1 Introduction to imaging (copy)
1/109
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
110 Terms
List the imaging modalities that use ionising radiation
Radiography, fluoroscopy, computed tomography, scintigraphy
How does ionising radiation damage cells?
It causes ionisation in atoms (electrons ejected from the atom), creating free radical atoms that lack an electron
Free radical atoms pull electrons off surrounding atoms, causing a free radical cascade that causes breaks in chemical bonds
List the three possible interactions of an x-ray with a patient
Pass through the patient to the detector
Be absorbed in the patient
Be scattered from the patient
Radiopaque
More x-rays are absorbed - whiter appearance
Radiolucent
More x-rays pass through - blacker appearance
What are the five radiographic opacities?
Gas
Fat
Soft tissue (and fluid)
Mineral
Metal
Why are gas and metal opacity contrast agents used?
They help outline organs by contrasting with surrounding structures, making it look black or white
Why are two orthogonal views required for radiography?
To create a 3D image from 2D radiographs
Try to take one from the side and one from the top
How is an image formed in radiography?
X-ray beams pass through the patient to a digital detector, recording the image
How does fluoroscopy create images?
It produces a continuous x-ray beam to create an x-ray movie
Opacity is reversed compared to radiographs
How is an ultrasound image formed?
Sound is sent into tissue and reflected back, with amplitude indicating brightness
What determines how dark/ bright the ultrasound image is?
Denser tissue = larger acoustic impedance difference = brighter dot
Acoustic impedance
The resistance the sound wave encounters through a tissue
What is computed tomography (CT)?
A method where an x-ray tube rotates around the patient and the patient move through the machine to create slices of tissue
Can be viewed in different windows
How does magnetic resonance imaging (MRI) work?
1. Radiofrequency pulse is applied → hydrogen atoms no longer spin aligned to the magnetic field
2. Radiofrequency pulse is turned off → alignment gradually returns to be aligned with the magnetic field
3. As the H+ atoms realign, they release energy, which is collected as a signal which forms the image - the time the realignment takes is different depending on which tissue the atom is in (slower in water c.f. fat)
What is scintigraphy?
A method involving injection of a radioactive substance to assess physiological processes
What is the most common imaging modality used in veterinary practice?
Radiography
What is the primary use of fluoroscopy in veterinary practice?
To evaluate collapsing trachea in small dogs
Also for evaluation of oesophageal dysfunction, orthopaedic surgery and stent placement
What is AFAST in veterinary ultrasound?
A technique for assessing abdominal fluid
What is TFAST in veterinary ultrasound?
A technique for assessing lungs, pericardial effusion, and pleural effusion
What is the primary use of ultrasound in veterinary practice?
To answer specific clinical questions, such as locating a mass
What is computed topography used for?
It is used for detailed imaging of various body structures (poor for the brain)
What imaging modality is the choice for the brain and spinal cord?
MRI
What are the advantages of low field MRI machines?
They are cheaper to buy and maintain but have poor image quality
What are the disadvantages of high field MRI machines?
They are very expensive but provide excellent image quality
What is scintigraphy used to assess?
It assesses function (kidney function, thyroid function, cardiac function)
What are the advantages of radiography?
All practices have an x-ray machine
What are the advantages of fluoroscopy?
Can see in real time during procedures
What are the advantages of ultrasound?
Movement can be seen
Function of organs can be evaluated as well as appearance
No ionising radiation
What are the advantages of CT?
Can be made in any plane
Can see different windows
What are the advantages of MRI?
Can be made in any plane
Essential for the spine
What are the advantages of scintigraphy?
Can examine function
What are the disadvantages of radiography?
Radiation risk
Only a 2D view
What are the disadvantages of fluoroscopy?
Biggest risk for radiation exposure
What are the disadvantages of ultrasound?
Requires training and practice
Can only go 10cm deep
What are the disadvantages of CT?
Can only do what can fit in it
Mostly specialists
What are the disadvantages of MRI?
Safety - any ferrous metallic object can become a projectile
ONLY specialists
What are the disadvantages of scintigraphy?
Uses gamma rays
What is the main advantage of cross-sectional imaging?
It simplifies complicated anatomy by eliminating superimposition of structures
What are the main advantages of MRI over CT?
Much better image of soft tissue structures
Best for brain and spine
What are the main advantages of CT over MRI?
Cheaper, quick
Good for all areas except the brain
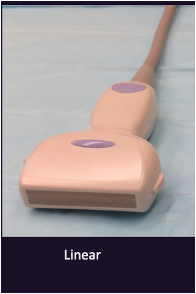
What is a linear transducer used for?
Scanning things close to the surface (up to 4cm deep) e.g. horse tendons
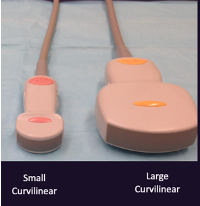
What is a curvilinear transducer used for?
Scanning the abdomen
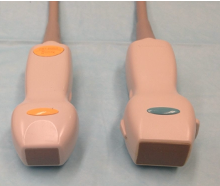
What is a phased array transducer used for?
Scanning the heart (echocardiography)
What are the key factors for taking good radiographs?
Sedation!!! (most important factor)
Proper positioning aids
List the four key factors for good radiology interpretation
Good quality radiographs
2 large monitors
Knowledge of normal anatomy
Systematic approach.
What does a left lateral view mean in radiography?
The left side of the patient is down
What is the dorsoventral (DV) view in radiography?
The patient is lying on their belly, and the X-ray hits the dorsal side first
What is the ventrodorsal (VD) view in radiography?
The patient is lying on their back, and the X-ray hits the ventral side first
What is the caudocranial view in radiography?
The X-ray hits the caudal surface and then the cranial surface of the limb
What is the craniocaudal view in radiography?
The X-ray hits the cranial surface and then the caudal surface of the limb
What should be done to prepare a patient for an abdominal radiograph?
The bladder should be emptied and the patient should be fasted for 12 hours
Why is a plan needed for the order of radiographs?
It saves time
When to take an x-ray for thorax?
Just before peak inspiration
When to take an x-ray for the abdomen?
Just after expiration as there is a pause, so there will be no movement blur
What is the effect of FFD (the distance between the x-ray machine and detector plate) on radiographs?
It affects exposure (greater if closer) and image detail (reduced if closer)
How many views should be taken for abdomen and thorax?
Three views: left lateral, right lateral, and ventrodorsal
What positioning aids are commonly used in radiography?
Foam, cotton wool, sandbags, tape
What do the left/right markers indicate on an abdomen/ thorax lateral radiograph?
Indicates what side is down
For example - R marker indicated right lateral radiograph (right side down)
What do the left/right markers indicate on an abdomen/ thorax VD radiograph?
Indicates what side of the patient
For example - L marker indicates that where the marker is is the left side of the patient
What do the left/right markers indicate on a limb radiograph?
Indicates whether it is the right or left limb
How should a limb marker be placed on a radiograph?
It must go on the lateral aspect of the limb
How are lateral radiographs viewed?
Cranial left and caudal right
How are VD/ DV radiographs viewed?
Left side of the patient on the right, right side of the patient on the left
How are CC radiographs viewed?
Lateral aspect of the limb (where the marker is) on the right side of the screen
List the 3 pitfalls in interpretation that are avoided by using the systematic approach
Satisfaction of search (stop after finding one lesion)
Distraction by obvious abnormalities (miss others)
Tunnel vision (preconceived idea of what will be found and stopping early)
What are roentgen signs?
Adjectives to describe abnormalities
List the roentgen signs
Size
Shape
Margins
Opacity
Number
Location
How are roentgen signs used in the systematic approach?
For each structure, ask if it is normal or abnormal
If abnormal, use roentgen signs for description
What is summation on radiographs?
When superimposed opacities add together, making overlapping structures more opaque
The structures are not in contact so their separate margins are seen
What is effacement on radiographs?
When 2 structures of the same opacity are in contact, their individual margins at the point of contact cannot be distinguished
What are the rules of effacement?
1. Same opacity
2. In contact
What is the purpose of contrast studies?
To visualise organs better by instilling a contrast agent
What are positive contrast agents?
Metal opacity - iohexol and barium (GI only) liquid
What are negative contrast agents?
Gas opacity - room air or carbon dioxide
What is the impact of collimating the beam in radiography?
It reduces the volume of tissue exposed and minimises scatter
List the 4 indications for contrast studies
Location
Rupture
Filling defect
Function
List the indication for a location contrast study and give an example
Locating an organ
Colon - pneumocolonogram
List the indication for a rupture contrast study and give an example
Is contrast leaking out? (extravasation)
Ureter - excretory urogram
List the indication for a filling defect contrast study and give an example
Is there something displacing the contrast?
Calculus in the urethra - urethrogram
List the indication for a function contrast study and give an example
Is the organ functioning normally?
Oesophagus function - oesophagram
Indications for a positive contrast cystogram
Bladder rupture
Bladder location if ultrasound not available
What contrast agent is used for a positive contrast cystogram?
Iohexol
How is iohexol instilled for a positive contrast cystogram?
Through a urinary catheter (Foley) with the balloon just inside the bladder
Indications for a positive contrast urethrogram
Filling defect causing an obstruction (calculus)
Urethra rupture
What contrast agent is used for a positive contrast urethrogram?
Iohexol
How is iohexol instilled for a positive contrast urethrogram?
Through a urinary catheter (Foley) with the balloon just inside the penis or vulva
Indications for an excretory urogram
Locate ectopic ureters
Rupture
Filling defects
What contrast agent is used for an excretory urogram?
Iohexol
How is iohexol instilled for an excretory urogram?
By intravenous injection
Indications for an upper gastrointestinal barium study
Function - the transit time of the barium
Filling defect - foreign body
What contrast agent is used for an upper gastrointestinal barium study?
Barium
How is barium instilled for an upper gastrointestinal study?
Through a stomach tube or diluted via a nasogastric tube
Indications for a pneumogastrogram
Filling defects - gastric foreign body
Location
What contrast agent is used for a pneumogastrogram?
Air
How is air instilled for a pneumogastrogram?
Stomach tube or nasogastric tube
Indications for a pneumocolonogram
Locate the colon
What contrast agent is used for a pneumocolonogram?
Air
How is air instilled for a pneumocolonogram?
Via a tube in the rectum
Indications for an oesophagram
Function of the oesophagus
Filling defect - oesophageal foreign body