NURS 3070: ADH1: MODULE 4: Gastrointestinal Disorders PRT 2
1/245
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
246 Terms
IBS: Irritable Bowel Syndrome TX (picture)
What is the main goal of IBS treatment?
Symptom relief and lifestyle modification.
What foods should be avoided in IBS treatment?
Gas-triggering foods such as beans, caffeine, corn, wheat, dairy, spicy foods, alcohol, and smoking.
How should constipation be managed in IBS?
Increase fiber intake, drink more fluids, and exercise regularly.
How should diarrhea be managed in IBS?
Use medications and avoid trigger foods.
What general lifestyle changes can help relieve IBS symptoms?
Healthy diet, drinking plenty of water, regular physical activity, massage, and proper medication use.
What non-dietary interventions help improve IBS symptoms?
Stress reduction, adequate sleep, and the use of medications such as antispasmodics, antidepressants, peppermint oil, and probiotics.
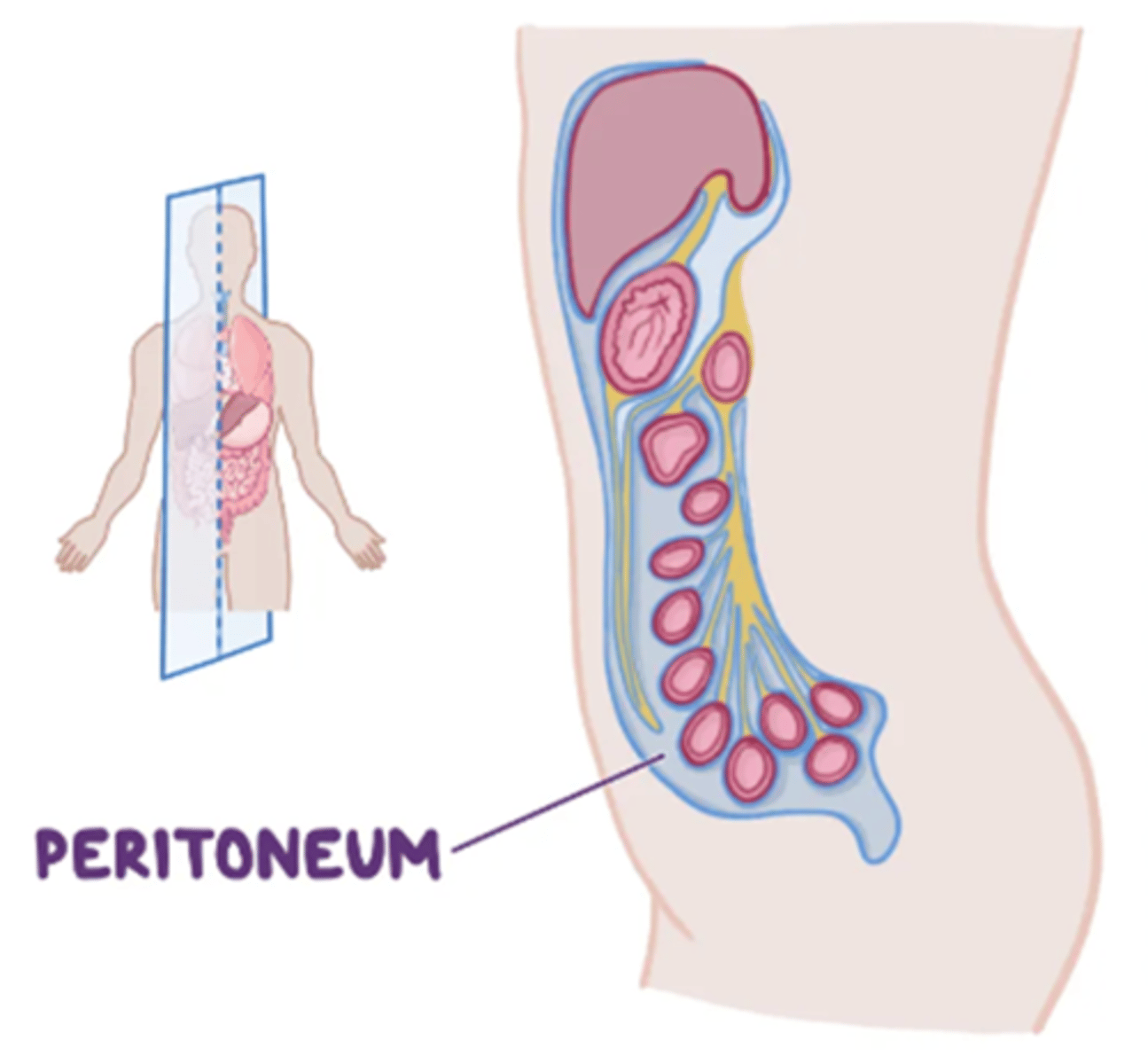
Peritoneum (picture)
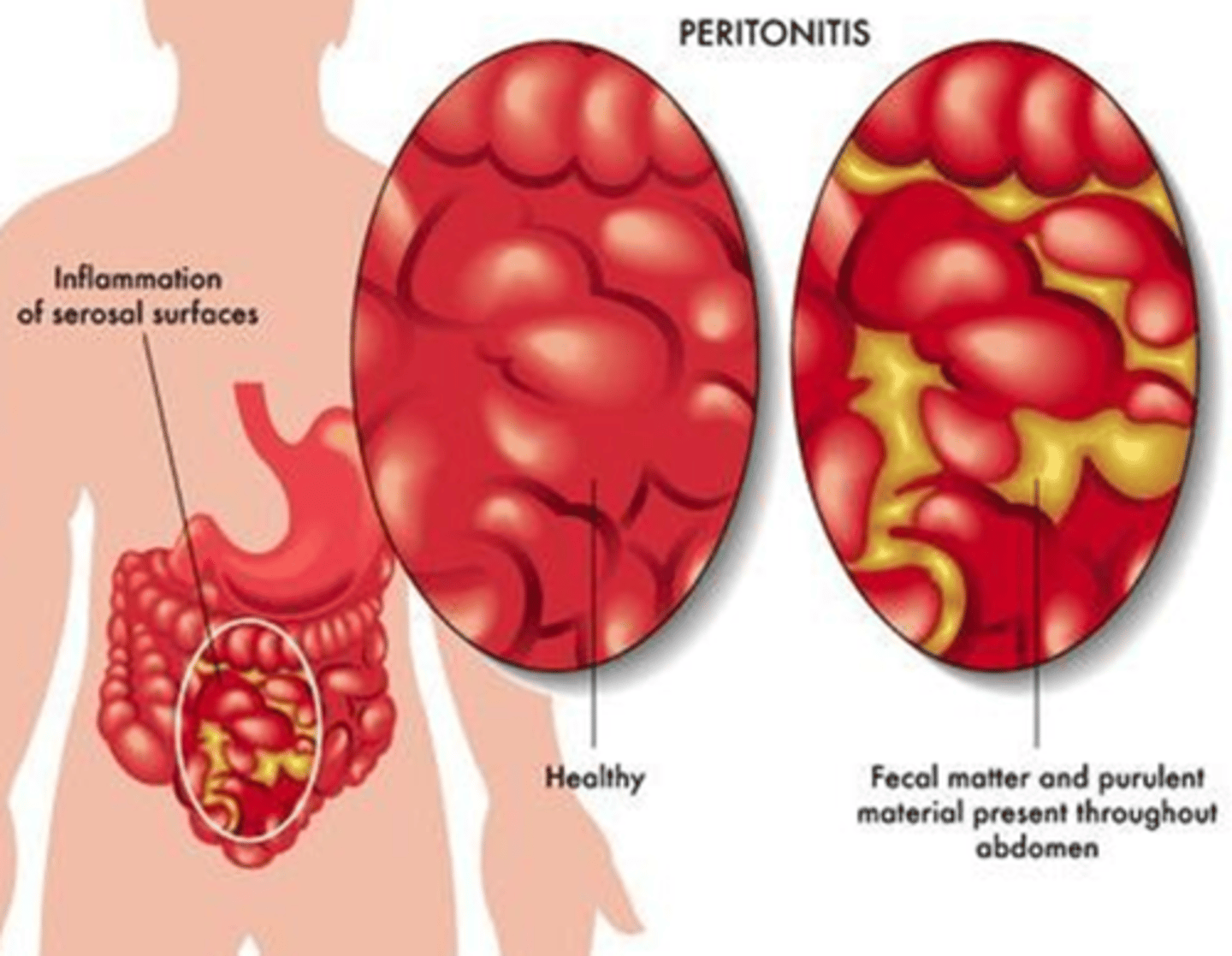
Peritonitis (picture)
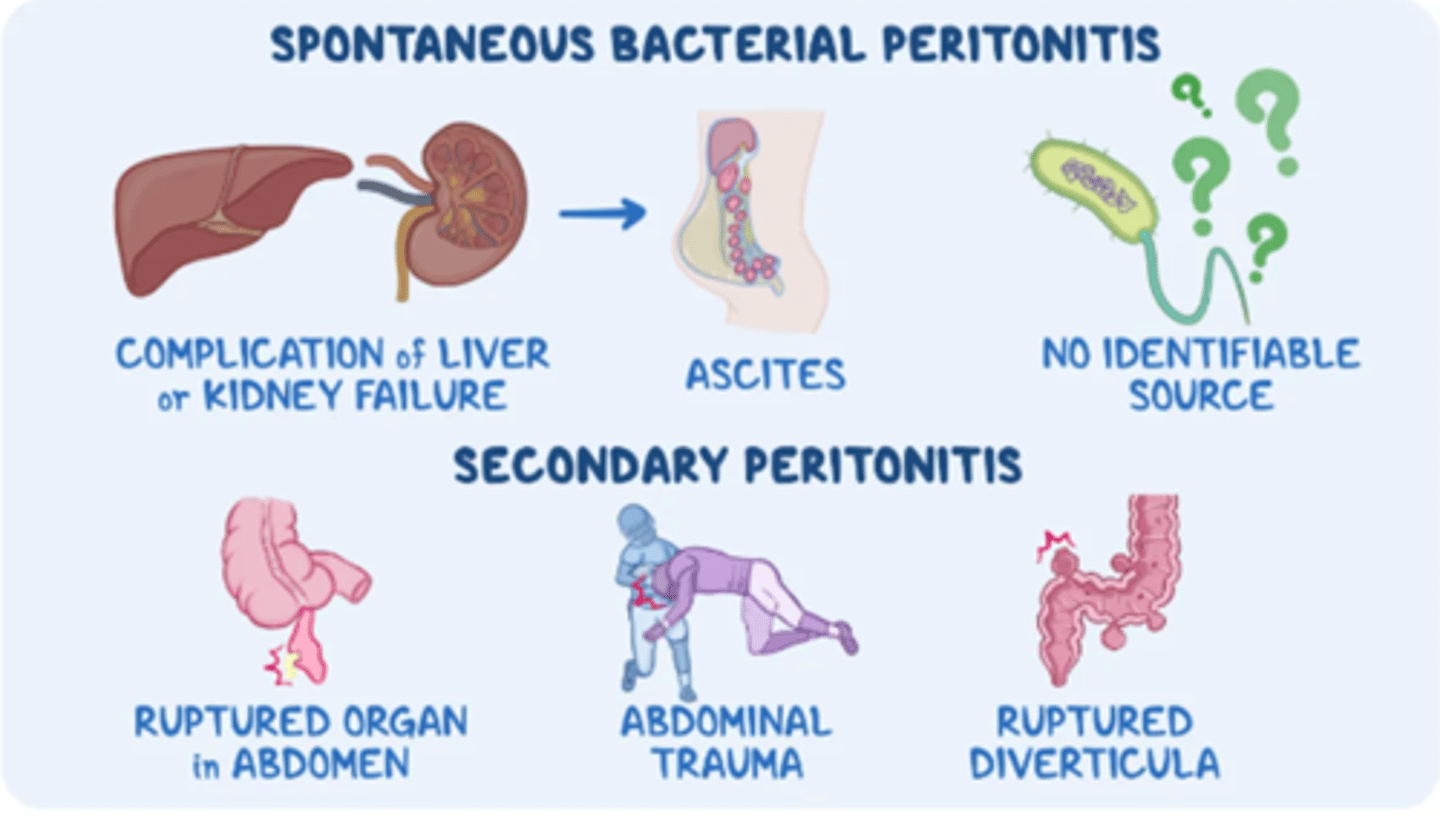
Spontaneous Bacterial Peritonitis and Secondary Peritonitis (picture)
What is peritonitis?
Inflammation of the peritoneum, the serous membrane lining the abdominal cavity and covering abdominal organs.
What is the difference between a healthy peritoneum and one with peritonitis?
A healthy peritoneum is smooth, while peritonitis shows fecal matter and purulent (pus-like) material throughout the abdomen.
What are the two main types of peritonitis?
Spontaneous bacterial peritonitis and secondary peritonitis.
What causes spontaneous bacterial peritonitis (SBP)?
Complications of liver or kidney failure leading to ascites and infection with no identifiable source.
What is a common underlying condition that leads to spontaneous bacterial peritonitis?
Liver failure with ascitic fluid buildup.
What is secondary peritonitis?
Peritonitis caused by the rupture or perforation of abdominal organs, releasing infectious material into the peritoneal cavity.
What are common causes of secondary peritonitis?
Ruptured organ in the abdomen, abdominal trauma, or ruptured diverticula.
What can cause peritonitis due to spillage of infected material?
Perforation of organs such as the appendix or colon.
What are the diagnostic tests used for peritonitis?
CBC, BMP, X-ray, Ultrasound, CT, and MRI.
Why are CBC and BMP performed for peritonitis?
To check for infection, electrolyte imbalance, and kidney function changes.
What does an X-ray show in peritonitis?
Air and fluid levels or distended bowel loops indicating perforation or infection.
What findings might an ultrasound reveal in peritonitis?
Abscesses and fluid collections.
What might CT and MRI scans show in peritonitis?
Abscess formation or fluid accumulation.
What are possible complications of peritonitis?
Infected ascitic fluid, ruptured organs, or trauma leading to bacterial infection.
What does ascites represent in relation to peritonitis?
Fluid accumulation in the abdominal cavity.
What are the hallmark abdominal symptoms of peritonitis?
Abdominal pain, rebound tenderness, and guarding.
What systemic symptoms are common with peritonitis?
Fever, chills, nausea, and vomiting.
What happens to the abdomen as peritonitis progresses?
Progressive abdominal distention develops.
What happens to peristalsis in patients with peritonitis?
It becomes diminished.
What are common cardiovascular and respiratory manifestations of peritonitis?
Restlessness, tachycardia, and tachypnea.
What laboratory finding is typically elevated in peritonitis?
White blood cell (WBC) count.
What gastrointestinal changes might occur in peritonitis?
Nausea, vomiting, diarrhea or constipation, and loss of appetite.
What early signs and symptoms may indicate peritonitis?
Abdominal pain, abdominal distention, and low-grade fever.
What are the progressive complications of untreated peritonitis?
Hypotension and septic shock.
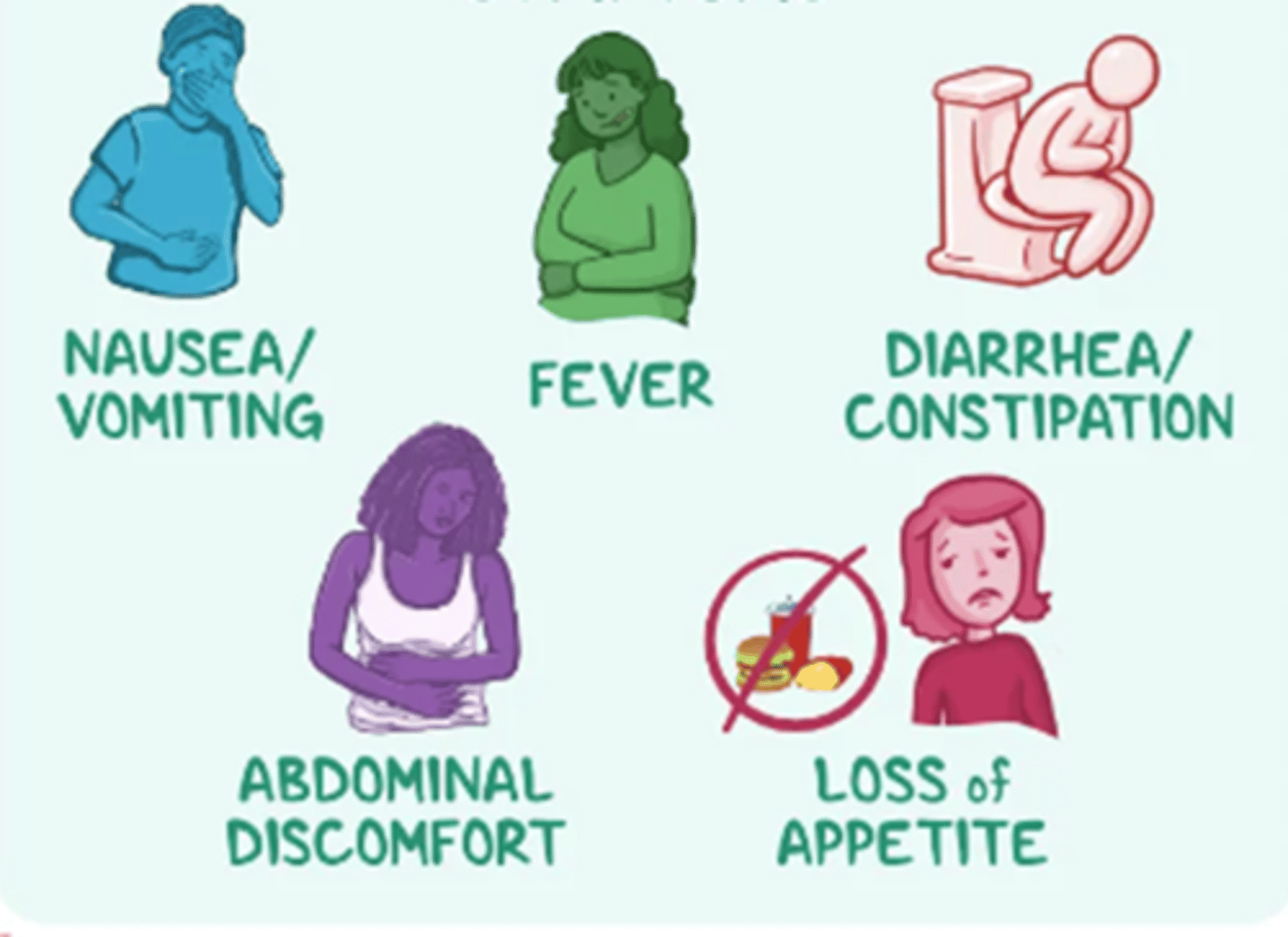
What does the image of the woman holding her abdomen represent?
Abdominal discomfort — a common symptom of peritonitis.
What does 'loss of appetite' indicate in the context of peritonitis?
It's a systemic response to infection and inflammation in the abdomen.
Peritonitis Manifestations (picture)
Abdominal pain, rebound tenderness, guarding
Fever and chills, N/V
Progressive abdominal distention
Diminished peristalsis
Restlessness; tachycardia and tachypnea
Elevated WBC
What is the goal of peritonitis treatment?
Identify the cause or source of infection.
Why is fluid and electrolyte replacement needed in peritonitis?
To restore balance and prevent complications.
What type of medication is given through IV for peritonitis?
IV antibiotics.
What two medication types help manage peritonitis symptoms?
Pain control and antiemetics.
What should be monitored during peritonitis treatment?
Vital signs (VS) and intake/output (I/O).
What can happen if peritonitis treatment is delayed?
It can be fatal.
What life-threatening condition can peritonitis lead to if untreated?
Sepsis or hypovolemic shock.
What procedure may possibly be done as part of treatment for peritonitis?
Paracentesis.
Peritonitis Hot Belly (picture)
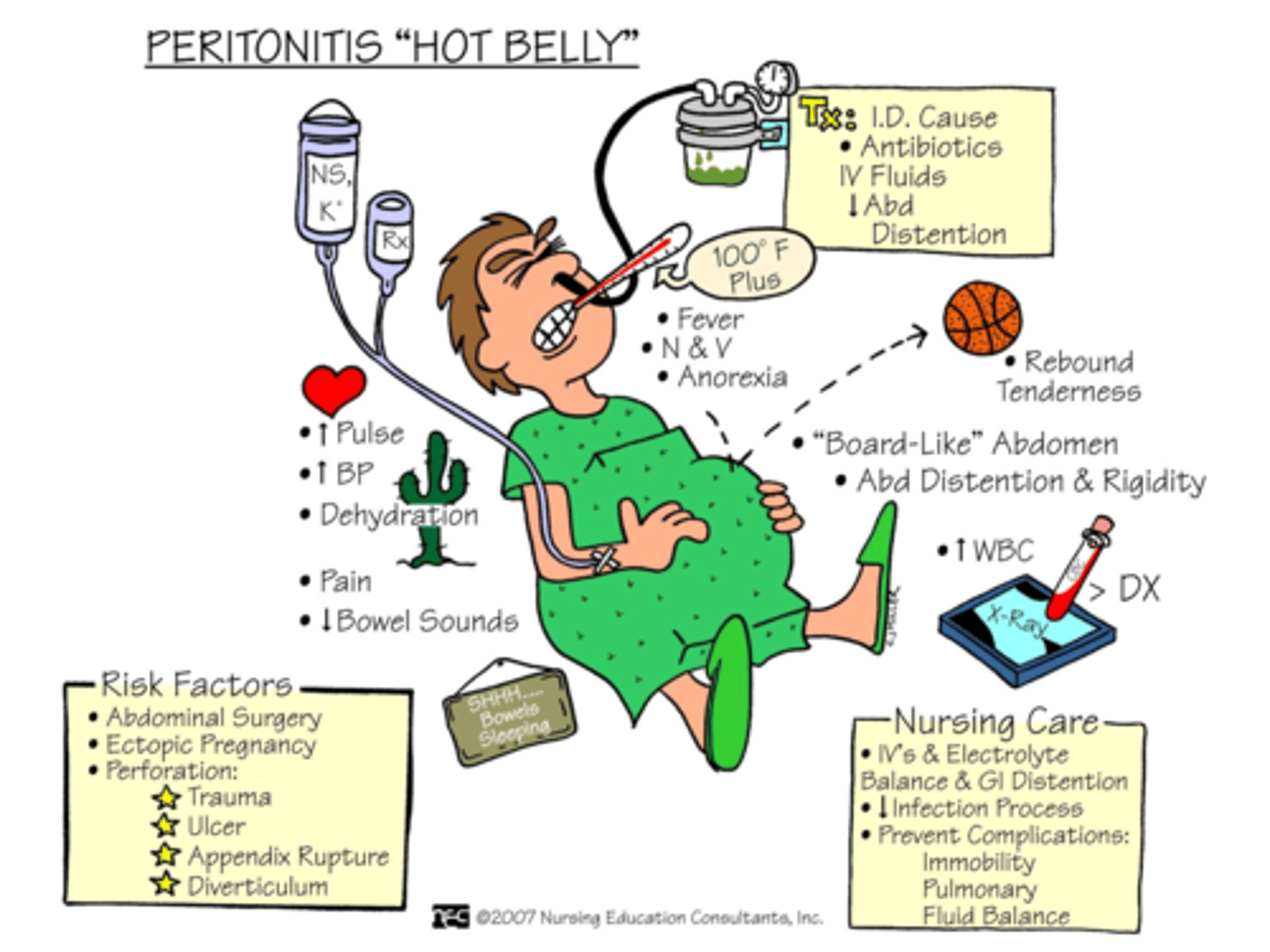
What is another name for peritonitis?
Hot belly.
What vital signs are elevated in peritonitis?
Pulse, blood pressure, and temperature (100°F+).
What symptoms are commonly seen with peritonitis?
Fever, nausea, vomiting, anorexia, pain, rebound tenderness, and abdominal distention.
What type of abdomen is seen in peritonitis?
Board-like abdomen with distention and rigidity.
What bowel sound changes occur with peritonitis?
Bowel sounds are decreased or absent.
What are common risk factors for peritonitis?
Abdominal surgery, ectopic pregnancy, perforation from trauma, ulcer, appendix rupture, or diverticulum.
What are the diagnostic indicators for peritonitis?
Elevated WBC and findings on X-ray.
What does peritonitis treatment focus on?
Identifying the cause, giving antibiotics, IV fluids, and reducing abdominal distention.
What are key nursing care priorities for peritonitis?
IVs and electrolyte balance, decrease GI distention, manage infection process, prevent complications like immobility, pulmonary issues, and fluid imbalance.
What are the early vital sign changes seen with peritonitis?
Tachycardia, fever (febrile), and hypertension.
What are the progressive signs of worsening peritonitis?
Hypotension and sepsis.
What is rebound tenderness?
Pain that occurs when pressure on the abdomen is quickly released (not when pressed down).
What does rebound tenderness indicate clinically?
It is a classic sign of peritoneal irritation, often seen in appendicitis.
In early appendicitis, where is the pain usually located?
Near the umbilicus (belly button).
As appendicitis progresses, where does the pain shift?
To the right lower quadrant (RLQ) at McBurney's point.
What happens to the pain in the late stages of appendicitis?
It becomes constant and severe, indicating possible perforation and peritonitis.
What are the manifestations of peritonitis (including picture symptoms)?
Abdominal pain, rebound tenderness, and guarding
Fever and chills
Nausea and vomiting
Diarrhea or constipation
Abdominal discomfort and progressive distention
Loss of appetite
Diminished peristalsis
Restlessness
Tachycardia and tachypnea
Elevated WBC
(Early: abdominal pain, distention, low-grade fever; Progressive: hypotension, septic shock)
Inflamed Appendix (picture)
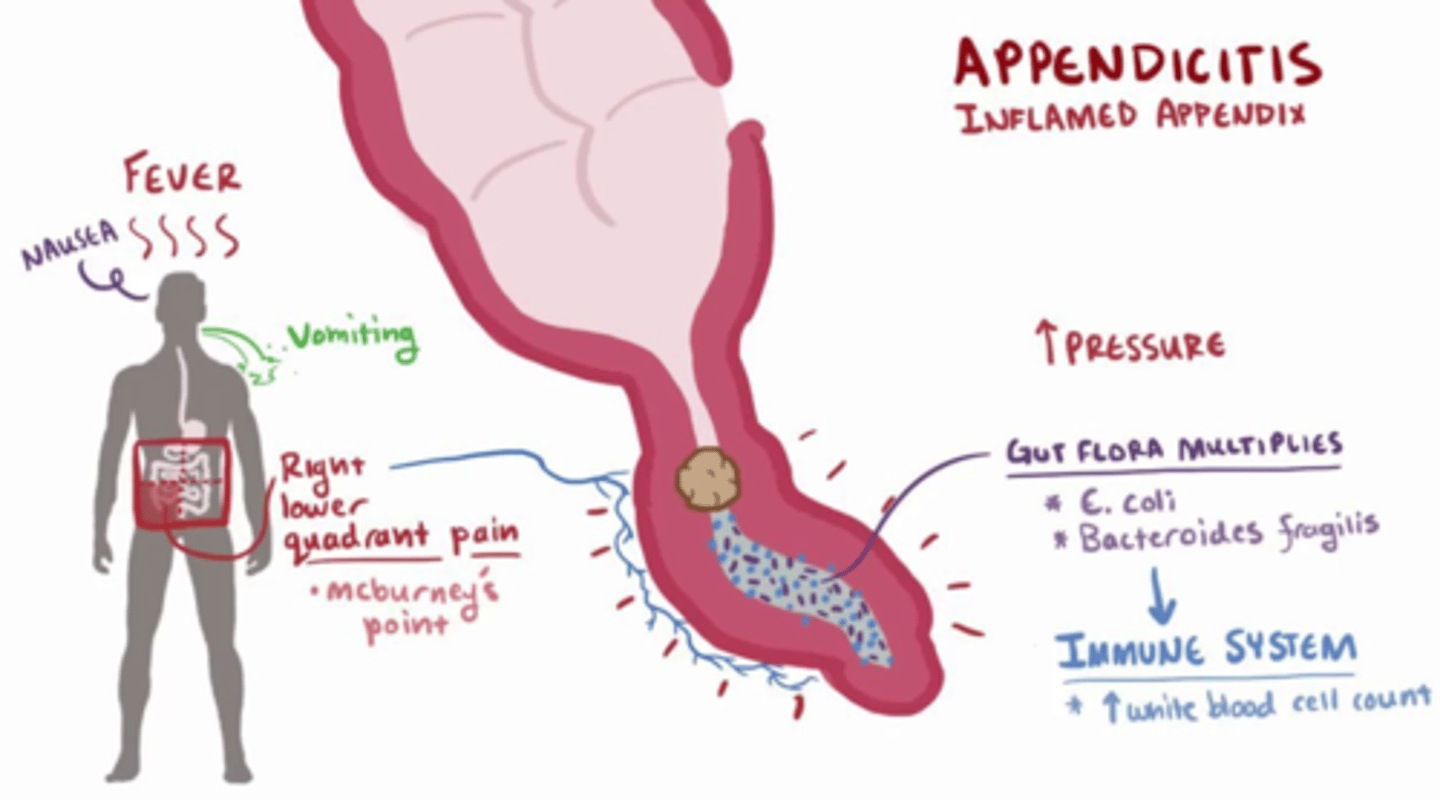
Appendicitis (picture)
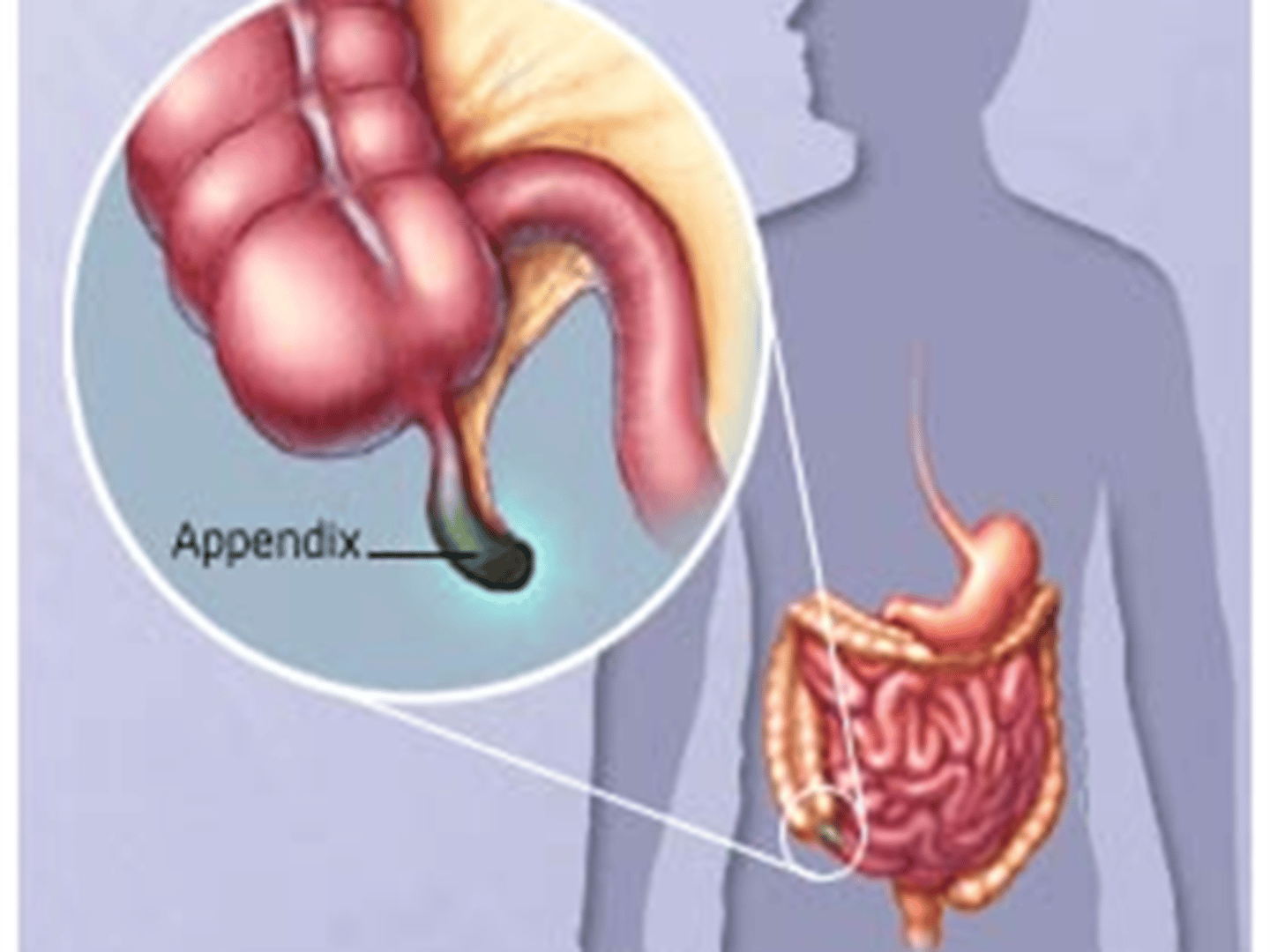
What is appendicitis?
Inflammation of the appendix.
What is the most frequent cause of abdominal pain requiring emergency abdominal surgery?
Appendicitis (10-30% of emergency abdominal surgeries).
What diagnostic tests are used for appendicitis?
Complete history and physical, CBC, CT scan, pregnancy test, and urinalysis.
Which diagnostic test is the number one priority to confirm appendicitis?
CT scan.
What laboratory finding supports appendicitis?
Elevated white blood cell count.
What bacteria commonly multiply in appendicitis?
E. coli and Bacteroides fragilis.
What is the immune system's response during appendicitis?
Increased white blood cell count.
What are common symptoms of appendicitis?
Fever, nausea, vomiting, and right lower quadrant (RLQ) pain.
What is the name of the specific location of pain in appendicitis?
McBurney's point (right lower quadrant).
What causes the pain in appendicitis?
Increased pressure and inflammation in the appendix.
Appendicitis Clinical Manifestations (picture)
McBurney's point (picture)
What is the first symptom of appendicitis?
Dull periumbilical pain followed by anorexia (loss of appetite).
What gastrointestinal symptoms commonly occur with appendicitis?
Nausea and vomiting.
As appendicitis progresses, where does the pain shift?
To the right lower quadrant (RLQ).
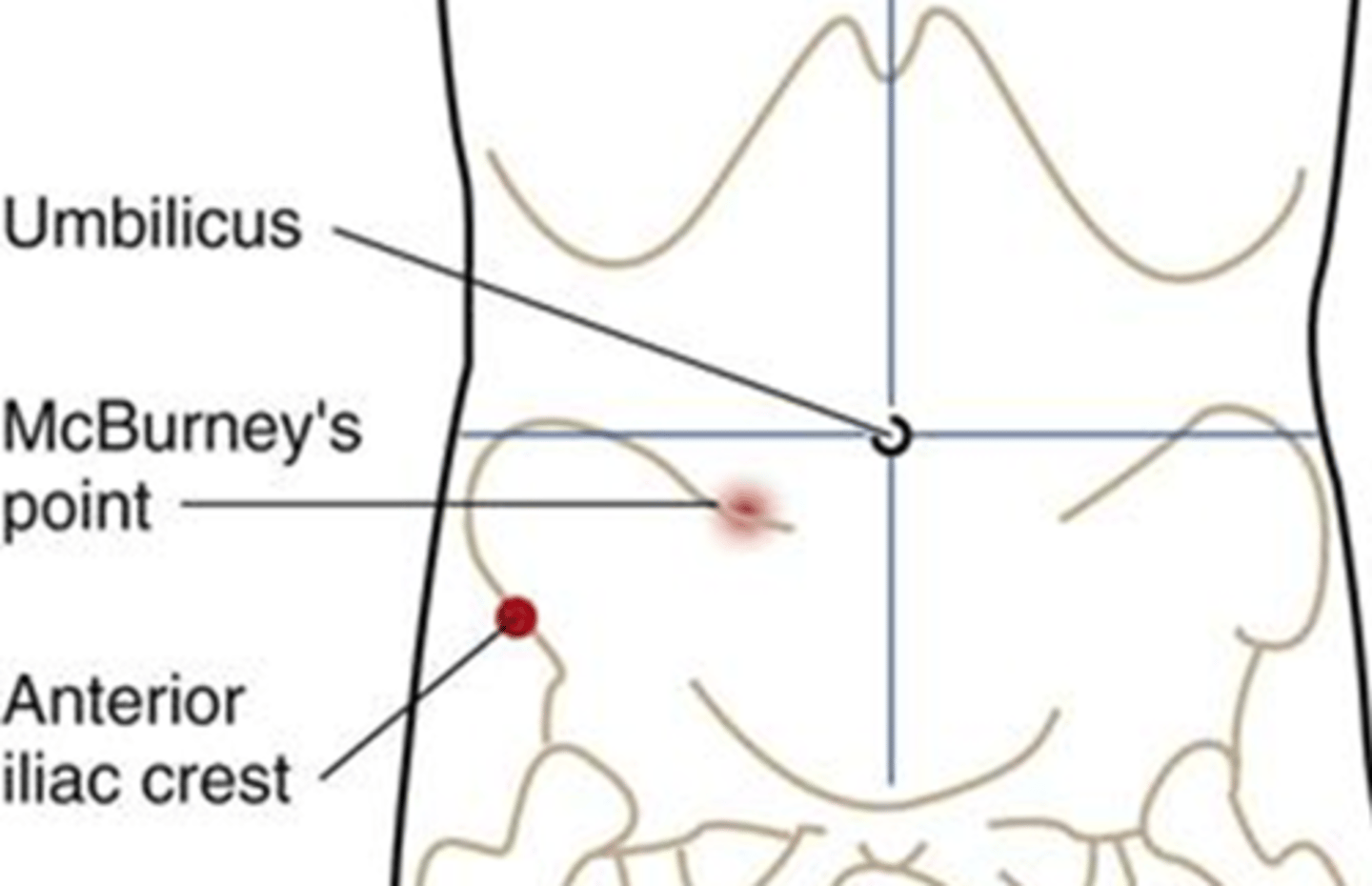
What is McBurney's point?
It is located 1/3 of the distance from the anterior superior iliac spine to the umbilicus.
What physical findings occur with appendicitis?
Rigidity and rebound tenderness with the patient preferring to lie still.
How do patients with appendicitis often position themselves for comfort?
With the right leg flexed (fetal position).
What happens if the appendix ruptures?
The patient may feel temporary relief at first, followed by consistent pain due to peritonitis.
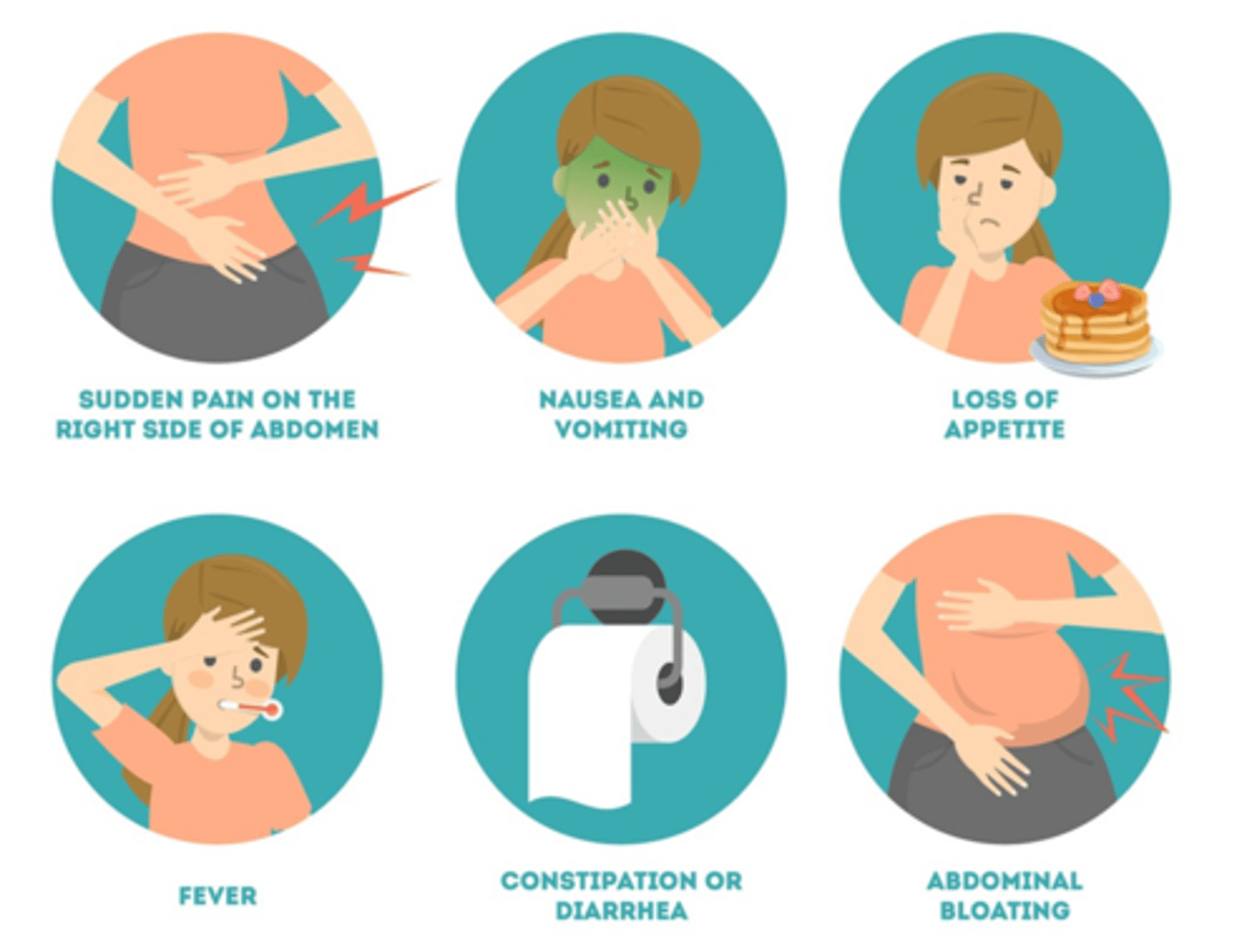
What are common visual symptoms shown in appendicitis?
Sudden pain on the right side of the abdomen, nausea and vomiting, loss of appetite, fever, constipation or diarrhea, abdominal bloating.
What are ALL of the clinical manifestations of appendicitis?
Dull periumbilical pain followed by anorexia (loss of appetite)
Nausea and vomiting
Pain that shifts to the right lower quadrant (RLQ)
Tenderness at McBurney's point (1/3 of the distance from the anterior superior iliac spine to the umbilicus)
Abdominal rigidity and rebound tenderness
Patient prefers to lie still, often with the right leg flexed (fetal position)
Fever
Constipation or diarrhea
Abdominal bloating
If rupture occurs: temporary pain relief followed by severe, consistent pain from peritonitis
What surgical procedure is performed to treat appendicitis?
Appendectomy.
What happens if the appendix ruptures?
The patient is at risk for peritonitis and infection; emergency treatment and antibiotics are required.
What therapies are included in the treatment of appendicitis?
Fluid and antibiotic therapy.
What vital signs should be monitored in a patient with appendicitis?
Temperature, heart rate, blood pressure, respiratory rate, and oxygen saturation (VS).
What medications are commonly used for appendicitis management?
Analgesics for pain and antiemetics for nausea and vomiting.
What are the main components of nursing management after an appendectomy?
Pain management, postoperative care, and ambulation.
How long does it usually take for an appendix to perforate if untreated?
Within 4-6 hours.
What are 'little lap sights' in an appendectomy?
Small laparoscopic incisions made to remove the appendix.
What should nurses assess for with a chest X-ray after appendectomy?
Atelectasis or a surgical site infection.
How does positioning help after appendectomy surgery?
High Fowler's position decreases abdominal pressure and strain on the incision.
How can nurses help patients reduce pain after surgery?
Teach splinting techniques and encourage ambulation.
Appendicitis (picture)
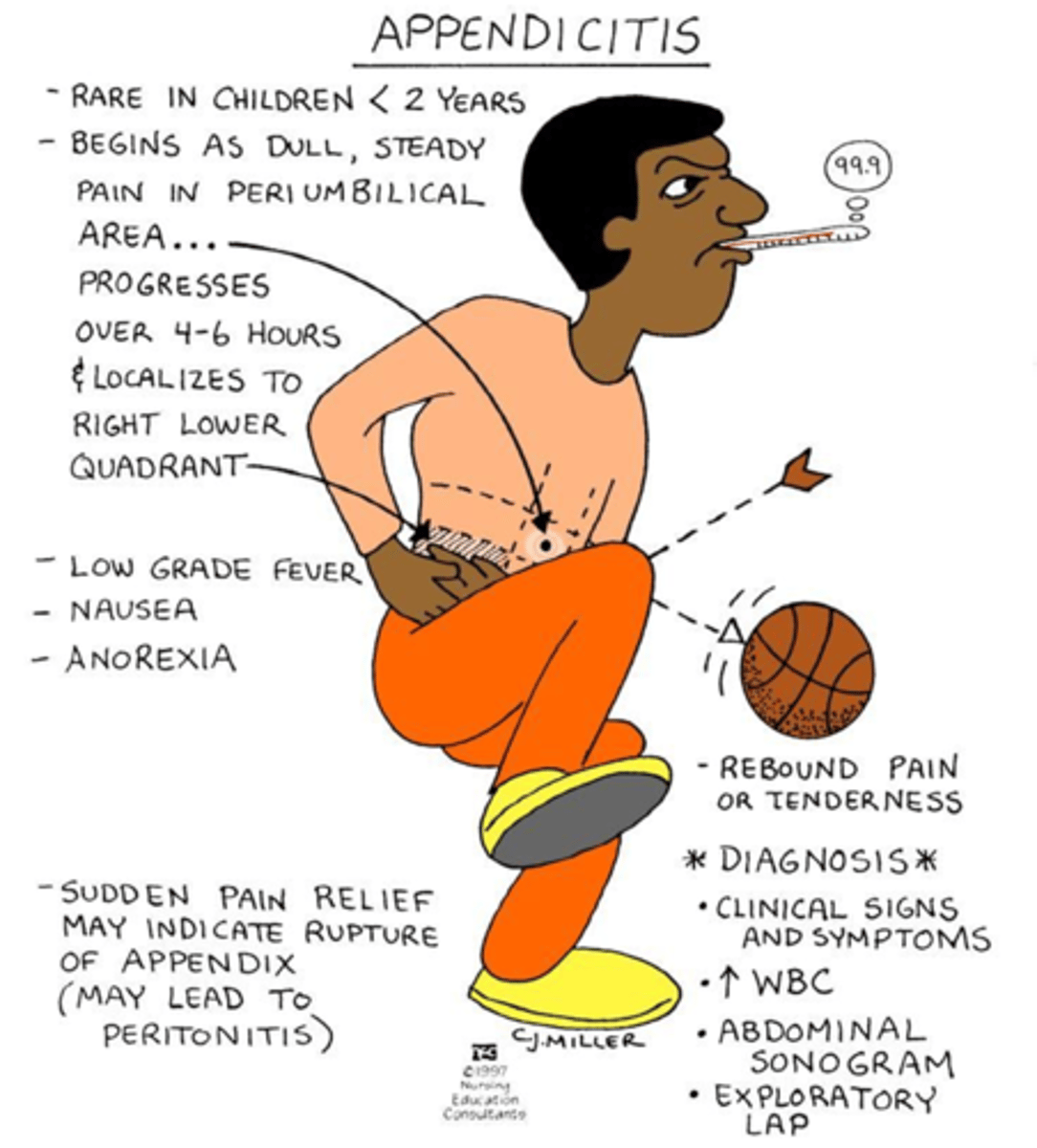
How common is appendicitis in children under 2 years old?
It is rare in children under 2 years old.
Where does the pain from appendicitis begin?
It begins as dull, steady pain in the periumbilical area.