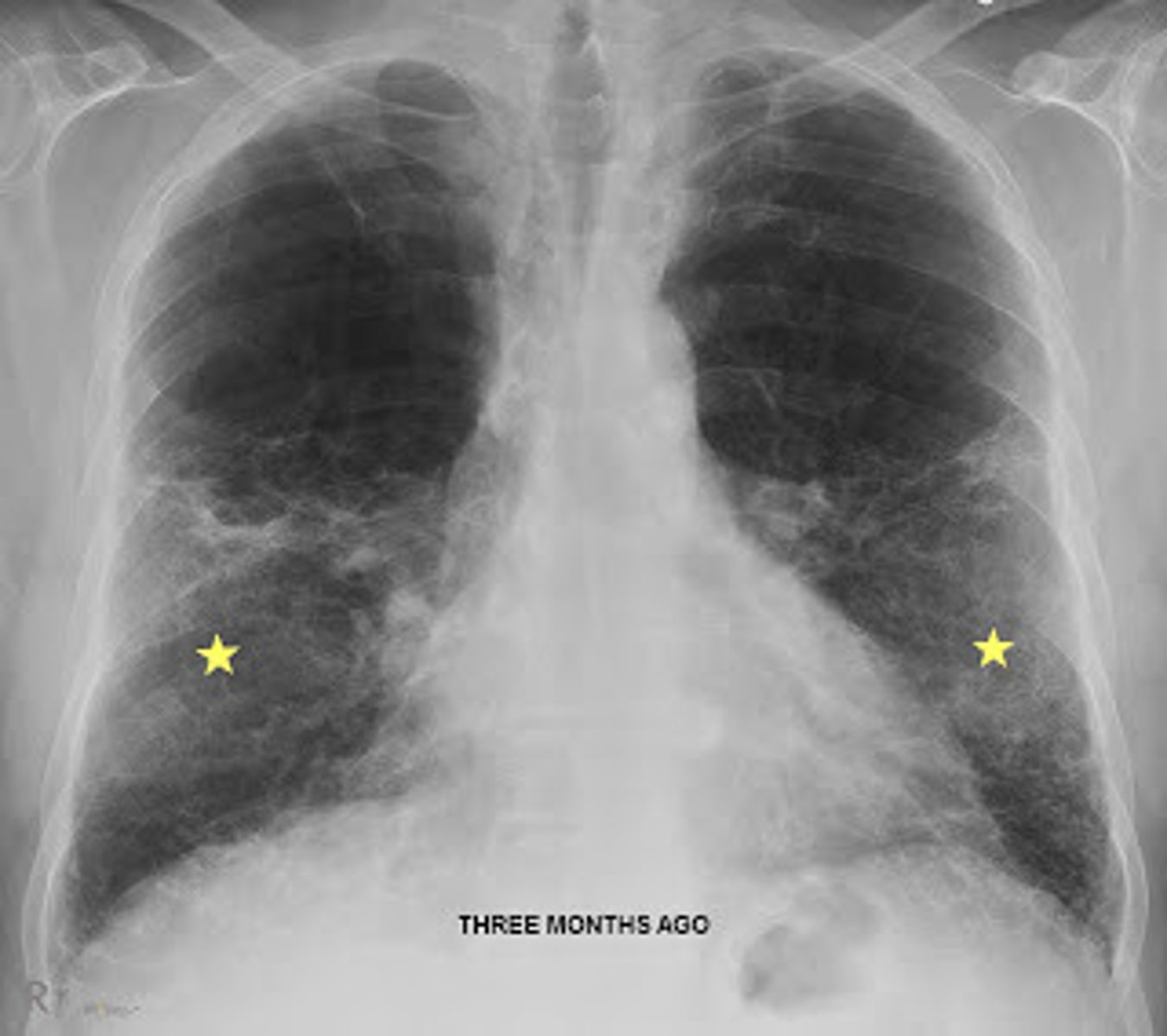
Basilar chest tube removes...
Blood or fluid
An apical chest tube is draining 300 mL the first hour
is expected or bad?
Bad.
Apical is air... so fluid shouldn't be draining.
A basilar chest tube is draining 200 mL the first hour is expected or bad?
Expected.
Basilar is blood/fluid... so draining is expected.
An apical chest tube that is not bubbling is expected or bad?
Bad.
Apical is air... so bubbling is expected.
A basilar chest tube is not bubbling is expected or bad?
Expected.
Basilar is blood/fluid... so draining is expected.
Pt presents with a unilateral hemopneumothorax. How would you care for this pt?
Place both an apical chest tube for
the pneumothorax and a basilar for the hemothorax ON the side of the surgery.
Where would you place a chest tube for a post-op right pneumonectomy?
Trick question. The right lung was REMOVED, so a chest tube is not needed.
Does a lobectomy require a chest tube? Why?
Yes. It's a removal of a LOBE, not the whole lung.
What are some types of closed-chest drainage devices?
Jackson-Pratt, Emission, pneumovac, hemovac, etc.
What does a Jackson-Pratt drainage look like?
What does a pneumovac drainage look like?
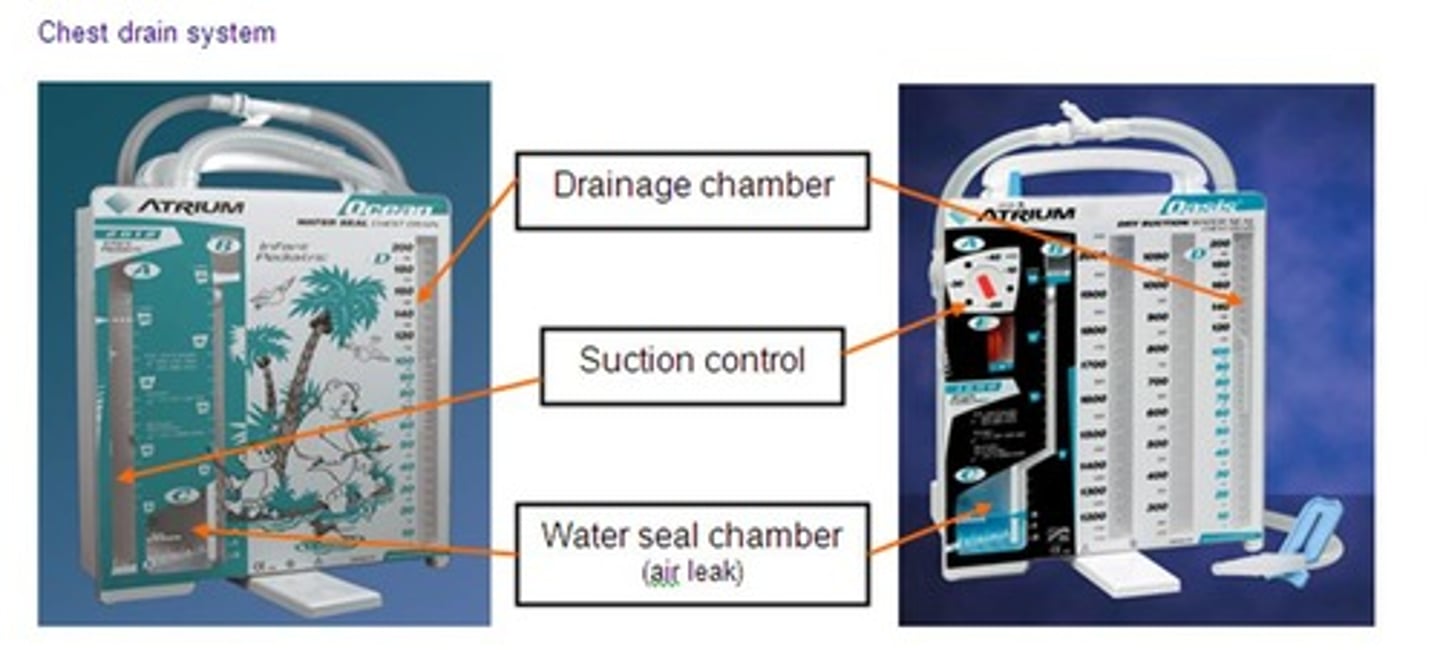
What does a hemovac drainage look like?

What happens if a drainage device gets knocked over?
Ask the patient to take a deep breath and set the device back. It's not a medical emergency, so there's no need to call the physician.
What should you do if the water seal of a chest tube breaks?
Clamp the tube.
Cut the tube away.
Submerge the end of the tube under sterile water.
Unclamp the tube.
All this must be done in 15 seconds or less.
The water seal chamber of the chest tube in a pt with a pneumothorax/hemothorax breaks. What is the first course of action for the nurse?
Clamp the tube.
The water seal chamber of the chest tube in a pt with a pneumothorax/hemothorax breaks. What is the priority (best) action of the nurse?
Submerge the end of the tube under sterile water. Re-establishes the water seal.
You notice on the monitor that a pt has v-fib. Pt is unresponsive and there is no pulse. What is the first step in the management of this pt?
a. Place a backboard under pt's back while pt is supine
b. Start chest compression
a. Place a backboard under pt's back while pt is supine
You notice on the monitor that a pt has v-fib. Pt is unresponsive and there is no pulse. What is the best step in the management of this pt?
a. Place a backboard under pt's back while pt is supine
b. Start chest compression
b. Start chest compression
If a chest tube gets pulled out, what is the first step you should do?
Take a gloved hand and cover the opening.
If a chest tube gets pulled out, what is the best step you should do?
Take a sterile Vaseline gauze and tape 3 sides.
What two questions should you ask when a chest tube is bubbling?
Ask (1) where is it bubbling, and (2) when is it bubbling.
If the water seal chamber is intermittently bubbling, is it good or bad?
Good. Document it.
If the water seal chamber is continuously bubbling, is it good or bad?
Bad. Find the break/leak and tape it.
If the suction control chamber is intermittently bubbling, is it good or bad?
Bad. Suction pressure is too low. Increase it at the wall until it's continuous.
If the suction control chamber is continuously bubbling, is it good or bad?
Good. Document it.
A straight catheter is to a Foley catheter, as a thoracentesis is to a chest tube. What is the comparison?
A straight catheter goes in and out.
A Foley goes in, is secured, and continually drains into a bad.
A thoracentesis goes in and out.
A chest tube goes in, is secured, and continually drains.
What are the rules for clamping chest tubes?
- Do not clamp a chest tube for longer than 15 seconds without a physician's order.
- Use a rubber tooth to double clamp (won't puncture tubing)
What is the MAIN word to think about when it comes to congenital heart defects?
TRouBLe
What does TRouBLe stand for?
- Congenital heart defect that shunts blood from (R) to (L)
- Blue (Cyanotic)
- All TRouBLe start with "T."
What are the 6 TRouBLe congenital heart defects?
It doesn't matter. Just remember it all starts with T except for Left ventricular hypoplastic syndrome.
Tetralogy of Fallot
Truncus Arteriosus
Transportation of the great vessels
Tricuspid atresia
Totally anomalous of pulmonary vasculature (TAPV)
Left ventricular hypoplastic syndrome
If a pediatric patient has a "TRouBLe" congenital heart defect, what does this mean?
- Needs surgery now/soon to live
- Has slowed/delayed growth and development (failure to thrive)
- Has a shortened life expectancy
- Parents will experience a lot of grief, financial and emotional stress
- Pt is likely to be discharged home on a cardiac monitor
- After birth, pt will be in the hospital for weeks
- Pediatrician or pediatric nurse will likely refer pt to a pediatric cardiologist
Whether TRouBLe defect or not, ALL children with a congenital heart defect have....
A murmur. An echocardiogram will need to be done to find the cause.
What word should you associate with Tetralogy of Fallot?
PROVe.
What does PROVe stand for?
The 4 defects of Tetralogy of Fallot.
Pulmonary arterial stenosis
Right ventricular hypertrophy
Overriding aorta
Ventricular septal defect
e just to make it a word.
What are the 4 transmission-based precautions?
Standard/Universal
Contact
Droplet
Airborne
What diseases require contact precaution?
Herpes
Staph
RSV (Droplets fall then is touched and transferred)
Anything enteric (GI or fecal/oral)
Hepatitis A
C. difficile
E. coli
Cholera
Dysentery
What PPE is required for contact precautions?
- Private room (preferred)
- Can be in same room of others w/ same culture, NOT symptoms
- Hand-washing, gown, gloves
- Disposable supplies (plates/utensils)
- Dedicated equipment stays in room (stethoscope, BP cuff, toys)
What diseases require droplet precaution?
Bugs that travel on large particles through coughing or sneezing in less than 3 feet.
- Meningitis
- Haemophilus influenza type b (Hib) = Epiglottitis
What PPE is required for droplet precautions?
- Private room (preferred)
- Can be in same room of others w/ same culture, NOT symptoms
- Hand-washing, mask, goggles, gloves
- Disposable supplies (plates/utensils)
- Dedicated equipment stays in room (stethoscope, BP cuff, toys)
What diseases require airborne precaution?
"MTV on AIR."
- MMR
- TB
- Varicella (chickenpox)
What PPE is required for airborne precautions?
- Private room (preferred)
- Can be in same room of others w/ same culture, NOT symptoms
- Hand-washing, goggles, gloves
- Wear mask when leaving the room
- Keep the door CLOSED
- Disposable supplies (plates/utensils)
- Dedicated equipment stays in room (stethoscope, BP cuff, toys)
In what order do you put on PPE?
Reverse alphabetical order, but mask is 2nd
In what order do you take off PPE?
Alphabetical order
How do you calculate IV drip rates?
(Volume x drop factor) / Time in minutes
How many drops are in a Micro/Mini drip?
60 drops per mL
How many drops are in a Macro drip?
10 drops per mL
How many lbs are in 1 kg?
2.2 lbs