20. Dairy Calf Nutrition
1/54
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
55 Terms
1. naive immune system which is suppressed at birth
2. poor thermoregulation due to lack of fat and mm. tone...inability to shiver effectively
3. risk of hypoglycemia
what are the challenges associated with newborn calves
1. provide adequate colostrum
2. maintain clean environment
3. minimize heat loss
how can we prevent disease in newborn calves
1. dry calf
2. dip navel in 7% iodine
3. seperate from dam
4. hand feed colostrum
what is involved in the immediate care of a newborn calf
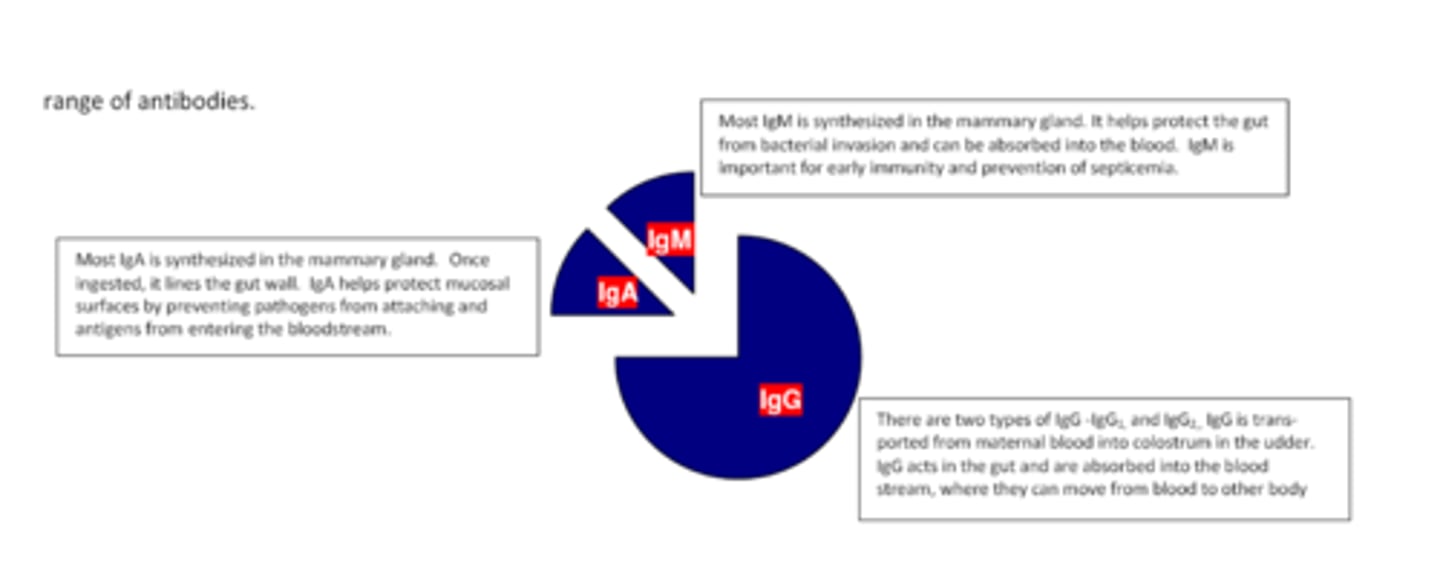
1. first milk produced after parturition
2. only 1st milking is high quality...the rest are considered "transitional"
3. high DM content
4. high IgG antibodies...largest Ab in milk
5. IgA produced in mammary glands and derived from blood
6. lactoferrin from mammary epithelial cells to protect against bacteria
what are the characteristics of colostrum
1. provide passive immunity
2. essential for disease prevention
why does colostrum matter
immediately and decreases linearly
intestinal absorption of antibodies declines...
decreased by 30%
what is gut absorption like 6hrs after birth
decreased by 50%
what is gut absorption like 8hrs after birth
24hrs after birth
when is "gut closure" considered complete marking the endpoint of when antibodies can be absorbed by the intestine
feed colostrum early
how can we achieve max absorption of antibodies
feed full amount (3-4qt) within 2-4hrs via voluntary consumption or feeding tube
what is the ideal colostrum feeding protocol

feed remainder by no later than 12hrs
if half to two-thirds of colostrum is consumed within 2hrs, what do we do with the rest of it

3 quarts
how much colostrum is needed for a 50-100lb calf
2 quarts
how much colostrum is needed for a <50lb calf
4 quarts
how much colostrum is needed for a >100lb calf
tube-fed/esophageal feeder
how should reluctant calves be fed colostrum
colostrometer: form of hydrometer which measures specific gravity and converts it to IgG concentration
how can we assess colostrum quality

>50-60 g/L (50mg/mL)
what IgG level is considered to be high quality

20-100mg/mL
what is the range of IgG in milk

measure total plasma protein using refractometer
how can we assess passive transfer

>5.5 g/dL total plasma protein
what value indicates adequate colostrum meal/passive transfer
1. affect ~40% of calves
2. increased disease risk
3. increased mortality
what are the characteristics of failure of passive transfer
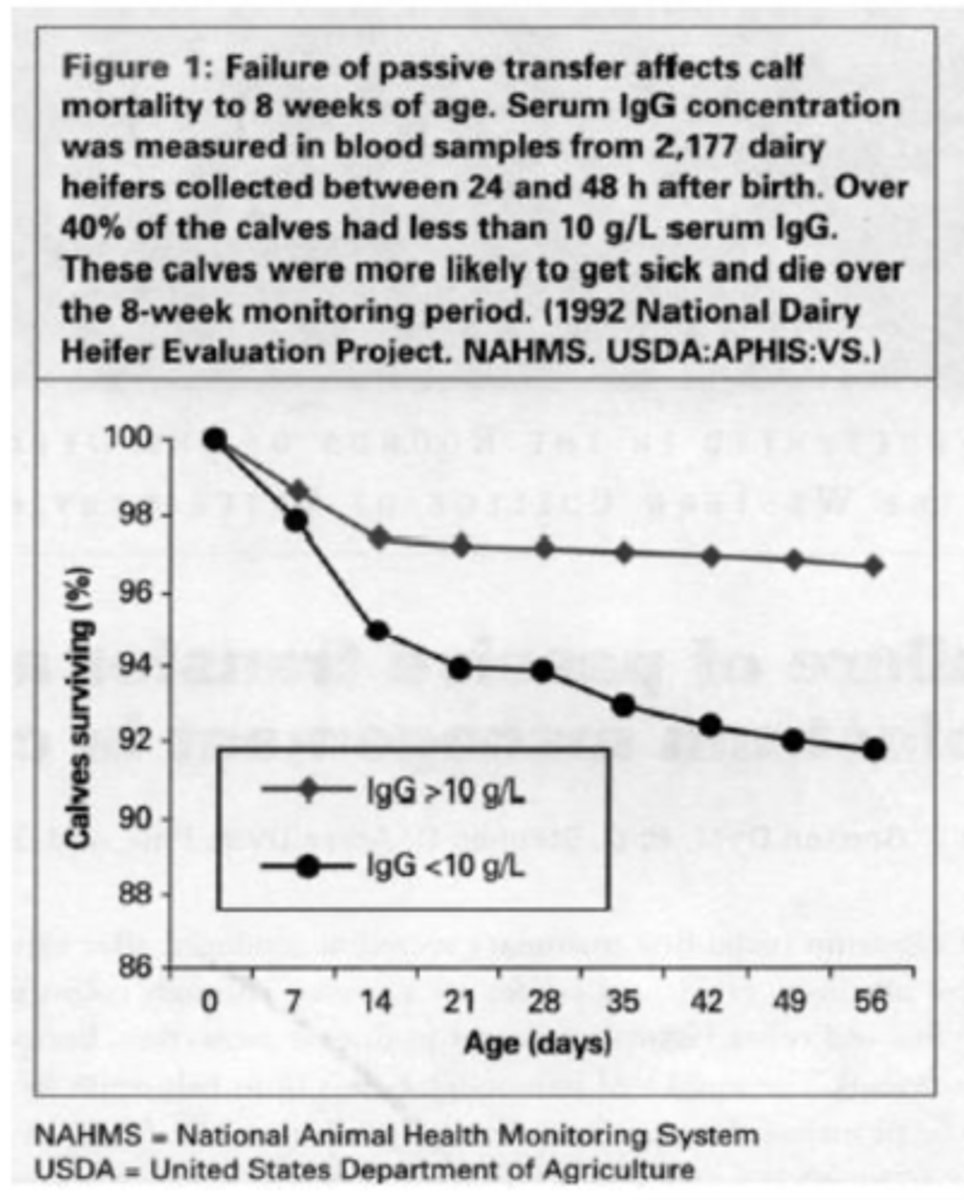
>8 g/L (0.8 g/dL) IgG
what is the critical serum IgG level to avoid failure of passive transfer
1. heifer colostrum
2. colostrum leakage pre-calving
3. delayed feeding
4. low IgG concentration
risk factors for poor immunity
adequate production of colostrum in both volume and quality (antibody content) ...dependent on adequate nutrition
what does adequate immunity depend on
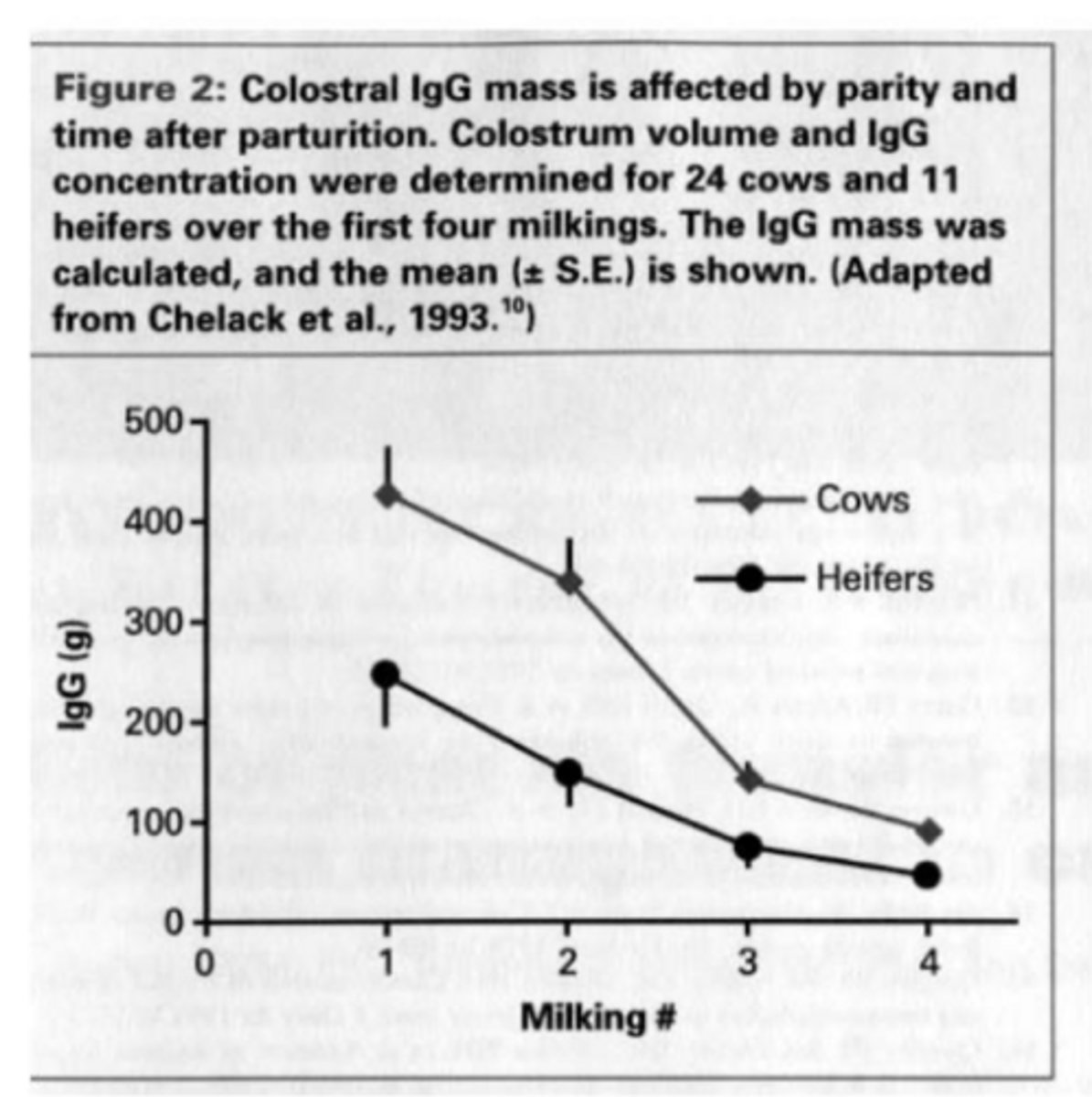
produce less volume with lower IgG concentration
how might you describe colostrum production of a heifer vs. that of a cow
high quality
high volume colostrum does NOT always equal ___ ___
lower IgG levels
how might you describe IgG levels in heifer colostrum vs. cow
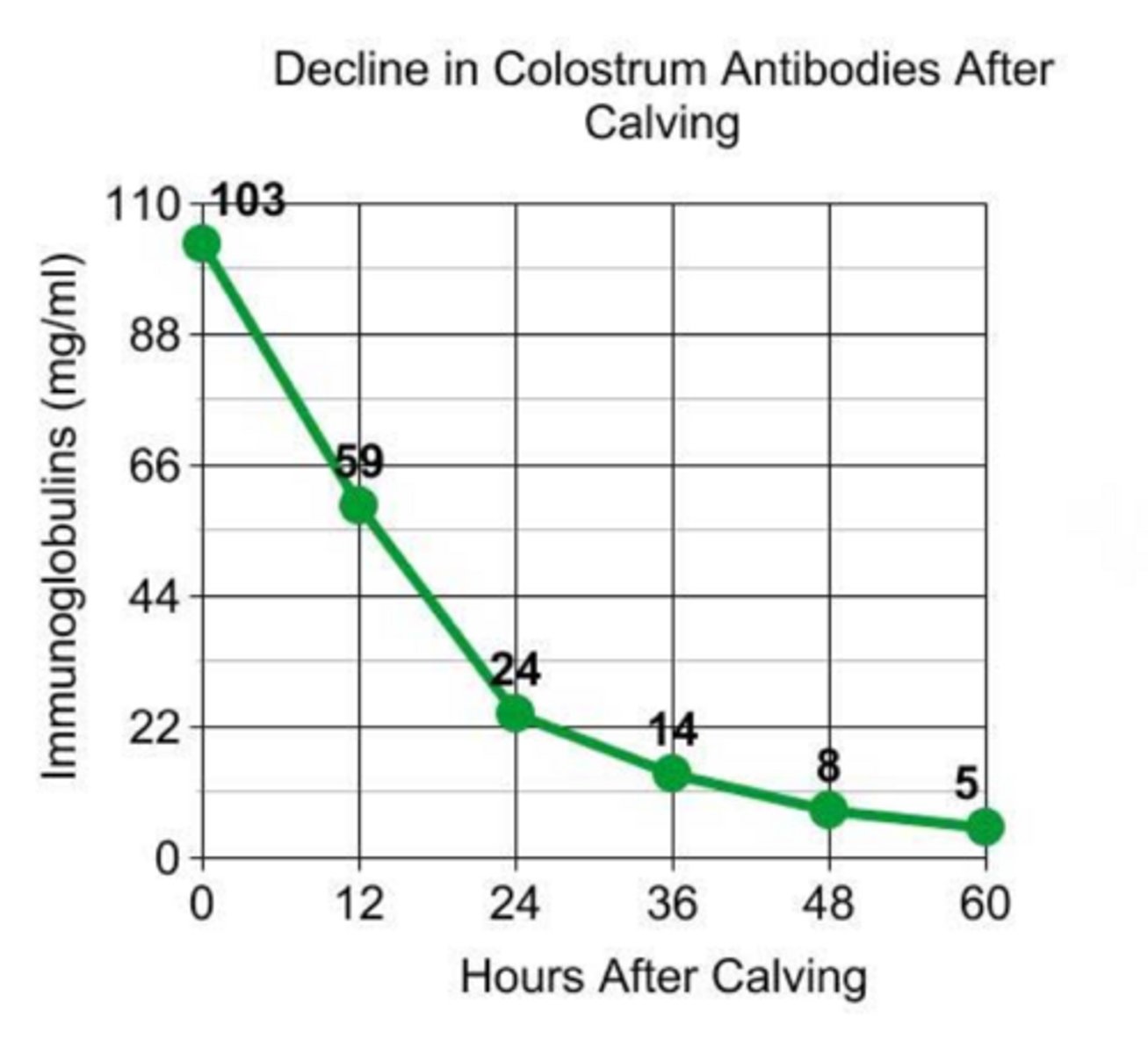
lower IgG levels
how might you describe IgG levels of high producing cows compared to those producing less
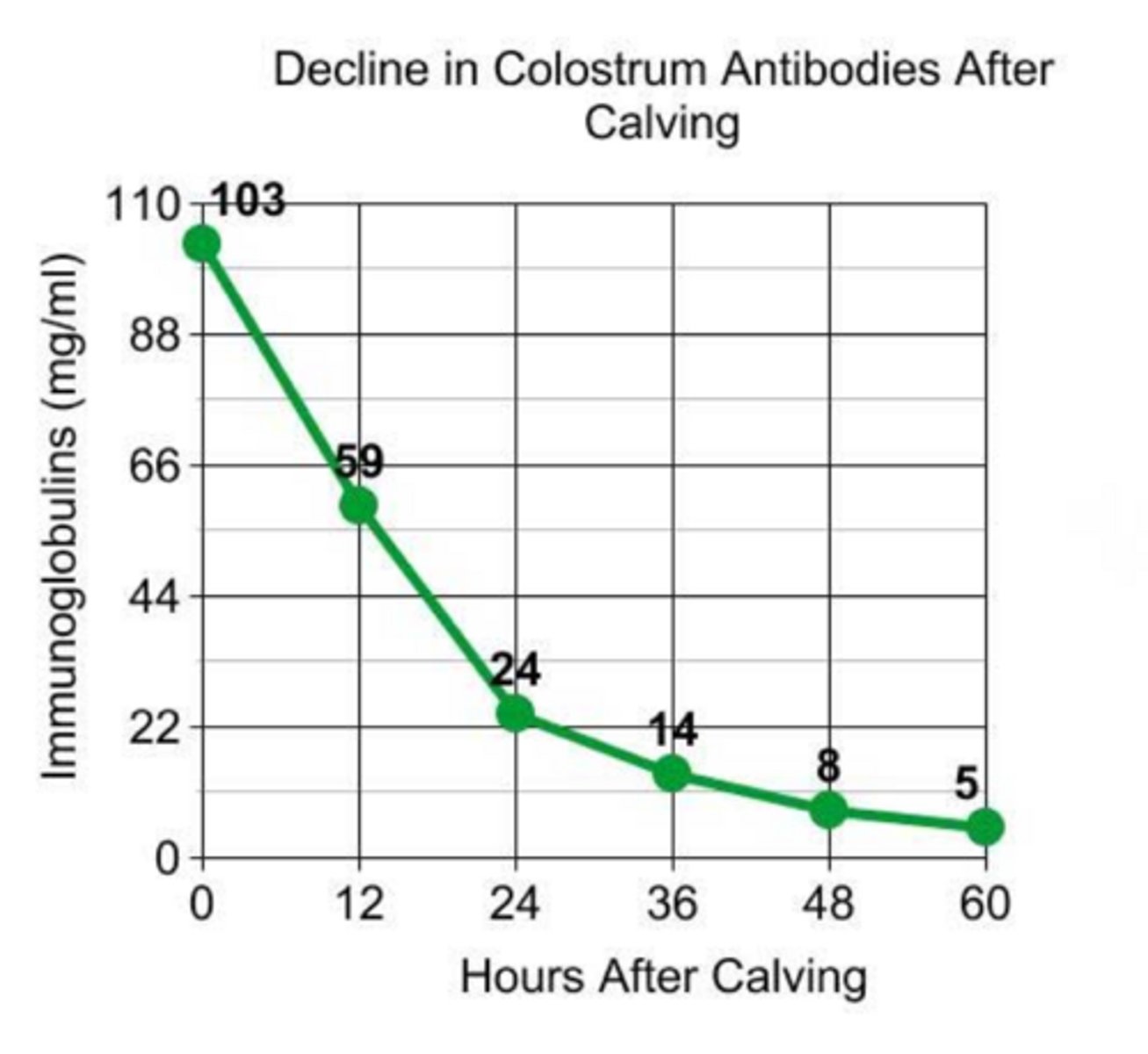
1. frozen colostrum from cow in the same herd that is BLV and Johne's negative
2. colostrum replacer with >80 g IgG
3. colostrum supplement to be added to low quality colostrum...NOT for use on its own
what are some options for colostrum substitutes

immediately
when does gut permeability of antibiotics begin to decline
1. colostrum at birth
2. milk/milk replacer for weeks 0-6
3. starter (grain mix) introduction at 7 days
4. weaning transition
what is the feeding timeline for calves
>10% BW (15-20% ideal)
how much milk do we try to feed cows roughly...split into two daily feedings
7-10 times daily; 10 L
a calf on a cow will nurse ____ times daily and may ingest ___ L of milk
1. whole milk or waste milk...add milk replacer if needed
2. mastitis milk but MUST PASTEURIZE and avoid in newborn calves dur to bacteria transfer risk
what are some milk sources we can use for calves
1. dairy-based replacer ideal but can use soy-based for older calves
2. mix by weight (NOT VOLUME) using warm water
3. feed 2x daily
what are the considerations for using milk replacer
10% BW
what is the minimum value for feeding milk to calves
conventional
which feeding system for calves involves lower milk intake (saves $$ on milk replacer) and encourages starter intake for growth
accelerated
which feeding system has higher intake of milk and allows faster growth early on...starter intake catches up later
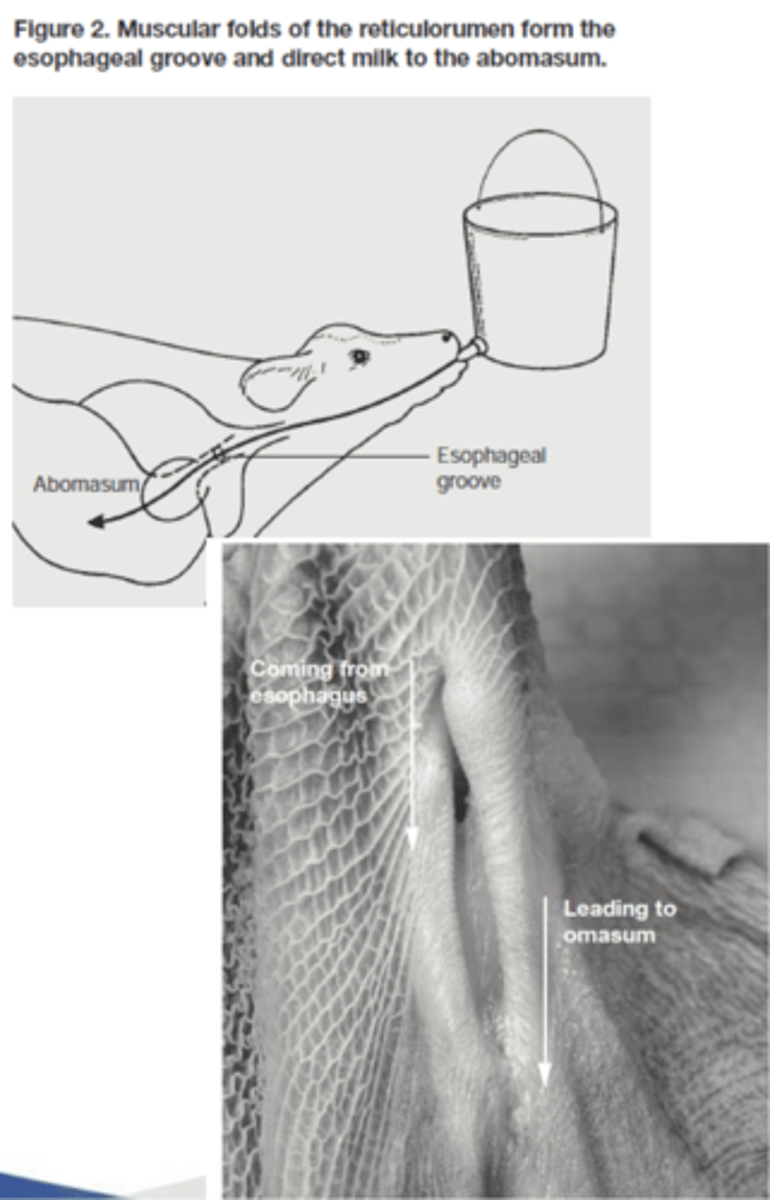
1. allow milk to bypass rumen by connecting cardia region to abomasum
2. fold of reticulum forms groove between esophagus and reticulo-omasal orifice
significance of the esophageal groove
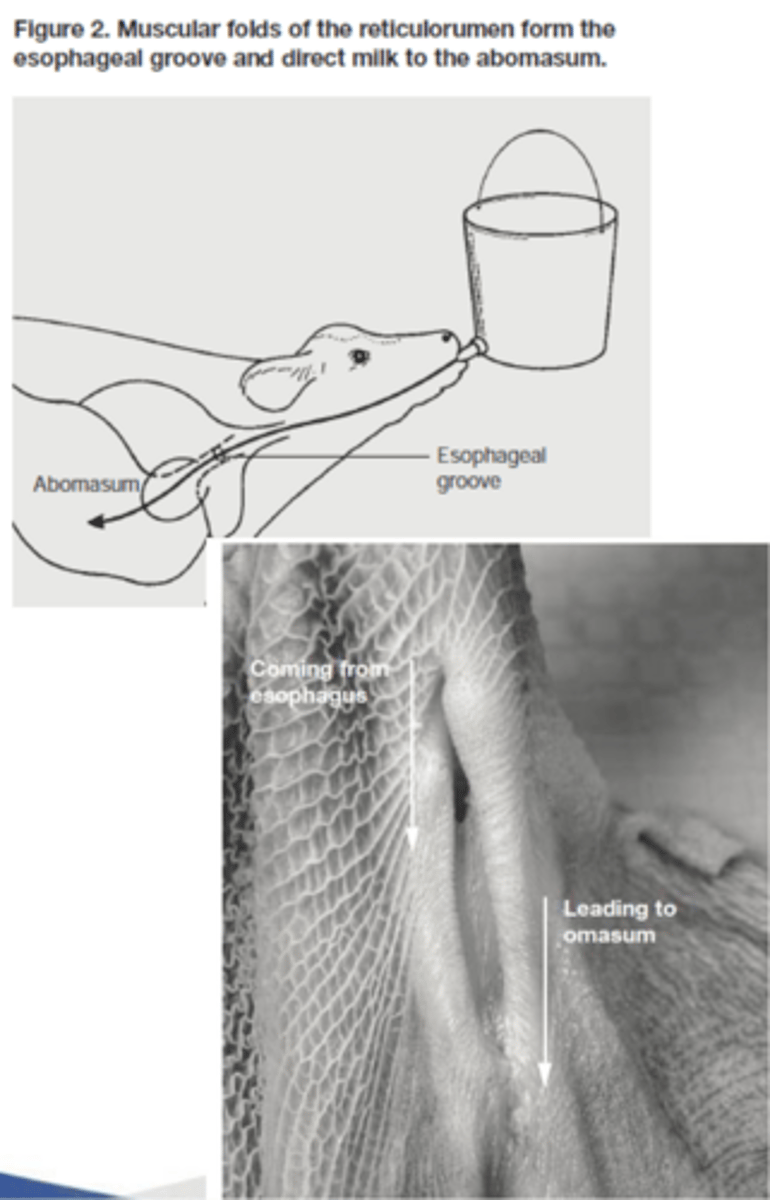
1. allows milk to clot forming casein (protein which is bound to rennin enzyme) and fat
2. whey (water, minerals, lactose, other proteins) goes straight to SI for digestion
what happens to milk when it is digested in the abomasum
starter intake (grain)---> VFA production
what stimulates rumen development
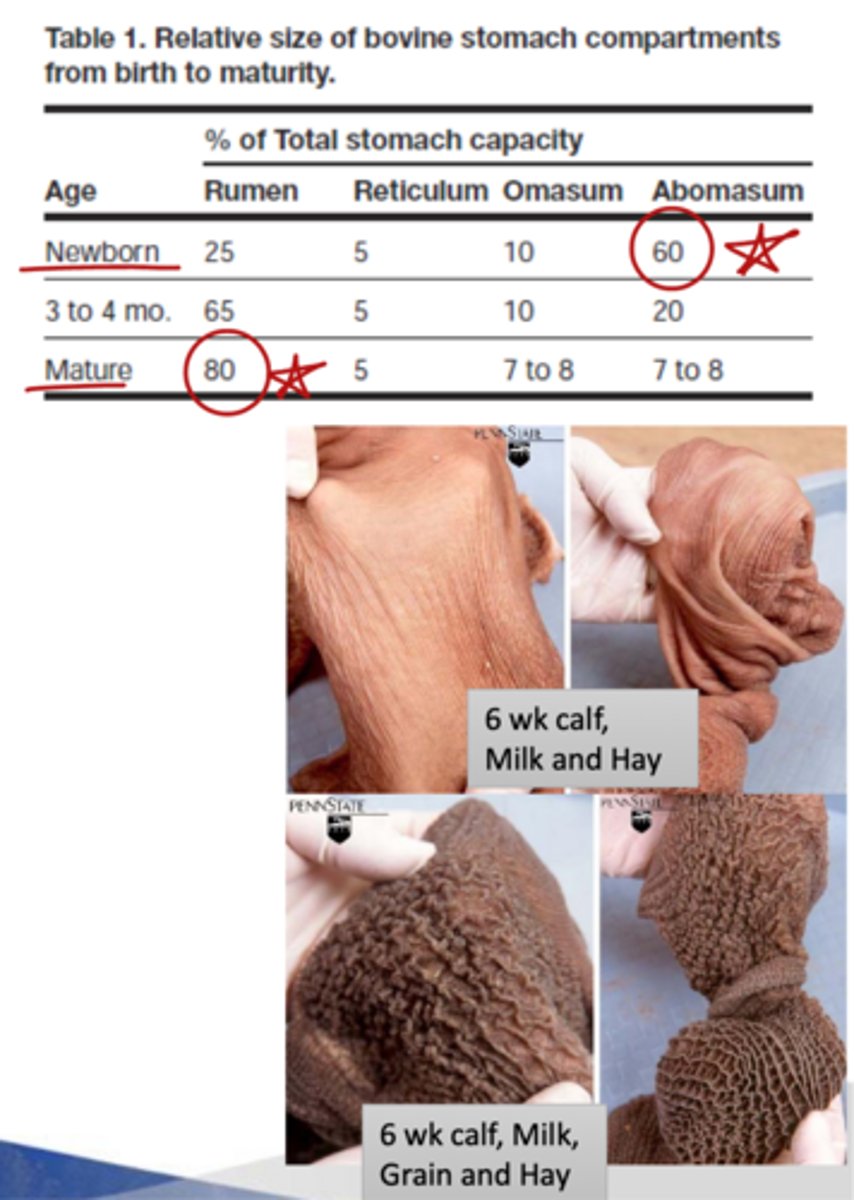
60%
what is the holding capacity of the newborn abomasum
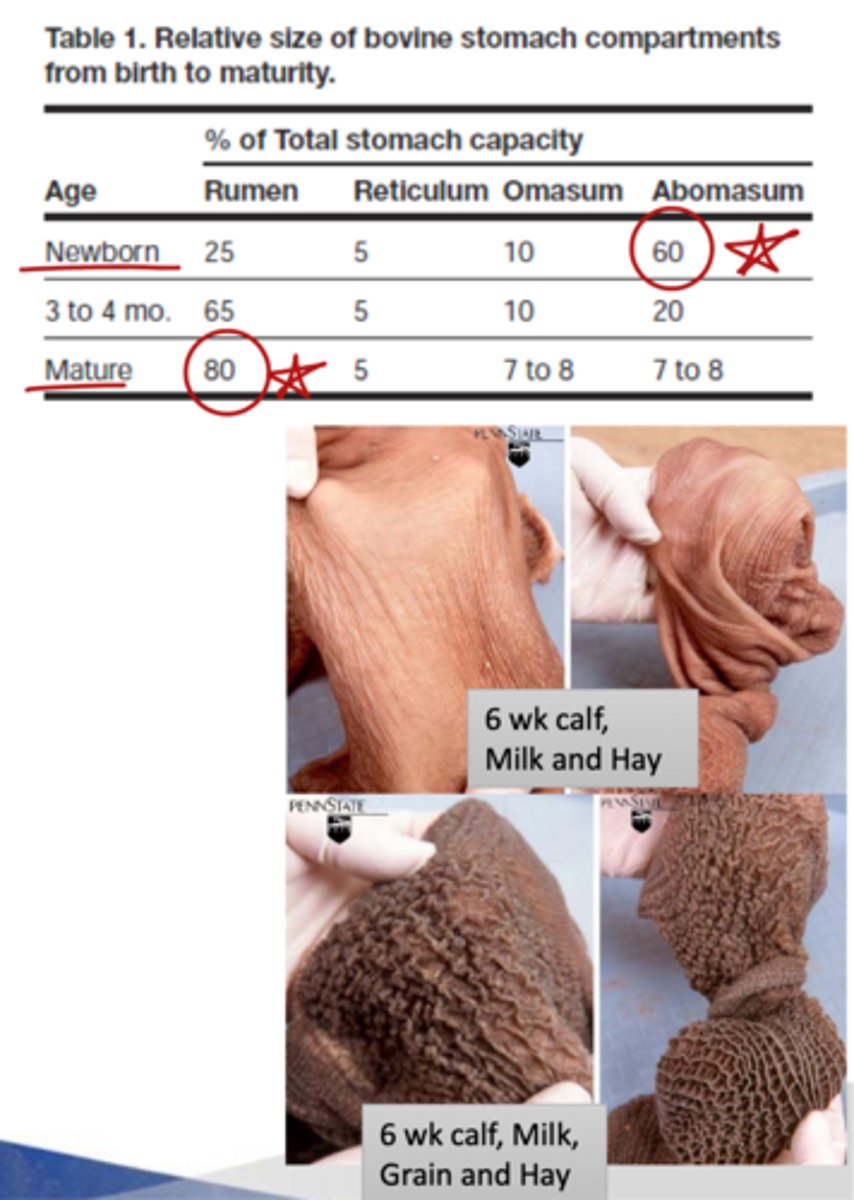
80%
what is the holding capacity of the mature rumen
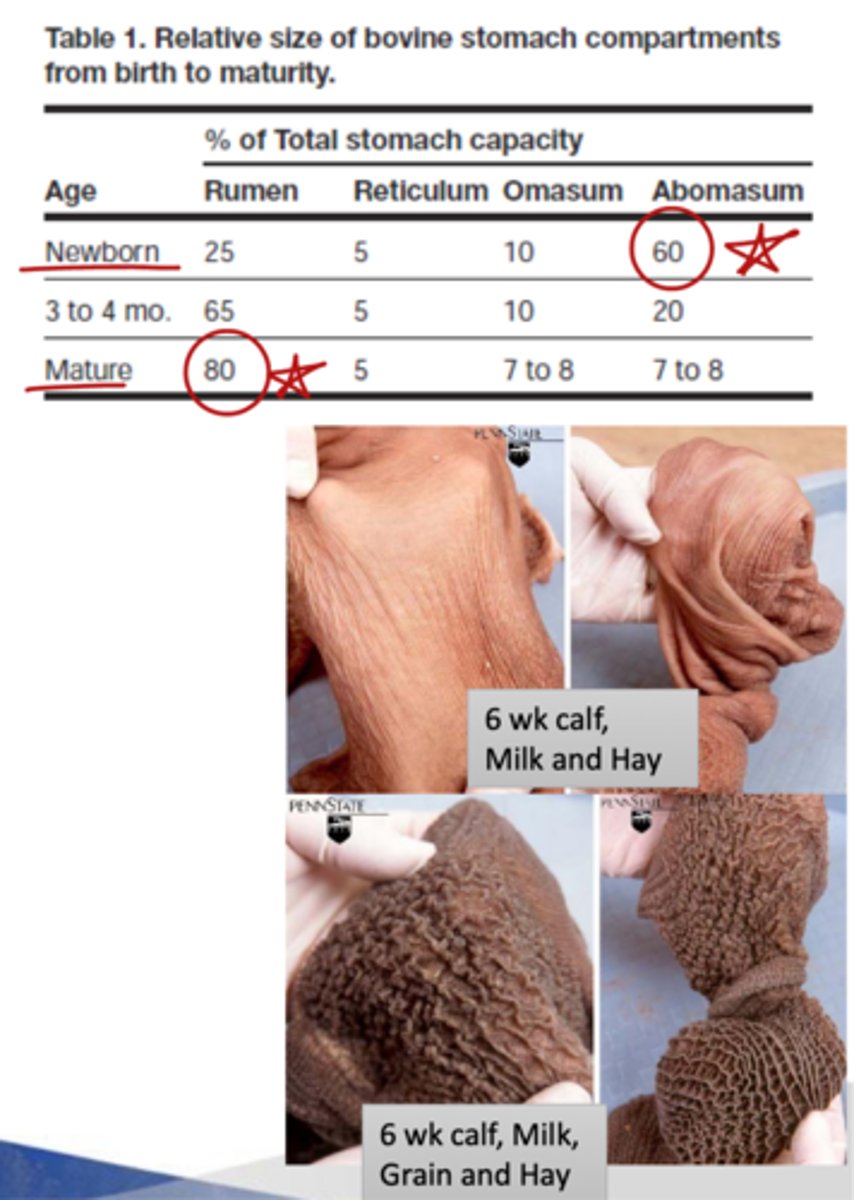
grain
what is more important for rumen dvlp, hay or grain?
after weaning (alfalfa is best)
when is hay introduced into the diet to help reduce non-nutritive suckling
1. cleaning feeding equipment
2. whole/replacer milk should contain <10,000 CFU/mL bacteria and no coliform contamination
3. use gloves and thoroughly wash hands to reduce pathogen transfer
hygiene for calves includes

1. provide free-choice water
2. especially important in sick calves
characteristics of water and dairy calves
1. introduce around 7d
2. pellets, meal, highly palatable, high-quality protein
3. provide small, fresh amounts daily
considerations for starter (grain) feeding
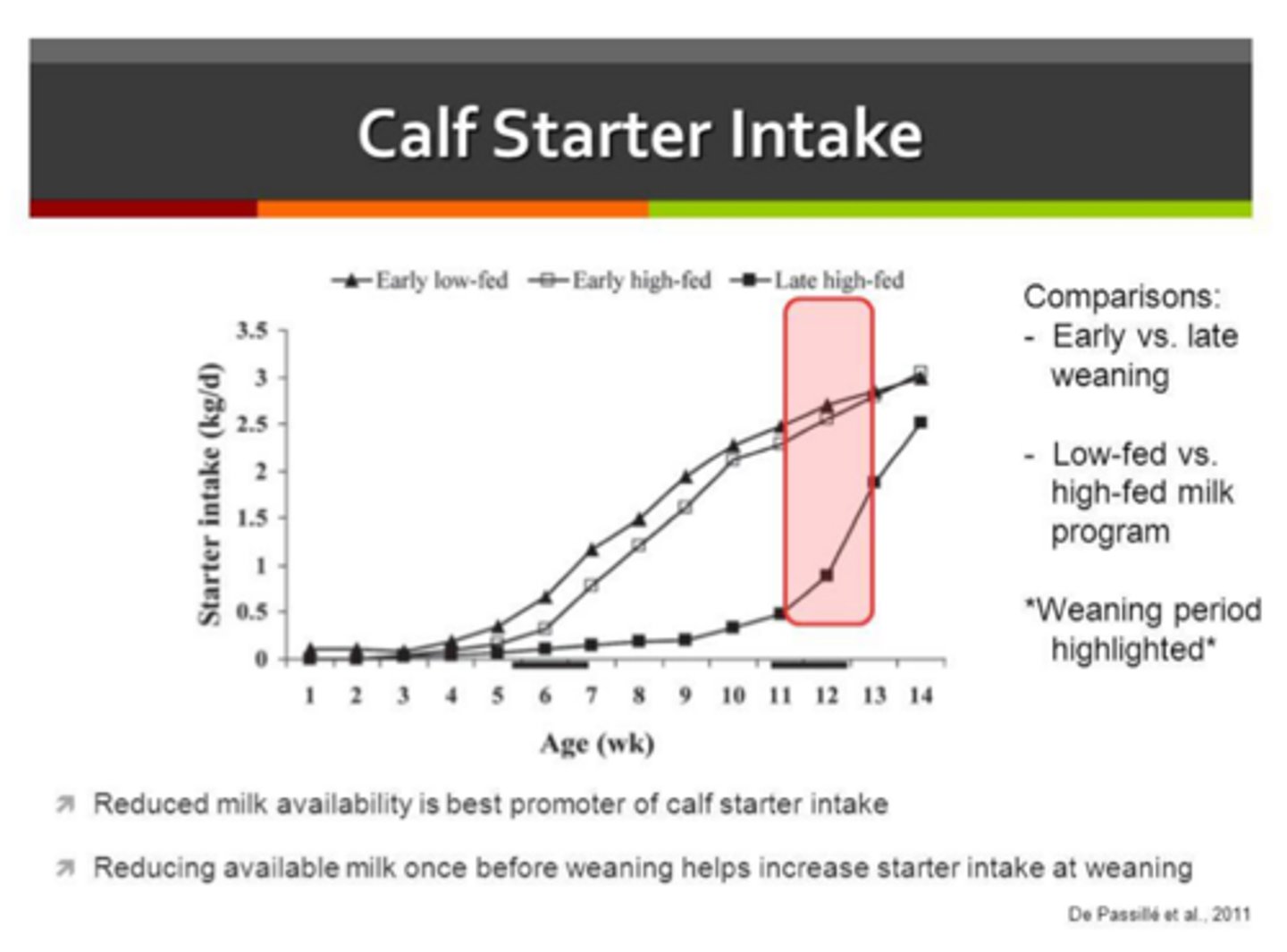
1. infection such as rotavirus, coronavirus, cryptosporidium, coccidia, E. coli, salmonella, clostridium
2. dietary management such as ingesting dirt or sand
what is related to causing calf scours
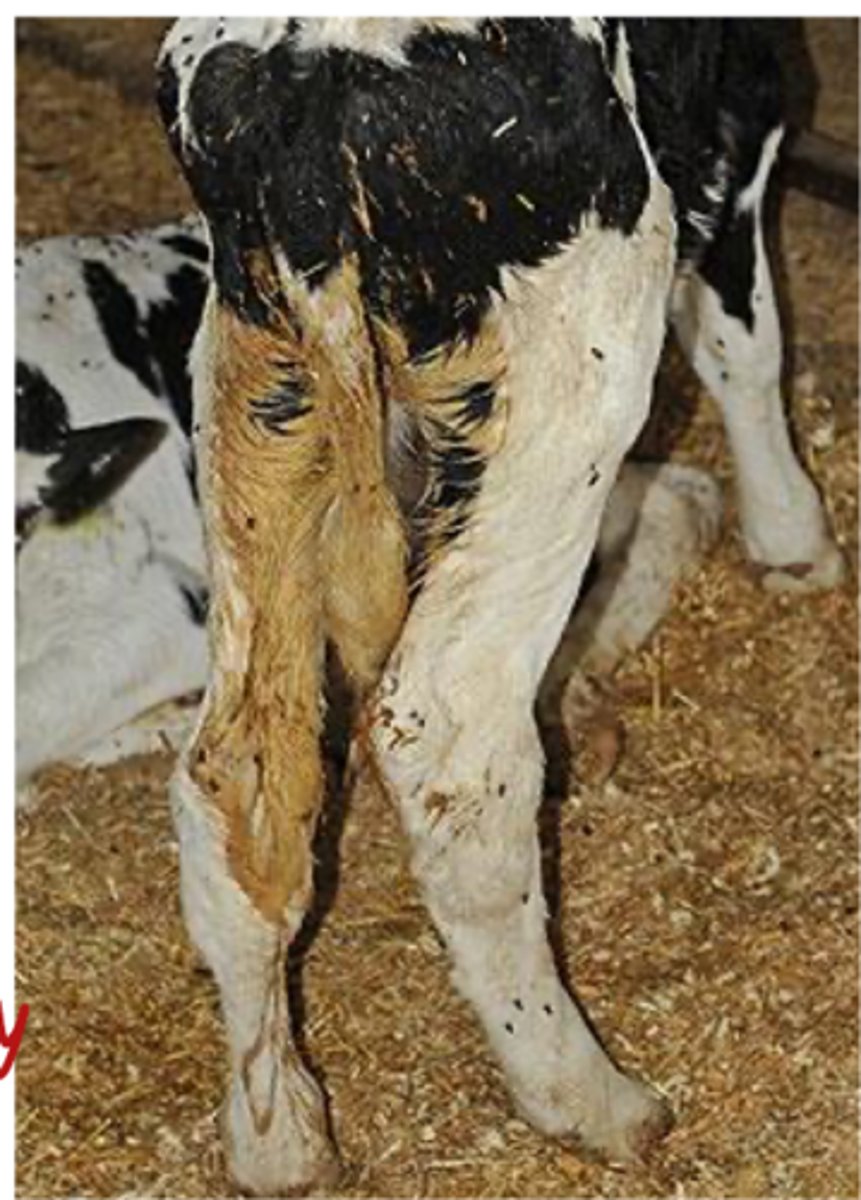
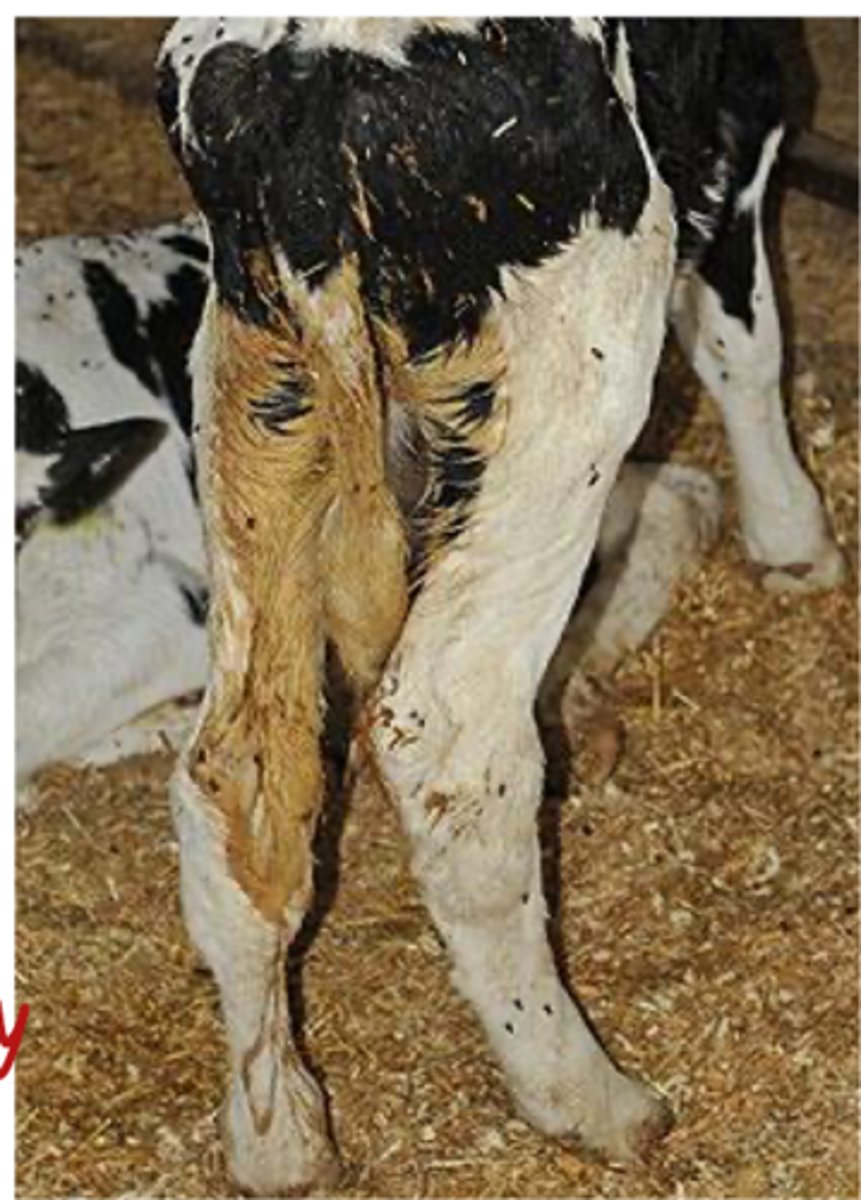
1. loss of H20 and electrolytes
2. inflammation of intestines which leads to loss of nutrient absorption ability and ultimately hypoglycemia
what are the concerns associated with scours
1. poor intake due to poor management or intentional restriction
2. poor milk replacer quality is most common cause
3. lack of fat at necropsy can indicate starvation
characteristics of starvation in calves
eating 2-2.5 lb starter/ d consistently for 3 days
what are important parts of weaning criteria
1. gradually reduce milk and feed 1x/d
2. transition to group housing
3. feed ad libitum starter and hay
what is included in the weaning process
1. colostrum timing is critical
2. failure of passive transfer is common
3. nutrition drives rumen development...particularly grain intake
4. starter intake determines weaning success
what are some key takeaways of dairy calf nutrition