Lec 19 - Anesthetic Monitoring pt I
1/58
Earn XP
Description and Tags
Dr. Castro - Exam 2
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
59 Terms
What is crucial to assess before perfoming anesthesia in a patient?
physical status
What group created the 5 classifications of patient physical status?
America Society of Anesthesiologists (ASA)
Which patients fall under ASA I?
normal healthy patients
Which patients fall under ASA II?
patients with mild systemic disease that does NOT limit normal function (murmur w no clinical signs)
Which patients fall under ASA III?
patients with moderate systemic disease that limits normal function (CKD, DM)
Which patients fall under ASA IV?
patients wiht severe systemic disease that is a constant threat to life (GDV, hemoabdomen)
Which patients fall under ASA V?
patients that are moribund and not expected to live 24 hours without surgery
What does the letter “E” following an ASA classification denote?
“emergency” → ASA IVE (resp distress)
What does the ASA define general anesthesia as?
“drug-induced loss of consciousness which patients are not arousable, even by painful stimulation”
What are the goals of successful general anesthesia?
reversible unconsciousness
amnesia
analgesia
skeletal muscle relaxation (immobility)
autonomic stability (maintain physiologic homestasis)
Why must we carefully monitor a patient receiving anesthesia?
anesthesia disrupts hemostasis
What systems does anesthetic drugs depress?
CNS
cardiovascular
respiratory
others
T/F: Monitoring helps us to make anesthesia as safe as possible achieving the best patient care.
TRUE
T/F: There are several solitary measurements we can rely soley on when monitoring a patient under anesthesia.
FALSE — no single measurement → multiple parameters need to be investigated simultaneously
What are some questions you should ask yourself when monitoring an anesthetized patient?
is the heart rate and rhythm satisfactory?
is contractility satisfactory?
are SV, CO, BP, vasomotor tone, tissue perfusion adequate?
how is the animal ventilating?
how is the animal’s oxygenation?
When do we monitor an anesthetized patient?
ALWAYS
There is no single value that can truly assess the patient. We need to evaluate what instead?
the TRENDS
What are the most common anesthetic complications?
“3 H’s” = hypotension, hypoventilation, hypothermia
bradycardia
pain/nociception
How do we as vets use our human senses to assess our anesthetized patients?
assessment of depth of anesthesia (sight)
palpation of peripheral pulses (touch)
detection of leaks when using volatile anesthetics (smell)
auscultation of heart & lung sounds (hearing)
What is clinically meant by “depth of anesthesia?”
observed as the extent to which a general anesthetic agent depresses the CNS, with primary focus on the cortex
What is the objective of monitoring depth of anesthesia?
prevent patient awareness
prevent movement (maintain depth)
minimize cardiorespiratory & other physiological side effects of anesthetics
When assessing depth of anesthesia, you must monitor which motor and autonomic reflexes associated with the eye?
eye reflexes (palpebral, corneal, PLR)
eye position in ruminants, dogs, & cats (motor)
lacrimation
nystagmus
When assessing depth of anesthesia, you must monitor which motor reflexes?
pedal (withdrawl) reflex → SA
anal sphincter tone/relfex → LA
auricular reflex (ear flick)
spontaneous movement of extremities (limbs or neck)
When assessing depth of anesthesia, you must monitor which autonomic reflexes?
respiratory rate
heart rate
arterial blood pressure
Guedel’s classic physical signs are used to assess what?
depth of anesthesia
How many stages of anesthetic depth are there?
4 → stage I-IV
Which stage of anesthetic depth do we aim to avoid by using premeds?
stage II
What is stage I of anesthetic depth?
stage of voluntary movement and loss of consciousness
What is stage II of anesthetic depth?
stage of involuntary excitement
What is stage III of anesthetic depth? What are the additional planes associated with this stage?
stage of surgical anesthesia
planes I, II, & III
What is stage IV of anesthetic depth?
stage of anesthetic overdose → death!
Explain what signs are observed during stage I.
fear (pre-med to sedate/remove anxiety)
increase in HR, RR, & BP from epinephrine release
pupillary dilation
SLUD signs
Explain what signs are observed during stage II.
reflex becomes more primitive and exaggerated
hyperventilation
catecholamine release (inc HR, BP, arrhythmias)
SLUD
laryngospasm (pigs & cats)
Explain what signs are observed during stage III.
unconsciousness w progressive depression of reflexes
cessation of spontaneous movement
muscle relaxation
ventilation slow and regular
loss of swallowing reflex (intubate)
no movement in response to surgical stimulus
What are the 3 planes of the surgical stage of anesthesia (stage III)?
plane I = light
plane II = medium (ideal)
plane III = deep
What will the eye position of a dog or cat look like at stage III, plane II of anesthesia?
rotate to a ventral medial position
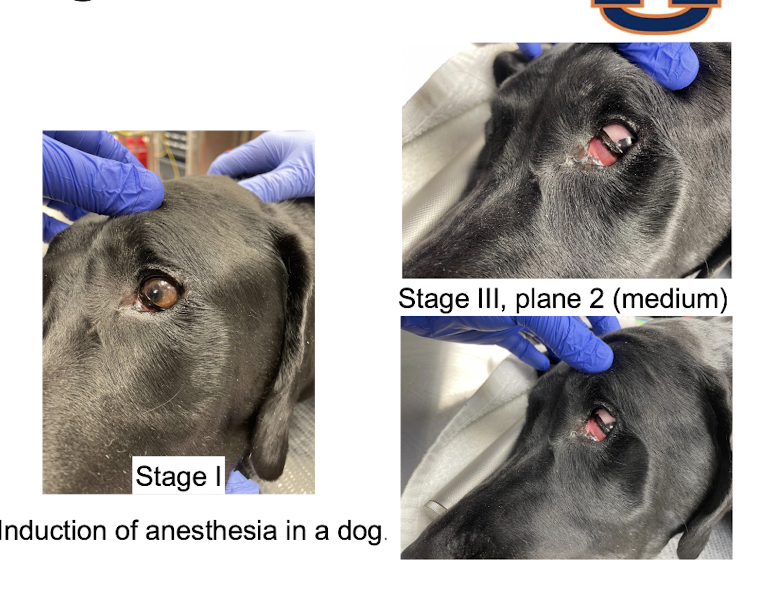
What will the eye position of a horse look like at stage III, plane II of anesthesia?
will remain centrally oriented
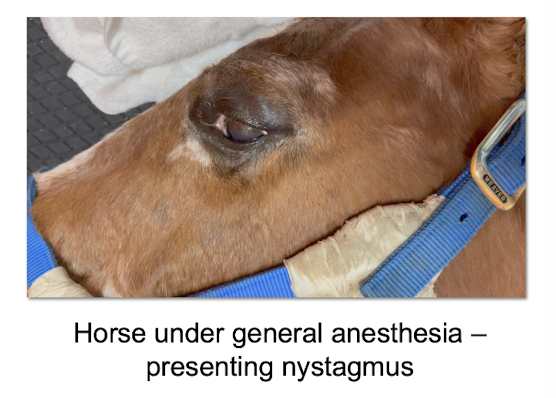
What will the eye position of a ruminant look like at stage III, plane II of anesthesia?
may rotate ventrally
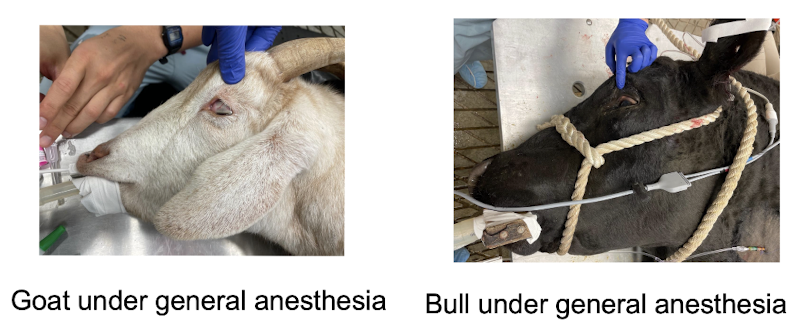
Explain what signs are observed during stage IV.
extreme CNS depression/overdose
corneal reflex absent
eyeball rotate to central position w pupillary dilation
respiratory arrest → cardiovascular collapse
T/F: Rotation of a horse’s eyeball is a reliable way to measure anesthetic depth.
FALSE — not reliable
What signs will a horse exhibit under stage III, plane I anesthesia?
spontaneous nystagmus
lacrimation
increase in muscle tone (neck and anal reflex)
What are the 3 gold standard metrics used to assess anesthetic depth in small animals?
eye position
palpebral reflex
jaw tone
look at the picture for the complete list
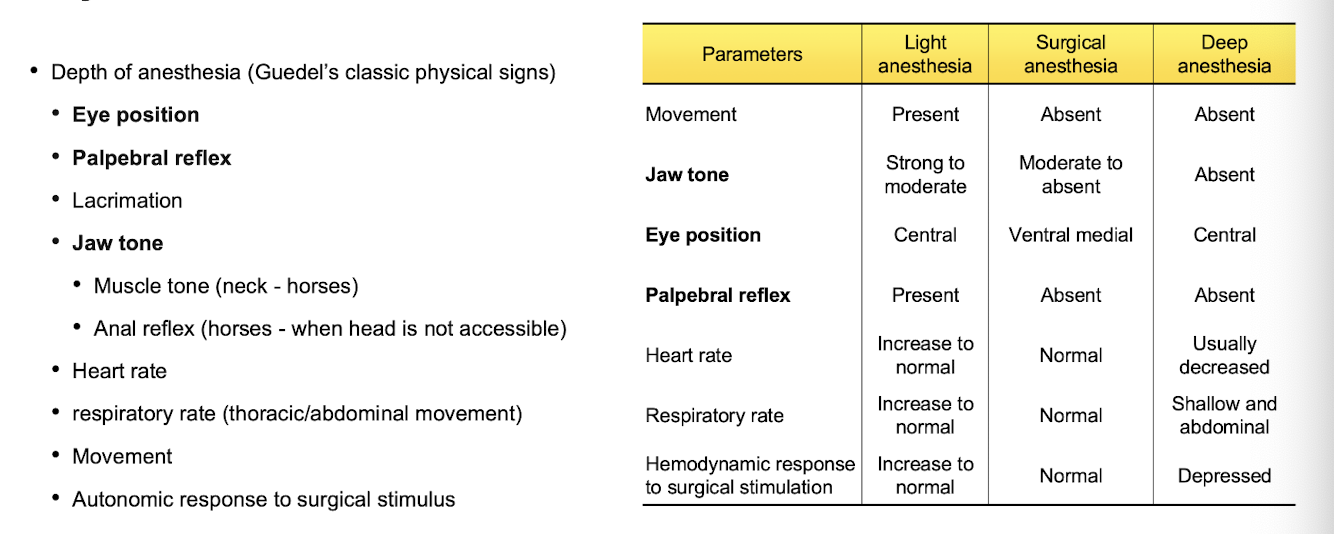
What type of responses do we expect from a patient undergoing anesthesia with volatile agents (iso, sevo)?
eye rotate ventromedially
palpebral reflex become sluggish to absent
relax jaw & body muscle tone
What type of responses do we expect from a patient undergoing anesthesia with injectable dissociative anesthetics?
may NOT follow classic progressive signs
reflex and muscle tone may remain present
What should you consider when evaluating peripheral pulses?
assess rate and quality
strong vs weak (vessel tone)
synchronicity w/ HR
T/F: Peripheral pulse does NOT indicate blood pressure.
TRUE — pulse pressure = systolic arterial pressure (SAP) - diastolic arterial pressure (DAP)
What are the sites of peripheral pulse palpation in dogs?
femoral, dorsal pedal, lingual
What are the sites of peripheral pulse palpation in cats?
femoral, dorsal pedal
What are the sites of peripheral pulse palpation in horses?
facial, auricular, metatarsal
What are the sites of peripheral pulse palpation in ruminants?
facial, auricular, metatarsal
Why should you try to avoid using the lingual artery of a dog for an arterial line?
risk of blowing which would result in swelling and potential blockage of the airway
What are the normal heart rates of small and large dogs?
small = 80-160 bpm
large = 60-120 bpm
What is the normal heart rate of a cat?
120-220 bpm
What is the normal heart rate of a horse?
34-45 bpm
What is the normal heart rate of a small ruminant?
70-90 bpm
What can you use to assess patient respiratory rate during a surgical procedure?
movement of chest or abdomen
resevior bag
What do you look for in terms of perfusion/cardiovascular monitoring under anesthesia?
color of mucous membranes
CRT
blood loss (in case there is need of infusion)
T/F: The higher the ASA status, the higher the anesthetic risk which requires more monitoring and preparation.
TRUE
T/F: Most anesthetic complications are unavoidable and spontaneous.
FALSE — most are predictable, knowing them tells you what to monitor